The Management of COVID-19-Related Coagulopathy: A Focus on the Challenges of Metabolic and Vascular Diseases
Abstract
1. Introduction
2. Materials and Methods
3. Proinflammatory and Procoagulant Effects of COVID-19
4. Low-Grade Chronic Inflammation and Its Consequences in COVID-19 Patients with Comorbidities
5. Assessment of Hemostatic Activity in COVID-19
6. Management of COVID-19 Patients
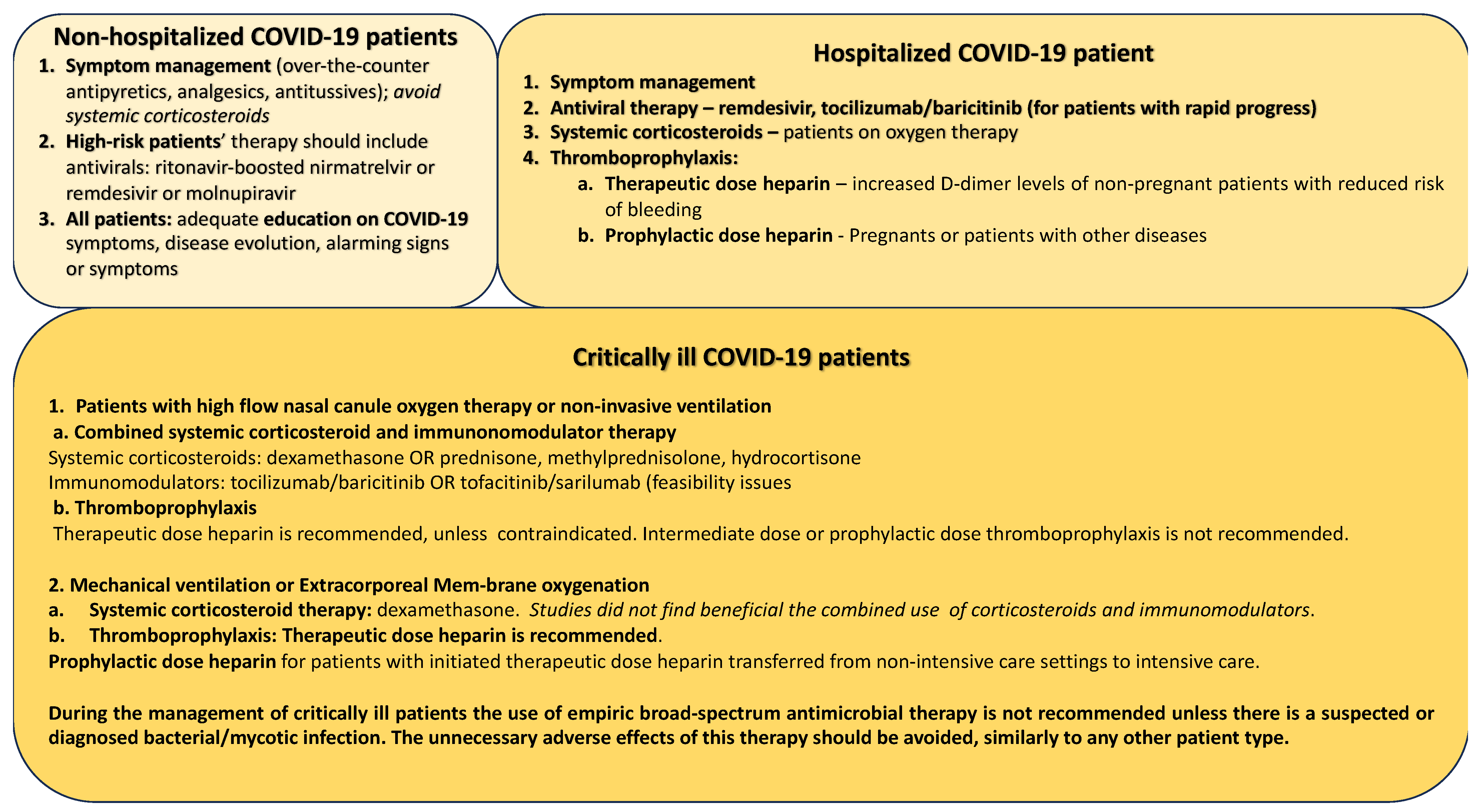
6.1. The Therapeutic Approach of COVID-19
Multisystem Inflammatory Syndrome (MIS)
6.2. The Therapeutic Approach to COVID-19 Coagulopathy
6.3. Therapy of Comorbidities in COVID-19 Patients
7. Discussion
8. Originality and Limitations of the Paper
9. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Djaharuddin, I.; Munawwarah, S.; Nurulita, A.; Ilyas, M.; Tabri, N.A.; Lihawa, N. Comorbidities and mortality in COVID-19 patients. Gac. Sanit. 2021, 35, S530–S532. [Google Scholar] [CrossRef]
- Fekete, M.; Szarvas, Z.; Fazekas-Pongor, V.; Kováts, Z.; Müller, V.; Varga, J.T. Ambuláns rehabilitációs programok COVID–19-betegek számára (Outpatient rehabilitation programs for COVID-19 patients). Orvosi Hetil. 2021, 162, 1671–1677. [Google Scholar]
- Mureșan, A.V.; Russu, E.; Arbănași, E.M.; Kaller, R.; Hosu, I.; Arbănași, E.M.; Voidăzan, S.T. Negative Impact of the COVID-19 Pandemic on Kidney Disease Management—A Single-Center Experience in Romania. J. Clin. Med. 2022, 11, 2452. [Google Scholar]
- Wu, Z.; McGoogan, J. Outbreak in China: Summary of a report of 72314 cases from the Chinese center for disease control and prevention. JAMA 2020, 323, 1239–1242. [Google Scholar]
- Li, Y.; Zhang, Z.; Yang, L.; Lian, X.; Xie, Y.; Li, S.; Xin, S.; Cao, P.; Lu, J. The MERS-CoV receptor DPP4 as a candidate binding target of the SARS-CoV-2 spike. Iscience 2020, 23, 101160. [Google Scholar]
- Onder, G.; Rezza, G.; Brusaferro, S. Case-fatality rate and characteristics of patients dying in relation to COVID-19 in Italy. JAMA 2020, 323, 1775–1776. [Google Scholar]
- Carvalho, D.B.; Ferreira, V.L.; Assunção, C.M.; Silva, J.A.; Augusto, M.F.; da Silva, R.V.; da Silva Lacerda Filho, S.L.; de Lima Goulart, T.; Fonseca, I.F.; de Figueiredo Júnior, H.S. Uma análise acerca das características das coagulopatias na Covid-19: Revisão de literatura (Analysis on the characteristics of coagulopathy in Covid-19: A literature review). Rev. Eletrônica Acervo Médico 2022, 6, e10074. [Google Scholar]
- Garreta, E.; Prado, P.; Stanifer, M.L.; Monteil, V.; Marco, A.; Ullate-Agote, A.; Moya-Rull, D.; Vilas-Zornoza, A.; Tarantino, C.; Romero, J.P.; et al. A diabetic milieu increases ACE2 expression and cellular susceptibility to SARS-CoV-2 infections in human kidney organoids and patient cells. Cell Metab. 2022, 34, 857–873. [Google Scholar]
- Kazakou, P.; Lambadiari, V.; Ikonomidis, I.; Kountouri, A.; Panagopoulos, G.; Athanasopoulos, S.; Korompoki, E.; Kalomenidis, I.; Dimopoulos, M.A.; Mitrakou, A. Diabetes and COVID-19; a bidirectional interplay. Front. Endocrinol. 2022, 13, 780663. [Google Scholar]
- Kedia-Mehta, N.; Tobin, L.; Zaiatz-Bittencourt, V.; Pisarska, M.M.; De Barra, C.; Choi, C.; Elamin, E.; O’Shea, D.; Gardiner, C.M.; Finlay, D.K.; et al. Cytokine-induced natural killer cell training is dependent on cellular metabolism and is defective in obesity. Blood Adv. 2021, 5, 4447–4455. [Google Scholar]
- Kreiner, F.F.; Kraaijenhof, J.M.; von Herrath, M.; Hovingh, G.K.; von Scholten, B.J. Interleukin 6 in diabetes, chronic kidney disease, and cardiovascular disease: Mechanisms and therapeutic perspectives. Expert Rev. Clin. Immunol. 2022, 18, 377–389. [Google Scholar]
- Martín-Núñez, E.; Donate-Correa, J.; Ferri, C.; López-Castillo, Á.; Delgado-Molinos, A.; Hernández-Carballo, C.; Pérez-Delgado, N.; Rodríguez-Ramos, S.; Cerro-López, P.; Tagua, V.G.; et al. Association between serum levels of Klotho and inflammatory cytokines in cardiovascular disease: A case-control study. Aging 2020, 12, 1952. [Google Scholar]
- Huang, C.; Wang, Y.; Li, X.; Ren, L.; Zhao, J.; Hu, Y.; Zhang, L.; Fan, G.; Xu, J.; Gu, X.; et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar]
- Lelapi, N.; Licastro, N.; Provenzano, M.; Andreucci, M.; Franciscis, S.D.; Serra, R. Cardiovascular disease as a biomarker for an increased risk of COVID-19 infection and related poor prognosis. Biomark. Med. 2020, 14, 713–716. [Google Scholar]
