Improving Stress Management and Sleep Hygiene in Intelligent Homes
Abstract
1. Introduction
2. Background Theory
2.1. Implications of Stress in Everyday Life
2.2. Stress Monitoring Techniques
2.3. Stress Reduction Methods
2.4. Implications of Poor Sleep Quality in Everyday Life
2.5. Sleep Monitoring Techniques
2.6. Sleep Improvement Methods
2.6.1. Following Sleep Hygiene Recommendations
- Sleep/Wake up Time Regularity: Sleepers should adhere to regular bed and wake times because this consistency promotes sleep propensity and consolidation [85].
- Caffeine Intake: Individuals should avoid caffeine close to bedtime [86].
- Nicotine Use: Smoking should ideally be avoided, and certainly for at least 2 h before bed. There is little evidence on the effects of nicotine on sleep in nonsmokers [86].
- Nutrition Intake: Food intake timing-mainly in the evening- is negatively correlated with several sleep-related parameters. Moreover, intake of high-fat food is associated with higher sleep latency [87].
- Exercise Regularity: Regular exercise promotes good sleep, but should be avoided close to bedtime [86].
- Stress: Individuals should reduce worry or engage in relaxing activities, particularly before bedtime.
- Naps: Daytime napping has been shown to decrease the depth of the major sleep episode and increase latency to sleep onset [85]. Thus, naps are detrimental to subsequent nocturnal sleep.
2.6.2. Creating an Optimal Sleep Environment
- Noise: It is easiest to sleep in a quiet place, since sudden or repetitive noises can interrupt sleep. When we hear noise, we may not become fully conscious, but we certainly will come out of the deeper stages of sleep. Interestingly, while certain noises cause interrupted sleep, soft, steady sounds can be soothing [88].
- Temperature: A slightly cool room contributes to good sleep, since a hot environment leads to more wake time and lighter sleep at night, while awakenings multiply. An optimal bedroom temperature is thought to be between 16 °C (60 °F) and 18 °C (65 °F). In most cases, temperatures above 75 °F and below 54 °F will disrupt sleep, but sleep researchers fail to agree on the ideal temperature for sleep. The point at which sleep is interrupted due to temperature or climate conditions varies from person to person and can be affected by bed clothes and bedding materials selected by the sleeper [89].
- Lighting: Lighting affects the perceived atmosphere [67]. Peripheral and non-uniform spatial lighting with low brightness helps to create a relaxing atmosphere, while at the same time, the right color temperature in lighting can be advantageous to human health, well-being, and productivity [90]. Under most circumstances, cool colors have been associated with peaceful, calm, and restful environments, while warm colors are physically and emotionally arousing, exciting, and distracting [68]. In addition, darkness promotes the releasement of melatonin, which relaxes the body and helps to fall asleep faster.
- Electronics and Blue Light: Electronic devices like TVs, computers, tablets, and smart phones, all have a high concentration of blue light. Blue light is the strongest wavelength, and thus the most disruptive to melatonin production. Melatonin is the hormone responsible for sleep which is produced in the evening by the brain. Leaving the lights on and using electronic devices tricks the brain into thinking it is still daytime, thus delaying melatonin production and keeping people awake longer [91]. So, sleep environments should be used only for sleep and any type of electronic device should be avoided just before and during bedtime in order to promote good sleep [89].
- Scents: Another way to make a room feel relaxing is through ambient scent, since specific scents have been shown to have a positive impact on mood [92] and induce relaxation [93]. Aromatherapy, has been used for centuries to promote relaxation, mental and physical wellness. In addition, it is found that it reduces anxiety and increases sleep [94]. In fact, inhaling essential oil molecules may activate brain chemicals involved in controlling sleep [69]. In order to tune the ambient scent, a smart aromatherapy diffuser, which spreads the essentials oils through air without human intervention, can be used.
2.6.3. Following Relaxation Techniques
3. Related Work
3.1. Systems Enabling Stress Management
3.2. Systems Improving Sleep Quality
4. The Intelligent Home of ICS-FORTH
4.1. Intelligent Spaces
4.2. AmIHomeOS
- User preferences and profile: provides access to users’ personal data, characteristics and configuration parameters.
- User tracking: monitors the presence of people and tracks their movements in the surrounding environment.
- User activity tracking: keeps track of the activities that a user is engaged with; for every activity the completed, ongoing and future steps are available (e.g., step 7 out of 15 in preparing dinner).
- User health state: this service stores—in a timely manner—various health-related information and exposes both aggregated and detailed (recent) data.
- User stress levels: provides access to users’ current and past stress levels, along with the identified stress factors.
- User sleep data: provides access to various sleep-related information (e.g., sleep duration, sleep score, time to fall asleep, snoring activity).
- User agenda: allows an ambient application to access and modify the user’s appointments, tasks, meetings, and events.
- Nutrition- and Diet-related services: such services provide information regarding the nutrition and ingredients of recipes, but they can also provide details regarding the meals that an individual had (e.g., type of meal, time that was consumed, quantity).
- Relaxation Programs: this service defines how the Intelligent Environment should be adapted in order to satisfy the requirements of a relaxation technique. It provides access to content (e.g., specific multimedia files) and information regarding the available/appropriate devices (along with their attributes) of a specific environment.
- Home Control: holds the current state and permits control of every application/device/service that is part of the Intelligent Environment (e.g., bed-side lamps are on, cake should be baked for seven more minutes).
5. Design Process
6. The CaLmi System
6.1. Overview
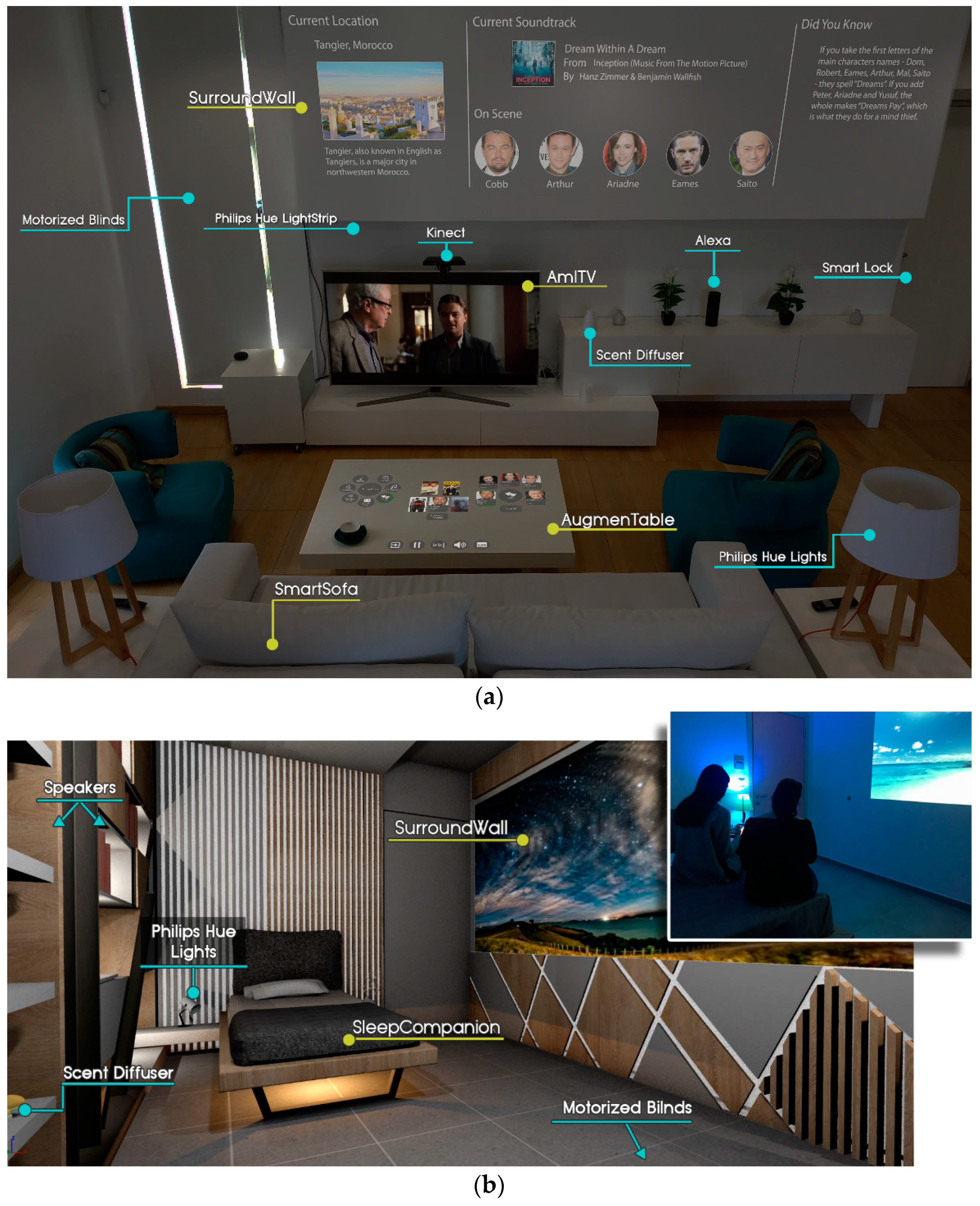
- Exposure to Nature: the main objective of this program is to make users feel like they are outdoors in a natural environment, such as a forest. In order to achieve this, when inside the intelligent home, the system can utilize all of the available artifacts of the user’s current room location. A collection of slideshows or videos is displayed in the largest and most convenient display area, while the lights adapt to a natural color, according to the displayed pictures or videos (e.g., when a sunset by the sea video is shown, lights take an orange hue). In addition, corresponding sounds can be heard from the sound system and the room is filled with a natural essence (e.g., when simulating a forest, the room takes a cypress scent).
- Meditation: this program gives the user the opportunity to practice a variety of meditation techniques, such as body scan, sitting meditation, and mindful hatha yoga. It consists of audio instructions and, when needed, guided meditation videos. Some of the techniques may require the user to have closed eyes, in which case meditation instructions are only given through the sound system, otherwise an instructional video is displayed on the screen closest to the user. In addition, the intelligent home automatically lowers the lights and a relaxing scent (e.g., sandalwood) fills the room.
- Relaxing Music: the sound system takes center role in this program. Relaxing songs (e.g., classical music tracks) can be heard from the room’s speakers and the lamps generate lighting patterns in real time based on the sound. Moreover, the user may choose to additionally use the aromatherapy system.
- Expressive Writing: this program consists of textual forms with questions that help the user to express their thoughts and feelings about problems of his/her everyday life that have affected their stress levels. The system supports multimodality by enabling the user to either express himself/herself in writing form or in a more natural way using his/her voice, which is then automatically transformed to text. While the user is interacting with the system, his/her written thoughts are displayed on the most convenient display. Additionally, the lighting in the room should be at appropriate levels for reading and writing. The user can also use the aromatherapy system in the same manner as the previous program.
- Customizable Programs: the developed relaxation player can be employed to support any of the aforementioned programs, either individually or in combination. For example, the user could be listening to music while he/she is writing about his/her feelings. This is possible, since the user is able to create his/her own relaxation program by combining the existing components. For example, the user could choose to display old family photographs on TV and his/her current stress level chart on the coffee table (which are two of the available display areas in the room he/she is currently in), to play Bach’s Prelude from the room’s speakers, not to use the scent diffuser, and to reduce the brightness of the lights.
