Physical Activity Assessed by Wrist and Thigh Worn Accelerometry and Associations with Cardiometabolic Health
Abstract
1. Introduction
2. Materials and Methods
2.1. Design and Participants
2.2. Demographics and Anthropometric Measures
2.3. Metabolic and Cardiovascular Markers
2.4. Accelerometer Data Collection and Processing
2.5. Statistical Analysis
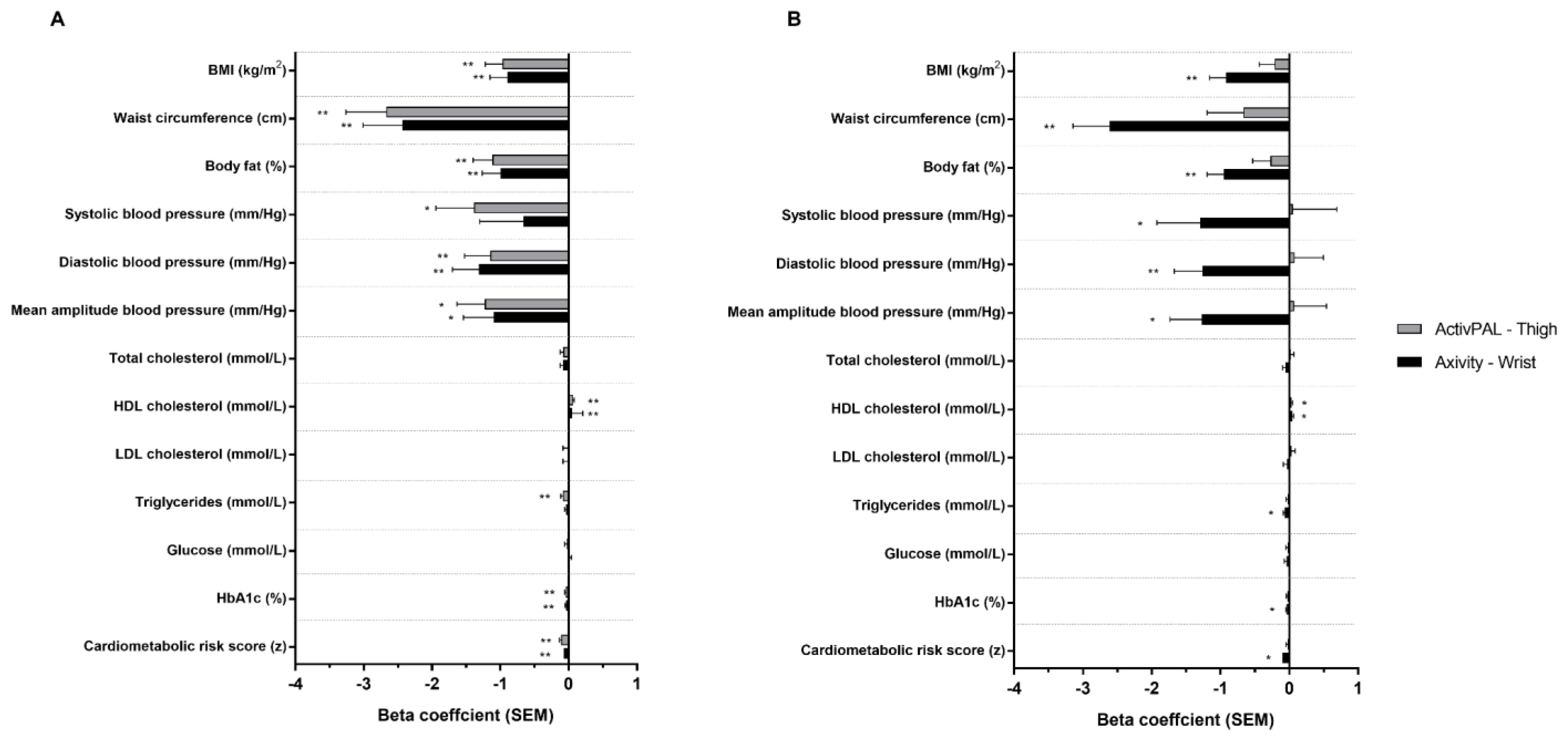
3. Results
MX Results
4. Discussion
Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Doherty, A.; Jackson, D.; Hammerla, N.; Plotz, T.; Olivier, P.; Granat, M.H.; White, T.; van Hees, V.T.; Trenell, M.I.; Owen, C.G.; et al. Large Scale Population Assessment of Physical Activity Using Wrist Worn Accelerometers: The UK Biobank Study. PLoS ONE 2017, 12, e0169649. [Google Scholar] [CrossRef]
- Sullivan, A.; Brown, M.; Hamer, M.; Ploubidis, G.B. Cohort Profile Update: The 1970 British Cohort Study (BCS70). Int. J. Epidemiol. 2022, 52, e179–e186. [Google Scholar] [CrossRef] [PubMed]
- Troiano, R.P.; McClain, J.J.; Brychta, R.J.; Chen, K.Y. Evolution of accelerometer methods for physical activity research. Br. J. Sports Med. 2014, 48, 1019–1023. [Google Scholar] [CrossRef] [PubMed]
- Wu, Y.; Petterson, J.L.; Bray, N.W.; Kimmerly, D.S.; O’Brien, M.W. Validity of the activPAL monitor to measure stepping activity and activity intensity: A systematic review. Gait Posture 2022, 97, 165–173. [Google Scholar] [CrossRef]
- Montoye, A.H.K.; Pivarnik, J.M.; Mudd, L.M.; Biswas, S.; Pfeiffer, K.A. Validation and Comparison of Accelerometers Worn on the Hip, Thigh, and Wrists for Measuring Physical Activity and Sedentary Behavior. AIMS Public Health 2016, 3, 298–312. [Google Scholar] [CrossRef] [PubMed]
- Suorsa, K.; Pulakka, A.; Leskinen, T.; Pentti, J.; Holtermann, A.; Heinonen, O.J.; Sunikka, J.; Vahtera, J.; Stenholm, S. Comparison of Sedentary Time Between Thigh-Worn and Wrist-Worn Accelerometers. J. Meas. Phys. Behav. 2020, 3, 234–243. [Google Scholar] [CrossRef]
- Ekelund, U.; Tarp, J.; Steene-Johannessen, J.; Hansen, B.H.; Jefferis, B.; Fagerland, M.W.; Whincup, P.; Diaz, K.M.; Hooker, S.P.; Chernofsky, A.; et al. Dose-response associations between accelerometry measured physical activity and sedentary time and all cause mortality: Systematic review and harmonised meta-analysis. BMJ 2019, 366, l4570. [Google Scholar] [CrossRef]
- Leroux, A.; Xu, S.; Kundu, P.; Muschelli, J.; Smirnova, E.; Chatterjee, N.; Crainiceanu, C. Quantifying the Predictive Performance of Objectively Measured Physical Activity on Mortality in the UK Biobank. J. Gerontol. A Biol. Sci. Med. Sci. 2021, 76, 1486–1494. [Google Scholar] [CrossRef] [PubMed]
