Comparison of Anti-Microbial Effects of Low-Level Laser Irradiation and Microwave Diathermy on Gram-Positive and Gram-Negative Bacteria in an In Vitro Model
Abstract
:1. Introduction
2. Materials and Methods
2.1. Bacterial Strains
2.2. Laser Parameters
2.3. Microwave Diathermy Parameters
2.4. Experimental Procedure
2.5. Data Analysis
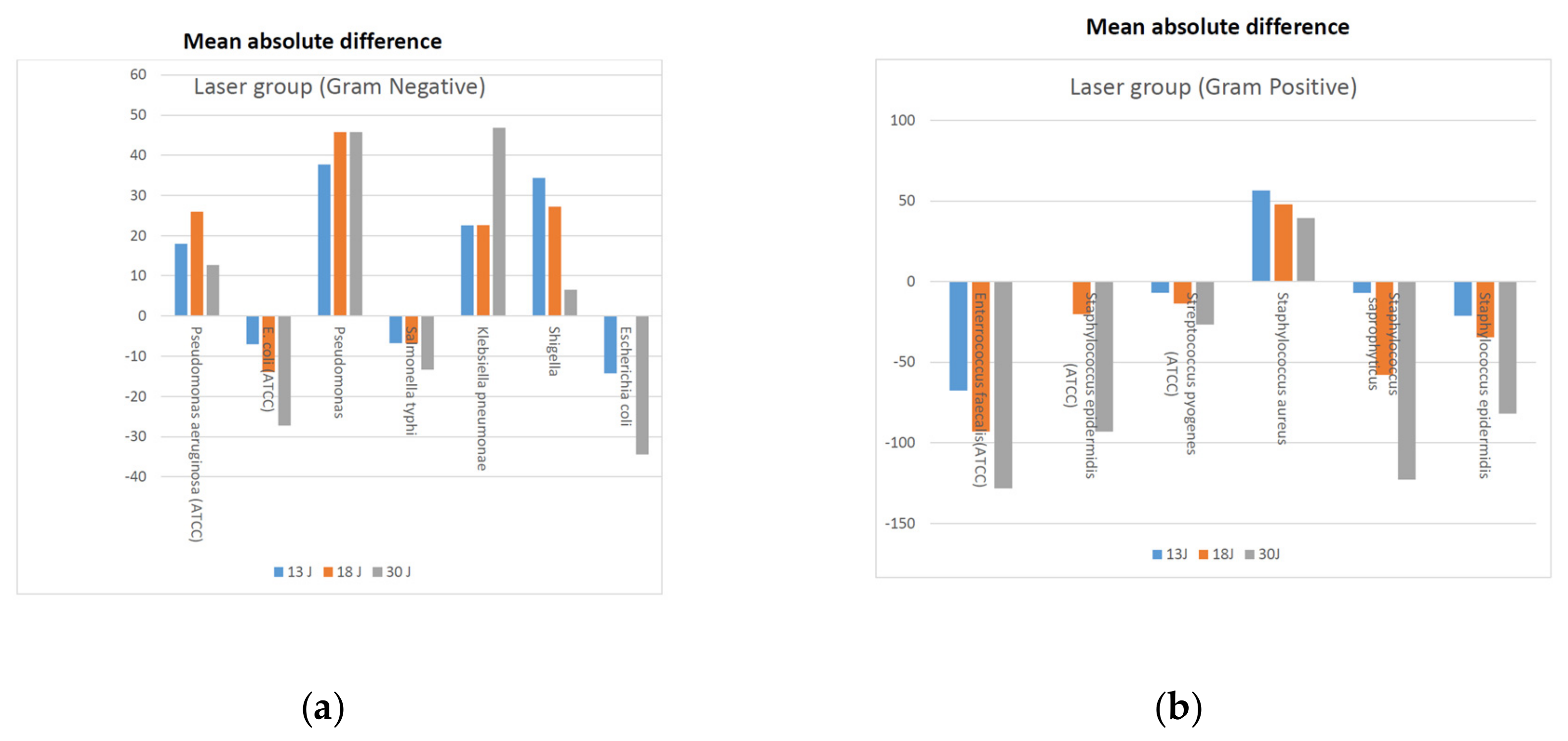
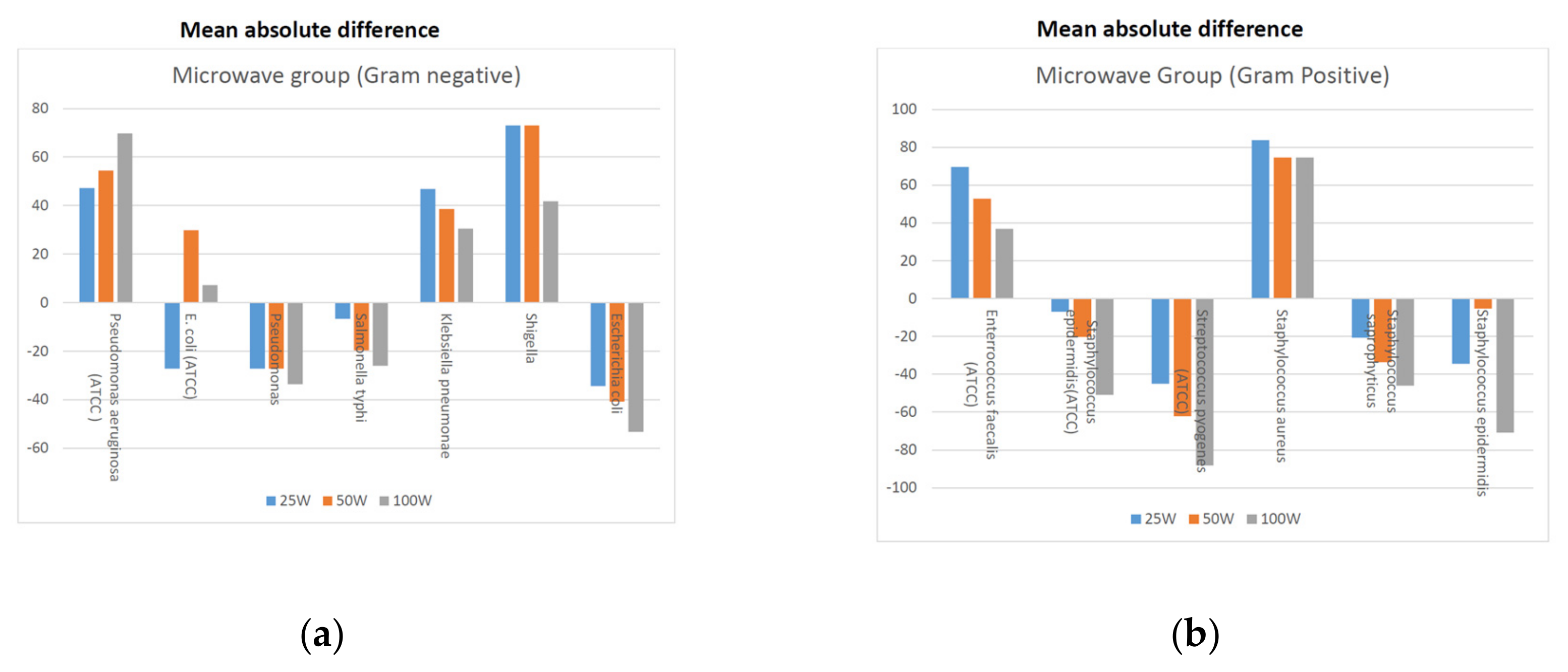
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Velez, R.; Sloand, E. Combating antibiotic resistance, mitigating future threats and ongoing. J. Clin. Nurs. 2016, 25, 1886–1889. [Google Scholar] [CrossRef] [PubMed]
- Akova, M. Epidemiology of antimicrobial resistance in bloodstream infections. Virulence 2016, 7, 252–266. [Google Scholar] [CrossRef] [PubMed]
- Vijayakumar, R.; Sandle, T.; Al-Aboody, M.S.; AlFonaisan, M.K.; Alturaiki, W.; Mickymaray, S.; Premanathan, M.; Alsagaby, S.A. Distribution of biocide resistant genes and biocides susceptibility in multidrug-resistant Klebsiella pneumoniae, Pseudomonas aeruginosa and Acinetobacter baumannii—A first report from the Kingdom of Saudi Arabia. J. Infect. Public Health 2018, 11, 812–816. [Google Scholar] [CrossRef] [PubMed]
- Balkhy, H.H.; Assiri, A.M.; Al, H.; Al-abri, S.S.; Al-katheeri, H.; Alansari, H.; Abdulrazzaq, N.M.; Aidara-Kane, A.; Pittet, D.; Erlacher-Vindel, E.; et al. The strategic plan for combating antimicrobial resistance in Gulf Cooperation Council States. J. Infect. Public Health 2016, 9, 375–385. [Google Scholar] [CrossRef] [PubMed]
- Tayyib, N.; Coyer, F.; Lewis, P. Saudi Arabian adult intensive care unit pressure ulcer incidence and risk factors: A prospective cohort study. Int. Wound J. 2016, 13, 912–919. [Google Scholar] [CrossRef]
- Smith, M.B.; Totten, A.; Hickam, H.D.; Fu, R.; Wasson, N.; Rahman, B.; Abdulrazzaq, N.M.; Aidara-Kane, A.; Pittet, D.; Erlacher-Vindel, E.; et al. Pressure ulcer treatment strategies: A systematic comparative effectiveness review. Ann. Intern. Med. 2013, 159, 39–50. 2013, 159, 39–50. Available online: http://search.ebscohost.com/login.aspx?direct=true&db=cin20&AN=2012175886&site=ehost-live (accessed on 16 December 2018). [CrossRef]
