Pancreatic Polypeptide-Secreting Tumour of the Proximal Pancreas (PPoma)—Ultra Rare Pancreatic Tumour: Clinically Malign, Histologically Benign
Abstract
1. Introduction
2. Materials and Methods
3. Results
3.1. Macroscopic Findings
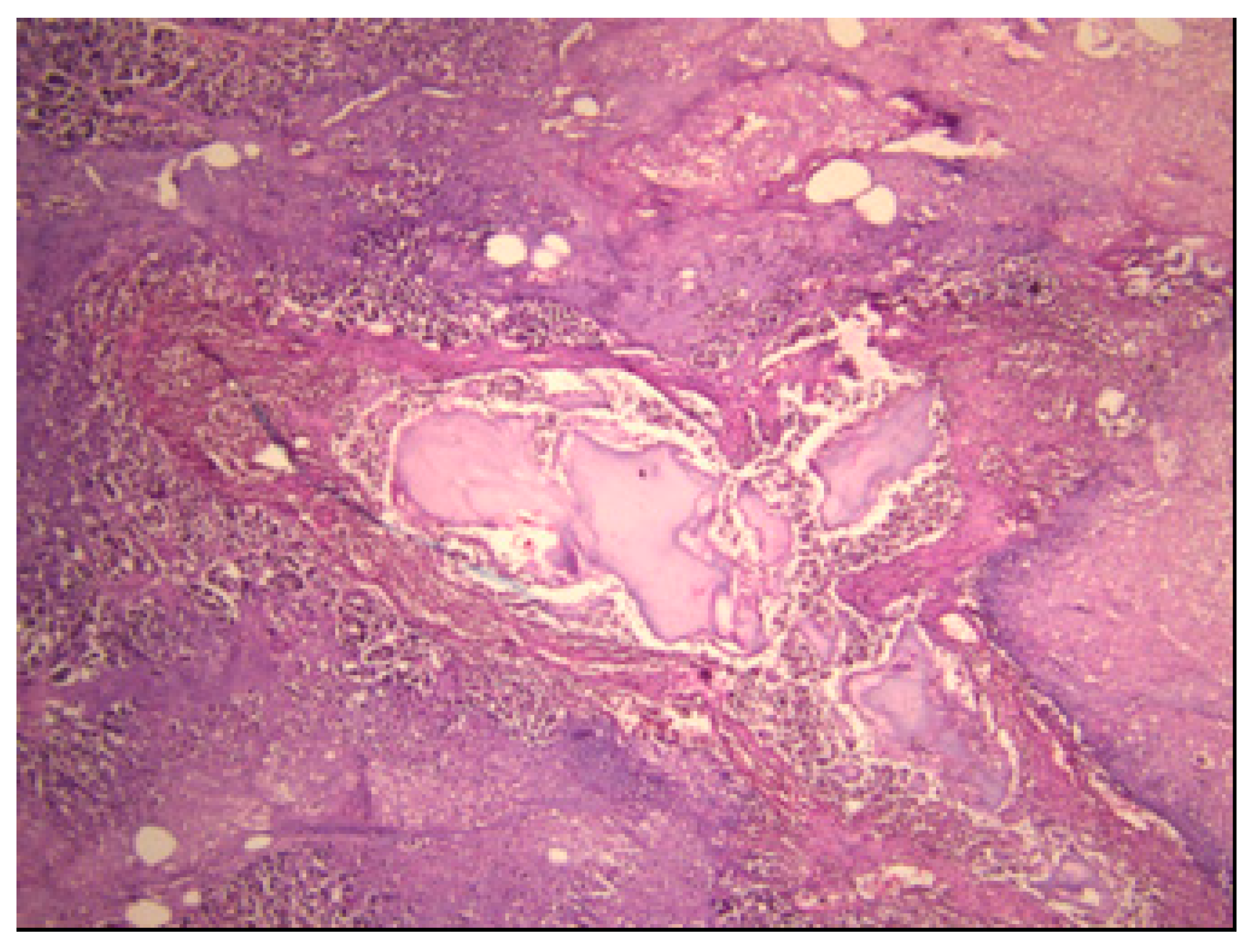
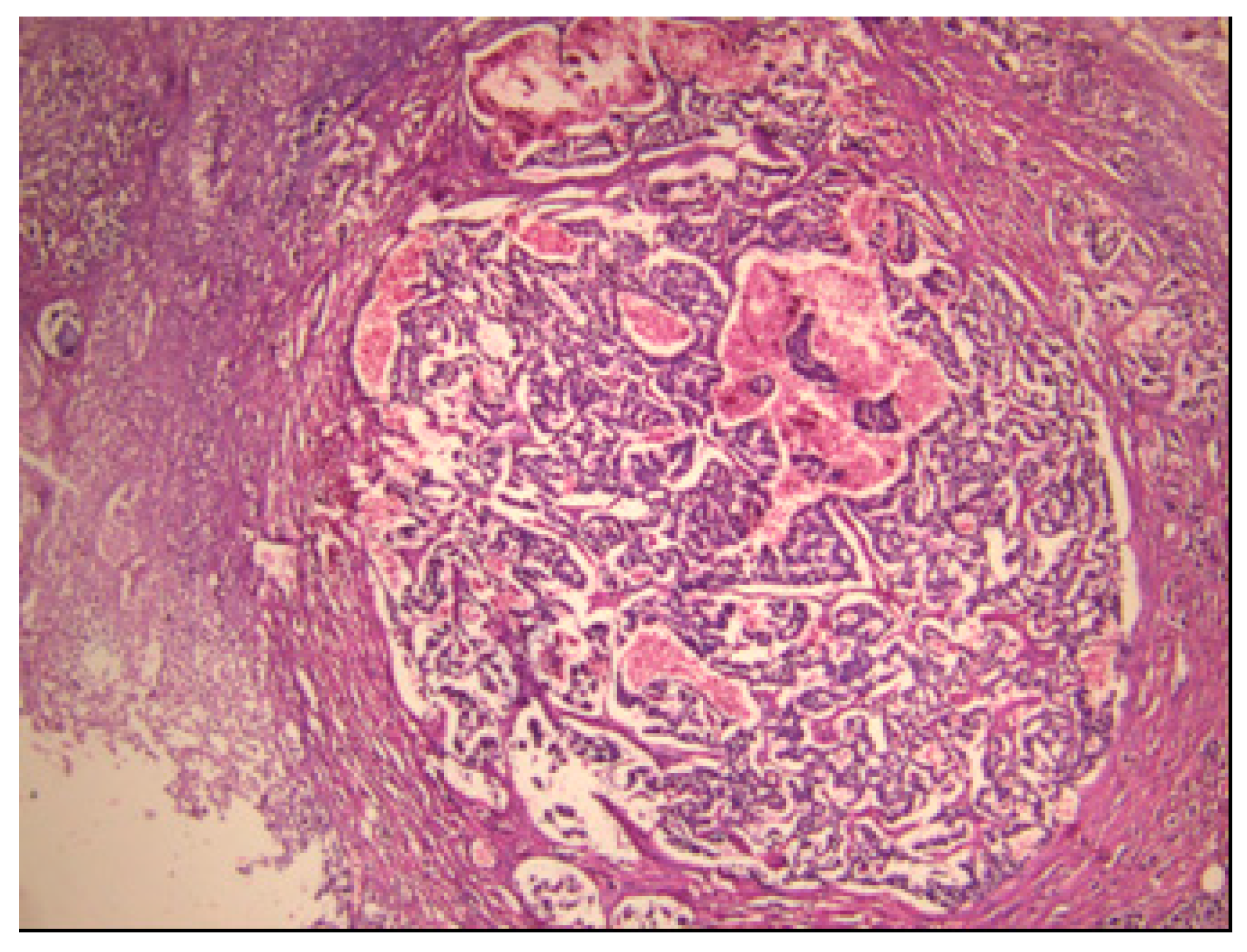
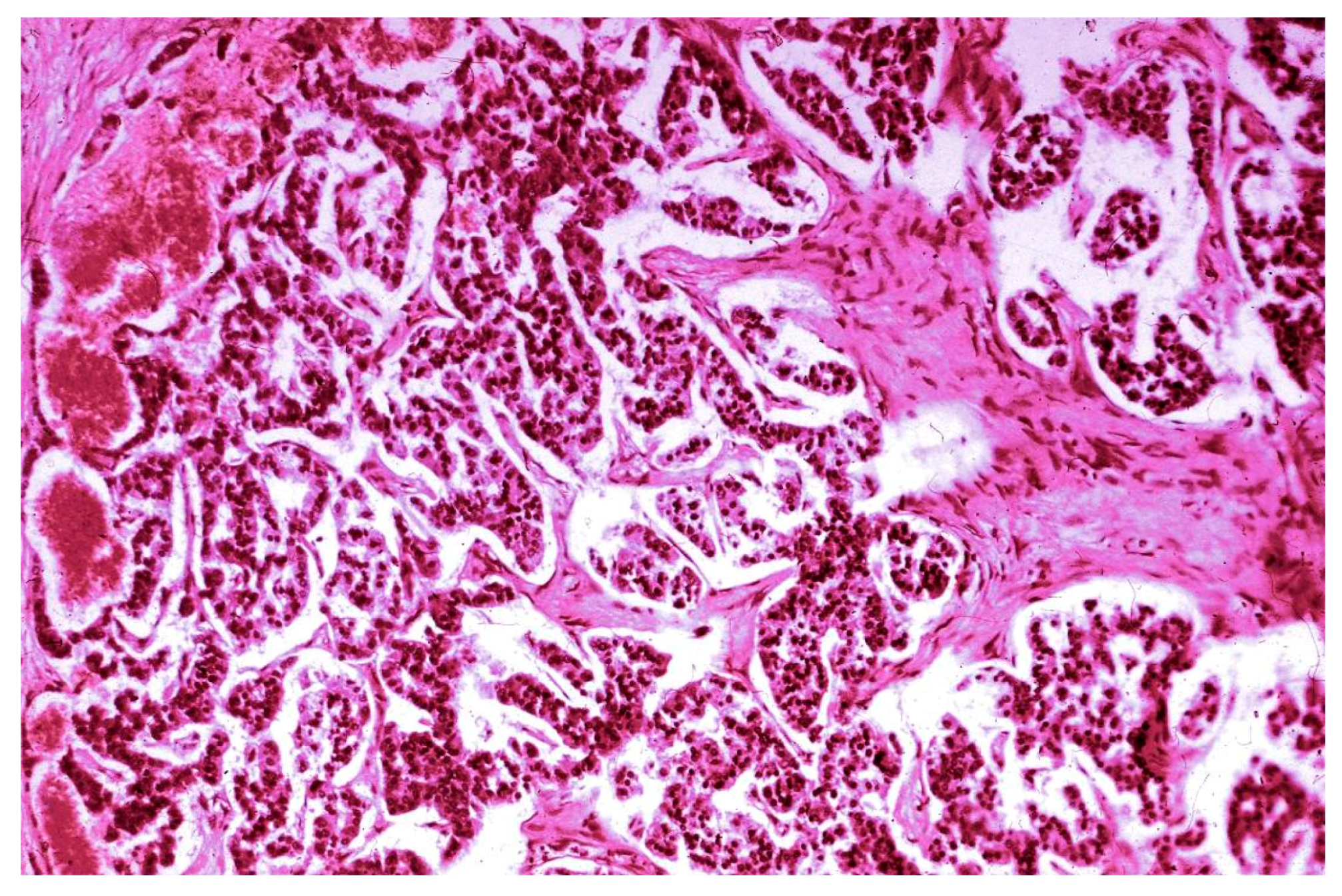
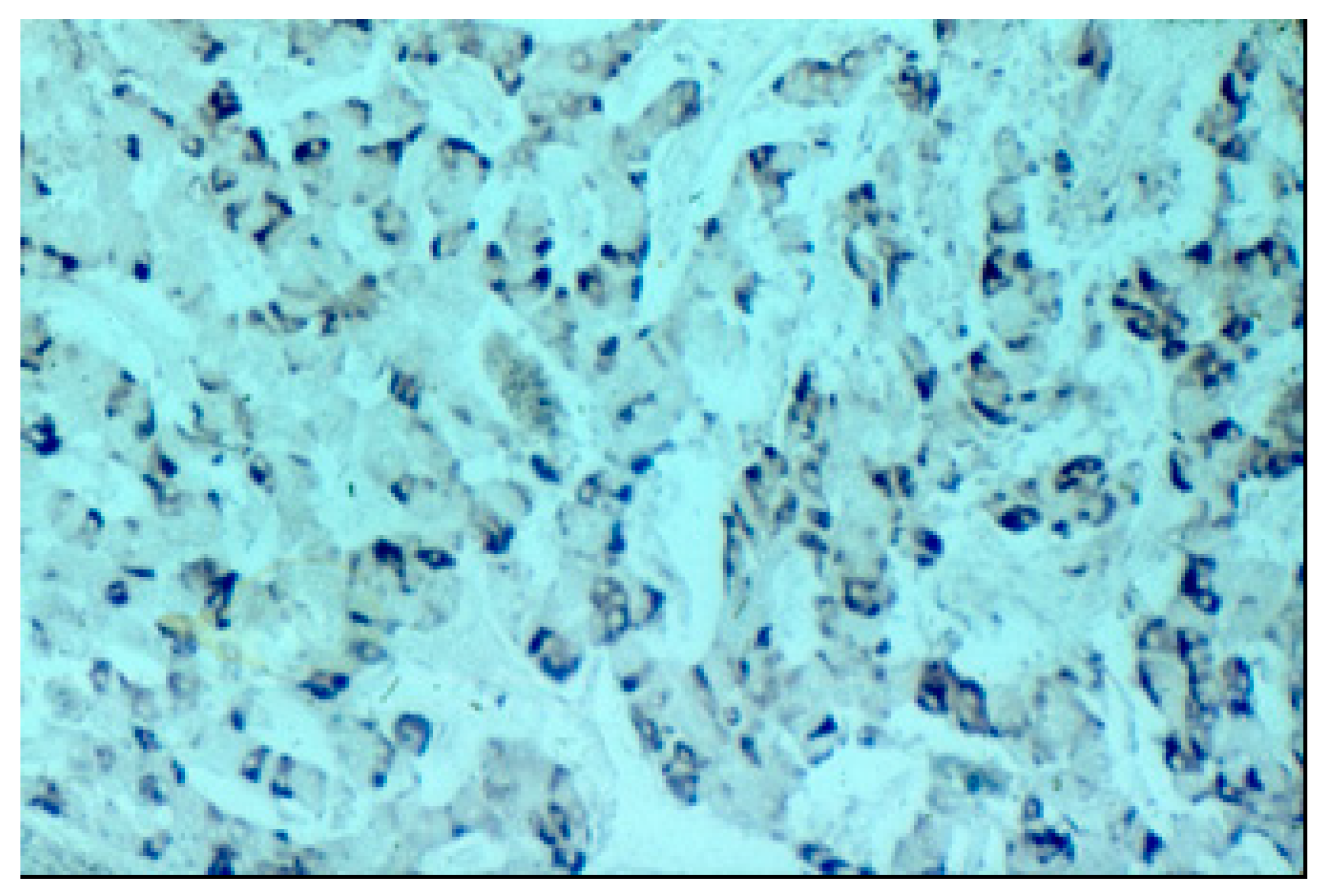
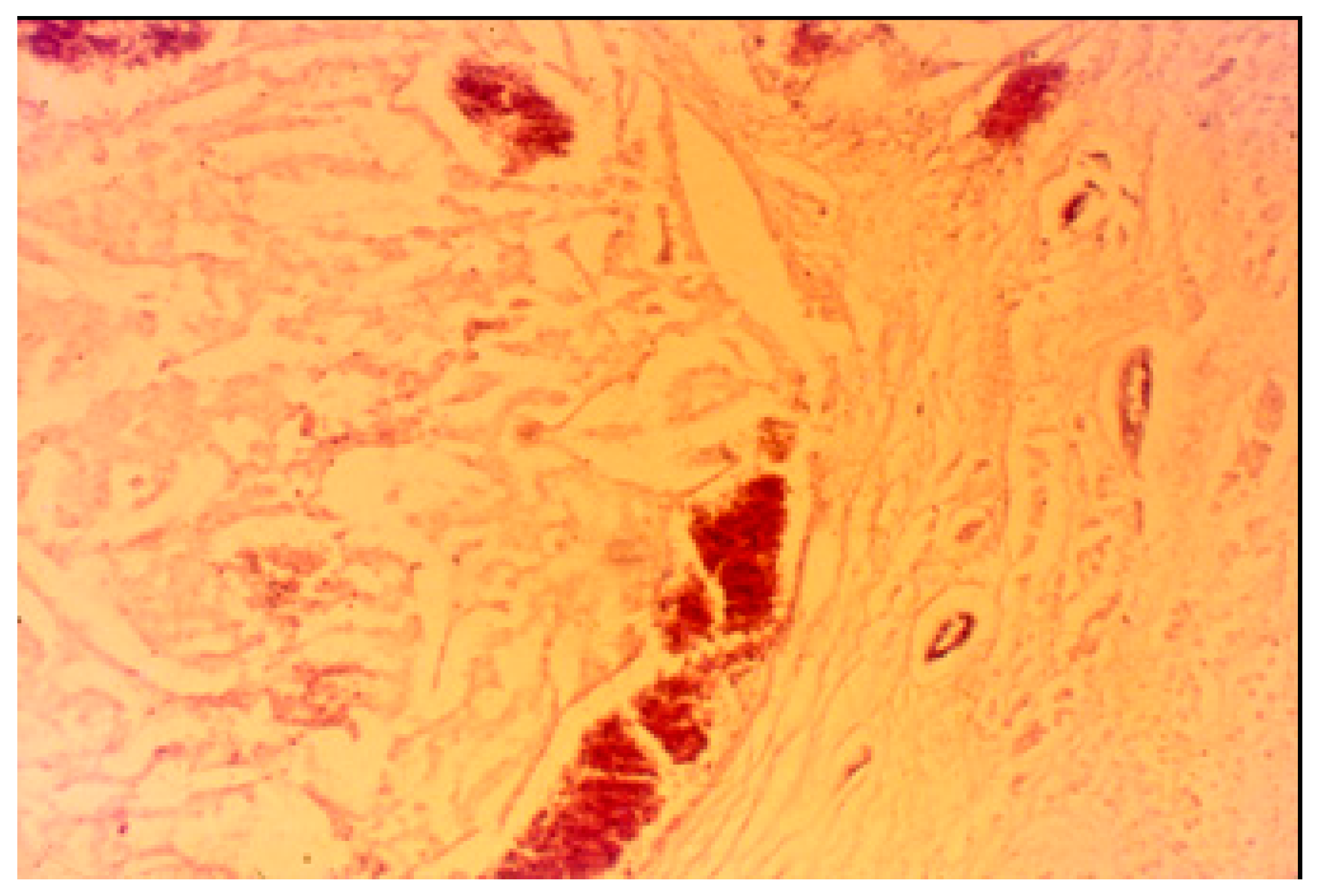
3.2. Histopathological Findings
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Pearse, A.G.; Polak, J.M. Neural crest origin of the endocrine polypeptide (APUD) cells of the gastrointestinal tract and pancreas. Gut 1971, 12, 783–788. [Google Scholar] [CrossRef] [PubMed]
