Measuring Health Vulnerability: An Interdisciplinary Indicator Applied to Mainland Portugal
Abstract
1. Introduction
- ▪
- Social factors determine populations health;
- ▪
- Social determinants of health produce inequalities;
- ▪
- Disadvantaged groups are more vulnerable to disease, die younger and experience worse health conditions;
- ▪
- Plans and actions to fight against health inequalities imply a multidisciplinary approach due to its complexity;
- ▪
- Development of instruments to measure social determinants in health are useful to provide knowledge to design tailored public health policies;
- ▪
- Monitoring is very important; thus, health inequalities diagnosis should not be the goal but the starting point of health plans and policies;
- ▪
- Health policies’ effects should be understood as a way to evaluate effectiveness in reducing inequalities.
2. Materials and Methods
2.1. Study Area
2.2. Model Construction and Data Collection
2.3. SEHVI Formula
- is the standard value of a variable vj for a municipality i;
- is the resident population (number of inhabitants) in a municipality i;
- is the value of a variable vj for a municipality i.
- is the standard value of a variable vj for a municipality i;
- is the geographical area (km2) of a municipality i;
- is the value of a variable vj for a municipality i.
- is the value of the standard individual indicator Ij for the municipality i in a certain year;
- is the value of the indicator Ij for Portugal (mean value for the country) for a certain year;
- is the normalized value of the indicator Ij for the municipality i.
2.4. Statistical Analysis
3. Results and Discussion
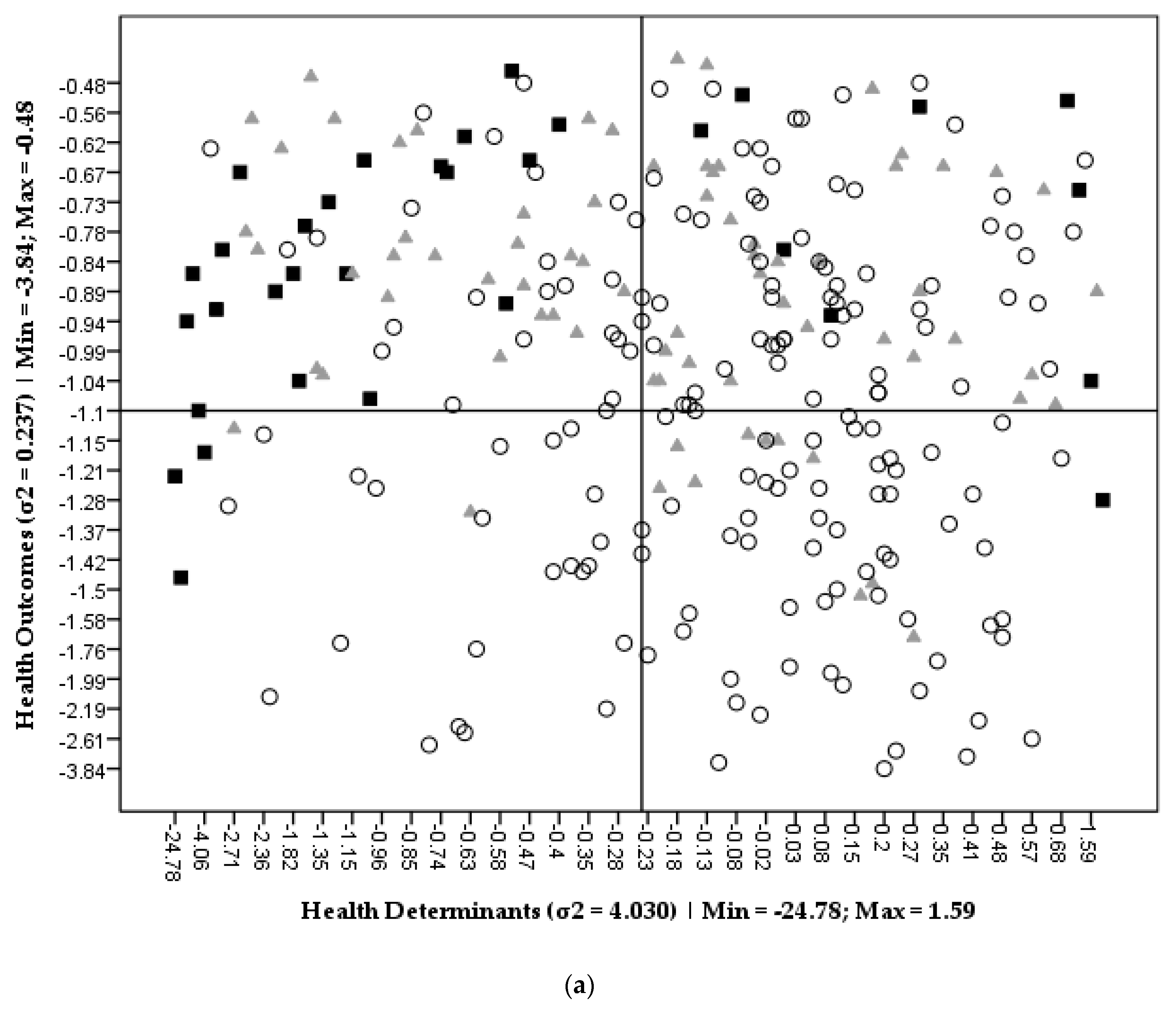
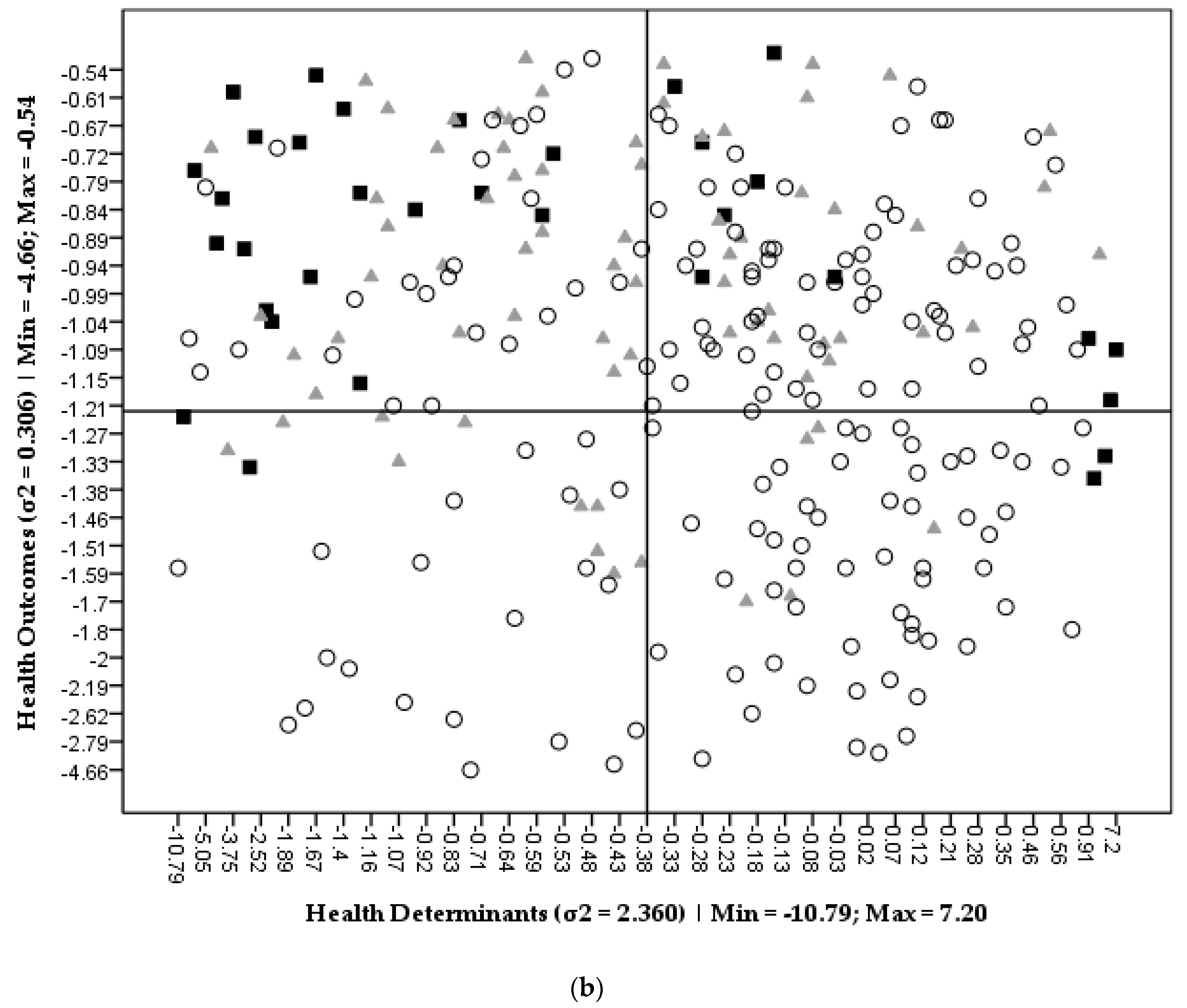
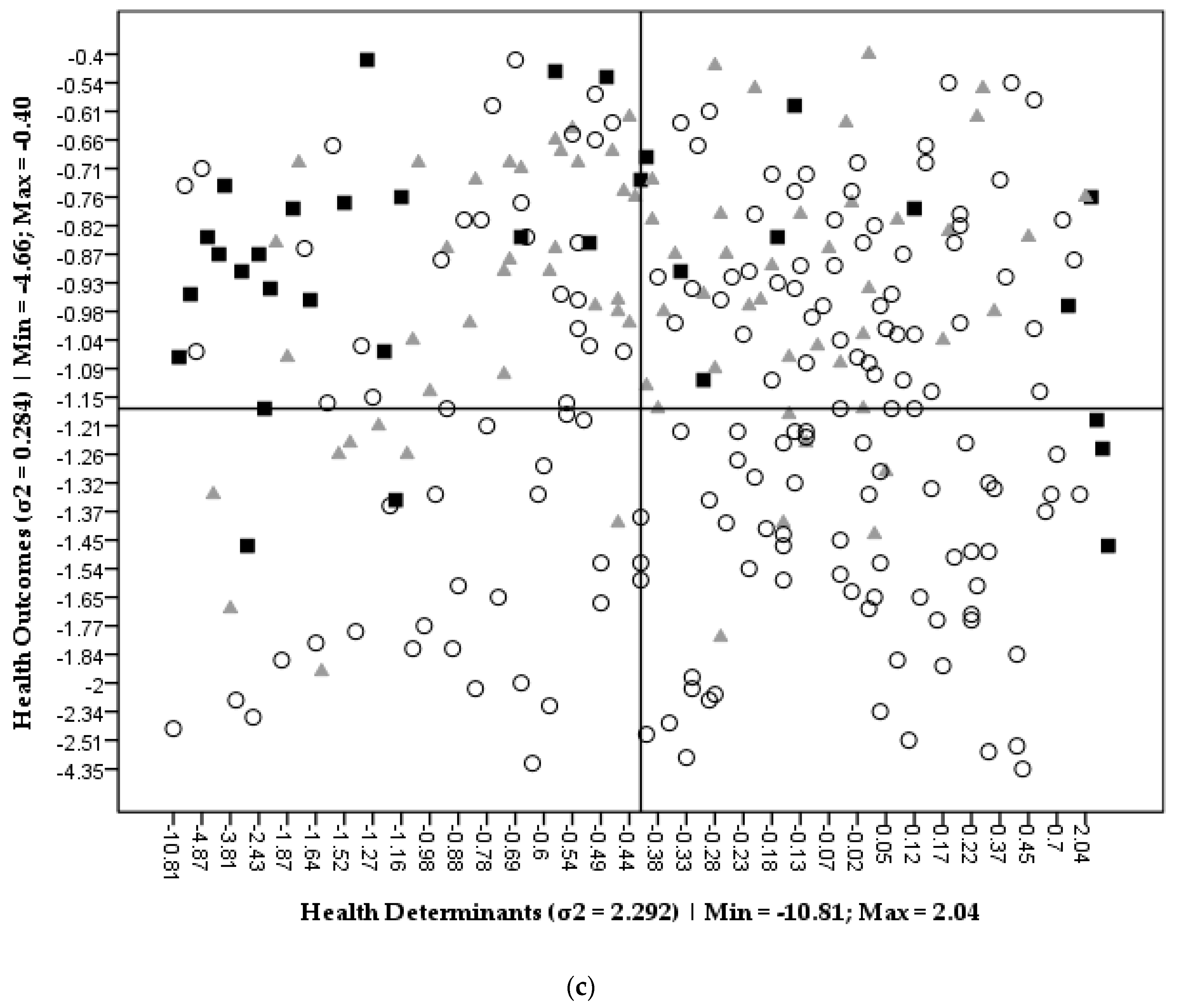
3.1. SEHVI Validation
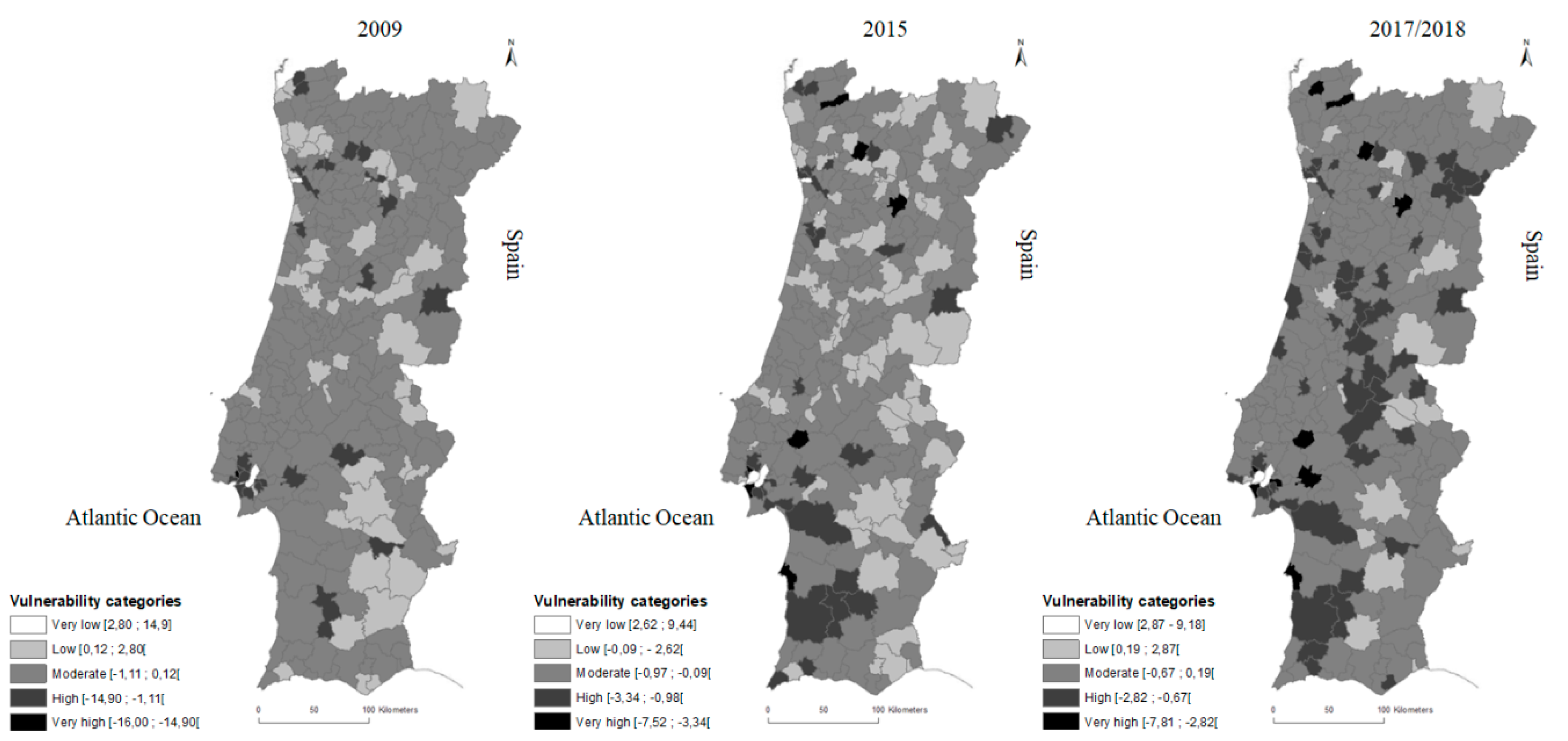
3.2. SEHVI Application
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Whitehead, M. The concepts and principles of equity and health. Health Promot. Int. 1991, 6, 217–228. [Google Scholar] [CrossRef]
- United Nations General Assembly. Transforming Our World: The 2030 Agenda for Sustainable Development (Resolution A/RES/70/1 Adopted by the UN General Assembly on 25 September 2015); United Nations: New York, NY, USA, 2015; p. 35. [Google Scholar]
- Carneiro, F.F.; Franco Netto, G.; Corvalan, C.; Freitas, C.M.D.; Sales, L.B.F. Environmental health and inequalities: Building indicators for sustainable development. Ciênc. Saúde Colet. 2012, 17, 1419–1425. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Bambra, C.; Gibson, M.; Sowden, A.; Wright, K.; Whitehead, M.; Petticrew, M. Tackling the wider social determinants of health and health inequalities: Evidence from systematic reviews. J. Epidemiol. Community Health 2010, 64, 284–291. [Google Scholar] [CrossRef] [PubMed]
- Costa, C.; Santana, P.; Dimitroulopoulou, S.; Burstrom, B.; Borrell, C.; Schweikart, J.; Dzurova, D.; Zangarini, N.; Katsouyanni, K.; Deboseree, P.; et al. Population Health Inequalities Across and Within European Metropolitan Areas through the Lens of the EURO-HEALTHY Population Health Index. Int. J. Environ. Res. Public Health 2019, 16, 836. [Google Scholar] [CrossRef] [PubMed]
