The Short-Term Effect of Ambient Temperature on Mortality in Wuhan, China: A Time-Series Study Using a Distributed Lag Non-Linear Model
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Area and Population
2.2. Data Collection
2.3. Data Analysis
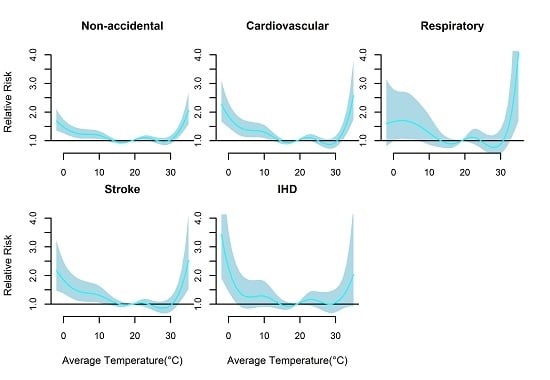
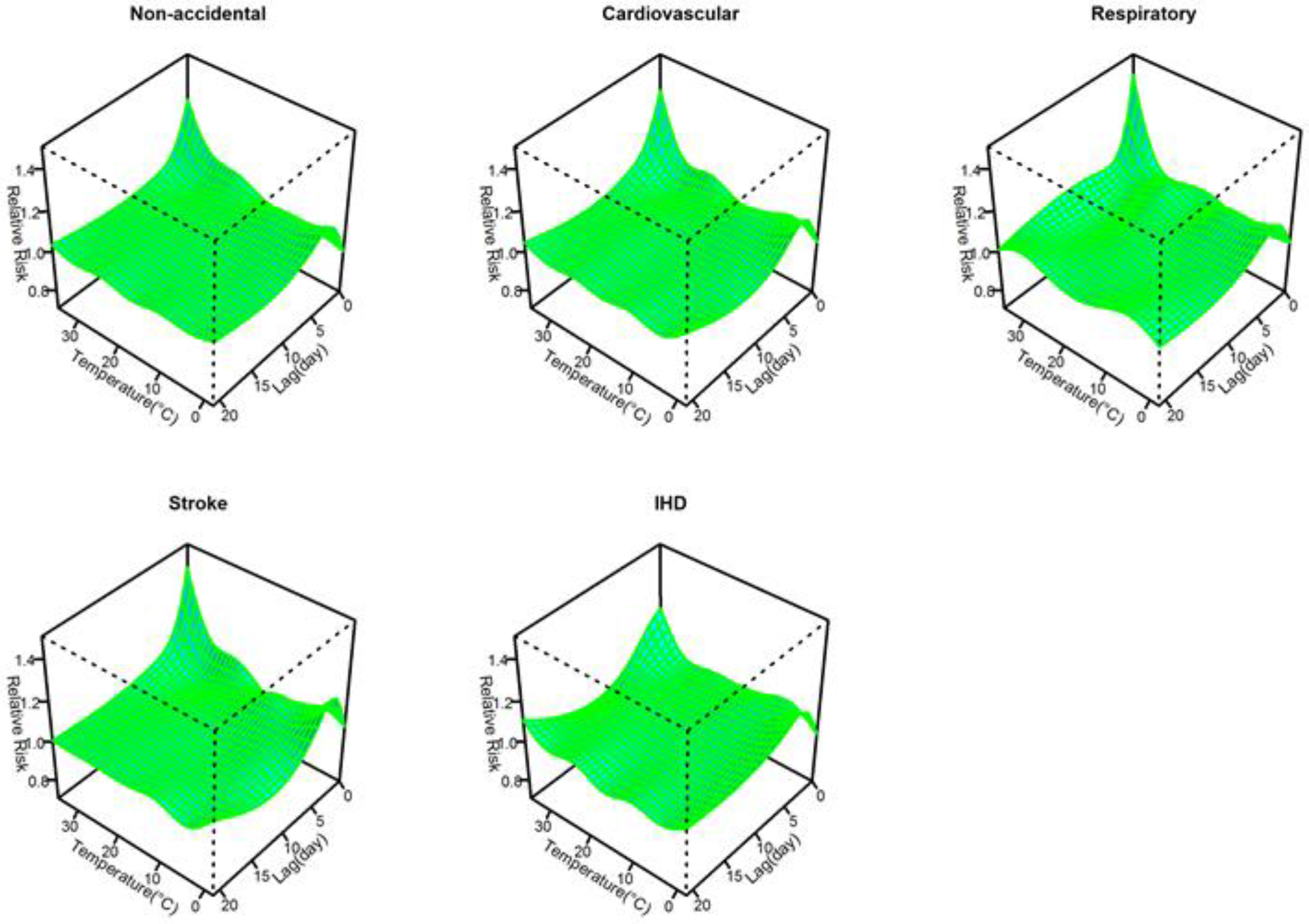
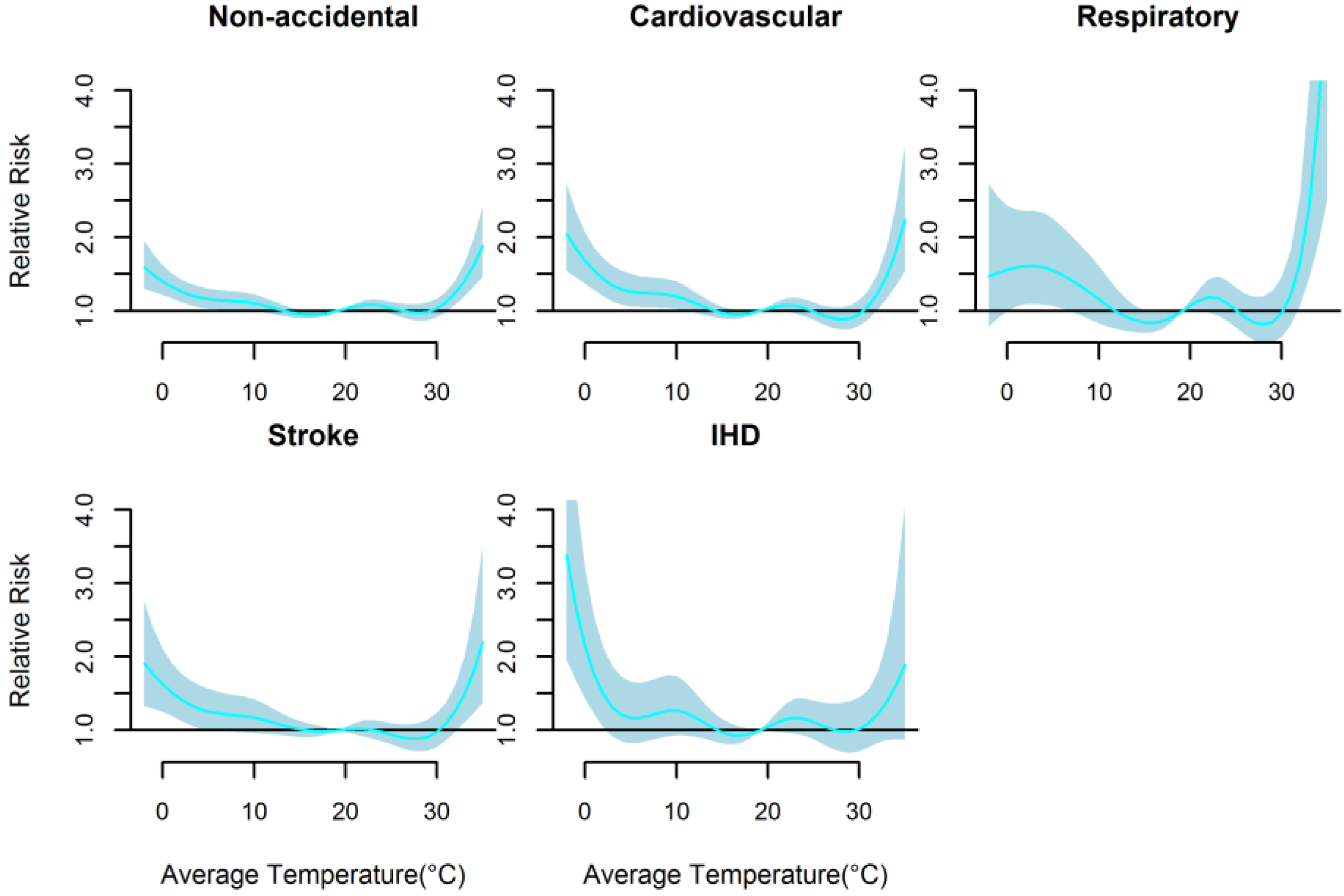
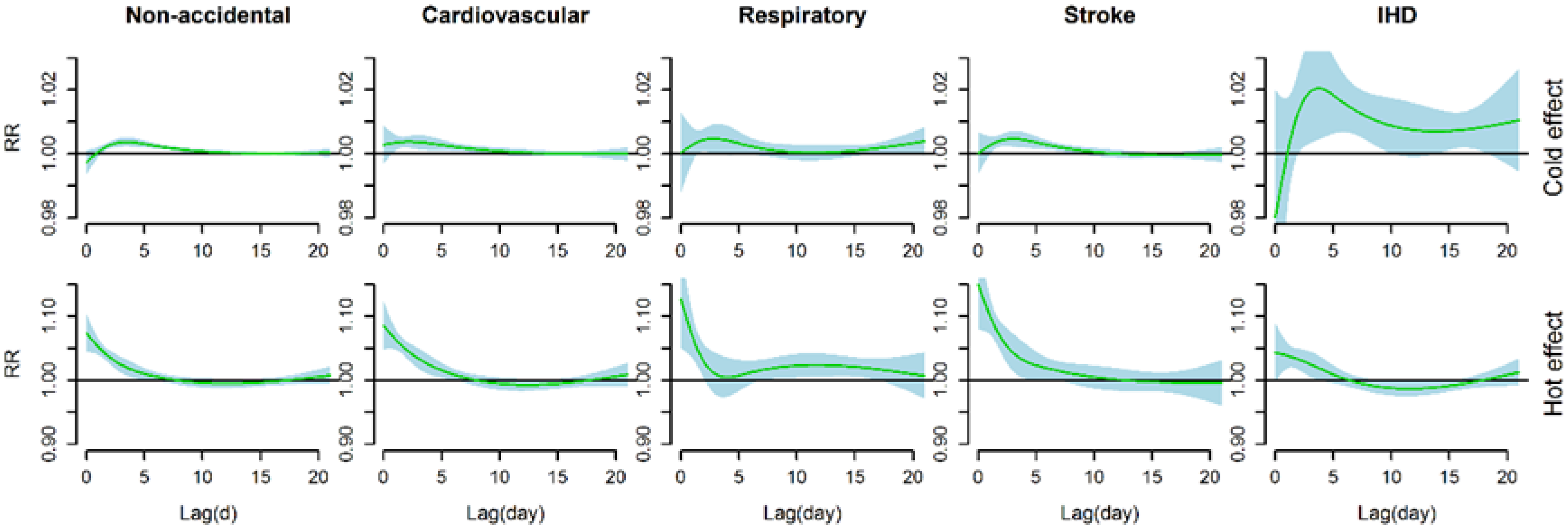
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Zhou, X.; Zhao, A.; Meng, X.; Chen, R.; Kuang, X.; Duan, X.; Kan, H. Acute effects of diurnal temperature range on mortality in 8 Chinese cities. Sci. Total Environ. 2014, 493, 92–97. [Google Scholar] [CrossRef] [PubMed]
- Anthony, C.; Mustafa, A.; Adriana, A.; Sarah, B.; Sarah, B.; Richard, B.; Sharon, F.; Nora, G.; Anne, J.; Maria, K.; et al. Managing the health effects of climate change: Lancet and University College London Institute for Global Health Commission. Lancet 2009, 373, 1693–1733. [Google Scholar]
- Wang, C.; Chen, R.; Kuang, X.; Duan, X.; Kan, H. Temperature and daily mortality in Suzhou, China: A time series analysis. Sci. Total Environ. 2014, 466–467, 985–990. [Google Scholar] [CrossRef] [PubMed]
