Anticoagulation in the Elderly
Abstract
:1. Introduction
2. General Indications for Anticoagulation
2.1. Venous Thromboembolism (VTE) Prophylaxis
2.2. Venous Thromboembolism (VTE) Treatment
2.3. Atrial Fibrillation (AF)
| CHADS2 score* | Stroke rate per 100 patient-years (95% CI) |
|---|---|
| 0 | 1.9 (1.2-3.0) |
| 1 | 2.8 (2.0-3.8) |
| 2 | 4.0 (3.1-5.1) |
| 3 | 5.9 (4.6-7.3) |
| 4 | 8.5 (6.3-11.1) |
| 5 | 12.5 (8.2-17.5) |
| 6 | 18.2 (10.5-27.4) |
| CHA2DS2-VASc score** | Stroke or other thromboembolism rate per 100 patients-years (95% CI) |
| 0 | 0 (0-0) |
| 1 | 0.6 (0.0-3.4) |
| 2 | 1.6 (0.3-4.7) |
| 3 | 3.9 (1.7-7.6) |
| 4 | 1.9 (0.5-4.9) |
| 5 | 3.2 (0.7-9.0) |
| 6 | 3.6 (0.4-12.3) |
| 7 | 8.0 (1.0-26.0) |
| 8 | 11.1 (0.3-48.3) |
| 9 | 100 (2.5-100) |
2.4. Valvular Heart Disease
3. Specific Considerations in the Elderly
3.1. Comorbidities and Co-Medication
3.2. Pharmacokinetics in the Elderly
3.3. Pharmacodynamics in the Elderly
3.4. Risk of Falls
3.5. Hemorrhagic Risk
4. Different Well Established Anticoagulant Options
4.1. Unfractionated Heparin (UFH)
| RIETE bleeding score * | Major bleeding per 100 patients within 3 months of anticoagulant therapy (95% CI) |
|---|---|
| 0 | 0.3 (0.1-0.6) |
| 1-4 | 2.6 (2.3-2.9) |
| >4 | 7.3 (5.6-9.3) |
| HEMORR2HAGES score ** | Major bleeding per 100 person-years (95% CI) |
| 0 | 1.9 (0.6-4.4) |
| 1 | 2.5 (1.3-4.3) |
| 2 | 5.3 (3.4-8.1) |
| 3 | 8.4 (4.9-13.6) |
| 4 | 10.4 (5.1-18.9) |
| ≥5 | 12.3 (5.8-23.1) |
| Any score | 4.9 (3.9-6.3) |
4.2. Low Molecular Weight Heparins (LMWH)
| Creatinine clearance (CrCl) | Prophylactic anticoagulation | Therapeutic anticoagulation |
|---|---|---|
| >50 mL/min |
|
|
| 30-50 mL/min |
|
|
| <30 mL/min |
|
|
4.3. Synthetic Pentasaccharides (Fondaparinux, Idraparinux)
4.4. Vitamin K Antagonists (VKA)
5. Newer Anticoagulants
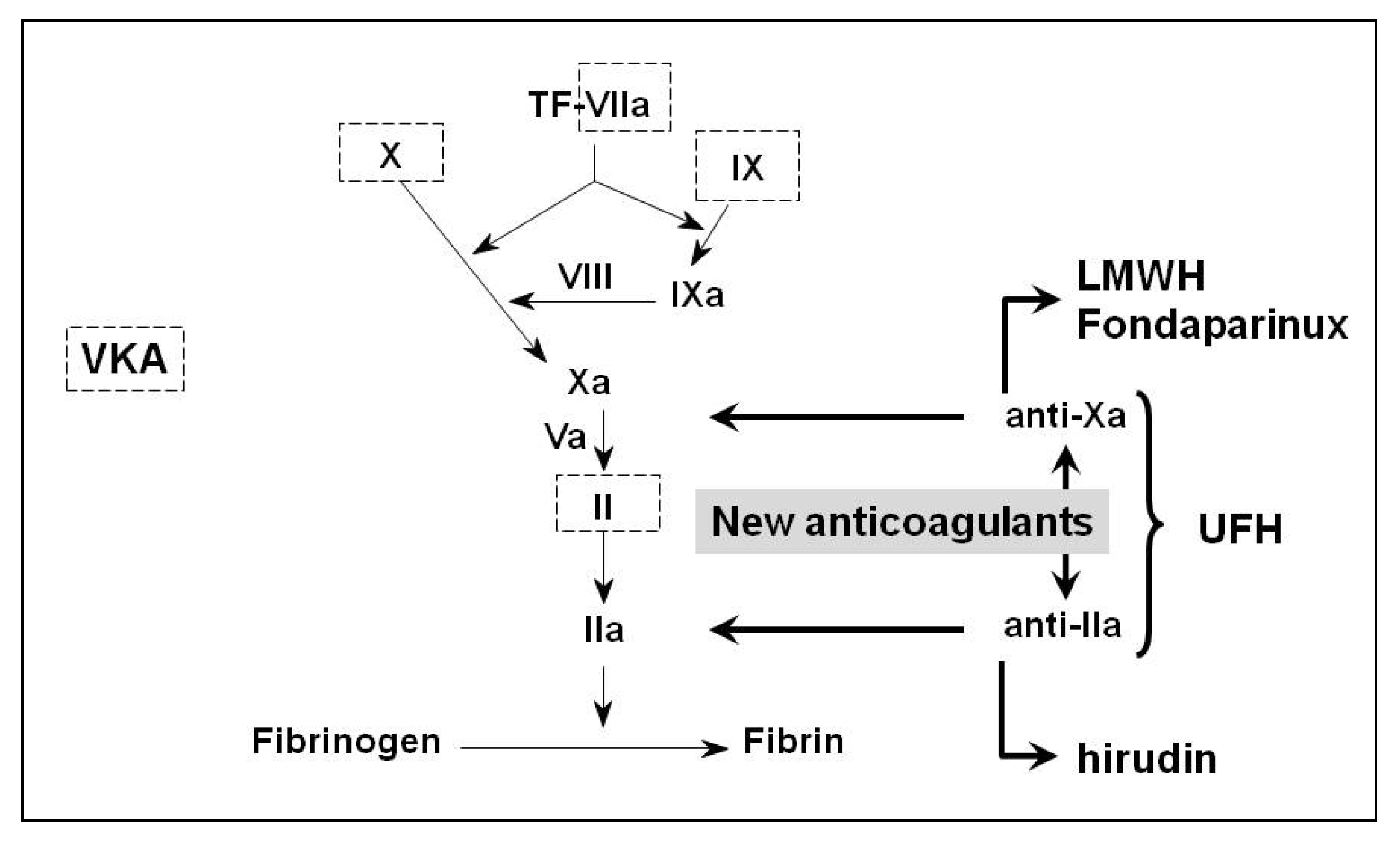
5.1. Direct Thrombin (Factor IIa) Inhibitors
| Characteristics | Dabigatran etexilate | Rivaroxaban | Apixaban |
|---|---|---|---|
| Target | Thrombin (factor IIa) | Factor Xa | Factor Xa |
| Dosing pattern (therapeutic anticoagulation) | Fixed, b.i.d. | Fixed, o.d. | Fixed, b.i.d. |
| Monitoring necessary | No | No | No |
| Prodrug | Yes | No | No |
| Bioavailability (%) | 6 | >80 | 50 |
| Half-life (hours) | 14–17 | 5–13 | 8-15 |
| Clearance | 80% renal 20% biliary | 1/3 renal: unchanged 1/3 renal: inactive 1/3 biliary | 25% renal |
5.2. Direct Factor Xa Inhibitors
6. Conclusions
References
- Go, A.S.; Hylek, E.M.; Phillips, K.A.; Chang, Y.; Henault, L.E.; Selby, J.V.; Singer, D.E. Prevalence of diagnosed atrial fibrillation in adults: national implications for rhythm management and stroke prevention: the AnTicoagulation and Risk Factors in Atrial Fibrillation (ATRIA) Study. JAMA 2001, 285, 2370–2375. [Google Scholar]
