Changes in Sitting Time and Sitting Fragmentation after a Workplace Sedentary Behaviour Intervention
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
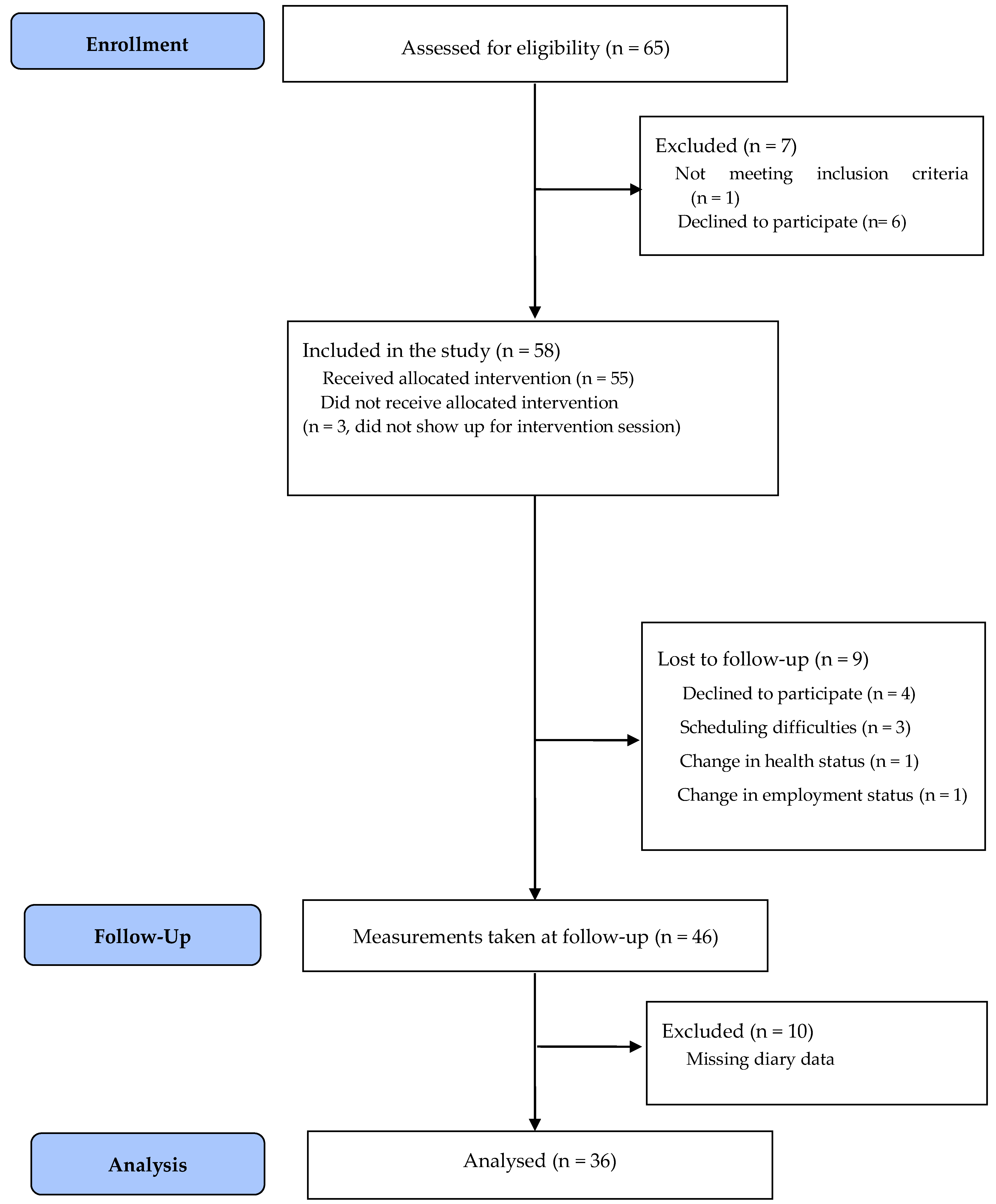
2.2. Participants
2.3. Procedures
2.4. Intervention
2.5. Outcome Measures and Statistical Analysis
3. Results
3.1. Whole Day Sedentary Behaviour
3.2. Working Day Sedentary Behaviour
4. Discussion
5. Conclusions
Author Contributions
Acknowledgments
Conflicts of Interest
References
- Sedentary Behaviour Research Network. Letter to the editor: Standardized use of the terms “sedentary” and “sedentary behaviours”. Appl. Physiol. Nutr. Metab. 2012, 37, 540–542. [Google Scholar]
- Benatti, F.B.; Larsen, S.A.; Kofoed, K.; Nielsen, S.T.; Harder-Lauridsen, N.M.; Lyngbaek, M.P.; Eriksen, D.; Karstoft, K.; Krogh-Madsen, R.; Pedersen, B.K.; et al. Intermittent Standing but not a moderate exercise bout reduces postprandial glycemia. Med. Sci. Sports Exerc. 2017, 49, 2305–2314. [Google Scholar] [CrossRef] [PubMed]
- Chastin, S.F.; Palarea-Albaladejo, J.; Dontje, M.L.; Skelton, D.A. Combined effects of time spent in physical activity, sedentary behaviors and sleep on obesity and cardio-metabolic health markers: A novel compositional data analysis approach. PLoS ONE 2015, 10, e0139984. [Google Scholar] [CrossRef] [PubMed]
- Katzmarzyk, P.T.; Church, T.S.; Craig, C.L.; Bouchard, C. Sitting time and mortality from all causes, cardiovascular disease, and cancer. Med. Sci. Sports Exerc. 2009, 41, 998–1005. [Google Scholar] [CrossRef] [PubMed]
- Lyden, K.; Keadle, S.K.; Staudenmayer, J.; Braun, B.; Freedson, P.S. Discrete features of sedentary behavior impact cardiometabolic risk factors. Med. Sci. Sport Exerc. 2015, 47, 1079–1086. [Google Scholar] [CrossRef] [PubMed]
- Wennberg, P.; Boraxbekk, C.-J.; Wheeler, M.; Howard, B.; Dempsey, P.C.; Lambert, G.; Eikelis, N.; Larsen, R.; Sethi, P.; Occleston, J.; et al. Acute effects of breaking up prolonged sitting on fatigue and cognition: A pilot study. BMJ Open 2016, 6, e009630. [Google Scholar] [CrossRef] [PubMed]
- Matthews, C.E.; Chen, K.Y.; Freedson, P.S.; Buchowski, M.S.; Beech, B.M.; Pate, R.R.; Troiano, R.P. Amount of time spent in sedentary behaviors in the United States, 2003–2004. Am. J. Epidemiol. 2008, 167, 875–881. [Google Scholar] [CrossRef] [PubMed]
- Ekblom-Bak, E.; Olsson, G.; Ekblom, Ö.; Ekblom, B.; Bergström, G.; Börjesson, M. The daily movement pattern and fulfilment of physical activity recommendations in Swedish middle-aged adults: The SCAPIS pilot study. PLoS ONE 2015, 10, e0126336. [Google Scholar] [CrossRef] [PubMed]
- Hagströmer, M.; Troiano, R.P.; Sjöström, M.; Berrigan, D. Levels and patterns of objectively assessed physical activity—A comparison between Sweden and the United States. Am. J. Epidemiol. 2010, 171, 1055–1064. [Google Scholar] [CrossRef] [PubMed]
