Dynamical Properties of Postural Control in Obese Community-Dwelling Older Adults †
Abstract
:1. Introduction
2. Materials and Methods
3. Results
3.1. Linear Measures
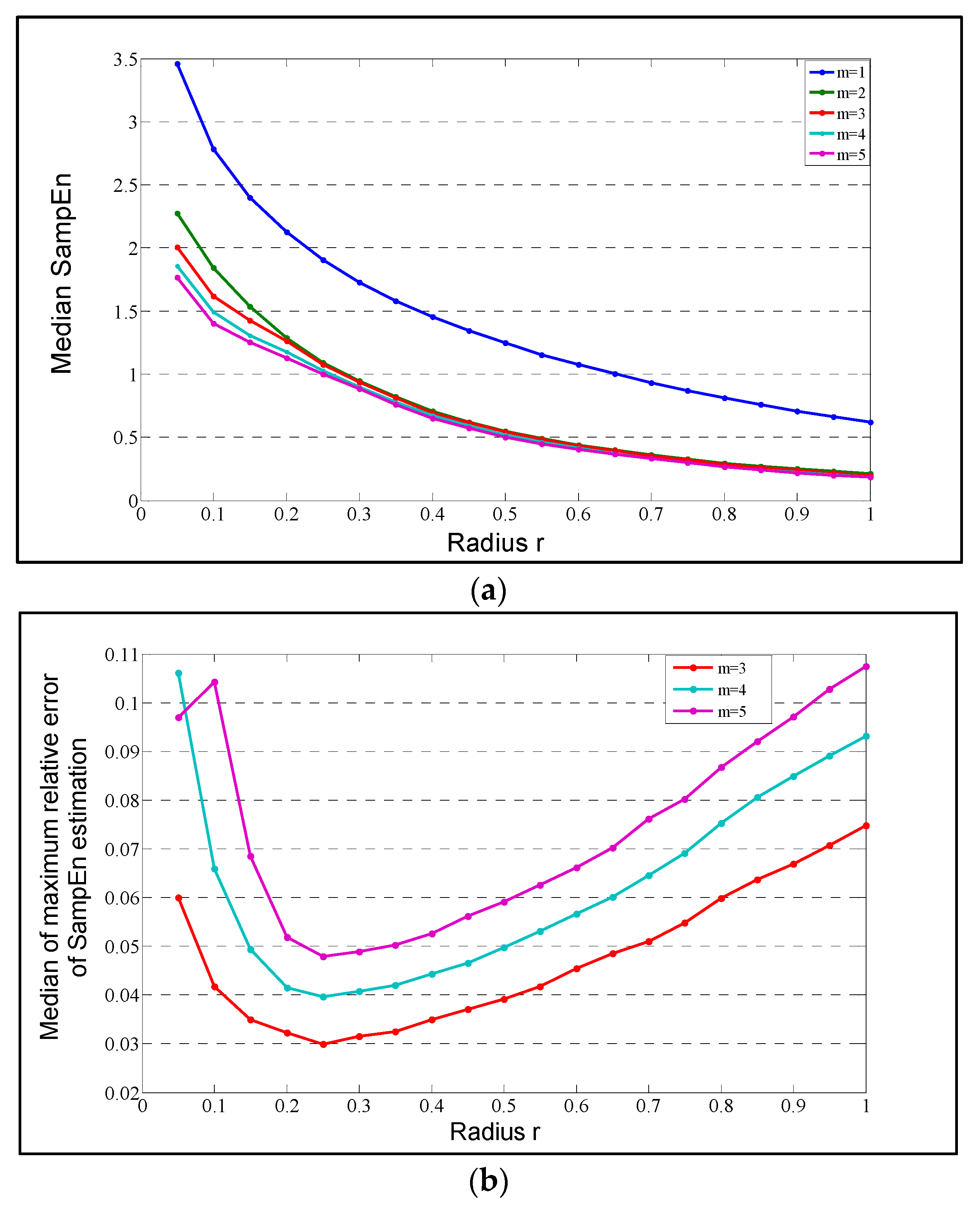
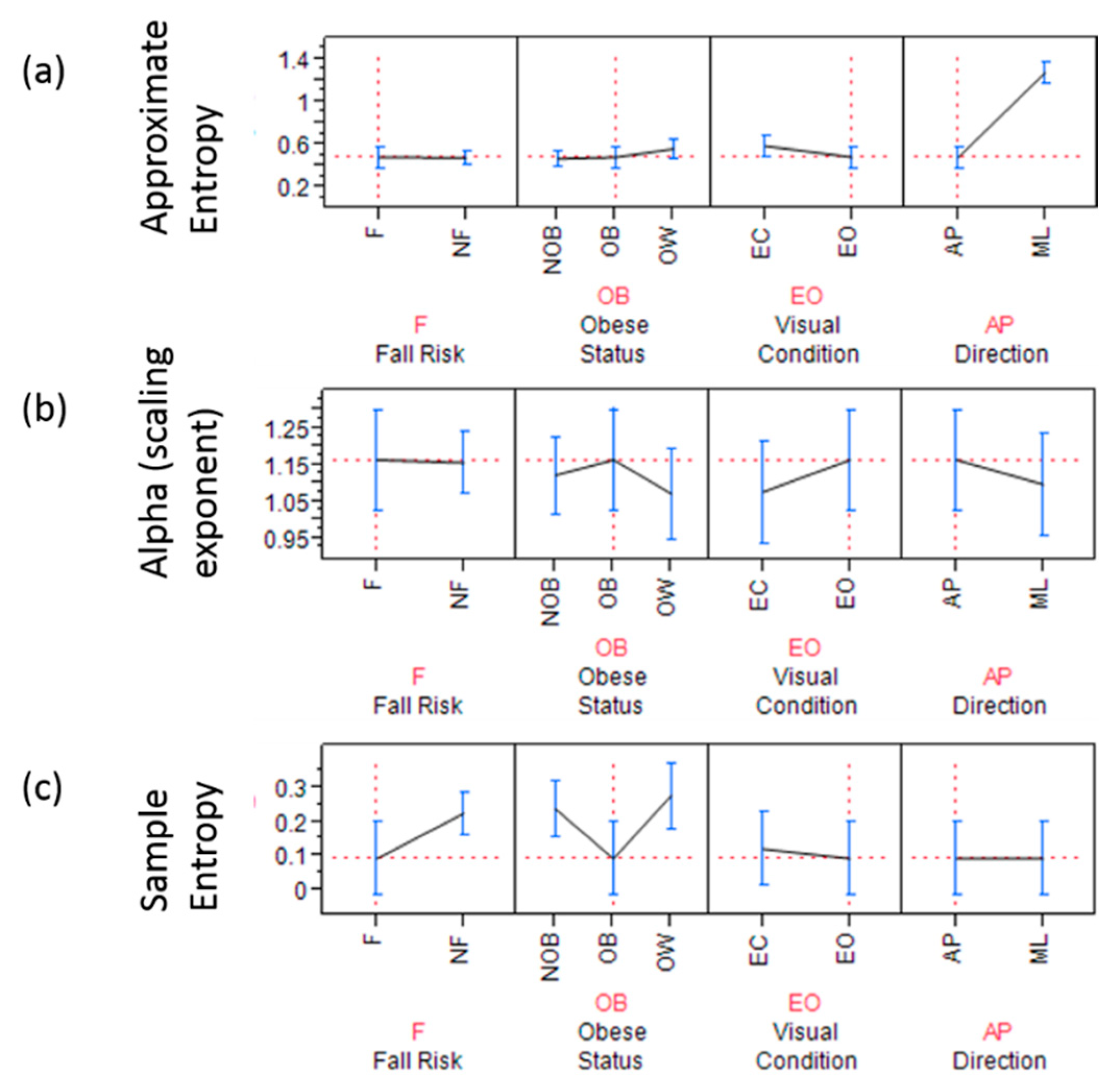
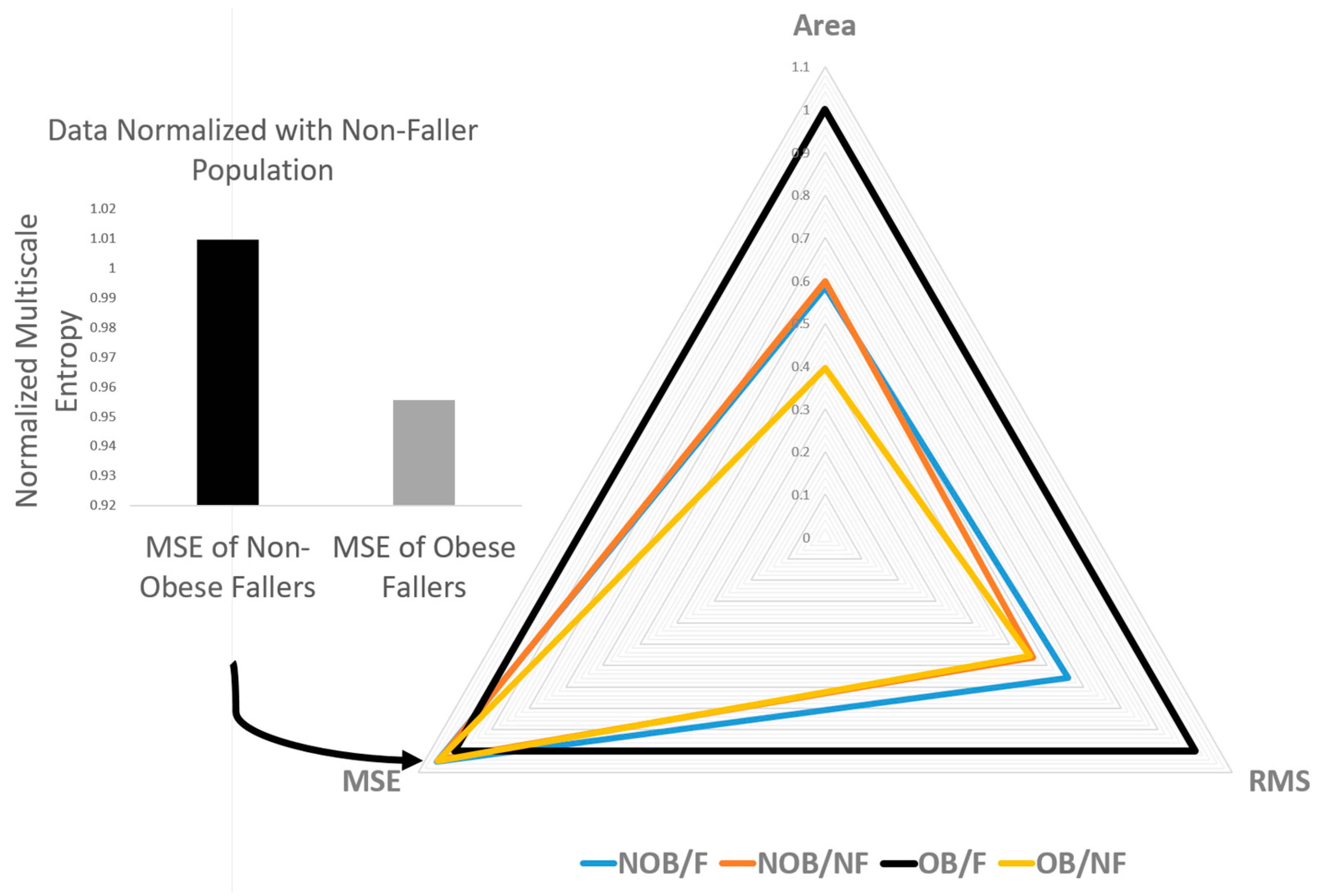
3.2. Nonlinear Measures
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Ethical Statements
References
- Mokdad, A.H.; Bowman, B.A.; Ford, E.S.; Vinicor, F.; Marks, J.S.; Koplan, J.P. The continuing epidemics of obesity and diabetes in the United States. JAMA 2001, 286, 1195–1200. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Beydoun, M.A. The Obesity Epidemic in the United States Gender, Age, Socioeconomic, Racial/Ethnic, and Geographic Characteristics: A Systematic Review and Meta-Regression Analysis. Epidemiol. Rev. 2007, 29, 6–28. [Google Scholar] [CrossRef] [PubMed]
- Lockhart, T.; Frame, C.; Soangra, R.; Lach, J. Fall Risk Prediction Using Wearable Wireless Sensors; SPIE Newsroom: Bellingham, WA, USA, 2014. [Google Scholar]
- Ogden, C.L.; Carroll, M.D.; Curtin, L.R.; McDowell, M.A.; Tabak, C.J.; Flegal, K.M. Prevalence of overweight and obesity in the United States, 1999–2004. JAMA 2006, 295, 1549–1555. [Google Scholar] [CrossRef] [PubMed]
- Wilson, P.W.; D’Agostino, R.B.; Sullivan, L.; Parise, H.; Kannel, W.B. Overweight and obesity as determinants of cardiovascular risk: The Framingham experience. Arch. Intern. Med. 2002, 162, 1867–1872. [Google Scholar] [CrossRef] [PubMed]
- Wang, T.J.; Parise, H.; Levy, D.; D’Agostino, R.B., Sr.; Wolf, P.A.; Vasan, R.S.; Benjamin, E.J. Obesity and the risk of new-onset atrial fibrillation. JAMA 2004, 292, 2471–2477. [Google Scholar] [CrossRef] [PubMed]
- Luppino, F.S.; de Wit, L.M.; Bouvy, P.F.; Stijnen, T.; Cuijpers, P.; Penninx, B.W.; Zitman, F.G. Overweight, obesity, and depression: A systematic review and meta-analysis of longitudinal studies. Arch. Gen. Psychiatry 2010, 67, 220–229. [Google Scholar] [CrossRef] [PubMed]
- Strazzullo, P.; D’Elia, L.; Cairella, G.; Garbagnati, F.; Cappuccio, F.P.; Scalfi, L. Excess body weight and incidence of stroke: Meta-analysis of prospective studies with 2 million participants. Stroke 2010, 41, e418–e426. [Google Scholar] [CrossRef] [PubMed]
- Kopelman, P.G. Obesity as a medical problem. Nature 2000, 404, 635–643. [Google Scholar] [CrossRef] [PubMed]