- Naess, I.A.; Christiansen, S.C.; Romundstad, P.; Cannegieter, S.C.; Rosendaal, F.R.; Hammerstrom, J. Incidence and mortality of venous thrombosis: a population-based study. J. Thromb. Haemost. 2007, 5, 692–699. [Google Scholar]
- Di Minno, G.; Tufano, A. Challenges in the prevention of venous thromboembolism in the elderly. J. Thromb. Haemost. 2004, 2, 1292–1298. [Google Scholar]
- Brotman, D.J.; Jaffer, A.K. Prevention of venous thromboembolism in the geriatric patient. Cardiol. Clin. 2008, 26, 221–234, vi. [Google Scholar]
- Weill-Engerer, S.; Meaume, S.; Lahlou, A.; Piette, F.; Saint-Jean, O.; Sachet, A.; Beinis, J.Y.; Gallinari, C.; Grancher, A.S.; Vincent, J.P.; Naga, H.; Belmin, J.; Salvatore, R.; Kazes, M.; Pautas, E.; Boiffin, A.; Piera, J.B.; Duviquet, M.; Knafo, D.; Piau, A.; Miric, D.; Jean, A.; Bellamy, V.; Tissandier, O.; Le Blanche, A.F. Risk factors for deep vein thrombosis in inpatients aged 65 and older: a case-control multicenter study. J. Am. Geriatr. Soc. 2004, 52, 1299–1304. [Google Scholar]
- Bosson, J.L.; Labarere, J.; Sevestre, M.A.; Belmin, J.; Beyssier, L.; Elias, A.; Franco, A.; Le Roux, P. Deep vein thrombosis in elderly patients hospitalized in subacute care facilities: a multicenter cross-sectional study of risk factors, prophylaxis, and prevalence. Arch. Intern. Med. 2003, 163, 2613–2618. [Google Scholar]
- White, R.H.; Zhou, H.; Gage, B.F. Effect of age on the incidence of venous thromboembolism after major surgery. J. Thromb. Haemost. 2004, 2, 1327–1333. [Google Scholar]
- Geerts, W.H.; Bergqvist, D.; Pineo, G.F.; Heit, J.A.; Samama, C.M.; Lassen, M.R.; Colwell, C.W. Prevention of venous thromboembolism: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest 2008, 133, 381S–453S. [Google Scholar]
- Kearon, C.; Kahn, S.R.; Agnelli, G.; Goldhaber, S.; Raskob, G.E.; Comerota, A.J. Antithrombotic therapy for venous thromboembolic disease: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest 2008, 133, 454S–545S. [Google Scholar]
- Monreal, M.; Lopez-Jimenez, L. Pulmonary embolism in patients over 90 years of age. Curr. Opin. Pulm. Med. 2010, 16, 432–436. [Google Scholar]
- Levine, M.N.; Hirsh, J.; Gent, M.; Turpie, A.G.; Weitz, J.; Ginsberg, J.; Geerts, W.; LeClerc, J.; Neemeh, J.; Powers, P.; et al. Optimal duration of oral anticoagulant therapy: a randomized trial comparing four weeks with three months of warfarin in patients with proximal deep vein thrombosis. Thromb. Haemost. 1995, 74, 606–611. [Google Scholar]