- Mitsakou, C.; Corman, D.; Freitas, Â.; Zengarini, N.; Schweikart, J.; Camprubí, L.; Gotsens, M.; Lustigova, M.; Santana, P. Population health inequalities across Metropolitan Areas: Evidence from the EURO-HEALTHY project. Eur. J. Public Health 2018, 28. [Google Scholar] [CrossRef]
- Calheiros, J.M. Promoting Health Promotion. Obs. Bol. Epidemiol. 2013, 5, 1–2. [Google Scholar]
- Graham, H.; White, P.C.L. Social determinants and lifestyles: Integrating environmental and public health perspectives. Public Health 2016, 141, 270–278. [Google Scholar] [CrossRef]
- Sant’Anna, S.R.; Hennington, É.A. Health promotion and reduction of vulnerabilities: A strategy for knowledge production and (trans)formation of healthcare work, based on Ergology. Interface Comun. Saúde Educ. 2010, 14, 207–215. [Google Scholar] [CrossRef]
- Mackenbach, J.P.; Hu, Y.; Artnik, B.; Bopp, M.; Costa, G.; Kalediene, R.; Martikainen, P.; Menvielle, G.; Strand, B.H.; Wojtyniak, B.; et al. Trends In Inequalities In Mortality Amenable To Health Care In 17 European Countries. Health Aff. 2017, 36, 1110–1118. [Google Scholar] [CrossRef]
- Santana, P.; Costa, C.; Freitas, Â.; Stefanik, I.; Quintal, C.; Bana e Costa, C.; Borrell, C. Atlas of Population Health in European Union Regions; Imprensa da Universidade de Coimbra: Coimbra, Portugal, 2017. [Google Scholar] [CrossRef]
- Commission on Social Determinants of Health. Closing the Gap in a Generation: Health Equity through Action on the Social Determinants of Health; World Health Organization: Geneva, Switzerland, 2008; p. 256. [Google Scholar]
- Nolte, E.; McKee, M.; Karanikolos, M.; Mackenbach, J.P.; Stuckler, D. Amenable mortality in the EU—Has the crisis changed its course? Eur. J. Public Health 2018, 28, 864–869. [Google Scholar] [CrossRef]
- Thomson, K.; Hillier-Brown, F.; Todd, A.; McNamara, C.; Huijts, T.; Bambra, C. The effects of public health policies on health inequalities in high-income countries: An umbrella review. Bmc Public Health 2018, 18, 869. [Google Scholar] [CrossRef] [PubMed]
- Barreto, M.L. Health inequalities: A global perspective. Ciênc. Saúde Colet. 2017, 22, 2097–2108. [Google Scholar] [CrossRef] [PubMed]
- Pontes, M.M.D.M. Lifestyles and Blood Pressure in Young Adults: A Study in the City of Porto. Ph.D. Thesis, Universidade Fernando Pessoa Porto, Porto, Portugal, 2015. [Google Scholar]
- WHO Regional Office for Europe. Ostrava Declaration of the Sixth Ministerial Conference on Environment and Health; EURO/Ostrava2017/6; World Health Organization (WHO): Ostrava, Czech Republic, 2017; p. 5. [Google Scholar]
- WHO Regional Office for Europe. Ostrava Declaration of the Sixth Ministerial Conference on Environment and Health. Annex 2. Institutional Arrangements for the European Environment and Health Process; EURO/Ostrava2017/8; World Health Organization (WHO): Ostrava, Czech Republic, 2017; p. 5. [Google Scholar]
- WHO Regional Office for Europe. Ostrava Declaration of the Sixth Ministerial Conference on Environment and Health. Annex 1. Compendium of Possible Actions to Advance the Implementation of the Ostrava Declaration; EURO/Ostrava2017/7; World Health Organization (WHO): Ostrava, Czech Republic, 2017; p. 16. [Google Scholar]
- WHO Regional Office for Europe. European Health Report 2018: More Than Numbers—Evidence for All; World Health Organization (WHO): Copenhagen, Denmark, 2018; p. 164. [Google Scholar]