- Brownson, R.C.; Boehmer, T.K.; Luke, D.A. Declining rates of physical activity in the United States: What are the contributors? Ann. Rev. Public Health 2005, 26, 421–443. [Google Scholar] [CrossRef] [PubMed]
- Straker, L.; Mathiassen, S.E. Increased physical work loads in modern work—A necessity for better health and performance? Ergonomics 2009, 52, 1215–1225. [Google Scholar] [CrossRef] [PubMed]
- Parry, S.; Straker, L. The contribution of office work to sedentary behaviour associated risk. BMC Public Health 2013, 13, 296. [Google Scholar] [CrossRef] [PubMed]
- Castillo-Retamal, M.; Hinckson, E.A. Measuring physical activity and sedentary behaviour at work: A review. Work 2011, 404, 345–357. [Google Scholar] [CrossRef]
- Labrique, A.B.; Vasudevan, L.; Kochi, E.; Fabricant, R.; Mehl, G. mHealth innovations as health system strengthening tools: 12 common applications and a visual framework. Glob. Health Sci. Pract. 2013, 1, 160–171. [Google Scholar] [CrossRef] [PubMed]
- Healy, G.N.; Eakin, E.G.; LaMontagne, A.D.; Owen, N.; Winkler, E.A.H.; Wiesner, G.; Gunning, L.; Neuhaus, M.; Lawler, S.; Fjeldsoe, B.S.; et al. Reducing sitting time in office workers: Short-term efficacy of a multicomponent intervention. Prev. Med. 2013, 57, 43–48. [Google Scholar] [CrossRef] [PubMed]
- Alkhajah, T.A.; Reeves, M.M.; Eakin, E.G.; Winkler, E.A.; Owen, N.; Healy, G.N. Sit–stand workstations: A pilot intervention to reduce office sitting time. Am. J. Prev. Med. 2012, 43, 298–303. [Google Scholar] [CrossRef] [PubMed]
- John, D.; Thompson, D.L.; Raynor, H.; Bielak, K.; Rider, B.; Bassett, D.R. Treadmill workstations: A worksite physical activity intervention in overweight and obese office workers. J. Phys. Act. Health 2011, 8, 1034–1043. [Google Scholar] [CrossRef] [PubMed]
- Urda, J.L.; Lynn, J.S.; Gorman, A.; Larouere, B. Effects of a minimal workplace intervention to reduce sedentary behaviors and improve perceived wellness in middle-aged women office workers. J. Phys. Act. Health 2016, 13, 838–844. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Tackling NCDs: ‘Best Buys’ and Other Recommended Interventions for the Prevention and Control of Noncommunicable Disease; World Health Organization: Geneva, Switzerland, 2017. [Google Scholar]
- Greaves, C.J.; Sheppard, K.E.; Abraham, C.; Hardeman, W.; Roden, M.; Evans, P.H.; Schwarz, P. Systematic review of reviews of intervention components associated with increased effectiveness in dietary and physical activity interventions. BMC Public Health 2011, 11, 119. [Google Scholar] [CrossRef] [PubMed]
- Chau, J.Y.; van der Ploeg, H.P.; van Uffelen, J.G.; Wong, J.; Riphagen, I.; Healy, G.N.; Gilson, N.D.; Dunstan, D.W.; Bauman, A.E.; Owen, N.; et al. Are workplace interventions to reduce effective sitting? A systematic review. Prev Med. 2010, 51, 352–356. [Google Scholar] [CrossRef] [PubMed]
