Progress Evaluation for Transnational Restaurant Chains to Reformulate Products and Standardize Portions to Meet Healthy Dietary Guidelines and Reduce Obesity and Non-Communicable Disease Risks, 2000–2018: A Scoping and Systematic Review to Inform Policy
Abstract
1. Introduction
1.1. Study Purpose
1.2. Restaurant Industry Structure and Global Presence
1.3. Customer Purchasing and Eating Trends at Restaurants
2. Materials and Methods
2.1. Search Strategy for Steps 1 and 2
2.2. Study Selection and Data Extraction
2.3. Study Quality Assessment
3. Results
3.1. Step 1: Scoping Review of Dietary Recommendations for Restaurant Chains
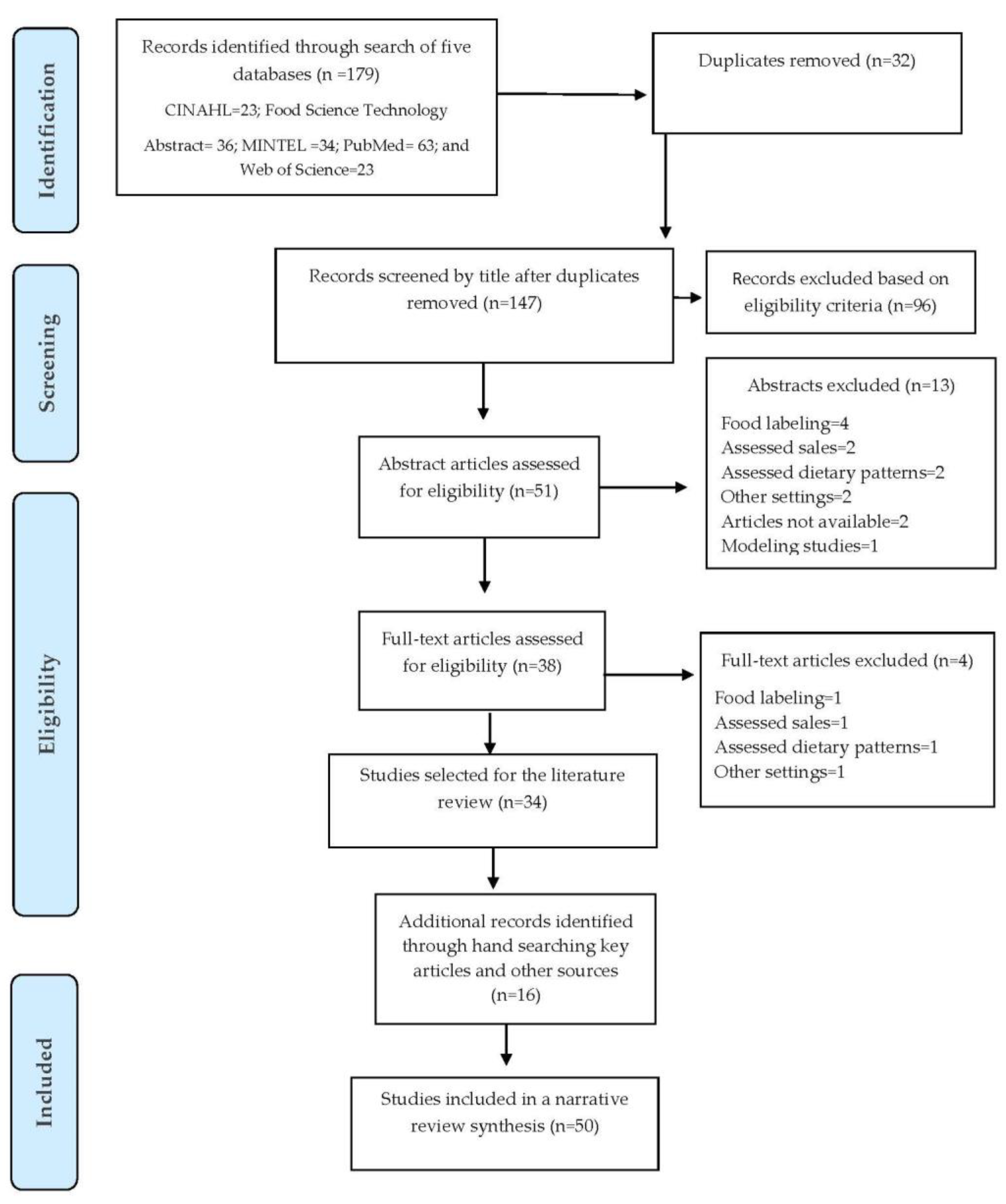
3.2. Step 2: Data Selection, Quality Assessment, and Analysis for the Systematic Review
3.3. Study Characteristics: Outcomes, Research Design, Duration, Restaurant Segment, Geographic Location
3.4. Study Characteristics by Evidence Sources, Assessment Methods, and Dietary Guidelines or Criteria
3.5. Energy
3.6. Fat, Saturated Fat, and TFA
3.7. Sodium or Salt
4. Discussion
Study Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Acknowledgments
Conflicts of Interest
References
- National Restaurant Association. 2017 Restaurant Industry Outlook. Available online: https://www.restaurant.org/Downloads/PDFs/News-Research/2017_Restaurant_outlook_summary-FINAL.pdf (accessed on 24 May 2019).
- Ritzer, G. The McDonaldization of Society, 8th ed.; Sage Publications: Thousand Oaks, CA, USA, 2015. [Google Scholar]
- Schlosser, E. Fast Food Nation: The Dark Side of the All-American Meal; Houghton Mifflin Harcourt: Boston, MA, USA, 2001. [Google Scholar]
- DeMaria, A.N. Of fast food and franchises. J. Am. Coll. Cardiol. 2003, 41, 1227–1228. [Google Scholar] [CrossRef]
- Jayaraman, S. The workers who feed us: Poverty and food insecurity among U.S. restaurant and retail workers. In From Farm to Fork: Perspectives on Growing Sustainable Food Systems in the Twenty-First Century; University of Akron Press: Akron, OH, USA, 2016. [Google Scholar]
- Bahadoran, Z.; Mirmiran, P.; Azizi, F. Fast food pattern and cardiometabolic disorders: A review of current studies. Health Promot. Perspect. 2016, 5, 231–240. [Google Scholar] [CrossRef] [PubMed]
- Braithwaite, I.; Stewart, A.W.; Hancox, R.J.; Beasley, R.; Murphy, R.; Mitchell, E.A.; ISAAC Phase Three Study Group. Fast-food consumption and body mass index in children and adolescents: An international cross-sectional study. BMJ Open 2014, 4, e005813. [Google Scholar] [CrossRef] [PubMed]
- Nago, E.S.; Lachat, C.K.; Dossa, R.A.; Kolsteren, P.W. Association of out-of-home eating with anthropometric changes: A systematic review of prospective studies. Crit. Rev. Food Sci. Nutr. 2014, 54, 1103–1116. [Google Scholar] [CrossRef] [PubMed]
- Powell, L.M.; Nguyen, B.T. Fast-food and full-service restaurant consumption among children and adolescents: Effect on energy, beverage, and nutrient intake. JAMA Pediatr. 2013, 167, 14–20. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, B.T.; Powell, L.M. The impact of restaurant consumption among US adults: Effects on energy and nutrient intakes. Public Health Nutr. 2014, 17, 2445–2452. [Google Scholar] [CrossRef] [PubMed]
- Rosenheck, R. Fast food consumption and increased caloric intake: A systematic review of a trajectory towards weight gain and obesity risk. Obes. Rev. 2008, 9, 535–547. [Google Scholar] [CrossRef] [PubMed]
- Seguin, R.A.; Aggarwal, A.; Vermeylen, F.; Drewnowski, A. Consumption frequency of foods away from home linked with higher body mass index and lower fruit and vegetable intake among adults: A cross sectional study. J. Environ. Public Health 2016, 2016, 3074241. [Google Scholar] [CrossRef] [PubMed]
- Smith, C.; Gray, A.R.; Fleming, E.A.; Parnell, W.R. Characteristics of fast food/takeaway-food and restaurant/café food consumers among New Zealand adults. Public Health Nutr. 2014, 17, 2368–2377. [Google Scholar] [CrossRef]
- Alturki, H.A.; Brooke, D.S.K. Comparative evidence of the consumption from fast-food restaurants between normal-weight and obese Saudi schoolchildren. Public Health Nutr. 2018, 21, 2280–2290. [Google Scholar] [CrossRef]
- Tambalis, K.D.; Panagiotakos, D.B.; Psarra, G.; Sidossis, L.S. Association between fast-food consumption and lifestyle characteristics in Greek children and adolescents; results from the EYZHN (National Action for Children’s Health) programme. Public Health Nutr. 2018, 21, 3386–3394. [Google Scholar] [CrossRef]
- Janssen, H.G.; Davies, I.G.; Richardson, L.D.; Stevenson, L. Determinants of takeaway and fast food consumption: A narrative review. Nutr. Res. Rev. 2018, 31, 16–34. [Google Scholar] [CrossRef]
- Zagorsky, J.L.; Smith, P.K. The association between socioeconomic status and adult fast-food consumption in the U.S. Econ. Hum. Biol. 2017, 27, 12–25. [Google Scholar] [CrossRef]
- Mackenbach, J.D.; Charreire, H.; Glonti, K.; Bárdos, H.; Rutter, H.; Compernolle, S.; de Bourdeaudhuij, I.; Nijpels, G.; Brug, J.; Oppert, J.; et al. Exploring the relation of spatial access to fast food outlets with body weight: A mediation analysis. Environ. Behav. 2018, 51, 1–30. [Google Scholar] [CrossRef]
- Jaworowska, A.; Blackham, T.; Davies, I.G.; Stevenson, L. Nutritional challenges and health implications of takeaway and fast food. Nutr. Rev. 2013, 71, 310–318. [Google Scholar] [CrossRef]
- Saksena, M.J.; Okrent, A.M.; Anekwe, T.D.; Cho, C.; Dicken, C.; Effland, A.; Elitzak, H.; Guthrie, J.; Hamrick, K.S.; Hyman, J.; et al. America’s Eating Habits: Food Away From Home, United States Department of Agriculture Economic Research Service, September 2018. Available online: https://www.ers.usda.gov/publications/pub-details/?pubid=90227 (accessed on 24 May 2019).
