Synthesis and In Vitro Antibacterial Evaluation of Mannich Base Nitrothiazole Derivatives
Abstract
1. Introduction
2. Results and Discussion
2.1. Results
Chemistry
2.2. Discussion
In Vitro Anti-Tubercular Activity and Calculated Drug-like Properties
3. Materials and Methods
3.1. General Methods
3.2. General Synthetic Procedure
- (i)
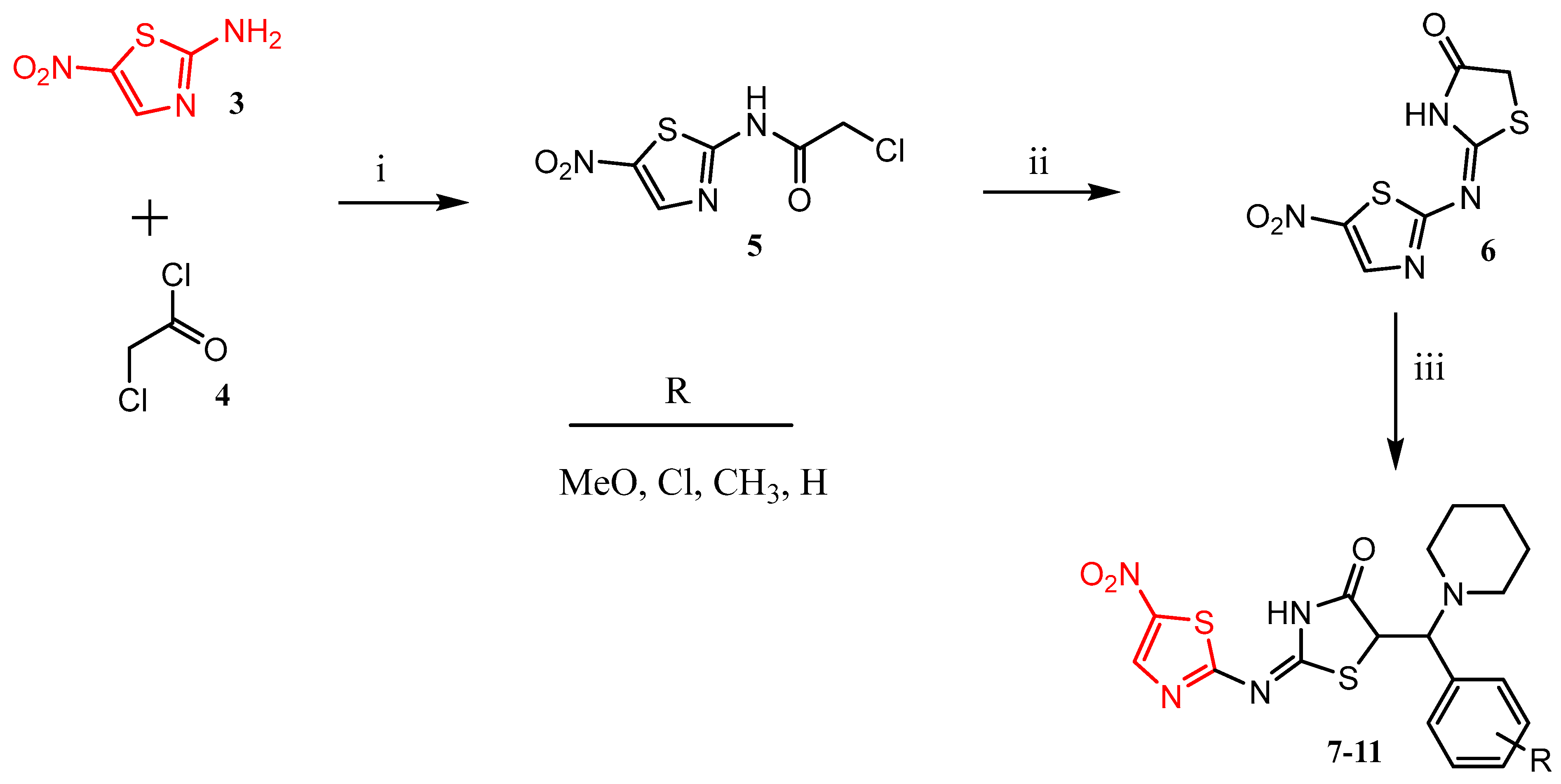
- N-acylation: 2-amino-5-nitrothiazole (2.3 g, 15.9 mmol) and 2-chloroacetyl chloride (2.2 eq) were added into an ice-cold round-bottom flask containing dichloromethane (DCM) and triethylamine (TEA) (1.2 eq). The mixture was stirred at room temperature for 24–36 h. The reaction was monitored by TLC, and upon completion, the reaction mixture was concentrated in vacuo. The resulting mixture was then washed with water, filtered, washed with hexane, filtered, and dried to afford intermediate 5 in 80% yields [17].
