β-Tricalcium Phosphate-Modified Aerogel Containing PVA/Chitosan Hybrid Nanospun Scaffolds for Bone Regeneration
Abstract
1. Introduction
2. Results
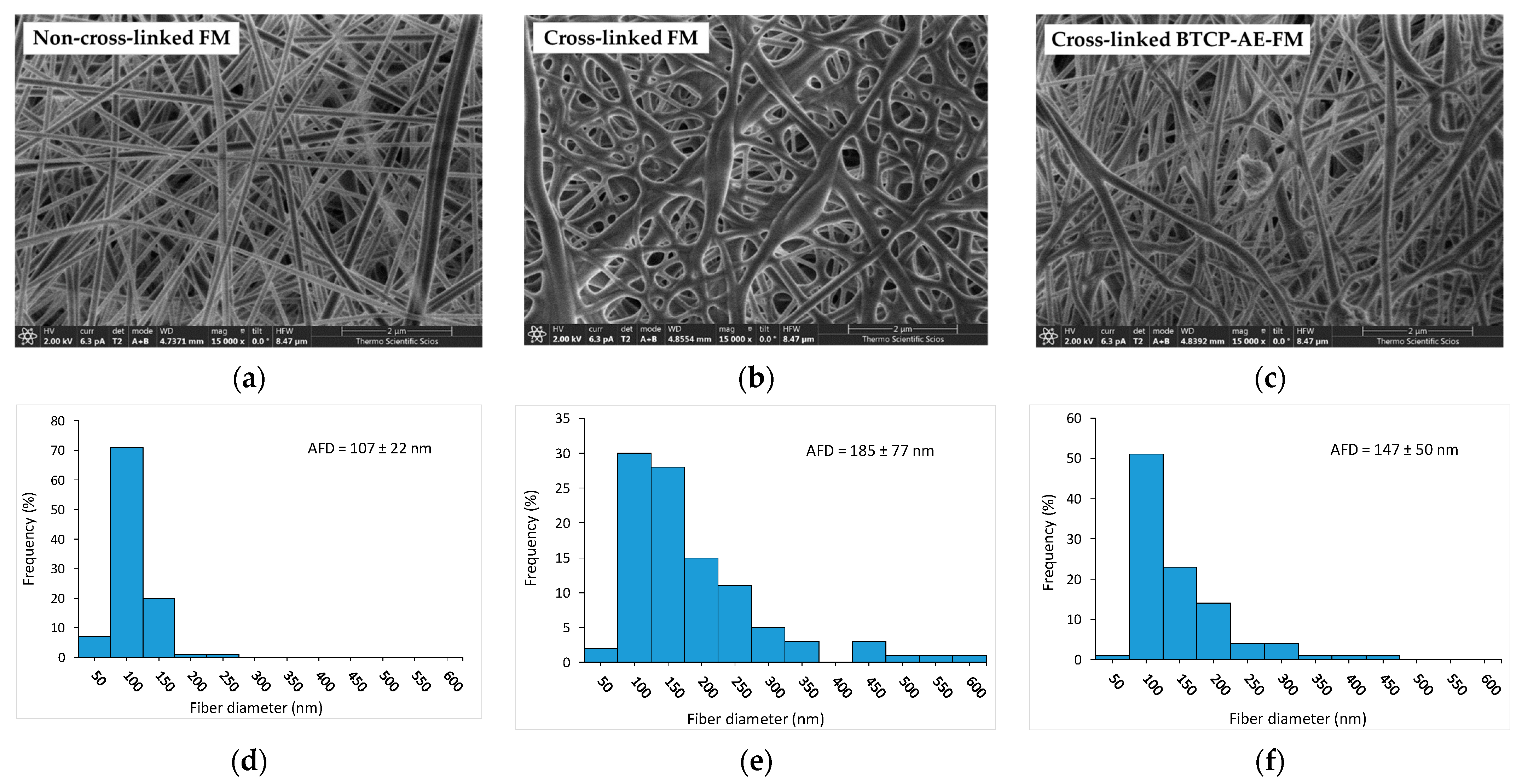
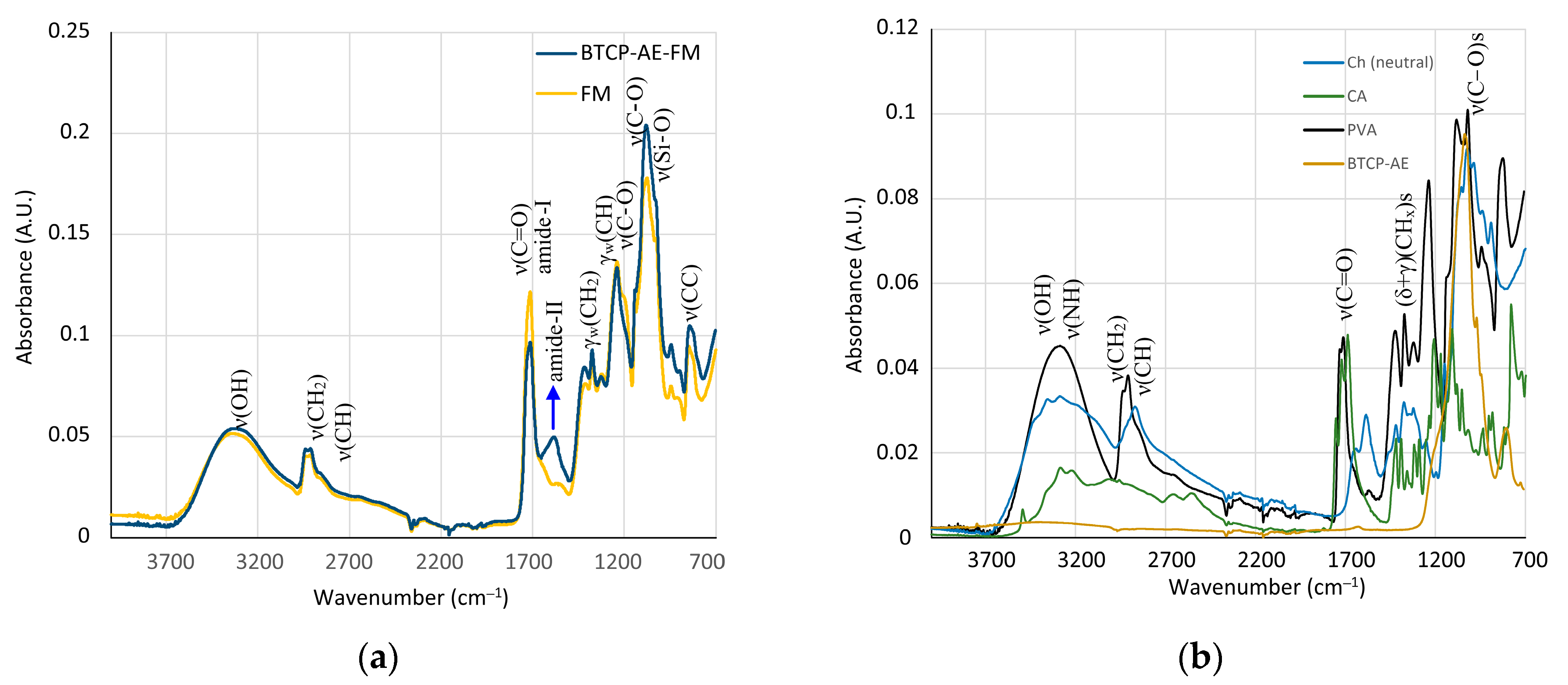
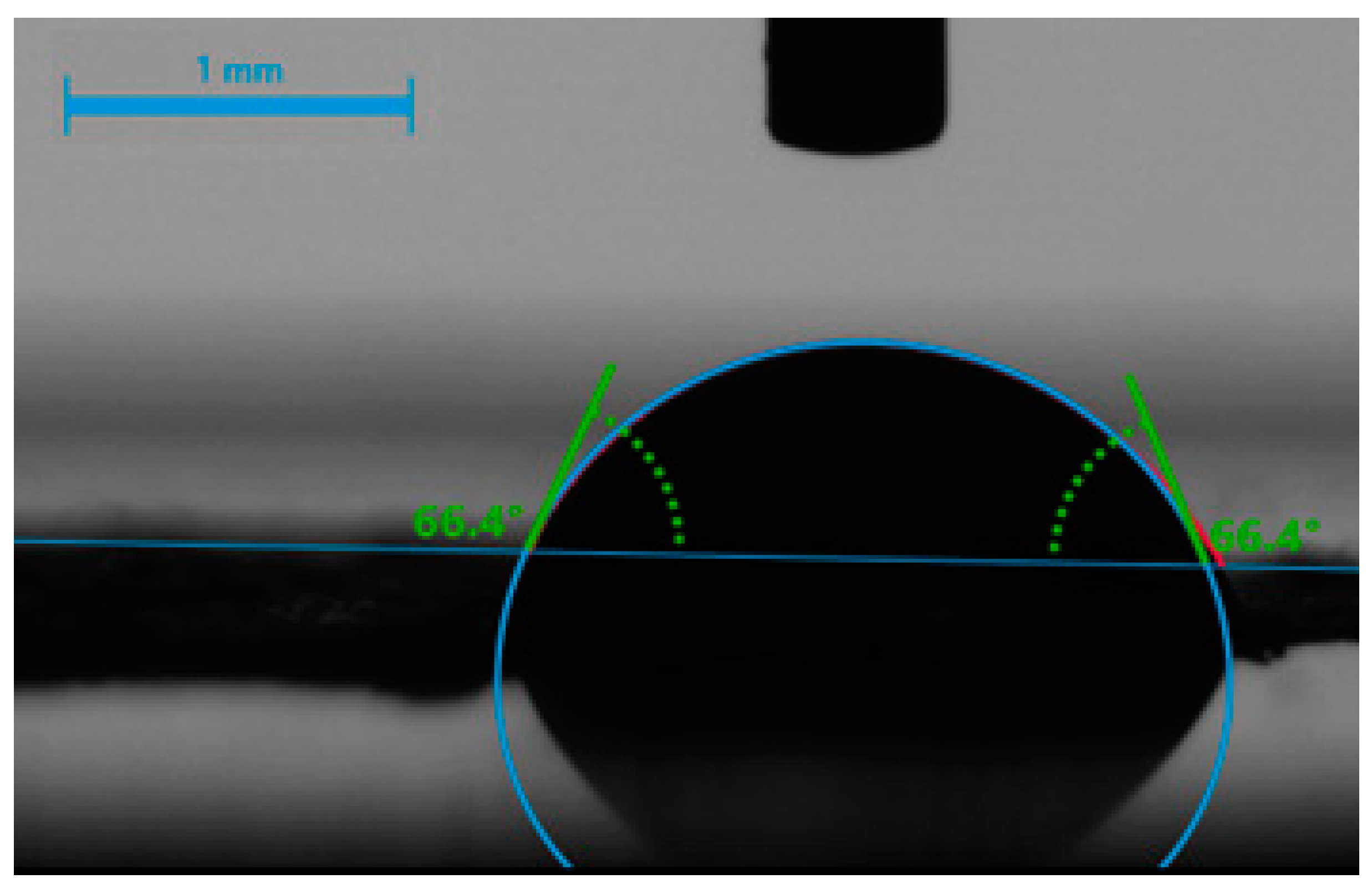
2.1. Morphological Characterization and Physicochemical Properties of Electrospun FMs and BTCP-AE-FMs
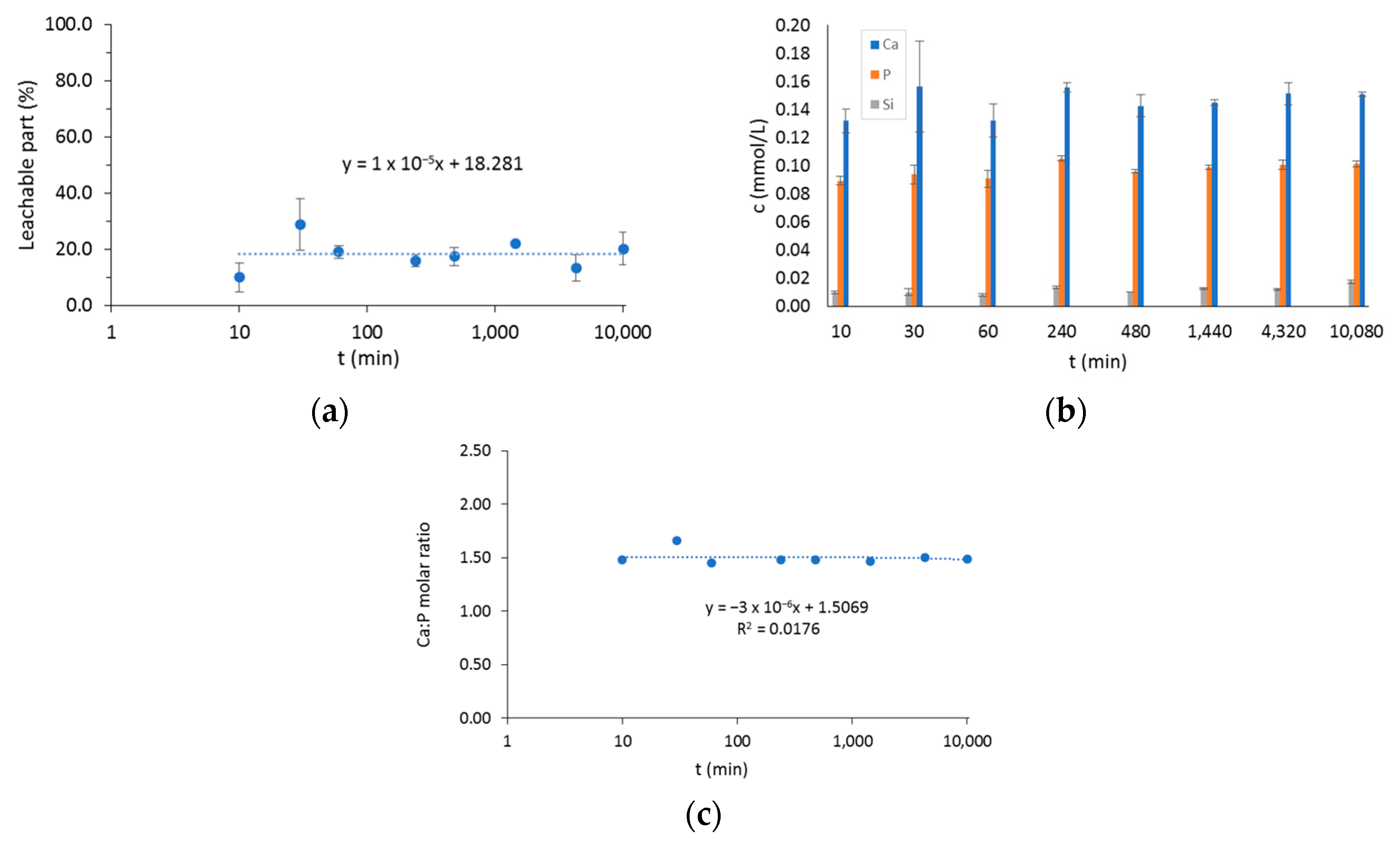
2.2. Leachable Part of the BTCP-AE-FM and Ca, P, and Si Releasing
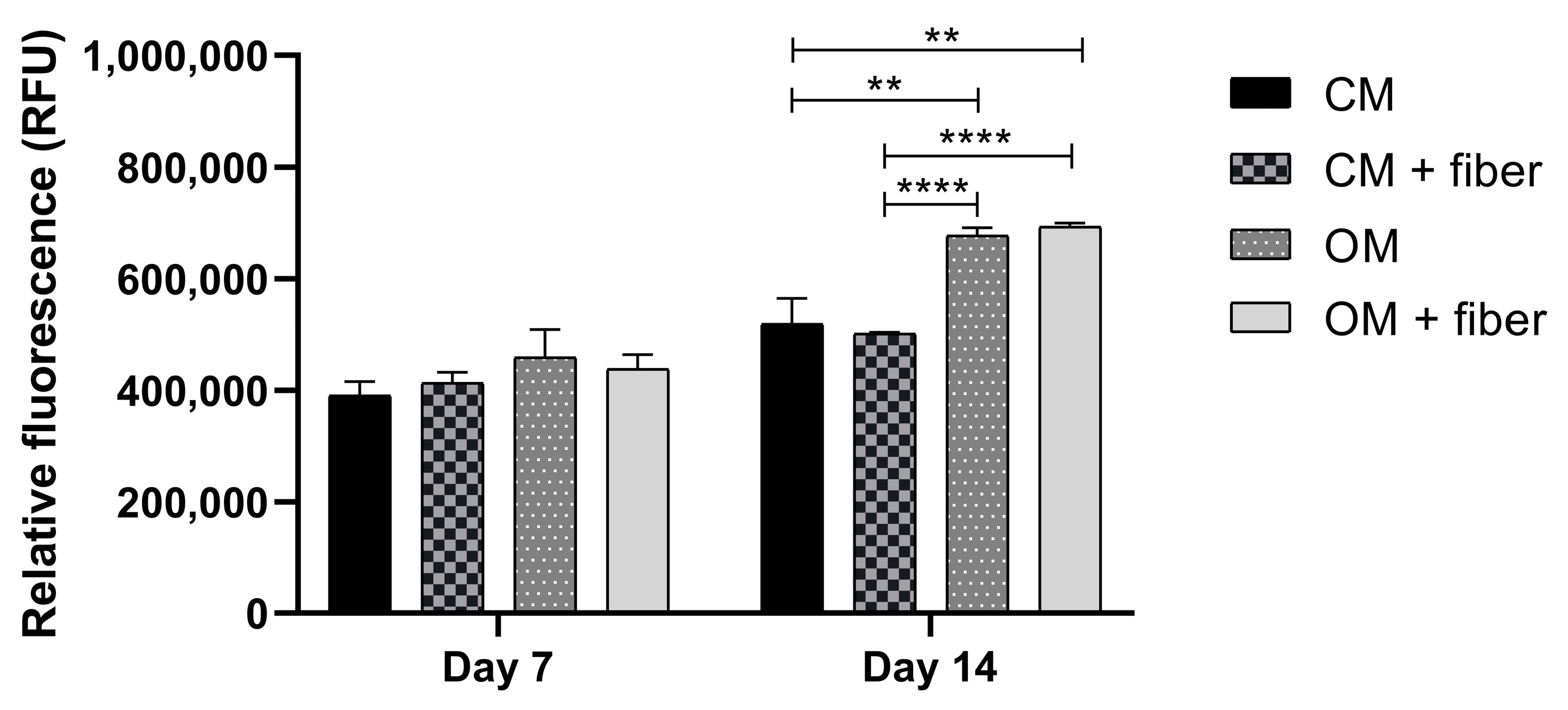
2.3. In Vitro Evaluation
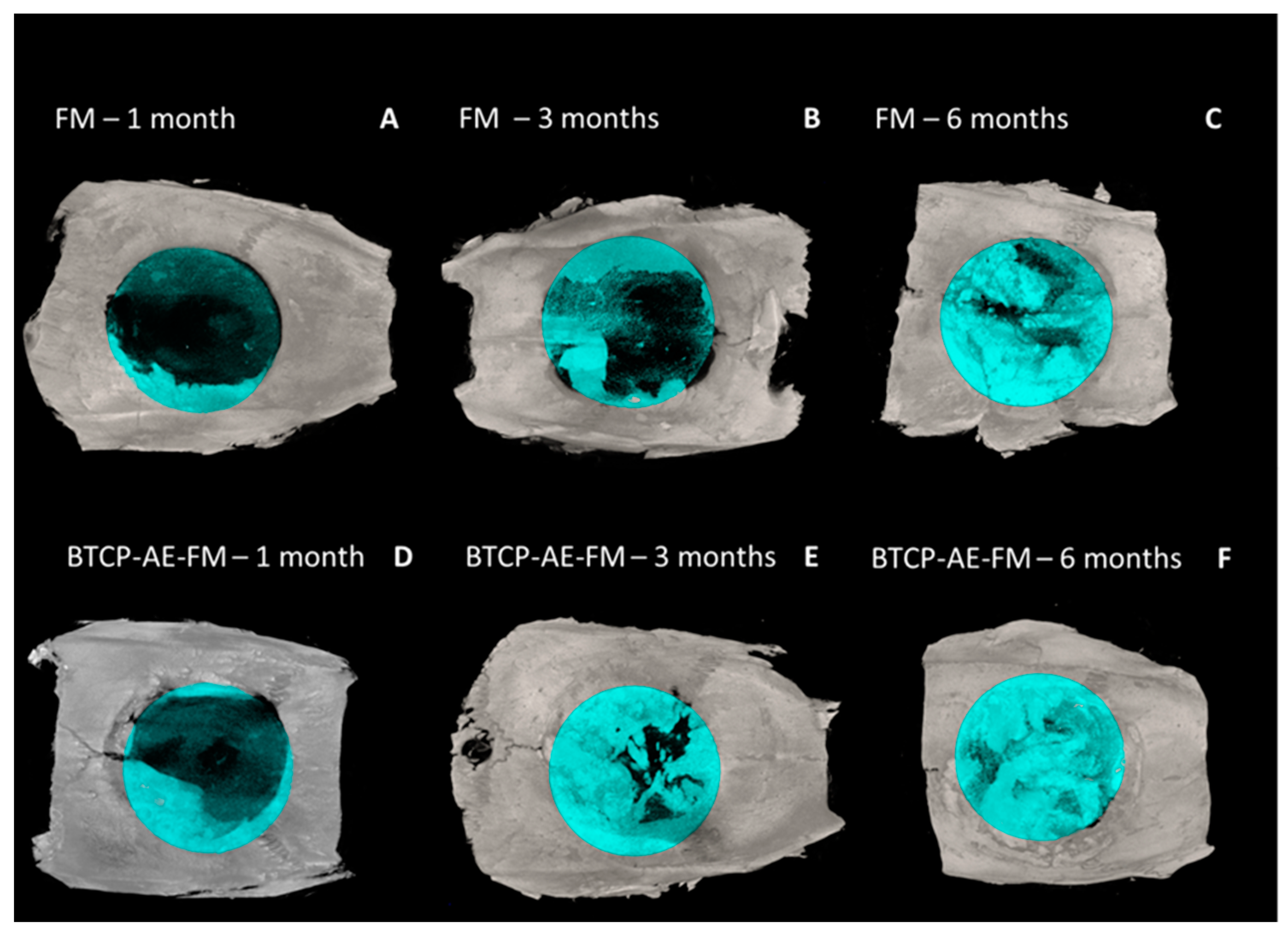
2.4. MicroCT
2.5. PET Imaging Using [18F]fluoride
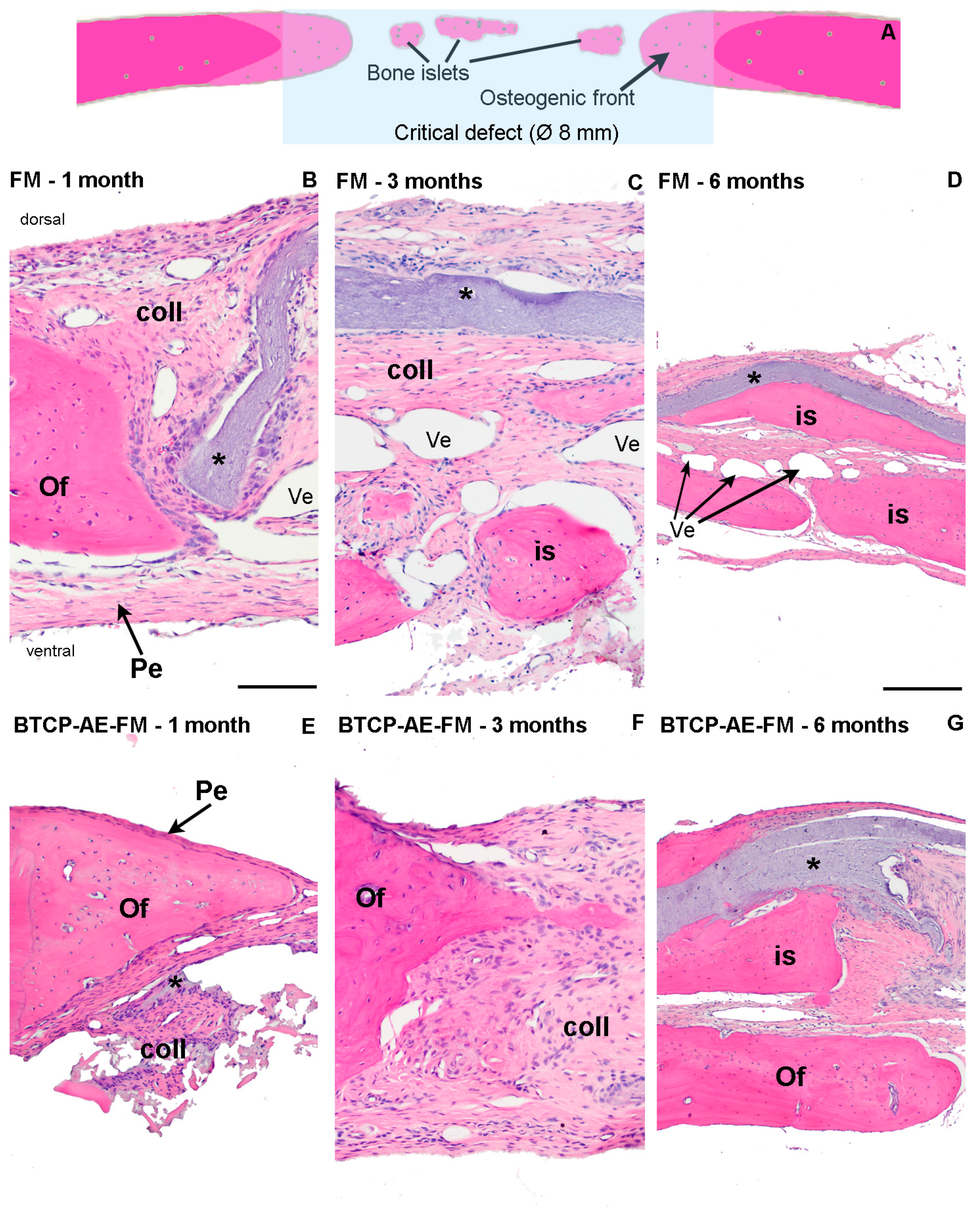
2.6. Histological Evaluation
3. Discussion
4. Materials and Methods
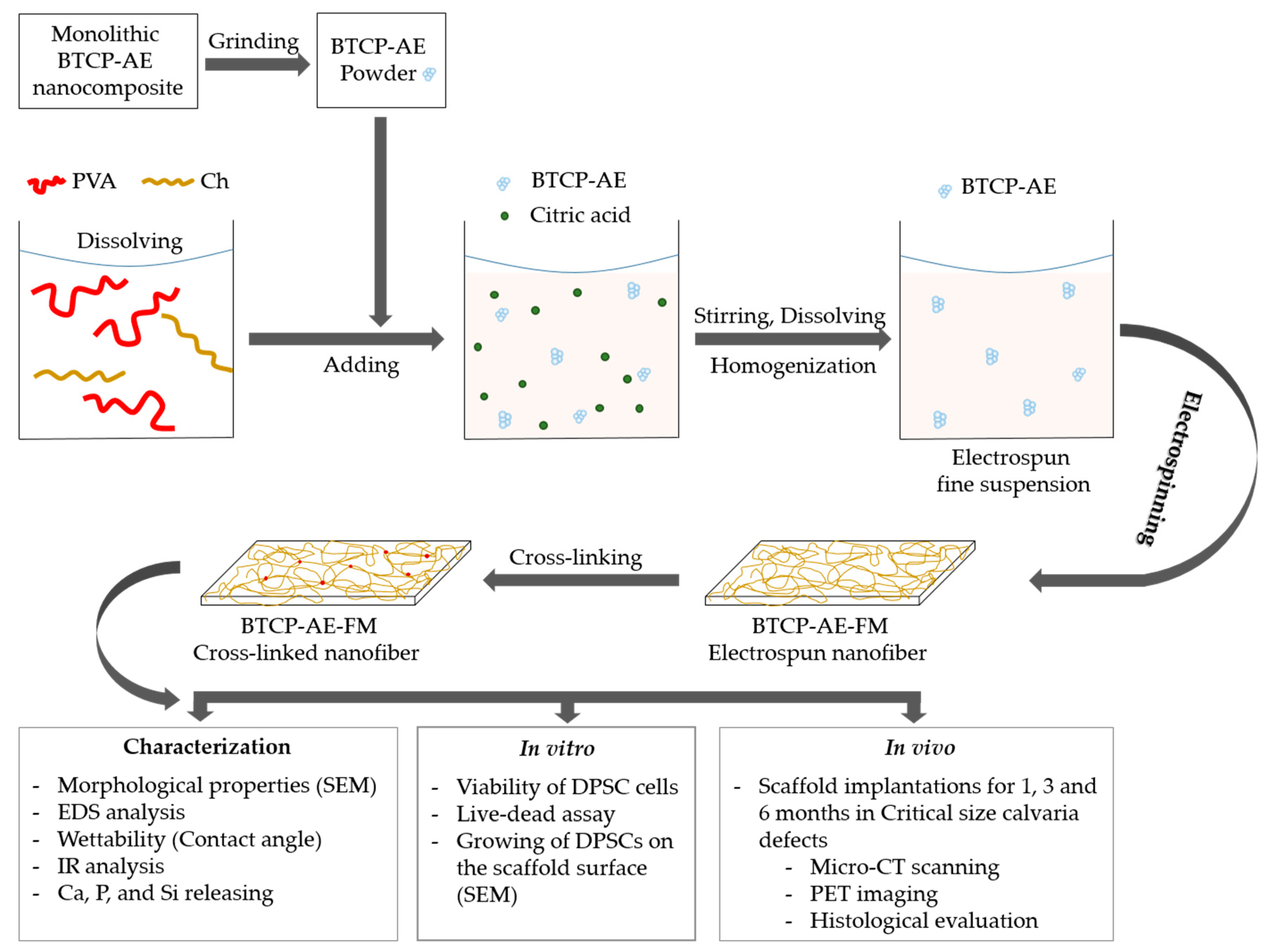
4.1. Sample Preparation
4.2. Infrared Spectroscopy
4.3. Scanning Electron Microscopy (SEM)
4.4. Hydrophilicity of BTCP-AE-FMs
4.5. Leachable Part of the BTCP-AE-FM and Ca, P, and Si Releasing
4.6. Cell Culturing and Viability Assays
4.7. Cell Morphology
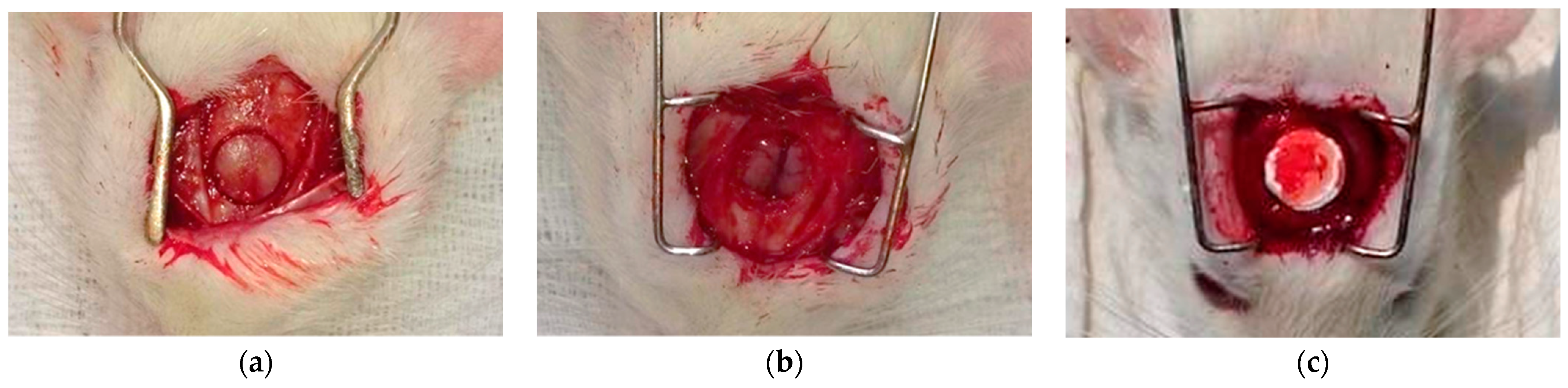
4.8. Surgical Procedures
4.9. Micro CT Measurement
4.10. In Vivo PET Imaging Using 18F-Sodium Fluoride (18F-NaF)
4.11. Histological Analysis