- Bray, G.A. Medical consequences of obesity. J. Clin. Endocrinol. Metab. 2004, 89, 2583–2589. [Google Scholar] [CrossRef] [PubMed]
- Ferraro, K.F.; Su, Y.P.; Gretebeck, R.J.; Black, D.R.; Badylak, S.F. Body mass index and disability in adulthood: A 20-year panel study. Am. J. Public Health 2002, 92, 834–840. [Google Scholar] [CrossRef] [PubMed]
- Peeters, A.; Bonneux, L.; Nusselder, W.J.; de Laet, C.; Barendregt, J.J. Adult obesity and the burden of disability throughout life. Obes. Res. 2004, 12, 1145–1151. [Google Scholar] [CrossRef] [PubMed]
- Metzger, J.S.; Catellier, D.J.; Evenson, K.R.; Treuth, M.S.; Rosamond, W.D.; Siega-Riz, A.M. Patterns of objectively measured physical activity in the United States. Med. Sci. Sports Exerc. 2008, 40, 630–638. [Google Scholar] [CrossRef] [PubMed]
- Reynolds, S.L.; Saito, Y.; Crimmins, E.M. The impact of obesity on active life expectancy in older American men and women. Gerontologist 2005, 45, 438–444. [Google Scholar] [CrossRef] [PubMed]
- Jenkins, K.R. Obesity’s effects on the onset of functional impairment among older adults. Gerontologist 2004, 44, 206–216. [Google Scholar] [CrossRef] [PubMed]
- Fontaine, K.R.; Barofsky, I. Obesity and health-related quality of life. Obes. Rev. 2001, 2, 173–182. [Google Scholar] [CrossRef] [PubMed]
- Corbeil, P.; Simoneau, M.; Rancourt, D.; Tremblay, A.; Teasdale, N. Increased risk for falling associated with obesity: Mathematical modeling of postural control. IEEE Trans. Neural Syst. Rehabil. Eng. 2001, 9, 126–136. [Google Scholar] [CrossRef] [PubMed]
- Fjeldstad, C.; Fjeldstad, A.S.; Acree, L.S.; Nickel, K.J.; Gardner, A.W. The influence of obesity on falls and quality of life. Dyn. Med. 2008, 7, 4. [Google Scholar] [CrossRef] [PubMed]
- Hasselkus, B.R.; Shambes, G.M. Aging and postural sway in women. J. Gerontol. 1975, 30, 661–667. [Google Scholar] [CrossRef] [PubMed]
- Era, P.; Heikkinen, E. Postural sway during standing and unexpected disturbance of balance in random samples of men of different ages. J. Gerontol. 1985, 40, 287–295. [Google Scholar] [CrossRef] [PubMed]
- Baloh, R.W.; Fife, T.D.; Zwerling, L.; Socotch, T.; Jacobson, K.; Bell, T.; Beykirch, K. Comparison of static and dynamic posturography in young and older normal people. J. Am. Geriatr. Soc. 1994, 42, 405–412. [Google Scholar] [CrossRef] [PubMed]
