Photoacoustic Imaging as a Tool for Assessing Hair Follicular Organization
Abstract
:1. Introduction
2. Materials and Methods
2.1. Photoacoustic Imaging System
2.2. Imaging and Data Collection
2.3. Data Analysis
2.4. Statistical Analysis
3. Results
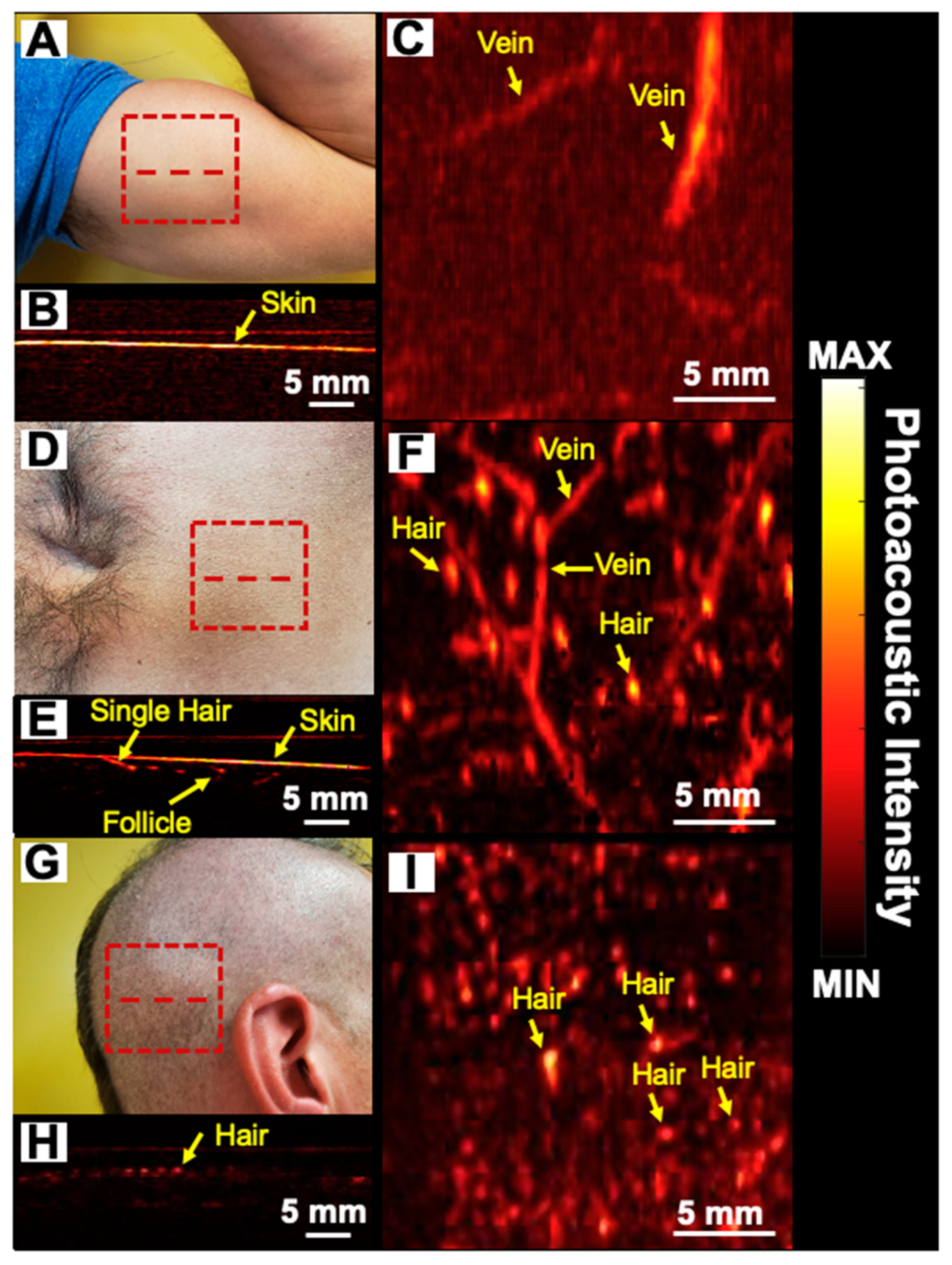
3.1. Hair Follicle Imaging Using PAI
3.2. Subdermal Imaging
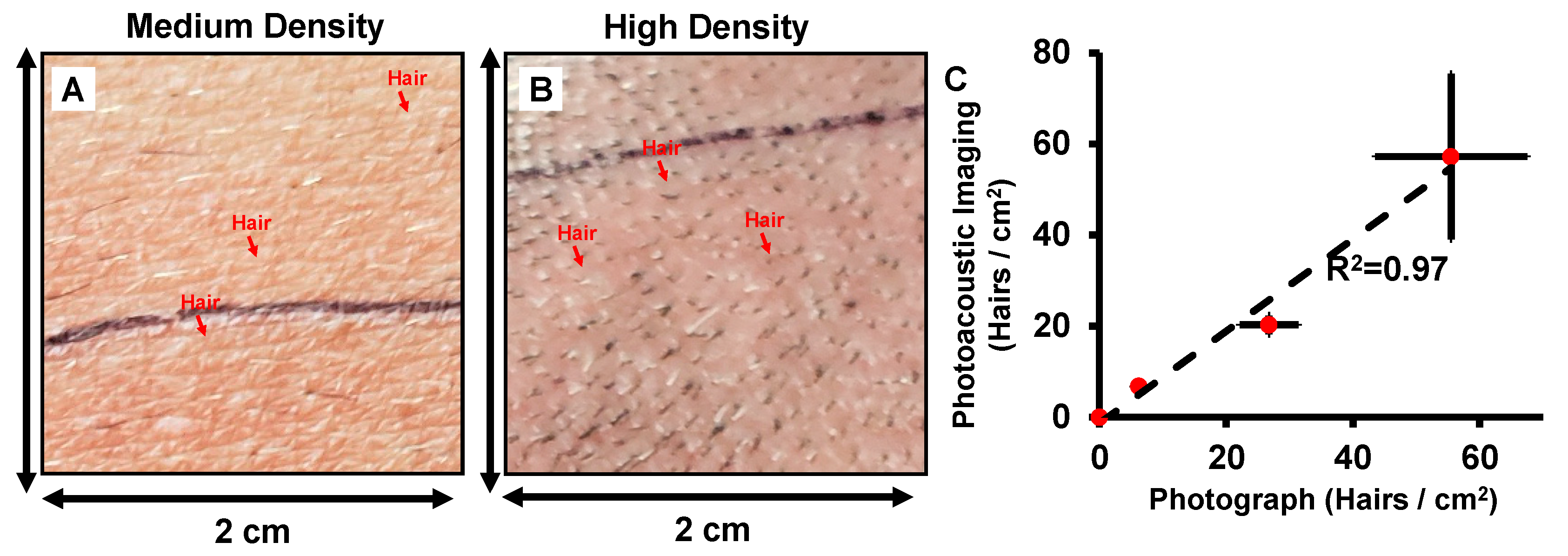
3.3. Follicle Density
3.4. Follicle Angle
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Vogel, J.E.; Jimenez, F.; Cole, J.; Keene, S.A.; Harris, J.A.; Barrera, A.; Rose, P.T. Hair Restoration Surgery: The State of the Art. Aesthetic Surg. J. 2013, 33, 128–151. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- International Society of Hair Restoration Surgery. 2017 Practice Census Results; International Society of Hair Restoration Surgery: Geneva, IL, USA, 2017. [Google Scholar]
- Unger, W.P.; Shapiro, R.; Unger, R.; Unger, M. Hair Transplantation; CRC Press: Boca Raton, FL, USA, 2010. [Google Scholar]
- Paus, R.; Cotsarelis, G. The biology of hair follicles. N. Engl. J. Med. 1999, 341, 491–497. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rassman, W.R.; Bernstein, R.M.; McClellan, R.; Jones, R.; Worton, E.; Uyttendaele, H. Follicular Unit Extraction: Minimally Invasive Surgery for Hair Transplantation. Dermatol. Surg. 2002, 28, 720–728. [Google Scholar] [CrossRef] [PubMed]
- Bernstein, R.M.; Rassman, W.R. Follicular unit transplantation: 2005. Dermatol. Clin. 2005, 23, 393–414. [Google Scholar] [CrossRef]
- Nirmal, B.; Somiah, S.; Sacchidanand, S.A. A study of donor area in follicular unit hair transplantation. J. Cutan. Aesthet. Surg. 2013, 6, 210. [Google Scholar]
- Avram, M.R.; Rogers, N.; Watkins, S. Side-effects from follicular unit extraction in hair transplantation. J. Cutan. Aesthet. Surg. 2014, 7, 177–179. [Google Scholar] [CrossRef]
- Alhaddab, M.; Kohn, T.; Sidloi, M. Effect of Graft Size, Angle, and Intergraft Distance on Dense Packing in Hair Transplant. Dermatol. Surg. 2005, 31, 650–654. [Google Scholar] [CrossRef]
- Jimenez, F.; Ruifernández, J.M. Distribution of human hair in follicular units: A mathematical model for estimating the donor size in follicular unit transplantation. Dermatol. Surg. 1999, 25, 294–298. [Google Scholar] [CrossRef]
- Loh, S.-H.; Lew, B.-L.; Sim, W.-Y. Localized Telogen Effluvium Following Hair Transplantation. Ann. Dermatol. 2018, 30, 214–217. [Google Scholar] [CrossRef] [Green Version]
