Housing Design and Community Care: How Home Modifications Reduce Care Needs of Older People and People with Disability
Abstract
1. Introduction
1.1. Home Modifications
1.1.1. Preventing Falls and Improving Safety
1.1.2. Improved Function and Independence
1.1.3. Physical Health and Wellbeing
1.1.4. Ageing Process
1.1.5. Caregiving
1.2. Concepts of Community Care and Housing
1.3. Substitution of Care
2. Materials and Methods
Sample Response Rate
3. Results
3.1. Descriptive Statistics
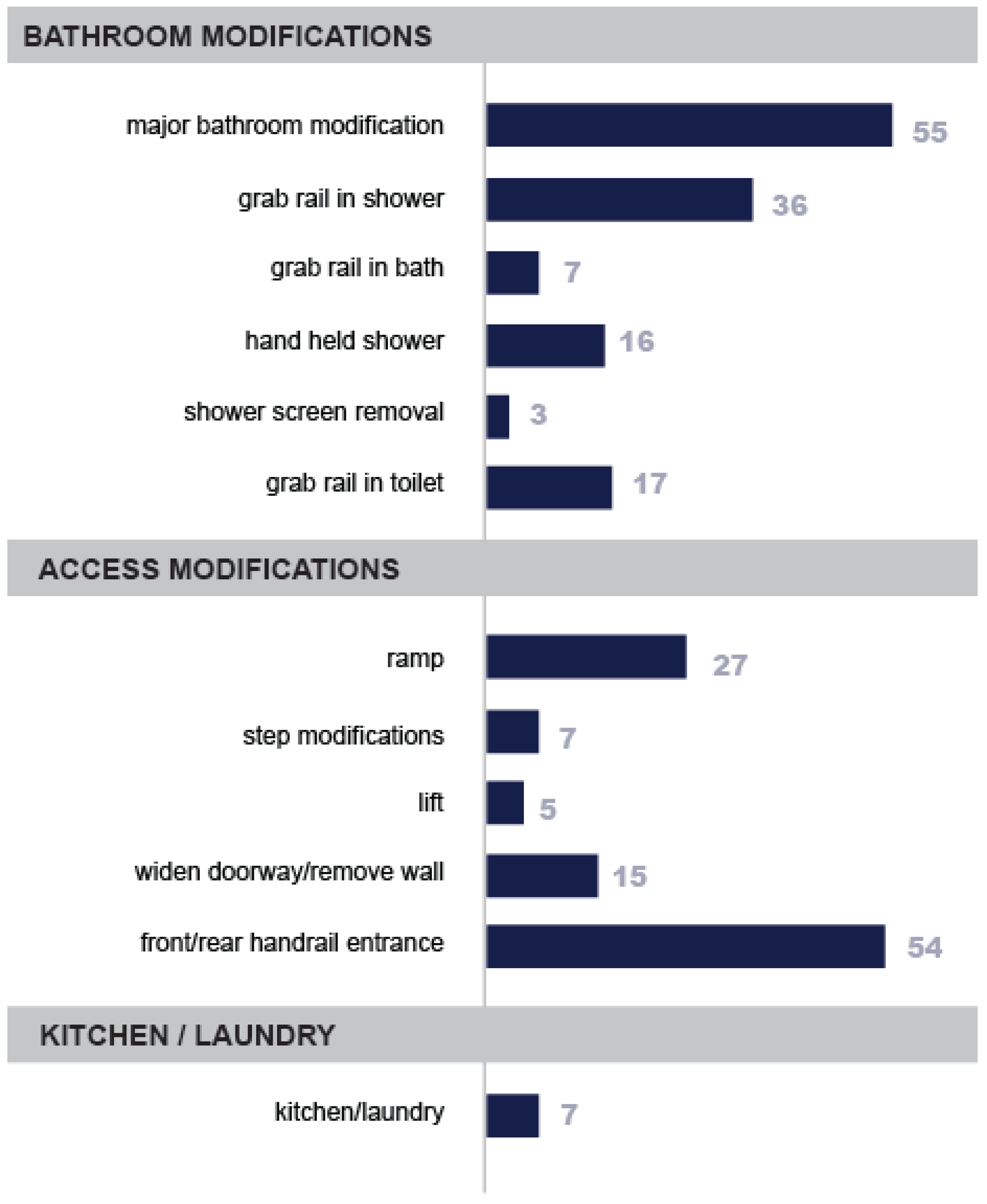
3.2. Home Modification Results
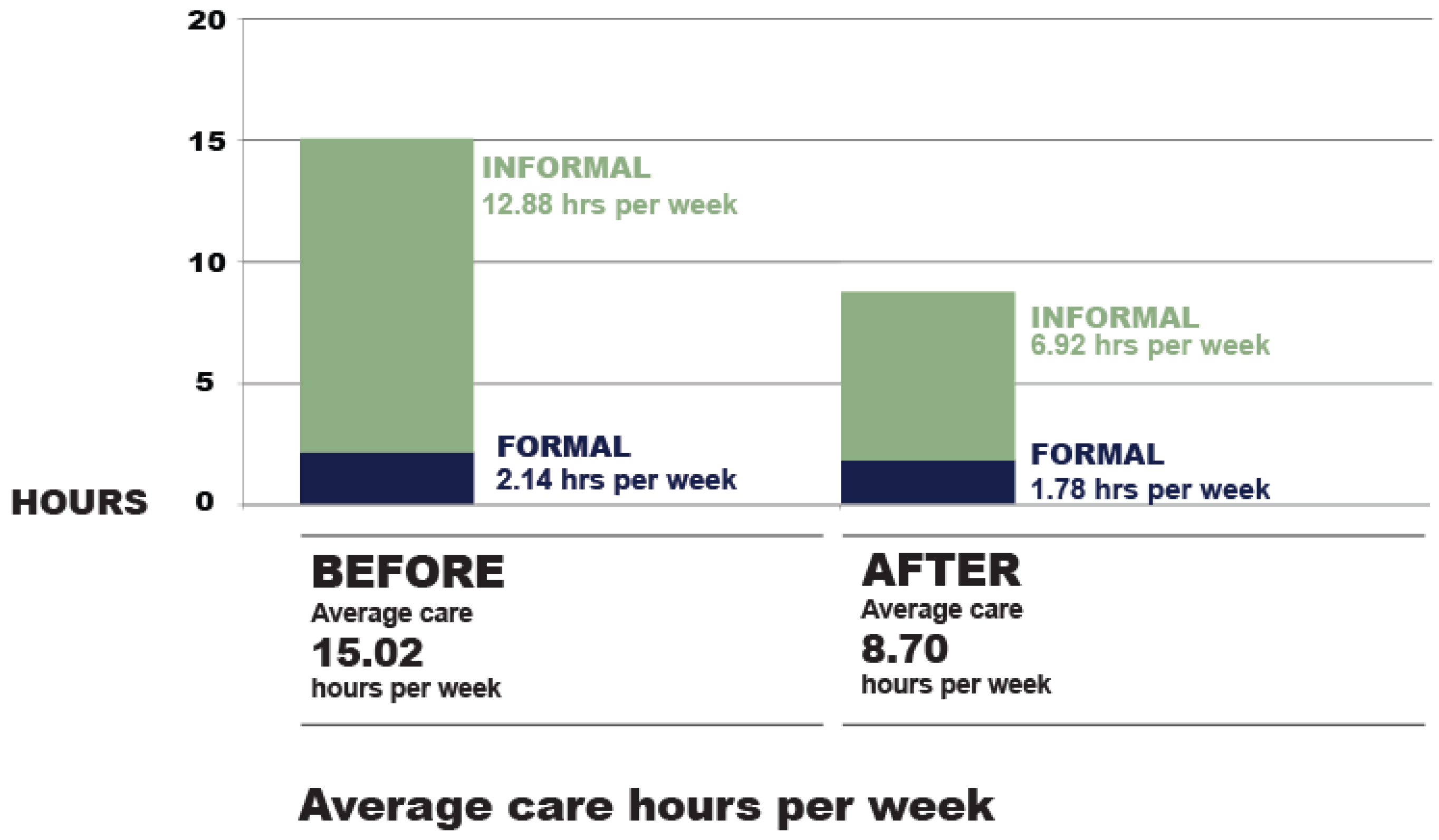
3.3. Care Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Oswald, F.; Wahl, H.W.; Schilling, O.; Nygren, C.; Fänge, A.; Sixsmith, A.; Iwarsson, S. Relationships between housing and healthy aging in very old age. Gerontologist 2007, 47, 96–107. [Google Scholar] [CrossRef] [PubMed]
- Carnemolla, P.; Bridge, C. A scoping review of home modifications interventions—Mapping the evidence base. Indoor Built Environ. 2018. [Google Scholar] [CrossRef]
- Altman, B.; Barnartt, S. Environmental Contexts and Disability; Emerald Group Publishing: London, UK, 2014; Volume 8. [Google Scholar]
- Straton, J.; Saunders, N.; Broe, T.; Brown, W.; Earle, L.; Gregory, B. Promoting Healthy Ageing in Australia. Available online: http://www.dest.gov.au/science/pmseic/documents/promoting healthy ageing report.doc (accessed on 12 January 2015).
