The Association between Migraine and Types of Sleep Disorder
Abstract
1. Introduction
2. Methods
2.1. Study Population
2.2. Variables
2.3. Ethical Consideration
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusion
Author Contributions
Funding
Conflicts of Interest
References
- Natoli, J.; Manack, A.; Dean, B.; Butler, Q.; Turkel, C.; Stovner, L.; Lipton, R. Global prevalence of chronic migraine: A systematic review. Cephalalgia 2010, 30, 599–609. [Google Scholar] [CrossRef] [PubMed]
- Silberstein, S.D.; Lipton, R.B.; Sliwinski, M. Classification of daily and near-daily headaches field trial of revised IHS criteria. Neurology 1996, 47, 871–875. [Google Scholar] [CrossRef] [PubMed]
- Katsarava, Z.; Manack, A.; Yoon, M.; Obermann, M.; Becker, H.; Dommes, P.; Turkel, C.; Lipton, R.; Diener, H. Chronic migraine: Classification and comparisons. Cephalalgia 2011, 31, 520–529. [Google Scholar] [CrossRef] [PubMed]
- Headache Classification Committee Of The International Headache Society (HIS). The international classification of headache disorders, (beta version). Cephalalgia 2013, 33, 629–808. [Google Scholar] [CrossRef] [PubMed]
- Silberstein, S.D. Migraine symptoms: Results of a survey of self-reported migraineurs. J. Head Face Pain 1995, 35, 387–396. [Google Scholar] [CrossRef]
- Lipton, R.B.; Stewart, W.F.; Diamond, S.; Diamond, M.L.; Reed, M. Prevalence and burden of migraine in the United States: Data from the American migraine study II. J. Head Face Pain 2001, 41, 646–657. [Google Scholar] [CrossRef]
- Bigal, M.; Rapoport, A.; Sheftell, F.; Tepper, S.; Lipton, R. Transformed migraine and medication overuse in a tertiary headache centre—Clinical characteristics and treatment outcomes. Cephalalgia 2004, 24, 483–490. [Google Scholar] [CrossRef] [PubMed]
- Limmroth, V.; Katsarava, Z.; Fritsche, G.; Przywara, S.; Diener, H.-C. Features of medication overuse headache following overuse of different acute headache drugs. Neurology 2002, 59, 1011–1014. [Google Scholar] [CrossRef] [PubMed]
- Breslau, N.; Davis, G.C.; Schultz, L.R.; Paterson, E.L. Migraine and major depression: A longitudinal study. J. Head Face Pain 1994, 34, 387–393. [Google Scholar] [CrossRef]
- Lipton, R.B.; Hamelsky, S.W.; Kolodner, K.B.; Steiner, T.; Stewart, W.F. Migraine, quality of life, and depression a population-based case-control study. Neurology 2000, 55, 629–635. [Google Scholar] [CrossRef] [PubMed]
- National Health Insurance Service. Statistics for diseases: Migraine; National Health Insurance Service: Seoul, South Korea, 2018. [Google Scholar]
