Abstract
Background and Objectives: An increase in the incidence of end-stage renal disease (ESRD) is associated with the need for a wider use of vascular access. Although arteriovenous (A-V) fistula is a preferred form of vascular access, for various reasons, permanent catheters are implanted in many patients. Materials and Methods: A retrospective analysis of clinical data was carried out in 398 patients (204 women) who in 2010–2016 were subjected to permanent dialysis catheters implantation as first vascular access or following A-V fistula dysfunction. The factors influencing the risk of complications related to vascular access and mortality were evaluated and the comparison of the group of patients with permanent catheter implantation after A-V fistula dysfunction with patients with first-time catheter implantation was carried out. Results: The population of 398 people with ESRD with mean age of 68.73 ± 13.26 years had a total of 495 permanent catheters implanted. In 129 (32.6%) patients, catheters were implanted after dysfunction of a previously formed dialysis fistula. An upward trend was recorded in the number of permanent catheters implanted in relation to A-V fistulas. Ninety-two infectious complications (23.1%) occurred in the study population in 65 patients (16.3%). Multivariate analysis showed that permanent catheters were more often used as the first vascular access option in elderly patients and cancer patients. Mortality in the mean 1.38 ± 1.17 years (min 0.0, max 6.70 years) follow-up period amounted to 50%. Older age and atherosclerosis were the main risk factors for mortality. Patients with dialysis fistula formed before the catheter implantation had a longer lifetime compared to the group in which the catheter was the first access. Conclusion: The use of permanent catheters for dialysis therapy is associated with a relatively high incidence of complications and low long-term survival. The main factors determining long-term survival were age and atherosclerosis. Better prognosis was demonstrated in patients after the use of A-V fistula as the first vascular access option.
1. Introduction
End-stage renal disease (ESRD) is an important medical and social problem, leading to an increase in the number of patients requiring dialysis and kidney transplantation. The concept of a global epidemic of chronic kidney disease (CKD) has appeared, and its incidence is increased mainly in developing countries [1]. About 75% of patients with ESRD require renal replacement therapy and access to dialysis [2,3]. In Poland, approximately 4.5 million people suffer from chronic kidney disease and 21,043 patients receive renal replacement therapy [4]. According to the Kidney Disease Outcomes Quality Initiative (KDOQI), the recommended form of vascular access is arteriovenous fistula (A-V) from the patient’s own vessels and 80%–90% of patients should be dialyzed using it [2,4,5,6,7,8]. Aging of the population and high morbidity in the CKD patients often makes the creation of the A-V fistula impossible and the permanent catheter becomes the only salvage for these patients [3,4]. Dialysis catheters are an alternative to the continuation of renal replacement therapy in patients with existing vascular access failure, when the surgical possibilities for the formation of an A-V fistula have been exhausted. They are also used as bridging therapy for those who are waiting for a live donor transplant and for the maturation of the dialysis fistula formed. Dialysis catheters are also used in people with severe heart failure and respiratory failure, in whom fistula formation would be associated with exacerbation of the underlying disease [9,10,11,12,13,14]. Although the dialysis fistula is the gold standard, in various clinical situations, a catheter inserted into the venous system is selected for dialysis [7,15]. The advantage of catheters is related to obtaining a fast access and the possibility of immediate dialysis and the limitation of high risk of infectious, thrombotic complications, dysfunctions leading to impairment of dialysis, associated with central vascular stenosis. These complications are likely to affect mortality in a catheter-dialyzed patient. Current reports more and more often show that the survival rate of dialyzed patients depends to a large extent on the type of vascular access used. The aim of the present study was to analyze trends in implantation of permanent catheters, compare populations with permanent catheters implanted as the first and subsequent access, and evaluate the risk of complications and mortality of patients dialyzed using permanent catheters during the observation period.
2. Materials and Methods
The study included 398 adults whom in the period from the 1 January 2010 to the 31 December 2016 had permanent dialysis catheters implanted for the first time. It was a retrospective study based on the data obtained from the regional branch of the National Health Fund and hospital medical documentation. The study group included patients who had a tunneled catheter inserted as means of first-time access and patients with a catheter implanted due to dysfunction of a previously developed dialysis fistula. The performed procedures of dialysis access and the diseases that led to the permanent catheter insertion were evaluated for the whole study group. The International Statistical Classification of Diseases and Related Health Problems (ICD10) unit codes were used for the analysis. The influence of the cause of implantation of the dialysis catheter on the time of its functioning was assessed. Based on this data, the frequency of vascular access implantation was assessed over the observation period. The catheter functioning time was compared in two groups: the first one was comprised of catheters inserted as a result of the initial renal reasons (these were diseases coded according to ICD 10 with codes: N03.9; N04.0; N10; N12.0; N13.2; N17.0; N17.8 N17.9; N27.0), the second consisted of those that were inserted as a result of initial nonrenal reasons (these are diseases according to ICD10: A41.0; A41.1; A41.5; E11.2; E11.5; I70.2; I70.9; I71.4; S68.8; T82.3). The analysis included clinical and procedural factors potentially affecting the risk of developing vascular access complications and mortality. The comparison of the group of patients with permanent catheter implantation after dysfunction of the dialysis fistula with patients with first-time catheter implantation was carried out. The procedural factors analysis included: reasons for permanent catheter insertion and removal; reasons for further hospitalizations once the catheter was implanted; impact of the disease that led to catheter insertion on its functioning time; the number of catheters implanted in one patient; time of functioning of the first catheter; functioning time of a catheter implemented after previously developed dialysis fistula. The catheter functioning time was calculated from the moment of its implantation until its removal, replacement, patient’s death or the end of the study. Survival time was calculated from the beginning of the study to its end or the patient’s death.
