The Effects of High-Temperature Weather on Human Sleep Quality and Appetite
Abstract
1. Introduction
2. Materials and Methods
2.1. Subjects
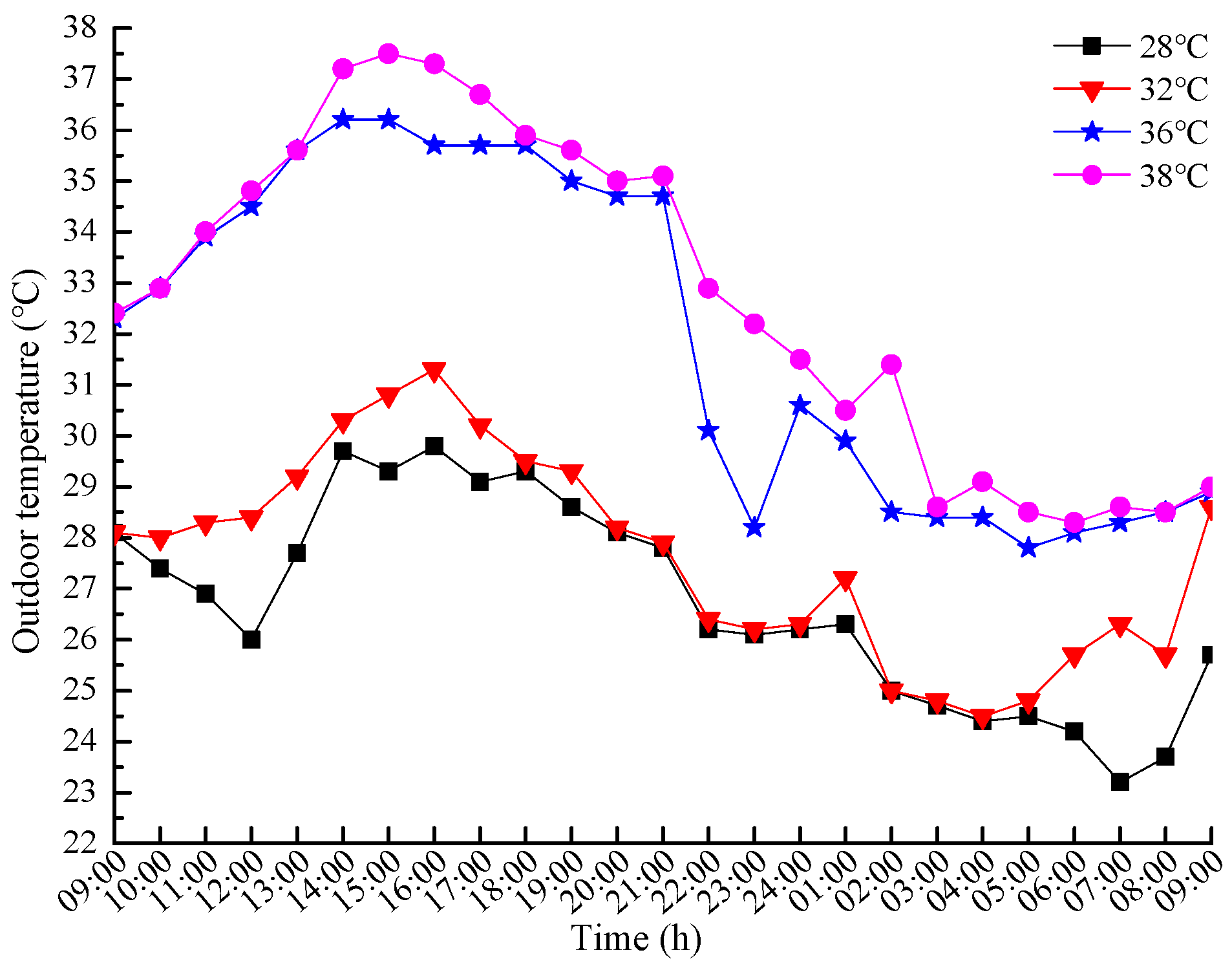
2.2. Experiment Conditions
2.3. Experiment Instruments
2.4. Sleep Quality
2.5. Appetite
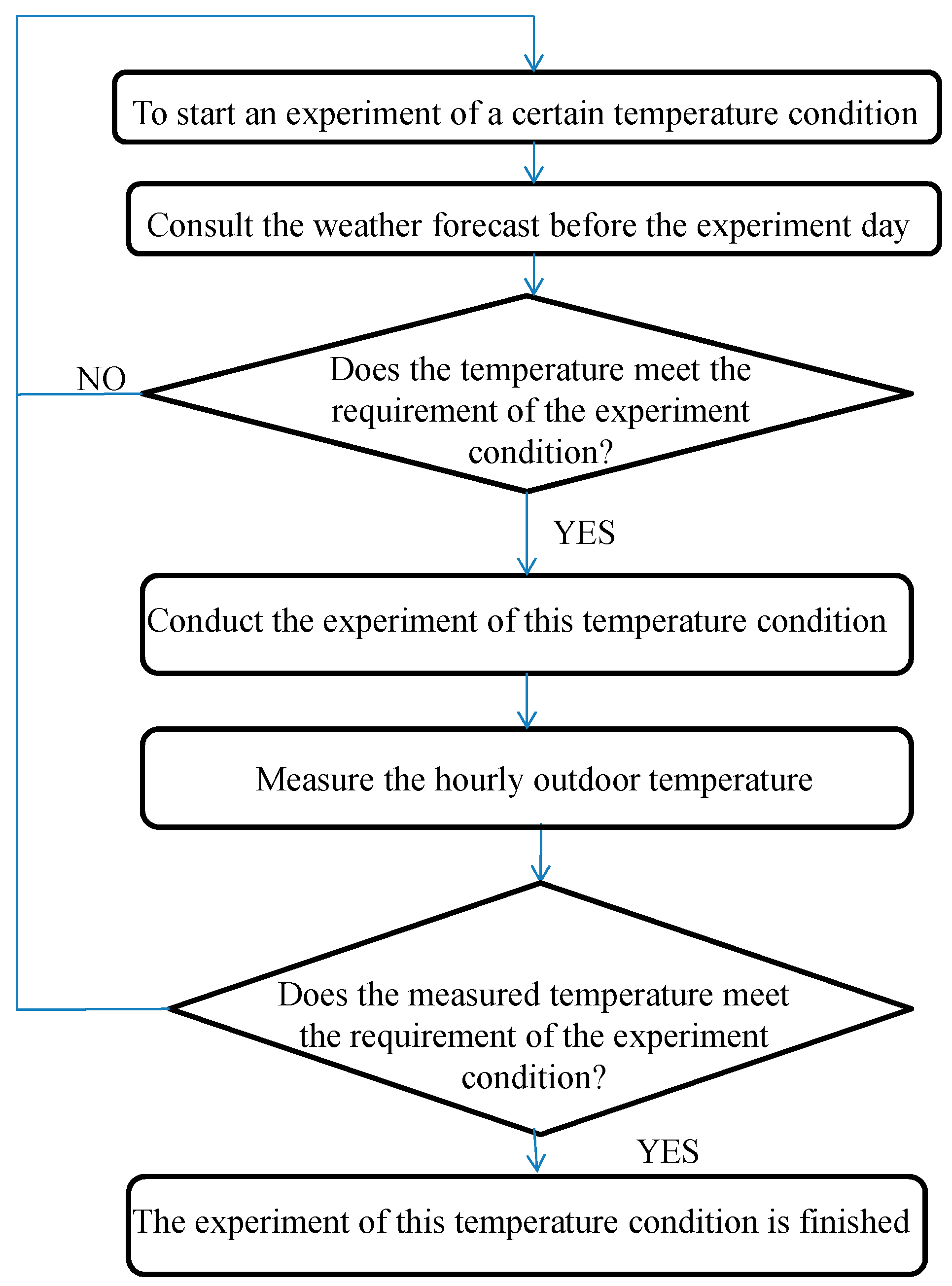
2.6. Experiment Process
2.7. Statistical Method
3. Results
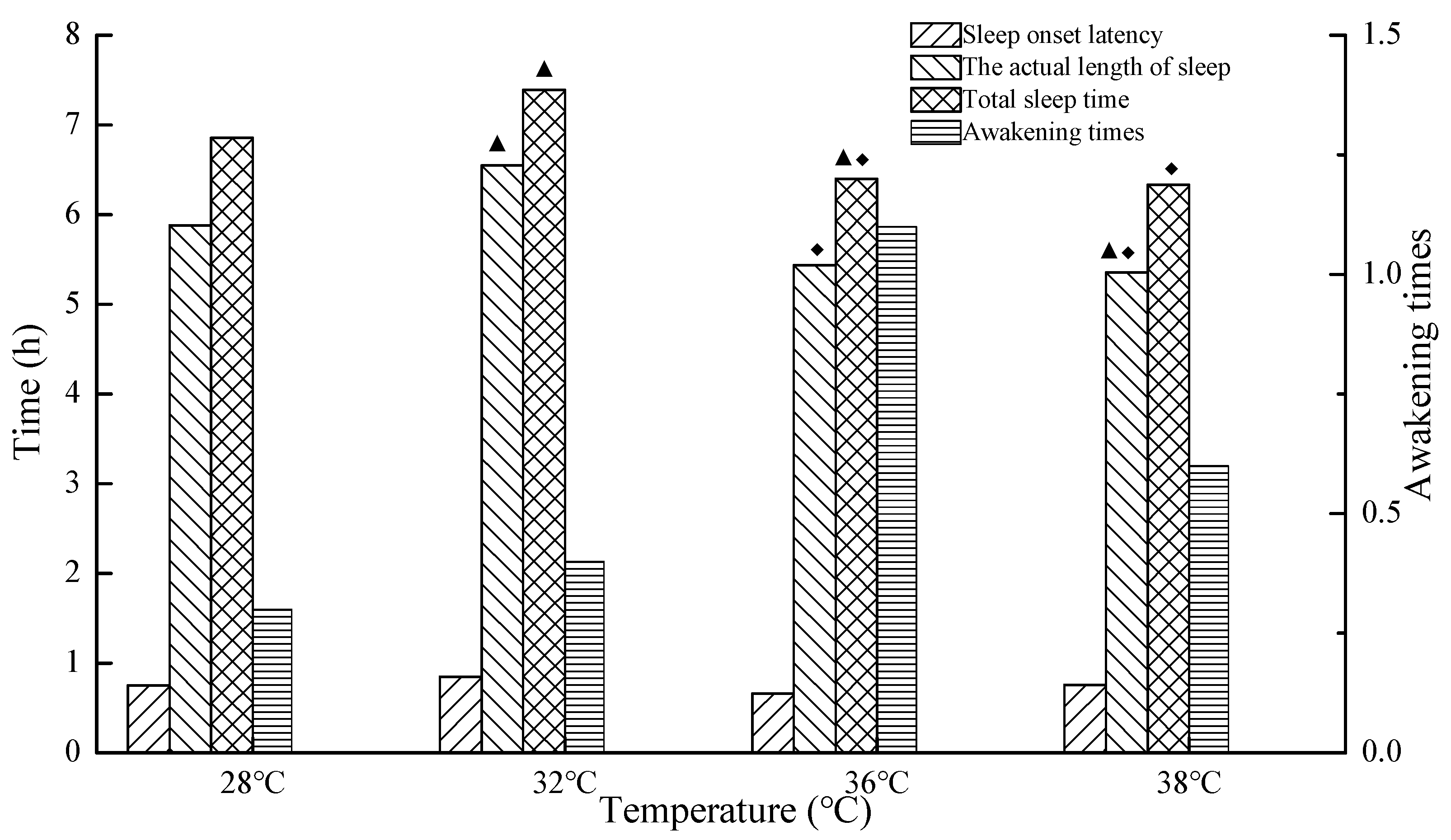
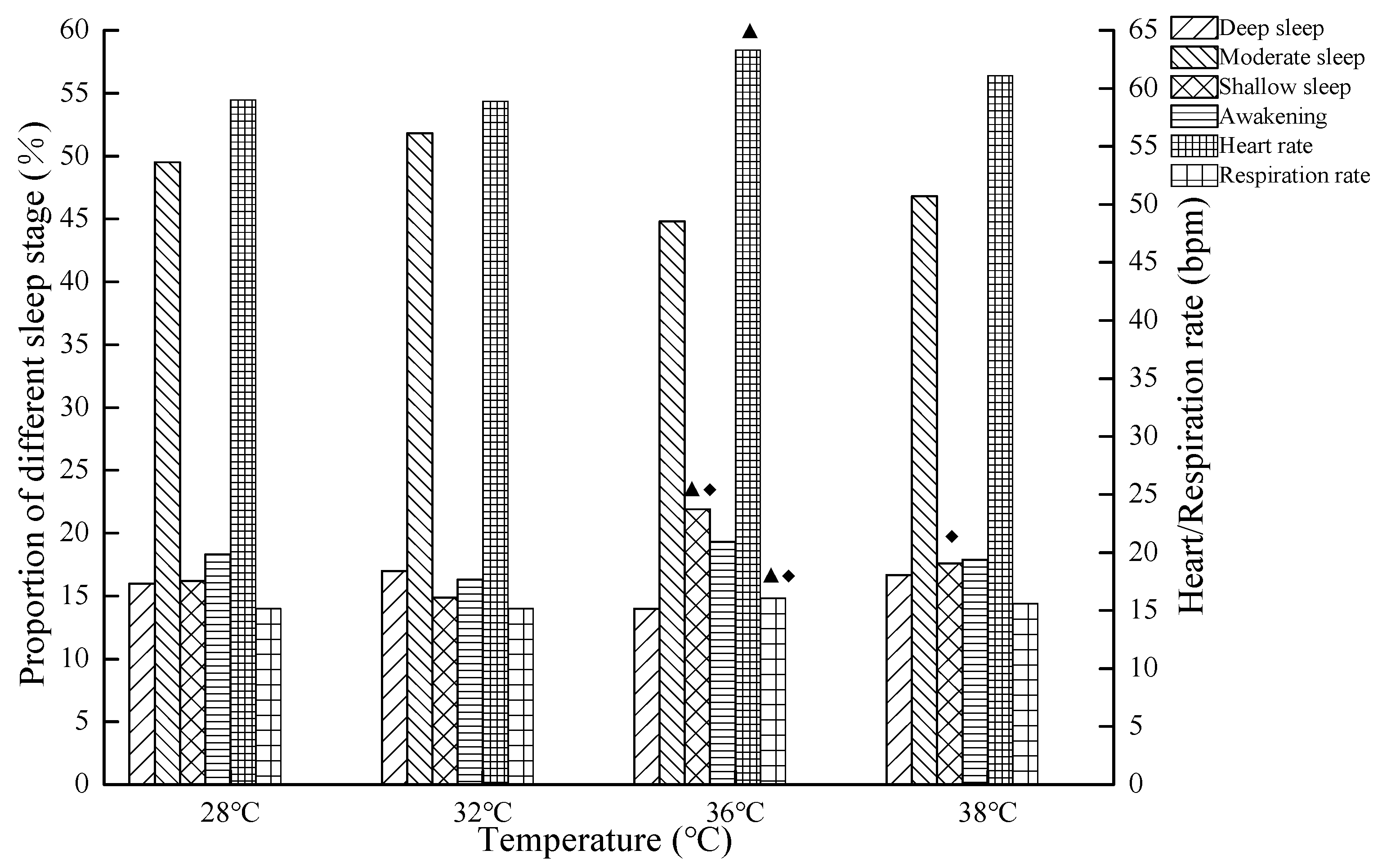
3.1. The Effects of Temperature on Sleep Quality
3.2. The Effects of Temperature on Appetite
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Masi, A.; Glozier, N.; Dale, R.; Guastella, A.J. The Immune System, Cytokines, and Biomarkers in Autism Spectrum Disorder. Neurosci. Bull. 2017, 33, 194–204. [Google Scholar] [CrossRef] [PubMed]
- Rao, R.M.; Vadiraja, H.S.; Nagaratna, R.; Gopinath, K.S.; Patil, S.; Diwakar, R.B.; Shahsidhara, H.B.; Ajaikumar, B.S.; Nagendra, H.R. Effect of Yoga on Sleep Quality and Neuroendocrine Immune Response in Metastatic Breast Cancer Patients. Indian J. Palliat. Care 2017, 23, 253–260. [Google Scholar] [CrossRef] [PubMed]
- Zheng, G.Z.; Li, K.; Bu, W.T.; Wang, Y.J. Fuzzy comprehensive evaluation of human physiological state in indoor high temperature environments. Build. Environ. 2019, 150, 108–118. [Google Scholar] [CrossRef]
- Ye, S.L.; Qi, X.H.; Cheng, Y.; Lin, R.P. Urban residents’ perception of high temperature and heat wave—Based on the survey of Fuzhou City. Acta Ecol. Sin. 2015, 35, 6814–6820. [Google Scholar]
- Zhu, M.L.; Ouyang, Q.; Zhu, Y.X.; Shen, H.G. Review on sleep thermal comfort research in hot environment. HVAC 2017, 47, 35–41. [Google Scholar]
