The Trade-Off between Optimizing Flight Patterns and Human Health: A Case Study of Aircraft Noise in Queens, NY, USA
Abstract
1. Introduction
2. Materials and Methods
2.1. Impacts of the Year-Round Use of TNNIS on Noise
2.2. Health Impacts of the Year-Round Use of TNNIS
2.3. Economic Impacts of the Year-Round Use of TNNIS
2.4. Simulation Model
2.5. Model Parameters
2.5.1. Background Rates and Probabilities
2.5.2. Other Costs Parameters
2.5.3. Health State Utility Values
2.5.4. Analysis
3. Results
3.1. Base Case Results
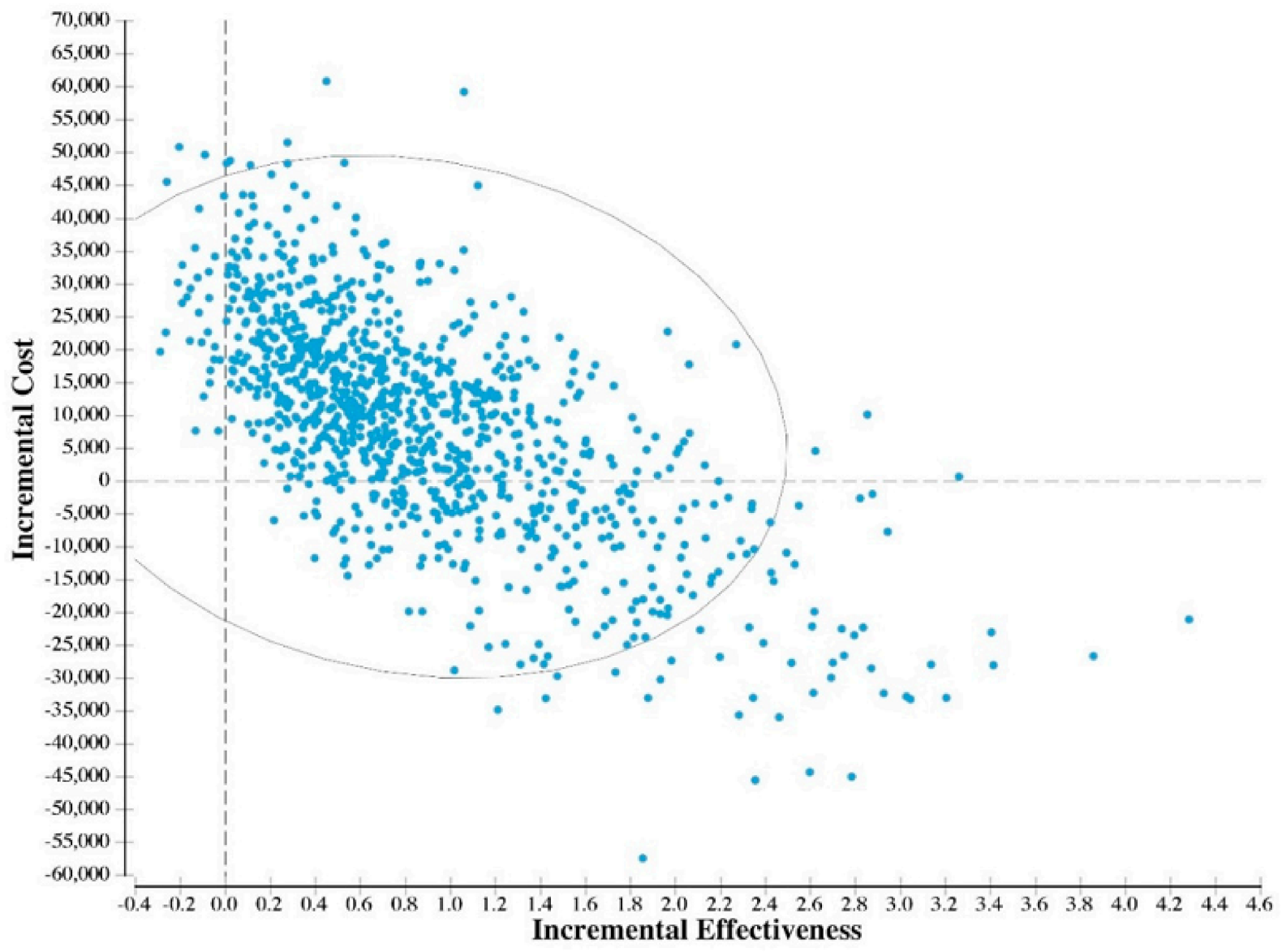
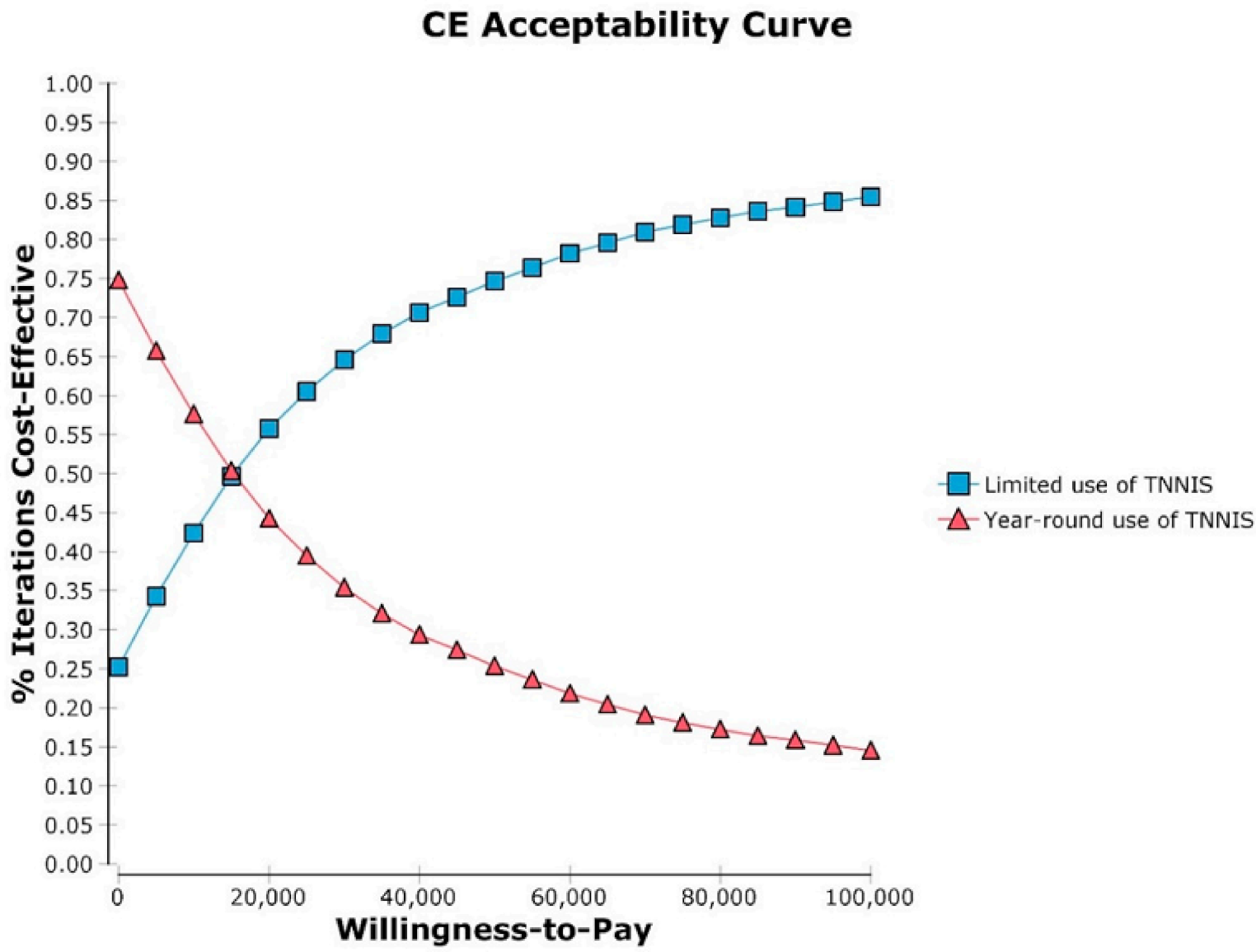
3.2. Probabilistic Results
3.3. One-Way Sensitivity Analysis
3.4. Scenario Analysis
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Prevot, T.; Homola, J.; Mercer, J.; Mainini, M.; Cabrall, C. Initial evaluation of NextGen air/ground operations with ground-based automated separation assurance. In Proceedings of the Eighth USA/Europe Air Traffic Management Research and Development Seminar, Napa, CA, USA, 29 June–2 July 2009. [Google Scholar]
- Nolan, M.S. Fundamentals of Air Traffic Control, 5th ed.; Delmar Cengage Learning: Clifton Park, NY, USA, 2010; 672p. [Google Scholar]
- Chiappe, D.; Vu, K.-P.L.; Strybel, T. Situation awareness in the NextGen air traffic management system. Int. J. Hum. Comput. Interact. 2012, 28, 140–151. [Google Scholar] [CrossRef]
- Strohmeier, M.; Schafer, M.; Lenders, V.; Martinovic, I. Realities and challenges of nextgen air traffic management: The case of ADS-B. IEEE Commun. Mag. 2014, 52, 111–118. [Google Scholar] [CrossRef]
- WebTrak: The Port Authority of New York and New Jersey. Available online: http://webtrak5.bksv.com/panynj4 (accessed on 2 June 2017).