- Cangiano, A.; Shutes, I.; Spencer, S.; Leeson, G. Migrant Care Workers in Ageing Societies: Research Findings in the UK; University of Oxford: Oxford, UK, 2009. [Google Scholar]
- Kelly, J. Industry View ACSA: Calling Attention to Ageing. From Australian Ageing Agenda, Nov/Dec 2013. 2013, p. 18. Available online: http://search.informit.com.au/documentSummary;dn=139496239444751;res=IELHEA (accessed on 25 May 2015).
- Simonazzi, A. Care regimes and national employment models. Camb. J. Econ. 2009, 33, 211–232. [Google Scholar] [CrossRef]
- Adams, T.; Bridge, C.; Carnemolla, P.; McNamara, N.; Quinn, J. Consumer Factsheet: Arranging Home Modifications. In Consumer Factsheet Series; Home Modification Information Clearinghouse: Sydney, Australia, 2014. [Google Scholar]
- Fänge, A.; Iwarsson, S. Changes in ADL dependence and aspects of usability following housing adaptation—A longitudinal perspective. Am. J. Occupational Ther. 2005, 59, 296–304. [Google Scholar] [CrossRef]
- Pynoos, J. Toward a national policy on home modification. Technol. Disabil. 1993, 2, 1–8. [Google Scholar]
- Johansson, K.; Lilja, M.; Petersson, I.; Borell, L. Performance of activities of daily living in a sample of applicants for home modification services. Scand. J. Occup. Ther. 2007, 14, 44–53. [Google Scholar] [CrossRef]
- Lord, S.; Menz, H.; Sherrington, C. Home environment risk factors for falls in older people and the efficacy of home modifications. Age Ageing 2006, 35, 55–59. [Google Scholar] [CrossRef]
- Coyte, P.C.; McKeever, P. Home care in Canada: Passing the buck. Can. J. Nursing Res 2001, 33, 11–26. [Google Scholar]
- Chang, J.T.; Morton, S.C.; Rubenstein, L.Z.; Mojica, W.A.; Maglione, M.; Suttorp, M.J.; Shekelle, P.G. Interventions for the prevention of falls in older adults: Systematic review and meta-analysis of randomised clinical trials. BMJ 2004, 328, 680. [Google Scholar] [CrossRef]
- Clemson, L.; Mackenzie, L.; Ballinger, C.; Close, J.; Cumming, R. Environmental interventions to prevent falls in community-dwelling older people a meta-analysis of randomized trials. J. Aging Health 2008, 20, 954–971. [Google Scholar] [CrossRef]
- Tse, T. The environment and falls prevention: Do environmental modifications make a difference? Aust. Occup. Ther. J. 2005, 52, 271–281. [Google Scholar] [CrossRef]
- Turner, S.; Arthur, G.; Lyons, R.A.; Weightman, A.L.; Mann, M.K.; Jones, S.J.; Lannon, S.; Rolfe, B.; Kemp, A.; Johansen, A. Modification of the home environment for the reduction of injuries. Cochrane Database Syst. Rev. 2011, 16. [Google Scholar] [CrossRef] [PubMed]
- Powell, J.; Mackintosh, S.; Bird, E.; Ige, J.; Garrett, H.; Roys, M. The role of home adaptations in later life. Centre for Ageing Better, University of the West of England, BRE. Available online: https://www.ageing-better.org.uk/sites/default/files/2017-12/The%20role%20of%20home%20adaptations%20in%20improving%20later%20life.pdf (accessed on 12 May 2019).
