E-Textiles for Healthy Ageing
Abstract
1. Introduction
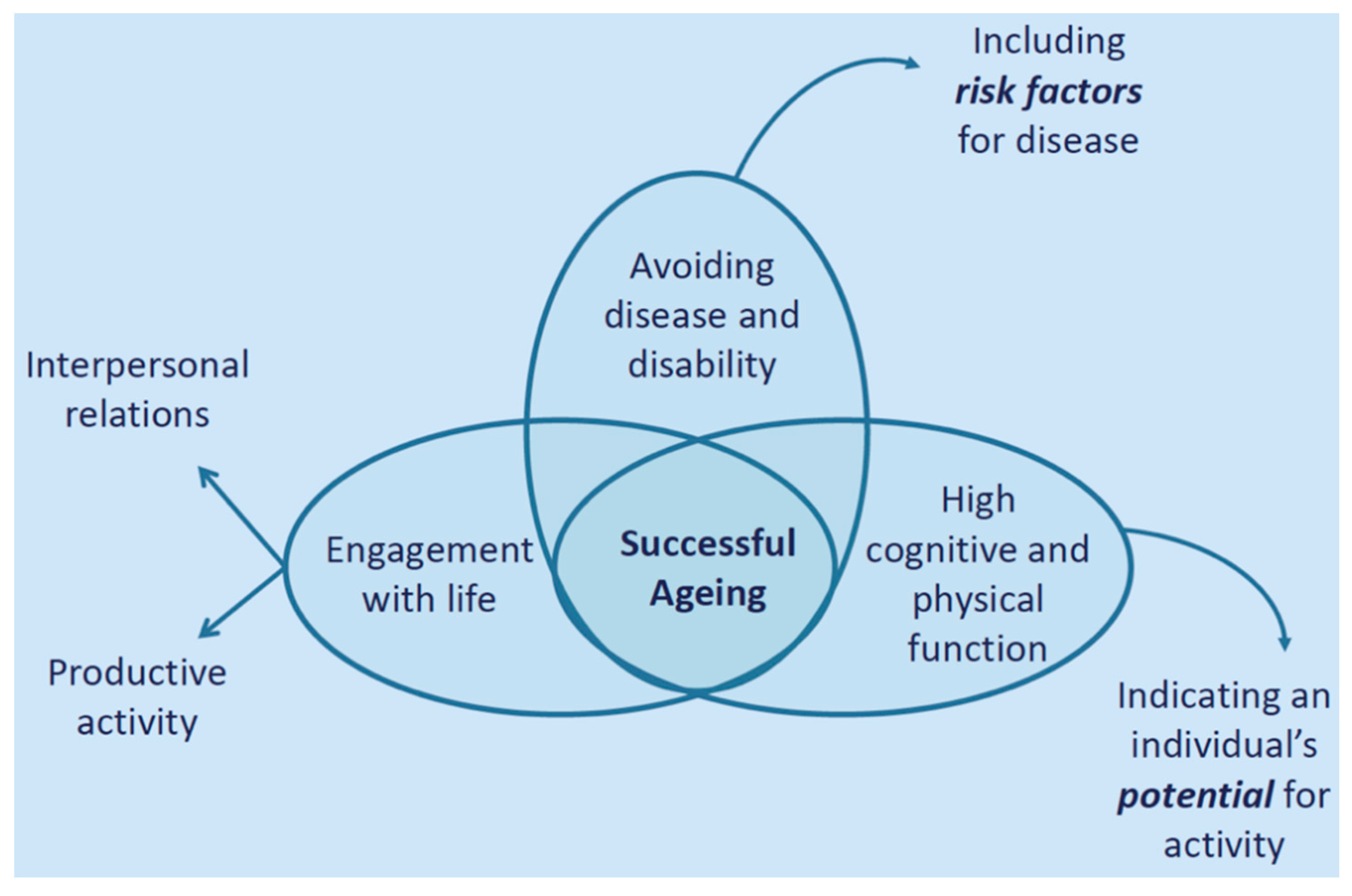
2. Healthy Ageing
2.1. Avoiding Disease and Disability
- Cardiovascular diseases (e.g., hypertension, atrial fibrillation, coronary heart disease, heart failure and stroke)
- Neuropsychiatric conditions (e.g., dementia, depression, epilepsy, mental health)
- Respiratory (e.g., asthma, chronic obstructive, pulmonary disease)
- Endocrine (e.g., diabetes, hypothyroidism)
- Chronic kidney disease (stage 3 to 5)
- Cancer in the previous 5 year (excluding non-melanoma skin cancer)
- Additional common conditions (e.g., anaemia, osteoarthritis, osteoporosis)
- Additional syndromes (e.g., falls, fragility issues, incontinence, skin ulcers/pressure sores)
2.2. High Cognitive and Physical Function
- Episodic memory
- Cognitive processing speed
- Executive functions
- Grip strength
- Gait speed
- Standing balance test etc.
