Label-Free Bioelectrochemical Methods for Evaluation of Anticancer Drug Effects at a Molecular Level
Abstract
1. Introduction
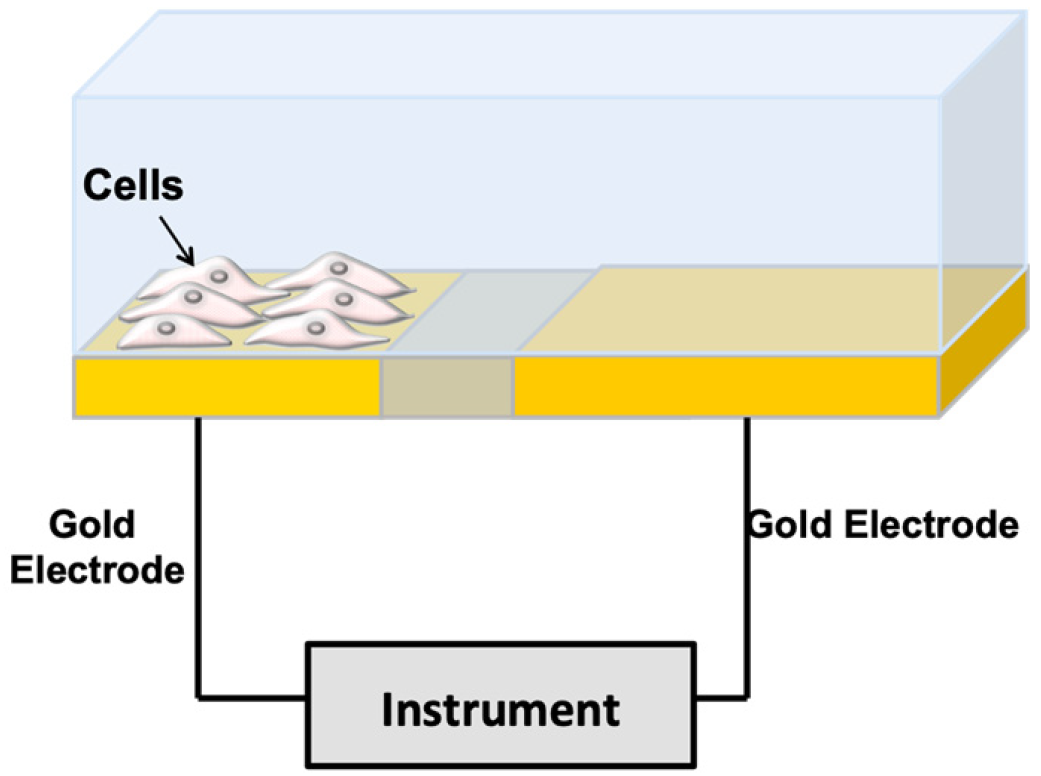
2. Impedance-Based Methods for Cell Monitoring
| Anticancer Drug | Tumor Derived Cell Lines | Observed Effect | Specific Comments | Comparison Biochemical Assay | Ref |
|---|---|---|---|---|---|
| Carboplatin, Paclitaxel | Breast cancer, melanoma and human prostate cancer cells | Cell viability | Microfluidic platform. Dynamic delivery of the drug to cancer cells seeded in a chamber containing interdigitated microelectrodes. | MTT assay | [21] |
| Cisplatin | Oral cancer | Cell viability | High concentration of nicotine exhibited inhibitory effect on 20 μM cisplatin-induced apoptosis. | - | [22] |
| Cisplatin | Brest cancer | Cell attachment, spreading and drug-induced apoptosis | Time dependent behavior. | Morphological analysis | [16] |
| Cisplatin | Esophageal cancer | Cell morphology | Morphology changes of cells adhesion, spreading, and proliferation can be detected by impedimetric analysis. | Fluorescence imaging | [23] |
| Doxorubicin | Neuroblastoma and glioblastoma | Cell viability | Time dependent IC50. IC50 at 48 h for neuroblastoma cells: 1.77 nM IC50 at 48 h for glioblastoma cells: 4.04 nM | Tunel assay, Flow cytometry | [17] |
| Doxorubicin | Laryngopharynx cancer | Cell viability | Microfluidic platform enabling both electrochemical and optical detection. | Fluorescence-based cytotoxicity assay (annexin V/propidium iodide end point staining). | [13] |
| Doxorubicin | Breast cancer | Cell morphology | Drug resistant breast cancer cells have been differentiated from their parental cells based on their dielectric properties. Drug response at different stages of the disease is described. | Fluorescence microscopy | [15] |
| Etoposide | Neuroblastoma and glioblastoma | Cell viability | Time dependent IC50. IC50 at 48 h for neuroblastoma cells: 3.83 nM | Tunel assay, flow cytometry | [17] |
| Fluorouracil | Cancer microtissue spheroids | Cell viability | Evaluation of a multiplexed EIS platform analysis in a microfluidic setting. | - | [24] |
| Nicotine, Antrodia Camphorata ext. | Different cell lines | Cell morphology | - | SEM imaging | [25] |
| Vemurafenib and other MAPK-targeting therapeutics | Melanoma | Cell viability | Comparability of chemosensitivity performed by correlation analysis, showing that impedance and ATP assay data were highly correlative (0.8 < r2 < 1.0) | ATP assay | [19] |
| Vincristine | Neuroblastoma and glioblastoma | Cell viability | IC50 at 48 h for neuroblastoma cells (3D cultures): 1.16 nM IC50 at 48 h for glioblastoma cells (3D cultures): 1.54 nM | Tunel assay, flow cytometry | [17] |
| ZD6474 | Breast cancer | Cell viability | Time and drug concentration dependent behavior | MTT assay | [26] |
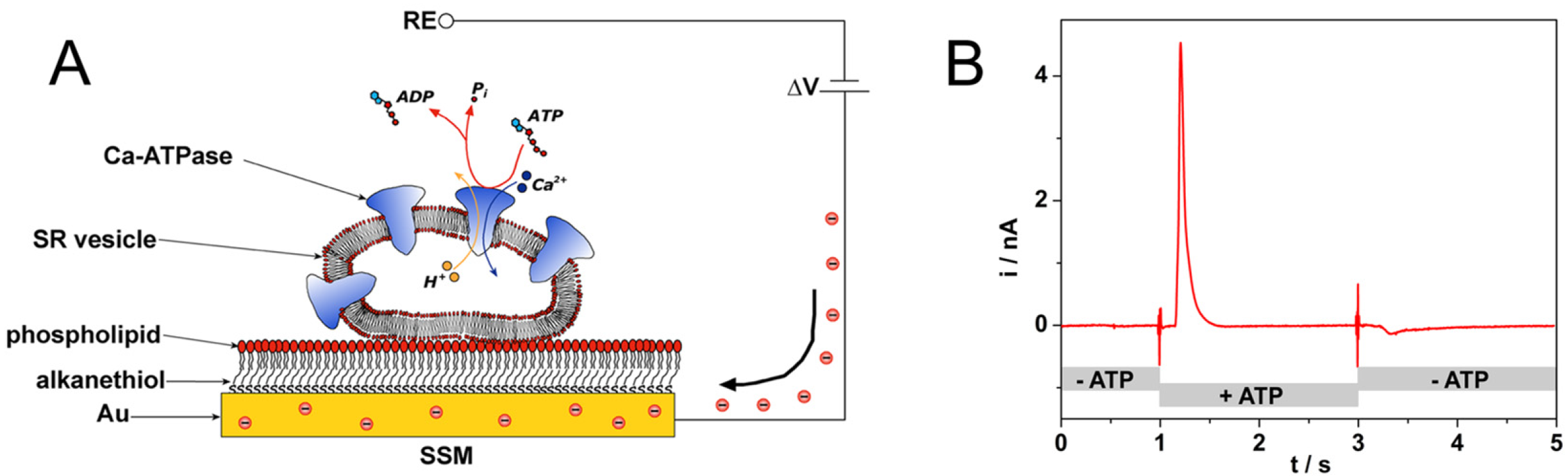
3. Solid Supported Membranes for Functional Analysis of Membrane Transporters
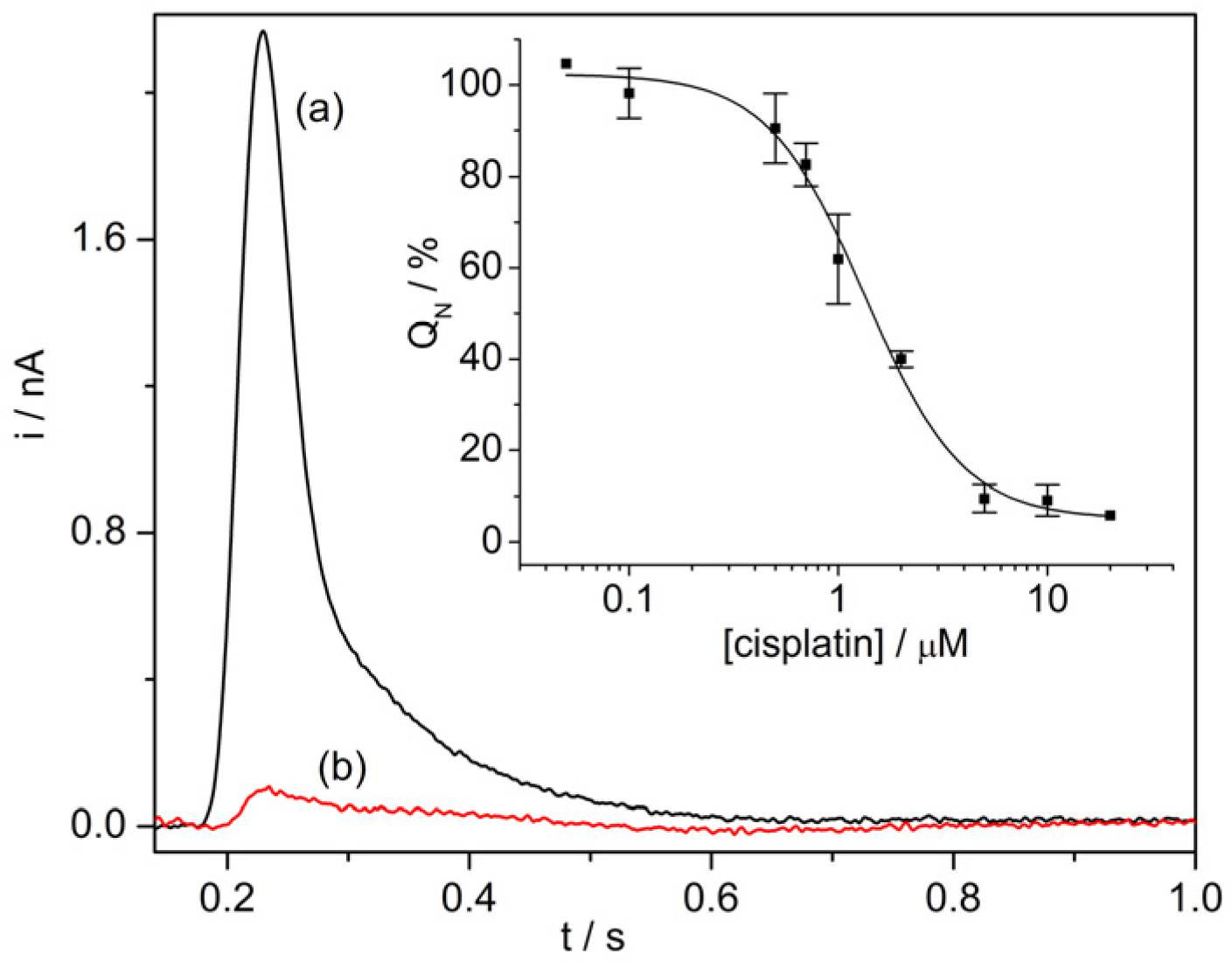
Anticancer Drug–Protein Interactions Monitored on SSMs
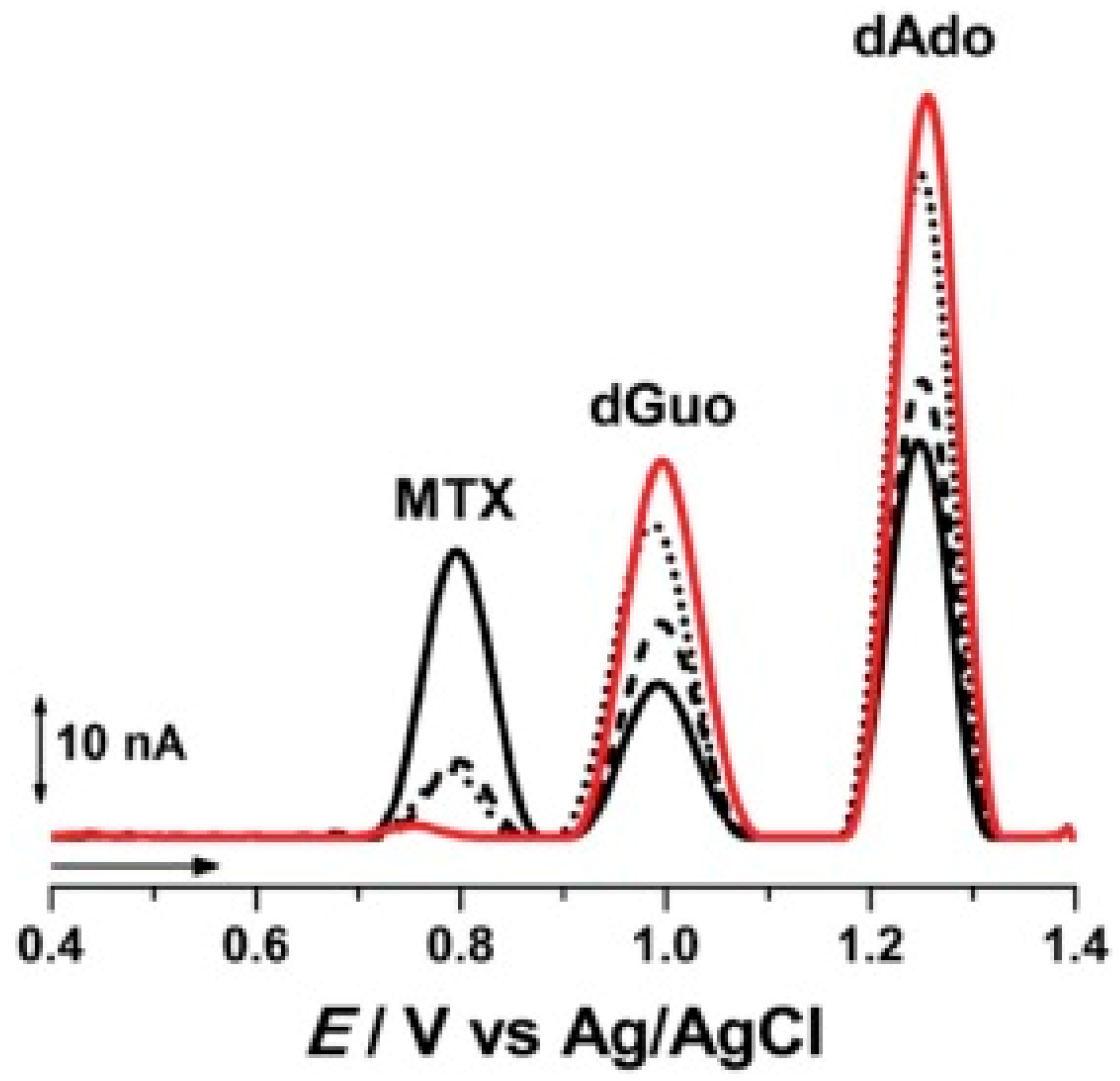
4. Electrochemical Nucleic Acid-Based Sensors
5. Other Bioelectrochemical Approaches
6. Conclusions
Author Contributions
Acknowledgments
Conflicts of Interest
References
- World Health Organisation. Cancer. Available online: https://www.who.int/health-topics/cancer#tab=tab_1 (accessed on 17 January 2020).
- Mitxelena-Iribarren, O.; Zabalo, J.; Arana, S.; Mujika, M. Improved microfluidic platform for simultaneous multiple drug screening towards personalized treatment. Biosens. Bioelectron. 2019, 123, 237–243. [Google Scholar] [CrossRef] [PubMed]
