Intraoperative Hypotension Prediction—A Proactive Perioperative Hemodynamic Management—A Literature Review
Abstract
1. Introduction
2. Intraoperative Hypotension—Definition and Incidence
3. Adverse Events Related to Intraoperative Hypotension
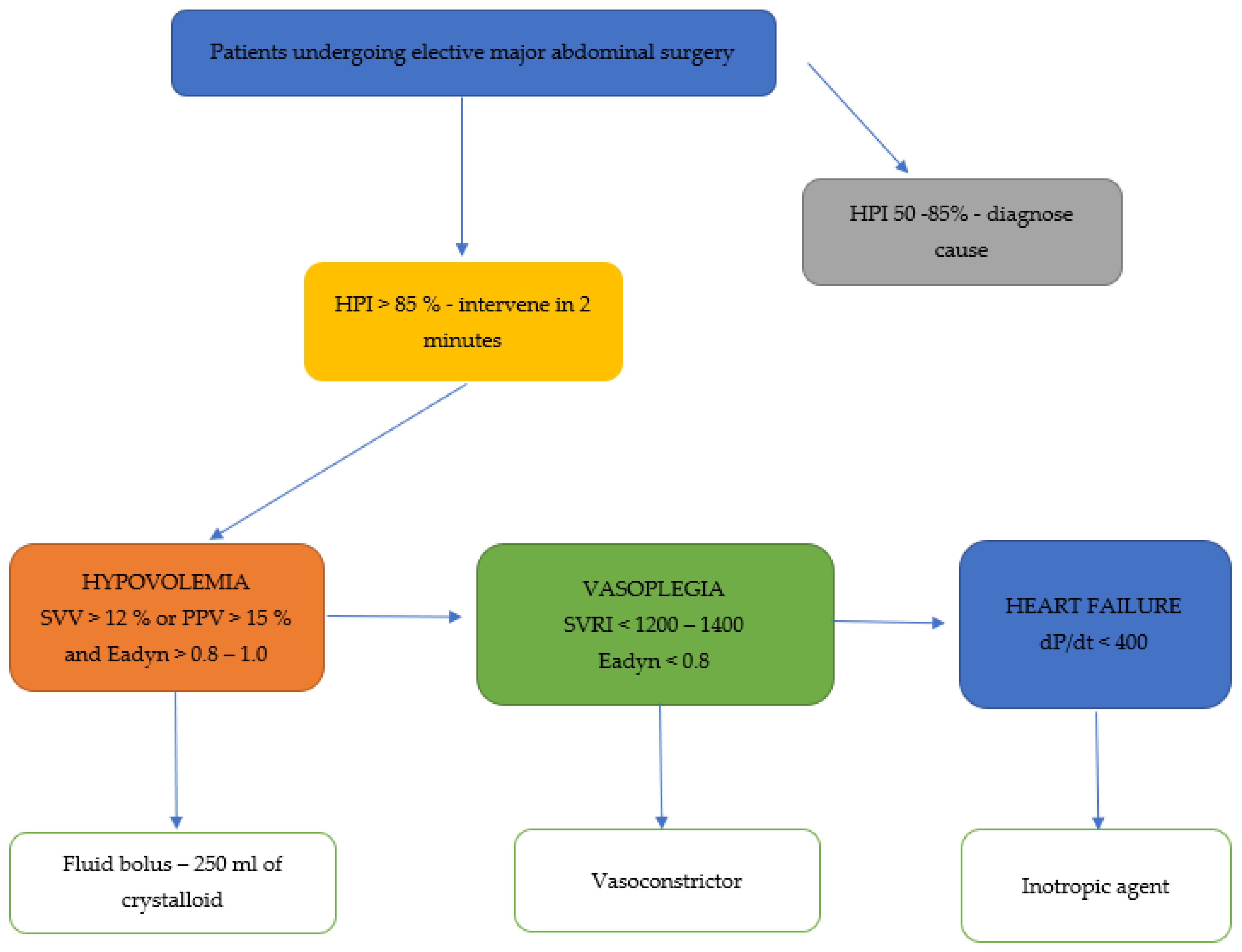
4. Prevention of Hypotension by the Hypotension Prediction Index
5. HPI Clinical Studies
Limitations of the HPI Technology
6. The HPI Future Directions
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Vincent, J.-L.; Pelosi, P.; Pearse, R.; Payen, D.; Perel, A.; Hoeft, A.; Romagnoli, S.; Ranieri, V.M.; Ichai, C.; Forget, P.; et al. Perioperative cardiovascular monitoring of high-risk patients: A consensus of 12. Crit. Care 2015, 19, 224. [Google Scholar] [CrossRef]
- Aseni, P.; Orsenigo, S.; Storti, E.; Pulici, M.; Arlati, S. Current concepts of perioperative monitoring in high-risk surgical patients: A review. Patient Saf. Surg. 2019, 13, 32–39. [Google Scholar] [CrossRef]
- Scheeren, T.W.L.; Saugel, B. Management of Intraoperative Hypotension: Prediction, Prevention and Personalization. Annu. Update Intensive Care Emerg. Med. 2018, 2018, 89–97. [Google Scholar]
- Vos, J.J.; Scheeren, T.W.L. Intraoperative hypotension and its prediction. Indian J. Anaesth. 2019, 63, 877–885. [Google Scholar]
- Wesselink, E.; Kappen, T.; Torn, H.; Slooter, A.; van Klei, W. Intraoperative hypotension and the risk of postoperative adverse outcomes: A systematic review. Br. J. Anaesth. 2018, 121, 706–721. [Google Scholar] [CrossRef]
- Maheshwari, K.; Turan, A.; Mao, G.; Yang, D.; Niazi, A.K.; Agarwal, D.; Sessler, D.I.; Kurz, A. The association of hypotension during non-cardiac surgery, before and after skin incision, with postoperative acute kidney injury: A retrospective cohort analysis. Anaesthesia 2018, 73, 1223–1228. [Google Scholar] [CrossRef]
- Walsh, M.; Devereaux, P.J.; Garg, A.X.; Kurz, A.; Turan, A.; Rodseth, R.N.; Cywinski, J.; Thabane, L.; Sessler, D.I. Relationship between intraoperative mean arterial pressure and clinical outcomes after noncardiac surgery: Toward an empirical definition of hypotension. Anesthesiology 2013, 119, 507–515. [Google Scholar] [CrossRef] [PubMed]
- Salmasi, V.; Maheshwari, K.; Yang, D.; Mascha, E.J.; Singh, A.; Sessler, D.I.; Kurz, A. Relationship between intraoperative hypotension, defined by either reduction from baseline or absolute thresholds, and acute kidney and myocardial injury after noncardiac surgery: A retrospective cohort analysis. Anesthesiology 2017, 126, 47–65. [Google Scholar] [CrossRef] [PubMed]
- Sun, L.Y.; Wijeysundera, D.N.; Tait, G.A.; Beattie, W.S. Association of intraoperative hypotension with acute kidney injury after elective noncardiac surgery. Anesthesiology 2015, 123, 515–523. [Google Scholar] [CrossRef] [PubMed]
- Sessler, D.I.; Khanna, A.K. Perioperative myocardial injury and the contribution of hypotension. Intensive Care Med. 2018, 44, 811–822. [Google Scholar] [CrossRef]
- Hallqvist, L.; Martensson, J.; Granath, F.; Sahlen, A.; Bell, M. Intraoperative hypotension is associated with myocardial damage in noncardiac surgery: An observational study. Eur. J. Anaesthesiol. 2016, 33, 450–456. [Google Scholar] [CrossRef] [PubMed]
