Wearable Health Devices—Vital Sign Monitoring, Systems and Technologies
Abstract
1. Introduction
2. Vital Signs—Most Important to be Monitored
3. Valuable Vital Signs
3.1. Electrocardiogram (ECG)
3.2. Heart Rate (HR)
3.3. Blood Pressure (BP)
3.4. Respiration Rate (RR)
3.5. Blood Oxygen Saturation (SpO2)
3.6. Blood Glucose (BG)
3.7. Skin Perspiration
- (1)
- Epidermal-based have a conformal contact between the electrodes surface and the biofluid, like elastomeric stamps to print electrodes directly on human epidermis for continuous monitoring
- (2)
- Fabric/flexible plastic-based sensors, the most used, having a main advantage of constant contact with a large surface area of the skin. These can be embedded into fabric or screen-printed into it, obtaining specifics measurements like pH and ions concentration as NH4+, K+ and Cl− [55].
3.8. Capnography
3.9. Body Temperature
3.10. Other Physiological Parameters
3.10.1. Motion Evaluation
3.10.2. Cardiac Implantable Devices
3.11. Ambiance Parameters
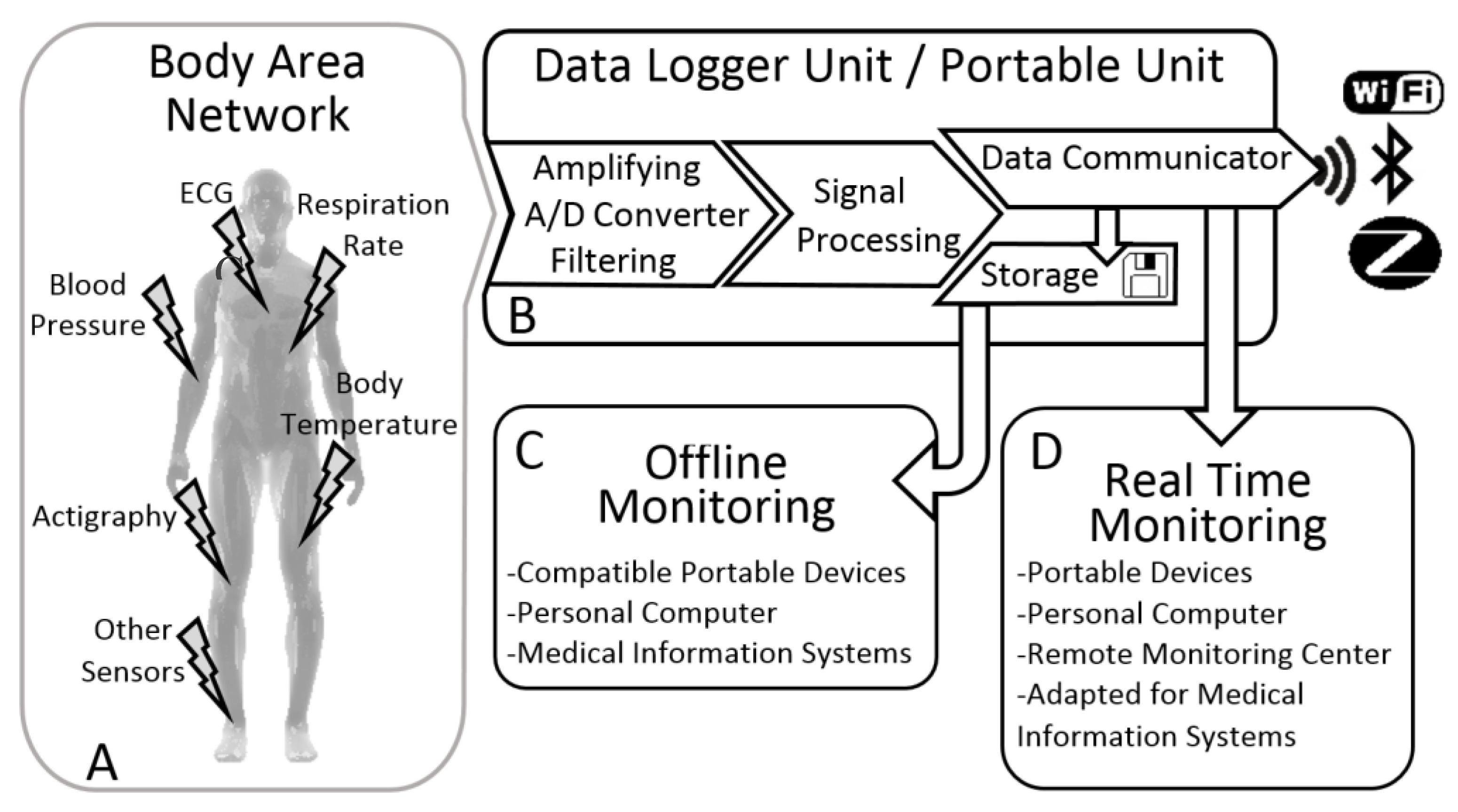
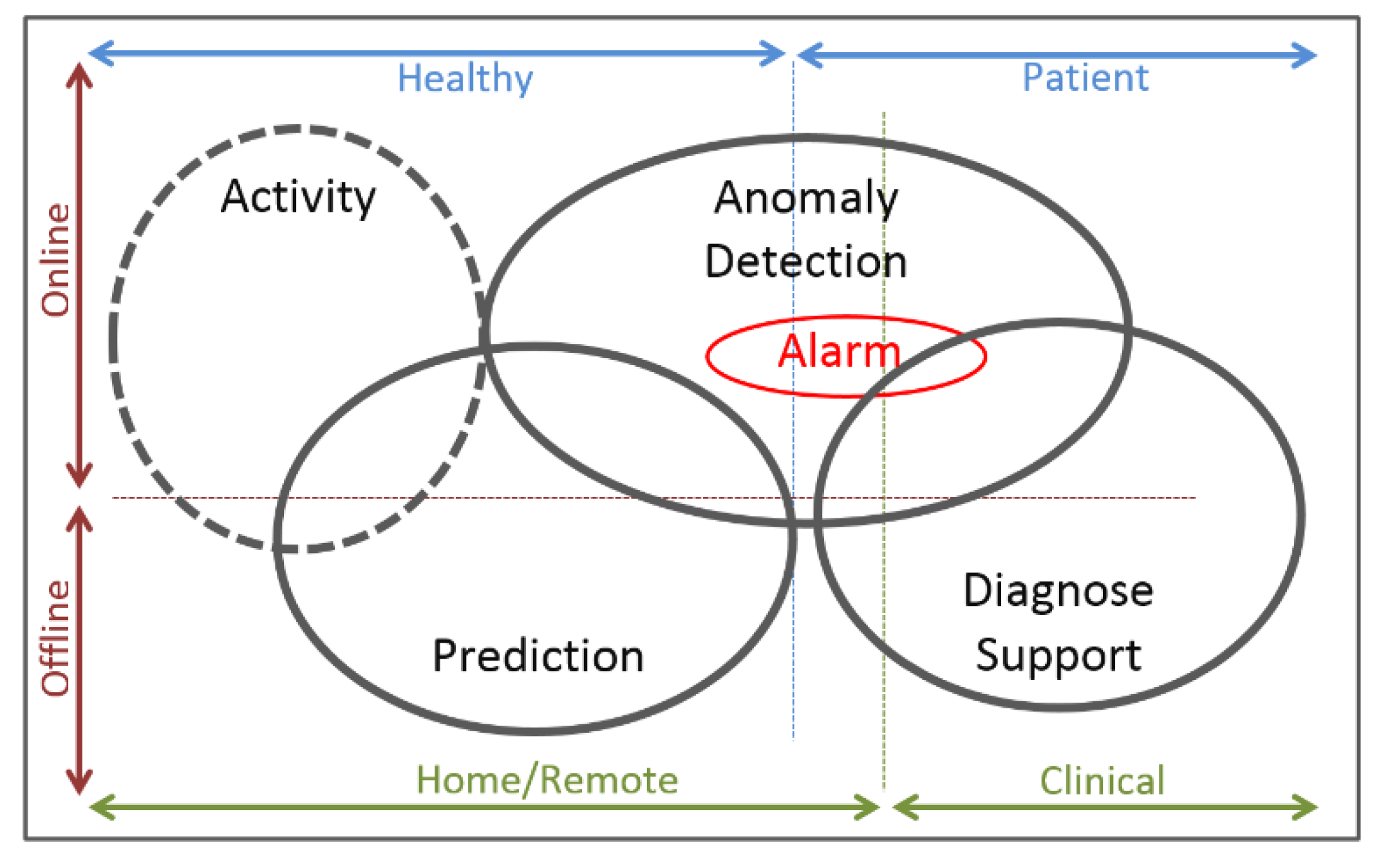
4. Wearable Health Devices Generic System Architecture
4.1. Body Area Network
4.2. Data Logger/Portable Unit
4.3. Real-Time Monitoring
4.4. Offline Monitoring
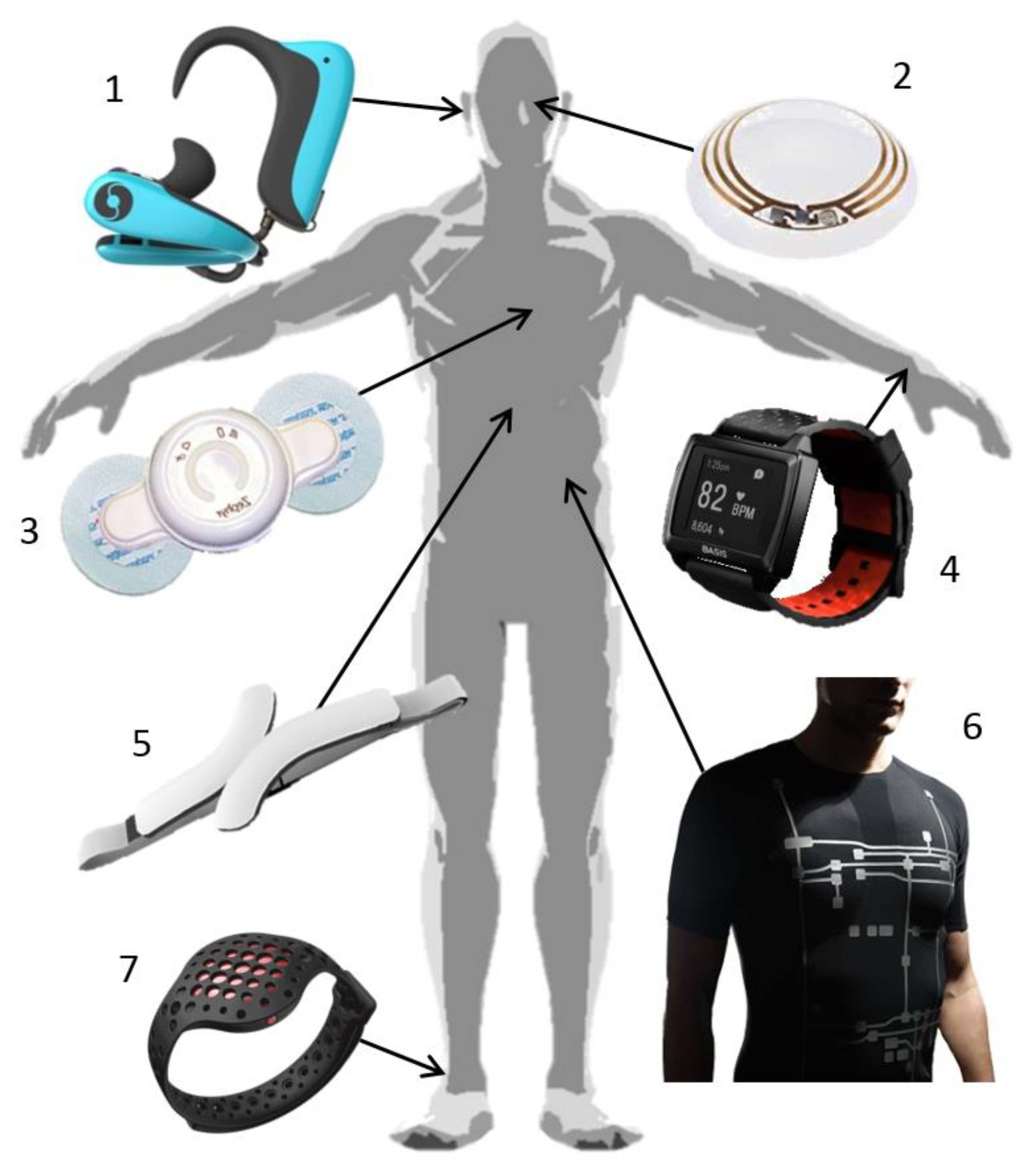
5. Wearable Health Devices—Systems
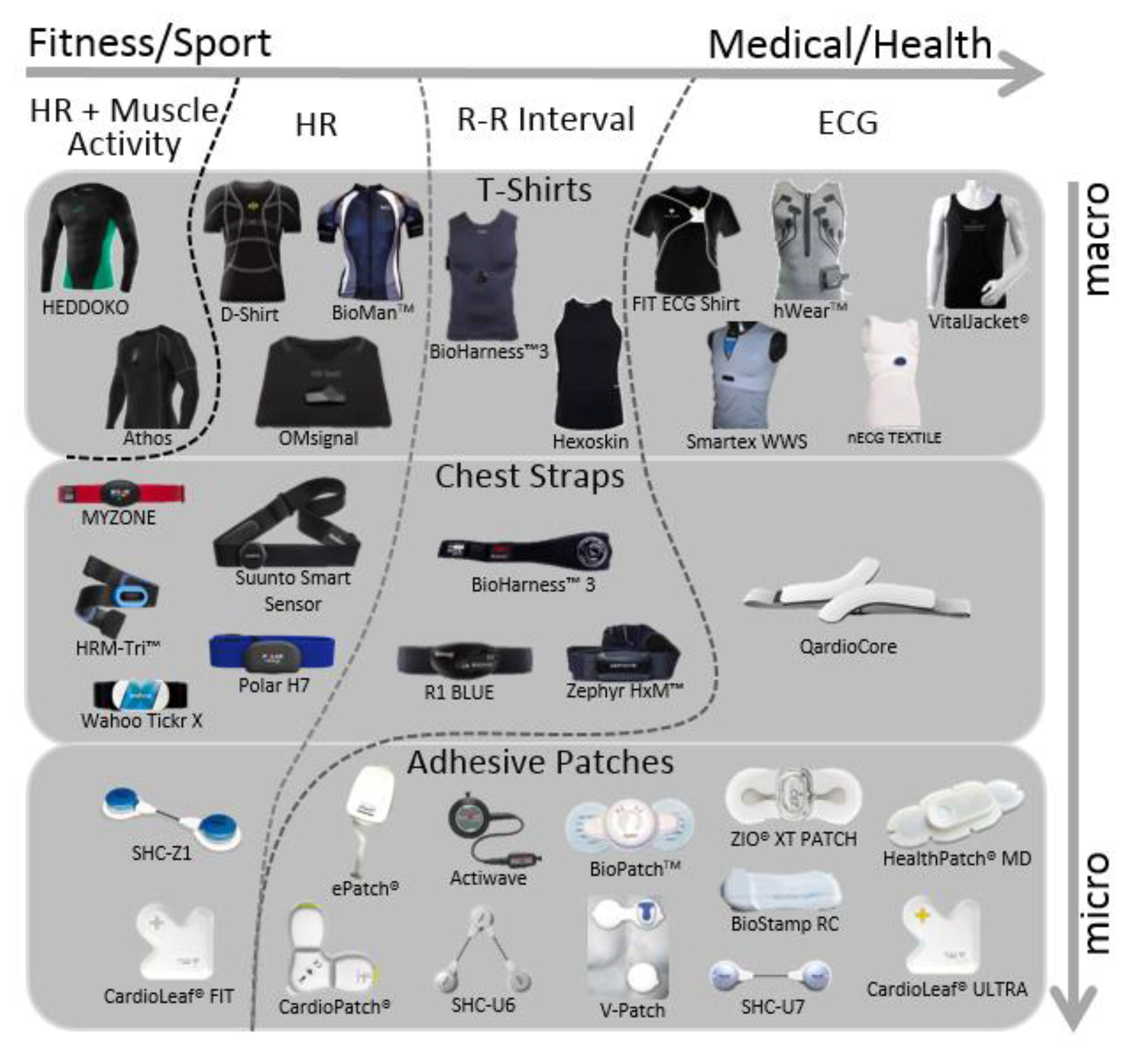
5.1. ECG T-Shirt Devices
5.2. WHDs Prototypes
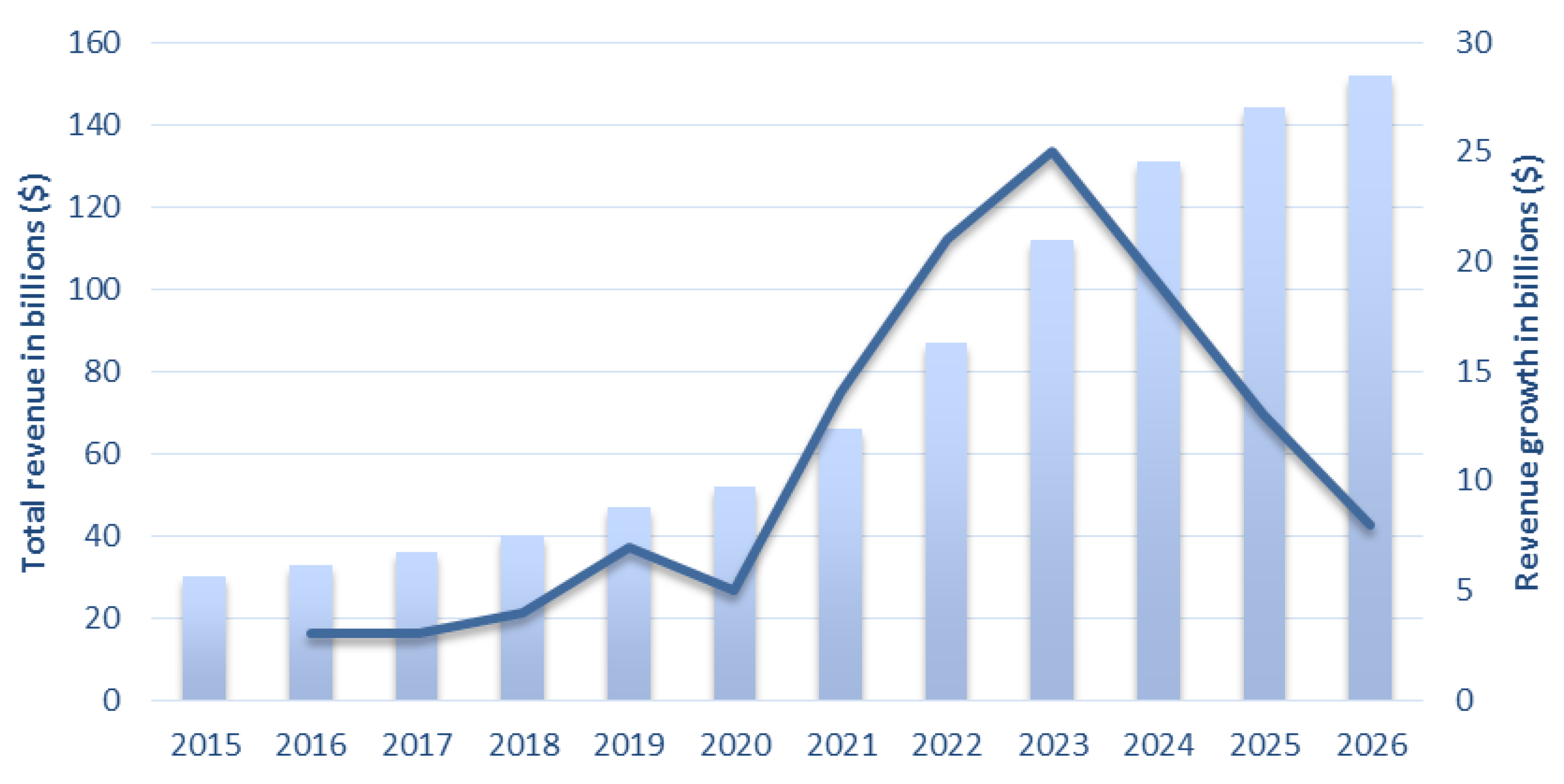
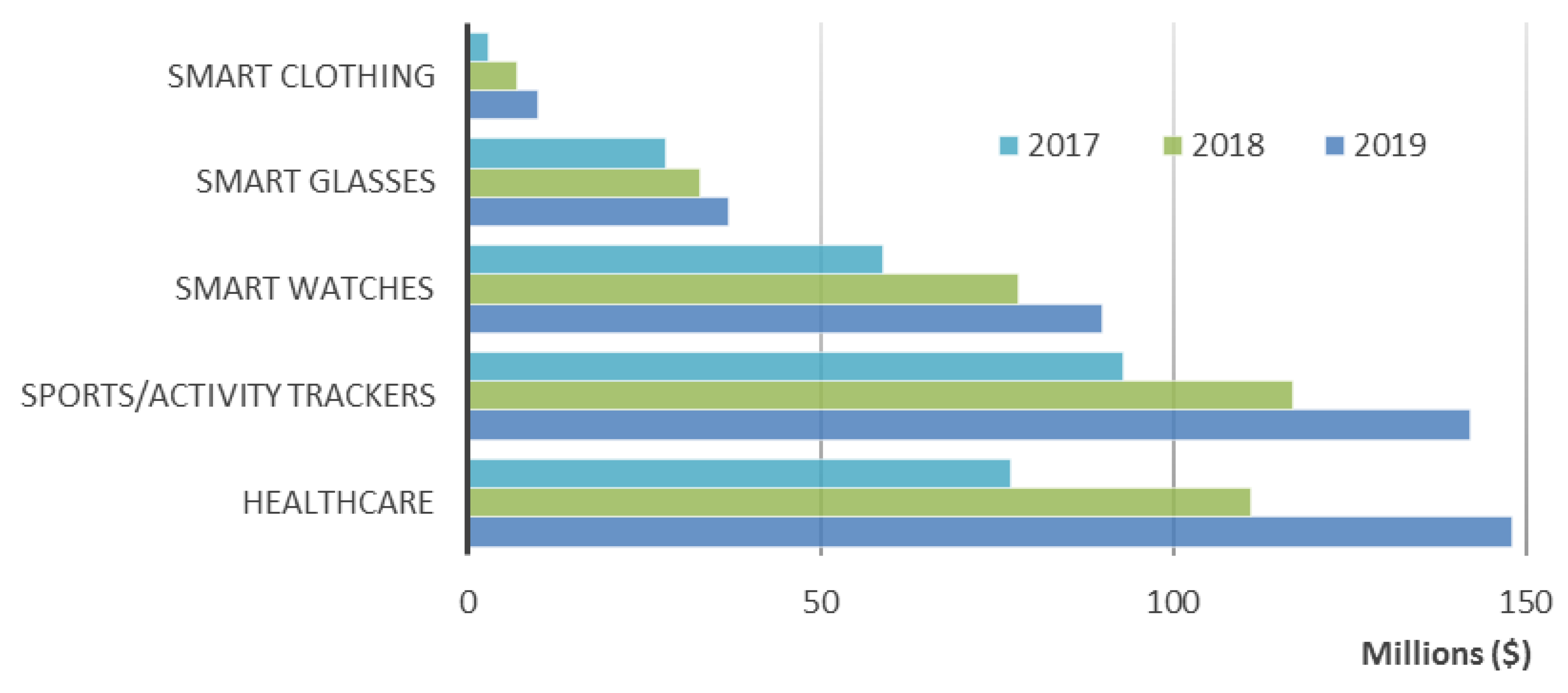
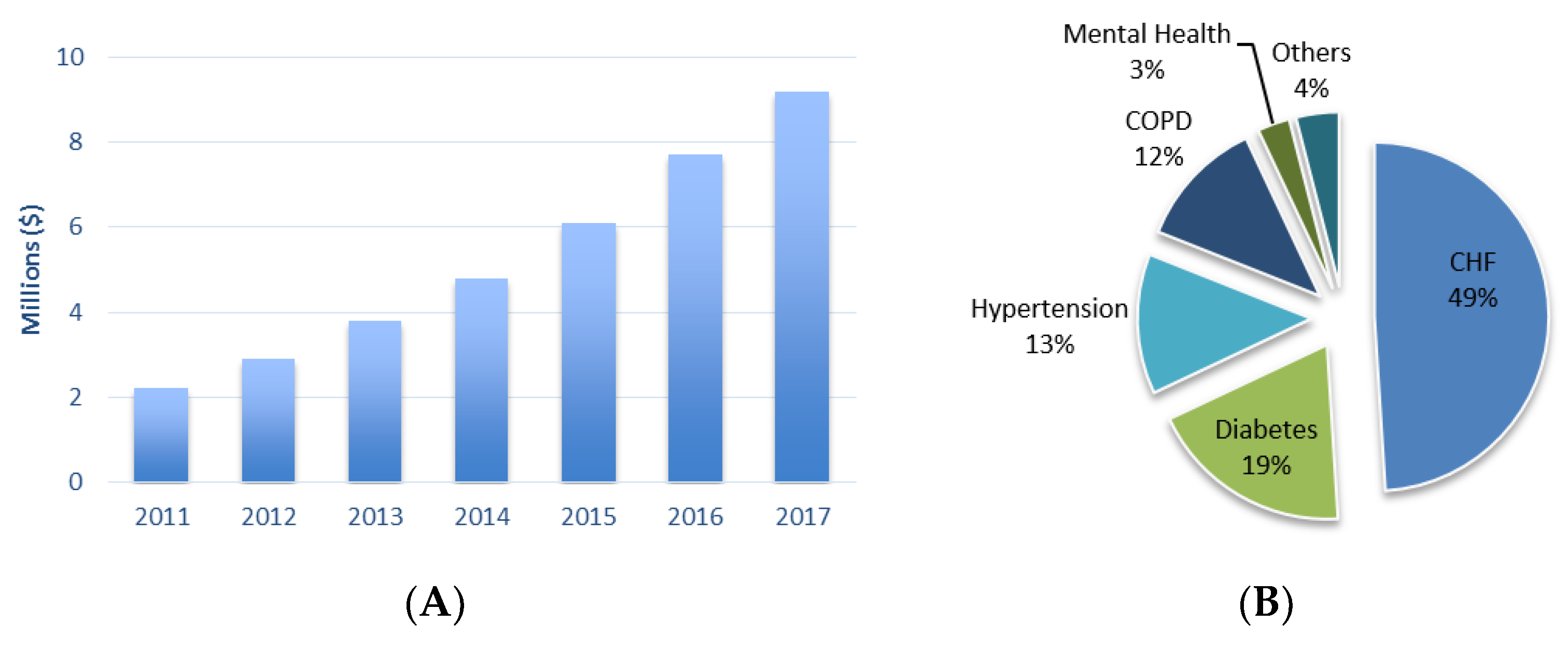
6. Wearable Health Devices Market Trends
7. Conclusions and Future Challenges
Author Contributions
Funding
Conflicts of Interest
References
- Marco Di Rienzo, G.P.; Brambilla, G.; Ferratini, M.; Castiglioni, P. MagIC System: A New Textile-BasedWearable Device for Biological Signal Monitoring. Applicability in Daily Life and Clinical Setting. In Proceedings of the 2005 IEEE, Engineering in Medicine and Biology 27th Annual Conference 2005, Shangai, China, 1–4 September 2005; pp. 7167–7169. [Google Scholar]
