Independent and Joint Contributions of Fine Particulate Matter Exposure and Population Vulnerability to Mortality in the Detroit Metropolitan Area
Abstract
1. Introduction
2. Materials and Methods
2.1. Data
2.2. Measures
2.3. Analysis
3. Results
4. Discussion
4.1. Limitations
4.2. Strengths
5. Conclusions
Supplementary Materials
Author Contributions
Acknowledgments
Conflicts of Interest
References
- Brook, R.D.; Rajagopalan, S.; Pope, C.A.; Brook, J.R.; Bhatnagar, A.; Diez-Roux, A.V.; Holguin, F.; Hong, Y.; Luepker, R.V.; Mittleman, M.A.; et al. On behalf of the American Heart Association Council on Epidemiology and Prevention, Council on the Kidney in Cardiovascular Disease, and Council on Nutrition, Physical Activity and Metabolism Particulate Matter Air Pollution and Cardiovascular Disease: An Update to the Scientific Statement From the American Heart Association. Circulation 2010, 121, 2331–2378. [Google Scholar] [CrossRef] [PubMed]
- Jerrett, M.; Burnett, R.T.; Beckerman, B.S.; Turner, M.C.; Krewski, D.; Thurston, G.; Martin, R.V.; van Donkelaar, A.; Hughes, E.; Shi, Y.; et al. Spatial Analysis of Air Pollution and Mortality in California. Am. J. Respir. Crit. Care Med. 2013, 188, 593–599. [Google Scholar] [CrossRef] [PubMed]
- Ostro, B.; Hu, J.; Goldberg, D.; Reynolds, P.; Hertz, A.; Bernstein, L.; Kleeman, M.J. Associations of mortality with long-term exposures to fine and ultrafine particles, species and sources: Results from the California Teachers Study Cohort. Environ. Health Perspect. 2015, 123, 549–556. [Google Scholar] [CrossRef] [PubMed]
- Neupane, B.; Jerrett, M.; Burnett, R.T.; Marrie, T.; Arain, A.; Loeb, M. Long-term exposure to ambient air pollution and risk of hospitalization with community-acquired pneumonia in older adults. Am. J. Respir. Crit. Care Med. 2010, 181, 47–53. [Google Scholar] [CrossRef] [PubMed]
- Fan, J.; Li, S.; Fan, C.; Bai, Z.; Yang, K. The impact of PM2.5 on asthma emergency department visits: A systematic review and meta-analysis. Environ. Sci. Pollut. Res. Int. 2016, 23, 843–850. [Google Scholar] [CrossRef] [PubMed]
- Li, S.; Batterman, S.; Wasilevich, E.; Wahl, R.; Wirth, J.; Su, F.-C.; Mukherjee, B. Association of daily asthma emergency department visits and hospital admissions with ambient air pollutants among the pediatric Medicaid population in Detroit: Time-series and time-stratified case-crossover analyses with threshold effects. Environ. Res. 2011, 111, 1137–1147. [Google Scholar] [CrossRef] [PubMed]
- Strickland, M.J.; Darrow, L.A.; Klein, M.; Flanders, W.D.; Sarnat, J.A.; Waller, L.A.; Sarnat, S.E.; Mulholland, J.A.; Tolbert, P.E. Short-term associations between ambient air pollutants and pediatric asthma emergency department visits. Am. J. Respir. Crit. Care Med. 2010, 182, 307–316. [Google Scholar] [CrossRef] [PubMed]
- Johannson, K.A.; Vittinghoff, E.; Lee, K.; Balmes, J.R.; Ji, W.; Kaplan, G.G.; Kim, D.S.; Collard, H.R. Acute exacerbation of idiopathic pulmonary fibrosis associated with air pollution exposure. Eur. Respir. J. 2014, 43, 1124–1131. [Google Scholar] [CrossRef] [PubMed]
- Stern, G.; Latzin, P.; Röösli, M.; Fuchs, O.; Proietti, E.; Kuehni, C.; Frey, U. A prospective study of the impact of air pollution on respiratory symptoms and infections in infants. Am. J. Respir. Crit. Care Med. 2013, 187, 1341–1348. [Google Scholar] [CrossRef] [PubMed]
- Gehring, U.; Gruzieva, O.; Agius, R.M.; Beelen, R.; Custovic, A.; Cyrys, J.; Eeftens, M.; Flexeder, C.; Fuertes, E.; Heinrich, J.; et al. Air pollution exposure and lung function in children: The ESCAPE project. Environ. Health Perspect. 2013, 121, 1357–1364. [Google Scholar] [CrossRef] [PubMed]
- Rice, M.B.; Ljungman, P.L.; Wilker, E.H.; Gold, D.R.; Schwartz, J.D.; Koutrakis, P.; Washko, G.R.; O’Connor, G.T.; Mittleman, M.A. Short-term exposure to air pollution and lung function in the Framingham Heart Study. Am. J. Respir. Crit. Care Med. 2013, 188, 1351–1357. [Google Scholar] [CrossRef] [PubMed]