- Fernie, G.R.; Gryfe, C.I.; Holliday, P.J.; Llewellyn, A. The relationship of postural sway in standing to the incidence of falls in geriatric subjects. Age Ageing 1982, 11, 11–16. [Google Scholar] [CrossRef] [PubMed]
- Maki, B.E.; Holliday, P.J.; Topper, A.K. A prospective study of postural balance and risk of falling in an ambulatory and independent elderly population. J. Gerontol. 1994, 49, M72–M84. [Google Scholar] [CrossRef] [PubMed]
- Flegal, K.M.; Williamson, D.F.; Pamuk, E.R.; Rosenberg, H.M. Estimating deaths attributable to obesity in the United States. Am. J. Public Health 2004, 94, 1486–1489. [Google Scholar] [CrossRef] [PubMed]
- Owusu, W.; Willett, W.; Ascherio, A.; Spiegelman, D.; Rimm, E.; Feskanich, D.; Colditz, G. Body anthropometry and the risk of hip and wrist fractures in men: Results from a prospective study. Obes. Res. 1998, 6, 12–19. [Google Scholar] [CrossRef] [PubMed]
- Compston, J.E.; Watts, N.B.; Chapurlat, R.; Cooper, C.; Boonen, S.; Greenspan, S.; Pfeilschifter, J.; Silverman, S.; Díez-Pérez, A.; Lindsay, R.; et al. Obesity is not protective against fracture in postmenopausal women: GLOW. Am. J. Med. 2011, 124, 1043–1050. [Google Scholar] [CrossRef] [PubMed]
- Handrigan, G.A.; Corbeil, P.; Simoneau, M.; Teasdale, N. Balance control is altered in obese individuals. J. Biomech. 2010, 43, 383–384. [Google Scholar] [CrossRef] [PubMed]
- Hue, O.; Simoneau, M.; Marcotte, J.; Berrigan, F.; Dore, J.; Marceau, P.; Marceau, S.; Tremblay, A.; Teasdale, N. Body weight is a strong predictor of postural stability. Gait Posture 2007, 26, 32–38. [Google Scholar] [CrossRef] [PubMed]
- Blaszczyk, J.W.; Cieslinska-Swider, J.; Plewa, M.; Zahorska-Markiewicz, B.; Markiewicz, A. Effects of excessive body weight on postural control. J. Biomech. 2009, 42, 1295–1300. [Google Scholar] [CrossRef] [PubMed]
- Teasdale, N.; Hue, O.; Marcotte, J.; Berrigan, F.; Simoneau, M.; Dore, J.; Marceau, P.; Marceau, S.; Tremblay, A. Reducing weight increases postural stability in obese and morbid obese men. Int. J. Obes. 2007, 31, 153–160. [Google Scholar] [CrossRef] [PubMed]
- Cavanaugh, J.T.; Guskiewicz, K.M.; Giuliani, C.; Marshall, S.; Mercer, V.; Stergiou, N. Detecting altered postural control after cerebral concussion in athletes with normal postural stability. Br. J. Sports Med. 2005, 39, 805–811. [Google Scholar] [CrossRef] [PubMed]
