The Short-Term Effects of Ambient Air Pollutants on Childhood Asthma Hospitalization in Taiwan: A National Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Asthma Hospitalization Data
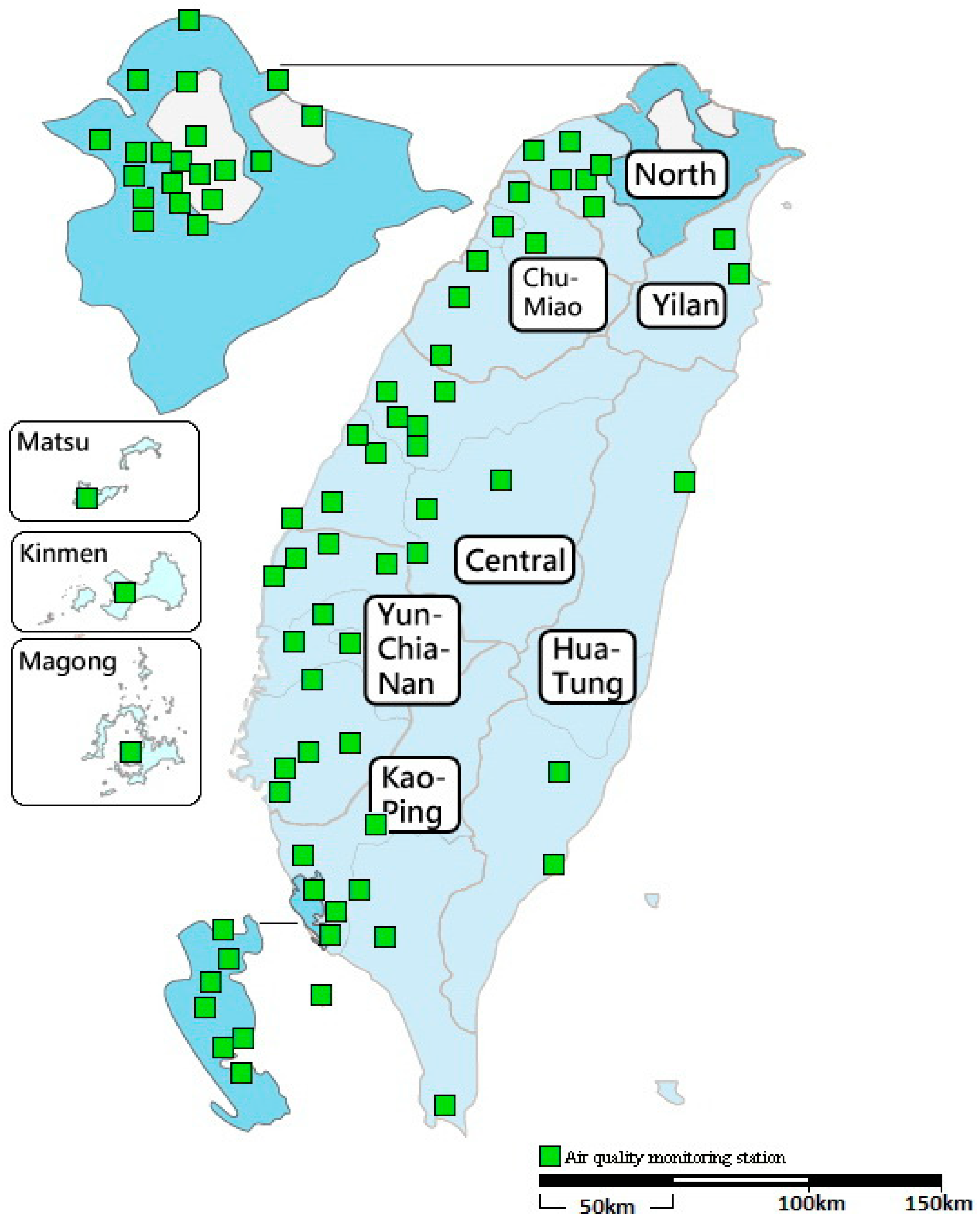
2.2. Air Pollution and Meteorological Data
2.3. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Duijts, L. Fetal and infant origins of asthma. Eur. J. Epidemiol. 2012, 27, 5–14. [Google Scholar] [CrossRef]
- Iskandar, A.; Andersen, Z.J.; Bønnelykke, K.; Ellermann, T.; Andersen, K.K.; Bisgaard, H. Coarse and fine particles but not ultrafine particles in urban air trigger hospital admission for asthma in children. Thorax 2011, 67, 252–257. [Google Scholar] [CrossRef] [PubMed]
- Hasegawa, K.; Tsugawa, Y.; Brown, D.F.; Camargo, C.A. Childhood asthma hospitalizations in the United States, 2000–2009. J. Pediatr. 2013, 163, 1127.e3–1133.e3. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Ambient Air Pollution—A Major Threat to Health and Climate. Available online: https://www.who.int/airpollution/ambient/en/ (accessed on 27 December 2018).