- Lymberis, A.G.L. Wearable health systems: From smart technologies to real applications. In Proceedings of the Annual International Conference of the IEEE Engineering in Medicine and Biology Society, New York, NY, USA, 30 August–3 September 2006; pp. 6789–6792. [Google Scholar]
- Rita Paradiso, G.L.; Taccini, N. A Wearable Health Care System Based on Knitted Integrated Sensors. IEEE Trans. Inf. Technol. Biomed. 2005, 9, 337–344. [Google Scholar] [CrossRef] [PubMed]
- Seoane, F.; Mohino-Herranz, I.; Ferreira, J.; Alvarez, L.; Buendia, R.; Ayllon, D.; Llerena, C.; Gil-Pita, R. Wearable biomedical measurement systems for assessment of mental stress of combatants in real time. Sensors 2014, 14, 7120–7141. [Google Scholar] [CrossRef] [PubMed]
- Yilmaz, T.; Foster, R.; Hao, Y. Detecting vital signs with wearable wireless sensors. Sensors 2010, 10, 10837–10862. [Google Scholar] [CrossRef] [PubMed]
- Statista, B.I. Wearable Device Sales Revenue Worldwide from 2016 to 2022 (in Billion U.S.Dollars); Statista Inc.: New York, NY, USA, 2017. [Google Scholar]
- Yussuff, V.; Sanderson, R. The World Market for Wireless Charging in Wearable Technology; IHS: Englewood, CO, USA, 2014. [Google Scholar]
- Khan, Y.; Ostfeld, A.E.; Lochner, C.M.; Pierre, A.; Arias, A.C. Monitoring of vital signs with flexible and wearable medical devices. Adv. Mater. 2016, 28, 4373–4395. [Google Scholar] [CrossRef] [PubMed]
- Majumder, S.; Mondal, T.; Deen, M.J. Wearable sensors for remote health monitoring. Sensors 2017, 17, 130. [Google Scholar] [CrossRef] [PubMed]
- Pantelopoulos, A.; Bourbakis, N.G. A Survey on Wearable Sensor-Based Systems for Health Monitoring and Prognosis. IEEE Trans. Syst. Man Cybern. Part C Appl. Rev. 2010, 40, 1–12. [Google Scholar] [CrossRef]