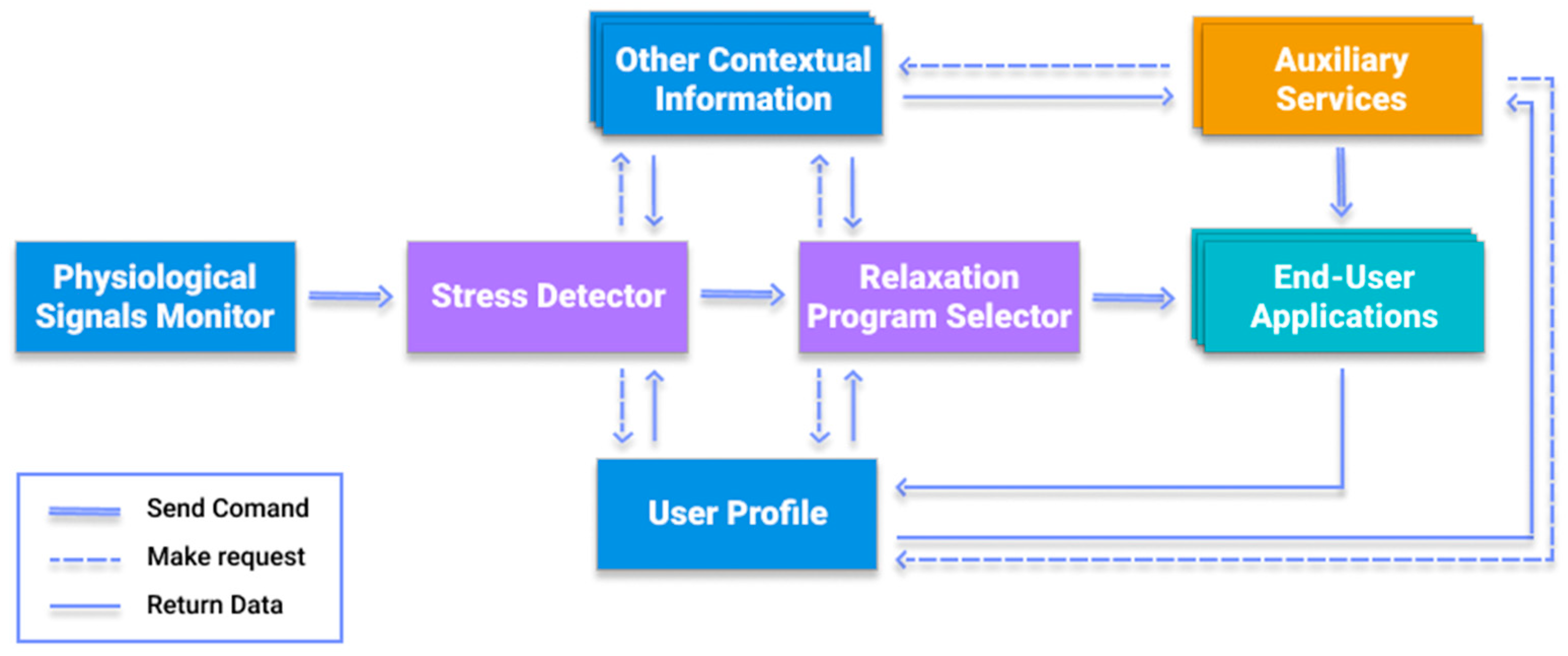
6.2. Architecture
6.3. End-User Applications
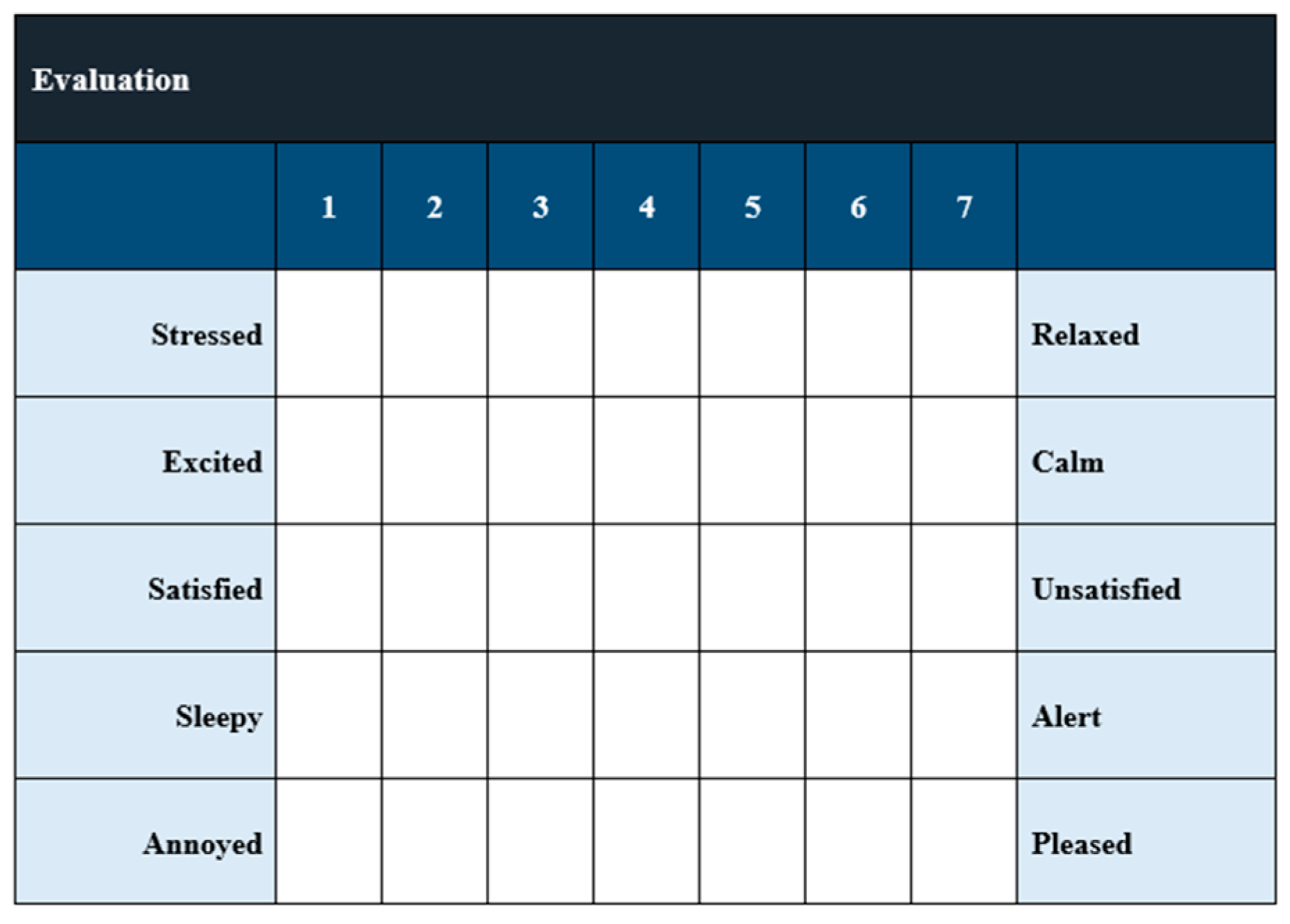
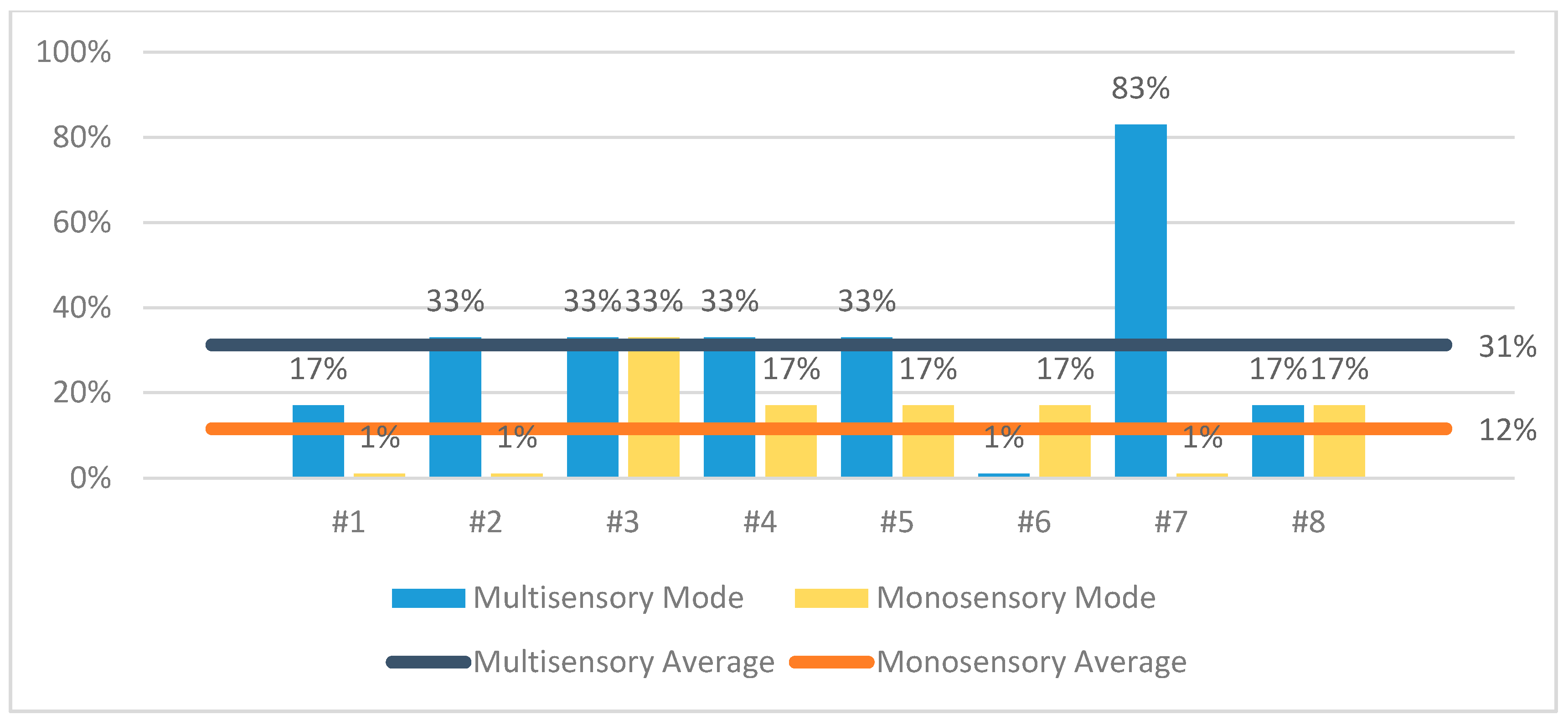
6.4. Evaluation
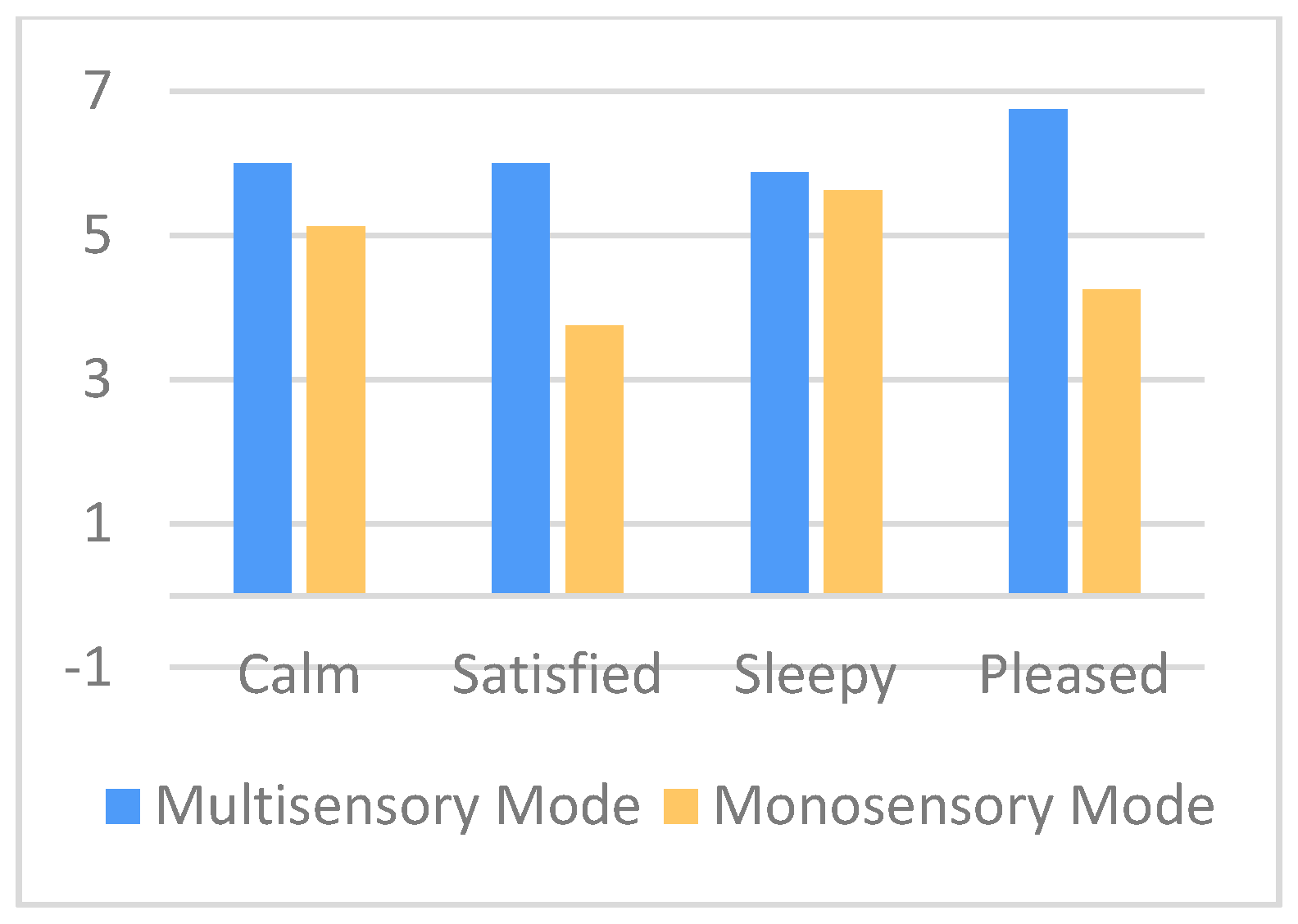
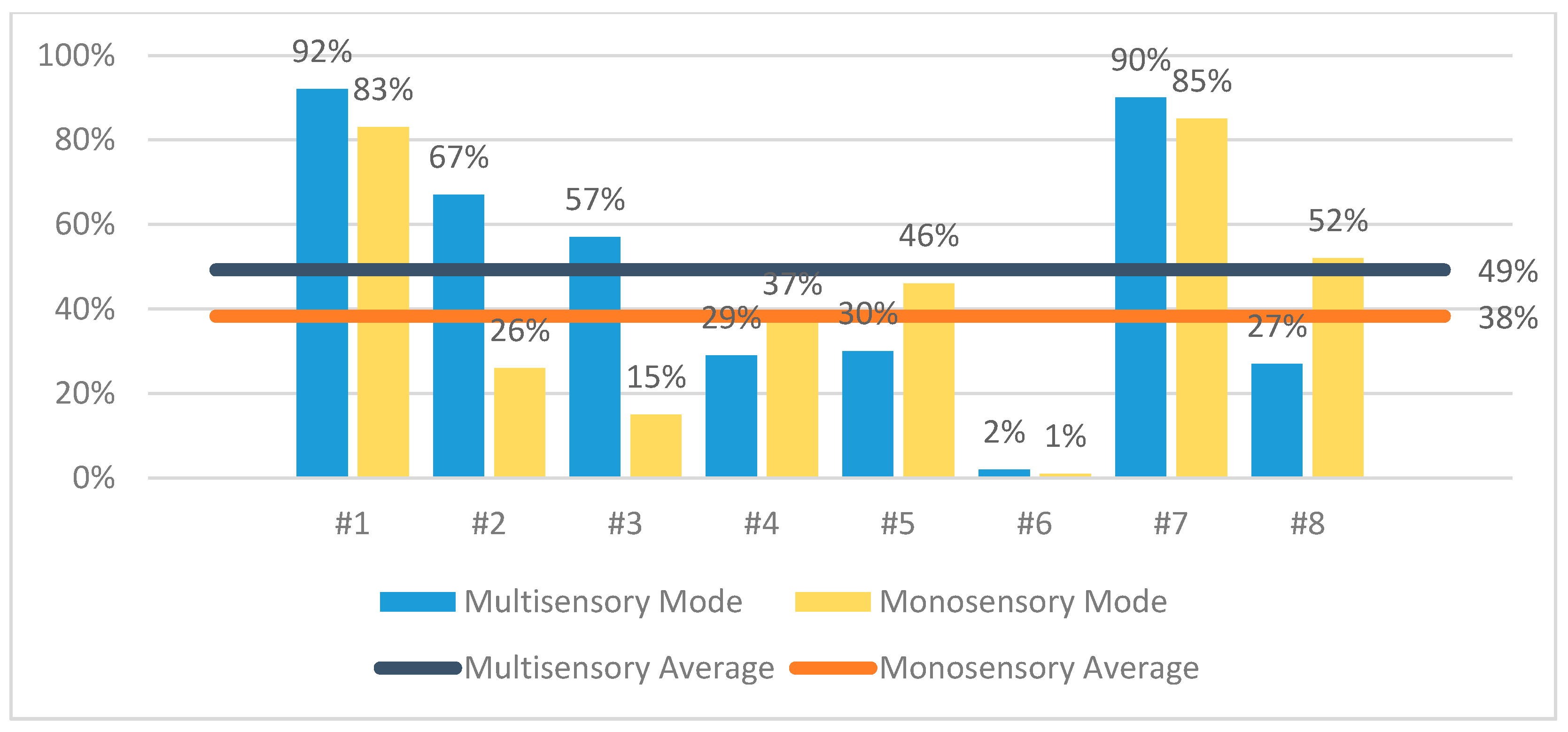
- Multisensory session: (a) displays a video of a forest waterfall on the main living room wall and adjusts the color (i.e., it takes a greenish-blue hue of the waterfall’s water) and the intensity (i.e., it decreases) of the room lighting, to activate the sense of sight. (b) Reproduces relaxing music and forest sounds (e.g., running water and birdsong) from the room’s speakers, to activate the sense of hearing. (c) Releases the lavender scent using the scent diffuser to activate the sense of smell.
- Monosensory session: displays the same video of a forest waterfall on a soundless tablet device to activate only the sense of sight.
7. The HypnOS System
7.1. Overview
7.2. Architecture
- Sleep Score Calculator predicts the “actual” sleep quality based on the monitored data. In particular, it detects sleep abnormalities in relation to the users’ sleep profile and daily history (e.g., increased bed movements, more awakenings after alcohol consumption) and it outlines their potential causes (e.g., eating a heavy dinner before going to bed). It is based on a heuristic algorithm that takes into account (a) the individual sleep scores that are calculated from the different sleep trackers (e.g., wearable activity tracker/watch), (b) the individual sleep scores that are extracted from the PSQI and SHI sleep questionnaires, which combine different sleep-related parameters (e.g., awakenings, total sleep duration) and