miR-1183 Is a Key Marker of Remodeling upon Stretch and Tachycardia in Human Myocardium
Abstract
1. Introduction
2. Results
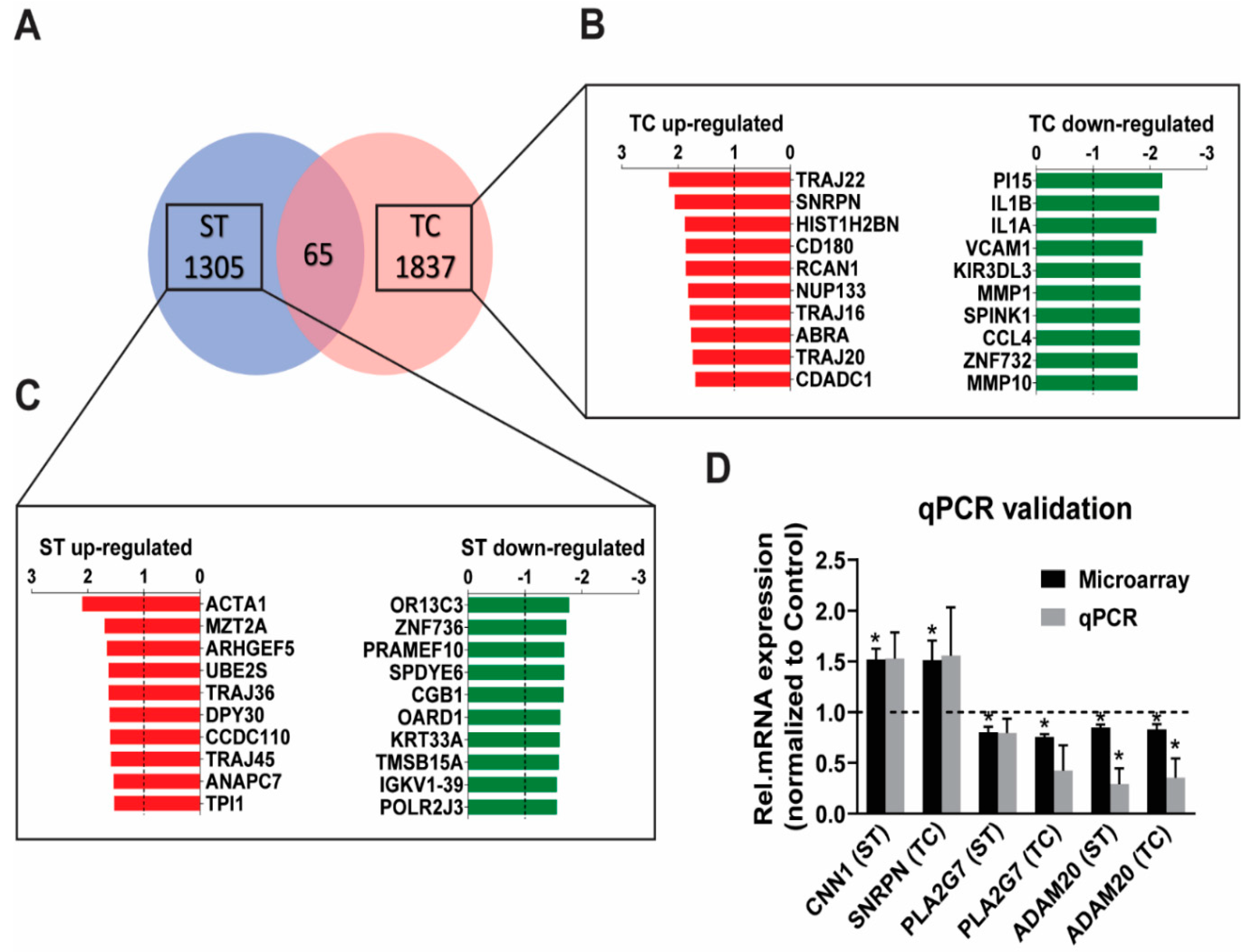
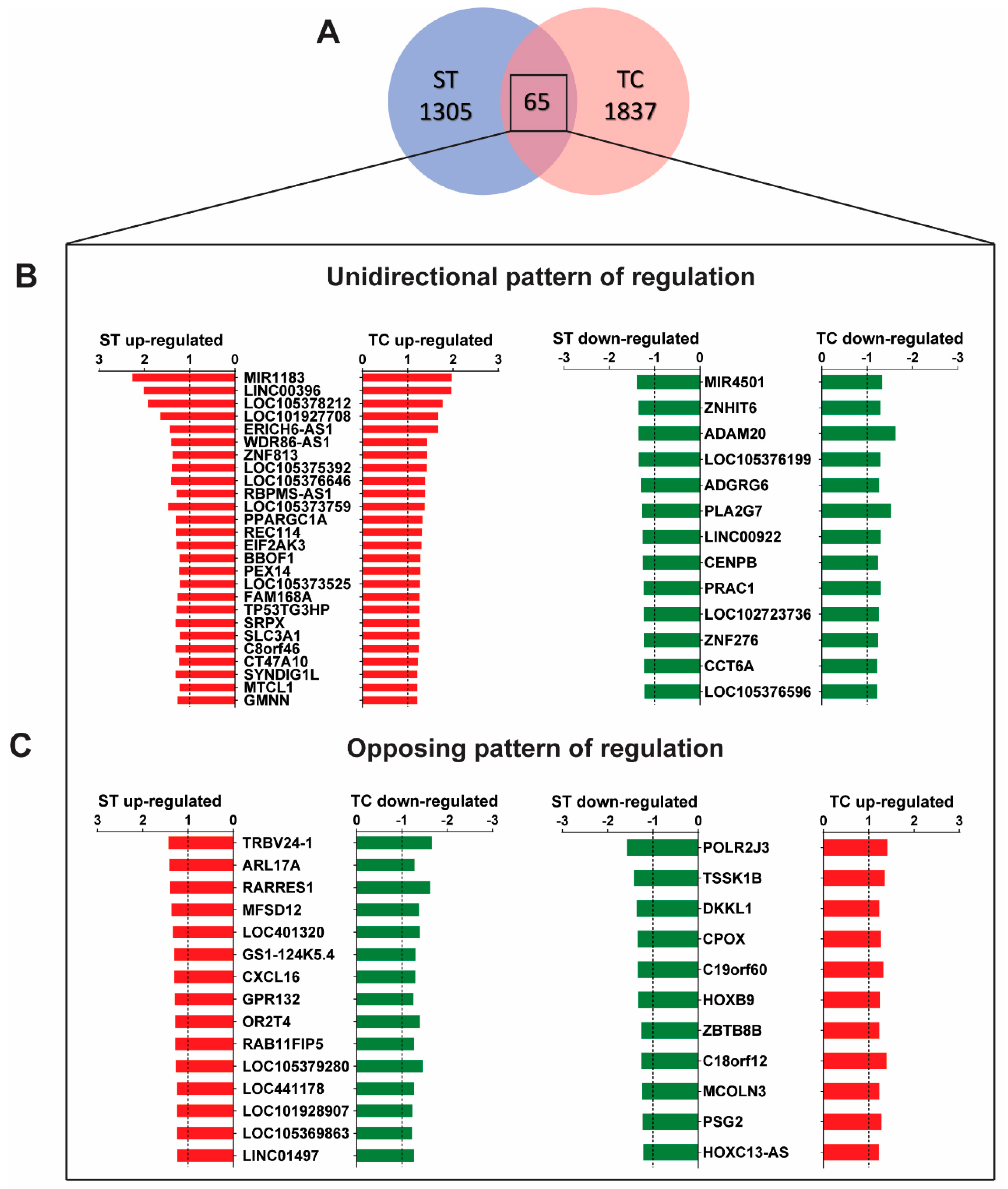
2.1. Stretch and Tachycardia Induced Differential and Common Patterns of Gene Expression
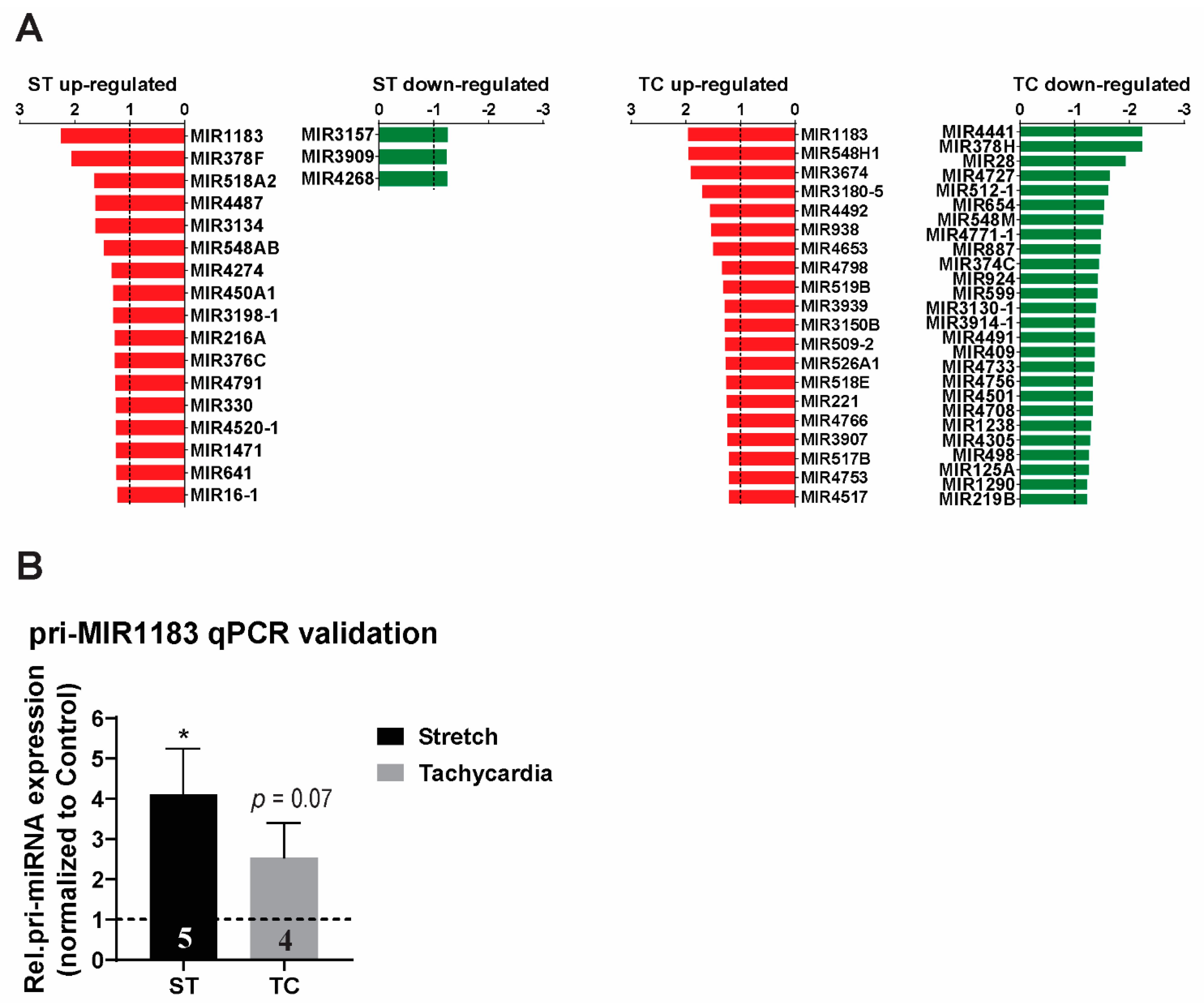
2.2. MicroRNA Expression Profile and Detection of miR-1183 Encoding Gene as the Strongest and Commonly Regulated Transcript
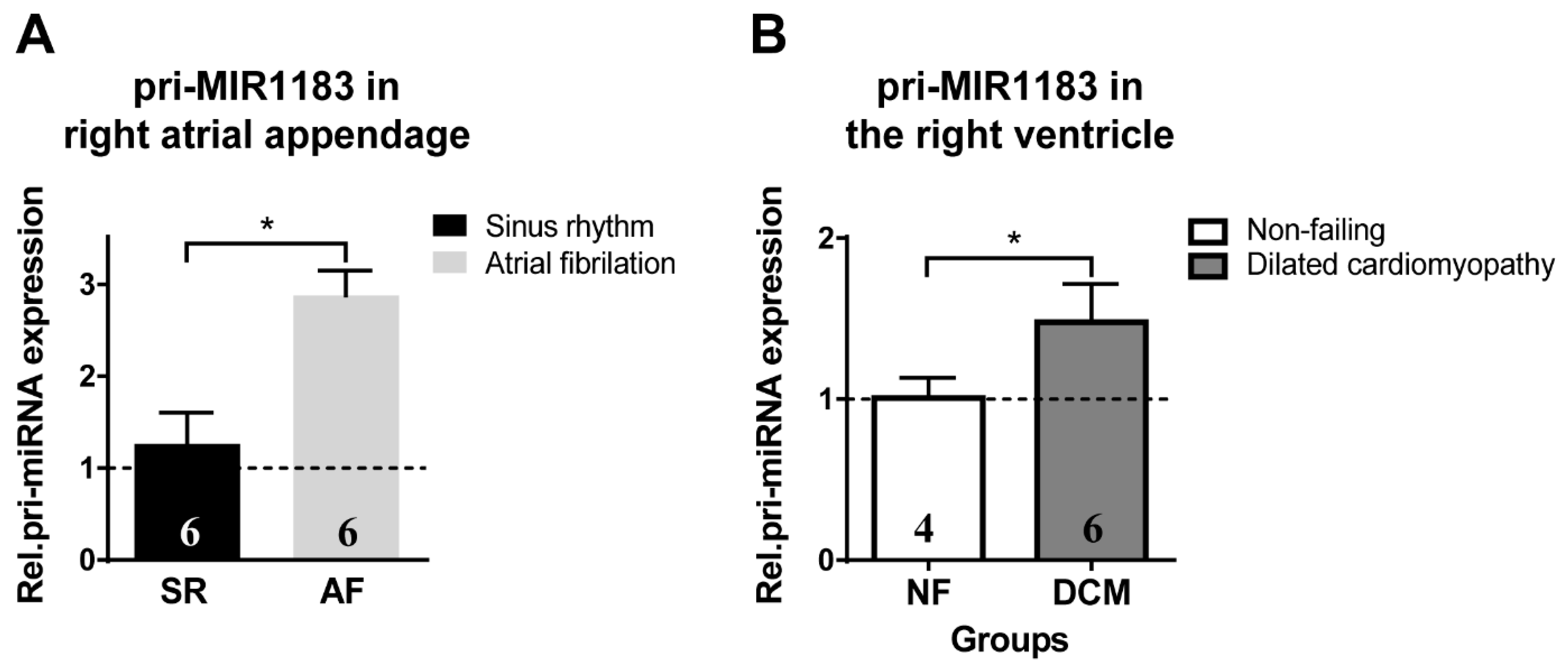
2.3. miR-1183 as a Biomarker in Human Cardiac Tissue
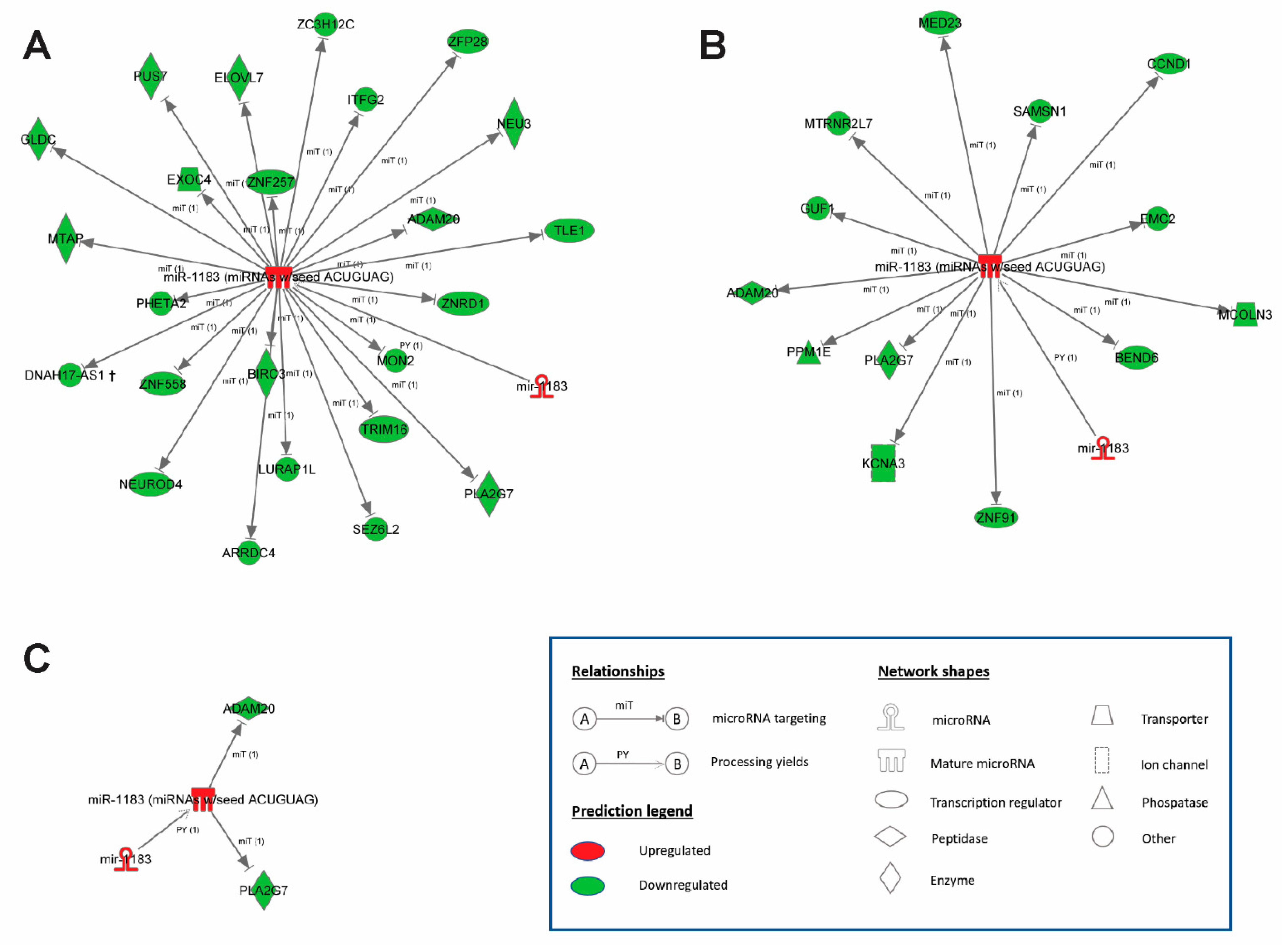
2.4. Bioinformatics Prediction of miR-1183 Downstream Targets
3. Discussion
3.1. Microarray Gene Expression Uncovers Independent Stretch and Tachycardia Gene Regulation
3.2. MicroRNA Regulation in Stretch Versus Tachycardia Induced Remodeling
3.3. miR-1183 as a Novel Marker in Atrial and Ventricular Remodeling
3.4. Upstream Regulators of miR-1183
3.5. Downstream Targets of miR-1183 and Cardiac Functional Effects
4. Material and Methods
4.1. Preparation, Processing, and Stretch and Tachycardia Induction in Human Myocardium
4.2. RNA Isolation
4.3. Microarray Hybridization
4.4. Quantitative Real-Time PCR (qPCR)
4.5. Statistical Analyses
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Corradi, D.; Callegari, S.; Maestri, R.; Benussi, S.; Alfieri, O. Structural remodeling in atrial fibrillation. Nat. Clin. Pract. Cardiovasc. Med. 2008, 5, 782–796. [Google Scholar] [CrossRef] [PubMed]
- Greiser, M.; Lederer, W.J.; Schotten, U. Alterations of atrial Ca2+ handling as cause and consequence of atrial fibrillation. Cardiovasc. Res. 2011, 89, 722–733. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Ma, J.; Chen, Q.; Ma, S. Left atrial fibrosis in atrial fibrillation: Mechanisms, clinical evaluation and management. J. Cell Mol. Med. 2021, 25, 2764–2775. [Google Scholar] [CrossRef]
- Al Ghamdi, B.; Hassan, W. Atrial Remodeling And Atrial Fibrillation: Mechanistic Interactions And Clinical Implications. J. Atr. Fibrillation 2009, 2, 125. [Google Scholar] [PubMed]
- Nattel, S.; Shiroshita-Takeshita, A.; Cardin, S.; Pelletier, P. Mechanisms of atrial remodeling and clinical relevance. Curr. Opin. Cardiol. 2005, 20, 21–25. [Google Scholar] [PubMed]
- Agarwal, V.; Bell, G.W.; Nam, J.W.; Bartel, D.P. Predicting effective microRNA target sites in mammalian mRNAs. eLife 2015, 4, e05005. [Google Scholar] [CrossRef]
- Suzuki, R.; Morishima, M.; Nakada, C.; Miyamoto, S.; Ono, K. Manifestations of gene expression profiles in human right atrial myocardium caused by mechanical stretch. Heart Vessel. 2021, 36, 577–588. [Google Scholar] [CrossRef]
- Joureau, B.; de Winter, J.M.; Conijn, S.; Bogaards, S.J.P.; Kovacevic, I.; Kalganov, A.; Persson, M.; Lindqvist, J.; Stienen, G.J.M.; Irving, T.C.; et al. Dysfunctional sarcomere contractility contributes to muscle weakness in ACTA1-related nemaline myopathy (NEM3). Ann. Neurol. 2018, 83, 269–282. [Google Scholar] [CrossRef]
