Morphometric Parameters and MRI Morphological Changes of the Knee and Patella in Physically Active Adolescents
Abstract
1. Introduction
2. Patients and Methods
3. Statistical Analysis
4. Results
5. Discussion
6. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Sweeney, E.; Rodenberg, R.; MacDonald, J. Overuse Knee Pain in the Pediatric and Adolescent Athlete. Curr. Sport. Med. Rep. 2020, 19, 479–485. [Google Scholar] [CrossRef] [PubMed]
- DiFiori, J.P.; Benjamin, H.J.; Brenner, J.S.; Gregory, A.; Jayanthi, N.; Landry, G.L.; Luke, A. Overuse injuries and burnout in youth sports: A position statement from the American Medical Society for Sports Medicine. Br. J. Sport. Med. 2014, 48, 287–288. [Google Scholar] [CrossRef] [PubMed]
- Caine, D.; Meyers, R.; Nguyen, J.; Schoffl, V.; Maffulli, N. Primary Periphyseal Stress Injuries in Young Athletes: A Systematic Review. Sport. Med. 2021, 52, 741–772. [Google Scholar] [CrossRef]
- Arnold, A.; Thigpen, C.A.; Beattie, P.F.; Kissenberth, M.J.; Shanley, E. Overuse Physeal Injuries in Youth Athletes. Sport. Health 2017, 9, 139–147. [Google Scholar] [CrossRef] [PubMed]
- Bateni, C.P.; Bindra, J.; Haus, B. MRI of Sports Injuries in Children and Adolescents: What s Different from Adults. Curr. Radiol. Rep. 2014, 2, 45. [Google Scholar] [CrossRef]
- Yen, Y.M. Assessment and treatment of knee pain in the child and adolescent athlete. Pediatr. Clin. N. Am. 2014, 61, 1155–1173. [Google Scholar] [CrossRef]
- Patel, D.R.; Villalobos, A. Evaluation and management of knee pain in young athletes: Overuse injuries of the knee. Transl. Pediatr. 2017, 6, 190–198. [Google Scholar] [CrossRef]
- Barton, C.J.; Lack, S.; Hemmings, S.; Tufail, S.; Morrissey, D. The ‘Best Practice Guide to Conservative Management of Patellofemoral Pain’: Incorporating level 1 evidence with expert clinical reasoning. Br. J. Sport. Med. 2015, 49, 923–934. [Google Scholar] [CrossRef]
- Pooley, R.A. AAPM/RSNA physics tutorial for residents: Fundamental physics of MR imaging. Radiographics 2005, 25, 1087–1099. [Google Scholar] [CrossRef]
- Gudas, R.; Šiupšinskas, L.; Gudaitė, A.; Vansevičius, V.; Stankevičius, E.; Smailys, A.; Vilkytė, A.; Simonaitytė, R. The Patello-Femoral Joint Degeneration and the Shape of the Patella in the Population Needing an Arthroscopic Procedure. Medicina 2018, 54, 21. [Google Scholar] [CrossRef]
- Zaffagnini, S.; Grassi, A.; Zocco, G.; Rosa, M.A.; Signorelli, C.; Marcheggiani Muccioli, G.M. The patellofemoral joint: From dysplasia to dislocation. EFORT Open Rev. 2017, 2, 204–214. [Google Scholar] [CrossRef]
- Meyers, A.B.; Laor, T.; Sharafinski, M.; Zbojniewicz, A.M. Imaging assessment of patellar instability and its treatment in children and adolescents. Pediatr. Radiol. 2016, 46, 618–636. [Google Scholar] [CrossRef]
- Stoller, D.W.; Sampson, T.G.; Li, A.E. The knee. In Magnetic Resonance Imaging in Orthopaedics and Sports Medicine, 3rd ed.; Stoller, D.W., Ed.; Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2007; pp. 305–732. [Google Scholar]
- Available online: https://www.healthychildren.org/English/ages-stages/teen/Pages/Stages-of-Adolescence.aspx (accessed on 5 June 2022).
