New Burnout Evaluation Model Based on the Brief Burnout Questionnaire: Psychometric Properties for Nursing
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Instruments
2.3. Procedure
2.4. Data Analysis
3. Results
3.1. Preliminary Analyses
3.2. Exploratory Factor Analysis of the Original CBB Model
3.3. Exploratory Factor Analysis of Revised CBB Model (CBB-R)
3.4. Confirmatory Factor Analysis of CBB Model and CBB-R Model
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- National Statistics Institute. España en Cifras; INE: Madrid, Spain, 2017.
- Profesionales Sanitarios Colegiados 2016. Available online: http://www.ine.es/jaxi/Datos.htm?path=/t15/p416/a2016/l0/&file=s08004.px (accessed on 15 August 2018).
- González-Cabanach, R.; Souto-Gestal, A.; Fernández-Cervantes, R. Emotion regulation profiles and academic stress in Physiotherapy students. Eur. J. Educ. Psychol. 2017, 10, 57–67. [Google Scholar] [CrossRef]
- Zhou, J.; Yang, Y.; Qiu, X.; Pan, H.; Ban, B.; Qiao, Z.; Wang, L.; Wang, W. Serial multiple mediation of organizational commitment and job burnout in the relationship between psychological capital and anxiety in Chinese female nurses: A cross-sectional questionnaire survey. Int. J. Nurs. Stud. 2018, 83, 75–82. [Google Scholar] [CrossRef] [PubMed]
- García-Camapayo, J.; Puebla-Guedea, M.; Herrera-Mercadal, P.; Daudén, E. Burnout Syndrome and Demotivation among Health Care Personnel. Managing Stressful Situations: The Importance of Teamwork. Actas Dermosifiliogr. 2016, 107, 400–406. [Google Scholar] [CrossRef]
- Maslach, C. Burnout. In Encyclopedia of Mental Health, 2nd ed.; Friedman, H., Ed.; Elsevier: Oxford, UK, 2016; pp. 222–227. ISBN 978-0-12-397045-9. [Google Scholar]
- Gómez, L.; Estrella, D. Síndrome de Burnout: Una revisión breve. Ciencia Humanismo Salud 2015, 2, 116–122. [Google Scholar]
- De Francisco, C.; Arce, C.; Vílchez, M.P.; Vales, A. Antecedents and consequences of burnout in athletes: Perceived stress and depression. Int. J. Clin. Health Psychol. 2016, 16, 221–314. [Google Scholar] [CrossRef]
- Pérez-Fuentes, M.C.; Gázquez, J.J.; Ruiz, M.D.; Molero, M.M. Inventory of Overburden in Alzheimer’s Patient Family Caregivers with no Specialized Training. Int. J. Clin. Health Psychol. 2017, 17, 56–64. [Google Scholar] [CrossRef] [PubMed]
