Moringa oleifera Leaf Extract Promotes Healing of Infected Wounds in Diabetic Rats: Evidence of Antimicrobial, Antioxidant and Proliferative Properties
Abstract
:1. Introduction
2. Results
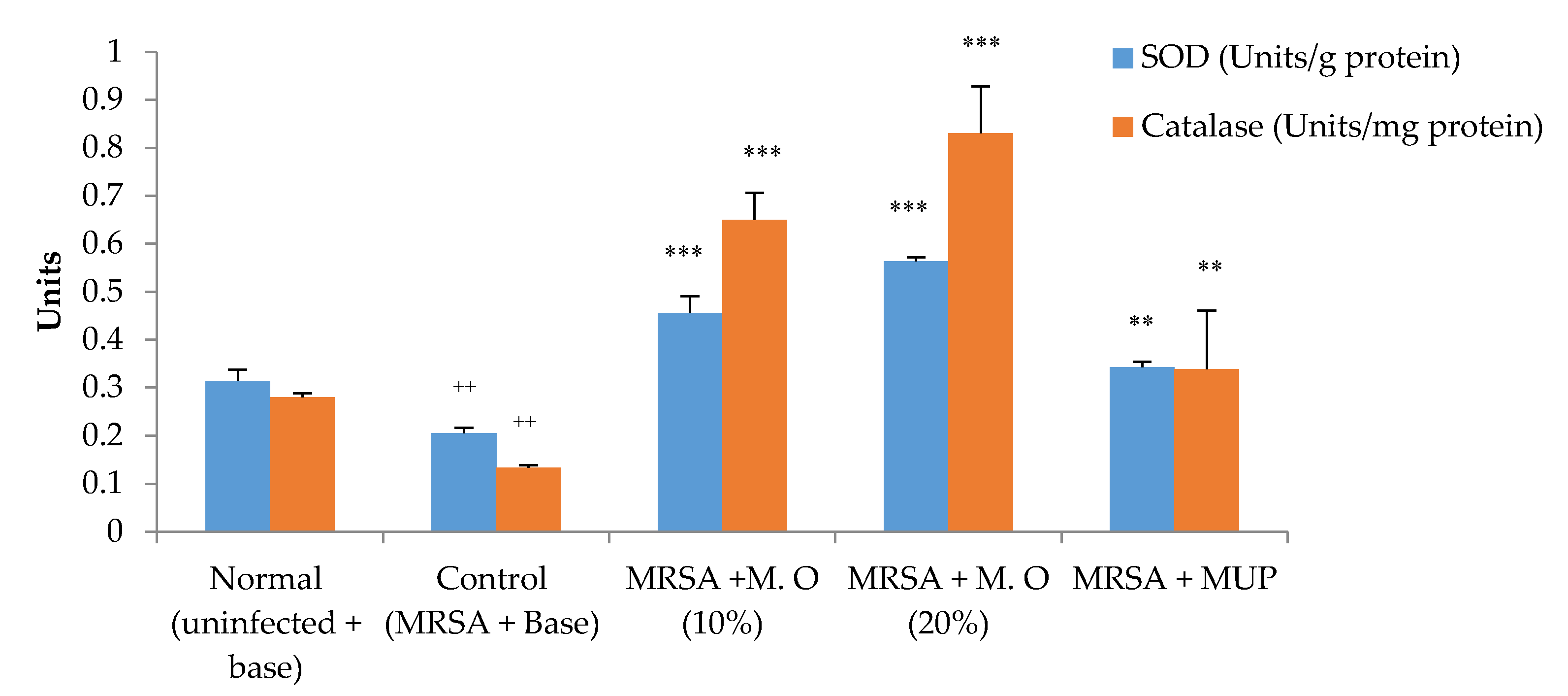
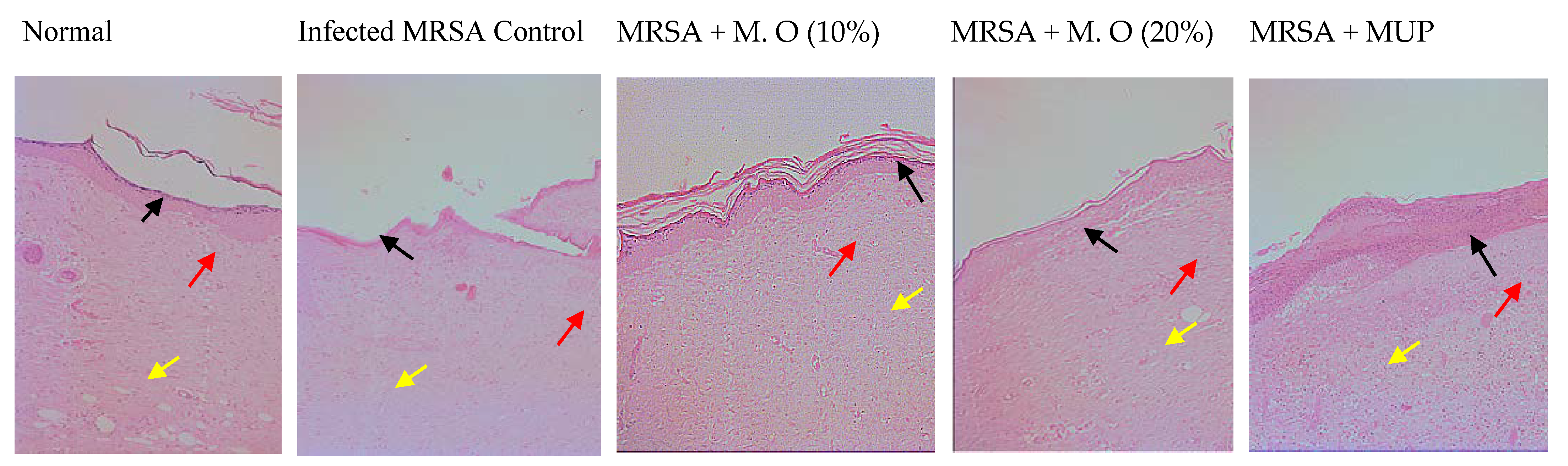
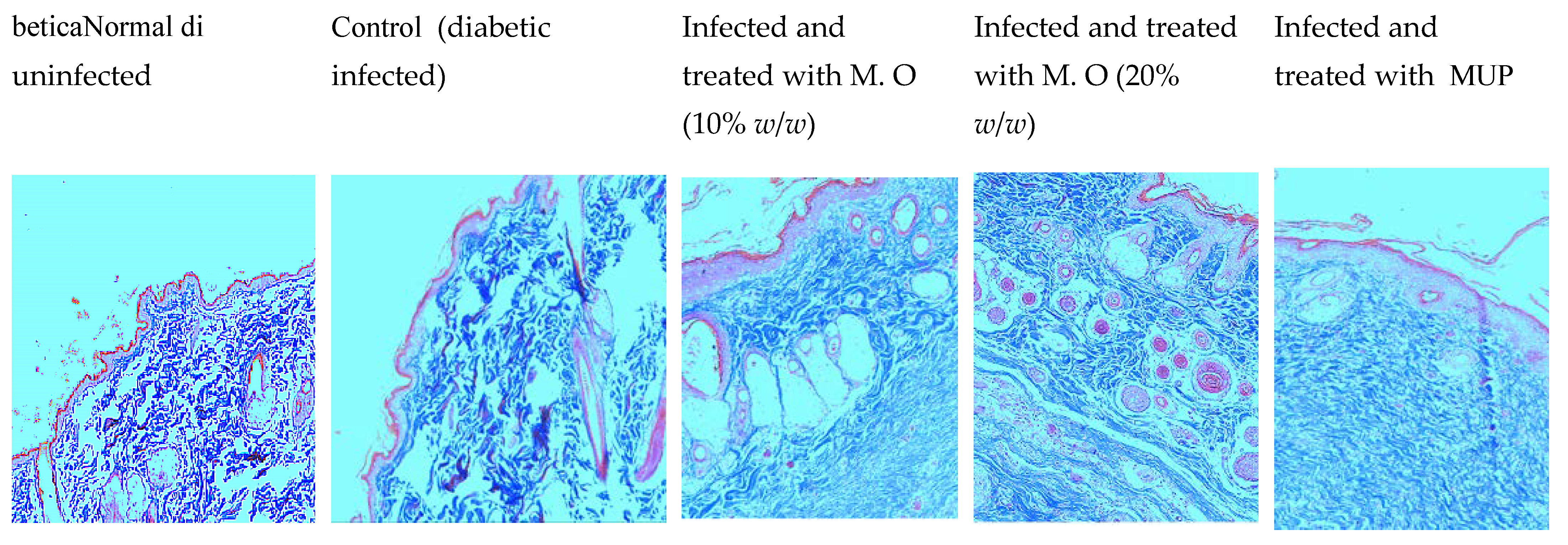
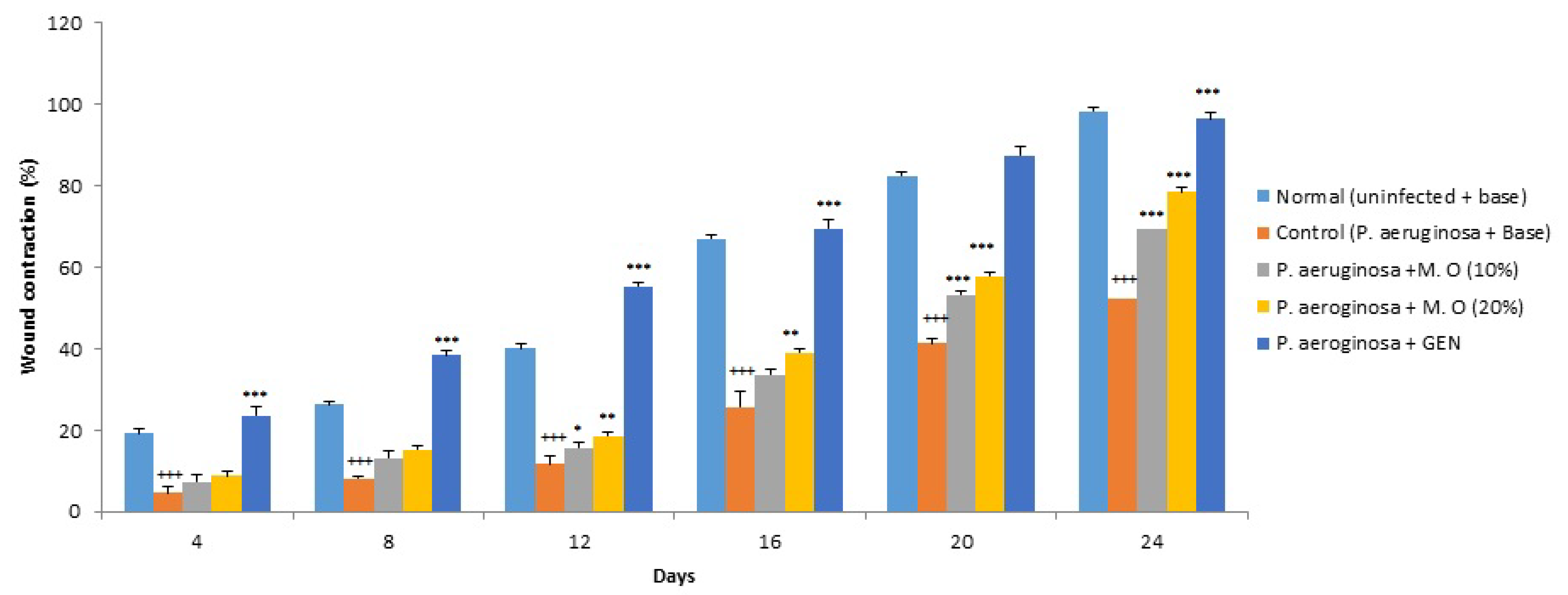
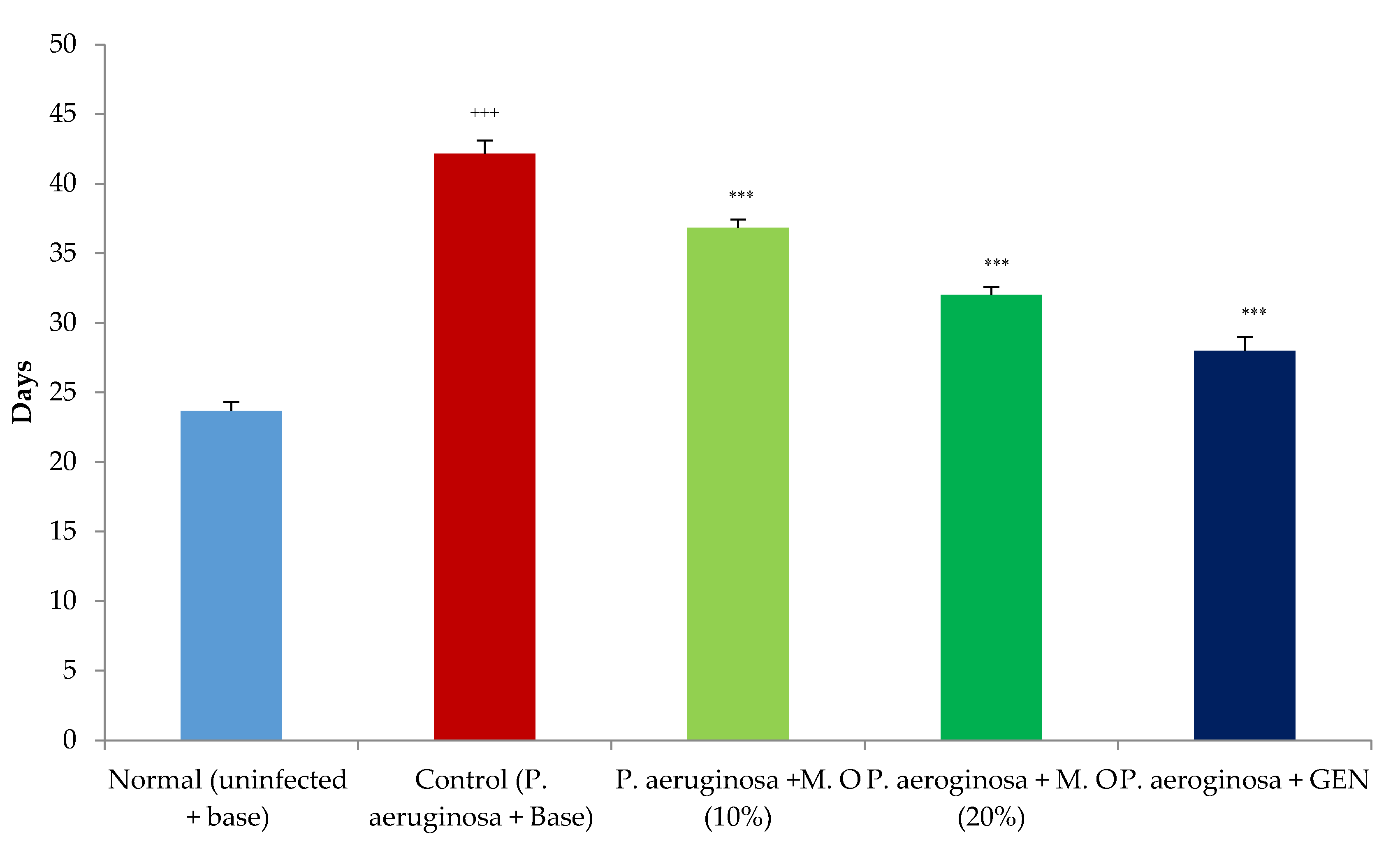
2.1. Effect on Wound Contraction and Duration for Epithelization
2.2. In Vitro Study on HaCaT Cells
3. Discussion
4. Materials and Methods
In Vitro Study on HaCaT Cells
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Conflicts of Interest
References
- Spampinato, S.F.; Caruso, G.I.; De Pasquale, R.; Sortino, M.A.; Merlo, S. The Treatment of Impaired Wound Healing in Diabetes: Looking among Old Drugs. Pharmaceuticals 2020, 13, 60. [Google Scholar] [CrossRef] [Green Version]
- Macdonald, K.E.; Boeckh, S.; Stacey, H.J.; Jones, J.D. The microbiology of diabetic foot infections: A meta-analysis. BMC Infect. Dis. 2021, 21, 770. [Google Scholar] [CrossRef] [PubMed]
- Boulton, A.J.M.; Armstrong, D.G.; Hardman, M.J.; Malone, M.; Embil, J.M.; Attinger, C.E.; Lipsky, B.A.; Aragón-Sánchez, J.; Li, H.K.; Schultz, G.; et al. Diagnosis and Management of Diabetic Foot Infections. Diagn. Manag. Diabet. Foot Infect. 2020. [Google Scholar] [CrossRef] [Green Version]
- Shedoeva, A.; Leavesley, D.; Upton, Z.; Fan, C. Wound healing and the use of medicinal plants. Evid.-Based Complement. Altern. Med. 2019, 2019, 2684108. [Google Scholar] [CrossRef] [PubMed]
- Kashyap, P.; Kumar, S.; Riar, C.S.; Jindal, N.; Baniwal, P.; Guiné, R.P.F.; Correia, P.M.R.; Mehra, R.; Kumar, H. Recent Advances in Drumstick (Moringa oleifera) Leaves Bioactive Compounds: Composition, Health Benefits, Bioaccessibility, and Dietary Applications. Antioxidants 2022, 11, 402. [Google Scholar] [CrossRef]