- Ross, K.; Chmiel, J.F.; Ferkol, T. The impact of the Clean Air Act. J. Pediatr. 2012, 161, 781–786. [Google Scholar] [CrossRef] [PubMed]
- Zheng, X.-Y.; Ding, H.; Jiang, L.-N.; Chen, S.-W.; Zheng, J.-P.; Qiu, M.; Zhou, Y.-X.; Chen, Q.; Guan, W.-J. Association between air pollutants and asthma emergency room visits and hospital admissions in time series studies: A systematic review and meta-analysis. PLoS ONE 2015, 10, e0138146. [Google Scholar] [CrossRef] [PubMed]
- National Health Insurance Administration. Background of National Health Insurance Research Database Taiwan: National Health Insurance Administration, Ministry of Health and Welfare. Available online: http://nhird.nhri.org.tw/en/index.html (accessed on 27 August 2018).
- Chen, R.; Chu, C.; Tan, J.; Cao, J.; Song, W.; Xu, X.; Jiang, C.; Ma, W.; Yang, C.; Chen, B. Ambient air pollution and hospital admission in Shanghai, China. J. Hazard. Mater. 2010, 181, 234–240. [Google Scholar] [CrossRef] [PubMed]
- Dominici, F.; Peng, R.D.; Barr, C.D.; Bell, M.L.J.E. Protecting human health from air pollution: Shifting from a single-pollutant to a multi-pollutant approach. Epidemiology 2010, 21, 187. [Google Scholar] [CrossRef]
- Sun, Z.; Tao, Y.; Li, S.; Ferguson, K.K.; Meeker, J.D.; Park, S.K.; Batterman, S.A.; Mukherjee, B.J.E.H. Statistical strategies for constructing health risk models with multiple pollutants and their interactions: Possible choices and comparisons. Environ. Health 2013, 12, 85. [Google Scholar] [CrossRef]
- Nascimento, L.F.C.; Vieira, L.C.P.F.; Mantovani, K.C.C.; Moreira, D.S. Air pollution and respiratory diseases: Ecological time series. Sao Paulo Med. J. 2016, 134, 315–321. [Google Scholar] [CrossRef]
- Samoli, E.; Nastos, P.; Paliatsos, A.; Katsouyanni, K.; Priftis, K. Acute effects of air pollution on pediatric asthma exacerbation: Evidence of association and effect modification. Environ. Res. 2011, 111, 418–424. [Google Scholar] [CrossRef]
- Nhung, N.T.T.; Schindler, C.; Dien, T.M.; Probst-Hensch, N.; Perez, L.; Künzli, N. Acute effects of ambient air pollution on lower respiratory infections in hanoi children: An eight-year time series study. Environ. Int. 2018, 110, 139–148. [Google Scholar] [CrossRef] [PubMed]
- Amâncio, C.T.; Nascimento, L.F.C. Asthma and ambient pollutants: A time series study. Revista da Associação Médica Brasileira 2012, 58, 302–307. [Google Scholar]
- Jung, C.-R.; Young, L.-H.; Hsu, H.-T.; Lin, M.-Y.; Chen, Y.-C.; Hwang, B.-F.; Tsai, P.-J. PM2.5 components and outpatient visits for asthma: A time-stratified case-crossover study in a suburban area. Environ. Pollut. 2017, 231, 1085–1092. [Google Scholar] [CrossRef] [PubMed]
- Wyzga, R.E.; Rohr, A. Long-term particulate matter exposure: Attributing health effects to individual PM components. J. Air Waste Manag. Assoc. 2015, 65, 523–543. [Google Scholar] [CrossRef] [PubMed]