2.3. Engagement with Life
2.4. Lay Perspectives
2.5. Interventions and Technologies to Support Healthy Ageing
|
|
3. Wearable Devices in General and the Need for E-Textiles
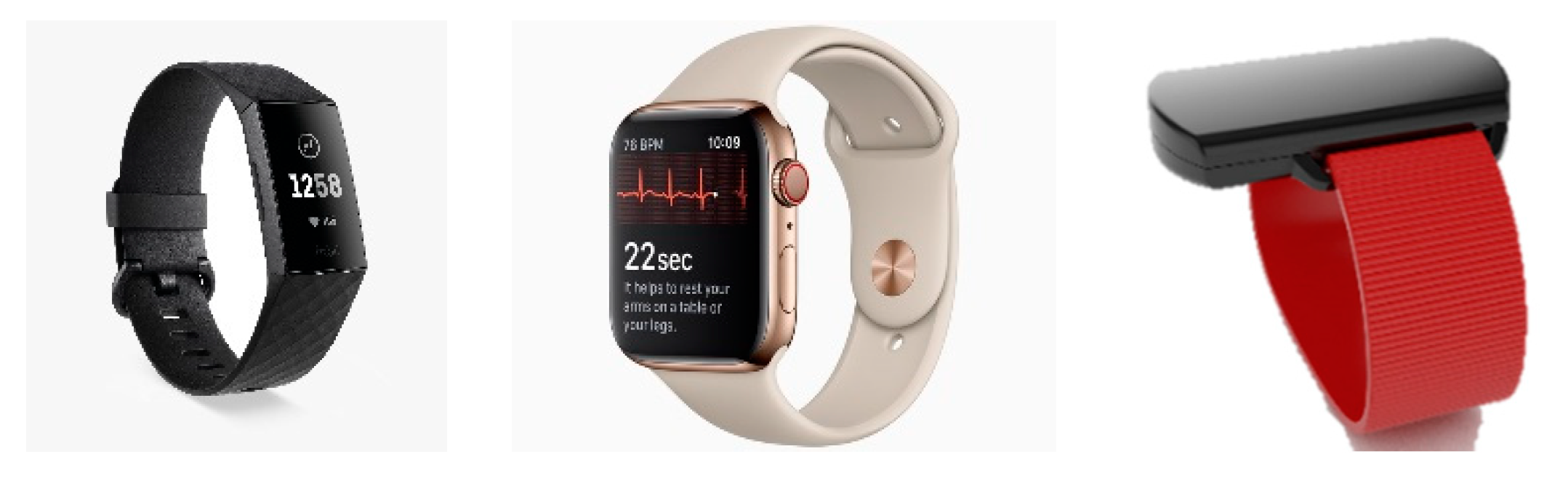
3.1. Wearable Technologies
3.2. Current and Future Applications of Devices to Support Healthy Ageing
3.2.1. Non-Physical Challenges Associated with Healthy Ageing
3.2.2. Physical Health and Functional Ability Related Challenges Associated with Healthy Ageing
3.3. Wearable Technology: The Motivation for E-Textiles
- Textile/clothing-based solutions provide a comfortable and familiar platform to users.
- E-textiles would enable unobtrusive and ubiquitous deployment sensors and actuators in clothing and furnishings.
- The integration in clothing will improve compliance (users might forget to use the conventional technology, but they always remember to get dressed).
- The unobtrusive nature of the technology will avoid any perceived stigma associated with wearing devices.
- Multiple sensors can be incorporated into a single platform (e.g., item of clothing) rather than requiring users to wear a number of separate devices.
- Information or alerts can be provided through the textile providing real time feedback to the user in a single platform.
- Textiles are the most common material that people interact with through, for example, clothing, soft toys, home furnishings and bed linen, and therefore providing an attractive platform for a range of applications.
- Ease of use and increased compliance can provide more data to better inform preventative interventions [77].
4. E-Textile Technologies for Assisting Healthy Ageing
4.1. Inertial Sensors (e.g., Accelerometers)
4.2. Fabric Electrodes
4.3. Textile Pulse Oximetry
4.4. Strain Gauges
4.5. Temperature Sensors (e.g., Thermistor-Change in Resistance with Temperature)
4.6. Moisture Sensors
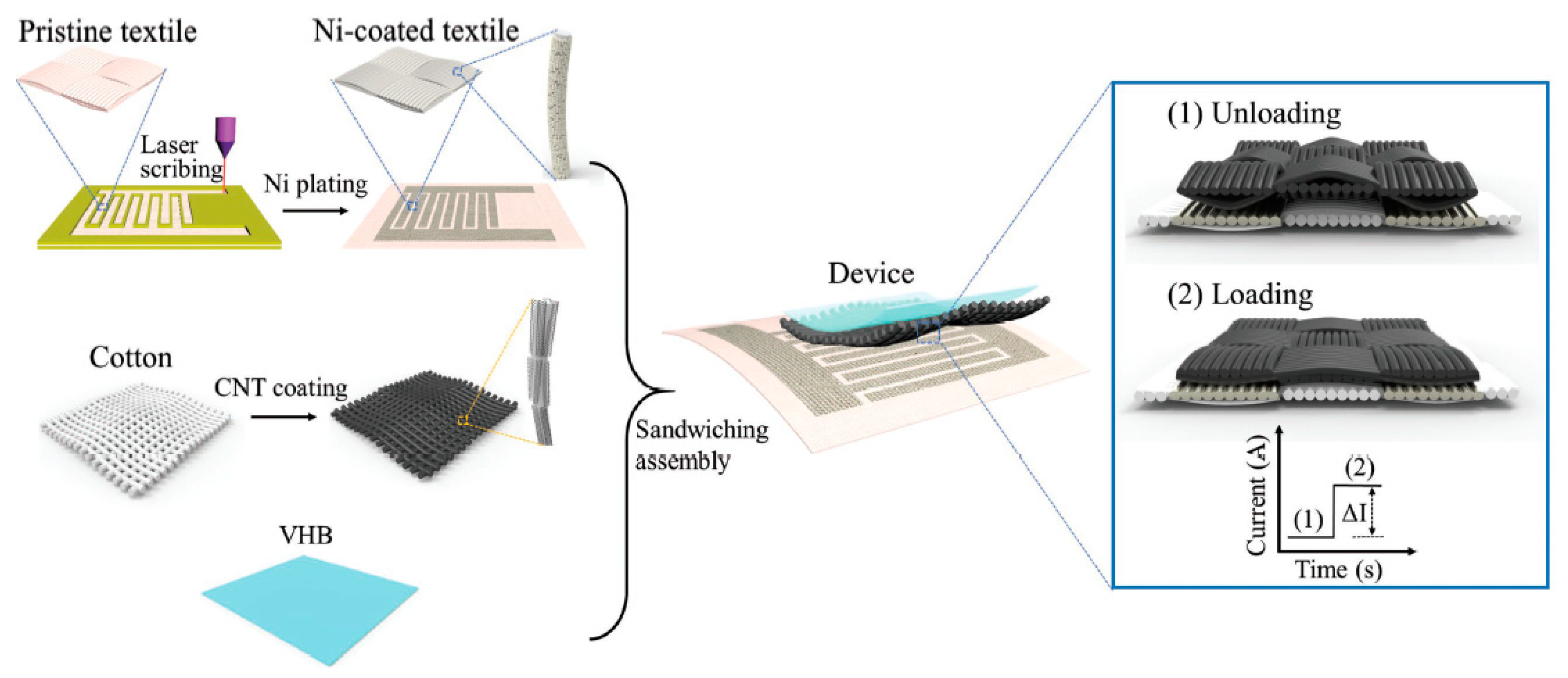
4.7. Textile Pressure Sensors
4.8. Fabric-Based Glucose Sensors
4.9. Actuators
4.10. Fabric Speakers
4.11. Breathing Sensors
4.12. Integrated Location Sensors
4.13. Antibacterial Textiles
4.14. Textiles for Releasing Drugs
4.15. Heated Fabrics
- (1)
- Materials and their performance in textiles—There have been a wide range of functional materials been used in healthcare care applications including fabric-based dry electrodes for monitoring, diagnosis and treatment; flexible stretchable resistive and piezoelectric materials for sensors; electroactive polymer for actuators (e.g., artificial muscles); carbon nanotube-based filament and dielectric coated conductive yarns for conductors and heaters; light emitting polymers for therapies. These materials must survive the rigours of use in the relevant application scenarios. Existing e-textiles are typically unsatisfactory in terms of reliability during use and durability (e.g., bending, stretching, washing). Biocompatibility (e.g., cytotoxicity, irritation, sensitisation) is also an essential requirement to ensure user safety and comfort is another issue.