- The Port Authority of NY & NJ, Benefit Cost Analysis of Runway 4L/22R RSA Compliance. Available online: http://corpinfo.panynj.gov/files/uploads/documents/freedom-of-information/foi-fulfilled-requests/13591-O.pdf (accessed on 1 March 2018).
- Port Authority NY/NJ Noise Contour Map for LaGuardia Airport (Official Noise Exposure Results of the 14 CFR Part 150 Study), Meeting Presentation for 21 June 2016. Available online: http://panynjpart150.com/LGA_TAC.asp (accessed on 1 March 2018).
- Federal Aviation Adminiatration. NextGen Operational Performance Assessment. Available online: https://www.faa.gov/nextgen/media/NGPA_2014.pdf (accessed on 7 July 2017).
- Queens Quiet Skies. Increases in Laguardia Airport Departures over Northeast Queens, Jackson Heights & Woodside. Available online: http://queensquietskies.org/2016/08/31/increases-in-lga-departures-over-northeast-queens-jackson-heights-woodside/ (accessed on 15 July 2017).
- Federal Aviation Administration. LaGuardia Five Departure. Available online: http://aeronav.faa.gov/d-tpp/1807/00289LAGUARDIA.PDF (accessed on 2 July 2018).
- Berglund, B.; Lindvall, T.; Schwela, D.H.; World Health Organization. Guidelines for Community Noise. 1999. Available online: http://www.who.int/iris/handle/10665/66217 (accessed on 11 July 2017).
- Basner, M.; Babisch, W.; Davis, A.; Brink, M.; Clark, C.; Janssen, S.; Stansfeld, S. Auditory and non-auditory effects of noise on health. Lancet 2014, 383, 1325–1332. [Google Scholar] [CrossRef]
- Beutel, M.E.; Jünger, C.; Klein, E.M.; Wild, P.; Lackner, K.; Blettner, M.; Binder, H.; Michal, M.; Wiltink, J.; Brähler, E.; et al. Noise annoyance Is associated with depression and anxiety in the general population—The contribution of aircraft noise. PLoS ONE 2016, 11, e0155357. [Google Scholar] [CrossRef] [PubMed]
- Hansell, A.L.; Blangiardo, M.; Fortunato, L.; Floud, S.; de Hoogh, K.; Fecht, D.; Ghosh, R.E.; Laszlo, H.E.; Pearson, C.; Beale, L.; et al. Aircraft noise and cardiovascular disease near Heathrow airport in London: Small area study. BMJ 2013, 347, f5432. [Google Scholar] [CrossRef] [PubMed]
- Hardoy, M.C.; Carta, M.G.; Marci, A.R.; Carbone, F.; Cadeddu, M.; Kovess, V.; Dell’Osso, L.; Carpiniello, B. Exposure to aircraft noise and risk of psychiatric disorders: The Elmas survey—Aircraft noise and psychiatric disorders. Soc. Psychiatry Psychiatr. Epidemiol. 2005, 40, 24–26. [Google Scholar] [CrossRef] [PubMed]
- The Port Authority of New York & New Jersey. Laguardia Airport Technical Advisory Committee Meeting No. 8. 2016. Available online: http://panynjpart150.com/LGA_TAC.asp (accessed on 15 July 2017).
- European Environmental Agency. Noise in Europe 2014. Available online: https://www.eea.europa.eu/publications/noise-in-europe-2014 (accessed on 2 March 2018).