4.12. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Putra, R.U.; Basri, H.; Prakoso, A.T.; Chandra, H.; Ammarullah, M.I.; Akbar, I.; Syahrom, A.; Kamarul, T. Level of Activity Changes Increases the Fatigue Life of the Porous Magnesium Scaffold, as Observed in Dynamic Immersion Tests, over Time. Sustainability 2023, 15, 823. [Google Scholar] [CrossRef]
- Qi, Y.; Wang, C.; Wang, Q.; Zhou, F.; Li, T.; Wang, B.; Su, W.; Shang, D.; Wu, S. A Simple, Quick, and Cost-Effective Strategy to Fabricate Polycaprolactone/Silk Fibroin Nanofiber Yarns for Biotextile-Based Tissue Scaffold Application. Eur. Polym. J. 2023, 186, 111863. [Google Scholar] [CrossRef]
- Nazarnezhad, S.; Baino, F.; Kim, H.W.; Webster, T.J.; Kargozar, S. Electrospun Nanofibers for Improved Angiogenesis: Promises for Tissue Engineering Applications. Nanomaterials 2020, 10, 1609. [Google Scholar] [CrossRef] [PubMed]
- Li, M.; Qiu, W.; Wang, Q.; Li, N.; Liu, L.; Wang, X.; Yu, J.; Li, X.; Li, F.; Wu, D. Nitric Oxide-Releasing Tryptophan-Based Poly(Ester Urea)s Electrospun Composite Nanofiber Mats with Antibacterial and Antibiofilm Activities for Infected Wound Healing. ACS Appl. Mater. Interfaces 2022, 14, 15911–15926. [Google Scholar] [CrossRef]
- Prakoso, A.T.; Basri, H.; Adanta, D.; Yani, I.; Ammarullah, M.I.; Akbar, I.; Ghazali, F.A.; Syahrom, A.; Kamarul, T. The Effect of Tortuosity on Permeability of Porous Scaffold. Biomedicines 2023, 11, 427. [Google Scholar] [CrossRef]