- Martos, Á.; Pérez-Fuentes, M.C.; Molero, M.M.; Gázquez, J.J.; Simón, M.M.; Barragán, A.B. Burnout y engagement en estudiantes de Ciencias de la Salud. Eur. J Investig. 2018, 8, 23–36. [Google Scholar] [CrossRef]
- Jodas, D.A.; Nesello, F.; Eumann, A.; Durán, A.; Lopez, F.; de Andrade, S.M. Physical, psychological and occupational consequences of job burnout: A systematic review of prospective studies. PLoS ONE 2017, 12, e0185781. [Google Scholar] [CrossRef]
- Iorga, M.; Socolov, V.; Muraru, D.; Dirtu, C.; Soponaru, C.; Ilea, C.; Socolov, D.G. Factors Influencing Burnout Syndrome in Obstetrics and Gynecology Physicians. BioMed Res. Int. 2017, 2017, 1–10. [Google Scholar] [CrossRef]
- Schneider, A.; Weigl, M. Associations between psychosocial work factors and provider mental well-being in emergency departments: A systematic review. PLoS ONE 2018, 13, e0197375. [Google Scholar] [CrossRef]
- Frenet, C.; Trépanier, S.G.; Demers, M.; Austin, S. Motivational pathways of occupational and organizational turnover intention among newly registered nurses in Canada. Nurs. Outlook 2017, 65, 444–454. [Google Scholar] [CrossRef]
- Obradovic, Z.; Obradovic, A.; Cesir-Skoro, I. Nurses and burnout síndrome. J. Health Biol. 2013, 3, 60–64. [Google Scholar]
- Basinska, B.A.; Wilczek-Ruzyczka, E. The role of rewards and demansd in burnout among surgical nurses. Int. J. Occup. Med. Environ. Health 2013, 26, 593–604. [Google Scholar] [CrossRef]
- Pucheu, A. ¿Existen diferencias en la motivación de distintas generaciones en enfermería? Rev. Méd. Clín. Las Condes 2018, 29, 336–342. [Google Scholar] [CrossRef]
- Achour, N.; Munokaran, S.; Barker, F.; Soetanto, R. Staff Stress: The Sleeping Cell of Healthcare Failure. Procedia Eng. 2018, 212, 459–466. [Google Scholar] [CrossRef]
- Contreras, F.; Espinal, L.; Pachón, A.M.; González, J. Burnout, liderazgo y satisfacción laboral en el personal asistencial de un hospital de tercer nivel en Bogotá. Perspect. Psicol. 2013, 9, 65–80. [Google Scholar] [CrossRef]
- Dill, J.; Erickson, R.J.; Diefendorff, J.M. Motivation in caring labor: Implications for the well-being and employment outcomes of nurses. Soc. Sci. Med. 2016, 167, 99–106. [Google Scholar] [CrossRef]
