Hyperprogressive Disease: Main Features and Key Controversies
Abstract
1. Introduction
2. Definition
3. Epidemiology
4. Biomarkers
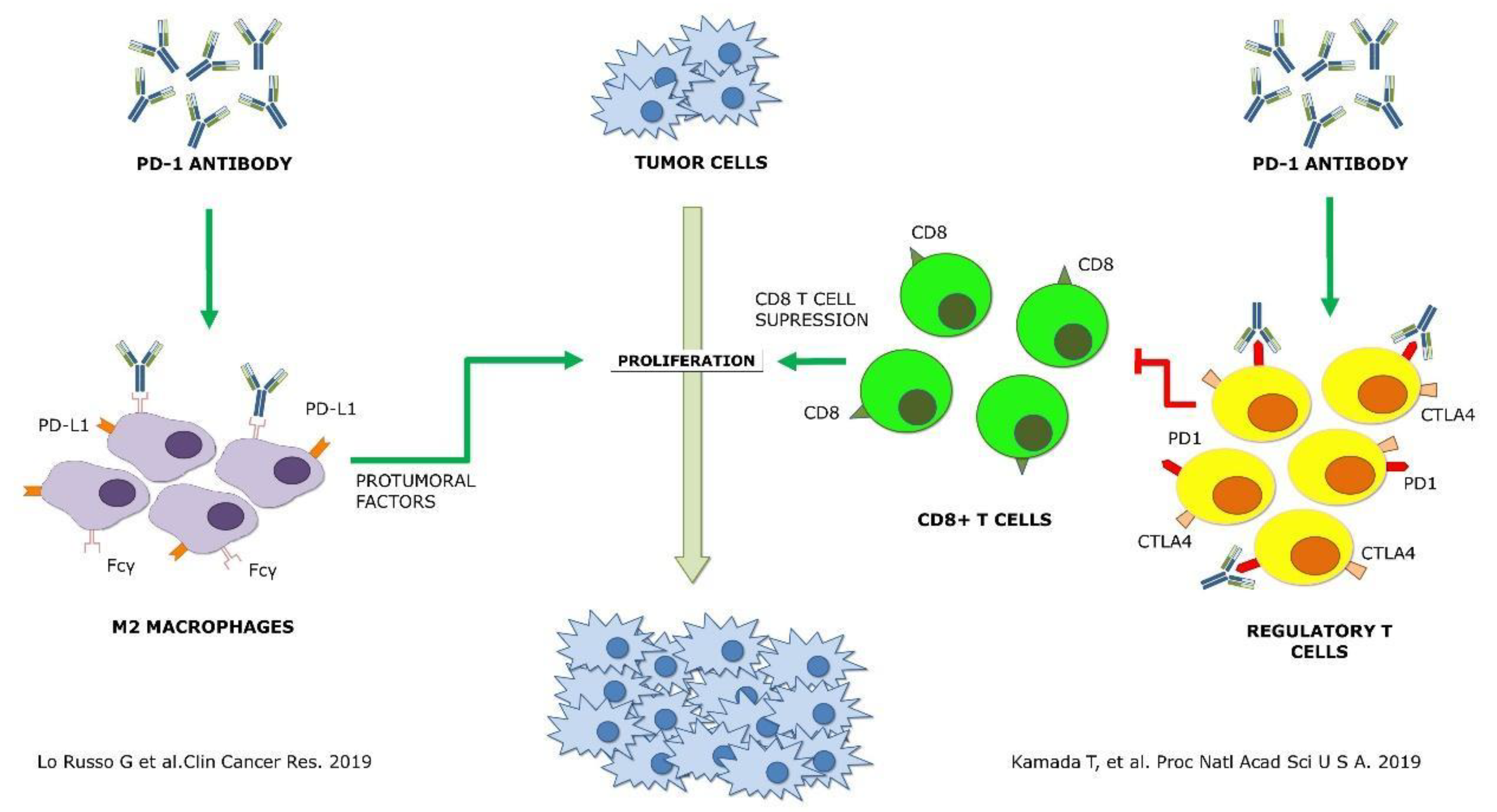
5. Mechanisms
6. Implications
7. Future Strategies and Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Chubachi, S.; Yasuda, H.; Irie, H.; Fukunaga, K.; Naoki, K.; Soejima, K.; Betsuyaku, T. A Case of Non-Small Cell Lung Cancer with Possible “Disease Flare” on Nivolumab Treatment. Case Rep. Oncol. Med. 2016, 2016, 1075641. [Google Scholar] [CrossRef]
- Ferrara, R.; Mezquita, L.; Texier, M.; Lahmar, J.; Audigier-Valette, C.; Tessonnier, L.; Mazieres, J.; Zalcman, G.; Brosseau, S.; Le Moulec, S.; et al. Hyperprogressive Disease in Patients With Advanced Non-Small Cell Lung Cancer Treated With PD-1/PD-L1 Inhibitors or With Single-Agent Chemotherapy. JAMA Oncol. 2018, 4, 1543–1552. [Google Scholar] [CrossRef] [PubMed]
- Aoki, M.; Shoji, H.; Nagashima, K.; Imazeki, H.; Miyamoto, T.; Hirano, H.; Honma, Y.; Iwasa, S.; Okita, N.; Takashima, A.; et al. Hyperprogressive disease during nivolumab or irinotecan treatment in patients with advanced gastric cancer. ESMO Open 2019, 4, e000488. [Google Scholar] [CrossRef] [PubMed]
- Saâda-Bouzid, E.; Defaucheux, C.; Karabajakian, A.; Coloma, V.P.; Servois, V.; Paoletti, X.; Even, C.; Fayette, J.; Guigay, J.; Loirat, D.; et al. Hyperprogression during anti-PD-1/PD-L1 therapy in patients with recurrent and/or metastatic head and neck squamous cell carcinoma. Ann. Oncol. 2017, 28, 1605–1611. [Google Scholar] [CrossRef]
- Champiat, S.; Dercle, L.; Ammari, S.; Massard, C.; Hollebecque, A.; Postel-Vinay, S.; Chaput, N.; Eggermont, A.; Marabelle, A.; Soria, J.C.; et al. Hyperprogressive Disease Is a New Pattern of Progression in Cancer Patients Treated by Anti-PD-1/PD-L1. Clin. Cancer Res. 2017, 23, 1920–1928. [Google Scholar] [CrossRef] [PubMed]
- Ferté, C.; Fernandez, M.; Hollebecque, A.; Koscielny, S.; Levy, A.; Massard, C.; Balheda, R.; Bot, B.; Gomez-Roca, C.; Dromain, C.; et al. Tumor growth rate is an early indicator of antitumor drug activity in phase I clinical trials. Clin. Cancer Res. 2014, 20, 246–252. [Google Scholar] [CrossRef]
- Kas, B.; Talbot, H.; Ferrara, R.; Richard, C.; Lamarque, J.P.; Pitre-Champagnat, S.; Planchard, D.; Balleyguier, C.; Besse, B.; Mezquita, L.; et al. Clarification of Definitions of Hyperprogressive Disease During Immunotherapy for Non-Small Cell Lung Cancer. JAMA Oncol. 2020, 6, 1039–1046. [Google Scholar] [CrossRef]