- Carrillon, Y.; Abidi, H.; Dejour, D.; Fantino, O.; Moyen, B.; Tran-Minh, V.A. Patellar instability: Assessment on MR images by measuring the lateral trochlear inclination-initial experience. Radiology 2000, 216, 582–585. [Google Scholar] [CrossRef] [PubMed]
- Diederichs, G.; Issever, A.S.; Scheffler, S. MR imaging of patellar instability: Injury patterns and assessment of risk factors. Radiographics 2010, 30, 961–981. [Google Scholar] [CrossRef] [PubMed]
- Pfirrmann, C.W.; Zanetti, M.; Romero, J.; Hodler, J. Femoral trochlear dysplasia: MR findings. Radiology 2000, 216, 858–864. [Google Scholar] [CrossRef] [PubMed]
- Wilcox, J.J.; Snow, B.J.; Aoki, S.K.; Hung, M.; Burks, R.T. Does landmark selection affect the reliability of tibial tubercle-trochlear groove measurements using MRI? Clin. Orthop. Relat. Res. 2012, 470, 2253–2260. [Google Scholar] [CrossRef]
- Charles, M.D.; Haloman, S.; Chen, L.; Ward, S.R.; Fithian, D.; Afra, R. Magnetic resonance imaging-based topographical differences between control and recurrent patellofemoral instability patients. Am. J. Sport. Med. 2013, 41, 374–384. [Google Scholar] [CrossRef]
- Dejour, H.; Walch, G.; Nove-Josserand, L.; Guier, C. Factors of patellar instability: An anatomic radiographic study. Knee Surg. Sport. Traumatol. Arthrosc. 1994, 2, 19–26. [Google Scholar] [CrossRef]
- Munch, J.L.; Sullivan, J.P.; Nguyen, J.T.; Mintz, D.; Green, D.W.; Shubin Stein, B.E.; Strickland, S. Patellar Articular Overlap on MRI Is a Simple Alternative to Conventional Measurements of Patellar Height. Orthop. J. Sport. Med. 2016, 4, 2325967116656328. [Google Scholar] [CrossRef]