- Kabir, M.N.; Parvin, M.M. Factors affecting employee job satisfaction of pharmaceutical sector. Aust. J. Bus. Manag. Res. 2011, 1, 113–123. [Google Scholar]
- Elbarazi, I.; Loney, T.; Yousef, S.; Elias, A. Prevalence of and factors associated with burnout among health care professionals in Arab countries: A systematic review. BMC Health Serv. Res. 2017, 17, 1–10. [Google Scholar] [CrossRef]
- Van Bogaert, P.; Van Heusden, D.; Verspuy, M.; Wouters, K.; Slootmans, S.; Van der Straeten, J.; Aken, V.; White, M. The Productive Ward Program™: A Two-Year Implementation Impact Review Using a Longitudinal Multilevel Study. Can. J. Nurs. Res. 2017, 49, 28–38. [Google Scholar] [CrossRef]
- Farnaz, R.; Kalateh, A.; Hemmati, S.; Ebrahimzade, N.; Sarikhani, Y.; Heydari, S.T.; Lankarani, K.B. The impact of environmental and demographic factors on nursing job satisfaction. Electron. Phys. 2018, 10, 6712–6717. [Google Scholar] [CrossRef]
- Molero, M.M.; Pérez-Fuentes, M.C.; Gázquez, J.J.; Simón, M.M.; Martos, Á. Burnout Risk and Protection Factors in Certified Nursing Aides. Int. J. Environ. Res. Public Health 2018, 15, 1116. [Google Scholar] [CrossRef] [PubMed]
- Mudallal, R.H.; Othman, W.M.; Al Hassan, N.F. Nurses’ Burnout: The Influence of Leader Empowering Behaviors, Work Conditions, and Demographic Traits. Inquiry 2017, 54, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Wei, H.; Sewell, K.A.; Woody, G.; Rose, M.A. The state of the science of nurse work environments in the United States: A systematic review. Int. J. Nurs. Sci. 2018, 5, 1–14. [Google Scholar] [CrossRef]
- Pérez-Fuentes, M.C.; Molero, M.M.; Gázquez, J.J.; Oropesa, N.F. The Role of Emotional Intelligence in Engagement in Nurses. Int. J. Environ. Res. Public Health 2018, 15, 1915. [Google Scholar] [CrossRef]
- Maslach, C.; Jackson, S.E. Maslach Burnout Inventory; Consulting Psychologists Press: Palo Alto, CA, USA, 1981. [Google Scholar]
- Squieres, A.; Finlayson, C.; Gerchow, L.; Cimiotti, J.P.; Matthews, A.; Schwendimann, R.; Griffiths, P.; Busse, R.; Heinen, M.; Brzostek, T.; et al. Methodological considerations when translating “burnout”. Burn Res. 2014, 1, 59–68. [Google Scholar] [CrossRef] [PubMed]