other external factors (e.g., drink coffee too close to bedtime, do important work before bedtime), (c) users’ sleep history (average sleep duration, user slept close to his usual time, user woke up easily and close to his usual time), and (d) parameters that are extracted from the pre- and post-sleep diaries (that were provided by the HypnOS mobile application).
- Sleep Insights Generator produces personalized sleep recommendations based on a collection of template sleep hygiene rules. In more detail, it combines sleep data of the previous night with other factors, including: (a) user profile and sleep history information, (b) previous night’s sleep score, and (c) answers to the questions of the sleep diary, to extract personalized insights that encourage inhabitants to adopt healthier routines for the improvement of their sleep quality.
- Smart Alarm Scheduler estimates, the optimal time to wake up residents (e.g., the lightest possible stage of sleep just before desirable wake up time) by exploiting the available data from residents’ sleep profile (e.g., usual wake up time), and daily sleep record (e.g., light sleep). In addition, it takes the wake-up time that the users explicitly have set before they go to sleep into account.
- Sleep Program Recommender suggests relaxation programs for sleep, based on user preferences (e.g., user usually falls asleep with the “Rain Droplets” program) by utilizing information from the user profile. Additionally, it is able to calculate the effectiveness of each program by analyzing information, such as how long the user was in bed trying to sleep, and then adjusts its logic, so as to recommend the most effective programs.