- Poswal, A.; Bhutia, S.; Mehta, R. When fue goes wrong! Indian J. Dermatol. 2011, 56, 517–519. [Google Scholar] [CrossRef]
- Harris, J.A. New Methodology and Instrumentation for Follicular Unit Extraction: Lower Follicle Transection Rates and Expanded Patient Candidacy. Dermatol. Surg. 2006, 32, 56–62. [Google Scholar] [CrossRef]
- Zito, P.M.; Raggio, B.S. Hair Transplantation. In StatPearls [Internet]; StatPearls Publishing: Treasure Island, FL, USA, 2019. [Google Scholar]
- Kleinerman, R.; Whang, T.B.; Bard, R.L.; Marmur, E.S. Ultrasound in dermatology: Principles and applications. J. Am. Acad. Dermatol. 2012, 67, 478–487. [Google Scholar] [CrossRef] [PubMed]
- Attia, A.B.E.; Balasundaram, G.; Moothanchery, M.; Dinish, U.S.; Bi, R.; Ntziachristos, V.; Olivo, M. A review of clinical photoacoustic imaging: Current and future trends. Photoacoustics 2019, 16, 100144. [Google Scholar] [CrossRef] [PubMed]
- Mantri, Y.; Davidi, B.; Lemaster, J.E.; Hariri, A.; Jokerst, J.V. Iodide-doped precious metal nanoparticles: Measuring oxidative stress in vivo via photoacoustic imaging. Nanoscale 2020, 12, 10511–10520. [Google Scholar] [CrossRef] [PubMed]
- Choi, W.; Park, E.-Y.; Jeon, S.; Kim, C. Clinical photoacoustic imaging platforms. Biomed. Eng. Lett. 2018, 8, 139–155. [Google Scholar] [CrossRef] [PubMed]
- Moore, C.; Jokerst, J.V. Strategies for Image-Guided therapy, surgery, and drug delivery using photoacoustic imaging. Theranostics 2019, 9, 1550. [Google Scholar] [CrossRef]
- Kim, J.; Kim, Y.; Park, B.; Seo, H.M.; Bang, C.; Park, G.; Park, Y.; Rhie, J.; Lee, J.; Kim, C. Multispectral ex vivo photoacoustic imaging of cutaneous melanoma for better selection of the excision margin. Br. J. Dermatol. 2018, 179, 780–782. [Google Scholar] [CrossRef]
- Petri, M.; Stoffels, I.; Jose, J.; Leyh, J.; Schulz, A.; Dissemond, J.; Schadendorf, D.; Klode, J. Photoacoustic imaging of real-time oxygen changes in chronic leg ulcers after topical application of a haemoglobin spray: A pilot study. J. Wound Care 2016, 25, 87–91. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Schwarz, M.; Aguirre, J.; Omar, M.; Ntziachristos, V. Chapter 26—Optoacoustic Imaging of Skin. In Imaging in Dermatology; Hamblin, M.R., Avci, P., Gupta, G.K., Eds.; Academic Press: Boston, MA, USA, 2016; pp. 375–385. [Google Scholar] [CrossRef]
- Zabihian, B.; Weingast, J.; Liu, M.; Zhang, E.; Beard, P.; Pehamberger, H.; Drexler, W.; Hermann, B. In vivo dual-modality photoacoustic and optical coherence tomography imaging of human dermatological pathologies. Biomed. Opt. Express 2015, 6, 3163–3178. [Google Scholar] [CrossRef] [Green Version]
