Latvian Primary Care Management of Children with Acute Infections: Antibiotic-Prescribing Habits and Diagnostic Process Prior to Treatment
Abstract
1. Introduction
2. Materials and Methods
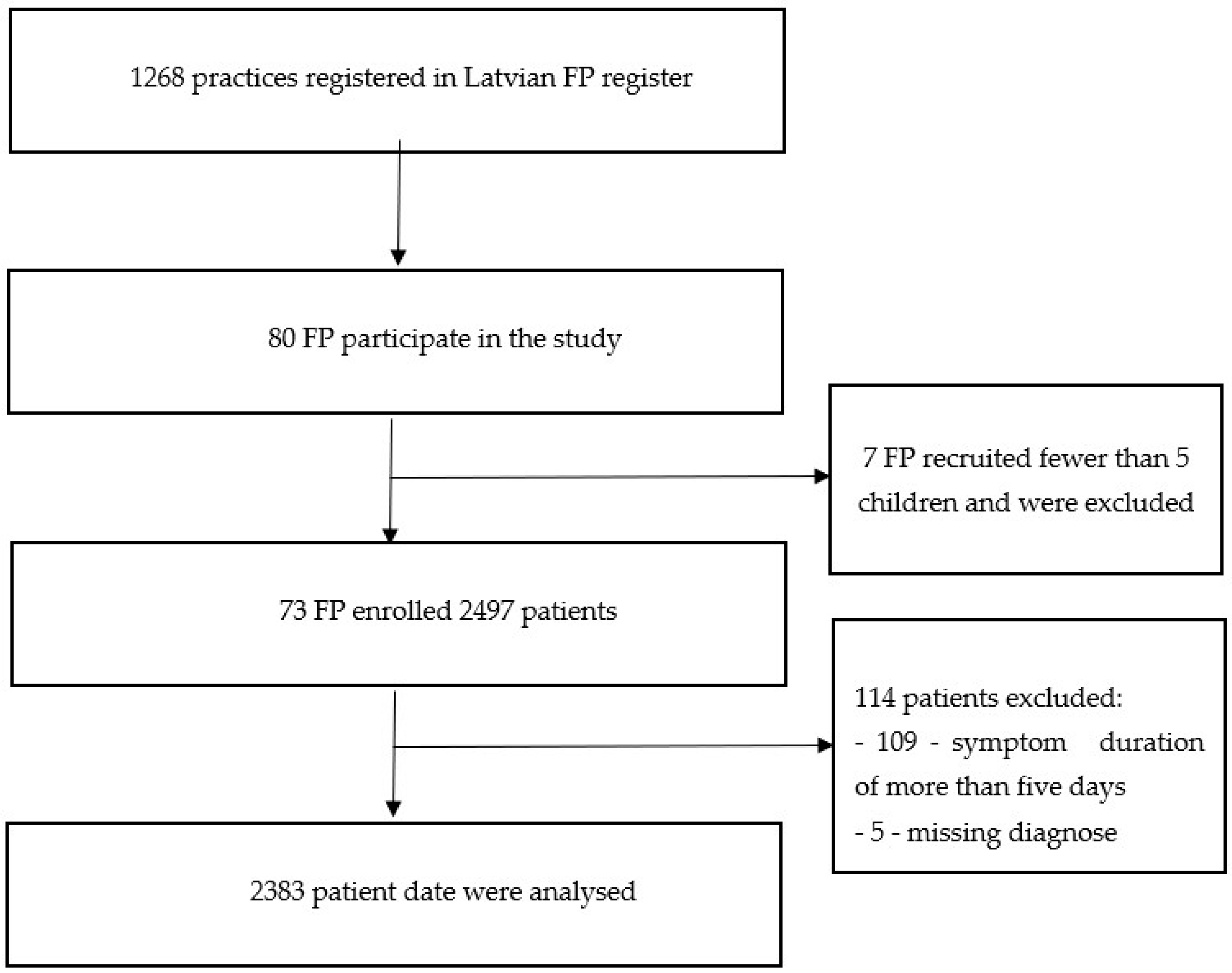
2.1. Participating Children
- Current clinical signs of acute infection for less than five days;
- Aged one month up to 17 years old;
- Exclusion criteria:
- Aged under 1 month;
- Re-convalescent stage of infectious disease;
- Use of antimicrobial therapy before the time of the visit.