- Martins, S.; Teixera, C.M.; Carvalho, A.S.; Hernández-Marrero, P. Compared to Palliative Care, Working in Intensive Care More than Doubles the Chances of Burnout: Results from a Nationwide Comparative Study. PLoS ONE 2016, 11, e0162340. [Google Scholar] [CrossRef]
- Merlani, P.; Verdon, M.; Businger, A.; Domenighetti, G.; Pargger, H.; Ricou, B. Burnout in ICU Caregivers: A Multicenter Study of Factors Associated to Centers. Am. J. Respir. Crit. 2011, 184, 1140–1146. [Google Scholar] [CrossRef]
- Poncet, M.C.; Toullic, P.; Papazian, L.; Barnes, N.K.; Timsit, J.F.; Pochard, F.; Chevret, S.; Schlemmer, B.; Azoulay, E. Burnout Syndrome in Critical Care Nursing Staff. Am. J. Respir. Crit. 2007, 175, 698–704. [Google Scholar] [CrossRef]
- Guerra, C.; Mújica, A.; Nahmias, A.; Rojas, N. Análisis psicométrico de la escala de conductas de autocuidado para psicólogos clínicos. Rev. Latinoam. Psicol. 2011, 43, 319–328. [Google Scholar] [CrossRef]
- Moreno, B.; Gálvez, M.; Garrosa, E.; Mingote, J.C. Nuevos planteamientos en la evaluación del burnout. La evaluación específica del desgaste profesional médico. Aten Prim. 2006, 38, 544–549. [Google Scholar] [CrossRef]
- Pisanti, R.; Lombardo, C.; Lucidi, F.; Violani, C.; Lazzari, D. Psychometric properties of the Maslach Burnout Inventory for Human Services among Italian nurses: A test of alternative models. J. Adv. Nurs. 2013, 69, 697–707. [Google Scholar] [CrossRef] [PubMed]
- Kalliath, T.J.; O´Driscoll, M.P.; Gillespie, D.F.; Bluedorn, A.C. A test of the Maslach Burnout Inventory in three samples of healthcare professionals. Work Stress 2000, 14, 35–50. [Google Scholar] [CrossRef]
- Kim, H.; Ji, J. Factor structure and longitudinal invariance of the Maslach Burnout Inventory. Res. Soc. Work Pract. 2009, 19, 325–339. [Google Scholar] [CrossRef]
- Densten, I.L. Re-thinking burnout. J. Organ. Behav. 2001, 22, 833–847. [Google Scholar] [CrossRef]
- García, J.M.; Herrero, S.; León, J.L. Validez factorial del Maslach Burnout Inventory (MBI) en una muestra de trabajadores del Hospital Psiquiátrico Penitenciario de Sevilla. Apuntes Psicol. 2007, 25, 157–174. [Google Scholar]
- Moreno-Jiménez, B.; Bustos, R.; Matallana, A.; Miralles, T. La evaluación del burnout. Problemas y alternativas. El CBB como evaluación de los elementos del proceso. Rev. Psicol. Trabajo Organ. 1997, 13, 185–207. [Google Scholar]
