Molecular Targeting of the BRAF Proto-Oncogene/Mitogen-Activated Protein Kinase (MAPK) Pathway across Cancers
Abstract
1. Introduction
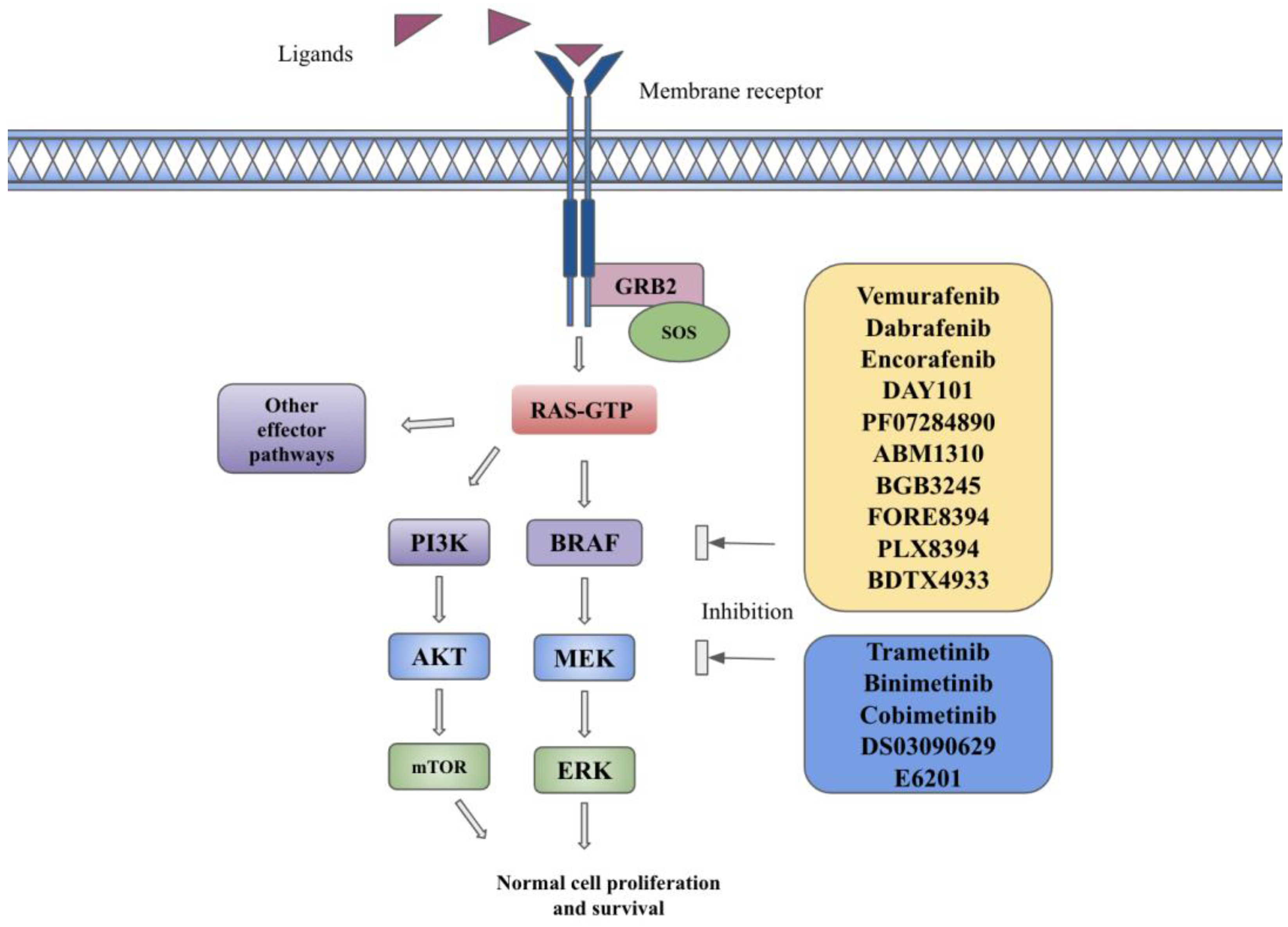
2. MAPK Pathway
3. Alterations in MAPK Pathway Causing Carcinogenesis
4. BRAF/MEK Inhibitors across Various Cancers
4.1. Melanoma
| Study | Phase | Study Population | Number of Patients/ Subgroup | Intervention/Subgroup | PFS Months | OS Months | ORR (%) | DOR Months | FDA Approval/Notes |
|---|---|---|---|---|---|---|---|---|---|
| Chapman et al. BRIM-3 2011 [9,12] | III | Metastatic melanoma with BRAFV600E mutation, treatment-naive | 337 | vemurafenib | 5.3 | 13.6 | 48 | - | 17 August 2011 |
| 338 | dacarbazine | 1.6 | 9.7 | 5 | - | ||||
| Ascierto et al. CoBRIM 2015 [28,29,30] | III | Unresectable or metastatic BRAFV600 mutated melanoma, treatment-naive | 247 | vemurafenib + cobimetinib | 12.3 | 22.3 | 70 | 13 | 10 November 2015 |
| 248 | vemurafenib + placebo | 7.2 | 17.4 | 50 | 9.2 | ||||
| McArthur et al. 2017 [13] | II | Metastatic BRAFV600 mutant melanoma with brain metastasis (BM). Cohort A: previously untreated BM; Cohort B: previously treated BM | Cohort A 90 | vemurafenib | 3.7 | 8.9 | 33 EC 18 IC | 4.1 | EC: extracranial response IC: intracranial response |
| Cohort B 56 | vemurafenib | 4 | 9.6 | 23 EC 18 IC | 4.1 | ||||
| Hauschild et al. BREAK-3 2012 [14,15] | III | Unresectable or metastatic melanoma with BRAFV600E mutation, treatment-naive | 187 | dabrafenib | 6.9 | 18.2 | 50 | 5.5 | 29 May 2013 |
| 63 | dacarbazine | 2.7 | 15.6 | 6 | NR | ||||
| Long et al. BREAK-MB 2012 [16] | II | Unresectable or metastatic melanoma with BRAFV600E or V600K mutation, with brain metastasis Cohort A with no prior local therapy for brain metastasis and Cohort B with prior local therapy | Cohort A 83 | dabrafenib V600E | 16.1 | 33.1 | 39.2 | 20.1 | 29 May 2013 (ORR here is overall intracranial response) |
| V600K | 8.1 | 16.3 | 30.8 | 28.1 | |||||
| Cohort B 139 | dabrafenib V600E | 16.6 | 31.4 | 6.7 | 12.4 | ||||
| V600K | 15.9 | 21.9 | 22.2 | 16.6 | |||||
| Long et al. COMBI-d 2014 [20,23] | III | Unresectable or metastatic BRAFV600E or V600K mutant melanoma | 211 | dabrafenib + trametinib | 9.3 | NR | 68 | 9.2 | 9 January 2014 |
| 212 | dabrafenib + placebo | 8.8 | NR | 55 | 10.2 | ||||
| Robert et al. COMBI-v 2014 [24] | III | Unresectable or metastatic melanoma with BRAFV600E/K mutation, treatment-naive | 353 | dabrafenib + trametinib | 11.4 | NR | 64 | 13.8 | |
| 353 | vemurafenib | 7.3 | 17.2 | 51 | 7.5 | ||||
| Davies et al. COMBI-MB 2017 [25] | II | Metastatic melanoma with BRAFV600E/K mutation with brain metastasis. Cohort A: asymptomatic patients with V600E mutation and no prior local brain therapy. Cohort B: asymptomatic patients with V600E mutation who had prior local therapy. Cohort C: asymptomatic patients with V600D/K/R mutations regardless of prior local therapy. Cohort D: symptomatic patients regardless of local therapy or mutation status | dabrafenib + trametinib | ||||||
| 76 | Cohort A | 5.6 | 10.8 | 58 | 6.5 | ||||
| 16 | Cohort B | 7.2 | 24.3 | 56 | 12.5 | ||||
| 16 | Cohort C | 4.2 | 10.1 | 44 | 6.6 | ||||
| 17 | Cohort D | 5.5 | 11.5 | 65 | 4.5 | ||||
| Long et al. COMBI-AD 2017 [26] | Stage III melanoma with completely resected BRAFV600E/K-mutated tumor | 438 | dabrafenib + trametinib | NR | NR | 37 (recurrence) | 30 April 2018 | ||
| 432 | placebo | NR | NR | 56 (recurrence) | |||||
| Flaherty et al. METRIC 2012 [17,19] | III | Unresectable or metastatic melanoma with BRAFV600E or V600K mutation, treatment-naive and previously treated | 214 | trametinib | 4.9 | 15.6 | 29 | 5.3 | 29 May 2013 |
| 108 | dacarbazine or paclitaxel | 1.5 | 11.3 | 9 | 8.1 | ||||
| Dummer et al. COLUMBUS 2018 [31,33,34] | III | Unresectable or metastatic melanoma, treatment-naive or progressed after first-line immunotherapy | 192 | encorafenib + binimetinib | 14.9 | 33.6 | 63 | 18.6 | 27 June 2018 |
| 194 | encorafenib | 9.6 | 23.5 | 51 | 14.9 | ||||
| 191 | vemurafenib | 7.3 | 16.9 | 40 | 12.3 | ||||
| Salama et al. NCI-MATCH subprotocol H 2020 [35] | II | Previously treated BRAFV600E-mutated tumors, excluding melanoma, thyroid, and colorectal cancer. Responses seen in 7 distinct tumor types | 35 | dabrafenib + trametinib | 11.4 | 28.6 | 38 | 25.1 | 23 June 2022 tumor-agnostic indication for solid tumors |
| Kopetz et al. BEACON CRC 2019 [36,37] | III | BRAFV600E-mutated mCRC, treatment-naive | 220 | encorafenib + cetuximab | 4.3 | 9.3 | 20 | - | 8 April 2020 for encorafenib and cetuximab for mCRC |
| 224 | encorafenib + cetuximab + binimetinib | 4.5 | 9.3 | 26 | - | ||||
| 221 | cetuximab + irinotecan or cetuximab + FOLFIRI | 1.5 | 5.9 | 2 | - | ||||
| Cutsem et al. ANCHOR CRC 2023 [38] | II | BRAFV600E-mutated mCRC, treatment-naive | 95 | encorafenib+ binimetinib+ cetuximab | 5.8 | 18.3 | 47.4 | - | |
| VE-BASKET 2015 [39,40,41,42,43] | BRAFV600-mutated nonmelanoma cancers (26 unique cancer types) | Total 172 | vemurafenib | 5.8 | 17.6 | 32.6 | 13.1 | vemurafenib for ECD on 6 November 2017 | |
| NSCLC (62) | vemurafenib | 6.5 | 15.4 | 37.1 | 7.2 | ||||
| ECD (22)/LCH (4) | vemurafenib | NR | NR | 61.5 | - | ||||
| Glioma (24) | vemurafenib | 5.5 | 28.2 | 25 | - | ||||
| CRC (27) | vemurafenib | 4.5 | 9.3 | 0 | - | ||||
| vemurafenib + cetuximab | 3.7 | 7.1 | 4 | - | |||||
| ATC (7) | vemurafenib | - | - | 29 | - | ||||
| BTC (26) | vemurafenib | - | - | 12 | - | ||||