- Urman, R.; McConnell, R.; Islam, T.; Avol, E.L.; Lurmann, F.W.; Vora, H.; Linn, W.S.; Rappaport, E.B.; Gilliland, F.D.; Gauderman, W.J. Associations of children’s lung function with ambient air pollution: Joint effects of regional and near-roadway pollutants. Thorax 2014, 69, 540–547. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, M.; Giorgis-Allemand, L.; Bernard, C.; Aguilera, I.; Andersen, A.-M.N.; Ballester, F.; Beelen, R.M.J.; Chatzi, L.; Cirach, M.; Danileviciute, A.; et al. Ambient air pollution and low birthweight: A European cohort study (ESCAPE). Lancet Respir. Med. 2013, 1, 695–704. [Google Scholar] [CrossRef]
- Shah, P.S.; Balkhair, T. Knowledge Synthesis Group on Determinants of Preterm/LBW births Air pollution and birth outcomes: A systematic review. Environ. Int. 2011, 37, 498–516. [Google Scholar] [CrossRef] [PubMed]
- Stieb, D.M.; Chen, L.; Eshoul, M.; Judek, S. Ambient air pollution, birth weight and preterm birth: A systematic review and meta-analysis. Environ. Res. 2012, 117, 100–111. [Google Scholar] [CrossRef] [PubMed]
- Fann, N.; Lamson, A.D.; Anenberg, S.C.; Wesson, K.; Risley, D.; Hubbell, B.J. Estimating the national public health burden associated with exposure to ambient PM2.5 and ozone. Risk Anal. 2012, 32, 81–95. [Google Scholar] [CrossRef] [PubMed]
- Nam, K.-M.; Selin, N.E.; Reilly, J.M.; Paltsev, S. Measuring welfare loss caused by air pollution in Europe: A CGE analysis. Energy Policy 2010, 38, 5059–5071. [Google Scholar] [CrossRef]
- U.S. Environmental Protection Agency (EPA). Health Assessment Document for Diesel Engine Exhaust; National Center for Environmental Assessment: Washington, DC, USA, 2002.
- Shi, L.; Zanobetti, A.; Kloog, I.; Coull, B.A.; Koutrakis, P.; Melly, S.J.; Schwartz, J.D. Low-Concentration PM2.5 and Mortality: Estimating Acute and Chronic Effects in a Population-Based Study. Environ. Health Perspect. 2016, 124, 46–52. [Google Scholar] [CrossRef] [PubMed]
- Lepeule, J.; Laden, F.; Dockery, D.; Schwartz, J. Chronic exposure to fine particles and mortality: An extended follow-up of the Harvard Six Cities study from 1974 to 2009. Environ. Health Perspect. 2012, 120, 965–970. [Google Scholar] [CrossRef] [PubMed]
- Mohai, P.; Lantz, P.M.; Morenoff, J.; House, J.S.; Mero, R.P. Racial and socioeconomic disparities in residential proximity to polluting industrial facilities: Evidence from the Americans’ Changing Lives Study. Am. J. Public Health 2009, 99 (Suppl. 3), S649–S656. [Google Scholar] [CrossRef] [PubMed]
- Schulz, A.J.; Mentz, G.; Sampson, N.; Ward, M.; Anderson, R.; de Majo, R.; Israel, B.A.; Lewis, T.C.; Wilkins, D. Race and the distribution of social and physical environmental risk: A case example from the Detroit metropolitan area. Du Bois Rev. Soc. Sci. Res. Race 2016, 13, 285–304. [Google Scholar] [CrossRef] [PubMed]
- Jones, M.R.; Diez-Roux, A.V.; Hajat, A.; Kershaw, K.N.; O’Neill, M.S.; Guallar, E.; Post, W.S.; Kaufman, J.D.; Navas-Acien, A. Race/ethnicity, residential segregation, and exposure to ambient air pollution: The Multi-Ethnic Study of Atherosclerosis (MESA). Am. J. Public Health 2014, 104, 2130–2137. [Google Scholar] [CrossRef] [PubMed]
- Gray, S.C.; Edwards, S.E.; Miranda, M.L. Race, socioeconomic status, and air pollution exposure in North Carolina. Environ. Res. 2013, 126, 152–158. [Google Scholar] [CrossRef] [PubMed]
- Williams, D.R.; Jackson, P.B. Social sources of racial disparities in health. Health Aff. 2005, 24, 325–334. [Google Scholar] [CrossRef] [PubMed]
- Darling-Hammond, L. The Color Line in American Education: Race, Resources, and Student Achievement. Du Bois Rev. Soc. Sci. Res. Race 2004, 1, 213–246. [Google Scholar] [CrossRef]
- Clark, N.M.; Quinn, M.; Dodge, J.A.; Nelson, B.W. Alliance system and policy change: Necessary ingredients for improvement in diabetes care and reduction of disparities. Health Promot. Pract. 2014, 15, 11S–22S. [Google Scholar] [CrossRef] [PubMed]