- Banaee, H.; Ahmed, M.U.; Loutfi, A. Data mining for wearable sensors in health monitoring systems: A review of recent trends and challenges. Sensors 2013, 13, 17472–17500. [Google Scholar] [CrossRef] [PubMed]
- Ahrens, T. The most important vital signs are not being measured. Aust. Crit Care 2008, 21, 3–5. [Google Scholar] [CrossRef] [PubMed]
- Elliott, M.C.A. Critical care: The eight vital signs of patient monitoring. Br. J. Nurs. 2012, 21, 621–625. [Google Scholar] [CrossRef] [PubMed]
- Xu, P.J.; Zhang, H.; Tao, X.M. Textile-structured electrodes for electrocardiogram. Text. Prog. 2008, 40, 183–213. [Google Scholar] [CrossRef]
- Chan, M.; Esteve, D.; Fourniols, J.Y.; Escriba, C.; Campo, E. Smart wearable systems: Current status and future challenges. Artif. Intell. Med. 2012, 56, 137–156. [Google Scholar] [CrossRef] [PubMed]
- Appelboom, G.; Camacho, E.; Abraham, M.E.; Bruce, S.S.; Dumont, E.L.; Zacharia, B.E.; D’Amico, R.; Slomian, J.; Reginster, J.Y.; Bruyere, O.; et al. Smart wearable body sensors for patient self-assessment and monitoring. Arch. Public Health 2014, 72, 28. [Google Scholar] [CrossRef] [PubMed]
- Saritha, C.; Sukanya, V.; Murthy, Y.N. ECG Signal Analysis Using Wavelet Transforms. Bulg. J. Phys. 2008, 35, 68–77. [Google Scholar]
- Luo, N.; Ding, J.; Zhao, N.; Leung, B.H.K.; Poon, C.C.Y. Mobile Health: Design of Flexible and Stretchable Electrophysiological Sensors for Wearable Healthcare Systems. In Proceedings of the 2014 11th International Conference on Wearable and Implantable Body Sensor Networks, Zurich, Switzerland, 16–19 June 2014; pp. 87–91. [Google Scholar] [CrossRef]
- Giovangrandi, L.; Inan, O.T.; Banerjee, D.; Kovacs, G.T. Preliminary results from BCG and ECG measurements in the heart failure clinic. In Proceedings of the 2012 Annual International Conference of the IEEE Engineering in Medicine and Biology Society, San Diego, CA, USA, 28 August–1 September 2012; pp. 3780–3783. [Google Scholar]
- Syduzzaman, M.; Patwary, S.U.; Farhana, K.; Ahmed, S. Smart textiles and nano-technology: A general overview. J. Text. Sci. Eng. 2015, 5, 1000181. [Google Scholar]
