Temporal Trends in Overweight and Obesity, Physical Activity and Screen Time among Czech Adolescents from 2002 to 2014: A National Health Behaviour in School-Aged Children Study
Abstract
:1. Introduction
- (i)
- Determine whether a gradual increase in the prevalence of overweight/obesity in boys continued in 2014, and also assess the direction of trends in the prevalence of overweight/obesity in girls;
- (ii)
- Describe temporal trends in the achievement of PA recommendations (MVPA—at least 60 min per day, VPA – at least 30 min per week and four or more days of the week);
- (iii)
- Consider whether a rapid increase in ST in boys and girls on weekdays and at weekends continued in the 2014 cycle;
- (iv)
- Identify correlates of overweight/obesity that potentially contributed to the high prevalence of overweight and obesity among Czech adolescents in the 2002–2014 period.
2. Methods
2.1. Study Design
2.2. Sample
2.3. Instrument and Variables
2.3.1. Weight Status
2.3.2. Physical Activity
2.3.3. Screen time (ST)
2.4. Data Treatment and Statistical Analyses
3. Results
| 2002 | 2006 | 2010 | 2014 | |||||
|---|---|---|---|---|---|---|---|---|
| Boys | Girls | Boys | Girls | Boys | Girls | Boys | Girls | |
| (n = 2412) | (n = 2600) | (n = 2410) | (n = 2364) | (n = 2135) | (n = 2269) | (n = 2803) | (n = 2947) | |
| % | % | % | % | % | % | % | % | |
| School grade § | ||||||||
| 5th grade | 34.3 | 33.3 | 31.7 | 31.5 | 33.7 | 31.2 | 30.9 | 31.4 |
| 7th grade | 32.3 | 33.8 | 33.4 | 33.7 | 31.3 | 34.7 | 34.3 | 34.5 |
| 9th grade | 33.4 | 32.8 | 34.9 | 34.8 | 35.0 | 34.2 | 34.8 | 34.1 |
| Weight status # | ||||||||
| Normal weight | 81.7 | 91.7 | 77.6 | 83.7 | 73.7 | 88.0 | 75.3 | 88.1 |
| Overweight/obese | 18.3 | 8.3 | 22.4 | 16.3 | 26.3 | 12.0 | 24.7 | 11.9 |
| Daily MVPA * | ||||||||
| ≥60 min | 32.2 | 23.2 | 27.4 | 17.9 | 28.3 | 19.2 | 25.6 | 19.2 |
| VPA per week † | ||||||||
| ≥4 times 30 or more minutes | - | - | 45.7 | 24.4 | 44.9 | 30.3 | 42.0 | 33.6 |
| Daily screen time ‡ | ||||||||
| >2 h per weekday | 75.1 | 61.3 | 86.0 | 73.4 | 87.6 | 81.4 | 88.7 | 76.6 |
| >2 h per weekend day | 78.3 | 65.1 | 88.6 | 79.8 | 89.4 | 84.8 | 91.8 | 83.7 |
3.1. Trends in Excess Body Weight (Overweight and Obesity)
3.2. Trends in Attainment of the Physical Activity Recommendation
3.3. Trends in Non-Excessive Screen Time
| 2002 | 2006 | 2010 | 2014 | 2014 vs. 2002 | |||
|---|---|---|---|---|---|---|---|
| Odds ratio to reach the variables 1−5 | 95% CI | ||||||
| % a | % a | % a | % a | OR | Lower | Upper | |
| Overweight/obese1 | |||||||
| Boys | 18.3 | 22.4 | 26.3 | 24.7 | 1.46 *** | 1.28 | 1.68 |
| 5th grade | 21.5 | 30.1 | 30.6 | 27.8 | 1.41 ** | 1.12 | 1.77 |
| 7th grade | 17.3 | 21.2 | 27.0 | 26.6 | 1.73 *** | 1.37 | 2.20 |
| 9th grade | 16.0 | 16.6 | 21.8 | 20.6 | 1.36 * | 1.06 | 1.74 |
| Girls | 8.3 | 16.3 | 12.0 | 11.9 | 1.49 *** | 1.24 | 1.78 |
| 5th grade | 10.1 | 22.7 | 15.3 | 14.0 | 1.45 * | 1.08 | 1.94 |
| 7th grade | 8.6 | 15.5 | 10.6 | 11.3 | 1.36 * | 1.00 | 1.86 |
| 9th grade | 6.2 | 11.5 | 10.7 | 10.7 | 1.80 *** | 1.27 | 2.55 |
| MVPA recommendations 2 | |||||||
| Boys | 32.2 | 27.4 | 28.3 | 25.6 | 0.72 *** | 0.64 | 0.82 |
| 5th grade | 36.2 | 25.7 | 29.0 | 29.5 | 0.74 ** | 0.60 | 0.91 |
| 7th grade | 32.6 | 28.6 | 30.6 | 27.2 | 0.77 * | 0.63 | 0.95 |
| 9th grade | 27.9 | 27.9 | 25.5 | 20.4 | 0.66 *** | 0.53 | 0.83 |