- Bigal, M.E.; Lipton, R.B. Modifiable risk factors for migraine progression. J. Head Face Pain 2006, 46, 1334–1343. [Google Scholar] [CrossRef] [PubMed]
- Lipton, R.B.; Bigal, M.E. Migraine: Epidemiology, impact, and risk factors for progression. J. Head Face Pain 2005, 45, S3–S13. [Google Scholar] [CrossRef] [PubMed]
- Breslau, N.; Rasmussen, B.K. The impact of migraine epidemiology, risk factors, and co-morbidities. Neurology 2001, 56, S4–S12. [Google Scholar] [CrossRef] [PubMed]
- Fuh, J.-L.; Wang, S.-J.; Lu, S.-R.; Juang, K.-D. Does medication overuse headache represent a behavior of dependence? Pain 2005, 119, 49–55. [Google Scholar] [CrossRef] [PubMed]
- Altevogt, B.M.; Colten, H.R. Sleep Disorders and Sleep Deprivation: An Unmet Public Health Problem; National Academies Press: Washington, DC, USA, 2006. [Google Scholar]
- Buysse, D.J. Sleep health: Can we define it? Does it matter? Sleep 2014, 37, 9–17. [Google Scholar] [CrossRef] [PubMed]
- Park, H.J.; Kim, M.S.; Park, E.-C.; Jang, S.-Y.; Kim, W.; Han, K.-T. Association between sleep disorder and panic disorder in South Korea: Nationwide nested case-control study of data from 2004 to 2013. Psychiatry Res. 2018, 260, 286–291. [Google Scholar] [CrossRef] [PubMed]
- Han, K.-T.; Kim, W.; Kim, S.J.; Jang, S.-Y.; Ju, Y.J.; Chun, S.Y.; Lee, S.G.; Park, E.-C. Sleep disorders and risk of hospitalization in patients with mood disorders: Analysis of the national sample cohort over 10 years. Psychiatry Res. 2016, 245, 259–266. [Google Scholar] [CrossRef] [PubMed]
- OECD. Society at a Glance 2009: Oecd Indicaters; OECD Publishing: Paris, Franch, 2009. [Google Scholar]
- Buysse, D.J.; Reynolds III, C.F.; Monk, T.H.; Berman, S.R.; Kupfer, D.J. The pittsburgh sleep quality index: A new instrument for psychiatric practice and research. Psychiatry Res. 1989, 28, 193–213. [Google Scholar] [CrossRef]
- Rains, J.C.; Poceta, J.S. Headache and sleep disorders: Review and clinical implications for headache management. J. Head Face Pain 2006, 46, 1344–1363. [Google Scholar] [CrossRef] [PubMed]
- Breslau, N.; Roth, T.; Rosenthal, L.; Andreski, P. Sleep disturbance and psychiatric disorders: A longitudinal epidemiological study of young adults. Biol. Psy. 1996, 39, 411–418. [Google Scholar] [CrossRef]
- Thorpy, M.J. Classification of sleep disorders. Neurotherapeutics 2012, 9, 687–701. [Google Scholar] [CrossRef] [PubMed]
- National Health Insurance Service. Statistics for Diseases: Sleep Disorder; National Health Insurance Service: Seoul, South Korea, 2018. [Google Scholar]
