Evaluation of the Efficacy of OSU-2S in the Treatment of Non-Small-Cell Lung Cancer and Screening of Potential Targets of Action
Abstract
1. Introduction
2. Results
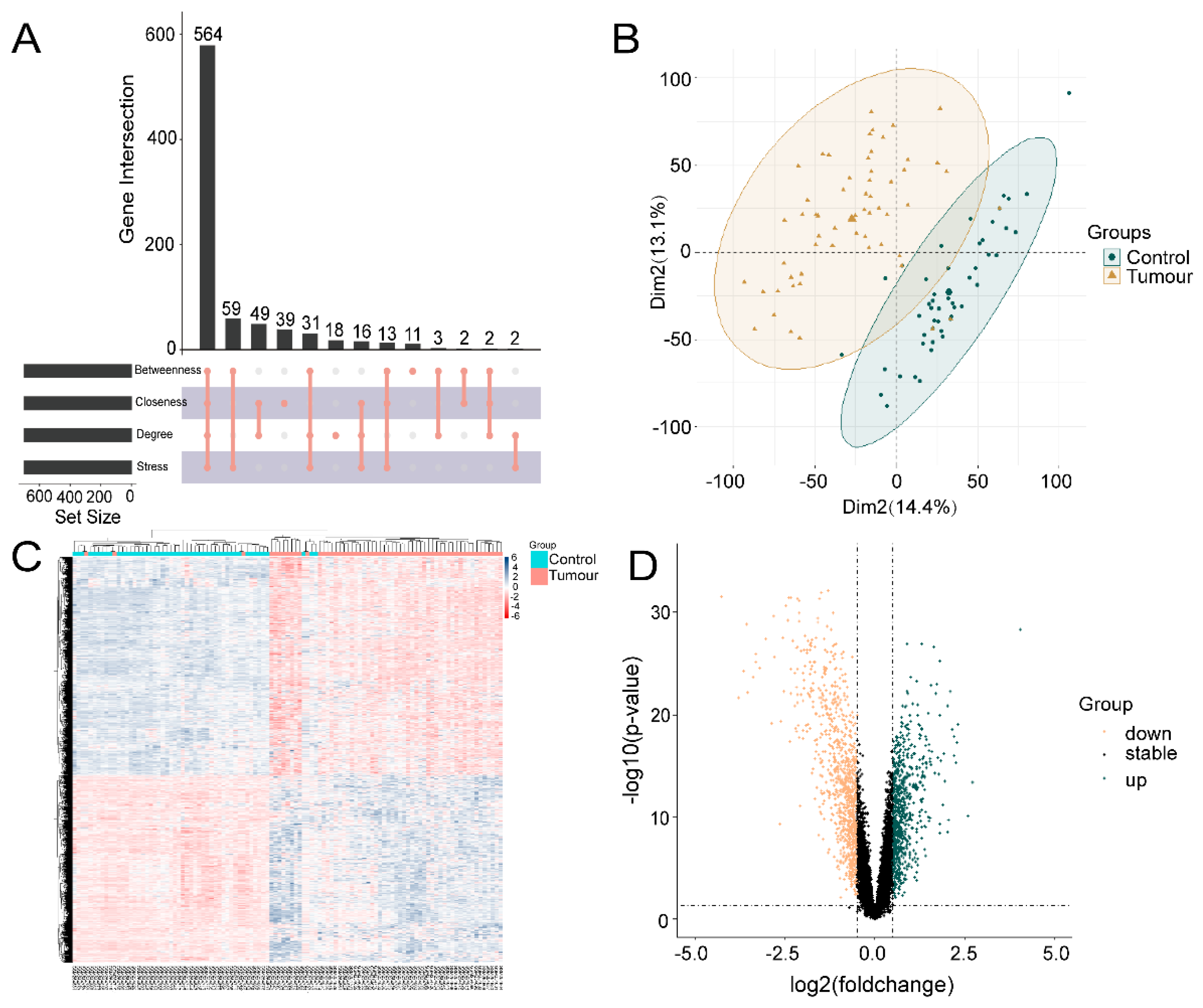
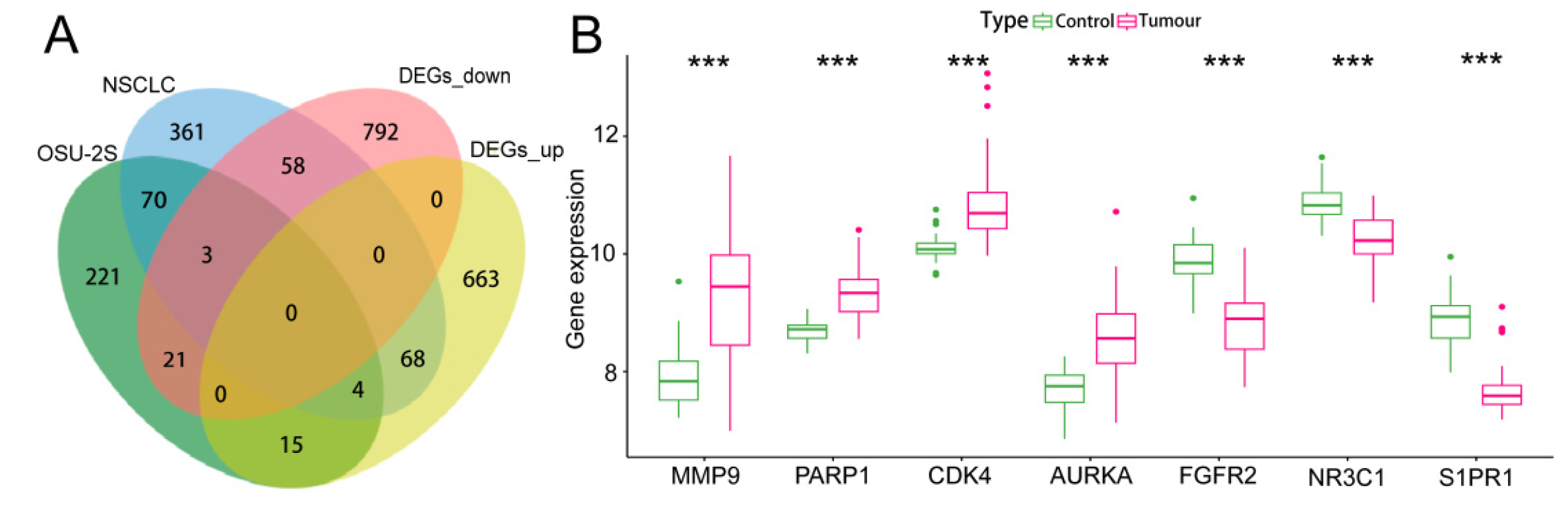
2.1. Acquisition of Marker Genes
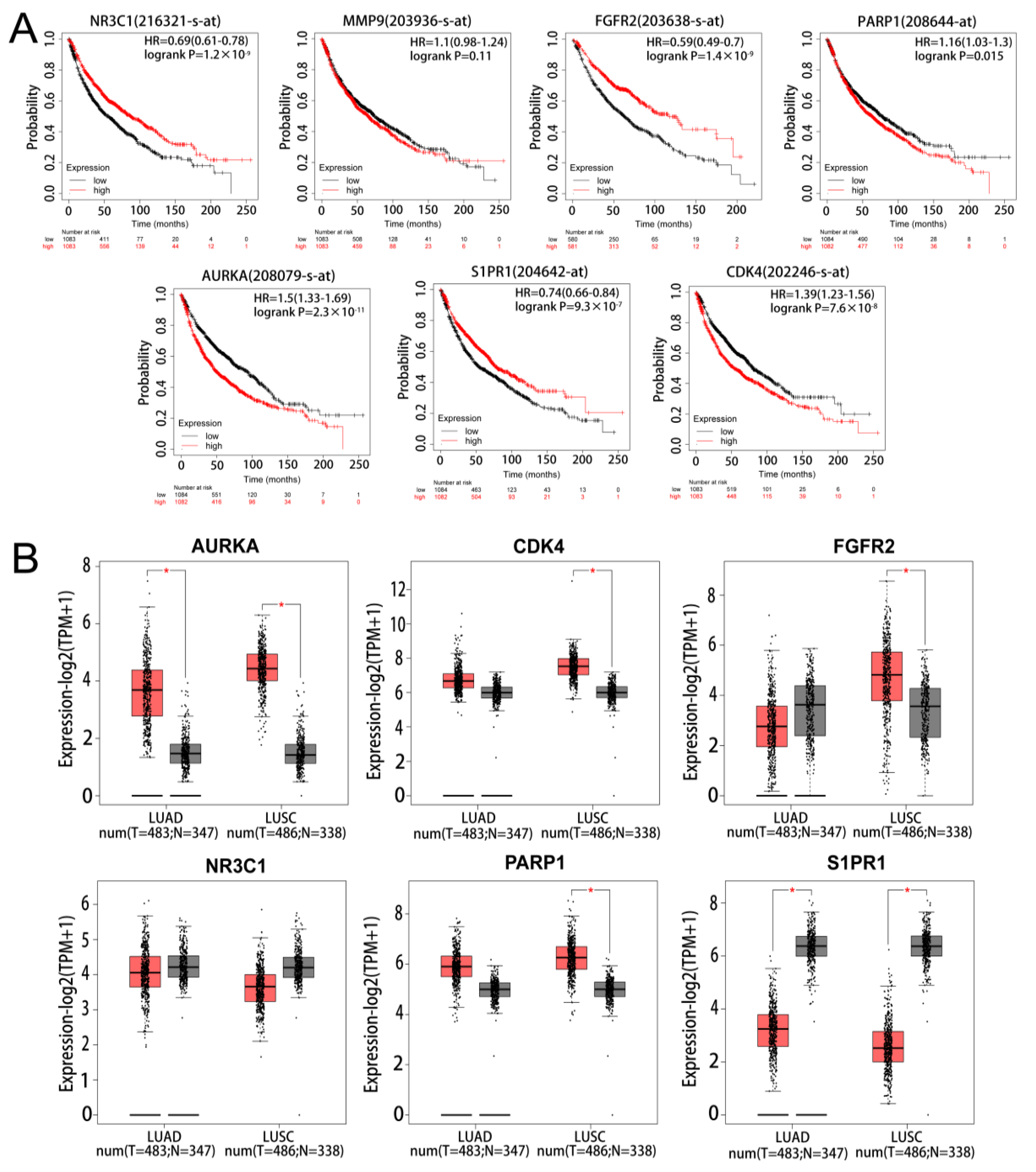
2.2. Survival and Expression Analysis of Marker Genes
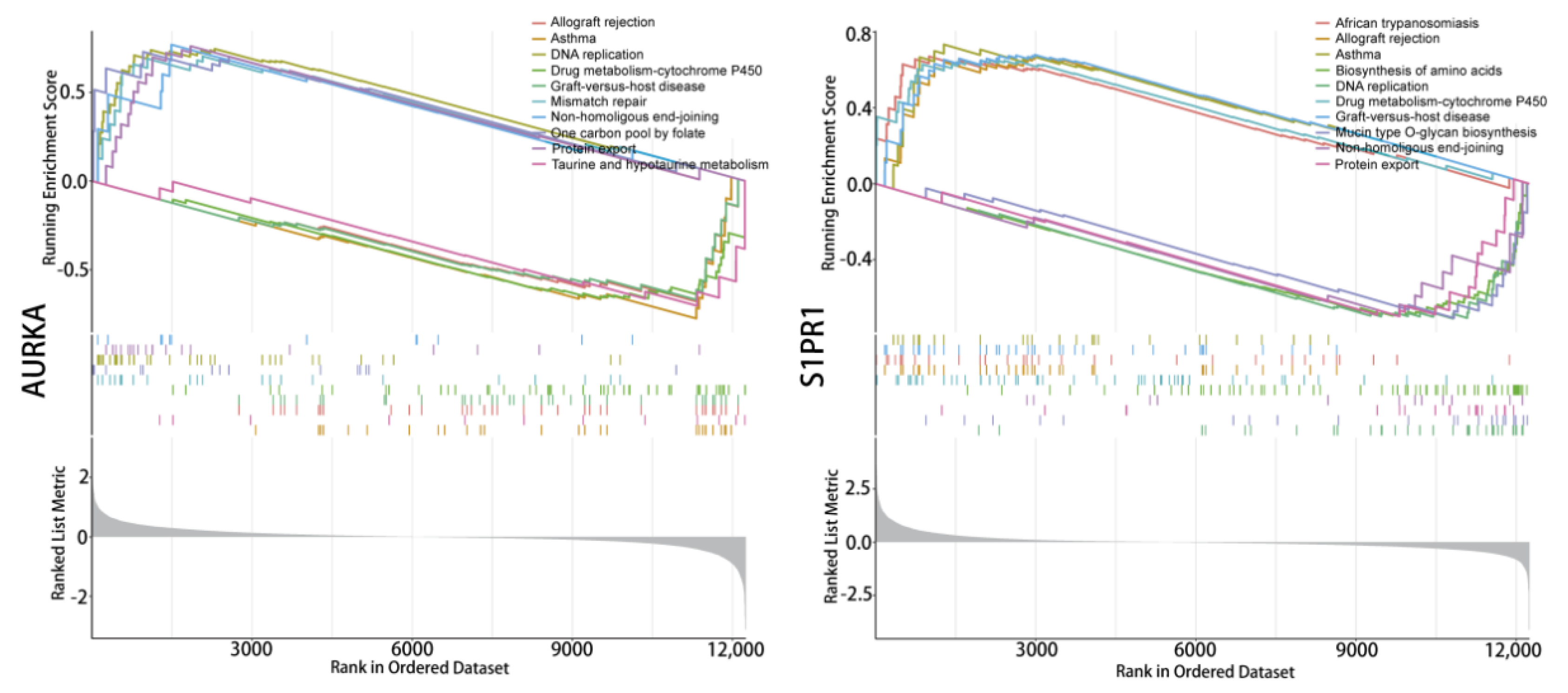
2.3. Functional Enrichment of Hub Genes
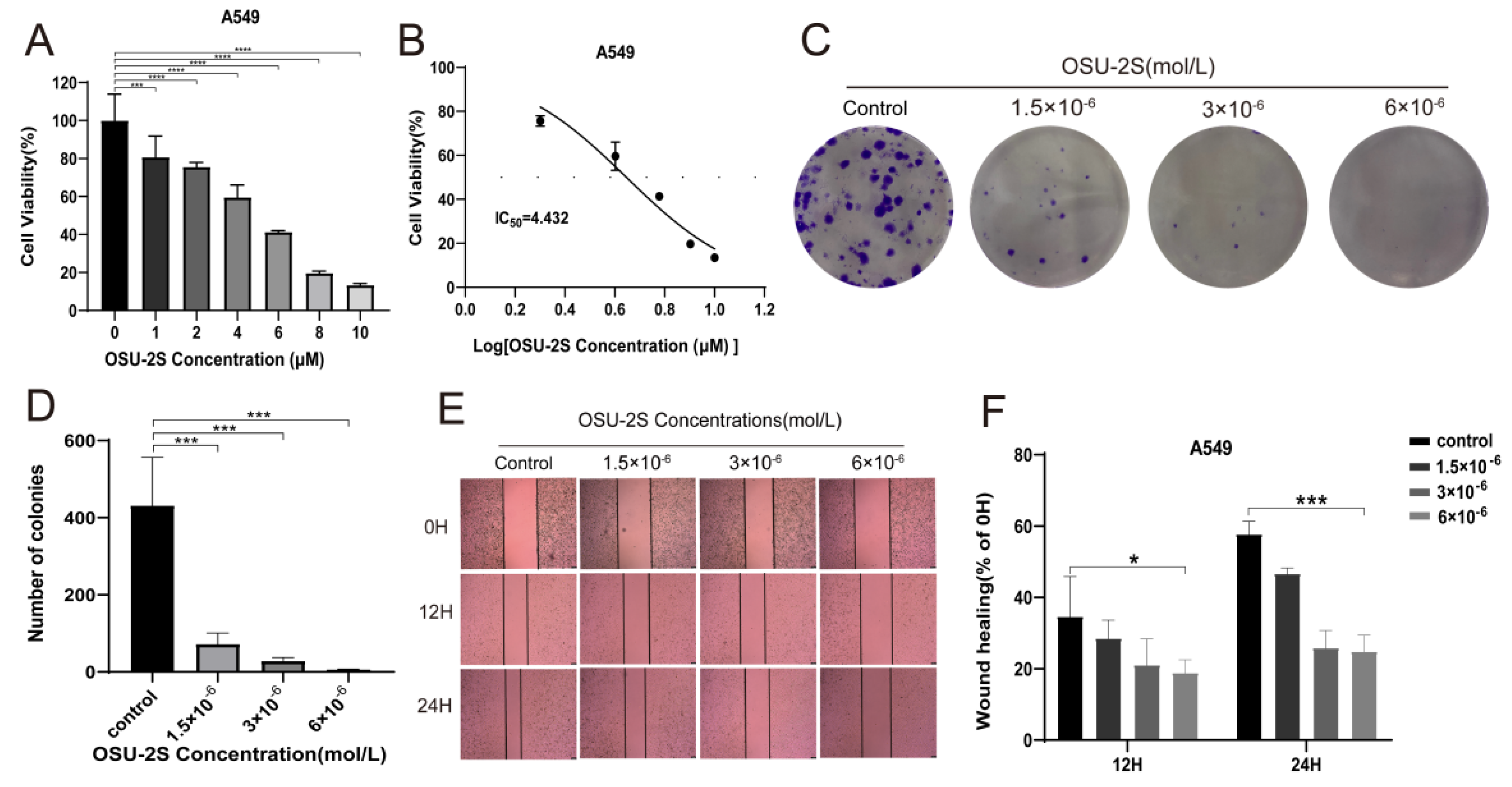
2.4. OSU-2S Effectively Inhibited the Cell Viability, Migration, and Colony Formation of A549 Cells
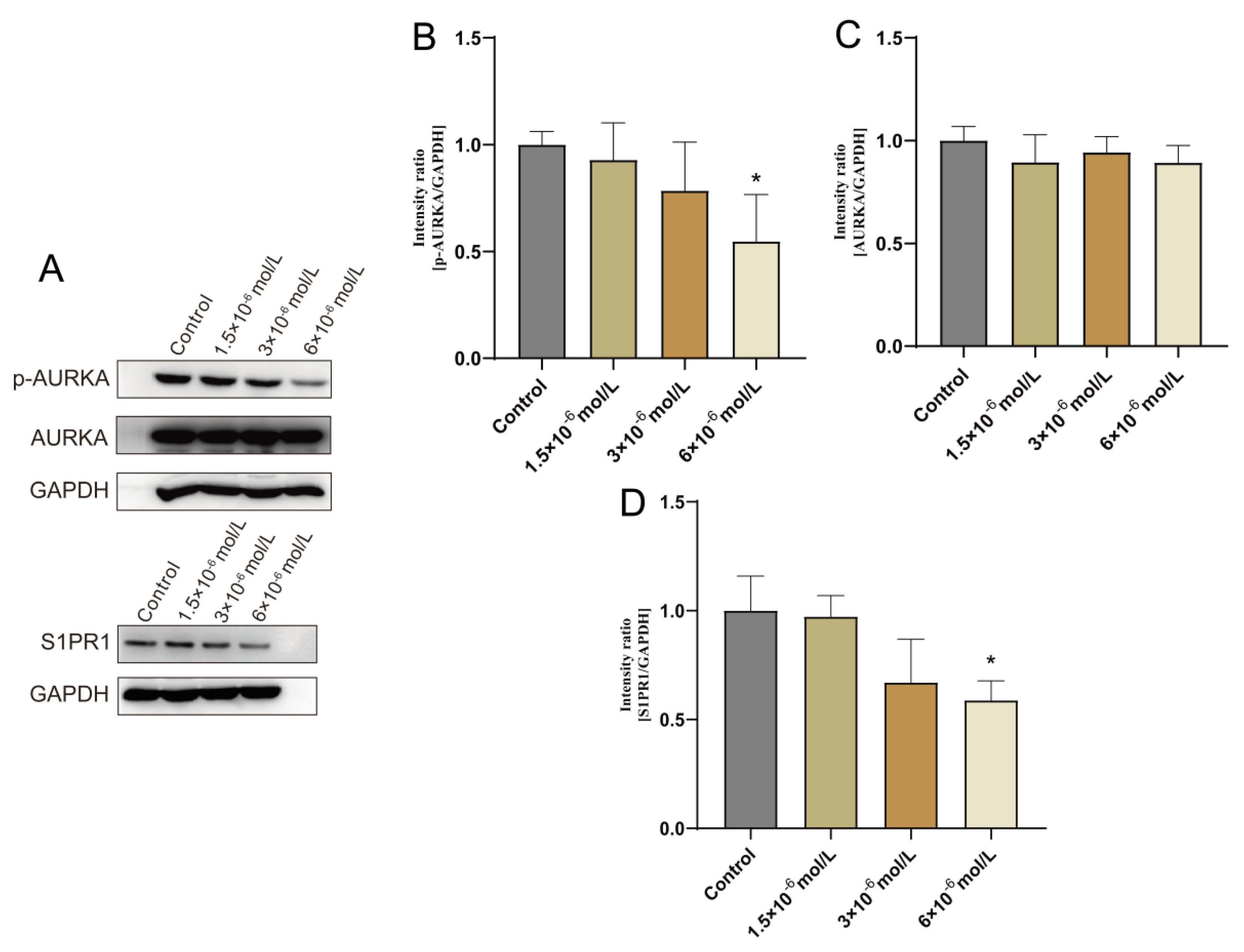
2.5. Validation of AURKA, S1PR1 Protein Expression
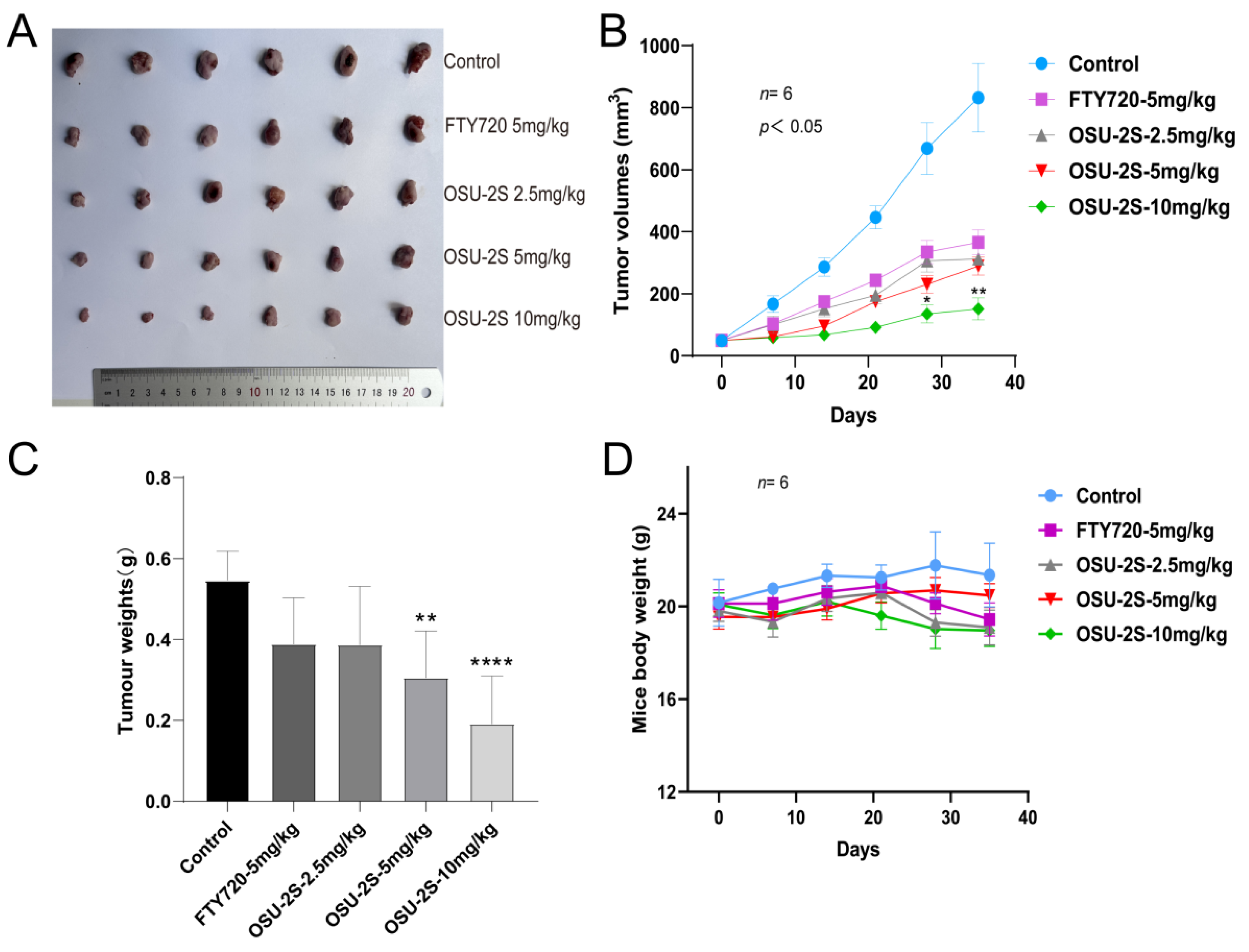
2.6. OSU-2S Showed Anti-Tumour Activity in a Mouse Lung Cancer Model
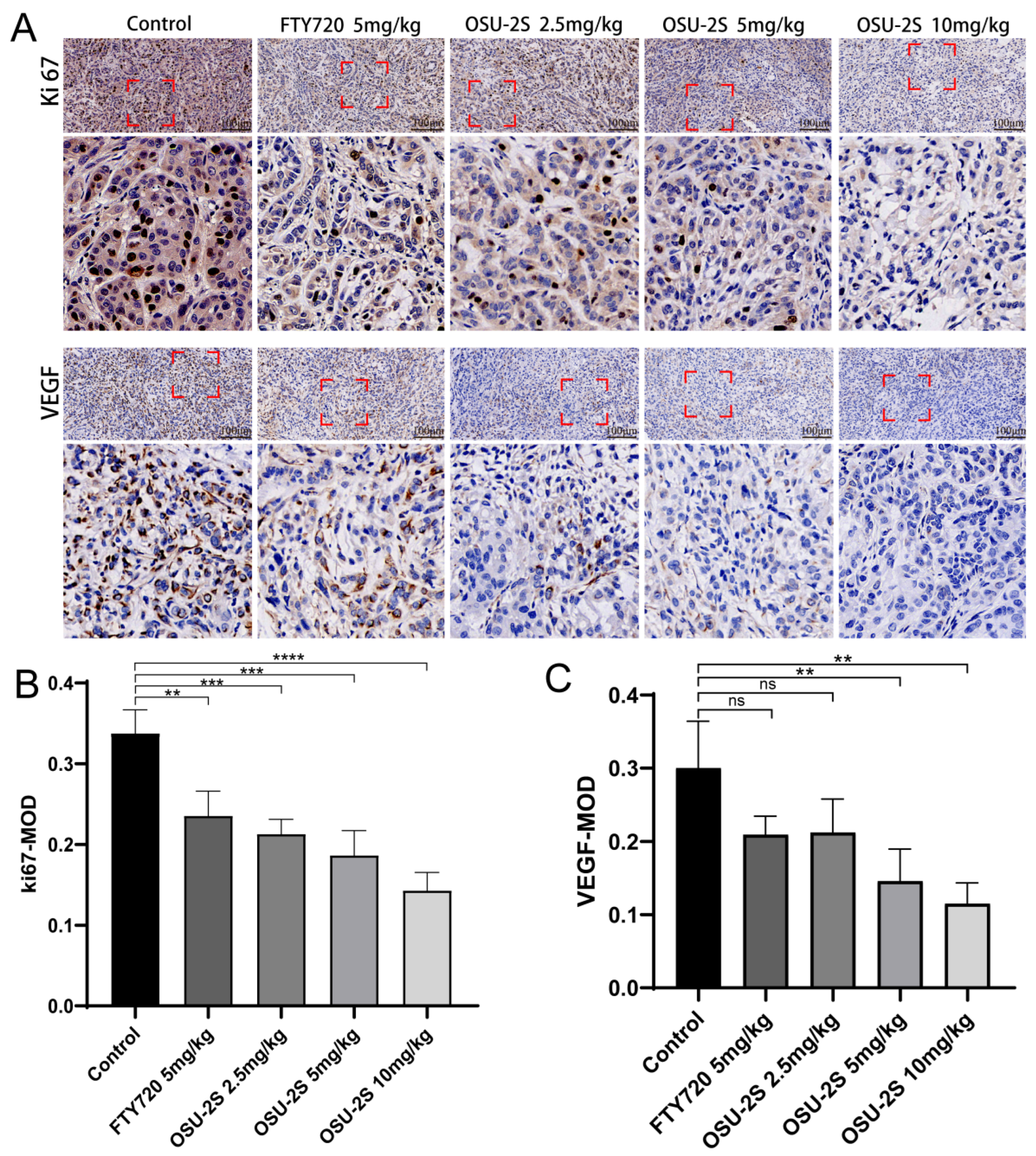
2.7. Immunohistochemical Detection of Vascular Endothelial Growth Factor and Tumor Proliferation Markers
3. Discussion
4. Materials and Methods
4.1. Data Sources
4.2. Screening of Disease Genes and Differentially Expressed Genes
4.3. Survival Analysis and Expression Analysis of Marker Genes
4.4. GSEA-KEGG Enrichment and Protein Expression Analysis of Hub Genes
4.5. Cell Experiments
4.5.1. Cell Culture
4.5.2. Cell Counting Kit (CCK)-8 Assay