- Semenza, J.C. Climate change and human health. Int. J. Environ. Res. Public Health 2014, 11, 7347–7353. [Google Scholar] [CrossRef] [PubMed]
- Breitner, S.; Wolf, K.; Devlin, R.B.; Diaz-Sanchez, D.; Peters, A.; Schneider, A. Short-term effects of air temperature on mortality and effect modification by air pollution in three cities of Bavaria, Germany: A time-series analysis. Sci. Total Environ. 2014, 485–486, 49–61. [Google Scholar] [CrossRef] [PubMed]
- Anderson, B.G.; Bell, M.L. Weather-related mortality: How heat, cold, and heat waves affect mortality in the United States. Epidemiology 2009, 20, 205–213. [Google Scholar] [CrossRef] [PubMed]
- Ma, W.; Chen, R.; Kan, H. Temperature-related mortality in 17 large Chinese cities: How heat and cold affect mortality in China. Environ. Res. 2014, 134, 127–133. [Google Scholar] [CrossRef] [PubMed]
- Xiao, J.; Peng, J.; Zhang, Y.; Liu, T.; Rutherford, S.; Lin, H.; Qian, Z.; Huang, C.; Luo, Y.; Zeng, W.; et al. How much does latitude modify temperature-mortality relationship in 13 Eastern U.S. cities? Int. J. Biometeorol. 2015, 59, 365–372. [Google Scholar] [CrossRef] [PubMed]