- Cavanaugh, J.T.; Guskiewicz, K.M.; Giuliani, C.; Marshall, S.; Mercer, V.S.; Stergiou, N. Recovery of postural control after cerebral concussion: New insights using approximate entropy. J. Athl. Train. 2006, 41, 305–313. [Google Scholar] [PubMed]
- Pincus, S. Approximate entropy (ApEn) as a complexity measure. Chaos 1995, 5, 110–117. [Google Scholar] [CrossRef] [PubMed]
- Pincus, S.M. Approximate entropy as a measure of irregularity for psychiatric serial metrics. Bipolar Disord. 2006, 8, 430–440. [Google Scholar] [CrossRef] [PubMed]
- Khandoker, A.H.; Palaniswami, M.; Begg, R.K. A comparative study on approximate entropy measure and poincare plot indexes of minimum foot clearance variability in the elderly during walking. J. Neuroeng. Rehabil. 2008, 5, 4. [Google Scholar] [CrossRef] [PubMed]
- Bartlett, S.A.; Maki, B.E.; Fernie, G.R.; Holliday, P.J.; Gryfe, C.I. On the classification of a geriatric subject as a faller or nonfaller. Med. Biol. Eng. Comput. 1986, 24, 219–222. [Google Scholar] [CrossRef] [PubMed]
- Pincus, S.M. Approximate entropy as a measure of system complexity. Proc. Natl. Acad. Sci. USA 1991, 88, 2297–2301. [Google Scholar] [CrossRef] [PubMed]
- Harbourne, R.T.; Stergiou, N. Nonlinear analysis of the development of sitting postural control. Dev. Psychobiol. 2003, 42, 368–377. [Google Scholar] [CrossRef] [PubMed]
- Pincus, S.M.; Goldberger, A.L. Physiological time-series analysis: What does regularity quantify? Am. J. Physiol. 1994, 266, H1643–H1656. [Google Scholar] [CrossRef] [PubMed]
- Vaillancourt, D.E.; Newell, K.M. The dynamics of resting and postural tremor in Parkinson’s disease. Clin. Neurophysiol. 2000, 111, 2046–2056. [Google Scholar] [CrossRef]
- Pincus, S.M. quantifying complexity and regularity of neurobiological systems. In Methods in Neurosciences; Michael, L.J., Johannes, D.V., Eds.; Academic Press: Cambridge, MA, USA, 1995; Volume 28, pp. 336–363. [Google Scholar]
- Richman, J.S.; Moorman, J.R. Physiological time-series analysis using approximate entropy and sample entropy. Am. J. Physiol. Heart Circ. Physiol. 2000, 278, H2039–H2049. [Google Scholar] [CrossRef] [PubMed]
- Peng, C.K.; Buldyrev, S.V.; Havlin, S.; Simons, M.; Stanley, H.E.; Goldberger, A.L. Mosaic organization of DNA nucleotides. Phys. Rev. E Stat. Phys. Plasmas Fluids Relat. Interdiscip. Top. 1994, 49, 1685–1689. [Google Scholar] [CrossRef]
- Carroll, J.P.; Freedman, W. Nonstationary properties of postural sway. J. Biomech. 1993, 26, 409–416. [Google Scholar] [CrossRef]