2.1. Statistical Methods
The distribution of continuous variables was assessed using the Shapiro–Wilk test. Values of continuous variables are presented as mean ± SD and number (%) for dichotomous variables.
Student’s t-test was used to compare continuous variables of parametric distribution. Variables with nonparametric distribution were compared with the Mann–Whitney "U" test, while the dichotomous variables-with the Chi2 test with the Yates correction. The Kruskal–Wallis ANOVA test was used to analyze the influence of the disease classification determining the need for renal replacement therapy for the duration of the catheter’s life.
To determine the risk factors for death during the follow-up period, the uni- and multifactorial Cox regression model was used. The analysis of factors influencing the selection of dialysis access options (catheter or fistula) was performed using uni- and multifactorial logistic regression. Multivariable analyses included variables whose differences in parametric and nonparametric tests reached p < 0.05.
Additionally, the Kaplan–Meier survival curves were plotted for groups of patients determined on the basis of the first-time dialysis access type. Differences in the course of the curves were assessed by the log rank test. Statistical significance was determined for p < 0.05.
2.2. Ethical Statement
The study was carried out in accordance with the Declaration of Helsinki and was approved by the Bioethics Commission of Regional Medical Board (Świętokrzyska Izba Lekarska, permit no. 21/2017; approved on 27 April 2017).
3. Results
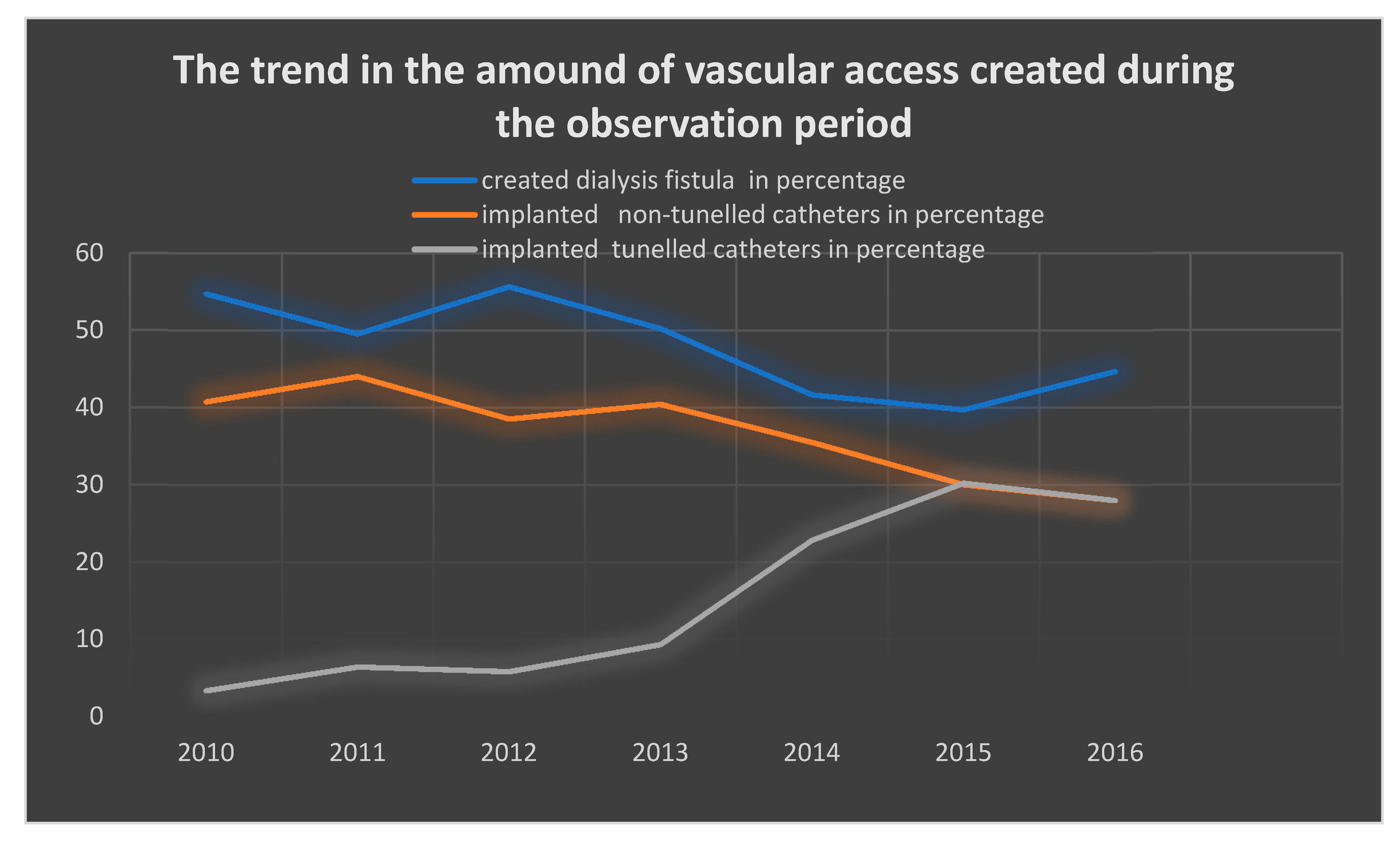
The study included 398 adults (204 women, 51.25%) of mean age 68.73 ± 13.26 years, who had a permanent catheter implanted for the first time. In total, 495 catheter implantations had been registered during the mean 1.38 ± 1.17 years (min 0.0 max 6.70 years) follow-up period. During that time, a significant increase in the frequency of permanent catheters implantation was observed. The percentage of implanted catheters in relation to developed dialysis fistulas increased from 3.35% in 2010 to 27.98% in 2016. Detailed analysis confirmed a linear upward trend in the number of implanted tunneled catheters, as seen in Figure 1.
