CRISPR/Cas Technology in Pig-to-Human Xenotransplantation Research
Abstract
1. Introduction
2. CRISPR/Cas Technology
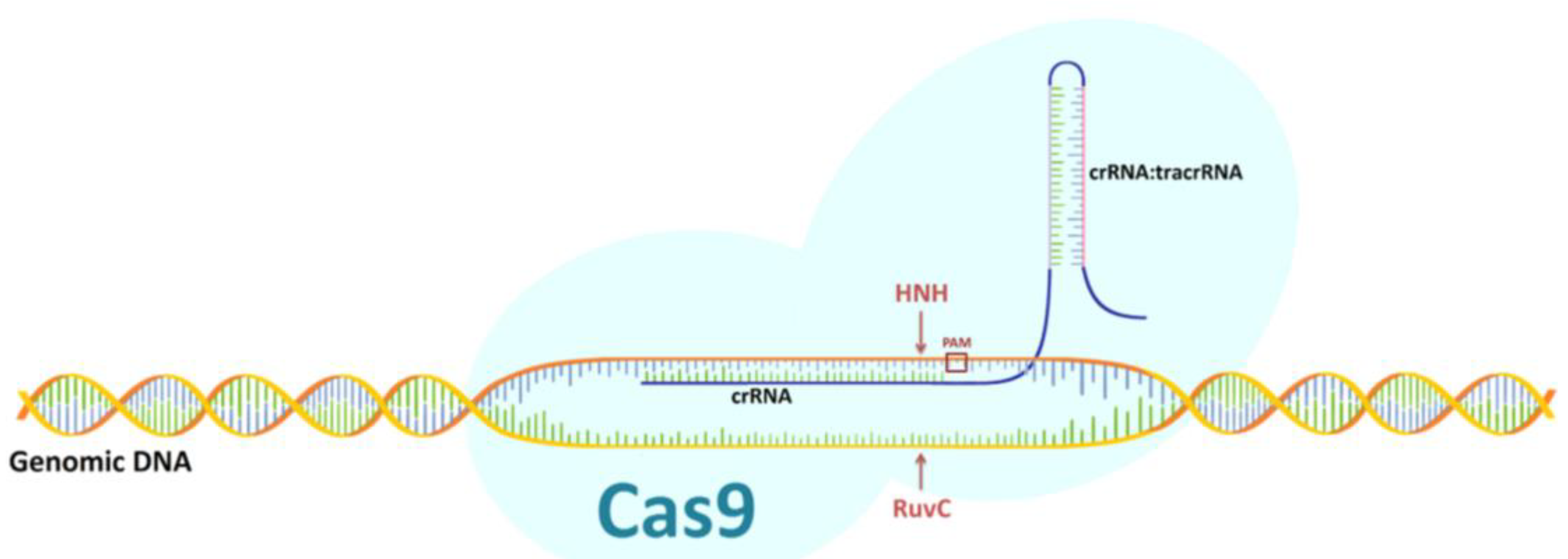
2.1. Origin and Mechanism of Action
2.2. Mechanisms of Repairing Double-Stranded DNA Breaks
2.3. Difficulties and Limitations of Technology
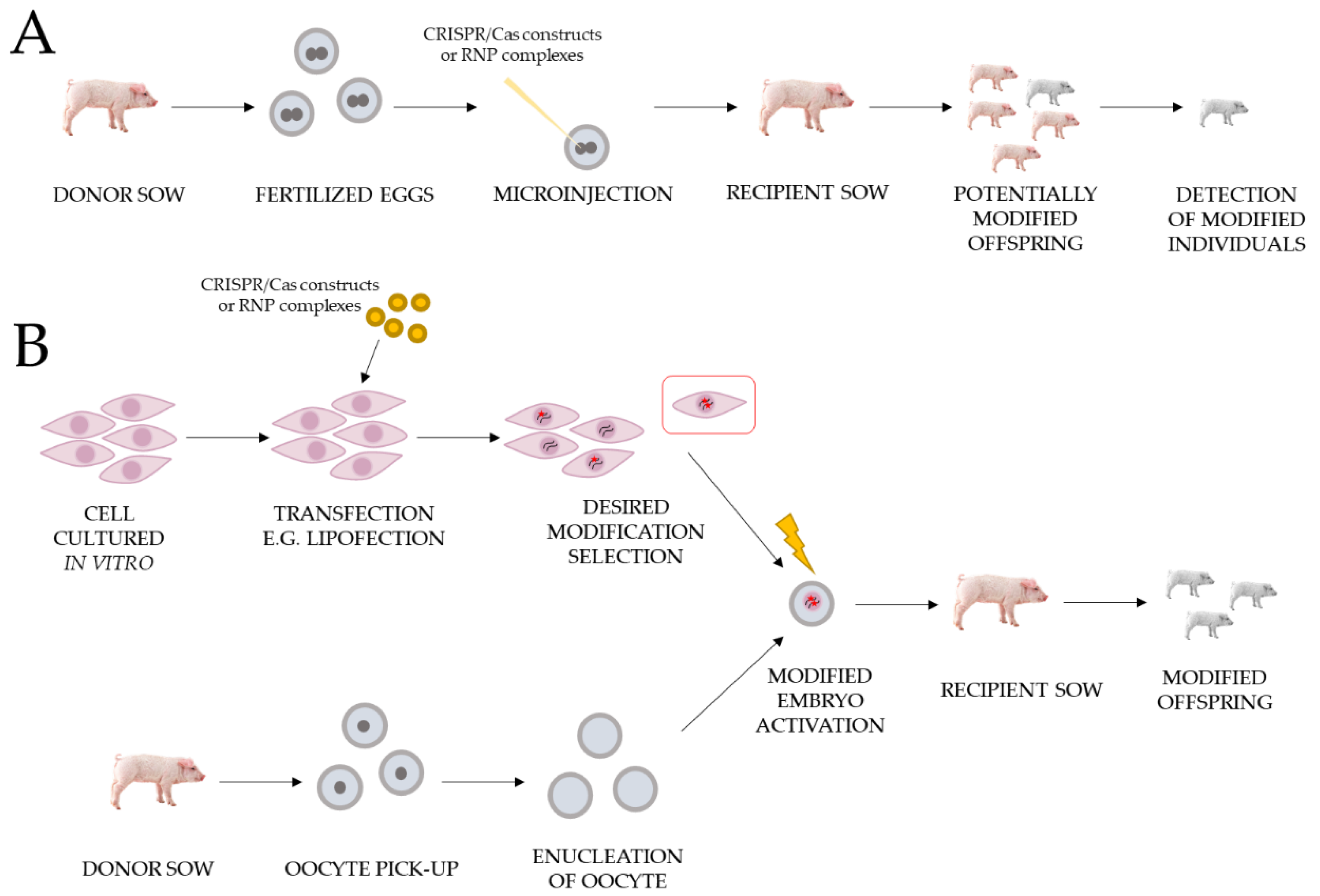
2.4. Limitations of CRISPR/Cas When Used in Large Animal Models
3. Xenotransplantation
3.1. Hyperacute Rejection (HAR)
3.2. Acute Humoral Xenograft Rejection (AHXR)
3.3. Acute Cellular Rejection (ACR)
3.4. Coagulation System Dysregulation
3.5. Preclinical Studies
3.6. Virological Concerns
3.7. Legal, Social and Ethical Concerns
4. Pigs Modified with CRISPR/Cas Technology in Xenotransplantation
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Boratyńska, M.; Patrzałek, D. Transplantology: Challenges for Today. Arch. Immunol. Ther. Exp. 2016, 64, 37–45. [Google Scholar] [CrossRef] [PubMed]
- Jinek, M.; Chylinski, K.; Fonfara, I.; Hauer, M.; Doudna, J.A.; Charpentier, E. A Programmable Dual-RNA–Guided DNA Endonuclease in Adaptive Bacterial Immunity. Science 2012, 337, 816–821. [Google Scholar] [CrossRef] [PubMed]
- Gasiunas, G.; Barrangou, R.; Horvath, P.; Siksnys, V. Cas9-crRNA ribonucleoprotein complex mediates specific DNA cleavage for adaptive immunity in bacteria. Proc. Natl. Acad. Sci. USA 2012, 109, E2579–E2586. [Google Scholar] [CrossRef] [PubMed]
- Grissa, I.; Vergnaud, G.; Pourcel, C. The CRISPRdb database and tools to display CRISPRs and to generate dictionaries of spacers and repeats. BMC Bioinform. 2007, 8, 178. [Google Scholar] [CrossRef]
- Haft, D.H.; Selengut, J.; Mongodin, E.F.; Nelson, K.E. A guild of 45 CRISPR-associated (Cas) protein families and multiple CRISPR/cas subtypes exist in prokaryotic genomes. PLoS Comput. Biol. 2005, 1, 474–483. [Google Scholar] [CrossRef]
- Ran, F.A.; Hsu, P.D.; Wright, J.; Agarwala, V.; Scott, D.A.; Zhang, F. Genome engineering using the CRISPR-Cas9 system. Nat. Protoc. 2013, 8, 2281–2308. [Google Scholar] [CrossRef]
- Du, J.; Yin, N.; Xie, T.; Zheng, Y.; Xia, N.; Shang, J.; Chen, F.; Zhang, H.; Yu, J.; Liu, F. Quantitative assessment of HR and NHEJ activities via CRISPR/Cas9-induced oligodeoxynucleotide-mediated DSB repair. DNA Repair 2018, 70, 67–71. [Google Scholar] [CrossRef] [PubMed]
- Miyaoka, Y.; Mayerl, S.J.; Chan, A.H.; Conklin, B.R. Detection and quantification of HDR and NHEJ induced by genome editing at endogenous gene loci using droplet digital PCR. Methods Mol. Biol. 2018, 1768, 349–362. [Google Scholar] [CrossRef]
- Sternberg, S.H.; Lafrance, B.; Kaplan, M.; Doudna, J.A. Conformational control of DNA target cleavage by CRISPR-Cas9. Nature 2015, 527, 110–113. [Google Scholar] [CrossRef]
- Hsu, P.D.; Scott, D.A.; Weinstein, J.A.; Ran, F.A.; Konermann, S.; Agarwala, V.; Li, Y.; Fine, E.J.; Wu, X.; Shalem, O.; et al. DNA targeting specificity of RNA-guided Cas9 nucleases. Nat. Biotechnol. 2013, 31, 827–832. [Google Scholar] [CrossRef]
- Sansbury, B.M.; Hewes, A.M.; Kmiec, E.B. Understanding the diversity of genetic outcomes from CRISPR-Cas generated homology-directed repair. Commun. Biol. 2019, 2, 458. [Google Scholar] [CrossRef]
- Pannunzio, N.R.; Watanabe, G.; Lieber, M.R. Nonhomologous DNA end-joining for repair of DNA double-strand breaks. J. Biol. Chem. 2018, 293, 10512–10523. [Google Scholar] [CrossRef] [PubMed]
- Deriano, L.; Roth, D.B. Modernizing the nonhomologous end-joining repertoire: Alternative and classical NHEJ share the stage. Annu. Rev. Genet. 2013, 47, 433–455. [Google Scholar] [CrossRef]
- Roth, D.B.; Wilson, J.H. Nonhomologous recombination in mammalian cells: Role for short sequence homologies in the joining reaction. Mol. Cell. Biol. 1986, 6, 4295–4304. [Google Scholar] [CrossRef]
- Rothkamm, K.; Krüger, I.; Thompson, L.H.; Löbrich, M. Pathways of DNA Double-Strand Break Repair during the Mammalian Cell Cycle. Mol. Cell. Biol. 2003, 23, 5706–5715. [Google Scholar] [CrossRef]
- Chang, H.H.Y.; Pannunzio, N.R.; Adachi, N.; Lieber, M.R. Non-homologous DNA end joining and alternative pathways to double-strand break repair. Nat. Rev. Mol. Cell Biol. 2017, 18, 495–506. [Google Scholar] [CrossRef]
- Simsek, D.; Jasin, M. Alternative end-joining is suppressed by the canonical NHEJ component Xrcc4-ligase IV during chromosomal translocation formation. Nat. Struct. Mol. Biol. 2010, 17, 410–416. [Google Scholar] [CrossRef] [PubMed]
- Zhu, C.; Mills, K.D.; Ferguson, D.O.; Lee, C.; Manis, J.; Fleming, J.; Gao, Y.; Morton, C.C.; Alt, F.W. Unrepaired DNA breaks in p53-deficient cells lead to oncogenic gene amplification subsequent to translocations. Cell 2002, 109, 811–821. [Google Scholar] [CrossRef]
- Guirouilh-Barbat, J.; Rass, E.; Plo, I.; Bertrand, P.; Lopez, B.S. Defects in XRCC4 and KU80 differentially affect the joining of distal nonhomologous ends. Proc. Natl. Acad. Sci. USA 2007, 104, 20902–20907. [Google Scholar] [CrossRef]
- Wood, R.D.; Doublié, S. DNA polymerase θ (POLQ), double-strand break repair, and cancer. DNA Repair 2016, 44, 22–32. [Google Scholar] [CrossRef] [PubMed]
- Davis, L.; Maizels, N. Homology-directed repair of DNA nicks via pathways distinct from canonical double-strand break repair. Proc. Natl. Acad. Sci. USA 2014, 111, E924–E932. [Google Scholar] [CrossRef] [PubMed]
- Daley, J.M.; Kwon, Y.; Niu, H.; Sung, P. Investigations of homologous recombination pathways and their regulation. Yale J. Biol. Med. 2013, 86, 453–461. [Google Scholar] [PubMed]