- Guo, Y.; Gasparrini, A.; Armstrong, B.; Li, S.; Tawatsupa, B.; Tobias, A.; Lavigne, E.; de Sousa Zanotti Stagliorio Coelho, M.; Leone, M.; Pan, X.; et al. Global variation in the effects of ambient temperature on mortality: A systematic evaluation. Epidemiology 2014, 25, 781–789. [Google Scholar] [CrossRef] [PubMed]
- Medina-Ramon, M.; Schwartz, J. Temperature, temperature extremes, and mortality: A study of acclimatisation and effect modification in 50 U.S. cities. Occup. Environ. Med. 2007, 64, 827–833. [Google Scholar] [CrossRef] [PubMed]
- McMichael, A.J.; Wilkinson, P.; Kovats, R.S.; Pattenden, S.; Hajat, S.; Armstrong, B.; Vajanapoom, N.; Niciu, E.M.; Mahomed, H.; Kingkeow, C.; et al. International study of temperature, heat and urban mortality: The “ISOTHURM” project. Int. J. Epidemiol. 2008, 37, 1121–1131. [Google Scholar] [CrossRef] [PubMed]
- Tian, Z.; Li, S.; Zhang, J.; Jaakkola, J.J.; Guo, Y. Ambient temperature and coronary heart disease mortality in Beijing, China: A time series study. Environ. Health 2012, 11, 56. [Google Scholar] [CrossRef] [PubMed]
- Liu, L.; Breitner, S.; Pan, X.; Franck, U.; Leitte, A.M.; Wiedensohler, A.; von Klot, S.; Wichmann, H.E.; Peters, A.; Schneider, A. Associations between air temperature and cardio-respiratory mortality in the urban area of Beijing, China: A time-series analysis. Environ. Health 2011, 10, 51. [Google Scholar] [CrossRef] [PubMed]
