Preliminary Assessment of Hurricane Harvey Exposures and Mental Health Impact
Abstract
:1. Introduction
2. Materials and Methods
2.1. Hurricane Exposures
2.2. Mental Health Outcomes
2.3. Statistical Analysis
3. Results
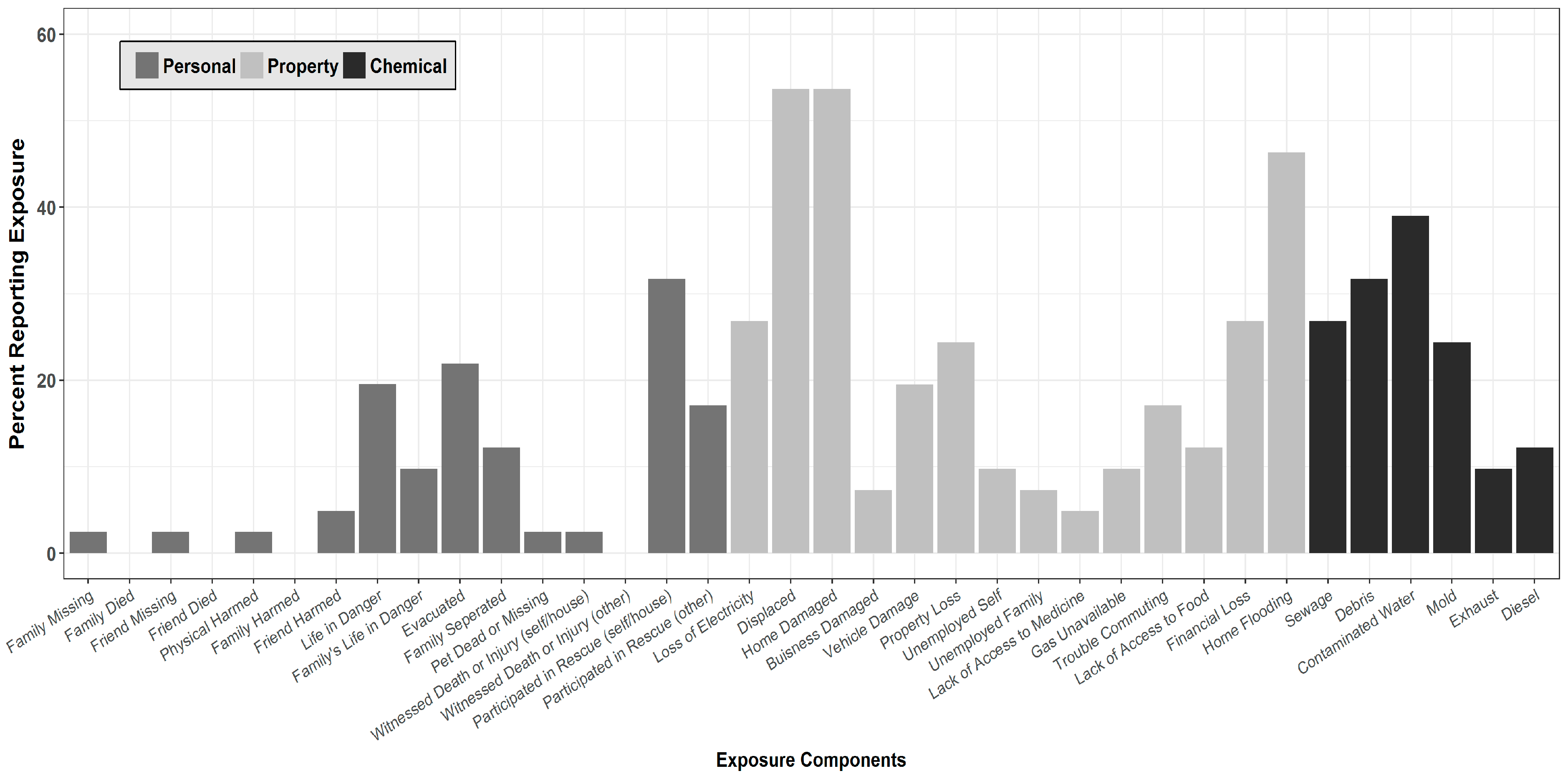
3.1. Hurricane Exposures
3.2. Mental Health Symptomology
4. Discussion
4.1. Hurricane Exposure and Mental Health
4.2. Strengths and Limitations
4.3. Future Research Implications
5. Conclusions
Supplementary Materials
Author Contributions
Acknowledgments
Conflicts of Interest
References
- CNN, B.G. CNN Design: Lansing Cai Harvey’s Devastating Impact by the Numbers. Available online: http://www.cnn.com/2017/08/27/us/harvey-impact-by-the-numbers-trnd/index.html (accessed on 25 October 2017).
