Altered Structural Expression and Enzymatic Activity Parameters in Quiescent Ulcerative Colitis: Are These Potential Normalization Criteria?
Abstract
1. Introduction
2. Results
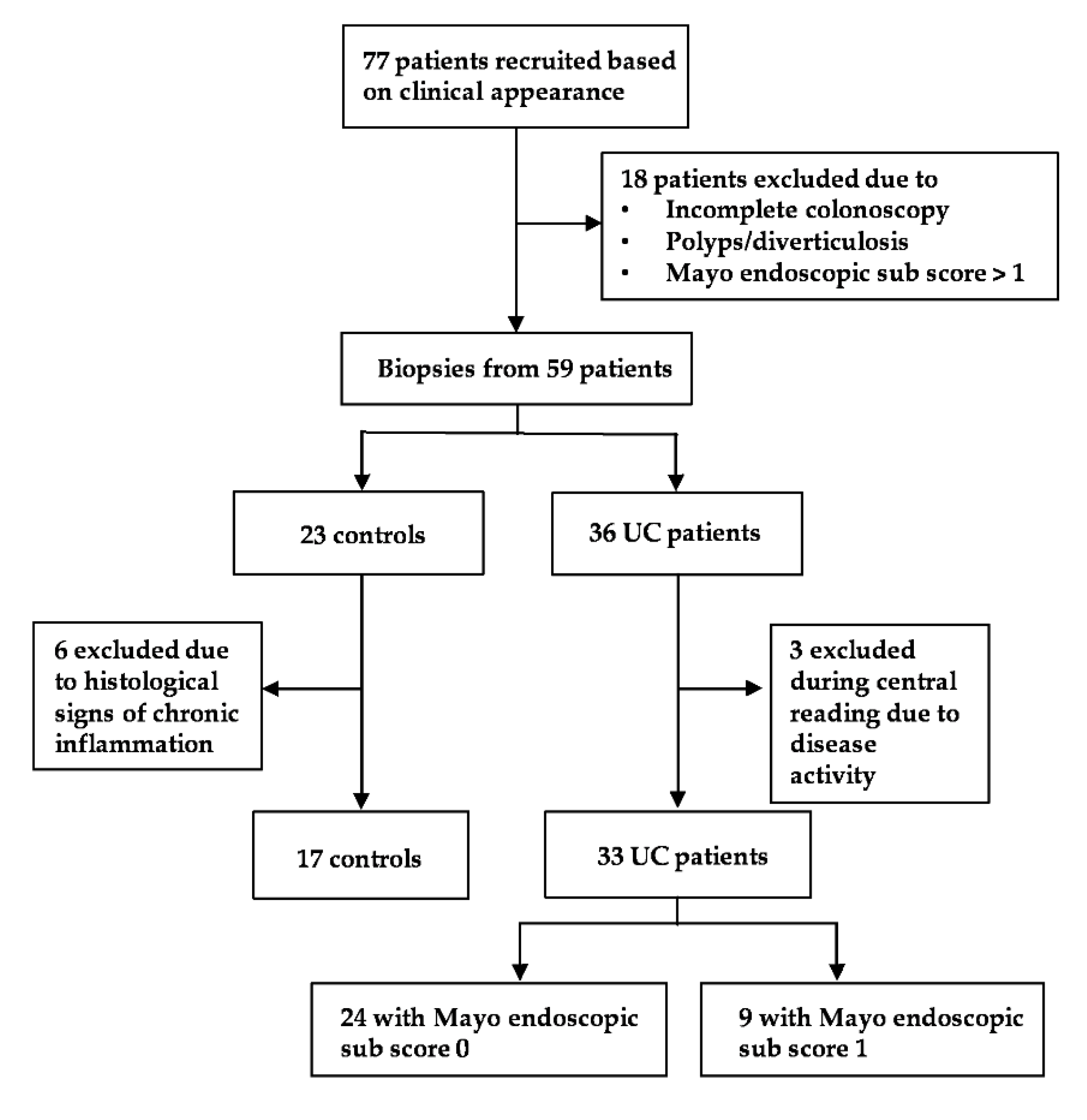
2.1. Clinical and Endoscopic Assessment
2.2. Histological Assessment
2.3. Mucosal Integrity Assessment
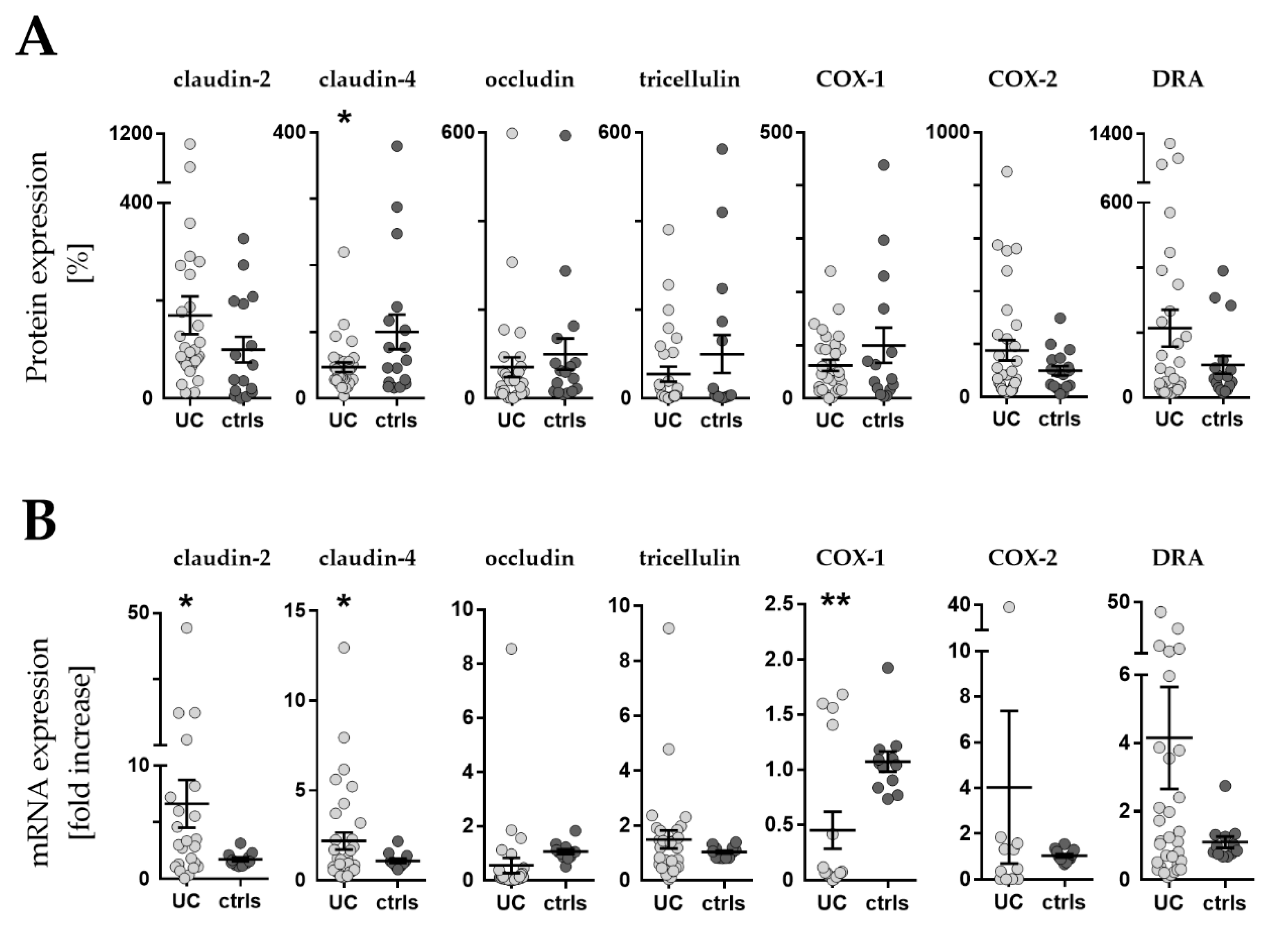
2.3.1. Protein levels
2.3.2. mRNA levels
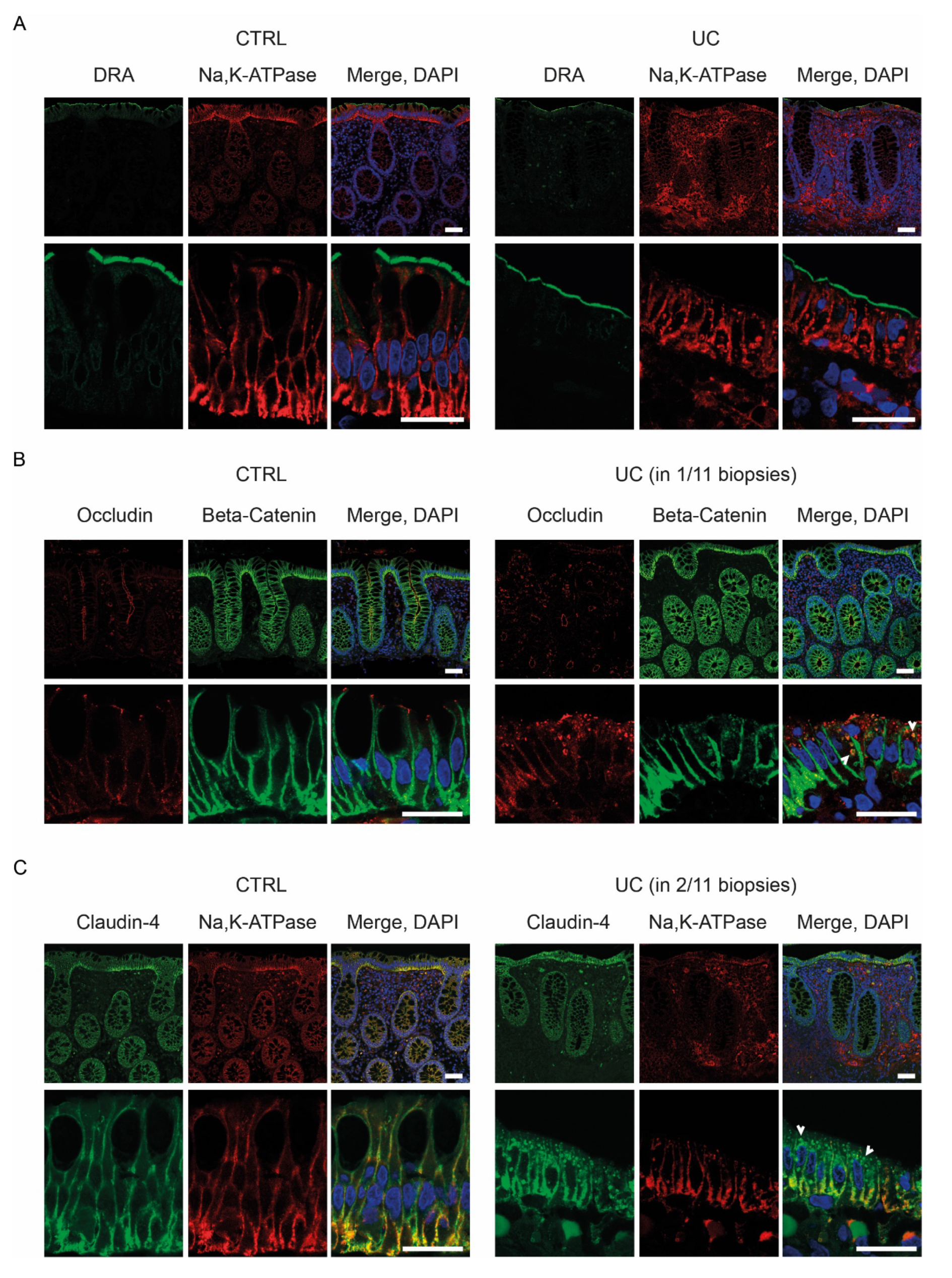
2.3.3. Protein Localization by Fluorescent Immunohistochemistry
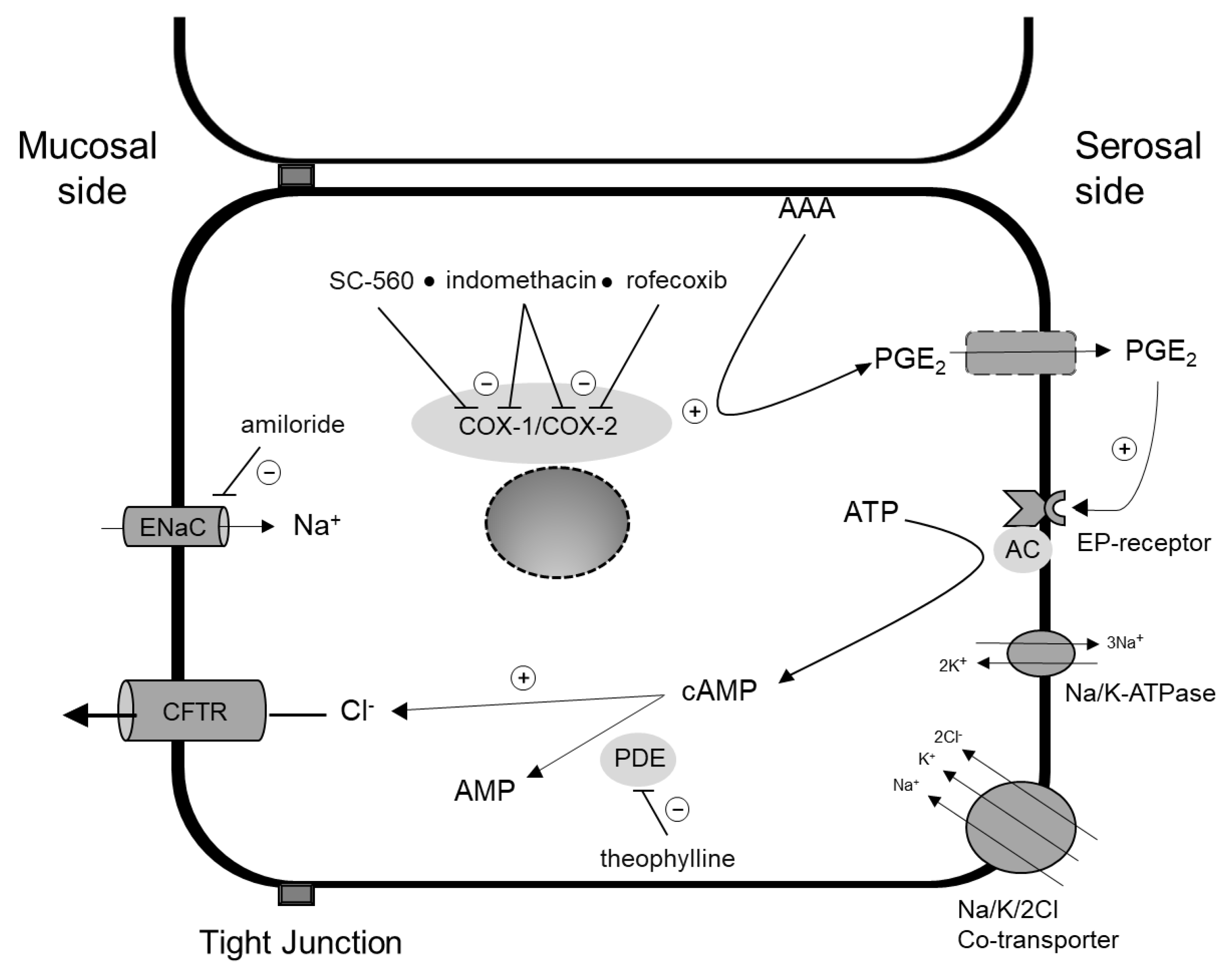
2.4. Transport Characteristics
3. Discussion
3.1. Mucosal Barrier Function
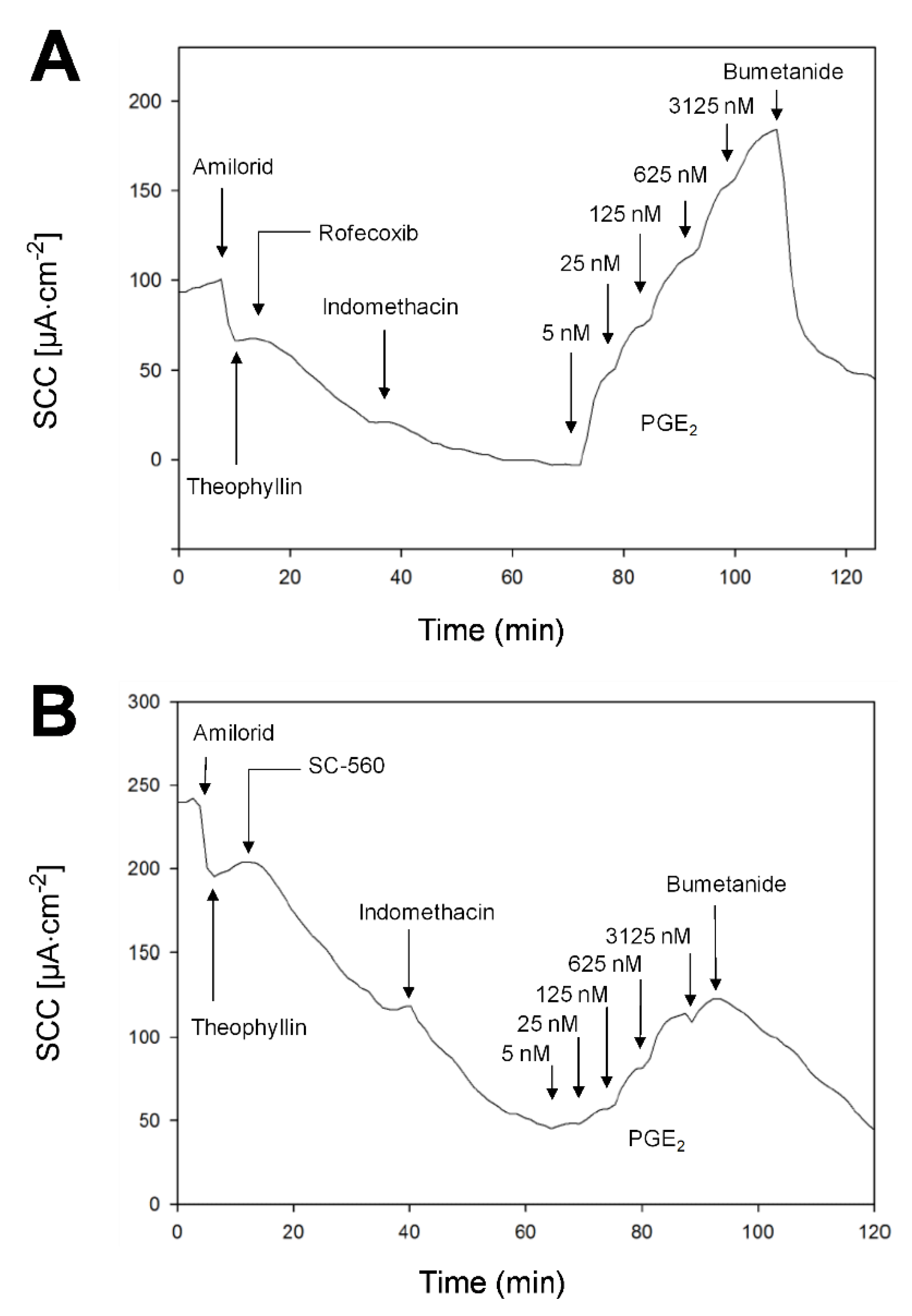
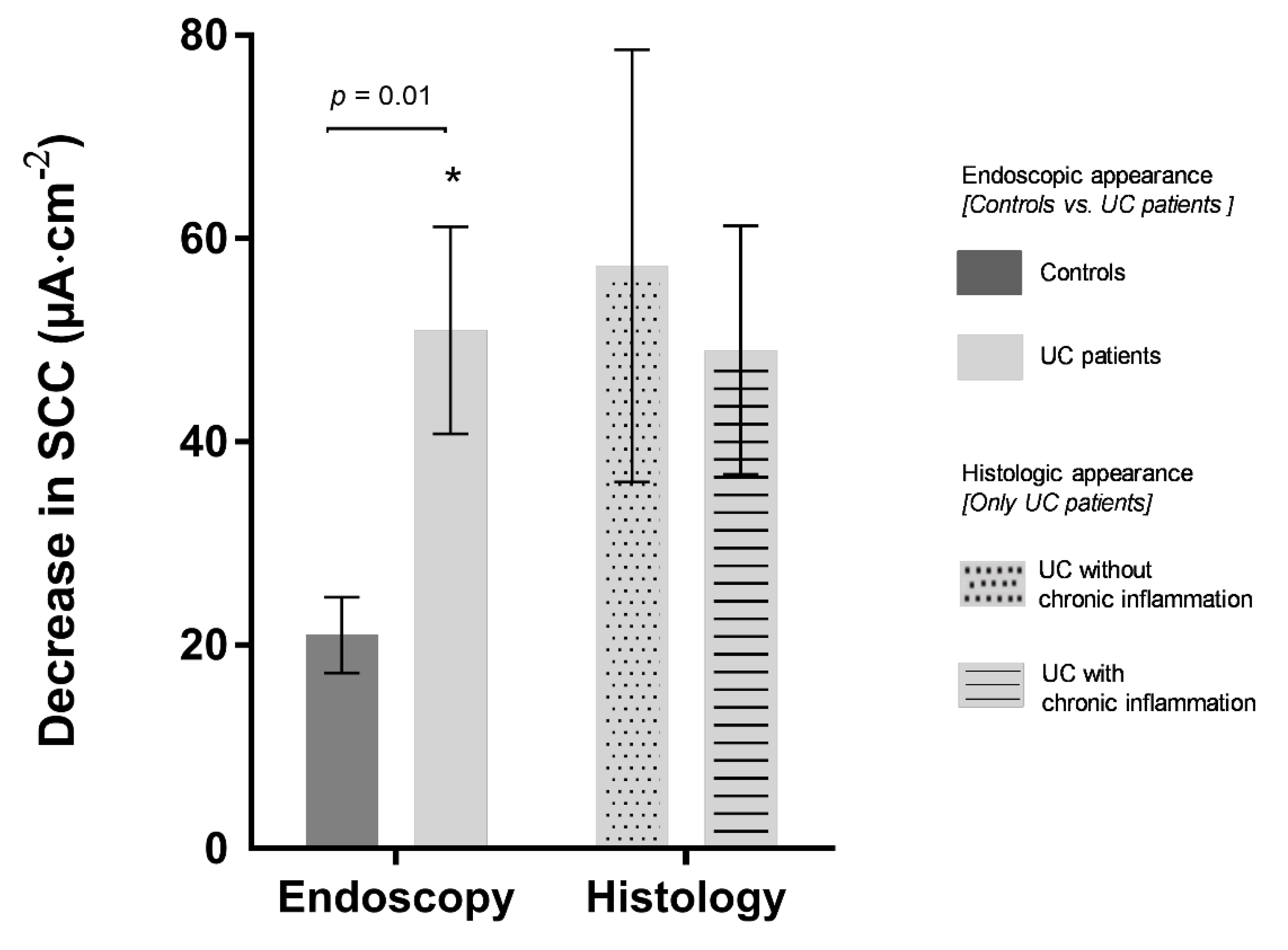
3.2. Ion Transport and COX-Enzyme Activity
3.3. Limitations of Study
3.4. Perspectives
4. Materials and Methods
4.1. Study Population
4.2. Biopsy Procedure
4.3. Chemicals, Antibodies and Primers
4.4. Study Methods
4.4.1. Clinical Assessment and Endoscopy
4.4.2. Histology
4.4.3. Mucosal Proteins and Function
Western Blot
mRNA Levels by Quantitative Real-time PCR
Protein Localization by Fluorescent Immunohistochemistry
4.4.4. Mini-Ussing-Air-Suction (MUAS) Chamber Technique
4.5. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
| cMH | Complete mucosal healing |
| COX | Cyclooxygenase |
| DRA | Downregulated-in-adenoma |
| EC50 | Half maximal effective concentration |
| ENaC | Epithelial sodium channel |
| eMH | Endoscopic mucosal healing |
| GI | Gastro-intestinal |
| hMH | Histological mucosal healing |
| IBD | Inflammatory bowel disease |
| MH | Mucosal healing |
| MUAS | Mini-Ussing-air-suction system |
| NSAID | Non-steroid anti-inflammatory drug |
| PDE | Phosphodiesterase |
