Relative Density of Away from Home Food Establishments and Food Spend for 24,047 Households in England: A Cross-Sectional Study
Abstract
1. Background
2. Methods
2.1. Data Source and Participants
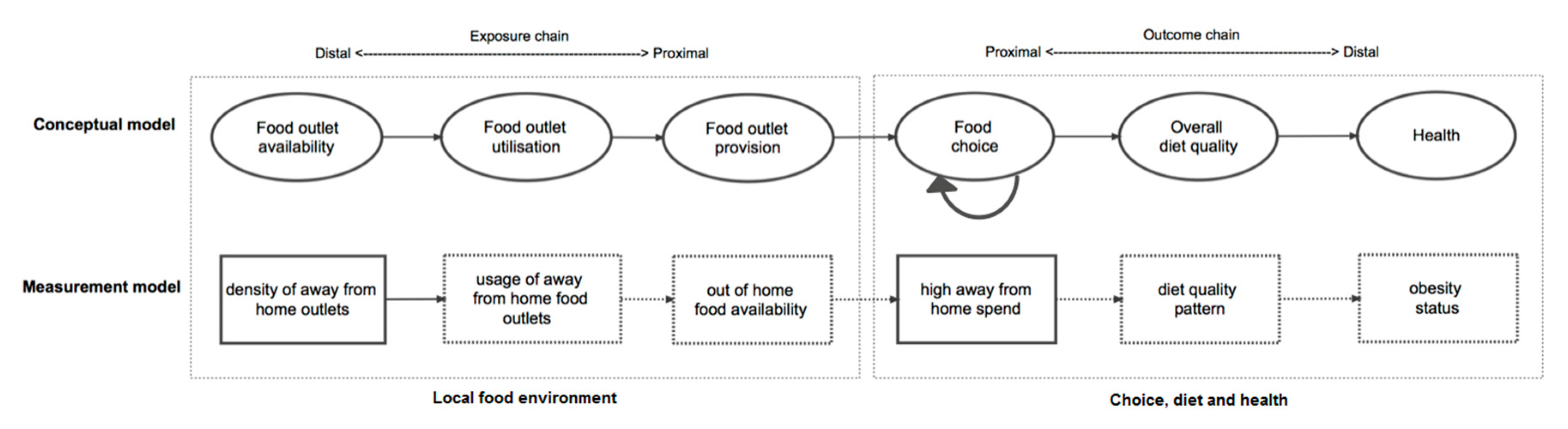
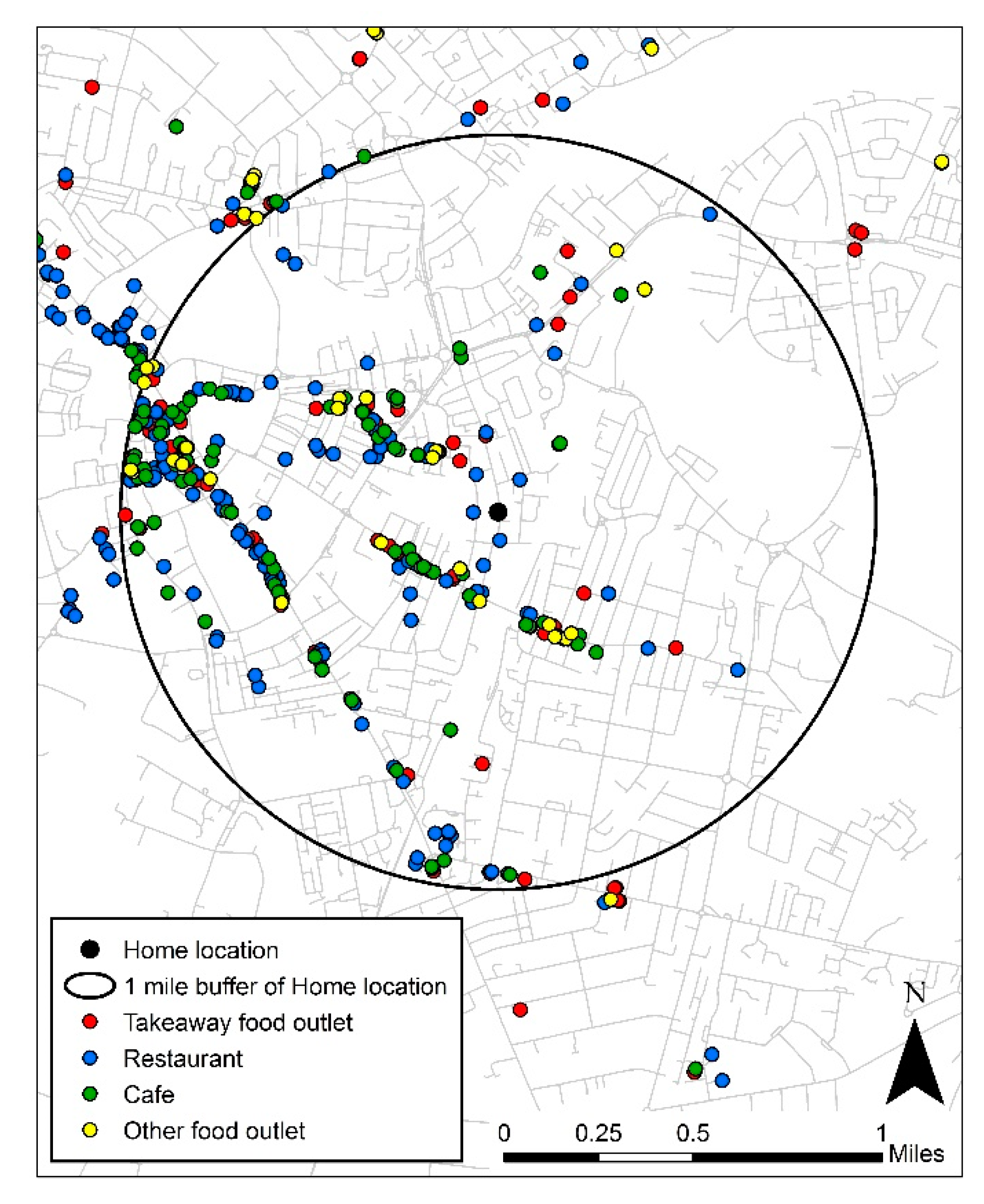
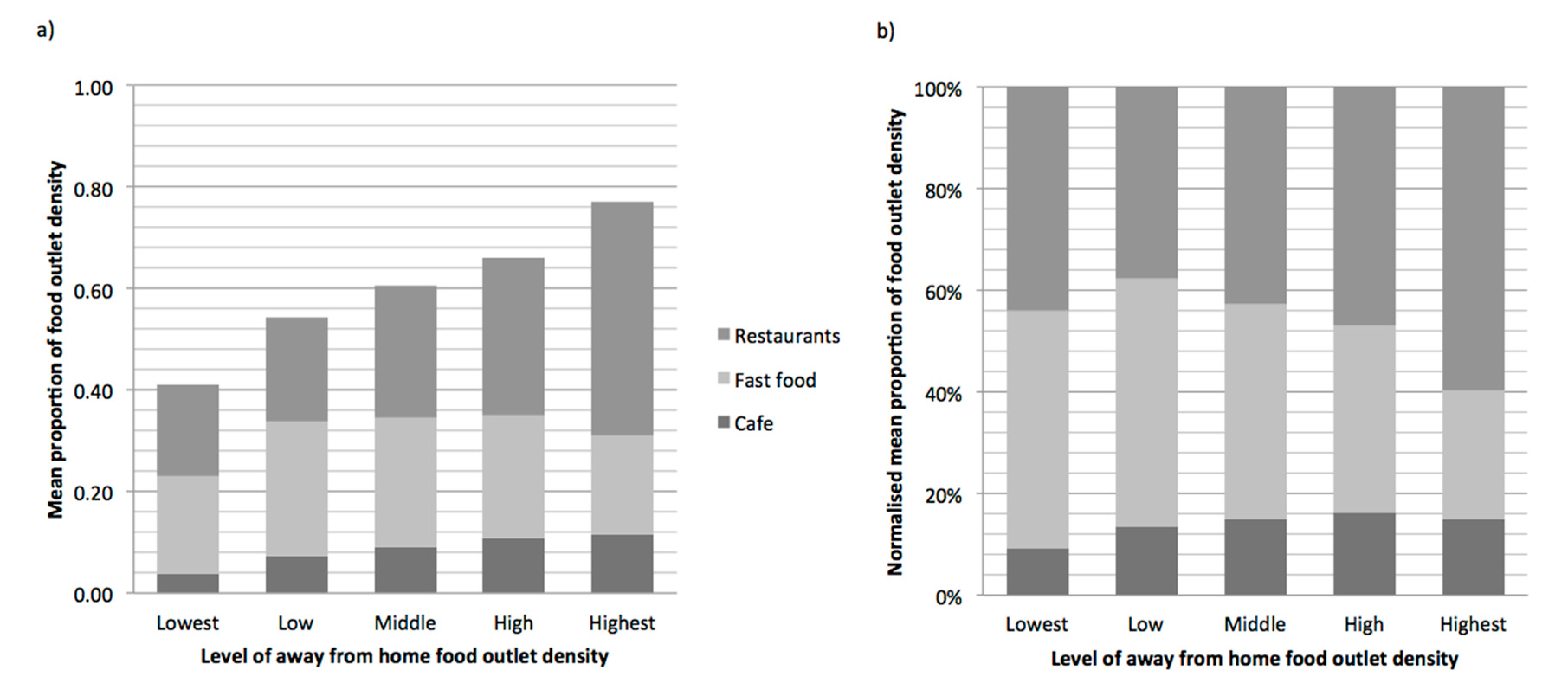
2.2. Exposure: Density of Away from Home Food Outlets to All Food Outlets
2.3. Outcome: Household with High Away from Home Food Spend
2.4. Additional Covariates
2.5. Statistical Analyses
2.6. Sensitivity Analyses
3. Results
4. Discussion
4.1. Policy Implications
4.2. Methodological Considerations and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Geneva: World Health Organization. Global Action Plan for the Prevention And Control of Noncommunicable Diseases 2013–2020. 2013. Available online: http://apps.who.int/iris/bitstream/10665/94384/1/9789241506236_eng.pdf (accessed on 3 December 2018).
- Newton, J.N.; Briggs, A.D.M.; Murray, C.J.L.; Dicker, D.; Foreman, K.J.; Wang, H.; Naghavi, M.; Forouzanfar, M.H.; Ohno, S.L.; Barber, R.M.; et al. Changes in health in England, with analysis by English regions and areas of deprivation, 1990–2013: A systematic analysis for the Global Burden of Disease Study 2013. Lancet 2015, 386, 2257–2274. [Google Scholar] [CrossRef]
- Bates, B.; Lennox, A.; Prentice, A.; Bates, C.; Page, P.; Nicholson, S.; Swan, G. National Diet and Nutrition Survey Results from Years 1, 2, 3 and 4 (combined) of the Rolling Programme (2008/2009–2011/2012); Food Standards Agency and Public Health England: London, England, 2014. Available online: https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/310995/NDNS_Y1_to_4_UK_report.pdf (accessed on 12 February 2018).