- European Environmental Agency. Good Practice Guide on Noise Exposure and Potential Health Effects. Available online: https://www.eea.europa.eu/publications/good-practice-guide-on-noise (accessed on 2 March 2018).
- Holzman, D. Plane pollution. Environ. Health Perspect. 1997, 105, 1300–1305. [Google Scholar] [CrossRef] [PubMed]
- Lawton, R.N.; Fujiwara, D. Living with aircraft noise: Airport proximity, aviation noise and subjective wellbeing in England. Transp. Res. Part D Transp. Environ. 2016, 42, 104–118. [Google Scholar] [CrossRef]
- Lefèvre, M.; Carlier, M.-C.; Champelovier, P.; Lambert, J.; Laumon, B.; Evrard, A.-S. Effects of aircraft noise exposure on saliva cortisol near airports in France. Occup. Environ. Med. 2017, 74, 612–618. [Google Scholar]
- Vienneau, D.; Schindler, C.; Perez, L.; Probst-Hensch, N.; Röösli, M. The relationship between transportation noise exposure and ischemic heart disease: A meta-analysis. Environ. Res. 2015, 138, 372–380. [Google Scholar] [CrossRef] [PubMed]
- Postorino, M.N.; Mantecchini, L.; Paganelli, F. Green Airport Investments to Mitigate Externalities: Procedural and Technological Strategies. In Sustainable Entrepreneurship and Investments in the Green Economy; IGI Global: Hershey, PA, USA, 2017; pp. 231–256. [Google Scholar]
- Postorino, M.N.; Mantecchini, L. A systematic approach to assess the effectiveness of airport noise mitigation strategies. J. Air Transp. Manag. 2016, 50, 71–82. [Google Scholar] [CrossRef]
- Miedema, H.M.; Oudshoorn, C.G. Annoyance from transportation noise: Relationships with exposure metrics DNL and DENL and their confidence intervals. Environ. Health Perspect. 2001, 109, 409–416. [Google Scholar] [CrossRef] [PubMed]
- Floud, S.; Blangiardo, M.; Clark, C.; de Hoogh, K.; Babisch, W.; Houthuijs, D.; Swart, W.; Pershagen, G.; Katsouyanni, K.; Velonakis, M.; et al. Exposure to aircraft and road traffic noise and associations with heart disease and stroke in six European countries: A cross-sectional study. Environ. Health 2013, 12, 89. [Google Scholar] [CrossRef] [PubMed]
- Harding, A.-H.; Frost, G.A.; Tan, E.; Tsuchiya, A.; Mason, H.M. The cost of hypertension-related ill-health attributable to environmental noise. Noise Health 2013, 15, 437–445. [Google Scholar] [CrossRef] [PubMed]
- Swinburn, T.K.; Hammer, M.S.; Neitzel, R.L. Valuing Quiet: An Economic Assessment of U.S. Environmental Noise as a Cardiovascular Health Hazard. Am. J. Prev. Med. 2015, 49, 345–353. [Google Scholar] [CrossRef] [PubMed]
- Wolfe, P.J.; Malina, R.; Barrett, S.R.H.; Waitz, I.A. Costs and benefits of US aviation noise land-use policies. Transp. Res. Part D Transp. Environ. 2016, 44, 147–156. [Google Scholar] [CrossRef]
- Queens Quiet Skies. Noise Compatibility Program Solutions. Available online: http://queensquietskies.org/wp-content/uploads/2016/12/TAC-Noise-Compatibility-Solutions-QQS-Dec-2016.pdf (accessed on 10 July 2017).
- Arias, E. United States Life Tables. 2007. Available online: http://www.cdc.gov (accessed on 2 August 2018).
- Mozaffarian, D.; Benjamin, E.J.; Go, A.S.; Arnett, D.K.; Blaha, M.J.; Cushman, M.; Das, S.R.; de Ferranti, S.; Després, J.P.; Fullerton, H.J.; et al. Heart Disease and Stroke Statistics—2016 Update. Circulation. Available online: http://circ.ahajournals.org/content/early/2015/12/16/CIR.0000000000000350 (accessed on 5 April 2017).