- Pereira, M.A.; Kartashov, A.I.; Ebbeling, C.B.; Van Horn, L.; Slattery, M.L.; Jacobs, D.R.J.; Ludwig, D.S. Fast-food habits, weight gain, and insulin resistance (the CARDIA study): 15-year prospective analysis. Lancet 2005, 365, 36–42. [Google Scholar] [CrossRef]
- Kant, A.K.; Graubard, B.I. A prospective study of frequency of eating restaurant prepared meals and subsequent 9-year risk of all-cause and cardiometabolic mortality in US adults. PLoS ONE 2018, 13, e0191584. [Google Scholar] [CrossRef]
- Neal, B.; Sacks, G.; Swinburn, B.; Vandevijvere, S.; Dunford, E.; Snowdon, W.; Webster, J.; Barquera, S.; Friel, S.; Hawkes, C.; et al. INFORMAS. Monitoring the levels of important nutrients in the food supply. Obes. Rev. 2013, 14, 49–58. [Google Scholar] [CrossRef]
- Ng, S.W.; Dunford, E. Complexities and opportunities in monitoring and evaluating US and global changes by the food industry. Obes. Rev. 2013, 14, 29–41. [Google Scholar] [CrossRef]
- Popkin, B.M.; Adair, L.S.; Ng, S.W. Global nutrition transition and the pandemic of obesity in developing countries. Nutr. Rev. 2012, 70, 3–21. [Google Scholar] [CrossRef]
- De Vogli, R.; Kouvonen, A.; Gimeno, D. The influence of market deregulation on fast food consumption and body mass index: A cross-national time series analysis. Bull. World Health Organ. 2014, 92, 99–107. [Google Scholar] [CrossRef]
- Daszkowski, D. The Expansion of American Fast Food Franchises, The Balance, 15 May 2018. Available online: https://www.thebalance.com/how-american-fast-food-franchises-expanded-abroad-1350955 (accessed on 24 May 2019).
- Rush Wirth, S. 2017 top 500: Limited Service Chains, Restaurant Business, 12 June 2017. Available online: http://www.restaurantbusinessonline.com/financing/2017-top-500-limited-service-chains (accessed on 24 May 2019).
- Popkin, B.M.; Reardon, T. Obesity and the Food System Transformation in Latin America. Obes. Rev. 2018, 19, 1028–1064. [Google Scholar] [CrossRef]
- Journalistic Inc. The Top 50 Fast Food Restaurants in America Ranked by Sales 2017, QSR Magazine, 2018. Available online: https://www.qsrmagazine.com/content/qsr50-2017-top-50-chart (accessed on 24 May 2019).
- Euromonitor International. Fast Food, 2018. Available online: http://www.euromonitor.com/fast-food (accessed on 24 May 2019).
- Searcy, D. The Global Siren Call of Fast Food, The New York Times, 2 October 2017. Available online: https://www.nytimes.com/series/obesity-epidemic (accessed on 24 May 2019).
- Searcey, D.; Ritchtel, M. Obesity was Rising as Ghana Embraced Fast Food, Then Came KFC. The New York Times, 2 October 2017. Available online: https://www.nytimes.com/series/obesity-epidemic (accessed on 24 May 2019).
- Zuckerman, J.C. Palm oil is everywhere in India—And Public-Health Experts are Concerned, The Nation, 28 September 2018. Available online: https://www.thenation.com/article/how-palm-oil-became-the-high-fructose-corn-syrup-of-the-developing-world/ (accessed on 24 May 2019).
- Langellier, B.A. Consumption and expenditure on food prepared away from home among Mexican adults in 2006. Salud Publica Mexico 2015, 57, 4–13. [Google Scholar] [CrossRef]
- Naidoo, N.; van Dam, R.M.; Ng, S.; Tan, C.S.; Chen, S.; Lim, J.Y.; Chan, M.F.; Chew, L.; Rebello, S.A. Determinants of eating at local and western fast-food venues in an urban Asian population: A mixed methods approach. Int. J. Behav. Nutr. Phys. Act. 2017, 14, 69. [Google Scholar] [CrossRef]
- Patel, O.; Shahulhameed, S.; Shivashankar, R.; Tayyab, M.; Rahman, A.; Prabhakaran, D.; Tandon, N.; Jaacks, L.M. Association between full service and fast food restaurant density, dietary intake and overweight/obesity among adults in Delhi, India. BMC Public Health 2017, 18, 36. [Google Scholar] [CrossRef]
- Olutayo, A.O.; Akanle, O. Fast food in Ibadan: An emerging consumption pattern. Africa 2009, 79, 207–227. [Google Scholar] [CrossRef]
- IBIS World. Global Fast Food Restaurants Industry Market. Research Report, January 2018. Available online: https://www.ibisworld.com/industry-trends/global-industry-reports/hotels-restaurants/fast-food-restaurants.html (accessed on 24 May 2019).
- Statista. Brand Value of the 10 Most Valuable Fast Food Brands Worldwide in 2018 (in Million U.S. Dollars), 2018. Available online: https://www.statista.com/statistics/273057/value-of-the-most-valuable-fast-food-brands-worldwide/ (accessed on 24 May 2019).
- Touryalai, H.; Stoller, K. (Eds.) Global 2000: The world’s Largest Public Companies: Restaurants, 2018. Available online: https://www.forbes.com/global2000/list/#industry:Restaurants (accessed on 24 May 2019).
- McDonald’s Corporation. 2017 Annual Report. Available online: https://corporate.mcdonalds.com/content/dam/gwscorp/investor-relations-content/annual-reports/McDonald%27s%202017%20Annual%20Report.pdf (accessed on 24 May 2019).
- Yum! Brands. 2017 Annual Report. Available online: http://www.yum.com/annualreport/ (accessed on 24 May 2019).
- Statista. Number of Domino’s Pizza Stores in Selected Countries Worldwide from 2010 to 2017, 2018. Available online: https://www.statista.com/statistics/207130/number-of-dominos-pizza-stores-worldwide-by-country/ (accessed on 24 May 2019).
- Fitzpatrick, H. The top 20 food franchises in the world, Business Insider, 25 July 2015. Available online: https://www.businessinsider.com/the-top-20-food-franchises-in-the-world-2015-7 (accessed on 24 May 2019).
