Blood Pressure and Cardio-Metabolic Risk Profile in Young Saudi Males in a University Setting
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Setting
2.2. Data Collection Tools
2.3. Indices’ Calculations
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Limitation
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Czeczelewski, M.; Czeczelewski, J.; Czeczelewska, E.; Galczak-Kondraciuk, A. Association of body composition indexes with cardio-metabolic risk factors. Obes. Med. 2020, 17, 100171. [Google Scholar] [CrossRef]
- Palaiodimos, L.; Kokkinidis, D.G.; Li, W.; Karamanis, D.; Ognibene, J.; Arora, S.; Southern, W.N.; Mantzoros, C.S. Severe obesity, increasing age and male sex are independently associated with worse in-hospital outcomes, and higher in-hospital mortality, in a cohort of patients with COVID-19 in the Bronx, New York. Metabolism 2020, 108, 154262. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Obesity and Overweight. Accessed February 2018. Available online: https://www.who.int/en/news-room/fact-sheets/detail/obesity-and-overweight (accessed on 9 June 2021).
- Al-Nozha, M.M.; Al-Mazrou, Y.Y.; Al-Maatouq, M.A.; Arafah, M.R.; Khalil, M.Z.; Khan, N.B.; Al-Marzouki, K.; Abdullah, M.A.; Al-Khadra, A.H.; Al-Harthi, S.S.; et al. Obesity in Saudi Arabia. Saudi Med. J. 2005, 26, 824–829. [Google Scholar]
- Al-Hariri, M.; Aldhafery, B. Association of Hypertension and Lipid Profile with Osteoporosis. Scientifica 2020, 2020, 7075815. [Google Scholar] [CrossRef] [PubMed]
- Al-Hariri, M.T.; Elkilany, A.M.; Alkahtani, S.A. Effects of potentially modifiable risk factors on the health of adults in the Eastern Province of KSA. J. Taibah Univ. Med. Sci. 2018, 13, 16–21. [Google Scholar] [CrossRef] [PubMed]
- Teo, K.K.; Rafiq, T.; Anand, S.S.; Schulze, K.M.; Yusuf, S.; McDonald, S.D.; Wahi, G.; Abdalla, N.; Desai, D.; Atkinson, S.A.; et al. Associations of cardiometabolic outcomes with indices of obesity in children aged 5 years and younger. PLoS ONE 2019, 14, e0218816. [Google Scholar] [CrossRef]
- WHO Expert Consultation. Appropriate body-mass index for Asian populations and its implications for policy and inter-vention strategies. Lancet 2004, 363, 157. [Google Scholar] [CrossRef]
- James, P.T.; Leach, R.; Kalamara, E.; Shayeghi, M. The Worldwide Obesity Epidemic. Obes. Res. 2001, 9, 228S–233S. [Google Scholar] [CrossRef]
- Kim, N.H.; Lee, J.; Kim, T.J.; Kim, N.H.; Choi, K.M.; Baik, S.H.; Choi, D.S.; Pop-Busui, R.; Park, Y.; Kim, S.G. Body Mass Index and Mortality in the General Population and in Subjects with Chronic Disease in Korea: A Nationwide Cohort Study (2002–2010). PLoS ONE 2015, 10, e0139924. [Google Scholar] [CrossRef]
- Mathers, C.D.; Loncar, D. Projections of Global Mortality and Burden of Disease from 2002 to 2030. PLoS Med. 2006, 3, e442. [Google Scholar] [CrossRef]
