Stage-Wise IoT Solutions for Alzheimer’s Disease: A Systematic Review of Detection, Monitoring, and Assistive Technologies
Abstract
1. Introduction
- Categorizing IoT interventions according to the stages of AD progression: early-stage cognitive assessments, mid-stage continuous activity monitoring, and late-stage assistive care;
- Analyzing technological enablers such as wearable sensors, smart home integration, remote monitoring platforms, and AI-driven cognitive evaluation systems;
- Identifying critical research gaps in interoperability, clinical adoption, scalability, data privacy, and the ethical deployment of IoT solutions within real-world clinical settings.
2. Scope of the Review
- Early detection, utilizing cognitive assessment tools and wearable sensors;
- Mild-stage management, including remote monitoring, memory aids, and fall detection systems;
- Severe-stage care, involving smart home automation, medication adherence systems, and patient safety through location tracking solutions.
- Scopus, using TITLE-ABS-KEY to restrict hits to titles, abstracts, and author keywords, reducing off-topic records;
- IEEE Xplore, Springer, MDPI, Wiley, and PubMed, using All Fields (or equivalent “All Metadata” scopes) to maximize sensitivity given varied indexing practices.
3. IoT at Different Stages of Alzheimer’s Disease
3.1. Early-Stage Detection and Diagnosis
3.1.1. IoT-Based Cognitive Assessment Tools
3.1.2. Wearable Sensors for Early Detection
3.2. Mild-Stage Management and Assistance
3.2.1. Remote Monitoring and Activity Tracking
3.2.2. IoT-Based Cognitive and Memory Aids
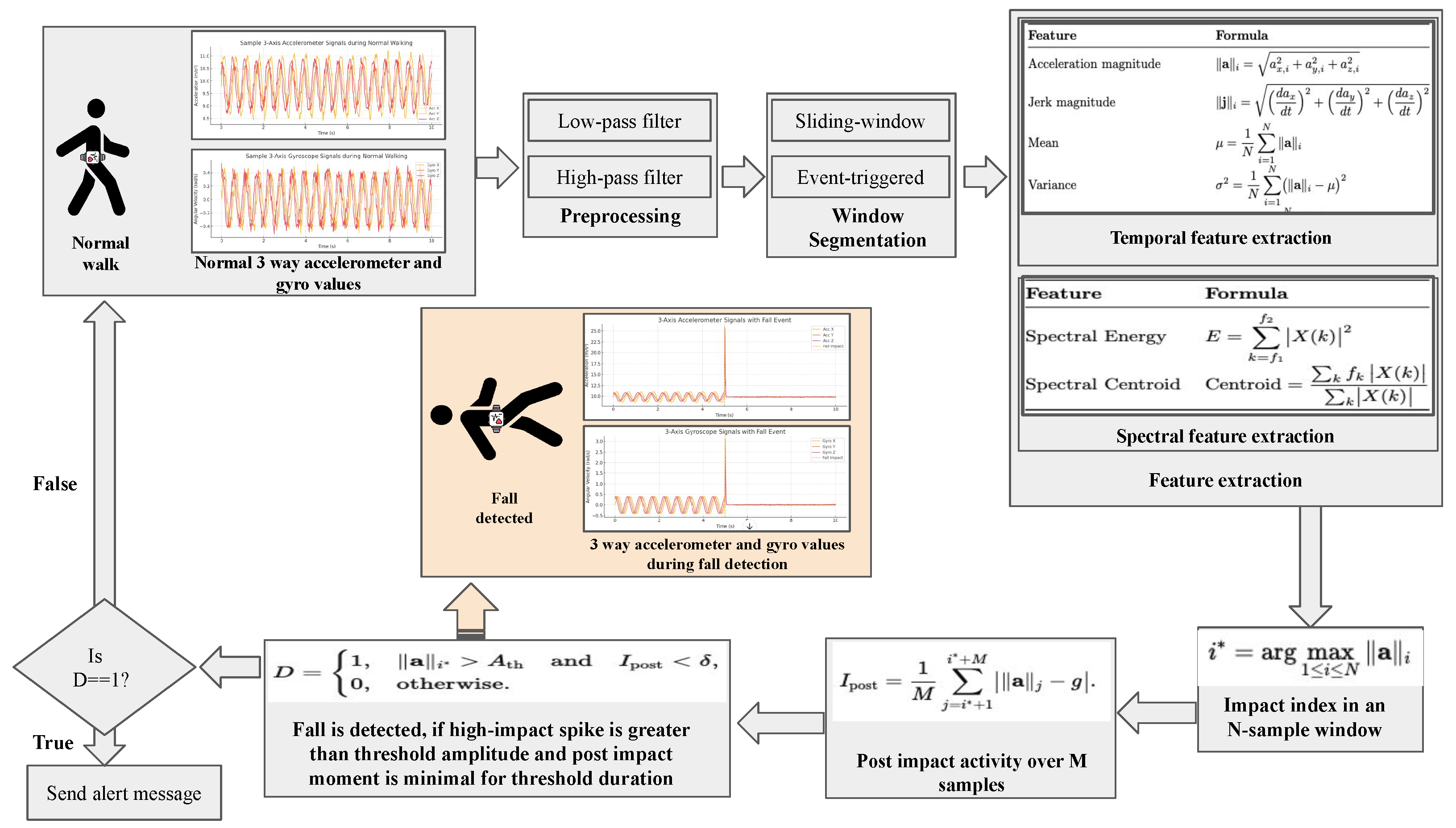
3.2.3. Fall Detection and Emergency Alerts
3.3. Severe-Stage Care and Supervision
3.3.1. IoT-Enabled Smart Home Systems
3.3.2. Automated Medication Reminders and Adherence Support
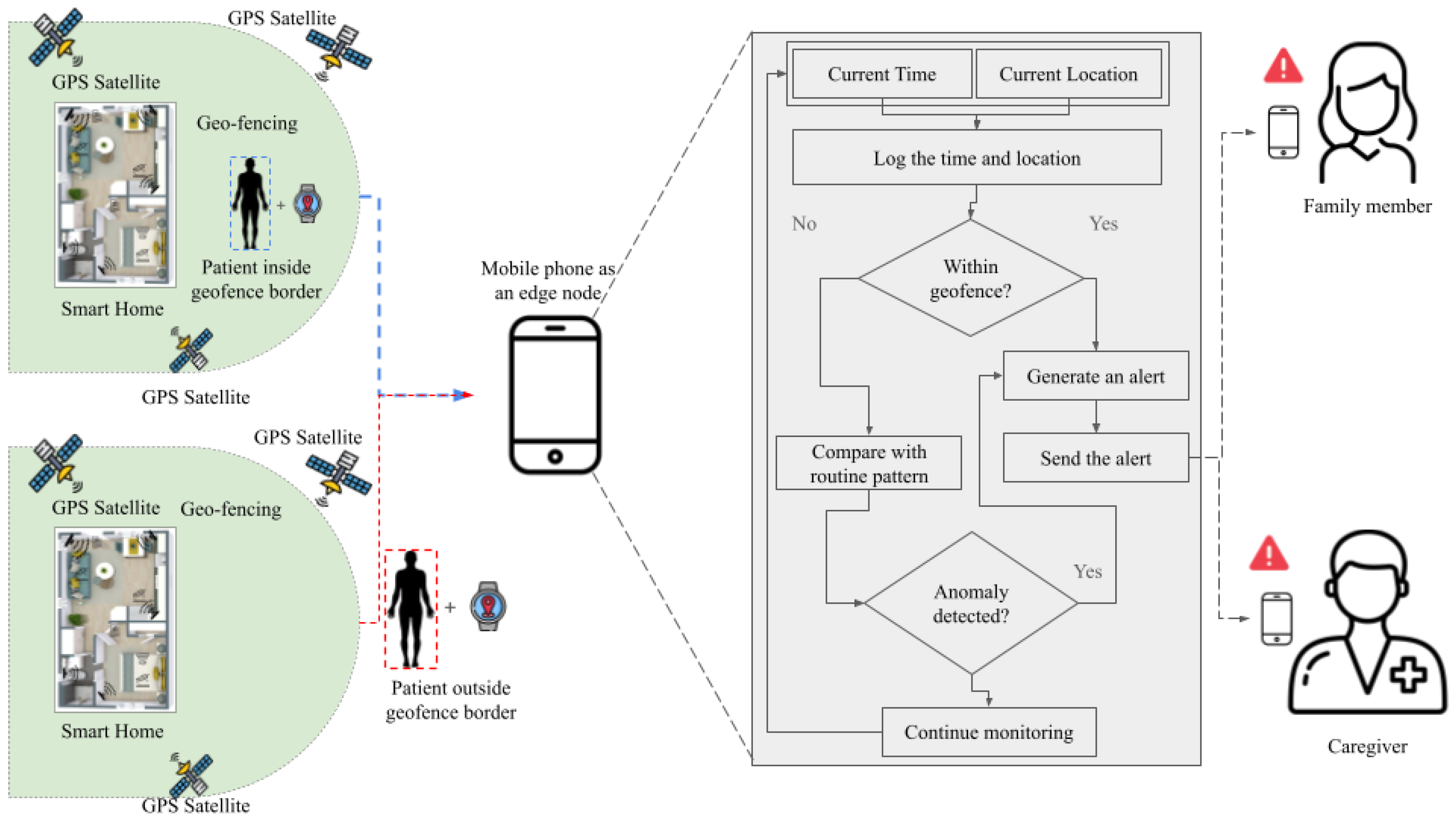
3.3.3. Location Tracking and Wandering Prevention
4. Discussion and Future Research Directions
4.1. Advancements in IoT for Early Diagnosis
4.2. Integration of AI with IoT for Personalized Treatment
4.3. Challenges and Ethical Considerations
4.4. Cost, Scalability, and LMIC Considerations
- Open-source hardware/software platforms: Leveraging Arduino and NodeMCU ecosystems reduces development costs and encourages local assembly and maintenance [233].
- Telecom partnerships: Collaborative agreements with mobile network operators can subsidize IoT data plans or piggyback on existing LPWAN networks, mitigating connectivity expenses [235].
- Low-power communication protocols: Adopting LPWAN standards (e.g., LoRaWAN and Sigfox) extends device lifetimes to multiple years on a single battery, drastically cutting maintenance and battery-replacement costs [236].