| Subbiah et al. ROAR Basket trial 2023 [44,45] | II | BRAFV600E mutated rare cancers, ATC, BTC, ASi, LGG, HGG, HCL, MM | ATC (36) | dabrafenib + trametinib | 6.7 | 14.5 | 56 | 14.4 | 4 May 2018 for ATC 23 June 2022 tumor-agnostic indication for solid tumors |
| BTC (43) | dabrafenib + trametinib | 9 | 13.5 | 53 | 8.9 | ||||
| ASi (3) | dabrafenib + trametinib | - | 21.8 | 67 | 7.7 | ||||
| LGG (13) | dabrafenib + trametinib | 9.5 | NR | 54 | NR | ||||
| HGG(45) | dabrafenib + trametinib | 5.5 | 17.6 | 33 | 31.2 | ||||
| HCL (55) | dabrafenib + trametinib | NR | NR | 89 | NR | ||||
| MM (10) | dabrafenib + trametinib | 6.3 | 33.9 | 50 | 11.1 | ||||
| Planchard et al. BRF113928 2016–2017 Updated 2022 [46,47,48] | II | BRAFV600E-mutated metastatic NSCLC. Cohorts A and B: previously treated and Cohort C: treatment-naive | Cohort A (78) | dabrafenib | 5.5 | 12.6 | 33 | 9.6 | 22 June 2017 for dabrafenib and trametinib |
| Cohort B (57) | dabrafenib + trametinib | 10.2 | 18.2 | 68.4 | 9.8 | ||||
| Cohort C (36) | dabrafenib + trametinib | 10.8 | 17.3 | 63.9 | 10.2 | ||||
| Mazieres et al. French AcSe 2020 [49] | II | BRAF-mutated NSCLC cohort, previously treated. Cohort A: BRAF nonV600 mutation. Cohort B: BRAFV600 mutations | Cohort A (15) | vemurafenib | 2.1–6.8 | - | 0 | - | |
| Cohort B (100) | vemurafenib | 5.2 | 10 | 44.8 | 6.4 | ||||
| Riely et al. PHAROS trial 2023 [50] | II | BRAFV600E-mutated metastatic NSCLC. Cohort A: treatment-naive and Cohort B: previously treated | Cohort A (59) | encorafenib + binimetinib | NR | NR | 75 | NR | 12 October 2023 |
| Cohort B (39) | encorafenib + binimetinib | 9.3 | NR | 46 | 16.7 | ||||
| Diamond et al. 2022 [51] | II | ECD/LCH/RDD patients regardless of BRAF mutations | 18 | cobimetinib | NR | - | 89 | NR | 1 November 2022 |
| Whitlock et al. CDRB436A2102 2023 [52] | I/II | R/R BRAFV600-mutated pediatric LCH | 13 | dabrafenib | NR | - | 76.9 | NR | |
| Whiltlock et al. CTMT212X2101 2023 [52] | I/II | R/R BRAFV600-mutated pediatric LCH | 12 | dabrafenib + trametinib | NR | - | 58.3 | NR | |
| Gershenson et al. 2022 [53] | II/ III | Recurrent LGSOC | 130 | trametinib | 13 | 37.6 | 26 | 13.6 | |
| 130 | SOC | 7.2 | 29.2 | 6 | 5.9 | ||||
| Ribas et al. KEYNOTE-022 2020 Updated 2022 [54] | I/II | BRAFV600E/K-mutated melanoma, treatment-naive | 60 | pembrolizumab + dabrafenib + trametinib | 17 | 46.3 | 65 | 30.2 | |
| 60 | dabrafenib + trametinib | 9.9 | 26.3 | 72 | 12.1 | ||||
| Gutzmer et al. IMspire150 2020 Updated 2023 [55] | III | Advanced or metastatic BRAFV600 mutant melanoma | 256 | atezolizumab + vemurafenib + cobimetinib | 15.1 | 39.0 | 67 | 21 | 30 July 2020 |
| 258 | vemurafenib + cobimetinib | 10.6 | 25.8 | 65 | 12.6 |
4.2. Gastrointestinal Cancers
4.2.1. Colorectal Cancer
4.2.2. Biliary Tract Cancers
4.3. Non-Small Cell Lung Cancer
4.4. Hematological Malignancies
4.4.1. Hairy Cell Leukemia
4.4.2. Langerhans Cell Histiocytosis/Erdheim–Chester Disease
4.5. Central Nervous System Tumors
4.6. Thyroid Cancers
4.7. Gynecological Cancers
5. Combinations of BRAF/MEK Inhibitors with Immunotherapy
6. Mechanism of Resistance to BRAF/MEK Inhibitors
7. Novel Agents and Current Ongoing Clinical Trials
8. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Schubert, L.; Mariko, M.L.; Clerc, J.; Huillard, O.; Groussin, L. MAPK Pathway Inhibitors in Thyroid Cancer: Preclinical and Clinical Data. Cancers 2023, 15, 710. [Google Scholar] [CrossRef] [PubMed]
- Sforza, V.; Palumbo, G.; Cascetta, P.; Carillio, G.; Manzo, A.; Montanino, A.; Sandomenico, C.; Costanzo, R.; Esposito, G.; Laudato, F.; et al. BRAF Inhibitors in Non-Small Cell Lung Cancer. Cancers 2022, 14, 4863. [Google Scholar] [CrossRef] [PubMed]
- Dillon, M.; Lopez, A.; Lin, E.; Sales, D.; Perets, R.; Jain, P. Progress on Ras/MAPK Signaling Research and Targeting in Blood and Solid Cancers. Cancers 2021, 13, 5059. [Google Scholar] [CrossRef] [PubMed]
- Bouchè, V.; Aldegheri, G.; Donofrio, C.A.; Fioravanti, A.; Roberts-Thomson, S.; Fox, S.B.; Schettini, F.; Generali, D. BRAF Signaling Inhibition in Glioblastoma: Which Clinical Perspectives? Front. Oncol. 2021, 11, 772052. [Google Scholar] [CrossRef] [PubMed]
- Gouda, M.A.; Subbiah, V. Precision oncology for BRAF-mutant cancers with BRAF and MEK inhibitors: From melanoma to tissue-agnostic therapy. ESMO Open 2023, 8, 100788. [Google Scholar] [CrossRef] [PubMed]
- Pugh, T.J.; Bell, J.L.; Bruce, J.P.; Doherty, G.J.; Galvin, M.; Green, M.F.; Hunter-Zinck, H.; Kumari, P.; Lenoue-Newton, M.L.; Li, M.M.; et al. AACR Project GENIE: 100,000 Cases and Beyond. Cancer Discov. 2022, 12, 2044–2057. [Google Scholar] [CrossRef]
- Szklener, K.; Mazurek, M.; Wieteska, M.; Wacławska, M.; Bilski, M.; Mańdziuk, S. New Directions in the Therapy of Glioblastoma. Cancers 2022, 14, 5377. [Google Scholar] [CrossRef]
- Savoia, P.; Fava, P.; Casoni, F.; Cremona, O. Targeting the ERK Signaling Pathway in Melanoma. Int. J. Mol. Sci. 2019, 20, 1483. [Google Scholar] [CrossRef]
- Chapman, P.B.; Hauschild, A.; Robert, C.; Haanen, J.B.; Ascierto, P.; Larkin, J.; Dummer, R.; Garbe, C.; Testori, A.; Maio, M.; et al. Improved Survival with Vemurafenib in Melanoma with BRAF V600E Mutation. N. Engl. J. Med. 2011, 364, 2507–2516. [Google Scholar] [CrossRef]
- Drugs.com. FDA Approves Zelboraf and Companion Diagnostic Test for Late-Stage Skin Cancer. Available online: https://www.drugs.com/newdrugs/fda-approves-zelboraf-companion-diagnostic-test-late-stage-skin-cancer-2814.html (accessed on 9 November 2023).