- Schwartz, R.M.; Sison, C.; Kerath, S.M.; Murphy, L.; Breil, T.; Sikavi, D.; Taioli, E. The impact of Hurricane Sandy on the mental health of New York area residents. Am. J. Disaster Med. 2015, 10, 339–346. [Google Scholar] [CrossRef] [PubMed]
- Cerdá, M.; Bordelois, P.M.; Galea, S.; Norris, F.; Tracy, M.; Koenen, K.C. The course of posttraumatic stress symptoms and functional impairment following a disaster: What is the lasting influence of acute versus ongoing traumatic events and stressors? Soc. Psychiatry Psychiatr. Epidemiol. 2013, 48, 385–395. [Google Scholar] [CrossRef] [PubMed]
- Neria, Y.; Nandi, A.; Galea, S. Post-traumatic stress disorder following disasters: A systematic review. Psychol. Med. 2008, 38, 467–480. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, R.M.; Liu, B.; Lieberman-Cribbin, W.; Taioli, E. Displacement and mental health after natural disasters. Lancet Planet. Health 2017, 1, e314. [Google Scholar] [CrossRef]
- Lê, F.; Tracy, M.; Norris, F.H.; Galea, S. Displacement, county social cohesion, and depression after a large-scale traumatic event. Soc Psychiatry Psychiatr. Epidemiol. 2013, 48, 1729–1741. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, R.M.; Rasul, R.; Kerath, S.M.; Watson, A.R.; Lieberman-Cribbin, W.; Liu, B.; Taioli, E. Displacement during Hurricane Sandy: The impact on mental health. J. Emerg. Manag. 2018, 16, 17–27. [Google Scholar] [CrossRef] [PubMed]
- Fullilove, M.T. Psychiatric implications of displacement: Contributions from the psychology of place. Am. J. Psychiatry 1996, 153, 1516–1523. [Google Scholar] [CrossRef] [PubMed]
- Wadsworth, M.E.; Santiago, C.D.; Einhorn, L. Coping with displacement from Hurricane Katrina: Predictors of one-year post-traumatic stress and depression symptom trajectories. Anxiety Stress Coping 2009, 22, 413–432. [Google Scholar] [CrossRef] [PubMed]
- CNBC Hurricane Harvey Rains Flood Toxic Superfund Sites in Texas. Available online: https://www.cnbc.com/2017/09/03/hurricane-harvey-rains-flood-toxic-superfund-sites-in-texas.html (accessed on 25 October 2017).