4.5.3. Cell Migration
4.5.4. Colony Formation Assay
4.5.5. Western Blotting
4.6. Animal Experimentation
4.6.1. Experimental Mouse
4.6.2. Establishment of a Xenograft Mouse Model and Grouping
4.6.3. Immunohistochemistry of Tumour Tissue
4.7. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Siegel, R.L.; Miller, K.D. Cancer statistics, 2023. CA Cancer J. Clin. 2023, 73, 17–48. [Google Scholar] [CrossRef] [PubMed]
- Ruiz-Cordero, R.; Devine, W.P. Targeted Therapy and Checkpoint Immunotherapy in Lung Cancer. Surg. Pathol. Clin. 2020, 13, 17–33. [Google Scholar] [CrossRef] [PubMed]
- Feng, R.M.; Zong, Y.N. Current cancer situation in China: Good or bad news from the 2018 Global Cancer Statistics? Cancer Commun. 2019, 39, 22. [Google Scholar] [CrossRef] [PubMed]
- Wu, Y.L.; Zhong, W.Z. Epidermal growth factor receptor mutations and their correlation with gefitinib therapy in patients with non-small cell lung cancer: A meta-analysis based on updated individual patient data from six medical centers in mainland China. J. Thorac. Oncol. 2007, 2, 430–439. [Google Scholar] [CrossRef] [PubMed]
- Miller, K.D.; Nogueira, L. Cancer treatment and survivorship statistics. CA Cancer J. Clin. 2022, 72, 409–436. [Google Scholar] [CrossRef]