7.3. End-User Applications
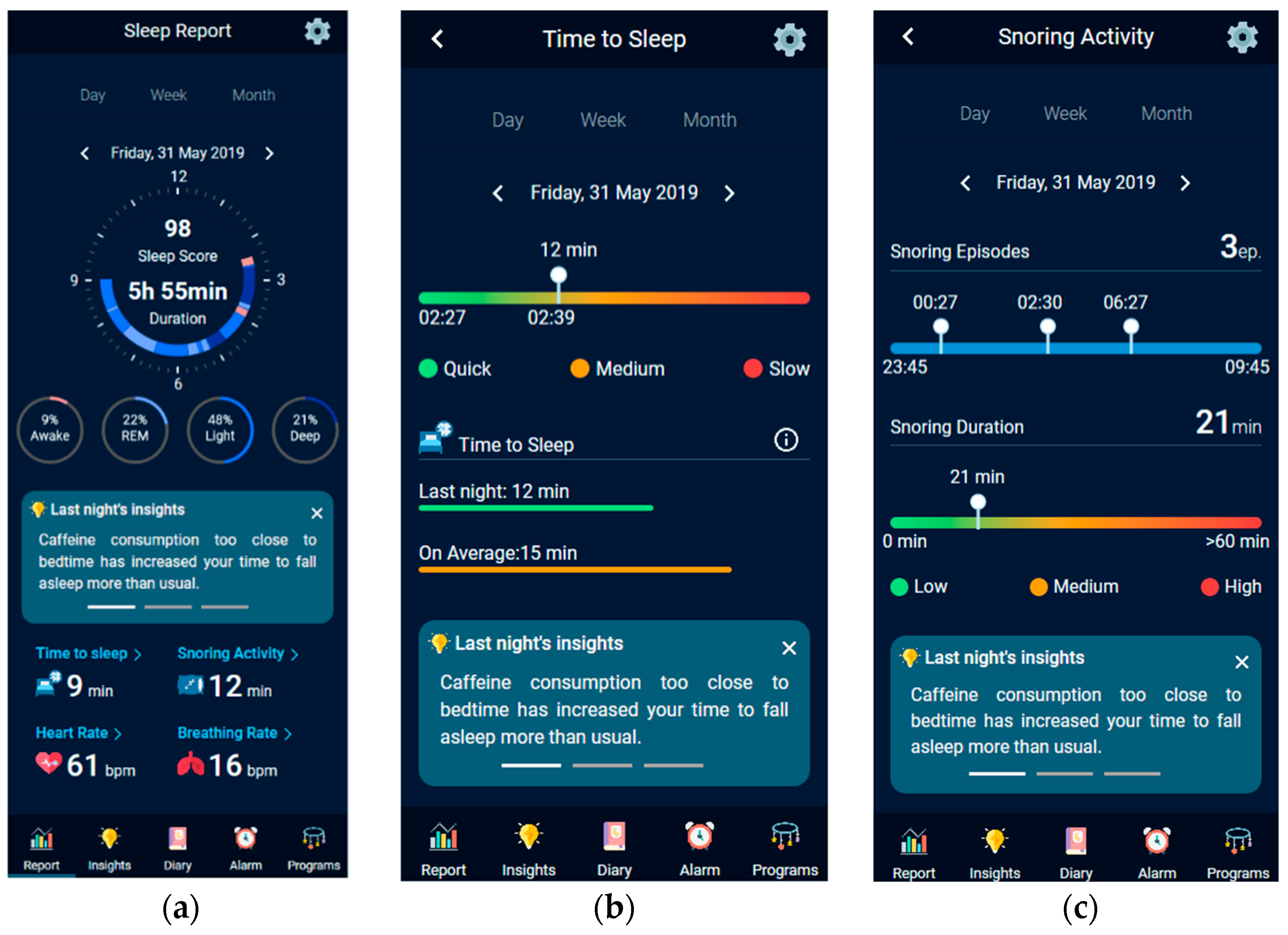
- Dashboard. Contains a detailed analysis of last night’s sleep (Figure 13a). Users can inspect information regarding (i) their sleep stages (i.e., duration of: Rapid Eye Movement stage, Light Sleep stage, and Deep Sleep stage), (ii) various sleep parameters (e.g., sleep duration, sleep score, time to fall asleep, snoring activity), and (iii) their bio-signals (e.g., nightly heart and breathing rate). Apart from the detailed report, users can find a list of useful sleep insights that they can follow to improve their sleep hygiene.
- Time to Sleep. Presents a horizontal bar chart that displays the time required to fall asleep (Figure 13b). This chart has a gradient fill which consists of three colors (i.e., green, orange, red), representing whether the required time was fast, medium, or slow. Additionally, the users can examine whether this time is in normal range according to their usual time required to fall asleep.
- Snoring activity. Displays two horizontal bar charts representing the user’s snoring episodes during the night, and the total snoring duration (Figure 13c).
- Heart Rate. Presents a spline chart displaying the user’s heart rate activity (Figure 14a), while it also shows the minimum, the maximum, and the average value of the heart rate during the previous night.
- Breathing Rate. Presents a spline chart, which represents the user’s breathing rate activity (Figure 14b). Furthermore, it shows the minimum, the maximum, and the average value of breathing during the previous night.
- Insights. Users are able to view personalized sleep insights on a daily basis. These insights are in the form of recommendations regarding users’ daily habits that affect sleep (e.g., “Drinking coffee two hours before bed time might negatively affect your sleep”). On the top of the page there is a date picker where users can select the date that they want to view their sleep insights. Each insight is associated with a specific category (e.g., Caffeine). Users can state whether they like an insight or not (i.e., upvote or downvote). In this way, this kind of insight does not show up again by clicking the buttons that are on the bottom of the sleep insight’s modal window (Figure 14c).
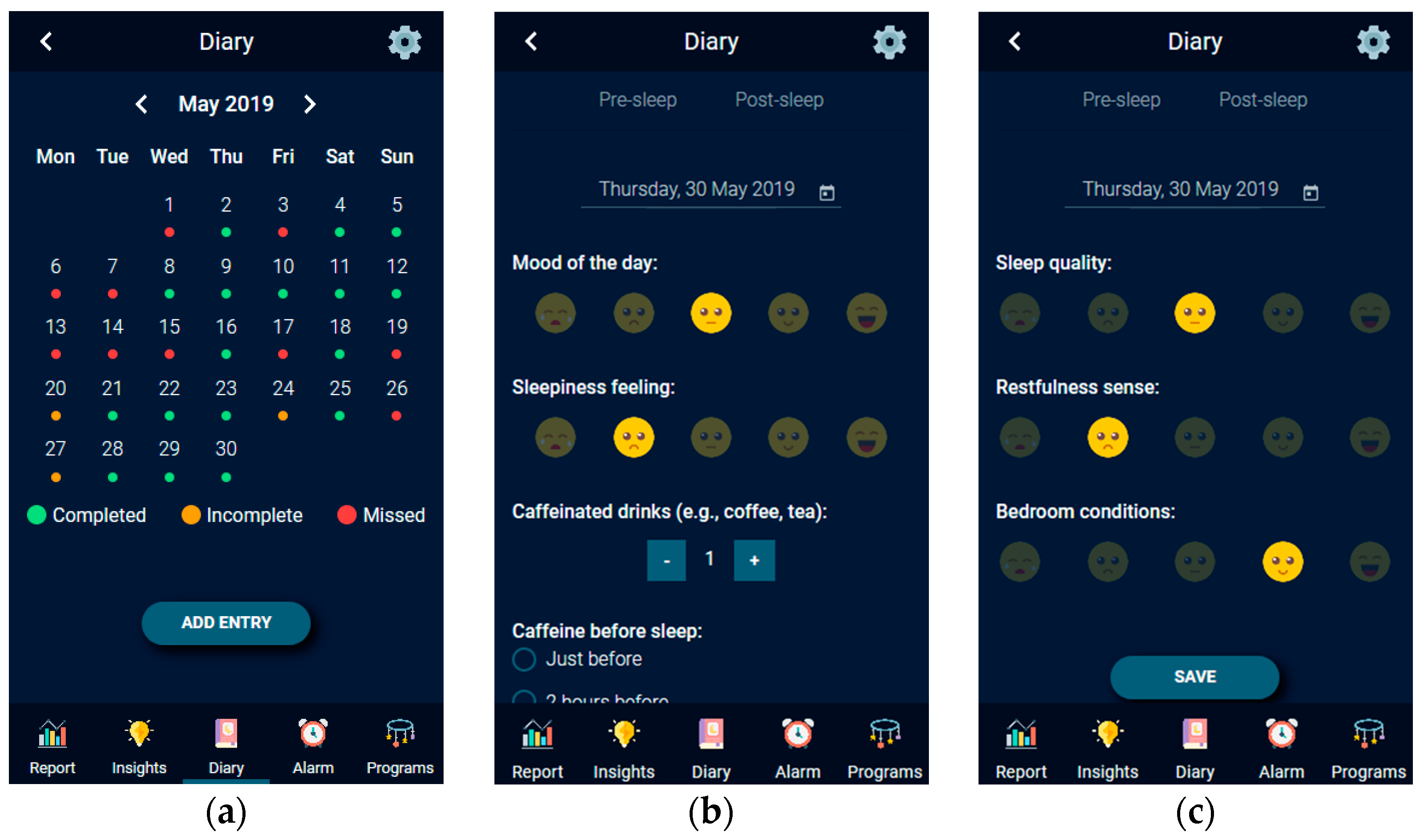
- Diary. Users are able to view a calendar displaying their diary entries for every day of the current month (Figure 15a). The calendar uses three colors to define the different diary entry states. The red color represents an empty diary entry, the orange represents an incomplete diary entry, and the green represents a successfully completed diary entry. Every day users receive two notification reminders to complete the sleep diary: one after waking up and one before going to bed. In case the users do not wish to fill-in the diary when prompted to do so by the system, they can manually select to do it at any time they wish.
- Pre-sleep Diary. Permits users to answer questions regarding their habits and feelings during the current day. These questions include subjective ratings for mood and sleepiness, as well as activities that may affect the sleep quality, such as caffeine and alcohol consumption (Figure 15b).
- Post-sleep Diary. Permits users to answer questions regarding their personal opinion about previous night’s sleep. These questions include subjective ratings for sleep quality, restfulness sense and bedroom conditions (Figure 15c).
- Alarm. Users can also set an alarm for a specific time, while they can also use the smart wake up feature that is offered by HypnOS. This feature permits users to select a timeframe within which the system must find the best possible moment to wake them up, based on when they are in their lightest stage of sleep. Finally, the users are able to adjust a variety of environmental factors (e.g., lights, sound, blinds, aroma scent), which are going to be activated in the morning, so as to facilitate the waking up process.
- Programs. Users are able to select relaxation programs (e.g., Sound Relaxation, Breathing Relaxation and Guided Imagery) in order to help them sleep. From the quick settings bar, users are able to stop the program at any time and activate or deactivate the ambient light, sound, scent, and projected multimedia.
7.4. Evaluation
7.4.1. Participants
7.4.2. Data Collection
7.4.3. Evaluation Experiment
7.4.4. Results
- Users’ impression of the Intelligent Bedroom was very positive. In particular, there were many positive comments regarding HypnOS’ ability to adjust the environment in order to create appropriate sleep/wake up conditions.
- The concept of HypnOS, although designed for those who have sleep issues, was found to be very useful and helpful for those who do not have any sleep difficulties as well.
- Users did not seem skeptical regarding HypnOS’ ability to collect information about their daily routine and habits, so as to provide personalized sleep insights. On the contrary, the majority of them stated that they do not mind if the system has access to their personal data, provided that they will be safe.