- Lachat, C.; Nago, E.; Verstraeten, R.; Roberfroid, D.; Van Camp, J.; Kolsteren, P. Eating out of home and its association with dietary intake: A systematic review of the evidence. Obes. Rev. 2012, 13, 329–346. [Google Scholar] [CrossRef] [PubMed]
- Penney, T.L.; Jones, N.R.V.; Adams, J.; Maguire, E.R.; Burgoine, T.; Monsivais, P. Utilization of Away-From-Home Food Establishments, Dietary Approaches to Stop Hypertension Dietary Pattern, and Obesity. Am. J. Prev. Med. 2017, 53, e155–e163. [Google Scholar] [CrossRef] [PubMed]
- Kant, A.K.; Whitley, M.I.; Graubard, B.I. Away from home meals: Associations with biomarkers of chronic disease and dietary intake in American adults, NHANES 2005-2010. Int. J. Obes. 2015, 39, 820–827. [Google Scholar] [CrossRef] [PubMed]
- Jaworowska, A.M.; Blackham, T.; Long, R.; Taylor, C. Nutritional composition of takeaway food in the UK. Nutr. Food Sci. 2014, 44, 414–430. [Google Scholar] [CrossRef]
- Nago, E.; Lachat, C.; Dossa, R.; Kolsteren, P. Association of out-of-home eating with anthropometric change: A systematic review of prospective studies. Crit. Rev. Food Sci. Nutr. 2014, 54, 1103–1116. [Google Scholar] [CrossRef]
- Bezerra, I.N.; Curioni, C.; Sichieri, R. Association between eating out of home and body weight. Nutr. Rev. 2012, 70, 65–79. [Google Scholar] [CrossRef]
- Luan, H.; Law, J.; Quick, M. Identifying food deserts and swamps based on relative healthy food access: A spatio-temporal Bayesian approach. Int. J. Health Geogr. 2015, 14, 1–11. [Google Scholar] [CrossRef]
- Larson, N.; Story, M. A review of environmental influences on food choices. Ann. Behav. Med. 2009, 38, 56–73. [Google Scholar] [CrossRef]
- Drewnowski, A. Taste Preferences and Food Intake. Annu. Rev. Nutr. 1997, 17, 237–253. [Google Scholar] [CrossRef]
- Cohen, D.; Farley, T.A. Eating as an automatic behavior. Prev. Chronic Dis. 2008, 5, A23. [Google Scholar] [PubMed]
- Sturm, R. Affordability and Obesity: Issues in the Multifunctionality of Agricultural/Food Systems. J. Hunger. Environ. Nutr. 2009, 4, 454–465. [Google Scholar] [CrossRef] [PubMed]
- Wang, M.C.; Cubbin, C.; Ahn, D.; Winkleby, M.A. Changes in neighbourhood food store environment, food behaviour and body mass index, 1981–1990. Public Health Nutr. 2008, 11, 963–970. [Google Scholar] [CrossRef] [PubMed]
- Office for National Statistics. Family Spending in the UK—Office for National Statistics. Available online: https://www.ons.gov.uk/peoplepopulationandcommunity/personalandhouseholdfinances/expenditure/bulletins/familyspendingintheuk/financialyearendingmarch2016 (accessed on 21 September 2017).
- Dubowitz, T.; Ghosh-Dastidar, M.; Eibner, C.; Slaughter, M.E.; Fernandes, M.; Whitsel, E.A.; Bird, C.E.; Jewell, A.; Margolis, K.L.; Li, W.; et al. The Women’s Health Initiative: The Food Environment, Neighborhood Socioeconomic Status, BMI, and Blood Pressure. Obesity 2012, 20, 862–871. [Google Scholar] [CrossRef]
- Dunn, R.A.; Sharkey, J.R.; Horel, S. The effect of fast-food availability on fast-food consumption and obesity among rural residents: An analysis by race/ethnicity. Econ. Hum. Biol. 2012, 10, 1–13. [Google Scholar] [CrossRef]
- Kruger, D.J.; Greenberg, E.; Murphy, J.B.; DiFazio, L.A.; Youra, K.R. Local concentration of fast-food outlets is associated with poor nutrition and obesity. Am. J. Health Promot. 2013, 28, 340–343. [Google Scholar] [CrossRef]
- Burgoine, T.; Forouhi, N.G.; Griffin, S.J.; Wareham, N.J.; Monsivais, P. Associations between exposure to takeaway food outlets, takeaway food consumption, and body weight in Cambridgeshire, UK: Population based, cross sectional study. BMJ 2014, 348, g1464. [Google Scholar] [CrossRef]
- Moore, L.V.; Diez Roux, A.V.; Nettleton, J.A.; Jacobs, D.R.; Franco, M. Fast-Food Consumption, Diet Quality, and Neighborhood Exposure to Fast Food: The Multi-Ethnic Study of Atherosclerosis. Am. J. Epidemiol. 2009, 170, 29–36. [Google Scholar] [CrossRef]
- Paquet, C.; Daniel, M.; Knäuper, B.; Gauvin, L.; Kestens, Y.; Dubé, L. Interactive effects of reward sensitivity and residential fast-food restaurant exposure on fast-food consumption. Am. J. Clin. Nutr. 2010, 91, 771–776. [Google Scholar] [CrossRef]
- Thornton, L.E.; Bentley, R.J.; Kavanagh, A.M. Fast food purchasing and access to fast food restaurants: A multilevel analysis of VicLANES. Int. J. Behav. Nutr. Phys. Act. 2009, 6, 28. [Google Scholar] [CrossRef]
- NatCen Social Research University of Essex, Institute for Social and Economic Research. Understanding Society: Waves 1-7, 2009-2016 and Harmonised BHPS: Waves 1-18, 1991-2009: Secure Access, 8th ed.; UK Data Service; University of Essex: Essex, UK, 2018. [Google Scholar] [CrossRef]
- Knies, G. Understanding Society The UK Household Longitudinal Study Waves 1-5, User Manual; University of Essex: Essex, UK, 2015. [Google Scholar]
- Lynn, P. Sample Design for Understanding Society. 2009. Available online: https://www.iser.essex.ac.uk/research/publications/working-papers/understanding-society/2009-01 (accessed on 3 December 2018).
