Effectiveness of Diabetes Community Sharp Disposal Education Module in Primary Care: An Experimental Study in North-East Peninsular Malaysia
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Study Setting
2.2. Eligibility Criteria and Recruitment Process
2.3. Diabetes Community Sharp Disposal Education Module
2.4. Malay Version of Diabetes Community Sharp Disposal (M-DCSD) Questionnaire
2.5. Follow Up and Assessment
2.6. Sample Size Determination
2.7. Statistical Analysis
2.8. Ethical Consideration
3. Results
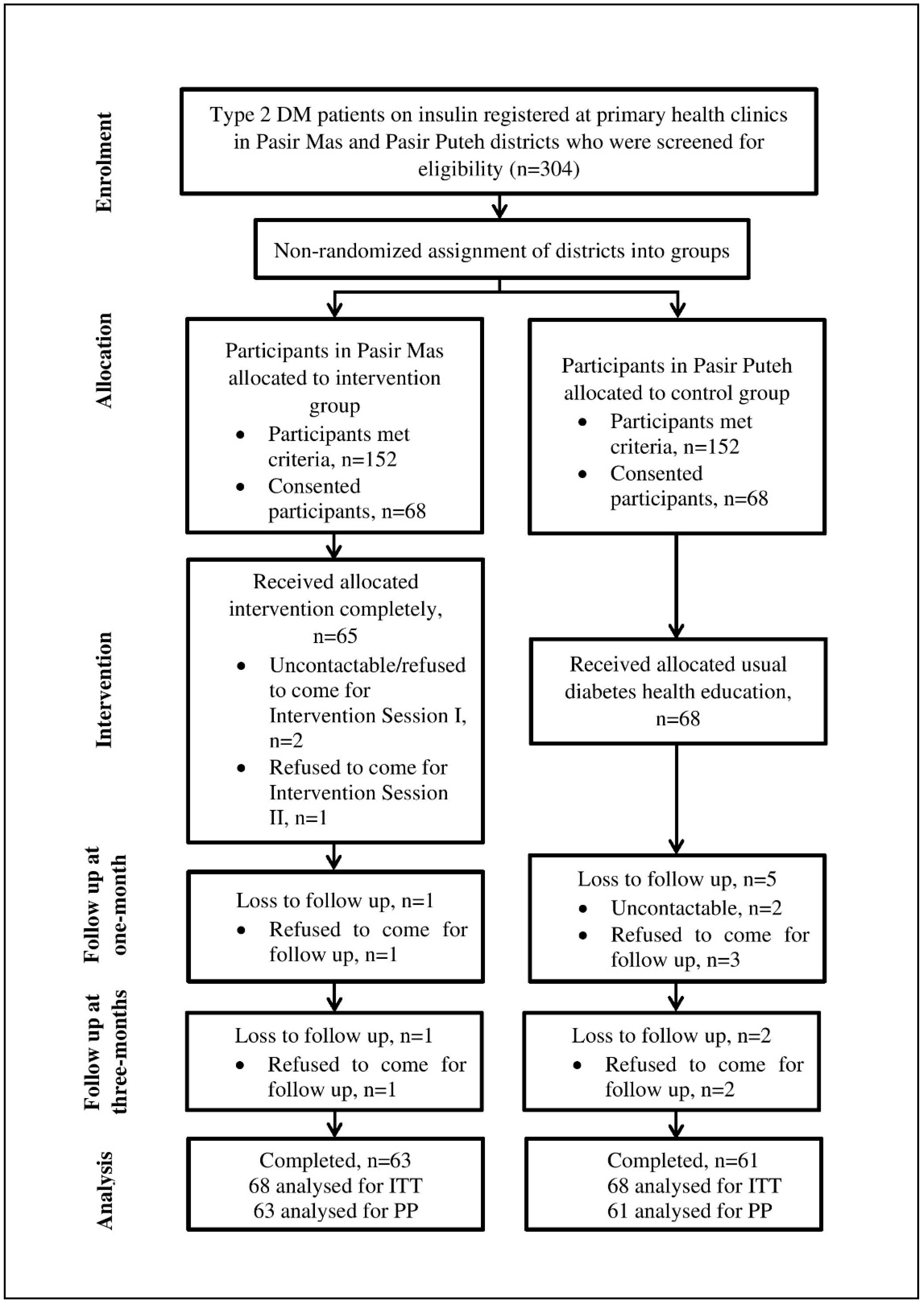
3.1. Subject Accrual
3.2. Groups Characteristics at Baseline
3.3. Effect of Intervention Using Intention to Treat Analysis
3.3.1. Knowledge Score
3.3.2. Community Sharp Disposal Practice
3.4. Effect of Intervention Using Per Protocol Analysis
3.4.1. Knowledge Score
3.4.2. Community Sharp Disposal Practice
4. Discussion
4.1. Effect of Intervention on Knowledge Scores
4.2. The Effect of Intervention on Community Sharp Disposal Practice
4.3. Study Limitations
4.4. Future Research
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- WHO. Global Report on Diabetes; WHO: Geneva, Switzerland, 2016; Available online: http://www.who.int/diabetes/global-report/en/ (accessed on 12 August 2017).