- Drugs.com. FDA Approves Tafinlar (Dabrafenib) for Advanced Melanoma. Available online: https://www.drugs.com/newdrugs/fda-approves-tafinlar-dabrafenib-advanced-melanoma-3797.html (accessed on 9 November 2023).
- Chapman, P.B.; Robert, C.; Larkin, J.; Haanen, J.B.; Ribas, A.; Hogg, D.; Hamid, O.; Ascierto, P.A.; Testori, A.; Lorigan, P.C.; et al. Vemurafenib in patients with BRAFV600 mutation-positive metastatic melanoma: Final overall survival results of the randomized BRIM-3 study. Ann. Oncol. 2017, 28, 2581–2587. [Google Scholar] [CrossRef]
- McArthur, G.A.; Maio, M.; Arance, A.; Nathan, P.; Blank, C.; Avril, M.F.; Garbe, C.; Hauschild, A.; Schadendorf, D.; Hamid, O.; et al. Vemurafenib in metastatic melanoma patients with brain metastases: An open-label, single-arm, phase 2, multicentre study. Ann. Oncol. 2017, 28, 634–641. [Google Scholar] [CrossRef] [PubMed]
- Hauschild, A.; Grob, J.-J.; Demidov, L.V.; Jouary, T.; Gutzmer, R.; Millward, M.; Rutkowski, P.; Blank, C.U.; Miller, W.H.; Kaempgen, E.; et al. Dabrafenib in BRAF-mutated metastatic melanoma: A multicentre, open-label, phase 3 randomised controlled trial. Lancet 2012, 380, 358–365. [Google Scholar] [CrossRef] [PubMed]
- Hauschild, A.; Grob, J.J.; Demidov, L.V.; Jouary, T.; Gutzmer, R.; Millward, M.; Rutkowski, P.; Blank, C.U.; Miller, W.H.; Kaempgen, E.; et al. An update on BREAK-3, a phase III, randomized trial: Dabrafenib (DAB) versus dacarbazine (DTIC) in patients with BRAF V600E-positive mutation metastatic melanoma (MM). J. Clin. Oncol. 2013, 31, 9013. [Google Scholar] [CrossRef]
- Long, G.V.; Trefzer, U.; Davies, M.A.; Kefford, R.F.; Ascierto, P.A.; Chapman, P.B.; Puzanov, I.; Hauschild, A.; Robert, C.; Algazi, A.; et al. Dabrafenib in patients with Val600Glu or Val600Lys BRAF-mutant melanoma metastatic to the brain (BREAK-MB): A multicentre, open-label, phase 2 trial. Lancet Oncol. 2012, 13, 1087–1095. [Google Scholar] [CrossRef] [PubMed]
- Flaherty, K.T.; Robert, C.; Hersey, P.; Nathan, P.; Garbe, C.; Milhem, M.; Demidov, L.V.; Hassel, J.C.; Rutkowski, P.; Mohr, P.; et al. Improved Survival with MEK Inhibition in BRAF-Mutated Melanoma. N. Engl. J. Med. 2012, 367, 107–114. [Google Scholar] [CrossRef] [PubMed]
- Drugs.com. FDA Approves Mekinist (Trametinib) for Advanced Melanoma. Available online: https://www.drugs.com/newdrugs/fda-approves-mekinist-trametinib-advanced-melanoma-3798.html (accessed on 9 November 2023).
- Robert, C.; Flaherty, K.; Nathan, P.; Hersey, P.; Garbe, C.; Milhem, M.; Demidov, L.; Mohr, P.; Hassel, J.C.; Rutkowski, P.; et al. Five-year outcomes from a phase 3 METRIC study in patients with BRAF V600 E/K–mutant advanced or metastatic melanoma. Eur. J. Cancer 2019, 109, 61–69. [Google Scholar] [CrossRef]
- Long, G.V.; Stroyakovskiy, D.; Gogas, H.; Levchenko, E.; De Braud, F.; Larkin, J.; Garbe, C.; Jouary, T.; Hauschild, A.; Grob, J.J.; et al. Combined BRAF and MEK Inhibition versus BRAF Inhibition Alone in Melanoma. N. Engl. J. Med. 2014, 371, 1877–1888. [Google Scholar] [CrossRef] [PubMed]
- Drugs.com. GSK Gains Accelerated FDA Approval for Combination Use of Mekinist (Trametinib) and Tafinlar (Dabrafenib). Available online: https://www.drugs.com/newdrugs/gsk-gains-accelerated-fda-approval-combination-mekinist-trametinib-tafinlar-dabrafenib-4003.html (accessed on 9 November 2023).
- Drugs.com. FDA Approves Cotellic (Cobimetinib) for the Combination Treatment of Advanced Melanoma. Available online: https://www.drugs.com/newdrugs/fda-approves-cotellic-cobimetinib-combination-advanced-melanoma-4295.html (accessed on 9 November 2023).
- Long, G.V.; Flaherty, K.T.; Stroyakovskiy, D.; Gogas, H.; Levchenko, E.; de Braud, F.; Larkin, J.; Garbe, C.; Jouary, T.; Hauschild, A.; et al. Dabrafenib plus trametinib versus dabrafenib monotherapy in patients with metastatic BRAF V600E/K-mutant melanoma: Long-term survival and safety analysis of a phase 3 study. Ann. Oncol. 2017, 28, 1631–1639. [Google Scholar] [CrossRef]
- Robert, C.; Karaszewska, B.; Schachter, J.; Rutkowski, P.; Mackiewicz, A.; Stroiakovski, D.; Lichinitser, M.; Dummer, R.; Grange, F.; Mortier, L.; et al. Improved Overall Survival in Melanoma with Combined Dabrafenib and Trametinib. N. Engl. J. Med. 2015, 372, 30–39. [Google Scholar] [CrossRef]
- Davies, M.A.; Saiag, P.; Robert, C.; Grob, J.-J.; Flaherty, K.T.; Arance, A.; Chiarion-Sileni, V.; Thomas, L.; Lesimple, T.; Mortier, L.; et al. Dabrafenib plus trametinib in patients with BRAFV600-mutant melanoma brain metastases (COMBI-MB): A multicentre, multicohort, open-label, phase 2 trial. Lancet Oncol. 2017, 18, 863–873. [Google Scholar] [CrossRef]
- Long, G.V.; Hauschild, A.; Santinami, M.; Atkinson, V.; Mandalà, M.; Chiarion-Sileni, V.; Larkin, J.; Nyakas, M.; Dutriaux, C.; Haydon, A.; et al. Adjuvant Dabrafenib plus Trametinib in Stage III BRAF-Mutated Melanoma. N. Engl. J. Med. 2017, 377, 1813–1823. [Google Scholar] [CrossRef] [PubMed]
- Drugs.com. Novartis Receives FDA Approval of Tafinlar + Mekinist for Adjuvant Treatment of BRAF V600-Mutant Melanoma. Available online: https://www.drugs.com/newdrugs/novartis-receives-fda-approval-tafinlar-mekinist-adjuvant-braf-v600-mutant-melanoma-4733.html (accessed on 9 November 2023).
- Larkin, J.; Ascierto, P.A.; Dréno, B.; Atkinson, V.; Liszkay, G.; Maio, M.; Mandalà, M.; Demidov, L.; Stroyakovskiy, D.; Thomas, L.; et al. Combined Vemurafenib and Cobimetinib in BRAF-Mutated Melanoma. N. Engl. J. Med. 2014, 371, 1867–1876. [Google Scholar] [CrossRef] [PubMed]
- Ascierto, P.A.; McArthur, G.A.; Dréno, B.; Atkinson, V.; Liszkay, G.; Di Giacomo, A.M.; Mandalà, M.; Demidov, L.; Stroyakovskiy, D.; Thomas, L.; et al. Cobimetinib combined with vemurafenib in advanced BRAFV600-mutant melanoma (coBRIM): Updated efficacy results from a randomised, double-blind, phase 3 trial. Lancet Oncol. 2016, 17, 1248–1260. [Google Scholar] [CrossRef] [PubMed]
- Ascierto, P.A.; Dréno, B.; Larkin, J.; Ribas, A.; Liszkay, G.; Maio, M.; Mandalà, M.; Demidov, L.; Stroyakovskiy, D.; Thomas, L.; et al. 5-Year Outcomes with Cobimetinib plus Vemurafenib in BRAFV600 Mutation–Positive Advanced Melanoma: Extended Follow-up of the coBRIM Study. Clin. Cancer Res. 2021, 27, 5225–5235. [Google Scholar] [CrossRef] [PubMed]
- Dummer, R.; Ascierto, P.A.; Gogas, H.J.; Arance, A.; Mandala, M.; Liszkay, G.; Garbe, C.; Schadendorf, D.; Krajsova, I.; Gutzmer, R.; et al. Encorafenib plus binimetinib versus vemurafenib or encorafenib in patients with BRAF-mutant melanoma (COLUMBUS): A multicentre, open-label, randomised phase 3 trial. Lancet Oncol. 2018, 19, 603–615. [Google Scholar] [CrossRef] [PubMed]
- Drugs.com. Array BioPharma Announces FDA Approval of Braftovi (Encorafenib) in Combination with Mektovi (Binimetinib) for Unresectable or Metastatic Melanoma with BRAF Mutations. Available online: https://www.drugs.com/newdrugs/array-biopharma-announces-fda-approval-braftovi-encorafenib-combination-mektovi-binimetinib-4771.html (accessed on 9 November 2023).