| PGE2 | Prostaglandin E2 |
| qRT-PCR | Quantitative reverse transcription polymerase chain reaction |
| Rmax | Maximum response |
| SCC | Short-circuit current |
| SEM | Standard error of the mean |
| SD | Standard deviation |
| TJ | Tight junction |
| UC | Ulcerative colitis |
| WB | Western blot |
References
- Ungaro, R.; Mehandru, S.; Allen, P.B.; Peyrin-Biroulet, L.; Colombel, J.F. Ulcerative colitis. Lancet 2017, 389, 1756–1770. [Google Scholar] [CrossRef]
- Shah, S.C.; Colombel, J.F.; Sands, B.E.; Narula, N. Mucosal Healing Is Associated With Improved Long-term Outcomes of Patients With Ulcerative Colitis: A Systematic Review and Meta-analysis. Clin. Gastroenterol. Hepatol. 2016, 14, 1245–1255. [Google Scholar] [CrossRef]
- Lemmens, B.; Arijs, I.; Van Assche, G.; Sagaert, X.; Geboes, K.; Ferrante, M.; Rutgeerts, P.; Vermeire, S.; De Hertogh, G. Correlation between the endoscopic and histologic score in assessing the activity of ulcerative colitis. Inflamm. Bowel Dis. 2013, 19, 1194–1201. [Google Scholar] [CrossRef]
- Truelove, S.C.; Richards, W.C.D. Biopsy Studies in Ulcerative Colitis. Br. Med. J. 1956, 1, 1315–1319. [Google Scholar] [CrossRef]
- Riley, S.A.; Mani, V.; Goodman, M.J.; Dutt, S.; Herd, M.E. Microscopic activity in ulcerative colitis: What does it mean? Gut 1991, 32, 174–178. [Google Scholar] [CrossRef]
- Dick, A.P.; Holt, L.P.; Dalton, E.R. Persistence of mucosal abnormality in ulcerative colitis. Gut 1966, 7, 355–360. [Google Scholar] [CrossRef]
- Bessissow, T.; Lemmens, B.; Ferrante, M.; Bisschops, R.; Van Steen, K.; Geboes, K.; Van Assche, G.; Vermeire, S.; Rutgeerts, P.; De Hertogh, G. Prognostic value of serologic and histologic markers on clinical relapse in ulcerative colitis patients with mucosal healing. Am. J. Gastroenterol. 2012, 107, 1684–1692. [Google Scholar] [CrossRef]