- Alkahtani, S.; Elkilany, A.; Alhariri, M. Association between sedentary and physical activity patterns and risk factors of metabolic syndrome in Saudi men: A cross-sectional study. BMC Public Health 2015, 15, 1234. [Google Scholar] [CrossRef] [PubMed]
- Gutierrez, J.; Alloubani, A.; Mari, M.; Alzaatreh, M. Cardiovascular Disease Risk Factors: Hypertension, Diabetes Mellitus and Obesity among Tabuk Citizens in Saudi Arabia. Open Cardiovasc. Med. J. 2018, 12, 41–49. [Google Scholar] [CrossRef]
- Bano, N. Prehypertension among young adult females in Dammam, Saudi Arabia. East. Mediterr. Health J. 2013, 19, 899–900. [Google Scholar] [CrossRef]
- Elliott, W.J.; Black, H.R. Prehypertension. Nat. Clin. Pract. Cardiovasc. Med. 2007, 4, 538–548. [Google Scholar] [CrossRef] [PubMed]
- Baig, M.; Gazzaz, Z.J.; Gari, A.M.; Al-Attallah, H.G.; Al-Jedaani, K.S.; Mesawa, A.T.; Al-Hazmi, A. Prevalence of obesity and hypertension among University students’ and their knowledge and attitude towards risk factors of Cardiovascular Disease (CVD) in Jeddah, Saudi Arabia. Pak. J. Med. Sci. 1969, 31, 816–820. [Google Scholar] [CrossRef]
- Pescatello, L.S.; Medicine, A.C.O.S.; Riebe, D.; Thompson, P.D. ACSM’s Guidelines for Exercise Testing and Prescription; Wolters Kluwer Health: Philadelphia, PA, USA, 2013. [Google Scholar]
- El Ansari, W.; El Ashker, S.; Moseley, L. Associations between physical activity and health parameters in adolescent pupils in Egypt. Int. J. Environ. Res. Public Health 2010, 7, 1649–1669. [Google Scholar] [CrossRef]
- Al-Attas, O.S.; Al-Daghri, N.M.; Alokail, M.S.; Alkharfy, K.M.; Draz, H.; Yakout, S.; Sabico, S.; Chrousos, G. Association of body mass index, sagittal abdominal diameter and waist-hip ratio with cardiometabolic risk factors and adipocytokines in Arab children and adolescents. BMC Pediatr. 2012, 12, 119. [Google Scholar] [CrossRef] [PubMed]
- Bilo, G.; Sala, O.; Perego, C.; Faini, A.; Gao, L.; Głuszewska, A.; Ochoa, J.E.; Pellegrini, D.; Lonati, L.M.; Parati, G. Impact of cuff positioning on blood pressure measurement accuracy: May a specially de-signed cuff make a difference? Hypertens. Res. 2017, 40, 573–580. [Google Scholar] [CrossRef]
- Chahine, M.N.; Topouchian, J.; Zelveian, P.; Hakobyan, Z.; Melkonyan, A.; Azaki, A.; Diab, R.; Harb, A.; Asmar, R. Validation of BP devices QardioArm® in the general population and Omron M6 Comfort® in type II diabetic patients according to the European Society of Hypertension International Protocol (ESH-IP). Med. Devices Évid. Res. 2017, 11, 11–20. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Faria, C.; Aguiar, L.; Lara, E.; Souza, L.; Martins, J.; Teixeira-Salmela, L. Dynamometry for the assessment of grip, pinch, and trunk strength in subjects with chronic stroke: Reliability and various sources of outcome values. Int. J. Phys. Med. Rehabil. 2013, 1, 1–5. [Google Scholar]