- Januariyasa, I.K.; Ana, I.D.; Yusuf, Y. Nanofibrous Poly(Vinyl Alcohol)/Chitosan Contained Carbonated Hydroxyapatite Nanoparticles Scaffold for Bone Tissue Engineering. Mater. Sci. Eng. C Mater. Biol. Appl. 2020, 107, 110347. [Google Scholar] [CrossRef] [PubMed]
- Udomluck, N.; Koh, W.G.; Lim, D.J.; Park, H. Recent Developments in Nanofiber Fabrication and Modification for Bone Tissue Engineering. Int. J. Mol. Sci. 2019, 21, 99. [Google Scholar] [CrossRef]
- Voniatis, C.; Balsevicius, L.; Barczikai, D.; Juriga, D.; Takács, A.; Kőhidai, L.; Nagy, K.; Jedlovszky-Hajdu, A. Co-Electrospun Polysuccinimide/Poly(Vinyl Alcohol) Composite Meshes for Tissue Engineering. J. Mol. Liq. 2020, 306, 112895. [Google Scholar] [CrossRef]
- Czibulya, Z.; Csík, A.; Tóth, F.; Pál, P.; Csarnovics, I.; Zelkó, R.; Hegedűs, C. The Effect of the PVA/Chitosan/Citric Acid Ratio on the Hydrophilicity of Electrospun Nanofiber Meshes. Polymers 2021, 13, 3557. [Google Scholar] [CrossRef]
- Castro, A.G.B.; Löwik, D.W.P.M.; Van Steenbergen, M.J.; Jansen, J.A.; Van Den Beucken, J.J.J.P.; Yang, F. Incorporation of Simvastatin in PLLA Membranes for Guided Bone Regeneration: Effect of Thermal Treatment on Simvastatin Release. RSC Adv. 2018, 8, 28546–28554. [Google Scholar] [CrossRef]