- Fitzsimons, C.F.; Kirk, A.; Baker, G.; Michie, F.; Kane, C.; Mutrie, N. Using an individualised consultation and activPAL™ feedback to reduce sedentary time in older Scottish adults: Results of a feasibility and pilot study. Prev. Med. 2013, 57, 718–720. [Google Scholar] [CrossRef] [PubMed]
- Edwardson, C.L.; Winkler, E.A.; Bodicoat, D.H.; Yates, T.; Davies, M.J.; Dunstan, D.W.; Healy, G.N. Considerations when using the activPAL monitor in field-based research with adult populations. J. Sport Health Sci. 2017, 6, 162–178. [Google Scholar] [CrossRef]
- Lewin, K. Frontiers in group dynamics: I. Concept, method and reality in social sciences; social equilibria and social change. Hum. Relat. 1947, 1, 5–41. [Google Scholar] [CrossRef]
- Kruglanski, A.W.; Bélanger, J.J.; Chen, X.; Köpetz, C.; Pierro, A.; Mannetti, L. The energetics of motivated cognition: A force-field analysis. Psychol. Rev. 2012, 119, 1–20. [Google Scholar] [CrossRef] [PubMed]
- Michie, S.; Richardson, M.; Johnston, M.; Abraham, C.; Francis, J.; Hardeman, W.; Eccles, M.P.; Cane, J.; Wood, C.E. The behavior change technique taxonomy (v1) of 93 hierarchically clustered techniques: Building an international consensus for the reporting of behavior change interventions. Ann. Behav. Med. 2013, 46, 81–95. [Google Scholar] [CrossRef] [PubMed]
- Conner, M.; Rhodes, R.E.; Morris, B.; McEachan, R.; Lawton, R. Changing exercise through targeting affective or cognitive attitudes. Psychol. Health 2011, 26, 133–149. [Google Scholar] [CrossRef] [PubMed]
- O’Keefe, D.J.; Jensen, J.D. The relative persuasiveness of gain-framed loss-framed messages for encouraging disease prevention behaviors: A meta-analytic review. J. Health Commun. 2007, 12, 623–644. [Google Scholar] [CrossRef] [PubMed]
- Lyden, K.; Kozey-Keadle, S.L.; Staudenmayer, J.W.; Freedson, P.S. Validity of two wearable monitors to estimate breaks from sedentary time. Med. Sci. Sports Exerc. 2012, 44, 2243–2252. [Google Scholar] [CrossRef] [PubMed]
- Warner, R. Applied Statistics from Bivariate through Multivariate Techniques; SAGE: Washington, DC, USA, 2013. [Google Scholar]
- Healy, G.N.; Matthews, C.E.; Dunstan, D.W.; Winkler, E.A.; Owen, N. Sedentary time and cardio-metabolic biomarkers in US adults: NHANES 2003–06. Eur. Heart J. 2011, 32, 590–597. [Google Scholar] [CrossRef] [PubMed]
- Manini, T.M.; Carr, L.J.; King, A.C.; Marshall, S.; Robinson, T.N.; Rejeski, W.J. Interventions to reduce sedentary behavior. Med. Sci. Sports Exerc. 2015, 47, 1306–1310. [Google Scholar] [CrossRef] [PubMed]
- O’Donnell, M.P. (Ed.) Health Promotion in the Workplace, 3rd ed.; Cengage Learning: Boston, MA, USA, 2002. [Google Scholar]