- Milla, P.G.; Peñalver, R.; Nieto, G. Health Benefits of Uses and Applications of Moringa oleifera in Bakery Products. Plants 2021, 10, 318. [Google Scholar] [CrossRef]
- Rani, N.Z.A.; Husain, K.; Kumolosasi, E. Moringa genus: A review of phytochemistry and pharmacology. Front. Pharmacol. 2018, 9, 108. [Google Scholar] [CrossRef] [Green Version]
- Lambole, V.; Kumar, U. Effect of Moringa oleifera Lam. on normal and dexamethasone suppressed wound healing. Asian Pac. J. Trop. Biomed. 2012, 2, S219–S223. [Google Scholar] [CrossRef]
- Gothai, S.; Arulselvan, P.; Tan, W.S.; Fakurazi, S. Wound healing properties of ethyl acetate fraction of Moringa oleifera in normal human dermal fibroblasts. J. Intercult. Ethnopharmacol. 2016, 5, 1–6. [Google Scholar] [CrossRef]
- Fayemi, O.E.; Ekennia, A.C.; Katata-Seru, L.; Ebokaiwe, A.P.; Ijomone, O.M.; Onwudiwe, D.C.; Ebenso, E.E. Antimicrobial and Wound Healing Properties of Polyacrylonitrile-Moringa Extract Nanofibers. ACS Omega 2018, 3, 4791–4797. [Google Scholar] [CrossRef]
- Muhammad, A.A.; Pauzi, N.A.S.; Arulselvan, P.; Abas, F.; Fakurazi, S. In vitro wound healing potential and identification of bioactive compounds from Moringa oleifera Lam. BioMed. Res. Int. 2013, 2013, 974580. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hukkeri, V.; Nagathan, C.; Karadi, R.; Patil, B. Antipyretic and wound healing activities of Moringa oleifera lam. in rats. Indian J. Pharm. Sci. 2006, 68, 124. [Google Scholar] [CrossRef] [Green Version]
- Azevedo, Í.M.; Araújo-Filho, I.; Teixeira, M.M.A.; Moreira, M.D.F.d.C.; Medeiros, A.C. Wound healing of diabetic rats treated with Moringa oleifera extract. Acta Cirúrgica Bras. 2018, 33, 799–805. [Google Scholar] [CrossRef]