- Loughlin, P.J.; Redfern, M.S.; Furman, J.M. Nonstationarities of postural sway. IEEE Eng. Med. Biol. Mag. 2003, 22, 69–75. [Google Scholar] [CrossRef] [PubMed]
- Peng, C.K.; Havlin, S.; Hausdorff, J.M.; Mietus, J.E.; Stanley, H.E.; Goldberger, A.L. Fractal mechanisms and heart rate dynamics. Long-range correlations and their breakdown with disease. J. Electrocardiol. 1995, 28, 59–65. [Google Scholar] [CrossRef]
- Lipsitz, L.A.; Goldberger, A.L. Loss of ‘complexity’ and aging. Potential applications of fractals and chaos theory to senescence. JAMA 1992, 267, 1806–1809. [Google Scholar] [CrossRef] [PubMed]
- Manor, B.; Costa, M.D.; Hu, K.; Newton, E.; Starobinets, O.; Kang, H.G.; Peng, C.K.; Novak, V.; Lipsitz, L.A. Physiological complexity and system adaptability: Evidence from postural control dynamics of older adults. J. Appl. Physiol. (1985) 2010, 109, 1786–1791. [Google Scholar] [CrossRef] [PubMed]
- Melzer, I.; Oddsson, L.I. Altered characteristics of balance control in obese older adults. Obes. Res. Clin. Pract. 2016, 10, 151–158. [Google Scholar] [CrossRef] [PubMed]
- Dutil, M.; Handrigan, G.A.; Corbeil, P.; Cantin, V.; Simoneau, M.; Teasdale, N.; Hue, O. The impact of obesity on balance control in community-dwelling older women. Age 2013, 35, 883–890. [Google Scholar] [CrossRef] [PubMed]
- Wu, X.; Madigan, M.L. Impaired plantar sensitivity among the obese is associated with increased postural sway. Neurosci. Lett. 2014, 583, 49–54. [Google Scholar] [CrossRef] [PubMed]
- Murray, M.P.; Gardner, G.M.; Mollinger, L.A.; Sepic, S.B. Strength of isometric and isokinetic contractions: Knee muscles of men aged 20 to 86. Phys. Ther. 1980, 60, 412–419. [Google Scholar] [CrossRef] [PubMed]
- Hurley, M.V.; Rees, J.; Newham, D.J. Quadriceps function, proprioceptive acuity and functional performance in healthy young, middle-aged and elderly subjects. Age Ageing 1998, 27, 55–62. [Google Scholar] [CrossRef] [PubMed]
- Duvigneaud, N.; Matton, L.; Wijndaele, K.; Deriemaeker, P.; Lefevre, J.; Philippaerts, R.; Thomis, M.; Delecluse, C.; Duquet, W. Relationship of obesity with physical activity, aerobic fitness and muscle strength in Flemish adults. J. Sports Med. Phys. Fit. 2008, 48, 201–210. [Google Scholar]
- Naugle, K.M.; Higgins, T.J.; Manini, T.M. Obesity and use of compensatory strategies to perform common daily activities in pre-clinically disabled older adults. Arch. Gerontol. Geriatr. 2012, 54, e134–e138. [Google Scholar] [CrossRef] [PubMed]