- (ii)
- Intramolecular cyclization: Into a round-bottom flask, 3 g (11.4 mmol) of compound 5 was added, followed by 1.7 g (2 eq, 22.7 mmol) of ammonium thiocyanate, and 20 mL of ethanol, and the mixture was refluxed for 3–4 h. Upon reaction completion (monitored by TLC), the mixture was left to stand still at room temperature (rt) overnight. The resulting precipitate was filtered and washed with ethanol and water to obtain intermediate 6 in 74% yields [17].
- (iii)
- Mannich base condensation: Samples of 0.3 g (1.2 mmol) of 6, piperidine (5 eq), and appropriate benzaldehydes (5 eq) were added into a round-bottom flask containing 10 mL of ethanol, and the resultant mixture was refluxed for 24–36 h. The reaction was monitored by TLC, and after completion, it was kept at ~8 °C overnight. The resulting precipitate was then filtered, washed with water, and finally recrystallized in 1,4-dioxane to achieve the target compounds (7–11) in low to moderate yields.
- (E)-2-((5-nitrothiazol-2-yl)imino)-5-(phenyl(piperidin-1-yl)methyl)thiazolidin-4-one, 7. Yellow powder; 32% yield; mp: 210–211 °C; 1H NMR (600 MHz, DMSO-d6) δ 7.63–7.52 (m, 5H), 7.45 (s, 1H), 3.92 (s, 2H), 3.63 (s, 2H), 1.62–1.50 (m, 10H). 13C NMR (151 MHz, DMSO-d6) δ 179.79, 173.84, 134.43, 130.13, 129.96, 129.94, 129.64, 129.35, 50.32, 49.62, 26.21, 25.59, 23.86. m/z HRMS (APCI) found 273.1096. Calcd for C12H21N2OS2: 273.1090 [M + H]+.
- (E)-2-((5-nitrothiazol-2-yl)imino)-5-(piperidin-1-yl(m-tolyl)methyl)thiazolidin-4-one, 8. Yellow powder; 32% yield; mp: 208 °C; 1HNMR (600 MHz, Chloroform-d) δ 8.00 (s, 1H), 7.55–7.53 (m, 1H), 7.28–7.25 (m, 3H), 4.05–4.02 (m, 2H), 3.57–3.55 (m, 2H), 2.46 (s, 3H), 1.99–1.21 (m, 10H). 13C NMR (151 MHz, CDCl3) δ 180.52, 174.95, 138.67, 133.94, 130.75, 130.33, 129.39, 129.11, 127.24, 126.17, 50.16, 49.60, 26.16, 25.45, 24.06, 19.98. m/z HRMS (APCI) found 287.1265. Calcd for C13H23N2OS2: 287.1246 [M + H]+.
- (E)-5-((3-chlorophenyl)(piperidin-1-yl)methyl)-2-((5-nitrothiazol-2-yl)imino)thiazolidin-4-one, 9. White powder; 25% yield; mp: 200–202 °C; 1H NMR (600 MHz, DMSO-d6) δ 7.83 (s, 1H), 7.69 (d, J = 6.6 Hz, 1H), 7.62 (d, J = 7.1 Hz, 1H), 7.52–7.46 (m, 3H), 3.98–3.91 (m, 2H), 3.62 (d, J = 5.4 Hz, 2H), 1.84–1.55 (m, 10H). 13C NMR (151 MHz, DMSO-d6) δ 179.16, 173.67, 134.59, 133.00, 132.63, 131.56, 130.65, 129.13, 128.41, 125.04, 50.48, 49.79, 26.22, 25.60, 23.82. m/z HRMS (APCI) found 307.0708. Calcd for C12H20ClN2OS2: 307.0700 [M + H]+.
- (E)-5-((3-methoxyphenyl)(piperidin-1-yl)methyl)-2-((5-nitrothiazol-2-yl)imino)thiazolidin-4-one, 10. Off white powder; 30% yield; mp: 130–132 °C; 1H NMR (600 MHz, DMSO-d6) δ 7.61 (s, 1H), 7.43 (t, J = 8.0 Hz,1H), 7.23–7.20 (m, 1H), 7.18–7.17 (m, 1H), 7.03 (d, J = 10.2 Hz, 1H), 3.97–3.91 (m, 2H), 3.82 (s, 3H), 3.64–3.63 (m, 2H), 2.11–1.04 (m, 10H). 13C NMR (151 MHz, DMSO-d6) δ 179.71, 173.78, 160.15, 135.83, 130.69, 129.89, 129.65, 122.01, 115.86, 115.41, 55.75, 50.31, 49.61, 26.22, 25.58, 23.85. m/z HRMS (APCI) found 307.0709. Calcd for C12H20ClN2OS2: 307.0700 [M + H]+.