- Bryant, R.V.; Burger, D.C.; Delo, J.; Walsh, A.J.; Thomas, S.; Von Herbay, A.; Buchel, O.C.; White, L.; Brain, O.; Keshav, S.; et al. Beyond endoscopic mucosal healing in UC: Histological remission better predicts corticosteroid use and hospitalisation over 6 years of follow-up. Gut 2016, 65, 408–414. [Google Scholar] [CrossRef]
- Christensen, B.; Hanauer, S.B.; Erlich, J.; Kassim, O.; Peter, R. Histologic Normalization Occurs in Ulcerative Colitis and Is Associated With Improved Clinical Outcomes. Clin. Gastroenterol. Hepatol. 2017, 15, 1557–1564. [Google Scholar] [CrossRef]
- Turner, J.R. Intestinal mucosal barrier function in health and disease. Nat. Rev. Immunol. 2009, 9, 799–809. [Google Scholar] [CrossRef]
- Heller, F.; Florian, P.; Bojarski, C.; Richter, J.; Christ, M.; Hillenbrand, B.; Mankertz, J.; Gitter, A.H.; Bürgel, N.; Fromm, M.; et al. Interleukin-13 is the key effector Th2 cytokine in ulcerative colitis that affects epithelial tight junctions, apoptosis, and cell restitution. Gastroenterology 2005, 129, 550–564. [Google Scholar] [CrossRef]
- Krug, S.M.; Bojarski, C.; Fromm, A.; Lee, I.M.; Dames, P.; Richter, J.F.; Turner, J.R.; Fromm, M.; Schulzke, J.-D. Tricellulin is regulated via interleukin-13-receptor α2, affects macromolecule uptake, and is decreased in ulcerative colitis. Mucosal Immunol. 2017, 11, 345–356. [Google Scholar] [CrossRef]
- Odenwald, M.A.; Turner, J.R. Intestinal Permeability Defects: Is It Time to Treat? Clin. Gastroenterol. Hepatol. 2013, 11, 1075–1083. [Google Scholar] [CrossRef]