- Ediriweera, M.K.; Tennekoon, K.H.; Samarakoon, S.R. In vitro assays and techniques utilized in anticancer drug discovery. J. Appl. Toxicol. 2019, 39, 38–71. [Google Scholar] [CrossRef] [PubMed]
- Couto, G.K.; Segatto, N.V.; Oliveira, T.L.; Seixas, F.K.; Schachtschneider, K.M.; Collares, T. The Melding of Drug Screening Platforms for Melanoma. Front. Oncol. 2019, 9, 1–20. [Google Scholar] [CrossRef]
- Szymański, P.; Markowicz, M.; Mikiciuk-Olasik, E. Adaptation of high-throughput screening in drug discovery-toxicological screening tests. Int. J. Mol. Sci. 2012, 13, 427–452. [Google Scholar] [CrossRef] [PubMed]
- Giaever, I.; Keese, C.R. Monitoring fibroblast behavior in tissue culture with an applied electric field. Proc. Natl. Acad. Sci. USA 1984, 81, 3761–3764. [Google Scholar] [CrossRef] [PubMed]
- Ramasamy, S.; Bennet, D.; Kim, S. Drug and bioactive molecule screening based on a bioelectrical impedance cell culture platform. Int. J. Nanomed. 2014, 9, 5789–5809. [Google Scholar]
- Asphahani, F.; Zhang, M. Cellular impedance biosensors for drug screening and toxin detection. Analyst 2007, 132, 835–841. [Google Scholar] [CrossRef]
- Lundstrom, K. Cell-impedance-based label-free technology for the identification of new drugs. Expert Opin. Drug Discov. 2017, 12, 335–343. [Google Scholar] [CrossRef]
- Bettazzi, F.; Palchetti, I. Nanotoxicity assessment: A challenging application for cutting edge electroanalytical tools. Anal. Chim. Acta 2019, 1072, 61–74. [Google Scholar] [CrossRef]
- Heileman, K.; Daoud, J.; Tabrizian, M. Dielectric spectroscopy as a viable biosensing tool for cell and tissue characterization and analysis. Biosens. Bioelectron. 2013, 49, 348–359. [Google Scholar] [CrossRef]
- Caviglia, C.; Zór, K.; Canepa, S.; Carminati, M.; Larsen, L.B.; Raiteri, R.; Andresen, T.L.; Heiskanen, A.; Emnéus, J. Interdependence of initial cell density, drug concentration and exposure time revealed by real-time impedance spectroscopic cytotoxicity assay. Analyst 2015, 140, 3623–3629. [Google Scholar] [CrossRef] [PubMed]
- Caviglia, C.; Zór, K.; Montini, L.; Tilli, V.; Canepa, S.; Melander, F.; Muhammad, H.B.; Carminati, M.; Ferrari, G.; Raiteri, R.; et al. Impedimetric Toxicity Assay in Microfluidics Using Free and Liposome-Encapsulated Anticancer Drugs. Anal. Chem. 2015, 87, 2204–2212. [Google Scholar] [CrossRef] [PubMed]
- Zór, K.; Heiskanen, A.; Caviglia, C.; Vergani, M.; Landini, E.; Shah, F.; Carminati, M.; Martínez-Serrano, A.; Moreno, T.R.; Kokaia, M.; et al. A compact multifunctional microfluidic platform for exploring cellular dynamics in real-time using electrochemical detection. RSC Adv. 2014, 4, 63761–63771. [Google Scholar] [CrossRef]
- Eker, B.; Meissner, R.; Bertsch, A.; Mehta, K.; Renaud, P. Label-free recognition of drug resistance via impedimetric screening of breast cancer cells. PLoS ONE 2013, 8, e57423. [Google Scholar] [CrossRef] [PubMed]
- Anh-Nguyen, T.; Tiberius, B.; Pliquett, U.; Urban, G.A. An impedance biosensor for monitoring cancer cell attachment, spreading and drug-induced apoptosis. Sens. Actuators A Phys. 2016, 241, 231–237. [Google Scholar] [CrossRef]
- Eichler, M.; Jahnke, H.-G.; Krinke, D.; Müller, A.; Schmidt, S.; Azendorf, R.; Robitzki, A.A. A novel 96-well multielectrode array based impedimetric monitoring platform for comparative drug efficacy analysis on 2D and 3D brain tumor cultures. Biosens. Bioelectron. 2015, 67, 582–589. [Google Scholar] [CrossRef] [PubMed]