- Trasolini, N.A.; Serino, J.; Dandu, N.; Yanke, A.B. Treatment of Proximal Trochlear Dysplasia in the Setting of Patellar Instability: An Arthroscopic Technique. Arthrosc. Tech. 2021, 10, e2253–e2258. [Google Scholar] [CrossRef]
- Steensen, R.N.; Bentley, J.C.; Trinh, T.Q.; Backes, J.R.; Wiltfong, R.E. The prevalence and combined prevalences of anatomic factors associated with recurrent patellar dislocation: A magnetic resonance imaging study. Am. J. Sport. Med. 2015, 43, 921–927. [Google Scholar] [CrossRef] [PubMed]
- Joseph, S.M.; Cheng, C.; Solomito, M.J.; Pace, J.L. Lateral Trochlear Inclination Angle: Measurement via a 2-Image Technique to Reliably Characterize and Quantify Trochlear Dysplasia. Orthop. J. Sport. Med. 2020, 8, 2325967120958415. [Google Scholar] [CrossRef]
- Paiva, M.; Blond, L.; Holmich, P.; Steensen, R.N.; Diederichs, G.; Feller, J.A.; Barfod, K.W. Quality assessment of radiological measurements of trochlear dysplasia; a literature review. Knee Surg. Sport. Traumatol. Arthrosc. 2018, 26, 746–755. [Google Scholar] [CrossRef] [PubMed]
- Stepanovich, M.; Bomar, J.D.; Pennock, A.T. Are the Current Classifications and Radiographic Measurements for Trochlear Dysplasia Appropriate in the Skeletally Immature Patient? Orthop. J. Sport. Med. 2016, 4, 2325967116669490. [Google Scholar] [CrossRef]
- Shen, J.; Qin, L.; Yao, W.W.; Li, M. The significance of magnetic resonance imaging in severe femoral trochlear dysplasia assessment. Exp. Ther. Med. 2017, 14, 5438–5444. [Google Scholar] [CrossRef]