- Nejdfors, P.; Wang, Q.; Ekelund, M.; Weström, B.R.; Jansson, O.; Lindström, C.L.; Karlsson, B.; Jeppsson, B. Increased colonic permeability in patients with ulcerative colitis: An in vitro study. Scand. J. Gastroenterol. 1998, 33, 749–753. [Google Scholar]
- Schmitz, H.; Barmeyer, C.; Fromm, M.; Runkel, N.; Foss, H.D.; Bentzel, C.J.; Riecken, E.O.; Schulzke, J.D. Altered tight junction structure contributes to the impaired epithelial barrier function in ulcerative colitis. Gastroenterology 1999, 116, 301–309. [Google Scholar] [CrossRef]
- Luettig, J.; Rosenthal, R.; Barmeyer, C.; Schulzke, J.; Luettig, J.; Rosenthal, R.; Barmeyer, C.; Schulzke, J. Claudin-2 as a mediator of leaky gut barrier during intestinal inflammation Claudin-2 as a mediator of leaky gut barrier during intestinal inflammation. Tissue Barriers 2014, 3, e977176. [Google Scholar] [CrossRef]
- Oshima, T.; Miwa, H.; Joh, T. Changes in the expression of claudins in active ulcerative colitis. J. Gastroenterol. Hepatol. 2008, 23, 146–150. [Google Scholar] [CrossRef]
- Montrose, D.C.; Nakanishi, M.; Murphy, R.C.; Zarini, S.; McAleer, J.P.; Vella, A.T.; Rosenberg, D.W. The role of PGE2 in intestinal inflammation and tumorigenesis. Prostaglandins Other Lipid Mediat. 2015, 116–117, 26–36. [Google Scholar] [CrossRef]
- Ricciotti, E.; Fitzgerald, G.A. Prostaglandins and Inflammation. Arterioscler. Thromb. Vasc. Biol. 2011, 31, 986–1000. [Google Scholar] [CrossRef]
- Vivinus-Nébot, M.; Frin-Mathy, G.; Bzioueche, H.; Dainese, R.; Bernard, G.; Anty, R.; Filippi, J.; Saint-Paul, M.C.; Tulic, M.K.; Verhasselt, V.; et al. Functional bowel symptoms in quiescent inflammatory bowel diseases: Role of epithelial barrier disruption and low-grade inflammation. Gut 2014, 63, 744–752. [Google Scholar] [CrossRef]