- Ko, S.; Stenholm, S.; Ferrucci, L. Characteristic gait patterns in older adults with obesity—Results from the Baltimore Longitudinal Study of Aging. J. Biomech. 2010, 43, 1104–1110. [Google Scholar] [CrossRef] [PubMed]
- Messier, S.P.; Legault, C.; Loeser, R.F.; van Arsdale, S.J.; Davis, C.; Ettinger, W.H.; DeVita, P. Does high weight loss in older adults with knee osteoarthritis affect bone-on-bone joint loads and muscle forces during walking? Osteoarthr. Cartil. 2011, 19, 272–280. [Google Scholar] [CrossRef] [PubMed]
- Delmonico, M.J.; Harris, T.B.; Visser, M.; Park, S.W.; Conroy, M.B.; Velasquez-Mieyer, P.; Boudreau, R.; Manini, T.M.; Nevitt, M.; Newman, A.B.; et al. Longitudinal study of muscle strength, quality, and adipose tissue infiltration. Am. J. Clin. Nutr. 2009, 90, 1579–1585. [Google Scholar] [PubMed]
- Rossi-Izquierdo, M.; Santos-Pérez, S.; Faraldo-García, A.; Vaamonde-Sánchez-Andrade, I.; Gayoso-Diz, P.; Del-Río-Valeiras, M.; Lirola-Delgado, A.; Soto-Varela, A. Impact of obesity in elderly patients with postural instability. Aging Clin. Exp. Res. 2016, 28, 423–428. [Google Scholar] [CrossRef] [PubMed]



| Health Status | Faller (F) | Non-Faller (NF) |
|---|---|---|
| Non-obese (NOB) | 14 | 20 |
| Obese (OB) | 8 | 22 |
| Overweight (OW) | 10 | 24 |
| Fall Risk | ||||
|---|---|---|---|---|
| Faller | Non-Faller | |||
| NOB | OB | NOB | OB | |
| Age (years) | 76.82 ± 6.87 | 72.29 ± 4.72 | 77.41 ± 8.49 | 72.68 ± 7.40 |
| Height (m) | 1.71 ± 0.06 | 1.61 ± 0.07 | 1.67 ± 0.11 | 1.64 ± 0.05 |
| Weight (kg) | 79.14 ± 8.18 | 80.77 ± 21.98 | 67.26 ± 12.41 | 87.66 ± 21.05 |
| BMI (kg/m2) | 26.85 ± 2.08 | 31.27 ± 8.09 | 24.29 ± 2.16 | 32.65 ± 7.62 |
| Gender | Fall Risk | Weight Status | |||
|---|---|---|---|---|---|
| F | NF | NOB | OB | OW | |
| Female | 12 | 53 | 21 | 19 | 25 |
| Male | 6 | 27 | 13 | 11 | 9 |
| NOB | OB | OW | ||||
|---|---|---|---|---|---|---|
| F | NF | F | NF | F | NF | |
| Area 1 | 9.69 ± 1.20 | 4.91 ± 3.57 | 13.36 ± 7.30 | 4.92 ± 3.90 | 5.19 ± 4.96 | 5.41 ± 3.52 |
| Range AP 2 | 34.29 ± 14.44 | 26.53 ± 8.68 | 51.78 ± 20.77 | 26.73 ± 10.48 | 29.24 ± 13.47 | 30.49 ± 7.58 |
| Range ML 2 | 15.40 ± 10.66 | 11.31 ± 5.36 | 17.42 ± 4.12 | 11.41 ± 6.39 | 11.31 ± 8.06 | 11.18 ± 5.54 |
| RMS AP | 6.20 ± 2.25 | 5.13 ± 1.87 | 8.87 ± 3.33 | 5.18 ± 2.06 | 5.60 ± 2.32 | 5.93 ± 1.82 |