- Ding, J.; Zhang, J.; Li, J.; Li, D.; Xiao, C.; Xiao, H.; Yang, H.; Zhuang, X.; Chen, X. Electrospun Polymer Biomaterials. Prog. Polym. Sci. 2019, 90, 1–34. [Google Scholar] [CrossRef]
- Sun, Y.; Cheng, S.; Lu, W.; Wang, Y.; Zhang, P.; Yao, Q. Electrospun Fibers and Their Application in Drug Controlled Release, Biological Dressings, Tissue Repair, and Enzyme Immobilization. RSC Adv. 2019, 9, 25712–25729. [Google Scholar] [CrossRef] [PubMed]
- Cary, R.L.; Waddell, S.; Racioppi, L.; Long, F.; Novack, D.V.; Voor, M.J.; Sankar, U. Inhibition of Ca2+/Calmodulin-Dependent Protein Kinase Kinase 2 Stimulates Osteoblast Formation and Inhibits Osteoclast Differentiation. J. Bone Miner. Res. 2013, 28, 1599–1610. [Google Scholar] [CrossRef] [PubMed]
- Liu, W.; Le, C.C.; Wang, D.; Ran, D.; Wang, Y.; Zhao, H.; Gu, J.; Zou, H.; Yuan, Y.; Bian, J.; et al. Ca2+/CaM/CaMK Signaling Is Involved in Cadmium-Induced Osteoclast Differentiation. Toxicology 2020, 441, 152520. [Google Scholar] [CrossRef] [PubMed]
- Dong, M.; Jiao, G.; Liu, H.; Wu, W.; Li, S.; Wang, Q.; Xu, D.; Li, X.; Liu, H.; Chen, Y. Biological Silicon Stimulates Collagen Type 1 and Osteocalcin Synthesis in Human Osteoblast-Like Cells Through the BMP-2/Smad/RUNX2 Signaling Pathway. Biol. Trace Elem. Res. 2016, 173, 306–315. [Google Scholar] [CrossRef] [PubMed]