- Mascha, E.J.; Yang, D.; Weiss, S.; Sessler, D.I. Intraoperative mean arterial pressure variability and 30-day mortality in patients having noncardiac surgery. Anesthesiology 2015, 123, 79–91. [Google Scholar] [CrossRef] [PubMed]
- Monk, T.G.; Bronsert, M.R.; Henderson, W.G.; Mangione, M.P.; Sum-Ping, S.T.J.; Bentt, D.R.; Nguyen, J.D.; Richman, J.S.; Meguid, R.A.; Hammermeister, K.E. Association between intraoperative hypotension and hypertension and 30-day postoperative mortality in noncardiac surgery. Anesthesiology 2015, 123, 307–319. [Google Scholar] [CrossRef] [PubMed]
- Nagre, A.S. Perioperative stroke-prediction, prevention, and protection. Indian J. Anaesth. 2018, 62, 738–742. [Google Scholar] [CrossRef]
- Bijker, J.B.; Persoon, S.; Peelen, L.M.; Moons, K.G.; Kalkman, C.J.; Kappelle, L.J.; van Klei, W.A. Intraoperative hypotension and perioperative ischemic stroke after general surgery: A nested case-controlstudy. Anesthesiology 2012, 116, 658–664. [Google Scholar] [CrossRef] [PubMed]
- Aya, H.; Cecconi, M.; Hamilton, M.; Rhodes, A. Goal-directed therapy in cardiac surgery: A systematic review and meta-analysis. Br. J. Anaesth. 2013, 110, 510–517. [Google Scholar] [CrossRef] [PubMed]
- Messina, A.; Robba, C.; Calabrò, L.; Zambelli, D.; Iannuzzi, F.; Molinari, E.; Scarano, S.; Battaglini, D.; Baggiani, M.; De Mattei, G.; et al. Association between perioperative fluid administration and postoperative outcomes: A 20-year systematic review and a meta-analysis of randomized goal-directed trials in major visceral/noncardiac surgery. Crit. Care 2021, 25, 43. [Google Scholar] [CrossRef]
- Jessen, M.K.; Vallentin, M.F.; Holmberg, M.J.; Bolther, M.; Hansen, F.B.; Holst, J.M.; Magnussen, A.; Hansen, N.S.; Johannsen, C.M.; Enevoldsen, J.; et al. Goal-directed haemodynamic therapy during general anaesthesia for noncardiac surgery: A systematic review and meta-analysis. Br. J. Anaesth. 2021, 128, 416–433. [Google Scholar] [CrossRef]
- Sidiropoulou, T.; Tsoumpa, M.; Griva, P.; Galarioti, V.; Matsota, P. Prediction and Prevention of Intraoperative Hypotension with the Hypotension Prediction Index: A Narrative Review. J. Clin. Med. 2022, 11, 5551. [Google Scholar] [CrossRef]
- Awad, H.; Alcodray, G.; Raza, A.; Boulos, R.; Essandoh, M.; Bhandary, S.; Dalton, R. Intraoperative Hypotension–Physiologic Basis and Future Directions. J. Cardiothorac. Vasc. Anesth. 2022, 36, 2154–2163. [Google Scholar] [CrossRef]
- Bijker, J.B.; van Klei, W.A.; Kappen, T.H.; van Wolfswinkel, L.; Moons, K.G.; Kalkman, C.J. Incidence of intraoperative hypotension as a function of the chosen definition: Literature definitions applied to a retrospective cohort using automated data collection. Anesthesiology 2017, 107, 213–220. [Google Scholar] [CrossRef]
- Van Klei, W.A.; van Waes, J.A.; Pasma, W.; Kappen, T.H.; van Wolfswinkel, L.; Peelen, L.M.; Kalkman, C.J. Relationship between preoperative evaluation blood pressure and preinduction blood pressure: A cohort study in patients undergoing general anesthesia. Anesth. Analg. 2017, 124, 431–437. [Google Scholar] [CrossRef]