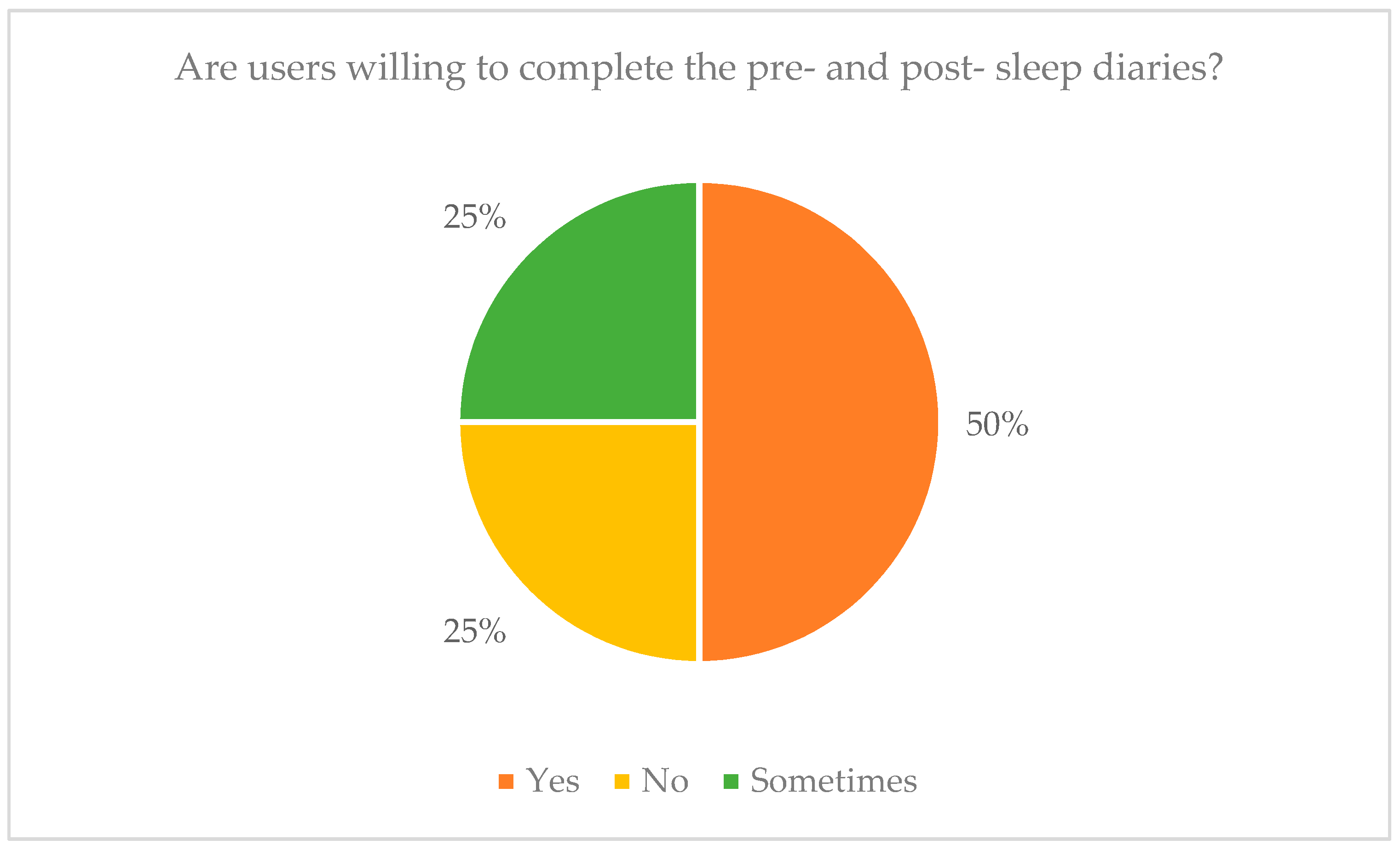
- Most of the users are willing to enter data manually if that means that the system will obtain useful information that result in personalized sleep insights. In more detail, 50% of the participants said that they would be willing to complete pre- and post-sleep diaries on a daily basis, especially if some fields were pre-selected. However, another 25% of participants reported that they would be bored to complete pre-sleep and post-sleep diaries on a daily basis, while the remaining 25% stated that they would complete them sometimes and not on a daily basis (Figure 18).
- The users would be willing to wear/use all the sleep trackers (e.g., wearable activity tracker/watch, under-the-mattress sleep tracker), except from the EEG headband, because they found it very obtrusive and irritating. However, given that individuals facing sleep issues are accustomed to wear various aids while they sleep, we are confident that they will be eager to use the headband provided that they will obtain useful insights regarding their sleep. For example, users that have obstructive sleep apnea and wearing a CPAP machine (a device that sends a steady flow of oxygen into nose and mouth as the wearer sleeps. This keeps the airways open and helps the individual to breathe normally) during sleep may be more willing to use it than others that do not have sleep issues.
8. Conclusions and Future Work
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Xia, F.; Yang, L.T.; Wang, L.; Vinel, A. Internet of Things. Int. J. Commun. Syst. 2012, 25, 1101. [Google Scholar] [CrossRef]
- Mell, P.; Grance, T. The NIST Definition of Cloud Computing; National Institute of Standards and Technologies: Gaithersburg, MD, USA, 2011.
- Aarts, E.; Wichert, R. Ambient intelligence. In Technology Guide; Springer: Berlin/Heidelberg, Germany, 2009; pp. 244–249. [Google Scholar]
- Cook, D.J.; Augusto, J.C.; Jakkula, V.R. Ambient Intelligence: Technologies, Applications, and Opportunities. Pervasive Mob. Comput. 2009, 5, 277–298. [Google Scholar] [CrossRef]
- Wilson, C.; Draper, S.; Brereton, M.; Johnson, D. Towards Thriving: Extending Computerised Cognitive Behavioural Therapy. In Proceedings of the 29th Australian Conference on Computer-Human Interaction, Brisbane, QLD, Australia, 28 November 2017; pp. 285–295. [Google Scholar]
- Alradhawi, M.; Shubber, N.; Sheppard, J.; Ali, Y. Effects of the COVID-19 Pandemic on Mental Well-Being amongst Individuals in Society-a Letter to the Editor on “The Socio-Economic Implications of the Coronavirus and COVID-19 Pandemic: A Review”. Int. J. Surg. Lond. Engl. 2020. [Google Scholar] [CrossRef]
- Cohen, S.; Janicki-Deverts, D.; Miller, G.E. Psychological Stress and Disease. JAMA 2007, 298, 1685–1687. [Google Scholar] [CrossRef] [PubMed]
- Brumitt, B.; Meyers, B.; Krumm, J.; Kern, A.; Shafer, S. Easyliving: Technologies for Intelligent Environments. In Proceedings of the International Symposium on Handheld and Ubiquitous Computing; Springer: Bristol, UK, 25 September 2000; pp. 12–29. [Google Scholar]
- Selye, H. Confusion and Controversy in the Stress Field. J. Human Stress 1975, 1, 37–44. [Google Scholar] [CrossRef]
- Rutten, P.F. Neuroepigenetics and Mental Illness; Elsevier Science: Maastricht, The Netherlands, 2018; ISBN 978-0-12-812593-9. [Google Scholar]
- Selye, H. The Stress of Life. J. Bone Jt. Surg. 1957, 39, 479. [Google Scholar]
- Chandola, T.; Brunner, E.; Marmot, M. Chronic Stress at Work and the Metabolic Syndrome: Prospective Study. BMJ 2006, 332, 521–525. [Google Scholar] [CrossRef]
- Hammen, C. Stress and Depression. Annu. Rev. Clin. Psychol. 2005, 1, 293–319. [Google Scholar] [CrossRef]
- Skosnik, P.D.; Chatterton Jr, R.T.; Swisher, T.; Park, S. Modulation of Attentional Inhibition by Norepinephrine and Cortisol after Psychological Stress. Int. J. Psychophysiol. 2000, 36, 59–68. [Google Scholar] [CrossRef]
- Lehner, P.; Seyed-Solorforough, M.-M.; O’Connor, M.F.; Sak, S.; Mullin, T. Cognitive Biases and Time Stress in Team Decision Making. IEEE Trans. Syst. Man Cybern.-Part Syst. Hum. 1997, 27, 698–703. [Google Scholar] [CrossRef]
- AXA Stress Index 2018|AXA UK. Available online: https://www.axa.co.uk/about/inside-axa/stress-index/ (accessed on 3 February 2021).
- Cohen, S.; Kamarck, T.; Mermelstein, R. Perceived Stress Scale. Meas. Stress Guide Health Soc. Sci. 1994, 10, 1–2. [Google Scholar]
- Gross, C.; Seebaß, K. The Standard Stress Scale (SSS): Measuring Stress in the Life Course. In Methodological Issues of Longitudinal Surveys; Springer: Berlin/Heidelberg, Germany, 2016; pp. 233–249. [Google Scholar]
- Dhole, N.P.; Gurjar, A.A. Detection of Speech under Stress: A Review. Int. J. Eng. Innov. Technol. IJEIT 2013, 2, 36–38. [Google Scholar]
- Lefter, I.; Burghouts, G.; Rothkrantz, L. Recognizing Stress Using Semantics and Modulation of Speech and Gestures. IEEE Trans. Affect. Comput. 2016. [Google Scholar] [CrossRef]
- Treigys, P.; Marcinkevičius, V.; Kaklauskas, A. Analysis of Iris and Pupil Parameters for Stress Recognition. Inf. Technol. Control 2012, 41, 7–14. [Google Scholar] [CrossRef]
- He, C.; Yao, Y.; Ye, X. An emotion recognition system based on physiological signals obtained by wearable sensors. In Wearable Sensors and Robots; Springer: Berlin/Heidelberg, Germany, 2017; pp. 15–25. [Google Scholar]
- Vrijkotte, T.G.; Van Doornen, L.J.; De Geus, E.J. Effects of Work Stress on Ambulatory Blood Pressure, Heart Rate, and Heart Rate Variability. Hypertension 2000, 35, 880–886. [Google Scholar] [CrossRef]
- Zangróniz, R.; Martínez-Rodrigo, A.; Pastor, J.M.; López, M.T.; Fernández-Caballero, A. Electrodermal Activity Sensor for Classification of Calm/Distress Condition. Sensors 2017, 17, 2324. [Google Scholar] [CrossRef]
- Karthikeyan, P.; Murugappan, M.; Yaacob, S. Descriptive Analysis of Skin Temperature Variability of Sympathetic Nervous System Activity in Stress. J. Phys. Ther. Sci. 2012, 24, 1341–1344. [Google Scholar] [CrossRef]
- McDuff, D.; Gontarek, S.; Picard, R. Remote Measurement of Cognitive Stress via Heart Rate Variability. In Proceedings of the Engineering in Medicine and Biology Society (EMBC), 2014 36th Annual International Conference of the IEEE, Chicago, IL, USA, 26–30 August 2014; pp. 2957–2960. [Google Scholar]
- Seo, S.-H.; Lee, J.-T. Stress and EEG. In Convergence and Hybrid Information Technologies; InTech: Rijeka, Croatia, 2010. [Google Scholar]
- Hellhammer, D.H.; Wüst, S.; Kudielka, B.M. Salivary Cortisol as a Biomarker in Stress Research. Psychoneuroendocrinology 2009, 34, 163–171. [Google Scholar] [CrossRef]
- Shields, S.A.; MacDowell, K.A.; Fairchild, S.B.; Campbell, M.L. Is Mediation of Sweating Cholinergic, Adrenergic, or Both? A Comment on the Literature. Psychophysiology 1987, 24, 312–319. [Google Scholar] [CrossRef] [PubMed]
- Westerink, J. Enhancing Well-Being through Psychophysiology. In Proceedings of the BIODEVICES, Porto, Portugal, 21 February 2017; p. 7. [Google Scholar]
- Kosti, R.; Alvarez, J.M.; Recasens, A.; Lapedriza, A. Emotion Recognition in Context. In Proceedings of the The IEEE Conference on Computer Vision and Pattern Recognition (CVPR), Honolulu, HI, USA, 21–26 July 2017; Volume 1. [Google Scholar]
- Australian Psychological Society. Stress & Wellbeing: How Australians Are Coping with Life: The Findings of the Australian Psychological Society Stress and Wellbeing in Australia Survey 2015; Australian Psychological Society: Melbourne, Australia, 2015. [Google Scholar]