- Machado, R.S.; Viana, S.; Sbruzzi, G. Low-level laser therapy in the treatment of pressure ulcers: Systematic review. Lasers Med. Sci. 2017, 32, 937–944. [Google Scholar] [CrossRef]
- Kitchen, S.; Partridge, C. Review of Shortwave Diathermy Continuous and Pulsed Patters. Physiother 1992, 78, 243–252. [Google Scholar] [CrossRef]
- Kumaran, B.; Watson, T. Radiofrequency-based treatment in therapy-related clinical practice–a narrative review. Part I: Acute conditions. Phys. Ther. Rev. 2015, 20, 241–254. Available online: http://www.tandfonline.co (accessed on 16 December 2018). [CrossRef]
- Goats, G.C. Microwave diathermy. Br. J. Sports Med. 1990, 24, 212–218. [Google Scholar] [CrossRef]
- Silveira, P.C.L.; Silva, L.A.; Tuon, T.; Freitas, T.P.; Streck, E.L.; Pinho, R.A. Effects of low-level laser therapy on epidermal oxidative response induced by wound healing. Rev. Bras. Fisioter. 2009, 13, 281–287. [Google Scholar] [CrossRef]
- Esnouf, A.; Wright, P.A.; Moore, J.C.; Ahmed, S. Depth of Penetration of an 850nm Wavelength Low Level Laser in Human Skin. Acupunct. Electro Ther. Res. 2007, 32, 81–86. [Google Scholar] [CrossRef]
- Commentary, C. Clinical commentary beyond statistical significance: Clinical interpretation of rehabilitation research corresponding author. Int. J. Sports Phys. Ther. 2014, 9, 726–736. [Google Scholar]
- Dixit, S.; Maiya, A.; Rao, L.; Rao, M.A.; Shastry, B.A.; Ramachandra, L. Photobiomodulation by helium neon and diode lasers in an excisional wound model: A single blinded trial. Adv. Biomed. Res. 2012, 1, 55–60. [Google Scholar] [CrossRef] [PubMed]
- Nussbaum, E.L.; Lilge, L.; Mazzulli, T. Effects of 810 nm laser irradiation on in vitro growth of bacteria: Comparison of continuous wave and frequency modulated light. Lasers Surg. Med. 2002, 31, 343–351. [Google Scholar] [CrossRef] [PubMed]
- Dixit, S.; Agrawal, P.R.; Sharma, D.K.; Singh, R.P. Closure of chronic non healing ankle ulcer with low level laser therapy in a patient presenting with thalassemia intermedia: Case report. Ind. J. Plast. Surg. 2014, 47, 432. [Google Scholar]
- Karlekar, A.; Bharati, S.; Saxena, R.; Mehta, K. Assessment of feasibility and efficacy of Class IV laser therapy for postoperative pain relief in off-pump coronary artery bypass surgery patients: A pilot study. Ann. Card. Anaesth. 2015, 18, 317–322. [Google Scholar] [CrossRef]