- Kim, H.K.; Parikh, S. Patellofemoral Instability in Children: Imaging Findings and Therapeutic Approaches. Korean J. Radiol. 2022, 23, 674–687. [Google Scholar] [CrossRef]
- Sidharthan, S.; Yau, A.; Almeida, B.A.; Shea, K.G.; Greditzer, H.G.; Jones, K.J.; Fabricant, P.D. Patterns of Articular Cartilage Thickness in Pediatric and Adolescent Knees: A Magnetic Resonance Imaging-Based Study. Arthrosc. Sport. Med. Rehabil. 2021, 3, e381–e390. [Google Scholar] [CrossRef]
- Hori, M.; Terada, M.; Suga, T.; Isaka, T. Changes in anterior femoral articular cartilage structure in collegiate rugby athletes with and without a history of traumatic knee joint injury following a five-month competitive season. Sci. Rep. 2021, 11, 15186. [Google Scholar] [CrossRef]
- Nagamine, R.; Miura, H.; Inoue, Y.; Tanaka, K.; Urabe, K.; Okamoto, Y.; Nishizawa, M.; Iwamoto, Y. Malposition of the tibial tubercle during flexion in knees with patellofemoral arthritis. Skelet. Radiol. 1997, 26, 597–601. [Google Scholar] [CrossRef]
- Verhulst, F.V.; van Sambeeck, J.D.P.; Olthuis, G.S.; van der Ree, J.; Koeter, S. Patellar height measurements: Insall-Salvati ratio is most reliable method. Knee Surg. Sport. Traumatol. Arthrosc. 2020, 28, 869–875. [Google Scholar] [CrossRef] [PubMed]
- Cavallo, F.; Mohn, A.; Chiarelli, F.; Giannini, C. Evaluation of Bone Age in Children: A Mini-Review. Front. Pediatr. 2021, 9, 580314. [Google Scholar] [CrossRef] [PubMed]