2.2. Sample Size Calculation
- The total number of children aged 0–17 in 2019 (column (b)), according to the population registry of Latvia [12];
- The proportion of children visiting FP within a year because of infectious diseases is 39% in children aged 0–4 years, and 8% in older ones [13] (respective calculated size of the target population—column (c));
- The time schedule of the research is 6 months (respective calculated size of the target population—column (d));
- The chosen confidence limit is ±5%.
| Strata (a) | Number of Inhabitants, Latvia (b) | Visiting FP within a Year (c) | Visiting FP within 6 Months (d) | Frequency of AB Prescriptions (%) (e) | Sample Size (f) | |
|---|---|---|---|---|---|---|
| 0–4 years | Urban | 56,072 | 21,868 | 10,934 | 56 | 366 |
| Rural | 70,412 | 27,461 | 13,730 | 56 | 369 | |
| 5–9 years | Urban | 50,574 | 4046 | 2023 | 23 | 240 |
| Rural | 66,470 | 5318 | 2659 | 23 | 247 | |
| 10–14 years | Urban | 50,408 | 4033 | 2016 | 22 | 234 |
| Rural | 69,916 | 5593 | 2797 | 22 | 242 | |
| 15–17 years | Urban | 26,225 | 2098 | 1049 | 22 | 211 |
| Rural | 38,128 | 3050 | 1525 | 22 | 225 | |
| Total: | 2134 | |||||
2.3. Participating Family Physicians
2.4. Data Collection
2.5. Statistical Analyses
3. Results