- Aleksandrowicz, A.; Leonhardt, S. Wireless and non-contact ECG measurement system—The “Aachen SmartChair”. Acta Polytech. 2007, 47, 4–5. [Google Scholar]
- Aarts, V.; Dellimore, K.H.; Wijshoff, R.; Derkx, R.; Laar, J.V.D.; Muehlsteff, J. Performance of an accelerometer-based pulse presence detection approach compared to a reference sensor. In Proceedings of the 14th Annual Body Sensor Networks Conference, Eindhoven, The Netherlands, 9–12 May 2017; pp. 165–168. [Google Scholar]
- Xiao-Fei, T.; Yuan-Ting, Z.; Poon, C.C.Y.; Bonato, P. Wearable Medical Systems for p-Health. IEEE Rev. Biomed. Eng. 2008, 1, 62–74. [Google Scholar] [CrossRef] [PubMed]
- Turner, J.R.; Viera, A.J.; Shimbo, D. Ambulatory blood pressure monitoring in clinical practice: A review. Am. J. Med. 2015, 128, 14–20. [Google Scholar] [CrossRef] [PubMed]
- Puke, S.; Suzuki, T.; Nakayama, K.; Tanaka, H.; Minami, S. Blood pressure estimation from pulse wave velocity measured on the chest. In Proceedings of the 2013 35th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Osaka, Japan, 3–7 July 2013; pp. 6107–6110. [Google Scholar]
- Yu-Pin, H.; Young, D.J. Skin-Coupled Personal Wearable Ambulatory Pulse Wave Velocity Monitoring System Using Microelectromechanical Sensors. IEEE Sens. J. 2014, 14, 3490–3497. [Google Scholar]
- Woo, S.H.; Choi, Y.Y.; Kim, D.J.; Bien, F.; Kim, J.J. Tissue-informative mechanism for wearable non-invasive continuous blood pressure monitoring. Sci. Rep. 2014, 4, 6618. [Google Scholar] [CrossRef] [PubMed]
- Guo, L.; Berglin, L.; Wiklund, U.; Mattila, H. Design of a garment-based sensing system for breathing monitoring. Text. Res. J. 2012, 83, 499–509. [Google Scholar] [CrossRef]
- Gandis, G.; Mazeika, M.; Rick Swanson, R. CRTT. Respiratory Inductance Plethysmography an Introduction. Available online: http://www.pro-tech.com/ (accessed on 5 June 2017).