- The Nielsen Company. What’s in Our Food and On Our Mind? Ingredient and Dining Out Trends around the World, August 2016. Available online: http://www.nielsen.com/content/dam/nielsenglobal/eu/docs/pdf/Global%20Ingredient%20and%20Out-of-Home%20Dining%20Trends%20Report%20FINAL%20(1).pdf (accessed on 24 May 2019).
- Technomic. 2018 Future of LSR Consumer Trend Report. Available online: https://www.technomic.com/available-studies/consumer-trend-reports/future-of-lsr (accessed on 24 May 2019).
- Marketforce Information. New Study from Market Force Information Reveals America’s Favorite Quick-Service Restaurants, 15 March 2017. Available online: http://www.marketforce.com/consumers-favorite-QSRs-2017-Market-Force-research (accessed on 24 May 2019).
- Wang, Y.; Wang, L.; Xue, H.; Qu, W. A review of the growth of the fast food industry in China and its potential impact on obesity. Int. J. Environ. Res. Public Health 2016, 13, 1112. [Google Scholar] [CrossRef]
- Newson, R.S.; van der Mass, R.; Beijersbergen, A.; Carlson, L.; Rosenbloom, C. International consumer insights into the desires and barriers of diners in choosing restaurant meals. Food Qual. Prefer. 2015, 43, 63–70. [Google Scholar] [CrossRef]
- Kraak, V.; Englund, T.; Misyak, S.; Serrano, E.L. A novel marketing mix and choice architecture framework to nudge restaurant customers toward healthy food environments to reduce obesity in the United States. Obes. Rev. 2017, 18, 852–868. [Google Scholar] [CrossRef]
- Kraak, V.; Englund, T.; Misyak, S.; Serrano, E. Progress evaluation for the restaurant industry assessed by a voluntary marketing-mix and choice-architecture framework that offers strategies to nudge American customers toward healthy food environments, 2006–2017. Int. J. Environ. Res. Public Health 2017, 14, 760. [Google Scholar] [CrossRef]
- Moher, D.; Shamseer, L.; Clarke, M.; Ghersi, D.; Liberati, A.; Petticrew, M.; Shekelle, P.; Stewart, L.A.; PRISMA-P Group. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst. Rev. 2015, 4, 1. [Google Scholar] [CrossRef]
- The Johanna Briggs Institute. Checklist for Analytical Cross-Sectional Studies, Adelaide, Australia, 2017. Available online: http://joannabriggs.org/research/critical-appraisal-tools.html (accessed on 24 May 2019).
- Food and Agriculture Organization of the United Nations. Food-Based Dietary Guidelines, 2018. Available online: http://www.fao.org/nutrition/education/food-based-dietary-guidelines/en/ (accessed on 24 May 2019).
- World Health Organization, Food and Agriculture Organization. Joint WHO/FAO Workshop on Fruit and Vegetables for Health. Kobe, Japan, 1–3 September 2004, WHO and FAO, 2005. Available online: http://www.who.int/dietphysicalactivity/publications/fruit_vegetables_report.pdf (accessed on 24 May 2019).
- World Health Organization. Global Strategy on Diet, Physical Activity, and Health. Report No. WHA57.17. Geneva: WHO, 2004. Available online: http://www.who.int/dietphysicalactivity/strategy/eb11344/en/index.html (accessed on 24 May 2019).
- World Health Organization. Follow-Up to the Political Declaration of the High-level Meeting of the General Assembly on the Prevention and Control of Non-communicable Diseases, 25 May 2013. Available online: http://apps.who.int/gb/ebwha/pdf_files/WHA66/A66_R10-en.pdf (accessed on 24 May 2019).
- World Health Organization. Potassium Intake for Adults and Children, Geneva: WHO, 2012. Available online: http://www.who.int/nutrition/publications/guidelines/potassium_intake/en/index.html (accessed on 24 May 2019).
- Food and Agriculture Organization of the United Nations. Fats and Fatty Acids in Human Nutrition, Report of an Expert Consultation, FAO Food and Nutrition Paper 91. Rome: FAO, 2010. Available online: http://www.fao.org/docrep/013/i1953e/i1953e00.pdf (accessed on 24 May 2019).
- World Health Organization. WHO Plan to Eliminate Industrially-Produced Trans-Fatty Acids from the Global Food Supply, 14 May 2018 [news release]. Available online: http://www.who.int/news-room/detail/14-05-2018-who-plan-to-eliminate-industrially-produced-trans-fatty-acids-from-global-food-supply (accessed on 24 May 2019).
- World Health Organization. Sugars Intake for Adults and Children, Guidelines. Geneva, Switzerland: WHO, 2015. Available online: https://www.who.int/nutrition/publications/guidelines/sugars_intake/en/ (accessed on 24 May 2019).
- World Health Organization. Guideline: Sodium Intake for Adults and Children, Geneva, Switzerland: WHO, 2012. Available online: http://www.who.int/nutrition/publications/guidelines/sodium_intake_printversion.pdf (accessed on 24 May 2019).
- U.S. Department of Health and Human Services and U.S. Department of Agriculture. 2015–2020 Dietary Guidelines for Americans, 8th Edition. Washington, DC: US Government Printing Office, December 2015. Available online: https://health.gov/dietaryguidelines/2015/ (accessed on 24 May 2019).
- National Health Service. The Eatwell Guide, 2016. England, United Kingdom. Available online: https://www.nhs.uk/live-well/eat-well/the-eatwell-guide/ (accessed on 24 May 2019).
- Australian Government. National Health and Medical Research Council. Department of Health and Ageing. Eat for Health: Educator Guide, Information for Nutrition Educators, 2013. Available online: https://www.eatforhealth.gov.au/guidelines (accessed on 24 May 2019).
- Canada’s Dietary Guidelines for Health Professionals and Policy Makers. Ottawa, Ontario: Health Canada, Minister of Health, 2019. Available online: https://food-guide.canada.ca/static/assets/pdf/CDG-EN-2018.pdf (accessed on 6 July 2019).
- National Health Service. One You Campaign. Keep Track of Calories with 400-600-600. Public Health England, United Kingdom, 2018. Available online: https://www.nhs.uk/oneyou/for-your-body/eat-better/keep-track-of-calories-400-600-600/ (accessed on 24 May 2019).
- Australian Government Department of Health. The Healthy Food Partnership. The Final Rationale and Recommendations of the Food Service Working Group, May 2018. Available online: http://health.gov.au/internet/main/publishing.nsf/Content/food-service (accessed on 24 May 2019).
- Raine, K.D.; Atkey, K.; Olstad, D.L.; Ferdinands, A.R.; Beaulieu, D.; Buhler, S.; Campbell, N.; Cook, B.; L’Abbé, M.; Lederer, A.; et al. Healthy food procurement and nutrition standards in public facilities: Evidence synthesis and consensus policy recommendations. Health Promot. Chronic Dis. Prev. Can. 2018, 38, 6–17. [Google Scholar] [CrossRef]
- Public Health England; Local Government Association. Strategies for Encouraging Healthier ‘Out of Home’ Food Provision. A Toolkit for Local Councils Working with Small Food Businesses, 2017. Available online: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/604912/Encouraging_healthier_out_of_home_food_provision_toolkit_for_local_councils.pdf (accessed on 24 May 2019).
- The Keystone Center. Forum on Away-From-Home Foods: Opportunities for Preventing Weight Gain and Obesity, Washington, DC: Keystone Center 2006. Available online: https://www.keystone.org/wp-content/uploads/2015/08/053006-Report-on-Keystone-Forum-on-Preventing-Weight-Gain-and-Obesity.pdf (accessed on 24 May 2019).
- Centers for Disease Control and Prevention. US Department of Health and Human Services. Healthy Food Service Guidelines, August 2018. Available online: https://www.cdc.gov/obesity/strategies/food-serv-guide.html (accessed on 24 May 2019).
- National Restaurant Association. About the Kids LiveWell Program, 2018. Available online: https://www.restaurant.org/Industry-Impact/Food-Healthy-Living/Kids-LiveWell/About (accessed on 24 May 2019).
- American Heart Association. Heart-Check Meal Certification Program Nutrition Requirements, May 2018. Available online: https://www.heart.org/en/healthy-living/company-collaboration/heart-check-certification/heart-check-meal-certification-program-foodservice/heart-check-meal-certification-program-nutrition-requirements (accessed on 24 May 2019).