- Schulman, S.; Rhedin, A.S.; Lindmarker, P.; Carlsson, A.; Larfars, G.; Nicol, P.; Loogna, E.; Svensson, E.; Ljungberg, B.; Walter, H. A comparison of six weeks with six months of oral anticoagulant therapy after a first episode of venous thromboembolism. Duration of Anticoagulation Trial Study Group. N. Engl. J. Med. 1995, 332, 1661–1665. [Google Scholar]
- Lee, A.Y.; Levine, M.N.; Baker, R.I.; Bowden, C.; Kakkar, A.K.; Prins, M.; Rickles, F.R.; Julian, J.A.; Haley, S.; Kovacs, M.J.; Gent, M. Low-molecular-weight heparin versus a coumarin for the prevention of recurrent venous thromboembolism in patients with cancer. N. Engl. J. Med. 2003, 349, 146–153. [Google Scholar]
- Schulman, S.; Granqvist, S.; Holmstrom, M.; Carlsson, A.; Lindmarker, P.; Nicol, P.; Eklund, S.G.; Nordlander, S.; Larfars, G.; Leijd, B.; Linder, O.; Loogna, E. The duration of oral anticoagulant therapy after a second episode of venous thromboembolism. The Duration of Anticoagulation Trial Study Group. N. Engl. J. Med. 1997, 336, 393–398. [Google Scholar]
- Kearon, C.; Gent, M.; Hirsh, J.; Weitz, J.; Kovacs, M.J.; Anderson, D.R.; Turpie, A.G.; Green, D.; Ginsberg, J.S.; Wells, P.; MacKinnon, B.; Julian, J.A. A comparison of three months of anticoagulation with extended anticoagulation for a first episode of idiopathic venous thromboembolism. N. Engl. J. Med. 1999, 340, 901–907. [Google Scholar]
- Kearon, C.; Ginsberg, J.S.; Kovacs, M.J.; Anderson, D.R.; Wells, P.; Julian, J.A.; MacKinnon, B.; Weitz, J.I.; Crowther, M.A.; Dolan, S.; Turpie, A.G.; Geerts, W.; Solymoss, S.; van Nguyen, P.; Demers, C.; Kahn, S.R.; Kassis, J.; Rodger, M.; Hambleton, J.; Gent, M. Comparison of low-intensity warfarin therapy with conventional-intensity warfarin therapy for long-term prevention of recurrent venous thromboembolism. N. Engl. J. Med. 2003, 349, 631–639. [Google Scholar]
- Ridker, P.M. Long-term low-dose warfarin use is effective in the prevention of recurrent venous thromboembolism: yes. J. Thromb. Haemost. 2004, 2, 1034–1037. [Google Scholar]
- Wolf, P.A.; Abbott, R.D.; Kannel, W.B. Atrial fibrillation as an independent risk factor for stroke: the Framingham Study. Stroke 1991, 22, 983–988. [Google Scholar]
- Risk factors for stroke and efficacy of antithrombotic therapy in atrial fibrillation. Analysis of pooled data from five randomized controlled trials. Arch. Intern. Med. 1994, 154, 1449–1457.
- Fang, M.C.; Go, A.S.; Chang, Y.; Borowsky, L.; Pomernacki, N.K.; Singer, D.E. Comparison of risk stratification schemes to predict thromboembolism in people with nonvalvular atrial fibrillation. J. Am. Coll. Cardiol. 2008, 51, 810–815. [Google Scholar]
- Comparison of 12 risk stratification schemes to predict stroke in patients with nonvalvular atrial fibrillation. Stroke 2008, 39, 1901–1910.