- Hartmann, J.; Ergang, A.; Mason, D.; Dias, J.D. The Role of TEG Analysis in Patients with COVID-19-Associated Coagulopathy: A Systematic Review. Diagnostics 2021, 11, 172. [Google Scholar]
- Pavoni, V.; Gianesello, L.; Pazzi, M.; Dattolo, P.; Prisco, D. Questions about COVID-19 associated coagulopathy: Possible answers from the viscoelastic tests. J. Clin. Monit. Comput. 2022, 36, 55–69. [Google Scholar]
- Tyler, A.; Yang, P.D.; Snider, L.M.; Lerner, S.B.; Aird, W.C.; Shapiro, N.I. New Uses for Thromboelastography and Other Forms of Viscoelastic Monitoring in the Emergency Department: A Narrative Review. Ann. Emerg. Med. 2021, 77, 357–366. [Google Scholar]
- Giubelan, L.; Dragonu, L.; Stoian, A.C.; Dumitrescu, F. O analiză intermediară a formelor medii şi severe de Covid-19 tratate în Clinica de Boli infecţioase Craiova (An intermediate analysis on moderate and severe Covid-19 cases treated at the Infectious Disease Clinic in Craiova). Rom. J. Infect. Dis. 2020, 23, 272–277. [Google Scholar] [CrossRef]
- Mureșan, A.V.; Hălmaciu, I.; Arbănași, E.M.; Kaller, R.; Arbănași, E.M.; Budișcă, O.A.; Melinte, R.M.; Vunvulea, V.; Filep, R.C.; Mărginean, L.; et al. Prognostic Nutritional Index, Controlling Nutritional Status (CONUT) Score, and Inflammatory Biomarkers as Predictors of Deep Vein Thrombosis, Acute Pulmonary Embolism, and Mortality in COVID-19 Patients. Diagnostics 2022, 12, 2757. [Google Scholar]
- Sun, D.W.; Zhang, D.; Tian, R.H.; Li, Y.; Wang, Y.S.; Cao, J.; Tang, Y.; Zhang, N.; Zan, T.; Gao, L.; et al. The underlying changes and predicting role of peripheral blood inflammatory cells in severe COVID-19 patients: A sentinel? Clin. Chim. Acta 2020, 508, 122–129. [Google Scholar]
- Zhang, H.; Penninger, J.M.; Li, Y.; Zhong, N.; Slutsky, A.S. Angiotensin-converting enzyme 2 (ACE2) as a SARS-CoV-2 receptor: Molecular mechanisms and potential therapeutic target. Intensive Care Med. 2020, 46, 586–590. [Google Scholar]
- Ragab, D.; Salah Eldin, H.; Taeimah, M.; Khattab, R.; Salem, R. The COVID-19 Cytokine Storm; What We Know So Far. Front. Immunol. 2020, 11, 1446. [Google Scholar]
- Gómez-Mesa, J.E.; Galindo-Coral, S.; Montes, M.C.; Martin, A.J.M. Thrombosis and Coagulopathy in COVID-19. Curr. Probl. Cardiol. 2021, 46, 100742. [Google Scholar]
- Tomerak, S.; Khan, S.; Almasri, M.; Hussein, R.; Abdelati, A.; Aly, A.; Salameh, M.A.; Saed Aldien, A.; Naveed, H.; Elshazly, M.B.; et al. Systemic inflammation in COVID-19 patients may induce various types of venous and arterial thrombosis: A systematic review. Scand. J. Immunol. 2021, 94, e13097. [Google Scholar]
- Savla, S.R.; Prabhavalkar, K.S.; Bhatt, L.K. Cytokine storm associated coagulation complications in COVID-19 patients: Pathogenesis and Management. Expert Rev. Anti-Infect. Ther. 2021, 19, 1397–1413. [Google Scholar]
- Lima-Martínez, M.M.; Boada, C.C.; Madera-Silva, M.D.; Marín, W.; Contreras, M. Covid-19 y diabetes mellitus: Una relación bidireccional (Covid-19 and diabetes: A bidirectional relationship). Clin. Investig. Arterioscler. 2021, 33, 151–157. [Google Scholar]
- Vudu, S.; Cazac, N.; Munteanu, D.; Vudu, L. Impactul COVID-19 la pacienţii cu diabet zaharat şi alte maladii endocrine (The impact of COVID-19 in patients with diabetes mellitus and other endocrine diseases). MJHS 2020, 2, 49–58. [Google Scholar]
- Lighter, J.; Phillips, M.; Hochman, S.; Sterling, S.; Johnson, D.; Francois, F.; Stachel, A. Obesity in patients younger than 60 years is a risk factor for COVID-19 hospital admission. Clin. Infect. Dis. 2020, 71, 896–897. [Google Scholar]
- García, L.F.; Gutiérrez, A.B.; Bascones, M.G. Relación entre obesidad, diabetes e ingreso en UCI en pacientes COVID-19 (Relationship between obesity, diabetes and ICU admission in COVID-19 patients). Med. Clin. 2020, 155, 314–315. [Google Scholar]
- Arentz, C.; Wild, F. Vergleich Europäischer Gesundheitssysteme in der COVID-19-Pandemie (Comparison of European Healthcare Systems in the COVID-19 Pandemic); WIP-Wissenschaftliches Institut der PKV: Köln, Germany, 2020; Volume 3. [Google Scholar]
- Simonnet, A.; Chetboun, M.; Poissy, J.; Raverdy, V.; Noulette, J.; Duhamel, A.; Labreuche, J.; Mathieu, D.; Pattou, F.; Jourdain, M.; et al. High prevalence of obesity in severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) requiring invasive mechanical ventilation. Obesity 2020, 28, 1195–1199. [Google Scholar]
- Ruan, Q.; Yang, K.; Wang, W.; Jiang, L.; Song, J. Clinical predictors of mortality due to COVID-19 based on an analysis of data of 150 patients from Wuhan, China. Intensive Care Med. 2020, 46, 846–848. [Google Scholar]
