Design and Accuracy of an Instrumented Insole Using Pressure Sensors for Step Count
Abstract
1. Introduction
2. Materials and Methods
2.1. Hardware
2.1.1. System Overview
2.1.2. Force Sensitive Resistor (FSR)
2.1.3. Circuit Board
2.1.4. Resistance
2.1.5. Battery
2.2. Software
| Algorithm 1: A step count algorithm using cumulative sum of all pressure signals. |
| 1: Input: N channels pressure Pi (t), 2: Calculate the sum pressure Psum (t); 3: Calculate the cumulative sum pressure Pcum_sum (t); 4: Initial: Npeak = step count = 0; A = 0; B = 0; 5: For j = 1 : M do 6: if Pheel ≥ 50% of Pi max then 7: A = Calculate Pcum_sum (t); 8: else 9: B = Calculate Psum (t); 10: end 11: if (A != 0 && B != 0) then 12: Step count = Npeak + 1 = step count + 1; 13: A = 0; B = 0; 14: else 15: Step count = Npeak = step count; 16: end 17: end 18: Return: step count. |
2.3. Data Collection Procedure and Analysis
3. Results
3.1. Designed Prototype of Instrumented Insole System and Quality of Signals
3.2. Accuracy of the Proposed System
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Bonato, P. Advances in wearable technology and applications in physical medicine and rehabilitation. J. Neuroeng. Rehabil. 2005, 2. [Google Scholar] [CrossRef] [PubMed]
- Jovanov, E.; Milenkovic, A.; Otto, C.; De Groen, P.C. A wireless body area network of intelligent motion sensors for computer assisted physical rehabilitation. J. Neuroeng. Rehabil. 2005, 2, 6. [Google Scholar] [CrossRef] [PubMed]
- Seto, E.; Martin, E.; Yang, A.; Yan, P.; Gravina, R.; Lin, I.; Wang, C.; Roy, M.; Shia, V.; Bajcsy, R. Opportunistic strategies for lightweight signal processing for body sensor networks. In Proceedings of the 3rd International Conference on PErvasive Technologies Related to Assistive Environments, Samos, Greece, 23–25 June 2010; ACM: New York, NY, USA, 2010. No. 56. [Google Scholar]