- Kan, H.; London, S.J.; Chen, H.; Song, G.; Chen, G.; Jiang, L.; Zhao, N.; Zhang, Y.; Chen, B. Diurnal temperature range and daily mortality in Shanghai, China. Environ. Res. 2007, 103, 424–431. [Google Scholar] [CrossRef] [PubMed]
- Wu, W.; Xiao, Y.; Li, G.; Zeng, W.; Lin, H.; Rutherford, S.; Xu, Y.; Luo, Y.; Xu, X.; Chu, C.; et al. Temperature-mortality relationship in four subtropical Chinese cities: A time-series study using a distributed lag non-linear model. Sci. Total Environ. 2013, 449, 355–362. [Google Scholar] [CrossRef] [PubMed]
- Yang, J.; Ou, C.Q.; Ding, Y.; Zhou, Y.X.; Chen, P.Y. Daily temperature and mortality: A study of distributed lag non-linear effect and effect modification in Guangzhou. Environ. Health 2012, 11, 63. [Google Scholar] [CrossRef] [PubMed]
- Guo, Y.; Barnett, A.G.; Pan, X.; Yu, W.; Tong, S. The impact of temperature on mortality in Tianjin, China: A case-crossover design with a distributed lag nonlinear model. Environ. Health Perspect. 2011, 119, 1719–1725. [Google Scholar] [CrossRef] [PubMed]
- China Meteorological Data Sharing Service System. Available online: http://cdc.cma.gov.cn (accessed on 6 June 2016).