- Hindelang, B.; Aguirre, J.; Schwarz, M.; Berezhnoi, A.; Eyerich, K.; Ntziachristos, V.; Biedermann, T.; Darsow, U. Non-invasive imaging in dermatology and the unique potential of raster-scan optoacoustic mesoscopy. J. Eur. Acad. Dermatol. Venereol. 2019, 33, 1051–1061. [Google Scholar] [CrossRef] [Green Version]
- Ford, S.J.; Bigliardi, P.L.; Sardella, T.C.P.; Urich, A.; Burton, N.C.; Kacprowicz, M.; Bigliardi, M.; Olivo, M.; Razansky, D. Structural and Functional Analysis of Intact Hair Follicles and Pilosebaceous Units by Volumetric Multispectral Optoacoustic Tomography. J. Investig. Dermatol. 2016, 136, 753–761. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hariri, A.; Lemaster, J.; Wang, J.; Jeevarathinam, A.S.; Chao, D.L.; Jokerst, J.V. The characterization of an economic and portable LED-based photoacoustic imaging system to facilitate molecular imaging. Photoacoustics 2018, 9, 10–20. [Google Scholar] [CrossRef] [PubMed]
- Raman, R.; Napel, S.; Rubin, G.D. Curved-slab maximum intensity projection: Method and evaluation. Radiology 2003, 229, 255–260. [Google Scholar] [CrossRef] [PubMed]
- Sakas, G.; Grimm, M.; Savopoulos, A. Optimized maximum intensity projection (MIP). In Rendering Techniques’ 95; Springer: Berlin/Heidelberg, Germany, 1995; pp. 51–63. [Google Scholar]
- Köstli, K.P.; Beard, P.C. Two-dimensional photoacoustic imaging by use of Fourier-transform image reconstruction and a detector with an anisotropic response. Appl. Opt. 2003, 42, 1899–1908. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rasband, W.S. ImageJ 1.48v; Bethesda: Rockville, MD, USA, 1997. [Google Scholar]
- Schmid-Wendtner, M.-H.; Dill-Müller, D. Ultrasound technology in dermatology. Semin. Cutan. Med. Surg. 2008, 27, 44–51. [Google Scholar] [CrossRef]
- Mohmand, M.H.; Ahmad, M. Effect of follicular unit extraction on the donor area. World J. Plast. Surg. 2018, 7, 193. [Google Scholar]
- Miri Rostami, S.R.; Mozaffarzadeh, M.; Ghaffari-Miab, M.; Hariri, A.; Jokerst, J. GPU-accelerated double-stage delay-multiply-and-sum algorithm for fast photoacoustic tomography using LED excitation and linear arrays. Ultrason. Imaging 2019, 41, 301–316. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Moaveni, M.K. A Multiple Scattering Field Theory Applied to Whole Blood. Ph.D. Thesis, University of Washington, Seattle, WA, USA, 1970. [Google Scholar]