- Chang, J.; Leong, R.W.; Wasinger, V.C.; Ip, M.; Yang, M.; Phan, T.G. Impaired Intestinal Permeability Contributes to Ongoing Bowel Symptoms in Patients With Inflammatory Bowel Disease and Mucosal Healing. Gastroenterology 2017, 153, 723–731. [Google Scholar] [CrossRef]
- Vuitton, L.; Peyrin-Biroulet, L.; Colombel, J.F.; Pariente, B.; Pineton de Chambrun, G.; Walsh, A.J.; Panes, J.; Travis, S.P.L.; Mary, J.Y.; Marteau, P. Defining endoscopic response and remission in ulcerative colitis clinical trials: An international consensus. Aliment. Pharmacol. Ther. 2017, 45, 801–813. [Google Scholar] [CrossRef]
- Karstensen, J.G.; SǍftoiu, A.; Brynskov, J.; Hendel, J.; Klausen, P.; CârtânǍ, T.; Klausen, T.W.; Riis, L.B.; Vilmann, P. Confocal laser endomicroscopy: A novel method for prediction of relapse in Crohn’s disease. Endoscopy 2016, 48, 364–372. [Google Scholar]
- Karstensen, J.G.; Săftoiu, A.; Brynskov, J.; Hendel, J.; Ciocalteu, A.; Klausen, P.; Klausen, T.W.; Riis, L.B.; Vilmann, P. Confocal laser endomicroscopy in ulcerative colitis: A longitudinal study of endomicroscopic changes and response to medical therapy (with videos). Gastrointest. Endosc. 2016, 84, 279–286. [Google Scholar] [CrossRef]
- Binder, H.J. Mechanisms of diarrhea in inflammatory bowel diseases. Ann. N. Y. Acad. Sci. 2009, 1165, 285–293. [Google Scholar] [CrossRef]
- Schmitz, H.; Barmeyer, C.; Gittera, H.; Wullstein, F.; Bentzel, C.J.; Fromm, M.; Riecken, E.O.; Schulzke, J.D. Epithelial barrier and transport function of the colon in ulcerative colitis. Ann. N. Y. Acad. Sci. 2000, 915, 312–326. [Google Scholar] [CrossRef]