- Graham, H. Social Determinants and Their Unequal Distribution: Clarifying Policy Understandings. Milbank Q. 2004, 82, 101–124. [Google Scholar] [CrossRef] [PubMed]
- Ribeiro, J.M.; Moreira, M.R. Regional inequalities, cooperative federalism and challenges facing the SUS. Ciênc. Saúde Colet. 2017, 22, 1028. [Google Scholar] [CrossRef]
- Mackenbach, J.P.; Bouvier-Colle, M.H.; Jougla, E. “Avoidable” Mortality and Health Services: A Review of Aggregate Data Studies. J. Epidemiol. Community Health 1990, 44, 106–111. [Google Scholar] [CrossRef]
- Mackenbach, J.P.; Looman, C.W.N.; Artnik, B.; Bopp, M.; Deboosere, P.; Dibben, C.; Kalediene, R.; Kovács, K.; Leinsalu, M.; Martikainen, P.; et al. ‘Fundamental causes’ of inequalities in mortality: An empirical test of the theory in 20 European populations. Sociol. Health Illn. 2017, 39, 1117–1133. [Google Scholar] [CrossRef]
- Saltarelli, R.M.F.; Prado, R.R.D.; Monteiro, R.A.; Machado, Í.E.; Teixeira, B.D.S.M.; Malta, D.C. Deaths preventable by actions of the Unified Health System in the population of the Brazilian Southeast Region. Ciênc. Saúde Colet. 2019, 24, 887–898. [Google Scholar] [CrossRef]
- Phelan, J.C.; Link, B.G.; Diez-Roux, A.; Kawachi, I.; Levin, B. “Fundamental Causes” of Social Inequalities in Mortality: A Test of the Theory. J. Health Soc. Behav. 2004, 45, 265–285. [Google Scholar] [CrossRef]
- Phelan, J.C.; Link, B.G.; Tehranifar, P. Social Conditions as Fundamental Causes of Health Inequalities: Theory, Evidence, and Policy Implications. J. Health Soc. Behav. 2010, 51, S28–S40. [Google Scholar] [CrossRef]
- Kelly, M.P.; Morgan, A.; Bonnefoy, J.; Butt, J.; Bergman, V.; Mackenbach, J.; Exworthy, M.; Popay, J.; Tugwell, P.; Robinson, V.; et al. The Social Determinants of Health: Developing an Evidence Base for Political Action. Final Report to World Health Organization Commission on the Social Determinants of Health; World Health Organization: Geneva, Switzerland, 2007; p. 165. [Google Scholar]
- Assembleia da República Portuguesa. Lei n.º 56/1979, de 15 de Setembro: Serviço Nacional de Saúde. In Diário da República n.º 214/1979, Série I de 1979-09-15; Diário da República: Lisboa, Portugal, 1979; pp. 2357–2363. [Google Scholar]
- Vidal, D.G.; Pontes, M.; Barreira, E.; Oliveira, G.M.; Maia, R.L. Differential mortality and inequalities in health services access in mainland Portugal. Finisterra 2018, 53, 37–54. [Google Scholar] [CrossRef]
- OECD; European Observatory on Health Systems and Policies. State of Health in the EU—Portugal: Country Health Profile 2017; OECD Publishing: Paris, France, 10 November 2017. [Google Scholar]
- Doetsch, J.; Pilot, E.; Santana, P.; Krafft, T. Potential barriers in healthcare access of the elderly population influenced by the economic crisis and the troika agreement: A qualitative case study in Lisbon, Portugal. Int. J. Equity Health 2017, 16, 184. [Google Scholar] [CrossRef] [PubMed]
- Rumbold, B.; Baker, R.; Ferraz, O.; Hawkes, S.; Krubiner, C.; Littlejohns, P.; Norheim, O.F.; Pegram, T.; Rid, A.; Venkatapuram, S.; et al. Universal health coverage, priority setting, and the human right to health. Lancet 2017, 390, 712–714. [Google Scholar] [CrossRef]
- Jamison, D.T.; Alwan, A.; Mock, C.N.; Nugent, R.; Watkins, D.; Adeyi, O.; Anand, S.; Atun, R.; Bertozzi, S.; Bhutta, Z.; et al. Universal health coverage and intersectoral action for health: Key messages from Disease Control Priorities. Lancet 2018, 391, 1108–1120. [Google Scholar] [CrossRef]