- Jacques, S.L.; McAuliffe, D.J. The melanosome: Threshold temperature for explosive vaporization and internal absorption coefficient during pulsed laser irradiation. Photochem. Photobiol. 1991, 53, 769–775. [Google Scholar] [CrossRef]
- Oltulu, P.; Ince, B.; Kökbudak, N.; Kılıç, F. Measurement of epidermis, dermis, and total skin thicknesses from six different body regions with a new ethical histometric technique. Türk Plastik Rekonstrüktif Estet. Cerrahi Derg. (Turk. J. Plast. Surg.) 2018, 26, 56–61. [Google Scholar] [CrossRef]
- Law, S.K. Thickness and resistivity variations over the upper surface of the human skull. Brain Topogr. 1993, 6, 99–109. [Google Scholar] [CrossRef]
- Lillie, E.M.; Urban, J.E.; Weaver, A.A.; Powers, A.K.; Stitzel, J.D. Estimation of skull table thickness with clinical CT and validation with microCT. J. Anat. 2015, 226, 73–80. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kim, J.; Kim, J.Y.; Jeon, S.; Baik, J.W.; Cho, S.H.; Kim, C. Super-resolution localization photoacoustic microscopy using intrinsic red blood cells as contrast absorbers. Light Sci. Appl. 2019, 8, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Weber, J.; Beard, P.C.; Bohndiek, S.E. Contrast agents for molecular photoacoustic imaging. Nat. Methods 2016, 13, 639–650. [Google Scholar] [CrossRef] [Green Version]
- Zhang, H.F.; Maslov, K.; Stoica, G.; Wang, L.V. Functional photoacoustic microscopy for high-resolution and noninvasive in vivo imaging. Nat. Biotechnol. 2006, 24, 848–851. [Google Scholar] [CrossRef] [PubMed]
- Singh, M.K.A.; Sato, N.; Ichihashi, F.; Sankai, Y. Real-time improvement of LED-based photoacoustic image quality using intermittent pulse echo acquisitions. In Proceedings of the Photons Plus Ultrasound: Imaging and Sensing 2020, San Francisco, CA, USA, 17 February 2020; p. 1124051. [Google Scholar]
- Hariri, A.; Alipour, K.; Mantri, Y.; Schulze, J.P.; Jokerst, J.V. Deep learning improves contrast in low-fluence photoacoustic imaging. Biomed. Opt. Express 2020, 11, 3360–3373. [Google Scholar] [CrossRef] [PubMed]
- Crippa, P.; Cristofoletti, V.t.; Romeo, N. A band model for melanin deduced from optical absorption and photoconductivity experiments. Biochim. Biophys. Acta (BBA)-Gen. Subj. 1978, 538, 164–170. [Google Scholar] [CrossRef]
- Hasegawa, H.; de Korte, C.L. Impact of element pitch on synthetic aperture ultrasound imaging. J. Med Ultrason. 2016, 43, 317–325. [Google Scholar] [CrossRef]
- Cheong, W.-F.; Prahl, S.A.; Welch, A.J. A review of the optical properties of biological tissues. IEEE J. Quantum Electron. 1990, 26, 2166–2185. [Google Scholar] [CrossRef] [Green Version]