- Hegedűs, V.; Kerényi, F.; Boda, R.; Horváth, D.; Lázár, I.; Tóth-Győri, E.; Dezső, B.; Hegedus, C. β-Tricalcium Phosphate-Silica Aerogel as an Alternative Bioactive Ceramic for the Potential Use in Dentistry. Adv. Appl. Ceram. 2019, 119, 364–371. [Google Scholar] [CrossRef]
- Dorozhkin, S.V. Calcium Orthophosphate (CaPO4)–Based Bone-Graft Substitutes and the Special Roles of Octacalcium Phosphate Materials. In Octacalcium Phosphate Biomaterials: Understanding of Bioactive Properties and Application; Woodhead Publishing: Cambridge, UK, 2020; pp. 213–288. [Google Scholar] [CrossRef]
- Liu, Y.; Shen, X.; Zhou, H.; Wang, Y.; Deng, L. Chemical Modification of Chitosan Film via Surface Grafting of Citric Acid Molecular to Promote the Biomineralization. Appl. Surf. Sci. 2016, 370, 270–278. [Google Scholar] [CrossRef]
- Guerrero, P.; Muxika, A.; Zarandona, I.; de la Caba, K. Crosslinking of Chitosan Films Processed by Compression Molding. Carbohydr. Polym. 2019, 206, 820–826. [Google Scholar] [CrossRef]
- Zhang, Y.; Huang, X.; Duan, B.; Wu, L.; Li, S.; Yuan, X. Preparation of Electrospun Chitosan/Poly(Vinyl Alcohol) Membranes. Colloid Polym. Sci. 2007, 285, 855–863. [Google Scholar] [CrossRef]