| Girls | 23.2 | 17.9 | 19.2 | 19.2 | 0.79 *** | 0.69 | 0.90 |
| 5th grade | 28.5 | 19.7 | 24.1 | 24.2 | 0.80 * | 0.65 | 0.99 |
| 7th grade | 22.5 | 17.6 | 19.4 | 20.1 | 0.87 | 0.69 | 1.08 |
| 9th grade | 18.4 | 16.5 | 14.9 | 13.6 | 0.70 ** | 0.54 | 0.90 |
| Non-excessive ST weekday 3 | |||||||
| Boys | 24.9 | 14.0 | 12.4 | 11.2 | 0.38 *** | 0.33 | 0.45 |
| 5th grade | 32.2 | 19.0 | 19.6 | 15.4 | 0.38 *** | 0.30 | 0.48 |
| 7th grade | 21.1 | 11.3 | 9.4 | 11.2 | 0.47 *** | 0.36 | 0.62 |
| 9th grade | 21.1 | 11.9 | 8.2 | 7.6 | 0.31 *** | 0.23 | 0.41 |
| Girls | 38.7 | 26.5 | 18.5 | 23.4 | 0.48 *** | 0.43 | 0.54 |
| 5th grade | 44.2 | 33.4 | 28.4 | 34.3 | 0.66 *** | 0.55 | 0.80 |
| 7th grade | 34.1 | 23.5 | 13.5 | 23.2 | 0.59 *** | 0.48 | 0.72 |
| 9th grade | 37.9 | 23.3 | 14.6 | 13.7 | 0.26 *** | 0.21 | 0.33 |
| Non-excessive ST weekend day 4 | |||||||
| Boys | 21.7 | 11.4 | 10.6 | 8.1 | 0.31 *** | 0.27 | 0.38 |
| 5th grade | 28.1 | 13.7 | 15.8 | 12.0 | 0.35 *** | 0.27 | 0.45 |
| 7th grade | 20.1 | 10.6 | 9.0 | 7.1 | 0.30 *** | 0.22 | 0.41 |
| 9th grade | 16.7 | 10.0 | 7.0 | 5.7 | 0.30 *** | 0.22 | 0.42 |
| Girls | 34.9 | 20.1 | 15.3 | 16.3 | 0.36 *** | 0.32 | 0.41 |
| 5th grade | 39.6 | 27.1 | 25.6 | 26.4 | 0.55 *** | 0.45 | 0.67 |
| 7th grade | 31.1 | 17.0 | 11.2 | 13.4 | 0.34 *** | 0.27 | 0.43 |
| 9th grade | 34.0 | 16.9 | 10.0 | 10.1 | 0.22 *** | 0.17 | 0.28 |
| VPA recommendations 5 | 2014 vs. 2006 | ||||||
| Boys | - | 45.8 | 44.9 | 42.2 | 0.86 ** | 0.77 | 0.96 |
| 5th grade | - | 45.4 | 46.3 | 39.4 | 0.78 * | 0.64 | 0.96 |
| 7th grade | - | 47.1 | 46.1 | 42.6 | 0.83 | 0.69 | 1.01 |
| 9th grade | - | 44.8 | 42.6 | 44.4 | 0.98 | 0.81 | 1.18 |
| Girls | - | 24.4 | 30.3 | 33.6 | 1.57 *** | 1.39 | 1.77 |
| 5th grade | - | 30.2 | 37.1 | 34.4 | 1.22 | 0.99 | 1.50 |
| 7th grade | - | 23.0 | 30.7 | 36.2 | 1.90 *** | 1.54 | 2.35 |
| 9th grade | - | 20.5 | 23.6 | 30.2 | 1.67 *** | 1.35 | 2.08 |
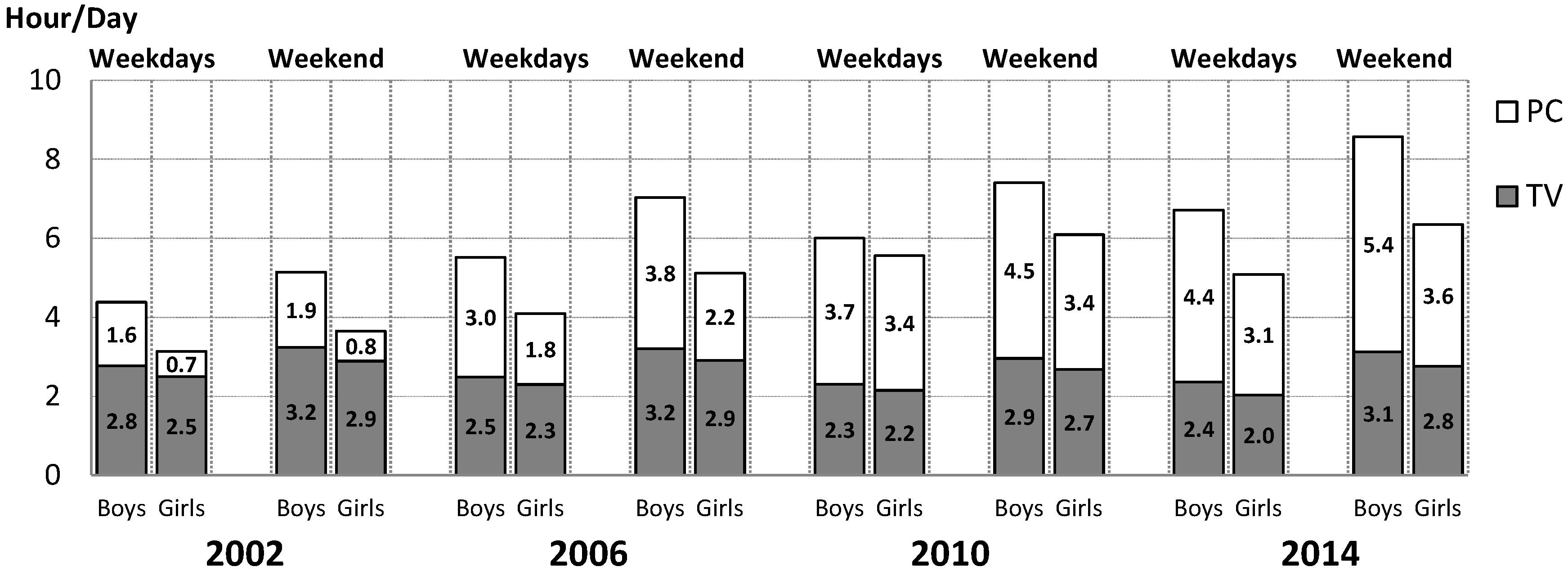
3.4. Correlates of Excessive Body Weight (Overweight/Obesity)
| Overweight/Obese | ||||
|---|---|---|---|---|
| 95% CI | ||||
| % | OR | Lower | Upper | |
| Year of data collection | ||||
| 2014 | 18.2 | Ref. | ||
| 2010 | 19.0 | 1.06 | 0.95 | 1.18 |
| 2006 | 19.4 | 1.09 | 0.98 | 1.21 |
| 2002 | 13.1 | 0.69 ** | 0.62 | 0.77 |
| Gender | ||||
| Boys | 22.9 | Ref. | ||
| Girls | 12.0 | 0.46 ** | 0.42 | 0.50 |
| School grade 1 | ||||
| 5th grade | 21.2 | Ref. | ||
| 7th grade | 17.0 | 0.72 ** | 0.66 | 0.79 |
| 9th grade | 14.2 | 0.58 ** | 0.53 | 0.64 |
| MVPA recommendations 2 | ||||
| <60 min of MVPA per day | 17.6 | Ref. | ||
| ≥60 min of MVPA per day | 15.9 | 0.81 ** | 0.74 | 0.89 |
| ST recommendations weekday 3 | ||||
| >2 h per week day | 18.3 | Ref. | ||
| ≤2 h per week day | 14.0 | 0.86 * | 0.77 | 0.97 |
| ST recommendations weekend day 3 | ||||
| >2 h per weekend day | 18.1 | Ref. | ||
| ≤2 h per weekend day | 14.1 | 0.90 | 0.80 | 1.02 |
4. Discussion
5. Strengths and Limitations
6. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Ng, M.; Fleming, T.; Robinson, M.; Thomson, B.; Graetz, N.; Margono, C.; Mullany, E.C.; Biryukov, S.; Abbafati, C.; Abera, S.F.; et al. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: A systematic analysis for the Global Burden of Disease Study 2013. Lancet 2014, 384, 766–781. [Google Scholar]