- Gardner, A.J.; Kirkin, D.J.; Rodriguez-Villar, S.; Abellanas, G.L.; Tee, A.; Valentin, A. Antithrombin III deficiency-induced coagulopathy in the context of COVID-19: A case series. Br. J. Haematol. 2021, 194, 1007–1009. [Google Scholar]
- Jonigk, D.; Werlein, C.; Lee, P.D.; Kauczor, H.U.; Länger, F.; Ackermann, M. Pulmonale und systemische Pathologie bei COVID-19 (Pulmonary and systemic pathology in COVID-19). Dtsch. Ärztebl. Int. 2022, 119, 429–435. [Google Scholar]
- Tang, N.; Li, D.; Wang, X.; Sun, Z. Abnormal coagulation parameters are associated with poor prognosis in patients with novel coronavirus pneumonia. J. Thromb. Haemost. 2020, 18, 844–847. [Google Scholar]
- Tilinca, M.C.; Merlan, I.; Salcudean, A.; Tilea, I.; Nemes-Nagy, E. Oxidative stress and cytokines’ involvement in the occurence and progression of diabetic complications in the COVID-19 pandemic context. Farmacia 2021, 69, 635–641. [Google Scholar]
- Zhang, Y.; Li, H.; Zhang, J.; Cao, Y.; Zhao, X.; Yu, N.; Gao, Y.; Ma, J.; Zhang, H.; Zhang, J.; et al. The clinical characteristics and outcomes of patients with diabetes and secondary hyperglycaemia with coronavirus disease 2019: A single-centre, retrospective, observational study in Wuhan. Diabetes Obes. Metab. 2020, 22, 1443–1454. [Google Scholar]
- Zhu, L.; She, Z.G.; Cheng, X.; Qin, J.J.; Zhang, X.J.; Cai, J.; Lei, F.; Wang, H.; Xie, J.; Wang, W.; et al. Association of blood glucose control and outcomes in patients with COVID-19 and pre-existing type 2 diabetes. Cell Metab. 2020, 31, 1068–1077. [Google Scholar]
- Iba, T.; Levy, J.H.; Levi, M.; Connors, J.M.; Thachil, J. Coagulopathy of coronavirus disease 2019. Crit. Care Med. 2020, 48, 1358–1364. [Google Scholar]
- Connors, J.M.; Levy, J.H. COVID-19 and its implications for thrombosis and anticoagulation. Blood 2020, 135, 2033–2040. [Google Scholar]
- Christensen, B.; Favaloro, E.J.; Lippi, G.; Van Cott, E.M. Hematology laboratory abnormalities in patients with coronavirus disease 2019 (COVID-19). Semin. Thromb. Hemost. 2020, 46, 845–849. [Google Scholar]
- Zhou, F.; Yu, T.; Du, R.; Fan, G.; Liu, Y.; Liu, Z.; Xiang, J.; Wang, Y.; Song, B.; Gu, X.; et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: A retrospective cohort study. Lancet 2020, 395, 1054–1062. [Google Scholar]
- Iba, T.; Levy, J.H.; Levi, M.; Thachil, J. Coagulopathy in COVID-19. J. Thromb. Haemost. 2020, 18, 2103–2109. [Google Scholar]
- Zhao, X.; Wang, K. Early decrease in blood platelet count is associated with poor prognosis in COVID-19 patients—Indications for predictive, preventive, and personalized medical approach. EPMA J. 2020, 11, 139–145. [Google Scholar]
- Tchachil, J. What do monitoring platelet counts in COVID-19 teach us? J. Thromb. Haemost. 2020, 18, 2071–2072. [Google Scholar] [CrossRef]
- Peyvandi, F.; Artoni, A.; Novembrino, C.; Aliberti, S.; Panigada, M.; Boscarino, M.; Gualtierotti, R.; Rossi, F.; Palla, R.; Martinelli, I.; et al. Hemostatic alterations in COVID-19. Haematologica 2021, 106, 1472–1475. [Google Scholar]
- Stefely, J.A.; Christensen, B.B.; Gogakos, T.; Cone Sullivan, J.K.; Montgomery, G.G.; Barranco, J.P.; Van Cott, E.M. Marked factor V activity elevation in severe COVID-19 is associated with venous thromboembolism. Am. J. Hematol. 2020, 95, 1522–1530. [Google Scholar]
- Asmis, L.; Hellstern, P. Thrombophilia Testing—A Systematic Review. Clin. Lab. 2023, 69, 670–691. [Google Scholar] [CrossRef]
- Ferrari, E.; Sartre, B.; Squara, F.; Contenti, J.; Occelli, C.; Lemoel, F.; Levraut, J.; Doyen, D.; Dellamonica, J.; Mondain, V.; et al. High Prevalence of Acquired Thrombophilia Without Prognosis Value in Patients with Coronavirus Disease 2019. J. Am. Heart Assoc. 2020, 9, e017773. [Google Scholar]
- Zhang, Y.; Cao, W.; Jiang, W.; Xiao, M.; Li, Y.; Tang, N.; Liu, Z.; Yan, X.; Zhao, Y.; Li, T.; et al. Profile of natural anticoagulant, coagulant factor and anti-phospholipid antibody in critically ill COVID-19 patients. J. Thromb. Thrombolysis 2020, 50, 580–586. [Google Scholar]
- Mitrovic, M.; Sabljic, N.; Cvetkovic, Z.; Pantic, N.; Zivkovic Dakic, A.; Bukumiric, Z.; Libek, V.; Savic, N.; Milenkovic, B.; Virijevic, M.; et al. Rotational Thromboelastometry (ROTEM) Profiling of COVID–19 Patients. Platelets 2021, 32, 690–696. [Google Scholar] [CrossRef]
