Systematic Review of Polygenic Risk Scores for Type 1 and Type 2 Diabetes
Abstract
1. Introduction
2. Methods
2.1. Search Strategies
2.2. Study Selection
2.3. Data Collection Processing
2.4. Synthesis of the Results
3. Results
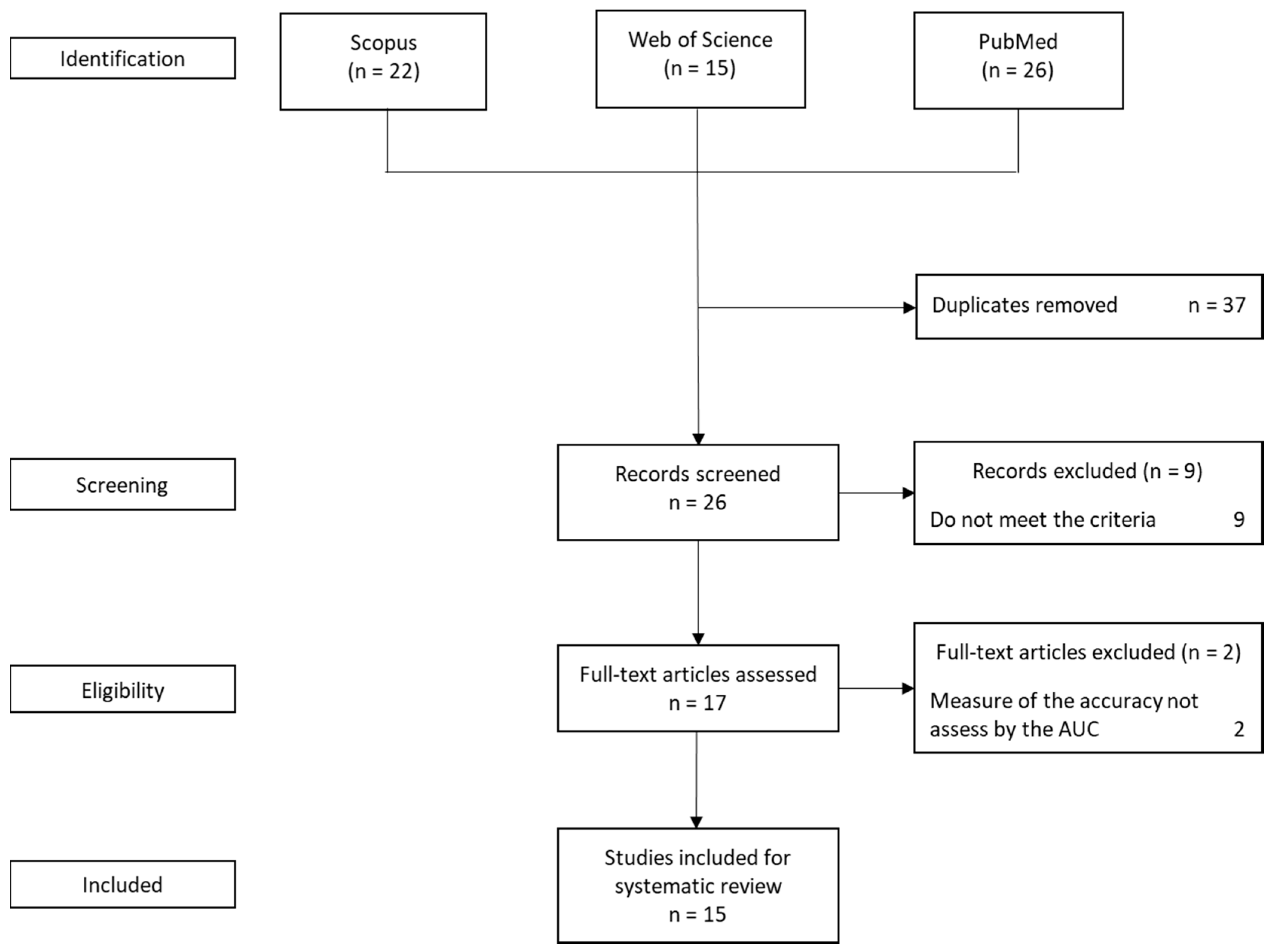
3.1. Selected Studies for the Systematic Review
3.2. Polygenic Risk Score for T1D prediction
3.3. Polygenic Risk Scores for T2D prediction
3.4. Polygenic Risk Scores to discriminate different subtypes of diabetes
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Zimmet, P.Z.; Magliano, D.J.; Herman, W.H.; Shaw, J.E. Diabetes: A 21st Century Challenge. Lancet Diabetes Endocrinol. 2014, 2, 56–64. [Google Scholar] [CrossRef]
- WHO. Available online: https://www.who.int/news-room/fact-sheets/detail/diabetes (accessed on 30 August 2019).
- Bluestone, J.A.; Herold, K.; Eisenbarth, G. Genetics, Pathogenesis and Clinical Interventions in Type\hspace0.167em1 Diabetes. Nature 2010, 464, 1293–1300. [Google Scholar]
- Kahn, S.E.; Mark, E.C.; Stefano, D.P. Pathophysiology and Treatment of Type 2 Diabetes: Perspectives on the Past, Present, and Future. Lancet 2014, 383, 1068–1083. [Google Scholar] [CrossRef]
- Boyle, J.P.; Thompson, T.J.; Gregg, E.W.; Barker, L.E.; Williamson, D.F. Projection of the Year 2050 Burden of Diabetes in the US Adult Population: Dynamic Modeling of Incidence, Mortality, and Prediabetes Prevalence. Popul. Health Metr. 2010, 8, 29. [Google Scholar] [CrossRef]
- Whiting, D.R.; Guariguata, L.; Weil, C.; Shaw, J. IDF Diabetes Atlas: Global Estimates of the Prevalence of Diabetes for 2011 and 2030. Diabetes Res. Clin. Pract. 2011, 94, 311–321. [Google Scholar] [CrossRef]
- Owen, K. Maturity-Onset Diabetes of the Young: From Clinical Description to Molecular Genetic Characterization. Best Pract. Res. Clin. Endocrinol. Metab. 2001, 15, 309–323. [Google Scholar] [CrossRef]
- Gloyn, A.L.; Ellard, S.; Shepherd, M.; Howell, R.T.; Parry, E.M.; Jefferson, A.; Levy, E.R.; Hattersley, A.T. Maturity-Onset Diabetes of the Young Caused by a Balanced Translocation Where the 20q12 Break Point Results in Disruption Upstream of the Coding Region of Hepatocyte Nuclear Factor-4 (HNF4A) Gene. Diabetes 2002, 51, 2329–2333. [Google Scholar] [CrossRef][Green Version]
- Stride, A.H.A. Different Genes, Different Diabetes: Lessons from Maturity Onset Diabetes of the Young. Ann. Med. 2002, 34, 207–216. [Google Scholar] [CrossRef]
- Mayer-Davis, E.J.; Lawrence, J.M.; Dabelea, D.; Divers, J.; Isom, S.; Dolan, L.; Imperatore, G.; Linder, B.; Marcovina, S.; Pettitt, D.J.; et al. Incidence Trends of Type 1 and Type 2 Diabetes among Youths, 2002–2012. N. Engl. J. Med. 2017, 376, 1419–1429. [Google Scholar] [CrossRef]
- Karvonen, M.; Viik-Kajander, M.; Moltchanova, E.; Libman, I.; LaPorte, R.; Tuomilehto, J. Incidence of Childhood Type 1 Diabetes Worldwide. Diabetes Mondiale (DiaMond) Project Group. Diabetes Care 2000, 23, 1516–1526. [Google Scholar] [CrossRef]
- Rawshani, A.; Rawshani, A.; Franzén, S.; Eliasson, B.; Svensson, A.-M.; Miftaraj, M.; McGuire, D.K.; Sattar, N.; Rosengren, A.; Gudbjörnsdottir, S. Mortality and Cardiovascular Disease in Type 1 and Type 2 Diabetes. N. Engl. J. Med. 2017, 376, 1407–1418. [Google Scholar] [CrossRef] [PubMed]
- Pan, C.; Shang, S.; Kirch, W.; Thoenes, M. Burden of Diabetes in the Adult Chinese Population: A Systematic Literature Review and Future Projections. Int. J. Gen. Med. 2010, 3, 173–179. [Google Scholar] [PubMed]
- Abubakari, A.R.; Lauder, W.; Jones, M.C.; Kirk, A.; Agyemang, C.; Bhopal, R.S. Prevalence and Time Trends in Diabetes and Physical Inactivity among Adult West African Populations: The Epidemic Has Arrived. Public Health 2009, 123, 602–614. [Google Scholar] [CrossRef] [PubMed]
- De Lusignan, S.; Khunti, K.; Belsey, J.; Hattersley, A.; van Vlymen, J.; Gallagher, H.; Millett, C.; Hague, N.J.; Tomson, C.; Harris, K.; et al. A Method of Identifying and Correcting Miscoding, Misclassification and Misdiagnosis in Diabetes: A Pilot and Validation Study of Routinely Collected Data. Diabet. Med. 2010, 27, 203–209. [Google Scholar] [CrossRef]
- Seidu, S.; Davies, M.J.; Mostafa, S.; de Lusignan, S.; Khunti, K. Prevalence and Characteristics in Coding, Classification and Diagnosis of Diabetes in Primary Care. Postgrad. Med. J. 2013, 90, 13–17. [Google Scholar] [CrossRef]
- Stone, M.A.; Camosso-Stefinovic, J.; Wilkinson, J.; Lusignan, S.D.; Hattersley, A.T.; Khunti, K. Incorrect and Incomplete Coding and Classification of Diabetes: A Systematic Review. Diabet. Med. 2009, 27, 491–497. [Google Scholar] [CrossRef]
- Vega, F.M.D.L.; Bustamante, C.D. Polygenic Risk Scores: A Biased Prediction? Genome Med. 2018, 10, 1–3. [Google Scholar]
- Khera, A.V.; Chaffin, M.; Aragam, K.G.; Haas, M.E.; Roselli, C.; Choi, S.H.; Natarajan, P.; Lander, E.S.; Lubitz, S.A.; Ellinor, P.T.; et al. Genome-Wide Polygenic Scores for Common Diseases Identify Individuals with Risk Equivalent to Monogenic Mutations. Nat. Genet. 2018, 50, 1219–1224. [Google Scholar] [CrossRef]