- Wöber, C.; Holzhammer, J.; Zeitlhofer, J.; Wessely, P.; Wöber-Bingöl, Ç. Trigger factors of migraine and tension-type headache: Experience and knowledge of the patients. J. Head Face Pain 2006, 7, 188–195. [Google Scholar] [CrossRef] [PubMed]
- Peres, M.F.P.; Del Rio, M.S.; Seabra, M.; Tufik, S.; Abucham, J.; Cipolla-Neto, J.; Silberstein, S.; Zukerman, E. Hypothalamic involvement in chronic migraine. J. Neurol. Neurosurg. Psychiatry 2001, 71, 747–751. [Google Scholar] [CrossRef] [PubMed]
- Kelman, L.; Rains, J.C. Headache and sleep: Examination of sleep patterns and complaints in a large clinical sample of migraineurs. J. Head Face Pain 2005, 45, 904–910. [Google Scholar] [CrossRef] [PubMed]
- Barbanti, P.; Fabbrini, G.; Aurilia, C.; Vanacore, N.; Cruccu, G. A case-control study on excessive daytime sleepiness in episodic migraine. Cephalalgia 2007, 27, 1115–1119. [Google Scholar] [CrossRef] [PubMed]
- Lateef, T.; Swanson, S.; Cui, L.; Nelson, K.; Nakamura, E.; Merikangas, K. Headaches and sleep problems among adults in the united states: Findings from the national comorbidity survey–replication study. Cephalalgia 2011, 31, 648–653. [Google Scholar] [CrossRef] [PubMed]
- Luc, M.E.; Gupta, A.; Birnberg, J.M.; Reddick, D.; Kohrman, M.H. Characterization of symptoms of sleep disorders in children with headache. Pediatr. Neurol. 2006, 34, 7–12. [Google Scholar] [CrossRef] [PubMed]
- Lin, Y.-K.; Lin, G.-Y.; Lee, J.-T.; Lee, M.-S.; Tsai, C.-K.; Hsu, Y.-W.; Lin, Y.-Z.; Tsai, Y.-C.; Yang, F.-C. Associations between sleep quality and migraine frequency: A cross-sectional case-control study. Medicine 2016, 95. [Google Scholar] [CrossRef] [PubMed]
- Engstrøm, M.; Hagen, K.; Bjørk, M.; Stovner, L.; Sand, T. Sleep quality and arousal in migraine and tension-type headache: The headache-sleep study. Acta Neurol. Scand. 2014, 129, 47–54. [Google Scholar]
- Bigal, M.E.; Lipton, R.B.; Winner, P.; Reed, M.; Diamond, S.; Stewart, W.F.; Group, A.A. Migraine in adolescents association with socioeconomic status and family history. Neurology 2007, 69, 16–25. [Google Scholar] [CrossRef] [PubMed]
- Stewart, W.F.; Roy, J.; Lipton, R.B. Migraine prevalence, socioeconomic status, and social causation. Neurology 2013, 81, 948–955. [Google Scholar] [CrossRef] [PubMed]
- Sundararajan, V.; Henderson, T.; Perry, C.; Muggivan, A.; Quan, H.; Ghali, W.A. New ICD-10 version of the charlson comorbidity index predicted in-hospital mortality. J. Clin. Epidem. 2004, 57, 1288–1294. [Google Scholar] [CrossRef] [PubMed]