- Saugel, B.; Reese, P.C.; Sessler, D.I.; Burfeindt, C.; Nicklas, J.Y.; Pinnschmidt, H.O.; Reuter, D.A.; Südfeld, S. Automated ambulatory blood pressure measurements and intraoperative hypotension in patients having noncardiac surgery with general anesthesia: A prospective observational study. Anesthesiology 2019, 131, 74–83. [Google Scholar] [CrossRef] [PubMed]
- Alcock, R.F.; Kouzios, D.; Naoum, C.; Hillis, G.S.; Brieger, D.B. Perioperative myocardial necrosis in patients at high cardiovascular risk undergoing elective non-cardiac surgery. Heart 2012, 98, 792–798. [Google Scholar] [CrossRef] [PubMed]
- Van Waes, J.A.; van Klei, W.A.; Wijeysundera, D.N.; van Wolfswinkel, L.; Lindsay, T.F.; Beattie, W.S. Association between intraoperative hypotension and myocardial injury after vascular surgery. Anesthesiology 2016, 124, 35–44. [Google Scholar] [CrossRef] [PubMed]
- Gu, W.-J.; Hou, B.-L.; Kwong, J.S.; Tian, X.; Qian, Y.; Cui, Y.; Hao, J.; Li, J.-C.; Ma, Z.-L.; Gu, X.-P. Association between intraoperative hypotension and 30-day mortality, major adverse cardiac events, and acute kidney injury after non-cardiac surgery: A meta-analysis of cohort studies. Int. J. Cardiol. 2018, 258, 68–73. [Google Scholar] [CrossRef]
- Davies, S.J.; Vistisen, S.T.; Jian, Z.; Hatib, F.; Scheeren, T.W.L. Ability of an arterial waveform analysis–derived hypotension prediction index to predict future hypotensive events in surgical patients. Anesth. Analg 2020, 130, 352–359. [Google Scholar] [CrossRef]
- Hatib, F.; Jian, Z.; Buddi, S.; Lee, C.; Settels, J.; Sibert, K.; Rinehart, J.; Cannesson, M. Machine-learning algorithm to predict hypotension based on high-fidelity arterial pressure waveform analysis. Anesthesiology 2018, 129, 663–674. [Google Scholar] [CrossRef]
- Ranucci, M.; Barile, L.; Ambrogi, F.; Pistuddi, V.; Surgical and Clinical Outcome Research (SCORE) Group. Discrimination and calibration properties of the hypotension probability indicator during cardiac and vascular surgery. Minerva Anestesiol. 2019, 85, 724–730. [Google Scholar] [CrossRef]
- Pinsky, M.R. Heart lung interactions during mechanical ventilation. Curr. Opin. Crit. Care 2012, 18, 256–260. [Google Scholar] [CrossRef] [PubMed]
- Sondergaard, S. Pavane for a pulse pressure variation defunct. Crit. Care 2013, 17, 327. [Google Scholar] [CrossRef] [PubMed]
- Morimont, P.; Lambermont, B.; Desaive, T.; Janssen, N.; Chase, G.; D’Orio, V. Arterial dP/dtmax accurately reflects left ventricular contractility during shock when adequate vascular filling is achieved. BMC Cardiovasc. Disord. 2012, 12, 13. [Google Scholar] [CrossRef] [PubMed]
- Monge Garcia, M.I.; Jian, Z.; Settels, J.J.; Hunley, C.; Cecconi, M.; Hatib, F.; Pinsky, M.R. Performance comparison of ventricular and arterial dP/dtmax for assessing left ventricular systolic function during different experimental loading and contractile conditions. Crit. Care 2018, 22, 325. [Google Scholar] [CrossRef]