- Kurihara, T.; Kouyama-Suzuki, E.; Satoga, M.; Li, X.; Badawi, M.; Baig, D.N.; Yanagawa, T.; Uemura, T.; Mori, T.; Tabuchi, K. DNA repair protein RAD51 enhances the CRISPR/Cas9-mediated knock-in efficiency in brain neurons. Biochem. Biophys. Res. Commun. 2020, 524, 621–628. [Google Scholar] [CrossRef] [PubMed]
- Rees, H.A.; Yeh, W.H.; Liu, D.R. Development of hRad51–Cas9 nickase fusions that mediate HDR without double-stranded breaks. Nat. Commun. 2019, 10, 2212. [Google Scholar] [CrossRef]
- Fu, Y.; Foden, J.A.; Khayter, C.; Maeder, M.L.; Reyon, D.; Joung, J.K.; Sander, J.D. High-frequency off-target mutagenesis induced by CRISPR-Cas nucleases in human cells. Nat. Biotechnol. 2013, 31, 822–826. [Google Scholar] [CrossRef] [PubMed]
- Chen, S.; Yao, Y.; Zhang, Y.; Fan, G. CRISPR system: Discovery, development and off-target detection. Cell. Signal. 2020, 70, 109577. [Google Scholar] [CrossRef]
- Ryczek, N.; Hryhorowicz, M.; Lipiński, D.; Zeyland, J.; Słomski, R. Evaluation of the CRISPR/Cas9 genetic constructs in efficient disruption of porcine genes for xenotransplantation purposes along with an assessment of the off-target mutation formation. Genes 2020, 11, 713. [Google Scholar] [CrossRef]
- Cui, Y.; Liao, X.; Peng, S.; Tang, T.; Huang, C.; Yang, C. OffScan: A universal and fast CRISPR off-target sites detection tool. BMC Genom. 2020, 21, 872. [Google Scholar] [CrossRef]
- Chiang, T.W.W.; Le Sage, C.; Larrieu, D.; Demir, M.; Jackson, S.P. CRISPR-Cas9D10A nickase-based genotypic and phenotypic screening to enhance genome editing. Sci. Rep. 2016, 6, 24356. [Google Scholar] [CrossRef]
- Zhou, Z.; Cao, G.; Li, Z.; Han, X.; Li, C.; Lu, Z.; Zhao, Y.; Li, X. ling Truncated gRNA reduces CRISPR/Cas9-mediated off-target rate for MSTN gene knockout in bovines. J. Integr. Agric. 2019, 18, 2835–2843. [Google Scholar] [CrossRef]
- Fu, Y.; Sander, J.D.; Reyon, D.; Cascio, V.M.; Joung, J.K. Improving CRISPR-Cas nuclease specificity using truncated guide RNAs. Nat. Biotechnol. 2014, 32, 279–284. [Google Scholar] [CrossRef]
- Ikeda, A.; Fujii, W.; Sugiura, K.; Naito, K. High-fidelity endonuclease variant HypaCas9 facilitates accurate allele-specific gene modification in mouse zygotes. Commun. Biol. 2019, 2, 1–7. [Google Scholar] [CrossRef]
- Kleinstiver, B.P.; Prew, M.S.; Tsai, S.Q.; Topkar, V.V.; Nguyen, N.T.; Zheng, Z.; Gonzales, A.P.W.; Li, Z.; Peterson, R.T.; Yeh, J.R.J.; et al. Engineered CRISPR-Cas9 nucleases with altered PAM specificities. Nature 2015, 523, 481–485. [Google Scholar] [CrossRef]
- Vakulskas, C.A.; Behlke, M.A. Evaluation and reduction of crispr off-target cleavage events. Nucleic Acid Ther. 2019, 29, 167–174. [Google Scholar] [CrossRef] [PubMed]
- Anzalone, A.V.; Randolph, P.B.; Davis, J.R.; Sousa, A.A.; Koblan, L.W.; Levy, J.M.; Chen, P.J.; Wilson, C.; Newby, G.A.; Raguram, A.; et al. Search-and-replace genome editing without double-strand breaks or donor DNA. Nature 2019, 576, 149–157. [Google Scholar] [CrossRef]
- Schene, I.F.; Joore, I.P.; Oka, R.; Mokry, M.; van Vugt, A.H.M.; van Boxtel, R.; van der Doef, H.P.J.; van der Laan, L.J.W.; Verstegen, M.M.A.; van Hasselt, P.M.; et al. Prime editing for functional repair in patient-derived disease models. Nat. Commun. 2020, 11, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Cencic, R.; Miura, H.; Malina, A.; Robert, F.; Ethier, S.; Schmeing, T.M.; Dostie, J.E.; Pelletier, J. Protospacer Adjacent Motif (PAM)—Distal Sequences Engage CRISPR Cas9 DNA Target Cleavage. PLoS ONE 2014, 9, e109213. [Google Scholar] [CrossRef]
- Zhang, Y. The CRISPR-Cas9 system in Neisseria spp. Pathog. Dis. 2017, 75, ftx036. [Google Scholar] [CrossRef]
- Kleinstiver, B.P.; Prew, M.S.; Tsai, S.Q.; Nguyen, N.T.; Topkar, V.V.; Zheng, Z.; Joung, J.K. Broadening the targeting range of Staphylococcus aureus CRISPR-Cas9 by modifying PAM recognition. Nat. Biotechnol. 2015, 33, 1293–1298. [Google Scholar] [CrossRef] [PubMed]
- Müller, M.; Lee, C.M.; Gasiunas, G.; Davis, T.H.; Cradick, T.J.; Siksnys, V.; Bao, G.; Cathomen, T.; Mussolino, C. Streptococcus thermophilus CRISPR-Cas9 systems enable specific editing of the human genome. Mol. Ther. 2016, 24, 636–644. [Google Scholar] [CrossRef]
- Chatterjee, P.; Jakimo, N.; Jacobson, J.M. Minimal PAM specificity of a highly similar SpCas9 ortholog. Sci. Adv. 2018, 4, eaau0766. [Google Scholar] [CrossRef]
- Dugar, G.; Leenay, R.T.; Eisenbart, S.K.; Bischler, T.; Aul, B.U.; Beisel, C.L.; Sharma, C.M. CRISPR RNA-Dependent Binding and Cleavage of Endogenous RNAs by the Campylobacter jejuni Cas9. Mol. Cell 2018, 69, 893–905. [Google Scholar] [CrossRef] [PubMed]
- Hirano, H.; Gootenberg, J.S.; Horii, T.; Abudayyeh, O.O.; Kimura, M.; Hsu, P.D.; Nakane, T.; Ishitani, R.; Hatada, I.; Zhang, F.; et al. Structure and Engineering of Francisella novicida Cas9. Cell 2016, 164, 950–961. [Google Scholar] [CrossRef] [PubMed]
- Karvelis, T.; Gasiunas, G.; Miksys, A.; Barrangou, R.; Horvath, P.; Siksnys, V. crRNA and tracrRNA guide Cas9-mediated DNA interference in Streptococcus thermophilus. RNA Biol. 2013, 10, 841–851. [Google Scholar] [CrossRef] [PubMed]
- Paul, B.; Montoya, G. CRISPR-Cas12a: Functional overview and applications. Biomed. J. 2020, 43, 8–17. [Google Scholar] [CrossRef] [PubMed]
- Fu, B.X.H.; Smith, J.D.; Fuchs, R.T.; Mabuchi, M.; Curcuru, J.; Robb, G.B.; Fire, A.Z. Target-dependent nickase activities of the CRISPR–Cas nucleases Cpf1 and Cas9. Nat. Microbiol. 2019, 4, 888–897. [Google Scholar] [CrossRef]