- Baaghideh, M.; Mayvaneh, F. Climate change and simulation of cardiovascular disease mortality: A case study of Mashhad, Iran. Iran. J. Public Health 2017, 46, 396–407. [Google Scholar] [PubMed]
- Lu, S.L.; Sun, L.W.; Peng, H.Y.; Ji, L.R. Research of interindividual differences in physiological response under hot-dry and warm-wet climates. Sustainability 2016, 8, 850. [Google Scholar] [CrossRef]
- Pilgrim, A.; Robinson, S.; Sayer, A.A.; Roberts, H. An overview of appetite decline in older people. Nurs. Older People 2015, 27, 29–35. [Google Scholar] [CrossRef]
- Lan, L. Influence of Indoor Environment on Human Sleep Quality. Ph.D. Thesis, Shanghai Jiaotong University, Shanghai, China, 2012. [Google Scholar]
- Pan, L. The Thermal Comfort Investigation of Awaking and Sleeping State Based on Physiological Parameters. Ph.D. Thesis, Shanghai Jiaotong University, Shanghai, China, 2012. [Google Scholar]
- Okamoto, M.K.; Tsuzuki, K.; Mizuno, K. Effects of mild heat exposure on sleep stages and body temperature in older men. Int. J. Biometeorol. 2004, 49, 32–36. [Google Scholar] [CrossRef]
- Lan, L.; Tsuzuki, K.; Liu, Y.F.; Lian, Z.W. Thermal environment and sleep quality: A review. Energy Build. 2017, 149, 101–113. [Google Scholar] [CrossRef]
- Zhu, M.L.; Ouyang, Q.; Zhu, Y.X.; Shen, H.G. Field study on the objective evaluation of sleep quality and sleeping thermal environment in summer. Energy Build. 2016, 133, 843–852. [Google Scholar] [CrossRef]
- Wang, J. Effects of jogging and swimming on human appetite and food intake. In Proceedings of the 2009 National Sports Physiology Development and Discipline Construction Seminar; 2009; pp. 95–96. [Google Scholar]