- Muhammad, A.A.; Arulselvan, P.; Cheah, P.S.; Abas, F.; Fakurazi, S. Evaluation of wound healing properties of bioactive aqueous fraction from Moringa oleifera Lam on experimentally induced diabetic animal model. Drug Des. Devel. Ther. 2016, 10, 1715–1730. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Eyarefe, O.D.; Idowu, A.; Afolabi, J.M. Healing Potentials of Oral Moringa oleifera Leaves Extract and Tetracycline on Methicillin Resistant Staphylococcus Aureus Infected Wounds of Wistar rats. Niger. J. Physiol. Sci. 2015, 30, 73–78. [Google Scholar]
- Singh, B.; Sharma, V.; Kumar, A. Designing moringa gum-sterculia gum-polyacrylamide hydrogel wound dressings for drug delivery applications. Carbohydr. Polym. Technol. Appl. 2021, 2, 100062. [Google Scholar] [CrossRef]
- Bhalla, N.; Ingle, N.; Patri, S.V.; Haranath, D. Phytochemical analysis of Moringa oleifera leaves extracts by GC-MS and free radical scavenging potency for industrial applications. Saudi J. Biol. Sci. 2021, 28, 6915–6928. [Google Scholar] [CrossRef] [PubMed]
- Kännaste, A.; Copolovici, L.; Niinemets, Ü. Gas chromatography-mass spectrometry method for determination of biogenic volatile organic compounds emitted by plants. Methods Mol. Biol. 2014, 1153, 161–169. [Google Scholar] [CrossRef] [PubMed]
- Emulsifying Ointment BP—Summary of Product Characteristics (SmPC)—(emc). Available online: https://www.medicines.org.uk/emc/product/4571/smpc#gref (accessed on 14 March 2022).
- Dinh, T.; Elder, S.; Veves, A. Delayed wound healing in diabetes: Considering future treatments. Diabetes Manag. 2011, 1, 509–519. [Google Scholar] [CrossRef]
- Greenhalgh, D.G. Wound healing and diabetes mellitus. Clin. Plast. Surg. 2003, 30, 37–45. [Google Scholar] [CrossRef]
- Furman, B.L. Streptozotocin-Induced Diabetic Models in Mice and Rats. Curr. Protoc. 2021, 1, e78. [Google Scholar] [CrossRef] [PubMed]
- Sardari, K.; Kakhki, E.G.; Mohri, M. Evaluation of wound contraction and epithelialization after subcutaneous administration of Theranekron® in cows. Comp. Clin. Pathol. 2006, 16, 197–200. [Google Scholar] [CrossRef]