- Strain, T.; Wijndaele, K.; Dempsey, P.C.; Sharp, S.J.; Pearce, M.; Jeon, J.; Lindsay, T.; Wareham, N.; Brage, S. Wearable-device-measured physical activity and future health risk. Nat. Med. 2020, 26, 1385–1391. [Google Scholar] [CrossRef] [PubMed]
- Klenk, J.; Dallmeier, D.; Denkinger, M.D.; Rapp, K.; Koenig, W.; Rothenbacher, D.; Acti, F.E.S.G. Objectively Measured Walking Duration and Sedentary Behaviour and Four-Year Mortality in Older People. PLoS ONE 2016, 11, e0153779. [Google Scholar] [CrossRef] [PubMed]
- Sjoros, T.; Vaha-Ypya, H.; Laine, S.; Garthwaite, T.; Lahesmaa, M.; Laurila, S.M.; Latva-Rasku, A.; Savolainen, A.; Miikkulainen, A.; Loyttyniemi, E.; et al. Both sedentary time and physical activity are associated with cardiometabolic health in overweight adults in a 1 month accelerometer measurement. Sci. Rep. 2020, 10, 20578. [Google Scholar] [CrossRef]
- Chastin, S.F.; Palarea-Albaladejo, J.; Dontje, M.L.; Skelton, D.A. Combined Effects of Time Spent in Physical Activity, Sedentary Behaviors and Sleep on Obesity and Cardio-Metabolic Health Markers: A Novel Compositional Data Analysis Approach. PLoS ONE 2015, 10, e0139984. [Google Scholar] [CrossRef] [PubMed]
- Cassidy, S.; Fuller, H.; Chau, J.; Catt, M.; Bauman, A.; Trenell, M.I. Accelerometer-derived physical activity in those with cardio-metabolic disease compared to healthy adults: A UK Biobank study of 52,556 participants. Acta Diabetol. 2018, 55, 975–979. [Google Scholar] [CrossRef] [PubMed]
- De Rooij, B.H.; van der Berg, J.D.; van der Kallen, C.J.; Schram, M.T.; Savelberg, H.H.; Schaper, N.C.; Dagnelie, P.C.; Henry, R.M.; Kroon, A.A.; Stehouwer, C.D.; et al. Physical Activity and Sedentary Behavior in Metabolically Healthy versus Unhealthy Obese and Non-Obese Individuals—The Maastricht Study. PLoS ONE 2016, 11, e0154358. [Google Scholar] [CrossRef]
- Buchan, D.S.; Maylor, B.D. Comparison of physical activity metrics from two research-grade accelerometers worn on the non-dominant wrist and thigh in children. J. Sports Sci. 2023, 41, 80–88. [Google Scholar] [CrossRef]
- Edwardson, C.L.; Henson, J.; Biddle, S.J.H.; Davies, M.J.; Khunti, K.; Maylor, B.; Yates, T. activPAL and ActiGraph Assessed Sedentary Behavior and Cardiometabolic Health Markers. Med. Sci. Sports Exerc. 2020, 52, 391–397. [Google Scholar] [CrossRef]
