Enzyme-Aided Extraction of Fucoidan by AMG Augments the Functionality of EPCs through Regulation of the AKT/Rheb Signaling Pathway
Abstract
1. Introduction
2. Results
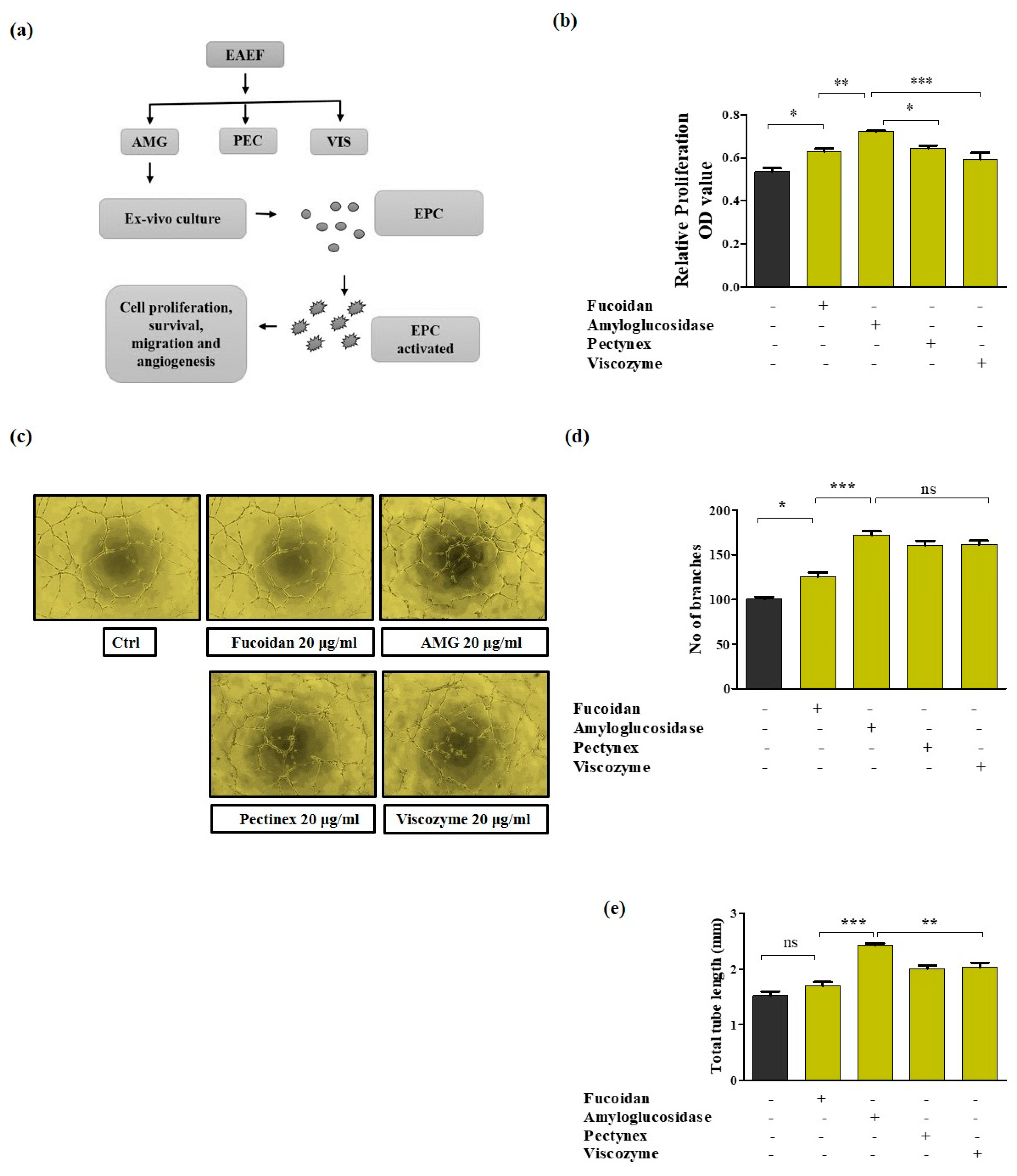
2.1. Development of Enzyme-Aided Extraction Protocols of Fucoidan
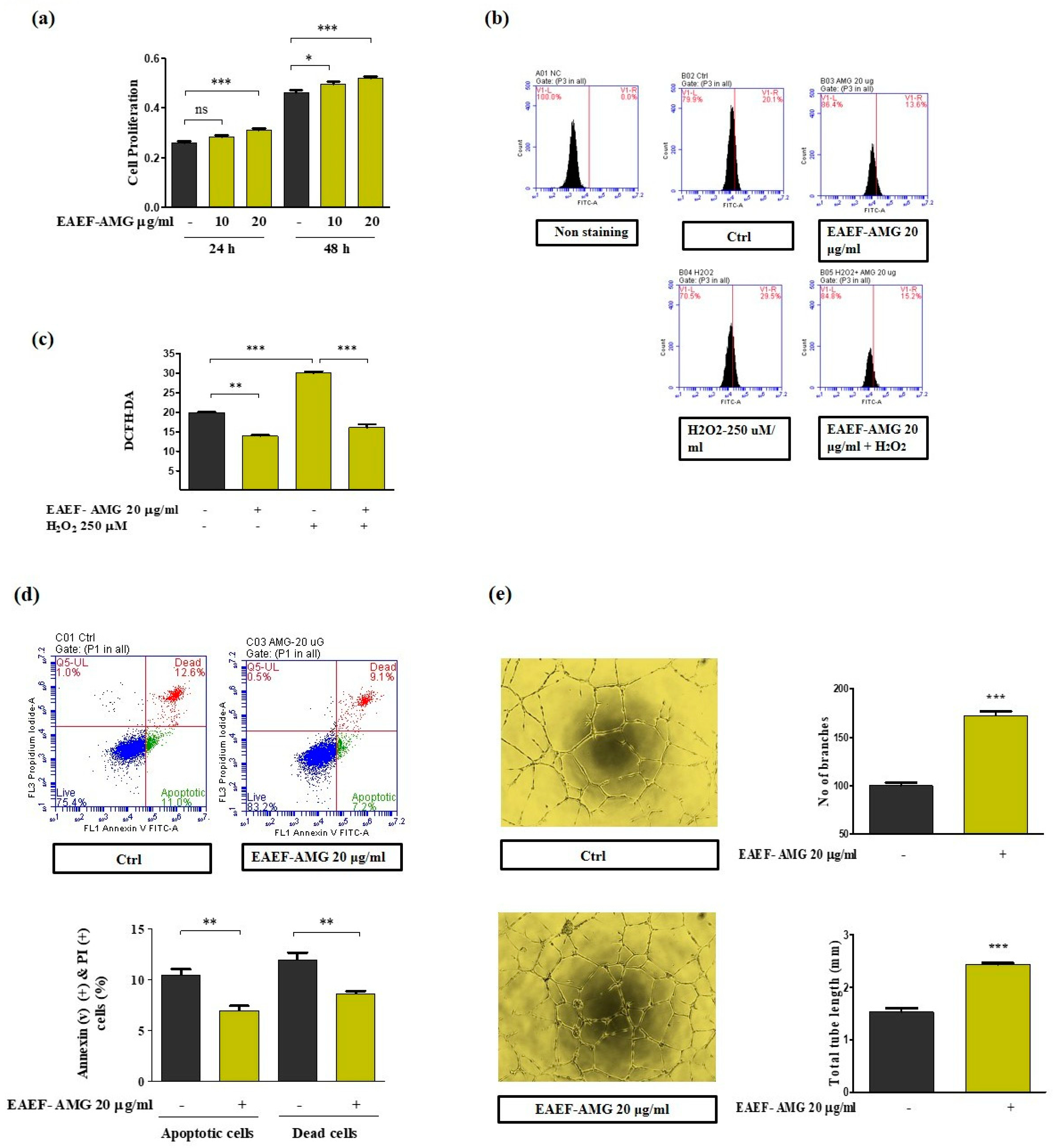
2.2. Priming of EAEF-AMG Protects EPCs Bioactivities from ROS Stress and Cell Apoptosis
2.3. Priming of EAEF-AMG Enhances Angiogenic Activity in EPCs
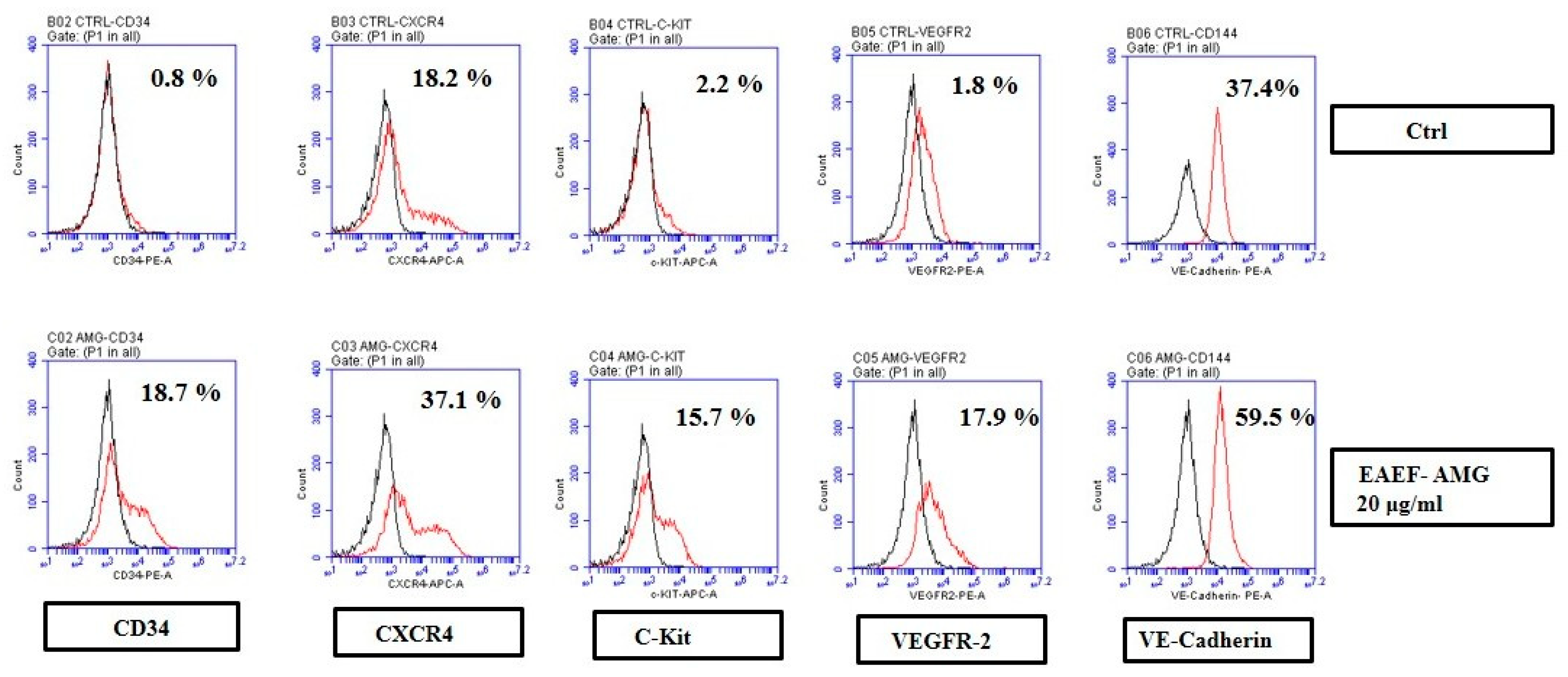
2.4. Priming of EAEF-AMG Enriches Functional EPCs
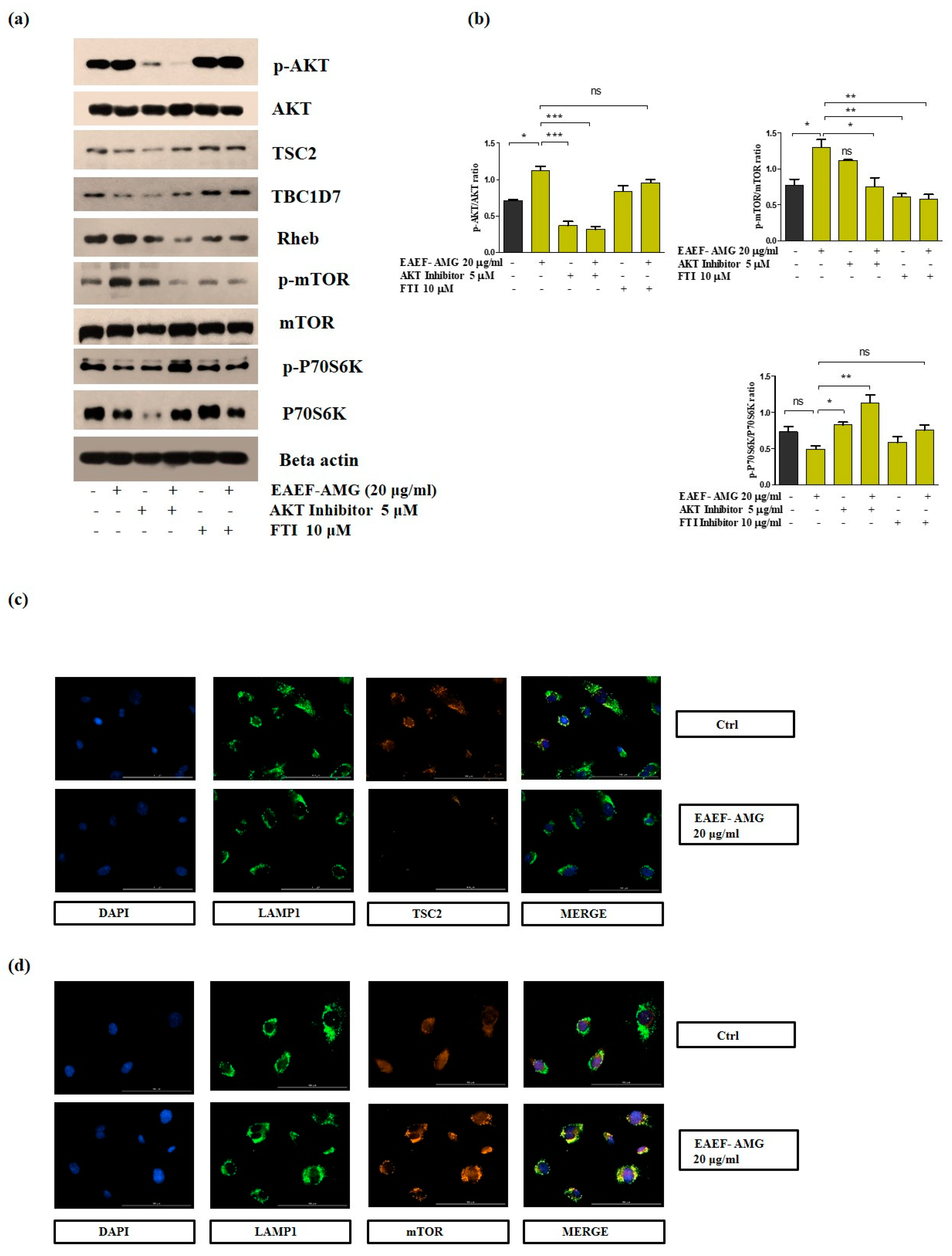
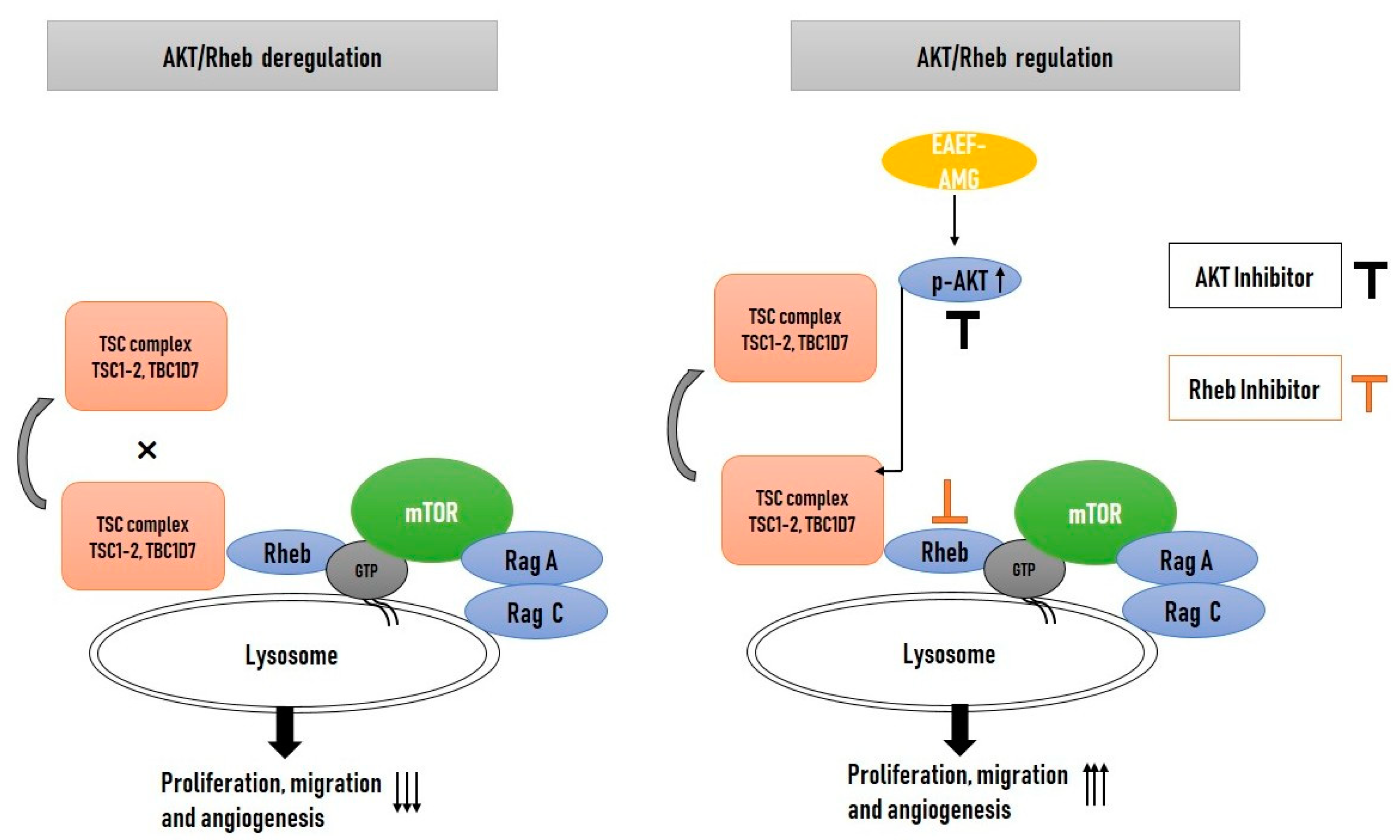
2.5. Priming of EAEF-AMG Regulates AKT/Rheb Signaling in EPCs
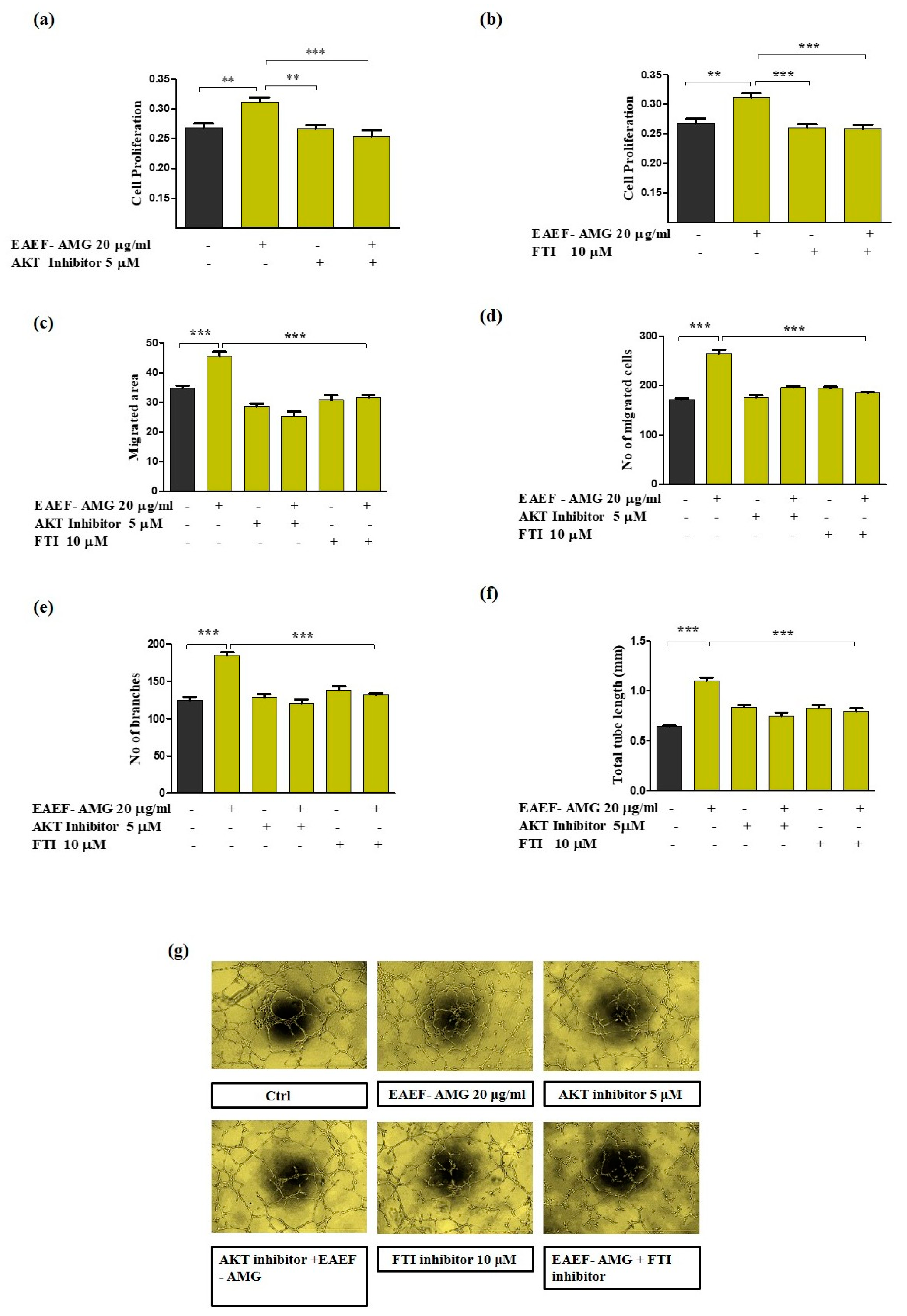
2.6. Priming of EAEF-AMG Augments the Functional Activities of EPC via Regulation of AKT/Rheb Signaling
3. Discussion
4. Materials and Methods
4.1. Isolation of EPCs and Cell Culture
4.2. Enzymatic Extraction of Fucoidan
4.3. Flow Cytometer Analysis
4.4. WST-1 Proliferation Assay
4.5. Carboxy-H2DFFDA Assay
4.6. Annexin V FITC/PI Staining Assay
4.7. Transwell Migration Assay
4.8. Scratch Wound Healing Assay
4.9. Matrigel Tube Formation Assay
4.10. Western Blotting
4.11. Immunofluorescence
4.12. Quantitative Reverse Transcription-Polymerase Chain Reaction
4.13. Statistical Analysis
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Kivimaki, M.; Steptoe, A. Effects of stress on the development and progression of cardiovascular disease. Nat. Rev. Cardiol. 2018, 15, 215–229. [Google Scholar] [CrossRef] [PubMed]