- American Cancer Society. Cancer Facts & Figures 2024; American Cancer Society: Atlanta, GA, USA, 2024. [Google Scholar]
- Weir, H.K.; Anderson, R.N. Peer reviewed: Heart disease and cancer deaths—Trends and projections in the United States, 1969–2020. Prev. Chronic Dis. 2016, 13, E157. [Google Scholar] [CrossRef]
- Ho, J.W.; Man, K. Effects of a novel immunomodulating agent, FTY720, on tumor growth and angiogenesis in hepatocellular carcinoma. Mol. Cancer Ther. 2005, 4, 1430–1438. [Google Scholar] [CrossRef] [PubMed]
- Adachi, K.; Chiba, K. FTY720 story. Its discovery and the following accelerated development of sphingosine 1-phosphate receptor agonists as immunomodulators based on reverse pharmacology. Perspect. Med. Chem. 2007, 1, 11–23. [Google Scholar] [CrossRef]
- Ahmed, D.; de Verdier, P.J. FTY720 (Fingolimod) sensitizes hepatocellular carcinoma cells to sorafenib-mediated cytotoxicity. Pharmacol. Res. Perspect. 2015, 3, e00171. [Google Scholar] [CrossRef]
- Hung, J.H.; Lu, Y.S. FTY720 induces apoptosis in hepatocellular carcinoma cells through activation of protein kinase C delta signaling. Cancer Res. 2008, 68, 1204–1212. [Google Scholar] [CrossRef]
- De Minicis, S.; Marzioni, M. New insights in hepatocellular carcinoma: From bench to bedside. Ann. Transl. Med. 2013, 1, 15. [Google Scholar]