- De Hert, S.G.; Robert, D.; Cromheecke, S.; Michard, F.; Nijs, J.; Rodrigus, I.E. Evaluation of left ventricular function in anesthetized patients using femoral artery dP/dt(max). J. Cardiothorac. Vasc. Anesth. 2006, 20, 325–330. [Google Scholar] [CrossRef] [PubMed]
- Schneck, E.; Schulte, D.; Habig, L.; Ruhrmann, S.; Edinger, F.; Markmann, M.; Habicher, M.; Rickert, M.; Koch, C.; Sander, M. Hypotension Prediction Index based protocolized haemodynamic management reduces the incidence and duration of intraoperative hypotension in primary total hip arthroplasty: A single centre feasibility randomised blinded prospective interventional trial. J. Clin. Monit. Comput. 2019, 34, 1149–1158. [Google Scholar] [CrossRef]
- Wijnberge, M.; Geerts, B.F.; Hol, L.; Lemmers, N.; Mulder, M.P.; Berge, P.; Schenk, J.; Terwindt, L.E.; Hollmann, M.W.; Vlaar, A.P.; et al. Effect of a Machine Learning-Derived Early Warning System for Intraoperative Hypotension vs. Standard Care on Depth and Duration of Intraoperative Hypotension during Elective Noncardiac Surgery: The HYPE Randomized Clinical Trial. JAMA 2020, 323, 1052–1060. [Google Scholar] [CrossRef] [PubMed]
- Maheshwari, K.; Shimada, T.; Yang, D.; Khanna, S.; Cywinski, J.B.; Irefin, S.A.; Ayad, S.; Turan, A.; Ruetzler, K.; Qiu, Y.; et al. Hypotension Prediction Index for Prevention of Hypotension during Moderate- to High-risk Noncardiac Surgery. Anesthesiology 2020, 133, 1214–1222. [Google Scholar] [CrossRef]
- Tsoumpa, M.; Kyttari, A.; Matiatou, S.; Tzoufi, M.; Griva, P.; Pikoulis, E.; Riga, M.; Matsota, P.; Sidiropoulou, T. The Use of the Hypotension Prediction Index Integrated in an Algorithm of Goal Directed Hemodynamic Treatment during Moderate and High-Risk Surgery. J. Clin. Med. 2021, 10, 5884. [Google Scholar] [CrossRef]
- Murabito, P.; Astuto, M.; Sanfilippo, F.; La Via, L.; Vasile, F.; Basile, F.; Cappellani, A.; Longhitano, L.; Distefano, A.; Volti, G.L. Proactive Management of Intraoperative Hypotension Reduces Biomarkers of Organ Injury and Oxidative Stress during Elective Non-Cardiac Surgery: A Pilot Randomized Controlled Trial. J. Clin. Med. 2022, 11, 392. [Google Scholar] [CrossRef]
- Grundmann, C.D.; Wischermann, J.M.; Fassbender, P.; Bischoff, P.; Frey, U.H. Hemodynamic monitoring with Hypotension Prediction Index versus arterial waveform analysis alone and incidence of perioperative hypotension. Acta Anaesthesiol. Scand. 2021, 65, 1404–1412. [Google Scholar] [CrossRef]
- Solares, G.J.; Garcia, D.; Garcia, M.I.M.; Crespo, C.; Rabago, J.L.; Iglesias, F.; Larraz, E.; Zubizarreta, I.; Rabanal, J.M. Real-world outcomes of the hypotension prediction index in the management of intraoperative hypotension during non-cardiac surgery: A retrospective clinical study. J. Clin. Monit. Comput. 2023, 37, 211–220. [Google Scholar] [CrossRef] [PubMed]
- Lorsomradee, S.; Lorsomradee, S.; Cromheecke, S.; De Hert, S.G. Uncalibrated arterial pulse contour analysis versus continuous thermodilution technique: Effects of alterations in arterial waveform. J. Cardiothorac. Vasc. Anesth. 2007, 21, 636–643. [Google Scholar] [CrossRef] [PubMed]
- Shehata, I.M.; Alcodray, G.; Essandoh, M.; Bhandary, S.P. Con: Routine Use of the Hypotension Prediction Index in Cardiac, Thoracic, and Vascular Surgery. J. Cardiothorac. Vasc. Anesth. 2021, 35, 1237–1240. [Google Scholar] [CrossRef] [PubMed]