- Duncker, D.J.; Koller, A.; Merkus, D.; Canty, J.M., Jr. Regulation of coronary blood flow in health and ischemic heart disease. Prog. Cardiovasc. Dis. 2015, 57, 409–422. [Google Scholar] [CrossRef] [PubMed]
- Yu, P.; Zhang, Z.; Li, S.; Wen, X.; Quan, W.; Tian, Q.; Chen, J.; Zhang, J.; Jiang, R. Progesterone modulates endothelial progenitor cell (EPC) viability through the CXCL12/CXCR4/PI3K/Akt signalling pathway. Cell Prolif. 2016, 49, 48–57. [Google Scholar] [CrossRef] [PubMed]
- Masuda, H.; Alev, C.; Akimaru, H.; Ito, R.; Shizuno, T.; Kobori, M.; Horii, M.; Ishihara, T.; Isobe, K.; Isozaki, M.; et al. Methodological development of a clonogenic assay to determine endothelial progenitor cell potential. Circ. Res. 2011, 109, 20–37. [Google Scholar] [CrossRef] [PubMed]
- Ke, X.; Shu, X.R.; Wu, F.; Hu, Q.S.; Deng, B.Q.; Wang, J.F.; Nie, R.Q. Overexpression of the beta2AR gene improves function and re-endothelialization capacity of EPCs after arterial injury in nude mice. Stem Cell Res. Ther. 2016, 7, 73. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.Y.; Su, C.; Cao, Z.; Xu, S.Y.; Xia, W.H.; Xie, W.L.; Chen, L.; Yu, B.B.; Zhang, B.; Wang, Y.; et al. CXCR7 upregulation is required for early endothelial progenitor cell-mediated endothelial repair in patients with hypertension. Hypertension (Dallas, Tex.: 1979) 2014, 63, 383–389. [Google Scholar] [CrossRef] [PubMed]
- Nollet, E.; Hoymans, V.Y.; Rodrigus, I.R.; De Bock, D.; Dom, M.; Vanassche, B.; Van Hoof, V.O.; Cools, N.; Van Ackeren, K.; Wouters, K.; et al. Bone Marrow-Derived Progenitor Cells Are Functionally Impaired in Ischemic Heart Disease. J. Cardiovasc. Transl. Res. 2016, 9, 266–278. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.H.; Chen, Y.; Zhen, Z.; Yeung, C.K.; Chan, J.; Chan, H.H.; Tse, H.F.; Yiu, K.H. Relation between endothelial progenitor cells and arterial stiffness in patients with psoriasis. J. Dermatol. 2016, 43, 888–893. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.H.; Lee, S.H.; Choi, S.H.; Asahara, T.; Kwon, S.M. The sulfated polysaccharide fucoidan rescues senescence of endothelial colony-forming cells for ischemic repair. Stem Cells (Dayton, Ohio) 2015, 33, 1939–1951. [Google Scholar] [CrossRef]
- Kim, E.A.; Lee, S.H.; Ko, C.I.; Cha, S.H.; Kang, M.C.; Kang, S.M.; Ko, S.C.; Lee, W.W.; Ko, J.Y.; Lee, J.H.; et al. Protective effect of fucoidan against AAPH-induced oxidative stress in zebrafish model. Carbohydr. Polym. 2014, 102, 185–191. [Google Scholar] [CrossRef]
- Ma, A.; Wang, L.; Gao, Y.; Chang, Z.; Peng, H.; Zeng, N.; Gui, Y.S.; Tian, X.; Li, X.; Cai, B.; et al. Tsc1 deficiency-mediated mTOR hyperactivation in vascular endothelial cells causes angiogenesis defects and embryonic lethality. Hum. Mol. Gen. 2014, 23, 693–705. [Google Scholar] [CrossRef] [PubMed]
- Menon, S.; Dibble, C.C.; Talbott, G.; Hoxhaj, G.; Valvezan, A.J.; Takahashi, H.; Cantley, L.C.; Manning, B.D. Spatial control of the TSC complex integrates insulin and nutrient regulation of mTORC1 at the lysosome. Cell 2014, 156, 771–785. [Google Scholar] [CrossRef] [PubMed]
- Carroll, B.; Maetzel, D.; Maddocks, O.D.; Otten, G.; Ratcliff, M.; Smith, G.R.; Dunlop, E.A.; Passos, J.F.; Davies, O.R.; Jaenisch, R.; et al. Control of TSC2-Rheb signaling axis by arginine regulates mTORC1 activity. eLife 2016, 5. [Google Scholar] [CrossRef] [PubMed]