- MOH. National Health and Morbidity Survey; MOH: Putrajaya, Malaysia, 2015. Available online: http://www.iku.gov.my/index.php/research-eng/list-of-research-eng/iku-eng/nhms-eng/nhms-2015 (accessed on 12 August 2017).
- Wan Nazaimoon, W.M.; Md Isa, S.H.; Wan Mohamad WBKhir, A.S.; Kamaruddin, N.A.; Kamarul Imran, M.; Mustafa, N.; Ismail ISAli, O.; Khalid, B.A.K. Prevalence of diabetes in Malaysia and usefulness of HbA1c as a diagnostic criterion. Diabet. Med. 2013, 30, 825–828. [Google Scholar] [CrossRef] [PubMed]
- MOH. Clinical Practice Guidelines: Management of Type 2 Diabetes Mellitus, 5th ed.; MOH: Putrajaya, Malaysia, 2015; Available online: http://www.acadmed.org.my/index.cfm?&menuid=67 (accessed on 15 August 2017).
- MOH. National Diabetes Registry Report 2009–2012; MOH: Putrajaya, Malaysia, 2013. Available online: http://www.moh.gov.my/index.php/pages/view/1779 (accessed on 12 August 2017).
- Aida, J.; Saharuddin, A.; Muhamed, O.; Mohd Radzniwan, R.; Mohd Rohaizat, H.; Ziti, A.S. Education of correct insulin injection technique amongst diabetic patients: Outcome study from Malaysia. Int. J. Med. Res. Health Sci. 2016, 5, 198–205. [Google Scholar]
- Singh, A.P.; Chapman, R.S. Knowledge, attitude and practices (KAP) on disposal of sharp waste, used for home management of Type 2 Diabetes Mellitus, in New Delhi, India. J. Health Res. 2011, 25, 135–140. [Google Scholar]
- WHO. Safe Management of Wastes from Health-Care Activities. 2014. Available online: https://www.who.int/water_sanitation_health/publications/wastemanag/en/ (accessed on 15 January 2018).
- WHO. Fact Sheet. Health-Care Waste. 2018. Available online: https://www.who.int/news-room/fact-sheets/detail/health-care-waste (accessed on 20 April 2018).