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| Acronym | Full Form |
| IoT | Internet of Things |
| AD | Alzheimer’s Disease |
| AI | Artificial Intelligence |
| RPM | Remote Patient Monitoring |
| ML | Machine Learning |
| PRISMA | Preferred Reporting Items for Systematic Reviews and Meta-Analyses |
| IoMT | Internet of Medical Things |
| EEG | Electroencephalogram |
| CL-ATBiLSTM | Convolutional Learning Attention-Bidirectional Time-Aware Long Short-Term Memory |
| CNN | Convolutional Neural Network |
| ADNI | Alzheimer’s Disease Neuroimaging Initiative |
| A | Amyloid Beta |
| MCI | Mild Cognitive Impairment |
| TUG | Timed Up and Go |
| MMSE | Mini-Mental State Examination |
| MDR | Micro-Doppler Radar |
| DB | Digital Biomarker |
| BCI | Brain–Computer Interface |
| CGM | Continuous Glucose Monitoring |
| T2DM | Type 2 Diabetes Mellitus |
| CNT-FET | Carbon Nanotube Field-Effect Transistor |
| CSF | Cerebrospinal Fluid |
| PET | Positron Emission Tomography |
| SVM | Support Vector Machine |
| RMSE | Root Mean Square Error |
| QMRA | Quantum Magnetic Resonance Analysis |
| WBAN | Wireless Body Area Network |
| IoRT | Internet of Robotic Things |
| DBN | Deep Belief Network |
| MOA | Mayfly Optimization Algorithm |
| BLE | Bluetooth Low Energy |
| LoRa | Long Range (communication protocol) |
| EMBC | Engineering in Medicine and Biology Conference |
| LSTM | Long Short-Term Memory |
| HAR | Human Activity Recognition |
| AUROC | Area Under the Receiver Operating Characteristic Curve |
| NIRF | Near-Infrared Fluorescence |
| LFA | Lateral Flow Assay |
| DBs | Digital Biomarkers |
| OLED | Organic Light-Emitting Diode |
| OPD | Organic Photodiode |
| HRP | Horseradish Peroxidase |
| TDP-43 | TAR DNA-Binding Protein 43 |
| NfL | Neurofilament Light |
| p-Tau | Phosphorylated Tau |
| t-Tau | Total Tau |
| HIPAA | Health Insurance Portability and Accountability Act |
| GDPR | General Data Protection Regulation |
| CCPA | California Consumer Privacy Act |
References
- GBD 2019 Dementia Forecasting Collaborators. Estimation of the global prevalence of dementia in 2019 and forecasted prevalence in 2050: An analysis for the Global Burden of Disease Study 2019. Lancet Public Health 2022, 7, e105–e125. [Google Scholar] [CrossRef]
- Jack, C.R.J.; Bennett, D.A.; Blennow, K.; Carrillo, M.C.; Dunn, B.; Haeberlein, S.B.; Holtzman, D.M.; Jagust, W.; Jessen, F.; Karlawish, J.; et al. NIA-AA Research Framework: Toward a biological definition of Alzheimer’s disease. Alzheimer’s Dement. 2018, 14, 535–562. [Google Scholar] [CrossRef]
- Jack, C.R.; Therneau, T.M.; Lundt, E.S.; Wiste, H.J.; Mielke, M.M.; Knopman, D.S.; Graff-Radford, J.; Lowe, A.J.; Vemuri, P.; Schwarz, C.G.; et al. Long-term associations between amyloid positron emission tomography, sex, apolipoprotein E and incident dementia and mortality among individuals without dementia: Hazard ratios and absolute risk. Brain Commun. 2022, 4, fcac017. [Google Scholar] [CrossRef]
- Horimoto, A.R.V.R.; Blue, E.; Grinde, K.; Nafikov, R.A.; Sohi, H.; Nato, A.Q.; Bis, J.C.; Brusco, L.I.; Morelli, L.; Ramirez, A.; et al. Admixture mapping implicates 13q33.3 as ancestry-of-origin locus for Alzheimer disease in Hispanic and Latino populations. HGG Adv. 2023, 4, 100207. [Google Scholar] [CrossRef]
- Leonard, H.L. Multi-ancestry meta-analysis and fine-mapping in Alzheimer’s disease. Mol. Psychiatry 2023, 28, 3121–3132. [Google Scholar] [CrossRef]
- Manly, J.J.; Jones, R.N.; Langa, K.M.; Ryan, L.H.; Levine, D.; McCammon, R.J.; Heeringa, S.G.; Weir, D. Estimating the Prevalence of Dementia and Mild Cognitive Impairment in the US: The 2016 Health and Retirement Study Harmonized Cognitive Assessment Protocol Project. JAMA Neurol. 2022, 79, 1242. [Google Scholar] [CrossRef] [PubMed]
- Yang, J.J.; Keohane, L.M.; Pan, X.F.; Qu, R.; Shu, X.O.; Lipworth, L.; Braun, K.; Steinwandel, M.; Dai, Q.; Shrubsole, M.J.; et al. Association of Healthy Lifestyles with Risk of Alzheimer Disease and Related Dementias in Low-Income Black and White Americans. Neurology 2022, 99, e944–e953. [Google Scholar] [CrossRef] [PubMed]
- Yu, D.; Yang, J.J.; Keohane, L.M.; Shu, X.O.; Lipworth, L.; Braun, K.; Dai, Q.; Steinwandel, M.; Shrubsole, M.J.; Zheng, W.; et al. Healthy Lifestyles and the Risk of Alzheimer’s Disease and Related Dementias among Low-Income Black and White Americans. Curr. Dev. Nutr. 2022, 6, 967. [Google Scholar] [CrossRef]
- Brookmeyer, R.; Johnson, E.; Ziegler-Graham, K.; Arrighi, H.M. Forecasting the global burden of Alzheimer’s disease. Alzheimer’s Dement. 2007, 3, 186–191. [Google Scholar] [CrossRef]
- Rajan, K.B.; Weuve, J.; Barnes, L.L.; McAninch, E.A.; Wilson, R.S.; Evans, D.A. Population estimate of people with clinical Alzheimer’s disease and mild cognitive impairment in the United States (2020–2060). Alzheimer’s Dement. 2021, 17, 1966–1975. [Google Scholar] [CrossRef]
- Mahendran, S.R.; Priya, H.A.G.; Mohsen, K.S.; Khan, M.S.; Obaid, A.J.; Shareef, A.M. IoT-based Health Monitoring System with AI-Powered Disease Prediction. In Proceedings of the 2024 IEEE 13th International Conference on Communication Systems and Network Technologies (CSNT), Jabalpur, India, 6–7 April 2024. [Google Scholar] [CrossRef]
- Singla, D.; Kumar, S.; Dhingra, D.; Ghandhi, A. Blockchain-powered Healthcare: Revolutionizing Security and Privacy in IoT-based Systems. In Proceedings of the 2024 International Conference on Computational Intelligence and Computing Applications (ICCICA), Samalkha, India, 23–24 May 2024; Volume 1, pp. 375–380. [Google Scholar] [CrossRef]
- Conduah, A.K.; Ofoe, S.; Siaw-Marfo, D. Data privacy in healthcare: Global challenges and solutions. Digit. Health 2025, 11, 20552076251343959. [Google Scholar] [CrossRef] [PubMed]
- Esquer-Rochin, M.; Rodríguez, L.F.; Gutiérrez-García, J.O. The Internet of Things in Dementia: A Systematic Review. Internet Things 2023, 22, 100824. [Google Scholar] [CrossRef]
- Taimoor, N.; Rehman, S. Reliable and Resilient AI and IoT-based Personalised Healthcare Services: A Survey. IEEE Access 2022, 10, 535–563. [Google Scholar] [CrossRef]
- Williamson, S.M.; Prybutok, V. Balancing Privacy and Progress: A Review of Privacy Challenges, Systemic Oversight, and Patient Perceptions in AI-Driven Healthcare. Appl. Sci. 2024, 14, 675. [Google Scholar] [CrossRef]
- Hajla, S.E.; Ennaji, E.M.; Maleh, Y.; Mounir, S. Security Challenges and Solutions in IoT; Advances in Computational Intelligence and Robotics Book Series; IGI Global Scientific Publishing: Hershey, PA, USA, 2024; pp. 25–50. [Google Scholar] [CrossRef]
- Sivan, R.; Zukarnain, Z.A. Security and Privacy in Cloud-Based E-Health System. Symmetry 2021, 13, 742. [Google Scholar] [CrossRef]
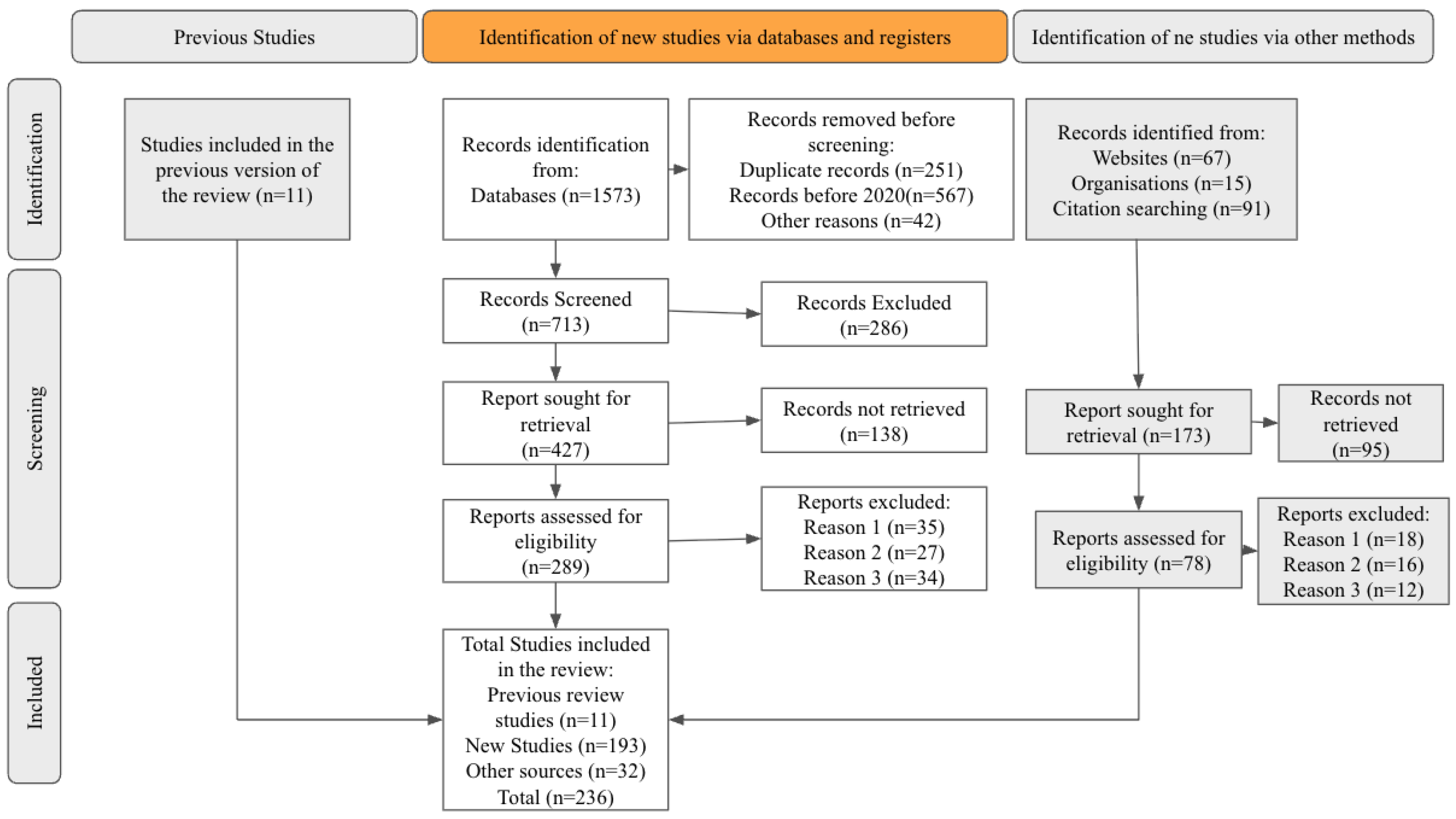
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; Group, P. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef]
- Sheikhtaheri, A.; Sabermahani, F. Applications and Outcomes of Internet of Things for Patients with Alzheimer’s Disease/Dementia: A Scoping Review. Biomed. Res. Int. 2022, 2022, 6274185. [Google Scholar] [CrossRef]
- Stavropoulos, T.G.; Papastergiou, A.; Mpaltadoros, L.; Nikolopoulos, S.; Kompatsiaris, I. IoT Wearable Sensors and Devices in Elderly Care: A Literature Review. Sensors 2020, 20, 2826. [Google Scholar] [CrossRef]
- Cote, A.C.; Phelps, R.J.; Kabiri, N.S.; Bhangu, J.S.; Thomas, K.K. Evaluation of Wearable Technology in Dementia: A Systematic Review and Meta-Analysis. Front. Med. 2021, 7, 501104. [Google Scholar] [CrossRef]
- Shaik, M.A.; Anik, F.I.; Hasan, M.M.; Chakravarty, S.; Ramos, M.D.; Rahman, M.A.; Ahamed, S.I.; Sakib, N. Advancing Remote Monitoring for Patients with Alzheimer Disease and Related Dementias: Systematic Review. JMIR Aging 2025, 8, e69175. [Google Scholar] [CrossRef]
- Hastie, T.; Tibshirani, R.; Friedman, J. The Elements of Statistical Learning: Data Mining, Inference, and Prediction, 2nd ed.; Springer: New York, NY, USA, 2009. [Google Scholar] [CrossRef]
- Bishop, C.M. Pattern Recognition and Machine Learning, 1st ed.; Information Science and Statistics; Springer: New York, NY, USA, 2006; p. 778. [Google Scholar]
- Fawcett, T. An Introduction to ROC Analysis. Pattern Recognit. Lett. 2006, 27, 861–874. [Google Scholar] [CrossRef]
- Xie, K.; Huang, J.; Chen, T.; Li, D.; Xia, T.; Chu, M.; Cui, Y.; Tang, M.; Peng, D.; Wang, J.; et al. A mobile interactive cognitive self-assessment scale for screening cognitive impairment due to Alzheimer’s disease. Age Ageing 2025, 54, afae293. [Google Scholar] [CrossRef] [PubMed]
- Berron, D.; Glanz, W.; Clark, L.; Basche, K.; Grande, X.; Billette, O.V.; Teipel, S.; Jessen, F.; Düzel, E. A remote digital memory composite to detect cognitive impairment in memory clinic samples in unsupervised settings using mobile devices. npj Digit. Med. 2024, 7, 79. [Google Scholar] [CrossRef] [PubMed]
- Sunderaraman, P.; De Anda-Duran, I.; Karjadi, C.; Peterson, J.; Ding, H.; Devine, S.A.; Shih, L.C.; Popp, Z.; Low, S.; Hwang, P.H. Design and feasibility analysis of a smartphone-based digital cognitive assessment study in the Framingham Heart Study. J. Am. Heart Assoc. 2024, 13, e031348. [Google Scholar] [CrossRef] [PubMed]
- Jacobs, D.M.; Peavy, G.M.; Banks, S.J.; Gigliotti, C.; Little, E.A.; Salmon, D.P. A survey of smartphone and interactive video technology use by participants in Alzheimer’s disease research: Implications for remote cognitive assessment. Alzheimer’s Dement. 2021, 13, e12188. [Google Scholar] [CrossRef]
- Fristed, E.; Skirrow, C.; Meszaros, M.; Lenain, R.; Meepegama, U.; Cappa, S.F.; Aarsland, D.; Weston, J. A remote speech-based AI system to screen for early Alzheimer’s disease via smartphones. Alzheimer’s Dement. 2022, 14, e12366. [Google Scholar] [CrossRef]
- Silva-Spínola, A.; Baldeiras, I.; Arrais, J.P.; Santana, I. The Road to Personalized Medicine in Alzheimer’s Disease: The Use of Artificial Intelligence. Biomedicines 2022, 10, 315. [Google Scholar] [CrossRef]
- Liu, Q.; Vaci, N.; Koychev, I.; Kormilitzin, A.; Li, Z.; Cipriani, A.; Nevado-Holgado, A.J. Personalised treatment for cognitive impairment in dementia: Development and validation of an artificial intelligence model. BMC Med. 2022, 20, 45. [Google Scholar] [CrossRef]
- Ziyad, S.R.; Alharbi, M.; Altulyan, M.S. Artificial Intelligence Model for Alzheimer’s Disease Detection with Convolution Neural Network for Magnetic Resonance Images. J. Alzheimer’s Dis. 2023, 93, 235–245. [Google Scholar] [CrossRef]
- Vanderlip, C.R.; Stark, C.E.L.; Initiative, A.D.N. Digital cognitive assessments as low-burden markers for predicting future cognitive decline and tau accumulation across the Alzheimer’s spectrum. Alzheimer’s Dement. 2024, 20, 6881–6895. [Google Scholar] [CrossRef]
- Rhodius-Meester, H.; Paajanen, T.; Lötjönen, J. cCOG Web-Based Cognitive Assessment Tool. In Biomarkers for Alzheimer’s Disease Drug Development; Methods in Molecular Biology; Perneczky, R., Ed.; Humana: New York, NY, USA, 2024; Volume 2785. [Google Scholar] [CrossRef]
- AlQahtani, N.G.; Alam, S.; Aqeel, I.; Shuaib, M.; Malibari, A. Deep Belief Networks (DBN) with IoT-Based Alzheimer’s Disease Detection and Classification. Appl. Sci. 2023, 13, 7833. [Google Scholar] [CrossRef]