- Gage, B.F.; Waterman, A.D.; Shannon, W.; Boechler, M.; Rich, M.W.; Radford, M.J. Validation of clinical classification schemes for predicting stroke: results from the National Registry of Atrial Fibrillation. JAMA 2001, 285, 2864–2870. [Google Scholar]
- Lip, G.Y.; Nieuwlaat, R.; Pisters, R.; Lane, D.A.; Crijns, H.J. Refining clinical risk stratification for predicting stroke and thromboembolism in atrial fibrillation using a novel risk factor-based approach: the euro heart survey on atrial fibrillation. Chest 2010, 137, 263–272. [Google Scholar]
- Singer, D.E.; Albers, G.W.; Dalen, J.E.; Fang, M.C.; Go, A.S.; Halperin, J.L.; Lip, G.Y.; Manning, W.J. Antithrombotic therapy in atrial fibrillation: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest 2008, 133, 546S–592S. [Google Scholar]
- Mant, J.; Hobbs, F.D.; Fletcher, K.; Roalfe, A.; Fitzmaurice, D.; Lip, G.Y.; Murray, E. Warfarin versus aspirin for stroke prevention in an elderly community population with atrial fibrillation (the Birmingham Atrial Fibrillation Treatment of the Aged Study, BAFTA): a randomised controlled trial. Lancet 2007, 370, 493–503. [Google Scholar]
- Zimetbaum, P.J.; Thosani, A.; Yu, H.T.; Xiong, Y.; Lin, J.; Kothawala, P.; Emons, M. Are atrial fibrillation patients receiving warfarin in accordance with stroke risk? Am. J. Med. 2010, 123, 446–453. [Google Scholar]
- Ogilvie, I.M.; Newton, N.; Welner, S.A.; Cowell, W.; Lip, G.Y. Underuse of oral anticoagulants in atrial fibrillation: a systematic review. Am. J. Med. 2010, 123, 638–645, e4. [Google Scholar]
- Tulner, L.R.; Van Campen, J.P.; Kuper, I.M.; Gijsen, G.J.; Koks, C.H.; Mac Gillavry, M.R.; van Tinteren, H.; Beijnen, J.H.; Brandjes, D.P. Reasons for undertreatment with oral anticoagulants in frail geriatric outpatients with atrial fibrillation: a prospective, descriptive study. Drugs Aging 2010, 27, 39–50. [Google Scholar]
- Baudet, E.M.; Puel, V.; McBride, J.T.; Grimaud, J.P.; Roques, F.; Clerc, F.; Roques, X.; Laborde, N. Long-term results of valve replacement with the St. Jude Medical prosthesis. J. Thorac. Cardiovasc. Surg. 1995, 109, 858–870. [Google Scholar]
- Salem, D.N.; O'Gara, P.T.; Madias, C.; Pauker, S.G. Valvular and structural heart disease: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest 2008, 133, 593S–629S. [Google Scholar]
- Mangoni, A.A.; Jackson, S.H. Age-related changes in pharmacokinetics and pharmacodynamics: basic principles and practical applications. Br. J. Clin. Pharmacol. 2004, 57, 6–14. [Google Scholar]
- Aymanns, C.; Keller, F.; Maus, S.; Hartmann, B.; Czock, D. Review on pharmacokinetics and pharmacodynamics and the aging kidney. Clin. J. Am. Soc. Nephrol. 2010, 5, 314–327. [Google Scholar]
- Lindeman, R.D.; Tobin, J.; Shock, N.W. Longitudinal studies on the rate of decline in renal function with age. J. Am. Geriatr. Soc. 1985, 33, 278–285. [Google Scholar]
- Schwartz, J.B. The current state of knowledge on age, sex, and their interactions on clinical pharmacology. Clin. Pharmacol. Ther. 2007, 82, 87–96. [Google Scholar]
- Spruill, W.J.; Wade, W.E.; Cobb, H.H., 3rd. Continuing the use of the Cockcroft-Gault equation for drug dosing in patients with impaired renal function. Clin. Pharmacol. Ther. 2009, 86, 468–470. [Google Scholar]
- Pautas, E.; Moreau, C.; Gouin-Thibault, I.; Golmard, J.L.; Mahe, I.; Legendre, C.; Taillandier-Heriche, E.; Durand-Gasselin, B.; Houllier, A.M.; Verrier, P.; Beaune, P.; Loriot, M.A.; Siguret, V. Genetic factors (VKORC1, CYP2C9, EPHX1, and CYP4F2) are predictor variables for warfarin response in very elderly, frail inpatients. Clin. Pharmacol. Ther. 2010, 87, 57–64. [Google Scholar]
- Mallet, L.; Spinewine, A.; Huang, A. The challenge of managing drug interactions in elderly people. Lancet 2007, 370, 185–191. [Google Scholar]
- Hirsh, J.; Bauer, K.A.; Donati, M.B.; Gould, M.; Samama, M.M.; Weitz, J.I. Parenteral anticoagulants: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest 2008, 133, 141S–159S. [Google Scholar]