- Mani, R.; Chiang, C.L. ROR1-targeted delivery of OSU-2S, a nonimmunosuppressive FTY720 derivative, exerts potent cytotoxicity in mantle-cell lymphoma in vitro and in vivo. Exp. Hematol. 2015, 43, 770–774.e772. [Google Scholar] [CrossRef]
- Mani, R.; Yan, R. Non-immunosuppressive FTY720-derivative OSU-2S mediates reactive oxygen species-mediated cytotoxicity in canine B-cell lymphoma. Vet. Comp. Oncol. 2017, 15, 1115–1118. [Google Scholar] [CrossRef] [PubMed]
- Omar, H.A.; Tolba, M.F. OSU-2S/Sorafenib Synergistic Antitumor Combination against Hepatocellular Carcinoma: The Role of PKCδ/p53. Front. Pharmacol. 2016, 7, 463. [Google Scholar] [CrossRef]
- Mani, R.; Mao, Y. Tumor antigen ROR1 targeted drug delivery mediated selective leukemic but not normal B-cell cytotoxicity in chronic lymphocytic leukemia. Leukemia 2015, 29, 346–355. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Han, X. Circular RNA-mediated ceRNA network was identified in human lung adenocarcinoma by high-throughput sequencing. Thorac. Cancer 2023, 14, 1430–1439. [Google Scholar] [CrossRef]
- Harrow, S.; Palma, D.A. Stereotactic Radiation for the Comprehensive Treatment of Oligometastases (SABR-COMET): Extended Long-Term Outcomes. Int. J. Radiat. Oncol. Biol. Phys. 2022, 114, 611–616. [Google Scholar] [CrossRef]