Figure 1.
Percentage of tunneled, nontunneled catheters, and dialysis fistulas during the observation period.
In the studied population, in 129 patients (32.16%), permanent catheters were implanted after A-V fistula dysfunction. In 322 (80.9%) patients, only a single catheter was implanted during the observation period, and 58 (14.57%) patients required at least one catheter replacement. The need to replace the catheter was more frequent in women (p < 0.05), as seen in Table 1.

Table 1.
Clinical characteristics of the studied population.
The etiology of renal failure did not affect the functioning time (age) of the first catheter, the functioning time of all catheters in one patient and the mean functioning time of one catheter (according to Kruskal–Wallis ANOVA p = 0.181 for the first catheter age, p = 0.485 for the age of all catheters, and p = 0.267 for the mean age of the catheter).
The reason for catheter implantation (due to initial renal disease or other nonrenal reasons) had no effect on the duration of its functioning time (according to Kruskal–Wallis ANOVA p = 0.3015 for the age of the first catheter, p = 0.535 for the age of all catheters, p = 0.148 for the mean age of the catheter).
The most common diseases associated with renal failure in the study group were hypertension (27.4%), generalized atherosclerosis (27.1%), heart failure (19.6%), and cancer (19.6%). There were no differences in the incidence of comorbidities between men and women. Ninety-two infectious complications (23.1%) in 65 patients (16.3%) were reported (mean infection ratio was 0.46 per 1000 catheter days) in the study population with the lower frequency of infection in the female population (p < 0.05), as seen in Table 1.
Patients with initially formed A-V fistula were younger, with less frequent diabetes mellitus and generalized atherosclerosis. The incidence of cardiovascular disease and number of infectious complications related to catheters was comparable to patients with a permanent catheter implanted as a first access. The total duration of functioning of all catheters was 182,613 days; the mean duration of one catheter functioning was 436 ± 398. The duration of functioning of catheters implanted after dysfunction of the dialysis fistula was longer compared to those implanted as the first-time access (565 days ± 409 vs. 476 days ± 434; p = 0.01), although the number of thrombotic complications and the need to replace catheters was more frequent in this group of patients. In patients with a permanent catheter as the first vascular access, diabetes, generalized atherosclerosis, and neoplastic disease were more common. In this group a tendency to higher mortality was also more frequent, as seen in Table 2.

Table 2.
Comparative analysis of clinical and procedural parameters of patients with permanent catheters implanted after A-V fistula and implanted as the first access.
Univariate logistic regression showed that the choice of a permanent catheter as the first option for dialysis access is determined by older age of the patient, diseases of the cardiovascular system of atherosclerotic etiology, and neoplastic disease (borderline statistical significance). Multivariate analysis confirmed the predictive effect of the age of patients and neoplastic disease (borderline statistical significance), as seen in Table 3.

Table 3.
Univariate and multivariate logistic regression of the probability of the first-time permanent catheter implantation.
Analysis of the survival rate of the entire study population of dialysis patients using permanent catheters showed that during the mean 1.38 ± 1.17 years follow-up period, 199 (50%) people died: 103 (50.49%) women and 96 (49.48%) men. Patients who died were older, with frequent generalized atherosclerosis. Catheter replacement had no effect on mortality; however, the time from the first implantation and the mean time of catheter functioning was longer in patients who survived the observation period, as seen in Table 4.

Table 4.
Comparative analysis of clinical and procedural parameters of patients, including the division into patients alive and deceased during the observation period.
Cox univariate regression analysis demonstrated that death risk factors for dialysis patients using permanent catheters included older age and the presence of generalized atherosclerosis. In the two-factor assessment, only the influence of older age was confirmed, as seen in Table 5.

Table 5.
Risk factors of death. Cox uni- and multivariate logistic regression.