- Nichols, G.A.; Bell, T.J.; Pedula, K.L.; O’Keeffe-Rosetti, M. Medical care costs among patients with established cardiovascular disease. Am. J. Manag. Care 2010, 16, e86–e93. [Google Scholar] [PubMed]
- Kessler, R.C.; Chiu, W.T.; Demler, O.; Walters, E.E. Prevalence, severity, and comorbidity of twelve-month DSM-IV disorders in the national comorbidity survey replication (NCS-R). Arch. Gen. Psychiatry 2005, 62, 617–627. [Google Scholar] [CrossRef] [PubMed]
- Fan, A.Z.; Strine, T.W.; Jiles, R.; Mokdad, A.H. Depression and anxiety associated with cardiovascular disease among persons aged 45 years and older in 38 states of the United States, 2006. Prev. Med. 2008, 46, 445–450. [Google Scholar] [CrossRef] [PubMed]
- Greenberg, P.E.; Sisitsky, T.; Kessler, R.C.; Finkelstein, S.N.; Berndt, E.R.; Davidson, J.R.; Fyer, A.J. The economic burden of anxiety disorders in the 1990s. J. Clin. Psychiatry 1999, 60, 427–435. [Google Scholar] [CrossRef] [PubMed]
- Members, W.G.; Lloyd-Jones, D.; Adams, R.J.; Brown, T.M.; Carnethon, M.; Dai, S.; De Simone, G.; Ferguson, T.B.; Ford, E.; Furie, K.; et al. Heart Disease and Stroke Statistics—2010 Update. Circulation 2010, 121, e46–e215. [Google Scholar] [CrossRef] [PubMed]
- Ara, R.; Brazier, J. Health Related Quality of Life by Age, Gender and History of Cardiovascular Disease: Results from the Health Survey for England. Health Economics and Decision Science Discussion Paper 09/12. 2009. Available online: http://eprints.whiterose.ac.uk/10880/1/HEDS_DP_09-12.pdf (accessed on 30 March 2017).
- Ara, R.; Brazier, J.E. Populating an economic model with health state utility values: Moving toward better practice. Value Health 2010, 13, 509–518. [Google Scholar] [CrossRef] [PubMed]
- Calculating the U.S. Population-Based EQ-5D Index Score|AHRQ Archive. Available online: https://archive.ahrq.gov/professionals/clinicians-providers/resources/rice/EQ5Dscore.html (accessed on 7 March 2017).
- US Inflation Calculator. US Inflation Calculator. Available online: http://www.usinflationcalculator.com/ (accessed on 16 October 2014).
- Bureau of Transportation Statistics, Form 41, Schedule T2. Available online: https://www.transtats.bts.gov/Tables.asp?DB_ID=130 (accessed on 5 June 2017).
- The Port Authority of New York and New Jersey Air Traffic Report 2016. Available online: http://www.panynj.gov/airports/pdf-traffic/ATR2016.pdf (accessed on 1 Jun 2017).
- Global Gateway Alliance Environmental Impact Statement on “TNNIS Climb” Would Fly in Wrong Direction for New York Area Airports. Available online: https://www.scribd.com/document/184257668/ENVIRONMENTAL-IMPACT-STATEMENT-ON-TENNIS-CLIMB-WOULD-FLY-IN-WRONG-DIRECTION-FOR-NEW-YORK-AREA-AIRPORTS-docx (accessed on 2 June 2017).
- Lin, P.-H.; Sun, W.-S.; Chen, J.-P. Inventory of Aircraft Emissions over the Taiwan Area. Terr. Atmos. Ocean. Sci. 2001, 12, 22. [Google Scholar] [CrossRef]
- Wyman, O. Airline Economic Analysis 2015–2016. Available online: http://www.oliverwyman.com/our-expertise/insights/2016/jan/airline-economic-analysis-2016.html (accessed on 2 June 2017).
- US DOT form 41 from the Bureau of Transportation Statistics, Schedule T2. Available online: http://web.mit.edu/airlinedata/www/2016%2012%20Month%20Documents/Aircraft%20and%20Related/Total%20Fleet/Average%20Seat%20Capacity%20of%20Total%20Operating%20Fleet.htm (accessed on 5 Jun 2017).
- Bureau, U.C. Income Distribution to $250,000 or More for Households: 2016. Available online: https://www.census.gov/data/tables/time-series/demo/income-poverty/cps-hinc/hinc-06.html (accessed on 29 June 2018).
- Flushing Demographics & Statistics. Available online: https://www.point2homes.com/US/Neighborhood/NY/Queens/Flushing-Demographics.html#Population (accessed on 5 June 2017).