- (2)
- Discrete sensor/device integration in textiles—Electronics (e.g., inertial sensors, pulse oximetry, temperature, circuit) and textile integration has progressed in three generations [125]. First generation e-textiles attached conventional rigid electronics to textiles i.e., the textiles acted only as a platform for the electronics (e.g., Philip-Levi ICD jacket [126]). Second generation e-textiles embedded functional devices such as switches and sensors into the textile [127]. Third generation e-textiles integrate flexible electronic functionality, including circuits [96], at the yarn level in e-yarns with significantly reduced size thus allowing the potential for electronics to be unobtrusive and effectively hidden within the textile. However, challenges remain on e-yarn length, reliable interconnections, and component sizes and flexibility limit integration.
- (3)
- Manufacturing—The widespread manufacturing of e-textiles has been limited by the diverse range of techniques required to produce a set of functions in an e-textile. Ideally the e-textiles manufacturing process should be compatible with existing equipment (e.g., spinning, knitting, weaving, printing, coating, dyeing, finishing) already in use for conventional textile manufacturing to enable mass production. This is not straightforward and the specific challenges will depend on the electronics functionality and manufacturing process. For example, printing functional materials requires a much higher quality print than would be the case for patterning a fabric since any errors will result in failure.
- (4)
- Regulatory—Compliance with medical device regulations is necessary for medical devices in order to demonstrate the safety and clinical effectiveness. This has set an entry barrier and lengthened the time required to take medical devices to market. The change in the EU medical device regulation with the Medical Device Regulation (MDR) replacing the Medical Device Directive (MDD), with full effect from May 2020, will make the entry barrier even higher. Clinical evaluation (e.g., randomized controlled trials) are needed for new emerging products.
- (5)
- End users need validation—The majority of scientific research has been carried out in the lab with little or no input from end users. This leads to a disconnection between the technology and the end user requirements which delays uptake and the development of new products. Involvement of the end user and other key stakeholders (e.g., clinicians, regulators) from the outset of the project is essential to ensure the research effectively addresses the users’ need and smooths the transfer from lab research to adoption in the market.
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Ageing and Health. Available online: https://www.who.int/news-room/fact-sheets/detail/ageing-and-health (accessed on 25 July 2019).
- Kaewkannate, K.; Kim, S. A comparison of wearable fitness devices. BMC Public Health 2016, 16. [Google Scholar] [CrossRef] [PubMed]
- Pantelopoulos, A.; Bourbakis, N.G. A survey on wearable sensor-based systems for health monitoring and prognosis. IEEE Trans. Syst. Man Cybern. Part C Appl. Rev. 2010, 40, 1–12. [Google Scholar] [CrossRef]
- Imani, S.; Bandodkar, A.J.; Mohan, A.M.V.; Kumar, R.; Yu, S.; Wang, J.; Mercier, P.P. A wearable chemical—Electrophysiological hybrid biosensing system for real-time health and fitness monitoring. Nat. Commun. 2016, 7, 11650. [Google Scholar] [CrossRef] [PubMed]
- Gandhi, N.; Khe, C.; Chung, D.; Chi, Y.M.; Cauwenberghs, G. Properties of Dry and Non-contact Electrodes for Wearable Physiological Sensors. In Proceedings of the 2011 International Conference on Body Sensor Networks, Dallas, TX, USA, 23–25 May 2011; pp. 107–112. [Google Scholar] [CrossRef]
- Hayward, J. E-Textiles 2019–2029: Technologies, Markets and Players; IDTechEx: Cambridge, UK, 2019. [Google Scholar]
- Boehm, A.; Yu, X.; Neu, W.; Leonhardt, S.; Teichmann, D. A novel 12-lead ECG T-shirt with Active Electrodes. Electronics 2016, 5, 75. [Google Scholar] [CrossRef]
- Yang, K.; Meadmore, K.; Freeman, C.; Grabham, N.; Hughes, A.-M.; Wei, Y.; Torah, R.; Glanc-Gostkiewicz, M.; Beeby, S.; Tudor, J. Development of user-friendly wearable electronic textiles for healthcare applications. Sensors 2018, 18, 2410. [Google Scholar] [CrossRef]
- Sim, S.Y.; Jeon, H.S.; Chung, G.S.; Kim, S.K.; Kwon, S.J.; Lee, W.K.; Park, K.S. Fall Detection Algorithm for the Elderly Using Acceleration Sensors on the Shoes. In Proceedings of the 2011 Annual International Conference of the IEEE Engineering in Medicine and Biology Society, Boston, MA, USA, 30 August–3 September 2011; pp. 4935–4938. [Google Scholar] [CrossRef]
- E-Textiles Network. Available online: https://e-textiles-network.com/ (accessed on 21 August 2019).
- United Nations, Department of Economic and Social Affairs, Population Division. World Population Ageing 2017—Highlights. Available online: https://www.un.org/en/development/desa/population/publications/pdf/ageing/WPA2017_Highlights.pdf (accessed on 25 July 2019).
- Healthy Ageing. Available online: https://www.ukri.org/innovation/industrial-strategy-challenge-fund/healthy-ageing/ (accessed on 25 July 2019).
- Friedman, S.M.; Mulhausen, P.; Cleveland, M.L.; Coll, P.P.; Daniel, K.M.; Hayward, A.D.; Shah, K.; Skudlarska, B.; White, H.K. Healthy aging: American Geriatrics Society white paper executive summary. J. Am. Geriatr. Soc. 2019, 67, 17–20. [Google Scholar] [CrossRef]
- Rowe, J.W.; Kahn, R.L. Successful aging. Gerontologist 1997, 37, 433–440. [Google Scholar] [CrossRef]
- Lu, W.; Pikhart, H.; Sacker, A. Domains and measurements of healthy aging in epidemiological studies: A review. Gerontologist 2018. [Google Scholar] [CrossRef]
- Melzer, D.; Delgado, J.C.; Winder, R.; Masoli, J.; Richards, S.; Ble, A. The Age UK Almanac of Disease Profiles in Later Life. Available online: https://www.ageuk.org.uk/Documents/EN-GB/For-professionals/Research/Age_UK_almanac_FINAL_9Oct15.pdf?dtrk=true (accessed on 25 July 2019).