4. Discussion
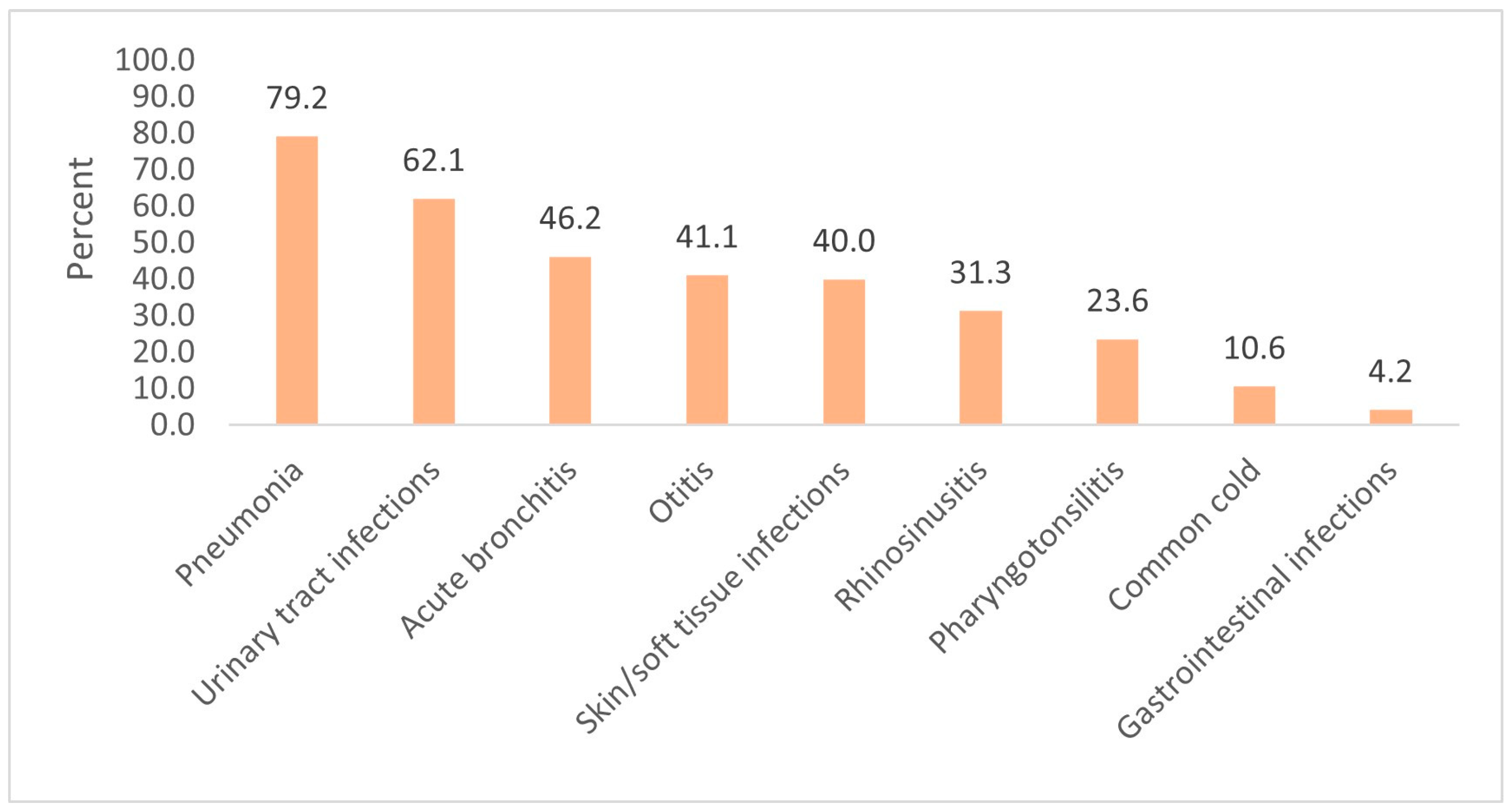
4.1. Diagnoses Treated with Antibiotics
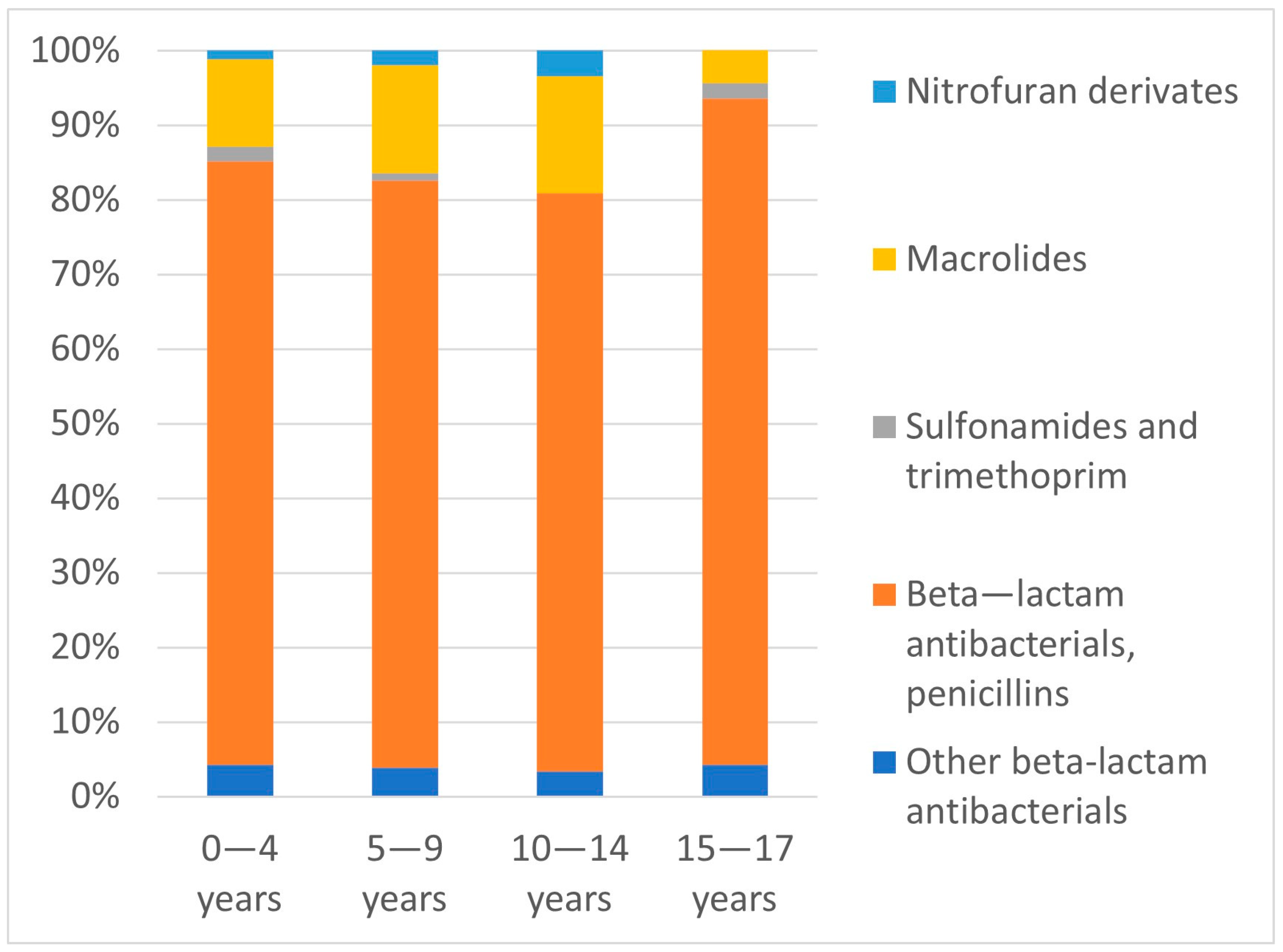
4.2. Choice of Antibiotic
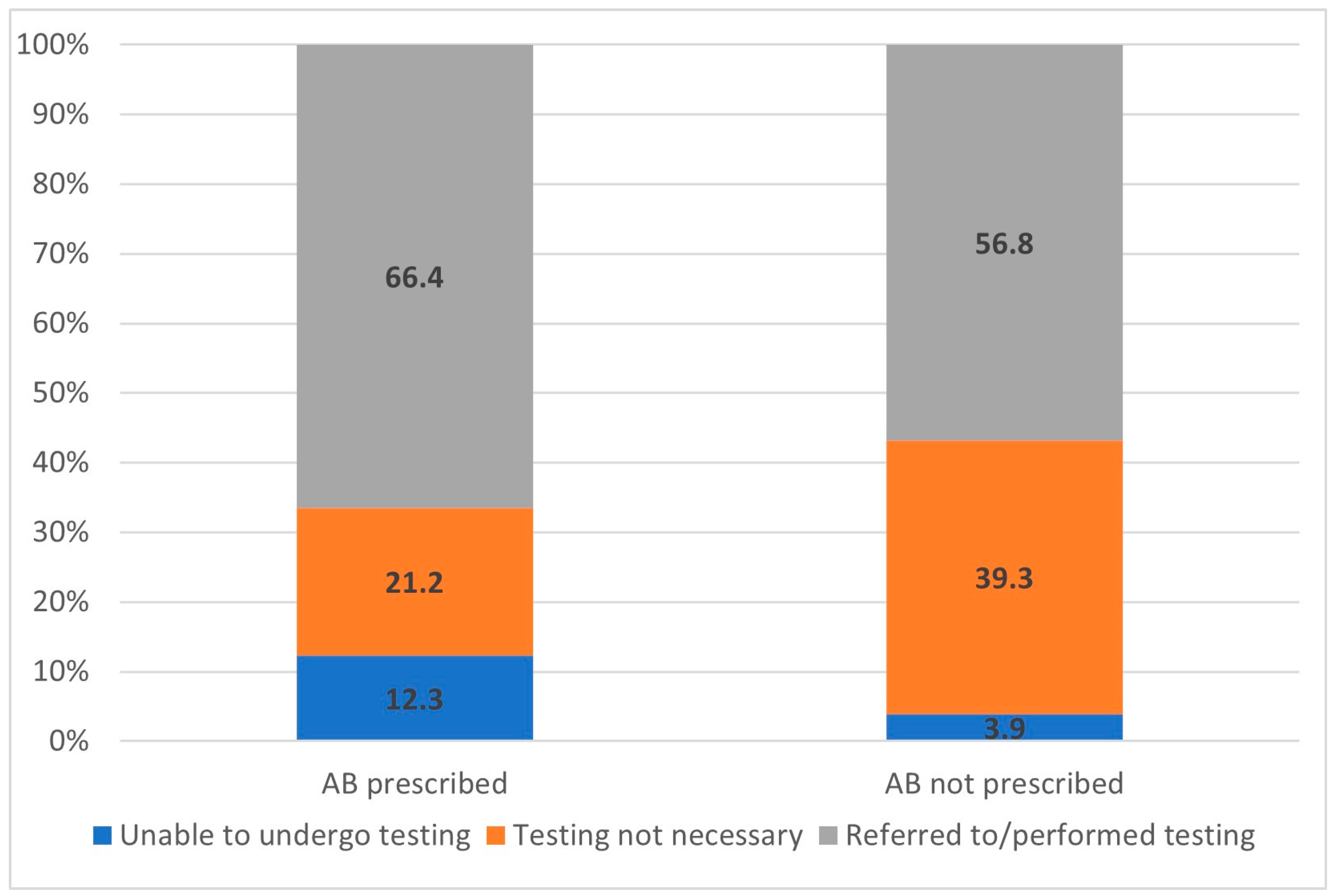
4.3. Diagnostic Management before Antibiotic Prescribing
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Clavenna, A.; Bonati, M. Drug prescriptions to outpatient children: A review of the literature. Eur. J. Clin. Pharmacol. 2009, 65, 749–755. [Google Scholar] [CrossRef] [PubMed]
- Jensen, J.N.; Bjerrum, L.; Boel, J.; Jarløv, J.O.; Arpi, M. Parents’ socioeconomic factors related to high antibiotic prescribing in primary health care among children aged 0–6 years in the Capital Region of Denmark. Scand. J. Prim. Health Care 2016, 34, 274–281. [Google Scholar] [CrossRef] [PubMed]
- Van Hecke, O.; Raymond, M.; Lee, J.J.; Turner, P.; Goyder, C.R.; Verbakel, J.Y.; van den Bruel, A.; Hayward, G. In-vitro diagnostic point-of-care tests in paediatric ambulatory care: A systematic review and meta-analysis. PLoS ONE 2020, 15. [Google Scholar] [CrossRef] [PubMed]
- Holstiege, J.; Schulz, M.; Akmatov, M.K.; Steffen, A.; Bätzing, J. Marked reductions in outpatient antibiotic prescriptions for children and adolescents—A population-based study covering 83% of the paediatric population, Germany, 2010 to 2018. Eurosurveillance 2020, 25, 1900599. [Google Scholar] [CrossRef]