- Collins, T.W.; Grineski, S.E.; Chakraborty, J.; Montgomery, M.C.; Hernandez, M. Downscaling Environmental Justice Analysis: Determinants of Household-Level Hazardous Air Pollutant Exposure in Greater Houston. Ann. Assoc. Am. Geogr. 2015, 105, 684–703. [Google Scholar] [CrossRef]
- Huang, G.; London, J. Mapping cumulative environmental effects, social vulnerability, and health in the San Joaquin Valley, California. Am. J. Public Health 2012, 102, 830–832. [Google Scholar] [CrossRef] [PubMed]
- Sadd, J.L.; Pastor, M.; Morello-Frosch, R.; Scoggins, J.; Jesdale, B. Playing it safe: Assessing cumulative impact and social vulnerability through an environmental justice screening method in the South Coast Air Basin, California. Int. J. Environ. Res. Public Health 2011, 8, 1441–1459. [Google Scholar] [CrossRef] [PubMed]
- Adamkiewicz, G.; Spengler, J.D.; Harley, A.E.; Stoddard, A.; Yang, M.; Alvarez-Reeves, M.; Sorensen, G. Environmental conditions in low-income urban housing: Clustering and associations with self-reported health. Am. J. Public Health 2014, 104, 1650–1656. [Google Scholar] [CrossRef] [PubMed]
- Jacobs, D.E. Environmental Health Disparities in Housing. Available online: http://ajph.aphapublications.org/ (accessed on 22 August 2017).
- Forno, E.; Celedon, J.C. Asthma and ethnic minorities: Socioeconomic status and beyond. Curr. Opin. Allergy Clin. Immunol. 2009, 9, 154–160. [Google Scholar] [CrossRef] [PubMed]
- Bell, J.; Lee, M.M. Why Place and Race Matter: Impacting Health through a Focus on Race and Place; Report; Policy Link: Oakland, CA, USA, 2011; Available online: http://www.policylink.org/atf/cf/%7B97c6d565-bb43-406d-a6d5-eca3bbf35af0%7D/WPRM%20FULL%20REPORT (accessed on 4 June 2018).
- Kelishadi, R.; Poursafa, P. Air pollution and non-respiratory health hazards for children. Arch. Med. Sci. 2010, 6, 483–495. [Google Scholar] [CrossRef] [PubMed]
- Sacks, J.D.; Stanek, L.W.; Luben, T.J.; Johns, D.O.; Buckley, B.J.; Brown, J.S.; Ross, M. Particulate matter-induced health effects: Who is susceptible? Environ. Health Perspect. 2011, 119, 446–454. [Google Scholar] [CrossRef] [PubMed]
- Solomon, G.M.; Morello-Frosch, R.; Zeise, L.; Faust, J.B. Cumulative Environmental Impacts: Science and Policy to Protect Communities. Annu. Rev. Public Health 2016, 37, 83–96. [Google Scholar] [CrossRef] [PubMed]
- National Environmental Justice Advisory Council. Recommendations for Integrating Environmental Justice into the EPA’s Research Enterprise; National Environmental Justice Advisory Council: Washington, DC, USA, 2014.
- Fry, R.; Taylor, P. The Rise of Residential Segregation by Income; Pew Research Center’s Social & Demographic Trends Project: Washington, DC, USA, 2012. [Google Scholar]
- Sugrue, T.J. The Origins of the Urban Crisis: Race and Inequality in Postwar Detroit; Princeton University Press: Princeton, NJ, USA, 2014; ISBN 978-1-4008-5121-8. [Google Scholar]
- Farley, R.; Danziger, S.; Holzer, H.J. Detroit Divided; Russell Sage Foundation: New York, NY, USA, 2000; ISBN 978-1-61044-198-8. [Google Scholar]
- 2015 Data Release New and Notable. Available online: https://www.census.gov/programs-surveys/acs/news/data-releases/2015/release.html (accessed on 24 August 2017).
- Rodriguez, E.M.; Bowie, J.V.; Frattaroli, S.; Gielen, A. A qualitative exploration of the community partner experience in a faith-based breast cancer educational intervention. Health Educ. Res. 2009, 24, 760–771. [Google Scholar] [CrossRef] [PubMed]
- Jargowsky, P.A. Architecture of Segregation: Civil Unrest, the Concentration of Poverty, and Public Policy; The Century Foundation: New York, NY, USA, 2015; Volume 7. [Google Scholar]
- Kids Count Data Book; Annie E. Casey Foundation: Baltimore: MD, USA, 2015.
- Metropolitan Detroit Race Equity Report; New Detroit Coalition: Detroit, MI, USA, 2014.