- Gustafsson, J.K.; Hansson, G.C.; Sjövall, H. Ulcerative colitis patients in remission have an altered secretory capacity in the proximal colon despite macroscopically normal mucosa. Neurogastroenterol. Motil. 2012, 24, 381–391. [Google Scholar] [CrossRef]
- Hendel, J.; Nielsen, O.H. Expression of cyclooxygenase-2 mRNA in active inflammatory bowel disease. Am. J. Gastroenterol. 1997, 92, 1170–1173. [Google Scholar]
- Sharon, P.; Ligumsky, M.; Rachmilewitz, D.; Zor, U. Role of prostaglandins in ulcerative colitis. Enhanced production during active disease and inhibition by sulfasalazine. Gastroenterology 1978, 75, 638–640. [Google Scholar] [CrossRef]
- Wang, D.; Dubois, R.N. Role of prostanoids in gastrointestinal cancer. J. Clin. Invest. 2018, 128, 2732–2742. [Google Scholar] [CrossRef]
- Pineton De Chambrun, G.; Peyrin-Biroulet, L.; Lémann, M.; Colombel, J.F. Clinical implications of mucosal healing for the management of IBD. Nat. Rev. Gastroenterol. Hepatol. 2010, 7, 15–29. [Google Scholar] [CrossRef] [PubMed]
- Ahn, H.J.; Kang, S. Can histologic remission be a better prognostic factor and therapeutic target beyond endoscopic mucosal healing in patients with ulcerative colitis? Intest. Res. 2018, 16, 1–3. [Google Scholar] [CrossRef] [PubMed]
- Peyrin-Biroulet, L.; Bressenot, A.; Kampman, W. Histologic Remission: The Ultimate Therapeutic Goal in Ulcerative Colitis? Clin. Gastroenterol. Hepatol. 2014, 12, 929–934. [Google Scholar] [CrossRef]
- Larsen, R.; Mertz-Nielsen, A.; Hansen, M.B.; Poulsen, S.S.; Bindslev, N. Novel modified Ussing chamber for the study of absorption and secretion in human endoscopic biopsies. Acta Physiol. Scand. 2001, 173, 213–222. [Google Scholar] [CrossRef]

