The Association between Salivary Metabolites and Gingival Bleeding Score in Healthy Subjects: A Pilot Study
Abstract
1. Introduction
2. Results
2.1. Clinical Data of the Study Participants
2.2. Eukaryotic and Prokaryotic Cell Counts in Saliva
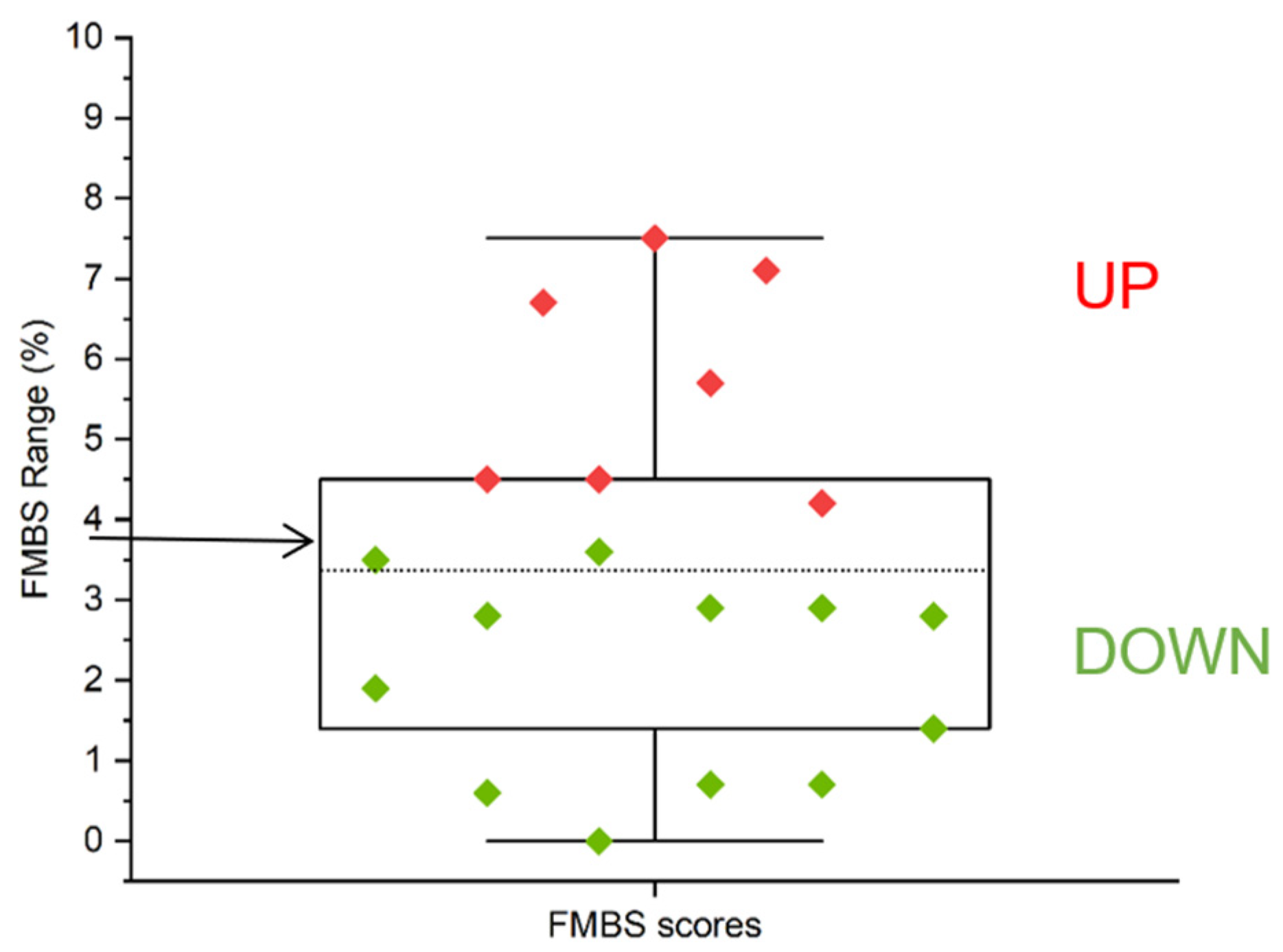