- Maneas, E.; Aughwane, R.; Huynh, N.; Xia, W.; Ansari, R.; Kuniyil Ajith Singh, M.; Hutchinson, J.C.; Sebire, N.J.; Arthurs, O.J.; Deprest, J. Photoacoustic imaging of the human placental vasculature. J. Biophotonics 2020, 13, e201900167. [Google Scholar] [CrossRef] [Green Version]
- Favazza, C.P.; Wang, L.V.; Cornelius, L.A. In vivo functional photoacoustic microscopy of cutaneous microvasculature in human skin. J. Biomed. Opt. 2011, 16, 026004. [Google Scholar] [CrossRef] [Green Version]
- Taruttis, A.; Timmermans, A.C.; Wouters, P.C.; Kacprowicz, M.; van Dam, G.M.; Ntziachristos, V. Optoacoustic imaging of human vasculature: Feasibility by using a handheld probe. Radiology 2016, 281, 256–263. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ahmad, M.; Mohmand, M.H. Analysis of the changes in scalp hair angles: In vivo and in vitro comparison before and after tumescence. J. Cosmet. Dermatol. 2019, 18, 390–394. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lam, S.; Williams, K. Hair Transplant 360 Follicular Unit Extraction (FUE) Jaypee Medical Inc; The Health Sciences Publisher: New Delhi, India, 2016. [Google Scholar]
- Lindelöf, B.; Forslind, B.; Hedblad, M.-A. Human hair form: Morphology revealed by light and scanning electron microscopy and computer aided three-dimensional reconstruction. Arch. Dermatol. 1988, 124, 1359–1363. [Google Scholar] [CrossRef] [PubMed]
- Fergus, R.; Singh, B.; Hertzmann, A.; Roweis, S.T.; Freeman, W.T. Removing Camera Shake from a Single Photograph; ACM Siggraph 2006 Papers: Boston, MA, USA, 2006; pp. 787–794. [Google Scholar]
- Yan, W.-Q.; Kankanhalli, M.S. Detection and removal of lighting & shaking artifacts in home videos. In Proceedings of the Tenth ACM International Conference on Multimedia, Juan les Pins, France, 1–6 December 2002; pp. 107–116. [Google Scholar]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hariri, A.; Moore, C.; Mantri, Y.; Jokerst, J.V. Photoacoustic Imaging as a Tool for Assessing Hair Follicular Organization. Sensors 2020, 20, 5848. https://doi.org/10.3390/s20205848
Hariri A, Moore C, Mantri Y, Jokerst JV. Photoacoustic Imaging as a Tool for Assessing Hair Follicular Organization. Sensors. 2020; 20(20):5848. https://doi.org/10.3390/s20205848
Chicago/Turabian StyleHariri, Ali, Colman Moore, Yash Mantri, and Jesse V. Jokerst. 2020. "Photoacoustic Imaging as a Tool for Assessing Hair Follicular Organization" Sensors 20, no. 20: 5848. https://doi.org/10.3390/s20205848




