Use of Collagen in Cosmetic Products
Abstract
1. Introduction
2. Characteristics of Collagen
2.1. Structure and Biosynthesis
2.2. Types of Collagen
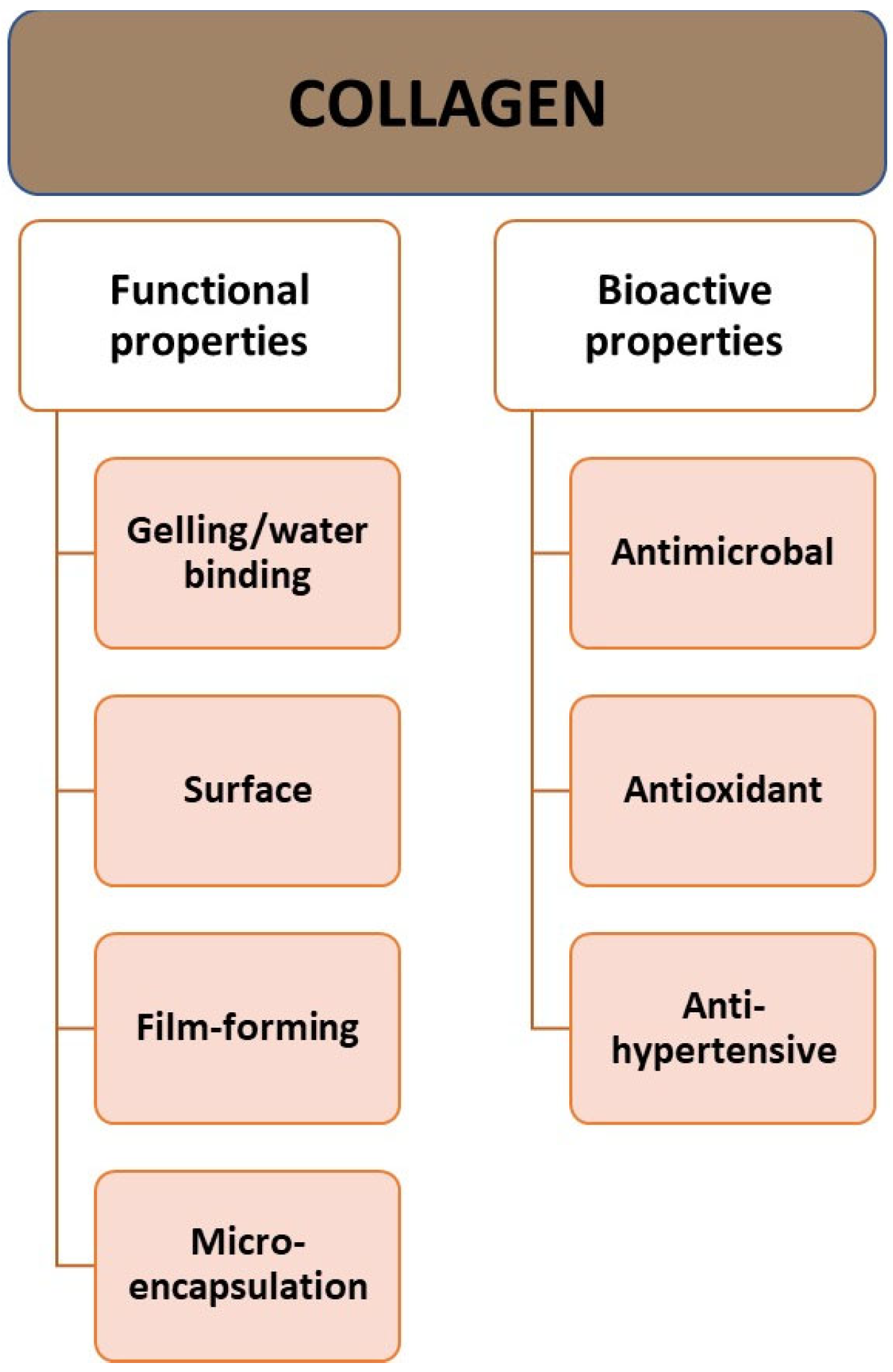
2.3. Physicochemical Characteristic of Collagen
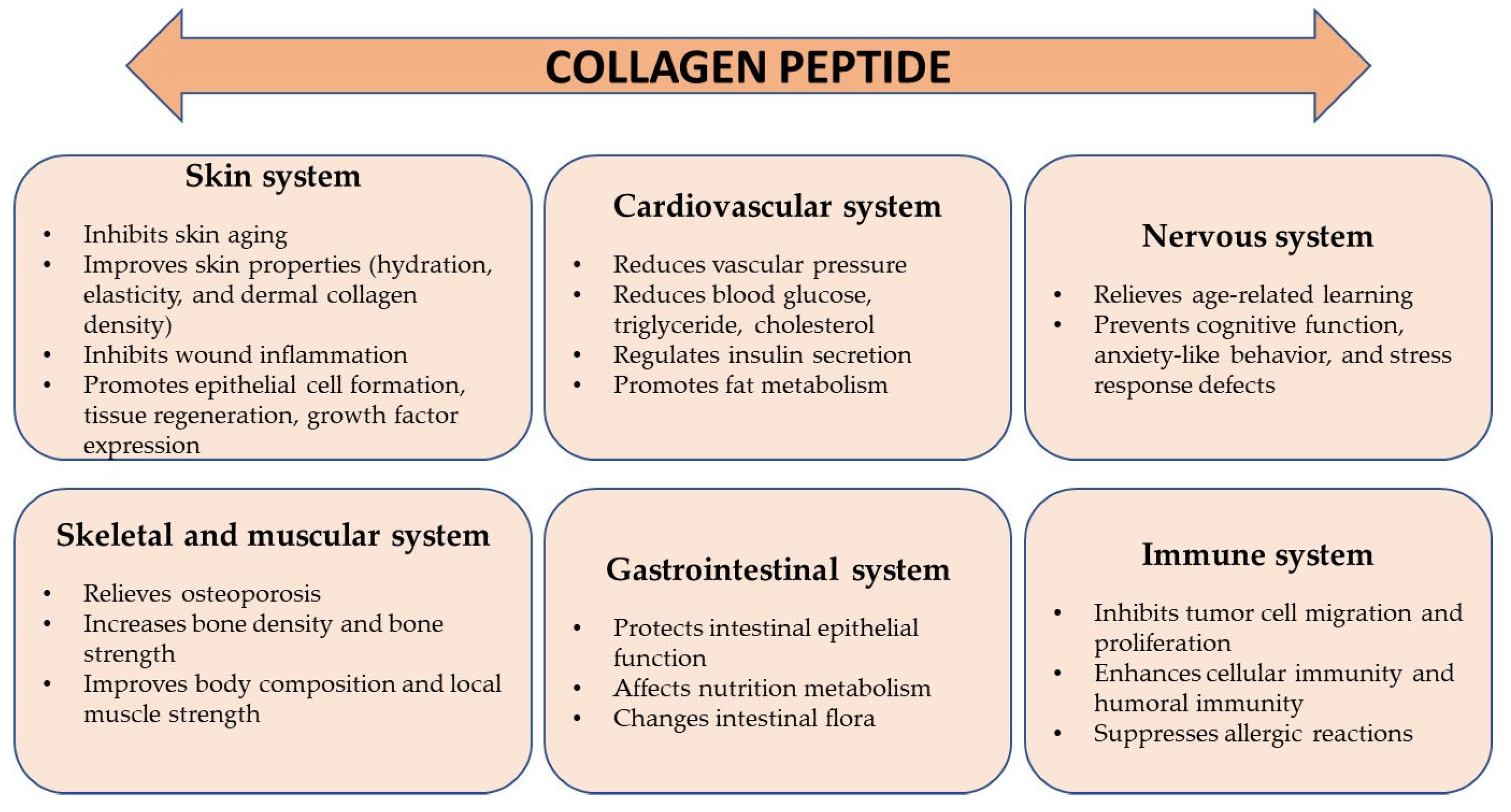
2.4. The Role of Collagen in the Body
2.5. Effects of Collagen Deficiency in the Body
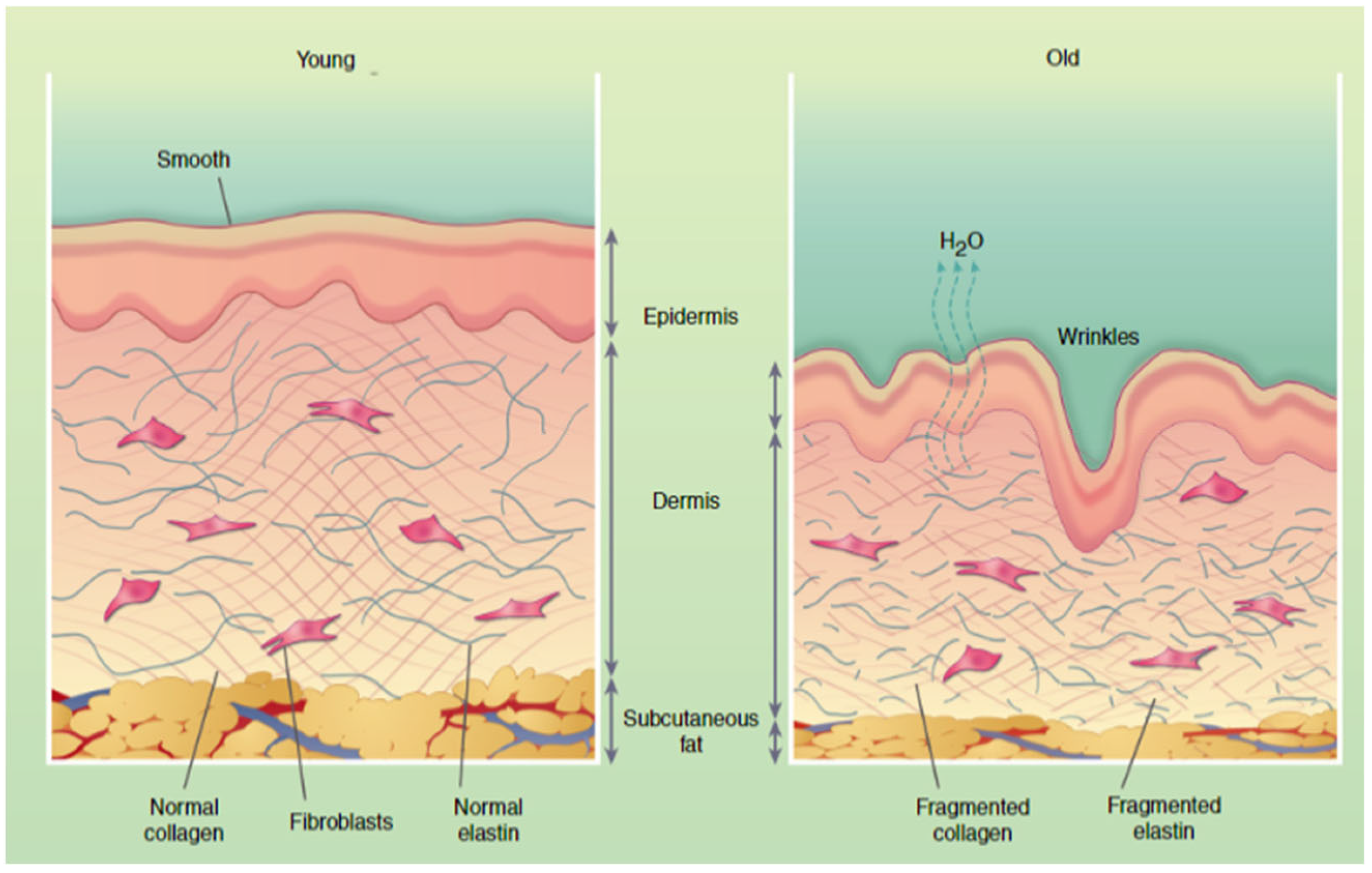
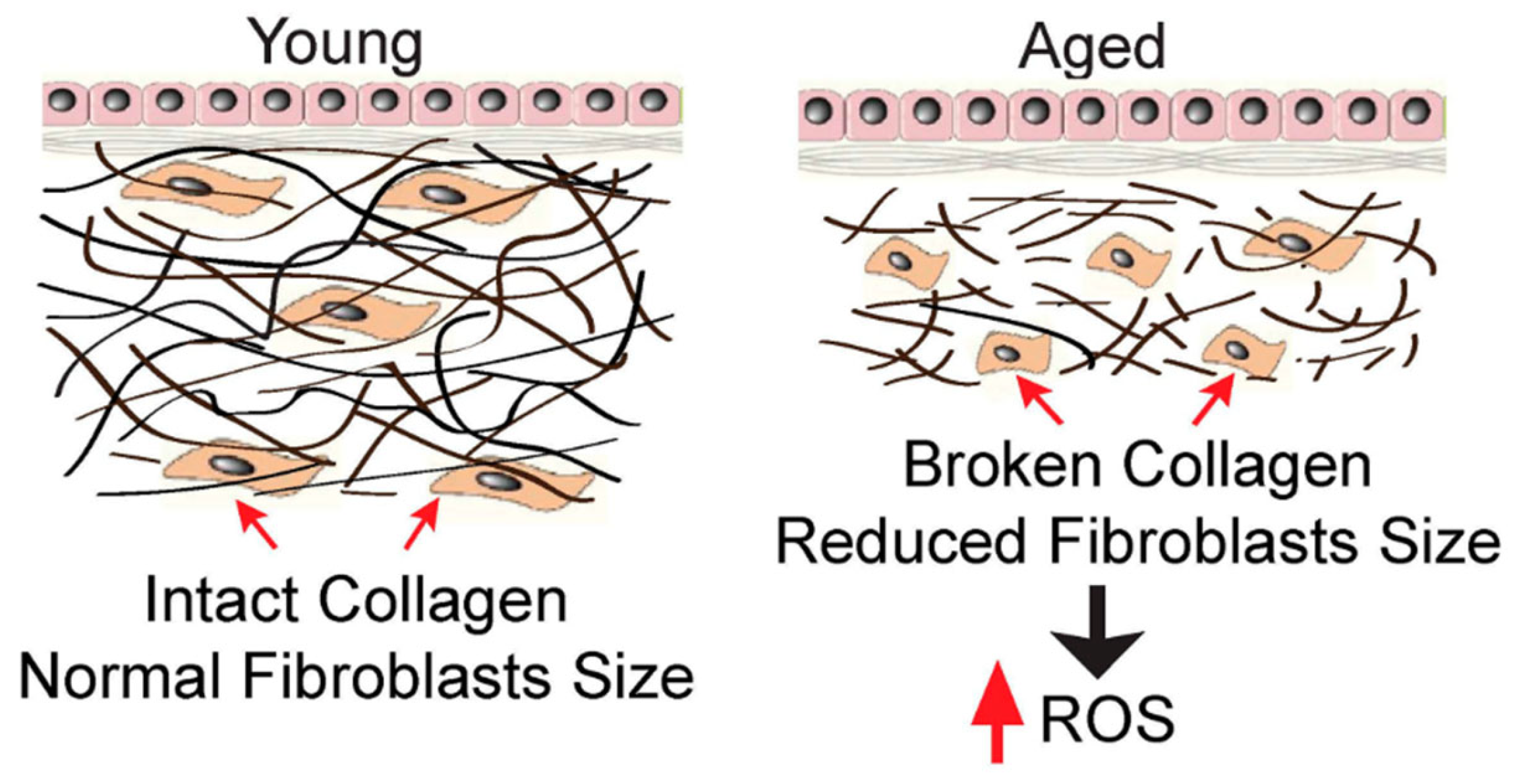
3. The Importance of Collagen in the Skin
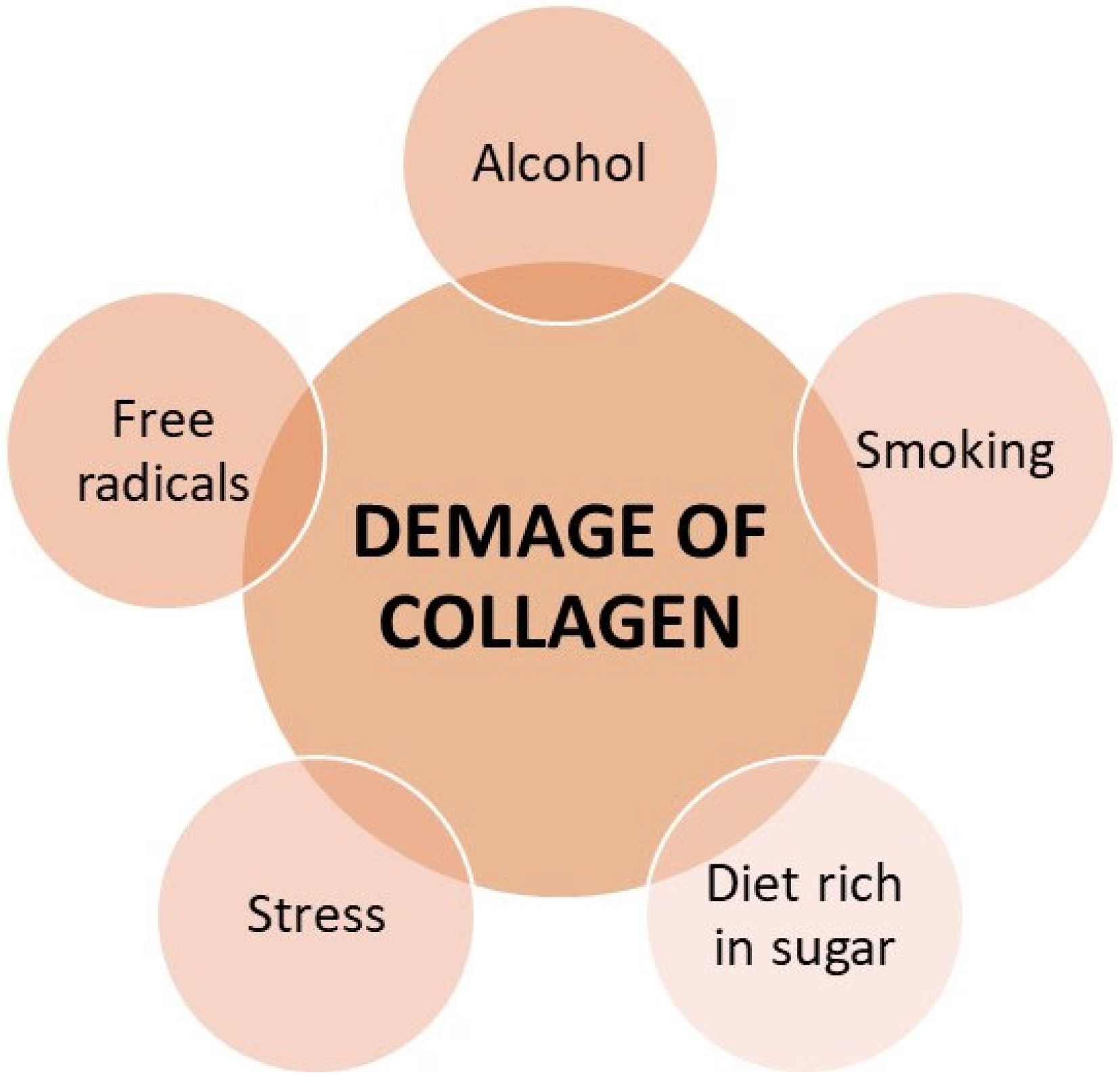
3.1. The Influence of External Factors on Collagen Fibers
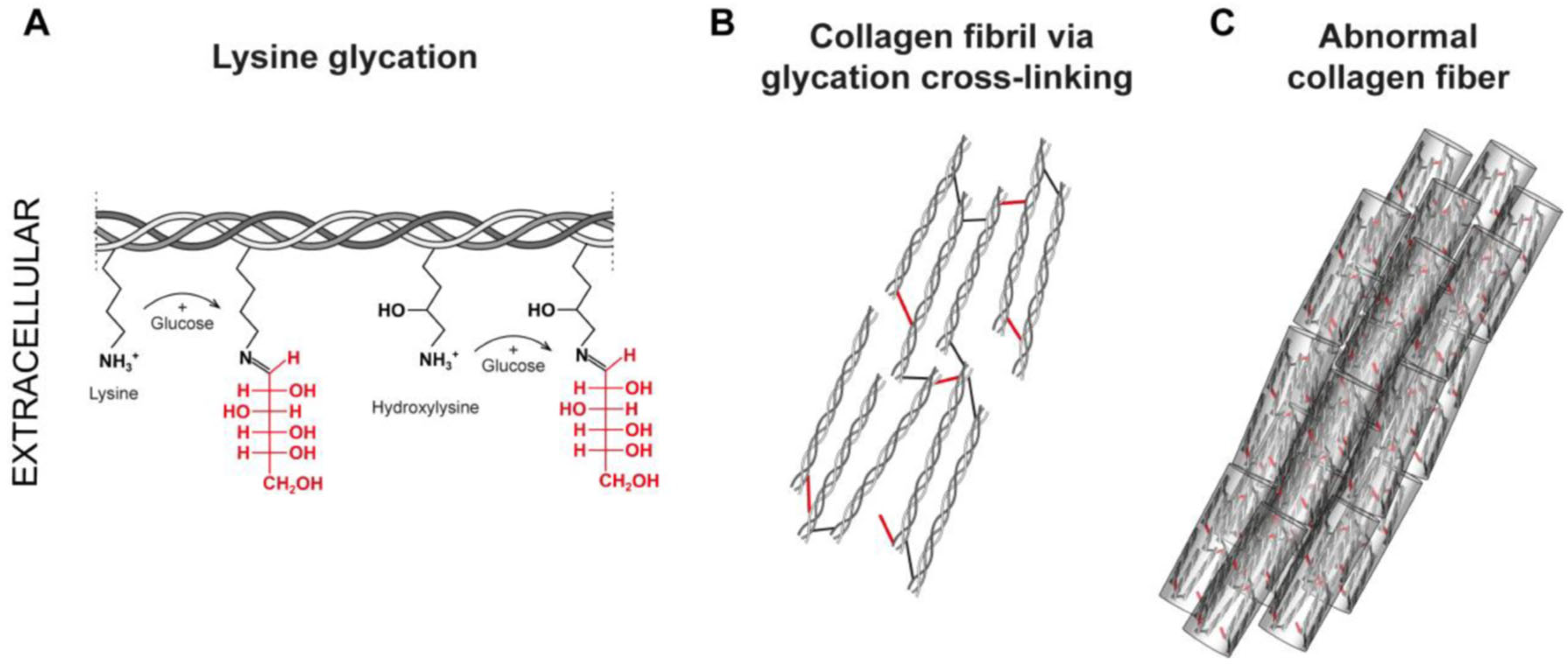
3.1.1. Collagen Glycation
3.1.2. The Effect of UV Radiation on Collagen Fibers
4. Characteristics of Cosmetic Products Containing Collagen
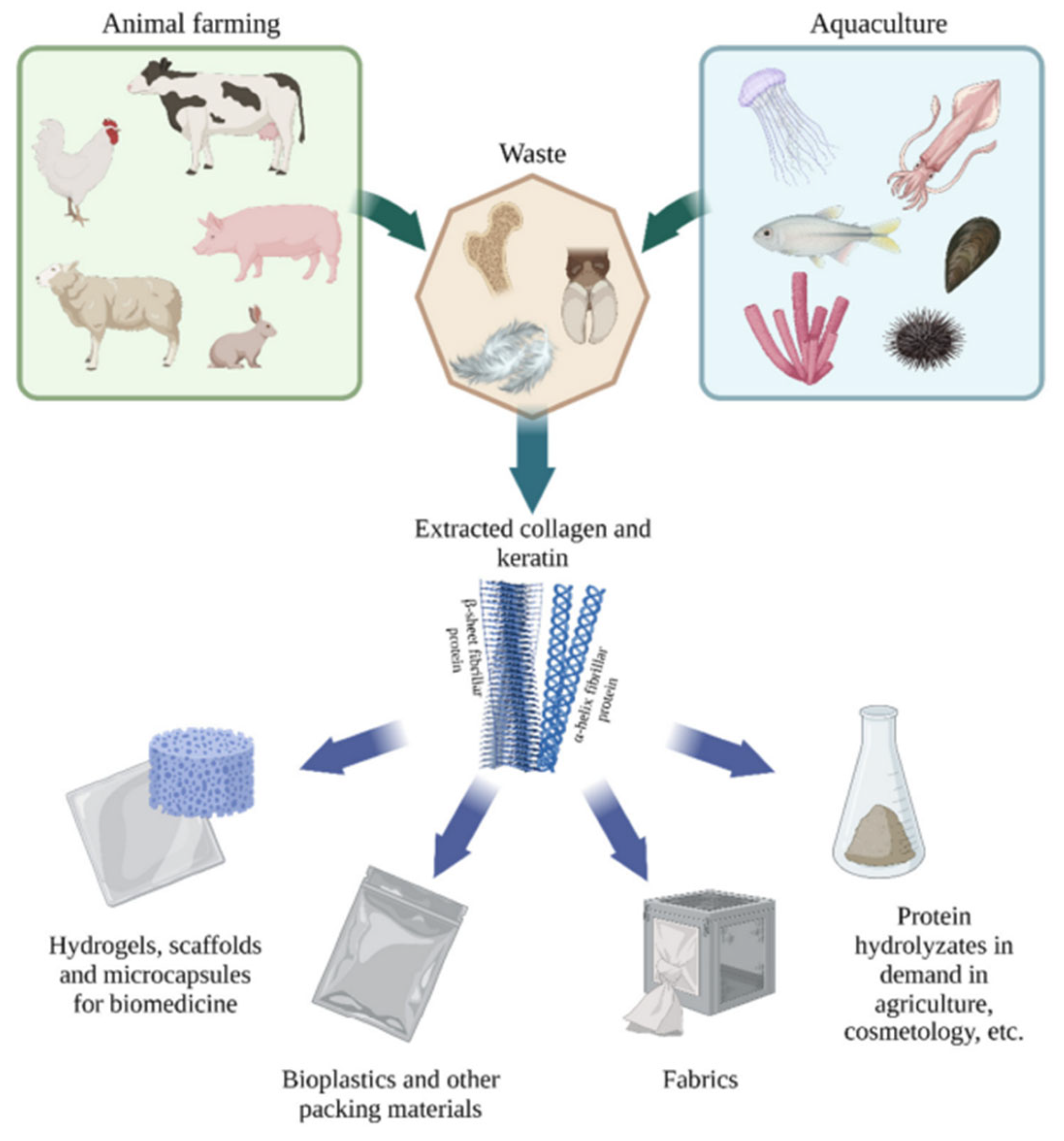
4.1. Sources of Collagen Used in Cosmetics
4.2. Collagen Fillers
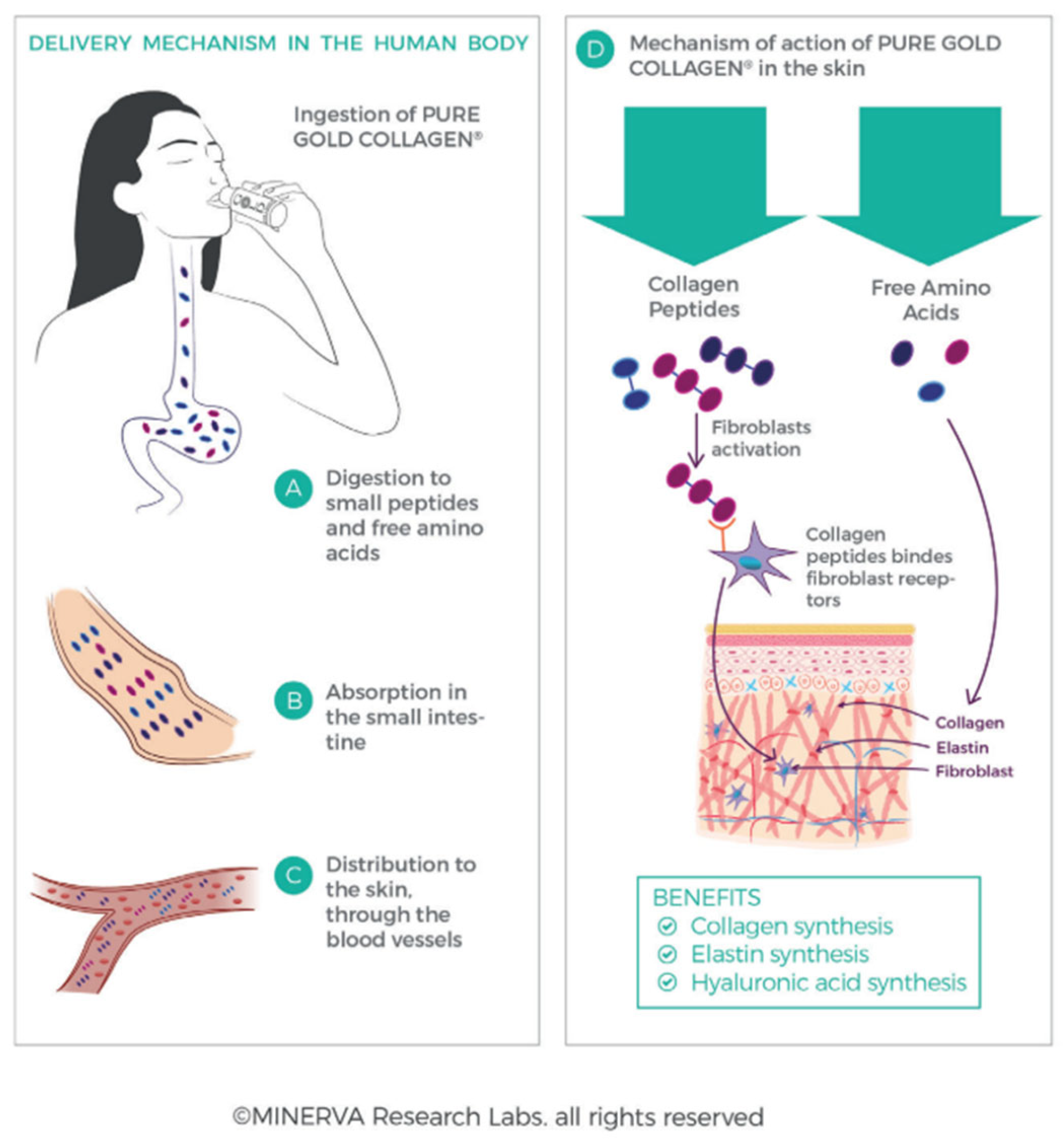
4.3. Oral Products with Collagen and Its Hydrolysates and Their Effects
4.4. Products with Collagen for Use on the Skin and Mucous Membrane
5. Side Effects of Overused of Collagen Products