- Kurowecki, D.; Shergill, R.; Cunningham, K.M.; Peterson, D.C.; Takrouri, H.S.R.; Habib, N.O.; Ainsworth, K.E. A comparison of sagittal MRI and lateral radiography in determining the Insall-Salvati ratio and diagnosing patella alta in the pediatric knee. Pediatr. Radiol. 2022, 52, 527–532. [Google Scholar] [CrossRef] [PubMed]
- Thévenin-Lemoine, C.; Ferrand, M.; Courvoisier, A.; Damsin, J.P.; Ducou le Pointe, H.; Vialle, R. Is the Caton-Deschamps index a valuable ratio to investigate patellar height in children? J. Bone Jt. Surg. 2011, 93, e35. [Google Scholar] [CrossRef] [PubMed]
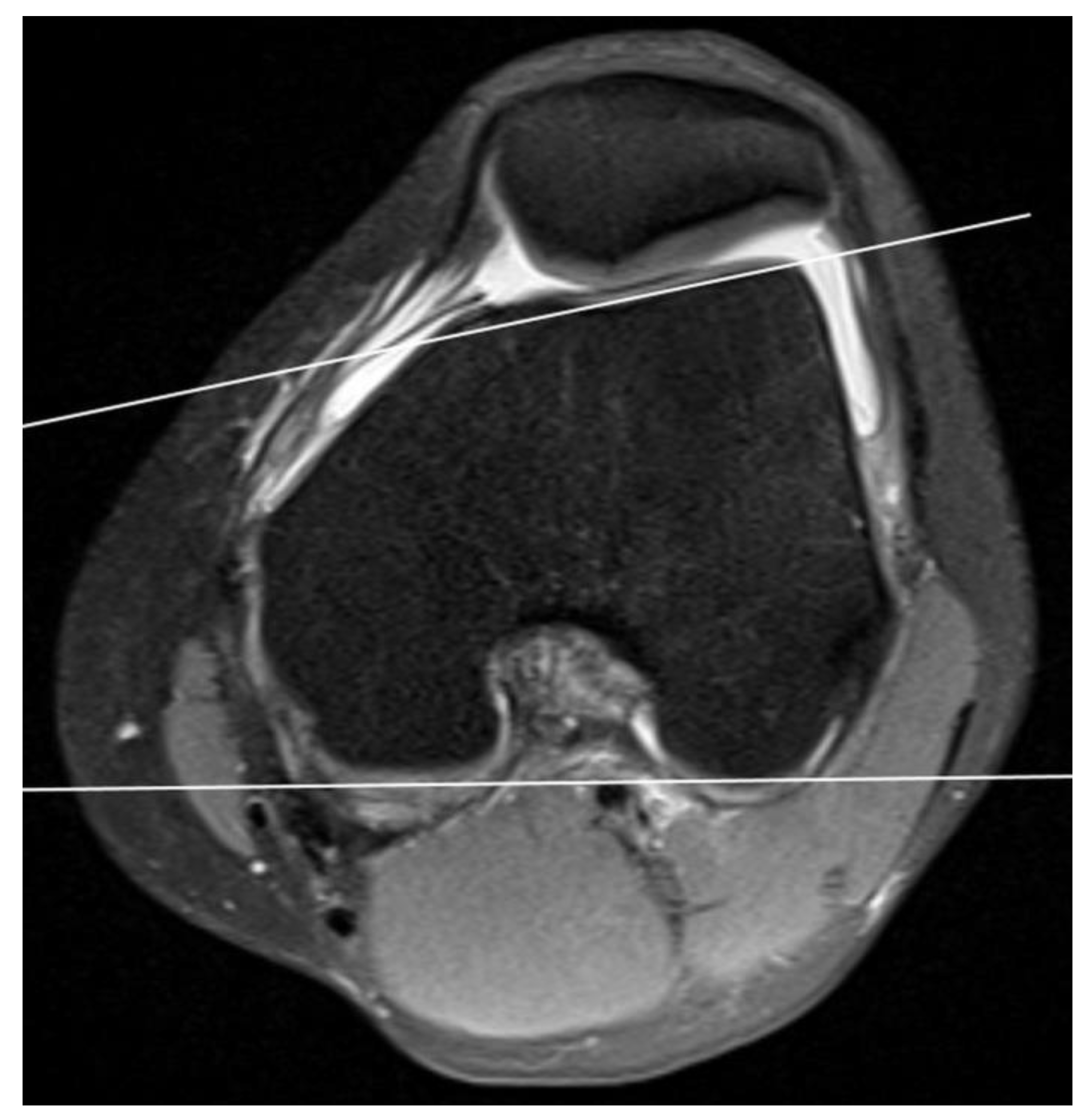
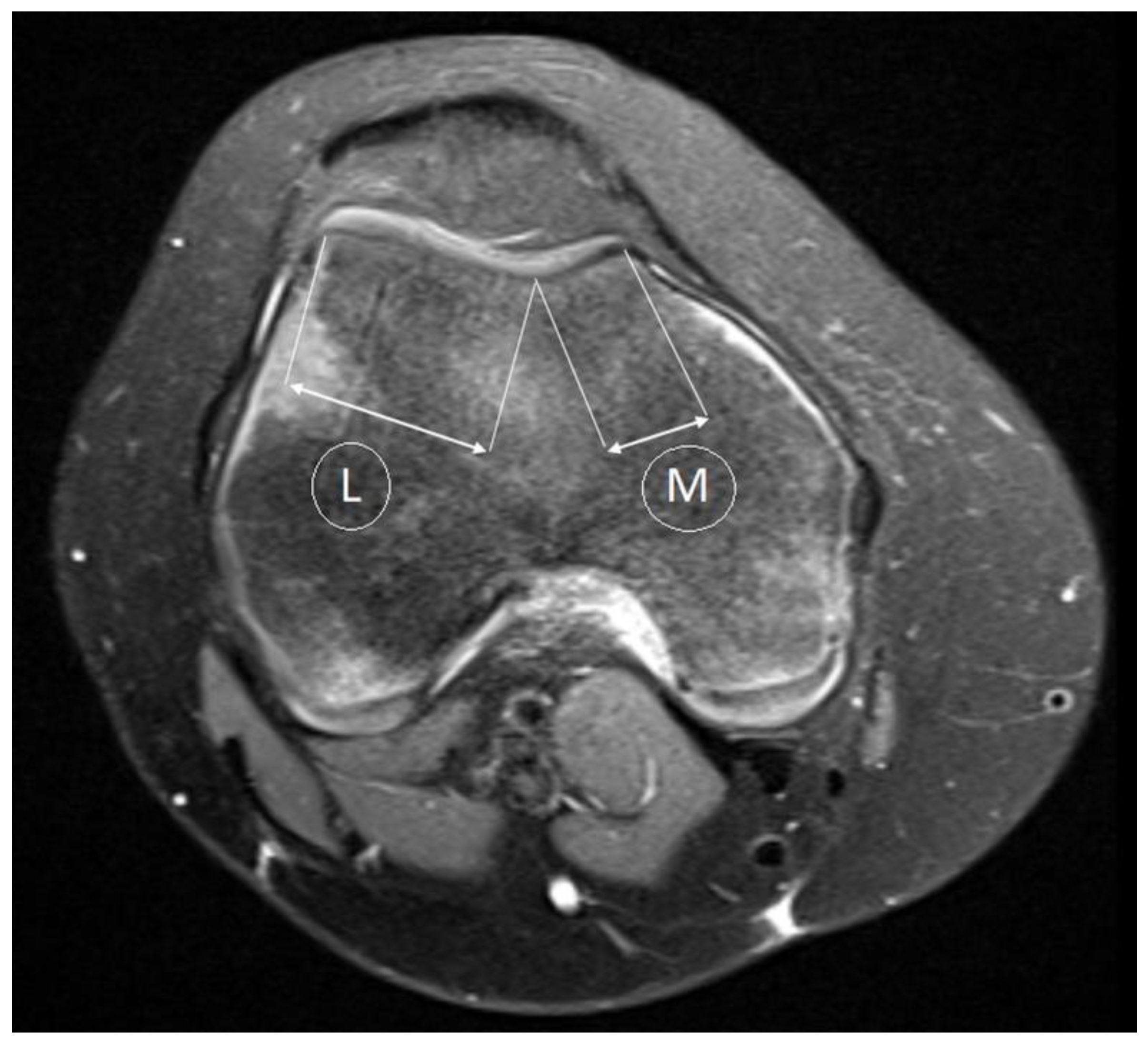
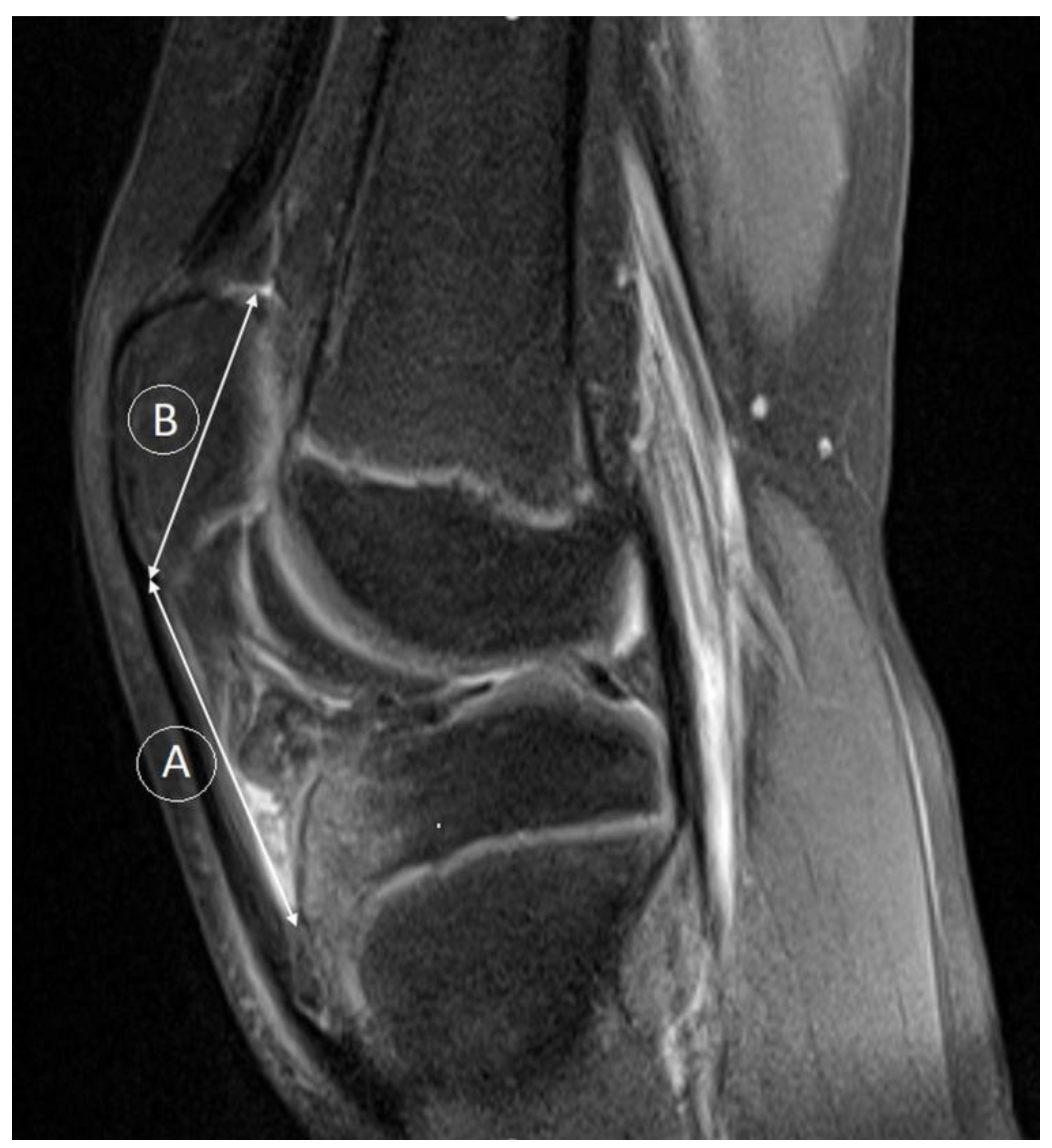
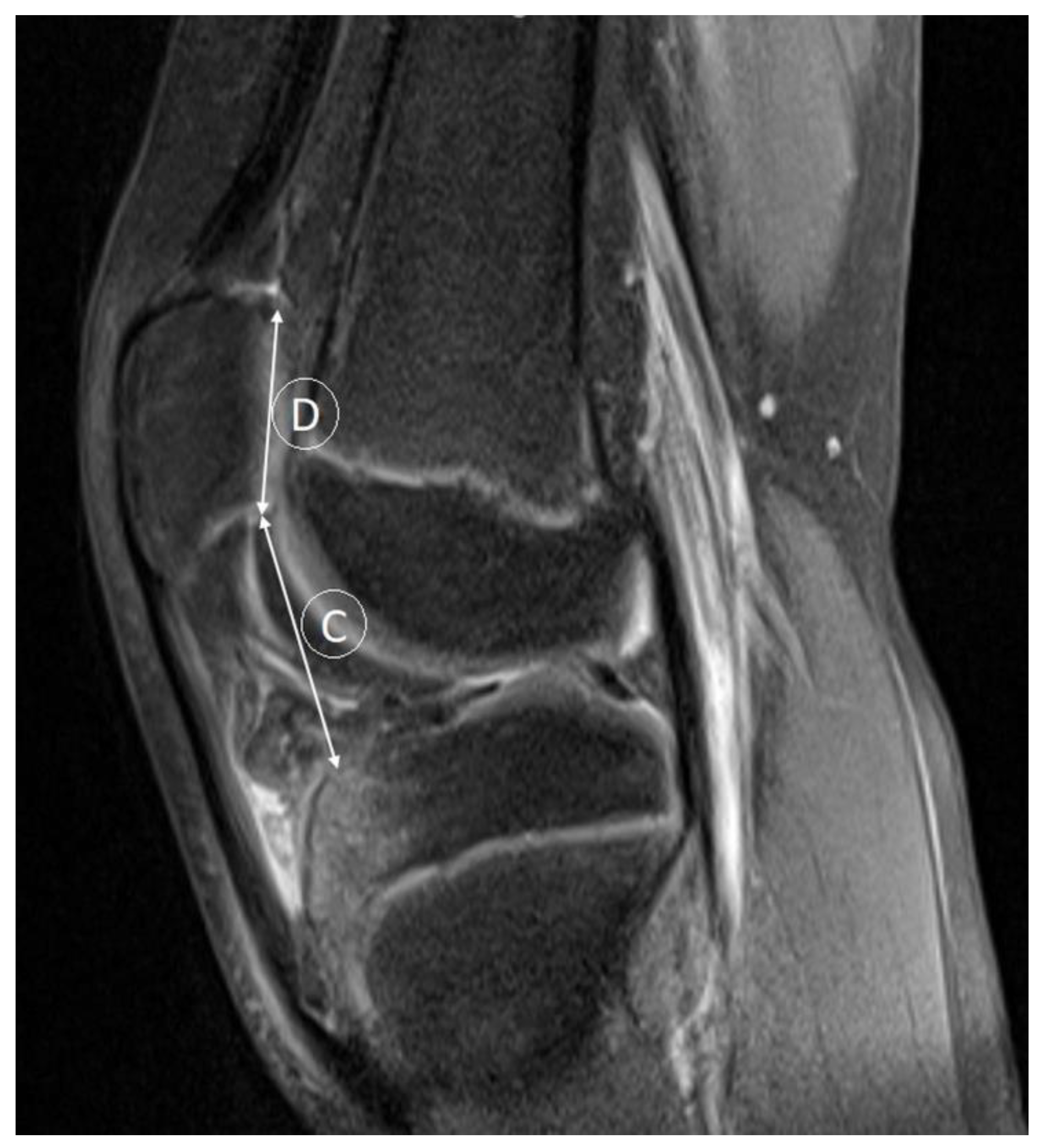
| Age (Years) | p-Value | |||||||
|---|---|---|---|---|---|---|---|---|
| 11–14 | 15–17 | 18–21 | ||||||
| N (%) | % | N | % | N | % | |||
| Gender | male | 22 (40.0) | 40.0 | 48 | 44.4 | 13 | 43.3 | 0.863 |
| female | 33 (60.0) | 60.0 | 60 | 55.6 | 17 | 56.7 | ||
| Knee | Left | 28 (50.9) | 50.9 | 57 | 52.8 | 13 | 43.3 | 0.658 |
| right | 27 (49.1) | 49.1 | 51 | 47.2 | 17 | 56.7 | ||
| Parameter Age Group (Years) | N | Mean ± SD | Median | p-Value | |
|---|---|---|---|---|---|
| LTI | Group 1 (11–14) | 55 | 15.75 ± 6.52 | 17.00 | 0.612 |
| Group 2 (15–17) | 108 | 15.40 ± 5.79 | 15.85 | ||
| Group 3 (18–21) | 30 | 14.41 ± 5.89 | 15.50 | ||
| medial facet | Group 1 (11–14) | 55 | 16.60 ± 2.78 | 16.60 | 0.357 |
| Group 2 (15–17) | 108 | 17.03 ± 3.49 | 17.00 | ||
| Group 3 (18–21) | 30 | 17.65 ± 2.95 | 17.95 | ||
| lateral facet | Group 1 (11–14) | 55 | 25.48 ± 3.72 | 25.00 | 0.861 |