- Dos Santos, F.K.; Maia, J.A.R.; Gomes, T.N.Q.F.; Daca, T.; Madeira, A.; Katzmarzyk, P.T.; Prista, A. Secular trends in growth and nutritional status of Mozambican school-aged children and adolescents. PLos ONE 2014, 9. [Google Scholar] [CrossRef]
- Van Nassau, F.; Singh, A.S.; Van Mechelen, W.; Brug, J.; Chinapaw, M.J.M. Body mass index, waist circumference and skin-fold thickness in 12- to 14-year-old Dutch adolescents: Differences between 2006 and 2011. Pediatr. Obes. 2014, 9, e137–e140. [Google Scholar] [CrossRef] [PubMed]
- Stamatakis, E.; Zaninotto, P.; Falaschetti, E.; Mindel, J.; Head, J. Time trends in childhood and adolescent obesity in England from 1995 to 2007 and projections of prevalence to 2015. J. Epidemiol. Community Health 2010, 64, 167–174. [Google Scholar] [CrossRef] [PubMed]
- Sigmundová, D.; Sigmund, E.; Hamrik, Z.; Kalman, M. Trends of overweight and obesity, physical activity and sedentary behaviour in Czech schoolchildren: HBSC study. Eur. J. Public Health 2014, 24, 210–215. [Google Scholar] [CrossRef] [PubMed]
- Wijnhoven, T.M.A.; Van Raaij, J.M.A.; Spinelli, A.; Starc, G.; Hassapidou, M.; Spiroski, I.; Rutter, H.; Martos, E.; Rito, A.I.; Hovengen, R.; et al. WHO European Childhood Obesity Surveillance Initiative: Body mass index and level of overweight among 6–9-year-old children from school year 2007/2008 to school year 2009/2010. BMC Public Health 2014, 14. [Google Scholar] [CrossRef] [PubMed]
- Marques, D.; De Matos, M.G. Trends and correlates of overweight and obesity among adolescents from 2002 to 2010: A three-cohort study on a representative sample of Portuguese adolescents. Am. J. Hum. Biol. 2014, 26, 844–849. [Google Scholar] [CrossRef] [PubMed]
- Ogden, C.L.; Carroll, M.D.; Kit, B.K.; Flegal, K.M. Prevalence of obesity and trends in body mass index among US children and adolescents, 1999–2010. J. Am. Med. Assoc. 2012, 307, 483–490. [Google Scholar] [CrossRef] [PubMed]
- Olds, T.; Maher, C.; Zumin, S.; Péneau, S.; Lioret, S.; Castetbon, K.; Bellisle; de Wilde, J.; Hohepa, M.; Maddison, R.; et al. Evidence that the prevalence of childhood overweight is plateauing: Data from nine countries. Int. J. Pediatr. Obes. 2011, 6, 342–360. [Google Scholar] [CrossRef] [PubMed]
- Moraeus, L.; Lissner, L.; Sjöberg, A. Stable prevalence of obesity in Swedish schoolchildren from 2008 to 2013 but widening socio-economic gap in girls. Acta Paediatr. 2014, 103, 1277–1284. [Google Scholar] [CrossRef] [PubMed]
- Keane, E.; Kearney, P.M.; Perry, I.; Kelleher, C.C.; Harrington, M. Trends and prevalence of overweight and obesity in primary school aged children in the Republic of Ireland from 2002–2012: A systematic review. BMC Public Health 2014, 14. [Google Scholar] [CrossRef] [PubMed]
- Lissner, L.; Sohlström, A.; Sundblom, E.; Sjöberg, A. Trends in overweight and obesity in Swedish schoolchildren 1999–2005: Has the epidemic reached a plateau? Obes. Rev. 2010, 11, 553–559. [Google Scholar] [CrossRef] [PubMed]
- Iannoti, R.J.; Wang, J. Trends in physical activity, sedentary behaviour, diet, and BMI among US adolescents, 2001–2009. Pediatrics 2013, 132, 606–614. [Google Scholar] [CrossRef] [PubMed]
- Ahluwalia, N.; Dalmasso, P.; Rasmussen, M.; Lipsky, L.; Currie, C.; Haug, E.; Kelly, C.; Damsgaard, M.T.; Due, P.; Tabak, I.; et al. Trends in overweight prevalence among 11-, 13- and 15-year-olds in 25 countries in Europe, Canada and USA from 2002 to 2010. Eur. J. Public Health 2014, 24, 28–32. [Google Scholar] [CrossRef] [PubMed]