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Usman, R.; Bharadvaja, N. Nutricosmetics: Role in health, nutrition, and cosmetics. Proc. Indian Natl. Sci. Acad. 2023, 89, 584–599. [Google Scholar] [CrossRef]
- Martin, I.K.; Glaser, D.A. Cosmeceuticals: The New Medicine of Beauty ‘Cosmeceuticals’ blur the line between drug and cosmetic, doctor and aesthetician, and patient and consumer. Sci. Med. 2011, 108, 60. [Google Scholar]
- Alves, A.L.; Marques, A.L.P.; Martins, E.; Silva, T.H.; Reis, R.L. Cosmetic Potential of Marine Fish Skin Collagen. Cosmetics 2017, 4, 39. [Google Scholar] [CrossRef]
- Prajaputra, V.; Isnaini, N.; Maryam, S.; Ernawati, E.; Deliana, F.; Haridhi, H.A.; Fadli, N.; Karina, S.; Agustina, S.; Nurfadillah, N.; et al. Exploring marine collagen: Sustainable sourcing, extraction methods, and cosmetic applications. S. Afr. J. Chem. Eng. 2024, 47, 197–211. [Google Scholar] [CrossRef]
- Al-Atif, H. Collagen Supplements for Aging and Wrinkles: A Paradigm Shift in the Fields of Dermatology and Cosmetics. Dermatol. Pr. Concept. 2022, 12, 2022018–2022019. [Google Scholar] [CrossRef]
- Felician, F.F.; Xia, C.; Qi, W.; Xu, H. Collagen from Marine Biological Sources and Medical Applications. Chem. Biodivers. 2018, 15, e1700557. [Google Scholar] [CrossRef]