- Williams, B.; Allen, B.; True, H.; Fell, N.; Levine, D.; Sartipi, M. A Real-Time, Mobile Timed up and Go System. In Proceedings of the 2015 IEEE 12th International Conference on Wearable and Implantable Body Sensor Networks (BSN), Cambridge, MA, USA, 9–12 June 2015; pp. 1–6. [Google Scholar]
- Tudor-Locke, C.; Bassett, D.R. How many steps/day are enough? Sports Med. 2004, 34, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Tudor-Locke, C.; Burkett, L.; Reis, J.; Ainsworth, B.; Macera, C.; Wilson, D. How many days of pedometer monitoring predict weekly physical activity in adults? Prev. Med. 2005, 40, 293–298. [Google Scholar] [CrossRef] [PubMed]
- Craig, C.L.; Bell, R.C.; A Croteau, K.; Ewald, B.; Hatano, Y.; Lutes, L.D.; Matsudo, S.M.; A Ramirez-Marrero, F.; Schmidt, M.D.; Tudor-Locke, C.; et al. How many steps/day are enough? For older adults and special populations. Int. J. Behav. Nutr. Phys. Act. 2011, 8, 80. [Google Scholar]
- Tudor-Locke, C.; Craig, C.L.; Thyfault, J.P.; Spence, J.C. A step-defined sedentary lifestyle index: <5000 steps/day. Appl. Physiol. Nutr. Metab. 2012, 38, 100–114. [Google Scholar] [PubMed]
- Tudor-Locke, C.; Leonardi, C.; Johnson, W.D.; Katzmarzyk, P.T.; Church, T.S. Accelerometer steps/day translation of moderate-to-vigorous activity. Prev. Med. 2011, 53, 31–133. [Google Scholar] [CrossRef] [PubMed]
- Tudor-Locke, C.; Sisson, S.B.; Collova, T.; Lee, S.M.; Swan, P.D. Pedometer-determined step count guidelines for classifying walking intensity in a young ostensibly healthy population. Can. J. Appl. Physiol. 2005, 30, 666–676. [Google Scholar] [CrossRef] [PubMed]
- Lin, F.; Wang, A.; Song, C.; Xu, W.; Li, Z.; Li, Q. A Comparative Study of Smart Insole on Real-World Step Count. In Proceedings of the IEEE Signal Processing in Medicine and Biology Symposium (SPMB), Philadelphia, PA, USA, 12 December 2015; pp. 1–6. [Google Scholar]