- Ueda, K.; Nitta, H.; Odajima, H. The effects of weather, air pollutants, and Asian dust on hospitalization for asthma in Fukuoka. Environ. Health Prev. Med. 2010, 15, 350–357. [Google Scholar] [CrossRef] [PubMed]
- Hwang, B.-F.; Lee, Y.-L.; Lin, Y.-C.; Jaakkola, J.J.; Guo, Y.J.T. Traffic related air pollution as a determinant of asthma among Taiwanese school children. Thorax 2005, 60, 467–473. [Google Scholar] [CrossRef] [PubMed]
- Orellano, P.; Quaranta, N.; Reynoso, J.; Balbi, B.; Vasquez, J. Effect of outdoor air pollution on asthma exacerbations in children and adults: Systematic review and multilevel meta-analysis. PLoS ONE 2017, 12, e0174050. [Google Scholar] [CrossRef]
- Guarnieri, M.; Balmes, J.R. Outdoor air pollution and asthma. Lancet 2014, 383, 1581–1592. [Google Scholar] [CrossRef]
- Reno, A.L.; Brooks, E.G.; Ameredes, B.T. Mechanisms of heightened airway sensitivity and responses to inhaled SO2 in asthmatics. Environ. Health Insights 2015, 9, EHI-S15671. [Google Scholar] [CrossRef]
- Deger, L.; Plante, C.; Jacques, L.; Goudreau, S.; Perron, S.; Hicks, J.; Kosatsky, T.; Smargiassi, A. Active and uncontrolled asthma among children exposed to air stack emissions of sulphur dioxide from petroleum refineries in Montreal, Quebec: A cross-sectional study. Can. Respir. J. 2012, 19, 97–102. [Google Scholar] [CrossRef]
- Nieminen, P.; Panychev, D.; Lyalyushkin, S.; Komarov, G.; Nikanov, A.; Borisenko, M.; Kinnula, V.L.; Toljamo, T. Environmental exposure as an independent risk factor of chronic bronchitis in northwest Russia. Int. J. Circumpolar Health 2013, 72, 19742. [Google Scholar] [CrossRef] [PubMed]
- Cai, C.; Xu, J.; Zhang, M.; Chen, X.D.; Li, L.; Wu, J.; Lai, H.W.; Zhong, N.S. Prior SO2 exposure promotes airway inflammation and subepithelial fibrosis following repeated ovalbumin challenge. Clin. Exp. Allergy 2008, 38, 1680–1687. [Google Scholar] [CrossRef]
- Gouveia, N.; Corrallo, F.P.; Leon, A.C.P.D.; Junger, W.; Freitas, C.U.D. Air pollution and hospitalizations in the largest Brazilian metropolis. Revista de Saude Publica 2017, 51, 117. [Google Scholar] [CrossRef] [PubMed]
- Esposito, S.; Tenconi, R.; Lelii, M.; Preti, V.; Nazzari, E.; Consolo, S.; Patria, M.F. Possible molecular mechanisms linking air pollution and asthma in children. BMC Pulm. Med. 2014, 14, 31. [Google Scholar] [CrossRef] [PubMed]
- Bowatte, G.; Lodge, C.; Lowe, A.; Erbas, B.; Perret, J.; Abramson, M.; Matheson, M.; Dharmage, S. The influence of childhood traffic-related air pollution exposure on asthma, allergy and sensitization: A systematic review and a meta-analysis of birth cohort studies. Allergy 2015, 70, 245–256. [Google Scholar] [CrossRef]
- Grineski, S.E.; Staniswalis, J.G.; Bulathsinhala, P.; Peng, Y.; Gill, T.E. Hospital admissions for asthma and acute bronchitis in El Paso, Texas: Do age, sex, and insurance status modify the effects of dust and low wind events? Environ. Res. 2011, 111, 1148–1155. [Google Scholar] [CrossRef] [PubMed]