- Alcaide-Ruggiero, L.; Molina-Hernández, V.; Granados, M.M.; Domínguez, J.M. Main and minor types of collagens in the articular cartilage: The role of collagens in repair tissue evaluation in chondral defects. Int. J. Mol. Sci. 2021, 22, 13329. [Google Scholar] [CrossRef]
- Engel, J.; Bächinger, H.P. Structure, stability and folding of the collagen triple helix. Top. Curr. Chem. 2005, 247, 7–33. [Google Scholar] [CrossRef]
- Gordon, M.K.; Hahn, R.A. Collagens. Cell Tissue Res. 2010, 339, 247–257. [Google Scholar] [CrossRef]
- Rittié, L.; Fisher, G.J. Natural and Sun-Induced Aging of Human Skin. Cold Spring Harb. Perspect. Med. 2015, 5, a015370. [Google Scholar] [CrossRef]
- Jariashvili, K.; Madhan, B.; Brodsky, B.; Kuchava, A.; Namicheishvili, L.; Metreveli, N. UV Damage of Collagen: Insights from Model Collagen Peptides. Biopolymers 2011, 97, 189–198. [Google Scholar] [CrossRef]
- Owczarzy, A.; Kurasiński, R.; Kulig, K.; Rogóż, W.; Szkudlarek, A.; Maciążek-Jurczyk, M. Collagen—Structure, properties and application. Eng. Biomater. 2020, 23, 17–23. [Google Scholar] [CrossRef]
- Ottani, V.; Raspanti, M.; Ruggeri, A. Collagen structure and functional implications. Micron 2001, 32, 251–260. [Google Scholar] [CrossRef]