- Jacobs, L.G. Warfarin pharmacology, clinical management, and evaluation of hemorrhagic risk for the elderly. Cardiol. Clin. 2008, 26, 157–167, v. [Google Scholar]
- Gage, B.F.; Birman-Deych, E.; Kerzner, R.; Radford, M.J.; Nilasena, D.S.; Rich, M.W. Incidence of intracranial hemorrhage in patients with atrial fibrillation who are prone to fall. Am. J. Med. 2005, 118, 612–617. [Google Scholar]
- Schulman, S.; Beyth, R.J.; Kearon, C.; Levine, M.N. Hemorrhagic complications of anticoagulant and thrombolytic treatment: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest 2008, 133, 257S–298S. [Google Scholar]
- Ruiz-Gimenez, N.; Suarez, C.; Gonzalez, R.; Nieto, J.A.; Todoli, J.A.; Samperiz, A.L.; Monreal, M. Predictive variables for major bleeding events in patients presenting with documented acute venous thromboembolism. Findings from the RIETE Registry. Thromb. Haemost. 2008, 100, 26–31. [Google Scholar]
- Gage, B.F.; Yan, Y.; Milligan, P.E.; Waterman, A.D.; Culverhouse, R.; Rich, M.W.; Radford, M.J. Clinical classification schemes for predicting hemorrhage: results from the National Registry of Atrial Fibrillation (NRAF). Am. Heart J. 2006, 151, 713–719. [Google Scholar]
- Kagansky, N.; Knobler, H.; Rimon, E.; Ozer, Z.; Levy, S. Safety of anticoagulation therapy in well-informed older patients. Arch. Intern. Med. 2004, 164, 2044–2050. [Google Scholar]
- Bounameaux, H. The novel anticoagulants: entering a new era. Swiss Med. Wkly. 2009, 139, 60–64. [Google Scholar]
- Hirsh, J. Heparin. N. Engl. J. Med. 1991, 324, 1565–1574. [Google Scholar]
- Greinacher, A. Heparin-induced thrombocytopenia. J. Thromb. Haemost. 2009, 7 Suppl. 1, 9–12. [Google Scholar]
- Kleber, F.X.; Witt, C.; Vogel, G.; Koppenhagen, K.; Schomaker, U.; Flosbach, C.W. Randomized comparison of enoxaparin with unfractionated heparin for the prevention of venous thromboembolism in medical patients with heart failure or severe respiratory disease. Am. Heart J. 2003, 145, 614–621. [Google Scholar]
- Campbell, N.R.; Hull, R.D.; Brant, R.; Hogan, D.B.; Pineo, G.F.; Raskob, G.E. Aging and heparin-related bleeding. Arch. Intern. Med. 1996, 156, 857–860. [Google Scholar]
- Samama, M.M.; Cohen, A.T.; Darmon, J.Y.; Desjardins, L.; Eldor, A.; Janbon, C.; Leizorovicz, A.; Nguyen, H.; Olsson, C.G.; Turpie, A.G.; Weisslinger, N. A comparison of enoxaparin with placebo for the prevention of venous thromboembolism in acutely ill medical patients. Prophylaxis in Medical Patients with Enoxaparin Study Group. N. Engl. J. Med. 1999, 341, 793–800. [Google Scholar]
- Alikhan, R.; Cohen, A.T.; Combe, S.; Samama, M.M.; Desjardins, L.; Eldor, A.; Janbon, C.; Leizorovicz, A.; Olsson, C.G.; Turpie, A.G. Prevention of venous thromboembolism in medical patients with enoxaparin: a subgroup analysis of the MEDENOX study. Blood Coagul. Fibrinolysis 2003, 14, 341–346. [Google Scholar]
- Kucher, N.; Leizorovicz, A.; Vaitkus, P.T.; Cohen, A.T.; Turpie, A.G.; Olsson, C.G.; Goldhaber, S.Z. Efficacy and safety of fixed low-dose dalteparin in preventing venous thromboembolism among obese or elderly hospitalized patients: a subgroup analysis of the PREVENT trial. Arch. Intern. Med. 2005, 165, 341–345. [Google Scholar]
- van Dongen, C.J.; van den Belt, A.G.; Prins, M.H.; Lensing, A.W. Fixed dose subcutaneous low molecular weight heparins versus adjusted dose unfractionated heparin for venous thromboembolism. Cochrane Database Syst. Rev. 2004, CD001100. [Google Scholar]
- Mismetti, P.; Laporte-Simitsidis, S.; Navarro, C.; Sie, P.; d'Azemar, P.; Necciari, J.; Duret, J.P.; Gaud, C.; Decousus, H.; Boneu, B. Aging and venous thromboembolism influence the pharmacodynamics of the anti-factor Xa and anti-thrombin activities of a low molecular weight heparin (nadroparin). Thromb. Haemost. 1998, 79, 1162–1165. [Google Scholar]
- Nagge, J.; Crowther, M.; Hirsh, J. Is impaired renal function a contraindication to the use of low-molecular-weight heparin? Arch. Intern. Med. 2002, 162, 2605–2609. [Google Scholar]