- Korpan, N.N.; Saradeth, T. Clinical effects of continuous microwave for postoperative septic wound treatment: A double-blind controlled trial. Am. J. Surg. 1995, 170, 271–276. [Google Scholar] [CrossRef]
- Yuan, X.; Song, Y.; Song, Y.; Xu, J.; Wu, Y.; Glidle, A.; Cusack, M.; Ijaz, U.Z.; Cooper, J.M.; Huang, W.E.; et al. Crossm effect of laser irradiation on cell function and its implications in raman spectroscopy. Appl. Environ. Microbiol. 2018, 84, 1–12. [Google Scholar] [CrossRef]
- Pereira, P.R.; De Paula, J.B.; Cielinski, J.; Pilonetto, M.; Von Bahten, L.C. Effects of low intensity laser in in vitro bacterial culture and in vivo infected wounds. Rev. Col. Bras. Cir. 2014, 41, 49–55. Available online: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0100-69912014000100049&lng=en&tlng=en (accessed on 16 December 2018). [CrossRef] [Green Version]
- Nussbaum, E.L.; Mg, O.N. Effects of low intensity laser irradiation during healing of infected skin wounds in the rat. Photonics lasers Med. 2015, 3, 23–36. [Google Scholar] [CrossRef] [PubMed]
- Sedgwick, P. Clinical significance versus statistical significance. BMJ 2014, 2130, 2–3. [Google Scholar] [CrossRef]
- Biener, G.; Masson-meyers, D.S.; Bumah, V.V.; Hussey, G.; Stoneman, M.R.; Enwemeka, C.S.; Raicu, V. Blue/violet laser inactivates methicillin-resistant Staphylococcus aureus by altering its transmembrane potential. J. Photochem. Photobiol. B Biol. 2017, 170, 118–124. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ye, D.; Xu, Y.; Zhang, H.; Fu, T.; Jiang, L.; Bai, Y. Effects of Low-Dose Microwave on Healing of Fractures with Titanium Alloy Internal Fixation: An Experimental Study in a Rabbit Model. PLoS ONE 2013, 8, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Zhou, B.W.; Shin, S.G.; Hwang, K. Effect of microwave irradiation on cellular disintegration of Gram positive and negative cells. Appl. Microbiol. Biotechnol. 2010, 87, 765–770. [Google Scholar] [CrossRef] [PubMed]
- Gedikli, S.; Tabak, Ö.; Tomsuk, Ö.; Cabuk, A. Effect of Microwaves on Some Gram Negative and Gram Positive Bacteria. J. Appl. Biol. Sci. 2008, 2, 67–71. [Google Scholar]