- Camidge, D.R.; Doebele, R.C. Comparing and contrasting predictive biomarkers for immunotherapy and targeted therapy of NSCLC. Nat. Rev. Clin. Oncol. 2019, 16, 341–355. [Google Scholar] [CrossRef]
- Lai, C.H.; Huang, Y.C. Translational upregulation of Aurora-A by hnRNP Q1 contributes to cell proliferation and tumorigenesis in colorectal cancer. Cell Death Dis. 2017, 8, e2555. [Google Scholar] [CrossRef] [PubMed]
- Li, G.; Tian, Y. The role of AURKA/miR-199b-3p in hepatocellular carcinoma cells. J. Clin. Lab. Anal. 2022, 36, e24758. [Google Scholar] [CrossRef] [PubMed]
- Jiang, J.; Wang, J. Direct Phosphorylation and Stabilization of MYC by Aurora B Kinase Promote T-cell Leukemogenesis. Cancer Cell. 2020, 37, 200–215.e205. [Google Scholar] [CrossRef]
- Yang, J.; Ikezoe, T. Bcr-Abl activates AURKA and AURKB in chronic myeloid leukemia cells via AKT signaling. Int. J. Cancer. 2014, 134, 1183–1194. [Google Scholar] [CrossRef] [PubMed]
- Liu, F.; Zhang, Y. Knockdown of AURKA sensitizes the efficacy of radiation in human colorectal cancer. Life Sci. 2021, 271, 119148. [Google Scholar] [CrossRef] [PubMed]