- Ordnance Survey. Points of Interest. 2015. Available online: https://www.ordnancesurvey.co.uk/business-and-government/products/points-of-interest.html (accessed on 12 February 2018).
- Ordnance Survey Limited. Available online: https://www.ordnancesurvey.co.uk/business-and-government/help-and-support/products/points-of-interest.html (accessed on 6 November 2018).
- Burgoine, T.; Harrison, F. Comparing the accuracy of two secondary food environment data sources in the UK across socio-economic and urban/rural divides. Int. J. Health Geogr. 2013, 12, 2. [Google Scholar] [CrossRef] [PubMed]
- Lake, A.A.; Burgoine, T.; Stamp, E.; Grieve, R. The foodscape: Classification and field validation of secondary data sources across urban/rural and socio-economic classifications in England. Int. J. Behav. Nutr. Phys. Act. 2012, 9, 37. [Google Scholar] [CrossRef] [PubMed]
- Powell, L.M.; Han, E.; Zenk, S.N.; Khan, T.; Quinn, C.M.; Gibbs, K.P.; Pugach, O.; Barker, D.C.; Resnick, E.A.; Myllyluoma, J.; et al. Field validation of secondary commercial data sources on the retail food outlet environment in the U.S. Health Place. 2011, 17, 1122–1131. [Google Scholar] [CrossRef] [PubMed]
- Cummins, S.; Macintyre, S. Are secondary data sources on the neighbourhood food environment accurate? Case-study in Glasgow, UK. Prev. Med. 2009, 49, 527–528. [Google Scholar] [CrossRef]
- Thornton, L.E.; Pearce, J.R.; Kavanagh, A.M. Using Geographic Information Systems (GIS) to assess the role of the built environment in influencing obesity: A glossary. Int. J. Behav. Nutr. Phys. Act. 2011, 8, 71. [Google Scholar] [CrossRef] [PubMed]
- Smith, G.; Gidlow, C.; Davey, R.; Foster, C. What is my walking neighbourhood? A pilot study of English adults’ definitions of their local walking neighbourhoods. Int. J. Behav. Nutr. Phys. Act. 2010, 7, 34. [Google Scholar] [CrossRef] [PubMed]
- Anyaegbu, G. Using the OECD equivalence scale in taxes and benefits analysis. Econ. Labour Mark. Rev. 2010, 4, 49–54. [Google Scholar] [CrossRef]
- Office for National Statistics. A Report on the Living Costs and Food Survey 2009. Fam. Spend. 2010. Available online: http://www.ons.gov.uk/ons/rel/family-spending/family-spending/2010-edition/index.html (accessed on 17 September 2017).
- Tang, W.; Aggarwal, A.; Liu, Z.; Acheson, M.; Rehm, C.D.; Moudon, A.V.; Drewnowski, A. Validating self-reported food expenditures against food store and eating-out receipts. Eur. J. Clin. Nutr. 2016, 70, 352–357. [Google Scholar] [CrossRef]
- Kim, S.; Egerter, S.; Cubbin, C.; Takahashi, E.R.; Braveman, P. Potential Implications of Missing Income Data in Population-Based Surveys: An Example from a Postpartum Survey in California. Public Health Rep. 2007, 122, 753–763. [Google Scholar] [CrossRef] [PubMed]
- StataCorp. Stata Statistical Software, StataCorp LP.: College Station, TX, USA, 2015.