- Bycroft, C.; Freeman, C.; Petkova, D.; Band, G.; Elliott, L.T.; Sharp, K.; Motyer, A.; Vukcevic, D.; Delaneau, O.; O’Connell, J.; et al. The UK Biobank Resource with Deep Phenotyping and Genomic Data. Nature 2018, 562, 203–209. [Google Scholar] [CrossRef]
- Evangelou, E.; Warren, H.R.; Mosen-Ansorena, D.; Mifsud, B.; Pazoki, R.; Gao, H.; Ntritsos, G.; Dimou, N.; Cabrera, C.P.; Karaman, I.; et al. Genetic Analysis of over 1 Million People Identifies 535 New Loci Associated with Blood Pressure Traits. Nat. Genet. 2018, 50, 1412–1425. [Google Scholar] [CrossRef]
- Whitfield, J.B. Genetic Insights and into Cardiometabolic and Risk Factors. Clin. Biochem. Rev. 2014, 35, 15. [Google Scholar] [PubMed]
- Zeng, P. Statistical Analysis for Genome-Wide Association Study. J. Biomed. Res. 2015, 29, 285. [Google Scholar] [PubMed]
- Golan, D.; Lander, E.S.; Rosset, S. Measuring Missing Heritability: Inferring the Contribution of Common Variants. Proc. Natl. Acad. Sci. USA 2014, 111, E5272–E5281. [Google Scholar] [CrossRef] [PubMed]
- Kolb, H.; Martin, S. Environmental/Lifestyle Factors in the Pathogenesis and Prevention of Type 2 Diabetes. BMC Med. 2017, 15, 131. [Google Scholar] [CrossRef]
- Sanna, S.; van Zuydam, N.R.; Mahajan, A.; Kurilshikov, A.; Vila, A.V.; Võsa, U.; Mujagic, Z.; Masclee, A.A.M.; Jonkers, D.M.A.E.; Oosting, M.; et al. Causal Relationships among the Gut Microbiome, Short-Chain Fatty Acids and Metabolic Diseases. Nat. Genet. 2019, 51, 600–605. [Google Scholar] [CrossRef]
- Mahajan, A.; Taliun, D.; Thurner, M.; Robertson, N.R.; Torres, J.M.; Rayner, N.W.; Payne, A.J.; Steinthorsdottir, V.; Scott, R.A.; Grarup, N.; et al. Fine-Mapping Type 2 Diabetes Loci to Single-Variant Resolution Using High-Density Imputation and Islet-Specific Epigenome Maps. Nat. Genet. 2018, 50, 1505–1513. [Google Scholar] [CrossRef]
- Onengut-Gumuscu, S.; Chen, W.-M.; Burren, O.; Cooper, N.J.; Quinlan, A.R.; Mychaleckyj, J.C.; Farber, E.; Bonnie, J.K.; Szpak, M.; Schofield, E.; et al. Fine Mapping of Type 1 Diabetes Susceptibility Loci and Evidence for Colocalization of Causal Variants with Lymphoid Gene Enhancers. Nat. Genet. 2015, 47, 381–386. [Google Scholar] [CrossRef]
- Sharp, S.A.; Weedon, M.N.; Hagopian, W.A.; Oram, R.A. Clinical and Research Uses of Genetic Risk Scores in Type 1 Diabetes. Curr. Opin. Genet. Dev. 2018, 50, 96–102. [Google Scholar] [CrossRef]
- Wareham, N.J.; Herman, W.H. The Clinical and Public Health Challenges of Diabetes Prevention: A Search for Sustainable Solutions. PLoS Med. 2016, 13, e1002097. [Google Scholar] [CrossRef]
- Poulsen, P.; Kyvik, K.O.; Vaag, A.; Beck-Nielsen, H. Heritability of Type II (Non-Insulin-Dependent) Diabetes Mellitus and Abnormal Glucose Tolerance - a Population-Based Twin Study. Diabetologia 1999, 42, 139–145. [Google Scholar] [CrossRef]
- Tuomilehto, J.; Lindström, J.; Eriksson, J.G.; Valle, T.T.; Hämäläinen, H.; Ilanne-Parikka, P.; Keinänen-Kiukaanniemi, S.; Laakso, M.; Louheranta, A.; Rastas, M.; et al. Prevention of Type 2 Diabetes Mellitus by Changes in Lifestyle among Subjects with Impaired Glucose Tolerance. N. Engl. J. Med. 2001, 344, 1343–1350. [Google Scholar] [CrossRef] [PubMed]
- Almgren, P. Heritability and Familiality of Type 2 Diabetes and Related Quantitative Traits in the Botnia Study. Diabetologia 2011, 54, 2811–2819. [Google Scholar] [CrossRef] [PubMed]
- Yang, J.; Benyamin, B.; McEvoy, B.P.; Gordon, S.; Henders, A.K.; Nyholt, D.R.; Madden, P.A.; Heath, A.C.; Martin, N.G.; Montgomery, G.W.; et al. Common SNPs Explain a Large Proportion of the Heritability for Human Height. Nat. Genet. 2010, 42, 565–569. [Google Scholar] [CrossRef] [PubMed]
- Bailey, J.N.C.; Igo, R.P. Genetic Risk Scores. Curr. Protoc. Hum. Genet. 2016, 91, 1291–1299. [Google Scholar] [CrossRef]
- Lall, K.; Mägi, R.; Morris, A.; Metspalu, A.; Fischer, K. Personalized Risk Prediction for Type 2 Diabetes: The Potential of Genetic Risk Scores. Genet. Med. 2016, 19, 322–329. [Google Scholar] [CrossRef]
- Wray, N.; Yang, J.; Goddard, M.E.; Visscher, P.M. The Genetic Interpretation of Area under the ROC Curve in Genomic Profiling. PLoS Genet. 2010, 6, e1000864. [Google Scholar] [CrossRef]
- Oram, R.A.; Patel, K.; Hill, A.; Shields, B.; McDonald, T.J.; Jones, A.; Hattersley, A.T.; Weedon, M.N. A Type 1 Diabetes Genetic Risk Score Can Aid Discrimination Between Type 1 and Type 2 Diabetes in Young Adults. Diabetes Care 2015, 39, 337–344. [Google Scholar] [CrossRef]
- Patel, K.A.; Oram, R.A.; Flanagan, S.E.; Franco, E.D.; Colclough, K.; Shepherd, M.; Ellard, S.; Weedon, M.N.; Hattersley, A.T. Type 1 Diabetes Genetic Risk Score: A Novel Tool to Discriminate Monogenic and Type 1 Diabetes. Diabetes 2016, 65, 2094–2099. [Google Scholar] [CrossRef]
- Kim, M.S.; Patel, K.P.; Teng, A.K.; Berens, A.J.; Lachance, J. Genetic Disease Risks Can Be Misestimated across Global Populations. Genome Biol. 2018, 19, 1–14. [Google Scholar] [CrossRef]