- Elbel, B.; Champagne, C.M.; Economos, C.D.; Cohen, D.; Harris, J.; Williams, J.D.; Shields, K.; Whitsel, L.P.; Lesser, L.I.; van Horn, L.; et al. Performance Standards for Restaurants. A New Approach to Addressing the Obesity Epidemic, Conference Proceedings, Santa Monica, CA: RAND Corporation 2013. Available online: https://www.rand.org/pubs/conf_proceedings/CF313.html (accessed on 24 May 2019).
- New York City Department of Health and Mental Hygiene. National Salt Reduction Initiative Restaurant Food Categories and Targets, 2014. Available online: https://www1.nyc.gov/assets/doh/downloads/pdf/cardio/cardio-salt-nsri-restaurant.pdf (accessed on 24 May 2019).
- Cohen, D.A.; Lesser, L.I.; Wright, C.; Story, M.; Economos, C. Kid’s menu portion sizes: How much should children be served? Nutr. Today 2016, 51, 273–280. [Google Scholar] [CrossRef]
- Ahuja, J.K.; Wasswa-Kintu, S.; Haytowitz, D.B.; Daniel, M.; Thomas, R.; Showell, B.; Nickle, M.; Roseland, J.M.; Gunn, J.; Cogswell, M.; et al. Sodium content of popular commercially processed and restaurant foods in the United States. Prev. Med. Rep. 2015, 2, 962–967. [Google Scholar] [CrossRef]
- Astiasarán, I.; Abella, E.; Gatta, G.; Ansorena, D. Margarines and fast-food french fries: Low content of trans fatty acids. Nutrients 2017, 9, 662. [Google Scholar] [CrossRef]
- Auchincloss, A.H.; Leonberg, B.L.; Glanz, K.; Bellitz, S.; Ricchezza, A.; Jervis, A. Nutritional value of meals at full-service restaurant chains. J. Nutr. Educ. Behav. 2014, 46, 75–81. [Google Scholar] [CrossRef]
- Bauer, K.W.; Hearst, M.O.; Earnest, A.A.; French, S.A.; Oakes, J.M.; Harnack, L.J. Energy content of U.S. fast-food restaurant offerings: 14-year trends. Am. J. Prev. Med. 2012, 43, 490–497. [Google Scholar] [CrossRef]
- Bleich, S.N.; Wolfson, J.A.; Jarlenski, M.P. Calorie changes in chain restaurant menu items: Implications for obesity and evaluations of menu labeling. Am. J. Prev. Med. 2015, 48, 70–75. [Google Scholar] [CrossRef]
- Bleich, S.N.; Wolfson, J.A.; Jarlenski, M.P. Calorie changes in large chain restaurants: Declines in new menu items but room for improvement. Am. J. Prev. Med. 2016, 50, e1–e8. [Google Scholar] [CrossRef]
- Bleich, S.N.; Wolfson, J.A.; Jarlenski, M.P. Calorie changes in large chain restaurants from 2008 to 2015. Prev. Med. 2017, 100, 112–116. [Google Scholar] [CrossRef]
- Brindal, E.; Mohr, P.; Wilson, C.; Wittert, G. Obesity and the effects of choice at a fast food restaurant. Obes. Res. Clin. Pract. 2008, 2, 111–117. [Google Scholar] [CrossRef] [PubMed]
- Bruemmer, B.; Krieger, J.; Saelens, B.E.; Chan, N. Energy, saturated fat, and sodium were lower in entrées at chain restaurants at 18 months compared with 6 months following the implementation of mandatory menu labeling regulation in King County, Washington. J. Assoc. Nutr. Diet. 2012, 112, 1169–1176. [Google Scholar] [CrossRef] [PubMed]
- Chand, A.; Eyles, H.; Ni Mhurchu, C. Availability and accessibility of healthier options and nutrition information at New Zealand fast food restaurants. Appetite 2012, 58, 227–233. [Google Scholar] [CrossRef] [PubMed]
- Deierlein, A.L.; Peat, K.; Claudio, L. Comparison of the nutrient content of children’s menu items at US restaurant chains, 2010–2014. Nutr. J. 2015, 14, 80. [Google Scholar] [CrossRef] [PubMed]
- Dunford, E.; Webster, J.; Barzi, F.; Neal, B. Nutrient content of products served by leading Australian fast food chains. Appetite 2010, 55, 484–489. [Google Scholar] [CrossRef] [PubMed]
- Dunford, E.; Webster, J.; Woodward, M.; Czernichow, S.; Yuan, W.L.; Jenner, K.; Ni Mhurchu, C.; Jacobson, M.; Campbell, N.; Neal, B. The variability of reported salt levels in fast foods across six countries: Opportunities for salt reduction. CMAJ 2012, 184, 1023–1028. [Google Scholar] [CrossRef] [PubMed]
- Eissa, M.A.; Hearne, K.; Saavedra, N. Comparison of children’s menu items at full- and quick-service restaurants. South. Med. J. 2018, 111, 192–197. [Google Scholar] [CrossRef] [PubMed]
- Eyles, H.; Jiang, Y.; Blakely, T.; Neal, B.; Crowley, J.; Cleghorn, C.; Ni Mhurchu, C. Five year trends in the serve size, energy, and sodium contents of New Zealand fast foods: 2012 to 2016. Nutr. J. 2018, 17, 65. [Google Scholar] [CrossRef]
- Garcia, J.; Dunford, E.K.; Sundtrom, J.; Neal, B.C. Changes in the sodium content of leading Australian fast-food products between 2009 and 2012. Med. J. Aust. 2014, 200, 340–344. [Google Scholar] [CrossRef]
- Garemo, M.; Naimi, A.A. Children’s meals at restaurants in Abu Dhabi, United Arab Emirates, have poor nutritional quality. Mediterr. J. Nutr. Metab. 2018, 11, 85–92. [Google Scholar] [CrossRef]
- Hearst, M.O.; Harnack, L.J.; Bauer, K.W.; Earnest, A.A.; French, S.A.; Michael Oakes, J. Nutritional quality at eight U.S. fast-food chains: 14-year trends. Am. J. Prev. Med. 2013, 44, 589–594. [Google Scholar] [CrossRef] [PubMed]
- Heredia-Blonval, K.; Blanco-Metzler, A.; Montero-Campos, M.; Dunford, E.K. The salt content of products from popular fast-food chains in Costa Rica. Appetite 2014, 83, 173–177. [Google Scholar] [CrossRef] [PubMed]
- Hobin, E.; White, C.; Li, Y.; Chiu, M.; O’Brien, M.F.; Hammond, D. Nutritional quality of food items on fast-food ‘kids’ menus’: Comparisons across countries and companies. Public Health Nutr. 2014, 17, 2263–2269. [Google Scholar] [CrossRef] [PubMed]
- Jacobson, M.F.; Havas, S.; McCarter, R. Changes in sodium levels in processed and restaurant foods, 2005 to 2011. JAMA Intern. Med. 2013, 173, 1285–1291. [Google Scholar] [CrossRef] [PubMed]
- Jarlenski, M.P.; Wolfson, J.A.; Bleich, S.N. Macronutrient composition of menu offerings in fast food restaurants in the U.S. Am. J. Prev. Med. 2016, 51, e91–e97. [Google Scholar] [CrossRef] [PubMed]
- Khan, M.A.; Khan, M.M.; Abdelhafiz Gadelrab, R.M. Sodium content in fast foods: Assessment of menu items in selected countries. J. Foodserv. Bus. Res. 2018, 21, 553–569. [Google Scholar] [CrossRef]
- Kirkpatrick, S.I.; Reedy, J.; Kahle, L.L.; Harris, J.L.; Ohri-Vachaspati, P.; Krebs-Smith, S.M. Fast-food menu offerings vary in dietary quality, but are consistently poor. Public Health Nutr. 2014, 17, 924–931. [Google Scholar] [CrossRef]
- Mazariegos, S.; Chacón, V.; Cole, A.; Barnoya, J. Nutritional quality and marketing strategies of fast food children’s combo meals in Guatemala. BMC Obes. 2016, 3, 52. [Google Scholar] [CrossRef]