- Altzibar, J.M.; Tamayo-Uria, I.; De Castro, V.; Aginagalde, X.; Albizu, M.V.; Lertxundi, A.; Benito, J.; Busca, P.; Antepara, I.; Landa, J.; et al. Epidemiology of asthma exacerbations and their relation with environmental factors in the Basque Country. Clin. Exp. Allergy 2015, 45, 1099–1108. [Google Scholar] [CrossRef]
- Kanatani, K.T.; Ito, I.; Al-Delaimy, W.K.; Adachi, Y.; Mathews, W.C.; Ramsdell, J.W.; Toyama Asian Desert, D.; Asthma Study, T. Desert dust exposure is associated with increased risk of asthma hospitalization in children. Am. J. Respir. Crit. Care Med. 2010, 182, 1475–1481. [Google Scholar] [CrossRef]
- Sheffield, P.E.; Zhou, J.; Shmool, J.L.; Clougherty, J.E. Ambient ozone exposure and children’s acute asthma in New York City: A case-crossover analysis. Environ. Health 2015, 14, 25. [Google Scholar] [CrossRef]
- Clougherty, J.E. A growing role for gender analysis in air pollution epidemiology. Environ. Health Perspect. 2009, 118, 167–176. [Google Scholar] [CrossRef]
- Weichenthal, S.; Belisle, P.; Lavigne, E.; Villeneuve, P.J.; Wheeler, A.; Xu, X.; Joseph, L. Estimating risk of emergency room visits for asthma from personal versus fixed site measurements of NO2. Environ. Res. 2015, 137, 323–328. [Google Scholar] [CrossRef] [PubMed]
- Wendt, J.K.; Symanski, E.; Stock, T.H.; Chan, W.; Du, X.L. Association of short-term increases in ambient air pollution and timing of initial asthma diagnosis among Medicaid-enrolled children in a metropolitan area. Environ. Res. 2014, 131, 50–58. [Google Scholar] [CrossRef] [PubMed]
| Region | Northern | Chu-Miao | Central | Yun-Chia-Nan | Kao-Ping | Yilan | Hua-Tung | Outlying Islands | Total | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | n | % | n | % | n | % | n | % | n | % | n | % | |
| Total subjects | 22,482 | 100 | 4105 | 100 | 11,222 | 100 | 8608 | 100 | 8657 | 100 | 2387 | 100 | 1410 | 100 | 329 | 100 | 59,204 | 100 |
| Age (years) | ||||||||||||||||||
| 0–2 | 4177 | 18.58 | 819 | 19.95 | 1833 | 16.33 | 2309 | 26.82 | 1403 | 16.21 | 396 | 16.59 | 393 | 27.87 | 51 | 15.50 | 11,382 | 19.23 |
| 3–5 | 10,326 | 45.93 | 1656 | 40.34 | 4526 | 40.33 | 3497 | 40.63 | 3515 | 40.60 | 892 | 37.37 | 473 | 33.55 | 158 | 48.02 | 25,043 | 42.30 |
| 6–18 | 7979 | 35.49 | 1630 | 39.71 | 4863 | 43.33 | 2802 | 32.55 | 3739 | 43.19 | 1099 | 46.04 | 544 | 38.58 | 120 | 36.47 | 22,779 | 38.48 |
| Gender | ||||||||||||||||||
| Male | 14,588 | 64.89 | 2529 | 61.61 | 7275 | 64.83 | 5431 | 63.09 | 5398 | 62.35 | 1508 | 63.18 | 862 | 61.13 | 232 | 70.52 | 37,825 | 63.89 |
| Female | 7894 | 35.11 | 1576 | 38.39 | 3947 | 35.17 | 3177 | 36.91 | 3259 | 37.65 | 879 | 36.82 | 548 | 38.87 | 97 | 29.48 | 21,379 | 36.11 |
| Season | ||||||||||||||||||