- Chen, R.; Zhou, B.; Kan, H.; Zhao, B. Associations of particulate air pollution and daily mortality in 16 Chinese cities: An improved effect estimate after accounting for the indoor exposure to particles of outdoor origin. Environ. Pollut. 2013, 182, 278–282. [Google Scholar] [CrossRef] [PubMed]
- Ma, W.; Zeng, W.; Zhou, M.; Wang, L.; Rutherford, S.; Lin, H.; Liu, T.; Zhang, Y.; Xiao, J.; Zhang, Y.; et al. The short-term effect of heat waves on mortality and its modifiers in China: An analysis from 66 communities. Environ. Int. 2015, 75, 103–109. [Google Scholar] [CrossRef] [PubMed]
- Qian, Z.; He, Q.; Lin, H.M.; Kong, L.; Bentley, C.M.; Liu, W.; Zhou, D. High temperatures enhanced acute mortality effects of ambient particle pollution in the “oven” city of Wuhan, China. Environ. Health Perspect. 2008, 116, 1172–1178. [Google Scholar] [CrossRef] [PubMed]
- Gasparrini, A.; Armstrong, B.; Kenward, M.G. Distributed lag non-linear models. Stat. Med. 2010, 29, 2224–2234. [Google Scholar] [CrossRef] [PubMed]
- Ma, W.; Wang, L.; Lin, H.; Liu, T.; Zhang, Y.; Rutherford, S.; Luo, Y.; Zeng, W.; Zhang, Y.; Wang, X.; et al. The temperature-mortality relationship in China: An analysis from 66 Chinese communities. Environ. Res. 2015, 137, 72–77. [Google Scholar] [CrossRef] [PubMed]
- Chen, R.J.; Wang, C.C.; Meng, X.; Chen, H.L.; Thach, T.Q.; Wong, C.M.; Kan, H.D. Both low and high temperature may increase the risk of stroke mortality. Neurology 2013, 81, 1064–1070. [Google Scholar] [CrossRef] [PubMed]
- Yu, W.; Mengersen, K.; Hu, W.; Guo, Y.; Pan, X.; Tong, S. Assessing the relationship between global warming and mortality: Lag effects of temperature fluctuations by age and mortality categories. Environ. Pollut. 2011, 159, 1789–1793. [Google Scholar] [CrossRef] [PubMed]
- Guo, Y.; Punnasiri, K.; Tong, S. Effects of temperature on mortality in Chiang Mai City, Thailand: A time series study. Environ. Health 2012, 11, 36. [Google Scholar] [CrossRef] [PubMed]
- Onozuka, D.; Hagihara, A. Variation in vulnerability to extreme-temperature-related mortality in Japan: A 40-year time-series analysis. Environ. Res. 2015, 140, 177–184. [Google Scholar] [CrossRef] [PubMed]
- Ma, W.; Yang, C.; Tan, J.; Song, W.; Chen, B.; Kan, H. Modifiers of the temperature-mortality association in Shanghai, China. Int. J. Biometeorol. 2012, 56, 205–207. [Google Scholar] [CrossRef] [PubMed]
- Ng, C.F.; Ueda, K.; Takeuchi, A.; Nitta, H.; Konishi, S.; Bagrowicz, R.; Watanabe, C.; Takami, A. Sociogeographic variation in the effects of heat and cold on daily mortality in Japan. J. Epidemiol. 2014, 24, 15–24. [Google Scholar] [CrossRef] [PubMed]
- Yu, W.; Guo, Y.; Ye, X.; Wang, X.; Huang, C.; Pan, X.; Tong, S. The effect of various temperature indicators on different mortality categories in a subtropical City of Brisbane, Australia. Sci. Total Environ. 2011, 409, 3431–3437. [Google Scholar] [CrossRef] [PubMed]