- Moran, A.J.; Block, J.P.; Goshev, S.G.; Bleich, S.N.; Roberto, C.A. Trends in nutrient content of children’s menu items in U.S. chain restaurants. Am. J. Prev. Med. 2017, 52, 284–291. [Google Scholar] [CrossRef]
- O’Donnell, S.I.; Hoerr, S.L.; Mendoza, J.A.; Tsuei Goh, E. Nutrient quality of fast food kids meals. Am. J. Clin. Nutr. 2008, 88, 1388–1395. [Google Scholar]
- Prentice, C.A.; Smith, C.; McLean, R.M. Sodium in commonly consumed fast foods in New Zealand: A public health opportunity. Public Health Nutr. 2016, 19, 958–966. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Reeves, S.; Wake, Y.; Zick, A. Nutrition labeling and portion size information on children’s menus in fast-food and table-service chain restaurants in London, UK. J. Nutr. Educ. Behav. 2011, 43, 543–547. [Google Scholar] [CrossRef] [PubMed]
- Roberts, S.B.; Das, S.K.; Suen, V.M.M.; Pihlajamäki, J.; Kuriyan, R.; Steiner-Asiedu, M.; Taetzsch, A.; Anderson, A.K.; Silver, R.E.; Barger, K.; et al. Measured energy content of frequently purchased restaurant meals: Multi-country cross sectional study. BMJ 2018, 363, k4864. [Google Scholar] [CrossRef] [PubMed]
- Rudelt, A.; French, S.; Harnack, L. Fourteen-year trends in sodium content of menu offerings at eight leading fast-food restaurants in the USA. Public Health Nutr. 2014, 17, 1682–1688. [Google Scholar] [CrossRef] [PubMed]
- Schoffman, D.E.; Davidson, C.R.; Hales, S.B.; Crimarco, A.E.; Dahl, A.A.; Turner-McGrievy, G.M. The fast-casual conundrum: Fast-casual restaurant entrees are higher in calories than fast food. J. Acad. Nutr. Diet. 2016, 116, 1606–1612. [Google Scholar] [CrossRef] [PubMed]
- Scourboutakos, M.J.; L’Abbé, M.R. Restaurant menus: Calories, calorie density, and serving size. Am. J. Prev. Med. 2012, 43, 249–255. [Google Scholar] [CrossRef]
- Scourboutakos, M.J.; Semnani-Azad, Z.; L’Abbe, M.R. Restaurant meals: Almost a full day’s worth of calories, fats, and sodium. JAMA Intern. Med. 2013, 173, 1373–1374. [Google Scholar] [CrossRef]
- Scourboutakos, M.J.; Semnani-Azad, Z.; L’Abbé, M.R. Added sugars in kids’ meals from chain restaurants. Prev. Med. Rep. 2016, 3, 391–393. [Google Scholar] [CrossRef]
- Scourboutakos, M.J.; L’Abbé, M.R. Sodium levels in fast-food and sit-down restaurants. Can. J. Public Health. 2013, 104, 2–8. [Google Scholar]
- Scourboutakos, M.J.; Murphy, S.A.; L’Abbé, M.R. Association between salt substitutes/enhancers and changes in sodium levels in fast-food restaurants: A cross-sectional analysis. CMAJ 2018, 6, E118–E125. [Google Scholar] [CrossRef][Green Version]
- Scourboutakos, M.J.; L’Abbé, M.R. Changes in sodium levels in chain restaurant foods in Canada (2010–2013): A longitudinal study. CMAJ 2014, 2, 343–351. [Google Scholar] [CrossRef] [PubMed]
- Sliwa, S.; Anzman-Frasca, S.; Lynskey, V.; Washburn, K.; Economos, C. Assessing the availability of healthier children’s meals at leading quick-serve and full-service restaurants. J. Nutr. Educ. Behav. 2016, 48, 242–249. [Google Scholar] [CrossRef] [PubMed]
- Soo, J.; Harris, J.L.; Davison, K.K.; Williams, D.R.; Roberto, C.A. Changes in the nutritional quality of fast-food items marketed at restaurants, 2010 v. 2013. Public Health Nutr. 2018, 21, 2117–2127. [Google Scholar] [CrossRef] [PubMed]
- Stender, S.; Dyerberg, J.; Astrup, A. High levels of industrially produced trans fat in popular fast foods. N. Engl. J. Med. 2006, 354, 1650–1652. [Google Scholar] [CrossRef] [PubMed]
- Uechi, K. Nutritional quality of meals offered to children (kids’ meals) at chain restaurants in Japan. Public Health Nutr. 2018, 21, 3101–3110. [Google Scholar] [CrossRef] [PubMed]
- Urban, L.E.; Roberts, S.B.; Fierstein, J.L.; Gary, C.E.; Lichtenstein, A.H. Temporal trends in fast-food restaurant energy, sodium, saturated fat, and trans fat content, United States, 1996–2013. Prev. Chronic Dis. 2014, 11, 140202. [Google Scholar] [CrossRef] [PubMed]
- Urban, L.E.; Roberts, S.B.; Fierstein, J.L.; Gary, C.E.; Lichtenstein, A.H. Sodium, saturated fat, and trans fat content per 1,000 kilocalories: Temporal trends in fast-food restaurants, United States, 2000–2013. Prev. Chronic Dis. 2014, 11, E228. [Google Scholar] [CrossRef] [PubMed]
- Waterlander, W.E.; Eyles, H.; Whitworth, L. Healthiness of popular fast food items in New Zealand: Plenty of room for improvement. N. Z. Med. J. 2014, 127, 102–105. [Google Scholar] [PubMed]
- Wellard, L.; Glasson, C.; Chapman, K. Fries or a fruit bag? Investigating the nutritional composition of fast food children’s meals. Appetite 2012, 58, 105–110. [Google Scholar] [CrossRef]
- Wellard-Cole, L.; Goldsbury, D.; Havill, M.; Hughes, C.; Watson, W.L.; Dunford, E.K.; Chapman, K. Monitoring the changes to the nutrient composition of fast foods following the introduction of menu labelling in New South Wales, Australia: An observational study. Public Health Nutr. 2018, 21, 1194–1199. [Google Scholar] [CrossRef]
- Wolfson, J.A.; Moran, A.J.; Jarlenski, M.P.; Bleich, S.N. Trends in sodium content of menu items in large chain restaurants in the U.S. Am. J. Prev. Med. 2018, 54, 28–36. [Google Scholar] [CrossRef] [PubMed]
- Ziauddeen, N.; Fitt, E.; Edney, L.; Dunford, E.; Neal, B.; Jebb, S.A. Variability in the reported energy, total fat and saturated fat contents in fast-food products across ten countries. Public Health Nutr. 2015, 18, 2962–2969. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Afshin, A.; Sur, P.J.; Fay, K.A. Health effects of dietary risks in 195 countries, 1990-2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet 2019, 393, 1958–1972. [Google Scholar] [CrossRef]
- Vandevijvere, S.; Jaacks, L.M.; Monteiro, C.A.; Moubarac, J.C.; Girling-Butcher, M.; Lee, A.C.; Pan, A.; Bentham, J.; Swinburn, B. Global trends in ultra-processed food and drink product sales and their association with adult body mass index trajectories. Obes. Rev. 2019, 1–10. [Google Scholar] [CrossRef]
- World Health Organization. Global Action Plan for the Prevention and Control of Noncommunicable Diseases 2013–2020, Geneva: WHO; 2013. Available online: http://apps.who.int/iris/bitstream/handle/10665/94384/9789241506236_eng.pdf;jsessionid=16A7E6805FBAB03802848E12F76944D9?sequence=1 (accessed on 24 May 2019).