- Mingote, J.C.; Moreno, B.; Gálvez, M. Desgaste profesional y salud de los profesionales médicos: Revisión y propuestas de prevención. Med. Clínica 2004, 123, 265–270. [Google Scholar] [CrossRef]
- Blanco-Álvarez, T.M.; Thoen, M.A. Factores asociados al estrés laboral en policías penitenciarios costarricenses. Rev. Costarric. Psicol. 2017, 36, 45–59. [Google Scholar] [CrossRef]
- Correa-Correa, Z.; Muñoz-Zambrano, I.; Chaparro, A.F. Síndrome de Burnout en docentes de dos universidades de Popayán, Colombia. Rev. Salud Pública 2010, 12, 589–598. [Google Scholar] [CrossRef]
- Roger, M.C.; Abalo, J.G.; Pérez, C.M.; Ochoa, I.I.; Abalo, R.G.; Abalo, Y. El control of burnout syndrome de desgaste professional o burnout en enfermeria oncológica: Una experiencia de intervención. Terapia Psicol. 2006, 24, 39–53. [Google Scholar]
- Ahola, K.; Toppinen-Tanner, S.; Seppänen, J. Interventions to alleviate burnout symptoms and to support return to work among employees with burnout: Systematic review and meta-analysis. Burn Res. 2017, 4, 1–11. [Google Scholar] [CrossRef]
- González-Ramírez, M.T.; Landero, R.; Moral de la Rubia, J.M. Cuestionario de Burnout para amas de casa (CUBAC): Evaluación de sus propiedades psicométricas y del Modelo Secuencial de Burnout. Univ. Psychol. 2009, 8, 533–544. [Google Scholar]
- Montero, J.; García-Campayo, J.; Andrés, E. Validez factorial de la estructura del Cuestionario Breve de Burnout (CBB) en una muestra de docentes en Aragón. Rev. Psicopatol. Psicol. Clin. 2009, 14, 123–132. [Google Scholar] [CrossRef]
- Domínguez-Lara, S.; Fernández-Arata, M. Cuestionario breve de Burnout, ¿una elección adecuada? Enferm Clín. 2018, 28, 214–215. [Google Scholar] [CrossRef] [PubMed]
- Domínguez-Lara, S.A. Análisis factorial y confiabilidad del Burnout Screening Inventory. Educ. Méd. 2017, 19, 125–130. [Google Scholar] [CrossRef]
- Pérez-Fuentes, M.C.; Molero, M.M.; Martos, A.; Barragán, A.B.; Gázquez, J.J.; Sánchez-Marchán, C. Spanish analysis and validation of Peer Conflict Scale. Eur. J. Educ. Psychol. 2016, 9, 56–62. [Google Scholar] [CrossRef]
- Álvarez-García, D.; Barreiro-Collazo, A.; Núñez, J.C.; Dobarro, A. Validity and reliability of the Cyber-aggression Questionnaire for Adolescents (CYBA). Eur. J. Psychol. Appl. Legal Context 2017, 8, 69–77. [Google Scholar] [CrossRef]