- Bassett, D.; Strath, S.J. Use of Pedometers to Assess Physical Activity. Available online: https://books.google.com.hk/books?hl=zh-TW&lr=&id=O9-vt1CZJp8C&oi=fnd&pg=PA163&dq=+Bassett,+D.%3B+Strath,+S.J.,+Use+of+pedometers+to+assess+physical+activity.+Physical+activity+assessments+for+health-related+research+2002,+163-177.&ots=OxCvw7wNYo&sig=uGrN1KWNQbDoFIU8B3WnTNKVlak&redir_esc=y#v=onepage&q&f=false (accessed on 22 February 2019).
- Freedson, P.S.; Miller, K. Objective monitoring of physical activity using motion sensors and heart rate. Res. Q. Exerc. Sport 2000, 71, 21–29. [Google Scholar] [CrossRef] [PubMed]
- Tudor-Locke, C.; Ainsworth, B.E.; Whitt, M.C.; Thompson, R.; Addy, C.L.; Jones, D. The relationship between pedometer-determined ambulatory activity and body composition variables. Int. J. Obes. 2001, 25, 1571–1578. [Google Scholar] [CrossRef] [PubMed]
- Fulk, G.D.; Combs, S.A.; Danks, K.A.; Nirider, C.D.; Raja, B.; Reisman, D.S. Accuracy of 2 activity monitors in detecting steps in people with stroke and traumatic brain injury. Phys. Ther. 2014, 94, 222–229. [Google Scholar] [CrossRef] [PubMed]
- Fini, N.A.; Holland, A.E.; Keating, J.; Simek, J.; Bernhardt, J. How is physical activity monitored in people following stroke? Disabil. Rehabil. 2015, 37, 1717–1731. [Google Scholar] [CrossRef] [PubMed]
- Dobkin, B.H.; Dorsch, A. The promise of mHealth: Daily activity monitoring and outcome assessments by wearable sensors. Neurorehabilit. Neural Repair. 2011, 25, 788–798. [Google Scholar] [CrossRef] [PubMed]
- Fulk, G.D.; Sazonov, E. Using sensors to measure activity in people with stroke. Top. Stroke Rehabil. 2011, 18, 746–757. [Google Scholar] [CrossRef] [PubMed]
- Shany, T.; Redmond, S.J.; Narayanan, M.R.; Lovell, N.H. Sensors-based wearable systems for monitoring of human movement and falls. IEEE Sens. J. 2012, 12, 658–670. [Google Scholar] [CrossRef]
- Hergenroeder, A.L.; Gibbs, B.B.; Kotlarczyk, M.P.; Perera, S.; Brach, J.S.; Kowalsky, R.J. Accuracy and Acceptability of Commercial Grade Physical Activity Monitors in Older Adults. J. Aging Phys. Act. 2018, 1–26. [Google Scholar] [CrossRef] [PubMed]