- Kalra, S.; Girdhar, R.; Sahay, R. Green diabetology. Indian J. Endocrinol. Metab. 2015, 19, 698–700. [Google Scholar] [CrossRef] [PubMed]
- Govender, D.; Ross, A. Sharps disposal practices among diabetic patients using insulin. S. Afr. Med. J. 2012, 102, 1–5. [Google Scholar] [CrossRef]
- Basazn Mekuria, A.; Melaku Gebresillassie, B.; Asfaw Erku, D.; Taye Haile, K.; Melese Birru, E. Knowledge and self-reported practice of insulin injection device disposal among diabetes patients in Gondar Town, Ethiopia: A cross-sectional study. J. Diabetes Res. 2016, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Ishtiaq, O.; Qadri, A.M.; Mehar, S.; Gondal, G.M.; Iqbal, T.; Ali, S.; Mati ur, R.; Janjua, N.Z. Disposal of syringes, needles, and lancets used by diabetic patients in Pakistan. J. Infect. Public Health 2012, 5, 182–188. [Google Scholar] [CrossRef] [PubMed]
- Costello, J.; Parikh, A. The sticking point: Diabetic sharps disposal practices in the community. J. Gen. Intern. Med. 2013, 28, 868–869. [Google Scholar] [CrossRef] [PubMed]
- Musselman, K.T.; Sicat, B.L.; Thomas, M.H.; Harpe, S.E. Patients’ knowledge of and practices relating to the disposal of used insulin needles. Innov. Pharm. 2010, 1, 1–10. [Google Scholar] [CrossRef]
- Majumdar, A.; Sahoo, J.; Roy, G.; Kamalanathan, S. Improper sharp disposal practices among diabetes patients in home care settings: Need for concern? Indian J. Endocrinol. Metab. 2015, 19, 420–425. [Google Scholar] [CrossRef]
- Gold, K. Analysis: The impact of needle, syringe, and lancet disposal on the community. J. Diabetes Sci. Technol. 2011, 5, 848–850. [Google Scholar] [CrossRef] [PubMed]
- Quiwa, L.; Jimeno, C. Knowledge, attitudes and practices on the disposal of sharps in patients of the UP-Philippine General Hospital Diabetes Clinic. J. ASEAN Fed. Endocr. Soc. 2014, 29, 141. [Google Scholar] [CrossRef]
- Cunha, G.H.; Barbosa, R.V.A.; Fontenele, M.S.M.; Lima, M.A.C.; Franco, K.B.; Fechine, F.V. Insulin therapy waste produced in the households of people with diabetes monitored in primary care. Braz. J. Nurs. 2017, 70, 618–625. [Google Scholar] [CrossRef] [PubMed]
- Furth, R.; Anderson, A.; Krishendat, G. Safer insulin needle use and disposal. Int. J. Infect. Control 2010, 6, 1–10. [Google Scholar] [CrossRef]
- Atukorala, K.; Wickramasinghe, S.; Sumanasekera, R. Practices related to sharps disposal among diabetic patients in Sri Lanka. Asia Pac. Fam. Med. 2018, 17, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Dorothy, L.M.; Robert, B.; Nova, S.; Joan, L.R.; Lindy, M.S. Needle stick injuries in the community. Paediatr. Child Health 2008, 13, 205–210. [Google Scholar]
- Jason, J. Community-acquired, non-occupational needlestick injuries treated in US Emergency Departments. J. Public Health 2013, 35, 422–430. [Google Scholar] [CrossRef]
- Udofia, E.A.; Gulis, G.; Fobil, J. Solid medical waste: A cross sectional study of household disposal practices and reported harm in Southern Ghana. BMC Public Health 2017, 17, 1–12. [Google Scholar] [CrossRef]
- EPA. Community Options for Safe NEEDLE Disposal. 2004. Available online: https://www.epa.gov/rcra/community-options-safe-needle-disposal (accessed on 12 September 2017).
- Debbie, H.; Debra, A.; Su, D.; David, M.; Fiona, K.; Hillary, W.; Joan, A.; June, J.; Patricia, C.; Sian, B.; et al. Injection Safety in UK and Ireland; Safety of Sharps in Diabetes Recommendations FIT4Safety (1st ed.). 2012. Available online: http://www.fit4diabetes.com/united-kingdom/fit-safety-recommendations/ (accessed on 12 February 2019).
- FDA. Safely Using Sharps (Needles and Syringes) at Home, at Work and on Travel. 2014. Available online: https://www.fda.gov/MedicalDevices/ProductsandMedicalProcedures/HomeHealthandConsumer/ConsumerProducts/Sharps/default.htm (accessed on 8 September 2017).
- Department of Statistics Malaysia. Population and Housing Census Malaysia 2010. Available online: https://www.dosm.gov.my/v1/index.php?r=home/index&menu_id=b2ROaWpITmQ5NnAvMHVmRjRkZzlBQT09 (accessed on 12 January 2019).
- Kelantan State Health Department. Primary Health Clinics in Kelantan; Kelantan State Health Department: Kelantan, Malaysia, 2017; Unpublished work.
- Kelantan State Health Department. Medications Used for Type 2 Diabetic Patients in Kelantan; Kelantan State Health Department: Kelantan, Malaysia, 2017; Unpublished work.