- Lei, K.F.; Lin, B.-Y.; Tsang, N.-M. Real-time and label-free impedimetric analysis of the formation and drug testing of tumor spheroids formed via the liquid overlay technique. RSC Adv. 2017, 7, 13939–13946. [Google Scholar] [CrossRef]
- Seidel, D.; Rothe, R.; Kirsten, M.; Jahnke, H.-G.; Dumann, K.; Ziemer, M.; Simon, J.-C.; Robitzki, A.A. A multidimensional impedance platform for the real-time analysis of single and combination drug pharmacology in patient-derived viable melanoma models. Biosens. Bioelectron. 2019, 123, 185–194. [Google Scholar] [CrossRef]
- Cheung, K.; Gawad, S.; Renaud, P. Impedance spectroscopy flow cytometry: On-chip label-free cell differentiation. Cytom. Part A 2005, 65A, 124–132. [Google Scholar] [CrossRef]
- Pandya, H.J.; Dhingra, K.; Prabhakar, D.; Chandrasekar, V.; Natarajan, S.K.; Vasan, A.S.; Kulkarni, A.; Shafiee, H. A microfluidic platform for drug screening in a 3D cancer microenvironment. Biosens. Bioelectron. 2017, 94, 632–642. [Google Scholar] [CrossRef]
- Arias, L.R.; Perry, C.A.; Yang, L. Real-time electrical impedance detection of cellular activities of oral cancer cells. Biosens. Bioelectron. 2010, 25, 2225–2231. [Google Scholar] [CrossRef] [PubMed]
- Liu, Q.; Yu, J.; Xiao, L.; Tang, J.C.O.; Zhang, Y.; Wang, P.; Yang, M. Impedance studies of bio-behavior and chemosensitivity of cancer cells by micro-electrode arrays. Biosens. Bioelectron. 2009, 24, 1305–1310. [Google Scholar] [CrossRef] [PubMed]
- Bürgel, S.C.; Diener, L.; Frey, O.; Kim, J.-Y.; Hierlemann, A. Automated, Multiplexed Electrical Impedance Spectroscopy Platform for Continuous Monitoring of Microtissue Spheroids. Anal. Chem. 2016, 88, 10876–10883. [Google Scholar] [CrossRef]
- Messina, W.; Fitzgerald, M.; Moore, E. SEM and ECIS Investigation of Cells Cultured on Nanopillar Modified Interdigitated Impedance Electrodes for Analysis of Cell Growth and Cytotoxicity of Potential Anticancer Drugs. Electroanalysis 2016, 28, 2188–2195. [Google Scholar] [CrossRef]
- Pradhan, R.; Rajput, S.; Mandal, M.; Mitra, A.; Das, S. Electric cell–substrate impedance sensing technique to monitor cellular behaviours of cancer cells. RSC Adv. 2014, 4, 9432–9438. [Google Scholar] [CrossRef]
- Plant, A.L. Supported Hybrid Bilayer Membranes as Rugged Cell Membrane Mimics. Langmuir 1999, 15, 5128–5135. [Google Scholar] [CrossRef]
- Florin, E.-L.; Gaub, H.E. Painted supported lipid membranes. Biophys. J. 1993, 64, 375–383. [Google Scholar] [CrossRef]
- Seifert, K.; Fendler, K.; Bamberg, E. Charge transport by ion translocating membrane proteins on solid supported membranes. Biophys. J. 1993, 64, 384–391. [Google Scholar] [CrossRef]
- Steinem, C.; Janshoff, A.; Ulrich, W.-P.; Sieber, M.; Galla, H.-J. Impedance analysis of supported lipid bilayer membranes: A scrutiny of different preparation techniques. Biochim. Biophys. Acta Biomembr. 1996, 1279, 169–180. [Google Scholar] [CrossRef]
- Castellana, E.T.; Cremer, P.S. Solid supported lipid bilayers: From biophysical studies to sensor design. Surf. Sci. Rep. 2006, 61, 429–444. [Google Scholar] [CrossRef]
- Pintschovius, J.; Fendler, K. Charge Translocation by the Na+/K+-ATPase Investigated on Solid Supported Membranes: Rapid Solution Exchange with a New Technique. Biophys. J. 1999, 76, 814–826. [Google Scholar] [CrossRef]
- Tadini-Buoninsegni, F.; Bartolommei, G. Electrophysiological Measurements on Solid Supported Membranes. Method. Mol. Biol. 2016, 1377, 293–303. [Google Scholar]