- Pomerleau, C.S.; Pomerleau, O.F. The Effects of a Psychological Stressor on Cigarette Smoking and Subsequent Behavioral and Physiological Responses. Psychophysiology 1987, 24, 278–285. [Google Scholar] [CrossRef]
- Adam, T.C.; Epel, E.S. Stress, Eating and the Reward System. Physiol. Behav. 2007, 91, 449–458. [Google Scholar] [CrossRef]
- de Wit, H.; Söderpalm, A.H.; Nikolayev, L.; Young, E. Effects of Acute Social Stress on Alcohol Consumption in Healthy Subjects. Alcohol. Clin. Exp. Res. 2003, 27, 1270–1277. [Google Scholar] [CrossRef]
- Ranjita, L.; Sarada, N. Progressive Muscle Relaxation Therapy in Anxiety: A Neurophysiological Study. J. Dent. Med. Sci. 2014, 13, 25–28. [Google Scholar] [CrossRef]
- Ulrich, R.S. Visual Landscapes and Psychological Well-being. Landsc. Res. 1979, 4, 17–23. [Google Scholar] [CrossRef]
- van den Berg, M.M.; Maas, J.; Muller, R.; Braun, A.; Kaandorp, W.; van Lien, R.; van Poppel, M.N.; van Mechelen, W.; van den Berg, A.E. Autonomic Nervous System Responses to Viewing Green and Built Settings: Differentiating between Sympathetic and Parasympathetic Activity. Int. J. Environ. Res. Public Health 2015, 12, 15860–15874. [Google Scholar] [CrossRef]
- Song, C.; Ikei, H.; Miyazaki, Y. Physiological Effects of Visual Stimulation with Forest Imagery. Int. J. Environ. Res. Public Health 2018, 15, 213. [Google Scholar] [CrossRef]
- Ulrich, R.S.; Simons, R.F.; Losito, B.D.; Fiorito, E.; Miles, M.A.; Zelson, M. Stress Recovery during Exposure to Natural and Urban Environments. J. Environ. Psychol. 1991, 11, 201–230. [Google Scholar] [CrossRef]
- Laumann, K.; Gärling, T.; Stormark, K.M. Selective Attention and Heart Rate Responses to Natural and Urban Environments. J. Environ. Psychol. 2003, 23, 125–134. [Google Scholar] [CrossRef]
- Alvarsson, J.J.; Wiens, S.; Nilsson, M.E. Stress Recovery during Exposure to Nature Sound and Environmental Noise. Int. J. Environ. Res. Public Health 2010, 7, 1036–1046. [Google Scholar] [CrossRef] [PubMed]
- Ikei, H.; Song, C.; Miyazaki, Y. Physiological Effect of Olfactory Stimulation by Hinoki Cypress (Chamaecyparis Obtusa) Leaf Oil. J. Physiol. Anthropol. 2015, 34, 44. [Google Scholar] [CrossRef]
- Toda, M.; Morimoto, K. Effect of Lavender Aroma on Salivary Endocrinological Stress Markers. Arch. Oral Biol. 2008, 53, 964–968. [Google Scholar] [CrossRef]
- Chiesa, A.; Serretti, A. Mindfulness-Based Stress Reduction for Stress Management in Healthy People: A Review and Meta-Analysis. J. Altern. Complement. Med. 2009, 15, 593–600. [Google Scholar] [CrossRef]
- Khoury, B.; Sharma, M.; Rush, S.E.; Fournier, C. Mindfulness-Based Stress Reduction for Healthy Individuals: A Meta-Analysis. J. Psychosom. Res. 2015, 78, 519–528. [Google Scholar] [CrossRef]
- Ledesma, D.; Kumano, H. Mindfulness-based Stress Reduction and Cancer: A Meta-analysis. Psycho-Oncol. J. Psychol. Soc. Behav. Dimens. Cancer 2009, 18, 571–579. [Google Scholar] [CrossRef]
- Baer, R.A. Mindfulness Training as a Clinical Intervention: A Conceptual and Empirical Review. Clin. Psychol. Sci. Pract. 2003, 10, 125–143. [Google Scholar] [CrossRef]
- Peterson, L.G.; Pbert, L. Effectiveness of a Meditation-Based Stress Reduction Program in the Treatment of Anxiety Disorders. Am. J. Psychiatry 1992, 149, 936–943. [Google Scholar]
- Shapiro, S.L.; Brown, K.W.; Biegel, G.M. Teaching Self-Care to Caregivers: Effects of Mindfulness-Based Stress Reduction on the Mental Health of Therapists in Training. Train. Educ. Prof. Psychol. 2007, 1, 105. [Google Scholar] [CrossRef]
- Kabat-Zinn, J.; Hanh, T.N. Full Catastrophe Living: Using the Wisdom of Your Body and Mind to Face Stress, Pain, and Illness; Delta: New York, NY, USA, 2009; ISBN 0-307-56757-5. [Google Scholar]
- Jacobson, E. Progressive Relaxation; University Chicago Press: Chicago, IL, USA, 1938. [Google Scholar]
- Martarelli, D.; Cocchioni, M.; Scuri, S.; Pompei, P. Diaphragmatic Breathing Reduces Exercise-Induced Oxidative Stress. Evid. Based Complement. Alternat. Med. 2011. [Google Scholar] [CrossRef] [PubMed]
- Menzies, V.; Taylor, A.G. The Idea of Imagination: An Analysis of “Imagery”. Adv. Mind Body Med. 2004, 20, 4–10. [Google Scholar] [PubMed]
- Vettese, L.C.; Toneatto, T.; Stea, J.N.; Nguyen, L.; Wang, J.J. Do Mindfulness Meditation Participants Do Their Homework? And Does It Make a Difference? A Review of the Empirical Evidence. J. Cogn. Psychother. 2009, 23, 198. [Google Scholar] [CrossRef]
- Pelletier, C.L. The Effect of Music on Decreasing Arousal Due to Stress: A Meta-Analysis. J. Music Ther. 2004, 41, 192–214. [Google Scholar] [CrossRef] [PubMed]
- Panteleeva, Y.; Ceschi, G.; Glowinski, D.; Courvoisier, D.S.; Grandjean, D. Music for Anxiety? Meta-Analysis of Anxiety Reduction in Non-Clinical Samples. Psychol. Music 2017, 0305735617712424. [Google Scholar] [CrossRef]
- Thoma, M.V.; La Marca, R.; Brönnimann, R.; Finkel, L.; Ehlert, U.; Nater, U.M. The Effect of Music on the Human Stress Response. PLoS ONE 2013, 8, e70156. [Google Scholar] [CrossRef] [PubMed]
- Khalfa, S.; Dalla Bella, S.; Roy, M.; Peretz, I.; Lupien, S.J. Effects of Relaxing Music on Salivary Cortisol Level after Psychological Stress. Ann. N. Y. Acad. Sci. 2003, 999, 374–376. [Google Scholar] [CrossRef] [PubMed]
- Burns, J.L.; Labbé, E.; Arke, B.; Capeless, K.; Cooksey, B.; Steadman, A.; Gonzales, C. The Effects of Different Types of Music on Perceived and Physiological Measures of Stress. J. Music Ther. 2002, 39, 101–116. [Google Scholar] [CrossRef] [PubMed]
- Labbé, E.; Schmidt, N.; Babin, J.; Pharr, M. Coping with Stress: The Effectiveness of Different Types of Music. Appl. Psychophysiol. Biofeedback 2007, 32, 163–168. [Google Scholar] [CrossRef]
- Chafin, S.; Roy, M.; Gerin, W.; Christenfeld, N. Music Can Facilitate Blood Pressure Recovery from Stress. Br. J. Health Psychol. 2004, 9, 393–403. [Google Scholar] [CrossRef]
- Yu, B.; Hu, J.; Funk, M.; Feijs, L. A Study on User Acceptance of Different Auditory Content for Relaxation. In Proceedings of the Audio Mostly 2016, Norrköping Sweden, 4–6 October 2016; pp. 69–76. [Google Scholar]
- Smyth, J.M. Written Emotional Expression: Effect Sizes, Outcome Types, and Moderating Variables. J. Consult. Clin. Psychol. 1998, 66, 174. [Google Scholar] [CrossRef]
- Pennebaker, J.W. Writing about Emotional Experiences as a Therapeutic Process. Psychol. Sci. 1997, 8, 162–166. [Google Scholar] [CrossRef]
- Wyon, D.P.; Wargocki, P. Room Temperature Effects on Office Work; Taylor & Francis: London, UK, 2006. [Google Scholar]
- Custers, P.J.; De Kort, Y.A.W.; IJsselsteijn, W.A.; De Kruiff, M.E. Lighting in Retail Environments: Atmosphere Perception in the Real World. Light. Res. Technol. 2010, 42, 331–343. [Google Scholar] [CrossRef]
- Bellizzi, J.A.; Hite, R.E. Environmental Color, Consumer Feelings, and Purchase Likelihood. Psychol. Mark. 1992, 9, 347–363. [Google Scholar] [CrossRef]
- Keegan, L. Alternative and Complementary Modalities for Managing Stress and Anxiety. Crit Care Nurse 2000, 20, 93–96. [Google Scholar] [CrossRef] [PubMed]
- Hirshkowitz, M.; Whiton, K.; Albert, S.M.; Alessi, C.; Bruni, O.; DonCarlos, L.; Hazen, N.; Herman, J.; Hillard, P.J.A.; Katz, E.S. National Sleep Foundation’s Updated Sleep Duration Recommendations. Sleep Health 2015, 1, 233–243. [Google Scholar] [CrossRef]
- Philips Global Sleep Survey Shows We Want Better Sleep, but Only If It Comes Easily. Available online: https://www.philips.com/a-w/about/news/archive/standard/news/press/2019/20190307-philips-global-sleep-survey-shows-we-want-better-sleep-but-only-if-it-comes-easily.html (accessed on 25 May 2020).