- Charlson, M.; Szatrowski, T.P.; Peterson, J.; Gold, J. Validation of a combined comorbidity index. J. Clin. Epidem. 1994, 47, 1245–1251. [Google Scholar] [CrossRef]
- Rasmussen, B.K. Migraine and tension-type headache in a general population: Precipitating factors, female hormones, sleep pattern and relation to lifestyle. Pain 1993, 53, 65–72. [Google Scholar] [CrossRef]
- Jeon, B.; Kwon, S. Effect of private health insurance on health care utilization in a universal public insurance system: A case of South Korea. Health Policy 2013, 113, 69–76. [Google Scholar] [CrossRef] [PubMed]
- Spiegel, K.; Leproult, R.; L’Hermite-Balériaux, M.; Copinschi, G.; Penev, P.D.; Van Cauter, E. Leptin levels are dependent on sleep duration: Relationships with sympathovagal balance, carbohydrate regulation, cortisol, and thyrotropin. J. Clin. Endocrinol. Metab. 2004, 89, 5762–5771. [Google Scholar] [CrossRef] [PubMed]
- Cappuccio, F.P.; D’Elia, L.; Strazzullo, P.; Miller, M.A. Sleep duration and all-cause mortality: A systematic review and meta-analysis of prospective studies. Sleep 2010, 33, 585–592. [Google Scholar] [CrossRef] [PubMed]
- Jang, Y.; Chiriboga, D.A.; Okazaki, S. Attitudes toward mental health services: Age-group differences in korean american adults. Aging Ment. Health 2009, 13, 127–134. [Google Scholar] [CrossRef] [PubMed]
- Strine, T.W.; Chapman, D.P. Associations of frequent sleep insufficiency with health-related quality of life and health behaviors. Sleep Med. 2005, 6, 23–27. [Google Scholar] [CrossRef] [PubMed]
| Variables | Total | Migraine | p-Value | ||||
|---|---|---|---|---|---|---|---|
| Diagnosed | None | ||||||
| N | % | N | % | N | % | ||
| Sleep disorder | |||||||
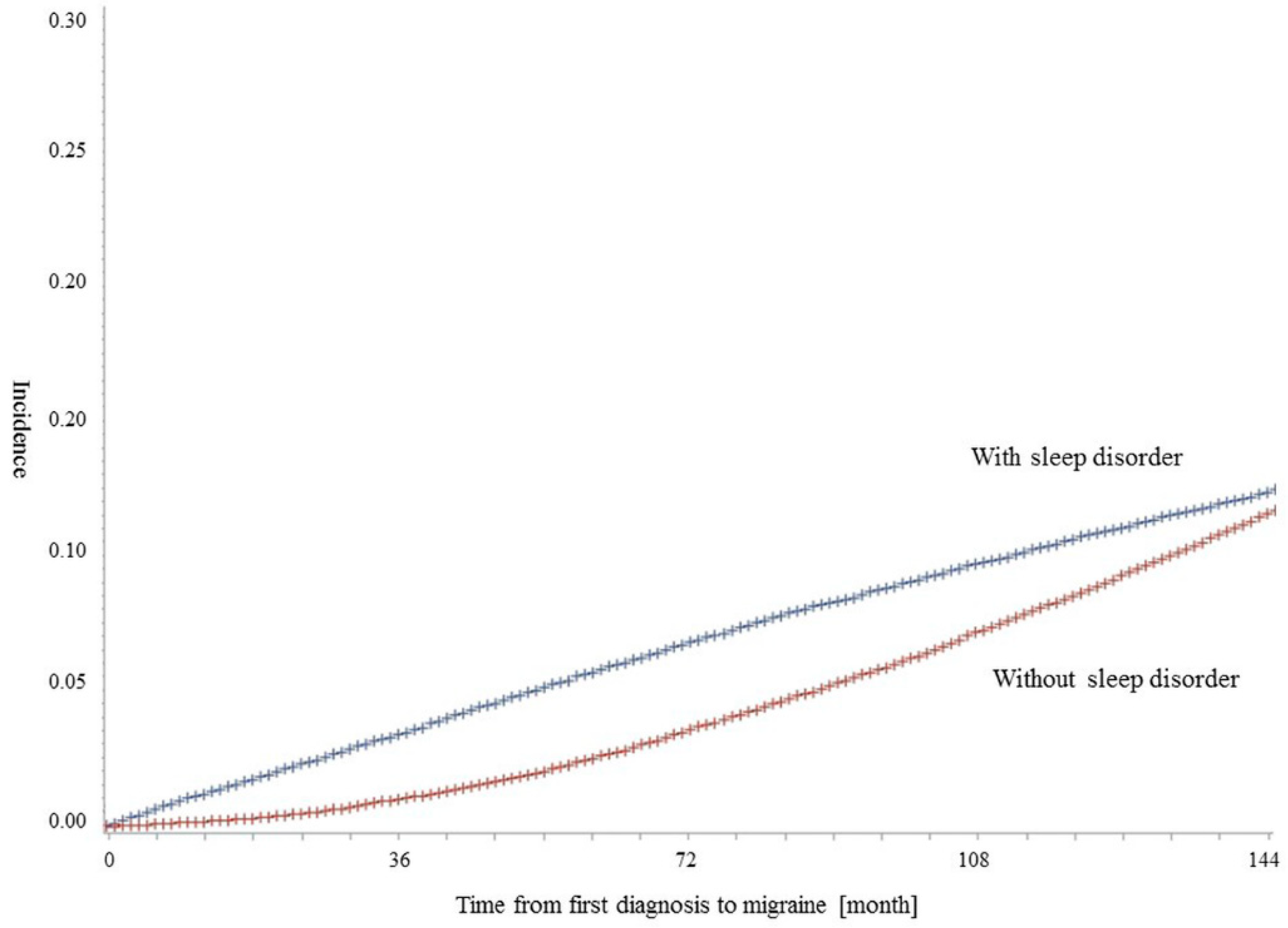
| Yes | 66,631 | 50.00 | 8025 | 12.04 | 58,606 | 87.96 | 0.0002 |
| No | 66,631 | 50.00 | 7591 | 11.39 | 59,040 | 88.61 | |
| Sex | |||||||
| Male | 55,614 | 41.73 | 4293 | 7.72 | 51,321 | 92.28 | <0.0001 |
| Female | 77,648 | 58.27 | 11,323 | 14.58 | 66,325 | 85.42 | |
| Age (Years) | |||||||
| ~29 | 6199 | 4.65 | 471 | 7.60 | 5728 | 92.40 | <0.0001 |
| 30–39 | 12,124 | 9.10 | 1290 | 10.64 | 10,834 | 89.36 | |
| 40–49 | 18,563 | 13.93 | 2148 | 11.57 | 16,415 | 88.43 | |
| 50–59 | 26,726 | 20.06 | 3374 | 12.62 | 23,352 | 87.38 | |
| 60–69 | 25,794 | 19.36 | 3059 | 11.86 | 22,735 | 88.14 | |
| 70–79 | 23,717 | 17.80 | 3182 | 13.42 | 20,535 | 86.58 | |
| 80~ | 20,139 | 15.11 | 2092 | 10.39 | 18,047 | 89.61 | |