| RMS ML | 3.05 ± 1.95 | 2.18 ± 1.15 | 3.53 ± 0.86 | 2.10 ± 1.21 | 2.15 ± 1.63 | 2.06 ± 0.94 |
| SD AP | 6.20 ± 2.25 | 5.13 ± 1.87 | 8.87 ± 3.33 | 5.19 ± 2.06 | 5.60 ± 2.32 | 5.94 ± 1.82 |
| SD ML | 3.05 ± 1.95 | 2.18 ± 1.15 | 3.53 ± 0.86 | 2.10 ± 1.21 | 2.16 ± 1.63 | 2.07 ± 0.94 |
| MPF AP | 0.36 ± 0.05 | 0.38 ± 0.06 | 0.38 ± 0.05 | 0.37 ± 0.05 | 0.40 ± 0.05 | 0.40 ± 0.06 |
| MPF ML | 0.39 ± 0.06 | 0.40 ± 0.07 | 0.38 ± 0.07 | 0.39 ± 0.06 | 0.42 ± 0.08 | 0.40 ± 0.06 |
| DFA α AP | 1.12 ± 0.16 | 1.14 ± 0.16 | 1.16 ± 0.23 | 1.15 ± 0.18 | 1.07 ± 0.15 | 1.09 ± 0.16 |
| DFA α ML | 1.37 ± 0.13 | 1.33 ± 0.12 | 1.40 ± 0.09 | 1.37 ± 0.10 | 1.30 ± 0.15 | 1.35 ± 0.12 |
| ApEn AP | 0.47 ± 0.12 | 0.54 ± 0.18 | 0.48 ± 0.14 | 0.48 ± 0.14 | 0.56 ± 0.12 | 0.52 ± 0.17 |
| ApEn ML | 0.55 ± 0.23 | 0.57 ± 0.23 | 0.44 ± 0.13 | 0.60 ± 0.26 | 0.62 ± 0.17 | 0.57 ± 0.21 |
| SaEn AP | 0.23 ± 0.22 | 0.25 ± 0.21 | 0.09 ± 0.03 | 0.22 ± 0.18 | 0.28 ± 0.21 | 0.19 ± 0.14 |
| SaEn ML | 0.23 ± 0.22 | 0.25 ± 0.21 | 0.09 ± 0.03 | 0.22 ± 0.18 | 0.28 ± 0.20 | 0.19 ± 0.14 |
| MSE AP | 3.41 ± 1.03 | 4.13 ± 1.51 | 3.73 ± 1.68 | 3.33 ± 1.13 | 4.18 ± 0.98 | 4.09 ± 1.52 |
| MSE ML | 3.41 ± 1.30 | 3.24 ± 1.03 | 3.17 ± 1.17 | 3.42 ± 1.51 | 3.58 ± 1.16 | 3.68 ± 1.27 |
| Weight Status | ||||||
|---|---|---|---|---|---|---|
| NOB | OB | OW | ||||
| Eyes Closed | Eyes Open | Eyes Closed | Eyes Open | Eyes Closed | Eyes Open | |
| MPF | 0.42 ± 0.07 | 0.39 ± 0.06 | 0.42 ± 0.08 | 0.38 ± 0.06 | 0.44 ± 0.07 | 0.41 ± 0.07 |
| RMS | 4.54 ± 2.65 | 4.06 ± 2.38 | 5.12 ± 3.93 | 4.33 ± 2.91 | 4.51 ± 2.51 | 3.97 ± 2.47 |
| Range | 24.66 ± 15.03 | 21.36 ± 13.14 | 26.08 ± 18.76 | 23.22 ± 16.69 | 24.00 ± 13.69 | 20.68 ± 12.42 |
| DFA | 0.99 ± 0.19 | 1.06 ± 0.21 | 1.04 ± 0.23 | 1.09 ± 0.21 | 0.98 ± 0.19 | 1.05 ± 0.18 |
| ApEn | 0.63 ± 0.21 | 0.54 ± 0.20 | 0.58 ± 0.18 | 0.52 ± 0.20 | 0.63 ± 0.17 | 0.56 ± 0.18 |
| MSE | 4.34 ± 1.74 | 3.58 ± 1.28 | 4.20 ± 1.58 | 3.40 ± 1.34 | 4.55 ± 1.59 | 3.89 ± 1.31 |
| NOB | OB | OW | ||||
|---|---|---|---|---|---|---|
| F | NF | F | NF | F | NF | |
| Area 1 | 40.17 ± 34.11 | 41.24 ± 43.69 | 68.87 ± 20.91 | 27.20 ± 14.16 | 32.83 ± 21.30 | 27.36 ± 15.74 |
| Range AP 2 | 0.36 ± 0.05 | 0.36 ± 0.04 | 0.37 ± 0.07 | 0.36 ± 0.04 | 0.38 ± 0.05 | 0.36 ± 0.05 |
| Range ML 2 | 1.58 ± 0.92 | 1.32 ± 0.44 | 2.17 ± 0.66 | 1.38 ± 0.50 | 1.16 ± 0.37 | 1.43 ± 0.55 |