- Westerterp-Plantenga, M.S.; Van Marken Lichtenbelt, W.D.; Cilissen, C.; Top, S. Energy metabolism in women during short exposure to the thermoneutral zone. Physiol. Behav. 2002, 75, 227–235. [Google Scholar] [CrossRef]
- Geeraerts, B.; Vandenberghe, J.; Oudenhove, L.V.; Gregory, L.J.; Aziz, Q.; DuPont, P.; Demyttenaere, K.; Janssens, J.; Tack, J. Influence of experimentally induced anxiety on gastric sensorimotor function in humans. Gastroenterology 2005, 129, 1437–1444. [Google Scholar] [CrossRef] [PubMed]
- Lin, L.; Jin, N.; Gu, W.J.; Yang, L.J.; Zang, L.; Du, J.; Chen, K.; Guo, Q.H.; Wang, X.L.; Yang, G.Q.; et al. Clinical analysis of seven cases of adrenal aldosterone-cortisol co-secretory tumor. Chin. Gen. Pract. 2017, 20, 3038–3041. [Google Scholar]
- Raynor, H.A.; Li, F.; Cardoso, C. Daily pattern of energy distribution and weight loss. Physiol. Behav. 2018, 192, 167–172. [Google Scholar] [CrossRef] [PubMed]
- Zhao, M.H. The Effect of Daily Cycle Rhythm Changes on the Anaerobic Capacity of Female College Students; Zhejiang Normal University: Jinhua, China, 2016. [Google Scholar]
- Paul, M.A.; Love, R.J.; Hawton, A.; Arendt, J. Sleep and the endogenous melatonin rhythm of high arctic residents during the summer and winter. Physiol. Behav. 2015, 141, 199–206. [Google Scholar] [CrossRef] [PubMed]
- Xu, X. Analysis of the Characteristics of Sleep-Wake Rhythm, Spontaneous Body Motion and Deep Body Temperature in Patients with Narcolepsy; Second Military Medical University: Shanghai, China, 2016. [Google Scholar]