- Tadini-Buoninsegni, F.; Bartolommei, G.; Moncelli, M.R.; Guidelli, R.; Inesi, G. Pre-steady State Electrogenic Events of Ca2+/H+ Exchange and Transport by the Ca2+-ATPase. J. Biol. Chem. 2006, 281, 37720–37727. [Google Scholar] [CrossRef] [PubMed]
- Schulz, P.; Garcia-Celma, J.J.; Fendler, K. SSM-based electrophysiology. Methods 2008, 46, 97–103. [Google Scholar] [CrossRef] [PubMed]
- Tadini-Buoninsegni, F.; Bartolommei, G.; Moncelli, M.R.; Fendler, K. Charge transfer in P-type ATPases investigated on planar membranes. Arch. Biochem. Biophys. 2008, 476, 75–86. [Google Scholar] [CrossRef]
- Zhou, A.; Wozniak, A.; Meyer-Lipp, K.; Nietschke, M.; Jung, H.; Fendler, K. Charge Translocation During Cosubstrate Binding in the Na+/Proline Transporter of E.coli. J. Mol. Biol. 2004, 343, 931–942. [Google Scholar] [CrossRef]
- Garcia-Celma, J.J.; Smirnova, I.N.; Kaback, H.R.; Fendler, K. Electrophysiological characterization of LacY. Proc. Natl. Acad. Sci. USA 2009, 106, 7373–7378. [Google Scholar] [CrossRef] [PubMed]
- Krause, R.; Watzke, N.; Kelety, B.; Dörner, W.; Fendler, K. An automatic electrophysiological assay for the neuronal glutamate transporter mEAAC1. J. Neurosci. Methods 2009, 177, 131–141. [Google Scholar] [CrossRef] [PubMed]
- Rycovska, A.; Hatahet, L.; Fendler, K.; Michel, H. The nitrite transport protein NirC from Salmonella typhimurium is a nitrite/proton antiporter. Biochim. Biophys. Acta Biomembr. 2012, 1818, 1342–1350. [Google Scholar] [CrossRef]
- Patiño-Ruiz, M.; Dwivedi, M.; Călinescu, O.; Karabel, M.; Padan, E.; Fendler, K. Replacement of Lys-300 with a glutamine in the NhaA Na+/H+ antiporter of Escherichia coli yields a functional electrogenic transporter. J. Biol. Chem. 2019, 294, 246–256. [Google Scholar] [CrossRef]
- Yatime, L.; Buch-Pedersen, M.J.; Musgaard, M.; Morth, J.P.; Winther, A.-M.L.; Pedersen, B.P.; Olesen, C.; Andersen, J.P.; Vilsen, B.; Schiøtt, B.; et al. P-type ATPases as drug targets: Tools for medicine and science. Biochim. Biophys. Acta Bioenerg. 2009, 1787, 207–220. [Google Scholar] [CrossRef]
- Pintschovius, J.; Fendler, K.; Bamberg, E. Charge Translocation by the Na+/K+-ATPase Investigated on Solid Supported Membranes: Cytoplasmic Cation Binding and Release. Biophys. J. 1999, 76, 827–836. [Google Scholar] [CrossRef]
- Liu, Y.; Pilankatta, R.; Lewis, D.; Inesi, G.; Tadini-Buoninsegni, F.; Bartolommei, G.; Moncelli, M.R. High-yield Heterologous Expression of Wild Type and Mutant Ca2+ ATPase: Characterization of Ca2+ Binding Sites by Charge Transfer. J. Mol. Biol. 2009, 391, 858–871. [Google Scholar] [CrossRef]
- Kelety, B.; Diekert, K.; Tobien, J.; Watzke, N.; Dörner, W.; Obrdlik, P.; Fendler, K. Transporter Assays Using Solid Supported Membranes: A Novel Screening Platform for Drug Discovery. Assay Drug Dev. Technol. 2006, 4, 575–582. [Google Scholar] [CrossRef]
- Tadini-Buoninsegni, F.; Bartolommei, G.; Moncelli, M.R.; Pilankatta, R.; Lewis, D.; Inesi, G. ATP dependent charge movement in ATP7B Cu+-ATPase is demonstrated by pre-steady state electrical measurements. FEBS Lett. 2010, 584, 4619–4622. [Google Scholar] [CrossRef] [PubMed]
- Mattle, D.; Zhang, L.; Sitsel, O.; Pedersen, L.T.; Moncelli, M.R.; Tadini-Buoninsegni, F.; Gourdon, P.; Rees, D.C.; Nissen, P.; Meloni, G. A sulfur-based transport pathway in Cu+-ATPases. EMBO Rep. 2015, 16, 728–740. [Google Scholar] [CrossRef] [PubMed]
- Tadini-Buoninsegni, F.; Mikkelsen, S.A.; Mogensen, L.S.; Molday, R.S.; Andersen, J.P. Phosphatidylserine flipping by the P4-ATPase ATP8A2 is electrogenic. Proc. Natl. Acad. Sci. USA 2019, 116, 16332–16337. [Google Scholar] [CrossRef] [PubMed]