- Jin, X.; Liu, X. Integrated Analysis of DNA Methylation and mRNA Expression Profiles Data to Identify Key Genes in Lung Adenocarcinoma. Biomed. Res. Int. 2016, 2016, 4369431. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Hu, T. Repression of the AURKA-CXCL5 axis induces autophagic cell death and promotes radiosensitivity in non-small-cell lung cancer. Cancer Lett. 2021, 509, 89–104. [Google Scholar] [CrossRef] [PubMed]
- Tao, Y.P.; Zhu, H.Y. S1PR1 regulates ovarian cancer cell senescence through the PDK1-LATS1/2-YAP pathway. Oncogene 2023, 42, 3491–3502. [Google Scholar] [CrossRef]
- Chen, C.L.; Meng, E. Targeting S1PR1 May Result in Enhanced Migration of Cancer Cells in Bladder Carcinoma. Cancers 2021, 13, 4474. [Google Scholar] [CrossRef] [PubMed]
- Huwiler, A.; Pfeilschifter, J. Altering the sphingosine-1-phosphate/ceramide balance: A promising approach for tumor therapy. Curr. Pharm. Des. 2006, 12, 4625–4635. [Google Scholar] [CrossRef]
- Aoki, M.; Aoki, H. Sphingosine-1-Phosphate Signaling in Immune Cells and Inflammation: Roles and Therapeutic Potential. Mediat. Inflamm. 2016, 2016, 8606878, Corrigendum in Mediat. Inflamm. 2016, 2016, 2856829. [Google Scholar]
- Zhu, Y.; Luo, G. Apolipoprotein M promotes proliferation and invasion in non-small cell lung cancers via upregulating S1PR1 and activating the ERK1/2 and PI3K/AKT signaling pathways. Biochem. Biophys. Res. Commun. 2018, 501, 520–526. [Google Scholar] [CrossRef]