- INE—Instituto Nacional de Estatística, I.P. Typology of Urban. Areas 2014—Technical Report; INE: Lisboa, Portugal, 2014; p. 20. [Google Scholar]
- Leadership Council of the Sustainable Development Solutions Network. Indicators and a Monitoring Framework for the Sustainable Development Goals: Launching a Data Revolution for the SDGs; Secretary-General of the United Nations: New York, NY, USA, 2015; p. 233. [Google Scholar]
- Nunes, A.R.; Lee, K.; O’Riordan, T. The importance of an integrating framework for achieving the Sustainable Development Goals: The example of health and well-being. BMJ Glob. Health 2016, 1. [Google Scholar] [CrossRef]
- United Nations General Assembly. Global Indicator Framework for the Sustainable Development Goals and Targets of the 2030 Agenda for the Sustainable Development; A/RES/71/313, E/CN.3/2018/2 (Annex II); United Nations: New York, NY, USA, 2018; p. 21. [Google Scholar]
- Yang, X.; Wang, Y.; Sun, M.; Wang, R.; Zheng, P. Exploring the environmental pressures in urban sectors: An energy-water-carbon nexus perspective. Appl. Energy 2018, 228, 2298–2307. [Google Scholar] [CrossRef]
- Oliveira, G.M.; Vidal, D.G.; Viterbo, L.M.F.; Maia, R.L. Measuring the implementation of Sustainable Development Goals at a local level: The WeGIx index. In Universities and Sustainable Communities: Meeting the Goals of the Agenda 2030, 1st ed.; Leal Filho, W., Tortato, U., Frankerberg, F., Eds.; Springer: Cham, Switzerland, 2020; in press. [Google Scholar] [CrossRef]
- Oliveira, G.M.; Vidal, D.G.; Maia, R.L. Monitoring Portuguese Living Conditions at Local Scale: A Case Study based on Sustainable Development Indicators. Int. J. Sustain. Dev. World Ecol. 2019, in press. [Google Scholar] [CrossRef]
- Papadimitriou, E.; Neves, A.R.; Becker, W. JRC Statistical Audit of the Sustainable Development Goals Index and Dashboards; 29776 EN; European Commission—Joint Research Centre: Luxembourg, 2019; p. 35. [Google Scholar]
- Nardo, M.; Saisana, M. OECD/JRC Handbook on constructing composite indicators. Putting theory into practice. In Proceedings of the NTTS (New Techniques and Technologies for Statistics) Seminar, Brussels, Belgium, 18–20 February 2009; p. 16. [Google Scholar]
- Nardo, M.; Saisana, M.; Saltelli, A.; Tarantola, S. Tools for Composite Indicators Building; European Commission—Joint Research Centre: Ispra, Italy, 2005; p. 134. [Google Scholar]
- Nardo, M.; Saisana, M.; Saltelli, A.; Tarantola, S.; Hoffman, A.; Giovannini, E. Handbook on Constructing Composite Indicators: Methodology and User Guide; OECD: Paris, France, 2005; p. 108. [Google Scholar]
- Sachs, J.; Schmidt-Traub, G.; Kroll, C.; Durand-Delacre, D.; Teksoz, K. SDG Index and Dashboards—Global Report; Bertelsmann Stiftung and Sustainable Development Solutions Network (SDSN): New York, NY, USA, 2016; p. 427. [Google Scholar]
- Mazziotta, M.; Pareto, A. Methods for Constructing Composite Indices: One for all or all for one? Riv. Ital. Econ. Demogr. E Stat. 2013, 67, 67–80. [Google Scholar]
- OECD; JRC European Commission. Handbook on Constructing Composite Indicators. Methodology and User Guide; OECD Publications: Paris, France, 2008; p. 162. [Google Scholar]