- Strecker, J.; Jones, S.; Koopal, B.; Schmid-Burgk, J.; Zetsche, B.; Gao, L.; Makarova, K.S.; Koonin, E.V.; Zhang, F. Engineering of CRISPR-Cas12b for human genome editing. Nat. Commun. 2019, 10, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Ihry, R.J.; Worringer, K.A.; Salick, M.R.; Frias, E.; Ho, D.; Theriault, K.; Kommineni, S.; Chen, J.; Sondey, M.; Ye, C.; et al. P53 inhibits CRISPR-Cas9 engineering in human pluripotent stem cells. Nat. Med. 2018, 24, 939–946. [Google Scholar] [CrossRef]
- Kosicki, M.; Tomberg, K.; Bradley, A. Repair of double-strand breaks induced by CRISPR–Cas9 leads to large deletions and complex rearrangements. Nat. Biotechnol. 2018, 36, 765–771. [Google Scholar] [CrossRef]
- Zuccaro, M.V.; Xu, J.; Mitchell, C.; Marin, D.; Zimmerman, R.; Rana, B.; Weinstein, E.; King, R.T.; Palmerola, K.L.; Smith, M.E.; et al. Allele-Specific Chromosome Removal after Cas9 Cleavage in Human Embryos. Cell 2020, 183, 1650–1664.e15. [Google Scholar] [CrossRef]
- Brezgin, S.; Kostyusheva, A.; Kostyushev, D.; Chulanov, V. Dead cas systems: Types, principles, and applications. Int. J. Mol. Sci. 2019, 20, 6041. [Google Scholar] [CrossRef]
- Hryhorowicz, M.; Lipiński, D.; Hryhorowicz, S.; Nowak-Terpiłowska, A.; Ryczek, N.; Zeyland, J. Application of genetically engineered pigs in biomedical research. Genes 2020, 11, 670. [Google Scholar] [CrossRef]
- Navarro-Serna, S.; Vilarino, M.; Park, I.; Gadea, J.; Ross, P.J. Livestock Gene Editing by One-step Embryo Manipulation. J. Equine Vet. Sci. 2020, 89, 103025. [Google Scholar] [CrossRef] [PubMed]
- Mehravar, M.; Shirazi, A.; Nazari, M.; Banan, M. Mosaicism in CRISPR/Cas9-mediated genome editing. Dev. Biol. 2019, 445, 156–162. [Google Scholar] [CrossRef]
- Ran, F.A.; Cong, L.; Yan, W.X.; Scott, D.A.; Gootenberg, J.S.; Kriz, A.J.; Zetsche, B.; Shalem, O.; Wu, X.; Makarova, K.S.; et al. In vivo genome editing using Staphylococcus aureus Cas9. Nature 2015, 520, 186–191. [Google Scholar] [CrossRef] [PubMed]
- Hryhorowicz, M.; Grześkowiak, B.; Mazurkiewicz, N.; Śledziński, P.; Lipiński, D.; Słomski, R. Improved Delivery of CRISPR/Cas9 System Using Magnetic Nanoparticles into Porcine Fibroblast. Mol. Biotechnol. 2019, 61, 173–180. [Google Scholar] [CrossRef]
- Aristizabal, A.M.; Caicedo, L.A.; Martínez, J.M.; Moreno, M.; Echeverri, G.J. Clinical Xenotransplantation, a Closer Reality: Literature Review. Cirugía Española (Engl. Ed.) 2017, 95, 62–72. [Google Scholar] [CrossRef]
- Deschamps, J.-Y.; Roux, F.A.; Sai, P.; Gouin, E. History of xenotransplantation. Xenotransplantation 2005, 12, 91–109. [Google Scholar] [CrossRef]
- Cooper, D.K.C.; Ekser, B.; Tector, A.J. A brief history of clinical xenotransplantation. Int. J. Surg. 2015, 23, 205–210. [Google Scholar] [CrossRef] [PubMed]
- Cooper, D.K.C.; Gaston, R.; Eckhoff, D.; Ladowski, J.; Yamamoto, T.; Wang, L.; Iwase, H.; Hara, H.; Tector, M.; Tector, A.J. Xenotransplantation—the current status and prospects. Br. Med. Bull. 2018, 125, 5–14. [Google Scholar] [CrossRef]
- Hryhorowicz, M.; Zeyland, J.; Słomski, R.; Lipiński, D. Genetically Modified Pigs as Organ Donors for Xenotransplantation. Mol. Biotechnol. 2017, 59, 435–444. [Google Scholar] [CrossRef] [PubMed]
- Vadori, M.; Cozzi, E. The immunological barriers to xenotransplantation. Tissue Antigens 2015, 86, 239–253. [Google Scholar] [CrossRef]
- Cooper, D.K.C.; Ekser, B.; Tector, A.J. Immunobiological barriers to xenotransplantation. Int. J. Surg. 2015, 23, 211–216. [Google Scholar] [CrossRef]
- Ngo, B.T.-T.; Beiras-Fernandez, A.; Hammer, C.; Thein, E. Hyperacute rejection in the xenogenic transplanted rat liver is triggered by the complement system only in the presence of leukocytes and free radical species. Xenotransplantation 2013, 20, 177–187. [Google Scholar] [CrossRef] [PubMed]
- Cooper, D.K.C.; Ekser, B.; Ramsoondar, J.; Phelps, C.; Ayares, D. The role of genetically engineered pigs in xenotransplantation research. J. Pathol. 2016, 238, 288–299. [Google Scholar] [CrossRef] [PubMed]
- Galili, U. Interaction of the natural anti-Gal antibody with α-galactosyl epitopes: A major obstacle for xenotransplantation in humans. Immunol. Today 1993, 14, 480–482. [Google Scholar] [CrossRef]
- Macher, B.A.; Galili, U. The Galα1,3Galβ1,4GlcNAc-R (α-Gal) epitope: A carbohydrate of unique evolution and clinical relevance. Biochim. Biophys. Acta Gen. Subj. 2008, 1780, 75–88. [Google Scholar] [CrossRef] [PubMed]
- Lin, S.S.; Hanaway, M.J.; Gonzalez-Stawinski, G.V.; Lau, C.L.; Parker, W.; Davis, R.D.; Byrne, G.W.; Diamond, L.E.; Logan, J.S.; Platt, J.L. The role of anti-Galalpha1-3Gal antibodies in acute vascular rejection and accommodation of xenografts. Transplantation 2000, 70, 1667–1674. [Google Scholar] [CrossRef] [PubMed]
- Chuang, C.K.; Chen, C.H.; Huang, C.L.; Su, Y.H.; Peng, S.H.; Lin, T.Y.; Tai, H.C.; Yang, T.S.; Tu, C.F. Generation of GGTA1 Mutant Pigs by Direct Pronuclear Microinjection of CRISPR/Cas9 Plasmid Vectors. Anim. Biotechnol. 2017, 28, 174–181. [Google Scholar] [CrossRef]
- Varki, A. Loss of N-glycolylneuraminic acid in humans: Mechanisms, consequences, and implications for hominid evolution. Am. J. Phys. Anthropol. 2001, 116, 54. [Google Scholar] [CrossRef] [PubMed]
- Basnet, N.B.; Ide, K.; Tahara, H.; Tanaka, Y.; Ohdan, H. Deficiency of N-glycolylneuraminic acid and Galα1-3Galβ1-4GlcNAc epitopes in xenogeneic cells attenuates cytotoxicity of human natural antibodies. Xenotransplantation 2010, 17, 440–448. [Google Scholar] [CrossRef] [PubMed]