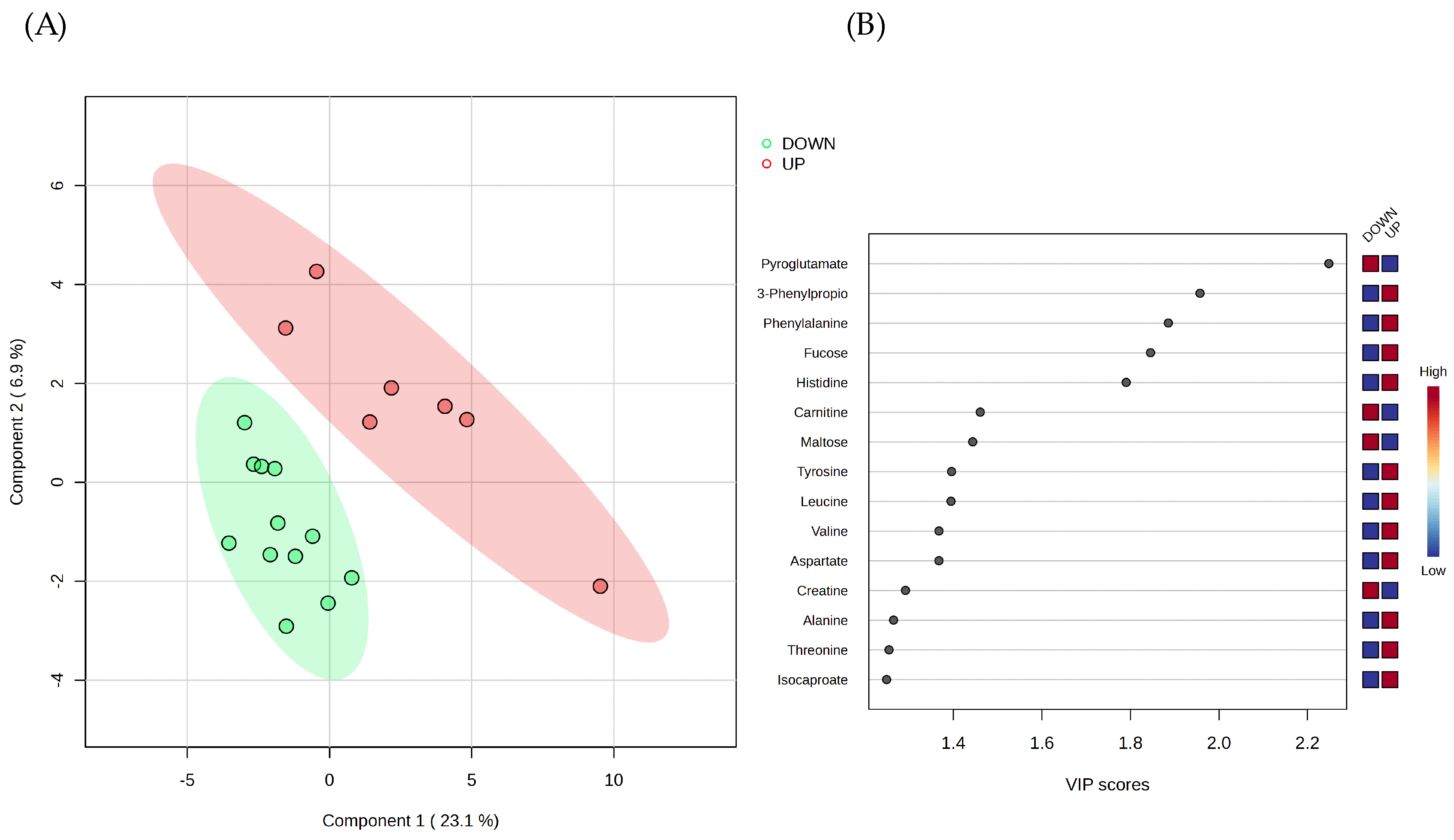
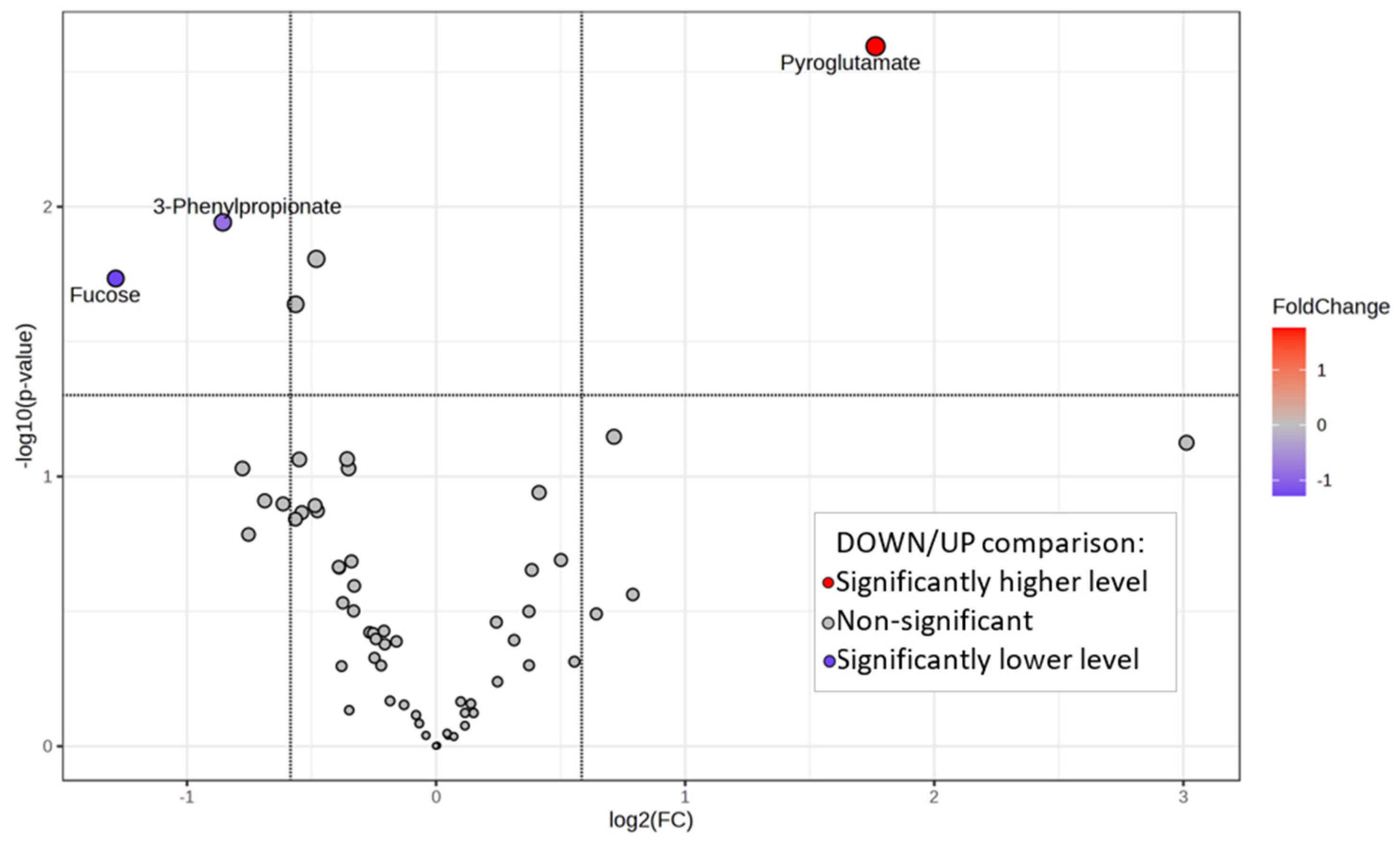
2.3. Bleeding Score and Salivary Metabolomes Analysis
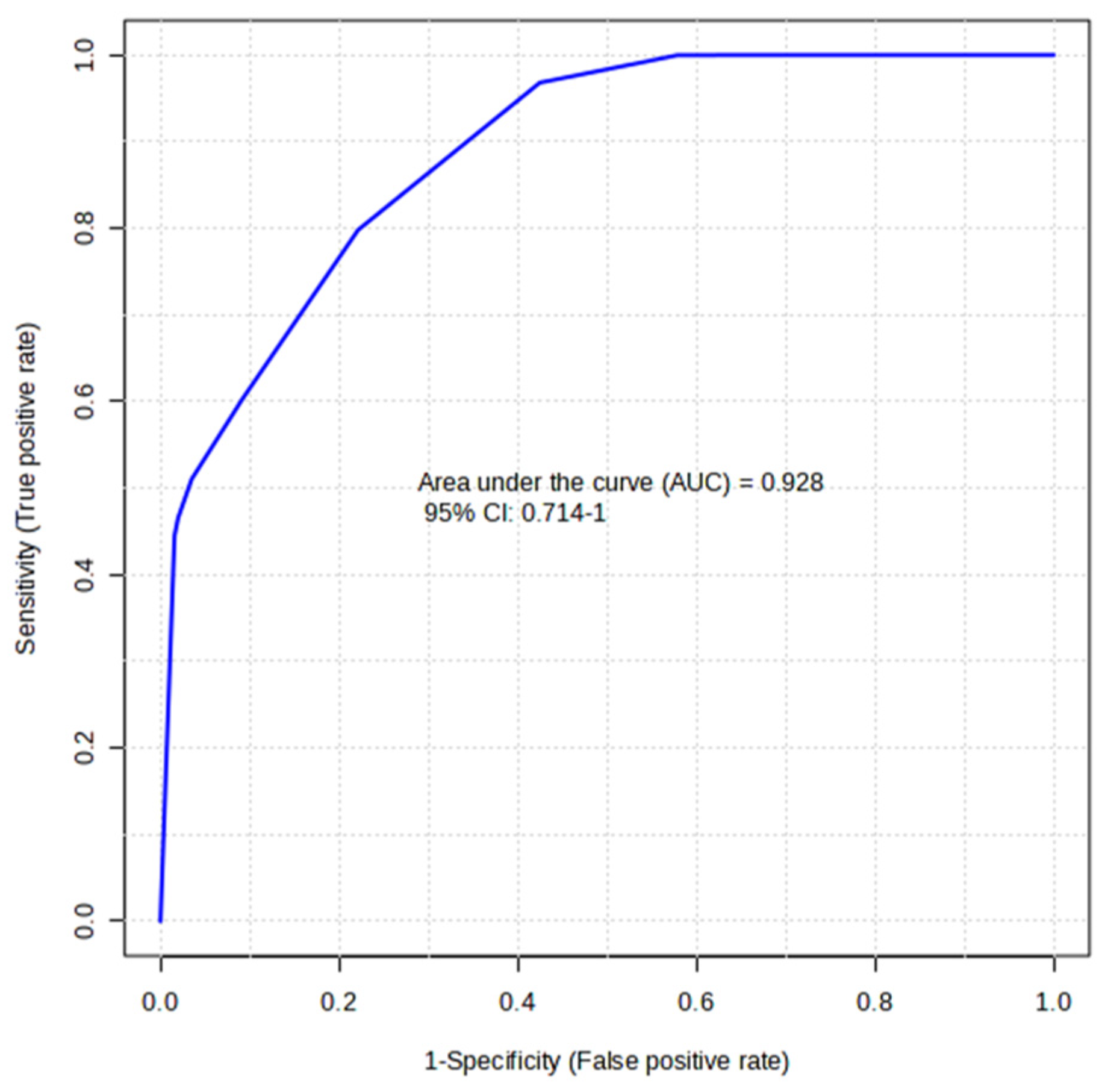
2.4. Biomarker Evaluation by Receiver Operating Characteristic (ROC) Curve Analysis
3. Discussion
4. Materials and Methods
4.1. Ethics Statement
4.2. Clinical Assessment of the Study Participants
4.3. Cell Counting in Whole Saliva
4.4. NMR Metabolomics
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Gasner, N.S.; Schure, R.S. Periodontal Disease In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2023. [Google Scholar]
- Global Burden of Disease Collaborative Network. Global Burden of Disease Study 2019 (GBD 2019); Institute of Health Metrics and Evaluation (IHME): Seattle, WA, USA, 2020; Available online: http://ghdx.healthdata.org/gbd-results-tool (accessed on 1 April 2024).