- Shoulders, M.D.; Raines, R.T. Collagen Structure and Stability. Annu. Rev. Biochem. 2009, 78, 929–958. [Google Scholar] [CrossRef]
- Sionkowska, A.; Skrzyński, S.; Śmiechowski, K.; Kołodziejczak, A. The review of versatile application of collagen. Polym. Adv. Technol. 2017, 28, 4–9. [Google Scholar] [CrossRef]
- Samad, N.; Sikarwar, A. Collagen: New Dimension in Cosmetic and Healthcare. Int. J. Biochem. Res. Rev. 2016, 14, 1–8. [Google Scholar] [CrossRef]
- Bolke, L.; Schlippe, G.; Gerß, J.; Voss, W. A Collagen Supplement Improves Skin Hydration, Elasticity, Roughness, and Density: Results of a Randomized, Placebo-Controlled, Blind Study. Nutrients 2019, 11, 2494. [Google Scholar] [CrossRef]
- Gr up SM Marine Collagen: Extraction and Applications. Available online: www.smgebooks.com (accessed on 4 January 2024).
- Venkatesan, J.; Anil, S.; Kim, S.-K.; Shim, M.S. Marine Fish Proteins and Peptides for Cosmeceuticals: A Review. Mar. Drugs 2017, 15, 143. [Google Scholar] [CrossRef]
- Sionkowska, A.; Adamiak, K.; Musiał, K.; Gadomska, M. Collagen Based Materials in Cosmetic Applications: A Review. Materials 2020, 13, 4217. [Google Scholar] [CrossRef]