- Janković, S.M.; Milošev, M.Z.; Novaković, M.L. The Effects of Microwave Radiation on Microbial Cultures. Hosp. Pharmacol. 2014, 1, 102–108. [Google Scholar] [CrossRef]
- Andraus, R.A.C.; Maia, L.P.; João Santos, P.M.; Mesquita, A.R.; Santos, T.G.; Braoios, A.; Prado, R.P. Analysis of low level laser therapy in vitro cultures of bacteria and fungi. MTP Rehab. J. 2015, 13, 304. [Google Scholar]
| Organisms | Origin | |||||||
|---|---|---|---|---|---|---|---|---|
| Treated (Cfu/mL) | ||||||||
| Control (cfu/mL) | Laser Group | Microwave | ||||||
| Energy | No Treatment | 13 J/cm2 | 18 J/cm2 | 30 J/cm2 | 25 W | 50 W | 100 W | |
| Pseudomonas aeruginosa (ATCC 27853) | R | 269.15 ± 3.02 (812.8–89.1) | 251.19 ± 3.48 (871–72.4) | 295.12 ± 3.39 (1000–87) | 281.84 ± 3.39 (977.2–81.3) | 316.23 ± 3.39 (1071.5–93.3) | 323.6 ± 3.16 (1023.3–102.3) | 338.84 ± 3.16 (1023.3–977.2) |
| E. coli (ATCC 25922) | R | 309.03 ± 3.02 (933.3–102.3) | 302 ± 3.55 (1071.5–85.1) | 295.12 ± 3.63 (1071.5–81.3) | 281.84 ± 0.57 (1047.1–85.1) | 281.84 ± 3.72 (1096.5–104.7) | 338.84 ± 3.24 (1096.5–104.7) | 316.23 ± 3.39 (1071.5–93.3) |
| Pseudomonas sp. | C | 309.03 ± 3.16 (977.2–97.7) | 346.74 ± 3.72 (1288.3–93.3) | 354.8 ± 3.47 (1230.3–10.2) | 354.8 ± 3.31 (1174.9–10.7) | 281.84 ± 3.31 (933.3–85.1) | 281.84 ± 3.89 (1096.5–72.4) | 275.42 ± 3.89 (1071.5–70.8) |
| Salmonella typhi | C | 295.12 ± 2.88 (851.1–102.3) | 288.4 ± 3.31 (955–87.1) | 288.4 ± 3.31 (955–87.1) | 281.84 ± 3.31 (933.3–85.1) | 288.4 ± 3.39 (955–87.1) | 275.43 ± 3.39 (933.3–81.3) | 269.15 ± 3.39 (912–79.4) |
| Klebsiella pneumonae | C | 316.23 ± 2.82 (891.3–112.2) | 338.8 ± 3.39 (1148.2–100) | 338.84 ± 3.31 (1122–102.3) | 346.74 ± 3.16 (1096.5–109.7) | 363.08 ± 3.09 (1122–117.5) | 354.81 ± 3.16 (1122–112.2) | 346.74 ± 3.16 (1096.5–109.7) |
| Shigella sp. | C | 281.84 ± 3.02 (851.14–93.3) | 316.23 ± 3.47 (1047.1–91.2) | 309.03 ± 3.47 (1071.5–89.1) | 288.4 ± 3.72 (1071.5–77.6) | 354.81 ± 2.69 (955–131.8) | 354.81 ± 2.69 (955–131.8) | 323.59 ± 3.02 (977.2–107.2) |
| Escherichia coli | C | 316.23 ± 2.95 (933.3–107.2) | 295.12 ± 3.46 (1023.2–85.1) | 316.2 ± 3.47 (1096.5–91.2) | 281.84 ± 3.63 (1023.3–77.63) | 281.84 ± 3.80 (1071.5–74.1) | 275.42 ± 3.89 (1071.5–70.8) | 263.03 ± 4.07 (1071.5–64.6) |