- Bentler, P.M. EQS Structural Equations Program Manual; BMDP Statistical Software: Los Angeles, CA, USA, 1989. [Google Scholar]
- Hair, J.F.; Black, W.C.; Babin, B.J.; Anderson, R.E.; Tatham, R.L. Multivariate Data Analysis, 7th ed.; Pearson Prentice Hall: Upper Saddle River, NJ, USA, 2006. [Google Scholar]
- Akaike, H. A new look at the statistical model identification. IEEE Trans. Autom. Control 1974, 19, 716–723. [Google Scholar] [CrossRef]
- Cronbach, L.J. Coefficient alpha and the internal structure of tests. Psychometrika 1951, 16, 297–334. [Google Scholar] [CrossRef]
- Byrne, B.M.; Stewart, S.M. The MACS approach to testing for multigroup invariance of a second-order structure: A walk through the process. Struct. Equ. Models 2006, 13, 287–321. [Google Scholar] [CrossRef]
- Cheung, G.W.; Rensvold, R.B. Evaluating goodness-of-fit indexes for testing measurement invariance. Struct. Equ. Models 2002, 9, 233–255. [Google Scholar] [CrossRef]
- Finney, S.J.; DiStefano, C. Non-normal and categorical data in structural equation modeling. In Structural Equation Modeling: A Second Course; Hancock, G.R., Mueller, R.O., Eds.; Information Age: Greenwich, CT, USA, 2006; pp. 269–314. [Google Scholar]
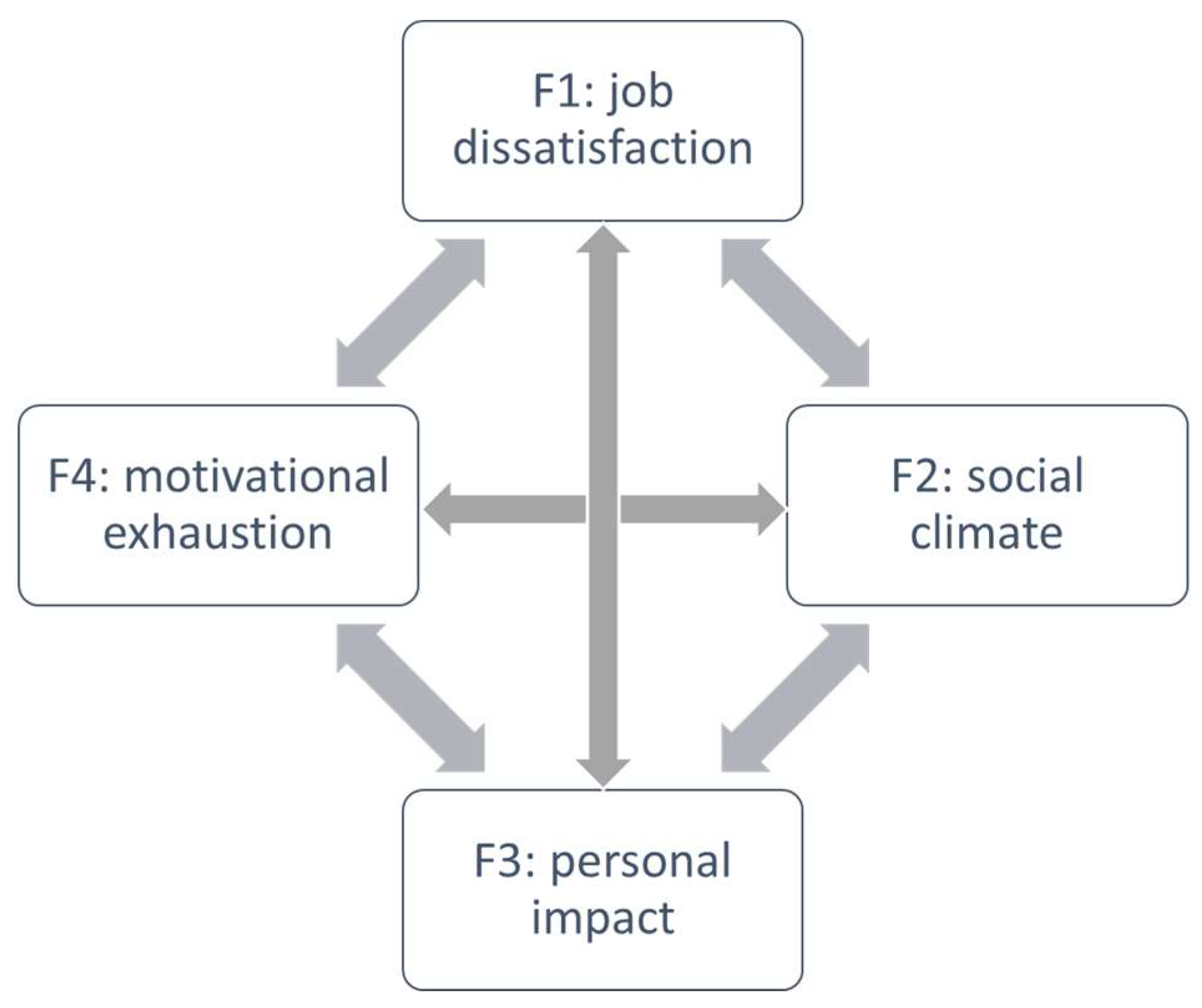
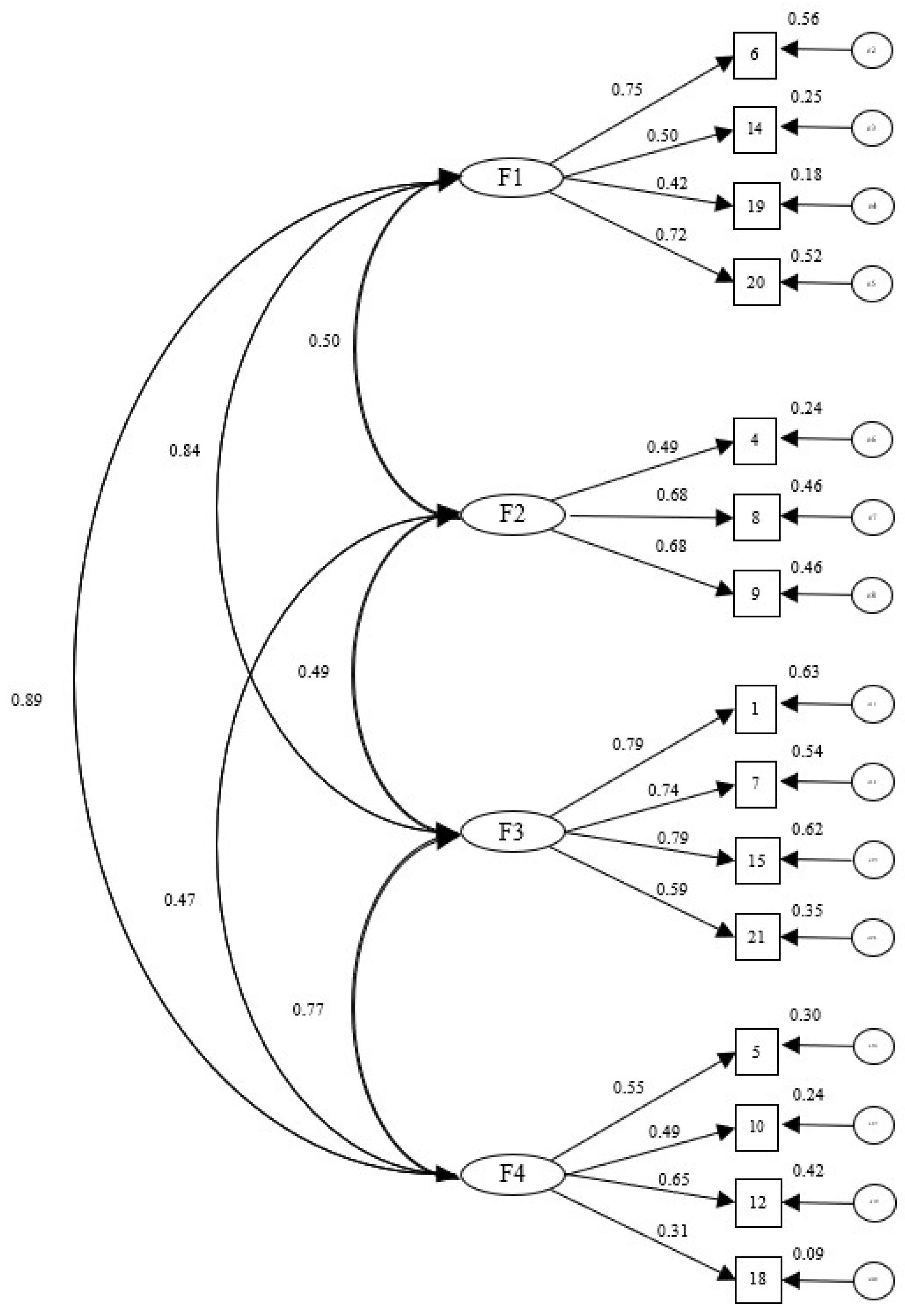
| Principal component analysis | F1 | F2 | h2 |
|---|---|---|---|
| Item 2 | 0.56 | 0.63 | 0.53 |
| Item 4 | 0.65 | 0.42 | |
| Item 6 | 0.79 | 0.63 | |
| Item 8 | 0.81 | 0.66 | |
| Item 9 | 0.79 | 0.62 | |
| Item 10 | 0.55 | 0.31 | |
| Item 14 | 0.68 | 0.48 | |
| Item 16 | 0.78 | 0.63 | |
| Item 20 | 0.80 | 0.64 | |
| Eigenvalue | 3.56 | 1.37 | |
| Percentage explained variance | 39.51 | 15.22 | 54.73 |
| Kaiser–Meyer–Olkin | 0.85 | ||
| Barlett’s sphericity | χ2(36) = 3019.35, p < 0.000 | ||
| Cronbach’s alpha | 0.75 | 0.73 | 0.79 |
| Principal component analysis | F1 | F2 | F3 | h2 |
|---|---|---|---|---|
| Item 1 | 0.76 | 0.68 | ||
| Item 3 | 0.72 | 0.58 | ||
| Item 5 | 0.49 | 0.27 | ||
| Item 7 | 0.60 | 0.48 | ||
| Item 11 | 0.44 | 0.37 | ||
| Item 12 | 0.50 | 0.33 | ||
| Item 15 | 0.72 | 0.66 | ||
| Item 18 | 0.28 | 0.11 | ||
| Item 19 | 0.30 | 0.17 | ||