- Byrne, G.W.; Du, Z.; Stalboerger, P.; Kogelberg, H.; McGregor, C.G.A. Cloning and expression of porcine β1,4 N-acetylgalactosaminyl transferase encoding a new xenoreactive antigen. Xenotransplantation 2014, 21, 543–554. [Google Scholar] [CrossRef]
- Byrne, G.; Ahmad-Villiers, S.; Du, Z.; McGregor, C. B4GALNT2 and xenotransplantation: A newly appreciated xenogeneic antigen. Xenotransplantation 2018, 25, e12394. [Google Scholar] [CrossRef] [PubMed]
- Wang, Z.-Y.; Burlak, C.; Estrada, J.L.; Li, P.; Tector, M.F.; Tector, A.J. Erythrocytes from GGTA1/CMAH knockout pigs: Implications for xenotransfusion and testing in non-human primates. Xenotransplantation 2014, 21, 376–384. [Google Scholar] [CrossRef] [PubMed]
- Estrada, J.L.; Martens, G.; Li, P.; Adams, A.; Newell, K.A.; Ford, M.L.; Butler, J.R.; Sidner, R.; Tector, M.; Tector, J. Evaluation of human and non-human primate antibody binding to pig cells lacking GGTA1/CMAH/β4GalNT2 genes. Xenotransplantation 2015, 22, 194–202. [Google Scholar] [CrossRef]
- Scobie, L.; Padler-Karavani, V.; Le Bas-Bernardet, S.; Crossan, C.; Blaha, J.; Matouskova, M.; Hector, R.D.; Cozzi, E.; Vanhove, B.; Charreau, B.; et al. Long-Term IgG Response to Porcine Neu5Gc Antigens without Transmission of PERV in Burn Patients Treated with Porcine Skin Xenografts. J. Immunol. 2013, 191, 2907–2915. [Google Scholar] [CrossRef] [PubMed]
- Fischer, K.; Rieblinger, B.; Hein, R.; Sfriso, R.; Zuber, J.; Fischer, A.; Klinger, B.; Liang, W.; Flisikowski, K.; Kurome, M.; et al. Viable pigs after simultaneous inactivation of porcine MHC class I and three xenoreactive antigen genes GGTA1, CMAH and B4GALNT2. Xenotransplantation 2020, 27, e12560. [Google Scholar] [CrossRef]
- Satyananda, V.; Hara, H.; Ezzelarab, M.B.; Phelps, C.; Ayares, D.; Cooper, D.K. New concepts of immune modulation in xenotransplantation. Transplantation 2013, 96, 937–945. [Google Scholar] [CrossRef]
- Fischer, K.; Kraner-Scheiber, S.; Petersen, B.; Rieblinger, B.; Buermann, A.; Flisikowska, T.; Flisikowski, K.; Christan, S.; Edlinger, M.; Baars, W.; et al. Efficient production of multi-modified pigs for xenotransplantation by “combineering”, gene stacking and gene editing. Sci. Rep. 2016, 6, 29081. [Google Scholar] [CrossRef] [PubMed]
- Hsieh, C.L.; Obara, H.; Ogura, Y.; Martinez, O.M.; Krams, S.M. NK cells and transplantation. Transpl. Immunol. 2002, 9, 111–114. [Google Scholar] [CrossRef]
- Wang, Y.; Du, Y.; Zhou, X.; Wang, L.; Li, J.; Wang, F.; Huang, Z.; Huang, X.; Wei, H. Efficient generation of B2m-null pigs via injection of zygote with TALENs. Sci. Rep. 2016, 6, 38854. [Google Scholar] [CrossRef]
- Puga Yung, G.; Bongoni, A.K.; Pradier, A.; Madelon, N.; Papaserafeim, M.; Sfriso, R.; Ayares, D.L.; Wolf, E.; Klymiuk, N.; Bähr, A.; et al. Release of pig leukocytes and reduced human NK cell recruitment during ex vivo perfusion of HLA-E/human CD46 double-transgenic pig limbs with human blood. Xenotransplantation 2018, 25, e12357. [Google Scholar] [CrossRef]
- Längin, M.; Mayr, T.; Reichart, B.; Michel, S.; Buchholz, S.; Guethoff, S.; Dashkevich, A.; Baehr, A.; Egerer, S.; Bauer, A.; et al. Consistent success in life-supporting porcine cardiac xenotransplantation. Nature 2018, 564, 430–433. [Google Scholar] [CrossRef] [PubMed]
- Watzl, C. How to trigger a killer: Modulation of natural killer cell reactivity on many levels. Adv. Immunol. 2014, 124, 137–170. [Google Scholar] [CrossRef] [PubMed]
- Joanna, Z.; Magdalena, H.; Agnieszka, N.T.; Jacek, J.; Ryszard, S.; Zdzisław, S.; Barbara, G.; Daniel, L. The production of UL16-binding protein 1 targeted pigs using CRISPR technology. 3 Biotech 2018, 8, 70. [Google Scholar] [CrossRef]
- Lilienfeld, B.G.; Garcia-Borges, C.; Crew, M.D.; Seebach, J.D. Porcine UL16-Binding Protein 1 Expressed on the Surface of Endothelial Cells Triggers Human NK Cytotoxicity through NKG2D. J. Immunol. 2006, 177, 2146–2152. [Google Scholar] [CrossRef]
- Griffiths, G.M.; Argon, Y. Structure and biogenesis of lytic granules. Curr. Top. Microbiol. Immunol. 1995, 198, 39–58. [Google Scholar] [CrossRef] [PubMed]
- Long, E.O.; Sik Kim, H.; Liu, D.; Peterson, M.E.; Rajagopalan, S. Controlling Natural Killer Cell Responses: Integration of Signals for Activation and Inhibition. Annu. Rev. Immunol. 2013, 31, 227–258. [Google Scholar] [CrossRef]
- Resch, T.; Fabritius, C.; Ebner, S.; Ritschl, P.; Kotsch, K. The Role of Natural Killer Cells in Humoral Rejection. Transplantation 2015, 99, 1335–1340. [Google Scholar] [CrossRef] [PubMed]
- Nowak-Terpiłowska, A.; Lipiński, D.; Hryhorowicz, M.; Juzwa, W.; Jura, J.; Słomski, R.; Mazurkiewicz, N.; Gawrońska, B.; Zeyland, J. Production of ULBP1-KO pigs with human CD55 expression using CRISPR technology. J. Appl. Anim. Res. 2020, 48, 93–101. [Google Scholar] [CrossRef]
- Liu, F.; Liu, J.; Yuan, Z.; Qing, Y.; Li, H.; Xu, K.; Zhu, W.; Zhao, H.; Jia, B.; Pan, W.; et al. Generation of GTKO Diannan Miniature Pig Expressing Human Complementary Regulator Proteins hCD55 and hCD59 via T2A Peptide-Based Bicistronic Vectors and SCNT. Mol. Biotechnol. 2018, 60, 550–562. [Google Scholar] [CrossRef]
- Barclay, A.N.; Brown, M.H. The SIRP family of receptors and immune regulation. Nat. Rev. Immunol. 2006, 6, 457–464. [Google Scholar] [CrossRef]
- Okazawa, H.; Motegi, S.; Ohyama, N.; Ohnishi, H.; Tomizawa, T.; Kaneko, Y.; Oldenborg, P.-A.; Ishikawa, O.; Matozaki, T. Negative regulation of phagocytosis in macrophages by the CD47-SHPS-1 system. J. Immunol. 2005, 174, 2004–2011. [Google Scholar] [CrossRef] [PubMed]