| Economic level | |||||||
| ~30% (low) | 36,151 | 27.13 | 4408 | 12.19 | 31,743 | 87.81 | 0.0001 |
| 31–60% | 33,177 | 24.90 | 3919 | 11.81 | 29,258 | 88.19 | |
| 61–90% | 44,898 | 33.69 | 5215 | 11.62 | 39,683 | 88.38 | |
| +91% (high) | 19,036 | 14.28 | 2074 | 10.90 | 16,962 | 89.10 | |
| Types of insurance coverage | |||||||
| Medical aid | 6733 | 5.05 | 932 | 13.84 | 5801 | 86.16 | <0.0001 |
| NHI, self-employed insured | 54,054 | 40.56 | 6492 | 12.01 | 47,562 | 87.99 | |
| NHI, employee insured | 72,475 | 54.39 | 8192 | 11.30 | 64,283 | 88.70 | |
| Charlson comorbidity index | |||||||
| 0 | 109,022 | 81.81 | 12,596 | 11.55 | 96,426 | 88.45 | <0.0001 |
| 1 | 15,257 | 11.45 | 1994 | 13.07 | 13,263 | 86.93 | |
| 2 | 6015 | 4.51 | 693 | 11.52 | 5322 | 88.48 | |
| 3 | 1165 | 0.87 | 130 | 11.16 | 1035 | 88.84 | |
| 4+ | 1803 | 1.35 | 203 | 11.26 | 1600 | 88.74 | |
| Region | |||||||
| Capital area | 55,652 | 41.76 | 5971 | 10.73 | 49,681 | 89.27 | <0.0001 |
| Metropolitan | 33,888 | 25.43 | 3848 | 11.36 | 30,040 | 88.64 | |
| Others | 43,722 | 32.81 | 5797 | 13.26 | 37,925 | 86.74 | |
| Total | 133,262 | 58.24 | 15,616 | 11.72 | 117,646 | 88.28 | |
| Variables | Migraine | |||
|---|---|---|---|---|
| HR | 95% CI | p-Value | ||
| Lower | Upper | |||
| Sleep disorder | ||||
| Yes | 1.591 | 1.543 | 1.641 | <0.0001 |
| No | 1.000 | — | — | — |
| Sex | ||||
| Male | 1.000 | — | — | — |
| Female | 1.833 | 1.780 | 1.887 | <0.0001 |
| Age (Years) | ||||
| ~29 | 1.000 | — | — | — |
| 30–39 | 1.450 | 1.335 | 1.575 | <0.0001 |
| 40–49 | 4.578 | 1.460 | 1.707 | <0.0001 |
| 50–59 | 1.690 | 1.567 | 1.822 | <0.0001 |
| 60–69 | 1.682 | 1.559 | 1.816 | <0.0001 |
| 70–79 | 1.898 | 1.759 | 2.048 | <0.0001 |
| 80~ | 1.625 | 1.500 | 1.761 | <0.0001 |
| Economic level | ||||
| ~30% (low) | 1.000 | — | — | — |
| 31–60% | 1.035 | 0.988 | 1.083 | 0.1447 |
| 61–90% | 1.069 | 1.022 | 1.117 | 0.0035 |
| 91%~ (high) | 1.020 | 0.977 | 1.064 | 0.3727 |
| Types of insurance coverage | ||||
| Medical aid | 1.251 | 1.175 | 1.330 | <0.0001 |
| NHI, self-employed insured | 1.011 | 0.984 | 1.039 | 0.4098 |
| NHI, employee insured | 1.000 | — | — | — |
| Charlson comorbidity index | ||||
| 0 | 1.000 | — | — | — |
| 1 | 1.151 | 1.107 | 1.197 | <0.0001 |
| 2 | 1.111 | 1.047 | 1.179 | 0.0005 |
| 3 | 1.090 | 0.954 | 1.245 | 0.2036 |
| 4+ | 1.164 | 1.049 | 1.291 | 0.0041 |
| Region | ||||
| Capital area | 1.000 | — | — | — |
| Metropolitan | 1.055 | 1.020 | 1.092 | 0.0017 |
| Others | 1.237 | 1.200 | 1.275 | <0.0001 |