- Clarkson, E.; Costa, C.F.; Machesky, L.M. Congenital myopathies: Diseases of the actin cytoskeleton. J. Pathol. 2004, 204, 407–417. [Google Scholar] [CrossRef]
- Gerçek, M.; Gerçek, M.; Kant, S.; Simsekyilmaz, S.; Kassner, A.; Milting, H.; Liehn, E.A.; Leube, R.E.; Krusche, C.A. Cardiomyocyte Hypertrophy in Arrhythmogenic Cardiomyopathy. Am. J. Pathol. 2017, 187, 752–766. [Google Scholar] [CrossRef][Green Version]
- Karakikes, I.; Chaanine, A.H.; Kang, S.; Mukete, B.N.; Jeong, D.; Zhang, S.; Hajjar, R.J.; Lebeche, D. Therapeutic cardiac-targeted delivery of miR-1 reverses pressure overload-induced cardiac hypertrophy and attenuates pathological remodeling. J. Am. Heart Assoc. 2013, 2, e000078. [Google Scholar] [CrossRef] [PubMed]
- Kee, H.J.; Bae, E.H.; Park, S.; Lee, K.E.; Suh, S.H.; Kim, S.W.; Jeong, M.H. HDAC Inhibition Suppresses Cardiac Hypertrophy and Fibrosis in DOCA-Salt Hypertensive Rats via Regulation of HDAC6/HDAC8 Enzyme Activity. Kidney Blood Press. Res. 2013, 37, 229–239. [Google Scholar] [CrossRef] [PubMed]
- Schaefer, A.; Schneeberger, Y.; Schulz, S.; Krasemann, S.; Werner, T.; Piasecki, A.; Höppner, G.; Müller, C.; Morhenn, K.; Lorenz, K.; et al. Analysis of fibrosis in control or pressure overloaded rat hearts after mechanical unloading by heterotopic heart transplantation. Sci. Rep. 2019, 9, 5710. [Google Scholar] [CrossRef] [PubMed]
- Wu, C.; Dong, S.; Li, Y. Effects of miRNA-455 on cardiac hypertrophy induced by pressure overload. Int. J. Mol. Med. 2015, 35, 893–900. [Google Scholar] [CrossRef]
- Kant, S.; Freytag, B.; Herzog, A.; Reich, A.; Merkel, R.; Hoffmann, B.; Krusche, C.A.; Leube, R.E. Desmoglein 2 mutation provokes skeletal muscle actin expression and accumulation at intercalated discs in murine hearts. J. Cell Sci. 2019, 132, jcs199612. [Google Scholar] [CrossRef]
- Olson, T.M.; Michels, V.V.; Thibodeau, S.N.; Tai, Y.S.; Keating, M.T. Actin mutations in dilated cardiomyopathy, a heritable form of heart failure. Science 1998, 280, 750–752. [Google Scholar] [CrossRef]
- Kluge, A.; Rangrez, A.Y.; Kilian, L.S.; Pott, J.; Bernt, A.; Frauen, R.; Rohrbeck, A.; Frey, N.; Frank, D. Rho-family GTPase 1 (Rnd1) is a biomechanical stress-sensitive activator of cardiomyocyte hypertrophy. J. Mol. Cell. Cardiol. 2019, 129, 130–143. [Google Scholar] [CrossRef]
- Rysä, J.; Tokola, H.; Ruskoaho, H. Mechanical stretch induced transcriptomic profiles in cardiac myocytes. Sci. Rep. 2018, 8, 4733. [Google Scholar] [CrossRef]
- Bardosi, A.; Eber, S.W.; Hendrys, M.; Pekrun, A. Myopathy with altered mitochondria due to a triosephosphate isomerase (TPI) deficiency. Acta Neuropathol. 1990, 79, 387–394. [Google Scholar] [CrossRef]
- Smith, L.E.; Hambly, B.; Cordwell, S.; White, M. Abstract 20301: Reversible Oxidation Of Metabolic Protein Triosephosphate Isomerase in the Type 2 Diabetic Heart. Circulation 2016, 134, A20301. [Google Scholar]