- Zhang, X.; Liu, Y. MiR-125b-1-3p Exerts Antitumor Functions in Lung Carcinoma Cells by Targeting S1PR1. Chin. Med. J. (Engl. Ed.) 2018, 131, 1909–1916. [Google Scholar] [CrossRef] [PubMed]
- Weichand, B.; Popp, R. S1PR1 on tumor-associated macrophages promotes lymphangiogenesis and metastasis via NLRP3/IL-1β. J. Exp. Med. 2017, 214, 2695–2713. [Google Scholar] [CrossRef]
- Dasari, S.; Tchounwou, P.B. Cisplatin in cancer therapy: Molecular mechanisms of action. Eur. J. Pharmacol. 2014, 740, 364–378. [Google Scholar] [CrossRef]
- Chaudhari, R.; Patel, P. Fabrication of methotrexate-loaded gold nanoconjugates and its enhanced anticancer activity in breast cancer. 3 Biotech 2021, 11, 175. [Google Scholar] [CrossRef] [PubMed]
- Hill, N.O. Cis-platinum for cancer. N. Engl. J. Med. 1979, 301, 47. [Google Scholar] [PubMed]
- Davis, S.; Meltzer, P.S. GEOquery: A bridge between the Gene Expression Omnibus (GEO) and BioConductor. Bioinformatics 2007, 23, 1846–1847. [Google Scholar] [CrossRef]