- Goossens, H.; Ferech, M.; Vander Stichele, R.; Elseviers, M. Outpatient antibiotic use in Europe and association with resistance: A cross-national database study. Lancet 2005, 365, 579–587. [Google Scholar] [CrossRef]
- Dumpis, U.; Hahlin, A.; Varvuolyte, S.; Stenmark, S.; Veide, S.; Valinteliene, R.; Jurkeviciene, A.; Struwe, J. Antibiotic prescription and clinical management of common infections among general practitioners in Latvia, Lithuania, and Sweden: A pilot survey with a simple protocol. Eur. J. Clin. Microbiol. Infect. Dis. 2018, 37, 355–361. [Google Scholar] [CrossRef]
- Rossignoli, A.; Clavenna, A.; Bonati, M. Antibiotic prescription and prevalence rate in the outpatient paediatric population: Analysis of surveys published during 2000–2005. Eur. J. Clin. Pharmacol. 2007, 63, 1099–1106. [Google Scholar] [CrossRef]
- Haldrup, S.; Thomsen, R.W.; Bro, F.; Skov, R.; Bjerrum, L.; Søgaard, M. Microbiological point of care testing before antibiotic prescribing in primary care: Considerable variations between practices. BMC Fam. Pract. 2017, 18, 9. [Google Scholar] [CrossRef]