- Dummer, R.; Ascierto, P.A.; Gogas, H.J.; Arance, A.; Mandala, M.; Liszkay, G.; Garbe, C.; Schadendorf, D.; Krajsova, I.; Gutzmer, R.; et al. Overall survival in patients with BRAF-mutant melanoma receiving encorafenib plus binimetinib versus vemurafenib or encorafenib (COLUMBUS): A multicentre, open-label, randomised, phase 3 trial. Lancet Oncol. 2018, 19, 1315–1327. [Google Scholar] [CrossRef] [PubMed]
- Dummer, R.; Flaherty, K.T.; Robert, C.; Arance, A.; De Groot, J.W.B.; Garbe, C.; Gogas, H.J.; Gutzmer, R.; Krajsová, I.; Liszkay, G.; et al. COLUMBUS 5-Year Update: A Randomized, Open-Label, Phase III Trial of Encorafenib Plus Binimetinib Versus Vemurafenib or Encorafenib in Patients with BRAF V600–Mutant Melanoma. J. Clin. Oncol. 2022, 40, 4178–4188. [Google Scholar] [CrossRef]
- Salama, A.K.S.; Li, S.; Macrae, E.R.; Park, J.-I.; Mitchell, E.P.; Zwiebel, J.A.; Chen, H.X.; Gray, R.J.; McShane, L.M.; Rubinstein, L.V.; et al. Dabrafenib and Trametinib in Patients with Tumors with BRAFV600E Mutations: Results of the NCI-MATCH Trial Subprotocol H. J. Clin. Oncol. 2020, 38, 3895–3904. [Google Scholar] [CrossRef]
- Kopetz, S.; Grothey, A.; Yaeger, R.; Van Cutsem, E.; Desai, J.; Yoshino, T.; Wasan, H.; Ciardiello, F.; Loupakis, F.; Hong, Y.S.; et al. Encorafenib, Binimetinib, and Cetuximab in BRAF V600E–Mutated Colorectal Cancer. N. Engl. J. Med. 2019, 381, 1632–1643. [Google Scholar] [CrossRef]
- Tabernero, J.; Grothey, A.; Van Cutsem, E.; Yaeger, R.; Wasan, H.; Yoshino, T.; Desai, J.; Ciardiello, F.; Loupakis, F.; Hong, Y.S.; et al. Encorafenib Plus Cetuximab as a New Standard of Care for Previously Treated BRAF V600E–Mutant Metastatic Colorectal Cancer: Updated Survival Results and Subgroup Analyses from the BEACON Study. J. Clin. Oncol. 2021, 39, 273–284. [Google Scholar] [CrossRef]
- Van Cutsem, E.; Taieb, J.; Yaeger, R.; Yoshino, T.; Grothey, A.; Maiello, E.; Elez, E.; Dekervel, J.; Ross, P.; Ruiz-Casado, A.; et al. ANCHOR CRC: Results From a Single-Arm, Phase II Study of Encorafenib Plus Binimetinib and Cetuximab in Previously Untreated BRAF(V600E)-Mutant Metastatic Colorectal Cancer. J. Clin. Oncol. 2023, 41, 2628–2637. [Google Scholar] [CrossRef] [PubMed]
- Subbiah, V.; Puzanov, I.; Blay, J.-Y.; Chau, I.; Lockhart, A.C.; Raje, N.S.; Wolf, J.; Baselga, J.; Meric-Bernstam, F.; Roszik, J.; et al. Pan-Cancer Efficacy of Vemurafenib in BRAFV600-Mutant Non-Melanoma Cancers. Cancer Discov. 2020, 10, 657–663. [Google Scholar] [CrossRef] [PubMed]
- Kaley, T.; Touat, M.; Subbiah, V.; Hollebecque, A.; Rodon, J.; Lockhart, A.C.; Keedy, V.; Bielle, F.; Hofheinz, R.-D.; Joly, F.; et al. BRAF Inhibition in BRAFV600-Mutant Gliomas: Results From the VE-BASKET Study. J. Clin. Oncol. 2018, 36, 3477–3484. [Google Scholar] [CrossRef] [PubMed]
- Subbiah, V.; Gervais, R.; Riely, G.; Hollebecque, A.; Blay, J.-Y.; Felip, E.; Schuler, M.; Gonçalves, A.; Italiano, A.; Keedy, V.; et al. Efficacy of Vemurafenib in Patients with Non–Small-Cell Lung Cancer with BRAFV600 Mutation: An Open-Label, Single-Arm Cohort of the Histology-Independent VE-BASKET Study. JCO Precis. Oncol. 2019, 3, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Diamond, E.L.; Subbiah, V.; Lockhart, A.C.; Blay, J.-Y.; Puzanov, I.; Chau, I.; Raje, N.S.; Wolf, J.; Erinjeri, J.P.; Torrisi, J.; et al. Vemurafenib for BRAF V600–Mutant Erdheim-Chester Disease and Langerhans Cell Histiocytosis. JAMA Oncol. 2018, 4, 384. [Google Scholar] [CrossRef] [PubMed]
- Hyman, D.M.; Puzanov, I.; Subbiah, V.; Faris, J.E.; Chau, I.; Blay, J.-Y.; Wolf, J.; Raje, N.S.; Diamond, E.L.; Hollebecque, A.; et al. Vemurafenib in Multiple Nonmelanoma Cancers with BRAF V600 Mutations. N. Engl. J. Med. 2015, 373, 726–736. [Google Scholar] [CrossRef] [PubMed]
- Subbiah, V.; Kreitman, R.J.; Wainberg, Z.A.; Gazzah, A.; Lassen, U.; Stein, A.; Wen, P.Y.; Dietrich, S.; De Jonge, M.J.A.; Blay, J.-Y.; et al. Dabrafenib plus trametinib in BRAFV600E-mutated rare cancers: The phase 2 ROAR trial. Nat. Med. 2023, 29, 1103–1112. [Google Scholar] [CrossRef]
- Kreitman, R.J.; Moreau, P.; Ravandi, F.; Hutchings, M.; Gazzah, A.; Michallet, A.-S.; Wainberg, Z.A.; Stein, A.; Dietrich, S.; de Jonge, M.J.A.; et al. Dabrafenib plus trametinib in patients with relapsed/refractory BRAF V600E mutation–positive hairy cell leukemia. Blood 2023, 141, 996–1006. [Google Scholar] [CrossRef]
- Planchard, D.; Besse, B.; Groen, H.J.M.; Hashemi, S.M.S.; Mazieres, J.; Kim, T.M.; Quoix, E.; Souquet, P.-J.; Barlesi, F.; Baik, C.; et al. Phase 2 Study of Dabrafenib Plus Trametinib in Patients with BRAF V600E-Mutant Metastatic NSCLC: Updated 5-Year Survival Rates and Genomic Analysis. J. Thorac. Oncol. 2022, 17, 103–115. [Google Scholar] [CrossRef]
- Planchard, D.; Besse, B.; Groen, H.J.M.; Souquet, P.-J.; Quoix, E.; Baik, C.S.; Barlesi, F.; Kim, T.M.; Mazieres, J.; Novello, S.; et al. Dabrafenib plus trametinib in patients with previously treated BRAFV600E-mutant metastatic non-small cell lung cancer: An open-label, multicentre phase 2 trial. Lancet Oncol. 2016, 17, 984–993. [Google Scholar] [CrossRef]
- Planchard, D.; Smit, E.F.; Groen, H.J.M.; Mazieres, J.; Besse, B.; Helland, Å.; Giannone, V.; D’Amelio, A.M.; Zhang, P.; Mookerjee, B.; et al. Dabrafenib plus trametinib in patients with previously untreated BRAFV600E-mutant metastatic non-small-cell lung cancer: An open-label, phase 2 trial. Lancet Oncol. 2017, 18, 1307–1316. [Google Scholar] [CrossRef] [PubMed]
- Mazieres, J.; Cropet, C.; Montané, L.; Barlesi, F.; Souquet, P.J.; Quantin, X.; Dubos-Arvis, C.; Otto, J.; Favier, L.; Avrillon, V.; et al. Vemurafenib in non-small-cell lung cancer patients with BRAFV600 and BRAFnonV600 mutations. Ann. Oncol. 2020, 31, 289–294. [Google Scholar] [CrossRef] [PubMed]
- Riely, G.J.; Smit, E.F.; Ahn, M.-J.; Felip, E.; Ramalingam, S.S.; Tsao, A.; Johnson, M.; Gelsomino, F.; Esper, R.; Nadal, E.; et al. Phase II, Open-Label Study of Encorafenib Plus Binimetinib in Patients with BRAFV600-Mutant Metastatic Non–Small-Cell Lung Cancer. J. Clin. Oncol. 2023, 41, 3700–3711. [Google Scholar] [CrossRef] [PubMed]
- Diamond, E.L.; Durham, B.H.; Ulaner, G.A.; Drill, E.; Buthorn, J.; Ki, M.; Bitner, L.; Cho, H.; Young, R.J.; Francis, J.H.; et al. Efficacy of MEK inhibition in patients with histiocytic neoplasms. Nature 2019, 567, 521–524. [Google Scholar] [CrossRef] [PubMed]
- Whitlock, J.A.; Geoerger, B.; Dunkel, I.J.; Roughton, M.; Choi, J.; Osterloh, L.; Russo, M.; Hargrave, D. Dabrafenib, alone or in combination with trametinib, in BRAF V600–mutated pediatric Langerhans cell histiocytosis. Blood Adv. 2023, 7, 3806–3815. [Google Scholar] [CrossRef] [PubMed]
- Gershenson, D.M.; Miller, A.; Brady, W.E.; Paul, J.; Carty, K.; Rodgers, W.; Millan, D.; Coleman, R.L.; Moore, K.N.; Banerjee, S.; et al. Trametinib versus standard of care in patients with recurrent low-grade serous ovarian cancer (GOG 281/LOGS): An international, randomised, open-label, multicentre, phase 2/3 trial. Lancet 2022, 399, 541–553. [Google Scholar] [CrossRef] [PubMed]
- Ribas, A.; Ferrucci, P.F.; Atkinson, V.; Stephens, R.; Long, G.V.; Lawrence, D.P.; Del Vecchio, M.; Hamid, O.; Schmidt, H.; Schachter, J.; et al. Pembrolizumab (pembro) plus dabrafenib (dab) and trametinib (tram) in BRAFV600E/K-mutant melanoma: Long-term follow-up of KEYNOTE-022 parts 1, 2, and 3. J. Clin. Oncol. 2022, 40, 9516. [Google Scholar] [CrossRef]
- Gutzmer, R.; Stroyakovskiy, D.; Gogas, H.; Robert, C.; Lewis, K.; Protsenko, S.; Pereira, R.P.; Eigentler, T.; Rutkowski, P.; Demidov, L.; et al. Atezolizumab, vemurafenib, and cobimetinib as first-line treatment for unresectable advanced BRAF(V600) mutation-positive melanoma (IMspire150): Primary analysis of the randomised, double-blind, placebo-controlled, phase 3 trial. Lancet 2020, 395, 1835–1844. [Google Scholar] [CrossRef]
- Ros, J.; Baraibar, I.; Sardo, E.; Mulet, N.; Salvà, F.; Argilés, G.; Martini, G.; Ciardiello, D.; Cuadra, J.L.; Tabernero, J.; et al. BRAF, MEK and EGFR inhibition as treatment strategies in BRAF V600E metastatic colorectal cancer. Ther. Adv. Med. Oncol. 2021, 13, 175883592199297. [Google Scholar] [CrossRef]
- Drugs.com. FDA Approves Braftovi (Encorafenib) in Combination with Cetuximab for the Treatment of BRAFV600E-Mutant Metastatic Colorectal Cancer (CRC) after Prior Therapy. Available online: https://www.drugs.com/newdrugs/fda-approves-braftovi-encorafenib-combination-cetuximab-brafv600e-mutant-metastatic-colorectal-5201.html (accessed on 9 November 2023).