- Anmin, J.; Bin, Y.; Morren, G.; Duric, H.; Aarts, R.M. Performance evaluation of a tri-axial accelerometry-based respiration monitoring for ambient assisted living. In Proceedings of the Engineering in Medicine and Biology Society, Minneapolis, MN, USA, 3–6 September 2009; pp. 5677–5680. [Google Scholar]
- Sharma, H.; Sharma, K.K.; Bhagat, O.L. Respiratory rate extraction from single-lead ECG using homomorphic filtering. Comput. Biol. Med. 2015, 59, 80–86. [Google Scholar] [CrossRef] [PubMed]
- Addison, P.S.; Watson, J.N.; Mestek, M.L.; Ochs, J.P.; Uribe, A.A.; Bergese, S.D. Pulse oximetry-derived respiratory rate in general care floor patients. J. Clin. Monit. Comput. 2015, 29, 113–120. [Google Scholar] [CrossRef] [PubMed]
- Chiu, Y.-Y.; Lin, W.-Y.; Wang, H.-Y.; Huang, S.-B.; Wu, M.-H. Development of a piezoelectric polyvinylidene fluoride (PVDF) polymer-based sensor patch for simultaneous heartbeat and respiration monitoring. Sens. Actuators A Phys. 2013, 189, 328–334. [Google Scholar] [CrossRef]
- Krehel, M.; Schmid, M.; Rossi, R.M.; Boesel, L.F.; Bona, G.L.; Scherer, L.J. An optical fibre-based sensor for respiratory monitoring. Sensors 2014, 14, 13088–13101. [Google Scholar] [CrossRef] [PubMed]
- AL-Khalidi, F.Q.; Saatchi, R.; Burke, D.; Elphick, H.; Tan, S. Respiration rate monitoring methods: A review. Pediat. Pulmonol. 2011, 46, 523–529. [Google Scholar] [CrossRef] [PubMed]
- Tognarelli, S.L.D.; Cecchi, F.; Scaramuzzo, R.; Cuttano, A.; Laschi, C.; Menciassi, A.; Dario, P. Analysis of a dielectric EAP as smart component for a neonatal respiratory simulator. In Proceedings of the 35th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Osaka, Japan, 3–7 July 2013; pp. 457–460. [Google Scholar]
- Guo, X.; Huang, Y.; Zhao, Y.; Mao, L.; Gao, L.; Pan, W.; Zhang, Y.; Liu, P. Highly stretchable strain sensor based on SWCNTs/CB synergistic conductive network for wearable human-activity monitoring and recognition. Smart Mater. Struct. 2017, 26, 095017. [Google Scholar] [CrossRef]
- Tamura, T.; Maeda, Y.; Sekine, M.; Yoshida, M. Wearable Photoplethysmographic Sensors—Past and Present. Electronics 2014, 3, 282–302. [Google Scholar] [CrossRef]
- Dias, D.; Ferreira, N.; Cunha, J.P.S. VitalLogger: An adaptable wearable physiology and body-area ambiance data logger for mobile applications. In Proceedings of the 2017 IEEE 14th International Conference on Wearable and Implantable Body Sensor Networks (BSN), Eindhoven, The Netherlands, 9–12 May 2017; pp. 71–74. [Google Scholar]
- Sola, J.; Castoldi, S.; Chetelat, O. SpO2 Sensor Embedded in a Finger Ring: Desing and implementation. In Proceedings of the 2006 International Conference of the IEEE Engineering in Medicine and Biology Society, New York, NY, USA, 30 August–3 September 2006; pp. 4495–4498. [Google Scholar]
- Mendelson, Y.; Dao, D.K.; Chon, K.H. Multi-channel pulse oximetry for wearable physiological monitoring. In Proceedings of the 2013 IEEE International Conference on Body Sensor Networks (BSN), MA, USA, USA, 6–9 May 2013; pp. 1–6. [Google Scholar]
- Chen, C.-M.; Kwasnicki, R.; Lo, B.; Yang, G.Z. Wearable Tissue Oxygenation Monitoring Sensor and a Forearm Vascular Phantom Design for Data Validation. In Proceedings of the 11th International Conference on Wearable and Implantable Body Sensor Networks, Zurich, Switzerland, 16–19 June 2014; pp. 64–68. [Google Scholar] [CrossRef]
- Zysset, C.; Nasseri, N.; Büthe, L.; Münzenrieder, N.; Kinkeldei, T.; Petti, L.; Kleiser, S.; Salvatore, G.A.; Wolf, M.; Tröster, G. Textile integrated sensors and actuators for near-infrared spectroscopy. Opt. Express 2013, 21, 3213. [Google Scholar] [CrossRef] [PubMed]
- Krehel, M.; Wolf, M.; Boesel, L.F.; Rossi, R.M.; Bona, G.L.; Scherer, L.J. Development of a luminous textile for reflective pulse oximetry measurements. Biomed. Opt. Express 2014, 5, 2537–2547. [Google Scholar] [CrossRef] [PubMed]
- Medtronic MiniMed, I. Continuous Glucose Monitoring. Available online: https://www.medtronicdiabetes.com (accessed on 7 July 2017).
- Dexcom, I. Dexcom G4 Platinum. Available online: http://www.dexcom.com/pt-PT (accessed on 7 July 2017).
- MedCityNews. FDA Approval for First Glucose Monitoring App. Available online: http://healthmanagement.org/ (accessed on 10 July 2017).