- Rugh, J.S.; Massey, D.S. Racial Segregation and the American Foreclosure Crisis. Am. Sociol. Rev. 2010, 75, 629–651. [Google Scholar] [CrossRef] [PubMed]
- Morello-Frosch, R.; Jesdale, B.M. Separate and Unequal: Residential Segregation and Estimated Cancer Risks Associated with Ambient Air Toxics in U.S. Metropolitan Areas. Environ. Health Perspect. 2006, 114, 386–393. [Google Scholar] [CrossRef] [PubMed]
- Morello-Frosch, R.; Lopez, R. The riskscape and the color line: Examining the role of segregation in environmental health disparities. Environ. Res. 2006, 102, 181–196. [Google Scholar] [CrossRef] [PubMed]
- Chen, H.; Goldberg, M.S.; Burnett, R.T.; Jerrett, M.; Wheeler, A.J.; Villeneuve, P.J. Long-Term Exposure to Traffic-Related Air Pollution and Cardiovascular Mortality. Epidemiology 2013, 24, 35–43. [Google Scholar] [CrossRef] [PubMed]
- Morello-Frosch, R.; Zuk, M.; Jerrett, M.; Shamasunder, B.; Kyle, A.D. Understanding the cumulative impacts of inequalities in environmental health: Implications for policy. Health Aff. 2011, 30, 879–887. [Google Scholar] [CrossRef] [PubMed]
- Berrocal, V.J.; Gelfand, A.E.; Holland, D.M. Space-Time Data fusion Under Error in Computer Model Output: An Application to Modeling Air Quality. Biometrics 2012, 68, 837–848. [Google Scholar] [CrossRef] [PubMed]
- Berrocal, V.; Gelfand, A.E.; Holland, D. A spatiotemporal downscaler for output from numerical models. J. Agric. Biol. Environ. Stat. 2010, 15, 176–197. [Google Scholar] [CrossRef] [PubMed]
- Berrocal, V.; Gelfand, A.E.; Holland, D. A bivariate space-time downscaler under space and time misalignment. Ann. Appl. Stat. 2010, 4, 1942–1975. [Google Scholar] [CrossRef] [PubMed]
- U.S. Census Bureau American Community Survey (ACS). Available online: https://www.census.gov/programs-surveys/acs (accessed on 22 December 2016).
- WHO|International Classification of Diseases. Available online: http://www.who.int/classifications/icd/en/ (accessed on 22 August 2017).
- Bullard, R.D.; Mohai, P.; Saha, R.; Wright, B. Toxic Wastes and Race at Twenty 1987–2007: Grassroots Struggles to Dismantle Environmental Racism in the United States; United Church of Christ Justice and Witness Ministries: Washington, DC, USA, 2007. [Google Scholar]
- Lim, S.S.; Vos, T.; Flaxman, A.D.; Danaei, G.; Shibuya, K.; Adair-Rohani, H.; AlMazroa, M.A.; Amann, M.; Anderson, H.R.; Andrews, K.G.; et al. A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990–2010: A systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012, 380, 2224–2260. [Google Scholar] [CrossRef]
- Evans, J.; van Donkelaar, A.; Martin, R.V.; Burnett, R.; Rainham, D.G.; Birkett, N.J.; Krewski, D. Estimates of global mortality attributable to particulate air pollution using satellite imagery. Environ. Res. 2013, 120, 33–42. [Google Scholar] [CrossRef] [PubMed]
- Cohen, A.; Anderson, H.; Ostro, B.; Pandey, K.; Krzyzanowski, M.; Kunzli, N.; Gutschmidt, K.; Pope, A., III; Romieu, I.; Samet, J.; et al. Urban Air Pollution. In Comparative Quantification of Health Risks: Global and Regional Burden of Disease Attributable to Selected Major Risk Factors; Ezzati, M., Lopez, A., Rodgers, A., Murray, C., Eds.; World Health Organization: Geneva, Switzerland, 2004; Volume 2, pp. 1353–1434. [Google Scholar]
- Giannadaki, D.; Lelieveld, J.; Pozzer, A. Implementing the US air quality standard for PM2.5 worldwide can prevent millions of premature deaths per year. Environ. Health 2016, 15, 88. [Google Scholar] [CrossRef] [PubMed]
- Chi, G.C.; Hajat, A.; Bird, C.E.; Cullen, M.R.; Griffin, B.A.; Miller, K.A.; Shih, R.A.; Stefanick, M.L.; Vedal, S.; Whitsel, E.A.; et al. Individual and Neighborhood Socioeconomic Status and the Association between Air Pollution and Cardiovascular Disease. Environ. Health Perspect. 2016, 124, 1840–1847. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Shi, L.; Lee, M.; Liu, P.; Di, Q.; Zanobetti, A.; Schwartz, J.D. Long-term exposure to PM2.5 and mortality among older adults in the Southeastern US. Epidemiology 2017, 28, 207–214. [Google Scholar] [CrossRef] [PubMed]
- Parker, J.D.; Kravets, N.; Vaidyanathan, A. Particulate Matter Air Pollution Exposure and Heart Disease Mortality Risks by Race and Ethnicity in the United States. Circulation 2018, 137, 1688–1697. [Google Scholar] [CrossRef] [PubMed]
- Kioumourtzoglou, M.-A.; Schwartz, J.; James, P.; Dominici, F.; Zanobetti, A. PM2.5 and mortality in 207 US cities: Modification by temperature and city characteristics. Epidemiology 2016, 27, 221–227. [Google Scholar] [CrossRef] [PubMed]
- Fann, N.; Roman, H.A.; Fulcher, C.M.; Gentile, M.A.; Hubbell, B.J.; Wesson, K.; Levy, J.I. Maximizing Health Benefits and Minimizing Inequality: Incorporating Local-Scale Data in the Design and Evaluation of Air Quality Policies. Risk Anal. 2011, 31, 908–922. [Google Scholar] [CrossRef] [PubMed]
- Kheirbeck, K.I.; Haney, J.; Douglas, S.; Ito, K.; Caputo, S.; Matte, S. The Public Health Benefits of Reducing Fine Particulate Matter through Conversion to Cleaner Heating Fuels in New York City. Available online: https://www.ncbi.nlm.nih.gov/pubmed/25365783/ (accessed on 21 May 2018).