- Geibel, S.; Flores-Herr, N.; Licher, T.; Vollert, H. Establishment of Cell-Free Electrophysiology for Ion Transporters: Application for Pharmacological Profiling. J. Biomol. Screen. 2006, 11, 262–268. [Google Scholar] [CrossRef] [PubMed]
- Bazzone, A.; Barthmes, M.; Fendler, K. SSM-Based Electrophysiology for Transporter Research. Method. Enzymol. 2017, 594, 31–83. [Google Scholar]
- Kaplan, J.H. Biochemistry of Na,K-ATPase. Annu. Rev. Biochem. 2002, 71, 511–535. [Google Scholar] [CrossRef]
- Møller, J.V.; Olesen, C.; Winther, A.-M.L.; Nissen, P. The sarcoplasmic Ca2+-ATPase: Design of a perfect chemi-osmotic pump. Q. Rev. Biophys. 2010, 43, 501–566. [Google Scholar] [CrossRef] [PubMed]
- Tadini-Buoninsegni, F.; Sordi, G.; Smeazzetto, S.; Natile, G.; Arnesano, F. Effect of cisplatin on the transport activity of PII-type ATPases. Metallomics 2017, 9, 960–968. [Google Scholar] [CrossRef] [PubMed]
- Wang, D.; Lippard, S.J. Cellular processing of platinum anticancer drugs. Nat. Rev. Drug Discov. 2005, 4, 307–320. [Google Scholar] [CrossRef] [PubMed]
- Dmitriev, O.Y. Mechanism of tumor resistance to cisplatin mediated by the copper transporter ATP7B. Biochem. Cell Biol. 2011, 89, 138–147. [Google Scholar] [CrossRef]
- Li, Y.-Q.; Yin, J.-Y.; Liu, Z.-Q.; Li, X.-P. Copper efflux transporters ATP7A and ATP7B: Novel biomarkers for platinum drug resistance and targets for therapy. IUBMB Life 2018, 70, 183–191. [Google Scholar] [CrossRef]
- Petruzzelli, R.; Polishchuk, S.R. Activity and Trafficking of Copper-Transporting ATPases in Tumor Development and Defense against Platinum-Based Drugs. Cells 2019, 8, 1080. [Google Scholar] [CrossRef]
- Lutsenko, S.; Barnes, N.L.; Bartee, M.Y.; Dmitriev, O.Y. Function and Regulation of Human Copper-Transporting ATPases. Physiol. Rev. 2007, 87, 1011–1046. [Google Scholar] [CrossRef]
- Safaei, R.; Otani, S.; Larson, B.J.; Rasmussen, M.L.; Howell, S.B. Transport of Cisplatin by the Copper Efflux Transporter ATP7B. Mol. Pharmacol. 2008, 73, 461–468. [Google Scholar] [CrossRef]
- Tadini-Buoninsegni, F.; Bartolommei, G.; Moncelli, M.R.; Inesi, G.; Galliani, A.; Sinisi, M.; Losacco, M.; Natile, G.; Arnesano, F. Translocation of Platinum Anticancer Drugs by Human Copper ATPases ATP7A and ATP7B. Angew. Chemie Int. Ed. 2014, 53, 1297–1301. [Google Scholar] [CrossRef]
- Calandrini, V.; Arnesano, F.; Galliani, A.; Nguyen, T.H.; Ippoliti, E.; Carloni, P.; Natile, G. Platination of the copper transporter ATP7A involved in anticancer drug resistance. Dalt. Trans. 2014, 43, 12085–12094. [Google Scholar] [CrossRef]
- Sadafi, F.-Z.; Massai, L.; Bartolommei, G.; Moncelli, M.R.; Messori, L.; Tadini-Buoninsegni, F. Anticancer Ruthenium(III) Complex KP1019 Interferes with ATP-Dependent Ca2+ Translocation by Sarco-Endoplasmic Reticulum Ca2+-ATPase (SERCA). ChemMedChem 2014, 9, 1660–1664. [Google Scholar] [CrossRef] [PubMed]
- Alessio, E.; Messori, L. NAMI-A and KP1019/1339, Two Iconic Ruthenium Anticancer Drug Candidates Face-to-Face: A Case Story in Medicinal Inorganic Chemistry. Molecules 2019, 24, 1995. [Google Scholar] [CrossRef] [PubMed]
- Labuda, J.; Oliveira Brett, A.M.; Evtugyn, G.; Fojta, M.; Mascini, M.; Ozsoz, M.; Palchetti, I.; Paleček, E.; Wang, J. Electrochemical nucleic acid-based biosensors: Concepts, terms, and methodology (IUPAC Technical Report). Pure Appl. Chem. 2010, 82, 1161–1187. [Google Scholar] [CrossRef]
- Voccia, D.; Sosnowska, M.; Bettazzi, F.; Roscigno, G.; Fratini, E.; De Franciscis, V.; Condorelli, G.; Chitta, R.; D’Souza, F.; Kutner, W.; et al. Direct determination of small RNAs using a biotinylated polythiophene impedimetric genosensor. Biosens. Bioelectron. 2017, 87, 1012–1019. [Google Scholar] [CrossRef]