- Takahashi, M.; Heo, Y.J.; Kawanishi, T.; Okitsu, T.; Takeuchi, S. Portable continuous glucose monitoring systems with implantable fluorescent hydrogel microfibers. In Proceedings of the 2013 IEEE 26th International Conference on Micro Electro Mechanical Systems (MEMS), Taipei, Taiwan, 20–24 January 2013; pp. 1089–1092. [Google Scholar]
- Tierney, M.J.; Tamada, J.A.; Potts, R.O.; Jovanovic, L.; Garg, S. Clinical evaluation of the GlucoWatch® biographer: A continual, non-invasive glucose monitor for patients with diabetes. Biosens. Bioelectron. 2001, 16, 621–629. [Google Scholar] [CrossRef]
- So, C.F.; Choi, K.S.; Wong, T.K.; Chung, J.W. Recent advances in noninvasive glucose monitoring. Med. Devices 2012, 5, 45–52. [Google Scholar]
- Sobel, S.I.; Chomentowski, P.J.; Vyas, N.; Andre, D.; Toledo, F.G. Accuracy of a Novel Noninvasive Multisensor Technology to Estimate Glucose in Diabetic Subjects During Dynamic Conditions. J. Diabetes Sci. Technol. 2014, 8, 54–63. [Google Scholar] [CrossRef] [PubMed]
- Wieringa, F.P.; Broers, N.J.H.; Kooman, J.P.; Van der Sande, F.M.; Van Hoof, C. Wearable sensors: Can they benefit patients with chronic kidney disease? Expert Rev. Med. Devices 2017, 14, 505–519. [Google Scholar] [CrossRef] [PubMed]
- Jeehoon, K.; Sungjun, K.; Sangwon, S.; Kwangsuk, P. Highly wearable galvanic skin response sensor using flexible and conductive polymer foam. In Proceedings of the 2014 36th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Chicago, IL, USA, 26–30 August 2014; pp. 6631–6634. [Google Scholar]
- Nikolic-Popovic, J.; Goubran, R. Measuring heart rate, breathing rate and skin conductance during exercise. In Proceedings of the 2011 IEEE International Workshop on the Medical Measurements and Applications Proceedings (MeMeA), Bari, Italy, 30–31 May 2011; pp. 507–511. [Google Scholar]
- Bandodkar, A.J.; Wang, J. Non-invasive wearable electrochemical sensors: A review. Trends Biotechnol. 2014, 32, 363–371. [Google Scholar] [CrossRef] [PubMed]
- Gengchen, L.; Smith, K.; Kaya, T. Implementation of a microfluidic conductivity sensor—A potential sweat electrolyte sensing system for dehydration detection. In Proceedings of the 2014 36th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Chicago, IL, USA, 26–30 August 2014; pp. 1678–1681. [Google Scholar]
- Koh, A.; Kang, D.; Xue, Y.; Lee, S.; Pielak, R.M.; Kim, J.; Hwang, T.; Min, S.; Banks, A.; Bastien, P. A soft, wearable microfluidic device for the capture, storage, and colorimetric sensing of sweat. Sci. Transl. Med. 2016, 8, 366ra165. [Google Scholar] [CrossRef] [PubMed]
- Kodali, B.S. Capnography outside the operating rooms. Anesthesiology 2013, 118, 192–201. [Google Scholar] [CrossRef] [PubMed]
- Wac, K.; Tsiourti, C. Ambulatory Assessment of Affect: Survey of Sensor Systems for Monitoring of Autonomic Nervous Systems Activation in Emotion. IEEE Trans. Affect. Comput. 2014, 5, 251–272. [Google Scholar] [CrossRef]
- Dziewas, R.E.A. Capnography screening for sleep apnea in patients with acute stroke. Neurol. Res. 2005, 27, 83–87. [Google Scholar] [CrossRef] [PubMed]
- Ontario, O.B.R.-T.O.J.F.B.I. Braebon Taps into the Growing Sleep Apnea Market. Available online: http://www.mri.gov.on.ca/obr/2012/07/braebon-taps-into-the-growing-sleep-apnea-market/ (accessed on 5 August 2017).
- Orlikowski, D.; Prigent, H.; Ambrosi, X.; Vaugier, I.; Pottier, S.; Annane, D.; Lofaso, F.; Ogna, A. Comparison of ventilator-integrated end-tidal CO2 and transcutaneous CO2 monitoring in home-ventilated neuromuscular patients. Respir. Med. 2016, 117, 7–13. [Google Scholar] [CrossRef] [PubMed]
- Chatterjee, M.; Ge, X.; Kostov, Y.; Luu, P.; Tolosa, L.; Woo, H.; Viscardi, R.; Falk, S.; Potts, R.; Rao, G. A rate-based transcutaneous CO2 sensor for noninvasive respiration monitoring. Physiol. Meas. 2015, 36, 883. [Google Scholar] [CrossRef] [PubMed]
- Horvath, C.M.; Brutsche, M.H.; Baty, F.; Rüdiger, J.J. Transcutaneous versus blood carbon dioxide monitoring during acute noninvasive ventilation in the emergency department—A retrospective analysis. Swiss Med. Wkly. 2016, 146, w14373. [Google Scholar] [CrossRef] [PubMed]
- Gaura, E.; Kemp, J.; Brusey, J. Leveraging knowledge from physiological data: On-body heat stress risk prediction with sensor networks. IEEE Trans. Biomed. Circuits Syst. 2013, 7, 861–879. [Google Scholar] [CrossRef] [PubMed]
- Buller, M.J.; Tharion, W.J.; Hoyt, R.W.; Jenkins, O.C. Estimation of human internal temperature from wearable physiological sensors. In Proceedings of the Twenty-Second Innovative Applications of Artificial Intelligence Conference (IAAI-10), Atlanta, GA, USA, 11–15 July 2010. [Google Scholar]
- Buller, M.J.; Tharion, W.J.; Cheuvront, S.N.; Montain, S.J.; Kenefick, R.W.; Castellani, J.; Latzka, W.A.; Roberts, W.S.; Richter, M.; Jenkins, O.C.; et al. Estimation of human core temperature from sequential heart rate observations. Physiol. Meas. 2013, 34, 781. [Google Scholar] [CrossRef] [PubMed]
- Popovic, Z.; Momenroodaki, P.; Scheeler, R. Toward wearable wireless thermometers for internal body temperature measurements. IEEE Commun. Mag. 2014, 52, 118–125. [Google Scholar] [CrossRef]
- Boano, C.A.; Lasagni, M.; Romer, K.; Lange, T. Accurate Temperature Measurements for Medical Research Using Body Sensor Networks. In Proceedings of the 2011 14th IEEE International Symposium on Object/Component/Service-Oriented Real-Time Distributed Computing Workshops, Newport Beach, CA, USA, 28–31 March 2011; pp. 189–198. [Google Scholar] [CrossRef]
- Webb, R.C.; Bonifas, A.P.; Behnaz, A.; Zhang, Y.; Yu, K.J.; Cheng, H.; Shi, M.; Bian, Z.; Liu, Z.; Kim, Y.S.; et al. Ultrathin conformal devices for precise and continuous thermal characterization of human skin. Nat. Mater. 2013, 12, 938–944. [Google Scholar] [CrossRef] [PubMed]
- Miozzi, C.; Amendola, S.; Bergamini, A.; Marrocco, G. Reliability of a Re-usable Wireless Epidermal Temperature Sensor in Real Conditions. In Proceedings of the 14th Annual Body Sensor Networks Conference, Eindhoven, The Netherlands, 9–12 May 2017; pp. 95–98. [Google Scholar]
- Looney, D.P.; Buller, M.J.; Gribok, A.V.; Leger, J.L.; Potter, A.W.; Rumpler, W.V.; Tharion, W.J.; Welles, A.P.; Friedl, K.E.; Hoyt, R.W. Estimating Resting Core Temperature Using Heart Rate. J. Meas. Phys. Behav. 2018, 20, 1–7. [Google Scholar] [CrossRef]
- Xu, X.; Karis, A.J.; Buller, M.J.; Santee, W.R. Relationship between core temperature, skin temperature, and heat flux during exercise in heat. Eur. J. Appl. Physiol. 2013, 113, 2381–2389. [Google Scholar] [CrossRef] [PubMed]
- Maglott, J.C.; Xu, J.; Shull, P.B. Differences in Arm Motion Timing Characteristics for Basketball Free Throw and Jump Shooting via a Body-worn Sensorized Sleeve. In Proceedings of the 14th Annual Body Sensor Networks Conference, Eindhoven, The Netherlands, 9–12 May 2017; pp. 31–34. [Google Scholar]
- Buckley, C.; Reilly, M.A.O.; Whelan, D.; Farrell, A.V.; Clark, L.; Longo, V.; Gilchrist, M.D.; Caulfield, B. Binary Classification of Running Fatigue using a Single Inertial Measurement Unit. In Proceedings of the 14th Annual Body Sensor Networks Conference, Eindhoven, The Netherlands, 9–12 May 2017; pp. 197–201. [Google Scholar]
- Lacirignola, J.; Weston, C.; Byrd, K.; Metzger, E.; Singh, N.; Davis, S.; Maurer, D.; Young, W.; Collins, P.; Balcius, J.; et al. Instrumented Footwear Inserts: A New Tool For Measuring Forces and Biomechanical State Changes During Dynamic Movements. In Proceedings of the 14th Annual Body Sensor Networks Conference, Eindhoven, The Netherlands, 9–12 May 2017. [Google Scholar]
- Mohammed, S.; Tashev, I. Unsupervised Deep Representation Learning to Remove Motion Artifacts in Free-mode Body Sensor Networks. In Proceedings of the 14th Annual Body Sensor Networks Conference, Eindhoven, The Netherlands, 9–12 May 2017; pp. 182–188. [Google Scholar]
- Lazarus, A. Remote, wireless, ambulatory monitoring of implantable pacemakers, cardioverter defibrillators, and cardiac resynchronization therapy systems: Analysis of a worldwide database. Pac. Clin. Electrophysiol. 2007, 30, S2–S12. [Google Scholar] [CrossRef] [PubMed]
- Jin, M.; Zou, H.; Weekly, K.; Jia, R.; Bayen, A.M.; Spanos, C.J. Environmental sensing by wearable device for indoor activity and location estimation. In Proceedings of the 40th Annual Conference of the IEEE Industrial Electronics Society, Dallas, TX, USA, 29 October–1 November 2014. [Google Scholar] [CrossRef]
- Ambulatory Monitoring, I. Application Areas. Available online: http://www.ambulatory-monitoring.com/environmental.html (accessed on 18 May 2017).