- Hoyer, M.; Foureman, G.; Valcovic, L. Health Assessment Document for Diesel Engine Exhaust—Google Scholar; United States Environmental Protection Agency: Washington, DC, USA, 2002.
- Escobedo, F.J.; Kroeger, T.; Wagner, J.E. Urban forests and pollution mitigation: Analyzing ecosystem services and disservices. Environ. Pollut. 2011, 159, 2078–2087. [Google Scholar] [CrossRef] [PubMed]
- Ellickson, K.M.; Sevcik, S.M.; Burman, S.; Pak, S.; Kohlasch, F.; Pratt, G.C. Cumulative Risk Assessment and Environmental Equity in Air Permitting: Interpretation, Methods, Community Participation and Implementation of a Unique Statute. Int. J. Environ. Res. Public Health 2011, 8, 4140–4159. [Google Scholar] [CrossRef] [PubMed]
- Phelan, J.; Link, B.; Tehranifar, P. Social conditions as fundamental causes of health inequalities: Theory, evidence, and policy implications. J. Health Soc. Behav. 2010, 51, S28–S40. [Google Scholar] [CrossRef] [PubMed]
- Williams, D.R.; Mohammed, S.A. Racism and Health I: Pathways and Scientific Evidence. Am. Behav. Sci. 2013, 57, 1152–1173. [Google Scholar] [CrossRef] [PubMed]
- Dvonch, J.T.; Kannan, S.S.; Schulz, A.J.; Keeler, G.J.; Mentz, G.; House, J.; Benjamin, A.; Max, P.; Bard, R.L.; Brook, R.D. Acute effects of ambient particulate matter on blood pressure: Differential effects across urban communities. Hypertension 2009, 53, 853–859. [Google Scholar] [CrossRef] [PubMed]
- Ensuring Risk Reduction in Communities with Multiple Stressors: Environmental Justice and Cumulative Risks; National Environmental Justice Advisory Council: Washington, DC, USA, 2004.
- Environmental Justice 2020 Action Agenda: The U.S. EPA’s Environmental Justice Strategic Plan for 2016–2020; United States Environmental Protection Agency: Washington, DC, USA, 2016.
| Individual Level (n = 171,000) | Percent | Mean (SD) | Range |
|---|---|---|---|
| Demographics | |||
| Age | 72.6 (18.7) | (0.0, 99.2) | |