- Van Cutsem, E.; Huijberts, S.; Grothey, A.; Yaeger, R.; Cuyle, P.-J.; Elez, E.; Fakih, M.; Montagut, C.; Peeters, M.; Yoshino, T.; et al. Binimetinib, Encorafenib, and Cetuximab Triplet Therapy for Patients with BRAF V600E–Mutant Metastatic Colorectal Cancer: Safety Lead-In Results From the Phase III BEACON Colorectal Cancer Study. J. Clin. Oncol. 2019, 37, 1460–1469. [Google Scholar] [CrossRef]
- Kopetz, S.; Grothey, A.; Yaeger, R.; Ciardiello, F.; Desai, J.; Kim, T.W.; Maughan, T.; Cutsem, E.V.; Wasan, H.S.; Yoshino, T.; et al. BREAKWATER: Randomized phase 3 study of encorafenib (enco) + cetuximab (cetux) ± chemotherapy for first-line (1L) treatment (tx) of BRAF V600E-mutant (BRAFV600E) metastatic colorectal cancer (mCRC). J. Clin. Oncol. 2021, 39, TPS3619. [Google Scholar] [CrossRef]
- Lamarca, A.; Edeline, J.; Goyal, L. How I treat biliary tract cancer. ESMO Open 2022, 7, 100378. [Google Scholar] [CrossRef] [PubMed]
- Subbiah, V.; Lassen, U.; Élez, E.; Italiano, A.; Curigliano, G.; Javle, M.; de Braud, F.; Prager, G.W.; Greil, R.; Stein, A.; et al. Dabrafenib plus trametinib in patients with BRAFV600E-mutated biliary tract cancer (ROAR): A phase 2, open-label, single-arm, multicentre basket trial. Lancet Oncol. 2020, 21, 1234–1243. [Google Scholar] [CrossRef] [PubMed]
- Jain, A.; Kwong, L.N.; Javle, M. Genomic Profiling of Biliary Tract Cancers and Implications for Clinical Practice. Curr. Treat. Options Oncol. 2016, 17, 58. [Google Scholar] [CrossRef] [PubMed]
- Drugs.com. Novartis Tafinlar + Mekinist Receives FDA Approval for First Tumor-Agnostic Indication for BRAF V600E Solid Tumors. Available online: https://www.drugs.com/newdrugs/novartis-tafinlar-mekinist-receives-fda-approval-first-tumor-agnostic-indication-braf-v600e-solid-5857.html (accessed on 9 November 2023).
- Negrao, M.V.; Raymond, V.M.; Lanman, R.B.; Robichaux, J.P.; He, J.; Nilsson, M.B.; Ng, P.K.S.; Amador, B.E.; Roarty, E.B.; Nagy, R.J.; et al. Molecular Landscape of BRAF-Mutant NSCLC Reveals an Association Between Clonality and Driver Mutations and Identifies Targetable Non-V600 Driver Mutations. J. Thorac. Oncol. 2020, 15, 1611–1623. [Google Scholar] [CrossRef] [PubMed]
- Guaitoli, G.; Zullo, L.; Tiseo, M.; Dankner, M.; Rose, A.A.; Facchinetti, F. Non-small-cell lung cancer: How to manage BRAF-mutated disease. Drugs Context 2023, 12. [Google Scholar] [CrossRef] [PubMed]
- Dudnik, E.; Peled, N.; Nechushtan, H.; Wollner, M.; Onn, A.; Agbarya, A.; Moskovitz, M.; Keren, S.; Popovits-Hadari, N.; Urban, D.; et al. BRAF Mutant Lung Cancer: Programmed Death Ligand 1 Expression, Tumor Mutational Burden, Microsatellite Instability Status, and Response to Immune Check-Point Inhibitors. J. Thorac. Oncol. 2018, 13, 1128–1137. [Google Scholar] [CrossRef]
- Reddy, V.P.; Gay, L.M.; Elvin, J.A.; Vergilio, J.-A.; Suh, J.; Ramkissoon, S.; Daniel, S.; Severson, E.A.; Ali, S.M.; Schrock, A.B.; et al. BRAF fusions in clinically advanced non-small cell lung cancer: An emerging target for anti-BRAF therapies. J. Clin. Oncol. 2017, 35, 9072. [Google Scholar] [CrossRef]
- Arcila, M.E.; Drilon, A.; Sylvester, B.E.; Lovly, C.M.; Borsu, L.; Reva, B.; Kris, M.G.; Solit, D.B.; Ladanyi, M. MAP2K1 (MEK1) Mutations Define a Distinct Subset of Lung Adenocarcinoma Associated with Smoking. Clin. Cancer Res. 2015, 21, 1935–1943. [Google Scholar] [CrossRef]
- FDA.gov. FDA Grants Regular Approval to Dabrafenib and Trametinib Combination for Metastatic NSCLC with BRAF V600E Mutation. Available online: https://www.fda.gov/drugs/resources-information-approved-drugs/fda-grants-regular-approval-dabrafenib-and-trametinib-combination-metastatic-nsclc-braf-v600e (accessed on 9 September 2023).
- Garutti, M.; Bergnach, M.; Polesel, J.; Palmero, L.; Pizzichetta, M.A.; Puglisi, F. BRAF and MEK Inhibitors and Their Toxicities: A Meta-Analysis. Cancers 2022, 15, 141. [Google Scholar] [CrossRef]
- Drugs.com. FDA Approves Braftovi (Encorafenib) with Mektovi (Binimetinib) for Metastatic Non-Small Cell Lung Cancer with a BRAF V600E Mutation. Available online: https://www.drugs.com/newdrugs/fda-approves-braftovi-encorafenib-mektovi-binimetinib-metastatic-non-small-cell-lung-cancer-braf-6111.html (accessed on 18 November 2023).