- Kaplan, N.M. The 6th Joint National Committee Report (JNC-6): New Guidelines for Hypertension Therapy from the USA. Keio J. Med. 1998, 47, 99–105. [Google Scholar] [CrossRef]
- Freedman, D.S.; Lawman, H.G.; Galuska, D.A.; Goodman, A.B.; Berenson, G.S. Tracking and Variability in Childhood Levels of BMI: The Bogalusa Heart Study. Obesity 2018, 26, 1197–1202. [Google Scholar] [CrossRef] [PubMed]
- Sesso, H.D.; Stampfer, M.J.; Rosner, B.; Hennekens, C.H.; Gaziano, J.M.; Manson, J.E.; Glynn, R.J. Systolic and Diastolic Blood Pressure, Pulse Pressure, and Mean Arterial Pressure as Predictors of Cardiovascular Disease Risk in Men. Hypertension 2000, 36, 801–807. [Google Scholar] [CrossRef] [PubMed]
- Bergman, R.N.; Stefanovski, D.; Buchanan, T.A.; Sumner, A.E.; Reynolds, J.C.; Sebring, N.G.; Xiang, A.; Watanabe, R.M. A Better Index of Body Adiposity. Obesity 2011, 19, 1083–1089. [Google Scholar] [CrossRef]
- Taing, K.Y.; Farkouh, M.E.; Moineddin, R.; Tu, J.V.; Jha, P. Age and sex-specific associations of anthropometric measures of adiposity with blood pressure and hypertension in India: A cross-sectional study. BMC Cardiovasc. Disord. 2016, 16, 247. [Google Scholar] [CrossRef] [PubMed]
- Deurenberg, P.; Weststrate, J.A.; Seidell, J. Body mass index as a measure of body fatness: Age- and sex-specific prediction formulas. Br. J. Nutr. 1991, 65, 105–114. [Google Scholar] [CrossRef]
- Skallerup, A.; Nygaard, L.; Olesen, S.S.; Vinter-Jensen, L.; Køhler, M.; Rasmussen, H.H. Can We Rely on Predicted Basal Metabolic Rate in Patients With Intestinal Failure on Home Parenteral Nutrition? J. Parenter. Enter. Nutr. 2017, 41, 1139–1145. [Google Scholar] [CrossRef] [PubMed]
- Mirmiran, P.; Esmaillzadeh, A.; Azizi, F. Detection of cardiovascular risk factors by anthropometric measures in Tehranian adults: Receiver operating characteristic (ROC) curve analysis. Eur. J. Clin. Nutr. 2004, 58, 1110–1118. [Google Scholar] [CrossRef] [PubMed]
- Gharipour, M.; Sadeghi, M.; Dianatkhah, M.; Bidmeshgi, S.; Ahmadi, A.; Tahri, M.; Sarrafzadegan, N. The Cut-Off Values of Anthropometric Indices for Identifying Subjects at Risk for Metabolic Syndrome in Iranian Elderly Men. J. Obes. 2014, 2014, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Aldiab, A.; Shubair, M.M.; Al-Zahrani, J.M.; Aldossari, K.K.; Al-Ghamdi, S.; Househ, M.; Razzak, H.A.; El-Metwally, A.; Jradi, H. Prevalence of hypertension and prehypertension and its associated cardioembolic risk factors; a population based cross-sectional study in Alkharj, Saudi Arabia. BMC Public Health 2018, 18, 1327. [Google Scholar] [CrossRef]