- Botelho, J.; Machado, V.; Leira, Y.; Proença, L.; Chambrone, L.; Mendes, J.J. Economic burden of periodontitis in the United States and Europe: An updated estimation. J. Periodontol. 2022, 93, 373–379. [Google Scholar] [CrossRef] [PubMed]
- Tonetti, M.S.; Jepsen, S.; Jin, L.; Otomo-Corgel, J. Impact of the global burden of periodontal diseases on health, nutrition and wellbeing of mankind: A call for global action. J. Clin. Periodontol. 2017, 44, 456–462. [Google Scholar] [CrossRef] [PubMed]
- Nazir, M.A. Prevalence of periodontal disease, its association with systemic diseases and prevention. Int. J. Health Sci. 2017, 11, 72–80. [Google Scholar]
- Mann, J.; Bernstein, Y.; Findler, M. Periodontal disease and its prevention, by traditional and new avenues. Exp. Ther. Med. 2020, 19, 1504–1506. [Google Scholar] [CrossRef] [PubMed]
- Papapanou, P.N. Systemic effects of periodontitis: Lessons learned from research on atherosclerotic vascular disease and adverse pregnancy outcomes. Int. Dent. J. 2015, 65, 283–291. [Google Scholar] [CrossRef] [PubMed]
- Janakiram, C.; Dye, B.A. A public health approach for prevention of periodontal disease. Periodontol. 2000 2020, 84, 202–214. [Google Scholar] [CrossRef] [PubMed]
- Martínez-García, M.; Hernández-Lemus, E. Periodontal inflammation and systemic diseases: An overview. Front. Physiol. 2021, 12, 709438. [Google Scholar] [CrossRef] [PubMed]
- Kassebaum, N.J.; Bernabé, E.; Dahiya, M.; Bhandari, B.; Murray, C.J.; Marcenes, W. Global burden of severe periodontitis in 1990-2010: A systematic review and meta-regression. J. Dent. Res. 2014, 93, 1045–1053. [Google Scholar] [CrossRef] [PubMed]
- American Academy of Periodontology. Parameter on plaque-induced gingivitis. J. Periodontol. 2000, 71, 851–852. [Google Scholar] [CrossRef]
- Chapple, I.L.C.; Mealey, B.L.; Van Dyke, T.E.; Bartold, P.M.; Dommisch, H.; Eickholz, P.; Geisinger, M.L.; Genco, R.J.; Glogauer, M.; Goldstein, M.; et al. Periodontal health and gingival diseases and conditions on an intact and a reduced periodontium: Consensus report of workgroup 1 of the 2017 world workshop on the classification of periodontal and peri-Implant Diseases and Conditions. J. Periodontol. 2018, 89, S74–S84. [Google Scholar] [CrossRef]
- Trombelli, L.; Farina, R.; Silva, C.O.; Tatakis, D.N. Plaque-induced gingivitis: Case definition and diagnostic considerations. J. Periodontol. 2018, 89, S46–S73. [Google Scholar] [CrossRef] [PubMed]
- Sanz, M.; Herrera, D.; Kebschull, M.; Chapple, I.; Jepsen, S.; Beglundh, T.; Sculean, A.; Tonetti, M.S. EFP workshop participants and methodological consultants. treatment of stage I-III periodontitis-The EFP S3 level clinical practice guideline. J. Clin. Periodontol. 2020, 47 (Suppl. S22), 4–60, Erratum in J. Clin. Periodontol. 2021, 48, 163. [Google Scholar]
- Becerra-Ruiz, J.S.; Guerrero-Velázquez, C.; Martínez-Esquivias, F.; Martínez-Pérez, L.A.; Guzmán-Flores, J.M. Innate and adaptive immunity of periodontal disease. From etiology to alveolar bone loss. Oral Dis. 2022, 28, 1441–1447. [Google Scholar] [CrossRef] [PubMed]
- Chapple, I.L.; Van der Weijden, F.; Doerfer, C.; Herrera, D.; Shapira, L.; Polak, D.; Madianos, P.; Louropoulou, A.; Machtei, E.; Donos, N.; et al. Primary prevention of periodontitis: Managing gingivitis. J. Clin. Periodontol. 2015, 42, S71–S76. [Google Scholar] [CrossRef]