- Ramsden, S.C.; Clayton-Smith, J.; Birch, R.; Buiting, K. Practice guidelines for the molecular analysis of Prader-Willi and Angelman syndromes. BMC Med. Genet. 2010, 11, 70. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.J.; Brune, C.W.; Kistner, E.O.; Christian, S.L.; Courchesne, E.H.; Cox, N.J.; Cook, E.H. Transmission disequilibrium testing of the chromosome 15q11-q13 region in autism. Am. J. Med. Genet. B Neuropsychiatr. Genet. 2008, 147, 1116–1125. [Google Scholar] [CrossRef] [PubMed]
- Wilk, J.B.; Walter, R.E.; Laramie, J.M.; Gottlieb, D.J.; O’Connor, G.T. Framingham Heart Study genome-wide association: Results for pulmonary function measures. BMC Med. Genet. 2007, 8, S8. [Google Scholar] [CrossRef] [PubMed]
- Davies, K.J.A.; Ermak, G.; Rothermel, B.A.; Pritchard, M.; Heitman, J.; Ahnn, J.; Henrique-Silva, F.; Crawford, D.; Canaider, S.; Strippoli, P.; et al. Renaming the DSCR1/Adapt78 gene family as RCAN: Regulators of calcineurin. FASEB J. 2007, 21, 3023–3028. [Google Scholar] [CrossRef]
- Shin, S.-Y.; Yang, J.M.; Choo, S.-M.; Kwon, K.-S.; Cho, K.-H. System-level investigation into the regulatory mechanism of the calcineurin/NFAT signaling pathway. Cell. Signal. 2008, 20, 1117–1124. [Google Scholar] [CrossRef]
- Vega, R.B.; Rothermel, B.A.; Weinheimer, C.J.; Kovacs, A.; Naseem, R.H.; Bassel-Duby, R.; Williams, R.S.; Olson, E.N. Dual roles of modulatory calcineurin-interacting protein 1 in cardiac hypertrophy. Proc. Natl. Acad. Sci. USA 2003, 100, 669–674. [Google Scholar] [CrossRef]
- Turpin, C.; Waikel, R. The role of myocyte-enriched calcineurin-inhibiting protein (MCIP1) in estrogen mediated repression of cardiac hypertrophy (795.5). FASEB J. 2014, 28, 795.5. [Google Scholar] [CrossRef]
- Sobrado, M.; Ramirez, B.G.; Neria, F.; Lizasoain, I.; Arbones, M.L.; Minami, T.; Redondo, J.M.; Moro, M.A.; Cano, E. Regulator of calcineurin 1 (Rcan1) has a protective role in brain ischemia/reperfusion injury. J. Neuroinflamm. 2012, 9, 48. [Google Scholar] [CrossRef]
- Bartoszewski, R.; Gebert, M.; Janaszak-Jasiecka, A.; Cabaj, A.; Króliczewski, J.; Bartoszewska, S.; Sobolewska, A.; Crossman, D.K.; Ochocka, R.; Kamysz, W.; et al. Genome-wide mRNA profiling identifies RCAN1 and GADD45A as regulators of the transitional switch from survival to apoptosis during ER stress. FEBS J. 2020, 287, 2923–2947. [Google Scholar] [CrossRef]
- Kuwahara, K.; Wang, Y.; McAnally, J.; Richardson, J.A.; Bassel-Duby, R.; Hill, J.A.; Olson, E.N. TRPC6 fulfills a calcineurin signaling circuit during pathologic cardiac remodeling. J. Clin. Investig. 2006, 116, 3114–3126. [Google Scholar] [CrossRef]
- Wang, X.; Feuerstein, G.Z.; Gu, J.-L.; Lysko, P.G.; Yue, T.-L. Interleukin-1β induces expression of adhesion molecules in human vascular smooth muscle cells and enhances adhesion of leukocytes to smooth muscle cells. Atherosclerosis 1995, 115, 89–98. [Google Scholar] [CrossRef]
- Ganesan, J.; Ramanujam, D.; Sassi, Y.; Ahles, A.; Jentzsch, C.; Werfel, S.; Leierseder, S.; Loyer, X.; Giacca, M.; Zentilin, L.; et al. MiR-378 controls cardiac hypertrophy by combined repression of mitogen-activated protein kinase pathway factors. Circulation 2013, 127, 2097–2106. [Google Scholar] [CrossRef] [PubMed]