- Bathory, E.; Tomopoulos, S. Sleep Regulation, Physiology and Development, Sleep Duration and Patterns, and Sleep Hygiene in Infants, Toddlers, and Preschool-Age Children. Curr. Probl. Pediatr. Adolesc. Health Care 2017, 47, 29–42. [Google Scholar] [CrossRef]
- Mukherjee, S.; Patel, S.R.; Kales, S.N.; Ayas, N.T.; Strohl, K.P.; Gozal, D.; Malhotra, A. An Official American Thoracic Society Statement: The Importance of Healthy Sleep. Recommendations and Future Priorities. Am. J. Respir. Crit. Care Med. 2015, 191, 1450–1458. [Google Scholar] [CrossRef] [PubMed]
- Barnes, C.M.; Drake, C.L. Prioritizing Sleep Health: Public Health Policy Recommendations. Perspect. Psychol. Sci. 2015, 10, 733–737. [Google Scholar] [CrossRef] [PubMed]
- Concepcion, T.; Barbosa, C.; Vélez, J.C.; Pepper, M.; Andrade, A.; Gelaye, B.; Yanez, D.; Williams, M.A. Daytime Sleepiness, Poor Sleep Quality, Eveningness Chronotype, and Common Mental Disorders among Chilean College Students. J. Am. Coll. Health 2014, 62, 441–448. [Google Scholar] [CrossRef] [PubMed]
- LeBlanc, M.; Beaulieu-Bonneau, S.; Mérette, C.; Savard, J.; Ivers, H.; Morin, C.M. Psychological and Health-Related Quality of Life Factors Associated with Insomnia in a Population-Based Sample. J. Psychosom. Res. 2007, 63, 157–166. [Google Scholar] [CrossRef] [PubMed]
- Strine, T.W.; Chapman, D.P. Associations of Frequent Sleep Insufficiency with Health-Related Quality of Life and Health Behaviors. Sleep Med. 2005, 6, 23–27. [Google Scholar] [CrossRef]
- Sadeh, A. III. Sleep Assessment Methods. Monogr. Soc. Res. Child Dev. 2015, 80, 33–48. [Google Scholar] [CrossRef] [PubMed]
- Holland, J.V.; Dement, W.C.; Raynal, D.M. Polysomnography: A Response to a Need for Improved Communication. Assoc. Psychophysiological Study Sleep 1974, 121–122. [Google Scholar]
- Butkov, N.; Keenan, S.A. An Overview of Polysomnographic Technique. In Sleep Disorders Medicine; Springer: Berlin/Heidelberg, Germany, 2017; pp. 267–294. [Google Scholar]
- Landry, G.J.; Best, J.R.; Liu-Ambrose, T. Measuring Sleep Quality in Older Adults: A Comparison Using Subjective and Objective Methods. Front. Aging Neurosci. 2015, 7, 166. [Google Scholar] [CrossRef]
- Monk, T.H.; Reynolds, C.F., III; Kupfer, D.J.; Buysse, D.J.; Coble, P.A.; Hayes, A.J.; Machen, M.A.; Petrie, S.R.; Ritenour, A.M. The Pittsburgh Sleep Diary. J. Sleep Res. 1994, 3, 111–120. [Google Scholar] [CrossRef] [PubMed]
- Buysse, D.J.; Reynolds, C.F.; Monk, T.H.; Berman, S.R.; Kupfer, D.J. The Pittsburgh Sleep Quality Index: A New Instrument for Psychiatric Practice and Research. Psychiatry Res 1989, 28, 193–213. [Google Scholar] [CrossRef]
- Hauri, P. Current Concepts: The Sleep Disorders; The Upjohn Company: Kalamazoo, MI, USA, 1977. [Google Scholar]
- Stepanski, E.J.; Wyatt, J.K. Use of Sleep Hygiene in the Treatment of Insomnia. Sleep Med. Rev. 2003, 7, 215–225. [Google Scholar] [CrossRef]
- Irish, L.A.; Kline, C.E.; Gunn, H.E.; Buysse, D.J.; Hall, M.H. The Role of Sleep Hygiene in Promoting Public Health: A Review of Empirical Evidence. Sleep Med. Rev. 2015, 22, 23–36. [Google Scholar] [CrossRef] [PubMed]
- Crispim, C.A.; Zimberg, I.Z.; dos Reis, B.G.; Diniz, R.M.; Tufik, S.; de Mello, M.T. Relationship between Food Intake and Sleep Pattern in Healthy Individuals. J. Clin. Sleep Med. 2011, 7, 659–664. [Google Scholar] [CrossRef]
- Sleep Environment. Available online: https://thesleepcharity.org.uk/information-support/adults/sleep-environment/ (accessed on 4 February 2021).
- Bedroom Environment: What Elements Are Important? Available online: https://www.sleepfoundation.org/bedroom-environment (accessed on 4 February 2021).
- Schubert, E.F.; Kim, J.K. Solid-State Light Sources Getting Smart. Science 2005, 308, 1274–1278. [Google Scholar] [CrossRef] [PubMed]
- Your Guide to Creating the Best Bedroom for Sleep. Available online: https://www.tuck.com/optimize-your-sleep-environment/ (accessed on 4 February 2021).
- Diego, M.A.; Jones, N.A.; Field, T.; Hernandez-Reif, M.; Schanberg, S.; Kuhn, C.; Galamaga, M.; McAdam, V.; Galamaga, R. Aromatherapy Positively Affects Mood, EEG Patterns of Alertness and Math Computations. Int. J. Neurosci. 1998, 96, 217–224. [Google Scholar] [CrossRef]
- Field, T.; Diego, M.; Hernandez-Reif, M.; Cisneros, W.; Feijo, L.; Vera, Y.; Gil, K.; Grina, D.; Claire He, Q. Lavender Fragrance Cleansing Gel Effects on Relaxation. Int. J. Neurosci. 2005, 115, 207–222. [Google Scholar] [CrossRef] [PubMed]
- Cho, M.-Y.; Min, E.S.; Hur, M.-H.; Lee, M.S. Effects of Aromatherapy on the Anxiety, Vital Signs, and Sleep Quality of Percutaneous Coronary Intervention Patients in Intensive Care Units. Evid. Based Complement. Alternat. Med. 2013, 2013. [Google Scholar] [CrossRef]
- Robb, S.L. Music Assisted Progressive Muscle Relaxation, Progressive Muscle Relaxation, Music Listening, and Silence: A Comparison of Relaxation Techniques. J. Music Ther. 2000, 37, 2–21. [Google Scholar] [CrossRef] [PubMed]
- Benson, H.; Klipper, M.Z. The Relaxation Response; Morrow: New York, NY, USA, 1975; ISBN 0-688-02955-8. [Google Scholar]
- Sykianaki, E.; Leonidis, A.; Antona, M.; Stephanidis, C. CaLmi: Stress Management in Intelligent Homes. In Proceedings of the Adjunct Proceedings of the 2019 ACM International Joint Conference on Pervasive and Ubiquitous Computing and Proceedings of the 2019 ACM International Symposium on Wearable Computers, London, UK, 11 September 2019; pp. 1202–1205. [Google Scholar]
- Freedman, R.; Papsdorf, J.D. Biofeedback and Progressive Relaxation Treatment of Sleep-Onset Insomnia. Biofeedback Self-Regul. 1976, 1, 253–271. [Google Scholar] [CrossRef]
- Hänsel, K. Wearable and Ambient Sensing for Well-Being and Emotional Awareness in the Smart Workplace. In Proceedings of the 2016 ACM International Joint Conference on Pervasive and Ubiquitous Computing: Adjunct, Heidelberg, Germany, 12 September 2016; pp. 411–416. [Google Scholar]
- Kocielnik, R.; Sidorova, N.; Maggi, F.M.; Ouwerkerk, M.; Westerink, J.H.D.M. Smart Technologies for Long-Term Stress Monitoring at Work. In Proceedings of the 26th IEEE International Symposium on Computer-Based Medical Systems, Porto, Portugal, 20–22 June 2013; pp. 53–58. [Google Scholar] [CrossRef]
- Bakker, J.; Pechenizkiy, M.; Sidorova, N. What’s Your Current Stress Level? Detection of Stress Patterns from GSR Sensor Data. In Proceedings of the 2011 IEEE 11th International Conference on Data Mining Workshops, Vancouver, BC, Canada, 11 December 2011; pp. 573–580. [Google Scholar]
- Trevia, F.G. Take Your Time: Combine Nature and Technology to Relieve Work Related Stress in the Office Environment. 2013. Available online: https://repository.tudelft.nl/islandora/object/uuid%3A714de8e5-21b8-44ff-a89a-3d9a9e6ee927 (accessed on 30 March 2021).
- de Aquino Lopes, R.; Cardoso, A.; Júnior, E.A.L.; Lopes, E.J. A Proposal for Stress Management Using Serious Games Associated to Virtual and Augmented Reality. J. Syst. 2014, 12, 1–7. [Google Scholar]
- Al Osman, H.; Dong, H.; El Saddik, A. Ubiquitous Biofeedback Serious Game for Stress Management. IEEE Access 2016, 4, 1274–1286. [Google Scholar] [CrossRef]
- Chen, J.; Zhu, B.; Balter, O.; Xu, J.; Zou, W.; Hedman, A.; Chen, R.; Sang, M. FishBuddy: Promoting Student Engagement in Self-Paced Learning through Wearable Sensing. In Proceedings of the 2017 IEEE International Conference on Smart Computing (SMARTCOMP), Hong Kong, China, 29–31 May 2017; pp. 1–9. [Google Scholar]
- Yu, B.; Hu, J.; Funk, M.; Feijs, L. DeLight: Biofeedback through Ambient Light for Stress Intervention and Relaxation Assistance. Pers. Ubiquitous Comput. 2018, 1–19. [Google Scholar] [CrossRef]
- Yu, B.; Hu, J.; Funk, M.; Liang, R.-H.; Xue, M.; Feijs, L. RESonance: Lightweight, Room-Scale Audio-Visual Biofeedback for Immersive Relaxation Training. IEEE Access 2018, 6, 38336–38347. [Google Scholar] [CrossRef]
- Hamon, M.; Ramadour, R.; Frey, J. Exploring Biofeedback with a Tangible Interface Designed for Relaxation. arXiv 2018, arXiv:180808711. [Google Scholar]
- Chen, Z.; Lin, M.; Chen, F.; Lane, N.D.; Cardone, G.; Wang, R.; Li, T.; Chen, Y.; Choudhury, T.; Campbell, A.T. Unobtrusive Sleep Monitoring Using Smartphones. In Proceedings of the 2013 7th International Conference on Pervasive Computing Technologies for Healthcare and Workshops, Venice, Italy, 5–8 May 2013; pp. 145–152. [Google Scholar]
- Hao, T.; Xing, G.; Zhou, G. ISleep: Unobtrusive Sleep Quality Monitoring Using Smartphones. In Proceedings of the 11th ACM Conference on Embedded Networked Sensor Systems, Rome, Italy, 11 November 2013; p. 4. [Google Scholar]
- Min, J.-K.; Doryab, A.; Wiese, J.; Amini, S.; Zimmerman, J.; Hong, J.I. Toss’n’turn: Smartphone as Sleep and Sleep Quality Detector. In Proceedings of the SIGCHI Conference on Human Factors in Computing Systems, Torronto, ON, Canada, 26 April 2014; pp. 477–486. [Google Scholar]
- Rahman, T.; Adams, A.T.; Ravichandran, R.V.; Zhang, M.; Patel, S.N.; Kientz, J.A.; Choudhury, T. Dopplesleep: A Contactless Unobtrusive Sleep Sensing System Using Short-Range Doppler Radar. In Proceedings of the 2015 ACM International Joint Conference on Pervasive and Ubiquitous Computing, Osaka, Japan, 7 September 2015; pp. 39–50. [Google Scholar]
- Choe, E.K.; Lee, B.; Kay, M.; Pratt, W.; Kientz, J.A. SleepTight: Low-Burden, Self-Monitoring Technology for Capturing and Reflecting on Sleep Behaviors. In Proceedings of the Proceedings of the 2015 ACM International Joint Conference on Pervasive and Ubiquitous Computing, Osaka, Japan, 7 September 2015; pp. 121–132. [Google Scholar]
- Bauer, J.S.; Consolvo, S.; Greenstein, B.; Schooler, J.; Wu, E.; Watson, N.F.; Kientz, J. ShutEye: Encouraging Awareness of Healthy Sleep Recommendations with a Mobile, Peripheral Display. In Proceedings of the Proceedings of the SIGCHI Conference on Human Factors in Computing Systems, Austin, TX, USA, 5–10 May 2012; pp. 1401–1410. [Google Scholar]
- Newman, S. Building Microservices: Designing Fine-Grained Systems; O’Reilly Media, Inc.: Boston, MA, USA, 2015; ISBN 1-4919-5033-1. [Google Scholar]
- Korozi, M.; Leonidis, A.; Antona, M.; Stephanidis, C. LECTOR: Towards Reengaging Students in the Educational Process Inside Smart Classrooms. In Proceedings of the International Conference on Intelligent Human Computer Interaction, Paris, France, 11 December 2017; pp. 137–149. [Google Scholar]
- Leonidis, A.; Arampatzis, D.; Louloudakis, N.; Stephanidis, C. The AmI-Solertis System: Creating User Experiences in Smart Environments. In Proceedings of the Wireless and Mobile Computing, Networking and Communications (WiMob), Rome, Italy, 9 October 2017; pp. 151–158. [Google Scholar]
- Poulter, A.J.; Johnston, S.J.; Cox, S.J. Using the MEAN Stack to Implement a RESTful Service for an Internet of Things Application. In Proceedings of the 2015 IEEE 2nd World Forum on Internet of Things (WF-IoT), Milan, Italy, 14–16 December 2015; pp. 280–285. [Google Scholar]
- Leonidis, A.; Korozi, M.; Kouroumalis, V.; Poutouris, E.; Stefanidi, E.; Arampatzis, D.; Sykianaki, E.; Anyfantis, N.; Kalligiannakis, E.; Nicodemou, V.C. Ambient Intelligence in the Living Room. Sensors 2019, 19, 5011. [Google Scholar] [CrossRef] [PubMed]
- Norman, D.A.; Draper, S.W. User Centered System Design: New Perspectives on Human-Computer Interaction; L. Erlbaum Assosiates Inc.: Hillsdale, NJ, USA, 1986; ISBN 1-4822-2963-3. [Google Scholar]
- Plattner, H.; Meinel, C.; Weinberg, U. Design-Thinking; Springer: Berlin/Heidelberg, Germany, 2009; ISBN 3-86880-013-1. [Google Scholar]
- What Is Design Thinking? Available online: https://www.interaction-design.org/literature/topics/design-thinking (accessed on 24 March 2020).