- Mikolaizak, A.S.; Rochester, L.; Maetzler, W.; Sharrack, B.; Demeyer, H.; Mazzà, C.; Caulfield, B.; Garcia-Aymerich, J.; Vereijken, B.; Arnera, V.; et al. Connecting real-world digital mobility assessment to clinical outcomes for regulatory and clinical endorsement—The Mobilise-D study protocol. PLoS ONE 2022, 17, e0269615. [Google Scholar] [CrossRef]
- Perumal, T.; Wolfer, A.; Veloso, M.; Kurniawan, I.T.; Aponte, E.A.; Keita, G.; Hagenbuch, N.; Shi, B.; Orfaniotou, F.; Colell, M.G.V.; et al. Convergent and clinical validity of a remote smartphone-based self-assessment of cognition, function, and behavior in early Alzheimer’s disease. Alzheimer’s Dement. 2023, 19, e077236. [Google Scholar] [CrossRef]
- Diggin, S.; Alexander-Sefre, A.; Murphy, B.; Nolan, H.; Rowe, J.B.; Rueda-Delgado, L.M.; Buick, A.R. A longitudinal real-world study in patients with Alzheimer’s Disease dementia using frequent multi-domain digital measurements performed at-home on the Cumulus Neuroassessment Platform: Usability and feasibility findings. Alzheimer’s Dement. 2024, 20, e094325. [Google Scholar] [CrossRef]
- Khosravi, M.; Parsaei, H.; Rezaee, K. Fusing convolutional learning and attention-based Bi-LSTM networks for early Alzheimer’s diagnosis from EEG signals towards IoMT. Sci. Rep. 2024, 14, 26002. [Google Scholar] [CrossRef]
- Sonia, S.V.E.; Mustare, N.B.; Sailaja, V.; Sunitha, P. IoT-Enabled Alzheimer Disease Detection: A Convolutional Encoder-Decoder Approach Enhanced by Alpine Skiing Optimization. In Proceedings of the 2024 Second International Conference on Intelligent Cyber Physical Systems and Internet of Things (ICoICI), Coimbatore, India, 28–30 August 2024; pp. 386–391. [Google Scholar] [CrossRef]
- Sathish, R.; Muthukumar, R.; Dhivya, K.; Karthikkumar, S. Deep Learning and IoT-Enabled Framework for Accurate Classification and Monitoring of Alzheimer’s Disease Based on EEG Signal Analysis. In Proceedings of the 2025 Fifth International Conference on Advances in Electrical, Computing, Communication and Sustainable Technologies (ICAECT), Bhilai, India, 9–10 January 2025; pp. 1–8. [Google Scholar] [CrossRef]
- Tarekegn, A.N.; Sajjad, M.; Cheikh, F.A.; Ullah, M.; Muhammad, K. Efficient Human Gait Activity Recognition Based on Sensor Fusion and Intelligent Stacking Framework. IEEE Sens. J. 2023, 23, 28355–28369. [Google Scholar] [CrossRef]
- Greco, D.; Masulli, F.; Rovetta, S.; Cabri, A.; Daffonchio, D. A Cost-Effective Eye-Tracker for Early Detection of Mild Cognitive Impairment. In Proceedings of the 2022 IEEE 21st Mediterranean Electrotechnical Conference (MELECON), Palermo, Italy, 14–16 June 2022; pp. 1141–1146. [Google Scholar] [CrossRef]
- Al-Rowaili, B.; Al-Obaidli, N.; Al-Marri, D.; Abualsaud, K.; Yaacoub, E. Fall Detection Wristband with Optimized Security and Health Monitoring. In Proceedings of the 2024 International Wireless Communications and Mobile Computing (IWCMC), Ayia Napa, Cyprus, 27–31 May 2024; pp. 697–702. [Google Scholar] [CrossRef]
- Chen, H. Design of Intelligent Positioning Shoes for Elderly Fall Monitoring Based on GPS and MPU-6000 Acceleration Sensor. In Proceedings of the 2022 International Conference on Wearables, Sports and Lifestyle Management (WSLM), Kunming, China, 14–16 January 2022; pp. 43–46. [Google Scholar] [CrossRef]
- Jeon, Y.; Kang, J.; Kim, B.C.; Lee, K.H.; Song, J.I.; Gwak, J. Early Alzheimer’s Disease Diagnosis Using Wearable Sensors and Multilevel Gait Assessment: A Machine Learning Ensemble Approach. IEEE Sens. J. 2023, 23, 10041–10053. [Google Scholar] [CrossRef]
- Jamshed, M.; Shahzad, A.; Riaz, F.; Kim, K. Exploring inertial sensor-based balance biomarkers for early detection of mild cognitive impairment. Sci. Rep. 2024, 14, 9829. [Google Scholar] [CrossRef]
- Yin, Y.; Wang, H.; Liu, S.; Sun, J.; Jing, P.; Liu, Y. Internet of Things for Diagnosis of Alzheimer’s Disease: A Multimodal Machine Learning Approach Based on Eye Movement Features. IEEE Internet Things J. 2023, 10, 11476–11485. [Google Scholar] [CrossRef]
- Huang, S.; Hou, X.; Liu, Y.; Shang, P.; Luo, J.; Lv, Z.; Zhang, W.; Lin, B.; Huang, Q.; Tao, S.; et al. Diagnostic accuracy of multi-component spatial-temporal gait parameters in older adults with amnestic mild cognitive impairment. Front. Hum. Neurosci. 2022, 16, 911607. [Google Scholar] [CrossRef]
- Dieffenderfer, J.; Brewer, A.; Noonan, M.A.; Smith, M.; Eichenlaub, E.; Haley, K.L.; Jacks, A.; Lobaton, E.; Neupert, S.D.; Hess, T.M.; et al. A Wearable System for Continuous Monitoring and Assessment of Speech, Gait, and Cognitive Decline for Early Diagnosis of ADRD. In Proceedings of the 2023 45th Annual International Conference of the IEEE Engineering in Medicine & Biology Society (EMBC), Sydney, Australia, 24–27 July 2023; pp. 1–6. [Google Scholar] [CrossRef]
- Wang, W.; Chen, J.; Hu, Y.; Liu, H.; Chen, J.; Gadekallu, T.R.; Garg, L.; Guizani, M.; Hu, X. Integration of Artificial Intelligence and Wearable Internet of Things for Mental Health Detection. Int. J. Cogn. Comput. Eng. 2024, 5, 307–315. [Google Scholar] [CrossRef]
- Massoud, M.A.; El-Bouridy, M.E.; Ahmed, W.A. Revolutionizing Alzheimer’s detection: An advanced telemedicine system integrating Internet-of-Things and convolutional neural networks. Neural Comput. Appl. 2024, 36, 16411–16426. [Google Scholar] [CrossRef]
- Kaye, J.; Marcoe, J.; Mar, A.; Hanna, E.; Pierce, A.; Silbert, L.; Shang, Y.; Schwartz, D.; Gothard, S.; Mattek, N.; et al. DETECT-AD (Digital Evaluations and Technologies Enabling Clinical Translation for Alzheimer’s Disease): A simulated anti-amyloid clinical trial using digital biomarkers as primary outcome measures. Alzheimer’s Dement. 2023, 19, e071888. [Google Scholar] [CrossRef]
- Karri, C.; Garg, L.; Prakash, V.; Pawar, B.D. Chapter 9—Healthcare 5.0 opportunities and challenges: A literature review. In Intelligent Biomedical Technologies and Applications for Healthcare 5.0; Garg, L., Mirajkar, G., Misra, S., Chattu, V.K., Eds.; Advances in Ubiquitous Sensing Applications for Healthcare; Academic Press: Cambridge, MA, USA, 2025; Volume 16, pp. 133–146. [Google Scholar] [CrossRef]
- Vo, D.K.; Trinh, K.T.L. Advances in Wearable Biosensors for Healthcare: Current Trends, Applications, and Future Perspectives. Biosensors 2024, 14, 560. [Google Scholar] [CrossRef]
- Sharma, A.; Badea, M.; Tiwari, S.; Marty, J.L. Wearable Biosensors: An Alternative and Practical Approach in Healthcare and Disease Monitoring. Molecules 2021, 26, 748. [Google Scholar] [CrossRef]
- Jain, D.K.; Srinivas, K.; Srinivasu, S.V.N.; Manikandan, R. Machine Learning-Based Monitoring System with IoT Using Wearable Sensors and Pre-Convoluted Fast Recurrent Neural Networks (P-FRNN). IEEE Sens. J. 2021, 21, 25517–25524. [Google Scholar] [CrossRef]
- Yang, G.; Pang, G.; Pang, Z.; Gu, Y.; Mäntysalo, M.; Yang, H. Non-Invasive Flexible and Stretchable Wearable Sensors with Nano-Based Enhancement for Chronic Disease Care. IEEE Rev. Biomed. Eng. 2019, 12, 34–71. [Google Scholar] [CrossRef]
- Shi, Q.; Yang, Y.; Sun, Z.; Lee, C. Progress of Advanced Devices and Internet of Things Systems as Enabling Technologies for Smart Homes and Health Care. ACS Mater. Sci. Au 2022, 2, 394–435. [Google Scholar] [CrossRef] [PubMed]
- Rhodus, E.; Onim, M.; Roberts, C.; Kumar, S.; Burhan, A.; Thapliyal, H. Utilization of Wearable Devices as Means for Remote Digital Biometric Data Collection in a Community-Based, Rural Randomized Controlled Trial among Alzheimer’s Disease Dyads. Alzheimer’s Dement. 2024, 20, e090883. [Google Scholar] [CrossRef]
- Butler, P.M.; Yang, J.; Brown, R.; Hobbs, M.; Becker, A.; Penalver-Andres, J.; Syz, P.; Muller, S.; Cosne, G.; Juraver, A.; et al. Smartwatch- and smartphone-based remote assessment of brain health and detection of mild cognitive impairment. Nat. Med. 2025, 31, 829–839. [Google Scholar] [CrossRef] [PubMed]
- Krizea, M.; Gialelis, J.; Protopsaltis, G.; Mountzouris, C.; Theodorou, G. Empowering People with a User-Friendly Wearable Platform for Unobtrusive Monitoring of Vital Physiological Parameters. Sensors 2022, 22, 5226. [Google Scholar] [CrossRef] [PubMed]
- Duan, H.; Peng, S.; He, S.; Tang, S.; Goda, K.; Wang, C.; Li, M. Wearable Electrochemical Biosensors for Advanced Healthcare Monitoring. Adv. Sci. 2024, 12, 2411433. [Google Scholar] [CrossRef]
- Erdem, A.; Eksin, E.; Senturk, H.; Yildiz, E.; Maral, M. Recent Developments in Wearable Biosensors for Healthcare and Biomedical Applications. TrAC Trends Anal. Chem. 2024, 171, 117510. [Google Scholar] [CrossRef]
- Bodily, T.A.; Ramanathan, A.; Wei, S.; Karkisaval, A.; Bhatt, N.; Jerez, C.; Haque, M.A.; Ramil, A.; Heda, P.; Wang, Y.; et al. In pursuit of degenerative brain disease diagnosis: Dementia biomarkers detected by DNA aptamer-attached portable graphene biosensor. Proc. Natl. Acad. Sci. USA 2023, 120, e2311565120. [Google Scholar] [CrossRef]
- Wang, J.; Lu, X.; He, Y. Electrochemical Technology for the Detection of Tau Proteins as a Biomarker of Alzheimer’s Disease in Blood. Biosensors 2025, 15, 85. [Google Scholar] [CrossRef]
- Phan, L.M.T.; Vo, T.A.T.; Pham, H.L.; Cho, S. Nanomaterial-based Optical and Electrochemical Biosensors for Amyloid-β and Tau: Potential for Early Diagnosis of Alzheimer’s Disease. Expert Rev. Mol. Diagn. 2021, 21, 175–193. [Google Scholar] [CrossRef]
- Liu, Y.; Huang, Z.; Xu, Q.; Zhang, L.; Liu, Q.; Xu, T. Portable electrochemical micro-workstation platform for simultaneous detection of multiple Alzheimer’s disease biomarkers. Mikrochim. Acta 2022, 189, 91. [Google Scholar] [CrossRef]
- Bocu, R. Extended Review Concerning the Integration of Electrochemical Biosensors into Modern IoT and Wearable Devices. Biosensors 2024, 14, 214. [Google Scholar] [CrossRef]
- Liu, Y.; Liu, X.; Li, M.; Liu, Q.; Xu, T. Portable Vertical Graphene@Au-Based Electrochemical Aptasensing Platform for Point-of-Care Testing of Tau Protein in the Blood. Biosensors 2022, 12, 564. [Google Scholar] [CrossRef] [PubMed]
- Li, M.; Zeng, Y.; Huang, Z.; Zhang, L.; Liu, Y. Vertical Graphene-Based Printed Electrochemical Biosensor for Simultaneous Detection of Four Alzheimer’s Disease Blood Biomarkers. Biosensors 2023, 13, 758. [Google Scholar] [CrossRef] [PubMed]
- Chakari-Khiavi, F.; Mirzaie, A.; Khalilzadeh, B.; Yousefi, H.; Abolhasan, R.; Kamrani, A.; Pourakbari, R.; Shahpasand, K.; Yousefi, M.; Rashidi, M.R. Application of Pt@ZIF-8 Nanocomposite-Based Electrochemical Biosensor for Sensitive Diagnosis of Tau Protein in Alzheimer’s Disease Patients. Sci. Rep. 2023, 13, 16163. [Google Scholar] [CrossRef] [PubMed]
- Ciou, S.H.; Hsieh, A.H.; Lin, Y.X.; Sei, J.L.; Govindasamy, M.; Kuo, C.F.; Huang, C.H. Sensitive Label-Free Detection of the Biomarker Phosphorylated Tau-217 Protein in Alzheimer’s Disease Using a Graphene-Based Solution-Gated Field Effect Transistor. Biosens. Bioelectron. 2023, 228, 115174. [Google Scholar] [CrossRef]
- Kong, Q.; Liu, C.; Zhang, Y.; He, Y.; Zhang, R.; Wang, Y.; Zhou, Q.; Cui, F. Nucleic Acid Aptamer-Based Electrochemical Sensor for the Detection of Serum P-tau231 and the Instant Screening Test of Alzheimer’s Disease. Mikrochim. Acta 2024, 191, 328. [Google Scholar] [CrossRef]