- Rodrigues, I.R.; de Camargo Forte, M.M.; Azambuja, D.S.; Castagno, K.R.L. Synthesis and Characterization of Hybrid Polymeric Networks (HPN) Based on Polyvinyl Alcohol/Chitosan. React. Funct. Polym. 2007, 67, 708–715. [Google Scholar] [CrossRef]
- Krimm, S.; Liang, C.Y.; Sutherland, G.B.B.M. Infrared Spectra of High Polymers. V. Polyvinyl Alcohol. J. Polym. Sci. 1956, 22, 227–247. [Google Scholar] [CrossRef]
- SDBS-2708. Available online: https://sdbs.db.aist.go.jp/sdbs/cgi-bin/landingpage?sdbsno=2708 (accessed on 28 March 2023).
- Kim, H.S.; Lee, J.H.; Mandakhbayar, N.; Jin, G.Z.; Kim, S.J.; Yoon, J.Y.; Jo, S.B.; Park, J.H.; Singh, R.K.; Jang, J.H.; et al. Therapeutic Tissue Regenerative Nanohybrids Self-Assembled from Bioactive Inorganic Core/Chitosan Shell Nanounits. Biomaterials 2021, 274, 120857. [Google Scholar] [CrossRef] [PubMed]
- Li, L.; Hsieh, Y. Lo Chitosan Bicomponent Nanofibers and Nanoporous Fibers. Carbohydr. Res. 2006, 341, 374–381. [Google Scholar] [CrossRef] [PubMed]
- Vega-Cázarez, C.A.; López-Cervantes, J.; Sánchez-Machado, D.I.; Madera-Santana, T.J.; Soto-Cota, A.; Ramírez-Wong, B. Preparation and Properties of Chitosan–PVA Fibers Produced by Wet Spinning. J. Polym. Environ. 2018, 26, 946–958. [Google Scholar] [CrossRef]