- Roblegg, E.; Coughran, A.; Sirjani, D. Saliva: An all-rounder of our body. Eur. J. Pharm. Biopharm. 2019, 142, 133–141. [Google Scholar] [CrossRef] [PubMed]
- Uchida, H.; Ovitt, C.E. Novel impacts of saliva with regard to oral health. J. Prosthet. Dent. 2022, 127, 383–391. [Google Scholar] [CrossRef]
- Ferrari, E.; Gallo, M.; Spisni, A.; Antonelli, R.; Meleti, M.; Pertinhez, T.A. Human Serum and Salivary Metabolomes: Diversity and Closeness. Int. J. Mol. Sci. 2023, 24, 16603. [Google Scholar] [CrossRef]
- Kumari, S.; Samara, M.; Ampadi Ramachandran, R.; Gosh, S.; George, H.; Wang, R.; Pesavento, R.P.; Mathew, M.T. A review on saliva-based health diagnostics: Bomarker selection and future directions. Biomed. Mater. Devices 2023, in press. [Google Scholar] [CrossRef]
- Ates, H.C.; Brunauer, A.; von Stetten, F.; Urban, G.A.; Güder, F.; Merkoçi, A.; Früh, S.M.; Dincer, C. Integrated devices for non-invasive diagnostics. Adv. Func. Matl. 2021, 31, 2010388. [Google Scholar] [CrossRef]
- Cui, B.Y.; Yang, M.; Zhu, J.; Zhang, H.; Duan, Z.; Wang, S.; Liao, Z.; Liu, W. Developments in diagnostic applications of saliva in human organ diseases. Med. Novel Technol. Dev. 2022, 13, 100115. [Google Scholar] [CrossRef]
- Mediouni, M.; Kaczor-Urbanowicz, K.E.; Madiouni, R. Suggestions for creating the International Scientific Foundation of Saliva Diagnosis (ISFSD): New research strategies, development, and technologies. Oral Sci. Int. 2019, 16, 138–146. [Google Scholar] [CrossRef]
- Meleti, M.; Quartieri, E.; Antonelli, R.; Pezzi, M.E.; Ghezzi, B.; Viani, M.V.; Setti, G.; Casali, E.; Ferrari, E.; Ciociola, T.; et al. Metabolic profiles of whole, parotid and submandibular/sublingual saliva. Metabolites 2020, 10, 318. [Google Scholar] [CrossRef] [PubMed]
- Gardner, A.; Carpenter, G.; So, P.W. Salivary metabolomics: From diagnostic biomarker Discovery to investigating biological function. Metabolites 2020, 10, 47. [Google Scholar] [CrossRef] [PubMed]
- Nijakowski, K.; Zdrojewski, J.; Nowak, M.; Gruszczyński, D.; Knoll, F.; Surdacka, A. Salivary metabolomics for systemic cancer diagnosis: A systematic review. Metabolites 2023, 13, 28. [Google Scholar] [CrossRef] [PubMed]
- Panneerselvam, K.; Ishikawa, S.; Krishnan, R.; Sugimoto, M. Salivary Metabolomics for Oral Cancer Detection: A Narrative Review. Metabolites 2022, 12, 436. [Google Scholar] [CrossRef] [PubMed]
- Patil, D.J.; Chandramani, B. More Salivary metabolomics—A diagnostic and biologic signature for oral cancer. J. Oral Max. Surg. Med. Path. 2021, 33, 546–554. [Google Scholar]
- Hyvärinen, E.; Savolainen, M.; Mikkonen, J.J.W.; Kullaa, A.M. Salivary metabolomics for diagnosis and monitoring diseases: Challenges and possibilities. Metabolites 2021, 11, 587. [Google Scholar] [CrossRef]
- Huang, S.; He, T.; Yue, F.; Xu, X.; Wang, L.; Zhu, P.; Teng, F.; Sun, Z.; Liu, X.; Jing, G.; et al. Longitudinal multi-omics and microbiome meta-analysis an asymptomatic gingival state that links gingivitis, periodontitis, and aging. mBio 2021, 2, e03281-20. [Google Scholar] [CrossRef] [PubMed]