- Zátroch, I.; Smudla, A.; Babik, B.; Tánczos, K.; Kóbori, L.; Szabó, Z.; Fazakas, J. Procoagulation, hypercoagulatio és fibrinolysis “shut down” kimutatása ClotPro® viszkoelasztikus tesztek segítségével COVID-19 betegekben (Procoagulation, hypercoagulation and fibrinolytic “shut down” detected with ClotPro® viscoelastic tests in COVID-19 patients). Orvosi Hetil. 2020, 161, 899–907. [Google Scholar]
- Volod, O.; Bunch, C.M.; Zackariya, N.; Moore, E.E.; Moore, H.B.; Kwaan, H.C.; Neal, M.D.; Al-Fadhl, M.D.; Patel, S.S.; Wiarda, G.; et al. Viscoelastic Hemostatic Assays: A Primer on Legacy and New Generation Devices. J. Clin. Med. 2022, 11, 860. [Google Scholar]
- Gergi, M.; Goodwin, A.; Freeman, K.; Colovos, C.; Volod, O. Viscoelastic hemostasis assays in septic, critically ill coronavirus disease 2019 patients: A practical guide for clinicians. Blood Coagul. Fibrinolysis 2021, 32, 225–228. [Google Scholar] [CrossRef]
- Bachler, M.; Bosch, J. Impaired fibrinolysis in critically ill COVID-19 patients. Br. J. Anaesth. 2021, 126, 590–598. [Google Scholar]
- Schrick, D.; Tőkés-Füzesi, M.; Réger, B.; Molnár, T. Plasma Fibrinogen Independently Predicts Hypofibrinolysis in Severe COVID-19. Metabolites 2021, 11, 826. [Google Scholar]
- Centers for Disease Control and Prevention. Underlying Medical Conditions Associated with HIGHER risk for Severe COVID-19: Information for Healthcare Professionals. 2023. Available online: https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-care/underlyingconditions.html (accessed on 20 June 2023).
- RECOVERY Collaborative Group. Dexamethasone in hospitalized patients with COVID-19. N. Engl. J. Med. 2021, 384, 693–704. [Google Scholar] [CrossRef]
- Caly, L.; Druce, J.D.; Catton, M.G.; Jans, D.A.; Wagstaff, K.M. The FDA-approved drug ivermectin inhibits the replication of SARS-CoV-2 in vitro. Antivir. Res. 2020, 178, 104787. [Google Scholar] [CrossRef]
- Chaccour, C.; Hammann, F.; Ramón-García, S.; Rabinovich, N.R. Ivermectin and COVID-19: Keeping rigor in times of urgency. Am. J. Trop. Med. Hyg. 2020, 102, 1156–1157. [Google Scholar] [CrossRef]
- TOGETHER Investigators. Effect of early treatment with ivermectin among patients with COVID-19. N. Engl. J. Med. 2022, 40, 1721–1731. [Google Scholar]
- Naggie, S.; Boulware, D.R.; Lindsell, C.J.; Stewart, T.G.; Gentile, N.; Collins, S.; McCarthy, M.W.; Jayaweera, D.; Castro, M.; Sulkowski, M.; et al. Effect of ivermectin vs placebo on time to sustained recovery in outpatients with mild to moderate COVID-19: A randomized controlled trial. JAMA 2022, 328, 1595–1603. [Google Scholar]
- Lim, S.C.L.; Hor, C.P.; Tay, K.H.; Jelani, A.M.; Tan, W.H.; Ker, H.B.; Chow, T.S.; Zaid, M.; Cheah, W.K.; Lim, H.H.; et al. Efficacy of ivermectin treatment on disease progression among adults with mild to moderate COVID-19 and comorbidities: The I-TECH randomized clinical trial. JAMA Intern. Med. 2022, 182, 426–435. [Google Scholar] [CrossRef] [PubMed]
- Food and Drug Administration. Fact Sheet for Healthcare Providers: Emergency Use Authorization for Paxlovid; Food and Drug Administration: Silver Spring, MD, USA, 2023.
- Toussi, S.S.; Neutel, J.M.; Navarro, J.; Preston, R.A.; Shi, H.; Kavetska, O.; LaBadie, R.R.; Binks, M.; Chan, P.L.; Demers, N.; et al. Pharmacokinetics of oral nirmatrelvir/ritonavir, a protease inhibitor for treatment of COVID-19, in subjects with renal impairment. Clin. Pharmacol. Ther. 2022, 112, 892–900. [Google Scholar] [CrossRef]
- Gliga, S.; Lübke, N.; Killer, A.; Gruell, H.; Walker, A.; Dilthey, A.T.; Thielen, A.; Lohr, C.; Flaßhove, C.; Krieg, S.; et al. Rapid selection of sotrovimab escape variants in severe acute respiratory syndrome coronavirus 2 Omicron-infected immunocompromised patients. Clin. Infect. Dis. 2023, 76, 408–415. [Google Scholar] [CrossRef] [PubMed]
- Food and Drug Administration. Fact Sheet for Healthcare Providers: Emergency Use Authorization (EUA) of Sotrovimab. 2022. Available online: https://www.fda.gov/media/149534/download (accessed on 13 May 2023).
- Food and Drug Administration. Fact Sheet for Healthcare Providers: Emergency Use Authorization for Evusheld (Tixagevimab Co-Packaged with Cilgavimab). 2023. Available online: https://www.fda.gov/media/154701/download (accessed on 13 May 2023).
- Food and Drug Administration. Fact Sheet for Healthcare Providers: Emergency Use Authorization for Bebtelovimab. 2022. Available online: https://www.fda.gov/media/156152/download (accessed on 13 May 2023).