| UC | Controls | |
|---|---|---|
| Total number | 33 | 17 |
| Males/females | 15/18 | 8/9 |
| Age, mean, years (range) | 39 (23–75) | 46 (20–68) |
| Smoking habit, active/ex-smoker/never | 2/3/28 | 0/3/14 |
| Maximum disease extent: | ||
| Proctitis | 7 | NA1 |
| Colitis 2 | 26 | |
| Disease duration, mean months (range) | 118 (3–420) 3 | NA |
| Remission duration, mean months (range) | 15 (1–61) 3 | NA |
| Mayo endoscopic sub score, 0/1 | 24/9 | NA |
| Medication: | ||
| No treatment | 8 | 3 |
| 5-ASA | 17 | 0 |
| Anti-TNFα | 6 | 0 |
| Immunosuppressants | 7 | 0 |
| Corticosteroid | 1 | 0 |
| α4β7 integrin inhibitor | 1 | 0 |
| Vitamin/iron supplements | 2 | 3 |
| Proton-pump inhibitor | 0 | 1 |
| Thiazides | 0 | 2 |
| Statins | 0 | 2 |
| Inhaler (β2-agonist, steroid) | 1 | 3 |
| Thyroid hormone | 0 | 2 |
| Antihistamine | 2 | 1 |
| Contraception | 3 | 2 |
| Anti-epileptic | 1 | 0 |
| Baseline | UC (µA · cm−2) | Controls (µA · cm−2) | p value | |||
|---|---|---|---|---|---|---|
| 107.6 ± 8.6 a | 107.5 ± 16.7 a | 0.99 | ||||
| ENaC inhibition | −35.1 ± 7.5 b | −37.2 ± 8.4 b | 0.85 | |||
| Baseline after ENaC inhibition | 70.8 ± 7.5 a | 66.0 ± 14.4 a | 0.77 | |||
| Non-specific PDE inhibition | 22.0 ± 3.7 b | 23.8 ± 5.2 b | 0.77 | |||
| COX-1 inhibition | −31.3 ± 3.8 b | −26.2 ± 4.7 b | 0.40 | |||
| COX-2 inhibition | −51.6 ± 10.5 b | −21.0 ± 3.7 b | 0.01 | |||
| PGE2 concentration response | EC50 (nM) | Rmax (µA cm−2) | EC50 (nM) | Rmax (µA cm−2) | EC50 (nM) | Rmax |
| High-affinity receptor | 14.2 ± 2.7 | 60.9 ± 5.8 | 11.0 ± 2.4 | 52.1 ± 6.9 | 0.39 | 0.34 |