- Tam, K.M.; Cheung, S.Y. Validation of Electronic Activity Monitor Devices During Treadmill Walking. Telemed. E-Health 2018, 24, 782–789. [Google Scholar] [CrossRef] [PubMed]
- Mooses, K.; Oja, M.; Reisberg, S.; Vilo, J.; Kull, M. Validating Fitbit Zip for monitoring physical activity of children in school: A cross-sectional study. BMC Public Health 2018, 18, 858. [Google Scholar] [CrossRef] [PubMed]
- Huang, Y.; Xu, J.; Yu, B.; Shull, P.B. Validity of FitBit, Jawbone UP, Nike+ and other wearable devices for level and stair walking. Gait Posture 2016, 48, 36–41. [Google Scholar] [CrossRef] [PubMed]
- Chow, J.J.; Thom, J.M.; Wewege, M.A.; Ward, R.E.; Parmenter, B.J. Accuracy of step count measured by physical activity monitors: The effect of gait speed and anatomical placement site. Gait Posture 2017, 57, 199–203. [Google Scholar] [CrossRef] [PubMed]
- Fulk, G.D.; Edgar, S.R.; Bierwirth, R.; Hart, P.; Lopez-Meyer, P.; Sazonov, E. Identifying activity levels and steps in people with stroke using a novel shoe-based sensor. J. Neurol. Phys. 2012, 36, 100–107. [Google Scholar] [CrossRef] [PubMed]
- Truong, P.H.; Lee, J.; Kwon, A.-R.; Jeong, G.-M. Stride counting in human walking and walking distance estimation using insole sensors. Sensors 2016, 16, 823. [Google Scholar] [CrossRef] [PubMed]
- Moufawad El Achkar, C.; Lenoble-Hoskovec, C.; Paraschiv-Ionescu, A.; Major, K.; Büla, C.; Aminian, K. Physical behavior in older persons during daily life: Insights from instrumented shoes. Sensors 2016, 16, 1225. [Google Scholar] [CrossRef] [PubMed]
- Bakhteri, R.; Al Satti, T.; Khalil-Hani, M.; Wen, H.Y. Microprocessor-Based Athlete Health Monitoring Device based on Heart Rate and Stride Length Calculation. J. Teknol. 2015, 74, 65–71. [Google Scholar] [CrossRef]