| Enterococcus faecalis (ATCC 29212) | R | 302 ± 2.69 (812.8–112.2) | 234.42 ± 2.88 (676.08–81.28) | 208.93 ± 2.82 (588.8–74.13) | 173.78 ± 2.88 (501.2–60.3) | 371.53 ± 2.46 (1148.2– 151.4) | 354.81 ± 2.51 (912–141.3) | 338.84 ± 2.57 (871–131.8) |
| Staphylococcus epidermidis (ATCC 12228) | R | 302 ± 2.95 (891.3–102.3) | 302 ± 3.47 (1023.3–85.1) | 281.84 ± 3.63 (1023.3–77.6) | 208.93 ± 4.07 (851.1–51.3) | 295.12 ± 3.47 (1023.3–85.1) | 281.84 ± 3.63 (1023.3–77.6) | 251.19 ± 4.17 (1047.1–60.3) |
| Streptococcus pyogenes (ATCC 19615) | R | 302 ± 3.09 (933.3–97.7) | 295.12 ± 3.55 (1047.1–83.2) | 288.4 ± 3.63 (1047.1–79.4) | 275.42 ± 3.8 (1047.1–72.4) | 257.04 ± 4.37 (1122–58.9) | 239.88 ± 5.62 (1174.9–38) | 213.8 ± 5.62 (1202.26–38) |
| Staphylococcus aureus | C | 323.59 ± 2.95 (954.99–109.7) | 380.19 ± 3.09 (1174.9–123.03) | 371.54 ± 3.09 (1148.2–120.2) | 363.08 ± 3.16 (1148.2–114.8) | 407.38 ± 2.69 (1096.48–151.4) | 398.11 ± 2.69 (1071.52–147.9) | 398.11 ± 2.69 (1071.52–147.9) |
| Staphylococcus saprophyticus | C | 309.02 ± 2.95 (912.01–104.7) | 302 ± 3.39 (1023.3–89.13) | 251.19 ± 3.55 (891.3–70.8) | 186.21 ± 3.31 (616.6–56.2) | 288.4 ± 3.47 (1000–287.9) | 275.42 ± 3.63 (1000–75.9) | 263.03 ± 3.89 (1023.29–1.8) |
| Staphylococcus epidermidis | C | 316.23 ± 2.88 (912–109.7) | 295.12 ± 3.47 (1023.3–85.1) | 281.84 ± 3.55 (1000–79.4) | 234.44 ± 3.88 (891.3–61.7) | 281.84 ± 3.63 (1023.3–77) | 263.03 ± 3.63 (1023.3–70.8) | 245.47 ± 4.27 (1047.1–57.5) |
| Organisms | ||||||
|---|---|---|---|---|---|---|
| Treated (cfu/mL) | ||||||
| Laser Group (R Value) | Microwave | |||||
| Energy | 13 J | 18 J | 30 J | 25 W | 50 W | 100 W |
| Gram-negative strains | ||||||
| Pseudomonas aeruginosa (ATCC 27853) | −0.94 * (LE) | +0.97 (LE) | +0.89 (LE) | +0.99 (LE) | +0.99 (LE) | +1 (LE) |
| E. coli (ATCC 25922) | −0.73 * (ME) | −0.90 * (LE) | −0.99 * (LE) | −0.97 * (LE) | +0.98 (LE) | +0.75 (ME) |
| Pseudomonas sp. | +0.98 (LE) | +0.99 (LE) | +0.99 (LE) | −0.97 * (LE) | −0.97 * (LE) | −0.98 * (LE) |
| Salmonella typhi | −0.74 * (ME) | −0.74 * (ME) | −0.91 * (LE) | −0.73 * (ME) | −0.95 * (LE) | −0.97 * (LE) |
| Klebsiella pneumonae | +0.96 (LE) | +0.97 (LE) | +0.98 (LE) | +0.99 (LE) | +0.99 (LE) | +0.98 (LE) |