- Lara, J.; Godfrey, A.; Evans, E.; Heaven, B.; Brown, L.J.; Barron, E.; Rochester, L.; Meyer, T.D.; Mathers, J.C. Towards measurement of the healthy ageing phenotype in lifestyle-based intervention studies. Maturitas 2013, 76, 189–199. [Google Scholar] [CrossRef]
- Lawton, M.P.; Broody, E.M. Assessment of older people: Self-maintaining and instrumental activities of daily living. Gerontologist 1969, 9, 179–186. [Google Scholar] [CrossRef]
- Ryff, C.D.; Keyes, C.L.M. The structure of psychological well-being revisited. J. Personal. Soc. Psychol. 1995, 69, 719–727. [Google Scholar] [CrossRef]
- Strawbridge, W.J.; Wallhagen, M.I.; Cohen, R.D. Successful aging and wellbeing: Self-rated compared with Rowe and Khan. Gerontologist 2002, 42, 727–733. [Google Scholar] [CrossRef] [PubMed]
- Cosco, T.D.; Prina, A.M.; Perales, J.; Stephan, B.C.M.; Brayne, C. Lay perspectives of successful ageing: A systematic review and meta-ethnography. BMJ Open 2013, 3, e002710. [Google Scholar] [CrossRef] [PubMed]
- Chian Teh, J.H.; Brown, L.J.E.; Bryant, C. Perspectives on successful ageing: The views of Chinese older adults living in Australia on what it means to age well. Australas. J. Ageing 2019. [Google Scholar] [CrossRef] [PubMed]
- Sphere. Available online: https://www.irc-sphere.ac.uk/ (accessed on 25 July 2019).
- Fafoutis, X.; Vafeas, A.; Janko, B.; Sherratt, R.S.; Pope, J.; Elsts, A.; Mellios, E.; Hilton, G.; Oikonomou, G.; Piechocki, R.; et al. Designing wearable sensing platforms for healthcare in a residential environment. EAI Endorsed Trans. Pervasive Health Technol. 2017, 3, 153063. [Google Scholar] [CrossRef]
- Phan, D.; Horne, M.; Pathirana, P.N.; Farzanehfar, P. Measurement of axial rigidity and postural instability using wearable sensors. Sensors 2018, 18, 495. [Google Scholar] [CrossRef]
- Mental Health of Older Adults. Available online: https://www.who.int/news-room/fact-sheets/detail/mental-health-of-older-adults (accessed on 21 August 2019).
- Guo, Q.; Deng, W.H.; Bebek, O.; Cavusoglu, M.C.; Mastrangelo, C.H.; Young, D.J. Personal inertial navigation system assisted by MEMS ground reaction sensor array and interface ASIC for GPS-denied environment. IEEE J. Solid-State Circuits 2018, 53, 3039–3049. [Google Scholar] [CrossRef]
- Woodberry, E.; Browne, G.; Hodges, S.; Watson, P.; Kapur, N.; Woodberry, K. The use of a wearable camera improves autobiographical memory in patients with Alzheimer’s disease. Memory 2014, 23, 340–349. [Google Scholar] [CrossRef]
- Ekström, A.; Ferm, U.; Samuelsson, C. Digital communication support and Alzheimer’s disease. Dementia 2015. [Google Scholar] [CrossRef]
- Kong, A.P.-H. The use of free non-dementia-specific Apps on iPad to conduct group communication exercises for individuals with Alzheimer’s disease (Innovative Practice). Dementia 2017. [Google Scholar] [CrossRef]
- Stavropoulos, T.G.; Meditskos, G.; Kompatsiaris, I. DemaWare2: Integrating sensors, multimedia and semantic analysis for the ambient care of dementia. Pervasive Mob. Comput. 2017, 34, 126–145. [Google Scholar] [CrossRef]
- Dayer, L.; Heldenbrand, S.; Anderson, P.; Gubbins, P.O. Martin BC.Smartphone medication adherence apps: Potential benefits to patients and providers. J. Am. Pharm. Assoc. 2013, 53, 172–181. [Google Scholar] [CrossRef] [PubMed]
- Aldeer, M.; Javanmard, M.; Martin, R.P. A review of medication adherence monitoring technologies. Appl. Syst. Innov. 2018, 1, 14. [Google Scholar] [CrossRef]
- Wang, W.; Sitová, Z.; Jia, X.; He, X.; Abramson, T.; Gasti, P.; Balagani, K.S.; Farajidavar, A. Automatic identification of solid-phase medication intake using wireless wearable accelerometers. In Proceedings of the 36th Annual International Conference of the IEEE Engineering in Medicine and Biology Society, Chicago, IL, USA, 26–30 August 2014; pp. 4168–4171. [Google Scholar] [CrossRef]
- Ten Breteler, M.R.; Nierstrasz, V.A.; Warmoeskerken, M.M.C.G. Textile slow-release systems with medical applications. AUTEX Res. J. 2002, 2, 4. [Google Scholar]
- Botella, C.; Etchemendy, E.; Castilla, D.; Baños, R.M.; García-Palacios, A.; Quero, S.; Alcañiz, M.; Lozano, J.A. An e-health system for the elderly (Butler Project): A pilot study on acceptance and satisfaction. Cyberpsychol. Behav. 2009, 12, 255–262. [Google Scholar] [CrossRef]
- Catalan-Matamoros, D.; Gomez-Conesa, A.; Stubbs, B.; Vancampfort, D. Exercise improves depressive symptoms in older adults: An umbrella review of systematic reviews and meta-analyses. Psychiatry Res. 2016, 244, 202–209. [Google Scholar] [CrossRef]
- Harris, M.A. Maintenance of behaviour change following a community-wide gamification based physical activity intervention. Prev. Med. Rep. 2019, 13, 37–40. [Google Scholar] [CrossRef]
- Soleymani, M.; Asghari-Esfeden, S.; Fu, Y.; Pantic, M. Analysis of EEG signals and facial expressions for continuous emotion detection. IEEE Trans. Affect. Comput. 2016, 7, 17–28. [Google Scholar] [CrossRef]
- The HugShirt. Available online: http://cutecircuit.com/the-hug-shirt/ (accessed on 1 May 2019).