- Hasan, U.A.; Mohd Hairon, S.; Yaacob, N.M.; Daud, A.; Abdul Hamid, A.; Hassan, N.; Ariffin, M.F.; Yi Vun, L. Factors Contributing to Sharp Waste Disposal at Health Care Facility Among Diabetic Patients in North-East Peninsular Malaysia. Int. J. Environ. Res. Public Health 2019, 16, 2251. [Google Scholar] [CrossRef]
- EPA. Handle with Care. 2003. Available online: https://www.epa.gov/rcra/medical-waste (accessed on 7 September 2017).
- MOH. Practical Guide to Insulin Therapy in Type 2 Diabetes; MOH: Putrajaya, Malaysia, 2011; Available online: http://www.mems.my/article.php?aid=372 (accessed on 5 May 2017).
- Kelantan State Health Department. Diabetes Education Module; Kelantan State Health Department: Kelantan, Malaysia, 2012.
- FDA. Sharps Disposal Containers. 2013. Available online: https://www.fda.gov/MedicalDevices/ProductsandMedicalProcedures/HomeHealthandConsumer/ConsumerProducts/Sharps/ucm263236.htm (accessed on 8 September 2017).
- MOH. Forum for Injection Technique Malaysia (FIT-MY): Recommendations for Best Practice in Injection Technique; MOH: Putrajaya, Malaysia, 2017. Available online: http://www.moh.gov.my/index.php/pages/view/118 (accessed on 5 May 2017).
- StataCorp. Stata Statistical Software: Release 14; StataCorp LP: College Station, TX, USA, 2015. [Google Scholar]
- Mahmoud, F.E.G.; Mona, A.E.; Hala, A.A.; Sheref, M.E. Effect of educational intervention on knowledge, attitude and practice of home waste management of used insulin injections among diabetics attending Benha University Hospital, Egypt. Eur. J. Prev. Med. 2017, 5, 1. [Google Scholar] [CrossRef]
- Ahmed, M.M.; Degwy, H.M.E.; Ali, M.I.; Hegazy, N.H. The effect of educational intervention on knowledge, attitude and glycemic control in patients with type 2 diabetes mellitus. Int. J. Community Med. Public Health 2015, 2, 302–307. [Google Scholar] [CrossRef]
- Ahmad, B.; Ramadas, A.; Kia Fatt, Q.; Zain, A.Z.M. A pilot study: The development of a culturally tailored Malaysian Diabetes Education Module (MY-DEMO) based on the Health Belief Model. BMC Endocr. Disord. 2014, 14, 31. [Google Scholar] [CrossRef] [PubMed]
- Caniza, M.A.; Maron, G.; Moore, E.J.; Quintana, Y.; Liu, T. Effective hand hygiene education with the use of flipcharts in a hospital in El Salvador. J. Hosp. Infect. 2007, 65, 58–64. [Google Scholar] [CrossRef] [PubMed]
- Atalla, H.R. Effectiveness of nursing intervention regarding self insulin administration among diabetic patients. Clin. Nurs. Stud. 2016, 4, 57–66. [Google Scholar] [CrossRef][Green Version]
- Huang, L.; Katsnelson, S.; Yang, J.; Argyrou, C.; Charitou, M.M. Factors contributing to appropriate sharps disposal in the community among patients with diabetes. Diabetes Spectr. 2018, 31, 155–158. [Google Scholar] [CrossRef] [PubMed]
- Tong, W.T.; Vethakkan, S.R.; Ng, C.J. Why do some people with type 2 diabetes who are using insulin have poor glycemic control? A qualitative study. BMJ Open 2015, 5, e006407. [Google Scholar] [CrossRef] [PubMed]
- Ko, S.H.; Park, S.A.; Cho, J.H.; Ko, S.H.; Shin, K.M.; Lee, S.H.; Song, K.H.; Park, Y.M.; Ahn, Y.B. Influence of the duration of diabetes on the outcome of a diabetes self-management education program. Diabetes Metab. J. 2012, 36, 222–229. [Google Scholar] [CrossRef] [PubMed]