- Barnett, A.G.; Tong, S.; Clements, A.C. What measure of temperature is the best predictor of mortality? Environ. Res. 2010, 110, 604–611. [Google Scholar] [CrossRef] [PubMed]
- Yu, W.; Mengersen, K.; Wang, X.; Ye, X.; Guo, Y.; Pan, X.; Tong, S. Daily average temperature and mortality among the elderly: A meta-analysis and systematic review of epidemiological evidence. Int. J. Biometeorol. 2012, 56, 569–581. [Google Scholar] [CrossRef] [PubMed]
- Basu, R.; Malig, B. High ambient temperature and mortality in California: Exploring the roles of age, disease, and mortality displacement. Environ. Res. 2011, 111, 1286–1292. [Google Scholar] [CrossRef] [PubMed]
- Saha, M.V.; Davis, R.E.; Hondula, D.M. Mortality displacement as a function of heat event strength in 7 U.S. cities. Am. J. Epidemiol. 2014, 179, 467–474. [Google Scholar] [CrossRef] [PubMed]
- Baccini, M.; Biggeri, A.; Accetta, G.; Kosatsky, T.; Katsouyanni, K.; Analitis, A.; Anderson, H.R.; Bisanti, L.; D’Ippoliti, D.; Danova, J.; et al. Heat effects on mortality in 15 European cities. Epidemiology 2008, 19, 711–719. [Google Scholar] [CrossRef] [PubMed]
- Gasparrini, A.; Armstrong, B.; Kovats, S.; Wilkinson, P. The effect of high temperatures on cause-specific mortality in England and Wales. Occup. Environ. Med. 2012, 69, 56–61. [Google Scholar] [CrossRef] [PubMed]
- Astrom, D.O.; Forsberg, B.; Rocklov, J. Heat wave impact on morbidity and mortality in the elderly population: A review of recent studies. Maturitas 2011, 69, 99–105. [Google Scholar] [CrossRef] [PubMed]
- Baccini, M.; Kosatsky, T.; Analitis, A.; Anderson, H.R.; D’Ovidio, M.; Menne, B.; Michelozzi, P.; Biggeri, A.; Group, P.C. Impact of heat on mortality in 15 European cities: Attributable deaths under different weather scenarios. J. Epidemiol. Commun. Health 2011, 65, 64–70. [Google Scholar] [CrossRef] [PubMed]
- Basu, R. High ambient temperature and mortality: A review of epidemiologic studies from 2001 to 2008. Environ. Health 2009, 8, 40. [Google Scholar] [CrossRef] [PubMed]
- Chen, K.; Bi, J.; Chen, J.; Chen, X.; Huang, L.; Zhou, L. Influence of heat wave definitions to the added effect of heat waves on daily mortality in Nanjing, China. Sci. Total Environ. 2015, 506–507, 18–25. [Google Scholar] [CrossRef] [PubMed]
- Xie, H.; Yao, Z.; Zhang, Y.; Xu, Y.; Xu, X.; Liu, T.; Lin, H.; Lao, X.; Rutherford, S.; Chu, C.; et al. Short-term effects of the 2008 cold spell on mortality in three subtropical cities in Guangdong Province, China. Environ. Health Perspect. 2013, 121, 210–216. [Google Scholar] [PubMed]
- Madrigano, J.; Ito, K.; Johnson, S.; Kinney, P.L.; Matte, T. A case-only study of vulnerability to heat wave-related mortality in New York City (2000–2011). Environ. Health Perspect. 2015, 123, 672–678. [Google Scholar] [CrossRef] [PubMed]
| Variable | Mean ± SD | Minimum | P25 | P50 | P75 | Maximum |