- Ganji, M.-R.; Broumand, B. Acute cellular rejection. Iran. J. Kidney Dis. 2007, 1, 54–56. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Ezzelarab, M.B.; Ayares, D.; Cooper, D.K.C. The Potential Role of Genetically-Modified Pig Mesenchymal Stromal Cells in Xenotransplantation. Stem Cell Rev. Rep. 2014, 10, 79–85. [Google Scholar] [CrossRef]
- Samy, K.P.; Butler, J.R.; Li, P.; Cooper, D.K.C.; Ekser, B. The Role of Costimulation Blockade in Solid Organ and Islet Xenotransplantation. J. Immunol. Res. 2017, 2017, 8415205. [Google Scholar] [CrossRef] [PubMed]
- Phelps, C.J.; Ball, S.F.; Vaught, T.D.; Vance, A.M.; Mendicino, M.; Monahan, J.A.; Walters, A.H.; Wells, K.D.; Dandro, A.S.; Ramsoondar, J.J.; et al. Production and characterization of transgenic pigs expressing porcine CTLA4-Ig. Xenotransplantation 2009, 16, 477–485. [Google Scholar] [CrossRef] [PubMed]
- Vabres, B.; Le Bas-Bernardet, S.; Riochet, D.; Chérel, Y.; Minault, D.; Hervouet, J.; Ducournau, Y.; Moreau, A.; Daguin, V.; Coulon, F.; et al. hCTLA4-Ig transgene expression in keratocytes modulates rejection of corneal xenografts in a pig to non-human primate anterior lamellar keratoplasty model. Xenotransplantation 2014, 21, 431–443. [Google Scholar] [CrossRef]
- Hara, H.; Witt, W.; Crossley, T.; Long, C.; Isse, K.; Fan, L.; Phelps, C.J.; Ayares, D.; Cooper, D.K.C.; Dai, Y.; et al. Human dominant-negative class II transactivator transgenic pigs—Effect on the human anti-pig T-cell immune response and immune status. Immunology 2013, 140, 39–46. [Google Scholar] [CrossRef] [PubMed]
- Reyes, L.M.; Estrada, J.L.; Wang, Z.Y.; Blosser, R.J.; Smith, R.F.; Sidner, R.A.; Paris, L.L.; Blankenship, R.L.; Ray, C.N.; Miner, A.C.; et al. Creating Class I MHC–Null Pigs Using Guide RNA and the Cas9 Endonuclease. J. Immunol. 2014, 193, 5751–5757. [Google Scholar] [CrossRef] [PubMed]
- Cooper, D.K.C.; Bottino, R. Recent advances in understanding xenotransplantation: Implications for the clinic. Expert Rev. Clin. Immunol. 2015, 11, 1379–1390. [Google Scholar] [CrossRef] [PubMed]
- Bühler, L.; Basker, M.; Alwayn, I.P.; Goepfert, C.; Kitamura, H.; Kawai, T.; Gojo, S.; Kozlowski, T.; Ierino, F.L.; Awwad, M.; et al. Coagulation and thrombotic disorders associated with pig organ and hematopoietic cell transplantation in nonhuman primates. Transplantation 2000, 70, 1323–1331. [Google Scholar] [CrossRef] [PubMed]
- Long, A.T.; Kenne, E.; Jung, R.; Fuchs, T.A.; Renné, T. Contact system revisited: An interface between inflammation, coagulation, and innate immunity. J. Thromb. Haemost. 2016, 14, 427–437. [Google Scholar] [CrossRef]
- Schmelzle, M.; Am Esch, J.S.; Robson, S.C. Coagulation, platelet activation and thrombosis in xenotransplantation. Curr. Opin. Organ Transplant. 2010, 15, 212–218. [Google Scholar] [CrossRef] [PubMed]
- Asada, Y.; Yamashita, A.; Sato, Y.; Hatakeyama, K. Thrombus formation and propagation in the onset of cardiovascular events. J. Atheroscler. Thromb. 2018, 25, 653–664. [Google Scholar] [CrossRef]
- Furie, B.; Furie, B.C. Mechanisms of thrombus formation. N. Engl. J. Med. 2008, 359, 938–949. [Google Scholar] [CrossRef]
- Lin, C.C.; Cooper, D.K.C.; Dorling, A. Coagulation dysregulation as a barrier to xenotransplantation in the primate. Transpl. Immunol. 2009, 21, 75–80. [Google Scholar] [CrossRef] [PubMed]
- Pierson, R.N.; Dorling, A.; Ayares, D.; Rees, M.A.; Seebach, J.D.; Fishman, J.A.; Hering, B.J.; Cooper, D.K.C. Current status of xenotransplantation and prospects for clinical application. Xenotransplantation 2009, 16, 263–280. [Google Scholar] [CrossRef] [PubMed]
- Maas, C.; Renne, T. Coagulation factor XII in thrombosis and inflammation. Blood 2018, 131, 1903–1909. [Google Scholar] [CrossRef]
- Zelaya, H.; Rothmeier, A.S.; Ruf, W. Tissue factor at the crossroad of coagulation and cell signaling. J. Thromb. Haemost. 2018, 16, 1941–1952. [Google Scholar] [CrossRef]
- Cowan, P.J.; D’Apice, A.J.F. Complement activation and coagulation in xenotransplantation. Immunol. Cell Biol. 2009, 87, 203–208. [Google Scholar] [CrossRef]
- Roussel, J.C.; Moran, C.J.; Salvaris, E.J.; Nandurkar, H.H.; d’Apice, A.J.F.; Cowan, P.J. Pig thrombomodulin binds human thrombin but is a poor cofactor for activation of human protein C and TAFI. Am. J. Transplant. 2008, 8, 1101–1112. [Google Scholar] [CrossRef] [PubMed]
- Pareti, F.I.; Mazzucato, M.; Bottini, E.; Mannucci, P.M. Interaction of porcine von Willebrand factor with the platelet glycoproteins Ib and IIb/IIIa complex. Br. J. Haematol. 1992, 82, 81–86. [Google Scholar] [CrossRef] [PubMed]
- Gawaz, M. Role of platelets in coronary thrombosis and reperfusion of ischemic myocardium. Cardiovasc. Res. 2004, 61, 498–511. [Google Scholar] [CrossRef]
- Pereboom, I.T.A.; Adelmeijer, J.; Van Leeuwen, Y.; Hendriks, H.G.D.; Porte, R.J.; Lisman, T. Development of a severe von willebrand factor/adamts13 dysbalance during orthotopic liver transplantation. Am. J. Transplant. 2009, 9, 1189–1196. [Google Scholar] [CrossRef] [PubMed]
- Iwase, H.; Ekser, B.; Hara, H.; Phelps, C.; Ayares, D.; Cooper, D.K.C.; Ezzelarab, M.B. Regulation of human platelet aggregation by genetically modified pig endothelial cells and thrombin inhibition. Xenotransplantation 2014, 21, 72–83. [Google Scholar] [CrossRef]
- Miwa, Y.; Yamamoto, K.; Onishi, A.; Iwamoto, M.; Yazaki, S.; Haneda, M.; Iwasaki, K.; Liu, D.; Ogawa, H.; Nagasaka, T.; et al. Potential value of human thrombomodulin and DAF expression for coagulation control in pig-to-human xenotransplantation. Xenotransplantation 2010, 17, 26–37. [Google Scholar] [CrossRef]