- Chong, I.-G.; Jun, C.-H. Performance of some variable selection methods when multicollinearity is present. Chemom. Intell. Lab. Syst. 2005, 78, 103–112. [Google Scholar] [CrossRef]
- Basic, A.; Dahlén, G. Microbial metabolites in the pathogenesis of periodontal diseases: A narrative review. Front. Oral Health 2023, 4, 1210200. [Google Scholar] [CrossRef]
- Hyvärinen, E.; Kashyap, B.; Kullaa, A.M. Oral sources of salivary metabolites. Metabolites 2023, 13, 498. [Google Scholar] [CrossRef]
- Messana, I.; Manconi, B.; Cabras, T.; Boroumand, M.; Sanna, M.T.; Iavarone, F.; Olianas, A.; Desiderio, C.; Rossetti, D.V.; Vincenzoni, F.; et al. The post-translational modifications of human salivary peptides and proteins evidenced by top-down platforms. Int. J. Mol. Sci. 2023, 24, 12776. [Google Scholar] [CrossRef] [PubMed]
- Liebsch, C.; Pitchika, V.; Pink, C.; Samietz, S.; Kastenmüller, G.; Artati, A.; Suhre, K.; Adamski, J.; Nauck, M.; Völzke, H.; et al. The saliva metabolome in association to oral health status. J. Dent. Res. 2019, 98, 642–651. [Google Scholar] [CrossRef] [PubMed]
- Gardner, A.; Parkes, H.G.; So, P.W.; Carpenter, G.H. Determining bacterial and host contributions to the human salivary metabolome. J. Oral Microbiol. 2019, 11, 1617014. [Google Scholar] [CrossRef] [PubMed]
- Galunska, B.T.; Salim, A.S.; Nikolova, M.N.; Angelova, S.T.; Kiselova-Kaneva, Y.D.; Peev, S.V.; Ivanova, D.G. Gingival status and prophylactic oral hygiene measures modulate salivary amino acids’ profile in children with plaque-induced gingivitis. Turkish J. Biochem. 2023, 49, 47–55. [Google Scholar] [CrossRef]
- Shetty, P.K.; Pattabiraman, T.N. Salivary glycoproteins as indicators of oral diseases. Indian. J. Clin. Biochem. 2004, 19, 97–101. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Wsoo, M.A.; Ahmed, B.M. Evaluation of salivary α-L-Fucose and its related parameters in periodontitis. Zanco J. Med. Sci. 2013, 17, 563–569. [Google Scholar] [CrossRef]
- Roopa, S.; Shivarajashankara, Y.M.; Manjula, S.; Shivashankar, A.R.; Dayakar, M.M. Salivary glycoconjugates as biomarkers of chronic periodontitis. J. Evol. Med. Dent. Sci. 2014, 3, 10542–10550. [Google Scholar]
- Kozak, M.; Pawlik, A. The role of the oral microbiome in the development of diseases. Int. J. Mol. Sci. 2023, 24, 5231. [Google Scholar] [CrossRef]
- Li, X.; Liu, Y.; Yang, X.; Li, C.; Song, Z. The Oral Microbiota: Community Composition, Influencing Factors, Pathogenesis, and Interventions. Front. Microbiol. 2022, 13, 895537. [Google Scholar] [CrossRef]
- Quartieri, E.; Casali, E.; Ferrari, E.; Ghezzi, B.; Gallo, M.; Spisni, A.; Meleti, M.; Pertinhez, T.A. Sample optimization for saliva 1H-NMR metabolic profiling. Anal. Biochem. 2022, 640, 114412. [Google Scholar] [CrossRef] [PubMed]
- Ko, T.J.; Byrd, K.M.; Kim, S.A. The Chairside Periodontal Diagnostic Toolkit: Past, Present, and Future. Diagnostics 2021, 11, 932. [Google Scholar] [CrossRef] [PubMed]
- Nomura, Y.; Morozumi, T.; Nakagawa, T.; Sugaya, T.; Kawanami, M.; Suzuki, F.; Takahashi, K.; Abe, Y.; Sato, S.; Makino-Oi, A.; et al. Site-level progression of periodontal disease during a follow-up period. PLoS ONE 2017, 12, e0188670. [Google Scholar] [CrossRef] [PubMed]
- Cuevas-Córdoba, B.; Santiago-García, J. Saliva: A fluid of study for OMICS. OMICS 2014, 18, 87–97. [Google Scholar] [CrossRef]