| Shigella sp. | +0.98 (LE) | +0.97 (LE) | +0.70 (LE) | +1 (LE) | +1 (LE) | +0.99 (LE) |
| Escherichia coli | −0.96 * (LE) | −0.01 * (TE) | −0.98 * (LE) | −0.98 * (LE) | −0.99 * (LE) | −0.99 * (LE) |
| Gram-positive strains | ||||||
| Enterococcus faecalis (ATCC 29212) | −1 * (LE) | +0.92 * (LE) | −1 * (LE) | +1 (LE) | +1 (LE) | +0.99 (LE) |
| Staphylococcus epidermidis (ATCC 12228) | 0 (TE) | −0.95 * (LE) | −1 * (LE) | −0.73 * (ME) | −0.95 * (LE) | −0.99 * (LE) |
| Streptococcus pyogenes (ATCC 19615) | −0.72 * (ME) | −0.90 * (LE) | −0.97 * (LE) | −0.99 * (LE) | −0.9 * (LE) | −1 * (LE) |
| Staphylococcus aureus | +0.99 (LE) | +0.99 (LE) | +0.99 (LE) | +1 (LE) | +1 (LE) | +1 (LE) |
| Staphylococcus saprophyticus | −0.74 * (ME) | −0.99 * (LE) | −1 * (LE) | −0.96 * (LE) | −0.98 * (LE) | −0.99 * (LE) |
| Staphylococcus epidermidis | −0.96 * (LE) | −0.98 * (LE) | −1 * (LE) | −0.98 * (LE) | −0.99 * (LE) | −1 * (LE) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dixit, S.; Ahmad, I.; Hakami, A.; Gular, K.; Tedla, J.S.; Abohashrh, M. Comparison of Anti-Microbial Effects of Low-Level Laser Irradiation and Microwave Diathermy on Gram-Positive and Gram-Negative Bacteria in an In Vitro Model. Medicina 2019, 55, 330. https://doi.org/10.3390/medicina55070330
Dixit S, Ahmad I, Hakami A, Gular K, Tedla JS, Abohashrh M. Comparison of Anti-Microbial Effects of Low-Level Laser Irradiation and Microwave Diathermy on Gram-Positive and Gram-Negative Bacteria in an In Vitro Model. Medicina. 2019; 55(7):330. https://doi.org/10.3390/medicina55070330
Chicago/Turabian StyleDixit, Snehil, Irfan Ahmad, Abdulrahim Hakami, Kumar Gular, Jaya Shanker Tedla, and Mohammed Abohashrh. 2019. "Comparison of Anti-Microbial Effects of Low-Level Laser Irradiation and Microwave Diathermy on Gram-Positive and Gram-Negative Bacteria in an In Vitro Model" Medicina 55, no. 7: 330. https://doi.org/10.3390/medicina55070330
APA StyleDixit, S., Ahmad, I., Hakami, A., Gular, K., Tedla, J. S., & Abohashrh, M. (2019). Comparison of Anti-Microbial Effects of Low-Level Laser Irradiation and Microwave Diathermy on Gram-Positive and Gram-Negative Bacteria in an In Vitro Model. Medicina, 55(7), 330. https://doi.org/10.3390/medicina55070330







