The Effect of Three Surgical Therapies to Increase Keratinized Mucosa Surrounding Dental Implants with Peri-Implantitis: A Pilot Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Sample Size Calculation
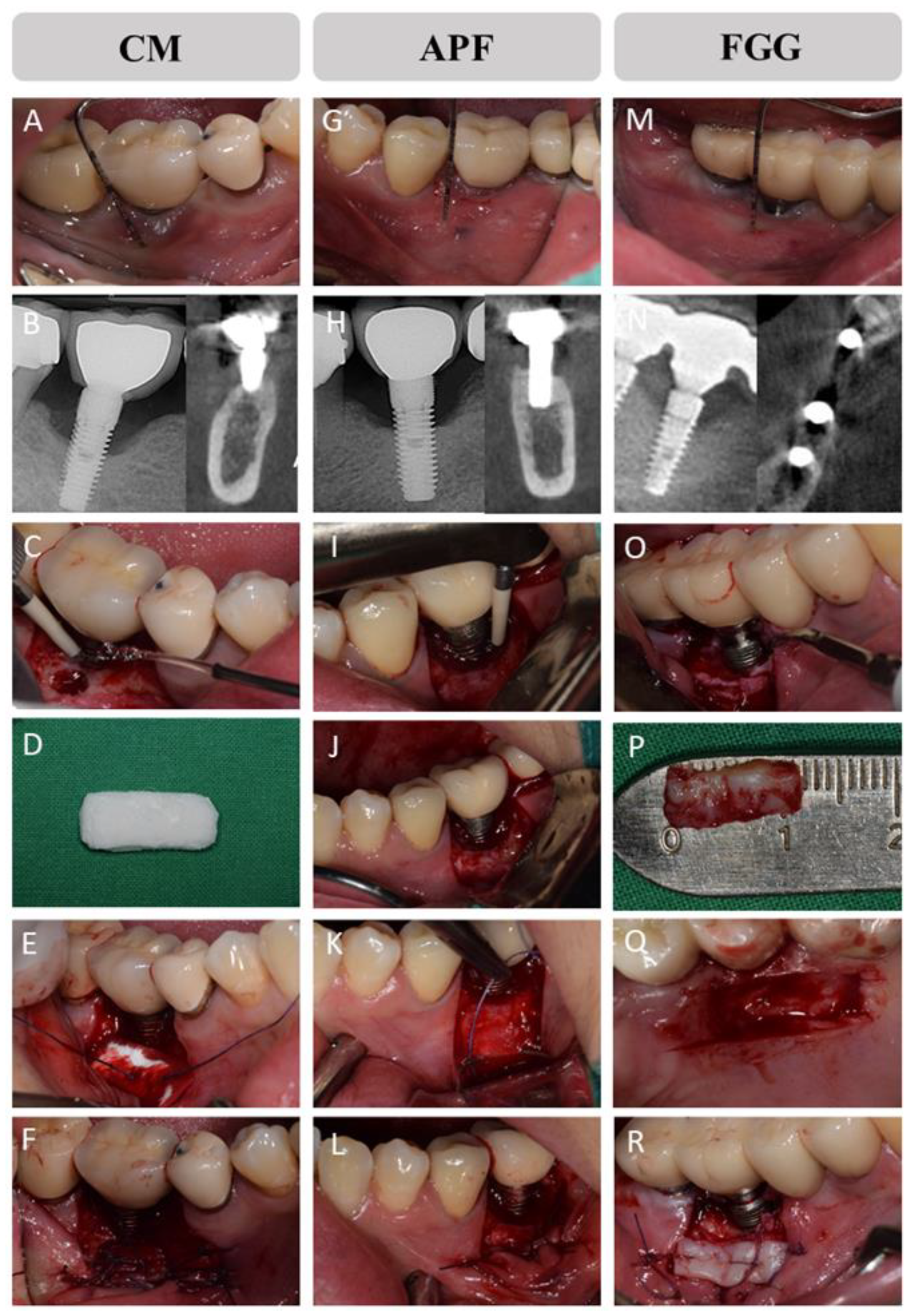
2.3. Allocation and Surgical Procedures
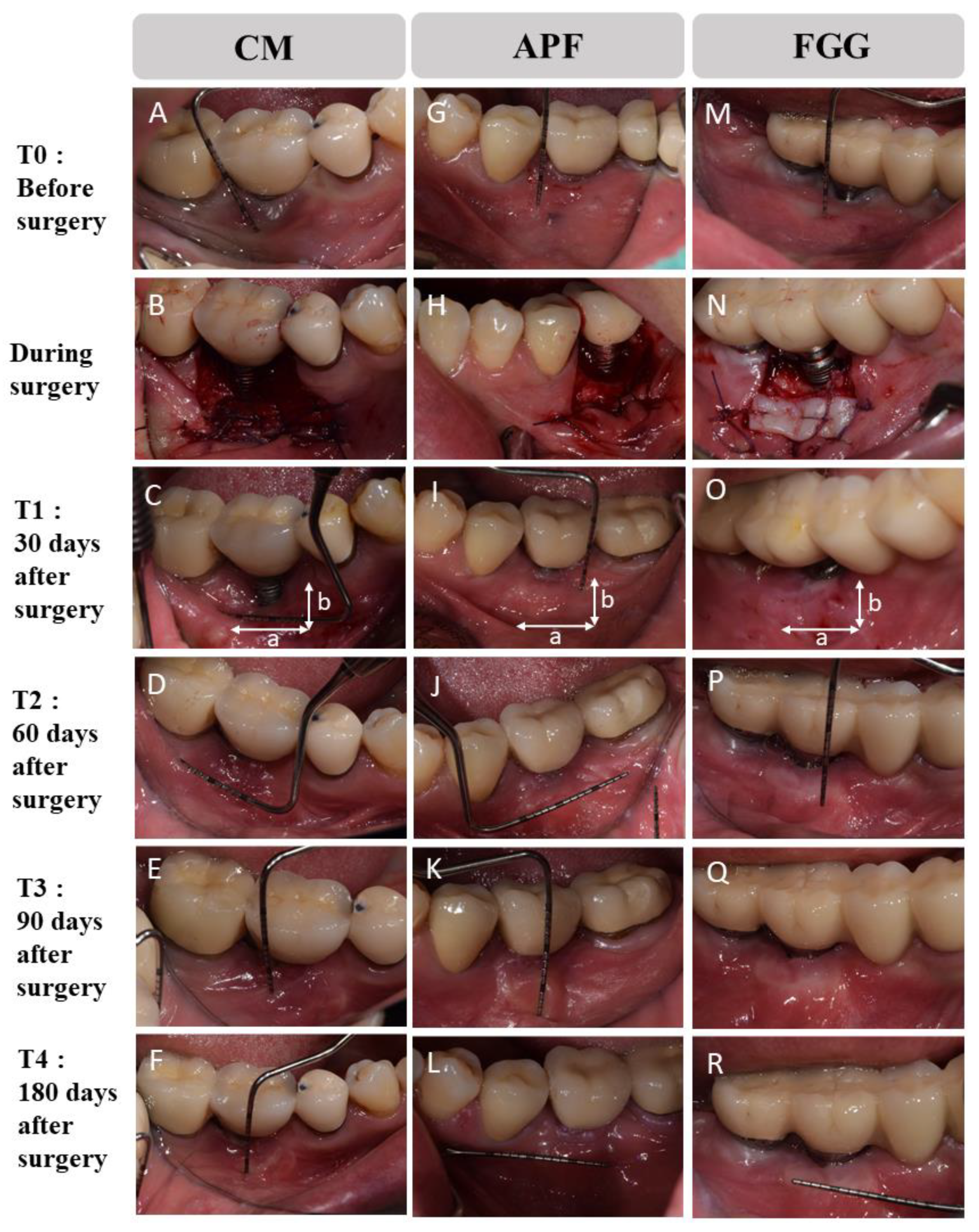
2.4. Clinical Assessment
2.5. Statistical Analysis
3. Results
3.1. Baseline Characteristics
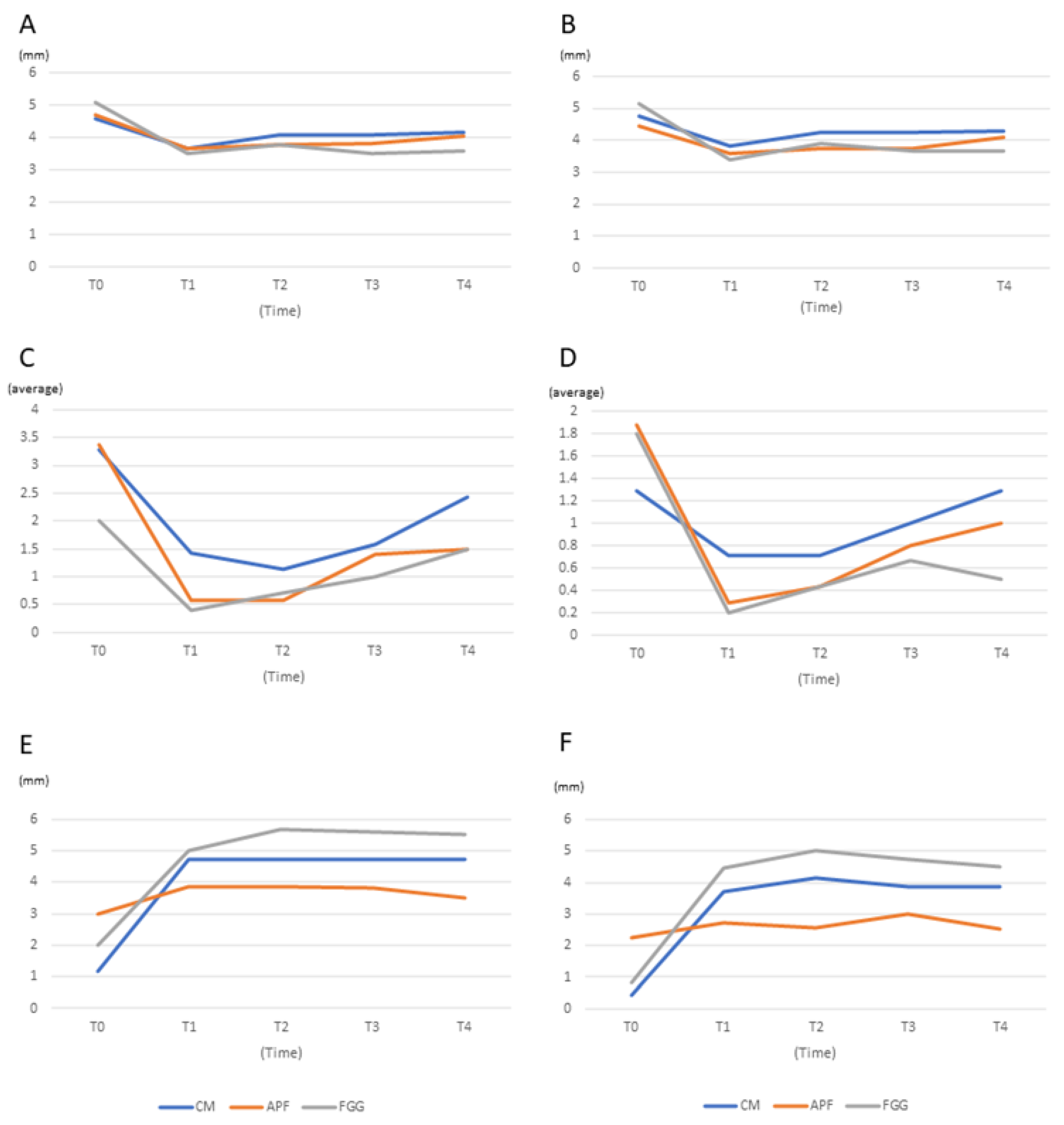
3.2. Width of KM
3.2.1. Horizontal Width
3.2.2. Vertical Width
3.3. Probing Pocket Depth (PPD)
3.3.1. Six Whole Sites
3.3.2. Three Buccal Sites
3.4. Bleeding on Probing (BOP)
3.4.1. Six Whole Sites
3.4.2. Three Buccal Sites
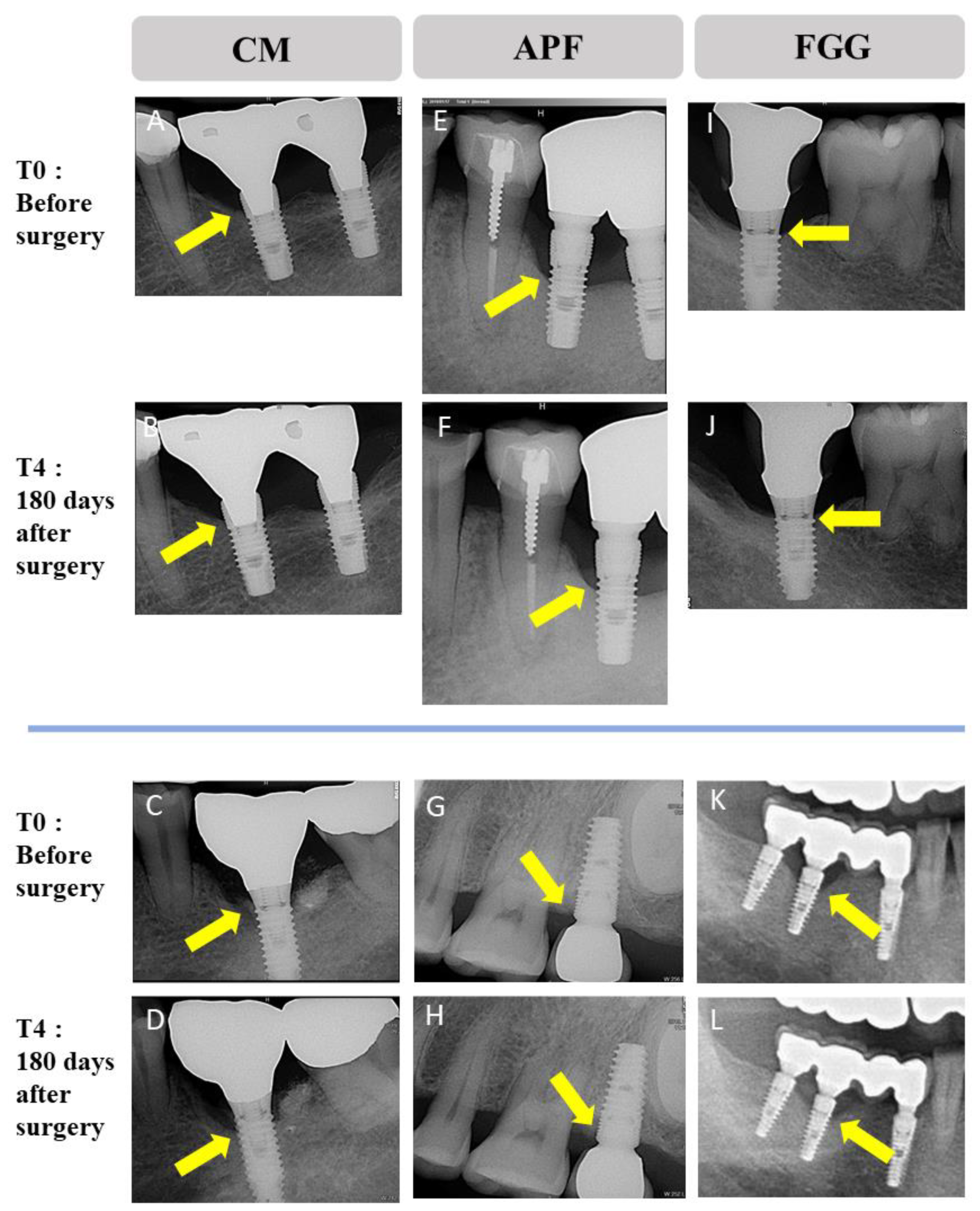
3.5. Bone-Level Change around Implant
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Arnoux, J.P.; Papasotiriou, A.; Weisgold, A.S. A revised technique for stage-two surgery in the severely resorbed mandible: A technical note. Int. J. Oral Maxillofac. Implant. 1998, 13, 565–568. [Google Scholar]
- Zigdon, H.; Machtei, E.E. The dimensions of keratinized mucosa around implants affect clinical and immunological parameters. Clin. Oral Implant. Res. 2008, 19, 387–392. [Google Scholar] [CrossRef] [PubMed]
- Wennström, J.L.; Derks, J. Is there a need for keratinized mucosa around implants to maintain health and tissue stability? Clin. Oral Implant. Res. 2012, 23, 136–146. [Google Scholar] [CrossRef] [PubMed]
- Lin, G.-H.; Chan, H.-L.; Wang, H.-L. The Significance of Keratinized Mucosa on Implant Health: A Systematic Review. J. Periodontol. 2013, 84, 1755–1767. [Google Scholar] [CrossRef] [PubMed]