| Spring | 5951 | 26.47 | 1108 | 26.99 | 3079 | 27.44 | 2383 | 27.68 | 2340 | 27.03 | 613 | 25.68 | 352 | 24.96 | 92 | 27.96 | 15,918 | 26.89 |
| Summer | 3986 | 17.73 | 780 | 19.00 | 2095 | 18.67 | 1656 | 19.24 | 1481 | 63.29 | 407 | 17.05 | 273 | 19.36 | 73 | 22.19 | 10,751 | 18.16 |
| Autumn | 4928 | 21.92 | 896 | 21.83 | 2522 | 22.47 | 1933 | 22.46 | 2069 | 23.90 | 534 | 22.37 | 333 | 23.62 | 83 | 25.23 | 13,298 | 22.46 |
| Winter | 7617 | 33.88 | 1321 | 32.18 | 3526 | 31.42 | 2636 | 30.62 | 2767 | 31.96 | 833 | 34.90 | 452 | 32.06 | 81 | 24.62 | 19,237 | 32.49 |
| Mean length of stay (days) | 3.54 | 4.25 | 3.68 | 3.55 | 4.23 | 3.79 | 4.51 | 3.89 | 3.93 | |||||||||
| Percentiles | ||||||||
|---|---|---|---|---|---|---|---|---|
| Pollutants | Mean | SD | Minimum | 25th | 50th | 75th | Maximum | p-Value * |
| PM2.5 (μg/m3) | ||||||||
| All regions | 33.15 | 20.22 | 0.01 | 16.45 | 26.62 | 41.42 | 234.71 | p < 0.001 |
| Northern | 27.21 | 15.53 | 0.59 | 14.96 | 23.13 | 33.46 | 206.21 | |
| Chu-Miao | 28.62 | 15.68 | 1.75 | 16.17 | 24.42 | 35.48 | 153.13 | |
| Central | 36.54 | 19.41 | 0.01 | 20.96 | 31.87 | 45.21 | 166.25 | |
| Yun-Chia-Nan | 38.33 | 20.24 | 1.25 | 21.46 | 33.54 | 48.04 | 234.71 | |
| Kao-Ping | 41.75 | 23.71 | 1 | 20.46 | 38.04 | 55.67 | 176.94 | |
| Yilan | 19.64 | 11.66 | 1.5 | 10.58 | 16.5 | 24.5 | 105.00 | |
| Hua-Tung | 16.43 | 9.55 | 1.67 | 8.96 | 13.62 | 19.88 | 90.50 | |
| Outlying islands | 32.08 | 21.15 | 1.33 | 15.47 | 26.25 | 41.08 | 174.21 | |
| PM10 (μg/m3) | ||||||||
| All regions | 57.82 | 33.51 | 1 | 30.96 | 47.33 | 71 | 772.71 | p < 0.001 |
| Northern | 48.94 | 26.34 | 1 | 28.83 | 42.46 | 59.3 | 510.58 | |
| Chu-Miao | 48.41 | 25.61 | 1 | 29.04 | 42.33 | 59.05 | 486.75 | |
| Central | 61.61 | 31.83 | 1 | 36.5 | 54 | 76.58 | 512.00 | |
| Yun-Chia-Nan | 68.94 | 35.93 | 5.13 | 39.17 | 61.33 | 86.23 | 594.38 | |
| Kao-Ping | 70.33 | 38.94 | 1 | 35.88 | 62.16 | 94.08 | 615.96 | |
| Yilan | 39.46 | 20.57 | 4.17 | 24.83 | 34.33 | 47.36 | 538.46 | |
| Hua-Tung | 32.01 | 17.89 | 1 | 20.33 | 27.25 | 36.92 | 313.46 | |
| Outlying islands | 59.04 | 38.85 | 4.52 | 30.17 | 47.58 | 71.75 | 772.71 | |
| O3 (ppb) | ||||||||
| All regions | 28.83 | 12.47 | 0.1 | 18.5 | 26.1 | 34.7 | 107.78 | p < 0.001 |
| Northern | 27.39 | 12.03 | 0.37 | 17.72 | 25.11 | 33.34 | 97.65 | |
| Chu-Miao | 28.89 | 10.98 | 0.5 | 20.01 | 27.04 | 34.84 | 84.18 | |
| Central | 27.49 | 11.09 | 0.13 | 18.45 | 25.52 | 33.32 | 83.12 | |
| Yun-Chia-Nan | 30.62 | 11.68 | 1.54 | 20.75 | 28.79 | 37.1 | 85.07 | |
| Kao-Ping | 30.02 | 13.78 | 0.13 | 17.9 | 27.69 | 38.47 | 93.83 | |
| Yilan | 25.99 | 10.54 | 0.62 | 17.66 | 24.86 | 31.98 | 78.52 | |
| Hua-Tung | 25.01 | 10.35 | 2.24 | 16.07 | 23.5 | 30.91 | 78.29 | |
| Outlying islands | 41.72 | 15.52 | 3.12 | 28.52 | 40.24 | 50.86 | 107.78 | |
| SO2 (ppb) | ||||||||
| All regions | 4.3 | 3.33 | 0.1 | 2.1 | 3.29 | 5 | 103.71 | p < 0.001 |