- Thomas, N.J.; Jones, S.E.; Weedon, M.N.; Shields, B.M.; Oram, R.A.; Hattersley, A.T. Frequency and Phenotype of Type 1 Diabetes in the First Six Decades of Life: A Cross-Sectional, Genetically Stratified Survival Analysis from UK Biobank. Lancet Diabetes Endocrinol. 2018, 6, 122–129. [Google Scholar] [CrossRef]
- Winkler, C.; Krumsiek, J.; Buettner, F.; Angermüller, C.; Giannopoulou, E.Z.; Theis, F.J.; Ziegler, A.-G.; Bonifacio, E. Feature Ranking of Type 1 Diabetes Susceptibility Genes Improves Prediction of Type 1 Diabetes. Diabetologia 2014, 57, 2521–2529. [Google Scholar] [CrossRef] [PubMed]
- Perry, D.J.; Wasserfall, C.H.; Oram, R.A.; Williams, M.D.; Posgai, A.; Muir, A.B.; Haller, M.J.; Schatz, D.A.; Wallet, M.A.; Mathews, C.E.; et al. Application of a Genetic Risk Score to Racially Diverse Type 1 Diabetes Populations Demonstrates the Need for Diversity in Risk-Modeling. Sci. Rep. 2018, 8, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Sharp, S.A.; Rich, S.S.; Wood, A.R.; Jones, S.E.; Beaumont, R.N.; Harrison, J.W.; Schneider, D.A.; Locke, J.M.; Tyrrell, J.; Weedon, M.N.; et al. Development and Standardization of an Improved Type 1 Diabetes Genetic Risk Score for Use in Newborn Screening and Incident Diagnosis. Diabetes Care 2019, 42, 200–207. [Google Scholar]
- Yaghootkar, H.; Abbasi, F.; Ghaemi, N.; Rabbani, A.; Wakeling, M.N.; Eshraghi, P.; Enayati, S.; Vakili, S.; Heidari, S.; Patel, K.; et al. Type 1 Diabetes Genetic Risk Score Discriminates between Monogenic and Type 1 Diabetes in Children Diagnosed at the Age of Less of 5 Years in the Iranian Population. Diabet. Med. 2019, 36, 1694–1702. [Google Scholar] [CrossRef] [PubMed]
- Weedon, M.N.; McCarthy, M.I.; Hitman, G.; Walker, M.; Groves, C.J.; Zeggini, E.; Rayner, N.W.; Shields, B.; Owen, K.R.; Hattersley, A.T.; et al. Combining Information from Common Type 2 Diabetes Risk Polymorphisms Improves Disease Prediction. PLoS Med. 2006, 3, e374. [Google Scholar] [CrossRef]
- Lango, H.; Palmer, C.N.A.; Morris, A.D.; Zeggini, E.; Hattersley, A.T.; McCarthy, M.I.; Frayling, T.M.; Weedon, M.N. Assessing the Combined Impact of 18 Common Genetic Variants of Modest Effect Sizes on Type 2 Diabetes Risk. Diabetes 2008, 57, 3129–3135. [Google Scholar] [CrossRef]
- Lyssenko, V.; Jonsson, A.; Almgren, P.; Pulizzi, N.; Isomaa, B.; Tuomi, T.; Berglund, G.; Altshuler, D.; Nilsson, P.; Groop, L. Clinical Risk Factors, DNA Variants, and the Development of Type 2 Diabetes. N. Engl. J. Med. 2008, 359, 2220–2232. [Google Scholar] [CrossRef]
- Meigs, J.B.; Shrader, P.; Sullivan, L.M.; McAteer, J.B.; Fox, C.S.; Dupuis, J.; Manning, A.K.; Florez, J.C.; Wilson, P.W.F.; D’Agostino, R.B.; et al. Genotype Score in Addition to Common Risk Factors for Prediction of Type 2 Diabetes. N. Engl. J. Med. 2008, 359, 2208–2219. [Google Scholar] [CrossRef]
- Chatterjee, N.; Wheeler, B.; Sampson, J.; Hartge, P.; Chanock, S.J.; Park, J.-H. Projecting the Performance of Risk Prediction Based on Polygenic Analyses of Genome-Wide Association Studies. Nat. Genet. 2013, 45, 400–405. [Google Scholar] [CrossRef]
- Vassy, J.L.; Hivert, M.-F.; Porneala, B.; Dauriz, M.; Florez, J.C.; Dupuis, J.; Siscovick, D.S.; Fornage, M.; Rasmussen-Torvik, L.J.; Bouchard, C.; et al. Polygenic Type 2 Diabetes Prediction at the Limit of Common Variant Detection. Diabetes 2014, 63, 2172–2182. [Google Scholar] [CrossRef]
- Bramer, W.M.; Rethlefsen, M.L.; Kleijnen, J.; Franco, O.H. Optimal Database Combinations for Literature Searches in Systematic Reviews: A Prospective Exploratory Study. Syst. Rev. 2017, 6, 245. [Google Scholar] [CrossRef] [PubMed]
- Little, J.; Higgins, J.P.T.; Ioannidis, J.P.A.; Moher, D.; Gagnon, F.; von Elm, E.; Khoury, M.J.; Cohen, B.; Davey-Smith, G.; Grimshaw, J.; et al. STrengthening the REporting of Genetic Association Studies (STREGA)-an Extension of the STROBE Statement. Genet. Epidemiol. 2009, 33, 581–598. [Google Scholar] [CrossRef] [PubMed]
- Chikowore, T.; van Zyl, T.; Feskens, E.J.M.; Conradie, K.R. Predictive Utility of a Genetic Risk Score of Common Variants Associated with Type 2 Diabetes in a Black South African Population. Diabetes Res. Clin. Pract. 2016, 122, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Rich, S.S.; Akolkar, B.; Concannon, P.; Erlich, H.; Hilner, J.E.; Julier, C.; Morahan, G.; Nerup, J.; Nierras, C.; Pociot, F.; et al. Overview of the Type I Diabetes Genetics Consortium. Genes Immun. 2009, 10, S1–S4. [Google Scholar] [CrossRef] [PubMed]
- Devuyst, O. The 1000 Genomes Project: Welcome to a New World. Perit. Dial. Int. 2015, 35, 676–677. [Google Scholar] [CrossRef] [PubMed]
- Chikowore, T.; Conradie, K.R.; Towers, G.W.; van Zyl, T. Common Variants Associated with Type 2 Diabetes in a Black South African Population of Setswana Descent: African Populations Diverge. OMICS: A J. Integr. Biol. 2015, 19, 617–626. [Google Scholar] [CrossRef]