- Sallis, J.F.; Cervero, R.B.; Ascher, W.; Henderson, K.A.; Kraft, M.K.; Kerr, J. An ecological approach to creating active living communities. Ann. Rev. Public Health 2006, 27, 297–322. [Google Scholar] [CrossRef] [PubMed]
- Evans, R.E.; Fawole, H.O.; Sheriff, S.A.; Dall, P.M.; Grant, P.M.; Ryan, C.G. Point-of-choice prompts to reduce sitting time at work: A randomized trial. Am. J. Prev. Med. 2012, 43, 293–297. [Google Scholar] [CrossRef] [PubMed]
- Spring, B.; Doran, N.; Pagoto, S.; Schneider, K.; Pingitore, R.; Hedeker, D. Randomized controlled trial for behavioral smoking and weight control treatment: Effect of concurrent versus sequential intervention. J. Consult. Clin. Psychol. 2004, 72, 785–796. [Google Scholar] [CrossRef] [PubMed]
- Chu, A.H.Y.; Ng, S.H.; Tan, C.S.; Win, A.M.; Koh, D.; Müller-Riemenschneider, F. A systematic review and meta-analysis of workplace intervention strategies to reduce sedentary time in white-collar workers. Obes. Rev. 2016, 17, 467–481. [Google Scholar] [CrossRef] [PubMed]
- Behrens, T.K.; Dinger, M.K. Motion sensor reactivity in physically active young adults. Res. Q. Exerc. Sport 2007, 78, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Davis, R.E.; Loprinzi, P.D. Examination of accelerometer reactivity among a population sample of children, adolescents, and adults. J. Phys. Act. Health 2016, 13, 1325–1332. [Google Scholar] [CrossRef] [PubMed]
| Intervention Stage | Objectives | Behaviour Change Techniques | Example |
|---|---|---|---|
| Stage 1 | Increase knowledge or understanding of sedentary behaviour (SB) health risks | Information about health consequences and the salience of such consequences from credible sources | Share information on health risks and consequences associated with SB using handout from the American College of Sports Medicine. |
| Stage 2 | Review and reflect upon own SB patterns using activPal output | Develop discrepancy between current behaviour and goal. Consider pros and cons of decreasing SB. | Review current patterns of SB relative to desired SB. List and compare the advantages and disadvantages of sitting less at work. |
| Stage 3 | Develop strategies to decrease SB in the workplace | Action planning | Plan times for standing breaks during the workday. |
| Prompts/cues | Keep a set of sneakers or comfortable shoes in the office. | ||
| Habit formation | Stand up every time the phone rings. | ||
| Restructuring the physical and social environment | Purchase or build a sit-stand desk. Promote standing/walking meetings. | ||
| Stage 4 | Identify barriers to decreasing SB in the workplace and provide solutions | Problem solving | Brainstorm ways to combine work with movement (e.g., walking office hours). |
| Prompts/cues | Set electronic reminders to take standing breaks. | ||