- Glassmeyer, S.T.; Hinchey, E.K.; Boehme, S.E.; Daughton, C.G.; Ruhoy, I.S.; Conerly, O. Disposal practices for unwanted residential medications in the United States. Environ. Int. 2009, 35, 566–572. [Google Scholar] [CrossRef]
- Carpenter, C.J. A meta-analysis of the effectiveness of Health Belief Model variables in predicting behavior. Health Commun. 2010, 25, 661–669. [Google Scholar] [CrossRef]
- Glanz, K.; Rimer, B.K.; Viswanath, K.V. Health Behavior and Health Education: Theory, Research, and Practice, 4th ed.; Jossey-Bass: San Francisco, CA, USA, 2008. [Google Scholar]
- Handley, M.A.; Lyles, C.R.; McCulloch, C.; Cattamanchi, A. Selecting and improving Quasi-Experimental designs in effectiveness and implementation research. Annu. Rev. Public Health 2018, 39, 5–25. [Google Scholar] [CrossRef]
| Variables | Frequency (%) | |||
|---|---|---|---|---|
| Overall (n = 136) | Intervention (n = 68) | Control (n = 68) | p-Value a | |
| Age (years) | 56.88 (9.35) * | 56.43 (10.71) * | 57.32 (7.80) * | 0.578 b |
| Sex | ||||
| Male | 43 (31.6) | 24 (35.3) | 19 (27.9) | 0.356 |
| Female | 93 (68.4) | 44 (64.7) | 49 (72.1) | |
| Marital status | ||||
| Single/Divorced/Widowed | 21 (15.4) | 10 (14.7) | 11 (16.2) | 0.812 |
| Married | 115 (84.6) | 58 (85.3) | 57 (83.8) | |
| Education | ||||
| None/Primary level | 33 (24.3) | 16 (23.5) | 17 (25.0) | 0.125 |
| Secondary level | 85 (62.5) | 39 (57.4) | 46 (67.6) | |
| Tertiary level | 18 (13.2) | 13 (19.1) | 5 (7.4) | |
| Occupation | ||||
| Unemployed/Retiree | 81 (59.6) | 41 (60.3) | 40 (58.8) | 0.861 |
| Employed | 55 (40.4) | 27 (39.7) | 28 (41.2) | |
| Monthly household income | ||||
| More than RM3000 | 22 (16.2) | 14 (20.6) | 8 (11.7) | 0.293 |
| RM1000–RM3000 | 70 (51.4) | 35 (51.5) | 35 (51.5) | |
| Less than R1000 | 44 (32.4) | 19 (27.9) | 25 (36.8) | |
| Variables | Frequency (%) | p-Value a | ||
|---|---|---|---|---|
| Overall (n = 136) | Intervention (n = 68) | Control (n = 68) | ||
| Duration of diabetes | ||||
| 5 years or more | 111 (81.6) | 55 (80.9) | 56 (82.4) | 0.825 |
| Less than 5 years | 25 (18.4) | 13 (19.1) | 12 (17.6) | |
| Duration of insulin use | ||||
| 5 years or more | 31 (22.8) | 17 (25.0) | 14 (20.6) | 0.540 |
| Less than 5 years | 105 (77.2) | 51 (75.0) | 54 (79.4) | |
| Insulin injection form | ||||
| Disposable insulin pen only | 5 (3.7) | 3 (4.4) | 2 (2.9) | 0.758 c |
| Reusable insulin pen only | 128 (94.1) | 63 (92.7) | 65 (95.6) | |
| Both disposable and reusable insulin pen | 3 (2.2) | 2 (2.9) | 1 (1.5) | |
| Self-monitoring of blood glucose | ||||
| No | 61 (44.9) | 33 (48.5) | 28 (41.2) | 0.389 |
| Yes | 75 (55.1) | 35 (51.5) | 40 (58.8) | |
| Previous advice on sharp disposal from health care providers | ||||
| No | 94 (69.1) | 49 (72.1) | 45 (66.2) | 0.458 |
| Yes | 42 (30.9) | 19 (27.9) | 23 (33.8) | |
| History of needle stick injury to self or family members | ||||
| No | 103 (75.7) | 50(73.5) | 53 (77.9) | 0.548 |
| Yes | 33 (24.3) | 18 (26.5) | 15 (22.1) | |
| M-DCSD knowledge score | 63.46 (19.38) * | 62.06 (19.97) * | 64.85 (18.81) * | 0.402 b |
| Disposing sharps at health care facilities | ||||
| No | 119 (87.5) | 57 (83.8) | 62 (91.2) | 0.195 |
| Yes | 17 (12.5) | 11 (16.2) | 6 (8.8) | |
| Proper community sharp disposal method | ||||