- Heidenreich, P.A.; Trogdon, J.G.; Khavjou, O.A.; Butler, J.; Dracup, K.; Ezekowitz, M.D.; Lloyd-Jones, D.M.; Nelson, S.A.; Wilson, P.W.; JosephWoo, Y.; et al. Forecasting the future of cardiovascular disease in the United States: A policy statement from the American Heart Association. Circulation 2011, 123, 933–944. [Google Scholar] [CrossRef] [PubMed]
- Brenes, G.A. Anxiety, Depression, and Quality of Life in Primary Care Patients. Prim. Care Companion J. Clin. Psychiatry 2007, 9, 437–443. [Google Scholar] [CrossRef] [PubMed]
- Ara, R.; Brazier, J. Deriving an algorithm to convert the eight mean SF-36 dimension scores into a mean EQ-5D preference-based score from published studies (where patient level data are not available). Value Health 2008, 11, 1131–1143. [Google Scholar] [CrossRef] [PubMed]
- Neumann, P.J.; Cohen, J.T.; Weinstein, M.C. Updating Cost-Effectiveness—The Curious Resilience of the $50,000-per-QALY Threshold. N. Engl. J. Med. 2014, 371, 796–797. [Google Scholar] [CrossRef] [PubMed]
- TreeAge Software Inc., Williamstown, MA, USA. Available online: https://www.treeage.com/ (accessed on 26 February 2017).
- Sanders, G.D.; Neumann, P.J.; Basu, A.; Brock, D.W.; Feeny, D.; Krahn, M.; Kuntz, K.M.; Meltzer, D.O.; Owens, D.K.; Prosser, L.A.; et al. Recommendations for Conduct, Methodological Practices, and Reporting of Cost-effectiveness Analyses: Second Panel on Cost-Effectiveness in Health and Medicine. JAMA 2016, 316, 1093–1103. [Google Scholar] [CrossRef] [PubMed]
- Muennig, P.; Woolf, S.H. Health and economic benefits of reducing the number of students per classroom in US primary schools. Am. J. Public Health 2007, 97, 2020–2027. [Google Scholar] [CrossRef] [PubMed]
- Jiao, B.; Zafari, Z.; Will, B.; Ruggeri, K.; Li, S.; Muennig, P. The Cost-Effectiveness of Lowering Permissible Noise Levels Around U.S. Airports. Int. J. Environ. Res. Public Health 2017, 14, 1497. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5750915/ (accessed on 12 March 2018). [CrossRef] [PubMed]
- 2010 New York City Population by Census Tracts. Available online: https://data.cityofnewyork.us/City-Government/2010-NYC-Population-by-Census-Tracts/si4q-zuzm (accessed on 1 March 2018).
| Parameters | Mean (Standard Error/Range) | Distribution | References |
|---|---|---|---|
| Probabilities | |||
| Population of Queens affected by TNNIS noise | 83,807 | - | [16,30] |
| Background mortality rates | U.S. Life Tables | [31] | |
| Risk of developing a CVD event (by age) | [32] | ||
| 35–44 | 0.0015 (0.0004) | Beta | |
| 45–54 | 0.0071 (0.0018) | Beta | |
| 55–64 | 0.0149 (0.0037) | Beta | |
| 65–74 | 0.0266 (0.0067) | Beta | |
| 75–84 | 0.0478 (0.0120) | Beta | |
| 85+ | 0.0681 (0.0170) | Beta | |
| Relative risk of CVD among those with prior history of CVD | 1.965 (1.67–2.30) | Log-normal | [33] |
| Risk of an anxiety disorder | 0.18 (0.0070) | Beta | [34] |
| Relative risk of anxiety for CVD patients | 1.66 (1.49–1.82) | Log-normal | [35] |
| Relative risk of CVD for aircraft noise exposure | 1.14 (1.08–1.20) | Log-normal | [14] |
| Relative risk of anxiety for aircraft noise exposure | 1.79 (1.00–3.06) | Log-normal | [15] |
| Costs | |||
| Direct medical costs of CVD | 23,229 (5807) | Gamma | [33] |
| Direct medical costs of anxiety | 2814 (704) | Gamma | [36] |
| Indirect medical costs of CVD | 12,837 (3209) | Gamma | [33,37] |
| Indirect medical costs of anxiety | 313 (78) | Gamma | [36] |
| Total incremental operating costs (limited vs. year-round use of TNNIS) | 127,040,655 (31,760,164) | Author estimation | |