- Morris, A.D.; Boyle, D.I.; MacAlpine, R.; Emslie-Smith, A.; Jung, R.T.; Newton, R.W.; MacDonald, T.M. The Diabetes Audit and Research in Tayside Scotland (Darts) Study: Electronic Record Linkage to Create a Diabetes Register. BMJ 1997, 315, 524–528. [Google Scholar] [CrossRef]
- Eriksson, K.-F.; Lindgarde, F. Prevention of Type 2 (Non-Insulin-Dependent) Diabetes Mellitus by Diet and Physical Exercise The 6-Year Malmö Feasibility Study. Diabetologia 1991, 34, 891–898. [Google Scholar] [CrossRef]
- Groop, L.; Forsblom, C.; Lehtovirta, M.; Tuomi, T.; Karanko, S.; Nissen, M.; Ehrnstrom, B.-O.; Forsen, B.; Isomaa, B.; Snickars, B.; et al. Metabolic Consequences of a Family History of NIDDM (The Botnia Study): Evidence for Sex-Specific Parental Effects. Diabetes 1996, 45, 1585–1593. [Google Scholar] [CrossRef]
- Feinleib, M.; Kannel, W.B.; Garrison, R.J.; McNamara, P.M.; Castelli, W.P. The Framingham Offspring Study. Design and Preliminary Data. Prev. Med. 1975, 4, 518–525. [Google Scholar] [CrossRef]
- Voight, B.F.; Scott, L.J.; Steinthorsdottir, V.; Morris, A.P.; Dina, C.; Welch, R.P.; Zeggini, E.; Huth, C.; Aulchenko, Y.S.; Thorleifsson, G.; et al. Twelve Type 2 Diabetes Susceptibility Loci Identified through Large-Scale Association Analysis. Nat. Genet. 2010, 42, 579–589. [Google Scholar] [CrossRef] [PubMed]
- Friedman, G.D.; Cutter, G.R.; Donahue, R.P.; Hughes, G.H.; Hulley, S.B.; Jacobs, D.R.; Liu, K.; Savage, P.J. Cardia: Study Design, Recruitment, and Some Characteristics of the Examined Subjects. J. Clin. Epidemiol. 1988, 41, 1105–1116. [Google Scholar] [CrossRef]
- Leitsalu, L.; Haller, T.; Esko, T.; Tammesoo, M.-L.; Alavere, H.; Snieder, H.; Perola, M.; Ng, P.C.; Mägi, R.; Milani, L.; et al. Cohort Profile: Estonian Biobank of the Estonian Genome Center, University of Tartu. Int. J. Epidemiol. 2015, 44, 1137–1147. [Google Scholar] [CrossRef] [PubMed]
- Sudlow, C.; Gallacher, J.; Allen, N.; Beral, V.; Burton, P.; Danesh, J.; Downey, P.; Elliott, P.; Green, J.; Landray, M.; et al. UK Biobank: An Open Access Resource for Identifying the Causes of a Wide Range of Complex Diseases of Middle and Old Age. PLoS Med. 2015, 12, e1001779. [Google Scholar] [CrossRef]
- Frayling, T.M. Genome–Wide Association Studies Provide New Insights into Type 2 Diabetes Aetiology. Nat. Rev. Genet. 2007, 8, 657–662. [Google Scholar] [CrossRef]
- Zeggini, E.; Scott, L.J.; Saxena, R.; Voight, B.F.; Marchini, J.L.; Hu, T.; de Bakker, P.I.; Abecasis, G.R.; Almgren, P.; Andersen, G.; et al. Meta-Analysis of Genome-Wide Association Data and Large-Scale Replication Identifies Additional Susceptibility Loci for Type 2 Diabetes. Nat. Genet. 2008, 40, 638–645. [Google Scholar] [CrossRef]
- Gloyn, A.L.; Weedon, M.N.; Owen, K.R.; Turner, M.J.; Knight, B.A.; Hitman, G.; Walker, M.; Levy, J.C.; Sampson, M.; Halford, S.; et al. Large-Scale Association Studies of Variants in Genes Encoding the Pancreatic -Cell KATP Channel Subunits Kir6.2 (KCNJ11) and SUR1 (ABCC8) Confirm That the KCNJ11 E23K Variant Is Associated With Type 2 Diabetes. Diabetes 2003, 52, 568–572. [Google Scholar] [CrossRef]
- Grant, S.F.A.; Thorleifsson, G.; Reynisdottir, I.; Benediktsson, R.; Manolescu, A.; Sainz, J.; Helgason, A.; Stefansson, H.; Emilsson, V.; Helgadottir, A.; et al. Variant of Transcription Factor 7-like 2 (TCF7L2) Gene Confers Risk of Type 2 Diabetes. Nat. Genet. 2006, 38, 320–323. [Google Scholar] [CrossRef]
- Saxena, R.; Voight, B.F.; Lyssenko, V.; Burtt, N.P.; de Bakker, P.I.W.; Chen, H.; Roix, J.J.; Kathiresan, S.; Hirschhorn, J.N.; Daly, M.J.; et al. Genome-Wide Association Analysis Identifies Loci for Type 2 Diabetes and Triglyceride Levels. Science 2007, 316, 1331–1336. [Google Scholar]
- Scott, L.J.; Mohlke, K.L.; Bonnycastle, L.L.; Willer, C.J.; Li, Y.; Duren, W.L.; Erdos, M.R.; Stringham, H.M.; Chines, P.S.; Jackson, A.U.; et al. A Genome-Wide Association Study of Type 2 Diabetes in Finns Detects Multiple Susceptibility Variants. Science 2007, 316, 1341–1345. [Google Scholar] [CrossRef]
- Sladek, R.; Rocheleau, G.; Rung, J.; Dina, C.; Shen, L.; Serre, D.; Boutin, P.; Vincent, D.; Belisle, A.; Hadjadj, S.; et al. A Genome-Wide Association Study Identifies Novel Risk Loci for Type 2 Diabetes. Nature 2007, 445, 881–885. [Google Scholar] [CrossRef] [PubMed]
- Steinthorsdottir, V.; Thorleifsson, G.; Reynisdottir, I.; Benediktsson, R.; Jonsdottir, T.; Walters, G.B.; Styrkarsdottir, U.; Gretarsdottir, S.; Emilsson, V.; Ghosh, S.; et al. A Variant in CDKAL1 Influences Insulin Response and Risk of Type 2 Diabetes. Nat. Genet. 2007, 39, 770–775. [Google Scholar] [CrossRef] [PubMed]
- Zeggini, E.; Weedon, M.N.; Lindgren, C.M.; Frayling, T.M.; Elliott, K.S.; Lango, H.; Timpson, N.J.; Perry, J.R.B.; Rayner, N.W.; Freathy, R.M.; et al. Replication of Genome-Wide Association Signals in UK Samples Reveals Risk Loci for Type 2 Diabetes. Science 2007, 316, 1336–1341. [Google Scholar] [CrossRef] [PubMed]