- Taber, K.S. The Use of Cronbach’s Alpha When Developing and Reporting Research Instruments in Science Education. Res. Sci. Educ. 2018, 48, 1273–1296. [Google Scholar] [CrossRef]
- Ribas-Mateos, N. Exploring the Shifting Contours. In Border Shifts: New Mobilities in Europe and Beyond, 1st ed.; Palgrave Macmillan: New York, NY, USA, 2015. [Google Scholar] [CrossRef]
- Fernandes, J.A.R.; Seixas, J. Cities and Urbanisation in Democratic Portugal. Méditerranée J. Mediterr. Geogr. 2018, 130. [Google Scholar] [CrossRef]
- Guimarães, M.H.; Barreira, A.P.; Panagopoulos, T. Shrinking Cities in Portugal—Where and Why. Rev. Port. Estud. Reg. 2013, 40, 23–41. [Google Scholar]
- Knoema Global Database. Portugal—Population density. In World Data—Atlas Portugal—Demographics; Knoema: Washington, DC, USA, 2019. [Google Scholar]
- Rodrigues, A.M.; Gregório, M.J.; Sousa, R.D.; Dias, S.S.; Santos, M.J.; Mendes, J.M.; Coelho, P.S.; Branco, J.C.; Canhão, H. Challenges of Ageing in Portugal: Data from the EpiDoC Cohort. Acta Med. Port. 2018, 31, 14. [Google Scholar] [CrossRef] [PubMed]
- Santana, P. Os Ganhos em Saúde e no Acesso aos Serviços de Saúde. Avaliação das Últimas Três Décadas. In Trinta Anos do Serviço Nacional de Saúde. Um Percurso Comentado; Simões, J.C., Ed.; Edição Gulbenkian/APES: Lisboa, Portugal, 2010; pp. 21–81. [Google Scholar]
- Tudor Hart, J. The Inverse Care Law. Lancet 1971, 297, 405–412. [Google Scholar] [CrossRef]
- Watt, G. The inverse care law today. Lancet 2002, 360, 252–254. [Google Scholar] [CrossRef]
- Vidal, D.G.; Barreira, E.; Oliveira, G.M.; Pontes, M.; Maia, R.L.; Ferraz, M.P.; Cabeda, J.M.; Calheiros, J.M. Assessment of Health and Well-Being of Portuguese Population by Environmental and Socioeconomic Determinants. In Proceedings of the International Congress of Health and Well-Being Intervention—ICHWBI2019, Viseu, Portugal, 31 May–1 June 2019. in press. [Google Scholar]
- Arruda, N.M.; Maia, A.G.; Alves, L.C. Inequality in access to health services between urban and rural areas in Brazil: A disaggregation of factors from 1998 to 2008. Cad. Saúde Pública 2018, 34, 1–14. [Google Scholar]
- Zhang, D.; Li, X.; Xue, J. Education Inequality between Rural and Urban Areas of the People’s Republic of China, Migrants’ Children Education, and Some Implications. Asian Dev. Rev. 2015, 32, 196–224. [Google Scholar] [CrossRef]
- Strosnider, H.; Kennedy, C.; Monti, M.; Yip, F. Rural and Urban Differences in Air Quality, 2008–2012, and Community Drinking Water Quality, 2010–2015—United States. Surveill. Summ. Morb. Mortal. Wkly. Rep. 2017, 66, 1–10. [Google Scholar] [CrossRef]
- Adinna, E. Environmental Pollution in Urban and Rural Areas: Sources and Ethical Implications. In Environmental Pollution and Management in the Tropics; Adinna, E.N., Ekop, O.B., Attah, V.I., Eds.; Snaap Press Ltd.: Enugu, Nigeria, 2003; pp. 298–316. [Google Scholar]
- Maia, R.L.; Vidal, D.G.; Oliveira, G.M. Ambiente e Saúde: Uma Leitura Comparada a Partir das Estatísticas dos Meios Rurais e Urbanos. Obra Nasce Rev. Arquit. Urban. Univ. Fernando Pessoa 2018, 13. [Google Scholar]
- Institute of Medicine. Rebuilding the Unity of Health and the Environment in Rural America: Workshop Summary; The National Academies Press: Washington, DC, USA, 2006. [Google Scholar] [CrossRef]
- Santana, P.; Almendra, R. The Health of the Portuguese over the Last Four Decades. Méditerranée J. Mediterr. Geogr. 2018, 130. [Google Scholar] [CrossRef]