- Sempionatto, J.R.; Lasalde-Ramírez, J.A.; Mahato, K.; Wang, J.; Gao, W. Wearable chemical sensors for biomarker discovery in the omics era. Nat. Rev. Chem. 2022, 6, 899–915. [Google Scholar] [CrossRef] [PubMed]
- Mukasa, D.; Wang, M.Q.; Min, J.; Yang, Y.; Solomon, S.A.; Ye, C.; Gao, W. A Computationally Assisted Approach for Designing Wearable Biosensors toward Non-invasive Personalized Molecular Analysis. Adv. Mater. 2023, 35, 2212161. [Google Scholar] [CrossRef] [PubMed]
- Zhou, J.; Sun, Y.; Zhang, J.; Luo, F.; Ma, H.; Guan, M.; Feng, J.; Dong, X. Dumbbell Aptamer Sensor Based on Dual Biomarkers for Early Detection of Alzheimer’s Disease. ACS Appl. Mater. Interfaces 2023, 15, 16394–16407. [Google Scholar] [CrossRef]
- Phan, L.M.T.; Cho, S. Fluorescent Aptasensor and Colorimetric Aptablot for p-tau231 Detection: Toward Early Diagnosis of Alzheimer’s Disease. Adv. Cardiovasc. Dis. 2022, 10, 93. [Google Scholar] [CrossRef]
- Chen, H.; Xiao, M.; He, J.; Zhang, Y.; Liang, Y.; Liu, H.; Zhang, Z. Aptamer-Functionalized Carbon Nanotube Field-Effect Transistor Biosensors for Alzheimer’s Disease Serum Biomarker Detection. ACS Sens. 2022, 7, 2075–2083. [Google Scholar] [CrossRef]
- Beduk, T.; Beduk, D.; Hasan, M.R.; Guler Celik, E.; Kosel, J.; Narang, J.; Salama, K.N.; Timur, S. Smartphone-Based Multiplexed Biosensing Tools for Health Monitoring. Biosensors 2022, 12, 583. [Google Scholar] [CrossRef]
- Duan, S.; Cai, T.; Liu, F.; Li, Y.; Yuan, H.; Yuan, W.; Huang, K.; Hoettges, K.; Chen, M.; Lim, E.G.; et al. Automatic offline-capable smartphone paper-based microfluidic device for efficient biomarker detection of Alzheimer’s disease. Anal. Chim. Acta 2024, 1308, 342575. [Google Scholar] [CrossRef]
- Kazanskiy, N.L.; Butt, M.A.; Khonina, S.N. Recent Advances in Wearable Optical Sensor Automation Powered by Battery versus Skin-like Battery-Free Devices for Personal Healthcare—A Review. Nanomaterials 2022, 12, 334. [Google Scholar] [CrossRef]
- Sun, X.; Sun, X.; Wang, Q.; Wang, X.; Feng, L.; Yang, Y.; Jing, Y.; Yang, C.; Zhang, S. Biosensors toward behavior detection in diagnosis of Alzheimer’s disease. Front. Bioeng. Biotechnol. 2022, 10, 1031833. [Google Scholar] [CrossRef] [PubMed]
- Zheng, Z.; Zhu, R.; Peng, I.; Xu, Z.; Jiang, Y. Wearable and implantable biosensors: Mechanisms and applications in closed-loop therapeutic systems. J. Mater. Chem. B 2024, 12, 8577–8604. [Google Scholar] [CrossRef] [PubMed]
- Savoy, A.; Holden, R.J.; Groot, N.D.; Clark, D.O.; Sachs, G.A.; Klonoff, D.C.; Weiner, M.W. Improving Care for People Living with Dementia and Diabetes: Applying the Human-Centered Design Process to Continuous Glucose Monitoring. J. Diabetes Sci. Technol. 2022, 18, 201–206. [Google Scholar] [CrossRef] [PubMed]
- Ergin, B.; Gadsby-Davis, K.; Mattishent, K.; Dhatariya, K.; Garner, N.; Hornberger, M. Continuous Glucose Monitoring in Comorbid Dementia and Diabetes: The Evidence So Far. J. Diabetes Sci. Technol. 2024. [Google Scholar] [CrossRef]
- Carroll, C.M.; Constantino, N.J.; Irmen, R.E.; Snipes, J.A.; Benca, R.M.; Macauley, S.L. Peripheral glucose metabolism bidirectionally modulates sleep in a model of Alzheimer’s disease. Sleep 2023, 46, A38–A39. [Google Scholar] [CrossRef]
- Robert, J.J. Continuous monitoring of blood glucose. Horm. Res. Paediatr. 2002, 57, 81–84. [Google Scholar] [CrossRef]
- Hanna, J.; Bteich, M.; Tawk, Y.; Ramadan, A.; Dia, B.; Asadallah, F.A.; Eid, A.; Kanj, R.; Costantine, J.; Eid, A.A. Noninvasive, wearable, and tunable electromagnetic multisensing system for continuous glucose monitoring, mimicking vasculature anatomy. Sci. Adv. 2020, 6, eaba5320. [Google Scholar] [CrossRef]
- Hanna, J.; Tawk, Y.; Azar, S.; Ramadan, A.H.; Dia, B.; Shamieh, E.; Zoghbi, S.; Kanj, R.; Costantine, J.; Eid, A.A. Wearable flexible body matched electromagnetic sensors for personalized non-invasive glucose monitoring. Sci. Rep. 2022, 12, 14885. [Google Scholar] [CrossRef]
- Zhao, J.; Zhang, S.; Sun, Y.; Zhou, N.; Yu, H.; Zhang, H.; Jia, D. Wearable Optical Sensing in the Medical Internet of Things (MIoT) for Pervasive Medicine: Opportunities and Challenges. ACS Photonics 2022, 9, 2579–2599. [Google Scholar] [CrossRef]
- Dcosta, J.V.; Ochoa, D.; Sanaur, S. Recent Progress in Flexible and Wearable All Organic Photoplethysmography Sensors for SpO2 Monitoring. Adv. Sci. 2023, 10, 2302752. [Google Scholar] [CrossRef]
- Kulkarni, M.B.; Rajagopal, S.; Prieto-Simón, B.; Pogue, B.W. Recent advances in smart wearable sensors for continuous human health monitoring. Talanta 2024, 272, 125817. [Google Scholar] [CrossRef]
- Barata, J.J.R.; Munoz, R.; Silva, R.D.D.C.; Rodrigues, J.J.P.C.; de Albuquerque, V.H.C. Internet of Things Based on Electronic and Mobile Health Systems for Blood Glucose Continuous Monitoring and Management. IEEE Access 2019, 7, 175116–175125. [Google Scholar] [CrossRef]
- Safarkhani, M.; Aldhaher, A.; Heidari, G.; Zare, E.N.; Warkiani, M.E.; Akhavan, O.; Huh, Y.; Rabiee, N. Nanomaterial-assisted wearable glucose biosensors for noninvasive real-time monitoring: Pioneering point-of-care and beyond. Nano Mater. Sci. 2023, 6, 263–283. [Google Scholar] [CrossRef]
- Phillips, N.E.; Collet, T.H.; Naef, F. Uncovering personalized glucose responses and circadian rhythms from multiple wearable biosensors with Bayesian dynamical modeling. Cell Rep. Methods 2023, 3, 100545. [Google Scholar] [CrossRef]
- Sharma, S.; Dudeja, R.K.; Aujla, G.S.; Bali, R.S.; Kumar, N. DeTrAs: Deep Learning-based Healthcare Framework for IoT-based Assistance of Alzheimer Patients. Neural Comput. Appl. 2020. [Google Scholar] [CrossRef]
- Popp, Z.; Low, S.; Igwe, A.; Rahman, M.S.; Kim, M.; Khan, R.; Oh, E.; Kumar, A.; Anda-Duran, I.D.; Ding, H.; et al. Shifting From Active to Passive Monitoring of Alzheimer Disease: The State of the Research. J. Am. Heart Assoc. 2024, 13, e031247. [Google Scholar] [CrossRef]
- Creese, B.; Arnold, J.; McDermid, J.; Medina-Lara, A.; Ismail, Z.; Steer, Z. Protocol for an acceptability and feasibility study of sensor-instrumented SmartSocks® for use by people with dementia. Alzheimer’s Dement. 2024, 20, e086878. [Google Scholar] [CrossRef]
- Grammatikopoulou, M.; Lazarou, I.; Alepopoulos, V.; Mpaltadoros, L.; Oikonomou, V.; Stavropoulos, T.G.; Nikolopoulos, S.; Kompatsiaris, I.; Tsolaki, M. Assessing the cognitive decline of people in the spectrum of AD by monitoring their activities of daily living in an IoT-enabled smart home environment: A cross-sectional pilot study. Front. Aging Neurosci. 2024, 16, 1375131. [Google Scholar] [CrossRef] [PubMed]
- Javheri, R.; Patil, D.; Kamble, A.; Yadav, A.; Kolhe, P.; Mate, G.S. A Review: Smart Wristwear for Alzheimer Patients with an Advanced Tracking System. In Proceedings of the 2024 IEEE Region 10 Symposium (TENSYMP), New Delhi, India, 27–29 September 2024; pp. 1–6. [Google Scholar] [CrossRef]
- Mani, K.; Singh, K.K.; Litoriya, R. Transformative Potential IoT Sensor Frameworks for Real-Time Alzheimer’s Detection and Monitoring in Elderly Populations. In Proceedings of the 2024 International Conference on Advances in Computing Research on Science Engineering and Technology (ACROSET), Indore, India, 27–28 September 2024; pp. 1–8. [Google Scholar] [CrossRef]
- Muurling, M.M.; de Boer, R.; Kozak, R.; Lucivero, F.; Lancaster, C.; Hinds, C.; Stravopoulos, T.G.; Nikolopoulos, S.; Kompatsiaris, I.; Manyakov, N.V.; et al. Remote monitoring technologies in Alzheimer’s disease: Design of the RADAR-AD study. Alzheimer’s Res. Ther. 2021, 13, 89. [Google Scholar] [CrossRef] [PubMed]
- Muurling, M.; de Boer, C.; Hinds, C.; Atreya, A.; Doherty, A.; Alepopoulos, V.; Curcic, J.; Brem, A.-K.; Conde, P.; Kuruppu, S.; et al. Feasibility and usability of remote monitoring in Alzheimer’s disease. Digit. Health 2024, 10, 20552076241238133. [Google Scholar] [CrossRef] [PubMed]
- Patil, V.; Chikkoppa, B. Advanced Alzheimer’s IoT solution for Real-time Monitoring in Healthcare Services. In Proceedings of the 2022 International Conference for Advancement in Technology (ICONAT), Goa, India, 21–22 January 2022; pp. 1–7. [Google Scholar] [CrossRef]
- Cardinali, L.; Mariano, V.; Rodriguez-Duarte, D.O.; Tobón Vasquez, J.A.; Scapaticci, R.; Crocco, L.; Vipiana, F. Early Detection of Alzheimer’s Disease via Machine Learning-Based Microwave Sensing: An Experimental Validation. Sensors 2025, 25, 2718. [Google Scholar] [CrossRef]
- David, M.C.B.; Kolanko, M.; Del Giovane, M.; Lai, H.; True, J.; Beal, E.; Li, L.M.; Nilforooshan, R.; Barnaghi, P.; Malhotra, P.A.; et al. Remote monitoring of physiology in people living with dementia: An observational cohort study. JMIR Aging 2023, 6, e43777. [Google Scholar] [CrossRef]
- Rawtaer, I.; Mahendran, S.R.; Kua, E.H.; Tan, H.P.; Tan, H.X.; Lee, T.S.; Ng, T.P. Early Detection of Mild Cognitive Impairment with In-Home Sensors to Monitor Behavior Patterns in Community-Dwelling Senior Citizens in Singapore: Cross-Sectional Feasibility Study. J. Med. Internet Res. 2020, 22, e16854. [Google Scholar] [CrossRef]
- Au-Yeung, W.T.M.; Miller, L.; Beattie, Z.; May, R.; Cray, H.V.; Kabelac, Z.; Katabi, D.; Kaye, J.A.; Vahia, I.V. Feasibility of deploying home-based digital technology, environmental sensors, and web-based surveys for assessing behavioral symptoms and identifying their precipitants in older adults: Longitudinal, observational study. JMIR Form. Res. 2024, 8, e53192. [Google Scholar] [CrossRef]
- Ford, C.T.; Galler, J.A.; He, Y.; Young, C.; Simpson, B.G.K.; Wu, C.; Pfaffenroth, J.; Wah, E.S.; Arnold, S.E.; Dodge, H.H.; et al. Using Apple Watches to Monitor Health and Behaviors of Individuals with Cognitive Impairment: A Case Series Study. J. Gerontol. A Biol. Sci. Med. Sci. 2025, 80, glae250. [Google Scholar] [CrossRef]
- Salehi, W.; Gupta, G.; Bhatia, S.; Koundal, D.; Mashat, A.A.; Belay, A. IoT-Based Wearable Devices for Patients Suffering from Alzheimer Disease. Contrast Media Mol. Imaging 2022, 2022, 3224939. [Google Scholar] [CrossRef] [PubMed]
- Chokri, R.; Hanini, W.; Daoud, W.B.; Chelloug, S.A.; Makhlouf, A.M. Secure IoT Assistant-Based System for Alzheimer’s Disease. IEEE Access 2022, 10, 44305–44314. [Google Scholar] [CrossRef]
- Shahzad, A.; Dadlani, A.; Lee, H.; Kim, K. Automated Prescreening of Mild Cognitive Impairment Using Shank-Mounted Inertial Sensors Based Gait Biomarkers. IEEE Access 2022, 10, 15835–15844. [Google Scholar] [CrossRef]
- Park, J.; Lee, H.J.; Park, J.S.; Won, S.H.; Bae, J.B.; Han, J.W.; Kim, K.W. Development of a Gait Feature–Based Model for Classifying Cognitive Disorders Using a Single Wearable Inertial Sensor. Neurology 2023, 101, e12–e19. [Google Scholar] [CrossRef] [PubMed]
- Cherachapridi, P.; Wachiraphan, P.; Rangpong, P.; Kiatthaveephong, S.; Kongwudhikunakorn, S.; Thanontip, K.; Piriyajitakonkij, M.; Chinkamol, A.; Likitvanichkul, C.; Dujada, P.; et al. Prescreening MCI and Dementia Using Shank-Mounted IMU During TUG Task. IEEE Sens. J. 2022, 22, 24550–24558. [Google Scholar] [CrossRef]
- Wu, T.; Lure, F.; Chen, V.C. STRIDE: Systematic Radar Intelligence Analysis for ADRD Risk Evaluation with Gait Signature Simulation and Deep Learning. IEEE Sens. J. 2023, 23, 10998–11006. [Google Scholar] [CrossRef]