- Wahl, H.; Fänge, A.; Oswald, F.; Gitlin, L.; Iwarsson, S. The home environment and disability-related outcomes in aging individuals: What is the empirical evidence? Gerontologist 2009, 49, 355–367. [Google Scholar] [CrossRef] [PubMed]
- Chase, C.; Mann, K.; Wasek, S.; Arbesman, M. Systematic review of the effect of home modification and fall prevention programs on falls and the performance of community-dwelling older adults. Am. J. Occup. Ther. 2012, 66, 284–291. [Google Scholar] [CrossRef]
- Gitlin, L.; Corcoran, M.; Winter, L.; Boyce, A.; Hauck, W. A randomized, controlled trial of a home environmental intervention: Effect on efficacy and upset in caregivers and on daily function of persons with dementia. Gerontologist 2001, 41, 4. [Google Scholar] [CrossRef]
- Mann, W.; Ottenbacher, K.; Fraas, L.; Tomita, M.; Granger, C. Effectiveness of assistive technology and environmental interventions in maintaining independence and reducing home care costs for the frail elderly: A randomized controlled trial. Arch. Family Med. 1999, 8, 210–217. [Google Scholar] [CrossRef]
- Szanton, S.; Wolff, J.; Leff, B.; Thorpe, R.; Tanner, E.; Boyd, C.; Gitlin, L. CAPABLE trial: A randomized controlled trial of nurse, occupational therapist and handyman to reduce disability among older adults: Rationale and design. Contemp. Clin. Trials 2014, 38, 102–112. [Google Scholar] [CrossRef]
- Wilson, D.; Mitchell, J.; Kemp, B.; Adkins, R.; Mann, W. Effects of assistive technology on functional decline in people aging with a disability. Assist. Technol. 2009, 21, 208–217. [Google Scholar] [CrossRef]
- Sheffield, C.; Smith, C.; Becker, M. Evaluation of an Agency-Based Occupational Therapy Intervention to Facilitate Aging in Place. Gerontologist 2013, 53, 907–918. [Google Scholar] [CrossRef][Green Version]
- Ahmad, J.; Shakil-ur-Rehman, S.; Sibtain, F. Effectiveness of home modification on quality of life on wheel chair user paraplegic population. Rawal Med. J. 2013, 38, 263–265. [Google Scholar]
- Lin, M.; Wolf, S.; Hwang, H.; Gong, S.; Chen, C. A randomized, controlled trial of fall prevention programs and quality of life in older fallers. J. Am. Geriatr. Soc. 2007, 55, 499–506. [Google Scholar] [CrossRef]
- Heywood, F.; Turner, L. Better Outcomes, Lower Costs. Implications for Health and Social Care Budgets of Investment in Housing Adaptations, Improvements and Equipment: Review of the Evidence; London Office for Disability Issues/Department of Work and Pensions: London, UK, 2007. [Google Scholar]
- Andrich, R.; Ferrario, M.; Moi, M. A model of cost-outcome analysis for assistive technology. Disability Rehabil. 1998, 20, 1–24. [Google Scholar] [CrossRef]
- Mitoku, K.; Shimanouchi, S. Home Modification and Prevention of Frailty Progression in Older Adults: A Japanese Prospective Cohort Study. J. Gerantol. Nursing 2014, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Hwang, E.; Cummings, L.; Sixsmith, A.; Sixsmith, J. Impacts of home modifications on aging-in-place. J. Housing Elderly 2011, 25, 246–257. [Google Scholar] [CrossRef]