- Brito, C.; Tenenbaum, H.C.; Wong, B.K.C.; Schmitt, C.; Nogueira-Filho, G. Is keratinized mucosa indispensable to maintain peri-implant health? A systematic review of the literature. J. Biomed. Mater. Res. Part B Appl. Biomater. 2013, 102, 643–650. [Google Scholar] [CrossRef]
- Bengazi, F.; Wennström, J.L.; Lekholm, U. Recession of the soft tissue margin at oral implants. A 2-year longitudinal prospective study. Clin. Oral Implant. Res 1996, 7, 303–310. [Google Scholar] [CrossRef] [PubMed]
- Wennstrom, J.; Lindhe, J. Role of attached gingiva for maintenance of periodontal health. Healing following excisional and grafting procedures in dogs. J. Clin. Periodontol. 1983, 10, 206–221. [Google Scholar] [CrossRef] [PubMed]
- Wennstrom, J.; Lindhe, J. Plaque-induced gingival inflammation in the absence of attached gingiva in dogs. J. Clin. Periodontol. 1983, 10, 266–276. [Google Scholar] [CrossRef]
- Kennedy, J.E.; Bird, W.C.; Palcanis, K.G.; Dorfman, H.S. A longitudinal evaluation of varying widths of attached gingiva. J. Clin. Periodontol. 1985, 12, 667–675. [Google Scholar] [CrossRef]
- Chung, D.M.; Oh, T.-J.; Shotwell, J.L.; Misch, C.E.; Wang, H.-L. Significance of Keratinized Mucosa in Maintenance of Dental Implants With Different Surfaces. J. Periodontol. 2006, 77, 1410–1420. [Google Scholar] [CrossRef] [Green Version]
- Boynueğri, D.; Nemli, S.K.; Kasko, Y.A. Significance of keratinized mucosa around dental implants: A prospective comparative study. Clin. Oral Implant. Res. 2012, 24, 928–933. [Google Scholar] [CrossRef] [PubMed]