- Yang, S.; Mi, X.; Chen, Y.; Feng, C.; Hou, Z.; Hui, R.; Zhang, W. MicroRNA-216a induces endothelial senescence and inflammation via Smad3/IkappaBalpha pathway. J. Cell Mol. Med. 2018, 22, 2739–2749. [Google Scholar] [CrossRef] [PubMed]
- Tao, J.; Wang, J.; Li, C.; Wang, W.; Yu, H.; Liu, J.; Kong, X.; Chen, Y. MiR-216a accelerates proliferation and fibrogenesis via targeting PTEN and SMAD7 in human cardiac fibroblasts. Cardiovasc. Diagn. Ther. 2019, 9, 535–544. [Google Scholar] [CrossRef] [PubMed]
- Ding, H.; Wang, Y.; Hu, L.; Xue, S.; Wang, Y.; Zhang, L.; Zhang, Y.; Qi, H.; Yu, H.; Aung, L.H.H.; et al. Combined detection of miR-21-5p, miR-30a-3p, miR-30a-5p, miR-155-5p, miR-216a and miR-217 for screening of early heart failure diseases. Biosci. Rep. 2020, 40, BSR20191653. [Google Scholar] [CrossRef]
- Greco, S.; Fasanaro, P.; Castelvecchio, S.; D’Alessandra, Y.; Arcelli, D.; Di Donato, M.; Malavazos, A.; Capogrossi, M.C.; Menicanti, L.; Martelli, F. MicroRNA dysregulation in diabetic ischemic heart failure patients. Diabetes 2012, 61, 1633–1641. [Google Scholar] [CrossRef]
- Ma, G.; Bi, S.; Zhang, P. Long non-coding RNA MIAT regulates ox-LDL-induced cell proliferation, migration and invasion by miR-641/STIM1 axis in human vascular smooth muscle cells. BMC Cardiovasc. Disord. 2021, 21, 248. [Google Scholar] [CrossRef]
- Sandhu, H.; Cooper, S.; Hussain, A.; Mee, C.; Maddock, H. Attenuation of Sunitinib-induced cardiotoxicity through the A3 adenosine receptor activation. Eur. J. Pharmacol. 2017, 814, 95–105. [Google Scholar] [CrossRef]
- Yang, H.L.; Zhang, H.Z.; Meng, F.R.; Han, S.Y.; Zhang, M. Differential expression of microRNA-411 and 376c is associated with hypertension in pregnancy. Braz. J. Med. Biol. Res. 2019, 52, e7546. [Google Scholar] [CrossRef]
- Santos-Faria, J.; Gavina, C.; Rodrigues, P.; Coelho, J.; da Costa Martins, P.; Leite-Moreira, A.; Falcao-Pires, I. MicroRNAs and ventricular remodeling in aortic stenosis. Rev. Port. Cardiol. 2020, 39, 377–387. [Google Scholar] [CrossRef]
- Li, F.; Sun, J.Y.; Wu, L.D.; Qu, Q.; Zhang, Z.Y.; Chen, X.F.; Kan, J.Y.; Wang, C.; Wang, R.X. Predictive Biomarkers for Postmyocardial Infarction Heart Failure Using Machine Learning: A Secondary Analysis of a Cohort Study. Evid. Based Complementary Altern. Med. 2021, 2021, 2903543. [Google Scholar] [CrossRef] [PubMed]
- Hou, J.; Wang, J.; Lin, C.; Fu, J.; Ren, J.; Li, L.; Guo, H.; Han, X.; Liu, J. Circulating MicroRNA Profiles Differ between Qi-Stagnation and Qi-Deficiency in Coronary Heart Disease Patients with Blood Stasis Syndrome. Evid Based Complementary Altern. Med. 2014, 2014, 926962. [Google Scholar] [CrossRef] [PubMed]
- Sanna, G.D.; Gabrielli, E.; De Vito, E.; Nusdeo, G.; Prisco, D.; Parodi, G. Atrial fibrillation in athletes: From epidemiology to treatment in the novel oral anticoagulants era. J. Cardiol. 2018, 72, 269–276. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.G.; Meng, X.; Han, J.; Li, Y.; Luo, T.G.; Wang, J.; Xin, M.; Xi, J.Z. [Differential expressions of miRNAs in patients with nonvalvular atrial fibrillation]. Zhonghua Yi Xue Za Zhi 2012, 92, 1816–1819. [Google Scholar] [PubMed]