| Eigenvalue | 3.38 | 0.98 | 0.96 | |
| Percentage explained variance | 31.93 | 4.99 | 3.74 | 40.66 |
| Kaiser–Meyer–Olkin | 0.84 | |||
| Barlett’s sphericity | χ2(36) = 2569.33, p < 0.000 | |||
| Cronbach’s alpha | 0.81 | 0.49 | 0.57 | 0.76 |
| Principal component analysis | F1 | F2 | F3 | F4 | h2 |
|---|---|---|---|---|---|
| Item 1 | 0.56 | 0.41 | 0.65 | 0.61 | |
| Item 2 | 0.59 | 0.58 | 0.55 | ||
| Item 3 | 0.62 | 0.45 | 0.49 | ||
| Item 4 | 0.65 | 0.43 | |||
| Item 5 | 0.43 | 0.57 | 0.41 | ||
| Item 6 | 0.70 | 0.56 | 0.64 | ||
| Item 7 | 0.44 | 0.62 | 0.51 | ||
| Item 8 | 0.80 | 0.66 | |||
| Item 9 | 0.78 | 0.62 | |||
| Item 10 | 0.61 | 0.38 | |||
| Item 11 | 0.40 | 0.67 | 0.51 | ||
| Item 12 | 0.44 | 0.62 | 0.47 | ||
| Item 13 | 0.78 | 0.62 | |||
| Item 14 | 0.56 | 0.41 | 0.40 | ||
| Item 15 | 0.56 | 0.70 | 0.66 | ||
| Item 16 | 0.77 | 0.41 | 0.64 | ||
| Item 17 | 0.66 | 0.47 | |||
| Item 18 | 0.53 | 0.30 | |||
| Item 19 | 0.66 | 0.44 | |||
| Item 20 | 0.76 | 0.64 | |||
| Item 21 | 0.62 | 0.46 | |||
| Eigenvalue | 6.67 | 1.76 | 1.39 | 1.06 | |
| Percentage explained variance | 31.77 | 8.41 | 6.64 | 5.05 | 51.86 |
| Kaiser–Meyer–Olkin | 0.92 | ||||
| Barlett’s sphericity | χ2(210) = 8449.54, p < 0.000 | ||||
| Cronbach’s alpha | 0.74 | 0.75 | 0.82 | 0.59 | 0.88 |
| Model | χ2 (df) | χ2/df | CFI | TLI | RMR | Est. | RMSEA | |
|---|---|---|---|---|---|---|---|---|
| CI 90% | ||||||||
| Bel. | Abv. | |||||||
| Original CBB model | 931.446 (179) | 5.204 | 0.822 | 0.791 | 0.042 | 0.083 | 0.078 | 0.089 |
| Unidimensional CBB model | 1305.043 (189) | 6.904 | 0.735 | 0.706 | 0.059 | 0.099 | 0.094 | 0.104 |
| Proposed CBB model | 664.676 (183) | 3.632 | 0.886 | 0.869 | 0.044 | 0.066 | 0.061 | 0.071 |
| Proposed CBB-R model | 176.497 (84) | 2.101 | 0.965 | 0.956 | 0.027 | 0.043 | 0.034 | 0.052 |
| Model | χ2 | gl | χ2/gl | Δχ2 | CFI | ΔCFI | IFI | RMSEA (CI 90%) |
|---|---|---|---|---|---|---|---|---|
| M0a (permanent) | 376.265 (p = 0.000) | 168 | 2.239 | 0.960 | 0.961 | 0.032 (0.027–0.036) | ||
| M0b (temporary) | 417.761 (p = 0.000) | 179 | 2.333 | 0.955 | 0.955 | 0.033 (0.029–0.037) | ||
| M1 (base model set) | 505.309 (p = 0.000) | 194 | 2.604 | 0.941 | 0.941 | 0.036 (0.032–0.040) | ||
| M2 (FS) | 544.696 (p = 0.000) | 209 | 2.606 | 39.387 | 0.936 | 0.005 | 0.936 | 0.036 (0.032–0.040) |