- Na, W.W.; Jang, J.Y.; Lee, K.E.; Kim, H.Y.; Jun, B.Y.; Kwon, J.W.; Jo, S.N. The effects of temperature on heat-related illness according to the characteristics of patients during the summer of 2012 in the Republic of Korea. J. Prev. Med. Public Health 2013, 46, 19–27. [Google Scholar] [CrossRef]
- Sugg, M.M.; Konrad, C.E., II; Fuhrmann, C.M. Relationships between maximum temperature and heat-relatedillness across North Carolina, USA. Int. J. Biometeorol. 2016, 60, 663–675. [Google Scholar] [CrossRef]
- Gu, S.H.; Huang, C.R.; Bai, L.; Chu, C.; Liu, Q.Y. Heat-related illness in China, summer of 2013. Int. J. Biometeorol. 2016, 60, 131–137. [Google Scholar] [CrossRef] [PubMed]
- Hartz, D.A.; Brazel, A.J.; Golden, J.S. A comparative climate analysis of heat-related emergency 911 dispatches: Chicago, Illinois and Phoenix, Arizona USA 2003 to 2006. Int. J. Biometeorol. 2013, 57, 669–678. [Google Scholar] [CrossRef]
- Ng, C.F.S.; Ueda, K.; Ono, M.; Nitta, H.; Takami, A. Characterizing the effect of summer temperature on heatstroke-related emergency ambulance dispatches in the Kanto area of Japan. Int. J. Biometeorol. 2014, 58, 941–948. [Google Scholar] [CrossRef] [PubMed]
- Zilli, I.; Ficca, G.; Salzarulo, P. Factors involved in sleep satisfaction in the elderly. Sleep Med. 2009, 10, 233–239. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, M.; Kimura, R.; Kido, Y.; Inoue, T.; Moritani, T.; Nagai, N. Color of hot soup modulates postprandial satiety, thermal sensation, and body temperature in young women. Appetite 2017, 114, 209–216. [Google Scholar] [CrossRef] [PubMed]
- Wang, S.Y. Effect of High Protein Breakfast on Intake, Appetite and Weight. Ph.D. Thesis, Chinese People’s Liberation Army Medical College, Beijing, China, 2014. [Google Scholar]