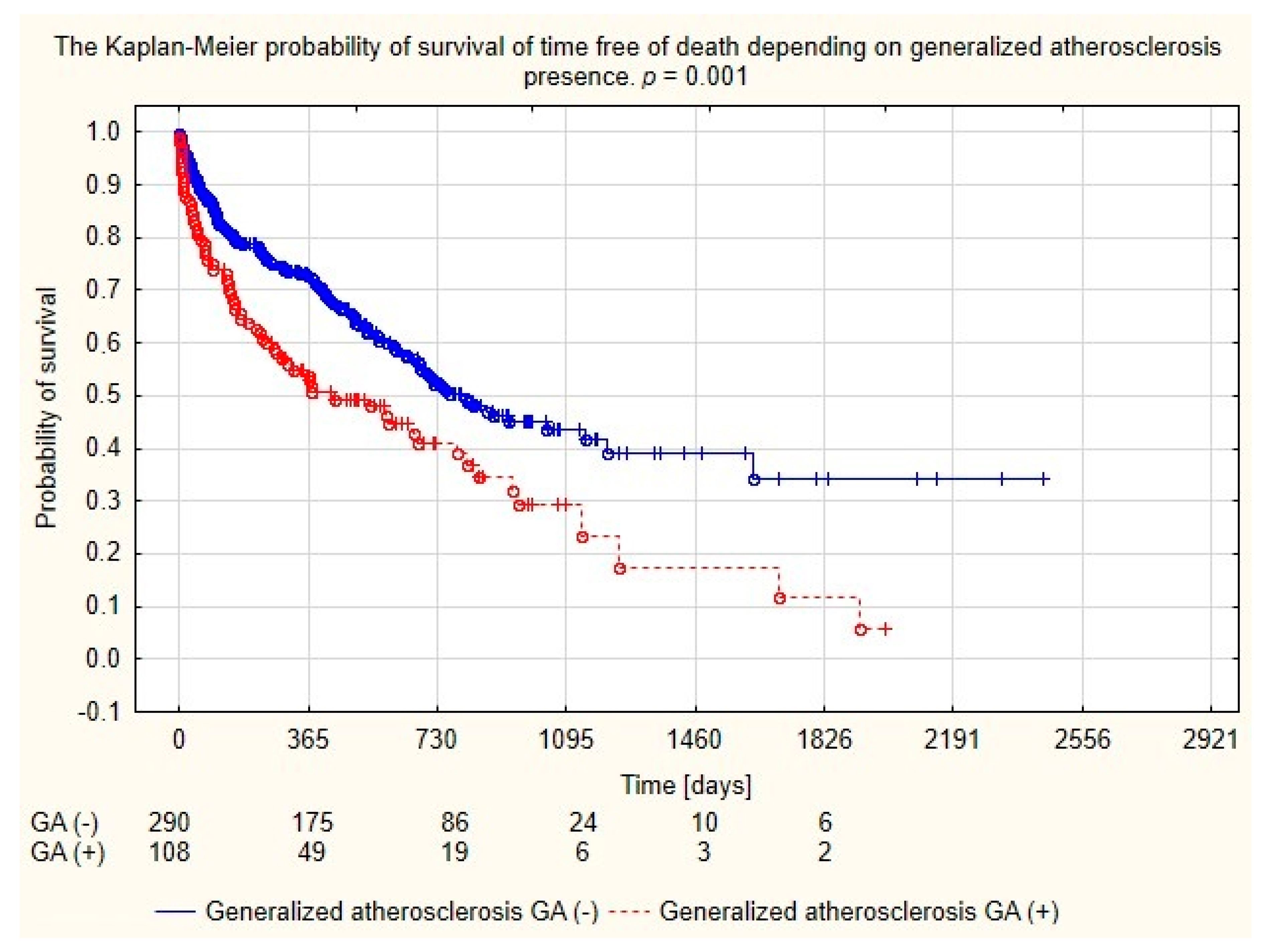
Analysis of the long-term survival of dialyzed patients demonstrated higher mortality of patients with generalized atherosclerosis, as seen in Figure 2.
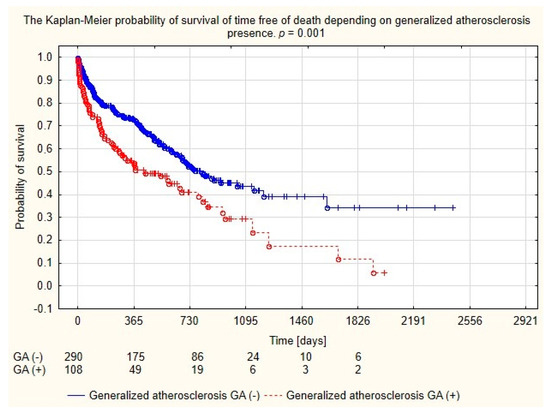
Figure 2.
Probability of survival depending on the generalized atherosclerosis in the population of patients dialyzed with permanent catheters.