- Kato, S.; Goodman, A.; Walavalkar, V.; Barkauskas, D.A.; Sharabi, A.; Kurzrock, R. Hyperprogressors after Immunotherapy: Analysis of Genomic Alterations Associated with Accelerated Growth Rate. Clin. Cancer Res. 2017, 23, 4242–4250. [Google Scholar] [CrossRef]
- Lo Russo, G.; Moro, M.; Sommariva, M.; Cancila, V.; Boeri, M.; Centonze, G.; Ferro, S.; Ganzinelli, M.; Gasparini, P.; Huber, V.; et al. Antibody-Fc/FcR Interaction on Macrophages as a Mechanism for Hyperprogressive Disease in Non-small Cell Lung Cancer Subsequent to PD-1/PD-L1 Blockade. Clin. Cancer Res. 2019, 25, 989–999. [Google Scholar] [CrossRef]
- Matos, I.; Martin-Liberal, J.; García-Ruiz, A.; Hierro, C.; Ochoa de Olza, M.; Viaplana, C.; Azaro, A.; Vieito, M.; Braña, I.; Mur, G.; et al. Capturing Hyperprogressive Disease with Immune-Checkpoint Inhibitors Using RECIST 1.1 Criteria. Clin. Cancer Res. 2020, 26, 1846–1855. [Google Scholar] [CrossRef] [PubMed]
- Gomes da Morais, A.L.; de Miguel, M.; Cardenas, J.M.; Calvo, E. Comparison of radiological criteria for hyperprogressive disease in response to immunotherapy. Cancer Treat. Rev. 2020, 91, 102116. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.Y.; Lee, K.H.; Kang, J.; Borcoman, E.; Saada-Bouzid, E.; Kronbichler, A.; Hong, S.H.; de Rezende, L.F.M.; Ogino, S.; Keum, N.; et al. Hyperprogressive Disease during Anti-PD-1 (PDCD1)/PD-L1 (CD274) Therapy: A Systematic Review and Meta-Analysis. Cancers 2019, 11, 1699. [Google Scholar] [CrossRef]
- Arasanz, H.; Zuazo, M.; Bocanegra, A.; Gato, M.; Martínez-Aguillo, M.; Morilla, I.; Fernández, G.; Hernández, B.; López, P.; Alberdi, N.; et al. Early Detection of Hyperprogressive Disease in Non-Small Cell Lung Cancer by Monitoring of Systemic T Cell Dynamics. Cancers 2020, 12, 344. [Google Scholar] [CrossRef] [PubMed]
- Kanjanapan, Y.; Day, D.; Wang, L.; Al-Sawaihey, H.; Abbas, E.; Namini, A.; Siu, L.L.; Hansen, A.; Razak, A.A.; Spreafico, A.; et al. Hyperprogressive disease in early-phase immunotherapy trials: Clinical predictors and association with immune-related toxicities. Cancer 2019, 125, 1341–1349. [Google Scholar] [CrossRef] [PubMed]
- Refae, S.; Gal, J.; Brest, P.; Giacchero, D.; Borchiellini, D.; Ebran, N.; Peyrade, F.; Guigay, J.; Milano, G.; Saada-Bouzid, E. Hyperprogression under Immune Checkpoint Inhibitor: A potential role for germinal immunogenetics. Sci. Rep. 2020, 10, 3565. [Google Scholar] [CrossRef] [PubMed]