- Beydoun, M.A.; Powell, L.M.; Wang, Y. Reduced away-from-home food expenditure and better nutrition knowledge and belief can improve quality of dietary intake among US adults. Public Health Nutr. 2008, 12, 1. [Google Scholar] [CrossRef]
- Cobb, L.K.; Appel, L.J.; Franco, M.; Jones-Smith, J.C.; Nur, A.; Anderson, C.A.M. The relationship of the local food environment with obesity: A systematic review of methods, study quality, and results. Obesity 2015, 23, 1331–1344. [Google Scholar] [CrossRef] [PubMed]
- Caspi, C.E.; Sorensen, G.; Subramanian, S.V.; Kawachi, I. The local food environment and diet: A systematic review. Health Place 2012, 18, 1172–1187. [Google Scholar] [CrossRef] [PubMed]
- Giskes, K.; van Lenthe, F.; Avendano-Pabon, M.; Brug, J. A systematic review of environmental factors and obesogenic dietary intakes among adults: Are we getting closer to understanding obesogenic environments? Obes. Rev. 2011, 12, e95–e106. [Google Scholar] [CrossRef] [PubMed]
- Burgoine, T.; Forouhi, N.G.; Griffin, S.J.; Brage, S.; Wareham, N.J.; Monsivais, P. Does neighborhood fast-food outlet exposure amplify inequalities in diet and obesity? A cross sectional study. Am. J. Clin. Nutr. 2016, 1540–1547. [Google Scholar] [CrossRef] [PubMed]
- Boone-Heinonen, J.; Gordon-Larsen, P.; Guilkey, D.K.; Jacobs, D.R.; Popkin, B.M. Environment and physical activity dynamics: The role of residential self-selection. Psychol. Sport Exerc. 2011, 12, 54–60. [Google Scholar] [CrossRef] [PubMed]
- Rydell, S.A.; Harnack, L.J.; Oakes, J.M.; Story, M.; Jeffery, R.W.; French, S.A. Why eat at fast-food restaurants: Reported reasons among frequent consumers. J. Am. Diet. Assoc. 2008, 108, 2066–2070. [Google Scholar] [CrossRef]
- Nestle, M.; Wing, R.; Birch, L.; DiSogra, L.; Drewnowski, A.; Middleton, S.; Sigman-Grant, M.; Sobal, J.; Winston, M.; Economos, C. Behavioral and Social Influences on Food Choice. Nutr. Rev. 2009, 56, 50–64. [Google Scholar] [CrossRef]
- Jabs, J.; Devine, C.M. Time scarcity and food choices: An overview. Appetite 2006, 47, 196–204. [Google Scholar] [CrossRef]
- Fleischhacker, S.E.; Evenson, K.R.; Rodriguez, D.A.; Ammerman, A.S. A systematic review of fast food access studies. Obes. Rev. 2011, 12, e460–e471. [Google Scholar] [CrossRef]
- Burgoine, T.; Sarkar, C.; Webster, C.J.; Monsivais, P. Examining the interaction of fast-food outlet exposure and income on diet and obesity: Evidence from 51,361 UK Biobank participants. Int. J. Behav. Nutr. Phys. Act. 2018, 15, 1–12. [Google Scholar] [CrossRef]
- Public Health England. Encouraging Healthier “Out of Home” Food Provision—A Toolkit. 2017. Available online: https://www.gov.uk/government/publications/encouraging-healthier-out-of-home-food-provision (accessed on 19 November 2018).
- Adams, J.; Mytton, O.; White, M.; Monsivais, P. Why Are Some Population Interventions for Diet and Obesity More Equitable and Effective Than Others? The Role of Individual Agency. PLOS Med. 2016, 13, e1001990. [Google Scholar] [CrossRef]
- Local Government Association. Tipping the Scales: Case Studies on the Use of Planning Powers to Limit Hot Food Takeaway | Local Government Association. 2017. Available online: https://www.local.gov.uk/tipping-scales-case-studies-use-planning-powers-limit-hot-food-takeaway (accessed on 19 November 2018).