- Liu, Y.J. The physiological changes during sleep. World J. Sleep Med. 2017, 4, 6–17. [Google Scholar]
- Wakamura, T.; Tokura, H. Circadian rhythm of rectal temperature in humans under different ambient temperature cycles. J. Therm. Biol. 2002, 27, 439–447. [Google Scholar] [CrossRef]
- Schweiker, M.; Huebner, G.M.; Kingma, B.R.M.; Kramer, R.; Pallubinsky, H. Drivers of diversity in human thermal perception—A review for holistic comfort models. Temperature 2018, 5, 308–342. [Google Scholar] [CrossRef] [PubMed]
- Ko, Y.L.; Lee, J.Y. Effects of feet warming using bed socks on sleep quality and thermoregulatory responses in a cool environment. J. Physiol. Anthropol. 2018, 37, 13. [Google Scholar] [CrossRef]
- Zhang, Y.F. Effects of thermal environment on sleep. HVAC 2016, 46, 55–61. [Google Scholar]
- Parmeggiani, P.L. Interaction between sleep and thermoregulation: An aspect of the control of behavioral states. Sleep 1987, 10, 426–435. [Google Scholar] [CrossRef]
- Van Someren, E.J. Sleep propensity is modulated by circadian and behavior—Induced changes in cutaneous temperature. J. Therm. Biol. 2004, 29, 437–444. [Google Scholar] [CrossRef]
- Silanikove, N. Effects of water scarcity and hot environment on appetite and digestion in ruminants: A review. Livest. Prod. Sci. 1992, 30, 175–194. [Google Scholar] [CrossRef]
- Liu, Y.H. Physiological mechanism and nutrients supplements of high temperature affecting human health. J. Liaoning Teach. Coll. 2006, 2, 66–67. [Google Scholar]