- Qiang, L.; Hong, L.; Ningfu, W.; Huaihong, C.; Jing, W. Expression of miR-126 and miR-508-5p in endothelial progenitor cells is associated with the prognosis of chronic heart failure patients. Int. J. Cardiol. 2013, 168, 2082–2088. [Google Scholar] [CrossRef]
- Fan, X.; Zhan, E.; Yao, Y.; Zhang, R.; Sun, Y.; Tian, X. MiR-599 Protects Cardiomyocytes against Oxidative Stress-Induced Pyroptosis. BioMed Res. Int. 2021, 2021, 3287053. [Google Scholar] [CrossRef]
- Chai, Q.; Zheng, M.; Wang, L.; Wei, M.; Yin, Y.; Ma, F.; Li, X.; Zhang, H.; Liu, G. Circ_0068655 Promotes Cardiomyocyte Apoptosis via miR-498/PAWR Axis. Tissue Eng. Regen. Med. 2020, 17, 659–670. [Google Scholar] [CrossRef]
- Zhu, R.Y.; Zhang, D.; Zou, H.D.; Zuo, X.S.; Zhou, Q.S.; Huang, H. MiR-28 inhibits cardiomyocyte survival through suppressing PDK1/Akt/mTOR signaling. In Vitro Cell Dev. Biol. Anim. 2016, 52, 1020–1025. [Google Scholar] [CrossRef]
- Li, S.P.; Liu, B.; Song, B.; Wang, C.X.; Zhou, Y.C. miR-28 promotes cardiac ischemia by targeting mitochondrial aldehyde dehydrogenase 2 (ALDH2) in mus musculus cardiac myocytes. Eur. Rev. Med. Pharmacol. Sci. 2015, 19, 752–758. [Google Scholar]
- Yang, L.; Liang, H.; Shen, L.; Guan, Z.; Meng, X. LncRNA Tug1 involves in the pulmonary vascular remodeling in mice with hypoxic pulmonary hypertension via the microRNA-374c-mediated Foxc1. Life Sci. 2019, 237, 116769. [Google Scholar] [CrossRef]
- Wang, Y.; Tan, J.; Wang, L.; Pei, G.; Cheng, H.; Zhang, Q.; Wang, S.; He, C.; Fu, C.; Wei, Q. MiR-125 Family in Cardiovascular and Cerebrovascular Diseases. Front. Cell Dev. Biol. 2021, 9, 799049. [Google Scholar] [CrossRef] [PubMed]
- Li, N.; Lian, J.; Zhao, S.; Zheng, D.; Yang, X.; Huang, X.; Shi, X.; Sun, L.; Zhou, Q.; Shi, H.; et al. Detection of Differentially Expressed MicroRNAs in Rheumatic Heart Disease: MiR-1183 and miR-1299 as Potential Diagnostic Biomarkers. BioMed Res. Int. 2015, 2015, 524519. [Google Scholar] [CrossRef] [PubMed]
- Ye, Y.; Yang, J.; Lv, W.; Lu, Y.; Zhang, L.; Zhang, Y.; Musha, Z.; Fan, P.; Yang, B.; Zhou, X.; et al. Screening of differentially expressed microRNAs of essential hypertension in Uyghur population. Lipids Health Dis. 2019, 18, 98. [Google Scholar] [CrossRef]
- Slagsvold, K.H.; Johnsen, A.B.; Rognmo, O.; Hoydal, M.; Wisloff, U.; Wahba, A. Comparison of left versus right atrial myocardium in patients with sinus rhythm or atrial fibrillation-an assessment of mitochondrial function and microRNA expression. Physiol. Rep. 2014, 2, e12124. [Google Scholar] [CrossRef]
- Zayas-Arrabal, J.; Alquiza, A.; Rodriguez-de-Yurre, A.; Echeazarra, L.; Fernandez-Lopez, V.; Gallego, M.; Casis, O. Kv1.3 Channel Blockade Improves Inflammatory Profile, Reduces Cardiac Electrical Remodeling, and Prevents Arrhythmia in Type 2 Diabetic Rats. Cardiovasc. Drugs Ther. 2021. [Google Scholar] [CrossRef]