- ((E)-5-((2-chlorophenyl)(piperidin-1-yl)methyl)-2-((5-nitrothiazol-2-yl)imino)thiazolidin-4-one, 11. Brown powder; 23% yield; mp: 201–202 °C; 1H NMR (600 MHz, DMSO-d6 δ 7.82 (s, 1H), 7.68 (dd, J = 7.7, 1.6 Hz, 1H), 7.61 (dd, J = 7.9, 1.3 Hz, 1H), 7.52–7.44 (m, 3H), 3.92–3.91 (m, 2H), 3.61–3.60 (m, 1H), 1.87–1.26 (m, 10H). 13C NMR (151 MHz, DMSO-d6) δ 183.94, 178.44, 139.36, 137.77, 137.40, 136.34, 135.42, 133.90, 133.18, 129.81, 55.24, 54.55, 30.97, 30.36, 28.57. m/z HRMS (APCI) found 303.1208. Calcd for C13H23N2O2S2: 303.1195 [M + H]+.
3.3. In Vitro Antitubercular Evaluation
3.4. In Vitro Cell Toxicity Evaluation
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- WHO. Global Tuberculosis Report 2018; World Health Organization: Geneva, Switzerland, 2018. [Google Scholar]
- Lam, K.K.; Zheng, X.; Forestieri, R.; Balgi, A.; Nodwell, M.; Vollett, S.; Anderson, H.; Andersen, R.; Av-Gay, Y.; Roberge, M. Nitazoxanide stimulates autophagy and inhibits mTORC1 signaling and intracellular proliferation of Mycobacterium tuberculosis. PLoS Pathog. 2012, 8, e1002691. [Google Scholar] [CrossRef] [PubMed]
- Gengenbacher, M.; Kaufmann, S.H. Mycobacterium tuberculosis: Success through dormancy. FEMS Microbiol. Rev. 2012, 36, 514–532. [Google Scholar] [CrossRef] [PubMed]
- Dietrich, J.; Doherty, T.M. Interaction of Mycobacterium tuberculosis with the host: Consequences for vaccine development. APMIS 2009, 117, 440–457. [Google Scholar] [CrossRef] [PubMed]
- Raffetseder, J.; Pienaar, E.; Blomgran, R.; Eklund, D.; Brodin, V.P.; Andersson, H.; Welin, A.; Lerm, M. Replication rates of Mycobacterium tuberculosis in human macrophages do not correlate with mycobacterial antibiotic susceptibility. PLoS ONE 2014, 9, e112426. [Google Scholar] [CrossRef] [PubMed]
- Connolly, L.E.; Edelstein, P.H.; Ramakrishnan, L. Why is long-term therapy required to cure tuberculosis? PLoS Med. 2007, 4, e120. [Google Scholar] [CrossRef] [PubMed]
- Riccardi, G.; Pasca, M.R.; Chiarelli, L.R.; Manina, G.; Mattevi, A.; Binda, C. The DprE1 enzyme, one of the most vulnerable targets of Mycobacterium tuberculosis. Appl. Microbiol. Biotechnol. 2013, 97, 8841–8848. [Google Scholar] [CrossRef] [PubMed]
- WHO. Global Tuberculosis Report 2022. Available online: https://www.who.int/publications/i/item/9789240061729 (accessed on 6 March 2024).