- Piau, A.; Charlon, Y.; Campo, E.; Vellas, B.; Nourhashemi, F. A smart insole to promote healthy aging for frail elderly individuals: Specifications, design, and preliminary results. JMIR Rehabil. Assist. Technol. 2015, 2, e5. [Google Scholar] [CrossRef] [PubMed]
- Rodriguez, A.; Balsamo, D.; Luo, Z.; Beeby, S.P.; Merrett, G.V.; Weddel, A.S. Intermittently-powered energy harvesting step counter for fitness tracking. In Proceedings of the 2017 IEEE Sensors Applications Symposium (SAS), Glassboro, NJ, USA, 13–15 March 2017; pp. 1–6. [Google Scholar]
- Benocci, M.; Rocchi, L.; Farella, E.; Chiari, L.; Benini, L. A Wireless System for Gait and Posture Analysis Based on Pressure Insoles and INERTIAL Measurement Units. In Proceedings of the 3rd International Conference on Pervasive Computing Technologies for Healthcare, PervasiveHealth, London, UK, 1–3 April 2009; pp. 1–6. [Google Scholar]
- Hegde, N.; Melanson, E.; Sazonov, E. Development of a Real Time Activity Monitoring Android Application Utilizing SmartStep. Conf. Proc. IEEE. Eng. Med. Biol. Soc. 2016, 1886–1889. [Google Scholar] [CrossRef]
- Cho, H. Design and Implementation of a Lightweight Smart Insole for Gait Analysis. In Proceedings of the 2017 IEEE Trustcom/BigDataSE/ICESS, Sydney, Australia, 1–4 August 2017; pp. 792–797. [Google Scholar]
- Zhang, T.; Lu, J.; Uswatte, G.; Taub, E.; Sazonov, E.S. Measuring gait symmetry in children with cerebral palsy using the SmartShoe. In Proceedings of the IEEE Healthcare Innovation Conference (HIC), Seattle, WA, USA, 8–10 October 2014; pp. 48–51. [Google Scholar]
- Lopez-Meyer, P.; Fulk, G.D.; Sazonov, E.S. Automatic detection of temporal gait parameters in poststroke individuals. IEEE Trans. Inf. Technol. Biomed. 2011, 15, 594–601. [Google Scholar] [CrossRef] [PubMed]
- Chen, B.; Wang, X.; Huang, Y.; Wei, K.; Wang, Q. A foot-wearable interface for locomotion mode recognition based on discrete contact force distribution. Mechatronics 2015, 32, 12–21. [Google Scholar] [CrossRef]