| Behaviour substitution | Use a bathroom on a different floor of the building. | ||
| Stage 5 | Set goal to break up SB bouts > 30 min | Goal setting | Make a behavioural resolution relative to target behaviour on reducing SB bouts >30 min |
| Variable | Mean (SD) |
|---|---|
| Sedentary time (h/day) | 9.4 (1.5) |
| Standing time (h/day) | 4.5 (1.3) |
| Stepping time (h/day) | 1.9 (0.5) |
| Sedentary time (h/working day) | 4.5 (1.5) |
| Standing time (h/working day) | 2.5 (1.1) |
| Stepping time (h/day) | 1.0 (0.5) |
| Variable | Baseline | Follow-Up | p-Value |
|---|---|---|---|
| Sedentary time (%) | 59.1 (8.3) | 58.6 (11.2) | 0.611 |
| Standing time (%) | 28.5 (7.4) | 29.0 (9.8) | 0.649 |
| Stepping time (%) | 12.3 (3.5) | 12.5 (4.3) | 0.765 |
| Bouts 10–19.99 min | 6.8 (2.2) | 6.8 (2.2) | 0.982 |
| Bouts 20–20.99 min | 3.1 (0.9) | 3.0 (1.0) | 0.917 |
| Bouts > 30 min | 4.8 (1.3) | 4.3 (1.6) | 0.010 |
| Sitting to upright transitions | 39.3 (7.8) | 37.6 (7.8) | 0.175 |
| Variable | Baseline | Follow-Up | p-Value |
|---|---|---|---|
| Sedentary time (%) | 56.0 (15.2) | 54.8 (17.4) | 0.575 |
| Standing time (%) | 30.9 (13.3) | 32.4 (16.8) | 0.428 |
| Stepping time (%) | 13.1 (7.1) | 12.8 (8.8) | 0.748 |
| Bouts 10–19.99 min | 3.9 (1.9) | 4.0 (2.0) | 0.886 |
| Bouts 20–20.99 min | 1.6 (0.9) | 1.7 (0.9) | 0.575 |
| Bouts > 30 min | 2.0 (1.3) | 1.9 (1.4) | 0.663 |
| Sitting to upright transitions | 22.3 (8.2) | 21.3 (7.7) | 0.415 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hutchinson, J.; Headley, S.; Matthews, T.; Spicer, G.; Dempsey, K.; Wooley, S.; Janssen, X. Changes in Sitting Time and Sitting Fragmentation after a Workplace Sedentary Behaviour Intervention. Int. J. Environ. Res. Public Health 2018, 15, 1148. https://doi.org/10.3390/ijerph15061148
Hutchinson J, Headley S, Matthews T, Spicer G, Dempsey K, Wooley S, Janssen X. Changes in Sitting Time and Sitting Fragmentation after a Workplace Sedentary Behaviour Intervention. International Journal of Environmental Research and Public Health. 2018; 15(6):1148. https://doi.org/10.3390/ijerph15061148
Chicago/Turabian StyleHutchinson, Jasmin, Samuel Headley, Tracey Matthews, Greg Spicer, Kristen Dempsey, Sarah Wooley, and Xanne Janssen. 2018. "Changes in Sitting Time and Sitting Fragmentation after a Workplace Sedentary Behaviour Intervention" International Journal of Environmental Research and Public Health 15, no. 6: 1148. https://doi.org/10.3390/ijerph15061148
APA StyleHutchinson, J., Headley, S., Matthews, T., Spicer, G., Dempsey, K., Wooley, S., & Janssen, X. (2018). Changes in Sitting Time and Sitting Fragmentation after a Workplace Sedentary Behaviour Intervention. International Journal of Environmental Research and Public Health, 15(6), 1148. https://doi.org/10.3390/ijerph15061148