| Low-affinity receptor | 588.8 ± 106.7 | 83.1 ± 11.2 | 493.2 ± 110.6 | 84.7 ± 13.4 | 0.54 | 0.93 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kjærgaard, S.; Damm, M.M.B.; Chang, J.; Riis, L.B.; Rasmussen, H.B.; Hytting-Andreasen, R.; Krug, S.M.; Schulzke, J.-D.; Bindslev, N.; Hansen, M.B. Altered Structural Expression and Enzymatic Activity Parameters in Quiescent Ulcerative Colitis: Are These Potential Normalization Criteria? Int. J. Mol. Sci. 2020, 21, 1887. https://doi.org/10.3390/ijms21051887
Kjærgaard S, Damm MMB, Chang J, Riis LB, Rasmussen HB, Hytting-Andreasen R, Krug SM, Schulzke J-D, Bindslev N, Hansen MB. Altered Structural Expression and Enzymatic Activity Parameters in Quiescent Ulcerative Colitis: Are These Potential Normalization Criteria? International Journal of Molecular Sciences. 2020; 21(5):1887. https://doi.org/10.3390/ijms21051887
Chicago/Turabian StyleKjærgaard, Sebastian, Morten M. B. Damm, Joan Chang, Lene B. Riis, Hanne B. Rasmussen, Rasmus Hytting-Andreasen, Susanne M. Krug, Jörg-Dieter Schulzke, Niels Bindslev, and Mark Berner Hansen. 2020. "Altered Structural Expression and Enzymatic Activity Parameters in Quiescent Ulcerative Colitis: Are These Potential Normalization Criteria?" International Journal of Molecular Sciences 21, no. 5: 1887. https://doi.org/10.3390/ijms21051887
APA StyleKjærgaard, S., Damm, M. M. B., Chang, J., Riis, L. B., Rasmussen, H. B., Hytting-Andreasen, R., Krug, S. M., Schulzke, J.-D., Bindslev, N., & Hansen, M. B. (2020). Altered Structural Expression and Enzymatic Activity Parameters in Quiescent Ulcerative Colitis: Are These Potential Normalization Criteria? International Journal of Molecular Sciences, 21(5), 1887. https://doi.org/10.3390/ijms21051887