- Harris, G.F.; Wertsch, J.J. Procedures for gait analysis. Arch. Phys. Med. Rehabil. 1994, 75, 216–225. [Google Scholar] [PubMed]
- Hars, M.; Trombetti, A. Evaluation de la marche, de l’équilibre et du muscle chez le sujet âgé. Rev. Med. Suisse 2013, 9, 1265–1271. [Google Scholar] [PubMed]
- Wuest, S.; Masse, F.; Aminian, K.; Gonzenbach, R.; De Bruin, E.D. Reliability and validity of the inertial sensor-based Timed “Up and Go” test in individuals affected by stroke. J. Rehabil. Res. Dev. 2016, 53, 599–610. [Google Scholar] [CrossRef] [PubMed]
- Fulk, G.D.; Lopez-Meyer, P.; Sazonov, E.S. Characterizing walking activity in people with stroke. Conf. Proc. IEEE Eng. Med. Biol. Soc. 2011, 5211–5214. [Google Scholar] [CrossRef]
- Chuckpaiwong, B.; Nunley, J.A.; Mall, N.A.; Queen, R.M. The effect of foot type on in-shoe plantar pressure during walking and running. Gait Posture 2008, 28, 405–411. [Google Scholar] [CrossRef] [PubMed]
- Nix, S.E.; Vicenzino, B.T.; Collins, N.J.; Smith, M.D. Gait parameters associated with hallux valgus: A systematic review. J. Foot Ankle Res. 2013, 6, 9. [Google Scholar] [CrossRef] [PubMed]
- Taylor, A.J.; Menz, H.B.; Keenan, A.-M. The influence of walking speed on plantar pressure measurements using the two-step gait initiation protocol. Foot 2004, 14, 49–55. [Google Scholar] [CrossRef]
- Viel, E. La Marche Humaine, la course et le saut: Biomécanique, Explorations, Normes et Dysfonctionnements; Elsevier Masson: Amsterdam, The Netherlands, 2000; Volume 9. [Google Scholar]
- Wafai, L.; Zayegh, A.; Woulfe, J.; Aziz, S.M.; Begg, R. Identification of foot pathologies based on plantar pressure asymmetry. Sensors 2015, 15, 20392–20408. [Google Scholar] [CrossRef] [PubMed]
- Tan, A.M.; Fuss, F.K.; Weizman, Y.; Woudstra, Y.; Troynikov, O. Design of low cost smart insole for real time measurement of plantar pressure. Procedia Technol. 2015, 20, 117–122. [Google Scholar] [CrossRef]