| Group 2 (15–17) | 108 | 25.52 ± 3.95 | 25.50 | ||
| Group 3 (18–21) | 30 | 25.92 ± 3.68 | 25.70 | ||
| trochlear facet asymmetry | Group 1 (11–14) | 55 | 0.67 ± 0.14 | 0.69 | 0.707 |
| Group 2 (15–17) | 108 | 0.68 ± 0.16 | 0.69 | ||
| Group 3 (18–21) | 30 | 0.69 ± 0.14 | 0.70 | ||
| TT-TG distance (mm) | Group 1 (11–14) | 55 | 10.23 ± 5.01 | 10.10 | 0.801 |
| Group 2 (15–17) | 108 | 9.75 ± 4.34 | 10.23 | ||
| Group 3 (18–21) | 30 | 9.81 ± 3.50 | 9.75 | ||
| Articular overlap | Group 1 (11–14) | 55 | 12.70 ± 3.17 | 12.80 | 0.650 |
| Group 2 (15–17) | 108 | 13.13 ± 2.94 | 13.10 | ||
| Group 3 (18–21) | 30 | 12.80 ± 2.58 | 12.55 | ||
| Insall–Salvati | Group 1 (11–14) | 55 | 1.24 ± 0.21 | 1.23 | 0.127 |
| Group 2 (15–17) | 108 | 1.20 ± 0.22 | 1.18 | ||
| Group 3 (18–21) | 30 | 1.14 ± 0.18 | 1.14 | ||
| MOD Insall–Salvati | Group 1 (11–14) | 55 | 1.66 ± 0.23 | 1.64 | 0.062 |
| Group 2 (15–17) | 108 | 1.57 ± 0.23 | 1.56 | ||
| Group 3 (18–21) | 30 | 1.56 ± 0.28 | 1.47 | ||
| Caton–Deschamps | Group 1 (11–14) | 55 | 1.13 ± 0.21 | 1.10 | 0.039 |
| Group 2 (15–17) | 108 | 1.07 ± 0.16 | 1.05 | ||
| Group 3 (18–21) | 30 | 1.03 ± 0.19 | 0.97 | ||
| Morphology ratio | Group 1 (11–14) | 55 | 0.81 ± 0.08 | 0.82 | 0.463 |
| Group 2 (15–17) | 108 | 0.82 ± 0.08 | 0.83 | ||
| Group 3 (18–21) | 30 | 0.82 ± 0.09 | 0.84 | ||
| Patellofemoral Contact Surface Ratio | Group 1 (11–14) | 55 | 2.75 ± 0.73 | 2.55 | 0.979 |
| Group 2 (15–17) | 108 | 2.77 ± 0.86 | 2.52 | ||
| Group 3 (18–21) | 30 | 2.77 ± 0.47 | 2.78 | ||