- Santana, P.C. Promoting Population Health and Equity in Europe: From Evidence to Policy; Imprensa da Universidade de Coimbra: Coimbra, Portugal, 2017. [Google Scholar] [CrossRef]
- Simões, J.D.A.; Augusto, G.F.; Hernández-Quevedo, C. Portugal: Health System Review. Health Syst. Transit. 2017, 19, 1–184. [Google Scholar]
- Directorate-General for Regional and Urban Policy (European Commission); United Nations Human Settlements Programme (UN-Habitat). The State of European Cities Report, 2016—Cities Leading the Way to a Better Future; European Comission: Brussels, Belgium, 2016. [Google Scholar]

| Dimension | Indicators | Time Series Available | Polarity | |
|---|---|---|---|---|
| Health Outcomes | Mortality | 1 Infant mortality rate (‰) | 2009–2017 | - |
| 2 Deaths by HIV and Tuberculosis (No.) | 2009–2017 | - | ||
| 3 Deaths by circulatory Diseases (No.) | 2009–2017 | - | ||
| 4 Deaths by Tumors (No.) | 2009–2017 | - | ||
| 5 Deaths by Diabetes (No.) | 2009–2017 | - | ||
| 6 Deaths by Respiratory Diseases (No.) | 2009–2017 | - | ||
| 7 Suicide (No.) | 2009–2017 | - | ||
| Health Determinants | Healthcare Resources | 8 Number of health care professionals (No.) | 2009–2017 | + |
| 9 Number of hospitals (No.) | 2009–2016 | + | ||
| 10 Number of primary health care centers (No.) | 2009–2012 | + | ||
| Education | 11 Number of illiterate persons (No.) | 2001;2011 | - | |
| 12 Number of persons enrolled in basic education (No.) | 2009–2017 | + | ||
| 13 Number of persons enrolled in pre-graduate studies (No.) | 2009–2017 | + | ||
| 14 Number of persons in higher education (No.) | 2009–2017 | + | ||
| 15 Number of persons in lifelong learning (No.) | 2008–2017 | + | ||
| Water and Sanitation | 16 Population connected to public water supply systems (%) | 2009 | + | |
| 17 Population connected to sewerage systems (%) | 2009–2016 | + | ||
| 18 Water supplied/consumed (m3) | 2009–2016 | - | ||
| 19 Water quality for human consumption (%) | 2009–2016 | + | ||
| Air Pollution and Land | 20 NOx emissions (ton/km2) | 2009;2015 | - | |
| 21 PM10 emissions and PM2.5 emissions (ton/km2) | 2009;2015 | - | ||
| 22 CO2 emissions (ton/km2) | 2009;2015 | - | ||
| 23 Burnt Area (ha) | 2009–2017 | - | ||
| Waste | 24 Selective urban waste collection (ton) | 2009–2016 | + | |
| 25 Undifferentiated urban waste collection (ton) | 2009–2016 | - | ||
| 26 Incinerators and Landfills (No.) | 2014;2016 | - | ||
| Safety | 27 Deaths by car accidents (No.) | 2009–2017 | - | |
| 28 Crimes registered (No.) | 2009–2017 | - | ||
| Housing | 29 Non-conventional dwellings (No.) | 2001;2011 | - | |
| 30 Buildings constructed before 1960 (No.) | 2001;2011 | - | ||
| Employment and Income | 31 Inactive young population (15–34 years) (No.) | 2001;2011 | - | |
| 32 Average monthly salary (Euro) | 2009–2016 | + | ||
| 33 Unemployed (No.) | 2009–2018 | - | ||
| Social Protection | 34 Social Security beneficiaries of Guaranteed Minimum Income and Social Integration Benefit (No.) | 2009–2018 | - | |
| Cultural and social participation | 35 Expenditures on cultural and creative activities of municipalities (Euro) | 2009–2017 | + | |
| Components | Individual Indicators | I | II | III | IV | V | VI | VII | VIII | IX | C | (α) * |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 12.9% | 30 Buildings constructed before 1960 | 0.83 | 0.87 | 0.79 | ||||||||