|---|---|---|---|---|---|---|
| Daily death | ||||||
| Non-accidental | 11.2 ± 4.0 | 1 | 8 | 11 | 14 | 34 |
| Cardiovascular | 5.2 ± 2.7 | 0 | 3 | 5 | 7 | 23 |
| Stroke | 3.1 ± 2.0 | 0 | 2 | 3 | 4 | 17 |
| IHD | 1.3 ± 1.3 | 0 | 0 | 1 | 2 | 7 |
| Respiratory | 1.1 ± 1.1 | 0 | 0 | 1 | 2 | 7 |
| Weather conditions | ||||||
| Relative humidity (%) | 71.3 ± 12.6 | 21 | 63 | 72 | 80 | 97 |
| Temperature(°C) | ||||||
| Maximum | 22.2 ± 9.7 | −1.9 | 14.3 | 23.7 | 30.5 | 39.6 |
| Mean | 17.9 ± 9.4 | −2.7 | 9.5 | 19.2 | 25.9 | 35.8 |
| Minimum | 14.6 ± 9.3 | −5.2 | 6.5 | 15.7 | 22.7 | 32.3 |
| Air pollutants (μg/m3) | ||||||
| PM10 | 115.0 ± 60.0 | 10.5 | 70.0 | 105.0 | 148.0 | 600.0 |
| SO2 | 50.2 ± 33.7 | 1.0 | 26.0 | 42.0 | 66.0 | 260.5 |
| NO2 | 57.6 ± 25.3 | 12.0 | 38.4 | 52.8 | 72.8 | 288.0 |
| Mean Temperature | Minimum Temperature | Relative Humidity | PM10 | SO2 | NO2 | |
|---|---|---|---|---|---|---|
| Maximum temperature | 0.983 | 0.947 | −0.229 | −0.169 | −0.227 | −0.196 |
| Mean temperature | 0.987 | −0.163 | −0.226 | −0.284 | −0.258 | |
| Minimum temperature | −0.079 | −0.274 | −0.334 | −0.315 | ||
| Relative humidity | −0.241 | −0.286 | −0.194 | |||
| PM10 | 0.632 | 0.721 | ||||
| SO2 | 0.693 |
| DLNM Type | Temperature Metrics | QAIC Value | ||||
|---|---|---|---|---|---|---|
| Non-Accidental | Cardiovascular | Respiratory | Stroke | IHD | ||
| Non-threshold a | Maximum temperature | 15,354.85 | 13,057.47 | 7587.25 | 11,367.90 | 8433.61 |
| Mean temperature | 15,323.12 | 13,043.74 | 7584.90 | 11,359.48 | 8432.13 | |
| Minimum temperature | 15,327.35 | 13,048.02 | 7590.40 | 11,370.68 | 8434.02 | |
| Double-threshold b | Maximum temperature | 15,336.71 | 13,038.42 | 7566.27 | 11,342.09 | 8410.93 |
| Mean temperature | 15,315.91 | 13,034.61 | 7568.58 | 11,339.88 | 8407.63 | |
| Minimum temperature | 15,315.93 | 13,040.98 | 7572.09 | 11,346.56 | 8408.51 | |
| Threshold Type | Temperature Metrics | Mortality Type | ||||
|---|---|---|---|---|---|---|
| Non-Accidental | Cardiovascular | Respiratory | Stroke | IHD | ||
| Cold threshold (°C) | Maximum temperature | 22.3 | 20.2 | 19.4 | 24.6 | 3.1 |
| Mean temperature | 18.1 | 15.6 | 14.6 | 20.2 | 3.5 | |
| Minimum temperature | 13.9 | 13.3 | 11.0 | 18.1 | −1.5 | |
| Hot threshold (°C) | Maximum temperature | 34.7 | 36.1 | 34.6 | 37.1 | 34.4 |
| Mean temperature | 31.7 | 31.4 | 31.2 | 32.2 | 30.0 | |
| Minimum temperature | 28.8 | 28.9 | 28.0 | 29.2 | 26.6 | |
| Effect | Lag (Days) | Percent Increase in Mortality (95% CI) | ||||
|---|---|---|---|---|---|---|
| Non-Accidental | Cardiovascular | Respiratory | Stroke | IHD | ||
| Cold effect a | 0 | −0.22(−0.63, 0.20) | 0.49(−0.16, 1.14) | −0.21(−1.59, 1.19) | 0.17(−0.56, 0.91) | −1.97(−5.92, 2.16) |
| 0–2 | 0.17 (−0.45, 0.80) | 1.41 (0.44, 2.39) | 0.32 (−1.75, 2.43) | 1.12 (0.01, 2.25) | −0.81 (−6.67, 5.41) | |