- Ferapontova, E.E. Basic concepts and recent advances in electrochemical analysis of nucleic acids. Curr. Opin. Electrochem. 2017, 5, 218–225. [Google Scholar] [CrossRef]
- Bettazzi, F.; Laschi, S.; Voccia, D.; Gellini, C.; Pietraperzia, G.; Falciola, L.; Pifferi, V.; Testolin, A.; Ingrosso, C.; Placido, T.; et al. Ascorbic acid-sensitized Au nanorods-functionalized nanostructured TiO2 transparent electrodes for photoelectrochemical genosensing. Electrochim. Acta 2018, 276, 389–398. [Google Scholar] [CrossRef]
- Mascini, M.; Palchetti, I.; Tombelli, S. Nucleic acid and peptide aptamers: Fundamentals and bioanalytical aspects. Angew. Chemie Int. Ed. 2012, 51, 1316–1332. [Google Scholar] [CrossRef]
- Lucarelli, F.; Kicela, A.; Palchetti, I.; Marrazza, G.; Mascini, M. Electrochemical DNA biosensor for analysis of wastewater samples. Bioelectrochemistry 2002, 58, 113–118. [Google Scholar] [CrossRef]
- Kadimisetty, K.; Malla, S.; Rusling, J.F. Automated 3-D Printed Arrays to Evaluate Genotoxic Chemistry: E-Cigarettes and Water Samples. ACS Sens. 2017, 2, 670–678. [Google Scholar] [CrossRef]
- Krejcova, L.; Richtera, L.; Hynek, D.; Labuda, J.; Adam, V. Current Trends in Electrochemical Sensing and Biosensing of DNA Methylation. Biosens. Bioelectron. 2017, 97, 384–399. [Google Scholar] [CrossRef]
- Diculescu, V.C.; Chiorcea-Paquim, A.-M.; Oliveira-Brett, A.M. Applications of a DNA-electrochemical biosensor. TrAC Trends Anal. Chem. 2016, 79, 23–36. [Google Scholar] [CrossRef]
- Fojta, M.; Daňhel, A.; Havran, L.; Vyskočil, V. Recent progress in electrochemical sensors and assays for DNA damage and repair. TrAC - Trends Anal. Chem. 2016, 79, 160–167. [Google Scholar] [CrossRef]
- Nemcekova, K.; Labuda, J.; Milata, V.; Blaškovičová, J.; Sochr, J. Interaction of DNA and mononucleotides with theophylline investigated using electrochemical biosensors and biosensing. Bioelectrochemistry 2018, 123, 182–189. [Google Scholar] [CrossRef]
- Svitková, V.; Hanzelyová, M.; Macková, H.; Blaškovičová, J.; Vyskočil, V.; Farkašová, D.; Labuda, J. Behaviour and detection of acridine-type DNA intercalators in urine using an electrochemical DNA-based biosensor with the protective polyvinyl alcohol membrane. J. Electroanal. Chem. 2018, 821, 87–91. [Google Scholar] [CrossRef]
- Kuzin, Y.; Kappo, D.; Porfireva, A.; Shurpik, D.; Stoikov, I.; Evtugyn, G.; Hianik, T. Electrochemical DNA Sensor Based on Carbon Black—Poly(Neutral Red) Composite for Detection of Oxidative DNA Damage. Sensors 2018, 18, 3489. [Google Scholar] [CrossRef] [PubMed]
- Wang, G.; Wang, H.; Cao, S.; Xiang, W.; Li, T.; Yang, M. Electrochemical determination of the activity and inhibition of telomerase based on the interaction of DNA with molybdate. Microchim. Acta 2019, 186, 96. [Google Scholar] [CrossRef]
- Kanat, E.; Eksin, E.; Karacicek, B.; Eraç, Y.; Erdem, A. Electrochemical Detection of Interaction between Dacarbazine and Nucleic Acids in Comparison to Agarose Gel Electrophoresis. Electroanalysis 2018, 30, 1566–1574. [Google Scholar] [CrossRef]
- Hagner, N.; Joerger, M. Cancer chemotherapy: Targeting folic acid synthesis. Cancer Manag. Res. 2010, 2, 293–301. [Google Scholar] [PubMed]
- Pontinha, A.D.R.; Jorge, S.M.A.; Chiorcea Paquim, A.-M.; Diculescu, V.C.; Oliveira-Brett, A.M. In situ evaluation of anticancer drug methotrexate–DNA interaction using a DNA-electrochemical biosensor and AFM characterization. Phys. Chem. Chem. Phys. 2011, 13, 5227–5234. [Google Scholar] [CrossRef]