- Custodio, V.; Herrera, F.J.; Lopez, G.; Moreno, J.I. A review on architectures and communications technologies for wearable health-monitoring systems. Sensors 2012, 12, 13907–13946. [Google Scholar] [CrossRef] [PubMed]
- Khan, Z.A.; Sivakumar, S.; Phillips, W.; Robertson, B. ZEQoS: A New Energy and QoS-Aware Routing Protocol for Communication of Sensor Devices in Healthcare System. Int. J. Distrib. Sens. Netw. 2014, 2014, 1–18. [Google Scholar] [CrossRef]
- Tennina, S.; Di Renzo, M.; Kartsakli, E.; Graziosi, F.; Lalos, A.S.; Antonopoulos, A.; Mekikis, P.V.; Alonso, L. WSN4QoL: A WSN-Oriented Healthcare System Architecture. Int. J. Distrib. Sens. Netw. 2014, 10, 503417. [Google Scholar] [CrossRef]
- Cunha, J.P.S.; Cunha, B.; Pereira, A.S.; Xavier, W.; Ferreira, N.; Meireles, L. Vital-Jacket®: A wearable wireless vital signs monitor for patients’ mobility in cardiology and sports. In Proceedings of the 2010 4th International Conference on Pervasive Computing Technologies for Healthcare, Munich, Germany, 22–25 March 2010; pp. 1–2. [Google Scholar]
- Kharel, J.; Reda, H.T.; Shin, S.Y. Fog Computing-Based Smart Health Monitoring System Deploying LoRa Wireless Communication. IETE Tech. Rev. 2018, 1–14. [Google Scholar] [CrossRef]
- Asensio, A.; Marco, A.; Blasco, R.; Casas, R. Protocol and architecture to bring things into internet of things. Int. J. Distrib. Sens. Netw. 2014. [Google Scholar] [CrossRef]
- Belle, A.; Thiagarajan, R.; Soroushmehr, S.; Navidi, F.; Beard, D.A.; Najarian, K. Big data analytics in healthcare. BioMed Res. Int. 2015, 2015, 370194. [Google Scholar] [CrossRef] [PubMed]
- Rifat Shahriyar, M.F.B.; Kundu, G.; Ahamed, S.I.; Akbar, M. Intelligent Mobile Health Monitoring System (IMHMS). Int. J. Control Autom. 2009, 2, 13–28. [Google Scholar]
- Lukowicz, P.; Anliker, U.; Ward, J.; Troster, G.; Hirt, E.; Neufelt, C. AMON: A wearable medical computer for high risk patients. In Proceedings of the Sixth International Symposium on Wearable Computers, Seattle, WA, USA, 10 October 2002; pp. 133–134. [Google Scholar]
- Bieber, G.; Haescher, M.; Vahl, M. Sensor requirements for activity recognition on smart watches. In Proceedings of the Proceedings of the 6th International Conference on PErvasive Technologies Related to Assistive Environments, Rhodes, Greece, 29–31 May 2013. [Google Scholar] [CrossRef]
- Withings—Inspire Health. Pulse Oₓ—Track. Improve. Available online: http://www.withings.com/eu/withings-pulse.html (accessed on 15 April 2017).
- BASIS. PEAK—The Ultimate Fitness and Sleep Tracker. Available online: https://www.mybasis.com/ (accessed on 15 April 2017).
- ™ M. MOOV NOW™. Available online: http://welcome.moov.cc/ (accessed on 15 April 2017).
- Biodevices, S.A. VitalJacket®. Available online: http://www.vitaljacket.com/ (accessed on 15 April 2017).
- Zephyr Performance Systems. BioHarness™ 3. Available online: http://www.zephyranywhere.com/products/bioharness-3 (accessed on 15 April 2017).
- Qardio Inc. QARDIOCORE. Available online: www.getqardio.com (accessed on 15 April 2017).
- Frank, M. Your Head Is Better for Sensors than Your Wrist; Outside-Live Bravely: Santa Fe, NM, USA, 2015. [Google Scholar]
- Andreoni, G.; Standoli, C.E.; Perego, P. Defining requirements and related methods for designing sensorized garments. Sensors 2016, 16, 769. [Google Scholar] [CrossRef] [PubMed]
- Athos. Meet Athos. Available online: https://www.liveathos.com/ (accessed on 22 April 2017).
- OM Signal Inc. OM Smart Shirt. Available online: http://omsignal.com (accessed on 22 April 2017).
- Cityzen Sciences. D-Shirt. Available online: http://www.cityzensciences.fr/en/ (accessed on 23 April 2017).
- AiQ Smart Clothing. Bioman. Available online: http://www.aiqsmartclothing.com/ (accessed on 23 April 2017).
- Hexoskin. Available online: http://www.hexoskin.com/ (accessed on 22 April 2017).
- Clearbridge Vitalsigns Pte Ltd. CardioLeaf® FIT Shirt. Available online: http://www.clearbridgevitalsigns.com/ (accessed on 24 April 2017).
- Vivonoetics. Smartex WWS. Available online: http://vivonoetics.com/ (accessed on 21 April 2017).
- Nuubo—Wearable Medical Technologies. Available online: http://www.nuubo.com/ (accessed on 21 April 2017).
- HealthWatch Technologies Ltd. Available online: http://www.personal-healthwatch.com/ (accessed on 23 April 2017).
- MYZONE. Available online: http://www.myzone.org/ (accessed on 24 April 2017).
- SUUNTO. SUUNTO SMART SENSOR. Available online: https://www.suunto.com (accessed on 24 April 2017).
- Wahoo Fitness. Wahoo Tickr. Available online: http://eu.wahoofitness.com/devices/hr (accessed on 24 April 2017).
- © Polar Electro 2016. H7 Heart Rate Sensor. Available online: www.polar.com (accessed on 24 April 2017).
- Garmin Ltd. HRM-Tri™. Available online: https://buy.garmin.com (accessed on 23 April 2017).
- Zephyr Technology Corp. Available online: http://zephyranywhere.com/ (accessed on 24 April 2017).
- SIGMA SPORT. Bluetooth® SMART Chest Belt. Available online: http://sigmasport.com (accessed on 24 April 2017).
- Solmitech. Patch-type SHC-Z1. Available online: http://www.solmitech.com/ (accessed on 25 April 2017).
- Solmitech. Patch-type SHC-U6. Available online: http://www.solmitech.com/ (accessed on 25 April 2017).
- Solmitech. Pacth-type SHC-U7. Available online: http://www.solmitech.com/ (accessed on 25 April 2017).
- Clearbridge Vitalsigns Pte Ltd. CardioLeaf FIT. Available online: http://www.clearbridgevitalsigns.com/ (accessed on 25 April 2017).
- BioTelemetry Technology ApS. The ePatch® technology. Available online: http://epatch.madebydelta.com/ (accessed on 26 April 2017).
- Vital Connect. HealthPatch® MD. Available online: http://www.vitalconnect.com/ (accessed on 26 April 2017).
- VPMS Asia Pacific. V-Patch. Available online: http://www.vpatchmedical.com/ (accessed on 26 April 2017).
- Clearbridge Vitalsigns Pte Ltd. CardioLeaf ULTRA. Available online: http://www.clearbridgevitalsigns.com/ (accessed on 25 April 2017).
- Vivonoetics. ActiWave Cardio. Available online: http://vivonoetics.com/ (accessed on 26 April 2017).
- Novosense, AB. CardioSenseSystem®. Available online: http://www.novosense.se/ (accessed on 26 April 2017).
- ZephyrTM Performance Systems. HxM. Available online: https://www.zephyranywhere.com (accessed on 24 April 2017).
- Paiva, J.S.; Rodrigues, S.; Cunha, J.P.S. Changes in ST, QT and RR ECG intervals during acute stress in firefighters: A pilot study. In Proceedings of the 2016 38th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Orlando, FL, USA, 16–20 August 2016. [Google Scholar]
- Georgia Tech Wearable Motherboard™: The Intelligent Garment for the 21st Century. Available online: http://www.gtwm.gatech.edu (accessed on 29 April 2017).