- Lyssenko, V.; Almgren, P.; Anevski, D.; Orho-Melander, M.; Sjögren, M.; Saloranta, C.; Tuomi, T.; Groop, L.; the Botnia Study Group. Genetic Prediction of Future Type 2 Diabetes. PLoS Med. 2005, 2, e345. [Google Scholar] [CrossRef]
- DIAbetes Genetics Replication And Meta-analysis (DIAGRAM) Consortium; Asian Genetic Epidemiology Network Type 2 Diabetes (AGEN-T2D) Consortium; South Asian Type 2 Diabetes (SAT2D) Consortium; Mexican American Type 2 Diabetes (MAT2D) Consortium; Type 2 Diabetes Genetic Exploration by Next-generation sequencing in multi-Ethnic Samples (T2D-GENES) Consortium; Mahajan, A.; Go, M.J.; Zhang, W.; Below, J.E.; Gaulton, K.J.; et al. Genome-Wide Trans-Ancestry Meta-Analysis Provides Insight into the Genetic Architecture of Type 2 Diabetes Susceptibility. Nat. Genet. 2014, 46, 234–244. [Google Scholar] [CrossRef]
- Redondo, M.J.; Jeffrey, J.; Fain, P.R.; Eisenbarth, G.S.; Orban, T. Concordance for Islet Autoimmunity among Monozygotic Twins. N. Engl. J. Med. 2008, 359, 2849–2850. [Google Scholar] [CrossRef]
- Kuo, C.-F.; Chou, I.-J.; Grainge, M.; Luo, S.-F.; See, L.-C.; Yu, K.-H.; Zhang, W.; Doherty, M.; Valdes, A. Familial Aggregation and Heritability of Type 1 Diabetes Mellitus and Coaggregation of Chronic Diseases in Affected Families. Clin. Epidemiol. 2018, 10, 1447–1455. [Google Scholar] [CrossRef]
- Gale, E.A.M. The Rise of Childhood Type 1 Diabetes in the 20th Century. Diabetes 2014, 51, 3353–3361. [Google Scholar] [CrossRef]
- Noble, J.A. Immunogenetics of Type 1 Diabetes: A Comprehensive Review. J. Autoimmun. 2015, 64, 101–112. [Google Scholar] [CrossRef]
- Roshandel, D.; Gubitosi-Klug, R.; Bull, S.B.; Canty, A.J.; Pezzolesi, M.G.; King, G.L.; Keenan, H.A.; Snell-Bergeon, J.K.; Maahs, D.M.; Klein, R.; et al. Meta-Genome-Wide Association Studies Identify a Locus on Chromosome 1 and Multiple Variants in the MHC Region for Serum C-Peptide in Type 1 Diabetes. Diabetologia 2018, 61, 1098–1111. [Google Scholar] [CrossRef]
- Baschal, E.E.; Baker, P.R.; Eyring, K.R.; Siebert, J.C.; Jasinski, J.M.; Eisenbarth, G.S. The HLA-B\ast3906 Allele Imparts a High Risk of Diabetes Only on Specific HLA-DR/DQ Haplotypes. Diabetologia 2011, 54, 1702–1709. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Noble, J.A.; Valdes, A.M.; Varney, M.D.; Carlson, J.A.; Moonsamy, P.; Fear, A.L.; Lane, J.A.; Lavant, E.; Rappner, R.; Louey, A.; et al. HLA Class I and Genetic Susceptibility to Type 1 Diabetes: Results From the Type 1 Diabetes Genetics Consortium. Diabetes 2010, 59, 2972–2979. [Google Scholar] [CrossRef] [PubMed]
- Barrett, J.C.; Clayton, D.G.; Concannon, P.; Akolkar, B.; Cooper, J.D.; Erlich, H.A.; Julier, C.; Morahan, G.; Nerup, J.; Nierras, C.; et al. Genome-Wide Association Study and Meta-Analysis Find That over 40 Loci Affect Risk of Type 1 Diabetes. Nat. Genet. 2009, 41, 703–707. [Google Scholar] [CrossRef] [PubMed]
- Pociot, F. Type 1 Diabetes Genome-Wide Association Studies: Not to Be Lost in Translation. Clin. Transl. Immunol. 2017, 6, e162. [Google Scholar] [CrossRef]
- Aly, T.A.; Ide, A.; Jahromi, M.M.; Barker, J.M.; Fernando, M.S.; Babu, S.R.; Yu, L.; Miao, D.; Erlich, H.A.; Fain, P.R.; et al. Extreme Genetic Risk for Type 1A Diabetes. Proc. Natl. Acad. Sci. USA 2006, 103, 14074–14079. [Google Scholar] [CrossRef]
- Knowler, W. Reduction in the Incidence of Type 2 Diabetes with Lifestyle Intervention or Metformin. N. Engl. J. Med. 2002, 346, 393–403. [Google Scholar]
- Lindstrom, J.; Louheranta, A.; Mannelin, M.; Rastas, M.; Salminen, V.; Eriksson, J.; Uusitupa, M.; Tuomilehto, J. The Finnish Diabetes Prevention Study (DPS): Lifestyle Intervention and 3-Year Results on Diet and Physical Activity. Diabetes Care 2003, 26, 3230–3236. [Google Scholar] [CrossRef]
- Morris, A. Large-Scale Association Analysis Provides Insights into the Genetic Architecture and Pathophysiology of Type 2 Diabetes. Nat. Genet. 2012, 44, 981–990. [Google Scholar]
- Fuchsberger, C.; Flannick, J.; Teslovich, T.M.; Mahajan, A.; Agarwala, V.; Gaulton, K.J.; Ma, C.; Fontanillas, P.; Moutsianas, L.; McCarthy, D.J.; et al. The Genetic Architecture of Type 2 Diabetes. Nature 2016, 536, 41–47. [Google Scholar] [CrossRef]
- Scott, R.A.; Scott, L.J.; Mägi, R.; Marullo, L.; Gaulton, K.J.; Kaakinen, M.; Pervjakova, N.; Pers, T.H.; Johnson, A.D.; Eicher, J.D.; et al. An Expanded Genome-Wide Association Study of Type 2 Diabetes in Europeans. Diabetes 2017, 66, 2888–2902. [Google Scholar] [CrossRef]
- Wray, N.; Yang, J.; Hayes, B.J.; Price, A.L.; Goddard, M.E.; Visscher, P.M. Pitfalls of Predicting Complex Traits from SNPs. Nat. Rev. Genet. 2013, 14, 507–515. [Google Scholar] [CrossRef] [PubMed]
- Lyssenko, V.; Laakso, M. Genetic Screening for the Risk of Type 2 Diabetes: Worthless or Valuable? Diabetes Care 2013, 36, S120–S126. [Google Scholar] [CrossRef] [PubMed]