- Treadaway, C.; Kenning, G. Sensor e-Textiles: Person centered co-design for people with late stage dementia. Work. Older People J. 2016, 20, 76–85. [Google Scholar] [CrossRef]
- Ko, P.R.; Kientz, J.A.; Choe, E.K.; Kay, M.; Landis, C.A. Watson NF6.Consumer sleep technologies: A review of the landscape. J. Clin. Sleep Med. 2015, 11, 1455–1461. [Google Scholar] [CrossRef]
- Mack, D.C.; Mack, D.C.; Patrie, J.T.; Suratt, P.M.; Felder, R.A.; Alwan, M. Development and preliminary validation of heart rate and breathing rate detection using a passive, ballistocardiography-based sleep monitoring system. IEEE Trans. Inf. Technol. Biomed. 2009, 13, 111–120. [Google Scholar] [CrossRef] [PubMed]
- Wu, J.; Dong, L.; Xiao, W. Real-time Physical Activity classification and tracking using wearable sensors. In Proceedings of the 6th International Conference on Information, Communications & Signal Processing, Singapore, 10–13 December 2007; pp. 1–6. [Google Scholar] [CrossRef]
- Qiu, S.; Wang, Z.; Zhao, H.; Qin, K.; Li, Z.; Hu, H. Inertial/magnetic sensors based pedestrian dead reckoning by means of multi-sensor fusion. Inf. Fus. 2017, 39, 108–119. [Google Scholar] [CrossRef]
- Fernández-Caramés, T.M. An intelligent power outlet system for the smart home of the internet of things. Int. J. Distrib. Sens. Netw. 2015. [Google Scholar] [CrossRef] [PubMed]
- Suryadevara, M.K.; Mukhopadhyay, S.C. Wireless sensor network based home monitoring system for wellness determination of elderly. IEEE Sens. J. 2012, 12, 1965–1972. [Google Scholar] [CrossRef]
- Arshad, A.; Khan, S.; Alam, A.H.M.Z.; Tasnim, R.; Gunawan, T.S.; Ahmad, R.; Nataraj, C. An activity monitoring system for senior citizens living independently using capacitive sensing technique. In Proceedings of the 2016 IEEE International Instrumentation and Measurement Technology Conference, Taipei, Taiwan, 23–26 May 2016. [Google Scholar] [CrossRef]
- Ejupi, A.; Menon, C. Detection of talking in respiratory signals: A feasibility study using machine learning and wearable textile-based sensors. Sensors 2018, 18, 2474. [Google Scholar] [CrossRef] [PubMed]
- Hodkin, E.F.; Lei, Y.; Humby, J.; Glover, I.S.; Choudhury, S.; Kumar, H.; Perez, M.A.; Rodgers, H.; Jackson, A. Automated FES for upper limb rehabilitation following stroke and spinal cord injury. IEEE Trans. Neural Syst. Rehabil. Eng. 2018, 26, 1067–1074. [Google Scholar] [CrossRef]
- Beckerle, P.; Salvietti, G.; Unal, R.; Prattichizzo, D.; Rossi, S.; Castellini, C.; Hirche, S.; Endo, S.; Amor, H.B.; Ciocarlie, M.; et al. A human–robot interaction perspective on assistive and rehabilitation robotics. Front. Neurorobot. 2017, 11. [Google Scholar] [CrossRef]
- Dirks, M.L.; Hansen, D.; Van Assche, A.; Dendale, P.; Van Loon, L.J. Neuromuscular electrical stimulation prevents muscle wasting in critically ill comatose patients. Clin. Sci. 2015, 128, 357–365. [Google Scholar] [CrossRef]
- Hassan, L.; Dias, A.; Hamari, J. How motivational feedback increases user’s benefits and continued use: A study on gamification, quantified-self and social networking. Int. J. Inf. Manag. 2019, 46, 151–162. [Google Scholar] [CrossRef]
- Sullivan, A.N.; Lachman, M.E. Behavior change with fitness technology in sedentary adults: A review of the evidence for increasing physical activity. Front. Public Health 2017, 4, 289. [Google Scholar] [CrossRef] [PubMed]
- Zak, R.B.; Hassenstab, B.M.; Zuehlke, L.K.; Heesch, M.W.S.; Shute, R.J.; Laursen, T.L.; LaSalle, D.T.; Slivka, D.R. Impact of local heating and cooling on skeletal muscle transcriptional response related to myogenesis and proteolysis. Eur. J. App. Physiol. 2018, 118, 101–109. [Google Scholar] [CrossRef] [PubMed]
- Broatch, J.R. Lower limb sports compression garments improve muscle blood flow and exercise performance during repeated-sprint cycling. Int. J. Sports Physiol. Perform. 2018, 13, 882–890. [Google Scholar] [CrossRef] [PubMed]
- Health Quality Ontario. Electronic monitoring systems to assess urinary incontinence: A health technology assessment. Ont. Health Technol. Assess. Ser. 2018, 18, 1–60. [Google Scholar]
- Stewart, F.; Gameiro, L.F.; El Dib, R.; Gameiro, M.O.; Kapoor, A.; Amaro, J.L. Electrical stimulation with non-implanted electrodes for overactive bladder in adults. Cochrane Database Syst. Rev. 2016. [Google Scholar] [CrossRef]
- Innovo. Available online: https://www.myinnovo.com/uk (accessed on 25 July 2019).