- Leppanen, M.H.; Migueles, J.H.; Cadenas-Sanchez, C.; Henriksson, P.; Mora-Gonzalez, J.; Henriksson, H.; Labayen, I.; Lof, M.; Esteban-Cornejo, I.; Ortega, F.B. Hip and wrist accelerometers showed consistent associations with fitness and fatness in children aged 8–12 years. Acta Paediatr. 2020, 109, 995–1003. [Google Scholar] [CrossRef]
- Rowlands, A.V.; Fairclough, S.J.; Yates, T.; Edwardson, C.L.; Davies, M.; Munir, F.; Khunti, K.; Stiles, V.H. Activity Intensity, Volume, and Norms: Utility and Interpretation of Accelerometer Metrics. Med. Sci. Sports Exerc. 2019, 51, 2410–2422. [Google Scholar] [CrossRef] [PubMed]
- Dawkins, N.P.; Yates, T.; Edwardson, C.L.; Maylor, B.; Henson, J.; Hall, A.P.; Davies, M.J.; Dunstan, D.W.; Highton, P.J.; Herring, L.Y.; et al. Importance of Overall Activity and Intensity of Activity for Cardiometabolic Risk in Those with and Without a Chronic Disease. Med. Sci. Sports Exerc. 2022, 54, 1582–1590. [Google Scholar] [CrossRef]
- Stamatakis, E.; Koster, A.; Hamer, M.; Rangul, V.; Lee, I.M.; Bauman, A.E.; Atkin, A.J.; Aadahl, M.; Matthews, C.E.; Mork, P.J.; et al. Emerging collaborative research platforms for the next generation of physical activity, sleep and exercise medicine guidelines: The Prospective Physical Activity, Sitting, and Sleep consortium (ProPASS). Br. J. Sports Med. 2020, 54, 435–437. [Google Scholar] [CrossRef] [PubMed]
- Hildebrand, M.; VT, V.A.N.H.; Hansen, B.H.; Ekelund, U. Age group comparability of raw accelerometer output from wrist- and hip-worn monitors. Med. Sci. Sports Exerc. 2014, 46, 1816–1824. [Google Scholar] [CrossRef] [PubMed]
- Loprinzi, P.D.; Smith, B. Comparison Between Wrist-Worn and Waist-Worn Accelerometry. J. Phys. Act. Health 2017, 14, 539–545. [Google Scholar] [CrossRef]
- Edwardson, C.L.; Rowlands, A.V.; Bunnewell, S.; Sanders, J.; Esliger, D.W.; Gorely, T.; O’Connell, S.; Davies, M.J.; Khunti, K.; Yates, T. Accuracy of Posture Allocation Algorithms for Thigh- and Waist-Worn Accelerometers. Med. Sci. Sports Exerc. 2016, 48, 1085–1090. [Google Scholar] [CrossRef]
- Edwardson, C.L.; Biddle, S.J.H.; Clemes, S.A.; Davies, M.J.; Dunstan, D.W.; Eborall, H.; Granat, M.H.; Gray, L.J.; Healy, G.N.; Jaicim, N.B.; et al. Effectiveness of an intervention for reducing sitting time and improving health in office workers: Three arm cluster randomised controlled trial. BMJ 2022, 378, e069288. [Google Scholar] [CrossRef]
- Bastianelli, K.; Ledin, S.; Chen, J. Comparing the Accuracy of 2 Point-of-Care Lipid Testing Devices. J. Pharm. Pract. 2017, 30, 490–497. [Google Scholar] [CrossRef] [PubMed]