- Imai, M.; Ito, M.; Kiso, M.; Yamayoshi, S.; Uraki, R.; Fukushi, S.; Watanabe, S.; Suzuki, T.; Maeda, K.; Sakai-Tagawa, Y.; et al. Efficacy of antiviral agents against Omicron subvariants BQ.1.1 and XBB. N. Engl. J. Med. 2023, 388, 89–91. [Google Scholar] [CrossRef] [PubMed]
- Wang, Q.; Iketani, S.; Li, Z.; Liu, L.; Guo, Y.; Huang, Y.; Bowen, A.D.; Liu, M.; Wang, M.; Yu, J.; et al. Alarming antibody evasion properties of rising SARS-CoV-2 BQ and XBB subvariants. Cell 2023, 186, 279–286.e8. [Google Scholar] [CrossRef]
- Wang, Q.; Li, Z.; Ho, J.; Guo, Y.; Yeh, A.Y.; Mohri, H.; Liu, M.; Wang, M.; Yu, J.; Shah, J.G.; et al. Resistance of SARS-CoV-2 Omicron subvariant BA.4.6. to antibody neutralisation. Lancet Infect. Dis. 2022, 22, 1666–1668. [Google Scholar] [CrossRef] [PubMed]
- Takashita, E.; Yamayoshi, S.; Simon, V.; Van Bakel, H.; Sordillo, E.M.; Pekosz, A.; Fukushi, S.; Suzuki, T.; Maeda, K.; Halfmann, P.; et al. Efficacy of antibodies and antiviral drugs against Omicron BA.2.12.1, BA.4, and BA.5 subvariants. N. Engl. J. Med. 2022, 387, 468–470. [Google Scholar] [CrossRef]
- Morris, S.B.; Schwartz, N.G.; Patel, P.; Abbo, L.; Beauchamps, L.; Balan, S.; Lee, E.H.; Paneth-Pollak, R.; Geevarughese, A.; Lash, M.K.; et al. Case series of multisystem inflammatory syndrome in adults associated with SARS-CoV-2 infection—United Kingdom and United States, March-August 2020. Morb. Mortal. Wkly. Rep. 2020, 69, 1450–1456. [Google Scholar] [CrossRef]
- Sansone, M.; Studahl, M.; Berg, S.; Gisslen, M.; Sundell, N. Severe multisystem inflammatory syndrome (MIS-C/A) after confirmed SARS-CoV-2 infection: A report of four adult cases. Infect. Dis. 2022, 54, 378–383. [Google Scholar] [CrossRef]
- Martins, A.; Policarpo, S.; Silva-Pinto, A.; Santos, A.S.; Figueiredo, P.; Sarmento, A.; Santos, L. SARS-CoV-2-related multisystem inflammatory syndrome in adults. Eur. J. Case Rep. Intern. Med. 2021, 8, 003025. [Google Scholar] [CrossRef]
- Available online: https://www.cdc.gov/mis/mis-a/hcp.html (accessed on 2 May 2023).
- Worku, D. Multisystem Inflammatory Syndrome in Adults (MIS-A) and SARS-CoV2: An Evolving Relationship. BioMed 2023, 3, 195–201. [Google Scholar] [CrossRef]
- Santos, M.O.; Gonçalves, L.C.; Silva, P.A.N.; Moreira, A.L.E.; Ito, C.R.M.; Peixoto, F.A.O.; Wastowski, I.J.; Carneiro, L.C.; Avelino, M.A.G. Multisystem inflammatory syndrome (MIS-C): A systematic review and meta-analysis of clinical characteristics, treatment, and outcomes. J. Pediatr. 2022, 98, 338–349. [Google Scholar] [CrossRef]
- Riollano-Cruz, M.; Akkoyun, E.; Briceno-Brito, E.; Kowalsky, S.; Reed, J.; Posada, R.; Sordillo, E.M.; Tosi, M.; Trachtman, R.; Paniz-Mondolfi, A. Multisystem inflammatory syndrome in children related to COVID-19: A New York City experience. J. Med. Virol. 2021, 93, 424–433. [Google Scholar] [CrossRef] [PubMed]
- Gross, O.; Moerer, O.; Rauen, T.; Boeckhaus, J.; Hoxha, E.; Joerres, A.; Kamm, M.; Elfanish, A.; Windisch, W.; Dreher, M.; et al. Validation of a Prospective Urinalysis-Based Prediction Model for ICU Resources and Outcome of COVID-19 Disease: A Multicenter Cohort Study. J. Clin. Med. 2021, 10, 3049. [Google Scholar] [CrossRef]
- ESC guidance for the diagnosis and management of cardiovascular disease during the COVID-19 pandemic: Part 2—Care pathways, treatment, and follow-up. Cardiovasc. Res. 2022, 118, 1618–1666. [CrossRef]
- Nykänen, A.I.; Selby, R.; McRae, K.M.; Zhao, Y.; Asghar, U.M.; Donahoe, L.; Granton, J.; de Perrot, M. Pseudo heparin resistance after pulmonary endarterectomy: Role of thrombus production of Factor VIII. Semin. Thorac. Cardiovasc. Surg. 2022, 34, 315–323. [Google Scholar] [CrossRef] [PubMed]
- White, D.; MacDonald, S.; Bull, T.; Hayman, M.; de Monteverde-Robb, R.; Sapsford, D.; Lavinio, A.; Varley, J.; Johnston, A.; Besser, M.; et al. Heparin resistance in COVID-19 patients in the intensive care unit. J. Thromb. Thrombolysis 2020, 50, 287–291. [Google Scholar] [CrossRef] [PubMed]
- Levy, J.H.; Connors, J.M. Heparin resistance—Clinical perspectives and management strategies. N. Engl. J. Med. 2021, 385, 826–832. [Google Scholar] [CrossRef] [PubMed]
- ATTACC Investigators; ACTIV-4a Investigators; REMAP-CAP Investigators. Therapeutic anticoagulation with heparin in noncritically ill patients with COVID-19. N. Engl. J. Med. 2021, 385, 790–802. [Google Scholar] [CrossRef] [PubMed]
- Sholzberg, M.; Tang, G.H.; Rahhal, H.; AlHamzah, M.; Kreuziger, L.B.; Áinle, F.N.; Alomran, F.; Alayed, K.; Alsheef, M.; AlSumait, F.; et al. Effectiveness of therapeutic heparin versus prophylactic heparin on death, mechanical ventilation, or intensive care unit admission in moderately ill patients with COVID-19 admitted to hospital: RAPID randomised clinical trial. BMJ 2021, 375, n2400. [Google Scholar] [CrossRef]
- Spyropoulos, A.C.; Goldin, M.; Giannis, D.; Diab, W.; Wang, J.; Khanijo, S.; Mignatti, A.; Gianos, E.; Cohen, M.; Sharifova, G.; et al. Efficacy and safety of therapeutic-dose heparin vs standard prophylactic or intermediate-dose heparins for thromboprophylaxis in high-risk hospitalized patients with COVID-19: The HEP-COVID randomized clinical trial. JAMA Int. Med. 2021, 181, 1612–1620. [Google Scholar] [CrossRef]
- INSPIRATION Investigators. Effect of Intermediate-Dose vs Standard-Dose Prophylactic Anticoagulation on Thrombotic Events, Extracorporeal Membrane Oxygenation Treatment, or Mortality Among Patients With COVID-19 Admitted to the Intensive Care Unit: The INSPIRATION Randomized Clinical Trial. JAMA 2021, 325, 1620–1630. [Google Scholar]