- Teixeira, M.A.; Amorim, M.T.P.; Felgueiras, H.P. Poly(Vinyl Alcohol)-Based Nanofibrous Electrospun Scaffolds for Tissue Engineering Applications. Polymers 2019, 12, 7. [Google Scholar] [CrossRef]
- Ameer, J.M.; Anil Kumar, P.R.; Kasoju, N. Strategies to Tune Electrospun Scaffold Porosity for Effective Cell Response in Tissue Engineering. J. Funct. Biomater. 2019, 10, 30. [Google Scholar] [CrossRef]
- Sisson, K.; Zhang, C.; Farach-Carson, M.C.; Chase, D.B.; Rabolt, J.F. Fiber Diameters Control Osteoblastic Cell Migration and Differentiation in Electrospun Gelatin. J. Biomed. Mater. Res. A 2010, 94, 1312–1320. [Google Scholar] [CrossRef] [PubMed]
- Osorio-Arciniega, R.; García-Hipólito, M.; Alvarez-Fregoso, O.; Alvarez-Perez, M.A. Composite Fiber Spun Mat Synthesis and In Vitro Biocompatibility for Guide Tissue Engineering. Molecules 2021, 26, 7597. [Google Scholar] [CrossRef]
- Xie, J.; Shen, H.; Yuan, G.; Lin, K.; Su, J. The Effects of Alignment and Diameter of Electrospun Fibers on the Cellular Behaviors and Osteogenesis of BMSCs. Mater. Sci. Eng. C 2021, 120, 111787. [Google Scholar] [CrossRef]
- Hegedűs, V. Experimental Studies with Novel Synthetic Bone Replacement Materials, Potentially Usable in Dentistry. Ph.D. Thesis, University of Debrecen, Debrecen, Hungary, 2022. Available online: https://hdl.handle.net/2437/341448 (accessed on 16 December 2022).