- Peddireddy, V.; Doddam, S.N.; Ahmed, N. Mycobacterial dormancy systems and host responses in tuberculosis. Front. Immunol. 2017, 8, 84. [Google Scholar] [CrossRef] [PubMed]
- Iacobino, A.; Piccaro, G.; Giannoni, F.; Mustazzolu, A.; Fattorinia, A. Mycobacterium tuberculosis is selectively killed by rifampin and rifapentine in hypoxia at neutral pH. Antimicrob. Agents Chemother. 2017, 61, e02296-16. [Google Scholar] [CrossRef] [PubMed]
- Yu, X.; Li, C.; Hong, W.; Pan, W.; Xie, J. Autophagy during Mycobacterium tuberculosis infection and implications for future tuberculosis medications. Cell. Signal. 2013, 25, 1272–1278. [Google Scholar] [CrossRef] [PubMed]
- Kumar, G.; Kapoor, S. Targeting mycobacterial membranes and membrane proteins: Progress and limitations. Bioorg. Med. Chem. Lett. 2023, 81, 117212. [Google Scholar] [CrossRef] [PubMed]
- Iacobino, A.; Piccaro, G.; Giannoni, F.; Mustazzolu, A.; Fattorini, L. Activity of drugs against dormant Mycobacterium tuberculosis. Int. J. Mycobacteriol. 2016, 5, 94. [Google Scholar] [CrossRef] [PubMed]
- Novoa-Aponte, L.; Ospina, C.Y. Mycobacterium tuberculosis P-type ATPases: Possible targets for drug or vaccine development. Biomed. Res. Int. 2014, 2014, 296986. [Google Scholar] [CrossRef] [PubMed]
- Dartois, V.A.; Rubin, E.J. Anti-tuberculosis treatment strategies and drug development: Challenges and priorities. Nat. Rev. Microbiol. 2022, 20, 685–701. [Google Scholar] [CrossRef] [PubMed]
- Odingo, J.; Bailey, M.A.; Files, M.; Early, J.V.; Alling, T.; Dennison, D.; Bowman, J.; Dalai, S.; Kumar, N.; Cramer, J.; et al. In Vitro Evaluation of Novel Nitazoxanide Derivatives against Mycobacterium tuberculosis. ACS Omega 2017, 2, 5873–5890. [Google Scholar] [CrossRef] [PubMed]
- Hart, D.; Legoabe, L.J.; Jesumoroti, O.J.; Jordaan, A.; Warner, D.F.; Steventon, R.; Beteck, R.M. Nitrothiazole-thiazolidinone hybrids: Synthesis and in vitro antimicrobial evaluation. Chem. Biodivers. 2022, 19, e202200729. [Google Scholar] [CrossRef] [PubMed]
- Beteck, R.M.; Jordaan, A.; Seldon, R.; Laming, D.; Hoppe, H.C.; Warner, D.F.; Khanye, S.D. Easy-To-Access Quinolone Derivatives Exhibiting Antibacterial and Anti-Parasitic Activities. Molecules 2021, 26, 1141. [Google Scholar] [CrossRef] [PubMed]
- Dube, P.S.; Legoabe, L.J.; Jordaan, A.; Jesumoroti, O.J.; Tshiwawa, T.; Warner, D.F.; Beteck, R.M. Easily accessed nitroquinolones exhibiting potent and selective anti-tubercular activity. Eur. J. Med. Chem. 2021, 213, 113207. [Google Scholar] [CrossRef] [PubMed]
- du Preez, C.; Legoabe, L.J.; Jordaan, A.; Jesumoroti, O.J.; Warner, D.F.; Beteck, R.M. Arylnitro monocarbonyl curcumin analogues: Synthesis and in vitro antitubercular evaluation. Chem. Biol. Drug Des. 2023, 101, 717–726. [Google Scholar] [CrossRef] [PubMed]
- Blaskovich, M.A.; Zuegg, J.; Elliott, A.G.; Cooper, M.A. Helping Chemists Discover New Antibiotics. ACS Infect. Dis. 2015, 1, 285–287. [Google Scholar] [CrossRef] [PubMed]



 | ||||||
|---|---|---|---|---|---|---|
| Entry | WM/Da | tPSA | a ClogP | R | HEK293 | MIC90 (µM) vs. Mtb on Day 14 |
| CC50 (µM) | CAS, GLU, TX | |||||
| 7 | 417 | 108 | 1.1 | H | 32 | 31.25 |
| 8 | 431 | 108 | 1.6 | m-CH3 | 32 | 3.795 |
| 9 | 451 | 108 | 1.8 | m-Cl | 32 | <0.244 |
| 10 | 447 | 118 | 1.0 | m-MeO | 32 | <0.244 |
| 11 | 451 | 108 | 1.8 | o-Cl | 32 | 125 |
| RF | - | - | - | - | - | 0.01 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dube, P.S.; Hart, D.; Legoabe, L.J.; Jordaan, A.; Warner, D.F.; Beteck, R.M. Synthesis and In Vitro Antibacterial Evaluation of Mannich Base Nitrothiazole Derivatives. Molbank 2024, 2024, M1793. https://doi.org/10.3390/M1793
Dube PS, Hart D, Legoabe LJ, Jordaan A, Warner DF, Beteck RM. Synthesis and In Vitro Antibacterial Evaluation of Mannich Base Nitrothiazole Derivatives. Molbank. 2024; 2024(1):M1793. https://doi.org/10.3390/M1793
Chicago/Turabian StyleDube, Phelelisiwe S., Dylan Hart, Lesetja J. Legoabe, Audrey Jordaan, Digby F. Warner, and Richard M. Beteck. 2024. "Synthesis and In Vitro Antibacterial Evaluation of Mannich Base Nitrothiazole Derivatives" Molbank 2024, no. 1: M1793. https://doi.org/10.3390/M1793
APA StyleDube, P. S., Hart, D., Legoabe, L. J., Jordaan, A., Warner, D. F., & Beteck, R. M. (2024). Synthesis and In Vitro Antibacterial Evaluation of Mannich Base Nitrothiazole Derivatives. Molbank, 2024(1), M1793. https://doi.org/10.3390/M1793