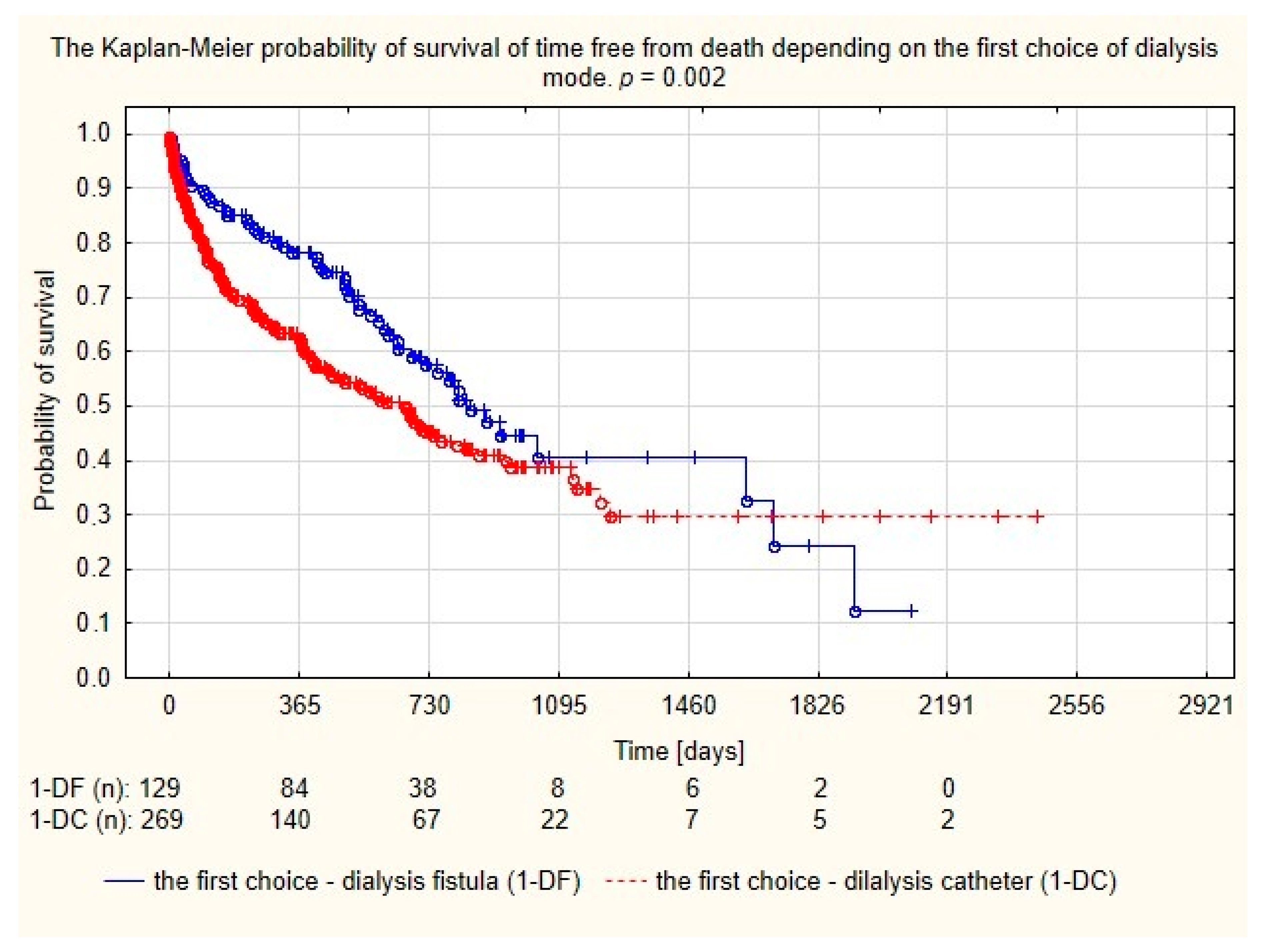
Assessment of survival probability using Kaplan–Meier curves showed that patients with dialysis fistula formed before the catheter implantation had a longer lifetime compared to the group in which the catheter was the first access, as seen in Figure 3.
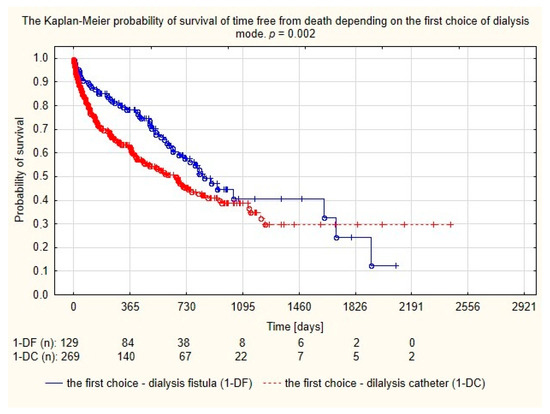
Figure 3.
Probability of survival depending on the first choice of dialysis mode.
4. Discussion
On the basis of the current analysis of clinical data of patients undergoing dialysis in 2010–2016, it was proved that despite the KDOQI’s recommendations for limiting the number of implanted catheters in relation to dialysis fistulas, their percentage is still increasing. The study showed that during the observation period, it increased from 3.35% in 2010 to 27.98% in 2016.