- Lim, W.; Dentali, F.; Eikelboom, J.W.; Crowther, M.A. Meta-analysis: low-molecular-weight heparin and bleeding in patients with severe renal insufficiency. Ann. Intern. Med. 2006, 144, 673–684. [Google Scholar]
- Mahe, I.; Gouin-Thibault, I.; Drouet, L.; Simoneau, G.; Di Castillo, H.; Siguret, V.; Bergmann, J.F.; Pautas, E. Elderly medical patients treated with prophylactic dosages of enoxaparin: influence of renal function on anti-Xa activity level. Drugs Aging 2007, 24, 63–71. [Google Scholar]
- Mahe, I.; Aghassarian, M.; Drouet, L.; Bal Dit-Sollier, C.; Lacut, K.; Heilmann, J.J.; Mottier, D.; Bergmann, J.F. Tinzaparin and enoxaparin given at prophylactic dose for eight days in medical elderly patients with impaired renal function: a comparative pharmacokinetic study. Thromb. Haemost. 2007, 97, 581–586. [Google Scholar]
- Samama, M.M.; Gerotziafas, G.T. Evaluation of the pharmacological properties and clinical results of the synthetic pentasaccharide (fondaparinux). Thromb. Res. 2003, 109, 1–11. [Google Scholar]
- Bijsterveld, N.R.; Moons, A.H.; Boekholdt, S.M.; van Aken, B.E.; Fennema, H.; Peters, R.J.; Meijers, J.C.; Buller, H.R.; Levi, M. Ability of recombinant factor VIIa to reverse the anticoagulant effect of the pentasaccharide fondaparinux in healthy volunteers. Circulation 2002, 106, 2550–2554. [Google Scholar]
- Cohen, A.T.; Davidson, B.L.; Gallus, A.S.; Lassen, M.R.; Prins, M.H.; Tomkowski, W.; Turpie, A.G.; Egberts, J.F.; Lensing, A.W. Efficacy and safety of fondaparinux for the prevention of venous thromboembolism in older acute medical patients: randomised placebo controlled trial. BMJ 2006, 332, 325–329. [Google Scholar]
- Lassen, M.R.; Bauer, K.A.; Eriksson, B.I.; Turpie, A.G. Postoperative fondaparinux versus preoperative enoxaparin for prevention of venous thromboembolism in elective hip-replacement surgery: a randomised double-blind comparison. Lancet 2002, 359, 1715–1720. [Google Scholar]
- Turpie, A.G.; Bauer, K.A.; Eriksson, B.I.; Lassen, M.R. Postoperative fondaparinux versus postoperative enoxaparin for prevention of venous thromboembolism after elective hip-replacement surgery: a randomised double-blind trial. Lancet 2002, 359, 1721–1726. [Google Scholar]
- Turpie, A.G.; Bauer, K.A.; Eriksson, B.I.; Lassen, M.R. Fondaparinux vs enoxaparin for the prevention of venous thromboembolism in major orthopedic surgery: a meta-analysis of 4 randomized double-blind studies. Arch. Intern. Med. 2002, 162, 1833–1840. [Google Scholar]
- Turpie, A.G.; Lensing, A.W.; Fuji, T.; Boyle, D.A. Pharmacokinetic and clinical data supporting the use of fondaparinux 1.5 mg once daily in the prevention of venous thromboembolism in renally impaired patients. Blood Coagul. Fibrinolysis 2009, 20, 114–121. [Google Scholar]
- Buller, H.R.; Davidson, B.L.; Decousus, H.; Gallus, A.; Gent, M.; Piovella, F.; Prins, M.H.; Raskob, G.; Segers, A.E.; Cariou, R.; Leeuwenkamp, O.; Lensing, A.W. Fondaparinux or enoxaparin for the initial treatment of symptomatic deep venous thrombosis: a randomized trial. Ann. Intern. Med. 2004, 140, 867–873. [Google Scholar]
- Buller, H.R.; Davidson, B.L.; Decousus, H.; Gallus, A.; Gent, M.; Piovella, F.; Prins, M.H.; Raskob, G.; van den Berg-Segers, A.E.; Cariou, R.; Leeuwenkamp, O.; Lensing, A.W. Subcutaneous fondaparinux versus intravenous unfractionated heparin in the initial treatment of pulmonary embolism. N. Engl. J. Med. 2003, 349, 1695–1702. [Google Scholar]
- Buller, H.R.; Cohen, A.T.; Davidson, B.; Decousus, H.; Gallus, A.S.; Gent, M.; Pillion, G.; Piovella, F.; Prins, M.H.; Raskob, G.E. Idraparinux versus standard therapy for venous thromboembolic disease. N. Engl. J. Med. 2007, 357, 1094–1104. [Google Scholar]
- Bousser, M.G.; Bouthier, J.; Buller, H.R.; Cohen, A.T.; Crijns, H.; Davidson, B.L.; Halperin, J.; Hankey, G.; Levy, S.; Pengo, V.; Prandoni, P.; Prins, M.H.; Tomkowski, W.; Torp-Pedersen, C.; Wyse, D.G. Comparison of idraparinux with vitamin K antagonists for prevention of thromboembolism in patients with atrial fibrillation: a randomised, open-label, non-inferiority trial. Lancet 2008, 371, 315–321. [Google Scholar]