- Napoli, C.; Schiano, C.; Soricelli, A. Increasing evidence of pathogenic role of the Mediator (MED) complex in the development of cardiovascular diseases. Biochimie 2019, 165, 1–8. [Google Scholar] [CrossRef]
- Ward-Caviness, C.K.; Neas, L.M.; Blach, C.; Haynes, C.S.; LaRocque-Abramson, K.; Grass, E.; Dowdy, Z.E.; Devlin, R.B.; Diaz-Sanchez, D.; Cascio, W.E.; et al. A genome-wide trans-ethnic interaction study links the PIGR-FCAMR locus to coronary atherosclerosis via interactions between genetic variants and residential exposure to traffic. PLoS ONE 2017, 12, e0173880. [Google Scholar] [CrossRef]
- Kang, H.; Yu, H.; Zeng, L.; Ma, H.; Cao, G. LncRNA Rian reduces cardiomyocyte pyroptosis and alleviates myocardial ischemia-reperfusion injury by regulating by the miR-17-5p/CCND1 axis. Hypertens. Res. 2022, 45, 976–989. [Google Scholar] [CrossRef]
- Bai, Q.; Li, Y.; Song, K.; Huang, J.; Qin, L. Knockdown of XIST up-regulates 263294miR-340-5p to relieve myocardial ischaemia-reperfusion injury via inhibiting cyclin D1. ESC Heart Fail. 2022, 9, 1050–1060. [Google Scholar] [CrossRef]
- Cubukcuoglu Deniz, G.; Durdu, S.; Dogan, Y.; Erdemli, E.; Ozdag, H.; Akar, A.R. Molecular Signatures of Human Chronic Atrial Fibrillation in Primary Mitral Regurgitation. Cardiovasc. Ther. 2021, 2021, 5516185. [Google Scholar] [CrossRef]
- Ghiroldi, A.; Piccoli, M.; Creo, P.; Cirillo, F.; Rota, P.; D’Imperio, S.; Ciconte, G.; Monasky, M.M.; Micaglio, E.; Garatti, A.; et al. Role of sialidase Neu3 and ganglioside GM3 in cardiac fibroblasts activation. Biochem. J. 2020, 477, 3401–3415. [Google Scholar] [CrossRef] [PubMed]
- Piccoli, M.; Conforti, E.; Varrica, A.; Ghiroldi, A.; Cirillo, F.; Resmini, G.; Pluchinotta, F.; Tettamanti, G.; Giamberti, A.; Frigiola, A.; et al. NEU3 sialidase role in activating HIF-1alpha in response to chronic hypoxia in cyanotic congenital heart patients. Int. J. Cardiol. 2017, 230, 6–13. [Google Scholar] [CrossRef] [PubMed]
- Wang, F.; Wang, H.; Wang, L.; Zhou, S.; Chang, M.; Zhou, J.; Dou, Y.; Wang, Y.; Shi, X. Association Between Single Nucleotide Polymorphisms in NFATC1 Signaling Pathway Genes and Susceptibility to Congenital Heart Disease in the Chinese Population. Pediatr. Cardiol. 2016, 37, 1548–1561. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Li, W.; Deng, K.Q.; Tian, S.; Liu, H.; Shi, H.; Fang, Q.; Liu, Z.; Chen, Z.; Tian, T.; et al. The E3 Ligase TRIM16 Is a Key Suppressor of Pathological Cardiac Hypertrophy. Circ. Res. 2022, 130, 1586–1600. [Google Scholar] [CrossRef] [PubMed]
- Liu, L.; Zhu, J.; Glass, P.S.; Brink, P.R.; Rampil, I.J.; Rebecchi, M.J. Age-associated changes in cardiac gene expression after preconditioning. Anesthesiology 2009, 111, 1052–1064. [Google Scholar] [CrossRef]
- Alikunju, S.; Niranjan, N.; Mohsin, M.; Sayed, N.; Sayed, D. G3bp1-microRNA-1 axis regulates cardiomyocyte hypertrophy. Cell Signal. 2022, 91, 110245. [Google Scholar] [CrossRef]
- Li, S.J.; Hu, W.L.; Liu, D.T.; Sun, F.H.; Zhang, Q.; Yang, X.C.; Yu, S.Z.; Jin, L.; Wang, X.F. MTAP gene is associated with ischemic stroke in Chinese Hans. J. Neurol. Sci. 2009, 284, 103–107. [Google Scholar] [CrossRef]