- Safran-Norton, C. Physical home environment as a determinant of aging in place for different types of elderly households. J. Housing Elderly 2010, 24, 208–231. [Google Scholar] [CrossRef]
- Pettersson, C.; Löfqvist, C.; Malmgren Fänge, A. Clients’ experiences of housing adaptations: A longitudinal mixed-methods study. Disability Rehabil. 2012, 34, 1706–1715. [Google Scholar] [CrossRef]
- Tanner, B.; Tilse, C.; De Jonge, D. Restoring and sustaining home: The impact of home modifications on the meaning of home for older people. J. Housing Elderly 2008, 22, 195–215. [Google Scholar] [CrossRef]
- Renaut, S.; Ogg, J.; Petite, S.; Chamahian, A. Home environments and adaptations in the context of ageing. Ageing Soc. 2014, 1–26. [Google Scholar] [CrossRef]
- Ahn, M.; Hegde, A. Perceived aspects of home environment and home modifications by older people living in rural areas. J. Housing Elderly 2011, 25, 18–30. [Google Scholar] [CrossRef]
- Agree, E.; Freedman, V.; Cornman, J.; Wolf, D.; Marcott, J. Reconsidering substitution in long-term care: When does assistive technology take the place of personal care? J. Gerontol. Series B Psychol. Sci. Soc. Sci. 2005, 60, 272–280. [Google Scholar] [CrossRef] [PubMed]
- Anderson, W.; Wiener, J. The impact of assistive technologies on formal and informal home care. Gerontologist 2013. [Google Scholar] [CrossRef] [PubMed]
- Naik, A.D.; Gill, T. Underutilization of environmental adaptations for bathing in community-living older persons. J. Am. Geriatrics Soc. 2005, 53, 1497–1503. [Google Scholar] [CrossRef] [PubMed]
- Newman, S.; Struyk, R.; Wright, P.; Rice, M. Overwhelming odds: Caregiving and the risk of institutionalization. J. Gerontol. 1990, 45, 173–183. [Google Scholar] [CrossRef]
- Hemingway, L. Disabled People and Housing: Choices, Opportunities and Barriers; Policy Press: Bristol, UK, 2011. [Google Scholar]
- Golant, S.M. The quest for residential normalcy by older adults: Relocation but one pathway. J. Aging Stud. 2011, 25, 193–205. [Google Scholar] [CrossRef]
- Beer, A.; Faulkner, D. The Housing Careers of People with a Disability and Carers of People with a Disability; Australian Housing and Urban Research Institute: Melbourne, Australia, 2008. [Google Scholar]
- Andrews, G.; Faulkner, D.; Andrews, M. A Glossary of Terms for Community Health Care and Services for Older Persons; World Health Organisation: Paris, France, 2004. [Google Scholar]
- Agree, E.; Freedman, V. Incorporating assistive devices into community-based long-term care: An analysis of the potential for substitution and supplementation. J. Aging Health 2000, 12, 426. [Google Scholar] [CrossRef] [PubMed]
- Bonsang, E. Does informal care from children to their elderly parents substitute for formal care in Europe? J. Health Econ. 2009, 28, 143–154. [Google Scholar] [CrossRef] [PubMed]
- Australian Bureau of Statistics. Disability, Ageing and Carers, Australia: Summary of Findings, 2012; Australian Government Publishing Service: Canberra, Australia, 2012.
- Australian Bureau of Statistics. Focus on Families: Caring Infamilies—Support for Persons Who are Older or Have Disabilities; Australian Government Publishing Service: Canberra, Australia, 1995.