- Mohiuddin, M.M.; Singh, A.K.; Corcoran, P.C.; Thomas, M.L.; Clark, T.; Lewis, B.G.; Hoyt, R.F.; Eckhaus, M.; Pierson, R.N.; Belli, A.J.; et al. Chimeric 2C10R4 anti-CD40 antibody therapy is critical for long-term survival of GTKO.hCD46.hTBM pig-to-primate cardiac xenograft. Nat. Commun. 2016, 7, 11138. [Google Scholar] [CrossRef]
- Singh, A.K.; Chan, J.L.; DiChiacchio, L.; Hardy, N.L.; Corcoran, P.C.; Lewis, B.G.T.; Thomas, M.L.; Burke, A.P.; Ayares, D.; Horvath, K.A.; et al. Cardiac xenografts show reduced survival in the absence of transgenic human thrombomodulin expression in donor pigs. Xenotransplantation 2019, 26, e12465. [Google Scholar] [CrossRef]
- Bae, J.-S.; Yang, L.; Rezaie, A.R. Receptors of the protein C activation and activated protein C signaling pathways are colocalized in lipid rafts of endothelial cells. Proc. Natl. Acad. Sci. USA 2007, 104, 2867–2872. [Google Scholar] [CrossRef]
- Lin, C.C.; Ezzelarab, M.; Hara, H.; Long, C.; Lin, C.W.; Dorling, A.; Cooper, D.K.C. Atorvastatin or transgenic expression of TFPI inhibits coagulation initiated by anti-nonGal IgG binding to porcine aortic endothelial cells. J. Thromb. Haemost. 2010, 8, 2001–2010. [Google Scholar] [CrossRef] [PubMed]
- Wheeler, D.G.; Joseph, M.E.; Mahamud, S.D.; Aurand, W.L.; Mohler, P.J.; Pompili, V.J.; Dwyer, K.M.; Nottle, M.B.; Harrison, S.J.; d’Apice, A.J.F.; et al. Transgenic swine: Expression of human CD39 protects against myocardial injury. J. Mol. Cell. Cardiol. 2012, 52, 958–961. [Google Scholar] [CrossRef]
- Lau, C.L.; Cantu, E.; Gonzalez-Stawinski, G.V.; Holzknecht, Z.E.; Nichols, T.C.; Posther, K.E.; Rayborn, C.A.; Platt, J.L.; Parker, W.; Davis, R.D. The role of antibodies and von Willebrand factor in discordant pulmonary xenotransplantation. Am. J. Transplant. 2003, 3, 1065–1075. [Google Scholar] [CrossRef] [PubMed]
- Cantu, E.; Balsara, K.R.; Li, B.; Lau, C.; Gibson, S.; Wyse, A.; Baig, K.; Gaca, J.; Gonzalez-Stawinski, G.V.; Nichols, T.; et al. Prolonged function of macrophage, von Willebrand factor-deficient porcine pulmonary xenografts. Am. J. Transplant. 2007, 7, 66–75. [Google Scholar] [CrossRef] [PubMed]
- Li, P.; Estrada, J.L.; Burlak, C.; Montgomery, J.; Butler, J.R.; Santos, R.M.; Wang, Z.-Y.; Paris, L.L.; Blankenship, R.L.; Downey, S.M.; et al. Efficient generation of genetically distinct pigs in a single pregnancy using multiplexed single-guide RNA and carbohydrate selection. Xenotransplantation 2015, 22, 20–31. [Google Scholar] [CrossRef] [PubMed]
- Paris, L.L.; Chihara, R.K.; Reyes, L.M.; Sidner, R.A.; Estrada, J.L.; Downey, S.M.; Milgrom, D.A.; Tector, A.J.; Burlak, C. ASGR1 expressed by porcine enriched liver sinusoidal endothelial cells mediates human platelet phagocytosis in vitro. Xenotransplantation 2011, 18, 245–251. [Google Scholar] [CrossRef]
- Yu, X.H.; Deng, W.Y.; Jiang, H.T.; Li, T.; Wang, Y. Kidney xenotransplantation: Recent progress in preclinical research. Clin. Chim. Acta 2021, 514, 15–23. [Google Scholar] [CrossRef]
- Kim, S.C.; Mathews, D.V.; Breeden, C.P.; Higginbotham, L.B.; Ladowski, J.; Martens, G.; Stephenson, A.; Farris, A.B.; Strobert, E.A.; Jenkins, J.; et al. Long-term survival of pig-to-rhesus macaque renal xenografts is dependent on CD4 T cell depletion. Am. J. Transplant. 2019, 19, 2174–2185. [Google Scholar] [CrossRef]
- Shah, J.A.; Patel, M.S.; Elias, N.; Navarro-Alvarez, N.; Rosales, I.; Wilkinson, R.A.; Louras, N.J.; Hertl, M.; Fishman, J.A.; Colvin, R.B.; et al. Prolonged Survival Following Pig-to-Primate Liver Xenotransplantation Utilizing Exogenous Coagulation Factors and Costimulation Blockade. Am. J. Transplant. 2017, 17, 2178–2185. [Google Scholar] [CrossRef]
- Burdorf, L.; Laird, C.; Sendil, S.; O’Neill, N.; Zhang, T.; Parsell, D.; Tatarov, I.; Abady, Z.; Cerel, B.M.; Pratts, S.; et al. 31 Day Xeno Lung Recipient Survival—Progress towards the Clinic. J. Hear. Lung Transplant. 2019, 38, S39. [Google Scholar] [CrossRef]
- Fiebig, U.; Fischer, K.; Bähr, A.; Runge, C.; Schnieke, A.; Wolf, E.; Denner, J. Porcine endogenous retroviruses: Quantification of the copy number in cell lines, pig breeds, and organs. Xenotransplantation 2018, 25, e12445. [Google Scholar] [CrossRef]
- Ericsson, T.; Oldmixon, B.; Blomberg, J.; Rosa, M.; Patience, C.; Andersson, G. Identification of Novel Porcine Endogenous Betaretrovirus Sequences in Miniature Swine. J. Virol. 2001, 75, 2765–2770. [Google Scholar] [CrossRef]
- Blusch, J.H.; Patience, C.; Martin, U. Pig endogenous retroviruses and xenotransplantation. Xenotransplantation 2002, 9, 242–251. [Google Scholar] [CrossRef] [PubMed]
- Denner, J. Why was PERV not transmitted during preclinical and clinical xenotransplantation trials and after inoculation of animals? Retrovirology 2018, 15, 28. [Google Scholar] [CrossRef] [PubMed]
- Hawthorne, W.J.; Cowan, P.J.; Bühler, L.H.; Yi, S.; Bottino, R.; Pierson, R.N., 3rd; Ahn, C.; Azimzadeh, A.; Cozzi, E.; Gianello, P.; et al. Third WHO Global Consultation on Regulatory Requirements for Xenotransplantation Clinical Trials, Changsha, Hunan, China December 12–14, 2018: “The 2018 Changsha Communiqué” The 10-Year Anniversary of The International Consultation on Xenotransplantation. Xenotransplantation 2019, 26, e12513. [Google Scholar] [CrossRef]
- Morozov, V.A.; Plotzki, E.; Rotem, A.; Barkai, U.; Denner, J. Extended microbiological characterization of Göttingen minipigs: Porcine cytomegalovirus and other viruses. Xenotransplantation 2016, 23, 490–496. [Google Scholar] [CrossRef]