| Variables | Migraine | |||
|---|---|---|---|---|
| HR | 95% CI | p-Value | ||
| Lower | Upper | |||
| Sleep disorder | ||||
| Insomnia | 1.792 | 1.740 | 1.846 | <0.0001 |
| Sleep apnea | 1.250 | 1.138 | 1.373 | <0.0001 |
| Other sleep disorders | 1.663 | 1.602 | 1.727 | <0.0001 |
| None | 1.000 | — | — | — |
| Sex | ||||
| Male | 1.000 | — | — | — |
| Female | 1.810 | 1.758 | 1.864 | <0.0001 |
| Age (Years) | ||||
| ~29 | 1.000 | — | — | — |
| 30–39 | 1.470 | 1.353 | 1.597 | <0.0001 |
| 40–49 | 1.603 | 1.483 | 1.733 | <0.0001 |
| 50–59 | 1.716 | 1.592 | 1.851 | <0.0001 |
| 60–69 | 1.723 | 1.596 | 1.859 | <0.0001 |
| 70–79 | 1.944 | 1.802 | 2.098 | <0.0001 |
| 80~ | 1.683 | 1.554 | 1.823 | <0.0001 |
| Economic level | ||||
| ~30% (low) | 1.000 | — | — | — |
| 31–60% | 1.032 | 0.986 | 1.080 | 0.1734 |
| 61–90% | 1.071 | 1.024 | 1.120 | 0.0025 |
| 91%~ (high) | 1.025 | 0.982 | 1.070 | 0.2510 |
| Types of insurance coverage | ||||
| Medical aid | 1.228 | 1.154 | 1.306 | <0.0001 |
| NHI, self-employed insured | 0.999 | 0.972 | 1.027 | 0.9436 |
| NHI, employee insured | 1.000 | — | — | — |
| Charlson comorbidity index | ||||
| 0 | 1.000 | — | — | — |
| 1 | 1.125 | 1.082 | 1.170 | <0.0001 |
| 2 | 1.027 | 0.968 | 1.090 | 0.3745 |
| 3 | 1.024 | 0.896 | 1.170 | 0.7254 |
| 4+ | 1.042 | 0.939 | 1.156 | 0.4372 |
| Region | ||||
| Capital area | 1.000 | — | — | — |
| Metropolitan | 1.054 | 1.019 | 1.090 | 0.0021 |
| Others | 1.238 | 1.201 | 1.277 | <0.0001 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kim, S.J.; Han, K.-T.; Jang, S.-Y.; Yoo, K.-B.; Kim, S.J. The Association between Migraine and Types of Sleep Disorder. Int. J. Environ. Res. Public Health 2018, 15, 2648. https://doi.org/10.3390/ijerph15122648
Kim SJ, Han K-T, Jang S-Y, Yoo K-B, Kim SJ. The Association between Migraine and Types of Sleep Disorder. International Journal of Environmental Research and Public Health. 2018; 15(12):2648. https://doi.org/10.3390/ijerph15122648
Chicago/Turabian StyleKim, Seung Ju, Kyu-Tae Han, Suk-Yong Jang, Ki-Bong Yoo, and Sun Jung Kim. 2018. "The Association between Migraine and Types of Sleep Disorder" International Journal of Environmental Research and Public Health 15, no. 12: 2648. https://doi.org/10.3390/ijerph15122648
APA StyleKim, S. J., Han, K.-T., Jang, S.-Y., Yoo, K.-B., & Kim, S. J. (2018). The Association between Migraine and Types of Sleep Disorder. International Journal of Environmental Research and Public Health, 15(12), 2648. https://doi.org/10.3390/ijerph15122648