- Cals, J.W.L.; Butler, C.C.; Hopstaken, R.M.; Hood, K.; Dinant, G.J. Effect of point of care testing for C reactive protein and training in communication skills on antibiotic use in lower respiratory tract infections: Cluster randomised trial. BMJ 2009, 338, 1112–1115. [Google Scholar] [CrossRef]
- Lemiengre, M.B.; Verbakel, J.Y.; Colman, R.; Van Roy, K.; De Burghgraeve, T.; Buntinx, F.; Aertgeerts, B.; De Baets, F.; De Sutter, A. Point-of-care CRP matters: Normal CRP levels reduce immediate antibiotic prescribing for acutely ill children in primary care: A cluster randomized controlled trial. Scand. J. Prim. Health Care 2018, 36, 423–436. [Google Scholar] [CrossRef]
- Schot, M.J.C.; Van den Bruel, A.; Broekhuizen, B.D.L.; Cals, J.W.L.; Noteboom, E.A.; Balemans, W.; Hopstaken, R.M.; van Delft, S.; de Wit, N.J.; Verheij, T.J.M. Point-of-care C-reactive protein to assist in primary care management of children with suspected non-serious lower respiratory tract infection: A randomised controlled trial. BJGP Open 2018, 2, 1–10. [Google Scholar] [CrossRef]
- Population in Regions and Cities by Age and Gender at the Beginning of the Year by Territorial Unit, Age, Sex and Time Period. Available online: https://data.stat.gov.lv/pxweb/en/OSP_PUB/START__POP__IR__IRD/IRD040/ (accessed on 11 August 2021).