- Okafor, C.I.; Fasanmade, O.; Ofoegbu, E.; Ohwovoriole, A.E. Comparison of the performance of two measures of central adiposity among apparently healthy Nigerians using the receiver operating characteristic analysis. Indian J. Endocrinol. Metab. 2011, 15, 320–326. [Google Scholar] [CrossRef] [PubMed]
- Ross, R.; Neeland, I.J.; Yamashita, S.; Shai, I.; Seidell, J.; Magni, P.; Santos, R.D.; Arsenault, B.; Cuevas, A.; Hu, F.B.; et al. Waist circumference as a vital sign in clinical practice: A Consensus Statement from the IAS and ICCR Working Group on Visceral Obesity. Nat. Rev. Endocrinol. 2020, 16, 177–189. [Google Scholar] [CrossRef] [PubMed]
- Hu, L.; Huang, X.; You, C.; Li, J.; Hong, K.; Li, P.; Wu, Y.; Wu, Q.; Bao, H.; Cheng, X. Prevalence and Risk Factors of Prehypertension and Hypertension in Southern China. PLoS ONE 2017, 12, e0170238. [Google Scholar] [CrossRef] [PubMed]
- Alhariri, M. Association of blood pressure and random blood glucose with weight status of normal male population in Dammam Saudi Arabia. Pak. J. Physiol. 2012, 8, 36–38. [Google Scholar]
- Sabra, A.A.; Taha, A.Z.; Al-Sebiany, A.M.; Al-Kurashi, N.Y.; Al-Zubier, A.G. Coronary heart disease risk factors: Prevalence and be-havior among male university students in Dammam City, Saudi Arabia. J. Egypt. Public Health Assoc. 2007, 82, 21–42. [Google Scholar]
- Al-Hazzaa, H.M. Rising trends in BMI of Saudi adolescents: Evidence from three national cross sectional studies. Asia Pac. J. Clin. Nutr. 2007, 16, 462–466. [Google Scholar] [PubMed]
- Al-Hariri, M. Life style activities and feeling state responses in community sample of diabetic patients in Eastern Providence Saudi Arabia. J. Diabetes Metab. Disord. 2019, 18, 301–305. [Google Scholar] [CrossRef] [PubMed]
- Alhariri, M.; Alkahtani, S.A.; Abdelgayed, A.M. Impact of life behaviour on students physical fitness at university of dammam in Saudi Arabia. Acad. Res. Int. 2014, 5, 87. [Google Scholar]
- Tayem, Y.I.; Yaseen, N.A.; Khader, W.T.; Abu Rajab, L.O.; Ramahi, A.B.; Saleh, M.H. Prevalence and risk factors of obesity and hyper-tension among students at a central university in the West Bank. Libyan J. Med. 2012, 7, 19222. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Y.; Wang, L.; Xue, B.; Wang, Y. Associations between general and central obesity and hypertension among children: The Childhood Obesity Study in China Mega-Cities. Sci. Rep. 2017, 7, 1–7. [Google Scholar] [CrossRef]
- DeMarco, V.; Aroor, A.R.; Sowers, J.R. The pathophysiology of hypertension in patients with obesity. Nat. Rev. Endocrinol. 2014, 10, 364–376. [Google Scholar] [CrossRef] [PubMed]
| Parameter | Formula | Reference |
|---|---|---|
| Mean arterial pressure | MAP = diastolic blood pressure (DBP) + 1/3 [systolic blood pressure (SBP) − DBP]. | [25] |