| Gender (Female = 1) | 51.2 | ||
| Race/ethnicity | |||
| Hispanic | 1.4 | ||
| Non-Hispanic White | 71.9 | ||
| Non-Hispanic Black | 25.6 | ||
| Non-Hispanic Other | 1.1 | ||
| Education Attainment | |||
| Less than high school | 17.3 | ||
| High school | 29.1 | ||
| More than high school | 17.2 | ||
| Not reported | 36.4 | ||
| Married | 33.6 | ||
| Smoking behavior | |||
| Yes | 7.4 | ||
| No | 36.1 | ||
| Probable | 5.7 | ||
| Not reported | 50.8 | ||
| Mortality rates | |||
| Ischemic heart | 19.3 | ||
| Cardiovascular | 34.3 | ||
| Cardiopulmonary | 42.7 | ||
| Tract Level (n = 1166) | |||
| Pollution Exposure | |||
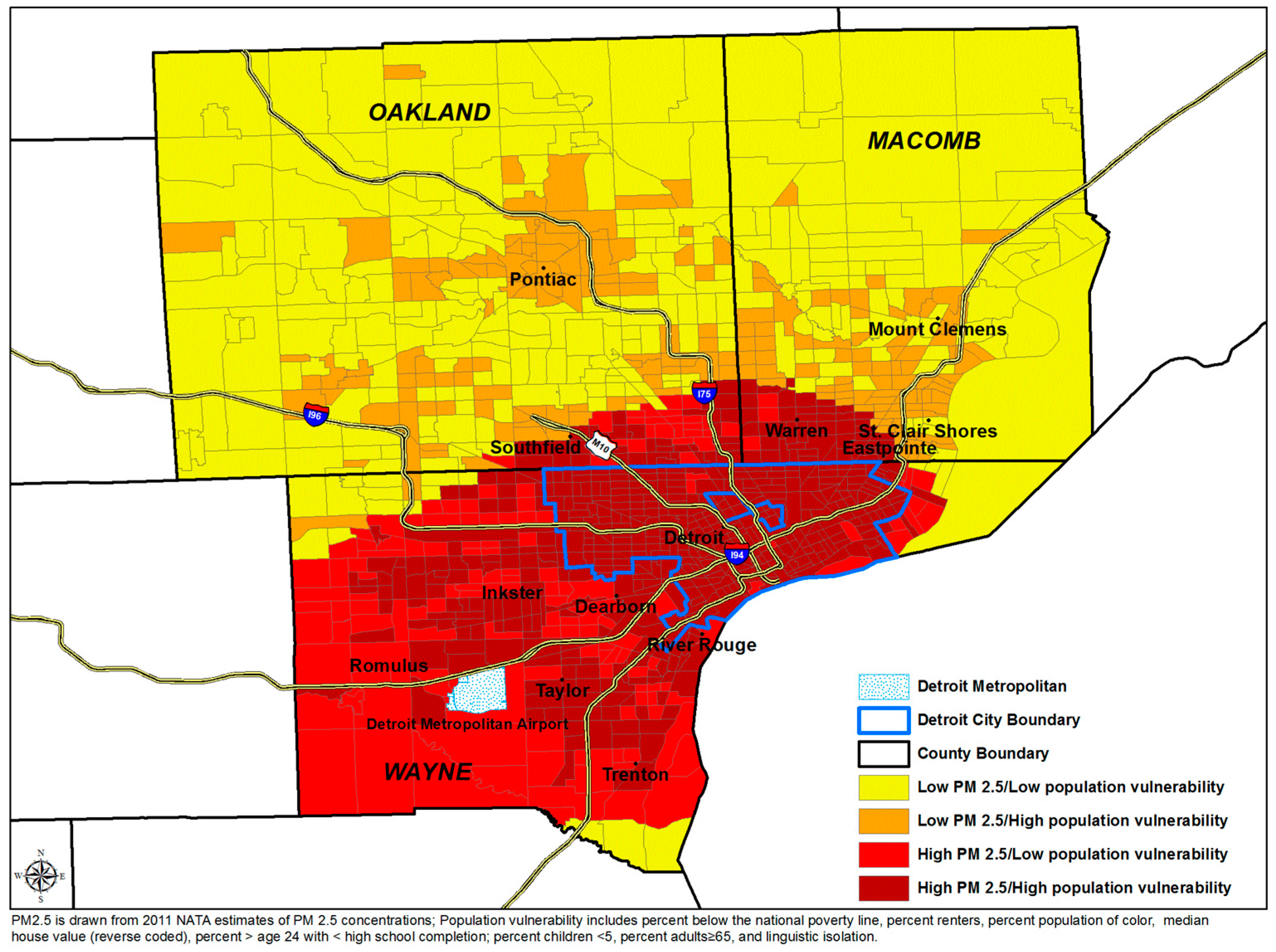
| PM2.5 (µg/m3) | 9.6 (0.3) | (8.9, 10.0) | |
| Vulnerability (mean percent at the tract level) | |||
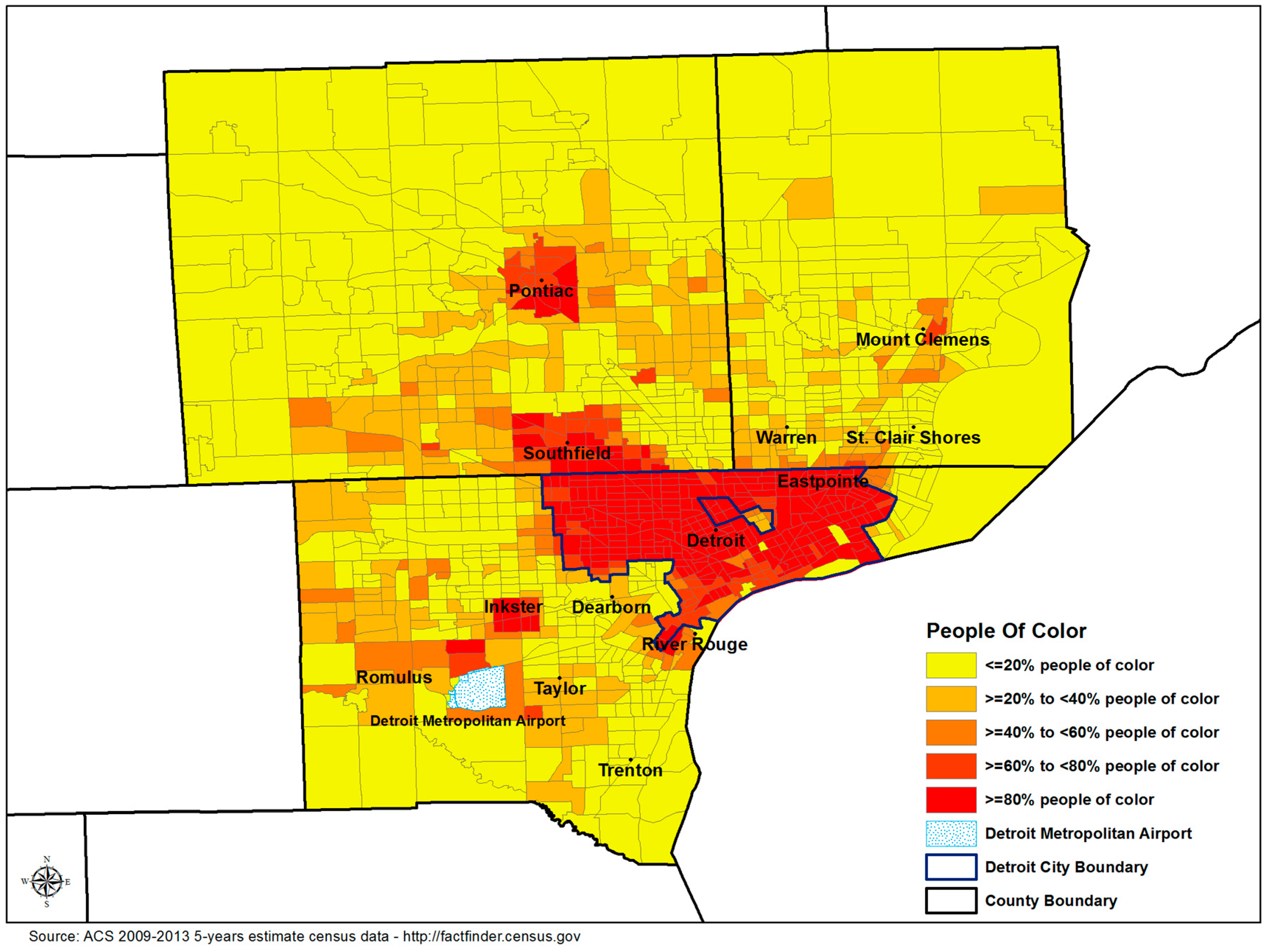
| Percent people of color | 40.3 (35.4) | (0.0, 100) | |
| Percent households living below poverty line | 19.9 (16.9) | (0.0, 100) | |
| Median home value (in thousands) | 121.5 (87.1) | (10.0, 761.3) | |
| Percent renter-occupied housing | 30.9 (20.9) | (0.0, 100) | |
| Percent aged ≥24 with <high school diploma | 13.7 (10.2) | (0.0, 61.7) | |
| Percent linguistically isolated | 0.4 (1.1) | (0.0, 9.7) | |
| Percent aged <5 | 5.8 (2.7) | (0.0, 17.8) | |
| Percent aged ≥60 | 19.9 (6.8) | (0.0, 57.5) |
| Tract Level Predictors | Ischemic Health Disease | Cardiovascular | Cardiopulmonary | |||
|---|---|---|---|---|---|---|
| Model 1 | Model 2 | Model 1 | Model 2 | Model 1 | Model 2 | |
| PM2.5 (1 = low) | OR 2 (95% CI) | OR (95% CI) | OR (95% CI) | OR (95% CI) | OR (95% CI) | OR (95% CI) |
| 2 | 1.06 (0.95, 1.19) | 1.00 (0.92, 1.08) | 0.98 (0.90, 1.07) | |||
| 3 | 1.17 (1.05, 1.31) b | 1.03 (0.95, 1.12) | 1.08 (0.99, 1.18) † | |||
| 4 | 1.19 (1.06, 1.34) b | 1.08 (0.99, 1.18) | 1.18 (1.08, 1.29) c | |||
| 5 | 1.31 (1.16, 1.48) c | 1.14 (1.03, 1.26) b | 1.22 (1.11, 1.34) c | |||