- Dias, D.; Paulo Silva Cunha, J. Wearable health devices—Vital sign monitoring, systems and technologies. Sensors 2018, 18, 2414. [Google Scholar] [CrossRef] [PubMed]
- Boyko, T.V.; Longaker, M.T.; Yang, G.P. Review of the current management of pressure ulcers. Adv. Wound Care 2018, 7, 57–67. [Google Scholar] [CrossRef]
- Tsuchiya, S.; Sato, A.; Azuma, E.; Urushidani, H.; Osawa, M.; Kadoya, K.; Takamura, M.; Nunomi, M.; Mitsuoka, A.; Nishizawa Yokono, T.; et al. The effectiveness of small changes for pressure redistribution; using the air mattress for small changes. J. Tissue Viability 2016, 25, 135–142. [Google Scholar] [CrossRef]
- Siddiqui, A.; Behrendt, R.; Lafluer, M.; Craft, S. A continuous bedside pressure mapping system for prevention of pressure ulcer development in the ICU: A retrospective analysis. Wounds 2013, 25, 333–339. [Google Scholar]
- Bailey, T.; Bode, B.W.; Christiansen, M.P.; Klaff, L.J.; Alva, S. The performance and usability of a factory-calibrated flash glucose monitoring system. Diabetes Technol. Ther. 2015, 17, 1. [Google Scholar] [CrossRef]
- Rodbard, D. Continuous glucose monitoring: A review of successes, challenges, and opportunities. Diabetes Technol. Ther. 2016, 18, S2. [Google Scholar] [CrossRef]
- Karpova, E.V.; Shcherbacheva, E.V.; Galushin, A.A.; Vokhmyanina, D.V.; Karyakina, E.E.; Karyakin, A.A. Noninvasive diabetes monitoring through continuous analysis of sweat using flow-through glucose biosensor. Anal. Chem. 2019, 91, 3778–3783. [Google Scholar] [CrossRef]
- Ascaso, F.J.; Huerva, V. Noninvasive continuous monitoring of tear glucose using glucose-sensing contact lenses. Optom. Vis. Sci. 2016, 93, 426–434. [Google Scholar] [CrossRef]
- Vieira, E.R.; Palmer, R.C.; Chaves, P.H.M. Prevention of falls in older people living in the community. BMJ 2016, 353, i1419. [Google Scholar] [CrossRef]
- Lee, C.H.; Sun, T.L. Evaluation of postural stability based on a force plate and inertial sensor during static balance measurements. J. Physiol. Anthropol. 2018, 37, 27. [Google Scholar] [CrossRef]
- Van de Veg, P.; O’Brien, H.; Nelson, J.; Clifford, A. Unobtrusive monitoring and identification of fall accidents. Med. Eng. Phys. 2015, 37, 499–504. [Google Scholar] [CrossRef]
- Phillips, L.J.; DeRoche, C.B.; Rantz, M.; Alexander, G.L.; Skubic, M.; Despins, L.; Abbott, C.; Harris, B.H.; Galambos, C.; Koopman, R.J. Using embedded sensors in independent living to predict gait changes and falls. Western J. Nurs. Res. 2016, 39, 78–94. [Google Scholar] [CrossRef]
- Pierleoni, P.; Belli, A.; Palma, L.; Pellegrini, M.; Pernini, L.; Valenti, S. A high reliability wearable device for elderly fall detection. IEEE Sens. J. 2015, 15, 4544–4553. [Google Scholar] [CrossRef]
- Feng, G.; Mai, J.; Ban, Z.; Guo, X.; Wang, G. Floor pressure imaging for fall detection with fiber-optic sensors. IEEE Pervasive Comput. 2016, 15, 40–47. [Google Scholar] [CrossRef]
- Russo, M.A.; Santarelli, D.M.; O’Rourke, D. The physiological effects of slow breathing in the healthy human. Breathe 2017, 13, 298–309. [Google Scholar] [CrossRef]
- Massaroni, C.; Venanzi, C.; Silvatti, A.P.; Lo Presti, D.; Saccomandi, P.; Formica, D.; Giurazza, F.; Caponero, M.A.; Schena, E. Smart textile for respiratory monitoring and thoraco-abdominal motion pattern evaluation. J. Biophoton. 2017, 11, e201700263. [Google Scholar] [CrossRef]
- Bauman, A.; Merom, D.; Bull, F.C.; Buchner, D.M.; Singh, M.A.F. Updating the evidence for physical activity: Summative reviews of the epidemiological evidence, prevalence, and interventions to promote “active aging”. Gerontologist 2016, 56, S268–S280. [Google Scholar] [CrossRef]
- Zheng, Y.; Ding, X.R.; Poon, C.C.; Lo, B.P.; Zhang, H.; Zhou, X.L.; Yang, G.Z.; Zhao, N.; Zhang, Y.T. Unobtrusive sensing and wearable devices for health informatics. IEEE Trans. Biomed. Eng. 2014, 61, 1538–1554. [Google Scholar] [CrossRef]
- Hardy, D.A.; Anastasopoulos, I.; Nashed, M.N.; Oliveira, C.; Hughes-Riley, T.; Komolafe, A.; Tudor, J.; Torah, R.; Beeby, S.; Dias, T. Automated insertion of package dies onto wire and into a textile yarn sheath. Microsyst. Technol. 2019. [Google Scholar] [CrossRef]
- Beeby, S.; Torah, R.; Tudor, J.; Li, M.; Komolafe, A.; Yang, K. Functional Electronic Textiles: Circuit Integration and Energy Harvesting Power Supplies. In Proceedings of the 2018 International Flexible Electronics Technology Conference (IFETC), Ottawa, ON, Canada, 7–9 August 2018; pp. 1–3. [Google Scholar] [CrossRef]
- Maresova, P.; Tomsone, S.; Lameski, P.; Madureira, J.; Mendes, A.; Zdravevski, E.; Chorbev, I.; Trajkovik, V.; Ellen, M.; Rodile, K. Technological solutions for older people with Alzheimer’s disease: Review. Curr. Alzheimer Res. 2018, 15, 975–983. [Google Scholar] [CrossRef]
- The Funding Landscape. Available online: https://epsrc.ukri.org/research/ourportfolio/themes/healthcaretechnologies/strategy/toolkit/landscape/ (accessed on 25 July 2019).
- Mokhlespour Esfahani, M.I.; Nussbaum, M.A. Preferred placement and usability of a smart textile system vs. inertial measurement units for activity monitoring. Sensors 2018, 18, 2501. [Google Scholar] [CrossRef]
- LilyPad Accelerometer. Available online: https://www.sparkfun.com/products/9267 (accessed on 25 July 2019).
- Tognetti, A.; Lorussi, F.; Carbonaro, N.; De Rossi, D. Wearable goniometer and accelerometer sensory fusion for knee joint angle measurement in daily life. Sensors 2015, 15, 28435–28455. [Google Scholar] [CrossRef]
- FETT. Available online: https://www.fett.ecs.soton.ac.uk/ (accessed on 25 July 2019).