- Sasaki, A.; Nakamura, Y.; Mishima, S.; Kawazoe, A.; Kuboki, Y.; Bando, H.; Kojima, T.; Doi, T.; Ohtsu, A.; Yoshino, T.; et al. Predictive factors for hyperprogressive disease during nivolumab as anti-PD1 treatment in patients with advanced gastric cancer. Gastric. Cancer 2019, 22, 793–802. [Google Scholar] [CrossRef] [PubMed]
- Kim, C.G.; Kim, K.H.; Pyo, K.H.; Xin, C.F.; Hong, M.H.; Ahn, B.C.; Kim, Y.; Choi, S.J.; Yoon, H.I.; Lee, J.G.; et al. Hyperprogressive disease during PD-1/PD-L1 blockade in patients with non-small-cell lung cancer. Ann. Oncol. 2019, 30, 1104–1113. [Google Scholar] [CrossRef] [PubMed]
- Ferrara, R.; Proto, C.; Lo Russo, G.; Signorelli, D.; Prelaj, A.; Galli, G.; Zilembo, N.; De Toma, A.; Viscardi, G.; Lobefaro, R.; et al. Circulating and tumor associated neutrophil subtypes correlate with hyperprogressive disease (HPD) upon immunecheckpoint inhibitors (ICI) in advanced non-small cell lung cancer (aNSCLC) patients (pts) and models. In Proceedings of the Annual Meeting of the American Association for Cancer Research 2020, Philadelphia, PA, USA, 27–28 April 2020. [Google Scholar]
- Singavi, A.K.; Menon, S.; Kilari, D.; Alqwasmi, A.; Ritch, P.S.; Thomas, J.P.; Martin, A.L.; Oxencis, C.; Ali, S.; George, B. Predictive biomarkers for Hyper-progression (HP) in response to Immune Checkpoint Inhibitors (ICI)–Analysis of Somatic Alterations (Sas). Ann. Oncol. 2017, 28. [Google Scholar] [CrossRef]
- Kamada, T.; Togashi, Y.; Tay, C.; Ha, D.; Sasaki, A.; Nakamura, Y.; Sato, E.; Fukuoka, S.; Tada, Y.; Tanaka, A.; et al. PD-1+ regulatory T cells amplified by PD-1 blockade promote hyperprogression of cancer. Proc. Natl. Acad. Sci. USA 2019, 116, 9999–10008. [Google Scholar] [CrossRef]
- Chen, Y.; Li, X.; Liu, G.; Chen, S.; Xu, M.; Song, L.; Wang, Y. ctDNA Concentration, MIKI67 Mutations and Hyper-Progressive Disease Related Gene Mutations Are Prognostic Markers for Camrelizumab and Apatinib Combined Multiline Treatment in Advanced NSCLC. Front. Oncol. 2020, 10, 1706. [Google Scholar] [CrossRef]
- Weiss, G.J.; Beck, J.; Braun, D.P.; Bornemann-Kolatzki, K.; Barilla, H.; Cubello, R.; Quan, W., Jr.; Sangal, A.; Khemka, V.; Waypa, J.; et al. Tumor Cell-Free DNA Copy Number Instability Predicts Therapeutic Response to Immunotherapy. Clin. Cancer Res. 2017, 23, 5074–5081. [Google Scholar] [CrossRef] [PubMed]