- Jing, Y.; Qin, P.; Fan, X.; Wencheng, Z.; Sun, W.; Tian, F.; Wang, D. Deep Learning–Assisted Gait Parameter Assessment for Neurodegenerative Diseases: Model Development and Validation. J. Med. Internet Res. 2023, 25, e46427. [Google Scholar] [CrossRef]
- Seifallahi, M.; Galvin, J.E.; Ghoraani, B. Detection of mild cognitive impairment using various types of gait tests and machine learning. Front. Neurol. 2024, 15, 1354092. [Google Scholar] [CrossRef]
- Choi, A.; Kim, T.H.; Yuhai, O.; Jeong, S.; Kim, K.; Kim, H.; Mun, J.H. Deep Learning-Based Near-Fall Detection Algorithm for Fall Risk Monitoring System Using a Single Inertial Measurement Unit. IEEE Trans. Neural Syst. Rehabil. Eng. 2022, 30, 2385–2394. [Google Scholar] [CrossRef]
- Agrawal, D.K.; Usaha, W.; Pojprapai, S.; Wattanapan, P. Fall Risk Prediction Using Wireless Sensor Insoles with Machine Learning. IEEE Access 2023, 11, 23119–23126. [Google Scholar] [CrossRef]
- Li, Z.; Zhu, J.; Liu, J.; Shi, M.; Liu, P.; Guo, J.; Hu, Z.; Liu, S.; Yang, D. Using dual-task gait to recognize Alzheimer’s disease and mild cognitive impairment: A cross-sectional study. Front. Hum. Neurosci. 2023, 17, 1284805. [Google Scholar] [CrossRef]
- Munteanu, D.; Bejan, C.; Munteanu, N.A.; Zamfir, C.; Vasić, M.; Petrea, S.M.; Cristea, D.S. Deep-Learning-Based System for Assisting People with Alzheimer’s Disease. Electronics 2022, 11, 3229. [Google Scholar] [CrossRef]
- Onthoni, D.D.; Sahoo, P.K. Artificial-Intelligence-Assisted Activities of Daily Living Recognition for Elderly in Smart Home. Electronics 2022, 11, 4129. [Google Scholar] [CrossRef]
- Gao, H.; Zhou, L.; Kim, J.Y.; Li, Y.; Huang, W. The Behavior Guidance and Abnormality Detection for A-MCI Patients under Wireless Sensor Network. ACM Trans. Sens. Netw. 2022, 19, 1–24. [Google Scholar] [CrossRef]
- Chimamiwa, G.; Giaretta, A.; Alirezaie, M.; Pecora, F.; Loutfi, A. Are Smart Homes Adequate for Older Adults with Dementia? Sensors 2022, 22, 4254. [Google Scholar] [CrossRef]
- Khodabandehloo, E.; Alimohammadi, A.; Riboni, D. FreeSia: A Cyber-physical System for Cognitive Assessment through Frequency-domain Indoor Locomotion Analysis. ACM Trans. Cyber-Phys. Syst. 2022, 6, 1–31. [Google Scholar] [CrossRef]
- Cantone, A.A.; Esposito, M.; Perillo, F.P.; Romano, M.; Sebillo, M.; Vitiello, G. Enhancing Elderly Health Monitoring: Achieving Autonomous and Secure Living through the Integration of Artificial Intelligence, Autonomous Robots, and Sensors. Electronics 2023, 12, 3918. [Google Scholar] [CrossRef]
- Mathunjwa, B.M.; Kor, R.Y.J.; Ngarnkuekool, W.; Hsu, Y.L. A Comprehensive Review of Home Sleep Monitoring Technologies: Smartphone Apps, Smartwatches, and Smart Mattresses. Sensors 2025, 25, 1771. [Google Scholar] [CrossRef] [PubMed]
- Gamel, S.A.; Talaat, F.M. SleepSmart: An IoT-enabled continual learning algorithm for intelligent sleep enhancement. Neural Comput. Appl. 2024, 36, 4293–4309. [Google Scholar] [CrossRef]
- Blackman, J.; Morrison, H.; Gabb, V.; Biswas, B.; Turner, N.; Jolly, A.; Trender, W.; Hampshire, A.; Whone, A.; Coulthard, E. Remote evaluation of sleep to enhance understanding of early dementia due to Alzheimer’s Disease (RESTED-AD): An observational cohort study protocol. BMC Geriatr. 2023, 23, 590. [Google Scholar] [CrossRef]
- Kolanko, M.; Soreq, E.; Golemme, M.; Walsh, C.; Giovane, M.D.; Sharp, D. Digital biomarkers of sleep and nocturnal behaviour derived from contactless longitudinal sleep monitoring predict cognitive decline and deterioration in daily function in people living with dementia. Alzheimer’s Dement. 2024, 20, e091826. [Google Scholar] [CrossRef]
- Griffiths, T.L.; McCreedy, E.; Reddy, A. Sleep in focus: Evaluating wearable biometric devices for dementia sleep monitoring- a scoping review of efficacy. Innov. Aging 2024, 8, 1275. [Google Scholar] [CrossRef]
- Tian, Y.J.; Felber, N.A.; Pageau, F.; Roulet Schwab, D.; Wangmo, T. Benefits and barriers associated with the use of smart home health technologies in the care of older persons: A systematic review. BMC Geriatr. 2024, 24, 152. [Google Scholar] [CrossRef] [PubMed]
- Islam, M.R.; Kabir, M.M.; Mridha, M.F.; Alfarhood, S.; Safran, M.; Che, D. Deep Learning-Based IoT System for Remote Monitoring and Early Detection of Health Issues in Real-Time. Sensors 2023, 23, 5204. [Google Scholar] [CrossRef]
- Jiang, Y.; Wang, J. Technological Innovations and Data-Driven Support for Older Adults. JMIR Aging 2023, 6, e48547. [Google Scholar] [CrossRef]
- Scullin, M.K.; Jones, W.E.; Phenis, R.; Beevers, S.; Rosen, S.; Dinh, K.; Kiselica, A.M.; Keefe, F.J.; Benge, J.F. Using smartphone technology to improve prospective memory functioning: A randomized controlled trial. J. Am. Geriatr. Soc. 2022, 70, 459–469. [Google Scholar] [CrossRef]
- Liu, C.L.; Chuang, C.J.; Chou, C.M. A Pilot Fuzzy System with Virtual Reality for Mild Cognitive Impairment (MCI) Assessment. Healthcare 2023, 11, 2503. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.J.; Jeong, S.Y.; Kang, S.J. Knowledge-Based Remote E-Coaching Framework Using IoT Devices for In-Home ADL Rehabilitation Treatment of Degenerative Brain Disease Patients. Sensors 2022, 22, 7957. [Google Scholar] [CrossRef] [PubMed]
- Salai, A.M.; Kirton, A.; Cook, G.; Holmquist, L.E. Views and experiences on the use of voice assistants by family and professionals supporting people with cognitive impairments. Front. Dement. 2022, 1, 1049464. [Google Scholar] [CrossRef] [PubMed]
- Machado, S.D.; Tavares, J.E.d.R.; Martins, M.G.; Barbosa, J.L.V.; González, G.V.; Leithardt, V.R.Q. Ambient intelligence based on IoT for assisting people with Alzheimer’s disease through context histories. Electronics 2021, 10, 1260. [Google Scholar] [CrossRef]
- Ghorbani, F.; Ahmadi, A.; Kia, M.; Rahman, Q.; Delrobaei, M. A Decision-Aware Ambient Assisted Living System with IoT Embedded Device for In-Home Monitoring of Older Adults. Sensors 2023, 23, 2673. [Google Scholar] [CrossRef]
- Zhu, K.; Zhang, Q.; He, B.; Huang, M.; Lin, R.; Li, H. Immersive Virtual Reality-Based Cognitive Intervention for the Improvement of Cognitive Function, Depression, and Perceived Stress in Older Adults with Mild Cognitive Impairment and Mild Dementia: Pilot Pre-Post Study. JMIR Serious Games 2022, 10, e32117. [Google Scholar] [CrossRef]
- Mao, Q.; Zhao, Z.; Yu, L.; Zhao, Y.; Wang, H. The Effects of Virtual Reality–Based Reminiscence Therapies for Older Adults with Cognitive Impairment: Systematic Review. J. Med. Internet Res. 2024, 26, e53348. [Google Scholar] [CrossRef]
- Dubbelman, M.; Hall, T.C.; Levesque, I.M.; Mimmack, K.J.; Sikkes, S.A.M.; Fischer, S.H.; Rentz, D.M.; Sperling, R.A.; Papp, K.V.; Amariglio, R.E.; et al. Using a digital tool to detect early changes in everyday functioning in older adults: A pilot study of the Assessment of Smartphone Everyday Tasks (ASSET). Alzheimer’s Dement. Diagn. Assess. Dis. Monit. 2023, 15, e12506. [Google Scholar] [CrossRef]
- Smith, A.M.; Marin, A.; DeCaro, R.E.; Feinn, R.; Wack, A.; Hughes, G.I.; Rivard, N.; Umashankar, A.; Turk, K.W.; Budson, A.E. Algorithmic Spaced Retrieval Enhances Long-Term Memory in Alzheimer Disease: Case-Control Pilot Study. JMIR Form. Res. 2024, 8, e51943. [Google Scholar] [CrossRef]
- Mahesh, G.; Kalidas, M. A Real-Time IoT Based Fall Detection and Alert System for Elderly. In Proceedings of the 2023 International Conference on Advances in Computation, Communication and Information Technology (ICAICCIT), Faridabad, India, 23–24 November 2023; pp. 327–331. [Google Scholar] [CrossRef]
- Abhishek, A.P.N.; T, A.G.C.; V, B.H.; Kanithan, S. Smart Biomedical Assisted System for Alzheimer Patient. In Proceedings of the 2023 7th International Conference on Design Innovation for 3 Cs Compute Communicate Control (ICDI3C), Karnataka, India, 2 November 2023; pp. 132–136. [Google Scholar] [CrossRef]
- Guamán-Egas, J.; Castro-Martin, A.P. Fall Detection with Artificial Intelligence and IoT Health Monitoring System. In Proceedings of the 2023 IEEE Seventh Ecuador Technical Chapters Meeting (ECTM), Ambato, Ecuador, 10–13 October 2023; pp. 1–6. [Google Scholar] [CrossRef]
- Syamlan, M.A.; Noor, R.A.M.; S., A.S.F.; Syamlan, M.A.; Arifin, A.; Pramudijanto, J.; Arrofiqi, F. Fuzzy Logic-Based Fall Detection System for Elderly Using a Single Inertial Measurement Unit. In Proceedings of the 2024 International Conference on Computer Engineering, Network, and Intelligent Multimedia (CENIM), Surabaya, Indonesia, 19–20 November 2024; pp. 1–5. [Google Scholar] [CrossRef]
- Al-Naami, B.; Abu Owida, H.; Abu Mallouh, M.; Al-Naimat, F.; Agha, M.; Al-Hinnawi, A.R. A New Prototype of Smart Wearable Monitoring System Solution for Alzheimer’s Patients. Med. Devices 2021, 14, 423–433. [Google Scholar] [CrossRef] [PubMed]
- Tibrewal, V. Fall Detection in Alzheimers Disease Patients using Machine Learning, Integrated with a Wrist-Wrap Design and Mobile App. Int. J. Electr. Eng. Technol. 2021, 12, 32–42. [Google Scholar] [CrossRef]
- Lin, H.C.; Chen, M.J.; Lee, C.H.; Kung, L.C.; Huang, J.T. Fall Recognition Based on an IMU Wearable Device and Fall Verification through a Smart Speaker and the IoT. Sensors 2023, 23, 5472. [Google Scholar] [CrossRef] [PubMed]
- Mishra, S.; Ngangbam, B.; Raj, S.; Pradhan, N.R. CURA: Real Time Artificial Intelligence and IoT based Fall Detection Systems for patients suffering from Dementia. EAI Endorsed Trans. Pervasive Health Technol. 2023, 9. [Google Scholar] [CrossRef]
- Al-Kababji, A.; Amira, A.; Bensaali, F.; Jarouf, A.; Shidqi, L.; Djelouat, H. An IoT-based framework for remote fall monitoring. Biomed. Signal Process. Control 2021, 67, 102532. [Google Scholar] [CrossRef]
- Karar, M.E.; Shehata, H.I.; Reyad, O. A survey of IoT-based fall detection for aiding elderly care: Sensors, methods, challenges and future trends. Appl. Sci. 2022, 12, 3276. [Google Scholar] [CrossRef]
- Lee, C.-W.; Chuang, H.-M. Design of a seniors and Alzheimer’s disease caring service platform. BMC Med. Inform. Decis. Mak. 2021, 21, 273. [Google Scholar] [CrossRef]
- Ambient Monitoring of Gait and Machine Learning Models for Dynamic and Short-Term Falls Risk Assessment in People with Dementia. IEEE J. Biomed. Health Inform. 2023, 27, 3599–3609. [CrossRef]
- Belmin, J.; Villani, P.; Gay, M.; Fabries, S.; Havreng-Théry, C.; Malvoisin, S.; Denis, F.; Veyron, J.H. Real-world Implementation of an eHealth System Based on Artificial Intelligence Designed to Predict and Reduce Emergency Department Visits by Older Adults: Pragmatic Trial. J. Med. Internet Res. 2022, 24, e40387. [Google Scholar] [CrossRef]
- Tiersen, F.; Batey, P.; Harrison, M.J.C.; Naar, L.; Serban, A.I.; Daniels, S.J.C.; Calvo, R.A. Smart Home Sensing and Monitoring in Households with Dementia: User-Centered Design Approach. JMIR Aging 2021, 4, e27047. [Google Scholar] [CrossRef]
- Davidoff, H.; Kraaij, A.V.; den Bulcke, L.V.; Lutin, E.; Vandenbulcke, M.; Helleputte, N.V.; Vos, M.D.; Hoof, C.V.; Bossche, M.V.D. Physiological Profiling of Agitation in Dementia: Insights From Wearable Sensor Data. Innov. Aging 2024, 8, igae057. [Google Scholar] [CrossRef]