The current literature includes few reports on the percentage of permanent catheters in dialysis therapy in Poland and in the world, but all of them confirm the increasing tendencies in the use of this form of vascular access. In one of the studies from south-eastern Poland conducted in 2006–2010, the percentage of patients dialyzed with a long-term catheter increased from 14.35%–20.5% [16]. The upward trend continues, and according to the data from Fresenius Nefrocare Polska presented at the First Congress of Polish Vascular Access to Dialysis Club in 2017, the number of patients dialyzed in Poland increased from 2345 in 2010 to 6112 in 2017. The data also showed an increase in the share of permanent vascular catheters from 17.7% in 2010 to 30.3% in 2017. This does not differ from the data presented in global reports. According to Dialysis Outcomes and Practice Patterns Study (DOPPS) in 2009–2011 in Europe, the percentage of catheters ranged from 12%% to 32%, and in Canada it reached 49% [17]. This tendency is probably associated with an increase in life expectancy and a high rate of morbidity in the group of dialysis patients. They are much more often burdened with cardiological, pulmonary, and oncological complications as well as diabetes, and the arteriovenous fistula often poses an additional risk of deteriorating health through burden of the circulatory system. Moreover, due to changes in the vessel wall in the elderly as a result of diabetes, atherosclerosis, and calcification, the creation of preferred access, i.e., A-V fistula, is often impossible, which is why permanent catheters were implanted more often in older patients with these comorbidities [18,19,20,21,22]. The catheter functioning time in the current study was similar to the period presented in the available publications. One of the papers compares the operating time of tunneled catheters installed first to those installed after the previous nontunneled catheters. The mean functioning duration of catheters in this material was 370 days, with a median of 287 days, and was comparable in both groups [16,23,24]. Another work showed a significant advantage on the functioning time of catheters implanted as first-time over the times of those implanted second [25]. The functioning duration of the catheter also depended on its location; e.g., in the right internal jugular vein, it was longer than in other locations. Nondiabetic patients had longer catheter operation times in relation to diabetic patients, and the time of catheter functioning was affected by the type of material used for their construction. The age and sex of the patient as well as the operator’s skills did not influence the catheter operation times [16,25,26]. In the present study, sex, location of the catheter, and the reasons for the catheter installation had no effect on its functioning time. This time was longer in the group of patients in whom the catheter was installed after the previous fistula as the next access in comparison with the catheter installed as the first access (565.248 vs. 476.342 days; p < 0.001). Patients in the group with an earlier fistula were younger and atherosclerosis, diabetes and neoplastic diseases were less common, which in comparison to the second group could have influenced the longer maintenance of the functioning of the catheter. All these factors contributed to the improved survival of patients in whom A-V fistula was used as the first vascular access.
The presented study identified 92 (23.1%) catheter-related infections of an average infection rate of 0.46 per 1000 catheter days. In the case of tunnelled catheters, according to various sources, frequency of infection ranges from 1.6 to 5.5 occurrences per 1000 catheter days [22,27]. Another observation of a large number of patients showed an infection rate of 0.514 per 1000 catheter days [28]. Another study indicated the impact of catheter location on the frequency of catheter-related infections and its dysfunction [29]. The present study showed that in the group of infected catheters, catheter location had no impact on operation time.
Some reports in the literature show a high risk of infection in patients dialyzed by catheter, compared to those using A-V fistulas. In one of them, infectious complications in dialysis patients using permanent catheters amounted to approximately 40% [30,31]. The present study demonstrated no difference in the number of infections between the patients dialyzed with catheters after dysfunction of the previously created fistula and those dialyzed first with a catheter. In the presented study, 50% of mortality was observed during the mean 1.38 ± 1.17 years follow-up period. These data are comparable to other reports. According to various sources, the survival rate in the dialysis group is 67% after two years of dialysis, 35% after five years, and 11% after 10 years [19]. Mortality in the dialysis patients depends to a large extent on the type of vascular access used. It has been proven that dialysis fistulas made of vascular prostheses and central catheters increase the risk of death [7,31,32,33,34,35]. One of the current publications showed two-fold higher mortality in patients dialized by catheter (22.7%) compared to the fistula group (12.2%), and increased hospitalization rates in the catheter group. Higher mortality was observed in the group of dialyzed older patients, over 65 years of age, and in patients with diabetes. Patients dialyzed with catheters had a 50% higher risk of death than those dialyzed with fistula [36]. The main causes of death in this study were cardiac complications, occurring in 9.4%, whereas infections occurred only in 2.9% of subjects. Another study of the 2666 patients dialyzed between 2009 and 2011 showed that 873 (32%) patients died during the follow-up period. Patients using tunneled catheters demonstrated, in relation to other forms of access, a higher risk of death from all causes of exposure to renal replacement therapy (HR = 1.83–2.08). Higher risk of death from cardiovascular causes (corrected HR: 2.20–2.95) and death from infection (corrected HR: 3.10–3.336) were also reported [14]. In general, cardiovascular disease caused by atherosclerotic lesions in the vessels was considered to be the main cause of death in patients undergoing dialysis in the course of ESRD [37,38]. In our study, atherosclerosis was the main risk factor of mortality, but the survival was mainly determined by the age of the patient.
5. Study Limitations
The current study was based on retrospective data of medical procedures, which limits the full clinical interpretation. It would be advisable to perform a prospective study with greater access to medical records in order to search for new risk factors of complications and mortality in this very burdened group of dialysis patients.
6. Conclusions
The use of permanent catheters for dialysis therapy is associated with low long-term survival rate, especially in patients in whom this catheter was used as the first vascular access option. Better prognosis of patients with A-V fistula at baseline has been documented by demonstrating a longer dialysis duration. The main factor determining long-term survival was age, and the significant impact of atherosclerosis on mortality was confirmed.
Author Contributions
A.S.-S. data collection, writing the article; W.J. statistical data analysis and interpretation; M.P. data collection; A.Ł. data collection; J.M. data collection, revision of the article; A.P. data collection, critical revision of the article and final approval. All authors discussed the results and contributed to the final manuscript. All authors have read and agreed to the published version of the manuscript.
Funding
The authors received no financial support for the research, authorship and publication of this article.
Acknowledgments
We thank Renata Kazanecka (Deputy Medical Director of National Health Fund, Swietorzyskie Region) for sharing the data required for the research.
Conflicts of Interest
The authors declare that there is no conflict of interest.