- Khorrami, M.; Prasanna, P.; Gupta, A.; Patil, P.; Velu, P.D.; Thawani, R.; Corredor, G.; Alilou, M.; Bera, K.; Fu, P.; et al. Changes in CT Radiomic Features Associated with Lymphocyte Distribution Predict Overall Survival and Response to Immunotherapy in Non-Small Cell Lung Cancer. Cancer Immunol. Res. 2020, 8, 108–119. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.Y.; Park, J.E.; Jo, Y.; Shim, W.H.; Nam, S.J.; Kim, J.H.; Yoo, R.E.; Choi, S.H.; Kim, H.S. Incorporating diffusion- and perfusion-weighted MRI into a radiomics model improves diagnostic performance for pseudoprogression in glioblastoma patients. Neuro Oncol. 2019, 21, 404–414. [Google Scholar] [CrossRef] [PubMed]
- Sun, R.; Limkin, E.J.; Vakalopoulou, M.; Dercle, L.; Champiat, S.; Han, S.R.; Verlingue, L.; Brandao, D.; Lancia, A.; Ammari, S.; et al. A radiomics approach to assess tumour-infiltrating CD8 cells and response to anti-PD-1 or anti-PD-L1 immunotherapy: An imaging biomarker, retrospective multicohort study. Lancet Oncol. 2018, 19, 1180–1191. [Google Scholar] [CrossRef]
- Sun, R.; Sundahl, N.; Hecht, M.; Putz, F.; Lancia, A.; Rouyar, A.; Milic, M.; Carré, A.; Battistella, E.; Alvarez Andres, E.; et al. Radiomics to predict outcomes and abscopal response of patients with cancer treated with immunotherapy combined with radiotherapy using a validated signature of CD8 cells. J. Immunother. Cancer. 2020, 8, e001429. [Google Scholar] [CrossRef]
- Trebeschi, S.; Drago, S.G.; Birkbak, N.J.; Kurilova, I.; Cǎlin, A.M.; Delli Pizzi, A.; Lalezari, F.; Lambregts, D.M.J.; Rohaan, M.W.; Parmar, C.; et al. Predicting response to cancer immunotherapy using noninvasive radiomic biomarkers. Ann. Oncol. 2019, 30, 998–1004. [Google Scholar] [CrossRef]
- Ji, Z.; Cui, Y.; Peng, Z.; Gong, J.; Zhu, H.T.; Zhang, X.; Li, J.; Lu, M.; Lu, Z.; Shen, L.; et al. Use of Radiomics to Predict Response to Immunotherapy of Malignant Tumors of the Digestive System. Med. Sci. Monit. 2020, 26, e924671. [Google Scholar] [CrossRef] [PubMed]
- Vaidya, P.; Bera, K.; Patil, P.D.; Gupta, A.; Jain, P.; Alilou, M.; Khorrami, M.; Velcheti, V.; Madabhushi, A. Novel, non-invasive imaging approach to identify patients with advanced non-small cell lung cancer at risk of hyperprogressive disease with immune checkpoint blockade. J. Immunother. Cancer 2020, 8, e001343. [Google Scholar] [CrossRef]
- Zaiss, D.M.; van Loosdregt, J.; Gorlani, A.; Bekker, C.P.; Gröne, A.; Sibilia, M.; van Bergen en Henegouwen, P.M.; Roovers, R.C.; Coffer, P.J.; Sijts, A.J. Amphiregulin enhances regulatory T cell-suppressive function via the epidermal growth factor receptor. Immunity 2013, 38, 275–284. [Google Scholar] [CrossRef]