- Wennström, J.L.; Bengazi, F.; Lekholm, U. The influence of the masticatory mucosa on the peri-implant soft tissue condition. Clin. Oral Implant. Res. 1994, 5, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Heckmann, S.M.; Schrott, A.; Graef, F.; Wichmann, M.G.; Weber, H.-P. Mandibular two-implant telescopic overdentures. 10-year clinical and radiographical results. Clin. Oral Implant. Res. 2004, 15, 560–569. [Google Scholar] [CrossRef]
- Lang, N.P.; Lindhe, J. Clinical Periodontology and Implant Dentistry, 5th ed.; John Wiley & Sons: New York, NY, USA, 2015; pp. 965–967. [Google Scholar]
- Lim, H.-C.; An, S.-C.; Lee, D.-W. A retrospective comparison of three modalities for vestibuloplasty in the posterior mandible: Apically positioned flap only vs. free gingival graft vs. collagen matrix. Clin. Oral Investig. 2017, 22, 2121–2128. [Google Scholar] [CrossRef] [PubMed]
- Renvert, S.; Persson, G.R.; Pirih, F.Q.; Camargo, P.M. Peri-implant health, peri-implant mucositis, and peri-implantitis: Case definitions and diagnostic considerations. J. Clin. Periodontol. 2018, 45, 278–285. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Heitz-Mayfield, L.J.; Salvi, G.E. Peri-implant mucositis. J. Clin. Periodontol. 2018, 45, 237–245. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Roos-Jansåker, A.M.; Lindahl, C.; Renvert, H.; Renvert, S. Nine to fourteen year follow up of implant treatment. Part II: Presence of peri-implant lesions. J. Clin. Periodontol. 2006, 33, 290–295. [Google Scholar] [CrossRef]