- Koohsari, H.; Ghaemi, E.A.; Sadegh Sheshpoli, M.; Jahedi, M.; Zahiri, M. The investigation of antibacterial activity of selected native plants from North of Iran. J. Med. Life 2015, 8, 38. [Google Scholar] [PubMed]
- Fitzmaurice, S.D.; Sivamani, R.K.; Isseroff, R.R. Antioxidant therapies for wound healing: A clinical guide to currently commercially available products. Skin Pharmacol. Physiol. 2011, 24, 113–126. [Google Scholar] [CrossRef]
- Xu, Y.; Chen, G.; Guo, M. Correlations between phytochemical fingerprints of Moringa oleifera leaf extracts and their antioxidant activities revealed by chemometric analysis. Phytochem. Anal. 2021, 32, 698–709. [Google Scholar] [CrossRef]
- Fischer, A.H.; Jacobson, K.A.; Rose, J.; Zeller, R. Hematoxylin and eosin staining of tissue and cell sections. CSH Protoc. 2008, 2008, pdb-prot4986. [Google Scholar] [CrossRef]
- Rieppo, L.; Janssen, L.; Rahunen, K.; Lehenkari, P.; Finnilä, M.A.J.; Saarakkala, S. Histochemical quantification of collagen content in articular cartilage. PLoS ONE 2019, 14, e0224839. [Google Scholar] [CrossRef] [Green Version]
- Schultz, G.S.; Chin, G.A.; Moldawer, L.; Diegelmann, R.F. Principles of Wound Healing. Diabet. Foot Probl. 2011, 9, 395–402. [Google Scholar] [CrossRef]
- Soybir, O.C.; Gürdal, S.Ö.; Oran, E.Ş.; Tülübaş, F.; Yüksel, M.; Akyildiz, A.I.; Bilir, A.; Soybir, G.R. Delayed cutaneous wound healing in aged rats compared to younger ones. Int. Wound J. 2012, 9, 478. [Google Scholar] [CrossRef] [PubMed]
- Gilliver, S.C.; Ruckshanthi, J.P.D.; Hardman, M.J.; Nakayama, T.; Ashcroft, G.S. Sex dimorphism in wound healing: The roles of sex steroids and macrophage migration inhibitory factor. Endocrinology 2008, 149, 5747–5757. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Colombo, I.; Sangiovanni, E.; Maggio, R.; Mattozzi, C.; Zava, S.; Corbett, Y.; Fumagalli, M.; Carlino, C.; Corsetto, P.A.; Scaccabarozzi, D.; et al. HaCaT Cells as a Reliable in Vitro Differentiation Model to Dissect the Inflammatory/Repair Response of Human Keratinocytes. Mediators Inflamm. 2017, 2017, 7435621. [Google Scholar] [CrossRef]
- Zhang, J.; Yang, P.; Liu, D.; Gao, M.; Wang, J.; Wang, X.; Liu, Y.; Zhang, X. c-Myc Upregulated by High Glucose Inhibits HaCaT Differentiation by S100A6 Transcriptional Activation. Front. Endocrinol. 2021, 12, 561. [Google Scholar] [CrossRef] [PubMed]
- Nunes, M.O.; Fátima Goebel de Souza, T.D.; Pierdoná, T.M.; Ramos, M.V.; Ferreira, K.Q.; Duarte, R.S.; Shahwar, D.E.; Wilke, D.V.; Wong, D.V.T.; Alencar, N.M.N. In vitro biocompatibility and wound healing properties of latex proteins dressing. Toxicol. Vitr. 2021, 76, 105230. [Google Scholar] [CrossRef]
- Mazumdar, S.; Ghosh, A.K.; Dinda, M.; Das, A.K.; Das, S.; Jana, K.; Karmakar, P. Evaluation of wound healing activity of ethanol extract of Annona reticulata L. leaf both in vitro and in diabetic mice model. J. Tradit. Complement. Med. 2021, 11, 27–37. [Google Scholar] [CrossRef] [PubMed]
- Bao, P.; Kodra, A.; Tomic-Canic, M.; Golinko, M.S.; Ehrlich, H.P.; Brem, H. The role of vascular endothelial growth factor in wound healing. J. Surg. Res. 2009, 153, 347–358. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zegers-Hochschild, F.; Adamson, G.D.; De Mouzon, J.; Ishihara, O.; Mansour, R.; Nygren, K.; Sullivan, E.; Van Der Poel, S. The International Committee for Monitoring Assisted Reproductive Technology (ICMART) and the World Health Organization (WHO) Revised Glossary on ART Terminology, 2009. Hum. Reprod. 2009, 24, 2683–2687. [Google Scholar] [CrossRef] [Green Version]