- Ankhili, A.; Tao, X.; Cochrane, C.; Coulon, D.; Koncar, V. Washable and reliable textile electrodes embedded into underwear fabric for electrocardiography (ECG) monitoring. Materials 2018, 11, 256. [Google Scholar] [CrossRef]
- Shu, L.; Xu, T.; Xu, X. Multilayer sweat-absorbable textile electrode for EEG measurement in forehead site. IEEE Sens. J. 2019, 19, 5995–6005. [Google Scholar] [CrossRef]
- Di Giminiani, R.; Lancia, S.; Ferrari, M.; Quaresima, V.; Tilma Vistisen, H.; Kliltgaard, A.; Arbjerg Heick, R.; Oestergard, K.; Yndgaard Soerensen, K.; Cardinale, M. A Wearable Integrated Textile EMG and Muscle Oximetry System for Monitoring Exercise-Induced Effects: A Feasibility Study. In Proceedings of the 2018 IEEE International Symposium on Medical Measurements and Applications (MeMeA), Rome, Italy, 11–13 June 2018; pp. 1–5. [Google Scholar] [CrossRef]
- Rothmaier, M.; Selm, B.; Spichtig, S.; Haensse, D.; Wolf, M. Photonic textiles for pulse oximetry. Opt. Express. 2008, 16, 12973–12986. [Google Scholar] [CrossRef]
- Satharasinghe, A.; Hughes-Riley, T.; Tilak, D. Photodiodes embedded within electronic textiles. Sci. Rep. 2018, 8, 16205. [Google Scholar] [CrossRef]
- Mokhlespour Esfahani, M.I.; Nussbaum, M.A. A “Smart” Undershirt for Tracking Upper Body Motions: Task Classification and Angle Estimation. IEEE Sens. J. 2018, 18, 7650–7658. [Google Scholar] [CrossRef]
- Lorussi, F.; Carbonaro, N.; De Rossi, D.; Tognetti, A. Strain- and angular-sensing fabrics for human motion analysis in daily life. In Smart Textiles; Schneegass, S., Amft, O., Eds.; Springer: Cham, Switzerland, 2017. [Google Scholar] [CrossRef]
- Liang, A.; Stewart, R.; Bryan-Kinns, N. Analysis of sensitivity, linearity, hysteresis, responsiveness, and fatigue of textile knit stretch sensors. Sensors 2019, 19, 3618. [Google Scholar] [CrossRef]
- Totaro, M.; Poliero, T.; Mondini, A.; Lucarotti, C.; Cairoli, G.; Ortiz, J.; Beccai, L. Soft smart garments for lower limb joint position analysis. Sensors 2017, 17, 2314. [Google Scholar] [CrossRef]
- Lugoda, P.; Hughes-Riley, T.; Morris, R.; Dias, T. A wearable textile thermograph. Sensors 2018, 18, 2369. [Google Scholar] [CrossRef]
- Komolafe, A.; Torah, R.; Wei, Y.; Nunes-Matos, H.; Li, M.; Hardy, D.; Dias, T.; Tudor, M.; Beeby, S. Integration flexible filament circuits for e-textile applications. Adv. Mater. Technol. 2019, 4. [Google Scholar] [CrossRef]
- Sakamoto, H.; Tanaka, A.; Suematsu, R.; Nakajima, Y.; Douseki, T. Self-Powered Wireless Urinary-Incontinence Sensor System Detecting Urine Amount and Diaper Change Timing in Under 10 Minutes. In Proceedings of the 12th International Symposium on Medical Information and Communication Technology (ISMICT), Sydney, Australia, 26–28 March 2018; pp. 1–4. [Google Scholar] [CrossRef]
- Zhou, G.; Byun, J.; Oh, Y.; Jung, B.M.; Cha, H.J.; Seong, D.G.; Um, M.K.; Hyun, S.; Chou, T.W. Highly sensitive wearable textile-based humidity sensor made of high-strength, single-walled carbon nanotube/poly(vinyl alcohol) filaments. ACS Appl. Mater. Interfaces 2017, 9, 4788–4797. [Google Scholar] [CrossRef]
- Lee, J.; Kwon, H.; Seo, J.; Shin, S.; Koo, J.H.; Pang, C.; Son, S.; Kim, J.H.; Jang, Y.H.; Kim, D.E.; et al. Conductive fiber-based ultrasensitive textile pressure sensor for wearable electronics. Adv. Mater. 2015, 27, 2433–2439. [Google Scholar] [CrossRef]
- Texisense. Available online: https://www.texisense.com/ (accessed on 25 July 2019).
- Liu, M.; Pu, X.; Jiang, C.; Liu, T.; Huang, X.; Chen, L.; Du, C.; Sun, J.; Hu, W.; Wang, Z.L. Large-area all-textile pressure sensors for monitoring human motion and physiological signals. Adv. Mater. 2017, 29, 1703700. [Google Scholar] [CrossRef]
- Samy, L.; Huang, M.C.; Liu, J.J.; Xu, W.; Sarrafzadeh, M. Unobtrusive sleep stage identification using a pressure-sensitive bed sheet. IEEE Sens. J. 2014, 14, 2092–2101. [Google Scholar] [CrossRef]
- Yang, S.Y.; Huang, M.; Liu, J.J.; Xu, W.; Sarrafzadeh, M. Soft Fabric Actuator for Robotic Applications. In Proceedings of the 2018 IEEE/RSJ International Conference on Intelligent Robots and Systems (IROS), Madrid, Spain, 1–5 October 2018; pp. 5451–5456. [Google Scholar] [CrossRef]
- Park, W.; Shin, E.J.; Yoo, Y.; Choi, S.; Kim, S.Y. Soft haptic actuator based on knitted PVC gel fabric. IEEE Trans. Ind. Electron. 2019, 67, 677–685. [Google Scholar] [CrossRef]
- Inose, H.; Mohri, S.; Yamada, Y.; Nakamura, T.; Yokoyama, K.; Kikutani, I. Development of a Lightweight Power-Assist Suit Using Pneumatic Artificial Muscles and Balloon-Amplification Mechanism. In Proceedings of the International Conference on Control, Automation, Robotics and Vision (ICARCV), Phuket, Thailand, 13–15 November 2016. [Google Scholar] [CrossRef]
- Diteesawat, R.S.; Helps, T.; Taghavi, M.; Rossiter, J. High strength bubble artificial muscles for walking assistance. In Proceedings of the 2018 IEEE International Conference on Soft Robotics (RoboSoft), Livorno, Italy, 24–28 April 2018; pp. 388–393. [Google Scholar] [CrossRef]