| 2 Deaths by HIV and Tuberculosis | 0.31 | 0.41 | 0.81 | |||||||||
| 8 Number of health care professionals | 0.70 | 0.80 | 0.81 | |||||||||
| 9 Number of hospitals | 0.90 | 0.91 | 0.79 | |||||||||
| 14 Number of persons in higher education | 0.71 | 0.82 | 0.81 | |||||||||
| 35 Expenditures on cultural and creative activities of municipalities | 0.86 | 0.87 | 0.78 | |||||||||
| 11.4% | 22 CO2 emissions | 0.93 | 0.92 | 0.77 | ||||||||
| 20 NOx emissions | 0.93 | 0.96 | 0.76 | |||||||||
| 21 PM10 emissions and PM2.5 emissions | 0.91 | 0.90 | 0.77 | |||||||||
| 10 Number of primary health care centers | 0.71 | 0.95 | 0.79 | |||||||||
| 11 Number of illiterate persons | 0.65 | 0.89 | 0.79 | |||||||||
| 9.7% | 26 Incinerators and Landfills | 0.46 | 0.44 | 0.81 | ||||||||
| 3 Deaths by circulatory Diseases | −0.80 | 0.69 | 0.81 | |||||||||
| 6 Deaths by Respiratory Diseases | −0.69 | 0.56 | 0.81 | |||||||||
| 4 Deaths by Tumors | −0.81 | 0.68 | 0.81 | |||||||||
| 12 Number of persons enrolled in basic education | 0.66 | 0.76 | 0.81 | |||||||||
| 5 Deaths by Diabetes | 0.63 | 0.62 | 0.81 | |||||||||
| 33 Unemployed | 0.56 | 0.62 | 0.81 | |||||||||
| 8.5% | 18 Water supplied/consumed | 0.65 | 0.50 | 0.81 | ||||||||
| 24 Selective urban waste collection | 0.84 | 0.74 | 0.81 | |||||||||
| 25 Undifferentiated urban waste collection | 0.85 | 0.76 | 0.81 | |||||||||
| 28 Crimes registered | 0.65 | 0.67 | 0.81 | |||||||||
| 31 Inactive young population (15–34 years) | −0.41 | 0.54 | 0.81 | |||||||||
| 6.8% | 13 Number of persons enrolled in pre-graduate studies | 0.77 | 0.73 | 0.81 | ||||||||
| 15 Number of persons in lifelong learning | 0.81 | 0.69 | 0.81 | |||||||||
| 5.9% | 23 Burnt Area | 0.61 | 0.50 | 0.81 | ||||||||
| 16 Population connected public water supply systems | −0.58 | 0.51 | 0.81 | |||||||||
| 34 Social Security beneficiaries of Guaranteed Minimum Income and Social Integration Benefit | 0.68 | 0.75 | 0.81 | |||||||||
| 32 Average monthly salary | −0.38 | 0.58 | 0.81 | |||||||||
| 4.6% | 29 Non-conventional dwellings | 0.66 | 0.61 | 0.81 | ||||||||
| 17 Population connected to sewerage systems | 0.47 | 0.46 | 0.81 | |||||||||
| 4.3% | 7 Suicide | 0.79 | 0.70 | 0.81 | ||||||||
| 27 Deaths by car accidents | 0.63 | 0.48 | 0.81 | |||||||||
| 3.5% | 19 Water quality for human consumption | 0.50 | 0.40 | 0.81 | ||||||||
| 1 Infant mortality rate | 0.77 | 0.66 | 0.81 |
| Municipality Typologies (N) | Area (km2) | Population (Inhabitants) | Population Density (Inhabitants/km2) | Ageing Index | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| 2009 | 2015 | 2017/2018 | 2009 | 2015 | 2017/2018 | 2009 | 2015 | 2017/2018 | ||
| PU (33) | 3478 (3.9%) | 4,676,005 (46.5%) | 4,627,128 (47.0%) | 4,630,237 (47.2%) | 1344.5 | 1330.4 | 1331.3 | 113.3 | 130.6 | 138.3 |
| SU (76) | 15,641 (17.6%) | 3,162,391 (31.4%) | 3,130,700 (31.8%) | 3,115,298 (31.8%) | 202.2 | 200.2 | 199.2 | 137.3 | 163.1 | 177 |
| PR (169) | 69,982 (78.5%) | 2,217,205 (22.0%) | 2,096,697 (21.3%) | 2,055,636 (21.0%) | 31.7 | 30.0 | 29.4 | 250 | 288 | 306.7 |
| Time | Territory Typology | Outcomes | Determinants | SEHVI | |||
|---|---|---|---|---|---|---|---|
| M ± SD | M ≠ | M ± SD | M ≠ | M ± SD | M ≠ | ||