- Kim, E.; Ham, S. Restaurants’ disclosure of nutritional information as a corporate social responsibility initiative: customers’ attitudinal and behavioral responses. Int. J. Hosp. Manag. 2016, 55, 96–106. [Google Scholar] [CrossRef]
- Marteau, T.M.; Hollands, G.J.; Shemilt, I.; Jebb, S.A. Downsizing: Policy options to reduce portion sizes to help tackle obesity. BMJ 2015, 351, h5863. [Google Scholar] [CrossRef]
- Cohen, D.A.; Story, M. Mitigating the health risks of dining out: The need for standardized portion sizes in restaurants. Am. J. Public Health 2014, 104, 586–590. [Google Scholar] [CrossRef]
- Gase, L.; Dunning, L.; Kuo, T.; Simon, P.; Fielding, J.E. Restaurant owners’ perspectives on a voluntary program to recognize restaurants for offering reduced-size portions, Los Angeles County, 2012. Prev. Chronic Dis. 2014, 11, E44. [Google Scholar] [CrossRef]
- Patel, A.A.; Lopez, N.V.; Lawless, H.T.; Njike, V.; Beleche, M.; Katz, D.L. Reducing calories, fat, saturated fat, and sodium in restaurant menu items: Effects on consumer acceptance. Obesity (Silver Spring) 2016, 12, 2497–2508. [Google Scholar] [CrossRef]
- Alliance for a Healthier Generation. McDonald’s Announces Global Commitments to Support Families with Increased Focus on Happy Meals, 15 February 2018 [news release]. Available online: https://www.healthiergeneration.org/news__events/2018/02/15/1968/mcdonalds_announces_global_commitment_to_support_families_with_increased_focus_on_happy_meals (accessed on 24 May 2019).
- McDonald’s & Alliance for a Healthier Generation. Five-Year Progress Report on 2013 Commitments, May 2019. Available online: https://www.healthiergeneration.org/our-work/businesses/impact/mcdonalds-commitment/five-year-interactive-report (accessed on 24 May 2019).
- Lee-Kwan, S.H.; Park, S.; Maynard, L.; Blanck, H.M. One menu please: Parents want affordable, right-sized portions for their children in restaurants. Clin. Nutr. Res. 2018, 7, 241–247. [Google Scholar] [CrossRef]
- Cleveland, L.P.; Simon, D.; Block, J.P. Compliance in 2017 with federal calorie labelling in 90 chain restaurants and 10 retail food outlets prior to required implementation. Am. J. Public Health 2018, 108, 1099–1102. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Fats, Oils, Food and Food Service Industries should Join Global Effort to Eliminate Industrial Trans Fat from Processed Food by 2023, 23 April 2019 [media release]. Available online: https://www.who.int/news-room/detail/23-04-2019-fats-oils-food-and-food-service-industries-should-join-global-effort-to-eliminate-industrial-trans-fat-from-processed-food-by-2023 (accessed on 24 May 2019).
- Food Monitoring Group. International collaborative project to compare and track the nutritional composition of fast foods. BMC Public Health 2012, 12, 559. [Google Scholar] [CrossRef] [PubMed]
- Access to Nutrition Index. Global Index 2018: Marketing, May 2018. Available online: https://www.accesstonutrition.org/sites/gl18.atnindex.org/files/resources/atni_report_global_index_2018.pdf (accessed on 24 May 2019).
- Sacks, G.; Vanderlee, L.; Robinson, E.; Vandevijvere, S.; Cameron, A.; Ni Mhurchu, C.; Lee, A.; See Hoe, W.; Karupaiah, T.; Vergeer, L.; et al. BIA-Obesity (Business Impact Assessment—Obesity and population-level nutrition): A tool and process to assess food company policies and commitments related to obesity prevention and population nutrition at the national level. Obes. Rev. 2019. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, J.; Riis, J.; Elbel, B.; Ariely, D. Inviting consumers to downsize fast-food portions significantly reduces calorie consumption. Health Aff. (Millwood) 2012, 31, 399–407. [Google Scholar] [CrossRef] [PubMed]
| QSR Chain | 2018 Brand Value 1 USD $ Billion | Franchise Units and # Countries |
|---|---|---|
| McDonald’s | $126.0 billion | >33,500 units in >100 countries |
| Starbucks | $44.5 billion | >29,000 units in 75 countries |
| Subway | $18.8 billion | >44,000 units in 112 countries |
| KFC 2 | $15.1 billion | >45,000 units in 139 countries 2 |
| Pizza Hut 2 | $7.4 billion | |
| Taco Bell 2 | $5.2 billion | |
| Domino’s Pizza | $7.4 billion | >11,000 units in 85 countries |
| Burger King 3 | $5.1 billion | >15,000 units in >100 countries |
| PICO | Inclusion Criteria | Exclusion Criteria |
|---|---|---|
| Population | QSR, FCR, and FSR chain restaurants or firms that operated businesses in high-, middle-, or low-income countries. | Study reported on non-chain restaurants or other food service industry settings (i.e., worksites, cafeterias, canteens, schools, childcare, and supermarkets). |
| Indicator | Standardized assessment methods used to determine the nutrient content of food or beverage products, side dishes, and meals sold at restaurants. | Study did not report or use standardized assessment methods to determine the nutrient content or portion size of meal items available to customers to purchase or consume. |
| Comparison | Nutrient content and portion size of food and beverage items compared to standardized or recommended healthy dietary criteria or targets. | Study did not report nutrient-profile criteria or targets to compare product profiles or product portion or serving size related to the outcomes of interest. |
| Outcomes | Nutrient profile or composition Energy (calories or kilojoules or energy density); Fats (total, saturated, and TFA); Sugars (total, added, or free); and Sodium (salt or sodium density). Portion or serving size Meals, non-alcoholic beverages or drinks, side dishes, desserts, or other edible products. | Study did not report on the nutrient profile, nutrient composition, or outcomes of interest. |
| Study Design | English language, published between 1 January 2000 and 18 December 2018. Longitudinal, cross-sectional, descriptive, observational, and/or intervention studies. | Study was non-English language, published before January 2000 or after December 2018, gray-literature source, or the full record was not available for review. |
| Year | Authoritative Body or Program | Recommended Food Groups, Dietary Guidelines or Nutrient Targets |
|---|---|---|
| 2011 | U.S. National Restaurant Association and Healthy Dining’s Kids LiveWell Program [74] | To participate in the Kids LiveWell Program, a restaurant must provide at least one meal that meets the following criteria:
|
| 2012 | American Heart Association’s (AHA’s) Heart Healthy Program [75] | To participate in the AHA’s certified Heart Healthy Program, an adult meal must meet the following criteria:
|
| 2013 | U.S. National Institutes of Health (NIH) and RAND Corporation Expert Panel for Healthy Restaurant Meal Standards [76] | The NIH and RAND healthy restaurant criteria define a meal (i.e., entrée, side, and beverage) as meeting the following criteria: Adult meals
|
| 2014 | U.S. National Salt Reduction Initiative Targets for Restaurants [77] | This initiative set targetsfor 10 restaurant food categories (i.e., hamburgers, chicken, seafood, sandwiches, pizza, potatoes, soup, and bakery products) to meet the following criteria/100 g for items sold by 2014:
|
| 2016 | U.S. Expert Panel on Children’s Menu Portions [78] | A single serving of a children’s menu entree should not exceed the following criteria:
|
| Lead Author, Year | 1. Were the Inclusion Criteria for the Sample Clearly Defined? | 2. Were the Study Subjects and the Setting Described in Detail? | 3. Was the Exposure Measured in a Valid and Reliable Way? | 4. Were Objective, Standard Criteria Used to Measure the Condition? | 5. Were Compounding Factors Identified? | 6. Were Strategies Stated to Manage Confounding Factors? | 7. Were the Outcomes Measured in a Valid and Reliable Way? | 8. Was the Appropriate Statistical Analysis Used? | Overall Study Quality Score 1 = Weak 2 = Moderate 3 = Strong | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Reviewers’ decision | 1 | 2 | 1&2 | 1 | 2 | 1&2 | 1 | 2 | 1&2 | 1 | 2 | 1&2 | 1 | 2 | 1&2 | 1 | 2 | 1&2 | 1 | 2 | 1&2 | 1 | 2 | 1&2 | |
| Ahuja et al., 2015 [79] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Astiasarán et al., 2017 [80] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Auchincloss et al., 2014 [81] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N | N | N | N | N | N | Y | Y | Y | Y | Y | Y | 2 |