- Zhang, Z.B.; Shen, Y.H.; Wang, W.D.; Wang, B.Q.; Zheng, J.W. Design and implementation of sensing shirt for ambulatory cardiopulmonary monitoring. J. Med. Biol. Eng. 2011, 31, 207–215. [Google Scholar] [CrossRef]
- Sardini, E.; Serpelloni, M.; Ometto, M. Multi-parameters wireless shirt for physiological monitoring. In Proceedings of the 2011 IEEE International Workshop on Medical Measurements and Applications Proceedings (MeMeA), Bari, Italym, 30–31 May 2011; pp. 316–321. [Google Scholar]
- Farjadian, A.B.; Sivak, M.L.; Mavroidis, C. SQUID: Sensorized shirt with smartphone interface for exercise monitoring and home rehabilitation. In Proceedings of the 2013 IEEE International Conference on Rehabilitation Robotics (ICORR), Seattle, WA, USA, 24–26 June 2013; pp. 1–6. [Google Scholar]
- Cafagna, C.; Diterlizzi, A.; Voorhorst, F. MyWear: Customized green, safe, healthy and smart work- and sports-wear. In Proceedings of the 2014 International ICE Conference on Engineering, Technology and Innovation (ICE), Bergamo, Italy, 23–25 June 2014; pp. 1–5. [Google Scholar]
- Statista, B.I. Wearable Device Market Value from 2010 to 2018 (in Million U.S. Dollars); Statista Inc.: New York, NY, USA, 2015. [Google Scholar]
- Hayward, J.; Chansin, G.; Zervos, H. Wearable Technology 2017–2027: Markets, Players, Forecasts; IDTechEx: Cambridge, UK, 2017. [Google Scholar]
- ABI Research. Global Wearable Computing Devices; World Market, Forecast: 2013 to 2019; ABI research: New York, NY, USA, 2014. [Google Scholar]
- Statista, B.I. Smart Clothing Unit Shipments Worldwide from 2016 to 2022 (in Millions); Statista Inc.: New York, NY, USA, 2017. [Google Scholar]
- IHS Technology. World Market for Telehealth—2014 Edition; IHS Markit: London, UK, 2014. [Google Scholar]
- Berg Insight. Connected Home Medical Monitoring Devices, Million Units (World 2011–2017); Berg Insight AB: Gothenburg, Sweden, 2014. [Google Scholar]
- IHS Technology. Top Healthcare Technology Trend Predictions for 2014—IHS Medical Devices & Healthcare IT; IHS Markit: London, UK, 2014. [Google Scholar]
- Lauren Soelberg Treasure. Mhealth in the Future—Key Trends (Infographic). Available online: http://healthdecide.orcahealth.com (accessed on 15 August 2017).
- Paiva, J.S.; Dias, D.; Cunha, J.P. Beat-ID: Towards a computationally low-cost single heartbeat biometric identity check system based on electrocardiogram wave morphology. PLoS ONE 2017, 12, e0180942. [Google Scholar] [CrossRef] [PubMed]
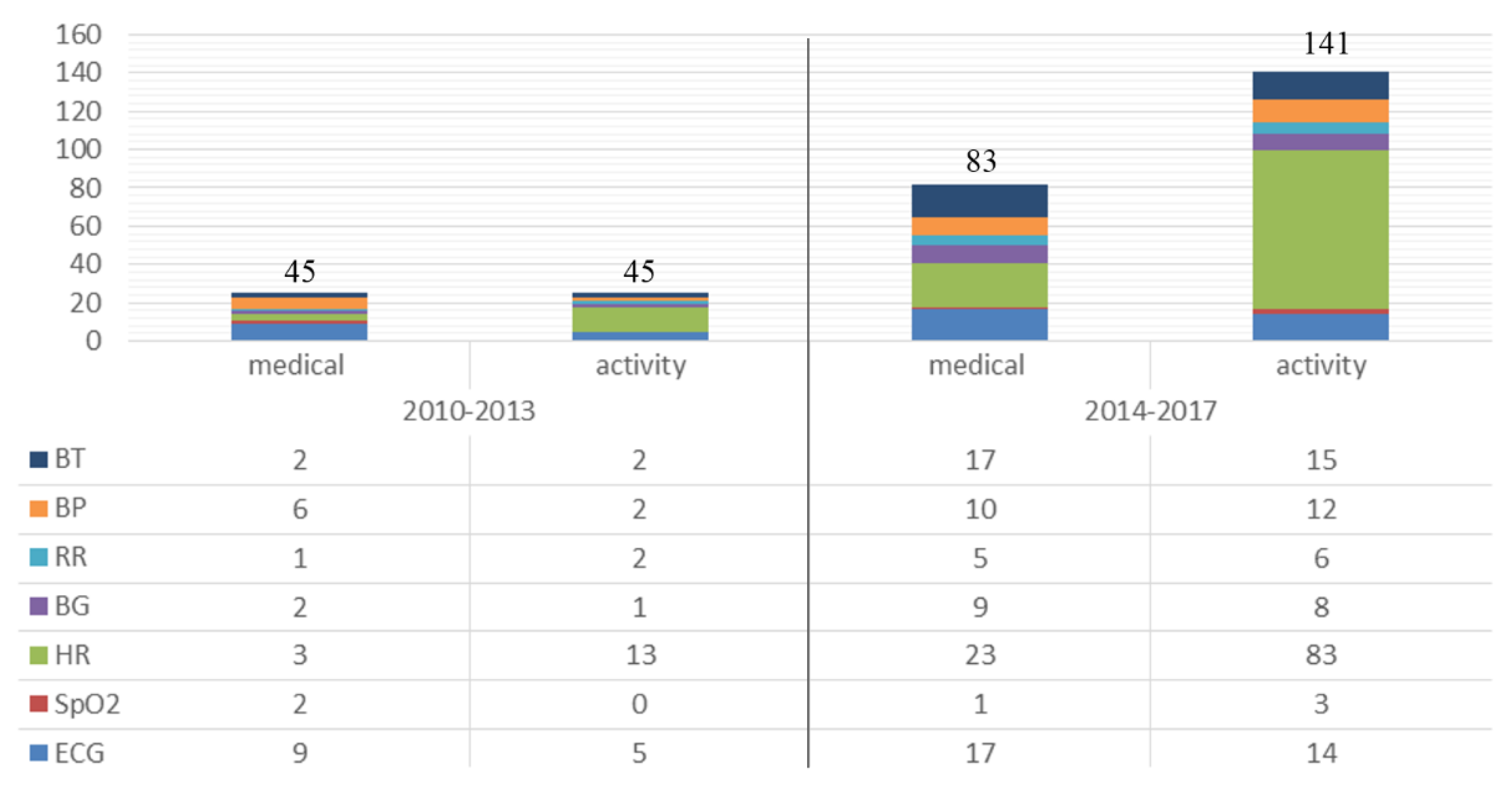
| Main Topic | Years Gaps | Purpose * | Vital Signs Words * |
|---|---|---|---|
| Wearable Device | 2010–2013; 2014–2017 | “Medical”, “Activity” | “Body Temperature”, “Blood Pressure”, “Respiration”, “Glucose”, “Heart Rate”, “oxygen saturation”, “Electrocardiogram” |
| Wireless Protocol | Max Range | Max Data Rate | Power Consumption |
|---|---|---|---|
| Bluetooth (before version 4.0) | 100 m | 1–3 Mbps | 2.5–100 mW |
| Bluetooth Low-Energy (BLE) | 100 m | 1 Mbps | 10 mW |
| Wi-Fi | 150–200 m | 54 Mbps | 1 W |
| ZigBee | 100 m | 250 kbps | 35 mW |
| LoRa | 50 km | 700 bps | (customizable) |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dias, D.; Paulo Silva Cunha, J. Wearable Health Devices—Vital Sign Monitoring, Systems and Technologies. Sensors 2018, 18, 2414. https://doi.org/10.3390/s18082414
Dias D, Paulo Silva Cunha J. Wearable Health Devices—Vital Sign Monitoring, Systems and Technologies. Sensors. 2018; 18(8):2414. https://doi.org/10.3390/s18082414
Chicago/Turabian StyleDias, Duarte, and João Paulo Silva Cunha. 2018. "Wearable Health Devices—Vital Sign Monitoring, Systems and Technologies" Sensors 18, no. 8: 2414. https://doi.org/10.3390/s18082414
APA StyleDias, D., & Paulo Silva Cunha, J. (2018). Wearable Health Devices—Vital Sign Monitoring, Systems and Technologies. Sensors, 18(8), 2414. https://doi.org/10.3390/s18082414