- Camporota, L.; Beale, R. Pitfalls in haemodynamic monitoring based on the arterial pressure waveform. Crit. Care 2010, 14, 124. [Google Scholar] [CrossRef]
- Monnet, X.; Shi, R.; Teboul, J.L. Prediction of fluid responsiveness. What’s new? Ann. Intensive Care 2022, 12, 46. [Google Scholar] [CrossRef] [PubMed]
- Hattori, K.; Maeda, T.; Masubuchi, T.; Yoshikawa, A.; Ebuchi, K.; Morishima, K.; Kamei, M.; Yoshitani, K.; Ohnishi, Y. Accuracy and Trending Ability of the Fourth-Generation FloTrac/Vigileo System in Patients with Low Cardiac Index. J. Cardiothorac. Vasc. Anesth. 2017, 31, 99–104. [Google Scholar] [CrossRef] [PubMed]
- Eisenried, A.; Klarwein, R.; Ihmsen, H.; Wehrfritz, A.; Tandler, R.; Heim, C.; Fechner, J. Accuracy and Trending Ability of the Fourth-Generation FloTrac/EV1000 System in Patients with Severe Aortic Valve Stenosis before and after Surgical Valve Replacement. J. Cardiothorac. Vasc. Anesth. 2019, 33, 1230–1236. [Google Scholar] [CrossRef]
- Maeda, T.; Hattori, K.; Sumiyoshi, M.; Kanazawa, H.; Ohnishi, Y. Accuracy and trending ability of the fourth-generation FloTrac/Vigileo System™ in patients undergoing abdominal aortic aneurysm surgery. J. Anesth. 2018, 32, 387–393. [Google Scholar] [CrossRef] [PubMed]
- Monge García, M.I.; Gil Cano, A.; Gracia Romero, M. Dynamic arterial elastance to predict arterial pressure response to volume loading in preload-dependent patients. Crit. Care 2011, 15, R15. [Google Scholar] [CrossRef]
- Geisen, M.; Ganter, M.T.; Hartnack, S.; Dzemali, O.; Hofer, C.K.; Zollinger, A. Accuracy, Precision, and Trending of 4 Pulse Wave Analysis Techniques in the Postoperative Period. J. Cardiothorac. Vasc. Anesth. 2018, 32, 715–722. [Google Scholar] [CrossRef]
| Study, Year of Publication | Study Type | Number of Patients | Study Group | Primary Outcome | Main Results |
|---|---|---|---|---|---|
| Schneck et al., 2019 [35] | Randomised prospective interventional trial | Total 99 patients—25 HPI, 50 historic control, 25 standard care, | Primary hip arthroplasty under general anesthesia | Frequency (n/hour), absolute and relative hypotension (defined as MAP < 65 mmHg for more than 1 min) duration (% of total anesthesia time) | Significant reduction of intraoperative hypotension in the HPI group (percentage of patients with at least one episode of hypotension; 48% vs. 80% and 87%, in the HPI, historic control and control group, respectively). Significant reduction of number of hypotensive episodes (HPI 0 (0–1), historic control 2 (1–3), and control group 5 (2–6); median value (interquartile range), p < 0.001) and duration of hypotension—minutes below MAP 65 mmHg in % of total anesthesia time (HPI 0 (0–1), historic control 7 (2–17) and control group 6 (2–12); median value (interquartile range) p < 0.001). |
| Wijnberge et al.,2020 [36] | Prospective randomized controlled trial | Total 68 (HPI = 34, standard care = 34) | Elective non cardiac surgery | TWA of hypotension with MAP < 65 mmHg | The median TWA of hypotension was 0.10 mmHg in the HPI group vs. 0.44 mmHg in the standard therapy group (p = 0.001). The median duration of hypotension per patient was 8.0 min in the HPI group vs. 32.7 min in the standard therapy group (p < 0.001). |