- Ono Minagi, H.; Yamanaka, Y.; Sakai, T. Evaluation of the Saxon test for patients with hyposalivation without Sjögren’s syndrome. J. Oral. Rehabil. 2020, 47, 1550–1556. [Google Scholar] [CrossRef]
- Bertoldi, C.; Forabosco, A.; Lalla, M.; Generali, L.; Zaffe, D.; Cortellini, P. How Intraday Index Changes Influence Periodontal Assessment: A preliminary study. Int. J. Dent. 2017, 2017, 7912158. [Google Scholar] [CrossRef] [PubMed]
- Gardner, A.; Parkes, H.G.; Carpenter, G.H.; So, P.W. Developing and standardizing a protocol for quantitative proton nuclear magnetic resonance (1H NMR) spectroscopy of saliva. J. Proteome Res. 2018, 17, 1521–1531. [Google Scholar] [CrossRef]
- Coico, R. Gram staining. Curr. Protoc. Immunol. 2001. [Google Scholar] [CrossRef]
- Gallo, M.; Giovati, L.; Magliani, W.; Pertinhez, T.A.; Conti, S.; Ferrari, E.; Spisni, A.; Ciociola, T. Metabolic plasticity of Candida albicans in response to different environmental conditions. J. Fungi 2022, 8, 723. [Google Scholar] [CrossRef]

| MALE (n = 10) | FEMALE (n = 9) | |
|---|---|---|
| Mean ± SD | Mean ± SD | |
| Age (years) | 23.7 ± 1.3 | 23.6 ± 2.1 |
| BMI (kg/m2) | 23.2 ± 1.4 | 20.9 ± 1.3 |
| Salivary flow a (mL/5 min) | 2.3 ± 1.2 | 2.2 ± 1.5 |
| % FMPS | 12.8 ± 7.1 | 14.1 ± 7.5 |
| % FMBS | 2.6 ± 1.9 | 4.6 ± 3.4 |
| DMFT | 1.7 ± 1.3 | 1.0 ± 1.3 |
| PSR | 0.9 ± 0.3 | 1 ± 0.0 |
| No. of subjects | No. of subjects | |
Drugs:
| ||
| - | 3 b | |
| 10 | 6 | |
Smoke:
| ||
| 2 | 3 | |
| 8 | 6 | |
Alcohol:
| ||
| 4 | 4 | |
| 6 | 5 |
| Metabolite | AUC § | Optimal Cutoff * | p-Value |
|---|---|---|---|
| Pyroglutamate | 0.99 | −0.66 | 0.0025 |
| Maltose | 0.90 | −0.45 | 0.0749 |
| Histidine | 0.88 | −0.24 | 0.0229 |
| Fucose | 0.88 | −0.14 | 0.0184 |
| Phenylalanine | 0.83 | −0.23 | 0.0156 |
| 3-Phenylpropionate | 0.82 | 0.30 | 0.0114 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Antonelli, R.; Ferrari, E.; Gallo, M.; Ciociola, T.; Calciolari, E.; Spisni, A.; Meleti, M.; Pertinhez, T.A. The Association between Salivary Metabolites and Gingival Bleeding Score in Healthy Subjects: A Pilot Study. Int. J. Mol. Sci. 2024, 25, 5448. https://doi.org/10.3390/ijms25105448
Antonelli R, Ferrari E, Gallo M, Ciociola T, Calciolari E, Spisni A, Meleti M, Pertinhez TA. The Association between Salivary Metabolites and Gingival Bleeding Score in Healthy Subjects: A Pilot Study. International Journal of Molecular Sciences. 2024; 25(10):5448. https://doi.org/10.3390/ijms25105448
Chicago/Turabian StyleAntonelli, Rita, Elena Ferrari, Mariana Gallo, Tecla Ciociola, Elena Calciolari, Alberto Spisni, Marco Meleti, and Thelma A. Pertinhez. 2024. "The Association between Salivary Metabolites and Gingival Bleeding Score in Healthy Subjects: A Pilot Study" International Journal of Molecular Sciences 25, no. 10: 5448. https://doi.org/10.3390/ijms25105448
APA StyleAntonelli, R., Ferrari, E., Gallo, M., Ciociola, T., Calciolari, E., Spisni, A., Meleti, M., & Pertinhez, T. A. (2024). The Association between Salivary Metabolites and Gingival Bleeding Score in Healthy Subjects: A Pilot Study. International Journal of Molecular Sciences, 25(10), 5448. https://doi.org/10.3390/ijms25105448