- Jacobs, B.L.; McNally, R.M.; Kim, K.J.; Blanco, R.; Privett, R.E.; You, J.S.; Hornberger, T.A. Identification of mechanically regulated phosphorylation sites on tuberin (TSC2) that control mechanistic target of rapamycin (mTOR) signaling. J. Biol. Chem. 2017, 292, 6987–6997. [Google Scholar] [CrossRef] [PubMed]
- Zhang, R.; Li, H.; Zhang, S.; Zhang, Y.; Wang, N.; Zhou, H.; He, H.; Hu, G.; Zhang, T.C.; Ma, W. RXRalpha provokes tumor suppression through p53/p21/p16 and PI3K-AKT signaling pathways during stem cell differentiation and in cancer cells. Cell Death Dis. 2018, 9, 532. [Google Scholar] [CrossRef] [PubMed]
- Tsuji-Tamura, K.; Ogawa, M. Inhibition of the PI3K-Akt and mTORC1 signaling pathways promotes the elongation of vascular endothelial cells. J. Cell Sci. 2016, 129, 1165–1178. [Google Scholar] [CrossRef] [PubMed]
- Incalza, M.A.; D’Oria, R.; Natalicchio, A.; Perrini, S.; Laviola, L.; Giorgino, F. Oxidative stress and reactive oxygen species in endothelial dysfunction associated with cardiovascular and metabolic diseases. Vasc. Pharmacol. 2018, 100, 1–19. [Google Scholar] [CrossRef] [PubMed]
- Dobi, A.; Bravo, S.B.; Veeren, B.; Paradela-Dobarro, B.; Alvarez, E.; Meilhac, O.; Viranaicken, W.; Baret, P.; Devin, A.; Rondeau, P. Advanced glycation end-products disrupt human endothelial cells redox homeostasis: New insights into reactive oxygen species production. Free Radic. Res. 2019, 1–20. [Google Scholar] [CrossRef]
- Masuda, H.; Asahara, T. Post-natal endothelial progenitor cells for neovascularization in tissue regeneration. Cardiovasc. Res. 2003, 58, 390–398. [Google Scholar] [CrossRef]