- Grant, D.A.; Dunseath, G.J.; Churm, R.; Luzio, S.D. Comparison of a point-of-care analyser for the determination of HbA1c with HPLC method. Pract. Lab. Med. 2017, 8, 26–29. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Dempsey, P.C.; Hadgraft, N.T.; Winkler, E.A.H.; Clark, B.K.; Buman, M.P.; Gardiner, P.A.; Owen, N.; Lynch, B.M.; Dunstan, D.W. Associations of context-specific sitting time with markers of cardiometabolic risk in Australian adults. Int. J. Behav. Nutr. Phys. Act. 2018, 15, 114. [Google Scholar] [CrossRef] [PubMed]
- Healy, G.N.; Winkler, E.A.H.; Eakin, E.G.; Owen, N.; Lamontagne, A.D.; Moodie, M.; Dunstan, D.W. A Cluster RCT to Reduce Workers’ Sitting Time: Impact on Cardiometabolic Biomarkers. Med. Sci. Sports Exerc. 2017, 49, 2032–2039. [Google Scholar] [CrossRef]
- Migueles, J.H.; Rowlands, A.V.; Huber, F.; Sabia, S.; Hees, V.T.v. GGIR: A Research Community—Driven Open Source R Package for Generating Physical Activity and Sleep Outcomes from Multi-Day Raw Accelerometer Data. J. Meas. Phys. Behav. 2019, 2, 188. [Google Scholar] [CrossRef]
- Van Hees, V.T.; Fang, Z.; Langford, J.; Assah, F.; Mohammad, A.; da Silva, I.C.; Trenell, M.I.; White, T.; Wareham, N.J.; Brage, S. Autocalibration of accelerometer data for free-living physical activity assessment using local gravity and temperature: An evaluation on four continents. J. Appl. Physiol. 2014, 117, 738–744. [Google Scholar] [CrossRef]
- Ricardo, L.I.C.; Wendt, A.; Galliano, L.M.; de Andrade Muller, W.; Niño Cruz, G.I.; Wehrmeister, F.; Brage, S.; Ekelund, U.; Crochemore, M.S.I. Number of days required to estimate physical activity constructs objectively measured in different age groups: Findings from three Brazilian (Pelotas) population-based birth cohorts. PLoS ONE 2020, 15, e0216017. [Google Scholar] [CrossRef] [PubMed]
- Rowlands, A.V.; Dawkins, N.P.; Maylor, B.; Edwardson, C.L.; Fairclough, S.J.; Davies, M.J.; Harrington, D.M.; Khunti, K.; Yates, T. Enhancing the value of accelerometer-assessed physical activity: Meaningful visual comparisons of data-driven translational accelerometer metrics. Sports Med. Open 2019, 5, 47. [Google Scholar] [CrossRef]
- Kingsnorth, A.P.; Rowlands, A.V.; Maylor, B.D.; Sherar, L.B.; Steiner, M.C.; Morgan, M.D.; Singh, S.J.; Esliger, D.W.; Orme, M.W. A More Intense Examination of the Intensity of Physical Activity in People Living with Chronic Obstructive Pulmonary Disease: Insights from Threshold-Free Markers of Activity Intensity. Int. J. Environ. Res. Public Health 2022, 19, 12355. [Google Scholar] [CrossRef]