| 0–7 | 1.73 (1.10, 2.37) | 2.95 (1.96, 3.95) | 2.08 (−0.02, 4.23) | 3.20 (2.06, 4.36) | 8.11 (1.59, 15.06) | |
| 0−14 | 2.25 (1.54, 2.98) | 3.59 (2.50, 4.71) | 2.62 (0.27, 5.03) | 3.44 (2.16, 4.75) | 15.14 (7.75, 23.05) | |
| 0–21 | 2.39 (1.71, 3.08) | 3.65 (2.62, 4.69) | 3.87 (1.57, 6.22) | 3.13 (1.88, 4.38) | 21.57 (12.59, 31.26) | |
| Hot effect b | 0 | 7.64 (4.51, 10.86) | 8.43 (4.48, 12.53) | 10.94 (2.45, 20.13) | 15.50 (7.83, 23.71) | 4.30 (−0.27, 9.07) |
| 0–2 | 17.67 (12.63, 22.94) | 21.55 (15.05, 28.41) | 19.37 (5.98, 34.47) | 36.94 (24.16, 51.03) | 11.62 (4.32, 19.43) | |
| 0–7 | 25.18 (18.74, 31.96) | 34.10 (25.63, 43.16) | 24.27 (7.55, 43.59) | 59.1 (41.81, 78.5) | 17.00 (7.91, 26.87) | |
| 0−14 | 23.03 (14.68, 31.99) | 28.97 (18.06, 40.89) | 46.94 (23.49, 74.85) | 65.88 (40.87, 95.32) | 8.59 (−1.82, 20.11) | |
| 0–21 | 24.74 (13.66, 36.89) | 30.17 (15.78, 46.35) | 56.74 (24.28, 97.69) | 61.59 (27.87, 104.19) | 9.83 (−2.85, 24.17) | |
| Location | Date Range | Study Design | Temperature Threshold | Main Results | ||
|---|---|---|---|---|---|---|
| Low (°C) | High (°C) | Cold Effect a | Hot Effect b | |||
| Tianjin | 2005–2007 | case-crossover | 0.8 | 24.9 | 2.99 (0.85, 5.17) c | 2.03 (0.70, 3.38) d |
| Changsha | 2006–2009 | time-series | 7 | 25 | 4.3 (1.3, 7.5) e | 2.0 (0.3, 3.7) f |
| Kunming | 2006–2009 | time-series | 15 | 19 | 4.4 (3.4, 5.5) e | 1.7 (0.4, 3.0) f |
| Guangzhou | 2006–2010 | time-series | 13 | 26 | 9.4 (7.6, 11.3) e | 2.9 (2.0, 3.9) f |
| Zhuhai | 2006–2010 | time-series | 15 | 26 | 10.3 (7.5, 13.3) e | 2.3 (0.4, 4.2) f |
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zhang, Y.; Li, C.; Feng, R.; Zhu, Y.; Wu, K.; Tan, X.; Ma, L. The Short-Term Effect of Ambient Temperature on Mortality in Wuhan, China: A Time-Series Study Using a Distributed Lag Non-Linear Model. Int. J. Environ. Res. Public Health 2016, 13, 722. https://doi.org/10.3390/ijerph13070722
Zhang Y, Li C, Feng R, Zhu Y, Wu K, Tan X, Ma L. The Short-Term Effect of Ambient Temperature on Mortality in Wuhan, China: A Time-Series Study Using a Distributed Lag Non-Linear Model. International Journal of Environmental Research and Public Health. 2016; 13(7):722. https://doi.org/10.3390/ijerph13070722
Chicago/Turabian StyleZhang, Yunquan, Cunlu Li, Renjie Feng, Yaohui Zhu, Kai Wu, Xiaodong Tan, and Lu Ma. 2016. "The Short-Term Effect of Ambient Temperature on Mortality in Wuhan, China: A Time-Series Study Using a Distributed Lag Non-Linear Model" International Journal of Environmental Research and Public Health 13, no. 7: 722. https://doi.org/10.3390/ijerph13070722
APA StyleZhang, Y., Li, C., Feng, R., Zhu, Y., Wu, K., Tan, X., & Ma, L. (2016). The Short-Term Effect of Ambient Temperature on Mortality in Wuhan, China: A Time-Series Study Using a Distributed Lag Non-Linear Model. International Journal of Environmental Research and Public Health, 13(7), 722. https://doi.org/10.3390/ijerph13070722