- REMAP-CAP Investigators; ACTIV-4a Investigators; ATTACC Investigators. Therapeutic anticoagulation with heparin in critically ill patients with COVID-19. N. Engl. J. Med. 2021, 385, 777–789. [Google Scholar] [CrossRef]
- Nopp, S.; Moik, F.; Jilma, B.; Pabinger, I.; Ay, C. Risk of venous thromboembolism in patients with COVID-19: A systematic review and meta-analysis. Res. Pract. Thromb. Haemost. 2020, 4, 1178–1191. [Google Scholar] [CrossRef]
- Cohen, A.T.; Davidson, B.L.; Gallus, A.S.; Lassen, M.R.; Prins, M.H.; Tomkowski, W.; Turpie, A.G.; Egberts, J.F.; Lensing, A.W. Efficacy and safety of fondaparinux for the prevention of venous thromboembolism in older acute medical patients: Randomised placebo controlled trial. BMJ 2006, 332, 325–329. [Google Scholar] [CrossRef] [PubMed]
- Leizorovicz, A.; Cohen, A.T.; Turpie, A.G.; Olsson, C.G.; Vaitkus, P.T.; Goldhaber, S.Z. Randomized, placebo-controlled trial of dalteparin for the prevention of venous thromboembolism in acutely ill medical patients. Circulation 2004, 110, 874–879. [Google Scholar] [CrossRef]
- PROTECT Investigators for the Canadian Critical Care Trials Group; Australian and New Zealand Intensive Care Society Clinical Trials Group. Dalteparin versus unfractionated heparin in critically ill patients. N. Engl. J. Med. 2011, 364, 1305–1314. [Google Scholar] [CrossRef] [PubMed]
- Kaplan, D.; Casper, T.C.; Elliott, C.G.; Men, S.; Pendleton, R.C.; Kraiss, L.W.; Weyrich, A.S.; Grissom, C.K.; Zimmerman, G.A.; Rondina, M.T. VTE incidence and risk factors in patients with severe sepsis and septic shock. Chest 2015, 148, 1224–1230. [Google Scholar] [CrossRef]
- Chow, J.H.; Yin, Y.; Yamane, D.P.; Davison, D.; Keneally, R.J.; Hawkins, K.; Parr, K.G.; Al-Mashat, M.; Berger, J.S.; Bushardt, R.L.; et al. Association of prehospital antiplatelet therapy with survival in patients hospitalized with COVID-19: A propensity score-matched analysis. J. Thromb. Haemost. 2021, 19, 2814–2824. [Google Scholar] [CrossRef]
- Chow, J.H.; Khanna, A.K.; Kethireddy, S.; Yamane, D.; Levine, A.; Jackson, A.M.; McCurdy, M.T.; Tabatabai, A.; Kumar, G.; Park, P.; et al. Aspirin use is associated with decreased mechanical ventilation, intensive care unit admission, and in-hospital mortality in hospitalized patients with coronavirus disease 2019. Anesth. Analg. 2021, 132, 930–941. [Google Scholar] [CrossRef] [PubMed]
- Chow, J.H.; Rahnavard, A.; Gomberg-Maitland, M.; Chatterjee, R.; Patodi, P.; Yamane, D.P.; Levine, A.R.; Davison, D.; Hawkins, K.; Jackson, A.M.; et al. Association of early aspirin use with in-hospital mortality in patients with moderate COVID-19. JAMA Netw. Open 2022, 5, e223890. [Google Scholar] [CrossRef] [PubMed]
- Abdi, M.; Hosseini, Z.; Shirjan, F.; Mohammadi, L.; Abadi, S.S.; Massoudi, N.; Zangiabadian, M.; Nasiri, M.J. The effect of aspirin on the prevention of pro-thrombotic states in hospitalized COVID-19 patients: Systematic review. Cardiovasc. Hematol. Agents Med. Chem. 2022, 20, 189–196. [Google Scholar] [PubMed]
- RECOVERY Collaborative Group. Aspirin in patients admitted to hospital with COVID-19 (RECOVERY): A randomised, controlled, open-label, platform trial. Lancet 2022, 399, 143–151. [Google Scholar] [CrossRef] [PubMed]
- Berger, J.S.; Kornblith, L.Z.; Gong, M.N.; Reynolds, H.R.; Cushman, M.; Cheng, Y.; McVerry, B.J.; Kim, K.S.; Lopes, R.D.; Atassi, B.; et al. Effect of P2Y12 inhibitors on survival free of organ support among non-critically ill hospitalized patients with COVID-19: A randomized clinical trial. JAMA 2022, 327, 227–236. [Google Scholar] [CrossRef]
- Karam, B.S.; Morris, R.S.; Bramante, C.T.; Puskarich, M.; Zolfaghari, E.J.; Lotfi-Emran, S.; Ingraham, N.E.; Charles, A.; Odde, D.J.; Tignanelli, C.J. mTOR inhibition in COVID-19: A commentary and review of efficacy in RNA viruses. J. Med. Virol. 2021, 93, 1843–1846. [Google Scholar] [CrossRef] [PubMed]
- Del Campo, J.A.; García-Valdecasas, M.; Gil-Gómez, A.; Rojas, Á.; Gallego, P.; Ampuero, J.; Gallego-Durán, R.; Pastor, H.; Grande, L.; Padillo, F.J.; et al. Simvastatin and metformin inhibit cell growth in hepatitis C virus infected cells via mTOR increasing PTEN and autophagy. PLoS ONE 2018, 13, e0191805. [Google Scholar] [CrossRef]
- Postler, T.S.; Peng, V.; Bhatt, D.M.; Ghosh, S. Metformin selectively dampens the acute inflammatory response through an AMPK-dependent mechanism. Sci. Rep. 2021, 11, 18721. [Google Scholar] [CrossRef]
- Xin, G.; Wei, Z.; Ji, C.; Zheng, H.; Gu, J.; Ma, L.; Huang, W.; Morris-Natschke, S.L.; Yeh, J.L.; Zhang, R.; et al. Metformin uniquely prevents thrombosis by inhibiting platelet activation and mtDNA release. Sci. Rep. 2016, 6, 36222. [Google Scholar] [CrossRef]
- Li, Y.; Yang, X.; Yan, P.; Sun, T.; Zeng, Z.; Li, S. Metformin in patients with COVID-19: A systematic review and meta-analysis. Front. Med. 2021, 8, 704666. [Google Scholar] [CrossRef] [PubMed]
- Bramante, C.T.; Buse, J.; Tamaritz, L.; Palacio, A.; Cohen, K.; Vojta, D.; Liebovitz, D.; Mitchell, N.; Nicklas, J.; Lingvay, I.; et al. Outpatient metformin use is associated with reduced severity of COVID-19 disease in adults with overweight or obesity. J. Med. Virol. 2021, 93, 4273–4279. [Google Scholar] [CrossRef]
- Luo, P.; Qiu, L.; Liu, Y.; Liu, X.L.; Zheng, J.L.; Xue, H.Y.; Liu, W.H.; Liu, D.; Li, J. Metformin treatment was associated with decreased mortality in COVID-19 patients with diabetes in a retrospective analysis. Am. J. Trop. Med. Hyg. 2020, 103, 69–72. [Google Scholar] [CrossRef] [PubMed]