- Javed, A.R.; Fahad, L.G.; Farhan, A.A.; Abbas, S.; Srivastava, G.; Parizi, R.M.; Khan, M.S. Automated cognitive health assessment in smart homes using machine learning. Sustain. Cities Soc. 2021, 65, 102572. [Google Scholar] [CrossRef]
- Palermo, F.; Chen, Y.; Capstick, A.; Fletcher-Loyd, N.; Walsh, C.; Kouchaki, S.; True, J.; Balazikova, O.; Soreq, E.; Scott, G.; et al. TIHM: An open dataset for remote healthcare monitoring in dementia. Sci. Data 2023, 10, 606. [Google Scholar] [CrossRef]
- Lee, M.; Mishra, R.K.; Momin, A.; El-Refaei, N.; Bagheri, A.B.; York, M.K.; Kunik, M.E.; Derhammer, M.; Fatehi, B.; Lim, J.; et al. Smart-Home Concept for Remote Monitoring of Instrumental Activities of Daily Living (IADL) in Older Adults with Cognitive Impairment: A Proof of Concept and Feasibility Study. Sensors 2022, 22, 6745. [Google Scholar] [CrossRef]
- Arthanat, S.; Wilcox, J.; LaRoche, D. Smart home automation technology to support caring of individuals with Alzheimer’s disease and related dementia: An early intervention framework. Disabil. Rehabil. Assist. Technol. 2022, 19, 779–789. [Google Scholar] [CrossRef]
- Sharanya, C.; S, K.; T. R, R.S. Pill Dispenser for Elderly Care using IOT. In Proceedings of the 2024 4th Asian Conference on Innovation in Technology (ASIANCON), Pimpri Chinchwad, India, 23–25 August 2024; pp. 1–4. [Google Scholar] [CrossRef]
- Peddisetti, V.; Kandregula, P.K.; John, J.A.; Poomdla, S.; George, K.; Panangadan, A. Smart Medication Management: Enhancing Medication Adherence with an IoT-Based Pill Dispenser and Smart Cup. In Proceedings of the 2024 IEEE First International Conference on Artificial Intelligence for Medicine, Health and Care (AIMHC), Laguna Hills, CA, USA, 5–7 February 2024; pp. 137–144. [Google Scholar] [CrossRef]
- Kamil, R.J.; Bakar, D.; Ehrenburg, M.; Wei, E.X.; Pletnikova, A.; Xiao, G.; Oh, E.S.; Mancini, M.; Agrawal, Y. Detection of Wandering Behaviors Using a Body-Worn Inertial Sensor in Patients with Cognitive Impairment: A Feasibility Study. Front. Neurol. 2021, 12, 529661. [Google Scholar] [CrossRef] [PubMed]
- Hsu, Y.L.; Chung, P.C.; Wang, W.H.; Pai, M.C.; Wang, C.Y.; Lin, C.W. Gait and balance analysis for patients with Alzheimer’s disease using an inertial-sensor-based wearable instrument. IEEE J. Biomed. Health Inform. 2014, 18, 1822–1830. [Google Scholar] [CrossRef] [PubMed]
- El-Gohary, M.; Pearson, S.; McNames, J.; Mancini, M.; Horak, F. Continuous monitoring of turning in patients with movement disability. Sensors 2013, 14, 356–369. [Google Scholar] [CrossRef] [PubMed]
- Howes, J.; Denier, Y.; Gastmans, C. Electronic Tracking Devices for People with Dementia: Content Analysis of Company Websites. JMIR Aging 2022, 5, e38865. [Google Scholar] [CrossRef]
- H L, G.; Flammini, F.; Srividhya, S.; M L, C.; Selvam, S. Computer Science Engineering: Proceedings of the 1st International Conference on Computing and Intelligent Information Systems (ICCIIS 2024), Bangalore, India, 19–20 April 2024, 1st ed.; CRC Press: Bangalore, India, 2024; Volume 2. [Google Scholar] [CrossRef]
- Bonilla, V.; Campoverde, B.; Yoo, S.G. A Systematic Literature Review of LoRaWAN: Sensors and Applications. Sensors 2023, 23, 8440. [Google Scholar] [CrossRef]
- Ponnuviji, N.P.; Elangovan, G.; Sujatha, K.; Ganesan, I.; Lalitha, S.D. IoT-Enabled Assistive Technologies Approach for Personalized Geriatric Health Monitoring and Safety. In Future of AI in Biomedicine and Biotechnology; Khade, S.M., Mishra, R.G., Eds.; IGI Global: Hershey, PA, USA, 2024; pp. 125–146. [Google Scholar] [CrossRef]
- Parameshwaran; Khan, V.; Gopi, B.; H, D.R.C. Intelligent Device for Monitoring the Dementia Patients in Real Time using IoT Technology. In Proceedings of the 2022 International Conference on Power, Energy, Control and Transmission Systems (ICPECTS), Chennai, India, 8–9 December 2022; pp. 1–3. [Google Scholar] [CrossRef]
- Nandini, B.P.; Reddy, P.; Mary, G.I.; Julian, A.; R., R.; Rele, M. Smart Watch with Machine Learning Based Fall Detection System. In Proceedings of the 2024 IEEE Region 10 Symposium (TENSYMP), New Delhi, India, 27–29 September 2024; pp. 1–7. [Google Scholar] [CrossRef]
- Adardour, H.; Hadjila, M.; Irid, S.; Baouch, T.; Belkhiter, S.E. Outdoor Alzheimer’s Patients Tracking Using an IoT System and a Kalman Filter Estimator. Wirel. Pers. Commun. 2021, 116, 249–265. [Google Scholar] [CrossRef]
- Li, W.; Du, Z. Research on spatial design method of rehabilitation environment based on behavioral characteristics of Alzheimer’s disease patients. In Proceedings of the 2020 International Conference on Innovation Design and Digital Technology (ICIDDT), Zhenjing, China, 5–6 December 2020; pp. 213–216. [Google Scholar] [CrossRef]
- Oliveira, R.; Feres, R.; Barreto, F.; Abreu, R. CNN for Elderly Wandering Prediction in Indoor Scenarios. SN Comput. Sci. 2022, 3, 230. [Google Scholar] [CrossRef]
- Akaike, H.; Katsuta, S.I.; Aramaki, S.; Moshnyaga, V.; Hashimoto, K.; Ikeda, S. Wandering Notification System for Caregivers of People with Dementia. In Proceedings of the 2022 IEEE 65th International Midwest Symposium on Circuits and Systems (MWSCAS), Fukuoka, Japan, 7–10 August 2022; pp. 1–2. [Google Scholar] [CrossRef]
- Oskouei, R.J.; MousaviLou, Z.; Bakhtiari, Z.; Jalbani, K.B. IoT-Based Healthcare Support System for Alzheimer’s Patients. Wirel. Commun. Mob. Comput. 2020, 2020, 8822598. [Google Scholar] [CrossRef]
- Kanchanamala, P.; Chippada, R.; Bennabatthula, T.; Muppidi, S. AI-Powered Alzheimer’s Care: Smart Face Recognition, Medicine Reminders, and Location. In Proceedings of the 2024 IEEE North Karnataka Subsection Flagship International Conference (NKCon), Bagalkote, India, 21–22 September 2024; pp. 1–8. [Google Scholar] [CrossRef]
- Doyle, M.; Nwofe, E.S.; Rooke, C.; Seelam, K.; Porter, J.; Bishop, D. Implementing global positioning system trackers for people with dementia who are at risk of wandering. Dementia 2024, 23, 964–980. [Google Scholar] [CrossRef]
- Cullen, A.; Mazhar, M.K.A.; Smith, M.D.; Lithander, F.E.; Ó Breasail, M.; Henderson, E.J. Wearable and Portable GPS Solutions for Monitoring Mobility in Dementia: A Systematic Review. Sensors 2022, 22, 3336. [Google Scholar] [CrossRef] [PubMed]
- Jafarpournaser, N.; Delavar, M.R.; Noroozian, M. A Wandering Detection Method Based on Processing GPS Trajectories Using the Wavelet Packet Decomposition Transform for People with Cognitive Impairment. ISPRS Int. J. Geo-Inf. 2023, 12, 379. [Google Scholar] [CrossRef]
- Wang, W.H.; Hsu, W.S. Integrating Artificial Intelligence and Wearable IoT System in Long-Term Care Environments. Sensors 2023, 23, 5913. [Google Scholar] [CrossRef]
- Iaboni, A.; Spasojevic, S.; Newman, K.; Schindel Martin, L.; Wang, A.; Ye, B.; Mihailidis, A.; Khan, S.S. Wearable multimodal sensors for the detection of behavioral and psychological symptoms of dementia using personalized machine learning models. Alzheimer’s Dement. 2022, 14, e12305. [Google Scholar] [CrossRef]
- Mitrovska, A.; Safari, P.; Ritter, K.; Shariati, B.; Fischer, J.K. Secure federated learning for Alzheimer’s disease detection. Front. Aging Neurosci. 2024, 16, 1324032. [Google Scholar] [CrossRef]
- Timon, C.M.; Hussey, P.; Lee, H.; Murphy, C.; Rai, H.V.; Smeaton, A.F. Automatically detecting activities of daily living from in-home sensors as indicators of routine behaviour in an older population. Digit. Health 2023, 9, 20552076231184084. [Google Scholar] [CrossRef] [PubMed]
- Chung, J.; Pretzer-Aboff, I.; Parsons, P.; Falls, K.; Bulut, E. Using a Device-Free Wi-Fi Sensing System to Assess Daily Activities and Mobility in Low-Income Older Adults: Protocol for a Feasibility Study. JMIR Res. Protoc. 2024, 13, e53447. [Google Scholar] [CrossRef] [PubMed]
- Ouyang, X.; Shuai, X.; Li, Y.; Pan, L.; Zhang, X.; Fu, H.; Cheng, S.; Wang, X.; Cao, S.; Xin, J.; et al. ADMarker: A Multi-Modal Federated Learning System for Monitoring Digital Biomarkers of Alzheimer’s Disease. In MobiCom ’24: Proceedings of the 30th Annual International Conference on Mobile Computing and Networking, Washington, DC, USA, 18–22 November 2024; ACM: New York, NY, USA, 2024; pp. 404–419. [Google Scholar] [CrossRef]
- Hussain, M.; Shiren, Y. Identifying Alzheimer Disease Dementia Levels Using Machine Learning Methods. Med. Res. Arch. 2023, 11. [Google Scholar] [CrossRef]
- Alayba, A.M.; Senan, E.M.; Alshudukhi, J.S. Enhancing Early Detection of Alzheimer’s Disease through Hybrid Models Based on Feature Fusion of Multi-CNN and Handcrafted Features. Sci. Rep. 2024, 14, 31203. [Google Scholar] [CrossRef]
- Arunachalam, R.; Sunitha, G.; Shukla, S.K.; Nath Pandey, S.; Urooj, S.; Rawat, S. A smart Alzheimer’s patient monitoring system with IoT-assisted technology through enhanced deep learning approach. Knowl. Inf. Syst. 2023, 65, 5561–5599. [Google Scholar] [CrossRef]
- Mascret, Q.; Gagnon-Turcotte, G.; Bielmann, M.; Fall, C.L.; Bouyer, L.J.; Gosselin, B. A Wearable Sensor Network with Embedded Machine Learning for Real-Time Motion Analysis and Complex Posture Detection. IEEE Sens. J. 2022, 22, 7868–7876. [Google Scholar] [CrossRef]
- Mohammad, Z.; Anwary, A.R.; Mridha, M.F.; Shovon, M.S.H.; Vassallo, M. An Enhanced Ensemble Deep Neural Network Approach for Elderly Fall Detection System Based on Wearable Sensors. Sensors 2023, 23, 4774. [Google Scholar] [CrossRef]
- Hussain, A.; Sheikh, Z.; Subramanian, M.L. The Eye as a Diagnostic Tool for Alzheimer’s Disease. Life 2023, 13, 726. [Google Scholar] [CrossRef]
- Salobrar-García, E. Value of the Retina in the Diagnosis of Alzheimer’s Disease. Acta Ophthalmol. 2022, 100, S275. [Google Scholar] [CrossRef]
- Leuenberger, R.C.; Verbraak, F.D.; Twisk, J.W.R.; de Ruyter, F.J.H.; Hoozemans, J.J.; de Boer, J.F.; Bouwman, F.H. Development of Retinal Biomarkers for Alzheimer’s Disease. Alzheimer’s Dement. 2022, 18, e063836. [Google Scholar] [CrossRef]
- Hao, J.; Kwapong, W.R.; Shen, T.; Fu, H.; Xu, Y.; Lu, Q.; Liu, S.; Zhang, J.; Liu, Y.; Zhao, Y.; et al. Early detection of dementia through retinal imaging and trustworthy AI. npj Digit. Med. 2024, 7, 294. [Google Scholar] [CrossRef]
- Shi, X.H.; Ju, L.; Dong, L.; Zhang, R.H.; Shao, L.; Yan, Y.N.; Wang, Y.X.; Fu, X.F.; Chen, Y.Z.; Ge, Z.Y.; et al. Deep Learning Models for the Screening of Cognitive Impairment Using Multimodal Fundus Images. Ophthalmol. Retin. 2024, 8, 666–677. [Google Scholar] [CrossRef]
- Cheung, C.Y.; Ran, A.R.; Wang, S.; Chan, V.T.T.; Sham, K.; Hilal, S.; Venketasubramanian, N.; Cheng, C.Y.; Sabanayagam, C.; Tham, Y.C.; et al. A deep learning model for detection of Alzheimer’s disease based on retinal photographs: A retrospective, multicentre case-control study. Lancet Digit. Health 2022, 4, e806–e815. [Google Scholar] [CrossRef]
- Vrahatis, A.G.; Skolariki, K.; Krokidis, M.G.; Exarchos, T.P.; Vlamos, P. Revolutionizing the Early Detection of Alzheimer’s Disease through Non-Invasive Biomarkers: The Role of Artificial Intelligence and Deep Learning. Sensors 2023, 23, 4184. [Google Scholar] [CrossRef]
- Hui, H.Y.; Ran, A.; Cheung, C.Y. Deep Reinforcement Learning-Based Retinal Imaging in Alzheimer’s Disease: Potential and Perspectives. J. Alzheimer’s Dis. 2023, 94, 39–50. [Google Scholar] [CrossRef]