- Du, S.; McCall, N.; Park, K.; Guan, Q.; Fontina, P.; Ertel, A.; Zhan, T.; Dicker, A.P.; Lu, B. Blockade of Tumor-Expressed PD-1 promotes lung cancer growth. Oncoimmunology 2018, 7, e1408747. [Google Scholar] [CrossRef]
- Tumeh, P.C.; Hellmann, M.D.; Hamid, O.; Tsai, K.K.; Loo, K.L.; Gubens, M.A.; Rosenblum, M.; Harview, C.L.; Taube, J.M.; Handley, N.; et al. Liver Metastasis and Treatment Outcome with Anti-PD-1 Monoclonal Antibody in Patients with Melanoma and NSCLC. Cancer Immunol. Res. 2017, 5, 417–424. [Google Scholar] [CrossRef] [PubMed]
- Mezquita, L.; Auclin, E.; Ferrara, R.; Charrier, M.; Remon, J.; Planchard, D.; Ponce, S.; Ares, L.P.; Leroy, L.; Audigier-Valette, C.; et al. Association of the Lung Immune Prognostic Index With Immune Checkpoint Inhibitor Outcomes in Patients With Advanced Non-Small Cell Lung Cancer. JAMA Oncol. 2018, 4, 351–357. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.; Lahl, K.; Hori, S.; Loddenkemper, C.; Chaudhry, A.; deRoos, P.; Rudensky, A.; Sparwasser, T. Cutting edge: Depletion of Foxp3+ cells leads to induction of autoimmunity by specific ablation of regulatory T cells in genetically targeted mice. J. Immunol. 2009, 183, 7631–7634. [Google Scholar] [CrossRef]
- Rech, A.J.; Mick, R.; Martin, S.; Recio, A.; Aqui, N.A.; Powell, D.J., Jr.; Colligon, T.A.; Trosko, J.A.; Leinbach, L.I.; Pletcher, C.H.; et al. CD25 blockade depletes and selectively reprograms regulatory T cells in concert with immunotherapy in cancer patients. Sci. Transl. Med. 2012, 4, 134ra62. [Google Scholar] [CrossRef] [PubMed]
- Solomon, I.; Amann, M.; Goubier, A.; Arce Vargas, F.; Zervas, D.; Qing, C.; Henry, J.Y.; Ghorani, E.; Akarca, A.U.; Marafioti, T.; et al. CD25-Treg-depleting antibodies preserving IL-2 signaling on effector T cells enhance effector activation and antitumor immunity. Nat. Cancer 2020, 1, 1153–1166. [Google Scholar] [CrossRef]
- De Simone, M.; Arrigoni, A.; Rossetti, G.; Gruarin, P.; Ranzani, V.; Politano, C.; Bonnal, R.J.P.; Provasi, E.; Sarnicola, M.L.; Panzeri, I.; et al. Transcriptional Landscape of Human Tissue Lymphocytes Unveils Uniqueness of Tumor-Infiltrating T Regulatory Cells. Immunity 2016, 45, 1135–1147. [Google Scholar] [CrossRef]
- Sugiyama, D.; Nishikawa, H.; Maeda, Y.; Nishioka, M.; Tanemura, A.; Katayama, I.; Ezoe, S.; Kanakura, Y.; Sato, E.; Fukumori, Y.; et al. Anti-CCR4 mAb selectively depletes effector-type FoxP3+CD4+ regulatory T cells, evoking antitumor immune responses in humans. Proc. Natl. Acad. Sci. USA 2013, 110, 17945–17950. [Google Scholar] [CrossRef]