- Plotzki, E.; Keller, M.; Ehlers, B.; Denner, J. Immunological methods for the detection of porcine lymphotropic herpesviruses (PLHV). J. Virol. Methods 2016, 233, 72–77. [Google Scholar] [CrossRef]
- Banks, M.; Bendall, R.; Grierson, S.; Heath, G.; Mitchell, J.; Dalton, H. Human and Porcine Hepatitis E Virus Strains, United Kingdom. Emerg. Infect. Dis. 2004, 10, 953–955. [Google Scholar] [CrossRef]
- Melo, H.; Brandao, C.; Rego, G.; Nunes, R. Ethical and Legal Issues in Xenotransplantation. Bioethics 2001, 15, 427–442. [Google Scholar] [CrossRef] [PubMed]
- Anderson, M. Xenotransplantation: A bioethical evaluation. J. Med. Ethics 2006, 32, 205–208. [Google Scholar] [CrossRef] [PubMed]
- Cook, P.S. The Social Aspects of Xenotransplantation. Sociol. Compass 2013, 7, 237–254. [Google Scholar] [CrossRef]
- Cengiz, N.; Wareham, C.S. Ethical considerations in xenotransplantation: A review. Curr. Opin. Organ Transplant. 2020, 25, 483–488. [Google Scholar] [CrossRef] [PubMed]
- Ellison, T. Xenotransplantation--ethics and regulation. Xenotransplantation 2006, 13, 505–509. [Google Scholar] [CrossRef]
- Brignier, A.; Gewirtz, A. Embryonic and adult stem cell therapy. J. Allergy Clin. Immunol. 2010, 125, S336–S344. [Google Scholar] [CrossRef] [PubMed]
- Butler, J.R.; Skill, N.J.; Priestman, D.L.; Platt, F.M.; Li, P.; Estrada, J.L.; Martens, G.R.; Ladowski, J.M.; Tector, M.; Tector, A.J. Silencing the porcine iGb3s gene does not affect Galα3Gal levels or measures of anticipated pig-to-human and pig-to-primate acute rejection. Xenotransplantation 2016, 23, 106–116. [Google Scholar] [CrossRef]
- Zhang, R.; Wang, Y.; Chen, L.; Wang, R.; Li, C.; Li, X.; Fang, B.; Ren, X.; Ruan, M.; Liu, J.; et al. Reducing immunoreactivity of porcine bioprosthetic heart valves by genetically-deleting three major glycan antigens, GGTA1/β4GalNT2/CMAH. Acta Biomater. 2018, 72, 196–205. [Google Scholar] [CrossRef] [PubMed]
- Adams, A.B.; Kim, S.C.; Martens, G.R.; Ladowski, J.M.; Estrada, J.L.; Reyes, L.M.; Breeden, C.; Stephenson, A.; Eckhoff, D.E.; Tector, M.; et al. Xenoantigen deletion and chemical immunosuppression can prolong renal xenograft survival. Ann. Surg. 2018, 268, 564–573. [Google Scholar] [CrossRef] [PubMed]
- Butler, J.R.; Paris, L.L.; Blankenship, R.L.; Sidner, R.A.; Martens, G.R.; Ladowski, J.M.; Li, P.; Estrada, J.L.; Tector, M.; Joseph Tector, A. Silencing porcine CMAH and GGTA1 genes significantly reduces xenogeneic consumption of human platelets by porcine livers. Transplantation 2016, 100, 571–576. [Google Scholar] [CrossRef]
- Butler, J.R.; Martens, G.R.; Li, P.; Wang, Z.Y.; Estrada, J.L.; Ladowski, J.M.; Tector, M.; Tector, A.J. The fate of human platelets exposed to porcine renal endothelium: A single-pass model of platelet uptake in domestic and genetically modified porcine organs. J. Surg. Res. 2016, 200, 698–706. [Google Scholar] [CrossRef] [PubMed]
- Petersen, B.; Frenzel, A.; Lucas-Hahn, A.; Herrmann, D.; Hassel, P.; Klein, S.; Ziegler, M.; Hadeler, K.G.; Niemann, H. Efficient production of biallelic GGTA1 knockout pigs by cytoplasmic microinjection of CRISPR/Cas9 into zygotes. Xenotransplantation 2016, 23, 338–346. [Google Scholar] [CrossRef] [PubMed]
- Gao, H.; Zhao, C.; Xiang, X.; Li, Y.; Zhao, Y.; Li, Z.; Pan, D.; Dai, Y.; Hara, H.; Cooper, D.K.C.; et al. Production of α1,3-galactosyltransferase and cytidine monophosphate-N-acetylneuraminic acid hydroxylase gene double-deficient pigs by CRISPR/Cas9 and handmade cloning. J. Reprod. Dev. 2017, 63, 17–26. [Google Scholar] [CrossRef]
- Zhang, J.; Xie, C.; Lu, Y.; Zhou, M.; Qu, Z.; Yao, D.; Qiu, C.; Xu, J.; Pan, D.; Dai, Y.; et al. Potential Antigens Involved in Delayed Xenograft Rejection in a Ggta1/Cmah Dko Pig-to-Monkey Model. Sci. Rep. 2017, 7, 10024. [Google Scholar] [CrossRef]
- Martens, G.R.; Reyes, L.M.; Butler, J.R.; Ladowski, J.M.; Estrada, J.L.; Sidner, R.A.; Eckhoff, D.E.; Tector, M.; Tector, A.J. Humoral Reactivity of Renal Transplant-Waitlisted Patients to Cells from GGTA1/CMAH/B4GalNT2, and SLA Class i Knockout Pigs. Transplantation 2017, 101, e86–e92. [Google Scholar] [CrossRef] [PubMed]
- Wang, Z.Y.; Martens, G.R.; Blankenship, R.L.; Sidner, R.A.; Li, P.; Estrada, J.L.; Tector, M.; Tector, A.J. Eliminating xenoantigen expression on swine rbc. Transplantation 2017, 101, 517–523. [Google Scholar] [CrossRef]
- Butler, J.R.; Martens, G.R.; Estrada, J.L.; Reyes, L.M.; Ladowski, J.M.; Galli, C.; Perota, A.; Cunningham, C.M.; Tector, M.; Joseph Tector, A. Silencing porcine genes significantly reduces human-anti-pig cytotoxicity profiles: An alternative to direct complement regulation. Transgenic Res. 2016, 25, 751–759. [Google Scholar] [CrossRef] [PubMed]
- Nottle, M.B.; Salvaris, E.J.; Fisicaro, N.; McIlfatrick, S.; Vassiliev, I.; Hawthorne, W.J.; O’Connell, P.J.; Brady, J.L.; Lew, A.M.; Cowan, P.J. Targeted insertion of an anti-CD2 monoclonal antibody transgene into the GGTA1 locus in pigs using FokI-dCas9. Sci. Rep. 2017, 7, 8383. [Google Scholar] [CrossRef]
- Fu, R.; Fang, M.; Xu, K.; Ren, J.; Zou, J.; Su, L.; Chen, X.; An, P.; Yu, D.; Ka, M.; et al. Generation of GGTA1-/-β2M-/-CIITA-/- Pigs Using CRISPR/Cas9 Technology to Alleviate Xenogeneic Immune Reactions. Transplantation 2020, 104, 1566–1573. [Google Scholar] [CrossRef] [PubMed]