- Pakyari, M.; Farrokhi, A.; Maharlooei, M.K.; Ghahary, A. Critical Role of Transforming Growth Factor Beta in Different Phases of Wound Healing. Adv. Wound Care 2013, 2, 215. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Xiao, X.; Wang, J.; Meng, C.; Liang, W.; Wang, T.; Zhou, B.; Wang, Y.; Luo, X.; Gao, L.; Zhang, L. Moringa oleifera Lam and its Therapeutic Effects in Immune Disorders. Front. Pharmacol. 2020, 11, 2188. [Google Scholar] [CrossRef] [PubMed]
- Borges, A.; José, H.; Homem, V.; Simões, M. Comparison of Techniques and Solvents on the Antimicrobial and Antioxidant Potential of Extracts from Acacia dealbata and Olea europaea. Antibiotics 2020, 9, 48. [Google Scholar] [CrossRef] [PubMed]
- Mukherjee, P.K. Evidence-Based Validation of Herbal Medicine; Elsevier: Amsterdam, The Netherlands, 2015; p. 537. [Google Scholar]
- Nayeem, N.; Mohammed Basheeruddin Asdaq, S.; Alamri, A.S.; Alsanie, W.F.; Alhomrani, M.; Mohzari, Y.; Alrashed, A.A.; Alotaibi, N.; Aalhathal, A.S.; Alharbi, M.A.; et al. Wound healing potential of Dodonaea viscosa extract formulation in experimental animals. J. King Saud Univ.-Sci. 2021, 33, 101476. [Google Scholar] [CrossRef]
- Kolhe, S.S.; Shinde, K.; Jori, R.; Gadhave, M.V.; Jadhav, S.L.; Gaikwad, D.D. Evaluation of polyherbal ointment for wound healing activity in Wistar rats. J. Drug Deliv. Ther. 2018, 8, 26–31. [Google Scholar] [CrossRef]
- Ekom, S.E.; Tamokou, J.D.D.; Kuete, V. Methanol extract from the seeds of Persea americana displays antibacterial and wound healing activities in rat model. J. Ethnopharmacol. 2022, 282, 114573. [Google Scholar] [CrossRef] [PubMed]
- Nivitabishekam, S.N.; Asad, M.; Prasad, V.S. Pharmacodynamic interaction of Momordica charantia with rosiglitazone in rats. Chem. Biol. Interact. 2009, 177, 247–253. [Google Scholar] [CrossRef] [PubMed]
- Anesthesia (Guideline). Vertebrate Animal Research. Available online: https://animal.research.uiowa.edu/iacuc-guidelines-anesthesia (accessed on 13 February 2022).