- Liu, K.; Manton, K.; Aragon, C. Changes in home care use by disabled elderly persons 1982–1994. J. Gerontol. Series B Psychol. Sci. Soc. Sci. 2000, 55, 245–253. [Google Scholar] [CrossRef] [PubMed]
- Pinquart, M.; Sörensen, S. Correlates of physical health of informal caregivers: A meta-analysis. J. Gerontol. Series B Psychol. Sci. Soc. Sci. 2007, 62, 126–137. [Google Scholar] [CrossRef] [PubMed]
- Bittman, M.; Hill, T.; Thomson, C. The impact of caring on informal carers’ employment, income and earnings: A longitudinal approach. Aust. J. Soc. Issues 2007, 42, 255–272. [Google Scholar] [CrossRef]
- Bolin, K.; Lindgren, B.; Lundborg, P. Informal and formal care among single-living elderly in Europe. Health Econ. 2008, 17, 393–409. [Google Scholar] [CrossRef]
- Van Houtven, C.H.; Coe, N.B.; Skira, M.M. The effect of informal care on work and wages. J. Health Econ. 2013, 32, 240–252. [Google Scholar] [CrossRef] [PubMed]
- Carers Australia. Combining Work and Care: The Benefits to Carers and the Economy. In Work and Care: The Necessary Investment; Carers Australia: Canberra, Australia, 2014. [Google Scholar]
- Davies, R.; Gray, C. Care pathways and designing the health-care built environment: An explanatory framework. Int. J. Care Pathw. 2009, 13, 7–16. [Google Scholar] [CrossRef]
- Ham, C.; Dixon, A.; Brooke, B. Transforming the Delivery of Health and Social Care. The Case for Fundamental Change; King’s Fund: London, UK, 2012. [Google Scholar]
- Desai, M.; Lentzner, H.; Weeks, J. Unmet need for personal assistance with activities of daily living among older adults. Gerontologist 2001, 41, 82–88. [Google Scholar] [CrossRef]
- Lansley, P.; McCreadie, C.; Tinker, A. Can adapting the homes of older people and providing assistive technology pay its way? Age Ageing 2004, 33, 571–576. [Google Scholar] [CrossRef] [PubMed]
- Australian Government. Housing Decisions of Older Australians, Productivity Commission Research Paper; Australian Government Publishing Service: Canberra, Australia, 2015.
- Jutkowitz, E.; Gitlin, L.; Pizzi, L.; Lee, E.; Dennis, M. Cost Effectiveness of a Home Based Intervention That Helps Functionally Vulnerable Older Adults Age in Place at Home. J. Aging Res. 2012. [Google Scholar] [CrossRef] [PubMed]
| Count | Percentage of Total Sample | |
|---|---|---|
| Mean age (years) | 72 | |
| Gender | 157 | |
| Female | 85 | 54.1% |
| Male | 72 | 45.9% |
| Housing tenure | ||
| Being purchased | 2 | 1.27% |
| Fully owned | 149 | 94.90% |
| Live with family members | 2 | 1.27% |
| Own caravan/annex and rent site | 1 | 0.64% |
| Rental (private) | 2 | 1.27% |
| Retirement village | 1 | 0.64% |
| Living arrangements | ||
| Lives alone | 43 | 26.75% |
| Lives with a spouse or partner | 84 | 53.50% |
| Lives with family or friends | 30 | 19.11% |
| Income source | ||
| Carers allowance | 2 | 1.27% |
| Disability support pension | 28 | 17.83% |
| Full aged pension | 102 | 64.97% |
| Part aged pension | 16 | 10.19% |
| Self-funded retiree | 8 | 5.10% |
| Wage or salary (full time) | 1 | 0.64% |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Carnemolla, P.; Bridge, C. Housing Design and Community Care: How Home Modifications Reduce Care Needs of Older People and People with Disability. Int. J. Environ. Res. Public Health 2019, 16, 1951. https://doi.org/10.3390/ijerph16111951
Carnemolla P, Bridge C. Housing Design and Community Care: How Home Modifications Reduce Care Needs of Older People and People with Disability. International Journal of Environmental Research and Public Health. 2019; 16(11):1951. https://doi.org/10.3390/ijerph16111951
Chicago/Turabian StyleCarnemolla, Phillippa, and Catherine Bridge. 2019. "Housing Design and Community Care: How Home Modifications Reduce Care Needs of Older People and People with Disability" International Journal of Environmental Research and Public Health 16, no. 11: 1951. https://doi.org/10.3390/ijerph16111951
APA StyleCarnemolla, P., & Bridge, C. (2019). Housing Design and Community Care: How Home Modifications Reduce Care Needs of Older People and People with Disability. International Journal of Environmental Research and Public Health, 16(11), 1951. https://doi.org/10.3390/ijerph16111951