- Los Angeles Fast Food Interim Control, Ordinance No. 180103 | Growing Food Connections. 2008. Available online: http://growingfoodconnections.org/gfc-policy/los-angeles-fast-food-interim-control-ordinance-no-180103/ (accessed on 19 November 2018).
- Lake, A.A.; Henderson, E.J.; Townshend, T.G. Exploring planners’ and public health practitioners’ views on addressing obesity: Lessons from local government in England. Cities Heal. 2018, 1, 185–193. [Google Scholar] [CrossRef]
| N (Unweighted) | Men | Women | All | |
|---|---|---|---|---|
| 10,236 | 13,811 | 24,047 | ||
| Demographic | ||||
| Age in years a | 50.5 (50.2–50.8) | 50.6 (50.2–51.0) | 50.3 (50.0–50.7) | |
| 18–35 years | 22.2 | 23.5 | 22.9 | |
| 36–50 years | 29.7 | 30.8 | 30.3 | |
| Over 50 years | 48.1 | 45.7 | 46.8 | |
| Socioeconomic | ||||
| Education | None | 14.7 | 20.5 | 17.9 |
| GCSE or equivalent (≤11 years) | 28.2 | 32.88 | 30.8 | |
| A-level (12–13 years) | 19.2 | 13.7 | 16.2 | |
| Vocational qualifications (12–13 years) | 10.3 | 12.8 | 11.7 | |
| Degree (>13 years) | 27.4 | 20.0 | 23.3 | |
| Missing | 0.40 | 0.28 | 0.35 | |
| Equivalised household Income | <£14,999 | 44.4 | 36.2 | 40.7 |
| £15,000–£24,999 | 28.2 | 28.9 | 29.1 | |
| £25,000–£34,999 | 13.9 | 16.3 | 15.0 | |
| £35,000–£49,999 | 7.81 | 10.9 | 9.26 | |
| £50,000+ | 4.49 | 7.23 | 5.74 | |
| Missing | 0.17 | 0.27 | 0.22 | |
| Density of AFH food establishments | ||||
| Restaurant to all other | 29.1 (28.6–29.5) | 28.5 (28.1–29.0) | 28.8 (28.4–29.1) | |
| Fast food to all other | 22.3 (22.0–22.7) | 22.7 (22.4–23.1) | 22.6 (22.3–22.9) | |
| Cafe to all other | 8.39 (8.16–8.61) | 8.14 (7.93–8.36) | 8.25 (8.07–8.44) | |
| Total AFH establishments to all other | 59.8 (59.4–60.3) | 59.5 (59.1–60.0) | 59.6 (59.3–60.0) | |
| Household food Spend | ||||
| Total Equivalised food spend/mo. a | £209 (207–211) | £200 (198–202) | £204 (203–206) | |
| Percent AFH food spend/mo. a | 19.4 (19.1–19.8) | 16.1 (15.8–16.4) | 17.6 (17.4–17.9) |
| Quintile of % Away from Home Food Outlet Exposure | |||||||
|---|---|---|---|---|---|---|---|
| Q1 = Lowest | Q2 | Q3 | Q4 | Q5 = Highest | All | ||
| N (unweighted) | 5177 | 4785 | 4871 | 4697 | 4517 | 24,047 | |
| Density of AFH establishments (min–max) | 0–0.50 | 0.50–0.57 | 0.57–0.63 | 0.63–0.69 | 0.69–1 | 0–1 | |
| Demographic | |||||||
| Age in years a | 52.1 (51.4–52.7) | 50.2 (49.5–50.9) | 50.2 (49.6–50.9) | 50.2 (49.5–50.9) | 49.8 (49.0–50.5) | 50.5 (50.2–50.8) | |
| 18–35 years | 19.8 | 22.5 | 22.9 | 24.7 | 24.9 | 22.9 | |
| 36–50 years | 29.6 | 32.1 | 31.2 | 29.4 | 29.4 | 30.3 | |
| Over 50 years | 50.7 | 45.5 | 45.9 | 45.9 | 45.7 | 46.8 | |
| Sex (% Male) | 44.1 | 45.2 | 44.5 | 46.3 | 47.3 | 45.5 | |
| Socioeconomic | |||||||