- Arvidsson, D.; Fridolfsson, J.; Buck, C.; Ekblom, Ö.; Ekblom-Bak, E.; Lissner, L.; Hunsberger, M.; Börjesson, M. Reexamination of Accelerometer Calibration with Energy Expenditure as Criterion: VO2net Instead of MET for Age-Equivalent Physical Activity Intensity. Sensors 2019, 19, 3377. [Google Scholar] [CrossRef] [PubMed]
- Chudasama, Y.V.; Khunti, K.K.; Zaccardi, F.; Rowlands, A.V.; Yates, T.; Gillies, C.L.; Davies, M.J.; Dhalwani, N.N. Physical activity, multimorbidity, and life expectancy: A UK Biobank longitudinal study. BMC Med. 2019, 17, 108. [Google Scholar] [CrossRef]
- Backes, A.; Aguayo, G.A.; Collings, P.J.; El Fatouhi, D.; Fagherazzi, G.; Malisoux, L.; Group, O.-L.S. Associations Between Wearable-Specific Indicators of Physical Activity Behaviour and Insulin Sensitivity and Glycated Haemoglobin in the General Population: Results from the ORISCAV-LUX 2 Study. Sports Med. Open 2022, 8, 146. [Google Scholar] [CrossRef] [PubMed]
- Lindsay, T.; Wijndaele, K.; Westgate, K.; Dempsey, P.; Strain, T.; De Lucia Rolfe, E.; Forouhi, N.G.; Griffin, S.; Wareham, N.J.; Brage, S. Joint associations between objectively measured physical activity volume and intensity with body fatness: The Fenland study. Int. J. Obes. 2022, 46, 169–177. [Google Scholar] [CrossRef]
- Tudor-Locke, C.; Schuna, J.M., Jr.; Han, H.O.; Aguiar, E.J.; Green, M.A.; Busa, M.A.; Larrivee, S.; Johnson, W.D. Step-Based Physical Activity Metrics and Cardiometabolic Risk: NHANES 2005–2006. Med. Sci. Sports Exerc. 2017, 49, 283–291. [Google Scholar] [CrossRef]
- Lu, Y.; Wiltshire, H.D.; Baker, J.S.; Wang, Q.; Ying, S.; Li, J.; Lu, Y. Associations between Objectively Determined Physical Activity and Cardiometabolic Health in Adult Women: A Systematic Review and Meta-Analysis. Biology 2022, 11, 925. [Google Scholar] [CrossRef]
- Small, S.; Khalid, S.; Dhiman, P.; Chan, S.; Jackson, D.; Doherty, A.; Price, A. Impact of Reduced Sampling Rate on Accelerometer-Based Physical Activity Monitoring and Machine Learning Activity Classification. J. Meas. Phys. Behav. 2021, 4, 298–310. [Google Scholar] [CrossRef]
- Fuzeki, E.; Engeroff, T.; Banzer, W. Health Benefits of Light-Intensity Physical Activity: A Systematic Review of Accelerometer Data of the National Health and Nutrition Examination Survey (NHANES). Sports Med. 2017, 47, 1769–1793. [Google Scholar] [CrossRef] [PubMed]
- Saint-Maurice, P.F.; Troiano, R.P.; Bassett, D.R., Jr.; Graubard, B.I.; Carlson, S.A.; Shiroma, E.J.; Fulton, J.E.; Matthews, C.E. Association of Daily Step Count and Step Intensity with Mortality among US Adults. JAMA 2020, 323, 1151–1160. [Google Scholar] [CrossRef] [PubMed]