- Paty, I.; Trellu, M.; Destors, J.M.; Cortez, P.; Boelle, E.; Sanderink, G. Reversibility of the anti-FXa activity of idrabiotaparinux (biotinylated idraparinux) by intravenous avidin infusion. J. Thromb. Haemost. 2010, 8, 722–729. [Google Scholar]
- Ansell, J.; Hirsh, J.; Hylek, E.; Jacobson, A.; Crowther, M.; Palareti, G. Pharmacology and management of the vitamin K antagonists: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest 2008, 133, 160S–198S. [Google Scholar]
- Siguret, V.; Gouin, I.; Debray, M.; Perret-Guillaume, C.; Boddaert, J.; Mahe, I.; Donval, V.; Seux, M.L.; Romain-Pilotaz, M.; Gisselbrecht, M.; Verny, M.; Pautas, E. Initiation of warfarin therapy in elderly medical inpatients: a safe and accurate regimen. Am. J. Med. 2005, 118, 137–142. [Google Scholar]
- Fang, M.C.; Go, A.S.; Hylek, E.M.; Chang, Y.; Henault, L.E.; Jensvold, N.G.; Singer, D.E. Age and the risk of warfarin-associated hemorrhage: the anticoagulation and risk factors in atrial fibrillation study. J. Am. Geriatr. Soc. 2006, 54, 1231–1236. [Google Scholar]
- Palareti, G.; Hirsh, J.; Legnani, C.; Manotti, C.; D'Angelo, A.; Pengo, V.; Moia, M.; Guazzaloca, G.; Musolesi, S.; Coccheri, S. Oral anticoagulation treatment in the elderly: a nested, prospective, case-control study. Arch. Intern. Med. 2000, 160, 470–478. [Google Scholar]
- Hylek, E.M.; Evans-Molina, C.; Shea, C.; Henault, L.E.; Regan, S. Major hemorrhage and tolerability of warfarin in the first year of therapy among elderly patients with atrial fibrillation. Circulation 2007, 115, 2689–2696. [Google Scholar]
- Shireman, T.I.; Mahnken, J.D.; Howard, P.A.; Kresowik, T.F.; Hou, Q.; Ellerbeck, E.F. Development of a contemporary bleeding risk model for elderly warfarin recipients. Chest 2006, 130, 1390–1396. [Google Scholar]
- Pisters, R.; Lane, D.A.; Nieuwlaat, R.; de Vos, C.B.; Crijns, H.J.; Lip, G.Y. A novel user-friendly score (HAS-BLED) to assess one-year risk of major bleeding in atrial fibrillation patients: The Euro Heart Survey. Chest 2010, 138, 1093–1100. [Google Scholar]
- Fang, M.C.; Chang, Y.; Hylek, E.M.; Rosand, J.; Greenberg, S.M.; Go, A.S.; Singer, D.E. Advanced age, anticoagulation intensity, and risk for intracranial hemorrhage among patients taking warfarin for atrial fibrillation. Ann. Intern. Med. 2004, 141, 745–752. [Google Scholar]
- Kimmel, S.E.; Chen, Z.; Price, M.; Parker, C.S.; Metlay, J.P.; Christie, J.D.; Brensinger, C.M.; Newcomb, C.W.; Samaha, F.F.; Gross, R. The influence of patient adherence on anticoagulation control with warfarin: results from the International Normalized Ratio Adherence and Genetics (IN-RANGE) Study. Arch. Intern. Med. 2007, 167, 229–235. [Google Scholar]
- Connolly, S.J.; Ezekowitz, M.D.; Yusuf, S.; Eikelboom, J.; Oldgren, J.; Parekh, A.; Pogue, J.; Reilly, P.A.; Themeles, E.; Varrone, J.; Wang, S.; Alings, M.; Xavier, D.; Zhu, J.; Diaz, R.; Lewis, B.S.; Darius, H.; Diener, H.C.; Joyner, C.D.; Wallentin, L. Dabigatran versus warfarin in patients with atrial fibrillation. N. Engl. J. Med. 2009, 361, 1139–1151. [Google Scholar]
- Man-Son-Hing, M.; Laupacis, A. Anticoagulant-related bleeding in older persons with atrial fibrillation: physicians' fears often unfounded. Arch. Intern. Med. 2003, 163, 1580–1586. [Google Scholar]
- Fiessinger, J.N.; Huisman, M.V.; Davidson, B.L.; Bounameaux, H.; Francis, C.W.; Eriksson, H.; Lundstrom, T.; Berkowitz, S.D.; Nystrom, P.; Thorsen, M.; Ginsberg, J.S. Ximelagatran vs low-molecular-weight heparin and warfarin for the treatment of deep vein thrombosis: a randomized trial. JAMA 2005, 293, 681–689. [Google Scholar]
- Testa, L.; Andreotti, F.; Biondi Zoccai, G.G.; Burzotta, F.; Bellocci, F.; Crea, F. Ximelagatran/melagatran against conventional anticoagulation: a meta-analysis based on 22,639 patients. Int. J. Cardiol. 2007, 122, 117–124. [Google Scholar]