- Katzmarzyk, P.T.; Barreira, T.V.; Broyles, S.T.; Champagne, C.M.; Chaput, J.P.; Fogelholm, M.; Hu, G.; Johnson, W.D.; Kuriyan, R.; Kurpad, A.; et al. The international study of childhood obesity, lifestyle and the environment (ISCOLE): Design and methods. BMC Public Health 2013, 13. [Google Scholar] [CrossRef] [PubMed]
- Parikh, T.; Stratton, G. Influence of intensity of physical activity on adiposity and cardiorespiratory fitness in 5–18 year olds. Sports Med. 2011, 41, 477–488. [Google Scholar] [CrossRef] [PubMed]
- Ness, A.R.; Leary, S.D.; Mattocks, C.; Blair, S.N.; Reilly, J.J.; Wells, J.; Ingle, S.; Tilling, K.; Smith, G.D.; Riddoch, C. Objectively measured physical activity and fat mass in a large cohort of children. PLos Med. 2007, 4, 476–484. [Google Scholar] [CrossRef] [PubMed]
- White, J.; Jago, R. Prospective associations between physical activity and obesity among adolescent girls. Arch. Pediatr. Adolesc. Med. 2012, 166, 522–527. [Google Scholar] [CrossRef] [PubMed]
- Lissner, L.; Lanfer, A.; Gwozdz, W.; Olafsdottir, S.; Eiben, G.; Moreno, L.A.; Santaliestra-Pasías, A.M.; Kovács, E.; Barba, G.; Loit, H.M.; et al. Television habits in relation to overweight, diet and taste preferences in European children: The IDEFICS study. Eur. J. Epidemiol. 2012, 27, 705–715. [Google Scholar] [CrossRef] [PubMed]
- Sigmundová, D.; El Ansari, W.; Sigmund, E.; Frömel, K. Secular trends: A ten-year comparison of the amount and type of physical activity and inactivity of random samples of adolescents in the Czech Republic. BMC Public Health 2011, 11. [Google Scholar] [CrossRef] [PubMed]
- Kalman, M.; Inchley, J.; Sigmundová, D.; Iannotti, R.J.; Tynjälä, J.A.; Hamrik, Z.; Haug, E.; Bucksch, J. Secular trends in moderate-to-vigorous physical activity in 32 countries from 2002 to 2010: A cross-national perspective. Eur. J. Public Health 2015, 24, 37–40. [Google Scholar] [CrossRef] [PubMed]
- Dos Santos, F.K.; Maia, J.A.R.; Gomes, T.N.Q.F.; Daca, T.; Madeira, A.; Damasceno, A.; Katzmarzyk, P.T.; Prista, A. Secular trends in habitual physical activities of Mozambican children and adolescents from Maputo city. Int. J. Environ. Res. Public Health 2014, 11, 10940–10950. [Google Scholar] [CrossRef] [PubMed]
- Raustorp, A.; Ekroth, Y. Eight-year secular trends of pedometer-determined physical activity in young Swedish adolescents. J. Phys. Act. Health 2010, 7, 369–374. [Google Scholar] [PubMed]
- Eithdóttir, S.T.; Kristjánsson, Á.L.; Sigfúsdóttir, I.D.; Allegrante, J.P. Trends in physical activity and participation in sports clubs among Icelandic adolescents. Eur. J. Public. Health 2008, 18, 289–293. [Google Scholar] [CrossRef] [PubMed]
- Bassett, D.R.; John, D.; Conger, S.A.; Fitzhugh, E.C.; Coe, D.P. Trends in physical activity and sedentary behaviors of U.S. youth. J. Phys. Act. Health 2014. [Google Scholar] [CrossRef] [PubMed]
- Bucksch, J.; Inchley, J.; Hamrik, Z.; Finne, E.; Kolip, Z.; HBSC Study Group Germany. Trends in television time, non-gaming PC use and moderate-to-vigorous physical activity among German adolescents 2002–2010. BMC Public Health 2014, 14. [Google Scholar] [CrossRef] [PubMed]
- Lopes, A.S.; Silva, K.S.; Filho, V.C.B.; Bezerra, J.; De Oliveira, E.S.A.; Nahas, M.V. Trends in screen time on week and weekend days in a representative sample of Southern Brazil students. J. Public Health 2014, 36, 608–614. [Google Scholar] [CrossRef] [PubMed]