- Janssen, P.; Vanden, B.P.; Verschueren, S.; Lehmann, A.; Depoortere, I.; Tack, J. The role of gastric motility in the control of food intake. Aliment. Pharmacol. Ther. 2011, 33, 880–894. [Google Scholar] [CrossRef] [PubMed]
- Huang, S.H.; Sheng, Y.Q. The Influence of high temperature and high humidity environment on human emotion. China Med. Sci. 2016, 6, 221–228. [Google Scholar]
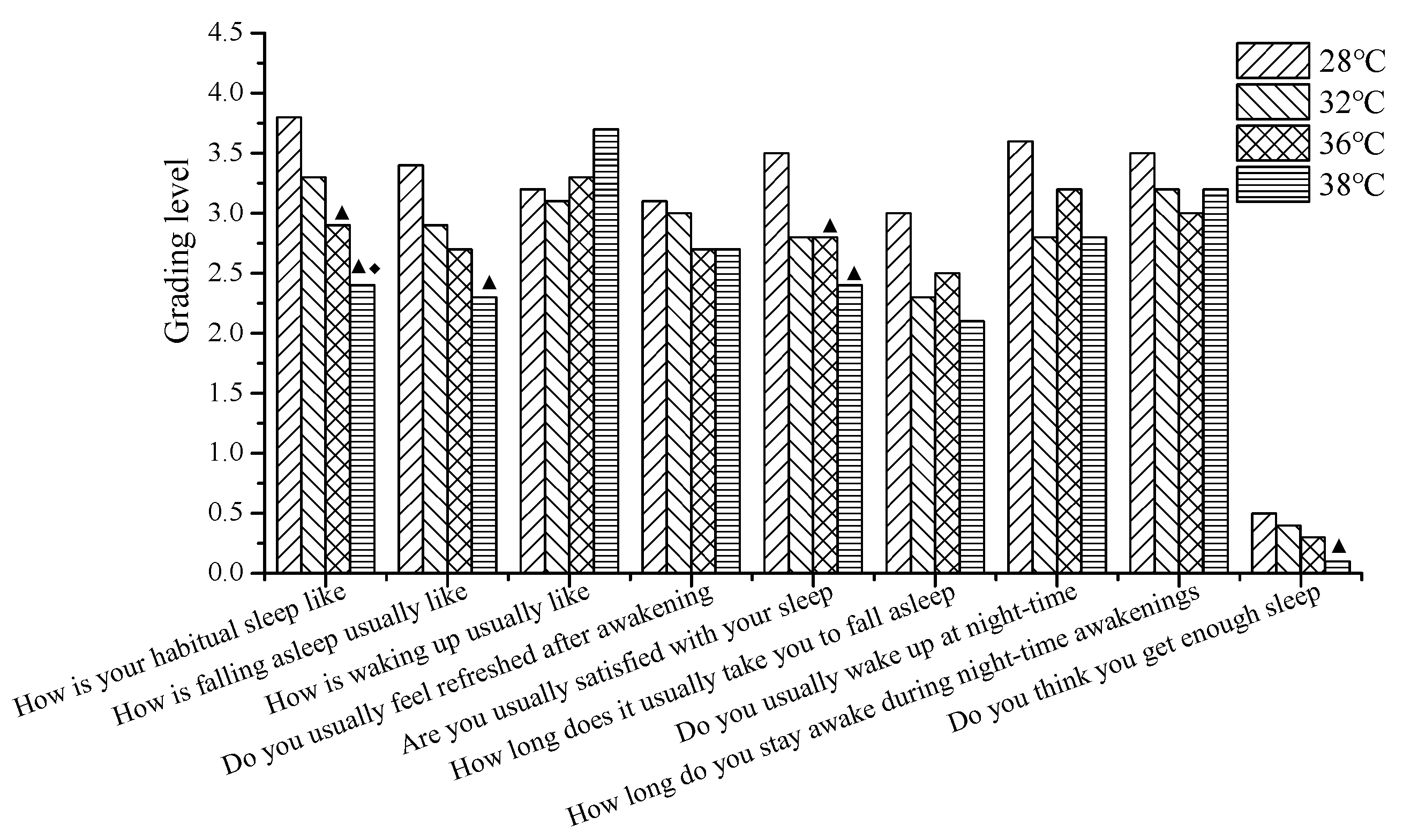
| Gender | Age (years old) | Height (cm) | Weight (kg) | BMI a (kg/m2) |
|---|---|---|---|---|
| Male | 22.4 ± 1.7 | 172.2 ± 5.1 | 69.2 ± 12.2 | 23.2 ± 2.9 |
| Female | 23.0 ± 1.4 | 161.4 ± 4.7 | 53.8 ± 8.1 | 20.6 ± 2.8 |
| Parameter | Instrument | Model | Precision |
|---|---|---|---|
| Outdoor temperature | Thermal index meter | AZ8778 | ±0.6 °C |
| Objective sleep quality | Sleep monitoring belt | Z101 | / |
| Subjective sleep quality | Sleep questionnaire | / | ±0.1 °C |
| Meal weight | Electronic scale | EK813 | ±1 g |
| Meal time | Watch | / | ±1 min |
| Subjective appetite | VAS scale | / | / |
| Questions | Score | |||||
|---|---|---|---|---|---|---|
| 5 | 4 | 3 | 2 | 1 | 0 | |
| How is your habitual sleep like? | Very calm | Fairly calm | Neither calm nor restless | Quite restless | Very restless | / |
| How is falling asleep usually like? | Very easy | Fairly easy | Neither easy nor difficult | Quite difficult | Very difficult | / |
| How is waking up usually like? | Very easy | Fairly easy | Neither easy nor difficult | Quite difficult | Very difficult | / |
| Do you usually feel refreshed after awakening? | Fully | Fairly | Moderately | Not much | Not at all | / |
| Are you usually satisfied with your sleep? | Fully | Fairly | Moderately | Not much | Not at all | / |