- Ji, Z.; Peng, Z.; Gong, J.; Zhang, X.; Li, J.; Lu, M.; Lu, Z.; Shen, L. Hyperprogression after immunotherapy in patients with malignant tumors of digestive system. BMC Cancer 2019, 19, 1–9. [Google Scholar] [CrossRef]
- Gomez-Roca, C.; Italiano, A.; Le Tourneau, C.; Cassier, P.; Toulmonde, M.; D’Angelo, S.; Campone, M.; Weber, K.; Loirat, D.; Cannarile, M.; et al. Phase I study of emactuzumab single agent or in combination with paclitaxel in patients with advanced/metastatic solid tumors reveals depletion of immunosuppressive M2-like macrophages. Ann. Oncol. 2019, 30, 1381–1392. [Google Scholar] [CrossRef]
- Strachan, D.C.; Ruffell, B.; Oei, Y.; Bissell, M.J.; Coussens, L.M.; Pryer, N.; Daniel, D. CSF1R inhibition delays cervical and mammary tumor growth in murine models by attenuating the turnover of tumor-associated macrophages and enhancing infiltration by CD8+T cells. OncoImmunology 2013, 2, e26968. [Google Scholar] [CrossRef]
- Germano, G.; Frapolli, R.; Belgiovine, C.; Anselmo, A.; Pesce, S.; Liguori, M.; Erba, E.; Uboldi, S.; Zucchetti, M.; Pasqualini, F.; et al. Role of Macrophage Targeting in the Antitumor Activity of Trabectedin. Cancer Cell 2013, 23, 249–262. [Google Scholar] [CrossRef] [PubMed]
| Authors | Tumor Type | Patients | HPD Definition | Incidence (%) | Biomarker |
|---|---|---|---|---|---|
| Arasanz H (2020) [13] | NSCLC | 70 | TGR ≥ 2 | 17.9% | Low CD4+ CD27− CD28− cells (blood) Increase CD4+ CD27− CD28− ≥ 30% |
| Champiat S (2017) [5] | Mixed Cohort | 131 | TGR ≥ 2 | 9% | Age ≥ 65 |
| Ferrara R (2018) [2] | NSCLC | 406 | ∆TGR > 50% | 13.8% | > 2 metastatic sites |
| Ferrara R (2020) [18] | NSCLC | 46 | TGR ≥ 2 ∆TGR > 50% | 9% | CD10− CD66b+ LDNs (blood) |
| Kanjanapan Y (2019) [14] | Mixed Cohort | 182 | TGR ≥ 2 | 7% | Female sex |
| Kamada T (2019) [20] | Gastric Cancer | 36 | Combined: - TTF < 2 months - > 50% increase in tumor burden - 2x increase in TGR | 11.1% | None |
| Kato S (2017) [8] | Mixed Cohort | 155 | Combined: - TTF < 2 months - > 50% increase in tumor burden - 2x increase in TGR | 3.9% | MDM2 amplification EGFR alteration |
| Kim CG (2019) [17] | NSCLC | 263 | TGKR ≥ 2 TGR ≥ 2 TTF < 2 mo | 20.9% (TGKR) 20.5% (TGR) 37.3% (TTF) | ≥2 metastatic locations Liver metastases Neutrophils (blood) NLR PCR (blood) LDH (blood) High CD8+ PD-1+ TIGIT + TL Low CD8+ CCR7− CD45RA− TL |
| Kim JY (2019) [12] | Mixed Cohort | 1519 | N/A | 14.3% | LDH (blood) Liver metastases > 2 metastatic locations Low tumor PD-L1 |