- Cui, Z.; Hardy, L.L.; Dibley, M.J.; Bauman, A. Temporal trends and recent correlates in sedentary behaviours in Chinese children. Int. J. Behav. Nutr. Phys. Act. 2011, 8. [Google Scholar] [CrossRef] [PubMed]
- Lehnert, T.; Sonntag, D.; Konnopka, A.; Riedel-Heller, S.; König, H.H. Economic costs of overweight and obesity. Best Pract. Res. Clin. Endocrinol. Metable 2013, 27, 105–115. [Google Scholar] [CrossRef] [PubMed]
- Von Lengerke, T.; Krauth, C. Economic costs of adult obesity: A review of recent European studies with a focus on subgroup-specific costs. Maturitas 2011, 69, 220–229. [Google Scholar] [CrossRef] [PubMed]
- Herman, K.M.; Craig, C.L.; Gauvin, L.; Katzmarzyk, P.T. Tracking of obesity and physical activity from childhood to adulthood: The Physical Activity Longitudinal Study. Int. J. Pediatr. Obes. 2009, 4, 281–288. [Google Scholar] [CrossRef] [PubMed]
- Wennberg, P.; Gustafsson, P.E.; Howard, B.; Wennberg, M.; Hammarström, A. Television viewing over the life course and the metabolic syndrome in mid-adulthood: A longitudinal population-based study. J. Epidemiol. Community Health 2014, 68, 928–933. [Google Scholar] [CrossRef] [PubMed]
- Rangul, V.; Bauman, A.; Holmen, T.L.; Midthjell, K. Is physical activity maintenance from adolescence to young adulthood associated with reduced CVD risk factors, improved mental health and satisfaction with life: The HUNT Study, Norway. Int. J. Behav. Nutr. Phys. Act. 2012, 9. [Google Scholar] [CrossRef] [PubMed]
- Sigmund, E.; El Ansari, W.; Sigmundová, D. Does school-based physical activity decrease overweight and obesity in children aged 6–9 years? A two-year non-randomized longitudinal intervention study in the Czech Republic. BMC Public Health 2012, 12. [Google Scholar] [CrossRef] [PubMed]
- Sigmund, E.; Sigmundová, D. Longitudinal 2-year follow-up on the effect of a non-randomised school-based physical activity intervention on reducing overweight and obesity of Czech children aged 10–12 years. Int. J. Environ. Res. Public Health 2013, 10, 3667–3683. [Google Scholar] [CrossRef] [PubMed]
- Webber, L.; Kilpi, F.; Marsh, T.; Rtveladze, K.; McPherson, K.; Brown, M. Modelling obesity trends and related diseases in Eastern Europe. Obes. Rev. 2012, 13, 744–751. [Google Scholar] [CrossRef] [PubMed]
- Currie, C.; Nic Gabhainn, S.; Godeau, E.; The International HBSC Network Coordinating Committee. The Health Behaviour in School-aged Children. WHO Collaborative Cross-National (HBSC) study: Origins, concept, history and development 1982–2008. Int. J. Public Health 2009, 54, 131–139. [Google Scholar] [CrossRef] [PubMed]
- Roberts, C.; Freeman, J.; Samdal, O.; Schnohr, C.W.; Looze, M.; Nic Gabhainn, S.; Iannotti, R.; Rasmussen, M.; the International HBSC Study Group. The Health Behaviour in School-aged Children (HBSC) study: Methodological developments and current tensions. Int. J. Public Health 2009, 54, 140–150. [Google Scholar] [CrossRef] [PubMed]
- Fonseca, H.; Silva, A.M.; Matos, M.G.; Esteves, I.; Costa, P.; Guerra, A.; Gomes-Pedro, J. Validity of BMI based on self-reported weight and height in adolescents. Acta Paediatr. 2010, 99, 83–88. [Google Scholar] [CrossRef] [PubMed]
- WHO. Growth Reference Data for 5–19 Years. WHO Reference 2007. Available online: http://www.who.int/growthref/en (accessed on 18 July 2015).