- Tiacci, E.; Trifonov, V.; Schiavoni, G.; Holmes, A.; Kern, W.; Martelli, M.P.; Pucciarini, A.; Bigerna, B.; Pacini, R.; Wells, V.A.; et al. BRAF Mutations in Hairy-Cell Leukemia. N. Engl. J. Med. 2011, 364, 2305–2315. [Google Scholar] [CrossRef] [PubMed]
- Tiacci, E.; Schiavoni, G.; Forconi, F.; Santi, A.; Trentin, L.; Ambrosetti, A.; Cecchini, D.; Sozzi, E.; Francia di Celle, P.; Di Bello, C.; et al. Simple genetic diagnosis of hairy cell leukemia by sensitive detection of the BRAF-V600E mutation. Blood 2012, 119, 192–195. [Google Scholar] [CrossRef] [PubMed]
- Tiacci, E.; Schiavoni, G.; Martelli, M.P.; Boveri, E.; Pacini, R.; Tabarrini, A.; Zibellini, S.; Santi, A.; Pettirossi, V.; Fortini, E.; et al. Constant activation of the RAF-MEK-ERK pathway as a diagnostic and therapeutic target in hairy cell leukemia. Haematologica 2013, 98, 635–639. [Google Scholar] [CrossRef] [PubMed]
- Mason, E.F.; Brown, R.D.; Szeto, D.P.; Gibson, C.J.; Jia, Y.; Garcia, E.P.; Jacobson, C.A.; Dal Cin, P.; Kuo, F.C.; Pinkus, G.S.; et al. Detection of activating MAP2K1 mutations in atypical hairy cell leukemia and hairy cell leukemia variant. Leuk. Lymphoma 2017, 58, 233–236. [Google Scholar] [CrossRef]
- Tiacci, E.; Park, J.H.; De Carolis, L.; Chung, S.S.; Broccoli, A.; Scott, S.; Zaja, F.; Devlin, S.; Pulsoni, A.; Chung, Y.R.; et al. Targeting Mutant BRAF in Relapsed or Refractory Hairy-Cell Leukemia. N. Engl. J. Med. 2015, 373, 1733–1747. [Google Scholar] [CrossRef]
- Tiacci, E.; De Carolis, L.; Simonetti, E.; Capponi, M.; Ambrosetti, A.; Lucia, E.; Antolino, A.; Pulsoni, A.; Ferrari, S.; Zinzani, P.L.; et al. Vemurafenib plus Rituximab in Refractory or Relapsed Hairy-Cell Leukemia. N. Engl. J. Med. 2021, 384, 1810–1823. [Google Scholar] [CrossRef] [PubMed]
- Aaroe, A.; Kurzrock, R.; Goyal, G.; Goodman, A.M.; Patel, H.; Ruan, G.; Ulaner, G.; Young, J.; Li, Z.; Dustin, D.; et al. Successful treatment of non-Langerhans cell histiocytosis with the MEK inhibitor trametinib: A multicenter analysis. Blood Adv. 2023, 7, 3984–3992. [Google Scholar] [CrossRef] [PubMed]
- Drugs.com. FDA Approves Zelboraf (Vemurafenib) for Erdheim-Chester Disease with BRAF V600 Mutation. Available online: https://www.drugs.com/newdrugs/fda-approves-zelboraf-vemurafenib-erdheim-chester-braf-v600-mutation-4625.html (accessed on 18 November 2023).
- Drugs.com. FDA Approves Oral MEK Inhibitor Cobimetinib for Histiocytic Neoplasms, Research Led by Memorial Sloan Kettering Cancer Center. Available online: https://www.drugs.com/newdrugs/fda-approves-oral-mek-inhibitor-cobimetinib-histiocytic-neoplasms-research-led-memorial-sloan-5984.html (accessed on 18 November 2023).
- Di Nunno, V.; Gatto, L.; Tosoni, A.; Bartolini, S.; Franceschi, E. Implications of BRAF V600E mutation in gliomas: Molecular considerations, prognostic value and treatment evolution. Front. Oncol. 2022, 12, 1067252. [Google Scholar] [CrossRef]
- Wen, P.Y.; Stein, A.; van den Bent, M.; De Greve, J.; Wick, A.; de Vos, F.Y.F.L.; von Bubnoff, N.; van Linde, M.E.; Lai, A.; Prager, G.W.; et al. Dabrafenib plus trametinib in patients with BRAFV600E-mutant low-grade and high-grade glioma (ROAR): A multicentre, open-label, single-arm, phase 2, basket trial. Lancet Oncol. 2022, 23, 53–64. [Google Scholar] [CrossRef]
- Brose, M.S.; Cabanillas, M.E.; Cohen, E.E.W.; Wirth, L.J.; Riehl, T.; Yue, H.; Sherman, S.I.; Sherman, E.J. Vemurafenib in patients with BRAFV600E-positive metastatic or unresectable papillary thyroid cancer refractory to radioactive iodine: A non-randomised, multicentre, open-label, phase 2 trial. Lancet Oncol. 2016, 17, 1272–1282. [Google Scholar] [CrossRef]
- Sukrithan, V.; Jain, P.; Shah, M.H.; Konda, B. Kinase inhibitors in thyroid cancers. Endocr. Oncol. 2023, 3, e220062. [Google Scholar] [CrossRef] [PubMed]
- Leboulleux, S.; Benisvy, D.; Taieb, D.; Attard, M.; Bournaud, C.; Terroir, M.; Al Ghuzlan, A.; Lamartina, L.; Schlumberger, M.J.; Godbert, Y.; et al. 1743MO MERAIODE: A redifferentiation phase II trial with trametinib followed by radioactive iodine for metastatic radioactive iodine refractory differentiated thyroid cancer patients with a RAS mutation. Ann. Oncol. 2021, 32, S1204. [Google Scholar] [CrossRef]
- Leboulleux, S.; Benisvy, D.; Taieb, D.; Attard, M.; Bournaud, C.; Terroir-Cassou-Mounat, M.; Lacroix, L.; Anizan, N.; Schiazza, A.; Garcia, M.E.; et al. MERAIODE: A Phase II Redifferentiation Trial with Trametinib and 131 I in Metastatic Radioactive Iodine Refractory RAS Mutated Differentiated Thyroid Cancer. Thyroid 2023, 33, 1124–1129. [Google Scholar] [CrossRef] [PubMed]
- Drugs.com. FDA Approves Tafinlar + Mekinist for the Treatment of BRAF-Positive Anaplastic Thyroid Cancer. Available online: https://www.drugs.com/newdrugs/fda-approves-tafinlar-mekinist-braf-positive-anaplastic-thyroid-cancer-4737.html (accessed on 18 November 2023).
- Subbiah, V.; Kreitman, R.J.; Wainberg, Z.A.; Cho, J.Y.; Schellens, J.H.M.; Soria, J.C.; Wen, P.Y.; Zielinski, C.; Cabanillas, M.E.; Urbanowitz, G.; et al. Dabrafenib and Trametinib Treatment in Patients with Locally Advanced or Metastatic BRAF V600–Mutant Anaplastic Thyroid Cancer. J. Clin. Oncol. 2018, 36, 7–13. [Google Scholar] [CrossRef] [PubMed]
- Grisham, R.N.; Vergote, I.; Banerjee, S.; Drill, E.; Kalbacher, E.; Mirza, M.R.; Romero, I.; Vuylsteke, P.; Coleman, R.L.; Hilpert, F.; et al. Molecular Results and Potential Biomarkers Identified from the Phase 3 MILO/ENGOT-ov11 Study of Binimetinib versus Physician Choice of Chemotherapy in Recurrent Low-Grade Serous Ovarian Cancer. Clin. Cancer Res. 2023, 29, 4068–4075. [Google Scholar] [CrossRef] [PubMed]
- Moujaber, T.; Balleine, R.L.; Gao, B.; Madsen, I.; Harnett, P.R.; DeFazio, A. New therapeutic opportunities for women with low-grade serous ovarian cancer. Endocr. Relat. Cancer 2021, 29, R1–R16. [Google Scholar] [CrossRef]
- Monk, B.J.; Grisham, R.N.; Banerjee, S.; Kalbacher, E.; Mirza, M.R.; Romero, I.; Vuylsteke, P.; Coleman, R.L.; Hilpert, F.; Oza, A.M.; et al. MILO/ENGOT-ov11: Binimetinib Versus Physician’s Choice Chemotherapy in Recurrent or Persistent Low-Grade Serous Carcinomas of the Ovary, Fallopian Tube, or Primary Peritoneum. J. Clin. Oncol. 2020, 38, 3753–3762. [Google Scholar] [CrossRef]
- Dummer, R.; Queirolo, P.; Gerard Duhard, P.; Hu, Y.; Wang, D.; de Azevedo, S.J.; Robert, C.; Ascierto, P.A.; Chiarion-Sileni, V.; Pronzato, P.; et al. Atezolizumab, vemurafenib, and cobimetinib in patients with melanoma with CNS metastases (TRICOTEL): A multicentre, open-label, single-arm, phase 2 study. Lancet Oncol. 2023, 23, 1145–1155. [Google Scholar] [CrossRef]
- Drugs.com. FDA Approves Genentech’s Tecentriq plus Cotellic and Zelboraf for People with Advanced Melanoma. Available online: https://www.drugs.com/newdrugs/fda-approves-genentech-s-tecentriq-plus-cotellic-zelboraf-advanced-melanoma-5311.html (accessed on 18 November 2023).