- Kawamoto, A.; Asahara, T.; Losordo, D.W. Transplantation of endothelial progenitor cells for therapeutic neovascularization. Cardiovasc. Radiat. Med. 2002, 3, 221–225. [Google Scholar] [CrossRef]
- Li, Y.; Chang, S.; Li, W.; Tang, G.; Ma, Y.; Liu, Y.; Yuan, F.; Zhang, Z.; Yang, G.Y.; Wang, Y. cxcl12-engineered endothelial progenitor cells enhance neurogenesis and angiogenesis after ischemic brain injury in mice. Stem Cell Res. Ther. 2018, 9, 139. [Google Scholar] [CrossRef] [PubMed]
- Pysna, A.; Bem, R.; Nemcova, A.; Fejfarova, V.; Jirkovska, A.; Hazdrova, J.; Jude, E.B.; Dubsky, M. Endothelial Progenitor Cells Biology in Diabetes Mellitus and Peripheral Arterial Disease and their Therapeutic Potential. Stem Cell Rev. 2019, 15, 157–165. [Google Scholar] [CrossRef] [PubMed]
- Li, N.; Wang, W.B.; Bao, H.; Shi, Q.; Jiang, Z.L.; Qi, Y.X.; Han, Y. MicroRNA-129-1-3p regulates cyclic stretch-induced endothelial progenitor cell differentiation by targeting Runx2. J. Cell. Biochem. 2019, 120, 5256–5267. [Google Scholar] [CrossRef] [PubMed]
- De la Puente, P.; Muz, B.; Azab, F.; Azab, A.K. Cell trafficking of endothelial progenitor cells in tumor progression. Clin. Cancer Res. Off. J. Am. Assoc. Cancer Res. 2013, 19, 3360–3368. [Google Scholar] [CrossRef] [PubMed]
- Schmidt-Lucke, C.; Rossig, L.; Fichtlscherer, S.; Vasa, M.; Britten, M.; Kamper, U.; Dimmeler, S.; Zeiher, A.M. Reduced number of circulating endothelial progenitor cells predicts future cardiovascular events: Proof of concept for the clinical importance of endogenous vascular repair. Circulation 2005, 111, 2981–2987. [Google Scholar] [CrossRef] [PubMed]