- Prochaska, J.J.; Sallis, J.F.; Long, B. A physical activity screening measure for use with adolescents in primary care. Arch. Pediatr. Adolesc. Med. 2001, 155, 554–559. [Google Scholar] [CrossRef] [PubMed]
- Ridgers, N.D.; Timperio, A.; Crawford, D.; Salmon, J. Validity of a brief self-report instrument for assessing compliance with physical activity guidelines amongst adolescents. J. Sci. Med. Sport 2012, 15, 136–141. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Wang, M.; Tynjälä, J.; Lv, Y.; Villberg, J.; Zhang, Z.; Kannas, L. Test-retest reliability of selected items of Health Behaviour in School-aged Children (HBSC) survey questionnaire in Beijing, China. BMC Med. Res. Methodol. 2010, 10. [Google Scholar] [CrossRef] [PubMed]
- Bobakova, D.; Hamrik, Z.; Badura, P.; Sigmundova, D.; Nalecz, H.; Kalman, M. Test-retest reliability of selected physical activity and sedentary behaviour HBSC items in the Czech Republic, Slovakia and Poland. Int. J. Public Health 2015, 60, 59–67. [Google Scholar] [CrossRef] [PubMed]
- Janssen, I.; Leblanc, A.G. Systematic review of the health benefits of physical activity and fitness in school-aged children and youth. Int. J. Behav. Nutr. Phys. Act. 2011, 7. [Google Scholar] [CrossRef]
- Tremblay, M.S.; Warburton, D.E.R.; Janssen, I.; Paterson, D.H.; Latimer, A.E.; Rhodes, R.E.; Kho, M.E.; Hicks, A.; LeBlanc, A.G.; Zehr, L.; et al. New Canadian physical activity guidelines. Appl. Physiol. Nutr. Metable 2011, 36, 36–46. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Global Recommendations on Physical Activity for Health. Geneva, Switzerland: World Health Organization, 2010. Available online: http://www.who.int/dietphysicalactivity/factsheet_recommendations/en/ (accessed on 18 July 2015).
- Schmitz, K.H.; Harnack, L.; Fulton, J.E.; Jacobs, D.R., Jr.; Gao, S.; Lytle, L.A.; Van Coevering, P. Reliability and validity of a brief questionnaire to assess television viewing and computer use by middle school children. J. Sch. Health 2004, 74, 370–377. [Google Scholar] [CrossRef] [PubMed]
- Vereecken, C.A.; Todd, J.; Roberts, C.; Mulvihill, C.; Maes, L. Television viewing behaviour and associations with food habits in different countries. Public Health Nutr. 2006, 9, 244–250. [Google Scholar] [CrossRef] [PubMed]
- Rey-López, J.P.; Vicente-Rodriguez, G.; Ortega, F.B.; Ruiz, J.R.; Martinez-Gómez, D.; De Henauw, S.; Manios, Y.; Molnar, D.; Polito, A.; Verloigne, M.; et al. Sedentary patterns and media availability in European adolescents: The HELENA study. Prev. Med. 2010, 51, 50–55. [Google Scholar] [CrossRef] [PubMed]
- Lau, D.C.W.; Douketis, J.D.; Morrison, K.M.; Hramiak, I.M.; Sharma, A.M.; Ur, E. Obesity Canada Clinical Practice Expert Panel. 2006 Canadian clinical practice guidelines on the management and prevention of obesity in adults and children [summary]. Can. Med. Assoc. J. 2007, 176, S1–S13. [Google Scholar] [CrossRef] [PubMed]
- Committee on Public Education. Children, adolescents, and television. Pediatrics 2001, 107, 423–426. [Google Scholar]
- Tremblay, M.S.; LeBlanc, A.G.; Kho, M.E.; Saunders, T.J.; Larouche, R.; Colley, R.C.; Goldfield, G.; Gorber, S.C. Systematic review of sedentary behaviour and health indicators in school-aged children and youth. Int. J. Behav. Nutr. Phys. Act. 2011, 8. [Google Scholar] [CrossRef] [PubMed]
- Branca, F.; Nikogosian, H.; Lobstein, T. The Challenge of Obesity in the WHO European Region and the Strategies for Response: Summary. Organization Regional Office for Europe: Copenhagen, Denmark, 2007. Available online: http://www.euro.who.int/__data/assets/pdf_file/0008/98243/E89858.pdf?ua=1 (accessed on 18 July 2015).