- Dummer, R.; Long, G.V.; Robert, C.; Tawbi, H.A.; Flaherty, K.T.; Ascierto, P.A.; Nathan, P.D.; Rutkowski, P.; Leonov, O.; Dutriaux, C.; et al. Randomized Phase III Trial Evaluating Spartalizumab Plus Dabrafenib and Trametinib for BRAF V600–Mutant Unresectable or Metastatic Melanoma. J. Clin. Oncol. 2022, 40, 1428–1438. [Google Scholar] [CrossRef]
- Ferrucci, P.F.; Di Giacomo, A.M.; Del Vecchio, M.; Atkinson, V.; Schmidt, H.; Schachter, J.; Queirolo, P.; Long, G.V.; Stephens, R.; Svane, I.M.; et al. KEYNOTE-022 part 3: A randomized, double-blind, phase 2 study of pembrolizumab, dabrafenib, and trametinib in BRAF-mutant melanoma. J. ImmunoTherapy Cancer 2020, 8, e001806. [Google Scholar] [CrossRef]
- Schadendorf, D.; Dummer, R.; Robert, C.; Ribas, A.; Sullivan, R.J.; Panella, T.; McKean, M.; Santos, E.S.; Brill, K.; Polli, A.; et al. STARBOARD: Encorafenib + binimetinib + pembrolizumab for first-line metastatic/unresectable BRAF V600-mutant melanoma. Future Oncol. 2022, 18, 2041–2051. [Google Scholar] [CrossRef] [PubMed]
- Tangella, L.P.; Clark, M.E.; Gray, E.S. Resistance mechanisms to targeted therapy in BRAF-mutant melanoma—A mini review. Biochim. Biophys. Acta (BBA)—Gen. Subj. 2021, 1865, 129736. [Google Scholar] [CrossRef] [PubMed]
- Johnson, D.B.; Menzies, A.M.; Zimmer, L.; Eroglu, Z.; Ye, F.; Zhao, S.; Rizos, H.; Sucker, A.; Scolyer, R.A.; Gutzmer, R.; et al. Acquired BRAF inhibitor resistance: A multicenter meta-analysis of the spectrum and frequencies, clinical behaviour, and phenotypic associations of resistance mechanisms. Eur. J. Cancer 2015, 51, 2792–2799. [Google Scholar] [CrossRef] [PubMed]
- Van Allen, E.M.; Wagle, N.; Sucker, A.; Treacy, D.J.; Johannessen, C.M.; Goetz, E.M.; Place, C.S.; Taylor-Weiner, A.; Whittaker, S.; Kryukov, G.V.; et al. The genetic landscape of clinical resistance to RAF inhibition in metastatic melanoma. Cancer Discov. 2014, 4, 94–109. [Google Scholar] [CrossRef] [PubMed]
- Jiang, C.C.; Lai, F.; Thorne, R.F.; Yang, F.; Liu, H.; Hersey, P.; Zhang, X.D. MEK-Independent Survival of B-RAFV600E Melanoma Cells Selected for Resistance to Apoptosis Induced by the RAF Inhibitor PLX4720. Clin. Cancer Res. 2011, 17, 721–730. [Google Scholar] [CrossRef]
- Atefi, M.; von Euw, E.; Attar, N.; Ng, C.; Chu, C.; Guo, D.; Nazarian, R.; Chmielowski, B.; Glaspy, J.A.; Comin-Anduix, B.; et al. Reversing melanoma cross-resistance to BRAF and MEK inhibitors by co-targeting the AKT/mTOR pathway. PLoS ONE 2011, 6, e28973. [Google Scholar] [CrossRef] [PubMed]
- Luo, H.; Umebayashi, M.; Doi, K.; Morisaki, T.; Shirasawa, S.; Tsunoda, T. Resveratrol Overcomes Cellular Resistance to Vemurafenib Through Dephosphorylation of AKT in BRAF-mutated Melanoma Cells. Anticancer Res. 2016, 36, 3585–3589. [Google Scholar] [PubMed]
- Straussman, R.; Morikawa, T.; Shee, K.; Barzily-Rokni, M.; Qian, Z.R.; Du, J.; Davis, A.; Mongare, M.M.; Gould, J.; Frederick, D.T.; et al. Tumour micro-environment elicits innate resistance to RAF inhibitors through HGF secretion. Nature 2012, 487, 500–504. [Google Scholar] [CrossRef]
- Shaffer, S.M.; Dunagin, M.C.; Torborg, S.R.; Torre, E.A.; Emert, B.; Krepler, C.; Beqiri, M.; Sproesser, K.; Brafford, P.A.; Xiao, M.; et al. Rare cell variability and drug-induced reprogramming as a mode of cancer drug resistance. Nature 2017, 546, 431–435. [Google Scholar] [CrossRef]
- Kemper, K.; de Goeje, P.L.; Peeper, D.S.; van Amerongen, R. Phenotype Switching: Tumor Cell Plasticity as a Resistance Mechanism and Target for Therapy. Cancer Res. 2014, 74, 5937–5941. [Google Scholar] [CrossRef]
- Müller, J.; Krijgsman, O.; Tsoi, J.; Robert, L.; Hugo, W.; Song, C.; Kong, X.; Possik, P.A.; Cornelissen-Steijger, P.D.M.; Foppen, M.H.G.; et al. Low MITF/AXL ratio predicts early resistance to multiple targeted drugs in melanoma. Nat. Commun. 2014, 5, 5712. [Google Scholar] [CrossRef] [PubMed]
- Golub, K.; Bai, W.; Zhang, Z.; Xiao, H.; Sun, R.; Shen, J.; Sun, J. The mechanism and consequences of BRAF inhibitor resistance in melanoma. Genome Instab. Dis. 2023, 4, 266–274. [Google Scholar] [CrossRef]
- Available online: https://clinicaltrials.gov/ (accessed on 18 November 2023).
- Landi, D.B.; Ziegler, D.S.; Franson, A.F.; Baxter, P.A.; Leary, S.; Larouche, V.; Waanders, A.J.; Lugt, J.V.d.; McCowage, G.B.; Doz, F.; et al. FIREFLY-1 (PNOC 026): A phase 2 study to evaluate the safety and efficacy of tovorafenib (DAY101) in pediatric patients with RAF-altered recurrent or progressive low-grade glioma or advanced solid tumors. J. Clin. Oncol. 2022, 40, TPS10062. [Google Scholar] [CrossRef]
- Subbiah, V.; Gutierrez, M.; Anders, C.K.; Ansstas, G.; Owonikoko, T.K.; Monga, V.; Forsyth, P.A.J.; Dagogo-Jack, I.; Chandra, S.; Tsai, K.K.; et al. Trial in progress: Phase 1a/b study of PF-07284890 (brain-penetrant BRAF inhibitor) with/without binimetinib in patients with BRAF V600-mutant solid tumors. J. Clin. Oncol. 2021, 39, TPS3152. [Google Scholar] [CrossRef]
- Govindan, R.; Awad, M.M.; Gadgeel, S.M.; Pachter, J.A.; Patrick, G.; Denis, L.J. A phase 1/2 study of VS-6766 (RAF/MEK clamp) in combination with sotorasib (G12C inhibitor) in patients with KRAS G12C mutant non–small cell lung cancer (NSCLC) (RAMP 203). J. Clin. Oncol. 2022, 40, TPS9148. [Google Scholar] [CrossRef]
- Banerjee, S.N.; Monk, B.J.; Nieuwenhuysen, E.V.; Moore, K.N.; Oaknin, A.; Fabbro, M.; Colombo, N.; O’Malley, D.M.; Coleman, R.L.; Oza, A.M.; et al. ENGOT-ov60/GOG-3052/RAMP 201: A phase 2 study of VS-6766 (RAF/MEK clamp) alone and in combination with defactinib (FAK inhibitor) in recurrent low-grade serous ovarian cancer (LGSOC). J. Clin. Oncol. 2022, 40, TPS5615. [Google Scholar] [CrossRef]
- Capelletto, E.; Bironzo, P.; Denis, L.; Koustenis, A.; Bungaro, M.; Novello, S. Single agent VS-6766 or VS-6766 plus defactinib in KRAS-mutant non-small-cell lung cancer: The RAMP-202 phase II trial. Future Oncol. 2022, 18, 1907–1915. [Google Scholar] [CrossRef]
- Shergill, A.; Liao, C.-Y.; Kindler, H.L.; Polite, B.N.; Catenacci, D.V.T. A phase 1b/2 study of VS-6766 in combination cetuximab in patients (pts) with advanced KRAS mt colorectal cancer (CRC). J. Clin. Oncol. 2022, 40, TPS219. [Google Scholar] [CrossRef]
- Kilburn, L.B.; Khuong-Quang, D.-A.; Hansford, J.R.; Landi, D.; van der Lugt, J.; Leary, S.E.S.; Driever, P.H.; Bailey, S.; Perreault, S.; McCowage, G.; et al. The type II RAF inhibitor tovorafenib in relapsed/refractory pediatric low-grade glioma: The phase 2 FIREFLY-1 trial. Nat. Med. 2023; online ahead of print. [Google Scholar] [CrossRef]
- Tilburg, C.M.v.; Kilburn, L.B.; Crotty, E.; Smith, A.A.; Perreault, S.; Franson, A.F.; Jabado, N.; Hoffman, L.M.; Schmidt, R.; Meeteren, A.Y.N.S.-v.; et al. LOGGIC/FIREFLY-2: A phase 3, randomized trial of tovorafenib vs. chemotherapy in pediatric and young adult patients with newly diagnosed low-grade glioma harboring an activating RAF alteration. J. Clin. Oncol. 2023, 41, TPS10067. [Google Scholar] [CrossRef]
- Rasco, D.W.; Medina, T.; Corrie, P.; Pavlick, A.C.; Middleton, M.R.; Lorigan, P.; Hebert, C.; Plummer, R.; Larkin, J.; Agarwala, S.S.; et al. Phase 1 study of the pan-RAF inhibitor tovorafenib in patients with advanced solid tumors followed by dose expansion in patients with metastatic melanoma. J. Clin. Oncol. 2023, 92, 15–28. [Google Scholar] [CrossRef] [PubMed]
- Bouhana, K.; Anderson, D.; DeWolf, W.; Brown, S.; Williams, L.; Ren, L.; Moreno, D.; Wallace, R.; Fell, J.B.; Hartley, D.; et al. Abstract 1473: Nonclinical development of PF-07284890 (ARRY-461), a potent, brain-penetrant, small molecule inhibitor of BRAF V600-mutation-driven tumors in vitro and in vivo. Cancer Res. 2021, 81, 1473. [Google Scholar] [CrossRef]