- Chu, K.; Jung, K.H.; Lee, S.T.; Park, H.K.; Sinn, D.I.; Kim, J.M.; Kim, D.H.; Kim, J.H.; Kim, S.J.; Song, E.C.; et al. Circulating endothelial progenitor cells as a new marker of endothelial dysfunction or repair in acute stroke. Stroke 2008, 39, 1441–1447. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Liu, L.; Cui, Y.; Li, X.; Que, X.; Xiao, Y.; Yang, C.; Zhang, J.; Xie, X.; Cowan, P.J.; Tian, J.; et al. Concomitant overexpression of triple antioxidant enzymes selectively increases circulating endothelial progenitor cells in mice with limb ischaemia. J. Cell. Mol. Med. 2019. [Google Scholar] [CrossRef]
- Galasso, G.; Schiekofer, S.; Sato, K.; Shibata, R.; Handy, D.E.; Ouchi, N.; Leopold, J.A.; Loscalzo, J.; Walsh, K. Impaired angiogenesis in glutathione peroxidase-1-deficient mice is associated with endothelial progenitor cell dysfunction. Circ. Res. 2006, 98, 254–261. [Google Scholar] [CrossRef]
- Wang, J.; Chen, S.; Ma, X.; Cheng, C.; Xiao, X.; Chen, J.; Liu, S.; Zhao, B.; Chen, Y. Effects of endothelial progenitor cell-derived microvesicles on hypoxia/reoxygenation-induced endothelial dysfunction and apoptosis. Oxid. Med. Cell. Longev. 2013, 2013, 572729. [Google Scholar] [CrossRef]
- Goligorsky, M.S.; Salven, P. Concise review: Endothelial stem and progenitor cells and their habitats. Stem Cells Transl. Med. 2013, 2, 499–504. [Google Scholar] [CrossRef]
- Guerra, G.; Perrotta, F.; Testa, G. Circulating endothelial progenitor cells biology and regenerative medicine in pulmonary vascular diseases. Curr. Pharm. Biotechnol. 2018, 19, 700–707. [Google Scholar] [CrossRef] [PubMed]