- Sun, F.-T.; Kuo, C.; Cheng, H.-T.; Buthpitiya, S.; Collins, P.; Griss, M. Activity-Aware Mental Stress Detection Using Physiological Sensors. In Proceedings of the International Conference on Mobile Computing, Applications, and Services, Santa Clara, CA, USA, 25 October 2010; pp. 282–301. [Google Scholar]
- Taylor, S.; Jaques, N.; Chen, W.; Fedor, S.; Sano, A.; Picard, R. Automatic Identification of Artifacts in Electrodermal Activity Data. In Proceedings of the 2015 37th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Milan, Italy, 25–29 August 2015; pp. 1934–1937. [Google Scholar]
- Peng, C.-Y.J.; Lee, K.L.; Ingersoll, G.M. An Introduction to Logistic Regression Analysis and Reporting. J. Educ. Res. 2002, 96, 3–14. [Google Scholar] [CrossRef]
- Sano, A.; Taylor, S.; McHill, A.W.; Phillips, A.J.; Barger, L.K.; Klerman, E.; Picard, R. Identifying Objective Physiological Markers and Modifiable Behaviors for Self-Reported Stress and Mental Health Status Using Wearable Sensors and Mobile Phones: Observational Study. J. Med. Internet Res. 2018. [Google Scholar] [CrossRef] [PubMed]
- Heiden, M.; Barnekow-Bergkvist, M.; Nakata, M.; Lyskov, E. Autonomic Activity, Pain, and Perceived Health in Patients on Sick Leave Due to Stress-Related Illnesses. Integr. Physiol. Behav. Sci. 2005, 40, 3–16. [Google Scholar] [CrossRef]
- Garwood, M.K.; Engel, B.T.; Quilter, R.E. Age Differences in the Effect of Epidermal Hydration on Electrodermal Activity. Psychophysiology 1979, 16, 311–317. [Google Scholar] [CrossRef] [PubMed]
- Sadeh, A.; Keinan, G.; Daon, K. Effects of Stress on Sleep: The Moderating Role of Coping Style. Health Psychol. 2004, 23, 542. [Google Scholar] [CrossRef]
- Carney, C.E.; Buysse, D.J.; Ancoli-Israel, S.; Edinger, J.D.; Krystal, A.D.; Lichstein, K.L.; Morin, C.M. The Consensus Sleep Diary: Standardizing Prospective Sleep Self-Monitoring. Sleep 2012, 35, 287–302. [Google Scholar] [CrossRef]
- Tonetti, L.; Mingozzi, R.; Natale, V. Comparison between Paper and Electronic Sleep Diary. Biol. Rhythm Res. 2016, 47, 743–753. [Google Scholar] [CrossRef]
- NSF Official Sleep Diary—National Sleep Foundation. Available online: https://www.sleepfoundation.org/articles/nsf-official-sleep-diary (accessed on 18 October 2019).
- Chen, C.; Härdle, W.K.; Unwin, A. Handbook of Data Visualization; Springer Science & Business Media: Berlin/Heidelberg, Germany, 2007; ISBN 3-540-33037-2. [Google Scholar]
- Accenture Always On, Always Connected-Finding Growth Opportunities in an Era of Hypermobile Consumers. Available online: https://www.accenture.com/t20150523T054032__w__/us-en/_acnmedia/Accenture/Conversion-Assets/DotCom/Documents/Global/PDF/Technology_1/Accenture-EHT-Research-2012-Consumer-Technology-Report.pdf (accessed on 4 February 2021).
- Levitas, D. Always Connected: How Smartphones and Social Keep Us Engaged. Available online: https://www.shrm.org/ResourcesAndTools/hr-topics/technology/Documents/PLAN-BB_Always_Connected_for_Facebook.pdf (accessed on 4 February 2021).
- Riley, W.T.; Rivera, D.E.; Atienza, A.A.; Nilsen, W.; Allison, S.M.; Mermelstein, R. Health Behavior Models in the Age of Mobile Interventions: Are Our Theories up to the Task? Transl. Behav. Med. 2011, 1, 53–71. [Google Scholar] [CrossRef]
- Peake, J.M.; Kerr, G.; Sullivan, J.P. A Critical Review of Consumer Wearables, Mobile Applications, and Equipment for Providing Biofeedback, Monitoring Stress, and Sleep in Physically Active Populations. Front. Physiol. 2018, 9, 743. [Google Scholar] [CrossRef] [PubMed]
- Ong, A.A.; Gillespie, M.B. Overview of Smartphone Applications for Sleep Analysis. World J. Otorhinolaryngol.-Head Neck Surg. 2016, 2, 45–49. [Google Scholar] [CrossRef]
- Nielsen, J. Usability Engineering; Morgan Kaufmann: San Francisco, CA, USA, 1994; ISBN 0-12-518406-9. [Google Scholar]
- Boulos, M.I.; Jairam, T.; Kendzerska, T.; Im, J.; Mekhael, A.; Murray, B.J. Normal Polysomnography Parameters in Healthy Adults: A Systematic Review and Meta-Analysis. Lancet Respir. Med. 2019, 7, 533–543. [Google Scholar] [CrossRef]
- Miner, B.; Kryger, M.H. Sleep in the Aging Population. Sleep Med. Clin. 2017, 12, 31–38. [Google Scholar] [CrossRef] [PubMed]
- Ohayon, M.M.; Carskadon, M.A.; Guilleminault, C.; Vitiello, M.V. Meta-Analysis of Quantitative Sleep Parameters from Childhood to Old Age in Healthy Individuals: Developing Normative Sleep Values across the Human Lifespan. Sleep 2004, 27, 1255–1273. [Google Scholar] [CrossRef] [PubMed]
- Katsanos, C.; Tselios, N.; Xenos, M. Perceived Usability Evaluation of Learning Management Systems: A First Step towards Standardization of the System Usability Scale in Greek. In Proceedings of the 2012 16th Panhellenic Conference on Informatics, Piraeus, Greece, 5 October 2012; pp. 302–307. [Google Scholar]
- Sauro, J.; Lewis, J.R. Quantifying the User Experience: Practical Statistics for User Research; Morgan Kaufmann: Burlington, MA, USA, 2016; ISBN 0-12-802548-4. [Google Scholar]
- Stress and Insomnia. Available online: https://www.sleepfoundation.org/insomnia/stress-and-insomnia (accessed on 9 February 2021).
- Stress and Sleep. Available online: https://www.apa.org/news/press/releases/stress/2013/sleep (accessed on 9 February 2021).
- Morin, C.M.; Carrier, J. The Acute Effects of the COVID-19 Pandemic on Insomnia and Psychological Symptoms. Sleep Med. 2020. [Google Scholar] [CrossRef]








Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Leonidis, A.; Korozi, M.; Sykianaki, E.; Tsolakou, E.; Kouroumalis, V.; Ioannidi, D.; Stavridakis, A.; Antona, M.; Stephanidis, C. Improving Stress Management and Sleep Hygiene in Intelligent Homes. Sensors 2021, 21, 2398. https://doi.org/10.3390/s21072398
Leonidis A, Korozi M, Sykianaki E, Tsolakou E, Kouroumalis V, Ioannidi D, Stavridakis A, Antona M, Stephanidis C. Improving Stress Management and Sleep Hygiene in Intelligent Homes. Sensors. 2021; 21(7):2398. https://doi.org/10.3390/s21072398
Chicago/Turabian StyleLeonidis, Asterios, Maria Korozi, Eirini Sykianaki, Eleni Tsolakou, Vasilios Kouroumalis, Danai Ioannidi, Andreas Stavridakis, Margherita Antona, and Constantine Stephanidis. 2021. "Improving Stress Management and Sleep Hygiene in Intelligent Homes" Sensors 21, no. 7: 2398. https://doi.org/10.3390/s21072398
APA StyleLeonidis, A., Korozi, M., Sykianaki, E., Tsolakou, E., Kouroumalis, V., Ioannidi, D., Stavridakis, A., Antona, M., & Stephanidis, C. (2021). Improving Stress Management and Sleep Hygiene in Intelligent Homes. Sensors, 21(7), 2398. https://doi.org/10.3390/s21072398