- Mismetti, P.; Laporte, S. Dabigatran: clinical pharmacology. Ann. Fr. Anesth. Reanim. 2009, 28, S8–S14. [Google Scholar]
- Gross, P.L.; Weitz, J.I. New antithrombotic drugs. Clin. Pharmacol. Ther. 2009, 86, 139–146. [Google Scholar]
- Wolzt, M.; Levi, M.; Sarich, T.C.; Bostrom, S.L.; Eriksson, U.G.; Eriksson-Lepkowska, M.; Svensson, M.; Weitz, J.I.; Elg, M.; Wahlander, K. Effect of recombinant factor VIIa on melagatran-induced inhibition of thrombin generation and platelet activation in healthy volunteers. Thromb. Haemost. 2004, 91, 1090–1096. [Google Scholar]
- Eriksson, B.I.; Dahl, O.E.; Rosencher, N.; Kurth, A.A.; van Dijk, C.N.; Frostick, S.P.; Kalebo, P.; Christiansen, A.V.; Hantel, S.; Hettiarachchi, R.; Schnee, J.; Buller, H.R. Oral dabigatran etexilate vs. subcutaneous enoxaparin for the prevention of venous thromboembolism after total knee replacement: the RE-MODEL randomized trial. J. Thromb. Haemost. 2007, 5, 2178–2185. [Google Scholar]
- Eriksson, B.I.; Dahl, O.E.; Rosencher, N.; Kurth, A.A.; van Dijk, C.N.; Frostick, S.P.; Prins, M.H.; Hettiarachchi, R.; Hantel, S.; Schnee, J.; Buller, H.R. Dabigatran etexilate versus enoxaparin for prevention of venous thromboembolism after total hip replacement: a randomised, double-blind, non-inferiority trial. Lancet 2007, 370, 949–956. [Google Scholar]
- Ginsberg, J.S.; Davidson, B.L.; Comp, P.C.; Francis, C.W.; Friedman, R.J.; Huo, M.H.; Lieberman, J.R.; Muntz, J.E.; Raskob, G.E.; Clements, M.L.; Hantel, S.; Schnee, J.M.; Caprini, J.A. Oral thrombin inhibitor dabigatran etexilate vs North American enoxaparin regimen for prevention of venous thromboembolism after knee arthroplasty surgery. J. Arthroplasty 2009, 24, 1–9. [Google Scholar]
- Friedman, R.J.; Dahl, O.E.; Rosencher, N.; Caprini, J.A.; Kurth, A.A.; Francis, C.W.; Clemens, A.; Hantel, S.; Schnee, J.M.; Eriksson, B.I. Dabigatran versus enoxaparin for prevention of venous thromboembolism after hip or knee arthroplasty: a pooled analysis of three trials. Thromb. Res. 2010, 126, 175–182. [Google Scholar]
- Schulman, S.; Kearon, C.; Kakkar, A.K.; Mismetti, P.; Schellong, S.; Eriksson, H.; Baanstra, D.; Schnee, J.; Goldhaber, S.Z. Dabigatran versus warfarin in the treatment of acute venous thromboembolism. N. Engl. J. Med. 2009, 361, 2342–2352. [Google Scholar]
- Stangier, J. Clinical pharmacokinetics and pharmacodynamics of the oral direct thrombin inhibitor dabigatran etexilate. Clin. Pharmacokinet. 2008, 47, 285–295. [Google Scholar]
- Eriksson, B.I.; Borris, L.C.; Friedman, R.J.; Haas, S.; Huisman, M.V.; Kakkar, A.K.; Bandel, T.J.; Beckmann, H.; Muehlhofer, E.; Misselwitz, F.; Geerts, W. Rivaroxaban versus enoxaparin for thromboprophylaxis after hip arthroplasty. N. Engl. J. Med. 2008, 358, 2765–2775. [Google Scholar]
- Lassen, M.R.; Ageno, W.; Borris, L.C.; Lieberman, J.R.; Rosencher, N.; Bandel, T.J.; Misselwitz, F.; Turpie, A.G. Rivaroxaban versus enoxaparin for thromboprophylaxis after total knee arthroplasty. N. Engl. J. Med. 2008, 358, 2776–2786. [Google Scholar]
- Turpie, A.G.; Lassen, M.R.; Davidson, B.L.; Bauer, K.A.; Gent, M.; Kwong, L.M.; Cushner, F.D.; Lotke, P.A.; Berkowitz, S.D.; Bandel, T.J.; Benson, A.; Misselwitz, F.; Fisher, W.D. Rivaroxaban versus enoxaparin for thromboprophylaxis after total knee arthroplasty (RECORD4): a randomised trial. Lancet 2009, 373, 1673–1680. [Google Scholar]
© 2010 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Robert-Ebadi, H.; Righini, M. Anticoagulation in the Elderly. Pharmaceuticals 2010, 3, 3543-3569. https://doi.org/10.3390/ph3123543
Robert-Ebadi H, Righini M. Anticoagulation in the Elderly. Pharmaceuticals. 2010; 3(12):3543-3569. https://doi.org/10.3390/ph3123543
Chicago/Turabian StyleRobert-Ebadi, Helia, and Marc Righini. 2010. "Anticoagulation in the Elderly" Pharmaceuticals 3, no. 12: 3543-3569. https://doi.org/10.3390/ph3123543
APA StyleRobert-Ebadi, H., & Righini, M. (2010). Anticoagulation in the Elderly. Pharmaceuticals, 3(12), 3543-3569. https://doi.org/10.3390/ph3123543