- Hak, E.; Verheij, T. Incidence of GP-diagnosed respiratory tract infections according to age, gender and high-risk co-morbidity: The Second Dutch National Survey of General Practice. Fam. Pract. 2006, 23, 291–294. [Google Scholar] [CrossRef] [PubMed]
- Pottegård, A.; Broe, A.; Aabenhus, R.; Bjerrum, L.; Hallas, J.; Damkier, P. Use of antibiotics in children: A Danish nationwide drug utilization study. Pediatr. Infect. Dis. J. 2015, 34, e16–e22. [Google Scholar] [CrossRef]
- AAbenhus, R.; Hansen, M.P.; Siersma, V.; Bjerrum, L. Clinical indications for antibiotic use in Danish general practice: Results from a nationwide electronic prescription database. Scand. J. Prim. Health Care 2017, 35, 162–169. [Google Scholar] [CrossRef] [PubMed]
- Dumpis, U.; Dimina, E.; Akermanis, M.; Tirans, E.; Veide, S. Assessment of antibiotic prescribing in Latvian general practitioners. BMC Fam. Pract. 2013, 14, 9. [Google Scholar] [CrossRef] [PubMed]
- Spurling, G.K.P.; Del Mar, C.B.; Dooley, L.; Foxlee, R.; Farley, R. Delayed antibiotic prescriptions for respiratory infections. Cochrane Database Syst. Rev. 2017, 9, CD004417. [Google Scholar] [CrossRef] [PubMed]
- Gradl, G.; Teichert, M.; Kieble, M.; Werning, J.; Schulz, M. Comparing outpatient oral antibiotic use in Germany and the Netherlands from 2012 to 2016. Pharmacoepidemiol. Drug Saf. 2018, 27, 1344–1355. [Google Scholar] [CrossRef] [PubMed]
- Ivanovska, V.; Hek, K.; Mantel-Teeuwisse, A.K.; Leufkens, H.G.M.; Van Dijk, L. Age-Specific Antibiotic Prescribing and Adherence to Guidelines in Pediatric Patients in Primary Care. Pediatr. Infect. Dis. J. 2018, 37, 218–223. [Google Scholar] [CrossRef] [PubMed]
- Lemiengre, M.; Verbakel, J.; De Burghgraeve, T.; Aertgeerts, B.; De Baets, F.; Buntinx, F.; De Sutter, A.; Bullens, D.; De Baets, F.; De Burghgraeve, T. Optimizing antibiotic prescribing for acutely ill children in primary care (ernie2 study protocol, part b): A cluster randomized, Factorial controlled trial evaluating the effect of a point-of-care c-reactive protein test and a brief intervention combined. BMC Pediatr. 2014, 14, 246. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Fleming-Dutra, K.E.; Hersh, A.L.; Shapiro, D.J.; Bartoces, M.; Enns, E.A.; File, T.M.; Finkelstein, J.A.; Gerber, J.S.; Hyun, D.Y.; Linder, J.A.; et al. Prevalence of inappropriate antibiotic prescriptions among us ambulatory care visits, 2010–2011. JAMA J. Am. Med. Assoc. 2016, 315, 1864–1873. [Google Scholar] [CrossRef]
- Lemiengre, M.B.; Verbakel, J.Y.; Colman, R.; De Burghgraeve, T.; Buntinx, F.; Aertgeerts, B.; De Baets, F.; De Sutter, A. Reducing inappropriate antibiotic prescribing for children in primary care: A cluster randomised controlled trial of two interventions. Br. J. Gen. Pract. 2018, 68, e204–e210. [Google Scholar] [CrossRef]