| Education | None | 19.4 | 19.6 | 19.6 | 17.0 | 14.1 | 17.9 |
| GCSE or equivalent (≤11 yrs) | 33.8 | 31.8 | 31.2 | 30.9 | 25.9 | 30.8 | |
| A-level (12–13 yrs) | 16.2 | 16.8 | 16.2 | 15.7 | 16.4 | 16.2 | |
| Vocational qualifications (12–13 yrs) | 12.3 | 11.4 | 11.2 | 11.0 | 12.5 | 11.7 | |
| Degree (>13 yrs) | 18.1 | 20.3 | 21.8 | 25.3 | 31.1 | 23.3 | |
| Income | <£14,999 | 42.5 | 44.8 | 41.1 | 38.3 | 37.2 | 40.7 |
| £15,000–£24,999 | 30.2 | 28.5 | 29.7 | 29.3 | 27.6 | 29.1 | |
| £25,000–£34,999 | 14.2 | 14.3 | 15.0 | 15.9 | 15.7 | 15.0 | |
| £35,000–£49,999 | 8.28 | 8.30 | 8.80 | 10.2 | 10.6 | 9.26 | |
| £50,000+ | 4.61 | 4.11 | 5.07 | 5.14 | 8.63 | 5.74 | |
| Household food spend | |||||||
| Total Equivalised food spend/mo. a | £207 (198–204) | £196 (193–199) | £201 (198–204) | £206 (202–209) | £217 (213–221) | £204 (203–206) | |
| Percent AFH food spend/mo. a | 15.9 (15.4–16.5) | 16.5 (15.9–17.7) | 17.8 (17.2–18.4) | 18.3 (17.7–18.9) | 19.5 (18.8–20.1) | 17.6 (17.4–17.8) | |
| Proportion of Food Outlet Density | Odds of High Monthly % Away from Home Food Spend 1 | ||
|---|---|---|---|
| Model 0 | Model 1 2 | Model 2 3 | |
| Away from home | |||
| Q1 | 1.00 (-) | 1.00 (-) | 1.00 (-) |
| Q2 | 0.99 [0.90, 1.10] | 0.97 [0.87, 1.07] | 0.96 [0.86, 1.06] |
| Q3 | 1.18 *** [1.07, 1.30] | 1.12 * [1.02, 1.24] | 1.09 [0.99, 1.21] |
| Q4 | 1.30 *** [1.18, 1.43] | 1.20 *** [1.08, 1.33] | 1.13 * [1.02, 1.25] |
| Q5 | 1.52 *** [1.37, 1.68] | 1.26 *** [1.13, 1.41] | 1.16 ** [1.04, 1.30] |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Penney, T.L.; Burgoine, T.; Monsivais, P. Relative Density of Away from Home Food Establishments and Food Spend for 24,047 Households in England: A Cross-Sectional Study. Int. J. Environ. Res. Public Health 2018, 15, 2821. https://doi.org/10.3390/ijerph15122821
Penney TL, Burgoine T, Monsivais P. Relative Density of Away from Home Food Establishments and Food Spend for 24,047 Households in England: A Cross-Sectional Study. International Journal of Environmental Research and Public Health. 2018; 15(12):2821. https://doi.org/10.3390/ijerph15122821
Chicago/Turabian StylePenney, Tarra L., Thomas Burgoine, and Pablo Monsivais. 2018. "Relative Density of Away from Home Food Establishments and Food Spend for 24,047 Households in England: A Cross-Sectional Study" International Journal of Environmental Research and Public Health 15, no. 12: 2821. https://doi.org/10.3390/ijerph15122821
APA StylePenney, T. L., Burgoine, T., & Monsivais, P. (2018). Relative Density of Away from Home Food Establishments and Food Spend for 24,047 Households in England: A Cross-Sectional Study. International Journal of Environmental Research and Public Health, 15(12), 2821. https://doi.org/10.3390/ijerph15122821