- Hexsel, D.; Zague, V.; Schunck, M.; Bsc, C.S.; Camozzato, F.O.; Oesser, S. Oral supplementation with specific bioactive collagen peptides improves nail growth and reduces symptoms of brittle nails. J. Cosmet. Dermatol. 2017, 16, 520–526. [Google Scholar] [CrossRef]
- Aguirre-Cruz, G.; León-López, A.; Cruz-Gómez, V.; Jiménez-Alvarado, R.; Aguirre-Álvarez, G. Collagen Hydrolysates for Skin Protection: Oral Administration and Topical Formulation. Antioxidants 2020, 9, 181. [Google Scholar] [CrossRef]
- Karsdal, M.A. Biochemistry of Collagens, Laminins and Elastin: Structure, Function and Biomarkers; Elsevier: Amsterdam, The Netherlands, 2023. [Google Scholar]
- Matinong, A.M.E.; Chisti, Y.; Pickering, K.L.; Haverkamp, R.G. Collagen Extraction from Animal Skin. Biology 2022, 11, 905. [Google Scholar] [CrossRef]
- Lindholm, M.; Manon-Jensen, T.; Karsdal, M.A. Chapter 14—Type XIV collagen. In Biochemistry of Collagens, Laminins and Elastin, 2nd ed.; Academic Press: Cambridge, MA, USA, 2019; pp. 121–125. Available online: https://www.sciencedirect.com/science/article/pii/B9780128170687000148 (accessed on 4 January 2024).