- Bloom, S.R.; Polak, J.M. The New Peptide hormones of the gut. In Progress in Gastroenterology; Glass, G.B.J., Ed.; Grune and Stratton: New York, NY, USA; London, UK, 1977; Volume III. [Google Scholar]
- Katić, V.; Dojčinov, D.; Ilić, R. New Pancreatic Tumor-PPoma. Pathol. Res. Pract. 1979, 165, 108–109. [Google Scholar]
- Williams, J.A. Pancreatic Polypeptide; Michigan Publishing: Ann Arbor, MI, USA, 2014; Version 1.0. [Google Scholar]
- Katić, V. Pathology of the Stomach, Monogfraphy; Medical Book: Belgrade-Zagreb, Serbia, 1989; pp. 1–231. [Google Scholar]
- Solcia, E.; Capella, C.; Kloppel, G. Tumors of the Pancreas; Armed Forces Institute of Pathology: Washington, DC, USA, 1997. [Google Scholar]
- Larsson, L.I.; Schwartz, T.; Lundqvist, G.; Chance, R.E.; Sundler, F.; Rehfeld, J.F.; Grimelius, L.; Fahrenkrug, J.; Schaffalitzky de Muckadell, O.; Moon, N. Occurrence of human pancreatic polypeptide in pancreatic endocrine tumors. Possible implication in the watery diarrhea syndrome. Am. J. Pathol. 1976, 85, 675–684. [Google Scholar] [PubMed]
- Larsson, L.I.; Grimelius, L.; Håkanson, R.; Rehfeld, J.F.; Stadil, F.; Holst, J.; Angervall, L.; Sundler, F. Mixed endocrine pancreatic tumors producing several peptide hormones. Am. J. Pathol. 1975, 79, 271–284. [Google Scholar] [PubMed]
- Solcia, E.; Kloppel, G.; Sobin, L.H. Histological Typing of Endocrine Tumours; Springer: Berlin, Germany; New York, NY, USA, 2000. [Google Scholar]