| Body adiposity index | BAI = (Hip circumference [HC] in centimeters)/((height in meters)1.5) − 18). | [26] |
| Waist-to-Hip Ratio | WHR = Waist circumference (WC) in centimeters ÷ HC in centimeters. | [27] |
| Body Mass Index (kg/m2) | BMI = (weight in kilograms)/(the squared height in meters). | [24] |
| Body fat percentage | BFP = (1.20 × BMI) + (0.23 × age) − (10.8 × sex) − 5.4, (sex: females = 0, males = 1). | [28] |
| Basal Metabolic Rate (kcal/day) | Men BMR = 66.5 + (13.8 × weight) + (5.0 × height) − (6.8 × age). | [29] |
| N | p Value for Trend | Hypertension Group | Total (n = 284) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Normal (n = 67) | Prehypertension (n = 175) | Stage-1 (n = 34) | Stage-2 (n = 8) | |||||||||
| Mean | S.E. | Mean | S.E. | Mean | S.E. | Mean | S.E. | Mean | S.E. | |||
| Age (years) | 284 | 0.181 | 18.5 | 0.1 | 18.7 | 0.1 | 18.6 | 0.2 | 19.3 | 0.3 | 18.6 | 0.1 |
| Heart Rate (BPM) | 284 | 0.001 * | 71.9 | 1.5 | 80.0 | 0.6 | 90.2 | 2.9 | 100.3 | 5.5 | 79.9 | 0.7 |
| Pulse pressure (mmHg) | 284 | 0.003 * | 45.8 | 0.6 | 55.5 | 0.5 | 67.3 | 2.2 | 81.3 | 8.9 | 55.4 | 0.7 |
| Mean arterial pressure | 284 | 0.008 * | 80.6 | 0.5 | 90.6 | 0.3 | 101.9 | 1.1 | 119.0 | 7.8 | 90.4 | 0.6 |
| Height (m) | 284 | 0.367 | 1.7 | 0.0 | 1.7 | 0.0 | 1.7 | 0.0 | 1.7 | 0.0 | 1.7 | 0.0 |
| Weight (kg) | 284 | 0.035 * | 59.4 | 1.2 | 82.7 | 1.7 | 119.2 | 5.3 | 123.5 | 14.2 | 82.7 | 1.7 |
| Hip circumference (cm) | 284 | 0.030 * | 90.2 | 1.1 | 107.3 | 1.0 | 124.7 | 2.8 | 128.4 | 8.4 | 105.9 | 1.0 |
| Waist circumference (cm) | 284 | 0.016 * | 72.2 | 1.3 | 91.5 | 1.2 | 113.5 | 3.4 | 121.2 | 12.5 | 90.4 | 1.2 |
| Body adiposity index | 284 | 0.014 * | 23.2 | 0.5 | 30.2 | 0.5 | 36.4 | 1.2 | 39.4 | 3.8 | 29.6 | 0.4 |
| Waist-to-Hip Ratio | 284 | 0.008 * | 0.8 | 0.0 | 0.8 | 0.0 | 0.9 | 0.0 | 0.9 | 0.1 | 0.8 | 0.0 |
| BMI (kg/m2) | 284 | 0.020 * | 20.9 | 0.4 | 28.4 | 0.6 | 39.3 | 1.6 | 42.2 | 4.9 | 28.3 | 0.6 |
| Body fat percentage | 284 | 0.020 * | 23.9 | 0.5 | 33.0 | 0.7 | 46.1 | 2.0 | 49.7 | 5.9 | 32.9 | 0.7 |
| Basal Metabolic Rate (kcal/day) | 284 | 0.042 * | 1561.9 | 13.0 | 1805.6 | 17.4 | 2190.0 | 54.9 | 2213.4 | 147.2 | 1805.6 | 17.6 |
| Normal vs. Prehypertension | Normal vs. Hypertension (Stage I or II) | |||||
|---|---|---|---|---|---|---|
| OR | 95% C.I. | OR | 95% C.I. | |||
| Lower | Upper | Lower | Upper | |||
| Age | 1.25 | 0.93 | 1.69 | 1.36 | 0.86 | 2.15 |
| Heart Rate | 1.09 | 1.06 | 1.13 | 1.10 | 1.06 | 1.14 |
| Pulse pressure | 1.37 | 1.26 | 1.49 | 1.33 | 1.18 | 1.49 |
| Mean arterial pressure | 1.94 | 1.60 | 2.37 | 1.72 | 1.29 | 2.30 |
| Weight | 1.13 | 1.09 | 1.18 | 1.12 | 1.07 | 1.17 |
| Hip circumference | 1.18 | 1.12 | 1.24 | 1.18 | 1.11 | 1.26 |
| Waist circumference | 1.14 | 1.10 | 1.19 | 1.12 | 1.08 | 1.16 |