| 2009 | PU | −0.83 ± 0.25 | MPU₋MSU = 0.05 | −1.97 ± 5.33 | MPU₋MSU = −1.63 * | −0.62 ± 4.00 | MPU₋MSU = −0.43 |
| SU | −0.88 ± 0.25 | MPU₋MPR = 0.38 * | −0.34 ± 0.81 | MPU₋MPR = −1.85 * | −0.19 ± 0.63 | MPU₋MPR = −0.41 | |
| PR | −1.21 ± 0.55 | MSU₋MPR = 0.33 * | −0.13 ± 0.60 | MSU₋MPR = −0.22 | −0.21 ± 0.47 | MSU₋MPR = 0.02 | |
| F = 18.7 * | F = 12.7 * | F = 1.21 | |||||
| 2015 | PU | −0.89 ± 0.23 | MPU₋MSU = 0.08 | −0.99 ± 3.15 | MPU₋MSU = −0.43 | 0.06 ± 3.15 | MPU₋MSU = 0.43 |
| SU | −0.97 ± 0.29 | MPU₋MPR = 0.46 * | −0.56 ± 0.89 | MPU₋MPR = −0.61 | −0.37 ± 0.69 | MPU₋MPR = 0.50 | |
| PR | −1.35 ± 0.63 | MSU₋MPR= 0.38 | −0.39 ± 1.25 | MSU₋MPR = −0.17 | −0.44 ± 0.89 | MSU₋MPR = 0.07 | |
| F = 20.3 * | F = 2.23 | F = 1.94 | |||||
| 2017/2018 | PU | −0.91 ± 0.25 | MPU₋MSU = 0.05 | −0.97 ± 3.07 | MPU₋MSU = 0.43 | 0.07 ± 3.06 | MPU₋MSU = 0.41 |
| SU | −0.96 ± 0.28 | MPU₋MPR = 0.40 * | −0.52 ± 0.85 | MPU₋MPR = 0.50 | −0.34 ± 0.68 | MPU₋MPR = 0.52 | |
| PR | −1.31 ± 0.61 | MSU₋MPR = 0.35 * | −0.42 ± 1.27 | MSU₋MPR = 0.07 | −0.45 ± 0.91 | MSU₋MPR = 0.11 | |
| F = 17.5 * | F = 1.95 | F = 1.17 | |||||
| SEHVI | 2009 | 2015 | 2017/2018 | |||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Municipalities (N) | Municipalities (N) | Municipalities (N) | ||||||||||||||
| PU | SU | PR | Total | Population (%) | PU | SU | PR | Total | Population (%) | PU | SU | PR | Total | Population (%) | ||
| Vulnerability categories | Very low | 1 | 0 | 0 | 1 | 2.4 | 3 | 0 | 0 | 3 | 7.6 | 3 | 0 | 0 | 3 | 7.6 |
| Low | 9 | 16 | 26 | 51 | 21.7 | 8 | 17 | 46 | 71 | 21.2 | 5 | 5 | 13 | 23 | 9.9 | |
| Moderate | 12 | 54 | 135 | 201 | 53.6 | 11 | 54 | 105 | 170 | 51.2 | 10 | 60 | 118 | 188 | 55.0 | |
| High | 10 | 6 | 8 | 24 | 20.6 | 9 | 4 | 14 | 27 | 16.0 | 13 | 9 | 33 | 55 | 22.7 | |
| Very high | 1 | 0 | 0 | 1 | 1.7 | 2 | 1 | 4 | 7 | 4.1 | 2 | 2 | 5 | 9 | 4.8 | |
| Total | 33 | 76 | 169 | 278 | 100 | 33 | 76 | 169 | 278 | 100 | 33 | 76 | 169 | 278 | 100 | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Oliveira, G.M.; Vidal, D.G.; Ferraz, M.P.; Cabeda, J.M.; Pontes, M.; Maia, R.L.; Calheiros, J.M.; Barreira, E. Measuring Health Vulnerability: An Interdisciplinary Indicator Applied to Mainland Portugal. Int. J. Environ. Res. Public Health 2019, 16, 4121. https://doi.org/10.3390/ijerph16214121
Oliveira GM, Vidal DG, Ferraz MP, Cabeda JM, Pontes M, Maia RL, Calheiros JM, Barreira E. Measuring Health Vulnerability: An Interdisciplinary Indicator Applied to Mainland Portugal. International Journal of Environmental Research and Public Health. 2019; 16(21):4121. https://doi.org/10.3390/ijerph16214121
Chicago/Turabian StyleOliveira, Gisela M., Diogo Guedes Vidal, Maria Pia Ferraz, José Manuel Cabeda, Manuela Pontes, Rui Leandro Maia, José Manuel Calheiros, and Esmeralda Barreira. 2019. "Measuring Health Vulnerability: An Interdisciplinary Indicator Applied to Mainland Portugal" International Journal of Environmental Research and Public Health 16, no. 21: 4121. https://doi.org/10.3390/ijerph16214121
APA StyleOliveira, G. M., Vidal, D. G., Ferraz, M. P., Cabeda, J. M., Pontes, M., Maia, R. L., Calheiros, J. M., & Barreira, E. (2019). Measuring Health Vulnerability: An Interdisciplinary Indicator Applied to Mainland Portugal. International Journal of Environmental Research and Public Health, 16(21), 4121. https://doi.org/10.3390/ijerph16214121