- Murphy, M.; Bradley, C.P.; Byrne, S. Antibiotic prescribing in primary care, adherence to guidelines and unnecessary prescribing—An Irish perspective. BMC Fam. Pract. 2012, 13. [Google Scholar] [CrossRef] [PubMed]
- van de Maat, J.S.; Peeters, D.; Nieboer, D.; van Wermeskerken, A.M.; Smit, F.J.; Noordzij, J.G.; Tramper-Stranders, G.; Driessen, G.J.A.; Obihara, C.C.; Punt, J.; et al. Evaluation of a clinical decision rule to guide antibiotic prescription in children with suspected lower respiratory tract infection in the Netherlands: A stepped-wedge cluster randomised trial. PLoS Med. 2020, 17, 1–19. [Google Scholar] [CrossRef] [PubMed]
- Akkerman, A.E.; Kuyvenhoven, M.M.; Van Der Wouden, J.C.; Verheij, T.J.M. Analysis of under-and overprescribing of antibiotics in acute otitis media in general practice. J. Antimicrob. Chemother. 2005, 56, 569–574. [Google Scholar] [CrossRef] [PubMed]
- Barrera, S.C.; Cancino, R.S.; Barreto, T.W. The impact of continuity of care on antibiotic prescribing in acute otitis media. Int. J. Pediatr. Otorhinolaryngol. 2019, 126, 109616. [Google Scholar] [CrossRef] [PubMed]
- Andre, M.; Vernby, Å.; Odenholt, I.; Stålsby Lundborg, C.; Axelsson, I.; Eriksson, M.; Runehagen, A.; Schwan, Å.; Molstad, S. Diagnosis-prescribing surveys in 2000, 2002 and 2005 in Swedish general practice: Consultations, diagnosis, diagnostics and treatment choices. Scand. J. Infect. Dis. 2008, 40, 648–654. [Google Scholar] [CrossRef]
- Cooke, J.; Butler, C.; Hopstaken, R.; Dryden, M.S.; McNulty, C.; Hurding, S.; Moore, M.; Livermore, D.M. Narrative review of primary care pointof- care testing (POCT) and antibacterial use in respiratory tract infection (RTI). BMJ Open Respir. Res. 2015, 2, 1–10. [Google Scholar] [CrossRef]
- Neumark, T.; Brudin, L.; Mölstad, S. Use of rapid diagnostic tests and choice of antibiotics in respiratory tract infections in primary healthcareA 6-y follow-up study. Scand. J. Infect. Dis. 2010, 42, 90–96. [Google Scholar] [CrossRef]
- Lindström, J.; Nordeman, L.; Hagström, B. What a difference a CRP makes. A prospective observational study on how point-of-care C-reactive protein testing influences antibiotic prescription for respiratory tract infections in Swedish primary health care. Scand. J. Prim. Health Care 2015, 33, 275–282. [Google Scholar] [CrossRef]
- Kip, M.M.A.; Hummel, J.M.; Eppink, E.B.; Koffijberg, H.; Hopstaken, R.M.; IJzerman, M.J.; Kusters, R. Understanding the adoption and use of point-of-care tests in Dutch general practices using multi-criteria decision analysis. BMC Fam. Pract. 2019, 20, 8. [Google Scholar] [CrossRef]
- Laurence, C.O.; Gialamas, A.; Bubner, T.; Yelland, L.; Willson, K.; Ryan, P.; Beilby, J. Patient satisfaction with point-of-care testing in general practice. Br. J. Gen. Pract. 2010, 60, 166–171. [Google Scholar] [CrossRef] [PubMed]