- Wolfsberg, T.G.; Straight, P.D.; Gerena, R.L.; Huovila, A.P.; Primakoff, P.; Myles, D.G.; White, J.M. ADAM, a widely distributed and developmentally regulated gene family encoding membrane proteins with a disintegrin and metalloprotease domain. Dev. Biol. 1995, 169, 378–383. [Google Scholar] [CrossRef]
- Hooft van Huijsduijnen, R. ADAM 20 and 21; two novel human testis-specific membrane metalloproteases with similarity to fertilin-alpha. Gene 1998, 206, 273–282. [Google Scholar] [CrossRef]
- Sudhir, K. Lipoprotein-associated phospholipase A 2, vascular inflammation and cardiovascular risk prediction. Vasc. Health Risk Manag. 2006, 2, 153–156. [Google Scholar] [CrossRef][Green Version]
- Feldmann, R.; Fischer, C.; Kodelja, V.; Behrens, S.; Haas, S.; Vingron, M.; Timmermann, B.; Geikowski, A.; Sauer, S. Genome-wide analysis of LXRα activation reveals new transcriptional networks in human atherosclerotic foam cells. Nucleic Acids Res. 2013, 41, 3518–3531. [Google Scholar] [CrossRef] [PubMed]
- Spadaro, O.; Youm, Y.; Shchukina, I.; Ryu, S.; Sidorov, S.; Ravussin, A.; Nguyen, K.; Aladyeva, E.; Predeus, A.N.; Smith, S.R.; et al. Caloric restriction in humans reveals immunometabolic regulators of health span. Science 2022, 375, 671–677. [Google Scholar] [CrossRef] [PubMed]
- Lv, S.L.; Zeng, Z.F.; Gan, W.Q.; Wang, W.Q.; Li, T.G.; Hou, Y.F.; Yan, Z.; Zhang, R.X.; Yang, M. Lp-PLA2 inhibition prevents Ang II-induced cardiac inflammation and fibrosis by blocking macrophage NLRP3 inflammasome activation. Acta Pharmacol. Sin. 2021, 42, 2016–2032. [Google Scholar] [CrossRef] [PubMed]
- Li, N.; Zhu, L.; Zhou, H.; Zheng, D.; Xu, G.; Sun, L.; Gao, J.; Shao, G. miRNA-1183-targeted regulation of Bcl-2 contributes to the pathogenesis of rheumatic heart disease. Biosci. Rep. 2020, 40, BSR20201573. [Google Scholar] [CrossRef]
- Chaanine, A.H.; Higgins, L.; Lauterboeck, L.; Markowski, T.; Yang, Q.; Delafontaine, P. Multiomics Approach Reveals an Important Role of BNIP3 in Myocardial Remodeling and the Pathogenesis of Heart Failure with Reduced Ejection Fraction. Cells 2022, 11, 1572. [Google Scholar] [CrossRef]
- Chaanine, A.H.; Joyce, L.D.; Stulak, J.M.; Maltais, S.; Joyce, D.L.; Dearani, J.A.; Klaus, K.; Nair, K.S.; Hajjar, R.J.; Redfield, M.M. Mitochondrial Morphology, Dynamics, and Function in Human Pressure Overload or Ischemic Heart Disease With Preserved or Reduced Ejection Fraction. Circ Heart Fail. 2019, 12, e005131. [Google Scholar] [CrossRef]
- Lammerich, A.; Bohm, J.; Schimke, I.; Wagner, K.D.; Storch, E.; Günther, J. Effects of hypoxia, simulated ischemia and reoxygenation on the contractile function of human atrial trabeculae. Mol. Cell. Biochem. 1996, 160, 143–151. [Google Scholar] [CrossRef]
| Demographic Parameters/Medical History | Medication (%) | ||
|---|---|---|---|
| Gender m/f (%) | 56.6/44.4 | ß-blockers | 44.4 |
| Age (y ± SD) | 66.8 ± 9.4 | ACE Inhibitors | 44.4 |