References
- Lugon, J.R. Doenca renal cronica no Brasil; um problema de saude publico. J. Bras. Nefrol. 2009, 31, 2–5. [Google Scholar]
- National Kidney Fundation. KDOQI Clinical Practice Guidelines and Clinical Practice Recommendations for 2006 Updates: Hemodialysis Adequacy, Peritoneal Dialysis Adequacy, Vascular Access. Am. J. Kidney Dis. 2006, 47, S11–S145. [Google Scholar]
- Horan, T.C.; Gaynes, R.P.; Martone, W.J.; Jarvis, W.R.; Emori, T.G. CDC definitions of nosocomial surgical site infections, 1992: A modification of CDC definitions of surgical would infections. Infect. Control. Hosp. Epidemiol. 1992, 13, 606–608. [Google Scholar] [CrossRef] [PubMed]
- Załuska, W.; Klinger, M.; Kusztal, M.; Lichodziejewska-Niemierko, M.; Miłkowski, A.; Stompór, T.; Sak, J.; Domański, L.; Drożdż, M.; Aksamit, D.; et al. Recommendations of the Working Group of the Polish Society of Nephrology for the criteria of quality treatment in dialysis patients with end-stage renal disease. Nefrol. Dial. Pol. 2015, 19, 6–11. [Google Scholar]
- Depner, T.A.; Daugirdas, J.T.; Goldstein, S.; Ing, T.S.; Kumar, V.; Meyer, K.B.; Norris, K.; Balk, E.; Uhlig, K.; Fares, G.; et al. Clinical Practice Guidelines and Clinical Practice Recommendations 2006 Updates Hemodialysis Adequacy, Peritoneal Dialysis Adequacy, Vascular Access. Am. J. Kidney Dis. 2006, 48, S1–S322. [Google Scholar]
- Summary of Recommendation Statements Kidney International Supplements (2013, 3, 19-111). KDIGO 2012 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease. Available online: http://www.kidney-international.org (accessed on 28 December 2012).
- Woo, K.; Lok, C.E. New Insights into Dialysis Vascular Access: What Is the Optimal Vascular Access Type and Timing of Access Creation in CKD and Dialysis Patients? Clin. J. Am. Soc. Nephrol. 2016, 11, 1487–1494. [Google Scholar] [CrossRef]
- Vats, H.S. Complications of Catheters: Tunneled and Nontunneled. Adv. Chronic Kidney Dis. 2012, 19, 188–194. [Google Scholar] [CrossRef]
- Białobrzeska, B. Jak dbać o dostęp naczyniowy do hemodializy (cz.2). Forum Nefrologiczne 2009, 2, 266–274. [Google Scholar]
- Labriola, L.; Pochet, J.-M. Any use for alternative lock solutions in the prevention of catheter-related blood stream infections? J. Vasc. Access 2017, 18, S34–S38. [Google Scholar] [CrossRef]
- Libeas-Lopez, J. New technology: Heparyn and atimicrobial-coated catheters. J. Vasc. Access 2015, 16, S48–S53. [Google Scholar] [CrossRef]
- Lai, N.M.; Chaiyakunapruk, N.; Lay, N.A.; O’Riordan, E.; Pau, W.S.; Saint, S. Catheter impregnation, coating or bonding for reducing central venous catheter-related infections in adults. Cochrane Database Syst. Rev. 2013, 3, CD007878. [Google Scholar]
- Van Dijk, P.C.; Jager, K.J.; de Charro, F.; Collart, F.; Cornet, R.; Dekker, F.W.; Grönhagen-Riska, C.; Kramar, R.; Leivestad, T.; Simpson, K.; et al. Renal replacement therapy in Europe: The results of a collaborative effort by the ERA-EDTA registry and six national or regional registries. Nephrol. Dial. Transplant. 2001, 16, 1120–1129. [Google Scholar] [CrossRef] [PubMed]
- Roca-Tey, R. Permanent arteriovenosus fistula or catheter dialysis for heart failure patients. J. Vasc. Access. 2016, 17, S23–S29. [Google Scholar] [CrossRef]
- Jain, D.; Haddad, D.B.; Goel, N. Choice of dialysis modality prior to kidney transplantation: Does it matter? World J. Nephrol. 2019, 8, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Leś, J.; Wańkowicz, Z. Cewniki długoterminowe do hemodializoterapii doświadczenia własne. Nefrol. Dial. Pol. 2013, 17, 19–23. [Google Scholar]
- Robinson, B.M.; Bieber, B.; Pisoni, R.L.; Port, F.K. Dialysis Outcames and Practice Patterns Study (DOOPS): Its Strengths, Limitations and Role in Informing Practices and Policies. Clin. J. Am. Soc. Nephrol. 2012, 7, 1897–1905. [Google Scholar] [CrossRef]
- Pawlaczyk, K. Prophylaxis and treatment of cardiovascular complications in patients with chronic renal failure. Przew Lek. 2009, 5, 47–50. [Google Scholar]
- Muntner, P.; He, J.; Astor, B.C.; Folsom, A.R.; Coresh, J. Traditional and nontraditional risk factors predict coronary heart disease in chronic kidney disease: Results from the atherosclerosis risk in communities study. J. Am. Soc. Nephrol. 2005, 16, 529–538. [Google Scholar] [CrossRef]