| Body adiposity index | 1.30 | 1.20 | 1.42 | 1.40 | 1.24 | 1.58 |
| BMI | 1.37 | 1.24 | 1.53 | 1.37 | 1.21 | 1.55 |
| Body fat percentage | 1.31 | 1.20 | 1.43 | 1.30 | 1.17 | 1.44 |
| Basal Metabolic Rate | 1.01 | 1.01 | 1.01 | 1.01 | 1.01 | 1.02 |
| Anthropometric Indicator | n (%) | Crude OR (95% CI) | Age Adjusted OR (95% CI) |
|---|---|---|---|
| Body mass index (kg/m2) | |||
| <18.5 | 20 (7.0) | 0.28 (0.10, 0.79) | 0.21 (0.07, 0.63) |
| 18.5–24.9 | 118 (41.5) | 1 | 1 |
| 25.0–29.9 | 47 (16.5) | 7.12 (2.40, 21.14) | 6.85 (2.28, 2.55) |
| 30+ | 99 (34.9) | 32.11 (7.55, 136.57) | 32.26 (7.54, 137.99) |
| Waist circumference (cm) | |||
| <cut-off (92) | 174 (61.3) | 1 | 1 |
| ≥cut-off | 110 (38.7) | 32.20 (7.69, 134.83) | 35.26 (8.36, 148.68) |
| Waist-hip circumference ratio | |||
| <cut-off (0.89) | 197 (69.4) | 1 | 1 |
| ≥cut-off | 87 (30.6) | 5.01 (2.18, 11.48) | 5.19 (2.24, 12.0) |
| Waist-height ratio | |||
| <0.5 | 263 (92.6) | 1 | 1 |
| ≥0.5 | 21 (7.4) | * | * |
| Cut Off | Sensitivity | Specificity | |
|---|---|---|---|
| BMI (kg/m2) | 22.23 | 0.811 | 0.806 |
| Waist circumference (cm) | 75.24 | 0.876 | 0.746 |
| Waist-hip circumference ratio | 0.785 | 0.908 | 0.092 |
| Waist-height ratio | 0.455 | 0.811 | 0.776 |
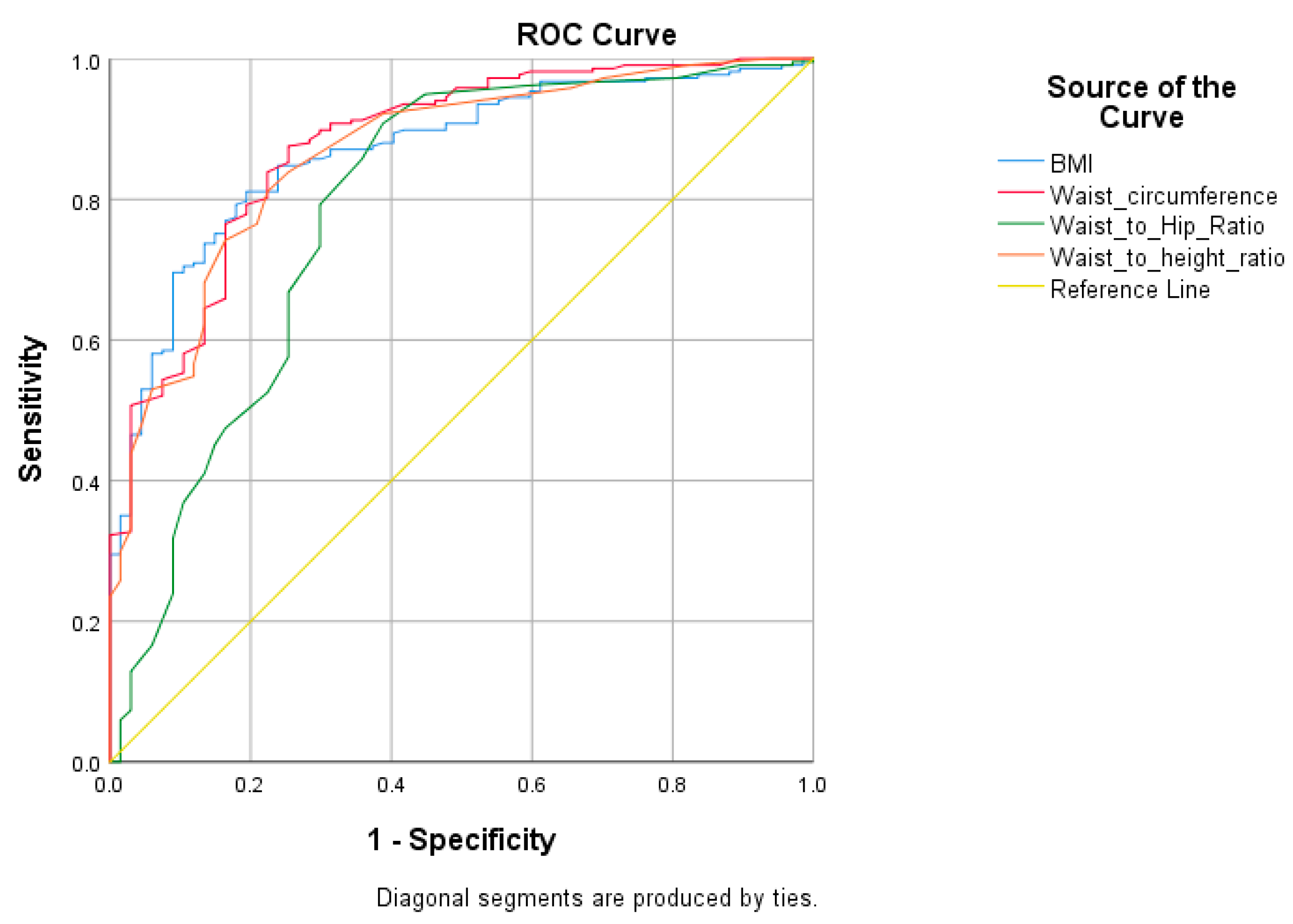
| Test Result Variable(s) | Area | Std. Error a | Asymptotic Sig.b | Asymptotic 95% Confidence Interval | |
|---|---|---|---|---|---|
| Lower Bound | Upper Bound | ||||
| Body Mass Index | 0.868 | 0.023 | <0.001 | 0.823 | 0.914 |
| Waist circumference | 0.878 | 0.024 | <0.001 | 0.831 | 0.924 |
| Waist-to-Hip Ratio | 0.787 | 0.036 | <0.001 | 0.716 | 0.858 |
| Waist-to-height ratio | 0.865 | 0.025 | <0.001 | 0.817 | 0.913 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
EL-Ashker, S.; Pednekar, M.S.; Narake, S.S.; Albaker, W.; Al-Hariri, M. Blood Pressure and Cardio-Metabolic Risk Profile in Young Saudi Males in a University Setting. Medicina 2021, 57, 755. https://doi.org/10.3390/medicina57080755
EL-Ashker S, Pednekar MS, Narake SS, Albaker W, Al-Hariri M. Blood Pressure and Cardio-Metabolic Risk Profile in Young Saudi Males in a University Setting. Medicina. 2021; 57(8):755. https://doi.org/10.3390/medicina57080755
Chicago/Turabian StyleEL-Ashker, Said, Mangesh S. Pednekar, Sameer S. Narake, Waleed Albaker, and Mohammed Al-Hariri. 2021. "Blood Pressure and Cardio-Metabolic Risk Profile in Young Saudi Males in a University Setting" Medicina 57, no. 8: 755. https://doi.org/10.3390/medicina57080755
APA StyleEL-Ashker, S., Pednekar, M. S., Narake, S. S., Albaker, W., & Al-Hariri, M. (2021). Blood Pressure and Cardio-Metabolic Risk Profile in Young Saudi Males in a University Setting. Medicina, 57(8), 755. https://doi.org/10.3390/medicina57080755