| Bauer et al., 2012 [82] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Bleich et al., 2015 [83] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Bleich et al., 2016 [84] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Bleich et al., 2017 [85] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Brindal et al., 2008 [86] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | N | N | N | 2 |
| Bruemmer et al., 2012 [87] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N | N | N | N | N | N | Y | Y | Y | Y | Y | Y | 3 |
| Chand et al., 2012 [88] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | N | Y | Y | Y | Y | Y | 3 |
| Cohen et al., 2017 [78] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Deierlein et al., 2015 [89] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 | |
| Dunford et al., 2010 [90] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Dunford et al., 2012 [91] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Eissa et al., 2017 [92] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Eyles et al., 2018 [93] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Garcia et al., 2014 [94] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N | N | N | N | N | N | Y | Y | Y | Y | Y | Y | 3 |
| Garemo and Naimi, 2018 [95] | N | N | N | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | N | N | N | 2 |
| Hearst et al., 2013 [96] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Heredia-Blonval et al., 2014 [97] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Hobin et al., 2014 [98] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Jacobson et al., 2013 [99] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Jarlenski et al., 2016 [100] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Khan et al., 2018 [101] | Y | Y | Y | N | N | N | N | N | N | N | N | N | N/A | N/A | N/A | N/A | N/A | N/A | N | Y | Y | Y | Y | Y | 2 |
| Kirkpatrick et al., 2013 [102] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Mazariegos et al., 2016 [103] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Moran et al., 2017 [104] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| O’Donnell et al., 2008 [105] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Prentice et al., 2015 [106] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Reeves et al., 2011 [107] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Roberts et al., [108] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Rudelt et al., 2014 [109] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Schoffman et al., 2016 [110] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Scourboutakos and L’Abbé, 2012 [111] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N | N | N | N | N | N | Y | Y | Y | Y | Y | Y | 3 |
| Scourboutakos et al., 2013 [112] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Scourboutakos et al., 2016 [113] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Scourboutakos and L’Abbé, 2013 [114] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Scourboutakos et al., 2018 [115] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Scourboutakos et al., 2014 [116] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Sliwa et al., 2016 [117] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Soo et al., 2018 [118] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Stender et al., 2006 [119] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Uechi, 2018 [120] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Urban et al., 2014 [121] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Urban et al., 2014 [122] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Waterlander et al., 2014 [123] | Y | Y | Y | Y | Y | Y | Y | Y | Y | N | N | N | N | N | N | N | N | N | N | N | N | N | N | N | 1 |
| Wellard et al., 2012 [124] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Wellard-Cole et al., 2018 [125] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Wolfson et al., 2018 [126] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 3 |
| Ziauddeen et al., 2015 [127] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | N/A | N/A | N/A | N/A | Y | Y | Y | Y | Y | Y | 3 |
| Lead Author, Year | Country | Study Design | Methods and Data Sources | Data Collection Period | Outcomes Measured #: Type | Chains Examined #: Type |
|---|---|---|---|---|---|---|
| Ahuja et al., 2015 [79] | USA | Cross-sectional | Menu info from restaurant websites, meal samples, lab analyses | 2010–2013 | 2: sodium (mg), sodium density (mg/100 g) | 4 QSR chains |
| Astiasarán et al., 2017 [80] | Spain | Cross-sectional | Lab analysis of fries using gas chromatography | 2017 | 4: energy (kcal), energy density (kcal/100 g), fat (g), TFA (g/100 g fat) | 5 QSR chains |
| Auchincloss et al., 2014 [81] | USA | Cross-sectional | Menu info from restaurant websites | 2011 | 4: energy (kcal), saturated fat (g), sodium (mg), sodium density (mg/1000 kcal) | 21 QSR, FCR and FSR chains |
| Bauer et al., 2012 [82] | USA | Longitudinal | Menu info from restaurant websites analyzed by University of Minnesota Nutrient Database | 2006–2010 | 3: energy (kcal), saturated fat (g), sodium (mg) | 8 QSR chains |
| Bleich et al., 2015 [83] | USA | Longitudinal | MenuStat Database | 2012–2013 | 1: energy (kcal) | 66 QSR, FCR and FSR chains |
| Bleich et al., 2016 [84] | USA | Longitudinal | MenuStat Database | 2012–2014 | 1: energy (kcal) | 66 QSR, FCR and FSR chains |
| Bleich et al., 2017 [85] | USA | Longitudinal | MenuStat Database | 2008 and 2012–2015 | 1: energy (kcal) | 44 QSR, FCR and FSR chains |
| Brindal et al., 2008 [86] | Australia | Cross-sectional | Menu info from restaurant websites, onsite visits, phone calls | 2005 | 3: energy (kcal), fat (g), saturated fat (g) | 6 QSR chains |
| Bruemmer et al., 2012 [87] | USA | Cross-sectional | Menu info from restaurant onsite visits and audits | 2009–2010 | 3: energy (kcal), saturated fat (g), sodium (mg) | 37 QSR, FCR and FSR chains |
| Chand et al., 2012 [88] | New Zealand | Cross-sectional | Menu info from restaurant websites, onsite visits, phone calls | 2010–2011 | 5: energy (kJ), fat (g), saturated fat (g), sugar (g), sodium (mg) | 12 QSR chains |
| Cohen et al., 2016 [78] | USA | Cross-sectional | Menustat Database and Delphi method to survey nutrition experts (n = 15) about ideal portion size for children’s menu items | 2012–2016 | 2: energy (kcal), portion size | 200 QSR, FCR and FSR and non-chain restaurants |
| Deierlein et al., 2015 [89] | USA | Cross-sectional | Menu info from restaurant websites | 2010 and 2014 | 6: energy (kcal), energy from fat (%), fat (g), saturated fat (g), energy from saturated fat (%), sodium (mg) | 29 QSR, FCR and FSR chains |
| Dunford et al., 2010 [90] | Australia | Cross-sectional | Survey of menu info from restaurant websites | 2009 | 5: energy (kcal), fat (g), saturated fat (g), sugar (g), sodium (mg) | 9 QSR chains |
| Dunford et al., 2012 [91] | Australia, Canada, France, New Zealand, UK, USA | Cross-sectional | Survey of menu info from restaurant websites | 2010 | 2: salt (mg), sodium density (mg/100 g) | 6 QSR chains |
| Eissa et al., 2017 [92] | USA | Cross-sectional | MenStat Database | 2012–2014 | 5: fat (g), saturated fat (g), TFA (g), sugar (g), portion size (g) | 42 QSR and FSR chains |
| Eyles et al., 2018 [93] | New Zealand | Cross-sectional | Annual surveys of menu info from restaurant websites | 2012–2016 | 4: energy (kJ), energy density (kJ/100 g), sodium (mg), portion size (g) | 10 QSR chins |
| Garcia et al., 2014 [94] | Australia | Cross-sectional | Survey of menu info from restaurant websites | 2009–2012 | 2: sodium (mg), sodium density (mg/100 g and mg/serving) | 6 QSR chains |
| Garemo and Naimi, 2018 [95] | UAE | Cross-sectional | Children’s menus collected and analyzed combined with onsite visits to question restaurant staff | 2016 | 3: energy (kcal), fat (g), sugar (g) | 58 restaurants |
| Hearst et al., 2013 [96] | USA | Sequential cross-sectional | Menu info from restaurant websites analyzed by University of Minnesota Nutrient Database | 2001–2002, 2003–2004, 2005–2006, 2007–2008, 2009–2010 | 3: energy (kcal), sodium (g), saturated fat (g) | 8 QSR chains |