| Lo Russo G (2019) [9] | NSCLC | 152 | 3 out of 5 of: - TTF < 2 months - ≥ 50% diameter increase - ≥ 2 new lesions - Spread to new organ - Decline to PS ≥ 2 | 25.7% | Tumor-infiltrating macrophages |
| Matos I (2020) [10] | Mixed Cohort | 270 | PD in the first 8 weeks and 1 of: - ≥ 40% diameter increase - new lesions in ≥ 2 new organs | 10.7% | Liver metastases >2 metastatic locations |
| Refae S (2020) [15] | Mixed Cohort | 98 | TGKR ≥ 2 | 14% | Age ≥ 70 VEGFR2 SNP PD-L1 SNP |
| Sâada-Bouzid E (2017) [4] | HNSCC | 34 | TGKR ≥ 2 | 29% | Local relapse |
| Sasaki A (2019) [16] | Gastric Cancer | 62 | TGR ≥ 2 | 21% | PS 1-2 Liver metastases Large tumor lesions Neutrophils (blood) PCR (blood) |
| Singavi A (2017) [19] | Mixed Cohort | Not specified | Increase tumor size > 50% TGR ≥ 2 | Not specified | MDM2/4 amplification EGFR alterations |
| Vaidya P (2020) [29] | NSCLC | 109 | TGKR ≥ 2 | 17.4% | Radiomic model (vessel tortuosity and peritumoral textures) |
| Weiss GJ (2017) [22] | Mixed Cohort | 56 | Not specified | 10.7% | Chromosomal instability changes |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Arasanz, H.; Zuazo, M.; Bocanegra, A.; Chocarro, L.; Blanco, E.; Martínez, M.; Morilla, I.; Fernández, G.; Teijeira, L.; Morente, P.; et al. Hyperprogressive Disease: Main Features and Key Controversies. Int. J. Mol. Sci. 2021, 22, 3736. https://doi.org/10.3390/ijms22073736
Arasanz H, Zuazo M, Bocanegra A, Chocarro L, Blanco E, Martínez M, Morilla I, Fernández G, Teijeira L, Morente P, et al. Hyperprogressive Disease: Main Features and Key Controversies. International Journal of Molecular Sciences. 2021; 22(7):3736. https://doi.org/10.3390/ijms22073736
Chicago/Turabian StyleArasanz, Hugo, Miren Zuazo, Ana Bocanegra, Luisa Chocarro, Ester Blanco, Maite Martínez, Idoia Morilla, Gonzalo Fernández, Lucía Teijeira, Pilar Morente, and et al. 2021. "Hyperprogressive Disease: Main Features and Key Controversies" International Journal of Molecular Sciences 22, no. 7: 3736. https://doi.org/10.3390/ijms22073736
APA StyleArasanz, H., Zuazo, M., Bocanegra, A., Chocarro, L., Blanco, E., Martínez, M., Morilla, I., Fernández, G., Teijeira, L., Morente, P., Echaide, M., Castro, N., Fernández, L., Garnica, M., Ramos, P., Escors, D., Kochan, G., & Vera, R. (2021). Hyperprogressive Disease: Main Features and Key Controversies. International Journal of Molecular Sciences, 22(7), 3736. https://doi.org/10.3390/ijms22073736