- Reis, G.; Silva, E.A.D.S.M.; Silva, D.C.M.; Thabane, L.; Milagres, A.C.; Ferreira, T.S.; Dos Santos, C.V.; de Figueiredo Neto, A.D.; Callegari, E.D.; Savassi, L.C.; et al. Effect of early treatment with metformin on risk of emergency care and hospitalization among patients with COVID-19: The TOGETHER randomized platform clinical trial. Lancet Reg. Health–Am. 2022, 6, 100142. [Google Scholar] [CrossRef] [PubMed]
- Thomas, S.; Patel, D.; Bittel, B.; Wolski, K.; Wang, Q.; Kumar, A.; Il’Giovine, Z.J.; Mehra, R.; McWilliams, C.; Nissen, S.E.; et al. Effect of high-dose zinc and ascorbic acid supplementation vs usual care on symptom length and reduction among ambulatory patients with SARS-CoV-2 infection: The COVID A to Z randomized clinical trial. JAMA Netw. Open 2021, 4, e210369. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.; Mei, K.; Xie, L.; Yuan, P.; Ma, J.; Yu, P.; Zhu, W.; Zheng, C.; Liu, X. Low vitamin D levels do not aggravate COVID-19 risk or death, and vitamin D supplementation does not improve outcomes in hospitalized patients with COVID-19: A meta-analysis and GRADE assessment of cohort studies and RCTs. Nutr. J. 2021, 20, 89. [Google Scholar] [CrossRef]
- National Institutes of Health (NIH). COVID-19 Treatment Guidelines 3 Office of Dietary Supplements, National Institutes of Health. In Zinc Fact Sheet for Health Professionals; National Institutes of Health (NIH): Bethesda, MD, USA, 2022. [Google Scholar]
- Moscatelli, F.; Sessa, F.; Valenzano, A.; Polito, R.; Monda, V.; Cibelli, G.; Villano, I.; Pisanelli, D.; Perrella, M.; Daniele, A.; et al. COVID-19: Role of nutrition and supplementation. Nutrients 2021, 13, 976. [Google Scholar] [CrossRef]
- Zhang, J.; Rao, X.; Li, Y.; Zhu, Y.; Liu, F.; Guo, G.; Luo, G.; Meng, Z.; De Backer, D.; Xiang, H.; et al. Pilot trial of high-dose vitamin C in critically ill COVID-19 patients. Ann. Intensive Care 2021, 11, 5. [Google Scholar] [CrossRef]
- Najjar-Debbiny, R.; Gronich, N.; Weber, G.; Khoury, J.; Amar, M.; Stein, N.; Goldstein, L.H.; Saliba, W. Effectiveness of Paxlovid in reducing severe coronavirus 2019 and mortality in high-risk patients. Clin. Infect. Dis. 2023, 76, 342–349. [Google Scholar] [CrossRef]
- Najjar-Debbiny, R.; Gronich, N.; Weber, G.; Khoury, J.; Amar, M.; Stein, N.; Goldstein, L.H.; Saliba, W. Efectiveness of molnupiravir in high-risk patients: A propensity score matched analysis. Clin. Infect. Dis. 2023, 76, 453–460. [Google Scholar] [CrossRef]
- Long, B.; Chavez, S.; Carius, B.M.; Brady, W.J.; Liang, S.Y.; Koyfman, A.; Gottlieb, M. Clinical update on COVID-19 for the emergency and critical care clinician: Medical management. Am. J. Emerg. Med. 2022, 56, 158–170. [Google Scholar] [CrossRef]
- Moores, L.K.; Tritschler, T.; Brosnahan, S.; Carrier, M.; Collen, J.F.; Doerschug, K.; Holley, A.B.; Jimenez, D.; Le Gal, G.; Rali, P.; et al. Prevention, Diagnosis, and Treatment of VTE in Patients with Coronavirus Disease 2019: CHEST Guideline and Expert Panel Report. Chest 2020, 158, 1143–1163. [Google Scholar] [CrossRef]
- Thachil, J.; Juffermans, N.P.; Ranucci, M.; Connors, J.M.; Warkentin, T.E.; Ortel, T.L.; Levi, M.; Iba, T.; Levy, J.H. ISTH DIC subcommittee communication on anticoagulation in COVID-19. J. Thromb. Haemost. 2020, 18, 2138–2144. [Google Scholar] [CrossRef] [PubMed]
- Thachil, J.; Tang, N.; Gando, S.; Falanga, A.; Cattaneo, M.; Levi, M.; Clark, C.; Iba, T. ISTH interim guidance on recognition and management of coagulopathy in COVID-19. J. Thromb. Haemost. 2020, 18, 1023–1026. [Google Scholar] [CrossRef] [PubMed]
- Arbănași, E.M.; Kaller, R.; Mureșan, V.A.; Voidăzan, S.; Arbănași, E.M.; Russu, E. Impact of COVID-19 Pandemic on Vascular Surgery Unit Activity in Central Romania. Front. Surg. 2022, 9, 883935. [Google Scholar]
- Arbănași, E.M.; Halmaciu, I.; Kaller, R.; Mureșan, V.A.; Arbănași, E.M.; Suciu, B.A.; Coșarcă, C.M.; Cojocaru, I.I.; Melinte, R.M.; Russu, E. Systemic Inflammatory Biomarkers and Chest CT Findings as Predictors of Acute Limb Ischemia Risk, Intensive Care Unit Admission, and Mortality in COVID-19 Patients. Diagnostics 2022, 12, 2379. [Google Scholar] [CrossRef] [PubMed]
- Casciato, D.J.; Yancovitz, S.; Thompson, J.; Anderson, S.; Bischoff, A.; Ayres, S.; Barron, I. Diabetes-related major and minor amputation risk increased during the Covid-19 pandemic. J. Am. Podiatr. Med. Assoc. 2020, 113, 202–224. [Google Scholar] [CrossRef]
- Goldman, I.A.; Ye, K.; Scheinfeld, M.H. Lower extremity arterial thrombosis associated with COVID-19 is characterized by greater thrombus burden and increased rate of amputation and death. Radiology 2020, 297, E263–E269. [Google Scholar] [CrossRef]
- Nana, P.; Dakis, K.; Spanos, K.; Tsolaki, V.; Karavidas, N.; Zakynthinos, G.; Kouvelos, G.; Giannoukas, A.; Matsagkas, M. COVID-19 related peripheral arterial thrombotic events in intensive care unit and non-intensive care unit patients: A retrospective case series. Vascular 2022, 17085381221140159. [Google Scholar] [CrossRef]
- Abd El-Lateef, A.E.; Alghamdi, S.; Ebid, G.; Khalil, K.; Kabrah, S.; Abdel Ghafar, M.T. Coagulation profile in COVID-19 patients and its relation to disease severity and overall survival: A single-center study. Br. J. Biomed. Sci. 2022, 79, 10098. [Google Scholar] [CrossRef]
- Rastogi, A.; Dogra, H.; Jude, E.B. Covid-19 and peripheral arterial complications in people with diabetes and hypertension: A systemic review. Diabetes Metab. Syndr. Clin. Res. Rev. 2021, 15, 102204. [Google Scholar] [CrossRef]