- Ligiero Braga, T.; Santos-Oliveira, R. PPoma Review: Epidemiology, Aetiopathogenesis, Prognosis and Treatment. Diseases 2018, 6, 8. [Google Scholar] [CrossRef] [PubMed]
- Yang, M.; Tian, B.; Zhang, Y.; Su, A.; Yue, P.; Xu, S.; Wang, L. Epidemiology, diagnosis, surgical treatment and prognosis of the pancreatic neuroendocrine tumors: Report of 125 patients from one single center. Indian J. Cancer 2015, 52, 343–349. [Google Scholar] [CrossRef] [PubMed]
- Hochwald, S.N.; Zee, S.; Conlon, K.C.; Colleoni, R.; Louie, O.; Brennan, M.F.; Klimstra, D.S. Prognostic factors in pancreatic endocrine neoplasms: An analysis of 136 cases with a proposal for low-grade and intermediate-grade groups. J. Clin. Oncol. 2002, 20, 2633–2642. [Google Scholar] [CrossRef] [PubMed]
- Klöppel, G.; Heitz, P.U. Pancreatic Endocrine Tumours. Pathol. Res. Pract. 1988, 183, 155–168. [Google Scholar] [CrossRef]
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ilić, I.; Katić, V.; Randjelović, P.; Stojanović, N.; Antovic, A.; Ilić, R. Pancreatic Polypeptide-Secreting Tumour of the Proximal Pancreas (PPoma)—Ultra Rare Pancreatic Tumour: Clinically Malign, Histologically Benign. Medicina 2019, 55, 523. https://doi.org/10.3390/medicina55090523
Ilić I, Katić V, Randjelović P, Stojanović N, Antovic A, Ilić R. Pancreatic Polypeptide-Secreting Tumour of the Proximal Pancreas (PPoma)—Ultra Rare Pancreatic Tumour: Clinically Malign, Histologically Benign. Medicina. 2019; 55(9):523. https://doi.org/10.3390/medicina55090523
Chicago/Turabian StyleIlić, Ivan, Vuka Katić, Pavle Randjelović, Nikola Stojanović, Aleksandra Antovic, and Ratko Ilić. 2019. "Pancreatic Polypeptide-Secreting Tumour of the Proximal Pancreas (PPoma)—Ultra Rare Pancreatic Tumour: Clinically Malign, Histologically Benign" Medicina 55, no. 9: 523. https://doi.org/10.3390/medicina55090523
APA StyleIlić, I., Katić, V., Randjelović, P., Stojanović, N., Antovic, A., & Ilić, R. (2019). Pancreatic Polypeptide-Secreting Tumour of the Proximal Pancreas (PPoma)—Ultra Rare Pancreatic Tumour: Clinically Malign, Histologically Benign. Medicina, 55(9), 523. https://doi.org/10.3390/medicina55090523