- Tonkin-Crine, S.K.G.; Tan, P.S.; van Hecke, O.; Wang, K.; Roberts, N.W.; Mccullough, A.; Hansen, M.P.; Butler, C.C.; Del Mar, C.B. Clinician-targeted interventions to influence antibiotic prescribing behaviour for acute respiratory infections in primary care: An overview of systematic reviews. Cochrane Database Syst. Rev. 2017, 9, CD012252. [Google Scholar] [CrossRef] [PubMed]
| Variable | Study Population |
|---|---|
| Mean age (all patients, years) | 6.1 (SD 4.3) |
| Age groups | |
| 0–4 years | 1094 (45.9%) |
| 5–9 years | 743 (31.2%) |
| 10–14 years | 371 (15.6%) |
| 15–17 years | 140 (5.9%) |
| Missing information on age | 35 (1.5%) |
| Gender | |
| Female | 1168 (49.0%) |
| Male | 1195 (50.1%) |
| Missing information on gender | 20 (0.8%) |
| Patients receiving an antibiotic prescription | 697 (29.2%) |
| Mean age of patients who received an antibiotic (years) | 5.8 (SD 4.4) |
| Diagnosis | Number of All Patients | Number of Patients Receiving an Antibiotic Prescription |
|---|---|---|
| Common cold | 973 (40.8%) | 103 (14.8%) |
| Otitis | 776 (32.6%) | 319 (45.8%) |
| Rhinosinusitis | 16 (0.7%) | 5 (0.7%) |
| Pharyngotonsillitis | 72 (3.0%) | 17 (2.4%) |
| Other otorhinolaryngological (ORL) infection | 14 (0.6%) | 0 (0.0%) |
| Acute bronchitis | 377 (15.8%) | 174 (25.0%) |
| Pneumonia | 72 (3.0%) | 57 (8.2%) |
| Gastrointestinal infections | 48 (2.0%) | 2 (0.3%) |
| Urinary tract infections | 29 (1.2%) | 18 (2.6%) |
| Skin/soft tissue infections | 5 (0.2%) | 2 (0.3%) |
| Bone and joint infections | 1 (0.0%) | 0 (0.0%) |
| Total | 2383 (100%) | 697 (100%) |
| Duration of Symptoms before Visit (Days) | AB Prescribed | AB Not Prescribed | Total |
|---|---|---|---|
| 1 | 23 (22.3%) | 80 (77.7%) | 103 (100.0%) |
| 2 | 159 (24.8%) | 482 (75.2%) | 641 (100.0%) |
| 3 | 222 (32.0%) | 472 (68.0%) | 694 (100.0%) |
| 4 | 140 (31.8%) | 300 (68.2%) | 440 (100.0%) |
| 5 | 74 (32.6%) | 153 (67.4%) | 227 (100.0%) |
| Total | 618 (29.4%) | 1487 (70.6%) | 2105 (100%) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Likopa, Z.; Kivite-Urtane, A.; Pavare, J. Latvian Primary Care Management of Children with Acute Infections: Antibiotic-Prescribing Habits and Diagnostic Process Prior to Treatment. Medicina 2021, 57, 831. https://doi.org/10.3390/medicina57080831
Likopa Z, Kivite-Urtane A, Pavare J. Latvian Primary Care Management of Children with Acute Infections: Antibiotic-Prescribing Habits and Diagnostic Process Prior to Treatment. Medicina. 2021; 57(8):831. https://doi.org/10.3390/medicina57080831
Chicago/Turabian StyleLikopa, Zane, Anda Kivite-Urtane, and Jana Pavare. 2021. "Latvian Primary Care Management of Children with Acute Infections: Antibiotic-Prescribing Habits and Diagnostic Process Prior to Treatment" Medicina 57, no. 8: 831. https://doi.org/10.3390/medicina57080831
APA StyleLikopa, Z., Kivite-Urtane, A., & Pavare, J. (2021). Latvian Primary Care Management of Children with Acute Infections: Antibiotic-Prescribing Habits and Diagnostic Process Prior to Treatment. Medicina, 57(8), 831. https://doi.org/10.3390/medicina57080831