- Knai, C.; Suhrcke, M.; Lobstein, T. Obesity in Eastern Europe: An overview of its health and economic implication. Econ. Hum. Biol. 2007, 5, 392–408. [Google Scholar] [CrossRef] [PubMed]
- Liang, Y.J.; Xi, B.; Song, A.Q.; Liu, J.X.; Mi, J. Trends in general and abdominal obesity among Chinese children and adolescents 1993–2009. Pediatr. Obes. 2012, 7, 355–364. [Google Scholar] [CrossRef] [PubMed]
- Raustorp, A.; Svensson, K.; Perlinger, T. Tracking of pedometer-determined physical activity: A 5-year follow-up study of adolescents in Sweden. Pediatr. Exerc. Sci. 2007, 19, 228–238. [Google Scholar] [PubMed]
- Lätt, E.; Mäestu, J.; Ortega, F.B.; Rääsk, T.; Jürimäe, T.; Jürimäe, J. Vigorous physical activity rather than sedentary behaviour predicts overweight and obesity in pubertal boys: A 2-year follow-up study. Scan. J. Public Health 2015, 43, 276–282. [Google Scholar] [CrossRef] [PubMed]
- Guttin, B.; Yin, Z.; Humphries, M.C.; Barbeau, P. Relations of moderate and vigorous physical activity to fitness and fatness in adolescents. Am. J. Clin. Nutr. 2005, 81, 746–750. [Google Scholar]
- Patrick, K.; Norman, G.J.; Calfas, K.J.; Sallis, J.F.; Zabinski, M.F.; Rupp, J.; Cella, J. Diet, physical activity, and sedentary behaviors as risk factors for overweight in adolescence. Arch. Pediatr. Adolesc. Med. 2004, 158, 385–390. [Google Scholar] [CrossRef] [PubMed]
- Zahner, L.; Muehlbauer, T.; Schmid, M.; Meyer, U.; Puder, J.J.; Kriemler, S. Association of sports club participation with fitness and fatness in children. Med. Sci. Sports Exerc. 2009, 41, 344–350. [Google Scholar] [CrossRef] [PubMed]
- Golle, K.; Granacher, U.; Hoffman, M.; Wick, D.; Muehlbauer, T. Effect of living area and sports club participation on physical fitness in children: A 4 year longitudinal study. BMC Public Health 2014, 14. [Google Scholar] [CrossRef] [PubMed]
- Drenowatz, C.; Steiner, R.P.; Brandstetter, S.; Klenk, J.; Wabitsch, M.; Steinacker, M. Organized sport, overweight, and physical fitness in primary school children in Germany. J. Obes. 2013, 2013. [Google Scholar] [CrossRef] [PubMed]
- Basterfield, L.; Reilly, J.K.; Pearce, M.S.; Parkinson, K.N.; Adamson, A.J.; Reilly, J.J.; Vella, S.A. Longitudinal associations between sports participation, body composition and physical activity from childhood to adolescence. J. Sci. Med. Sport 2014, 18, 178–182. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, J.A.; Pate, R.R.; Nader, P.R. Time spent in sedentary behavior and changes in childhood BMI: A longitudinal study from ages 9 to 15 years. Int. J. Obes. 2013, 37, 54–60. [Google Scholar] [CrossRef] [PubMed]
- Madden, M.; Lenhart, A.; Duggan, M.; Cortesi, S.; Gasser, U. Teen and Technology. Washington, DC: Pew Internet & American Life Project, 2013. Available online: http://www.pewinternet.org/Reports/2013/Teens-and-Tech.aspx. (accessed 18 Mar 2015).
- Hysing, M.; Pallesen, S.; Stormark, K.M.; Jakobsen, R.; Lundervold, A.J.; Sivertsen, B. Sleep and use of electronic devices in adolescence: Results from a large population-based study. BMJ Open 2015, 5. [Google Scholar] [CrossRef] [PubMed]
- Ekelund, U.; Luan, J.; Sherar, L.B.; Esliger, D.W.; Griew, P.; Cooper, A. Moderate to vigorous physical activity and sedentary time and cardiometabolic risk factors in children and adolescents. J. Am. Med. Assoc. 2012, 307, 704–712. [Google Scholar] [CrossRef] [PubMed]
- Chaput, J.P.; Saunders, T.J.; Mathieu, M.-È.; Henderson, M.; Tremblay, M.S.; O’Loughlin, J.; Tremblay, A. Combined associations between moderate to vigorous physical activity and sedentary behaviour with cardiometabolic risk factors in children. Appl. Physiol. Nutr. Metab 2013, 38, 477–483. [Google Scholar] [CrossRef] [PubMed]
- Ekelund, U.; Brage, S.; Froberg, K.; Harro, M.; Anderssen, S.A.; Sardinha, L.B.; Riddoch, C.; Andersen, L.B. TV viewing and physical activity are independently associated with metabolic risk in children: The European Youth Heart Study. PLoS. Med. 2006, 3. [Google Scholar] [CrossRef] [PubMed]
- Fakhouri, T.H.I.; Hughes, J.P.; Brody, J.D.; Kit, B.K.; Ogden, C.L. Physical activity and screen-time viewing among elementary school-aged children in the United States from 2009 to 2010. JAMA Pediatr. 2013, 167, 223–229. [Google Scholar] [CrossRef] [PubMed]