- Sazonov, E.S.; Hegde, N.; Tang, W. Development of SmartStep: An insole-based physical activity monitor. Conf. Proc. IEEE Eng. Med. Biol. Soc. 2013, 7209–7212. [Google Scholar] [CrossRef]
- Mei, Z.; Ivanov, K.; Zhao, G.; Li, H.; Wang, L. An explorative investigation of functional differences in plantar center of pressure of four foot types using sample entropy method. Med. Biol. Eng. Comput. 2017, 55, 537–548. [Google Scholar] [CrossRef] [PubMed]
- Hegde, N.; Bries, M.; Swibas, T.; Melanson, E.; Sazonov, E. Automatic recognition of activities of daily living utilizing insole based and wrist worn wearable sensors. IEEE J. Biomed. Health Inform. 2017, 22, 979–988. [Google Scholar] [CrossRef] [PubMed]
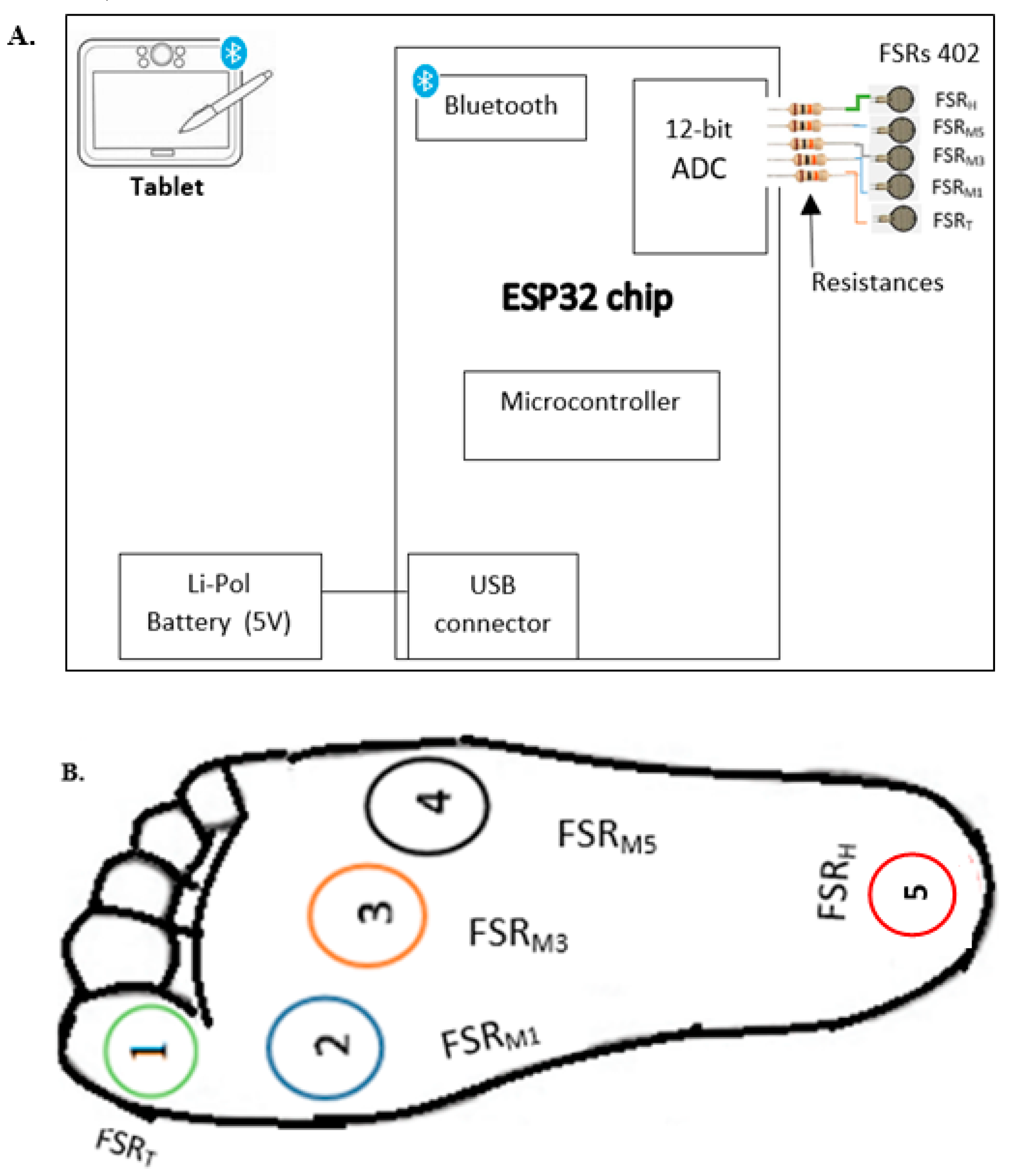
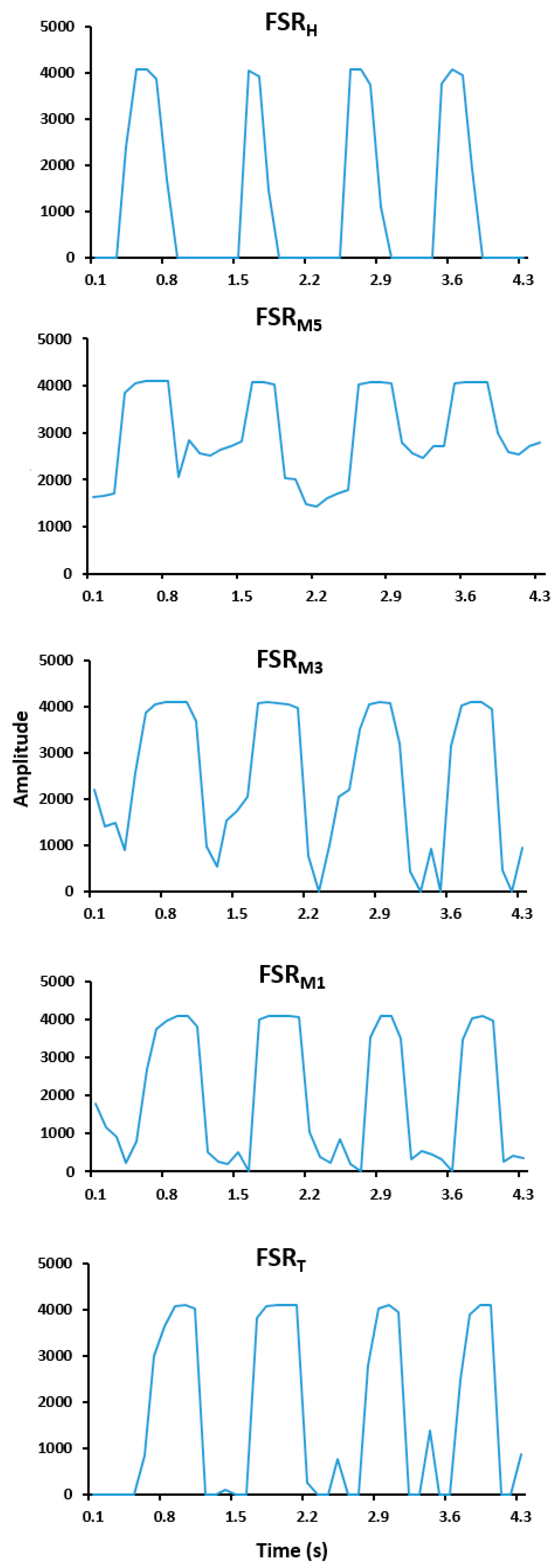
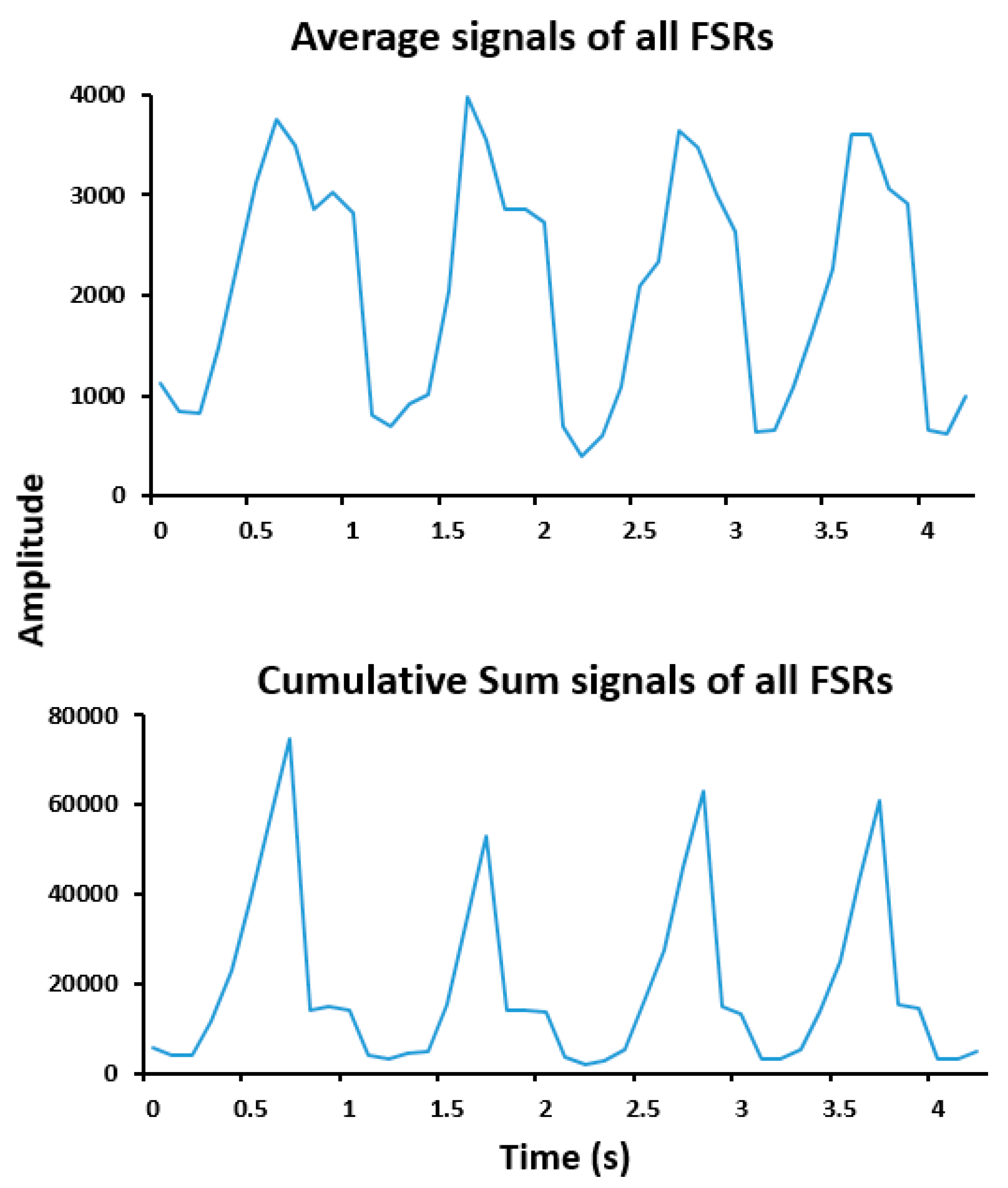
| Function | Function Description | Components |
|---|---|---|
| Power supplying | Supply power to sensor system with a battery module of 5 V | Rechargeable lithium polymer battery |
| Regulate power bank at 3.3 V | Voltage regulator of 3.3 V | |
| Data sensing | Digitalize the resistance of FSRs | Analog-to-digital converter (8 channels) of ESP32 |
| Data storage | Store the digital data for later processing | Memory (ESP32) and file in tablet |
| Data transmission | Establish wireless communication between ESP32 and tablet | Bluetooth module |
| Data processing | Count number of steps taken based on the digital data | Arduino IDE and Matlab Software |
| Participants | Gender | Age (years) | Weight (kg) | Height (m) | Foot Size (cm) |
|---|---|---|---|---|---|
| 1 | M | 29 | 90 | 1.74 | 28.7 |
| 2 | F | 25 | 53 | 1.6 | 24.5 |
| 3 | M | 27 | 70 | 1.75 | 24.5 |
| 4 | M | 28 | 55 | 1.65 | 24.5 |
| 5 | M | 26 | 85 | 1.82 | 27.3 |
| 6 | M | 31 | 69 | 1.8 | 27.6 |
| 7 | F | 31 | 60 | 1.74 | 26 |
| 8 | F | 26 | 62 | 1.65 | 23 |
| 9 | M | 35 | 68 | 1.66 | 26.3 |
| 10 | F | 29 | 76 | 1.61 | 25.2 |
| 11 | F | 21 | 56 | 1.62 | 23 |
| 12 | M | 31 | 70 | 1.83 | 28 |
| F: female; M: male | |||||