- Yu, G.; Wang, L.G. clusterProfiler: An R package for comparing biological themes among gene clusters. Omics 2012, 16, 284–287. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Han, M.; Liu, X.; Hailati, S.; Nurahmat, N.; Dilimulati, D.; Baishan, A.; Aikebaier, A.; Zhou, W. Evaluation of the Efficacy of OSU-2S in the Treatment of Non-Small-Cell Lung Cancer and Screening of Potential Targets of Action. Pharmaceuticals 2024, 17, 582. https://doi.org/10.3390/ph17050582
Han M, Liu X, Hailati S, Nurahmat N, Dilimulati D, Baishan A, Aikebaier A, Zhou W. Evaluation of the Efficacy of OSU-2S in the Treatment of Non-Small-Cell Lung Cancer and Screening of Potential Targets of Action. Pharmaceuticals. 2024; 17(5):582. https://doi.org/10.3390/ph17050582
Chicago/Turabian StyleHan, Mengyuan, Xiangran Liu, Sendaer Hailati, Nurbiya Nurahmat, Dilihuma Dilimulati, Alhar Baishan, Alifeiye Aikebaier, and Wenting Zhou. 2024. "Evaluation of the Efficacy of OSU-2S in the Treatment of Non-Small-Cell Lung Cancer and Screening of Potential Targets of Action" Pharmaceuticals 17, no. 5: 582. https://doi.org/10.3390/ph17050582
APA StyleHan, M., Liu, X., Hailati, S., Nurahmat, N., Dilimulati, D., Baishan, A., Aikebaier, A., & Zhou, W. (2024). Evaluation of the Efficacy of OSU-2S in the Treatment of Non-Small-Cell Lung Cancer and Screening of Potential Targets of Action. Pharmaceuticals, 17(5), 582. https://doi.org/10.3390/ph17050582