| Heredia-Blonval et al., 2014 [97] | Costa Rica | Cross-sectional | Menu info from restaurant websites | 2013 | 3: energy (kcal), salt (mg), sodium density (mg/100 g and mg/serving) | 7 QSR chains |
| Hobin et al., 2014 [98] | Australia, Canada, New Zealand, UK, USA | Cross-sectional | Children’s menu info from restaurant websites or phone calls | 2012 | 5: energy (kcal), fat (g), saturated fat (g), sodium (mg), serving size (g) | 4 QSR chains |
| Jacobson et al., 2013 [99] | USA | Longitudinal | Menu info from restaurant websites | 2005–2011 | 1: sodium (g) | 16 QSR and FCR chains |
| Jarlenski et al., 2016 [100] | USA | Longitudinal | MenuStat Database | 2012–2014 | 4: energy (kcal), fat (g), saturated fat (g), sugar (g) | 37 QSR and FCR chains |
| Khan et al., 2018 [101] | Australia, Egypt, India, USA | Cross-sectional | Menu info from restaurant websites or print materials | 2015 | 2: energy (kcal), sodium density (g/100 g) | 3 QSR chains |
| Kirkpatrick et al., 2013 [102] | USA | Cross-sectional | Children’s menu info from restaurant websites | 2008–2009 | 5: energy (kcal), energy from fat (%), energy from added sugars (%), saturated fat (g), sodium (g) | 5 QSR chains |
| Mazariegos et al., 2016 [103] | Guatemala | Cross-sectional | Children’s menu info from restaurant websites, onsite visits or phone calls | 2016 | 6: energy (kcal), sodium (mg), sugar (g), TFA (g), saturated fat (%), energy from fat (%) | 6 QSR chains |
| Moran et al., 2017 [104] | USA | Cross-sectional | Children’s menu items from MenuStat Database | 2012–2015 | 3: energy (kcal), sodium (mg), saturated fat (g) | 45 QSR, FCR and FSR chains |
| O’Donnell et al., 2008 [105] | USA | Cross-sectional | Menu items from restaurant websites and phone calls | 2007 | 6: energy (kcal), fat (g), energy from fat (%), saturated fat (g), sugars (g), sodium (mg) | 10 QSR chains |
| Prentice et al., 2015 [106] | New Zealand | Cross-sectional | Menu items from restaurant websites | 2008–2009 | 1: sodium (mg) | 8 QSR chains |
| Reeves et al., 2011 [107] | England | Cross-sectional | Menu items from restaurant websites | 2009 | 4: energy (kcal), fat (g), sodium (mg), portion size (g) | 7 QSR chains and 15 non-chain FSR |
| Roberts et al., [108] | Brazil, China, Finland, Ghana, India, USA | Cross-sectional | Menu items from restaurant websites, onsite visits, and lab analysis of selected items using bomb calorimetry | 2014 and 2017 | 2: energy (kcal), energy density (kcal/g) | 111 QSR and FSR chains |
| Rudelt et al., 2014 [109] | USA | Cross-sectional | Menu info from restaurant websites analyzed by University of Minnesota Nutrient Database | 2000 and 2009/2010 | 1: sodium (mg) | 8 QSR chains |
| Schoffman et al., 2016 [110] | USA | Cross-sectional | MenuStat Database | 2014 | 1: energy (kcal) | 62 QSR and FCR chains |
| Scourboutakos and L’Abbé, 2012 [111] | Canada | Cross-sectional | Menu items from restaurant websites | 2010 | 3: energy (kcal), energy density (% kcal/100 g food), portion size (g) | 85 QSR and FSR chains |
| Scourboutakos et al., 2013 [112] | Canada | Cross-sectional | Menu items from restaurant websites | 2910–2011 | 5: energy (kcal), fat (g), saturated fat (g), TFA (g), sodium (mg) | 19 FSR chains |
| Scourboutakos et al., 2016 [113] | Canada | Cross-sectional | Menu items from restaurant websites | 2010 | 2: total sugar (g), added sugar (g) | 17 QSR and FSR chains |
| Scourboutakos and L’Abbé, 2013 [114] | Canada | Cross-sectional | Canadian MENU-Food Label Information Program (FLIP) Database of nutrition info of restaurant menu items | 2010 | 1: sodium (mg) | 85 QSR and FSR chains |
| Scourboutakos et al., 2018 [115] | Canada | Longitudinal | Menu items from restaurant websites | 2010–2016 | 1: sodium (mg) | 12 QSR, FCR and FSR chains |
| Scourboutakos et al., 2014 [116] | Canada | Longitudinal | Menu items from restaurant websites | 2010–2013 | 4: energy (kcal), sodium (mg), sodium density (mg/100 g), portion size (g) | 61 QSR, FCR and FSR chains |
| Sliwa et al., 2016 [117] | USA | Cross-sectional | Children’s menu info from restaurant websites | 2014 | 5: energy (kcal), fat (g), saturated fat (g), sodium (mg), portion size (g) | 20 QSR, FCR and FSR chains |
| Soo et al., 2018 [118] | USA | Cross-sectional | Menu info from restaurant signs and menu boards | 2010 and 2013 | 5: energy (kcal), saturated fat (g), sugar (g), sodium (mg), portion size (g) | 4 QSR chains |
| Stender et al., 2006 [119] | Austria, Czech Republic, Denmark, England, Hungary Finland, France Germany, Italy Netherlands, Norway Peru, Poland Portugal, Russia Scotland, Spain South Africa, Sweden, USA | Cross-sectional | Lab analysis of two items (i.e., chicken and fries) at each restaurant chain using gas chromatography | 2004 and 2005 | 1: TFA (g) | 2 QSR chains |
| Uechi, 2018 [120] | Japan | Cross-sectional | Children’s menu info from restaurant websites | 2017 | 4: energy (kJ), sugar (g), fat (g), sodium (mg) | 20 restaurant chains |
| Urban et al., 2014 [121] | USA | Longitudinal | Children’s menu info from restaurant websites | 2000–2013 | 4: energy (kcal), sodium (mg), saturated fat (g), TFA (g) | 3 QSR chains |
| Urban et al., 2014 [122] | USA | Longitudinal | Children’s menu info from restaurant websites | 2000–2013 | 3: sodium density (mg/1000 kcal), saturated fat (g/1000 kcal), TFA (g/1000 kcal) | 3 QSR chains |
| Waterlander et al., 2014 [123] | New Zealand | Cross-sectional | Children’s menu info from restaurant websites | 2014 | 4: energy (kcal), saturated fat (g), sugar (g), sodium (mg) | 4 QSR chains |
| Wellard et al., 2012 [124] | Australia | Cross-sectional | Children’s menu info from restaurant websites | 2010 | 4: energy (kJ), saturated fat (g), sugar (g), sodium (mg) | 6 QSR chains |
| Wellard-Cole et al., 2018 [125] | Australia | Cross-sectional | Children’s menu info from restaurant websites | 2009 and 2015 | 2: energy (kJ), energy density (kJ/100 g and kJ/serving) | 5 QSR chains |
| Wolfson et al., 2018 [126] | USA | Cross-sectional | MenuStat Database | 2012 and 2016 | 1: sodium (mg) | 66 QSR, FCR and FSR chains |
| Ziauddeen et al., 2015 [127] | Australia, Canada, China, Germany, Japan, Netherlands, New Zealand, UAE, UK, USA | Cross-sectional | Menu info from restaurant websites | 2012 | 3: energy (kcal), fat (g), saturated fat (g) | 5 QSR chains |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kraak, V.; Rincón-Gallardo Patiño, S.; Renukuntla, D.; Kim, E. Progress Evaluation for Transnational Restaurant Chains to Reformulate Products and Standardize Portions to Meet Healthy Dietary Guidelines and Reduce Obesity and Non-Communicable Disease Risks, 2000–2018: A Scoping and Systematic Review to Inform Policy. Int. J. Environ. Res. Public Health 2019, 16, 2732. https://doi.org/10.3390/ijerph16152732
Kraak V, Rincón-Gallardo Patiño S, Renukuntla D, Kim E. Progress Evaluation for Transnational Restaurant Chains to Reformulate Products and Standardize Portions to Meet Healthy Dietary Guidelines and Reduce Obesity and Non-Communicable Disease Risks, 2000–2018: A Scoping and Systematic Review to Inform Policy. International Journal of Environmental Research and Public Health. 2019; 16(15):2732. https://doi.org/10.3390/ijerph16152732
Chicago/Turabian StyleKraak, Vivica, Sofia Rincón-Gallardo Patiño, Deepthi Renukuntla, and Eojina Kim. 2019. "Progress Evaluation for Transnational Restaurant Chains to Reformulate Products and Standardize Portions to Meet Healthy Dietary Guidelines and Reduce Obesity and Non-Communicable Disease Risks, 2000–2018: A Scoping and Systematic Review to Inform Policy" International Journal of Environmental Research and Public Health 16, no. 15: 2732. https://doi.org/10.3390/ijerph16152732
APA StyleKraak, V., Rincón-Gallardo Patiño, S., Renukuntla, D., & Kim, E. (2019). Progress Evaluation for Transnational Restaurant Chains to Reformulate Products and Standardize Portions to Meet Healthy Dietary Guidelines and Reduce Obesity and Non-Communicable Disease Risks, 2000–2018: A Scoping and Systematic Review to Inform Policy. International Journal of Environmental Research and Public Health, 16(15), 2732. https://doi.org/10.3390/ijerph16152732