| Maheshwari et al.,2020 [37] | Prospective randomized controlled trial | Total 214 (HPI 105, standard care = 109) | Moderate or high-risk non cardiac surgery | TWA of hypotension with MAP < 65 mmHg | The median TWA of hypotension was 0.14 mmHg in the HPI group vs. 0.14 mmHg in the standard therapy group (p = 0.757). |
| Tsoumpa et al., 2021 [38] | Prospective randomized controlled trial | Total 99 (HPI = 49, standard care = 50) | Moderate or high-risk non cardiac surgery | TWA of hypotension with MAP < 65 mmHg | The median TWA of hypotension was 0.16 mmHg in the HPI group vs. 0.50 mmHg in the standard therapy group (p = 0.0003). |
| Murabito et al.,2022 [39] | Prospective randomized controlled trial | Total 40 (HPI = 20, standard care = 20) | Major general surgery | TWA of hypotension with MAP < 65 mmHg | The median TWA of hypotension was 0.12 mmHg in the HPI group vs. 0.37 mmHg in the standard therapy group (p = 0.025). |
| Grundmann et al., 2021 [40] | Retrospective observational study | Total 100 (HPI = 50, Flotrac = 50) | Moderate or high-risk non cardiac surgery | TWA of hypotension with MAP < 65 mmHg | The median TWA of hypotension was 0.10 mmHg in the HPI group vs. 0.27 mmHg in the standard therapy group (p = 0.001). In the HPI group 26 patients (52%) vs. 42 patients (84%) experienced a hypotension (p = 0.001). |
| Solares et al., 2022 [41] | Retrospective study | Total 104 (HPI = 52, Flotrac = 52) | Urgent or elective non cardiac surgery with moderate to high risk of bleeding | TWA of hypotension with MAP < 65 mmHg | The median TWA of hypotension was 0.09 mmHg in the HPI group vs. 0.23 mmHg in the Flotrac group (p = 0.037). Postoperative complications were less frequent in the HPI group (p = 0.035). Hospital length of stay was 2 days shorter in the HPI group (0.019). |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Szrama, J.; Gradys, A.; Bartkowiak, T.; Woźniak, A.; Kusza, K.; Molnar, Z. Intraoperative Hypotension Prediction—A Proactive Perioperative Hemodynamic Management—A Literature Review. Medicina 2023, 59, 491. https://doi.org/10.3390/medicina59030491
Szrama J, Gradys A, Bartkowiak T, Woźniak A, Kusza K, Molnar Z. Intraoperative Hypotension Prediction—A Proactive Perioperative Hemodynamic Management—A Literature Review. Medicina. 2023; 59(3):491. https://doi.org/10.3390/medicina59030491
Chicago/Turabian StyleSzrama, Jakub, Agata Gradys, Tomasz Bartkowiak, Amadeusz Woźniak, Krzysztof Kusza, and Zsolt Molnar. 2023. "Intraoperative Hypotension Prediction—A Proactive Perioperative Hemodynamic Management—A Literature Review" Medicina 59, no. 3: 491. https://doi.org/10.3390/medicina59030491
APA StyleSzrama, J., Gradys, A., Bartkowiak, T., Woźniak, A., Kusza, K., & Molnar, Z. (2023). Intraoperative Hypotension Prediction—A Proactive Perioperative Hemodynamic Management—A Literature Review. Medicina, 59(3), 491. https://doi.org/10.3390/medicina59030491