- Paparella, R.; Tarani, L.; Properzi, E.; Costantino, F.; Saburri, C.; Lucibello, R.; Richetta, A.; Spalice, A.; Leonardi, L. Chilblain-like lesions onset during SARS-CoV-2 infection in a COVID-19-vaccinated adolescent: Case report and review of literature. Ital. J. Pediatr. 2022, 48, 93. [Google Scholar] [CrossRef]
- Stoian, A.; Bajko, Z.; Stoian, M.; Cioflinc, R.A.; Niculescu, R.; Arbănași, E.M.; Russu, E.; Botoncea, M.; Bălașa, R. The Occurrence of Acute Disseminated Encephalomyelitis in SARS-CoV-2 Infection/Vaccination: Our Experience and a Systematic Review of the Literature. Vaccines 2023, 11, 1225. [Google Scholar] [CrossRef] [PubMed]
- Anar, M.A.; Foroughi, E.; Sohrabi, E.; Peiravi, S.; Tavakoli, Y.; Khouzani, M.K.; Behshood, P.; Shamshiri, M.; Faridzadeh, A.; Keylani, K.; et al. Selective serotonin reuptake inhibitors: New hope in the fight against COVID-19. Front. Pharmacol. 2022, 13, 1036093. [Google Scholar] [CrossRef] [PubMed]
| Test | Reagents Used | Assessed Mechanism | Diagnosis |
|---|---|---|---|
| EX-test | Tissue factor (TF), CaCl2, polybrene (to inactivate heparin therapy) | Potential and dynamics of clot formation during tissue damage | Factor deficiencies of extrinsic pathway |
| IN-test | phospholipid, ellagic acid, CaCl2 | Potential and dynamics of clot formation during foreign-body contact | Intrinsic pathway factor deficiencies |
| FIB-test | TF, Ca2+, polybrene, cytochalasin D, GPIIb-IIIa inhibitor | Potential and dynamics of secondary clot formation during tissue damage | Fibrinogen deficiency, factor deficiencies of extrinsic pathway |
| HI-test | lyophilized heparinase, phospholipid, ellagic acid, CaCl2 | Intrinsic pathway deficiency | Presence of heparin compared to IN-test |
| tPA-test | TF, CaCl2, polybrene, recombinant tissue plasminogen activator (rtPA) | Potential and dynamics of extrinsic coagulation and fibrinolysis | Diagnosis of pathologic fibrinolysis |
| AP-test | TF, CaCl2, polybrene, aprotinin | Extrinsic and common pathway activation and fibrinolysis inhibition | Hyperfibrinolytic bleeding |
| RVV-test | Russell’s viper venom, CaCl2 | Factor X activation, common pathway activation, potential and dynamics of clot formation | Direct-acting oral anticoagulant effect |
| ECA-test | Saw-scaled viper venom (ecarin) | Prothrombin–thrombin activation, dynamics of clot formation | Direct acting oral anticoagulant effect and antithrombin activity |
| Obese Patients | Diabetic Patients | Patients with Cardiovascular Diseases |
|---|---|---|
| Patient information about COVID-19 symptoms and algorithms to follow in case of symptom progression—telemedicine | ||
| Prevention of infection/reinfection through vaccination; recommendation of wearing a facial mask in crowds, especially during the outbreaks of newer variants | ||
| Monitoring blood pressure and heart rate, with consecutive therapy initiation/modification according to the findings | Monitoring blood pressure and heart rate with consecutive therapy initiation/modification according to the findings and, additionally, dynamic monitoring of carbohydrate balance (blood glucose, HbA1c, C peptide) and, eventually, acid–base balance | Monitoring blood pressure and heart rate, with consecutive therapy modification according to the findings |
| Diagnosis and therapy of further comorbidities; cardiometabolic risk reduction | ||
| Ensure the availability of hospitalization and eventual intensive care for an unfavorable course of COVID-19 | ||
| Weight-loss strategy modification/initiation including diet and physical activity | Considering treatment administration for diabetes mellitus, depending on the type of DM and the severity of COVID-19 symptoms | Treatment of hypertension and/or heart failure focusing on thromboprophylaxis and secondary prevention of complications in the context of COVID-19 |
| Outpatient care after discharge specifically considering the comorbidities of each patient; ideally, an individualized care would be recommended | ||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Szilveszter, M.; Pál, S.; Simon-Szabó, Z.; Akácsos-Szász, O.-Z.; Moldován, M.; Réger, B.; Dénes, L.; Faust, Z.; Tilinca, M.C.; Nemes-Nagy, E. The Management of COVID-19-Related Coagulopathy: A Focus on the Challenges of Metabolic and Vascular Diseases. Int. J. Mol. Sci. 2023, 24, 12782. https://doi.org/10.3390/ijms241612782
Szilveszter M, Pál S, Simon-Szabó Z, Akácsos-Szász O-Z, Moldován M, Réger B, Dénes L, Faust Z, Tilinca MC, Nemes-Nagy E. The Management of COVID-19-Related Coagulopathy: A Focus on the Challenges of Metabolic and Vascular Diseases. International Journal of Molecular Sciences. 2023; 24(16):12782. https://doi.org/10.3390/ijms241612782
Chicago/Turabian StyleSzilveszter, Mónika, Sándor Pál, Zsuzsánna Simon-Szabó, Orsolya-Zsuzsa Akácsos-Szász, Mihály Moldován, Barbara Réger, Lóránd Dénes, Zsuzsanna Faust, Mariana Cornelia Tilinca, and Enikő Nemes-Nagy. 2023. "The Management of COVID-19-Related Coagulopathy: A Focus on the Challenges of Metabolic and Vascular Diseases" International Journal of Molecular Sciences 24, no. 16: 12782. https://doi.org/10.3390/ijms241612782
APA StyleSzilveszter, M., Pál, S., Simon-Szabó, Z., Akácsos-Szász, O.-Z., Moldován, M., Réger, B., Dénes, L., Faust, Z., Tilinca, M. C., & Nemes-Nagy, E. (2023). The Management of COVID-19-Related Coagulopathy: A Focus on the Challenges of Metabolic and Vascular Diseases. International Journal of Molecular Sciences, 24(16), 12782. https://doi.org/10.3390/ijms241612782