- Li, W.; Torres, D.; Díaz, M.; Wang, Z.; Wu, C.; Wang, C.; Wang, Z.L.; Sepúlveda, N. Nanogenerator-based dual-functional and self-powered thin patch loudspeaker or microphone for flexible electronics. Nat. Commun. 2017, 8, 15310. [Google Scholar] [CrossRef] [PubMed]
- Park, S.; Ahn, S.; Kim, J.; Jeong, J.; Park, T.H.; Yoon, H.; Hur, J.; Park, J.J. Textile speaker using polyvinylidene fluoride/ZnO nanopillar on Au textile for enhancing the sound pressure level. Sci. Adv. Mater. 2018, 10, 1788–1792. [Google Scholar] [CrossRef]
- Li, Y.; Torah, R.; Wei, Y.; Grabham, N.; Tudor, J. Dispenser-printed sound-emitting fabrics for applications in the creative fashion and smart architecture industry. J. Text. Inst. 2019, 110, 1–9. [Google Scholar] [CrossRef]
- Chu, M.; Nguyen, T.; Pandey, V.; Zhou, Y.; Pham, H.N.; Bar-Yoseph, R.; Radom-Aizik, S.; Jain, R.; Cooper, D.M.; Khine, M. Respiration rate and volume measurements using wearable strain sensors. NPJ Digit. Med. 2019, 2, 8. [Google Scholar] [CrossRef]
- Ramos-Garcia, R.I.; Da Silva, F.; Kondi, Y.; Sazonov, E.; Dunne, L.E. Analysis of a Coverstitched Stretch Sensor for Monitoring of Breathing. In Proceedings of the 2016 10th International Conference on Sensing Technology (ICST), Nanjing, China, 11–13 November 2016; pp. 1–6. [Google Scholar] [CrossRef]
- Ciocchetti, M.; Massaroni, C.; Saccomandi, P.; Caponero, M.A.; Polimadei, A.; Formica, D.; Schena, E. Smart textile based on fiber bragg grating sensors for respiratory monitoring: Design and preliminary trials. Biosensors 2015, 5, 602–615. [Google Scholar] [CrossRef]
- Guay, P.; Gorgutsa, S.; LaRochelle, S.; Messaddeq, Y. Wearable contactless respiration sensor based on multi-material fibers integrated into textile. Sensors 2017, 17, 1050. [Google Scholar] [CrossRef]
- White, N.M.; Ash, J.; Wei, Y.; Akerman, H. A planar respiration sensor based on a capaciflector structure. IEEE Sens. Lett. 2017, 1. [Google Scholar] [CrossRef]
- Karacocuk, G.; Karacocuk, G.; Höflinger, F.; Zhang, R.; Reindl, L.M.; Laufer, B.; Möll, K.; Röell, M.; Zdzieblik, D. Inertial sensor-based respiration analysis. IEEE Trans. Instrum. Meas. 2019, 68, 4268–4275. [Google Scholar] [CrossRef]
- FIFA Approved GPS Performance Tracker. Available online: https://statsports.com/apex-athlete-series/ (accessed on 25 July 2019).
- Morais, D.S.; Guedes, R.M.; Lopes, M.A. Antimicrobial approaches for textiles: From research to market. Materials 2016, 9, 498. [Google Scholar] [CrossRef]
- Derakhshandeh, H.; Kashaf, S.S.; Aghabaglou, F.; Ghanavati, I.O.; Tamayol, A. Smart bandages: The future of wound care. Trends Biotechnol. 2016, 36, 1259–1274. [Google Scholar] [CrossRef]
- Mostafalu, P.; Kiaee, G.; Giatsidis, G.; Khalilpour, A.; Nabavinia, M.; Dokmeci, M.R.; Sonkusale, S.; Orgill, D.P.; Tamayol, A.; Khademhosseini, A. A textile dressing for temporal and dosage controlled drug delivery. Adv. Funct. Mater. 2017, 27, 1702399. [Google Scholar] [CrossRef]
- Blazewear. Available online: https://www.blazewear.com/ (accessed on 25 July 2019).
- Stoppa, M.; Chiolerio, A. Wearable electronics and smart textiles: A critical review. Sensors 2014, 14, 11957–11992. [Google Scholar] [CrossRef]
- Castano, L.M.; Flatau, A.B. mart fabric sensors and e-textile technologies: A review. Smart Mater. Struct. 2014, 23. [Google Scholar] [CrossRef]
- McLaren, R.; Joseph, F.; Baguley, C.; Taylor, D. A review of e-textiles in neurological rehabilitation: How close are we? J. Neuroeng. Rehabil. 2016, 13. [Google Scholar] [CrossRef]
- Liu, Y.; Wang, H.; Zhao, W.; Zhang, M.; Qin, H.; Xie, Y. Flexible, stretchable sensors for wearable health monitoring: Sensing mechanisms, materials, fabrication strategies and features. Sensors 2018, 18, 645. [Google Scholar] [CrossRef]
- Hughes-Riles, T.; Dias, T.; Cork, C. A historical review of the development of electronic textiles. Fibers 2018, 6, 34. [Google Scholar] [CrossRef]
- Malmivaara, M. The emergence of wearable computing. In Smart Clothes and Wearable Technology; McCann, J., Bryson, D., Eds.; Woodhead Publishing: Sawston, UK, 2009; pp. 3–24. ISBN 9781845693572. [Google Scholar] [CrossRef]
- Kinkeldei, T.; Zysset, C.; Cherenack, K.; Troester, G. Development and Evaluation of Temperature Sensors for Textile Integration. In Proceedings of the IEEE Sensors, Christchurch, New Zealand, 25–28 October 2009. [Google Scholar]


© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yang, K.; Isaia, B.; Brown, L.J.E.; Beeby, S. E-Textiles for Healthy Ageing. Sensors 2019, 19, 4463. https://doi.org/10.3390/s19204463
Yang K, Isaia B, Brown LJE, Beeby S. E-Textiles for Healthy Ageing. Sensors. 2019; 19(20):4463. https://doi.org/10.3390/s19204463
Chicago/Turabian StyleYang, Kai, Beckie Isaia, Laura J.E. Brown, and Steve Beeby. 2019. "E-Textiles for Healthy Ageing" Sensors 19, no. 20: 4463. https://doi.org/10.3390/s19204463
APA StyleYang, K., Isaia, B., Brown, L. J. E., & Beeby, S. (2019). E-Textiles for Healthy Ageing. Sensors, 19(20), 4463. https://doi.org/10.3390/s19204463