- Elstner, E.F.; Heupel, A. Inhibition of nitrite formation from hydroxylammoniumchloride: A simple assay for superoxide dismutase. Anal. Biochem. 1976, 70, 616–620. [Google Scholar] [CrossRef]
- Link, E.M. The mechanism of pH-dependent hydrogen peroxide cytotoxicity in vitro. Arch. Biochem. Biophys. 1988, 265, 362–372. [Google Scholar] [CrossRef]


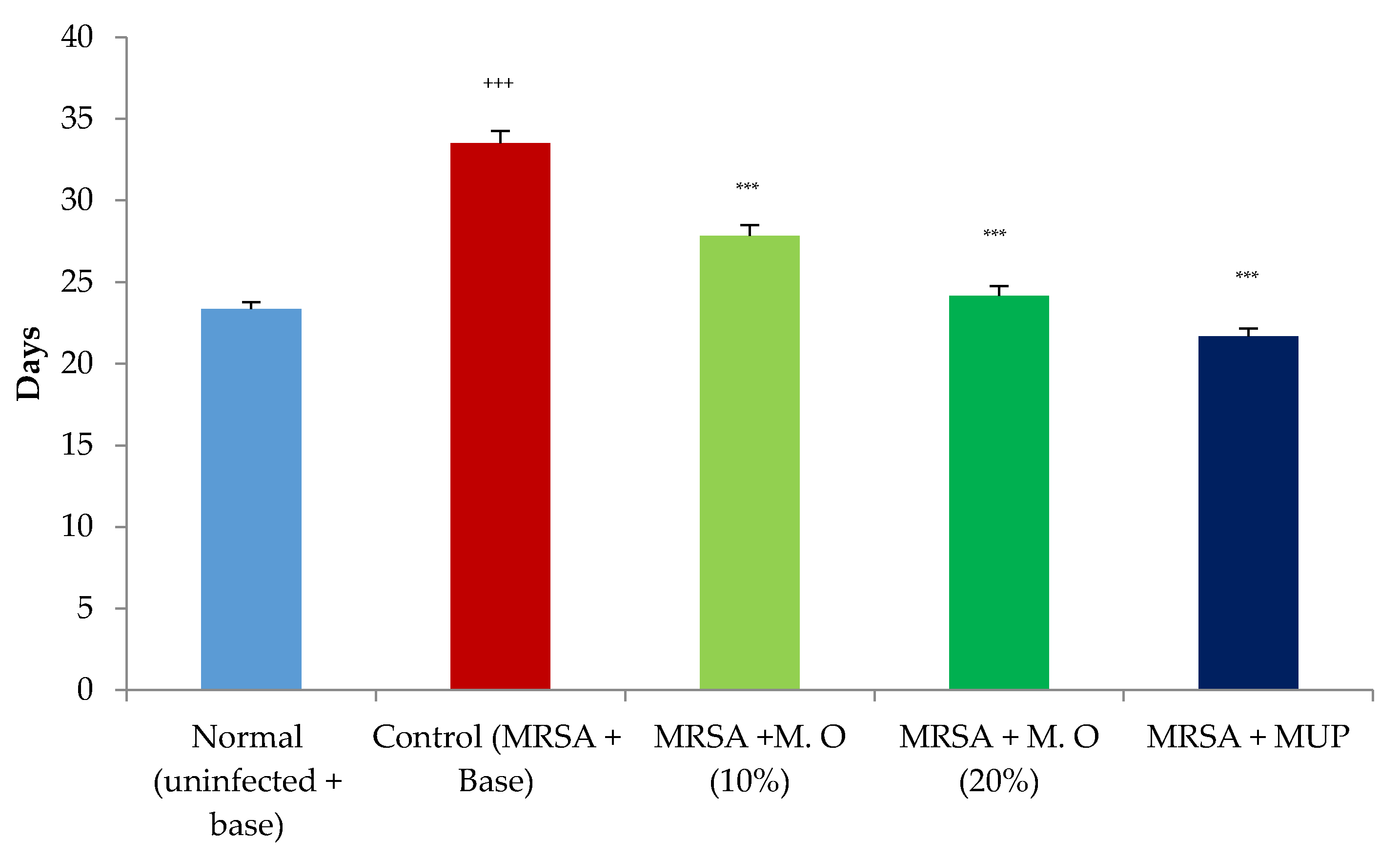



| Peak | Retention Time | Area | Area % | Name | Chemical Class |
|---|---|---|---|---|---|
| 1. | 6.164 | 561,733 | 1.56 | Thymine | Nucleic acid |
| 2. | 7.153 | 737,325 | 2.05 | 4H-Pyran-4-one | Ketone |
| 3. | 8.320 | 260,314 | 0.72 | 1H-Pyrrole-2,5-dione | Aromatic compounds |
| 4. | 10.364 | 503,628 | 1.40 | 1-chloro-4-methoxy- | Organochloride |
| 5. | 10.864 | 251,139 | 0.70 | Carbanilonitrile | Nitriles |
| 6. | 11.219 | 1,812,161 | 5.04 | Benzeneacetonitrile | Nitriles |
| 7. | 11.486 | 2,201,783 | 6.13 | 1-Nitro-2-acetamido-1,2-dideoxy-d-mannitol | Sugar derivative |
| 8. | 11.853 | 267,585 | 0.74 | 2(4H)-Benzofuranone | Terpene |
| 9. | 12.764 | 291,739 | 0.81 | Tricyclo [4.2.2.0(2,5)]dec-7-ene | Aromatic compound |
| 10. | 12.986 | 1,612,692 | 4.49 | n-Decanoic acid | Fatty acid derviative |
| 11. | 14.141 | 306,874 | 0.85 | 5-Ethylcyclopent-1-ene-1-carboxylic acid | Organic acid |
| 12. | 14.608 | 373,434 | 1.04 | 1-Methoxy-3-(2-hydroxyethyl)nonane | Alkane |
| 13. | 14.986 | 198,031 | 0.55 | Bicyclo [3.1.1]heptane | Alkane |
| 14. | 15.674 | 2,975,163 | 8.28 | n-Hexadecanoic acid | Fatty acid derivative |
| 15. | 15.941 | 232,175 | 0.65 | Nerol methyl ether | |
| 16. | 16.330 | 349,104 | 0.97 | Butanoic acid, 3-methylphenyl ester | Ester |
| 17. | 16.852 | 617,839 | 1.72 | Phytol | Alcohol |
| 18. | 17.085 | 2,433,077 | 6.77 | 9,12,15-Octadecatrienoic acid | Fatty acid derivative |
| 19 | 17.241 | 860,247 | 2.39 | Octadecanoic acid | Fatty acid derivative |
| 20. | 17.996 | 561,413 | 1.56 | Benzyl beta-d-glucoside | Glycoside |
| 21. | 18.774 | 320,095 | 0.89 | Nerolidyl acetate | Terpenoid |
| 22. | 19.640 | 11,188,937 | 31.13 | 1H-Indol-3-ol, acetate | Amino acid derivative |
| 23 | 19.707 | 858,357 | 2.39 | Hexadecanoic acid | Fatty acids derivative |
| 24. | 19.863 | 1,194,469 | 3.32 | Malonic acid | Organic acid |