- Berglundh, T.; Armitage, G.; Araujo, M.G.; Avila-Ortiz, G.; Blanco, J.; Camargo, P.M.; Chen, S.; Cochran, D.; Derks, J.; Figuero, E.; et al. Peri-implant diseases and conditions: Consensus report of workgroup 4 of the 2017 World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions. J. Periodontol. 2018, 89, 313–318. [Google Scholar] [CrossRef]
- Del Amo, F.S.L.; Yu, S.-H.; Sammartino, G.; Sculean, A.; Zucchelli, G.; Rasperini, G.; Felice, P.; Pagni, G.; Iorio-Siciliano, V.; Grusovin, M.G.; et al. Peri-implant Soft Tissue Management: Cairo Opinion Consensus Conference. Int. J. Environ. Res. Public Heal. 2020, 17, 2281. [Google Scholar] [CrossRef] [Green Version]
- Temmerman, A.; Cleeren, G.J.; Castro, A.B.; Teughels, W.; Quirynen, M. L-PRF for increasing the width of keratinized mucosa around implants: A split-mouth, randomized, controlled pilot clinical trial. J. Periodontal Res. 2018, 53, 793–800. [Google Scholar] [CrossRef]
- Maiorana, C.; Pivetti, L.; Signorino, F.; Grossi, G.B.; Herford, A.S.; Beretta, M. The efficacy of a porcine collagen matrix in keratinized tissue augmentation: A 5-year follow-up study. Int. J. Implant. Dent. 2018, 4, 1–7. [Google Scholar] [CrossRef] [Green Version]
- Le, B.; Borzabadi-Farahani, A.; Nielsen, B. Treatment of Labial Soft Tissue Recession Around Dental Implants in the Esthetic Zone Using Guided Bone Regeneration With Mineralized Allograft: A Retrospective Clinical Case Series. J. Oral Maxillofac. Surg. 2016, 74, 1552–1561. [Google Scholar] [CrossRef] [Green Version]