| Do you think you get enough sleep? | / | / | / | / | Yes | No |
| How long does it usually take you to fall asleep? | <5 min | 5–10 min | 10–20 min | 20–30 min | >30 min | / |
| Do you usually wake up at night-time? | Never | Seldom | Sometimes | Often | Always | / |
| How long do you stay awake during night-time awakenings? | 0 | <5 min | 5–15 min | 15–30 min | 30–60 min | / |
| Item | VAS Scale |
|---|---|
| Desire to eat |  |
| Hunger | 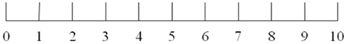 |
| Prospective consumption | 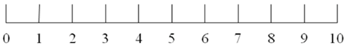 |
| Fullness | 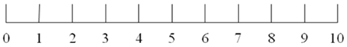 |
| Food greasy |  |
| Index | Meal | Objective Appetite | |||
|---|---|---|---|---|---|
| 28 °C | 32 °C | 36 °C | 38 °C | ||
| Meal weight (g) | Breakfast | 398.9 ± 170.1 | 389.8 ± 160.5 | 447.2 ± 182.4 | 389.8 ± 153.5 |
| Lunch | 529.1 ± 178.6 | 614.6 ± 240.1 | 507.7 ± 225.1 | 568.2 ± 146.9 | |
| Supper | 570.9 ± 321.2 | 567.8 ± 266.9 | 471.4 ± 159.9 | 530.7 ± 165.9 | |
| Meal time (min) | Breakfast | 9.4 ± 4.2 | 10.9 ± 2.9 | 11.6 ± 4.3 | 8.5 ± 4.2 |
| Lunch | 13.3 ± 8.2 | 19.8 ± 7.9 | 10.6 ± 3.9 | 16.9 ± 3.9 | |
| Supper | 12.6 ± 3.2 | 14.9 ± 6.8 | 15.7 ± 5.4 | 14.1 ± 5.5 | |
| Index | Meal | Subjective Appetite | |||
|---|---|---|---|---|---|
| 28 °C | 32 °C | 36 °C | 38 °C | ||
| Desire to eat | Breakfast | 4.0 ± 2.3 | 4.4 ± 1.8 | 5.3 ± 2.1 | 4.8 ± 1.8 |
| Lunch | 5.0 ± 1.6 | 5.5 ± 0.9 | 3.7 ± 1.5 ◆ | 4.8 ± 1.8 | |
| Supper | 5.7 ± 1.2 | 5.6 ± 1.3 | 6.1 ± 1.7 | 5.8 ± 1.8 | |
| Hunger | Breakfast | 4.7 ± 2.6 | 4.4 ± 0.9 | 5.3 ± 1.9 | 4.4 ± 1.2 |
| Lunch | 4.8 ± 1.8 | 5.4 ± 1.2 | 3.2 ± 1.8 ◆ | 5.1 ± 2.1 | |