- Fernandez, G.; Mendez, L.; Lopera, F.; Parra-Rodriguez, M.A. The Eye as a Biomarker for Alzheimer’s Disease: Oculomotor Behaviours Yield a Novel Digital Biomarker for Preclinical Risk Detection. Alzheimer’s Dement. 2022, 18, e066784. [Google Scholar] [CrossRef]
- Liu, Y.; Zhuang, D.; Wang, J.; Huang, H.; Li, R.; Wu, C.; Deng, Y.; Hu, G.; Guo, B. Recent Advances in Small Molecular Near-Infrared Fluorescence Probes for a Targeted Diagnosis of the Alzheimer Disease. Analyst 2022, 147, 4701–4723. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Ni, W.; Jin, D.; Yu, Y.; Xiao, M.; Zhang, Z.; Zhang, G.J. Nanosensor-Driven Detection of Neuron-Derived Exosomal Aβ42 with Graphene Electrolyte-Gated Transistor for Alzheimer’s Disease Diagnosis. Anal. Chem. 2023, 95, 5719–5728. [Google Scholar] [CrossRef] [PubMed]
- Jyothi, E.V.N.; Sailaja, S.; Reddy, M.S.L.; Sunitha, T. Automated Health Monitoring: Integrating AI and IoT for Continuous Patient Observation. In Proceedings of the 2024 International Conference on IoT Based Control Networks and Intelligent Systems (ICICNIS), Bengaluru, India, 17–18 December 2024; pp. 519–524. [Google Scholar] [CrossRef]
- Tsvetanov, F. Integrating AI Technologies into Remote Monitoring Patient Systems. Eng. Proc. 2024, 70, 54. [Google Scholar] [CrossRef]
- Jameil, A.K.; Al-Raweshidy, H. A Digital Twin Framework for Real-Time Healthcare Monitoring: Leveraging AI and Secure Systems for Enhanced Patient Outcomes. Smart Health 2025, 5, 37. [Google Scholar] [CrossRef]
- Ianculescu, M.; Nicolau, D.; Petrache, C.; Vasilevschi, A. Advancing Neurodegenerative Disease Management: The NeuroPredict Platform Integrating IoT, AI, and Cloud Technologies. In Proceedings of the 2024 15th International Conference on Communications (COMM), Bucharest, Romania, 3–4 October 2024; pp. 1–6. [Google Scholar] [CrossRef]
- Kale, M.B.; Wankhede, N.L.; Pawar, R.S.; Ballal, S.; Kumawat, R.; Goswami, M.; Khalid, M.; Taksande, B.; Upaganlawar, A.; Umekar, M.; et al. AI-Driven Innovations in Alzheimer’s Disease: Integrating Early Diagnosis, Personalized Treatment, and Prognostic Modelling. Ageing Res. Rev. 2024, 101, 102497. [Google Scholar] [CrossRef] [PubMed]
- Alturki, B.; Abu Al-Haija, Q.; Alsemmeari, R.A.; Alsulami, A.A.; Alqahtani, A.; Alghamdi, B.M.; Bakhsh, S.T.; Shaikh, R.A. IoMT landscape: Navigating current challenges and pioneering future research trends. Discov. Appl. Sci. 2025, 7, 26. [Google Scholar] [CrossRef]
- Alhaj, T.A.; Abdulla, S.M.; Iderss, M.A.E.; Ali, A.A.A.; Elhaj, F.A.; Remli, M.A.; Gabralla, L.A. A Survey: To Govern, Protect, and Detect Security Principles on Internet of Medical Things (IoMT). IEEE Access 2022, 10, 124777–124791. [Google Scholar] [CrossRef]
- Bi, H.; Liu, J.; Kato, N. Deep Learning-Based Privacy Preservation and Data Analytics for IoT Enabled Healthcare. IEEE Trans. Ind. Inform. 2022, 18, 4798–4807. [Google Scholar] [CrossRef]
- Zhu, F.; Yi, X.; Abuadbba, A.; Khalil, I.; Nepal, S.; Huang, X. Authenticated Data Sharing with Privacy Protection and Batch Verification for Healthcare IoT. IEEE Trans. Sustain. Comput. 2023, 8, 32–42. [Google Scholar] [CrossRef]
- Negi, L.; Kumar, D. ECC based certificateless aggregate signature scheme for healthcare wireless sensor networks. J. Reliable Intell. Environ. 2024, 10, 489–500. [Google Scholar] [CrossRef]
- Shaik, T.; Tao, X.; Higgins, N.; Li, L.; Gururajan, R.; Zhou, X.; Acharya, U.R. Remote patient monitoring using artificial intelligence: Current state, applications, and challenges. Wiley Interdiscip. Rev.-Data Min. Knowl. Discov. 2023, 13, e1485. [Google Scholar] [CrossRef]
- Moonga, J. Digital Biomarkers and Wearable Neurotechnologies: A Cost of Privacy and Security for Alzheimer’s Patients. Alzheimer’s Dement. 2023, 19, e065477. [Google Scholar] [CrossRef]
- Smallman, M. Multi Scale Ethics—Why We Need to Consider the Ethics of AI in Healthcare at Different Scales. Sci. Eng. Ethics 2022, 28, 63. [Google Scholar] [CrossRef]
- McLennan, S.; Fiske, A.; Tigard, D.W.; Müller, R.; Haddadin, S.; Buyx, A. Embedded ethics: A proposal for integrating ethics into the development of medical AI. BMC Med. Ethics 2022, 23, 6. [Google Scholar] [CrossRef]
- Yang, C.L.; Tampubolon, H.; Setyoko, A.; Hua, K.L.; Tanveer, M.; Wei, W. Secure and Privacy-Preserving Human Interaction Recognition of Pervasive Healthcare Monitoring. IEEE Trans. Netw. Sci. Eng. 2022, 10, 2439–2454. [Google Scholar] [CrossRef]
- Bernier, A.; Molnár-Gábor, F.; Knoppers, B.M. The international data governance landscape. J. Law Biosci. 2022, 9, lsac005. [Google Scholar] [CrossRef] [PubMed]
- Bernier, A.; Molnár-Gábor, F.; Knoppers, B.M.; Borry, P.; Devriendt, T.; Goisauf, M.; Murtagh, M.J.; Jiménez, P.N.; Recuero, M.M.; Rial-Sebbag, E.; et al. Reconciling the biomedical data commons and the GDPR: Three lessons from the EUCAN ELSI collaboratory. Eur. J. Hum. Genet. 2023, 32, 69–76. [Google Scholar] [CrossRef] [PubMed]
- Rocha, P. Digital Innovation on Integrated Care for Ageing: A qualitative case study in South Europe with NASSS Framework. Int. J. Integr. Care 2022, 22, 134. [Google Scholar] [CrossRef]
- Garcia, R.D.; Ramachandran, G.S.; Jurdak, R.; Ueyama, J. Blockchain-Aided and Privacy-Preserving Data Governance in Multi-Stakeholder Applications. IEEE Trans. Netw. Serv. Manag. 2022, 19, 3781–3793. [Google Scholar] [CrossRef]
- Upadrista, V.; Nazir, S.; Tianfield, H. Secure data sharing with blockchain for remote health monitoring applications: A review. J. Reliab. Intell. Environ. 2023, 9, 349–368. [Google Scholar] [CrossRef]
- Velmurugan, S.; Prakash, M.; Neelakandan, S.; Ofori, M.E. An Efficient Secure Sharing of Electronic Health Records Using IoT-Based Hyperledger Blockchain. Int. J. Intell. Syst. 2024, 2024, 6995202. [Google Scholar] [CrossRef]
- Guimarães, T.; Duarte, R.; Hak, F.; Santos, M. Context-Aware Electronic Health Record—Internet of Things and Blockchain Approach. Informatics 2024, 11, 98. [Google Scholar] [CrossRef]
- Singh, P.; Sagar, S.; Singh, S.; Alshahrani, H.M.; Getahun, M.; Soufiene, B.O. Blockchain-enabled verification of medical records using soul-bound tokens and cloud computing. Sci. Rep. 2024, 14, 24830. [Google Scholar] [CrossRef]
- Zheng, M.; Wu, Y.; Weng, C. A digital intelligence visualization health monitoring device for Alzheimer’s disease patients based on WBAN technology. Sci. Rep. 2025, 15, 15997. [Google Scholar] [CrossRef]
- Okubanjo, A.A.; Ifeanyi, C.A.; Ajayi, R.; Ojo, D.; Iwuanyanwu, H.U. Development of a Low-Cost IoT-Based E-Health Monitoring System for Diabetic Patients. J. Electr. Syst. Inf. Technol. 2024, 11, 54. [Google Scholar] [CrossRef]
- Liu, Z.; Cascioli, V.; McCarthy, P.W. Healthcare Monitoring Using Low-Cost Sensors to Supplement and Replace Human Sensation: Does It Have Potential to Increase Independent Living and Prevent Disease? Sensors 2023, 23, 2139. [Google Scholar] [CrossRef] [PubMed]
- Yi, S.; Yam, E.L.Y.; Cheruvettolil, K.; Linos, E.; Gupta, A.; Palaniappan, L.; Rajeshuni, N.; Vaska, K.G.; Schulman, K.; Eggleston, K.N. Perspectives of Digital Health Innovations in Low- and Middle-Income Health Care Systems From South and Southeast Asia. J. Med. Internet Res. 2024, 26, e57612. [Google Scholar] [CrossRef] [PubMed]
- Casals, L.; Mir, B.; Vidal, R.; Gomez, C. Modeling the Energy Performance of LoRaWAN. Sensors 2017, 17, 2364. [Google Scholar] [CrossRef]



| Database | Field Scope | Search String |
|---|---|---|
| Scopus | TITLE-ABS-KEY | As above |
| PubMed | All Fields | As above |
| IEEE Xplore | All Metadata | As above |
| Springer | All Fields | As above |
| MDPI | All Fields | As above |
| Wiley | All Fields | As above |
| Article | Scope | IoT Dimensions Covered | Notable Novelty/Gaps |
|---|---|---|---|
| Sheikhtaheri & Sabermahani (2022) [20] | Scoping review of IoT applications in dementia care | Smart home automation and wearable sensors for home monitoring | Broad overview across dementia; lacks AD-stage organization and limited AI focus |
| Thanos et al. (2020) [21] | Review of wearable IoT devices for Alzheimer’s patients | Wearable trackers, smartwatches, mobile-app integration | Detailed wearable-device survey; excludes ambient/nonwearable IoT modalities |
| Esquer-Rochín et al. (2023) [14] | Systematic review and taxonomy of IoT in all dementias | Wearables, ambient sensorsc | Comprehensive IoT taxonomy; not Alzheimer’s-specific or stage-structured |
| Rocha et al. (2024) [22] | Review of wearable monitoring devices for dementia ADLs | Sensorized clothing, wristbands, and ADL task monitoring | In-depth design/usability guidance; limited to wearables and ADL tracking |
| Shaik et al. (2025) [23] | Systematic review of remote monitoring in AD and ADRD | Multimodal IoT: wearables, ambient sensors, and companion robots | Focus on monitoring and AI analytics; lacks early detection tools and stage-wise view. |
| This work (2025) | Stage-wise review of IoT interventions across AD progression | Wearable biosensors, smart home systems, cognitive assessment tools, AI analytics, and LMIC considerations | Holistic coverage of all AD stages; emphasizes real-world deployment, ethics, interoperability, and LMIC scalability |
| Study | Sensor Type | Biomarker(s) | Linear Range | LOD | Key Metrics/IoT Integration |
|---|---|---|---|---|---|
| Liu et al. (2022) [72] | VG@Au aptasensor | Tau | 0.1–1000 pg/mL | 0.034 pg/mL | Bluetooth to smartphone; accuracy comparable to commercial device. |
| Li et al. (2023) [73] | Printed VG@nanoAu array | – | 0.072–0.089– 0.071–0.051 pg/mL | Smartphone micro-workstation; high specificity and stability. | |
| Chakari-Khiavi et al. (2023) [74] | Pt@ZIF-8 immunosensor | Cis-p-tau | 1 fg/mL–10 ng/mL | 1 fg/mL | Validated in patient serum; reproducibility and stability. |
| Ciou et al. (2023) [75] | GO/G SGFET | P-tau217 | 10 fg/mL–100 pg/mL | 10 fg/mL | 18.6 mV/dec sensitivity; ≈90% specificity; <2% drift over 7 days. |
| Kong et al. (2024) [76] | AuNP-GCE aptasensor | P-tau231 | 10–107 pg/mL | 2.31 pg/mL | Recovery 97.6–103.3%; RSD 3.27%; 7-day stability. |
| Category | Methods | Results | Evaluation Metrics and Performance |
|---|---|---|---|
| Wearable Biosensors for Alzheimer’s Monitoring | Smart watches, fitness bands, and smart textiles with flexible electronics for long-term tracking [57,58,59,60] | High feasibility and adherence; Empatica E4 and Apple Watch widely accepted, including in rural settings [62,63] | High adherence; no specific metrics |
| Digital Biomarkers and AI-Driven Diagnostics | IoT-enabled wearables with cloud-based ML for digital biomarker extraction [50,64] | Eye tracking distinguished AD patients with 86% accuracy [50]; real-time alerts provided [64] | Accuracy: 86% (eye tracking) [50] |
| Advances in Biosensors for Broader Healthcare | Electrochemical and optical biosensors for vital signs and analytes [65,93,94,95] | Enhanced noninvasive monitoring via OLED/OPD sensors [94] | Improved signal quality; no quantitative metrics |
| Behavioral Detection and AI-Enabled Monitoring | Biosensors for movement, eye tracking, and speech analysis [85,86] | Real-time behavioral symptom tracking via sensor fusion | Objective assessments; no metrics provided |