- Orgel, J.P.R.O.; Antonio, J.D.S.; Antipova, O. Molecular and structural mapping of collagen fibril interactions. Connect. Tissue Res. 2011, 52, 2–17. [Google Scholar] [CrossRef] [PubMed]
- Okuyama, K. Revisiting the Molecular Structure of Collagen. Connect. Tissue Res. 2008, 49, 299–310. [Google Scholar] [CrossRef]
- Jafari, H.; Lista, A.; Siekapen, M.M.; Ghaffari-Bohlouli, P.; Nie, L.; Alimoradi, H.; Shavandi, A. Fish Collagen: Extraction, Characterization, and Applications for Biomaterials Engineering. Polymers 2020, 12, 2230. [Google Scholar] [CrossRef]
- Silvipriya, K.S.; Kumar, K.K.; Bhat, A.R.; Kumar, B.D.; John, A.; Lakshmanan, P. Collagen: Animal sources and biomedical application. J. Appl. Pharm. Sci. 2015, 5, 123–127. [Google Scholar] [CrossRef]
- Wang, H. A Review of the Effects of Collagen Treatment in Clinical Studies. Polymers 2021, 13, 3868. [Google Scholar] [CrossRef]
- Collier, T.A.; Nash, A.; Birch, H.L.; De Leeuw, N.H. Effect on the mechanical properties of type I collagen of intra-molecular lysine-arginine derived advanced glycation end-product cross-linking. J. Biomech. 2017, 67, 55–61. [Google Scholar] [CrossRef]
- Chang, S.W.; Buehler, M.J. Molecular biomechanics of collagen molecules. Mater. Today 2014, 17, 70–76. [Google Scholar] [CrossRef]
- Reilly, D.M.; Lozano, J. Skin collagen through the lifestages: Importance for skin health and beauty. Plast. Aesthetic Res. 2021, 8, 231801211. [Google Scholar] [CrossRef]
- Sibilla, S.; Godfrey, M.; Brewer, S.; Budh-Raja, A.; Genovese, L. An overview of the beneficial effects of hydrolysed collagen as a nutraceutical on skin properties: Scientific background and clinical studies. Open Nutraceuticals J. 2015, 8, 29–42. [Google Scholar] [CrossRef]
- Li, G.Y.; Fukunaga, S.; Takenouchi, K.; Nakamura, F. Comparative study of the physiological properties of collagen, gelatin and collagen hydrolysate as cosmetic materials. Int. J. Cosmet. Sci. 2005, 27, 101–106. [Google Scholar] [CrossRef] [PubMed]
- Calleja-Agius, J.; Brincat, M.; Borg, M. Skin connective tissue and ageing. Best Pr. Res. Clin. Obs. Gynaecol. 2013, 27, 727–740. [Google Scholar] [CrossRef]
- Shekhter, A.B.; Fayzullin, A.L.; Vukolova, M.N.; Rudenko, T.G.; Osipycheva, V.D.; Litvitsky, P.F. Medical Applications of Collagen and Collagen-Based Materials. Curr. Med. Chem. 2017, 26, 506–516. [Google Scholar] [CrossRef]
- Asserin, J.; Lati, E.; Shioya, T.; Prawitt, J. The effect of oral collagen peptide supplementation on skin moisture and the dermal collagen network: Eevidence from an ex vivo model and randomized, placebo-controlled clinical trials. J. Cosmet. Dermatol. 2015, 14, 291–301. [Google Scholar] [CrossRef]
- Inoue, N.; Sugihara, F.; Wang, X. Ingestion of bioactive collagen hydrolysates enhance facial skin moisture and elasticity and reduce facial ageing signs in a randomised double-blind placebo-controlled clinical study. J. Sci. Food Agric. 2016, 96, 4077–4081. [Google Scholar] [CrossRef]
- Davison-Kotler, E.; Marshall, W.S.; García-Gareta, E. Sources of collagen for biomaterials in skin wound healing. Bioengineering 2019, 6, 56. [Google Scholar] [CrossRef]
- Dong, C.; Lv, Y. Application of collagen scaffold in tissue engineering: Recent advances and new perspectives. Polymers 2016, 8, 42. [Google Scholar] [CrossRef]
- Shimizu, J.; Asami, N.; Kataoka, A.; Sugihara, F.; Inoue, N.; Kimira, Y.; Wada, M.; Mano, H. Oral collagen-derived dipeptides, prolyl-hydroxyproline and hydroxyprolyl-glycine, ameliorate skin barrier dysfunction and alter gene expression profiles in the skin. Biochem. Biophys. Res. Commun. 2015, 456, 626–630. [Google Scholar] [CrossRef]
- Chung, J.H.; Seo, J.Y.; Choi, H.R.; Lee, M.K.; Youn, C.S.; Rhie, G.-E.; Cho, K.H.; Kim, K.H.; Park, K.C.; Eun, H.C. Modulation of skin collagen metabolism in aged and photoaged human skin in vivo. J. Investig. Dermatol. 2001, 117, 1218–1224. [Google Scholar] [CrossRef] [PubMed]
- Bansode, S.; Bashtanova, U.; Li, R.; Clark, J.; Müller, K.H.; Puszkarska, A.; Goldberga, I.; Chetwood, H.H.; Reid, D.G.; Colwell, L.J.; et al. Glycation changes molecular organization and charge distribution in type I collagen fibrils. Sci. Rep. 2020, 10, 1–13. [Google Scholar] [CrossRef]
- Chambers, E.S.; Vukmanovic-Stejic, M. Skin barrier immunity and ageing. Immunology 2020, 160, 116–125. [Google Scholar] [CrossRef]
- Mohania, D.; Chandel, S.; Kumar, P.; Verma, V.; Digvijay, K.; Tripathi, D.; Choudhury, K.; Mitten, S.K.; Shah, D. Ultraviolet radiations: Skin defense-damage mechanism. Adv. Exp. Med. Biol. 2017, 996, 71–87. [Google Scholar] [CrossRef]
- De Luca, C.; Mikhal’Chik, E.V.; Suprun, M.V.; Papacharalambous, M.; Truhanov, A.I.; Korkina, L.G. Skin antiageing and systemic Redox effects of supplementation with marine collagen peptides and plant-derived antioxidants: A single-blind case-control clinical study. Oxid. Med. Cell Longev. 2016, 2016, 4389410. [Google Scholar] [CrossRef]
- Cherim, M.; Mustafa, A.; Cadar, E.; Lupașcu, N.; Paris, S.; Sirbu, R. Collagen Sources and Areas of Use. Eur. J. Med. Nat. Sci. 2019, 2, 8–13. [Google Scholar] [CrossRef]
- Tu, Y.; Quan, T. Oxidative Stress and Human Skin Connective Tissue Aging. Cosmetics 2016, 3, 28. [Google Scholar] [CrossRef]