- Bienz, S.P.; Jung, R.E.; Sapata, V.; Hämmerle, C.H.F.; Hüsler, J.; Thoma, D.S. Volumetric changes and peri-implant health at implant sites with or without soft tissue grafting in the esthetic zone, a retrospective case-control study with a 5-year follow-up. Clin. Oral Implant. Res. 2017, 56, 1459–1465. [Google Scholar] [CrossRef] [Green Version]
- Schwarz, F.; Herten, M.; Sager, M.; Bieling, K.; Sculean, A.; Becker, J. Comparison of naturally occurring and ligature-induced peri-implantitis bone defects in humans and dogs. Clin. Oral Implant. Res. 2007, 18, 161–170. [Google Scholar] [CrossRef]
- Schwarz, F.; Sahm, N.; Schwarz, K.; Becker, J. Impact of defect configuration on the clinical outcome following surgical regenerative therapy of peri-implantitis. J. Clin. Periodontol. 2010, 37, 449–455. [Google Scholar] [CrossRef]
- Ravidà, A.; Saleh, I.; Siqueira, R.; Garaicoa-Pazmiño, C.; Saleh, M.H.A.; Monje, A.; Wang, H. Influence of keratinized mucosa on the surgical therapeutical outcomes of peri-implantitis. J. Clin. Periodontol. 2020, 47, 529–539. [Google Scholar] [CrossRef]
- Schmitt, C.M.; Moest, T.; Lutz, R.; Wehrhan, F.; Neukam, F.W.; Schlegel, K.A. Long-term outcomes after vestibuloplasty with a porcine collagen matrix (Mucograft®) versus the free gingival graft: A comparative prospective clinical trial. Clin. Oral Implant. Res. 2016, 27, 125–133. [Google Scholar] [CrossRef]
- Brügger, O.E.; Bornstein, M.M.; Kuchler, U.; Janner, S.F.M.; Chappuis, V.; Buser, D. Implant Therapy in a Surgical Specialty Clinic: An Analysis of Patients, Indications, Surgical Procedures, Risk Factors, and Early Failures. Int. J. Oral Maxillofac. Implant. 2015, 30, 151–160. [Google Scholar] [CrossRef] [PubMed]