| Northern | 4.23 | 2.85 | 0.1 | 2.12 | 3.47 | 5.18 | 69.16 | |
| Chu-Miao | 3.39 | 2.04 | 0.1 | 2 | 3.01 | 4.1 | 36.98 | |
| Central | 3.32 | 1.85 | 0.1 | 2.01 | 2.91 | 4.03 | 68.58 | |
| Yun-Chia-Nan | 3.66 | 1.94 | 0.1 | 2.32 | 3.27 | 4.37 | 43.23 | |
| Kao-Ping | 6.39 | 4.49 | 0.1 | 2.87 | 5.16 | 7.98 | 53.43 | |
| Yilan | 2.19 | 1.42 | 0.1 | 1.24 | 1.9 | 2.63 | 22.03 | |
| Hua-Tung | 1.67 | 1.13 | 0.1 | 0.88 | 1.61 | 2.12 | 41.48 | |
| Outlying islands | 4.18 | 3.53 | 0.1 | 1.67 | 2.73 | 5.2 | 34.13 | |
| NO2 (ppb) | ||||||||
| All regions | 18.13 | 10.43 | 0.01 | 9.54 | 15.53 | 22.71 | 116.2 | p < 0.001 |
| Northern | 21.75 | 11.55 | 0.03 | 12.2 | 19.63 | 27.12 | 116.2 | |
| Chu-Miao | 15.44 | 6.29 | 0.28 | 10.62 | 13.98 | 18.5 | 51.4 | |
| Central | 18 | 8.54 | 0.01 | 10.9 | 16.03 | 22.21 | 76.03 | |
| Yun-Chia-Nan | 14.86 | 7.06 | 0.22 | 9.26 | 13.2 | 18.17 | 64.65 | |
| Kao-Ping | 19.75 | 12 | 0.02 | 10.05 | 17.54 | 25.75 | 103.77 | |
| Yilan | 11.22 | 3.96 | 0.84 | 8.01 | 10.42 | 13.15 | 27.76 | |
| Hua- Tung | 8.36 | 4.63 | 0.59 | 4.91 | 6.9 | 10 | 73.87 | |
| Outlying islands | 7.37 | 5.23 | 0.05 | 3.52 | 5.49 | 8.95 | 44.41 | |
| 0–18 Years Old | ||||||
|---|---|---|---|---|---|---|
| Single Pollutant Model | Multiple Pollutants Model | |||||
| Pollutants | RR | 95% CI | p-Value | RR | 95% CI | p-Value |
| PM2.5 | 1.156 *** | 1.142–1.170 | 0.000 | 0.968 ** | 0.948–0.988 | 0.002 |
| PM10 | 1.120 *** | 1.107–1.134 | 0.000 | 1.028 * | 1.005–1.050 | 0.015 |
| O3 | 0.969 *** | 0.957–0.981 | 0.000 | 0.950 *** | 0.937–0.964 | 0.000 |
| SO2 | 1.367 *** | 1.349–1.385 | 0.000 | 1.537 *** | 1.507–1.566 | 0.000 |
| NO2 | 1.065 *** | 1.053–1.076 | 0.000 | 0.862 *** | 0.849–0.874 | 0.000 |
| Single Pollutant Model | ||||||
| 0–5 Years Old | 6–18 Years Old | |||||
| Pollutants | RR | 95% CI | p-Value | RR | 95% CI | p-Value |
| PM2.5 | 1.190 *** | 1.172–1.208 | 0.000 | 1.088 *** | 1.067–1.109 | 0.000 |
| PM10 | 1.123 *** | 1.106–1.140 | 0.000 | 1.100 *** | 1.078–1.121 | 0.000 |
| O3 | 0.962 *** | 0.947–0.977 | 0.000 | 0.977 * | 0.958–0.997 | 0.025 |
| SO2 | 1.428 *** | 1.405–1.452 | 0.000 | 1.245 *** | 1.219–1.271 | 0.000 |
| NO2 | 1.060 *** | 1.045–1.075 | 0.000 | 1.064 *** | 1.045–1.082 | 0.000 |
| Multiple Pollutants Model | ||||||
| 0–5 Years Old | 6–18 Years Old | |||||
| Pollutants | RR | 95% CI | p-Value | RR | 95% CI | p-Value |
| PM2.5 | 1.008 | 0.982–1.035 | 0.526 | 0.909 *** | 0.879–0.939 | 0.000 |
| PM10 | 0.987 | 0.958–1.016 | 0.369 | 1.083 *** | 1.047–1.119 | 0.000 |
| O3 | 0.940 *** | 0.924–0.957 | 0.000 | 0.967 ** | 0.945–0.989 | 0.003 |
| SO2 | 1.647 *** | 1.607–1.689 | 0.000 | 1.346 *** | 1.306–1.387 | 0.000 |
| NO2 | 0.827 *** | 0.811–0.843 | 0.000 | 0.924 *** | 0.902–0.946 | 0.000 |
| Single Pollutant Model | ||||||
| Male | Female | |||||
| Pollutants | RR | 95% CI | p-Value | RR | 95% CI | p-Value |