| Vulnerability (1 = low) | ||||||
| 2 | 1.06 (0.94,1.19) | 1.10 (1.01, 1.19) a | 1.09 (1.00, 1.19) | |||
| 3 | 1.12 (1.00,1.26) a | 1.16 (1.07, 1.26) c | 1.19 (1.09, 1.29) c | |||
| 4 | 1.17 (1.04,1.31) b | 1.17 (1.07, 1.27) c | 1.22 (1.12, 1.33) c | |||
| 5 | 1.24 (1.09,1.42) c | 1.16 (1.05, 1.29) b | 1.23 (1.11, 1.35) c | |||
| Quintile | Ischemic Heart | ||
|---|---|---|---|
| Disease | Cardiovascular | Cardiopulmonary | |
| OR (95% CI) | OR (95% CI) | OR (95% CI) | |
| PM2.5 (1 = low, 5 = high) | |||
| 1 | ref | ref | ref |
| 2 | 1.04 (0.92, 1.17) | 0.95 (0.87, 1.04) | 0.94 (0.86, 1.03) |
| 3 | 1.15 (1.02, 1.29) a | 0.99 (0.91, 1.08) | 1.03 (0.94, 1.13) |
| 4 | 1.15 (1.02, 1.31) a | 1.02 (0.93, 1.13) | 1.11 (1.01, 1.23) a |
| 5 | 1.24 (1.08, 1.42) c | 1.10 (0.98, 1.22) | 1.15 (1.04, 1.28) b |
| Vulnerability (1 = low, 5 = high) | |||
| 1 | ref | ref | ref |
| 2 | 1.03 (0.91, 1.16) | 1.10 (1.00, 1.20) a | 1.08 (0.98, 1.18) |
| 3 | 1.07 (0.95, 1.21) | 1.16 (1.06, 1.27) c | 1.17 (1.07, 1.28) c |
| 4 | 1.09 (0.96, 1.24) | 1.15 (1.05, 1.26) c | 1.19 (1.08, 1.30) c |
| 5 | 1.13 (0.98, 1.31) | 1.11 (0.99, 1.24) † | 1.15 (1.03, 1.28) b |
| Percent Attributable Risk | Low Vulnerability | High Vulnerability | ||
|---|---|---|---|---|
| Low PM2.5 | High PM2.5 | Low PM2.5 | High PM2.5 | |
| Population estimates | 1,301,007 (30.3%) | 657,199 (15.3%) | 677,435 (15.8%) | 1,659,342 (38.6%) |
| Cardiopulmonary Mortality Estimates (Total) | 1000 (20.8%) | 633 (13.2%) | 767 (16.0%) | 2400 (50.0%) |
| Attributable to PM2.5 (3%) | 30 (20.8%) | 19 (13.2%) | 23 (16.0%) | 72 (50%) |
| Attributable to PM2.5 (5%) | 50 (20.7%) | 32 (13.3%) | 39 (16.2%) | 120 (49.8%) |
| Attributable to PM2.5 (10%) | 100 (20.8%) | 64 (13.3%) | 77 (16.0%) | 239 (49.8%) |
| Attributable to PM2.5 (15%) | 150 (20.8%) | 96 (13.3%) | 116 (16.1%) | 359 (49.8%) |
| Cardiopulmonary deaths averted | ||||