- Thoma, D.S.; Buranawat, B.; Hämmerle, C.H.F.; Held, U.; Jung, R.E. Efficacy of soft tissue augmentation around dental implants and in partially edentulous areas: A systematic review. J. Clin. Periodontol. 2014, 41, 77–91. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- De Resende, D.R.B.; Greghi, S.L.A.; Siqueira, A.F.; Benfatti, C.A.M.; Damante, C.; Zangrando, M.S.R. Acellular dermal matrix allograft versus free gingival graft: A histological evaluation and split-mouth randomized clinical trial. Clin. Oral Investig. 2019, 23, 539–550. [Google Scholar] [CrossRef] [PubMed]
- Wei, P.-C.; Laurell, L.; Geivelis, M.; Lingen, M.W.; Maddalozzo, D. Acellular Dermal Matrix Allografts to Achieve Increased Attached Gingiva. Part 1. A Clinical Study. J. Periodontol. 2000, 71, 1297–1305. [Google Scholar] [CrossRef] [PubMed]
- Burkhardt, R.; Hämmerle, C.H.; Lang, N.P.; the Research Group on Oral Soft Tissue Biology & Wound Healing. Self-reported pain perception of patients after mucosal graft harvesting in the palatal area. J. Clin. Periodontol. 2015, 42, 281–287. [Google Scholar] [CrossRef] [PubMed]
| Characteristics | CM | APF | FGG |
|---|---|---|---|
| N | 7 | 8 | 5 |
| Age (years) (Mean (SD) | 60.43 (4.61) | 63.88 (4.03) | 58.00 (3.83) |
| Sex | |||
| Male | 4 | 4 | 3 |
| Female | 3 | 4 | 2 |
| Jaw position | |||
| Upper | 1 | 6 | 2 |
| Lower | 6 | 2 | 3 |
| Oral regions | |||
| Anterior teeth | 1 | 1 | |
| Premolars | 1 | ||
| Molars | 6 | 6 | 5 |
| Classification of peri-implantitis | |||
| Class Ib | 1 | 2 | |
| Class Id | 1 | 1 | |
| Class Ib + II | 1 | ||
| Class Ic + II | 2 | 2 | 1 |
| Class Id + II | 3 | 2 | 2 |
| Class Ie + II | 2 | ||