- Piha-Paul, S.A.; Nagpal, S.; Weise, A.M.; Braiteh, F.S.; Chen, C.; Huang, C.Q.; Liu, W.; Hu, Y.; Yang, Z.; Tsai, K.K. A phase 1, multicenter, open-label study of a new BRAF inhibitor ABM-1310 in adult patients (pts) with BRAFv600-mutated solid tumors. J. Clin. Oncol. 2023, 41, 3098. [Google Scholar] [CrossRef]
- Schram, A.M.; Subbiah, V.; Sullivan, R.; Cosman, R.; Liu, J.; Sbar, E.I.; Hoang, T.; Chen, J.; Johnson, M.; Amoruccio, V.; et al. Abstract CT031: A first-in-human, phase 1a/1b, open-label, dose-escalation and expansion study to investigate the safety, pharmacokinetics, and antitumor activity of the RAF dimer inhibitor BGB-3245 in patients with advanced or refractory tumors. Cancer Res. 2023, 83, CT031. [Google Scholar] [CrossRef]
- Fuente, M.I.D.L.; Ahnert, J.R.; Yaeger, R.; Tsai, F.Y.-C.; Janku, F.; Butowski, N.A.; Allen, C.E.; Ammakkanavar, N.R.; Taylor, J.W.; Michelson, G.; et al. Safety and efficacy of the novel BRAF inhibitor FORE8394 in patients with advanced solid and CNS tumors: Results from a phase 1/2a study. J. Clin. Oncol. 2023, 41, 3006. [Google Scholar] [CrossRef]
- Takano, K.; Munehira, Y.; Hatanaka, M.; Murakami, R.; Shibata, Y.; Shida, T.; Takeuchi, K.; Takechi, S.; Tabata, T.; Shimada, T.; et al. Discovery of a Novel ATP-Competitive MEK Inhibitor DS03090629 that Overcomes Resistance Conferred by BRAF Overexpression in BRAF-Mutated Melanoma. Mol. Cancer Ther. 2023, 22, 317–332. [Google Scholar] [CrossRef] [PubMed]
- Janku, F.; Vaishampayan, U.N.; Khemka, V.; Bhatty, M.; Sherman, E.J.; Tao, J.; Whisenant, J.R.; Hong, D.S.; Bui, N.; Kummar, S.; et al. Phase 1/2 precision medicine study of the next-generation BRAF inhibitor PLX8394. J. Clin. Oncol. 2018, 36, 2583. [Google Scholar] [CrossRef]
- Han, Y.-C.; Ng, P.-Y.; Ogawa, L.S.; Yang, S.N.; Chen, M.; Ishiyama, N.; Lin, T.-A.; Buck, E. Abstract 3415: Preclinical characterization of a brain penetrant RAF inhibitor, BDTX-4933, targeting oncogenic BRAF Class I/II/III and RAS mutations. Cancer Res. 2023, 83, 3415. [Google Scholar] [CrossRef]
- Babiker, H.M.; Byron, S.A.; Hendricks, W.P.D.; Elmquist, W.F.; Gampa, G.; Vondrak, J.; Aldrich, J.; Cuyugan, L.; Adkins, J.; De Luca, V.; et al. E6201, an intravenous MEK1 inhibitor, achieves an exceptional response in BRAF V600E-mutated metastatic malignant melanoma with brain metastases. Investig. New Drugs 2019, 37, 636–645. [Google Scholar] [CrossRef]
- Tibes, R.; Borad, M.J.; Dutcus, C.E.; Reyderman, L.; Feit, K.; Eisen, A.; Verbel, D.A.; Von Hoff, D.D. Safety, pharmacokinetics, and preliminary efficacy of E6201 in patients with advanced solid tumours, including melanoma: Results of a phase 1 study. Br. J. Cancer 2018, 118, 1580–1585. [Google Scholar] [CrossRef]
| Agent | Trial | Status | Conditions | Phase |
|---|---|---|---|---|
| Vemurafenib + cobimetinib | NCT05768178 | R | Arm 5: adult patients with BRAF-positive solid and hematology malignancies (DETERMINE trial) | II/III |
| Vemurafenib + cobimetinib + atezolizumab | NCT02908672 | A, NR | Previously untreated BRAFV600-mutated patients with metastatic or unresectable locally advanced melanoma | III |
| Dabrafenib + trametinib | NCT04940052 | R | Previously treated patients with locally advanced or metastatic, radioactive iodine refractory BRAFV600E-mutated differentiated thyroid cancer | III |
| Dabrafenib + trametinib | NCT03340506 | R | Rollover study, patients with solid tumors, melanoma, NSCLC, high-grade gliomas | IV |
| Encorafenib + binimetinib | NCT05270044 | R | High-risk patients with stage II melanoma with BRAF-mutations as adjuvant treatment (COLUMBUS-AD) | III |
| Encorafenib + cetuximab +/− chemotherapy | NCT04607421 | R | Previously untreated metastatic CRC (BREAKWATER) | III |
| Encorafenib + cetuximab + pembrolizumab vs. pembrolizumab alone | NCT05217446 | R | Previously untreated BRAFV600E mutant, MSI high/DMMR metastatic CRC (SEAMARK) | II |
| Encorafenib + binimetinib + pembrolizumab | NCT04657991 | R | Treatment-naive patients with advanced or metastatic melanoma with BRAF alterations (STEABOARD) | III |
| Encorafenib + binimetinib + palbociclib | NCT04720768 | R | BRAF mutant metastatic melanoma (CELEBRATE) | I/II |
| Encorafenib + binimetinib +/− nivolumab | NCT04061980 | R | Patients with metastatic radioiodine refractory BRAFV600 mutant thyroid cancer | II |
| Trametinib vs. Standard of care | NCT02101788 | A, NR | Recurrent or progressive low-grade ovarian cancer or peritoneal cavity cancer | II/III |
| Binimetinib + palbociclib | NCT03170206 | R | Patients with advanced KRAS mutant NSCLC | I/II |
| Binimetinib + pembrolizumab | NCT03991819 | R | Advanced NSCLC | I |
| Cobimetinib | NCT04409639 | R | Newly diagnosed or HMA-treated CMML patients with RAS pathway mutations (CONCERTO trial) | II |
| Cobimetinib + atezolizumab | NCT04216953 | R | Locally advanced and/or metastatic soft tissue sarcoma (COTESARC) | I/II |
| Novel Drugs | ||||
| BDTX-4933 | NCT05786924 | R | Patients with BRAF and other RAS/MAPK mutation-positive neoplasms | I |
| ABM-1310 +/− cobimetinib | NCT04190628 | R | Patients with BRAF-mutated advanced solid tumors | I |
| BGB-3245 + mirdametinib | NCT05580770 | R | Advanced metastatic or unresectable solid cancers with at least one prior line | I |
| Tovorafenib (DAY101) +/− pimasertib | NCT04985604 | R | Recurrent, progressive, or refractory solid tumors harboring MAPK pathway aberrations | I |
| PF07284890 | NCT05538130 | R | Advanced solid tumors for which available treatments are no longer effective | I |
| VS6766 +/− everolimus | NCT02407509 | R | Advanced solid tumors with BRAF, KRAS, and/or NRAS mutations | I |
| VS6766 + defactinib | NCT05512208 | R | Recurrent gynecological cancers (endometrioid cancer, mucinous ovarian cancer, high-grade serous ovarian cancer, or cervical cancer) | II |
| VS6766 + sotorasib | NCT05074810 | R | Previously treated KRASG12C-mutated NSCLC patients +/− prior G12C inhibitor (RAMP203) | I/II |
| VS6766 + cetuximab | NCT05200442 | R | Previously treated KRAS mutant advanced CRC patients | I/II |
| E6201 + Dabrafenib | NCT05388877 | R | BRAFV600 mutated metastatic with CNS metastasis | I |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Shan, K.S.; Rehman, T.U.; Ivanov, S.; Domingo, G.; Raez, L.E. Molecular Targeting of the BRAF Proto-Oncogene/Mitogen-Activated Protein Kinase (MAPK) Pathway across Cancers. Int. J. Mol. Sci. 2024, 25, 624. https://doi.org/10.3390/ijms25010624
Shan KS, Rehman TU, Ivanov S, Domingo G, Raez LE. Molecular Targeting of the BRAF Proto-Oncogene/Mitogen-Activated Protein Kinase (MAPK) Pathway across Cancers. International Journal of Molecular Sciences. 2024; 25(1):624. https://doi.org/10.3390/ijms25010624
Chicago/Turabian StyleShan, Khine S., Tauseef U. Rehman, Stan Ivanov, Gelenis Domingo, and Luis E. Raez. 2024. "Molecular Targeting of the BRAF Proto-Oncogene/Mitogen-Activated Protein Kinase (MAPK) Pathway across Cancers" International Journal of Molecular Sciences 25, no. 1: 624. https://doi.org/10.3390/ijms25010624
APA StyleShan, K. S., Rehman, T. U., Ivanov, S., Domingo, G., & Raez, L. E. (2024). Molecular Targeting of the BRAF Proto-Oncogene/Mitogen-Activated Protein Kinase (MAPK) Pathway across Cancers. International Journal of Molecular Sciences, 25(1), 624. https://doi.org/10.3390/ijms25010624