- Hope, S.V.; Wienand-Barnett, S.; Shepherd, M.; King, S.M.; Fox, C.; Khunti, K.; Oram, R.A.; Knight, B.A.; Hattersley, A.T.; Jones, A.G.; et al. Practical Classification Guidelines for Diabetes in Patients Treated with Insulin: A Cross-Sectional Study of the Accuracy of Diabetes Diagnosis. Br. J. Gen. Pract. 2016, 66, e315–e322. [Google Scholar] [CrossRef] [PubMed]
- Pearson, E.R.; Starkey, B.J.; Powell, R.J.; Gribble, F.M.; Clark, P.M.; Hattersley, A.T. Genetic Cause of Hyperglycaemia and Response to Treatment in Diabetes. Lancet 2003, 362, 1275–1281. [Google Scholar] [CrossRef]
- Pearson, E.R.; Flechtner, I.; Njølstad, P.R.; Malecki, M.T.; Flanagan, S.E.; Larkin, B.; Ashcroft, F.M.; Klimes, I.; Codner, E.; Iotova, V.; et al. Switching from Insulin to Oral Sulfonylureas in Patients with Diabetes Due to Kir6.2 Mutations. N. Engl. J. Med. 2006, 355, 467–477. [Google Scholar] [CrossRef]
- Bonifacio, E.; Beyerlein, A.; Hippich, M.; Winkler, C.; Vehik, K.; Weedon, M.N.; Laimighofer, M.; Hattersley, A.T.; Krumsiek, J.; Frohnert, B.I.; et al. Genetic Scores to Stratify Risk of Developing Multiple Islet Autoantibodies and Type 1 Diabetes: A Prospective Study in Children. PLoS Med. 2018, 15, e1002548. [Google Scholar] [CrossRef]
- Ashley, E.A.; Butte, A.J.; Wheeler, M.T.; Chen, R.; Klein, T.E.; Dewey, F.E.; Dudley, J.T.; Ormond, K.E.; Pavlovic, A.; Morgan, A.A.; et al. Clinical Assessment Incorporating a Personal Genome. Lancet 2010, 375, 1525–1535. [Google Scholar] [CrossRef]
- Manolio, T.A. Bringing Genome-Wide Association Findings into Clinical Use. Nat. Rev. Genet. 2013, 14, 549–558. [Google Scholar] [CrossRef]
- Shmueli, G. To Explain or To Predict? SSRN Electron. J. 2010, 25, 289–310. [Google Scholar]
- Wei, Z.; Wang, K.; Qu, H.-Q.; Zhang, H.; Bradfield, J.; Kim, C.; Frackleton, E.; Hou, C.; Glessner, J.T.; Chiavacci, R.; et al. From Disease Association to Risk Assessment: An Optimistic View from Genome-Wide Association Studies on Type 1 Diabetes. PLoS Genet. 2009, 5, e1000678. [Google Scholar] [CrossRef]
- Abraham, G.; Inouye, M. Genomic Risk Prediction of Complex Human Disease and Its Clinical Application. Curr. Opin. Genet. Dev. 2015, 33, 10–16. [Google Scholar] [CrossRef] [PubMed]
- Dasgupta, A.; Sun, Y.V.; König, I.R.; Bailey-Wilson, J.E.; Malley, J.D. Brief Review of Regression-Based and Machine Learning Methods in Genetic Epidemiology: The Genetic Analysis Workshop 17 Experience. Genet. Epidemiol. 2011, 35, S5–S11. [Google Scholar] [CrossRef] [PubMed]
- Okser, S.; Pahikkala, T.; Airola, A.; Salakoski, T.; Ripatti, S.; Aittokallio, T. Regularized Machine Learning in the Genetic Prediction of Complex Traits. PLoS Genet. 2014, 10, e1004754. [Google Scholar] [CrossRef] [PubMed]
- Mehta, P.; Bukov, M.; Wang, C.-H.; Day, A.G.R.; Richardson, C.; Fisher, C.K.; Schwab, D.J. A High-Bias, Low-Variance Introduction to Machine Learning for Physicists. Phys. Rep. 2019, 810, 1–124. [Google Scholar] [CrossRef]
- Cruz, J.A.; Wishart, D.S. Applications of Machine Learning in Cancer Prediction and Prognosis. Cancer Inform. 2006, 2, 117693510600200. [Google Scholar] [CrossRef]
- Palaniappan, S.; Awang, R. Intelligent Heart Disease Prediction System Using Data Mining Techniques. In Proceedings of the 2008 IEEE/ACS International Conference on Computer Systems and Applications, Doha, Qatar, 31 March–4 April 2008. [Google Scholar]
- Yu, W.; Liu, T.; Valdez, R.; Gwinn, M.; Khoury, M.J. Application of Support Vector Machine Modeling for Prediction of Common Diseases: The Case of Diabetes and Pre-Diabetes. BMC Med. Inform. Decis. Mak. 2010, 10, 16. [Google Scholar] [CrossRef]
- Zhang, D.; Shen, D. Multi-Modal Multi-Task Learning for Joint Prediction of Multiple Regression and Classification Variables in Alzheimer\textquotesingles Disease. NeuroImage 2012, 59, 895–907. [Google Scholar] [CrossRef]
- Paré, G.; Mao, S.; Deng, W.Q. A Machine-Learning Heuristic to Improve Gene Score Prediction of Polygenic Traits. Sci. Rep. 2017, 7, 12665. [Google Scholar] [CrossRef]
- Choi, S.W.; Mak, T.S.H.; O’Reilly, P.F. A Guide to Performing Polygenic Risk Score Analyses. BioRxiv 2018. [Google Scholar] [CrossRef]
- Reisberg, S.; Iljasenko, T.; Läll, K.; Fischer, K.; Vilo, J. Comparing Distributions of Polygenic Risk Scores of Type 2 Diabetes and Coronary Heart Disease within Different Populations. PLoS ONE 2017, 12, e0179238. [Google Scholar] [CrossRef]
- Dick, D.M. Gene-Environment Interaction in Psychological Traits and Disorders. Annu. Rev. Clin. Psychol. 2011, 7, 383–409. [Google Scholar] [CrossRef] [PubMed]
- Franks, P.W. Gene × Environment Interactions in Type 2 Diabetes. Curr. Diabetes Rep. 2011, 11, 552–561. [Google Scholar] [CrossRef] [PubMed]
- Thomas, D. Gene–Environment-Wide Association Studies: Emerging Approaches. Nat. Rev. Genet. 2010, 11, 259–272. [Google Scholar] [CrossRef] [PubMed]