| PM2.5 | 1.151 *** | 1.133–1.168 | 0.000 | 1.143 *** | 1.121–1.166 | 0.000 |
| PM10 | 1.115 *** | 1.098–1.131 | 0.000 | 1.113 *** | 1.091–1.136 | 0.000 |
| O3 | 0.965 *** | 0.950–0.980 | 0.000 | 0.968 ** | 0.968–0.988 | 0.002 |
| SO2 | 1.359 *** | 1.337–1.381 | 0.000 | 1.332 *** | 1.304–1.361 | 0.000 |
| NO2 | 1.063 *** | 1.049–1.078 | 0.000 | 1.051 *** | 1.032–1.070 | 0.000 |
| Multiple Pollutants Model | ||||||
| Male | Female | |||||
| Pollutants | RR | 95% CI | p-Value | RR | 95% CI | p-Value |
| PM2.5 | 0.970 * | 0.945–0.995 | 0.020 | 0.969 | 0.936–1.002 | 0.067 |
| PM10 | 1.023 | 0.995–1.052 | 0.099 | 1.037 * | 1.000–1.075 | 0.048 |
| O3 | 0.947 *** | 0.931–0.964 | 0.000 | 0.947 *** | 0.925–0.970 | 0.000 |
| SO2 | 1.525 *** | 1.489–1.562 | 0.000 | 1.495 *** | 1.448–1.543 | 0.000 |
| NO2 | 0.865 *** | 0.849–0.881 | 0.000 | 0.855 *** | 0.834–0.876 | 0.000 |
| Single Pollutant Model | ||||||
| Northern | Chu-Miao | |||||
| Pollutants | RR | 95%CI | p-Value | RR | 95%CI | p-Value |
| PM2.5 | 1.075 *** | 1.057–1.093 | 0.000 | 1.022 | 0.954–1.093 | 0.539 |
| PM10 | 1.038 *** | 1.021–1.054 | 0.000 | 1.020 | 0.953–1.090 | 0.560 |
| O3 | 0.989 | 0.970–1.008 | 0.237 | 0.981 | 0.911–1.055 | 0.598 |
| SO2 | 1.109 *** | 1.093–1.126 | 0.000 | 1.049 | 0.979–1.124 | 0.175 |
| NO2 | 0.995 | 0.977–1.014 | 0.610 | 1.022 | 0.964–1.082 | 0.459 |
| Central Taiwan | Yun-Chia-Nan | |||||
| Pollutants | RR | 95%CI | p-Value | RR | 95%CI | p-Value |
| PM2.5 | 1.026 * | 1.001–1.052 | 0.043 | 1.049 * | 1.005–1.094 | 0.027 |
| PM10 | 1.085 *** | 1.058–1.113 | 0.000 | 1.054 * | 1.008–1.099 | 0.018 |
| O3 | 0.952 *** | 0.926–0.979 | 0.000 | 0.992 | 0.951–1.0034 | 0.689 |
| SO2 | 1.216 *** | 1.182–1.251 | 0.000 | 1.152 *** | 1.094–1.213 | 0.000 |
| NO2 | 1.011 | 0.985–1.037 | 0.424 | 1.069 *** | 1.030–1.110 | 0.000 |
| Kao-Ping | Yilan | |||||
| Pollutants | RR | 95%CI | p-Value | RR | 95%CI | p-Value |
| PM2.5 | 1.083 *** | 1.045–1.123 | 0.000 | 0.995 | 0.924–1.070 | 0.899 |
| PM10 | 1.096 *** | 1.053–1.141 | 0.000 | 0.980 | 0.918–1.039 | 0.529 |
| O3 | 1.033 | 0.995–1.073 | 0.091 | 0.956 | 0.884–1.033 | 0.255 |
| SO2 | 1.185 *** | 1.129–1.244 | 0.000 | 1.070 | 0.987–1.160 | 0.101 |
| NO2 | 1.079 *** | 1.044–1115 | 0.000 | 1.025 | 0.964–1.088 | 0.416 |
| Hua-Tung | Outlying Islands | |||||
| Pollutants | RR | 95%CI | p-Value | RR | 95%CI | p-Value |
| PM2.5 | 0.986 | 0.901–1.077 | 0.764 | 1.026 | 0.849–1.23 | 0.784 |
| PM10 | 1.023 | 0.936–1.115 | 0.603 | 1.030 | 0.834–1.257 | 0.780 |
| O3 | 1.019 | 0.928–1.118 | 0.686 | 1.079 | 0.868–1.340 | 0.492 |
| SO2 | 0.977 | 0.882–1.080 | 0.652 | 1.023 | 0.857–1.210 | 0.794 |
| NO2 | 1.005 | 0.931–1.082 | 0.900 | 1.049 | 0.825–1.320 | 0.690 |
| Multiple Pollutants Model | ||||||
| Northern | Chu-Miao | |||||
| Pollutants | RR | 95% CI | p-Value | RR | 95% CI | p-Value |
| PM2.5 | 1.076 *** | 1.046–1.107 | 0.000 | 0.981 | 0.787–1.227 | 0.867 |