- Brug, J.; Te Velde, S.J.; Chinapaw, M.J.M.; Bere, E.; De Bourdeaudhuij, I.M.M.; Moore, H.; Maes, L.; Jensen, J.; Manios, Y.; Lien, N.; et al. Evidence-based development of school-based and family-involved prevention of overweight across Europe: The ENERGY-project’s design and conceptual framework. BMC Public Health 2010, 10. [Google Scholar] [CrossRef] [PubMed]
- Brug, J.; Van Stralen, M.M.; Te Velde, S.J.; Chinapaw, M.J.M.; De Bourdeaudhuij, I.; Lien, N.; Bere, E.; Maskini, V.; Singh, A.S.; Maes, L.; et al. Difference in weight status and energy-balance related behaviors among schoolchildren across Europe: The ENERGY-project. PLoS ONE 2014, 7. [Google Scholar] [CrossRef] [PubMed]
- Simon, C.; Schweitzer, B.; Oujaa, M.; Wagner, A.; Arveiler, D.; Triby, E.; Copi, N.; Blanc, S.; Platat, C. Successful overweight prevention in adolescents by increasing physical activity: A 4-year randomized controlled intervention. Int. J. Obes. 2008, 32, 1489–1498. [Google Scholar] [CrossRef] [PubMed]
- Simon, C.; Kellou, N.; Dugas, J.; Platat, C.; Copin, N.; Schweitzer, B.; Hausser, F.; Bergouignan, A.; Lefai, E.; Blanc, S. A socio-ecological approach promoting physical activity and limiting sedentary behaviour in adolescence showed weight benefits maintained 2.5 years after intervention cessation. Int. J. Obes. 2014, 38, 936–943. [Google Scholar] [CrossRef] [PubMed]
- Telama, R.; Yang, X.; Viikari, J.; Välimäki, I.; Wanne, O.; Raitakari, O. Physical activity from childhood to adulthood: A 21-year tracking study. Am. J. Prev. Med. 2005, 28, 267–273. [Google Scholar] [CrossRef] [PubMed]
- Craigie, A.M.; Lake, A.A.; Kelly, S.A.; Adamson, A.J.; Mathers, J.C. Tracking of obesity-related behaviours from childhood to adulthood: A systematic review. Maturitas 2011, 70, 266–284. [Google Scholar] [CrossRef] [PubMed]
- Adamo, K.B.; Prince, S.A.; Tricco, A.C.; Connor-Gorber, S.; Tremblay, M. A comparison of indirect versus direct measures for assessing physical activity in the pediatric population: A systematic review. Int. J. Pediatr. Obes. 2009, 4, 2–27. [Google Scholar] [CrossRef] [PubMed]
- Armstrong, N.; Welsman, J.R. The physical activity patterns of European youth with reference to methods of assessment. Sports Med. 2006, 36, 1067–1086. [Google Scholar] [CrossRef] [PubMed]
- Lindsay, R.S.; Hanson, R.L.; Roumain, J.; Ravussin, E.; Knowler, W.C.; Tataranni, P.A. Body mass index as a measure of adiposity in children and adolescents: Relationship to adiposity by dual energy X-ray absorptiometry and to cardiovascular risk factors. J. Clin. Endocrinol. Metab. 2001, 86, 4061–4067. [Google Scholar] [CrossRef] [PubMed]
- Freedman, D.S.; Sherry, B. The validity of BMI as an indicator of body fatness and risk among children. Pediatrics 2009, 124, 23–34. [Google Scholar] [CrossRef] [PubMed]
- Elgar, F.J.; Stewart, J.M. Validity of self-report screening for overweight and obesity: Evidence from the Canadian Community Health Survey. Can. J. Public. Health 2008, 99, 423–427. [Google Scholar] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sigmund, E.; Sigmundová, D.; Badura, P.; Kalman, M.; Hamrik, Z.; Pavelka, J. Temporal Trends in Overweight and Obesity, Physical Activity and Screen Time among Czech Adolescents from 2002 to 2014: A National Health Behaviour in School-Aged Children Study. Int. J. Environ. Res. Public Health 2015, 12, 11848-11868. https://doi.org/10.3390/ijerph120911848
Sigmund E, Sigmundová D, Badura P, Kalman M, Hamrik Z, Pavelka J. Temporal Trends in Overweight and Obesity, Physical Activity and Screen Time among Czech Adolescents from 2002 to 2014: A National Health Behaviour in School-Aged Children Study. International Journal of Environmental Research and Public Health. 2015; 12(9):11848-11868. https://doi.org/10.3390/ijerph120911848
Chicago/Turabian StyleSigmund, Erik, Dagmar Sigmundová, Petr Badura, Michal Kalman, Zdenek Hamrik, and Jan Pavelka. 2015. "Temporal Trends in Overweight and Obesity, Physical Activity and Screen Time among Czech Adolescents from 2002 to 2014: A National Health Behaviour in School-Aged Children Study" International Journal of Environmental Research and Public Health 12, no. 9: 11848-11868. https://doi.org/10.3390/ijerph120911848
APA StyleSigmund, E., Sigmundová, D., Badura, P., Kalman, M., Hamrik, Z., & Pavelka, J. (2015). Temporal Trends in Overweight and Obesity, Physical Activity and Screen Time among Czech Adolescents from 2002 to 2014: A National Health Behaviour in School-Aged Children Study. International Journal of Environmental Research and Public Health, 12(9), 11848-11868. https://doi.org/10.3390/ijerph120911848