- Boffetta, P.; Winn, D.M.; Ioannidis, J.P.; Thomas, D.C.; Little, J.; Smith, G.D.; Cogliano, V.J.; Hecht, S.S.; Seminara, D.; Vineis, P.; et al. Recommendations and Proposed Guidelines for Assessing the Cumulative Evidence on Joint Effects of Genes and Environments on Cancer Occurrence in Humans. Int. J. Epidemiol. 2012, 41, 686–704. [Google Scholar] [CrossRef]
- McAllister, K.; Mechanic, L.E.; Amos, C.; Aschard, H.; Blair, I.A.; Chatterjee, N.; Conti, D.; Gauderman, W.J.; Hsu, L.; Hutter, C.M.; et al. Current Challenges and New Opportunities for Gene-Environment Interaction Studies of Complex Diseases. Am. J. Epidemiol. 2017, 186, 753–761. [Google Scholar] [CrossRef]
- Kraft, P.; Yen, Y.-C.; Stram, D.O.; Morrison, J.; Gauderman, W.J. Exploiting Gene-Environment Interaction to Detect Genetic Associations. Hum. Hered. 2007, 63, 111–119. [Google Scholar] [CrossRef]
- Aschard, H. A Perspective on Interaction Effects in Genetic Association Studies. Genet. Epidemiol. 2016, 40, 678–688. [Google Scholar] [CrossRef]
- Murea, M.; Ma, L.; Freedman, B.I. Genetic and Environmental Factors Associated with Type 2 Diabetes and Diabetic Vascular Complications. Rev. Diabet. Stud. 2012, 9, 6–22. [Google Scholar] [CrossRef]
- Manolio, T.A.; Collins, F.S.; Cox, N.J.; Goldstein, D.B.; Hindorff, L.A.; Hunter, D.J.; McCarthy, M.I.; Ramos, E.M.; Cardon, L.R.; Chakravarti, A.; et al. Finding the Missing Heritability of Complex Diseases. Nature 2009, 461, 747–753. [Google Scholar] [CrossRef]
- Eze, I.C.; Imboden, M.; Kumar, A.; von Eckardstein, A.; Stolz, D.; Gerbase, M.W.; Künzli, N.; Pons, M.; Kronenberg, F.; Schindler, C.; et al. Air Pollution and Diabetes Association: Modification by Type 2 Diabetes Genetic Risk Score. Environ. Int. 2016, 94, 263–271. [Google Scholar] [CrossRef]
- Lee, Y.-C.; Lai, C.-Q.; Ordovas, J.M.; Parnell, L.D. A Database of Gene-Environment Interactions Pertaining to Blood Lipid Traits, Cardiovascular Disease and Type 2 Diabetes. J. Data Min. Genom. Proteom. 2011, 2. [Google Scholar] [CrossRef] [PubMed]
- Visscher, P.M.; Hill, W.G.; Wray, N.R. Heritability in the Genomics Era—Concepts and Misconceptions. Nat. Rev. Genet. 2008, 9, 255–266. [Google Scholar] [CrossRef] [PubMed]
- Zheng, J.-S.; Arnett, D.K.; Lee, Y.-C.; Shen, J.; Parnell, L.D.; Smith, C.E.; Richardson, K.; Li, D.; Borecki, I.B.; Ordovás, J.M.; et al. Genome-Wide Contribution of Genotype by Environment Interaction to Variation of Diabetes-Related Traits. PLoS ONE 2013, 8, e77442. [Google Scholar] [CrossRef] [PubMed]
| Study | Year | Country/Ethnicity | Patients | Controls | Database | |
|---|---|---|---|---|---|---|
| Studies focusing on type 1 diabetes | ||||||
| Winkler et al. [42] | 2014 | Caucasian | 4574 | 1207 | PubMed, Scopus | |
| Oram et al. [38] | 2015 | Caucasian | n = 1938 | PubMed | ||
| Patel et al. [39] | 2016 | Caucasian | 1963 | 805 | PubMed, Scopus | |
| Perry et al. [43] | 2018 | Caucasian, Hispanic, African-American and Asian-American | 627 | 423 | PubMed, Scopus, Web of Science | |
| Sharp et al. [44] | 2019 | Caucasian | 6670 | 9416 | PubMed | |
| Yaghootkar et al. [45] | 2019 | Iranian | 121 | 6 | PubMed, Web of Science | |
| Studies focusing on type 2 diabetes | ||||||
| Weedon et al. [46] | 2006 | British | 2409 | 3669 | PubMed, Scopus | |
| Lango et al. [47] | 2008 | Scotland | 2309 | 2598 | PubMed | |
| Lyssenko et al. [48] | 2008 | Finland | 2201 | 16,630 | PubMed | |
| Meigs et al. [49] | 2008 | European ancestry in USA | n = 2776 | PubMed, Scopus, Web of Science | ||
| Chatterjee et al. [50] | 2013 | Caucasian | 130 | 38,987 | PubMed | |
| Vassy et al. [51] | 2014 | European ancestry in USA | 5941 | 5942. | PubMed, Scopus | |
| Läll et al. [36] | 2016 | Estonia | 1181 | 9092 | PubMed, Scopus | |
| Chikowore et al. [54] | 2016 | South African | 178 | 178 | PubMed | |
| Amit et al. [19] | 2018 | British | 26,676 | 120,280 | PubMed, Web of Science | |
| Study | Year | Data Set | Panel of Genes | Platform |
|---|---|---|---|---|
| Studies focusing on type 1 diabetes | ||||
| Winkler et al. [42] | 2014 | T1DGC | T1DGC | TaqMan 5’nuclease assay |
| Oram et al. [38] | 2015 | WTCCC | 1000 genomes and T1DGC | Affymetrix 500K SNP chip |
| Patel et al. [39] | 2016 | WTCCC | 1000 genomes and T1DGC | Affymetrix 500K SNP chip |
| Perry et al. [43] | 2018 | University of Florida diabetes institute (UFDI) | Immunobase.org October 2017 | Taqman SNP genotyping array |
| Sharp et al. [44] | 2019 | T1DGC | 1000 genomes | Affymetrix Axiom Array |
| Yaghootkar et al. [45] | 2019 | Imam Reza Hospital and Children’s Medical Centre in Iran | 1000 genomes and T1DGC | Targeted next- generation sequencing (unspecified) |
| Studies focusing on type 2 diabetes | ||||
| Weedon et al. [46] | 2006 | UK | KCNK11, PPARG, TCF7L2. | Modified TaqMan |
| Lango et al. [47] | 2008 | GoDARTS | Frayling [66] and Zeggini et al. [67] | Modified TaqMan |
| Lyssenko et al. [48] | 2008 | Malmö Preventive Project (MPP) and Botnia Prospective Study (BPS). | Gloyn et al. [68], Grant et al. [69], Saxena et al. [70], Frayling [66], Scott et al. [71], Sladek et al. [72], Steinthorsdottir et al. [73], Zeggini et al. [74], Zeggini et al. [67], Lyssenko et al. [75]. | Allelic discrimination assay-by-design method, Allele-specific (KASPar) |