| 25. | 20.063 | 2,649,088 | 7.37 | Quinoline | Alkaloid |
| 26. | 20.863 | 695,246 | 1.93 | Tritetracontane | Alkane |
| 27. | 21.007 | 210,785 | 0.59 | Octadecanoic acid | Fatty acids |
| 28. | 21.874 | 279,596 | 0.78 | 1-Pyrrolidinebutanoic acid | Amino acid derivative |
| 29. | 22.040 | 257,036 | 0.72 | Eicosane | Lipid |
| 30. | 23.684 | 880,180 | 2.45 | d- alpha -Tocopherol | Vitamin E derivative |
| Bacterial Pathogens | |||
|---|---|---|---|
| MRSA ATCC 43300 | P. aeruginosa ATCC 27853 | ||
| Zone of Inhibition (mm) | |||
| M.oleifera extract formulation (mg/mL) | 20 | 7 | 7 |
| 40 | 9 | 8 | |
| 80 | 13 | 12 | |
| Minimum inhibitory concentration (mg/mL) | 0.512 | 1.024 | |
| Minimum bactericidal concentration (mg/mL) | 1.024 | 2.048 | |
| Gene | Forward | Reverse |
|---|---|---|
| GAPDH | 5′CGGAGTCAACGGATTTGGTCGTAT3′ | 5′AGTCTTCTCCATGGTGGTGAAGAC3′ |
| TGF-β1 | 5′CTTCTCCACCAACTACTGCTTC3′ | 5′GGGTCCCAGGCAGAAGTT3′ |
| VEGF | 5′CTGGCCTGCAGACATCAAAGTGAG3′ | 5′CTTCCCGTTCTCAGCTCCACAAAC3′ |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Al-Ghanayem, A.A.; Alhussaini, M.S.; Asad, M.; Joseph, B. Moringa oleifera Leaf Extract Promotes Healing of Infected Wounds in Diabetic Rats: Evidence of Antimicrobial, Antioxidant and Proliferative Properties. Pharmaceuticals 2022, 15, 528. https://doi.org/10.3390/ph15050528
Al-Ghanayem AA, Alhussaini MS, Asad M, Joseph B. Moringa oleifera Leaf Extract Promotes Healing of Infected Wounds in Diabetic Rats: Evidence of Antimicrobial, Antioxidant and Proliferative Properties. Pharmaceuticals. 2022; 15(5):528. https://doi.org/10.3390/ph15050528
Chicago/Turabian StyleAl-Ghanayem, Abdullah A., Mohammed Sanad Alhussaini, Mohammed Asad, and Babu Joseph. 2022. "Moringa oleifera Leaf Extract Promotes Healing of Infected Wounds in Diabetic Rats: Evidence of Antimicrobial, Antioxidant and Proliferative Properties" Pharmaceuticals 15, no. 5: 528. https://doi.org/10.3390/ph15050528
APA StyleAl-Ghanayem, A. A., Alhussaini, M. S., Asad, M., & Joseph, B. (2022). Moringa oleifera Leaf Extract Promotes Healing of Infected Wounds in Diabetic Rats: Evidence of Antimicrobial, Antioxidant and Proliferative Properties. Pharmaceuticals, 15(5), 528. https://doi.org/10.3390/ph15050528