- Li, L.; Liu, H.; Xu, C.; Deng, M.; Song, M.; Yu, X.; Xu, S.; Zhao, X. Vegf promotes endothelial progenitor cell differentiation and vascular repair through connexin 43. Stem Cell Res. Ther. 2017, 24, 237. [Google Scholar] [CrossRef] [PubMed]
- Fang, S.; Wei, J.; Pentinmikko, N.; Leinonen, H.; Salven, P. Generation of functional blood vessels from a single c-kit+ adult vascular endothelial stem cell. PLoS Biol. 2012, 10, e1001407. [Google Scholar] [CrossRef] [PubMed]
- Sabatini, D.M. Twenty-five years of mTOR: Uncovering the link from nutrients to growth. Proc. Natl. Acad. Sci. USA 2017, 114, 11818–11825. [Google Scholar] [CrossRef] [PubMed]
- Sciarretta, S.; Forte, M.; Frati, G.; Sadoshima, J. New Insights into the Role of mTOR Signaling in the Cardiovascular System. Circ. Res. 2018, 122, 489–505. [Google Scholar] [CrossRef] [PubMed]
- Walton, Z.E.; Patel, C.H.; Brooks, R.C.; Yu, Y.; Ibrahim-Hashim, A.; Riddle, M.; Porcu, A.; Jiang, T.; Ecker, B.L.; Tameire, F.; et al. Acid Suspends the Circadian Clock in Hypoxia through Inhibition of mTOR. Cell 2018, 174, 72–87. [Google Scholar] [CrossRef] [PubMed]
- Adalbjornsson, B.V.; Jonsdottir, R. Enzyme-Enhanced Extraction of Antioxidant Ingredients from Algae. Methods Mol. Biol. (Clifton, N.J.) 2015, 1308, 145–150. [Google Scholar] [CrossRef]
- Hammed, A.M.; Jaswir, I.; Amid, A.; Alam, Z.; Asiyanbi-H, T.T.; Ramli, N. Enzymatic Hydrolysis of Plants and Algae for Extraction of Bioactive Compounds. Food Rev. Int. 2013, 29, 352–370. [Google Scholar] [CrossRef]