| Systemic disease | |||
| Osteoporosis | 2 | 0 | 1 |
| Heart disease | 2 | 1 | 0 |
| Hypertension | 2 | 3 | 0 |
| None | 1 | 4 | 4 |
| Medicine | |||
| Osteoporosis | 2 | 2 | 1 |
| Anticoagulant | 2 | 0 | 0 |
| Hypertension | 2 | 1 | 0 |
| None | 1 | 5 | 4 |
| Smoking | |||
| Now | 0 | 2 | 0 |
| Past | 1 | 1 | 1 |
| Not | 6 | 5 | 4 |
| CM | APF | FGG | CM | APF | FGG | CM | APF | FGG | |||
|---|---|---|---|---|---|---|---|---|---|---|---|
| KM | PPD | BOP | |||||||||
| Horizontal width | 6 sites | 6 sites | |||||||||
| T0 | 1.14 (1.95) | 3.00 (2.07) | 2.00 (2.35) | T0 | 4.57 (0.86) | 4.71 (0.81) | 5.07 (0.35) | 3.29 (2.56) | 3.38 (2.13) | 2.00 (1.23) | |
| T1 | 4.71 (0.95) ‖ | 3.86 (0.90) | 5.00 (1.00) | T1 | 3.64 (0.58) | 3.64 (0.78) ‖ | 3.50 (0.59) ‖ | 1.43 (1.13) | 0.57 (0.79) ‖ | 0.40 (0.55) ‖ | |
| T2 | 4.71 (0.49) ‖ | 3.86 (1.22) | 5.67 (0.58) | T2 | 4.07 (0.71) | 3.79 (0.67) ‖ | 3.78 (0.95) ‖ | 1.14 (1.46) | 0.57 (1.13) ‖ | N/A ‖ | |
| T3 | 4.71 (0.76) †,‖ | 3.80 (1.10) *,‡ | N/A †,‖,§ | T3 | 4.10 (0.72) ¶ | 3.80 (0.77) | 3.50 (0.67) ‖ | 1.57 (1.51) | 1.40 (0.90) ‖ | 1.00 (1.00) | |
| T4 | 4.71 (0.76) †,‖ | 3.50 (1.23) *,‡ | 5.50 (0.71) †,§ | T4 | 4.17 (0.75) ¶ | 4.06 (0.82) | 3.58 (1.06) ‖ | 2.43 (1.99) | 1.50 (1.05) ‖ | 1.50 (0.71) | |
| Vertical width | Buccal 3 sites | Buccal 3 sites | |||||||||
| T0 | 0.43 (0.79) | 0.88 (0.64) | 0.80 (0.84) | T0 | 4.76 (1.05) | 4.46 (0.87) | 5.13 (0.30) | 1.29 (1.60) | 1.85 (0.99) | 1.80 (1.30) | |
| T1 | 3.71 (1.60) ‖ | 2.71 (0.95) ‡,‖ | 4.40 (0.55) § | T1 | 3.81 (0.74) | 3.57 (0.79) | 3.40 (0.83) ‖ | 0.71 (0.76) | 0.29 (0.49) ‖ | 0.2 (0.45) ‖ | |