- Gröninger, O.; Hess, S.; Mohn, D.; Schneider, E.; Stark, W.; Märsmann, S.; Wolint, P.; Calcagni, M.; Cinelli, P.; Buschmann, J. Directing Stem Cell Commitment by Amorphous Calcium Phosphate Nanoparticles Incorporated in PLGA: Relevance of the Free Calcium Ion Concentration. Int. J. Mol. Sci. 2020, 21, 2627. [Google Scholar] [CrossRef]
- Wang, S.; Hu, F.; Li, J.; Zhang, S.; Shen, M.; Huang, M.; Shi, X. Design of Electrospun Nanofibrous Mats for Osteogenic Differentiation of Mesenchymal Stem Cells. Nanomed. Nanotechnol. Biol. Med. 2018, 14, 2505–2520. [Google Scholar] [CrossRef] [PubMed]
- Gosain, A.K.; Santoro, T.D.; Song, L.S.; Capel, C.C.; Sudhakar, P.V.; Matloub, H.S. Osteogenesis in Calvarial Defects: Contribution of the Dura, the Pericranium, and the Surrounding Bone in Adult versus Infant Animals. Plast. Reconstr. Surg. 2003, 112, 515–527. [Google Scholar] [CrossRef] [PubMed]
- Özerdem, Ö.R.; Anlatici, R.; Bahar, T.; Kayaselçuk, F.; Barutçu, Ö.; Tuncer, I.; Şen, O. Roles of Periosteum, Dura, and Adjacent Bone on Healing of Cranial Osteonecrosis. J. Craniofac. Surg. 2003, 14, 359. [Google Scholar] [CrossRef]
- Wang, J.; Glimcher, M.J. Characterization of Matrix-Induced Osteogenesis in Rat Calvarial Bone Defects: II. Origins of Bone-Forming Cells. Calcif. Tissue Int. 1999, 65, 486–493. [Google Scholar] [CrossRef]
- Park, P.S.U.; Raynor, W.Y.; Sun, Y.; Werner, T.J.; Rajapakse, C.S.; Alavi, A. 18F-Sodium Fluoride PET as a Diagnostic Modality for Metabolic, Autoimmune, and Osteogenic Bone Disorders: Cellular Mechanisms and Clinical Applications. Int. J. Mol. Sci. 2021, 22, 6504. [Google Scholar] [CrossRef] [PubMed]
- Lienemann, P.S.; Metzger, S.; Kiveliö, A.S.; Blanc, A.; Papageorgiou, P.; Astolfo, A.; Pinzer, B.R.; Cinelli, P.; Weber, F.E.; Schibli, R.; et al. Longitudinal in Vivo Evaluation of Bone Regeneration by Combined Measurement of Multi-Pinhole SPECT and Micro-CT for Tissue Engineering. Sci. Rep. 2015, 5, 10238. [Google Scholar] [CrossRef]
- Ventura, M.; Boerman, O.C.; De Korte, C.; Rijpkema, M.; Heerschap, A.; Oosterwijk, E.; Jansen, J.A.; Walboomers, X.F. Preclinical Imaging in Bone Tissue Engineering. Tissue Eng. Part B Rev. 2014, 20, 578–595. [Google Scholar] [CrossRef]
- Jamari, J.; Ammarullah, M.I.; Santoso, G.; Sugiharto, S.; Supriyono, T.; van der Heide, E. In Silico Contact Pressure of Metal-on-Metal Total Hip Implant with Different Materials Subjected to Gait Loading. Metals 2022, 12, 1241. [Google Scholar] [CrossRef]
- Van hede, D.; Liang, B.; Anania, S.; Barzegari, M.; Verlée, B.; Nolens, G.; Pirson, J.; Geris, L.; Lambert, F. 3D-Printed Synthetic Hydroxyapatite Scaffold With In Silico Optimized Macrostructure Enhances Bone Formation In Vivo. Adv. Funct. Mater. 2022, 32, 2105002. [Google Scholar] [CrossRef]
- Hegedűs, C.; Czibulya, Z.; Tóth, F.; Dezső, B.; Hegedűs, V.; Boda, R.; Horváth, D.; Csík, A.; Fábián, I.; Tóth-Győri, E.; et al. The Effect of Heat Treatment of β-Tricalcium Phosphate-Containing Silica-Based Bioactive Aerogels on the Cellular Metabolism and Proliferation of MG63 Cells. Biomedicines 2022, 10, 662. [Google Scholar] [CrossRef]
- Vajgel, A.; Mardas, N.; Farias, B.C.; Petrie, A.; Cimões, R.; Donos, N. A Systematic Review on the Critical Size Defect Model. Clin. Oral Implants Res. 2014, 25, 879–893. [Google Scholar] [CrossRef] [PubMed]








| Wavenumber (cm−1) | Assignation | Wavenumber (cm−1) | Assignation |
|---|---|---|---|
| 3317.5 m br | ν(OH) | 1328.3 | δ(CH + OH) |
| 2939.5 w | ν(CH2) | 1239.5 | γw(CH) |
| 2913.0 w | ν(CH2) | 1200 sh | ν(C-O) |
| 2873.5 vw sh | ν(CH) | 1081.4 | ν(C-O) |
| 1713.0 | ν(C=O), amide-I | 944.5 | |
| 1585.2 | amide-II | 899.2 | γr(CH2) |
| 1417.0 | δ(CH2) | 842.8 | ν(CC) |
| 1375.0 | γw(CH2) |
| 1 Month SUVmean | 3 Months SUVmean | 6 Months SUVmean | |
|---|---|---|---|
| FM implant | 5.41 ± 1.12 | 6.84 ± 1.01 | 7.40 ± 1.03 |
| BTCP-AE-FM implant | 5.53 ± 1.08 | 8.48 ± 0.94 | 10.72 ± 1.11 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Boda, R.; Lázár, I.; Keczánné-Üveges, A.; Bakó, J.; Tóth, F.; Trencsényi, G.; Kálmán-Szabó, I.; Béresová, M.; Sajtos, Z.; D. Tóth, E.; et al. β-Tricalcium Phosphate-Modified Aerogel Containing PVA/Chitosan Hybrid Nanospun Scaffolds for Bone Regeneration. Int. J. Mol. Sci. 2023, 24, 7562. https://doi.org/10.3390/ijms24087562
Boda R, Lázár I, Keczánné-Üveges A, Bakó J, Tóth F, Trencsényi G, Kálmán-Szabó I, Béresová M, Sajtos Z, D. Tóth E, et al. β-Tricalcium Phosphate-Modified Aerogel Containing PVA/Chitosan Hybrid Nanospun Scaffolds for Bone Regeneration. International Journal of Molecular Sciences. 2023; 24(8):7562. https://doi.org/10.3390/ijms24087562
Chicago/Turabian StyleBoda, Róbert, István Lázár, Andrea Keczánné-Üveges, József Bakó, Ferenc Tóth, György Trencsényi, Ibolya Kálmán-Szabó, Monika Béresová, Zsófi Sajtos, Etelka D. Tóth, and et al. 2023. "β-Tricalcium Phosphate-Modified Aerogel Containing PVA/Chitosan Hybrid Nanospun Scaffolds for Bone Regeneration" International Journal of Molecular Sciences 24, no. 8: 7562. https://doi.org/10.3390/ijms24087562
APA StyleBoda, R., Lázár, I., Keczánné-Üveges, A., Bakó, J., Tóth, F., Trencsényi, G., Kálmán-Szabó, I., Béresová, M., Sajtos, Z., D. Tóth, E., Deák, Á., Tóth, A., Horváth, D., Gaál, B., Daróczi, L., Dezső, B., Ducza, L., & Hegedűs, C. (2023). β-Tricalcium Phosphate-Modified Aerogel Containing PVA/Chitosan Hybrid Nanospun Scaffolds for Bone Regeneration. International Journal of Molecular Sciences, 24(8), 7562. https://doi.org/10.3390/ijms24087562