- Yue, Y.; Xu, W.; Kan, Y.; Zhao, H.Y.; Zhou, Y.; Song, X.; Wu, J.; Xiong, J.; Goswami, D.; Yang, M.; et al. Extensive germline genome engineering in pigs. Nat. Biomed. Eng. 2020, 5, 134–143. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Güell, M.; Niu, D.; George, H.; Lesha, E.; Grishin, D.; Aach, J.; Shrock, E.; Xu, W.; Poci, J.; et al. Genome-wide inactivation of porcine endogenous retroviruses (PERVs). Science 2015, 350, 1101–1104. [Google Scholar] [CrossRef]
- Godehardt, A.W.; Fischer, N.; Rauch, P.; Gulich, B.; Boller, K.; Church, G.M.; Tönjes, R.R. Characterization of porcine endogenous retrovirus particles released by the CRISPR/Cas9 inactivated cell line PK15 clone 15. Xenotransplantation 2019, 27, e12563. [Google Scholar] [CrossRef]
- Niu, D.; Wei, H.J.; Lin, L.; George, H.; Wang, T.; Lee, I.H.; Zhao, H.Y.; Wang, Y.; Kan, Y.; Shrock, E.; et al. Inactivation of porcine endogenous retrovirus in pigs using CRISPR-Cas9. Science 2017, 357, 1303–1307. [Google Scholar] [CrossRef] [PubMed]
- Xie, Z.; Jiao, H.; Xiao, H.; Jiang, Y.; Liu, Z.; Qi, C.; Zhao, D.; Jiao, S.; Yu, T.; Tang, X.; et al. Generation of pRSAD2 gene knock-in pig via CRISPR/Cas9 technology. Antivir. Res. 2020, 174, 104696. [Google Scholar] [CrossRef] [PubMed]
| Ortholog | Host Organism | PAM Sequence (5′→3′) | References |
|---|---|---|---|
| NmeCas9 | Neisseria meningitidis | NNNNG(A/C)TT | [38] |
| SaCas9 | Staphylococcus aureus | NNGRRT or NNNRRT | [39] |
| St1Cas9 | Streptococcus thermophilus | NNAGAA or NNAGAAW | [40] |
| ScCas9 | Streptococcus canis | NNG | [41] |
| CjCas9 | Campylobacter jejuni | NNNNACA | [42] |
| FnCas9 | Francisella novicida | YG | [43] |
| St2Cas9 | Streptococcus thermophilus | NGGNG | [44] |
| Modification | Number 1 | Occurred Repair | References | ||
|---|---|---|---|---|---|
| Alleles | Mutation Type | Length (bp) | |||
| GGTA1-KO | 1 | 1 2 | deletion deletion | −5 −7 | [75] |
| CMAH-KO | 1 | 1 2 | deletion deletion & insertion | −12 −3/+5 | |
| β4GalNT2-KO | 1 | 1 2 3 * | insertion deletion deletion | +1 −5 −12 | |
| SLA class I KO | 1 | 1 2 | deletion deletion | −276 −276 | [100] |
| 2 | 1 2 | deletion deletion | −276 −4 | ||
| GGTA1-KO | 1 | nd # | insertion | +1 | [125] |
| 2 | nd # | deletion | −4 | ||
| 3 | nd # | deletion | −7 | ||
| 4 | nd # | insertion | +1 | ||
| 5 | nd # | insertion | +1 | ||
| CMAH-KO | 1 | nd # | deletion | −5 | |
| 2 | nd # | insertion | +1 | ||
| 3 | nd # | deletion | −5 | ||
| 4 | nd # | deletion | −15 | ||
| 5 | nd # | insertion | +1 | ||
| iGb3S-KO | 1 | 1 | deletion | −2 | |
| 2 | deletion | −72 | |||
| 2 | 1 | deletion | −15 | ||
| 2 | insertion | +1 | |||
| 3 | nd # | insertion | +1 | ||
| GGTA1-KO | 1 | nd # | insertion | +1 | [149] |
| CMAH-KO | 1 | nd # | deletion | −15 | |
| GGTA1-KO | 1 | 1 | insertion | +1 | [151] |
| 2 | insertion | +421 | |||
| CMAH-KO | 1 | 1 | deletion | −103 | |
| 2 | deletion | −103 | |||
| GGTA1-KO | 1 | 1 | insertion | +1 | [150] |
| 2 | insertion | +1 | |||
| 2 | 1 | insertion | +1 | ||
| 2 | none | − | |||
| 3 | insertion | +2 | |||
| 3 | 1 | deletion | −12 | ||
| 2 | deletion | −3 | |||
| 3 | none | − | |||
| 4 | 1 | deletion & insertion | −10/+4 | ||
| 2 | insertion | +1 | |||
| 5 | 1 | deletion & insertion | −1/+3 | ||
| 2 | deletion | −4 | |||
| GGTA1-KO | 1 | nd # | insertion | +1 | [146] |
| CMAH-KO | 1 | nd # | insertion | +1 | |
| β4GalNT2-KO | 1 | nd # | deletion | −10 | |
| ULBP1-KO | 1 | 1 | deletion & insertion | −21/+2 | [85] |
| 2 | deletion & insertion | −4/+13 | |||
| 2 | 1 | deletion | −40 | ||
| 2 | deletion | −29 | |||
| 3 | 1 | deletion & insertion | −21/+1 | ||
| 2 | deletion | −27 | |||
| 4 | 1 | deletion | −29 | ||
| 2 | deletion | −34 | |||
| 5 | 1 | deletion | −29 | ||
| 2 | deletion & insertion | −18/+2 | |||
| GGTA1-KO | 1 | 1, 2 | deletion | −271 | [157] |
| β2M-KO | 1 | 1 | double deletion | −2/−11 | |
| 2 | deletion & double insertion | −6/+1, +27 | |||
| CIITA-KO | 1 | 1, 2 | double deletion & insertion | −5, −6/+4 | |
| GGTA1-KO | 1 | 1, 2 | deletion | −11 | [77] |
| CMAH-KO | 1 | 1 | insertion | +1 | |
| 2 | deletion | −3 | |||
| β4GalNT2-KO | 1 | 1 | deletion | −5 | |
| 2 | insertion | +367 | |||
| β2M-KO | 1 | 1 | deletion & transversion | −2/T→G | |
| 2 | deletion | −53 | |||
| 3 * | insertion | +279 | |||
| GGTA1-KO | 1 | 1 | deletion | −10 | [158] |
| 2 | vector insertion | − | |||
| CMAH-KO | 1 | 1 | deletion | −391 | |
| 2 | insertion | +2 | |||
| β4GalNT2-KO | 1 | 1 | deletion | −13 | |
| 2 | deletion | −13 | |||
| 3 | deletion | −14 | |||
| 4 | deletion | −14 | |||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ryczek, N.; Hryhorowicz, M.; Zeyland, J.; Lipiński, D.; Słomski, R. CRISPR/Cas Technology in Pig-to-Human Xenotransplantation Research. Int. J. Mol. Sci. 2021, 22, 3196. https://doi.org/10.3390/ijms22063196
Ryczek N, Hryhorowicz M, Zeyland J, Lipiński D, Słomski R. CRISPR/Cas Technology in Pig-to-Human Xenotransplantation Research. International Journal of Molecular Sciences. 2021; 22(6):3196. https://doi.org/10.3390/ijms22063196
Chicago/Turabian StyleRyczek, Natalia, Magdalena Hryhorowicz, Joanna Zeyland, Daniel Lipiński, and Ryszard Słomski. 2021. "CRISPR/Cas Technology in Pig-to-Human Xenotransplantation Research" International Journal of Molecular Sciences 22, no. 6: 3196. https://doi.org/10.3390/ijms22063196
APA StyleRyczek, N., Hryhorowicz, M., Zeyland, J., Lipiński, D., & Słomski, R. (2021). CRISPR/Cas Technology in Pig-to-Human Xenotransplantation Research. International Journal of Molecular Sciences, 22(6), 3196. https://doi.org/10.3390/ijms22063196