| BMI (% ± SD) | 29 ± 6.4 | AT1 Antagonist | 22.2 |
| SR (%) | 100 | MRA | 0 |
| AFIB | 0 | Statins | 77.7 |
| Paroxysmal AFIB | 0 | Ca2+ Antagonist | 44.4 |
| EF (% ± SD) | 54.9 ± 9.4 | ||
| CABG (%) | 77.8 | ||
| AVR (%) | 11.1 | ||
| MVR (%) | 11.1 | ||
| Groups | SR | AFIB |
|---|---|---|
| Demographic parameters | ||
| Gender m/f | 1/5 | 4/2 |
| Age (y ± SD) | 66 ± 10 | 73.7 ± 9.8 |
| BMI (% ± SD) | 29.2 ± 3.5 | 24.8 ± 2.9 |
| Cardiac function | ||
| EF (%± SD) | 60.8 ± 9.2 | 56.2 ± 1.5 |
| LVEDD | 49.2 ± 2.4 | 57.2 ± 3.1 |
| RVEDD | 33.8 ± 1.3 | 33.3 ± 0.9 |
| IVS | 11.8 ± 0.9 | 12.8 ± 0.4 |
| LA major axis | 62.8 ± 3.6 | 70.4 ± 2.3 |
| Comorbidities (%) | ||
| Hypertension | 83 | 100 |
| Diabetes | 17 | 0 |
| CABG | 17 | 67 |
| AVR | 17 | 17 |
| MVR | 100 | 100 |
| Medication (%) | ||
| ß-blockers | 67 | 83 |
| ACE Inhibitors | 50 | 33 |
| AT1 Antagonist | 17 | 33 |
| MRA | 17 | 17 |
| Statins | 50 | 33 |
| Ca2+ Antagonist | 17 | 0 |
| Groups | NF | DCM |
|---|---|---|
| Gender m/f (%) | 50/50 | 100/0 |
| Age (y ± SD) | 63 ± 16.3 | 59 ± 14 |
| BMI (% ± SD) | 25.4 ± 5.1 | 25.8 ± 2 |
| SR (%) | 75 | 33.3 |
| AFIB (%) | 25 | 66.7 |
| EF (%± SD) | 58 ± 0.13 | 22.5 ± 6.12 |
| CHD | 0 | 16.7 |
| Hypertension | 25 | 83.3 |
| Diabetes | 0 | 33.3 |
| Hyperlipidemia | 0 | 50 |
| Paroxysmal AFIB | 25 | 33.3 |
| CABG | 0 | 0 |
| AVR | 0 | 0 |
| MVR | 0 | 0 |
| ß-blockers | 25 | 33.3 |
| ACE Inhibitors | 25 | 50 |
| AT1 Antagonist | 0 | 0 |
| MRA | 0 | 50 |
| Statins | 0 | 16.7 |
| Ca2+ Antagonist | 0 | 0 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Djalinac, N.; Kolesnik, E.; Maechler, H.; Scheruebel-Posch, S.; Pelzmann, B.; Rainer, P.P.; Foessl, I.; Wallner, M.; Scherr, D.; Heinemann, A.; et al. miR-1183 Is a Key Marker of Remodeling upon Stretch and Tachycardia in Human Myocardium. Int. J. Mol. Sci. 2022, 23, 6962. https://doi.org/10.3390/ijms23136962
Djalinac N, Kolesnik E, Maechler H, Scheruebel-Posch S, Pelzmann B, Rainer PP, Foessl I, Wallner M, Scherr D, Heinemann A, et al. miR-1183 Is a Key Marker of Remodeling upon Stretch and Tachycardia in Human Myocardium. International Journal of Molecular Sciences. 2022; 23(13):6962. https://doi.org/10.3390/ijms23136962
Chicago/Turabian StyleDjalinac, Natasa, Ewald Kolesnik, Heinrich Maechler, Susanne Scheruebel-Posch, Brigitte Pelzmann, Peter P. Rainer, Ines Foessl, Markus Wallner, Daniel Scherr, Akos Heinemann, and et al. 2022. "miR-1183 Is a Key Marker of Remodeling upon Stretch and Tachycardia in Human Myocardium" International Journal of Molecular Sciences 23, no. 13: 6962. https://doi.org/10.3390/ijms23136962
APA StyleDjalinac, N., Kolesnik, E., Maechler, H., Scheruebel-Posch, S., Pelzmann, B., Rainer, P. P., Foessl, I., Wallner, M., Scherr, D., Heinemann, A., Sedej, S., Ljubojevic-Holzer, S., von Lewinski, D., & Bisping, E. (2022). miR-1183 Is a Key Marker of Remodeling upon Stretch and Tachycardia in Human Myocardium. International Journal of Molecular Sciences, 23(13), 6962. https://doi.org/10.3390/ijms23136962