| If PM2.5 moves from High to Low (3%) | 4 (21.1%) | 15 (78.9%) | ||
| If PM2.5 moves from High to Low (5%) | 7 (21.9%) | 25 (78.1%) | ||
| If PM2.5 moves from High to Low (10%) | 13 (20.6%) | 50 (79.4%) | ||
| If PM2.5 moves from High to Low (15%) | 20 (21.1%) | 75 (78.9%) | ||
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Schulz, A.J.; Mentz, G.B.; Sampson, N.; Ward, M.; Dvonch, J.T.; De Majo, R.; Israel, B.A.; Reyes, A.G.; Wilkins, D. Independent and Joint Contributions of Fine Particulate Matter Exposure and Population Vulnerability to Mortality in the Detroit Metropolitan Area. Int. J. Environ. Res. Public Health 2018, 15, 1209. https://doi.org/10.3390/ijerph15061209
Schulz AJ, Mentz GB, Sampson N, Ward M, Dvonch JT, De Majo R, Israel BA, Reyes AG, Wilkins D. Independent and Joint Contributions of Fine Particulate Matter Exposure and Population Vulnerability to Mortality in the Detroit Metropolitan Area. International Journal of Environmental Research and Public Health. 2018; 15(6):1209. https://doi.org/10.3390/ijerph15061209
Chicago/Turabian StyleSchulz, Amy J., Graciela B. Mentz, Natalie Sampson, Melanie Ward, J. Timothy Dvonch, Ricardo De Majo, Barbara A. Israel, Angela G. Reyes, and Donele Wilkins. 2018. "Independent and Joint Contributions of Fine Particulate Matter Exposure and Population Vulnerability to Mortality in the Detroit Metropolitan Area" International Journal of Environmental Research and Public Health 15, no. 6: 1209. https://doi.org/10.3390/ijerph15061209
APA StyleSchulz, A. J., Mentz, G. B., Sampson, N., Ward, M., Dvonch, J. T., De Majo, R., Israel, B. A., Reyes, A. G., & Wilkins, D. (2018). Independent and Joint Contributions of Fine Particulate Matter Exposure and Population Vulnerability to Mortality in the Detroit Metropolitan Area. International Journal of Environmental Research and Public Health, 15(6), 1209. https://doi.org/10.3390/ijerph15061209