- Grattan, L.M.; Roberts, S.; Mahan, W.T.; McLaughlin, P.K.; Otwell, W.S.; Morris, J.G. The early psychological impacts of the Deepwater Horizon oil spill on Florida and Alabama communities. Environ. Health Perspect. 2011, 119, 838–843. [Google Scholar] [CrossRef] [PubMed]
- Osofsky, H.J.; Osofsky, J.D.; Hansel, T.C. Deepwater horizon oil spill: Mental health effects on residents in heavily affected areas. Disaster Med. Public Health Prep. 2011, 5, 280–286. [Google Scholar] [CrossRef] [PubMed]
- Clark, K.A.; Chanda, D.; Balte, P.; Karmaus, W.J.; Cai, B.; Vena, J.; Lawson, A.B.; Mohr, L.C.; Gibson, J.J.; Svendsen, E.R. Respiratory symptoms and lung function 8–10 months after community exposure to chlorine gas: A public health intervention and cross-sectional analysis. BMC Public Health 2013, 13, 945. [Google Scholar] [CrossRef] [PubMed]
- Shenassa, E.D.; Daskalakis, C.; Liebhaber, A.; Braubach, M.; Brown, M. Dampness and Mold in the Home and Depression: An Examination of Mold-Related Illness and Perceived Control of One’s Home as Possible Depression Pathways. Am. J. Public Health 2007, 97, 1893–1899. [Google Scholar] [CrossRef] [PubMed]
- Dalton, P.; Wysocki, C.J.; Brody, M.J.; Lawley, H.J. The influence of cognitive bias on the perceived odor, irritation and health symptoms from chemical exposure. Int. Arch. Occup. Environ. Health 1997, 69, 407–417. [Google Scholar] [CrossRef] [PubMed]
- Peek, M.; Cutchin, M.; Freeman, D.; Stowe, R.; Goodwin, J. Environmental hazards and stress: Evidence from the Texas City Stress and Health Study. J. Epidemiol. Community Health 2009, 63, 792–798. [Google Scholar] [CrossRef] [PubMed]
- Flory, K.; Kloos, B.; Hankin, B.L.; Cheely, C.A. Clinical Research After Catastrophic Disasters: Lessons Learned From Hurricane Katrina. Prof. Psychol. Res. Pract. 2008, 39, 107–112. [Google Scholar] [CrossRef] [PubMed]
- Ochi, S.; Hodgson, S.; Landeg, O.; Mayner, L.; Murray, V. Disaster-driven evacuation and medication loss: A systematic literature review. PLoS Curr. 2014, 6. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, R.; Liu, B.; Sison, C.; Kerath, S.M.; Breil, T.; Murphy, L.; Taioli, E. Study Design and Results of a Population-Based Study on Perceived Stress Following Hurricane Sandy. Disaster Med. Public Health Prep. 2016, 10, 325–332. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, R.M.; Gillezeau, C.N.; Liu, B.; Lieberman-Cribbin, W.; Taioli, E. Longitudinal Impact of Hurricane Sandy Exposure on Mental Health Symptoms. Int. J. Environ. Res. Public Health 2017, 14, 957. [Google Scholar] [CrossRef] [PubMed]
- Rebecca, M.; Schwartz, P.; Patricia Rothenberg, B.A.; Samantha M. Kerath, M.S.; Bian Liu, P.; Emanuela Taioli, M.D. The lasting mental health effects of Hurricane Sandy on residents of the Rockaways. J. Emerg. Manag. 2016, 14, 269–279. [Google Scholar] [CrossRef]
- Ginsberg, J.P.; Holbrook, J.R.; Chanda, D.; Bao, H.; Svendsen, E.R. Posttraumatic stress and tendency to panic in the aftermath of the chlorine gas disaster in Graniteville, South Carolina. Soc. Psychiatry Psychiatr. Epidemiol. 2012, 47, 1441–1448. [Google Scholar] [CrossRef] [PubMed]
- Fussell, E.; Lowe, S.R. The impact of housing displacement on the mental health of low-income parents after Hurricane Katrina. Soc. Sci. Med. 2014, 113, 137–144. [Google Scholar] [CrossRef] [PubMed]
- Sullivan, G.; Vasterling, J.J.; Han, X.; Tharp, A.T.; Davis, T.; Deitch, E.A.; Constans, J.I. Preexisting Mental Illness and Risk for Developing a New Disorder After Hurricane Katrina. J. Nerv. Ment. Dis. 2013, 201, 161–166. [Google Scholar] [CrossRef] [PubMed]