- Gromkowska-Kępka, K.J.; Puścion-Jakubik, A.; Markiewicz-Żukowska, R.; Socha, K. The impact of ultraviolet radiation on skin photoaging—Review of in vitro studies. J. Cosmet. Dermatol. 2021, 20, 3427–3431. [Google Scholar] [CrossRef] [PubMed]
- Yamauchi, M.; Sricholpech, M.; Terajima, M.; Tomer, K.B.; Perdivara, I. Glycosylation of Type I Collagen. Methods Mol. Biol. 2019, 1934, 127–144. [Google Scholar] [CrossRef]
- Hennet, T. Collagen glycosylation. Curr. Opin. Struct. Biol. 2019, 56, 131–138. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, M.; Koyama, Y.I.; Nomura, Y. Effects of collagen peptide ingestion on UV-B-induced skin damage. Biosci. Biotechnol. Biochem. 2009, 73, 930–932. [Google Scholar] [CrossRef] [PubMed]
- Oba, C.; Ohara, H.; Morifuji, M.; Ito, K.; Ichikawa, S.; Kawahata, K.; Koga, J. Collagen hydrolysate intake improves the loss of epidermal barrier function and skin elasticity induced by UVB irradiation in hairless mice. Photodermatol. Photoimmunol. Photomed. 2013, 29, 204–211. [Google Scholar] [CrossRef] [PubMed]
- Silveira, J.E.P.S.; Pedroso, D.M.M. UV light and skin aging. Rev. Environ. Health 2014, 29, 243–254. [Google Scholar] [CrossRef]
- Choi, S.Y.; Ko, E.J.; Lee, Y.H.; Kim, B.G.; Shin, H.J.; Seo, D.B.; Lee, S.J.; Kim, B.J.; Kim, M.N. Effects of collagen tripeptide supplement on skin properties: A prospective, randomized, controlled study. J. Cosmet. Laser Ther. 2014, 16, 132–137. [Google Scholar] [CrossRef]
- Evans, M.; Lewis, E.D.; Zakaria, N.; Pelipyagina, T.; Guthrie, N. A randomized, triple-blind, placebo-controlled, parallel study to evaluate the efficacy of a freshwater marine collagen on skin wrinkles and elasticity. J. Cosmet. Dermatol. 2021, 20, 825–834. [Google Scholar] [CrossRef]
- Añazco, C.; Riedelsberger, J.; Vega-Montoto, L.; Rojas, A. Exploring the Interplay between Polyphenols and Lysyl Oxidase Enzymes for Maintaining Extracellular Matrix Homeostasis. Int. J. Mol. Sci. 2023, 24, 10985. [Google Scholar] [CrossRef]
- Sionkowska, A.; Lewandowska, K.; Adamiak, K. The Influence of UV Light on Rheological Properties of Collagen Extracted from Silver Carp Skin. Materials 2020, 13, 4453. [Google Scholar] [CrossRef]
- Adamiak, K.; Sionkowska, A. The influence of UV irradiation on fish skin collagen films in the presence of xanthohumol and propanediol. Spectrochim. Acta Part A Mol. Biomol. Spectrosc. 2022, 282, 121652. [Google Scholar] [CrossRef]
- Song, H.H.; Hong, K.-B.; Kim, S.; Kim, B.-Y.; Shik, S.H.; Suh, H.J.; Ahn, Y. Effects of fish collagen on hairless mice skin photoaging induced by ultraviolet irradiation via regulation of the TGF-β signaling pathway Anti-photoaging effect of fish collagen in UVB-induced hairless mice. J. Funct. Foods 2023, 105, 105554. [Google Scholar] [CrossRef]
- Timorshina, S.; Popova, E.; Osmolovskiy, A. Sustainable Applications of Animal Waste Proteins. Polymers 2022, 14, 1601. [Google Scholar] [CrossRef]
- León-López, A.; Morales-Peñaloza, A.; Martínez-Juárez, V.M.; Vargas-Torres, A.; Zeugolis, D.I.; Aguirre-Álvarez, G. Hydrolyzed Collagen—Sources and Applications. Molecules 2019, 24, 4031. [Google Scholar] [CrossRef]
- Feng, B.; Yang, H.; Zhu, M.; Li, J.; Chang, H.-M.; Leung, P.C.K.; Guo, J.; Zhang, Y. Collagen-based biomaterials in organoid technology for reproductive medicine: Composition, characteristics, and applications. Collagen Leather 2023, 5, 1–26. [Google Scholar] [CrossRef]
- Coppola, D.; Oliviero, M.; Vitale, G.A.; Lauritano, C.; D’ambra, I.; Iannace, S.; de Pascale, D. Marine Collagen from Alternative and Sustainable Sources: Extraction, Processing and Applications. Mar. Drugs 2020, 18, 214. [Google Scholar] [CrossRef] [PubMed]
- Sotelo, C.G.; Comesaña, M.B.; Ariza, P.R.; Pérez-Martín, R.I. Characterization of Collagen from Different Discarded Fish Species of the West Coast of the Iberian Peninsula. J. Aquat. Food Prod. Technol. 2016, 25, 388–399. [Google Scholar] [CrossRef]
- Silva, T.H.; Moreira-Silva, J.; Marques, A.L.P.; Domingues, A.; Bayon, Y.; Reis, R.L. Marine origin collagens and its potential applications. Mar. Drugs 2014, 12, 5881–5901. [Google Scholar] [CrossRef] [PubMed]
- Mahboob, S. Isolation and characterization of collagen from fish waste material- skin, scales and fins of Catla catla and Cirrhinus mrigala. J. Food Sci. Technol. 2015, 52, 4296–4305. [Google Scholar] [CrossRef]
- Rodríguez, M.I.A.; Barroso, L.G.R.; Sánchez, M.L. Collagen: A review on its sources and potential cosmetic applications. J. Cosmet. Dermatol. 2018, 17, 20–26. [Google Scholar] [CrossRef]
- Prokopová, A.; Pavlačková, J.; Mokrejš, P.; Gál, R.; Marrocchi, A.; Marconi, O. Collagen Hydrolysate Prepared from Chicken By-Product as a Functional Polymer in Cosmetic Formulation. Molecules 2021, 26, 2021. [Google Scholar] [CrossRef] [PubMed]
- Bernat, M.; Matysek-Nawrocka, M.; Cioczek, W.; Społecznych, W.N.; Medycznych, N.; Nauk, W.S. Składniki aktywne w kosmetykach przeciwstarzeniowych Active agents in anti-aging cosmetics. Kosmetol. Estet. 2016, 5, 575–579. [Google Scholar]
- Żelaszczyk, D.; Waszkielewicz, A.; Marona, H. Kolagen—Struktura oraz zastosowanie w kosmetologii i medycynie estetycznej. Estetologia Med. Kosmetol. 2012, 2, 14–20. [Google Scholar] [CrossRef]
- Prokopowicz, M.; Różycki, K.M. News, and Undefined 2017. Innovation in Cosmetics. Available online: https://bibliotekanauki.pl/articles/1179767.pdf (accessed on 4 January 2024).