| Incremental operating costs per person exposed to noise (limited vs. year-round use of TNNIS) (Total divided by 83,807) | 1516 (379) | Gamma | |
| Total incremental productivity loss (limited vs. year-round use of TNNIS) | $19,956,042 ($4,989,010) | Author estimation | |
| Incremental productivity loss per person exposed to noise (limited vs. year-round use of TNNIS) (Total divided by 83,807) | 238 (59) | Gamma | |
| Utilities | |||
| Disutility associated with a CVD event | 0.283 (0.0130) | Beta | [38,39] |
| Disutility associated with anxiety | 0.16 (0.04 *) | Beta | [40] |
| Utility of prior history of CVD event health state | 0.844 (0.0096) | Beta | [38,39] |
| Scenario | Costs | Incremental Costs | QALYs | Incremental QALYs | ICER ($/QALY) |
|---|---|---|---|---|---|
| Limited use of TNNIS | 656,173 | 11,288 | 18.72 | 1.13 | 10,006 |
| Year-round use of TNNIS | 644,885 | 17.6 | Reference |
| Input Parameters | Low | High |
|---|---|---|
| RR of anxiety for aircraft noise exposure (1.00–3.06) | −3574 | 208,108 |
| Probability of anxiety for people without CVD (0.08 to 0.28) | 1694 | 33,826 |
| Incremental operating costs per person exposed to noise (limited vs. year-round use of TNNIS) (1137 to 1895) | 2345 | 17,668 |
| Health utility decrement for anxiety (−0.26 to −0.06) | 6508 | 21,641 |
| RR of CVD for aircraft noise exposure (1.0–1.18) | 5065 | 15,876 |
| Direct costs of anxiety (2111 to 3518) | 6947 | 13,062 |
| Direct costs of CVD (17,422 to 29,036) | 7041 | 12,972 |
| RR of anxiety for CVD patients (1.49–1.82) | 8303 | 12,109 |
| Prevalence of CVD in general population (0.25 to 0.45) | 8431 | 11,566 |
| Age at baseline (31 to 51) | 8625 | 11,655 |
| Incremental productivity loss per person exposed to noise (limited vs. year-round use of TNNIS) (178.5, 297.5) | 8804 | 11,209 |
| Indirect costs of CVD (9628 to 16,046) | 8951 | 11,062 |
| Health utility decrement for CVD (−0.38 to −0.18) | 9374 | 10,771 |
| Health utility of people with a prior history of CVD (0.74 to 0.94) | 9669 | 10,401 |
| Indirect costs of anxiety (235 to 391) | 9668 | 10,346 |
| RR of CVD for people with a prior history of CVD (1.7 to 2.3) | 9764 | 10,238 |
| Discount rate (0.00 to 0.05) | 9978 | 10,365 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zafari, Z.; Jiao, B.; Will, B.; Li, S.; Muennig, P.A. The Trade-Off between Optimizing Flight Patterns and Human Health: A Case Study of Aircraft Noise in Queens, NY, USA. Int. J. Environ. Res. Public Health 2018, 15, 1753. https://doi.org/10.3390/ijerph15081753
Zafari Z, Jiao B, Will B, Li S, Muennig PA. The Trade-Off between Optimizing Flight Patterns and Human Health: A Case Study of Aircraft Noise in Queens, NY, USA. International Journal of Environmental Research and Public Health. 2018; 15(8):1753. https://doi.org/10.3390/ijerph15081753
Chicago/Turabian StyleZafari, Zafar, Boshen Jiao, Brian Will, Shukai Li, and Peter Alexander Muennig. 2018. "The Trade-Off between Optimizing Flight Patterns and Human Health: A Case Study of Aircraft Noise in Queens, NY, USA" International Journal of Environmental Research and Public Health 15, no. 8: 1753. https://doi.org/10.3390/ijerph15081753
APA StyleZafari, Z., Jiao, B., Will, B., Li, S., & Muennig, P. A. (2018). The Trade-Off between Optimizing Flight Patterns and Human Health: A Case Study of Aircraft Noise in Queens, NY, USA. International Journal of Environmental Research and Public Health, 15(8), 1753. https://doi.org/10.3390/ijerph15081753