| No | 134 (98.5) | 67 (98.5) | 67 (98.5) | 1.000 c |
| Yes | 2 (1.5) | 1 (1.5) | 1 (1.5) | |
| Comparison | Intervention (n = 68) | Control (n = 68) | ||
|---|---|---|---|---|
| Adjusted Mean Diff. (95% CI) | p-Value | Adjusted Mean Diff. (95% CI) | p-Value | |
| Baseline to one month follow up | 22.79 (17.43, 28.16) | <0.001 | −0.29 (−3.89, 3.31) | >0.950 |
| Baseline to three months follow up | 22.65 (17.19, 28.12) | <0.001 | 0.44 (−3.42, 4.31) | >0.950 |
| One month to three months follow up | −0.15 (−1.11, 0.81) | >0.950 | 0.74 (−2.88, 4.35) | >0.950 |
| Time | Adjusted Mean (95% CI) | p-Value | ||
|---|---|---|---|---|
| Intervention Group | Control Group | Time-Intervention Interaction Effect c | Overall Intervention Effect b | |
| At baseline | 62.06 (57.41, 66.71) | 64.85 (60.20, 69.51) | 0.402 | <0.001 |
| At one month follow up | 84.85 (80.30, 89.41) | 64.56 (60.00, 69.12) | <0.001 | |
| At three months follow up | 84.71 (80.28, 89.13) | 65.29 (60.87, 69.72) | <0.001 | |
| Time effect p-Value a | <0.001 | 0.884 | ||
| Treatment Group | Comparison | Disposal Method | X2(2) (df) | ap-Value | |
|---|---|---|---|---|---|
| Improper | Proper | ||||
| Intervention | Baseline | 67 | 1 | 52.061 (2) | <0.001 |
| One month follow up | 57 | 11 | |||
| Three months follow up | 34 | 34 | |||
| Control | Baseline | 67 | 1 | 0.000 (2) | 1.000 |
| One month follow up | 67 | 1 | |||
| Three months follow up | 67 | 1 | |||
| Comparison | Sharp Disposal Method | ap-Value | ||
|---|---|---|---|---|
| Improper | Proper | |||
| One month follow up | Control | 67 | 1 | 0.004 |
| Intervention | 57 | 11 | ||
| Three months follow up | Control | 67 | 1 | <0.001 |
| Intervention | 34 | 34 | ||
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hasan, U.A.; Mohd Hairon, S.; Yaacob, N.M.; Daud, A.; Abdul Hamid, A.; Hassan, N.; Ariffin, M.F.; Yi Vun, L. Effectiveness of Diabetes Community Sharp Disposal Education Module in Primary Care: An Experimental Study in North-East Peninsular Malaysia. Int. J. Environ. Res. Public Health 2019, 16, 3356. https://doi.org/10.3390/ijerph16183356
Hasan UA, Mohd Hairon S, Yaacob NM, Daud A, Abdul Hamid A, Hassan N, Ariffin MF, Yi Vun L. Effectiveness of Diabetes Community Sharp Disposal Education Module in Primary Care: An Experimental Study in North-East Peninsular Malaysia. International Journal of Environmental Research and Public Health. 2019; 16(18):3356. https://doi.org/10.3390/ijerph16183356
Chicago/Turabian StyleHasan, Ummu Atiyyah, Suhaily Mohd Hairon, Najib Majdi Yaacob, Aziah Daud, Anees Abdul Hamid, Norzaihan Hassan, Mohd Faiz Ariffin, and Lau Yi Vun. 2019. "Effectiveness of Diabetes Community Sharp Disposal Education Module in Primary Care: An Experimental Study in North-East Peninsular Malaysia" International Journal of Environmental Research and Public Health 16, no. 18: 3356. https://doi.org/10.3390/ijerph16183356
APA StyleHasan, U. A., Mohd Hairon, S., Yaacob, N. M., Daud, A., Abdul Hamid, A., Hassan, N., Ariffin, M. F., & Yi Vun, L. (2019). Effectiveness of Diabetes Community Sharp Disposal Education Module in Primary Care: An Experimental Study in North-East Peninsular Malaysia. International Journal of Environmental Research and Public Health, 16(18), 3356. https://doi.org/10.3390/ijerph16183356