| RMS AP | 1.74 ± 1.01 | 1.41 ± 0.42 | 2.49 ± 0.57 | 1.47 ± 0.57 | 1.23 ± 0.38 | 1.63 ± 0.62 |
| RMS ML | 8.19 ± 5.19 | 7.01 ± 2.26 | 12.45 ± 2.75 | 6.89 ± 2.17 | 6.41 ± 2.30 | 7.06 ± 2.19 |
| SD AP | 1.11 ± 0.21 | 1.11 ± 0.16 | 1.15 ± 0.22 | 1.01 ± 0.19 | 1.06 ± 0.12 | 1.05 ± 0.18 |
| SD ML | 1.26 ± 0.10 | 1.29 ± 0.12 | 1.27 ± 0.09 | 1.31 ± 0.09 | 1.36 ± 0.02 | 1.27 ± 0.09 |
| MPF AP | 1.40 ± 0.31 | 1.54 ± 0.27 | 1.35 ± 0.19 | 1.54 ± 0.21 | 1.67 ± 0.11 | 1.47 ± 0.21 |
| MPF ML | 8.43 ± 2.28 | 9.23 ± 2.25 | 7.84 ± 1.96 | 9.20 ± 2.04 | 10.71 ± 1.40 | 8.21 ± 2.28 |
| DFA α AP | 0.44 ± 0.07 | 0.41 ± 0.05 | 0.43 ± 0.04 | 0.41 ± 0.05 | 0.44 ± 0.07 | 0.42 ± 0.06 |
| DFA α ML | 0.49 ± 0.21 | 0.55 ± 0.32 | 0.62 ± 0.15 | 0.44 ± 0.13 | 0.54 ± 0.34 | 0.42 ± 0.13 |
| ApEn AP | 0.56 ± 0.28 | 0.59 ± 0.33 | 0.75 ± 0.18 | 0.52 ± 0.18 | 0.61 ± 0.34 | 0.47 ± 0.14 |
| ApEn ML | 3.12 ± 1.52 | 3.93 ± 3.50 | 3.87 ± 0.70 | 2.51 ± 0.64 | 3.57 ± 2.41 | 2.62 ± 1.09 |
| SaEn AP | 0.96 ± 0.25 | 0.95 ± 0.14 | 0.93 ± 0.22 | 0.95 ± 0.15 | 0.88 ± 0.24 | 0.97 ± 0.16 |
| SaEn ML | 1.40 ± 0.04 | 1.39 ± 0.04 | 1.41 ± 0.04 | 1.42 ± 0.03 | 1.39 ± 0.08 | 1.41 ± 0.03 |
| MSE AP | 1.82 ± 0.15 | 1.82 ± 0.14 | 1.82 ± 0.12 | 1.90 ± 0.10 | 1.86 ± 0.21 | 1.88 ± 0.09 |
| MSE ML | 12.60 ± 2.00 | 12.48 ± 1.71 | 12.01 ± 1.32 | 12.57 ± 1.36 | 12.64 ± 1.97 | 12.78 ± 1.28 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Frames, C.W.; Soangra, R.; Lockhart, T.E.; Lach, J.; Ha, D.S.; Roberto, K.A.; Lieberman, A. Dynamical Properties of Postural Control in Obese Community-Dwelling Older Adults. Sensors 2018, 18, 1692. https://doi.org/10.3390/s18061692
Frames CW, Soangra R, Lockhart TE, Lach J, Ha DS, Roberto KA, Lieberman A. Dynamical Properties of Postural Control in Obese Community-Dwelling Older Adults. Sensors. 2018; 18(6):1692. https://doi.org/10.3390/s18061692
Chicago/Turabian StyleFrames, Christopher W., Rahul Soangra, Thurmon E. Lockhart, John Lach, Dong Sam Ha, Karen A. Roberto, and Abraham Lieberman. 2018. "Dynamical Properties of Postural Control in Obese Community-Dwelling Older Adults" Sensors 18, no. 6: 1692. https://doi.org/10.3390/s18061692
APA StyleFrames, C. W., Soangra, R., Lockhart, T. E., Lach, J., Ha, D. S., Roberto, K. A., & Lieberman, A. (2018). Dynamical Properties of Postural Control in Obese Community-Dwelling Older Adults. Sensors, 18(6), 1692. https://doi.org/10.3390/s18061692