| T2 | 4.14 (1.35) †,‖ | 2.57 (1.13) *,‡,‖ | 5.00 (1.00) †,‖,§ | T2 | 4.24 (0.88) | 3.76 (0.66) | 3.90 (1.02) | 0.71 (0.95) | 0.43 (0.79) ‖ | N/A ‖ | |
| T3 | 3.86 (1.22) †,‖ | 3.00 (0.71) *,‡,‖ | N/A ‖,§ | T3 | 4.24 (0.88) | 3.73 (0.68) | 3.67 (0.88) ‖ | 1.00 (0.82) | 0.80 (0.45) ‖ | 0.67 (0.58) | |
| T4 | 3.86 (1.22) †,‖ | 2.50 (0.55) *,‡,‖ | 4.50 (0.71) †,‖,§ | T4 | 4.29 (0.89) | 4.11 (0.81) | 3.67 (0.94) ‖ | 1.29 (1.11) | 1.00 (0.63) ‖ | 0.50 (0.71) ‖ |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lee, I.-K.; Choi, H.-S.; Jeong, S.-H.; Lee, J.-T. The Effect of Three Surgical Therapies to Increase Keratinized Mucosa Surrounding Dental Implants with Peri-Implantitis: A Pilot Study. Medicina 2021, 57, 1093. https://doi.org/10.3390/medicina57101093
Lee I-K, Choi H-S, Jeong S-H, Lee J-T. The Effect of Three Surgical Therapies to Increase Keratinized Mucosa Surrounding Dental Implants with Peri-Implantitis: A Pilot Study. Medicina. 2021; 57(10):1093. https://doi.org/10.3390/medicina57101093
Chicago/Turabian StyleLee, In-Kyung, Hyun-Seok Choi, Sang-Heon Jeong, and Jung-Tae Lee. 2021. "The Effect of Three Surgical Therapies to Increase Keratinized Mucosa Surrounding Dental Implants with Peri-Implantitis: A Pilot Study" Medicina 57, no. 10: 1093. https://doi.org/10.3390/medicina57101093
APA StyleLee, I.-K., Choi, H.-S., Jeong, S.-H., & Lee, J.-T. (2021). The Effect of Three Surgical Therapies to Increase Keratinized Mucosa Surrounding Dental Implants with Peri-Implantitis: A Pilot Study. Medicina, 57(10), 1093. https://doi.org/10.3390/medicina57101093