- Shlipak, M.G.; Fried, L.F.; Cushman, M.; Manolio, T.A.; Peterson, D.; Stehman-Breen, C.; Bleyer, A.; Newman, A.; Siscovick, D.; Psaty, B. Cardiovascular mortality risk in chronic kidney disease: Comparison of traditional and novel risk factors. JAMA 2005, 293, 1737–1745. [Google Scholar] [CrossRef]
- Asif, A.; Bakr, M.M.; Levitt, M.; Vachharajani, T. Best Vascular Access in the Elderly: Time for Innovation? Blood Purif 2019, 47, 236–239. [Google Scholar] [CrossRef]
- Lee, T.; Mokrzycki, M.; Moist, L.; Maya, I.; Vazquez, M.; Lok, C.E.; North American Vascular Access Consortium. Standardized Definitions for Hemodialysis Vascular Access. Semin. Dial. 2011, 21, 515–524. [Google Scholar] [CrossRef] [PubMed]
- Weber, E.; Wołyniec, W.; Liberko, T.; Rutkowski, B. Cewniki tunelizowane w dializoterapii dobrodziejstwo czy zło konieczne? Forum Nefrologiczne 2015, 8, 205–213. [Google Scholar]
- Gellert, R.; Żelek, T.; Czystowski, M.; Daniewska, D. S-shaped-tunneled femoral catheter for permanent hemodialysis access. Postępy Nauk Medycznych 2010, 23, 604–607. [Google Scholar]
- Fry, A.C.; Stratton, J.; Farrington, K.; Mahna, K.; Selvakumar, S.; Thompson, H.; Warwicker, P. Factors affecting long-term survival of tunnelled haemodialysis catheters a prospective audit of 812 tunnelled catheters. Nephrol. Dial. Transplant. 2008, 23, 275–281. [Google Scholar] [CrossRef]
- Wejmer, M.C.; Vervloet, M.G.; ter Wee, P.M. Compared to tunnelled cuffed haemodialysis catheters, temporary untunnelled catheters are associated with more complications already within 2 weeks of use. Nephrol. Dial. Transplant. 2004, 19, 670–677. [Google Scholar] [CrossRef]
- Beathard, G.; Urbanes, A. Infection Associated with Tunneled Hemodialysis Catheters. Semin. Dial. 2008, 21, 528–538. [Google Scholar] [CrossRef]
- Lemaire, X.; Morena, M.; Leray-Moragués, H.; Henriet-Viprey, D.; Chenine, L.; Defez-Fougeron, C.; Canaud, B. Analysis of risk factors for catheter-related bacteremia in 2000 permanent dual catheters for hemodialysis. Blood Purif. 2009, 28, 21–28. [Google Scholar] [CrossRef]
- Engstrom, B.I.; Horvath, J.J.; Stewart, J.K.; Sydnor, R.H.; Miller, M.J.; Smith, T.P.; Kim, C.Y. Tunneled internal jugular hemodialysis catheters: Impact of laterality and tip position on catheter dysfunction and infection rates. J. Vasc. Interv. Radiol. 2013, 24, 1295–1302. [Google Scholar] [CrossRef]
- El Minschawy, O.; Abd El Aziz, T.; Abd El Ghani, H. Evaluation of vascular access complications in acute and chronic hemodialysis. J. Vasc. Access 2004, 5, 76–82. [Google Scholar] [CrossRef]
- Nelveg-Kristensen, K.E.; Laier, G.H.; Heaf, J.G. Risk of death after first-time blood stream infection in incident dialysis patients with specific consideration on vascular access and comorbidity. BMC Infect. Dis. 2018, 18, 688. [Google Scholar] [CrossRef]
- Brala, M.; Kamiński, R.; Trudnowski, S.; Grzybiak, M.; Kozłowski, D.; Raczak, G. Long-term complications after implantation of catheters for hemodialysis. Geriatrics 2014, 8, 1–5. [Google Scholar]
- Polkinghorne, K.R.; McDonald, S.P.; Atkins, R.C.; Kerr, P.G. Vascular access and all-cause mortality: A propensity score analysis. J. Am. Soc. Nephrol. 2004, 15, 477–486. [Google Scholar] [CrossRef] [PubMed]
- Weyde, W.; Krajewska, M.; Klinger, M. Dostęp naczyniowy do hemodializy. Forum Nefrologiczne 2008, 3, 119–126. [Google Scholar]
- Quarello, F.; Forneris, G.; Borca, M.; Pozzato, M. Do central venous catheters have advantages over arteriovenous fistulas or grafts? J. Nephrol. 2006, 19, 265. [Google Scholar] [PubMed]
- Hamadneh, S.A.; Nueirat, S.A.; Qadoomi, J.; Shurrab, M.; Qunibi, W.Y.; Hamdan, Z. Vascular access aortality and hospitalisation among hemodialysis patients in Palestine. Saudi J. Kidney Dis. Transpl. 2018, 29, 120–126. [Google Scholar] [PubMed]
- Stenvinkel, P.; Carrero, J.J.; Axelsson, J.; Linholm, B.; Heimburger, O.; Massy, Z. Emerging biomarkers for evaluating cardiovascular risk in the chronic kidney disease patient: How do new pieces fit into the uremic puzzle? Clin. J. Am. Soc. Nephrol. 2008, 3, 505–521. [Google Scholar] [CrossRef]
- Wanner, C.; Zimmermann, J.; Schwedler, R.S.; Metzger, T. Inflammation and cardiovascular risk in dialysis patients. Kidney Int. Suppl. 2002, 80, 99–102. [Google Scholar] [CrossRef]
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).