| Supper | 5.6 ± 1.1 | 5.4 ± 1.6 | 6.0 ± 1.4 | 6.2 ± 1.5 | |
| Prospective consumption | Breakfast | 4.2 ± 2.6 | 4.4 ± 1.1 | 5.6 ± 2.4 | 4.7 ± 1.6 |
| Lunch | 5.5 ± 2.1 | 5.9 ± 1.3 | 3.7 ± 1.8 ◆ | 5.4 ± 2.3 | |
| Supper | 5.9 ± 1.4 | 5.4 ± 1.4 | 5.6 ± 1.4 | 6.2 ± 1.6 | |
| Fullness | Breakfast | 5.0 ± 1.6 | 4.6 ± 1.7 | 4.6 ± 2.1 | 5.0 ± 1.9 |
| Lunch | 5.3 ± 1.7 | 6.8 ± 1.9 ▲ | 5.7 ± 0.8 | 5.1 ± 1.6 ◆ | |
| Supper | 5.5 ± 1.4 | 6.9 ± 1.8 | 6.4 ± 1.4 | 5.6 ± 1.8 ◆ | |
| Food greasy | Breakfast | 2.5 ± 2.5 | 3.9 ± 1.6 | 4.9 ± 2.1 | 4.8 ± 2.7 |
| Lunch | 5.5 ± 1.1 | 7.7 ± 2.0 ▲ | 5.6 ± 0.9 ◆ | 4.8 ± 2.5 ◆ | |
| Supper | 5.9 ± 1.6 | 5.8 ± 1.5 | 5.1 ± 1.2 | 5.5 ± 1.3 | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zheng, G.; Li, K.; Wang, Y. The Effects of High-Temperature Weather on Human Sleep Quality and Appetite. Int. J. Environ. Res. Public Health 2019, 16, 270. https://doi.org/10.3390/ijerph16020270
Zheng G, Li K, Wang Y. The Effects of High-Temperature Weather on Human Sleep Quality and Appetite. International Journal of Environmental Research and Public Health. 2019; 16(2):270. https://doi.org/10.3390/ijerph16020270
Chicago/Turabian StyleZheng, Guozhong, Ke Li, and Yajing Wang. 2019. "The Effects of High-Temperature Weather on Human Sleep Quality and Appetite" International Journal of Environmental Research and Public Health 16, no. 2: 270. https://doi.org/10.3390/ijerph16020270
APA StyleZheng, G., Li, K., & Wang, Y. (2019). The Effects of High-Temperature Weather on Human Sleep Quality and Appetite. International Journal of Environmental Research and Public Health, 16(2), 270. https://doi.org/10.3390/ijerph16020270