- Chen, J.; Fu, B.; Liu, T.; Yan, Z.; Li, K. A Graphene Oxide-DNA Electrochemical Sensor Based on Glassy Carbon Electrode for Sensitive Determination of Methotrexate. Electroanalysis 2018, 30, 288–295. [Google Scholar] [CrossRef]
- Shoja, Y.; Kermanpur, A.; Karimzadeh, F.; Ghodsi, J.; Rafati, A.A.; Adhami, S. Electrochemical molecularly bioimprinted siloxane biosensor on the basis of core/shell silver nanoparticles/EGFR exon 21 L858R point mutant gene/siloxane film for ultra-sensing of Gemcitabine as a lung cancer chemotherapy medication. Biosens. Bioelectron. 2019, 145, 111611. [Google Scholar] [CrossRef] [PubMed]
- Hillard, E.A.; de Abreu, F.C.; Ferreira, D.C.M.; Jaouen, G.; Goulart, M.O.F.; Amatore, C. Electrochemical parameters and techniques in drug development, with an emphasis on quinones and related compounds. Chem. Commun. 2008, 23, 2612–2628. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Peng, Z.; Wang, E. Tackling Grand Challenges of the 21st Century with Electroanalytical Chemistry. J. Am. Chem. Soc. 2018, 140, 10629–10638. [Google Scholar] [CrossRef] [PubMed]
- Clausmeyer, J.; Schuhmann, W. Nanoelectrodes: Applications in electrocatalysis, single-cell analysis and high-resolution electrochemical imaging. TrAC Trends Anal. Chem. 2016, 79, 46–59. [Google Scholar] [CrossRef]
- Ino, K.; Şen, M.; Shiku, H.; Matsue, T. Micro/nanoelectrochemical probe and chip devices for evaluation of three-dimensional cultured cells. Analyst 2017, 142, 4343–4354. [Google Scholar] [CrossRef]
- Li, Y.; Sella, C.; Lemaître, F.; Guille-Collignon, M.; Amatore, C.; Thouin, L. Downstream Simultaneous Electrochemical Detection of Primary Reactive Oxygen and Nitrogen Species Released by Cell Populations in an Integrated Microfluidic Device. Anal. Chem. 2018, 90, 9386–9394. [Google Scholar] [CrossRef]
- Ino, K.; Shiku, H.; Matsue, T. Bioelectrochemical applications of microelectrode arrays in cell analysis and engineering. Curr. Opin. Electrochem. 2017, 5, 146–151. [Google Scholar] [CrossRef]
- Odijk, M.; Olthuis, W.; van den Berg, A.; Qiao, L.; Girault, H. Improved Conversion Rates in Drug Screening Applications Using Miniaturized Electrochemical Cells with Frit Channels. Anal. Chem. 2012, 84, 9176–9183. [Google Scholar] [CrossRef]
- Torisawa, Y.; Shiku, H.; Yasukawa, T.; Nishizawa, M.; Matsue, T. Multi-channel 3-D cell culture device integrated on a silicon chip for anticancer drug sensitivity test. Biomaterials 2005, 26, 2165–2172. [Google Scholar] [CrossRef]
- Zhang, M.-N.; Ding, Z.; Long, Y.-T. Sensing cisplatin-induced permeation of single live human bladder cancer cells by scanning electrochemical microscopy. Analyst 2015, 140, 6054–6060. [Google Scholar] [CrossRef]
- Alvau, M.D.; Tartaggia, S.; Meneghello, A.; Casetta, B.; Calia, G.; Serra, P.A.; Polo, F.; Toffoli, G. Enzyme-Based Electrochemical Biosensor for Therapeutic Drug Monitoring of Anticancer Drug Irinotecan. Anal. Chem. 2018, 90, 6012–6019. [Google Scholar] [CrossRef] [PubMed]
- Lima, H.R.S.; da Silva, J.S.; de Oliveira Farias, E.A.; Teixeira, P.R.S.; Eiras, C.; Nunes, L.C.C. Electrochemical sensors and biosensors for the analysis of antineoplastic drugs. Biosens. Bioelectron. 2018, 108, 27–37. [Google Scholar] [CrossRef] [PubMed]
- Palchetti, I.; Laschi, S.; Marrazza, G.; Mascini, M. Electrochemical imaging of localized sandwich DNA hybridization using scanning electrochemical microscopy. Anal. Chem. 2007, 79, 7206–7213. [Google Scholar] [CrossRef] [PubMed]