| Continuous Glucose Monitoring in ADRD-DM Patients | IoT-integrated CGM for hypoglycemia detection in ADRD-DM patients [87,88] | Reduced hypoglycemic events; limited ADRD-DM data [88] | Correlation >90% with blood glucose [91] |
| Wearable Glucose Monitoring and Non-Invasive Systems | Flexible electromagnetic sensors with ML-based processing [92,96,97] | 99.01% human and 100% animal accuracy [92] | Accuracy: 99.01% (human), 100% (animal) [92] |
| Multi-Sensor Integration for Personalized Healthcare | Multi-sensor glucose monitoring with Bayesian inference [98] | Explained 40–65% HR variance; 15% glucose variability | Correlation: 40–65% (HR), 15% (glucose) [98] |
| IoT and Smart Clothing for Healthcare | AI-driven IoT models and smart textiles for passive monitoring [99,100,101] | Enhanced adherence and unobtrusive monitoring | No quantitative evaluation |
| Technology and Study | Sample Size (n) | Setting | Performance Metrics | Key Limitations |
|---|---|---|---|---|
| CogSAS mobile self-assessment [27] | 1272 (validation); 83 MCI/AD | Community and clinical | Cronbach’s ; ICC = 0.82; sensitivity = 100%; specificity = 78% | Cross-sectional; limited longitudinal data; clinically confirmed only |
| Remote digital memory composite [28] | 199 (memory clinic) | Multicenter memory clinics | AUC = 0.83 (95% CI [0.66,0.99]); sens = 0.82; spec = 0.72 | No home-use validation; moderate specificity |
| Smartphone-based assessments [29] | 537 (Framingham cohort) | Community (longitudinal study) | User confidence = 76%; ease of use = 81% | Lacks diagnostic accuracy metrics; self-report bias |
| Video-based cognitive testing survey [30] | 369 (participants) | Community (survey) | Willingness = 82% for remote testing | Access disparities by cognitive status; no efficacy data |
| Ambient smart home ADL monitoring [102] | 36 (pilot: healthy, SCD, MCI) | In-home smart apartments | Classification accuracy up to 90% on ADL task durations | Small pilot; single site; task-based only |
| Multi-kinematic gait IMU [51] | 94 (33 CN, 61 aMCI) | Lab-controlled walking tasks | AUC = 0.96; sens = 0.90; spec = 0.91; acc = 0.90 | Controlled setting; sensor placement variability |
| Waist-mounted balance IMU [49] | 60 (30 CN, 30 MCI) | Four static standing tasks | Accuracy = 75.8% after SHAP feature selection | Cross-sectional; no dynamic walking analysis |
| Eye-tracking IoT system [50] | 48 (early-stage AD) | Clinical oculomotor lab | Accuracy = 86% in detecting anomalies | Requires specialized hardware; small cohort |
| Study | Sensor | Protocol | Key Metrics | Performance |
|---|---|---|---|---|
| Li et al. (2023) [123] | MATRIX 2.0 IMU | Single/dual task (walking; minus-seven subtraction) | Pace asymmetry; rhythm; variability | ST: AUC 0.744 (sens 100%, spec 45%); DT: rhythm AUC 0.734 (sens 85.2%, spec 57.5%), variability AUC 0.719 (sens 55.6%, spec 97.5%) |
| Huang et al. (2022) [51] | JiBuEn® inertial-shoe system | Simple gait tasks | TUG time; stride length; joint angles; OLS time; braking force | AUC 0.96; sens 0.90; spec 0.91; acc 0.90 |
| Seifallahi et al. (2024) [120] | Kinect v2 depth camera | Straight and oval-path walking | Skeletal features (25 joints) | RF: acc 85.5%; F1 83.9% (oval) |
| Technology and Study | Sample Size (n) | Setting | Performance Metrics | Key Limitations |
|---|---|---|---|---|
| [102] | 36 (healthy, SCD, MCI) | Smart home apartment | ADL task duration classification accuracy up to 88% | Pilot scale; single environment; limited ADL scope |
| [109] | 82 | Community-dwelling homes | 147,203 measurements over 958,000 h; 56.2% daily engagement; alert rate of 0.066–0.233/person-day; early detection of acute events | Single-site cohort; no long-term outcome data |
| [110] | 49 (28 MCI, 21 controls) | In-home passive sensors | Steps/day: 3407 vs. 4033; awakenings/night: 2 vs. 1; trends NS | Underpowered; lack of refined biomarkers |
| [112] | 7 | Home (Apple Watch) | >700,000 observations; 84.9% wear adherence (11.48 h/day) over 6 months | Very small sample; no control; limited generalizability |
| [111] | 30 | Home (infrared + mattress sensors) | ∼ 85% accuracy detecting gait and sleep changes | Limited home diversity; short monitoring window; needs larger trials |
| Study | Domain | Method | Sample (n) | Performance Metrics | Limitations |
|---|---|---|---|---|---|
| [102] | Cognitive Assessment | IoT-based sensor monitoring of ADLs across groups | 37 (11 HC, 15 MCI, 11 AD) | Statistically significant group-wise variation | No prediction modeling; short duration |
| [188] | Behavioral Monitoring | Personalized ML on multimodal wearable sensors (e.g., PPG, EDA) | 28 participants; 16 training, 12 testing | F1 = 0.69; precision = 0.75; recall = 0.65 | Small cohort; requires personalization |
| [189] | Cognitive Detection | Secure Federated Learning on neuroimaging + clinical data | ADNI dataset (n = 1004) | Accuracy = 91.4%, F1 = 91.7% | No real-world IoT sensor integration |
| [190] | Routine Behavior Monitoring | ML on in-home sensor event logs for ADL routines | 35 older adults over 8 weeks | Differentiation of routines and changes | No clinical dementia categorization |
| [191] | Passive Monitoring | Device-free Wi-Fi sensing for motion and ADL tracking | 16 older adults in low-income housing | Feasibility of ADL trend monitoring | No dementia-specific outcomes yet |
| [192] | Biomarker Monitoring | Multimodal federated learning across edge sensors | 91 elderly subjects in 4-week trial | Accuracy = 93.8%; Early AD detection = 88.9% | Complex system; short deployment duration |
| [127] | Smart Home Systems | Systematic review of motion/contact sensors | — | Qualitative insights | No longitudinal validation |
| [161] | Smart Home Systems | Interviews & workshops | 9 PWD, 9 CG, 10 HP; 35 pairs; 12 clinicians | Stakeholder engagement | No quantitative metrics |
| [167] | Smart Home Systems | NFC pill dispenser prototype | — | Bench testing feasibility | No clinical data |
| [162] | Behavioral Monitoring | Wearable sensor profiling (PPG, EDA, ST, and ACC) + GLMM | 30 | Agitation detection ( = 0.224–0.753) | Small cohort; patient-specific tuning |
| [163] | Cognitive Assessment | ML on ambient + wearable sensor data in smart homes | — (Simulated) | Accuracy = 94.1% | No real-world deployment |
| [164] | Smart Home Systems | TIHM dataset (PIR, door, mattress sensors) | 56 homes | — | Dataset only; no evaluation |
| [168] | Medication Support | IoT pill dispenser and smart cup | 33 | Adherence: 58%→94%; accuracy: 97% | Small n, <6-week trial |
| [183] | Medication Support | Face recognition and geofencing reminders | 21 | 95% on time; recall: +40% | Small n |
| [184] | Location Tracking | Commercial GPS trackers | 45 dyads | Satisfaction: 93% | No formal accuracy |
| [186] | Location Tracking | Wavelet and geofencing on GPS data | 182 trajectories | Acc: 83.06%; Prec: 92.62%; F1: 87.58% | No in situ testing |
| [169] | Wandering Prevention | Waist IMU sensors and ML models | 12 | Sensitivity: 80%; specificity: 85% | Small cohort |
| [170] | Wandering Prevention | Gait and balance IMUs | 35 | Accuracy: 89% | No AD-specific validation |
| [171] | Wandering Prevention | Chest-worn IMU turn detection | 23 | Sub-second turn detection | No wandering metrics |
| Model | Dataset | Input Modality | Accuracy | AUC | Precision | Recall |
|---|---|---|---|---|---|---|
| SVM [193] | Augmented gait lifelog (wearable IMUs) | Pace, rhythm, and variability features | 87.9% | 76.4% | 100% | 42.9% |
| Random Forest [193] | Augmented gait lifelog (wearable IMUs) | Pace, rhythm, and variability features | 78.8% | 80.8% | 50.0% | 57.1% |
| XGBoost [194] | ADNI fMRI (n ≈ 800) | Cortical ROI features (CNN-extracted + handcrafted) | 98.8% | 98.82% | — | 98.9% |
| CNN [194] | ADNI fMRI (n ≈ 800) | Raw fMRI volumes (3D CNN) | 88% | — | 92% | 89% |
| DRN–LSTM [195] | IoT-assisted hospital testbed | Audio, video, and motion sensors (DRN-LSTM + PI-HHO) | 98% | — | 97% | — |
| Gap/Challenge | Implication | Future Study Direction |
|---|---|---|
| Limited multicenter, longitudinal datasets | Restricts generalizability and external validity | Design coordinated multi-site, year-long cohorts with standardized outcome measures |
| Small sample sizes/modality silos | Inflated performance estimates; weak comparison across approaches | Aggregate multimodal datasets; adopt shared benchmarking protocols |
| Interoperability and data standard gaps | Fragmented pipelines; integration overhead | Implement and evaluate unified data models and open APIs across platforms |
| Privacy, security, and governance weaknesses | Risk of data misuse; reduced stakeholder trust | Embed privacy by design, continuous security monitoring, and clear governance workflows |
| Energy and on-device resource constraints | Limits continuous monitoring and scalability | Optimize models (compression and quantization) and adaptive sensing schedules |
| Bias and demographic under-representation | Potential inequitable performance across groups | Enforce stratified reporting; collect diverse cohorts; apply bias auditing and mitigation |
| Lack of standardized evaluation metrics | Difficult cross-study comparison | Define core metric set (clinical + technical) and publish reporting templates |
| Sparse validation of emerging retinal/nanosensor tools | Uncertain durability and clinical readiness | Conduct stability, calibration, and real-world deployment studies |
| Edge–cloud integration complexity | Latency and reliability variability | Develop adaptive orchestration frameworks with performance monitoring |
| Insufficient explainability and clinician usability evidence | Hinders adoption in clinical workflows | Integrate interpretable outputs and perform user-centered usability trials |
| Cost and scalability barriers in resource-constrained settings | Limits global deployment | Evaluate low-cost architectures, local maintenance models, and implementation economics |
| Regulatory pathway uncertainty | Delays translation to practice | Map compliance requirements and pilot regulatory sandbox evaluations |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Salvi, S.; Garg, L.; Gurupur, V. Stage-Wise IoT Solutions for Alzheimer’s Disease: A Systematic Review of Detection, Monitoring, and Assistive Technologies. Sensors 2025, 25, 5252. https://doi.org/10.3390/s25175252
Salvi S, Garg L, Gurupur V. Stage-Wise IoT Solutions for Alzheimer’s Disease: A Systematic Review of Detection, Monitoring, and Assistive Technologies. Sensors. 2025; 25(17):5252. https://doi.org/10.3390/s25175252
Chicago/Turabian StyleSalvi, Sanket, Lalit Garg, and Varadraj Gurupur. 2025. "Stage-Wise IoT Solutions for Alzheimer’s Disease: A Systematic Review of Detection, Monitoring, and Assistive Technologies" Sensors 25, no. 17: 5252. https://doi.org/10.3390/s25175252
APA StyleSalvi, S., Garg, L., & Gurupur, V. (2025). Stage-Wise IoT Solutions for Alzheimer’s Disease: A Systematic Review of Detection, Monitoring, and Assistive Technologies. Sensors, 25(17), 5252. https://doi.org/10.3390/s25175252