| Characteristic | Mean (SD) |
|---|---|
| Age (years) | 44.6 (10.4) |
| Sex, n women | 445 (72.9%) |
| Ethnicity, n White European | 432 (70.8%) |
| Cardiometabolic risk score (z) | −0.01 (0.66) |
| Body Mass Index (kg/m2) | 26.5 (5.9) |
| Fasting Glucose (mmol/L) | 5.49 (0.96) |
| HbA1c (%) | 5.25 (0.49) |
| Total cholesterol (mmol/L) | 4.70 (1.07) |
| HDL-C (mmol/L) | 1.43 (0.40) |
| LDL-C (mmol/L) | 2.59 (1.10) |
| Triglycerides (mmol/L) | 1.22 (0.64) |
| Systolic blood pressure (mmHg) | 117.9 (15.9) |
| Diastolic blood pressure (mmHg) | 79.1 (10.3) |
| Mean Amplitude of blood pressure (mmHg) | 92.1 (11.6) |
| Variable | Axivity | ActivPAL | Mean Axivity-Activpal Delta | p |
|---|---|---|---|---|
| Number of valid days | 7.8 (0.5) | 7.6 (0.9) | 0.2 (1.1) | <0.001 |
| Average acceleration (mg) | 27.40 (7.11) | 22.52 (6.58) | 4.81 (5.71) | <0.001 |
| Intensity gradient | −2.55 (0.21) | −2.05 (0.22) | −0.49 (0.26) | <0.001 |
| Intensity gradient R2 | 0.89 (0.04) | 0.81 (0.07) | −0.08 (0.06) | <0.001 |
| Average acceleration—Intensity gradient Correlation | 0.570 | 0.543 | - | - |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Maylor, B.D.; Edwardson, C.L.; Clarke-Cornwell, A.M.; Davies, M.J.; Dawkins, N.P.; Dunstan, D.W.; Khunti, K.; Yates, T.; Rowlands, A.V. Physical Activity Assessed by Wrist and Thigh Worn Accelerometry and Associations with Cardiometabolic Health. Sensors 2023, 23, 7353. https://doi.org/10.3390/s23177353
Maylor BD, Edwardson CL, Clarke-Cornwell AM, Davies MJ, Dawkins NP, Dunstan DW, Khunti K, Yates T, Rowlands AV. Physical Activity Assessed by Wrist and Thigh Worn Accelerometry and Associations with Cardiometabolic Health. Sensors. 2023; 23(17):7353. https://doi.org/10.3390/s23177353
Chicago/Turabian StyleMaylor, Benjamin D., Charlotte L. Edwardson, Alexandra M. Clarke-Cornwell, Melanie J. Davies, Nathan P. Dawkins, David W. Dunstan, Kamlesh Khunti, Tom Yates, and Alex V. Rowlands. 2023. "Physical Activity Assessed by Wrist and Thigh Worn Accelerometry and Associations with Cardiometabolic Health" Sensors 23, no. 17: 7353. https://doi.org/10.3390/s23177353
APA StyleMaylor, B. D., Edwardson, C. L., Clarke-Cornwell, A. M., Davies, M. J., Dawkins, N. P., Dunstan, D. W., Khunti, K., Yates, T., & Rowlands, A. V. (2023). Physical Activity Assessed by Wrist and Thigh Worn Accelerometry and Associations with Cardiometabolic Health. Sensors, 23(17), 7353. https://doi.org/10.3390/s23177353