| PM10 | 0.977 | 0.949–1.006 | 0.126 | 1.003 | 0.812–1.228 | 0.980 |
| O3 | 0.965 *** | 0.946–0.986 | 0.000 | 0.993 | 0.914–1.077 | 0.859 |
| SO2 | 1.193 *** | 1.167–1.219 | 0.000 | 1.054 | 0.956–1.161 | 0.289 |
| NO2 | 0.833 *** | 0.809–0.856 | 0.000 | 1.009 | 0.935–1.088 | 0.807 |
| Central Taiwan | Yun-Chia-Nan | |||||
| Pollutants | RR | 95% CI | p-Value | RR | 95% CI | p-Value |
| PM2.5 | 0.860 *** | 0.822–0.901 | 0.054 | 0.917 | 0.839–1.003 | 0.059 |
| PM10 | 1.121 *** | 1.068–1.174 | 0.189 | 1.051 | 0.971–1.131 | 0.201 |
| O3 | 0.989 | 0.959–1.019 | 0.919 | 0.988 | 0.941–1.037 | 0.621 |
| SO2 | 1.347 *** | 1.292–1.404 | 0.000 | 1.178 *** | 1.092–1.271 | 0.000 |
| NO2 | 0.888 *** | 0.857–0.920 | 0.143 | 1.023 | 0.973–1.075 | 0.377 |
| Kao-Ping | Yilan | |||||
| Pollutants | RR | 95% CI | p-Value | RR | 95% CI | p-Value |
| PM2.5 | 0.992 | 0.933–1.055 | 0.794 | 1.023 | 0.881–1.192 | 0.767 |
| PM10 | 1.004 | 0.933–1.078 | 0.914 | 0.944 | 0.826–1.055 | 0.355 |
| O3 | 1.015 | 0.972–1.060 | 0.490 | 0.978 | 0.894–1.071 | 0.637 |
| SO2 | 1.172 *** | 1.086–1.265 | 0.000 | 1.073 | 0.973–1.184 | 0.160 |
| NO2 | 1.014 | 0.972–1.058 | 0.512 | 1.015 | 0.947–1.086 | 0.671 |
| Hua-Tung | Outlying islands | |||||
| Pollutants | RR | 95% CI | p-Value | RR | 95% CI | p-Value |
| PM2.5 | 0.914 | 0.791–1.059 | 0.231 | 0.957 | 0.605–1.51 | 0.850 |
| PM10 | 1.082 | 0.945–1.226 | 0.236 | 0.992 | 0.609–1.533 | 0.973 |
| O3 | 1.032 | 0.931-1.143 | 0.550 | 1.098 | 0.844-1.423 | 0.482 |
| SO2 | 0.972 | 0.873–1.079 | 0.598 | 1.021 | 0.805–1.279 | 0.857 |
| NO2 | 1.019 | 0.935–1.109 | 0.662 | 1.051 | 0.757–1.424 | 0.760 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kuo, C.-Y.; Chan, C.-K.; Wu, C.-Y.; Phan, D.-V.; Chan, C.-L. The Short-Term Effects of Ambient Air Pollutants on Childhood Asthma Hospitalization in Taiwan: A National Study. Int. J. Environ. Res. Public Health 2019, 16, 203. https://doi.org/10.3390/ijerph16020203
Kuo C-Y, Chan C-K, Wu C-Y, Phan D-V, Chan C-L. The Short-Term Effects of Ambient Air Pollutants on Childhood Asthma Hospitalization in Taiwan: A National Study. International Journal of Environmental Research and Public Health. 2019; 16(2):203. https://doi.org/10.3390/ijerph16020203
Chicago/Turabian StyleKuo, Ching-Yen, Chin-Kan Chan, Chiung-Yi Wu, Dinh-Van Phan, and Chien-Lung Chan. 2019. "The Short-Term Effects of Ambient Air Pollutants on Childhood Asthma Hospitalization in Taiwan: A National Study" International Journal of Environmental Research and Public Health 16, no. 2: 203. https://doi.org/10.3390/ijerph16020203
APA StyleKuo, C.-Y., Chan, C.-K., Wu, C.-Y., Phan, D.-V., & Chan, C.-L. (2019). The Short-Term Effects of Ambient Air Pollutants on Childhood Asthma Hospitalization in Taiwan: A National Study. International Journal of Environmental Research and Public Health, 16(2), 203. https://doi.org/10.3390/ijerph16020203