| Accuracy (%) a, mean ± SD (n = 12) | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Settings | Walking Speed (m/s) b | Individual FSR | Combined FSRs | GaitUp | |||||
| FSRH | FSRM5 | FSRM3 | FSRM1 | FSRT | Average | Cumulative sum | |||
| Indoor | Self-selected speed (1.43 ± 0.18) | 98.5 ± 2.1% | 98.1 ± 2.5% | 97.0 ± 3.5% | 94.8 ± 9.4% | 96.7 ± 3.1% | 95.5 ± 3.5% | 99.5 ± 0.7% | 99.9 ± 0.2% |
| Maximal speed (1.73 ± 0.08) | 98.4 ± 1.2% | 99.0 ± 0.7% | 98.1 ± 2.7% | 98.6 ± 1.2% | 98.6 ± 1.3% | 98.6 ± 2.2% | 99.6 ± 0.4% | 99.8 ± 0.2% | |
| Outdoor | Self-selected speed (1.45 ± 0.20) | 98.0 ± 2.3% | 96.7 ± 5.1% | 97.4 ± 2.3% | 96.7 ± 5.6% | 96.6 ± 4.8% | 96.5 ± 3.9% | 99.5 ± 0.4% | 99.8 ± 0.3% |
| Maximal speed (1.78 ± 0.12) | 99.4 ± 1.2% | 97.0 ± 6.2% | 99.0 ± 1.1% | 99.0 ± 0.9% | 99.4 ± 0.7% | 97.0 ± 3.6% | 99.6 ± 0.4% | 99.8 ± 0.2% | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ngueleu, A.M.; Blanchette, A.K.; Bouyer, L.; Maltais, D.; McFadyen, B.J.; Moffet, H.; Batcho, C.S. Design and Accuracy of an Instrumented Insole Using Pressure Sensors for Step Count. Sensors 2019, 19, 984. https://doi.org/10.3390/s19050984
Ngueleu AM, Blanchette AK, Bouyer L, Maltais D, McFadyen BJ, Moffet H, Batcho CS. Design and Accuracy of an Instrumented Insole Using Pressure Sensors for Step Count. Sensors. 2019; 19(5):984. https://doi.org/10.3390/s19050984
Chicago/Turabian StyleNgueleu, Armelle M., Andréanne K. Blanchette, Laurent Bouyer, Désirée Maltais, Bradford J. McFadyen, Hélène Moffet, and Charles S. Batcho. 2019. "Design and Accuracy of an Instrumented Insole Using Pressure Sensors for Step Count" Sensors 19, no. 5: 984. https://doi.org/10.3390/s19050984
APA StyleNgueleu, A. M., Blanchette, A. K., Bouyer, L., Maltais, D., McFadyen, B. J., Moffet, H., & Batcho, C. S. (2019). Design and Accuracy of an Instrumented Insole Using Pressure Sensors for Step Count. Sensors, 19(5), 984. https://doi.org/10.3390/s19050984