| Patellar Type | p-Value | |||||||
|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | ||||||
| N | % | N | % | N | % | |||
| Gender | male | 10 | 47.6 | 55 | 38.2 | 18 | 64.3 | 0.035 |
| female | 11 | 52.4 | 89 | 61.8 | 10 | 35.7 | ||
| Knee | Left | 12 | 57.1 | 72 | 50.0 | 14 | 50.0 | 0.826 |
| right | 9 | 42.9 | 72 | 50.0 | 14 | 50.0 | ||
| Parameter Patellar Type | N | Mean (± SD) | Median | p-Value | |
|---|---|---|---|---|---|
| LTI | 1 | 21 | 14.79 ± 4.94 | 16.10 | <0.001 |
| 2 | 144 | 16.29 ± 5.63 | 16.80 | ||
| 3 | 28 | 10.89 ± 6.72 | 9.25 | ||
| medial facet | 1 | 21 | 19.17 ± 2.58 | 19.50 | <0.001 |
| 2 | 144 | 17.33 ± 2.95 | 17.40 | ||
| 3 | 28 | 13.69 ± 2.66 | 13.70 | ||
| lateral facet | 1 | 21 | 22.59 ± 2.95 | 22.20 | <0.001 |
| 2 | 144 | 25.13 ± 3.25 | 25.25 | ||
| 3 | 28 | 30.09 ± 3.54 | 30.00 | ||
| trochlear facet asymmetry | 1 | 21 | 0.85 ± 0.10 | 0.87 | <0.001 |
| 2 | 144 | 0.69 ± 0.11 | 0.70 | ||
| 3 | 28 | 0.46 ± 0.11 | 0.46 | ||
| TT-TG distance (mm) | 1 | 21 | 9.20 ± 3.98 | 10.20 | 0.086 |
| 2 | 144 | 10.29 ± 4.40 | 10.05 | ||
| 3 | 28 | 8.40 ± 4.51 | 7.77 | ||
| Articular overlap | 1 | 21 | 13.15 ± 3.35 | 13.10 | 0.952 |
| 2 | 144 | 12.93 ± 2.70 | 13.00 | ||
| 3 | 28 | 12.94 ± 3.85 | 13.15 | ||
| Insall–Salvati | 1 | 21 | 1.22 ± 0.23 | 1.18 | 0.001 |
| 2 | 144 | 1.17 ± 0.20 | 1.15 | ||
| 3 | 28 | 1.33 ± 0.21 | 1.36 | ||
| MOD Insall–Salvati | 1 | 21 | 1.60 ± 0.19 | 1.59 | 0.834 |
| 2 | 144 | 1.59 ± 0.25 | 1.56 | ||
| 3 | 28 | 1.62 ± 0.22 | 1.61 | ||
| Caton–Deschamps | 1 | 21 | 1.07 ± 0.13 | 1.04 | 0.018 |