| M3 (FS + Int) | 376.265 (p = 0.000) | 168 | 2.239 | 129.044 | 0.960 | 0.024 | 0.961 | 0.032 (0.027–0.036) |
| M4 (FS + Int + Err) | 376.265 (p = 0.000) | 168 | 2.239 | 129.044 | 0.960 | 0.024 | 0.961 | 0.032 (0.027–0.036) |
| M0a (male) | 383.819 (p = 0.000) | 168 | 2.284 | 0.959 | 0.960 | 0.032 (0.028–0.037) | ||
| M0b (female) | 407.567 (p = 0.000) | 179 | 2.276 | 0.957 | 0.957 | 0.032 (0.028–0.036) | ||
| M1 (base model set) | 446.771 (p = 0.000) | 194 | 2.302 | 0.952 | 0.953 | 0.032 (0.029–0.036) | ||
| M2 (FS) | 474.727 (p = 0.000) | 209 | 2.271 | 27.956 | 0.950 | 0.002 | 0.950 | 0.032 (0.028–0.036) |
| M3 (FS + Int) | 383.819 (p = 0.000) | 168 | 2.284 | 62.952 | 0.959 | 0.009 | 0.960 | 0.032 (0.028–0.037) |
| M4 (FS + Int + Err) | 376.265 (p = 0.000) | 168 | 2.284 | 62.952 | 0.959 | 0.009 | 0.960 | 0.032 (0.028–0.037) |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pérez-Fuentes, M.d.C.; Molero Jurado, M.d.M.; Martos Martínez, Á.; Gázquez Linares, J.J. New Burnout Evaluation Model Based on the Brief Burnout Questionnaire: Psychometric Properties for Nursing. Int. J. Environ. Res. Public Health 2018, 15, 2718. https://doi.org/10.3390/ijerph15122718
Pérez-Fuentes MdC, Molero Jurado MdM, Martos Martínez Á, Gázquez Linares JJ. New Burnout Evaluation Model Based on the Brief Burnout Questionnaire: Psychometric Properties for Nursing. International Journal of Environmental Research and Public Health. 2018; 15(12):2718. https://doi.org/10.3390/ijerph15122718
Chicago/Turabian StylePérez-Fuentes, María del Carmen, María del Mar Molero Jurado, África Martos Martínez, and José Jesús Gázquez Linares. 2018. "New Burnout Evaluation Model Based on the Brief Burnout Questionnaire: Psychometric Properties for Nursing" International Journal of Environmental Research and Public Health 15, no. 12: 2718. https://doi.org/10.3390/ijerph15122718
APA StylePérez-Fuentes, M. d. C., Molero Jurado, M. d. M., Martos Martínez, Á., & Gázquez Linares, J. J. (2018). New Burnout Evaluation Model Based on the Brief Burnout Questionnaire: Psychometric Properties for Nursing. International Journal of Environmental Research and Public Health, 15(12), 2718. https://doi.org/10.3390/ijerph15122718