- Potęga, A.; Żelaszczyk, D.; Mazerska, Z. Electrochemical simulation of metabolism for antitumor-active imidazoacridinone C-1311 and in silico prediction of drug metabolic reactions. J. Pharm. Biomed. Anal. 2019, 169, 269–278. [Google Scholar] [CrossRef]
- Potęga, A.; Garwolińska, D.; Nowicka, A.M.; Fau, M.; Kot-Wasik, A.; Mazerska, Z. Phase I and phase II metabolism simulation of antitumor-active 2-hydroxyacridinone with electrochemistry coupled on-line with mass spectrometry. Xenobiotica 2019, 49, 922–934. [Google Scholar] [CrossRef]
- Portychová, L.; Schug, K.A. Instrumentation and applications of electrochemistry coupled to mass spectrometry for studying xenobiotic metabolism: A review. Anal. Chim. Acta 2017, 993, 1–21. [Google Scholar] [CrossRef]
- Löffler, S.; Melican, K.; Nilsson, K.P.R.; Richter-Dahlfors, A. Organic bioelectronics in medicine. J. Intern. Med. 2017, 282, 24–36. [Google Scholar] [CrossRef]
- Pappa, A.-M.; Parlak, O.; Scheiblin, G.; Mailley, P.; Salleo, A.; Owens, R.M. Organic Electronics for Point-of-Care Metabolite Monitoring. Trends Biotechnol. 2018, 36, 45–59. [Google Scholar] [CrossRef]
- Kim, J.; Jeerapan, I.; Sempionatto, J.R.; Barfidokht, A.; Mishra, R.K.; Campbell, A.S.; Hubble, L.J.; Wang, J. Wearable Bioelectronics: Enzyme-Based Body-Worn Electronic Devices. Acc. Chem. Res. 2018, 51, 2820–2828. [Google Scholar] [CrossRef]
- Feron, K.; Lim, R.; Sherwood, C.; Keynes, A.; Brichta, A.; Dastoor, C.P. Organic Bioelectronics: Materials and Biocompatibility. Int. J. Mol. Sci. 2018, 19, 2382. [Google Scholar] [CrossRef]
- Yu, Y.; Nyein, H.Y.Y.; Gao, W.; Javey, A. Flexible Electrochemical Bioelectronics: The Rise of In Situ Bioanalysis. Adv. Mater. 2019, e1902083. [Google Scholar] [CrossRef] [PubMed]


| Anticancer Drug | Observed Effect | Specific Comments | Ref |
|---|---|---|---|
| Cisplatin | Inhibition of Na+,K+-ATPase and SR Ca2+-ATPase | Strong and irreversible inhibition of SR Ca2+-ATPase activity. Reversible inhibition of Na+,K+-ATPase activity. | [53] |
| Cisplatin and Oxaliplatin | Translocation by Cu+-ATPases (ATP7A and ATP7B) | Binding and translocation of Pt-drugs across the vesicle membrane. | [60] |
| NAMI-A, RAPTA-C and KP1019 | Inhibition of SR Ca2+-ATPase | Strong inhibition of Ca2+ translocation by SR Ca2+-ATPase. | [62] |
| Anticancer Drug | Observed Effect | Specific Comments | Ref |
|---|---|---|---|
| Dacarbazine | Guanine oxidation signal | Analysis of PCR amplicons and comparison with Gel electrophoresis | [78] |
| Methotrexate | Guanine oxidation signal and MTX oxidation signal | Analysis of spiked serum samples and urine samples | [81] |
| Gemcitabine | Guanine and adenine oxidation signal | Analysis of spiked serum samples | [82] |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tadini-Buoninsegni, F.; Palchetti, I. Label-Free Bioelectrochemical Methods for Evaluation of Anticancer Drug Effects at a Molecular Level. Sensors 2020, 20, 1812. https://doi.org/10.3390/s20071812
Tadini-Buoninsegni F, Palchetti I. Label-Free Bioelectrochemical Methods for Evaluation of Anticancer Drug Effects at a Molecular Level. Sensors. 2020; 20(7):1812. https://doi.org/10.3390/s20071812
Chicago/Turabian StyleTadini-Buoninsegni, Francesco, and Ilaria Palchetti. 2020. "Label-Free Bioelectrochemical Methods for Evaluation of Anticancer Drug Effects at a Molecular Level" Sensors 20, no. 7: 1812. https://doi.org/10.3390/s20071812
APA StyleTadini-Buoninsegni, F., & Palchetti, I. (2020). Label-Free Bioelectrochemical Methods for Evaluation of Anticancer Drug Effects at a Molecular Level. Sensors, 20(7), 1812. https://doi.org/10.3390/s20071812