| 2 | 144 | 1.06 ± 0.19 | 1.03 | ||
| 3 | 28 | 1.17 ± 0.16 | 1.14 | ||
| Morphology ratio | 1 | 21 | 0.82 ± 0.07 | 0.82 | 0.059 |
| 2 | 144 | 0.81 ± 0.08 | 0.83 | ||
| 3 | 28 | 0.85 ± 0.06 | 0.85 | ||
| PF Contact Surface Ratio | 1 | 21 | 2.76 ± 0.87 | 2.48 | 0.308 |
| 2 | 144 | 2.73 ± 0.67 | 2.56 | ||
| 3 | 28 | 2.97 ± 1.10 | 2.53 | ||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Djuricic, G.; Milanovic, F.; Ducic, S.; Radlović, V.; Lazovic, M.; Soldatovic, I.; Nikolic, D. Morphometric Parameters and MRI Morphological Changes of the Knee and Patella in Physically Active Adolescents. Medicina 2023, 59, 213. https://doi.org/10.3390/medicina59020213
Djuricic G, Milanovic F, Ducic S, Radlović V, Lazovic M, Soldatovic I, Nikolic D. Morphometric Parameters and MRI Morphological Changes of the Knee and Patella in Physically Active Adolescents. Medicina. 2023; 59(2):213. https://doi.org/10.3390/medicina59020213
Chicago/Turabian StyleDjuricic, Goran, Filip Milanovic, Sinisa Ducic, Vladimir Radlović, Mikan Lazovic, Ivan Soldatovic, and Dejan Nikolic. 2023. "Morphometric Parameters and MRI Morphological Changes of the Knee and Patella in Physically Active Adolescents" Medicina 59, no. 2: 213. https://doi.org/10.3390/medicina59020213
APA StyleDjuricic, G., Milanovic, F., Ducic, S., Radlović, V., Lazovic, M., Soldatovic, I., & Nikolic, D. (2023). Morphometric Parameters and MRI Morphological Changes of the Knee and Patella in Physically Active Adolescents. Medicina, 59(2), 213. https://doi.org/10.3390/medicina59020213