| Meigs et al. [49] | 2008 | The Framingham Offspring Study | Saxena et al. [70], Zeggini et al. [67] | iPLEX technology |
| Chatterjee et al. [50] | 2013 | Voight [62] | Voight et al. [62] | Illumina Omni 2.5M Platform |
| Vassy et al. [51] | 2014 | The Framingham Offspring Study and CARDIA | DIAGRAMv3 | Taqman, Illumina’s OPA technology, Affymetrix 6.0, llumina 370 and 550 |
| Läll et al. [36] | 2016 | The Estonian Biobank | DIAGRAM Consortium | Illumina Human OmniExpress, Illumina Cardio-MetaboChip |
| Chikowore et al. [54] | 2016 | The PURE study | Chikowore et al. [57] | BeadXpress platform, Illumina |
| Amit et al. [19] | 2018 | The UK Biobank | 1000 genome phase 3 version 5 (Linkage disequilibrium panel) | Affymetrix UK BiLEVE Axiom array, Affymetrix UK Biobank Axiom |
| Year | Author | Polygenic Risk Scores | Single-Nucleotide Polymorphism | Area under the Curve for Polygenic Risk Scores | Ethnicity |
|---|---|---|---|---|---|
| 2014 | Winkler et al. [42] | T1D | 41 | 0.87 | Caucasian |
| 2015 | Oram et al. [38] | T1D | 30 | 0.88 | Caucasian |
| 2015 | Oram et al. [38] | T1D + T2D | 99 | 0.89 | Caucasian |
| 2018 | Perry et al. [43] | T1D | 32 | 0.86 | Caucasian |
| 2018 | Perry et al. [43] | T1D | 32 | 0.90 | Caucasian Hispanic |
| 2018 | Perry et al. [43] | T1D | 32 | 0.75 | African-American |
| 2018 | Perry et al. [43] | T1D | 32 | 0.92 | Asian-American |
| 2019 | Sharp et al. [44] | T1D | 67 | 0.93 | Caucasian |
| Year | Author | Polygenic Risk Cores (PRS) | Single-Nucleotide Polymorphism | Area under the Curve (AUC) for Clinical Risk Factors | AUC PRS + Clinical Risk Factors | Difference | Clinical Risk Factors | Ethnicity |
|---|---|---|---|---|---|---|---|---|
| 2006 | Weedon et al. [46] | T2D | 3 | - | 0.580 | - | - | Caucasian |
| 2008 | Lango et al. [47] | T2D | 18 | 0.780 | 0.800 | 0.020 | Age, BMI, sex | Caucasian |
| 2008 | Lyssenko et al. [48] | T2D | 16 | 0.740 | 0.750 | 0.010 | Age, sex, family, BMI, blood pressure, triglycerides, glucose | Caucasian |
| 2008 | Meigs et al. [49] | T2D | 18 | 0.534 | 0.581 | 0.047 | Age, sex | Caucasian |
| 2008 | Meigs et al. [49] | T2D | 18 | 0.595 | 0.615 | 0.020 | Sex, age, family | Caucasian |
| 2008 | Meigs et al. [49] | T2D | 18 | 0.900 | 0.910 | 0.010 | Age, sex, family, BMI, glucose, cholesterol, triglycerides | Caucasian |
| 2013 | Chatterjee et al. [50] | T2D | 22 | 0.570 | 0.740 | 0.170 | Age, sex, family | Caucasian |
| 2014 | Vassy et al. [51] | T2D | 62 | 0.698 | 0.726 | 0.028 | Age, sex | Caucasian, USA population |
| 2014 | Vassy et al. [51] | T2D | 62 | 0.903 | 0.906 | 0.003 | Sex, family, BMI, blood pressure, HDL cholesterol, triglyceride levels, age | Caucasian, USA population |
| 2016 | Läll et al. [36] | T2D-double weighted | 1000 | 0.699 | 0.74 | 0.042 | Sex, age | Caucasian |
| 2016 | Läll et al. [36] | T2D-dw | 1000 | 0.718 | 0.767 | 0.049 | Sex, age, BMI | Caucasian |
| 2016 | Läll et al. [36] | T2D-dw | 1000 | 0.777 | 0.79 | 0.012 | Sex, age, BMI, hypertension, high blood glucose, physical activity, smoking, food consumption | Caucasian |
| 2016 | Chikowore et al. [54] | T2D | 4 | 0.652 | 0.665 | 0.013 | Sex, age, BMI and blood pressure | African |
| 2018 | Amit et al. [19] | T2D | 7 million | 0.66 | 0.73 | 0.070 | Sex, age | Caucasian |
| Year | Author | Polygenic Risk Scores | Single-Nucleotide Polymorphism | Area under the Curve for Polygenic Risk Scores | Ethnicity |
|---|---|---|---|---|---|
| 2015 | Oram et al. [38] | T1D vs. T2D | 30 | 0.88 | Caucasian |
| 2015 | Oram et al. [38] | T1D vs. T2D | 9 | 0.87 | Caucasian |
| 2016 | Patel et al. [39] | T1D vs. MODY | 30 | 0.87 | Caucasian |
| 2019 | Yaghootkar et al. [45] | T1D vs. Monogenic | 9 | 0.90 | Iranian |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Padilla-Martínez, F.; Collin, F.; Kwasniewski, M.; Kretowski, A. Systematic Review of Polygenic Risk Scores for Type 1 and Type 2 Diabetes. Int. J. Mol. Sci. 2020, 21, 1703. https://doi.org/10.3390/ijms21051703
Padilla-Martínez F, Collin F, Kwasniewski M, Kretowski A. Systematic Review of Polygenic Risk Scores for Type 1 and Type 2 Diabetes. International Journal of Molecular Sciences. 2020; 21(5):1703. https://doi.org/10.3390/ijms21051703
Chicago/Turabian StylePadilla-Martínez, Felipe, Francois Collin, Miroslaw Kwasniewski, and Adam Kretowski. 2020. "Systematic Review of Polygenic Risk Scores for Type 1 and Type 2 Diabetes" International Journal of Molecular Sciences 21, no. 5: 1703. https://doi.org/10.3390/ijms21051703
APA StylePadilla-Martínez, F., Collin, F., Kwasniewski, M., & Kretowski, A. (2020). Systematic Review of Polygenic Risk Scores for Type 1 and Type 2 Diabetes. International Journal of Molecular Sciences, 21(5), 1703. https://doi.org/10.3390/ijms21051703