- Heo, S.J.; Park, E.J.; Lee, K.W.; Jeon, Y.J. Antioxidant activities of enzymatic extracts from brown seaweeds. Bioresour. Technol. 2005, 96, 1613–1623. [Google Scholar] [CrossRef]

© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rethineswaran, V.K.; Kim, Y.-J.; Jang, W.B.; Ji, S.T.; Kang, S.; Kim, D.Y.; Park, J.H.; Van, L.T.H.; Giang, L.T.T.; Ha, J.S.; et al. Enzyme-Aided Extraction of Fucoidan by AMG Augments the Functionality of EPCs through Regulation of the AKT/Rheb Signaling Pathway. Mar. Drugs 2019, 17, 392. https://doi.org/10.3390/md17070392
Rethineswaran VK, Kim Y-J, Jang WB, Ji ST, Kang S, Kim DY, Park JH, Van LTH, Giang LTT, Ha JS, et al. Enzyme-Aided Extraction of Fucoidan by AMG Augments the Functionality of EPCs through Regulation of the AKT/Rheb Signaling Pathway. Marine Drugs. 2019; 17(7):392. https://doi.org/10.3390/md17070392
Chicago/Turabian StyleRethineswaran, Vinoth Kumar, Yeon-Ju Kim, Woong Bi Jang, Seung Taek Ji, Songhwa Kang, Da Yeon Kim, Ji Hye Park, Le Thi Hong Van, Ly Thanh Truong Giang, Jong Seong Ha, and et al. 2019. "Enzyme-Aided Extraction of Fucoidan by AMG Augments the Functionality of EPCs through Regulation of the AKT/Rheb Signaling Pathway" Marine Drugs 17, no. 7: 392. https://doi.org/10.3390/md17070392
APA StyleRethineswaran, V. K., Kim, Y.-J., Jang, W. B., Ji, S. T., Kang, S., Kim, D. Y., Park, J. H., Van, L. T. H., Giang, L. T. T., Ha, J. S., Yun, J., Lee, D. H., Yu, S.-N., Park, S.-G., Ahn, S.-C., & Kwon, S.-M. (2019). Enzyme-Aided Extraction of Fucoidan by AMG Augments the Functionality of EPCs through Regulation of the AKT/Rheb Signaling Pathway. Marine Drugs, 17(7), 392. https://doi.org/10.3390/md17070392