- Hou, H.; Li, B.; Zhang, Z.; Xue, C.; Yu, G.; Wang, J.; Bao, Y.; Bu, L.; Sun, J.; Peng, Z.; et al. Moisture absorption and retention properties, and activity in alleviating skin photodamage of collagen polypeptide from marine fish skin. Food Chem. 2012, 135, 1432–1439. [Google Scholar] [CrossRef]
- Cohen, S.R.; Berner, C.F.; Busso, M.; Gleason, M.C.; Hamilton, D.; Holmes, R.E.; Romano, J.J.; Rullan, P.P.; Thaler, M.P.; Ubogy, Z.; et al. ArteFill: A long-lasting injectable wrinkle filler material—Summary of the U.S. Food and Drug Administration trials and a progress report on 4- to 5-year outcomes. Plast. Reconstr. Surg. 2006, 118, 64S–76S. [Google Scholar] [CrossRef] [PubMed]
- Bauman, L. CosmoDerm/CosmoPlast (Human Bioengineered Collagen) for the Aging Face. Facial Plast. Surg. 2004, 20, 125–128. [Google Scholar] [CrossRef]
- Baumann, L. Collagen-Containing Fillers: Alone and in Combination. Clin. Plast. Surg. 2006, 33, 587–596. [Google Scholar] [CrossRef]
- Watanabe-Kamiyama, M.; Shimizu, M.; Kamiyama, S.; Taguchi, Y.; Sone, H.; Morimatsu, F.; Shirakawa, H.; Furukawa, Y.; Komai, M. Absorption and effectiveness of orally administered low molecular weight collagen hydrolysate in rats. J. Agric. Food Chem. 2010, 58, 835–841. [Google Scholar] [CrossRef] [PubMed]
- Yoon, H.S.; Cho, H.H.; Cho, S.; Lee, S.R.; Shin, M.H.; Chung, J.H. Supplementating with dietary astaxanthin combined with collagen hydrolysate improves facial elasticity and decreases matrix metalloproteinase-1 and -12 expression: A comparative study with placebo. J. Med. Food 2014, 17, 810–816. [Google Scholar] [CrossRef] [PubMed]
- Baumann, L.; Kaufman, J.; Saghari, S. Collagen fillers. Dermatol. Ther. 2006, 19, 134–140. [Google Scholar] [CrossRef]
- Proksch, E.; Segger, D.; Degwert, J.; Schunck, M.; Zague, V.; Oesser, S. Oral supplementation of specific collagen peptides has beneficial effects on human skin physiology: A double-blind, placebo-controlled study. Ski. Pharmacol. Physiol. 2013, 27, 47–55. [Google Scholar] [CrossRef]
- Proksch, E.; Schunck, M.; Zague, V.; Segger, D.; Degwert, J.; Oesser, S. Oral intake of specific bioactive collagen peptides reduces skin wrinkles and increases dermal matrix synthesis. Skin Pharmacol. Physiol. 2014, 27, 113–119. [Google Scholar] [CrossRef]
- Addor, F.A.S.; Vieira, J.C.; Melo, C.S.A. Improvement of dermal parameters in aged skin after oral use of a nutrient supplement. Clin. Cosmet. Investig. Dermatol. 2018, 11, 195–201. [Google Scholar] [CrossRef]
- Ciszek, A. Variability of skin pH after the use of different collagen gels. J. Cosmet. Dermatol. 2017, 16, 531–536. [Google Scholar] [CrossRef]
- Luebberding, S.; Krueger, N.; Kerscher, M. Skin physiology in men and women: In vivo evaluation of 300 people including TEWL, SC hydration, sebum content and skin surface pH. Int. J. Cosmet. Sci. 2013, 35, 477–483. [Google Scholar] [CrossRef] [PubMed]
- Lubart, R.; Yariv, I.; Fixler, D.; Lipovsky, A. A Novel Facial Cream Based on Skin-penetrable Fibrillar Collagen Microparticles. J. Clin. Aesthet. Dermatol. 2022, 15, 59–64. [Google Scholar] [PubMed]
- Lehmann, K.M. Skin care of atopic dermatitis in a beauty salon. Aesthetic Cosmetol. Med. 2022, 11, 87–90. [Google Scholar] [CrossRef]
- Aust, M.C.; Fernandes, D.; Kolokythas, P.; Kaplan, H.M.; Vogt, P.M. Percutaneous collagen induction therapy: An alternative treatment for scars, wrinkles, and skin laxity. Plast. Reconstr. Surg. 2008, 121, 1421–1429. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.I.; Lee, S.G.; Jung, I.; Suk, J.; Lee, M.-H.; Kim, D.-U.; Lee, J.H. Effect of a Topical Collagen Tripeptide on Antiaging and Inhibition of Glycation of the Skin: A Pilot Study. Int. J. Mol. Sci. 2022, 23, 1101. [Google Scholar] [CrossRef]





| Type | Structure | Localization | Function |
|---|---|---|---|
| I | Triple superhelix composed of two identical α1 and one α2 chain; a form consisting of three α1 chains (homotrimeric) is also found | Bones, tendons, ligaments, skin, cornea | Tensile strength of tissues and bone stiffness |
| II | Three identical α1[III]3 chains—homotrimer; similar properties and size to type I, but higher content of hydroxylysine and glucose and galactose residues | The dominant component of vitreous tissue (approx. 80%), corneal epithelium, and cartilage | One of the main components of ECM (extracellular matrix), maintains chondrocyte functions, induces cell adhesion and proliferation |
| III | Three identical α1[III]3 chains | Element of the dermis, liver and lung tissues, spleen and blood vessels | Gives elasticity to tissues |
| V | Three different chains—heterotrimers | Bones, skin, placenta, cornea | Initiation of collagen fibrillogenesis |
| XI | Three different chains—heterotrimers | Cartilage, intervertebral discs | Initiation of collagen fibrillogenesis |
| XXIV | The fragment of the Gly-Xaa-Yaa repeated sequence is relatively short, constitutes approximal | Bones, cornea | A marker of osteoblast differentiation and bone formation in mice |
| XXVII | Forms non-striated, thread-like structures, unlike other members of the subfamily | Cartilage | Deposited mainly in skeletal tissues at the junction of cartilage and bone |
| Collagen | Type | Localization |
|---|---|---|
| Basement membrane | IV | Basement membranes, capillaries |
| Forming microfibers | XVI | Bones, vessels, skin, cornea, cartilage |
| XXVIII | Cells of the nervous system | |
| XXIX | Skin | |
| Anchoring | VII | Mucosa, skin, bladder, umbilical cord, amnion |
| Forming hexagonal lattice systems | VIII | Mucosa, skin, bladder, umbilical cord, amnion |
| X | Cartilage | |
| FACITs type | IX | Cornea, vitreous body, cartilage |
| XII | Cartilage, tendons, skin | |
| XIV | Vessels, eye, nerves, tendons, bones, skin, cartilage | |
| XVI | Heart, smooth muscles, skin, kidney | |
| XIX | Band of basement membranes in skeletal muscles, skin, kidneys, liver, placenta, spleen, prostate | |
| XX | Corneal epithelium | |
| XXI | Stomach, kidneys, vessels, heart, placenta, skeletal muscles | |
| XXII | Tissue connections | |
| XXVI | Testicles, ovaries | |
| MACITs type | XII | Skeletal muscles, heart, eye, skin, endothelial cells |
| XVII | Skin | |
| XXIII | Metastatic carcinogenic cells | |
| XXV | Eye, brain, heart, testicles | |
| MULTIPLEXINs type | X | Capillaries, ovaries, heart, testicles, skin, placenta, kidneys |
| XVIII | Kidney, lungs, liver |
| Place of Action | Effect of Supplementation |
|---|---|
| Immune system | Inhibition of inflammatory processes resulting from autoimmunity. |
| Hormone system | Amino acids included in collagen may be involved in the production of hormones and neurotransmitters, e.g., GABA. |
| Cartilage and skeletal system | Increased production of collagen in cartilage—improved resistance to mechanical loads, reduction in joint pain and joint inflammation, stimulation of the production of synovial fluid. |
| Skin | Bioactive short peptides (dipeptide glycine—hydroxyproline) send signals to fibroblasts, stimulating the collagen production process, reducing wrinkles, improving the smoothness, tension, and elasticity of the skin, reducing cellulite and stretch marks by improving the elasticity and cohesion of the skin. |
| Hair, nails | Preventing graying and hair loss and brittle nails. |
| Liver | Assistance in the removal of toxic substances and alcohol metabolites. |
| Muscle | Increase in muscle mass, increased energy efficiency of the body. |
| Circulatory system | Amino acids contained in collagen, such as proline and lysine, prevent the accumulation of fats in the walls of arteries—protection of the circulatory system. |
| Digestive system | The amino acids proline and glycine seal the walls of the small intestine; collagen helps absorb water in the intestines. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jadach, B.; Mielcarek, Z.; Osmałek, T. Use of Collagen in Cosmetic Products. Curr. Issues Mol. Biol. 2024, 46, 2043-2070. https://doi.org/10.3390/cimb46030132
Jadach B, Mielcarek Z, Osmałek T. Use of Collagen in Cosmetic Products. Current Issues in Molecular Biology. 2024; 46(3):2043-2070. https://doi.org/10.3390/cimb46030132
Chicago/Turabian StyleJadach, Barbara, Zofia Mielcarek, and Tomasz Osmałek. 2024. "Use of Collagen in Cosmetic Products" Current Issues in Molecular Biology 46, no. 3: 2043-2070. https://doi.org/10.3390/cimb46030132
APA StyleJadach, B., Mielcarek, Z., & Osmałek, T. (2024). Use of Collagen in Cosmetic Products. Current Issues in Molecular Biology, 46(3), 2043-2070. https://doi.org/10.3390/cimb46030132