- Springgate, B.F.; Wennerstrom, A.; Meyers, D.; Allen, C.E.; Vannoy, S.D.; Bentham, W.; Wells, K.B. Building community resilience through mental health infrastructure and training in post-Katrina New Orleans. Ethn. Dis. 2011, 21, S1–29. [Google Scholar] [PubMed]
| Demographics | N = 41 |
|---|---|
| Gender | |
| Female | 23 (56.1%) |
| Male | 18 (41.9%) |
| Ethnicity | |
| White | 14 (35.0%) |
| Black | 13 (32.5%) |
| American Indian | 1 (2.5%) |
| Hispanic | 8 (20.0%) |
| Pacific Islander/Asian | 4 (10.0%) |
| US Born | |
| No | 9 (22.0%) |
| Yes | 32 (78.0%) |
| Education | |
| <High School Degree | 3 (7.9%) |
| High School Degree | 6 (15.8%) |
| Some College | 8 (21.0%) |
| College Degree | 8 (21.1%) |
| Post-Graduate Degree | 13 (34.2%) |
| Health Insurance | |
| No | 9 (22.0%) |
| Yes | 32 (78.0%) |
| Mental Health Condition Prior to Harvey | |
| No | 29 (70.7%) |
| Yes | 12 (29.3%) |
| Age (years) | 44.2 ± 10.3 |
| Household Size (# of people) | 2.4 ± 1.1 |
| Exposure | PTSD (PCL ≥ 30) Mean (SD) | Anxiety (PHQ-4 ≥ 3) Mean (SD) | Depression (PHQ-4 ≥ 3) Mean (SD) | ||||||
|---|---|---|---|---|---|---|---|---|---|
| No | Yes | ORadj * (95% CI) | No | Yes | ORadj * (95% CI) | No | Yes | ORadj * (95% CI) | |
| Chemical/Toxin | 0.77 (1.45) | 2.21 (2.35) ^ | 1.45 (0.95–2.21) | 0.53 (1.12) | 2.23 (2.31) + | 1.96 (1.16–3.32) | 1.04 (1.85) | 2.06 (2.21) | 1.36 (0.94–1.96) |
| Hurricane overall | 2.36 (2.32) | 6.95 (5.29) ^ | 1.42 (1.06–2.05) | 2.36 (2.34) | 6.33 (5.22) ^ | 1.50 (1.09–2.06) | 3.72 (4.66) | 5.69 (4.25) @ | 1.10 (0.93–1.31) |
| Hurricane Personal | 0.68 (0.84) | 2.00 (2.26) # | 2.29 (0.92–5.71) | 0.79 (0.92) | 1.73 (2.19) | 1.97 (0.92–4.27) | 1.20 (1.68) | 1.44 (1.93) | 1.10 (0.72–1.68) |
| Hurricane Property | 1.68 (1.94) | 4.95 (3.44) | 1.53 (1.07–2.18) | 1.58 (1.92) | 4.59 (3.39) ^ | 1.60 (1.13–2.28) | 2.52 (3.28) | 4.25 (2.74) + | 1.18 (0.93–1.51) |
| Displacement (%) | |||||||||
| No | 17 (89) | 2 (11) ^ | 1 (ref) | 13 (68) | 6 (32) ^ | 1 (ref) | 16 (84) | 3 (16) ^ | 1 (ref) |
| Yes | 5 (23) | 17 (77) | 12.50 (1.43–108.92) | 6 (27) | 16 (73) | 6.66 (0.922–48.09) | 9 (41) | 13 (59) | 15.76 (1.22–203.06) |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Schwartz, R.M.; Tuminello, S.; Kerath, S.M.; Rios, J.; Lieberman-Cribbin, W.; Taioli, E. Preliminary Assessment of Hurricane Harvey Exposures and Mental Health Impact. Int. J. Environ. Res. Public Health 2018, 15, 974. https://doi.org/10.3390/ijerph15050974
Schwartz RM, Tuminello S, Kerath SM, Rios J, Lieberman-Cribbin W, Taioli E. Preliminary Assessment of Hurricane Harvey Exposures and Mental Health Impact. International Journal of Environmental Research and Public Health. 2018; 15(5):974. https://doi.org/10.3390/ijerph15050974
Chicago/Turabian StyleSchwartz, Rebecca M., Stephanie Tuminello, Samantha M. Kerath, Janelle Rios, Wil Lieberman-Cribbin, and Emanuela Taioli. 2018. "Preliminary Assessment of Hurricane Harvey Exposures and Mental Health Impact" International Journal of Environmental Research and Public Health 15, no. 5: 974. https://doi.org/10.3390/ijerph15050974
APA StyleSchwartz, R. M., Tuminello, S., Kerath, S. M., Rios, J., Lieberman-Cribbin, W., & Taioli, E. (2018). Preliminary Assessment of Hurricane Harvey Exposures and Mental Health Impact. International Journal of Environmental Research and Public Health, 15(5), 974. https://doi.org/10.3390/ijerph15050974






