TERT Promoter Mutation as a Potential Predictive Biomarker in BCG-Treated Bladder Cancer Patients
Abstract
1. Introduction
2. Results
2.1. TERTp and FGFR3 Mutation Analysis
2.2. Clinicopathological Characteristics and Genetic Alterations
2.3. Clinicopathological and Molecular Characteristics with BCG Therapy Success
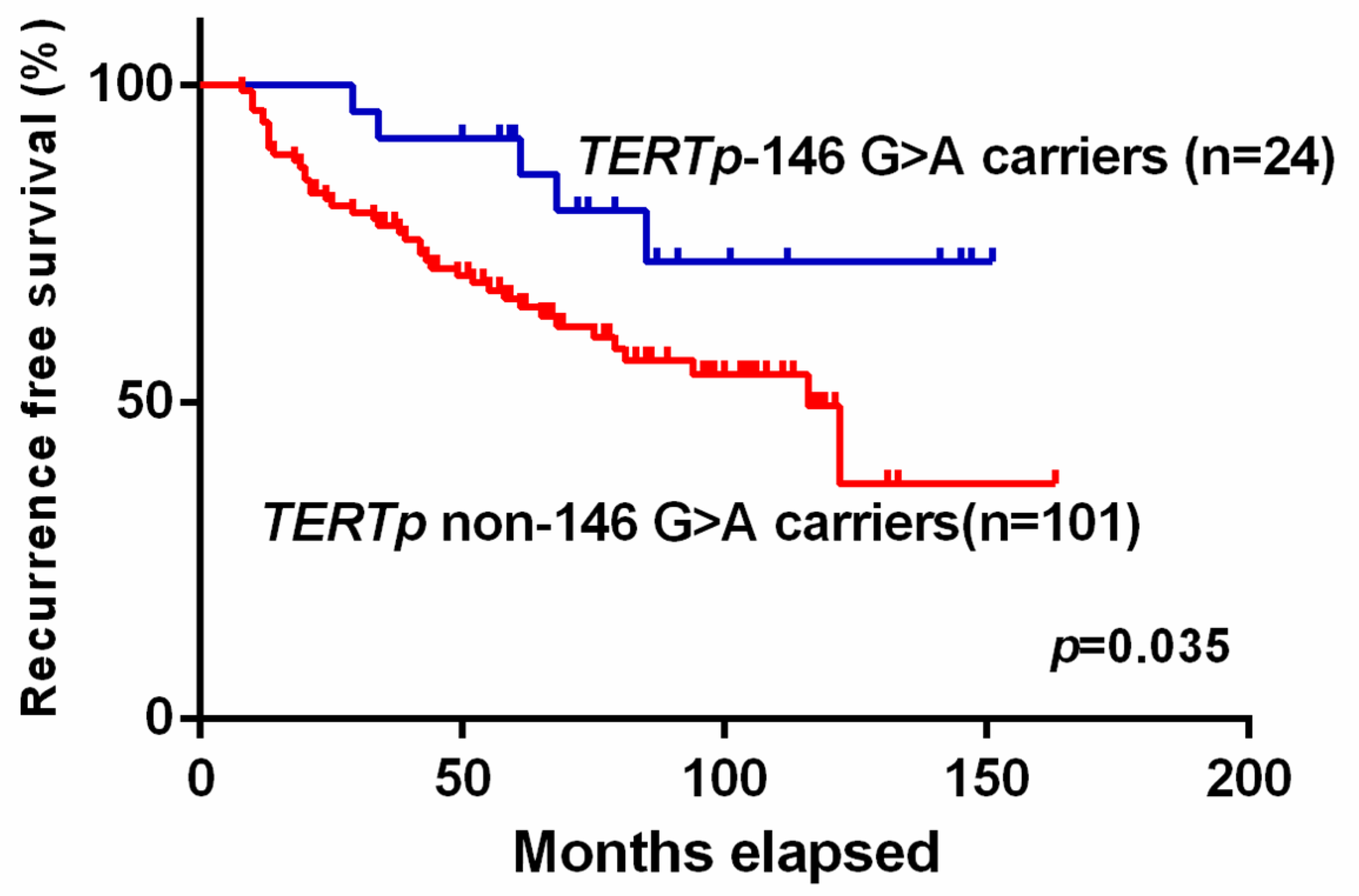
2.4. TERTp Mutations and Recurrence-Free Survival
3. Discussion
4. Materials and Methods
4.1. Human Cancer Samples and Clinicopathological Data
4.2. DNA Extraction, PCR, and Sanger Sequencing
4.3. Single Nucleotide Polymorphism Assay
4.4. Uromonitor Real-Time PCR screening Assay
4.5. Statistical Analysis
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| BC | Bladder cancer |
| BCG | Bacillus Calmette–Guérin |
| BCG-NMI | BCG-treated nonmuscle invasive |
| NMI | Nonmuscle invasive |
References
- Ferlay, J.; Colombet, M.; Soerjomataram, I.; Mathers, C.; Parkin, D.M.; Pineros, M.; Znaor, A.; Bray, F. Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods. J. Int. Cancer 2019, 144, 1941–1953. [Google Scholar] [CrossRef]
- Ploeg, M.; Aben, K.K.; Kiemeney, L.A. The present and future burden of urinary bladder cancer in the world. World J. Urol. 2009, 27, 289–293. [Google Scholar] [CrossRef] [PubMed]
- van Rhijn, B.W.; Burger, M.; Lotan, Y.; Solsona, E.; Stief, C.G.; Sylvester, R.J.; Witjes, J.A.; Zlotta, A.R. Recurrence and progression of disease in non-muscle-invasive bladder cancer: from epidemiology to treatment strategy. Eur. Urol. 2009, 56, 430–442. [Google Scholar] [CrossRef] [PubMed]
- Netto, G.J. Molecular biomarkers in urothelial carcinoma of the bladder: are we there yet? Nat. Rev. Urol. 2011, 9, 41–51. [Google Scholar] [CrossRef] [PubMed]
- Northrup, H.; Krueger, D.A.; International Tuberous Sclerosis Complex Consensus, G. Tuberous sclerosis complex diagnostic criteria update: recommendations of the 2012 Iinternational Tuberous Sclerosis Complex Consensus Conference. Pediatr. Neurol. 2013, 49, 243–254. [Google Scholar] [CrossRef]
- Horn, S.; Figl, A.; Rachakonda, P.S.; Fischer, C.; Sucker, A.; Gast, A.; Kadel, S.; Moll, I.; Nagore, E.; Hemminki, K.; et al. TERT promoter mutations in familial and sporadic melanoma. Science 2013, 339, 959–961. [Google Scholar] [CrossRef]
- Huang, F.W.; Hodis, E.; Xu, M.J.; Kryukov, G.V.; Chin, L.; Garraway, L.A. Highly recurrent TERT promoter mutations in human melanoma. Science 2013, 339, 957–959. [Google Scholar] [CrossRef]
- Killela, P.J.; Reitman, Z.J.; Jiao, Y.; Bettegowda, C.; Agrawal, N.; Diaz, L.A., Jr.; Friedman, A.H.; Friedman, H.; Gallia, G.L.; Giovanella, B.C.; et al. TERT promoter mutations occur frequently in gliomas and a subset of tumors derived from cells with low rates of self-renewal. Proc. Natl. Acad. Sci. USA 2013, 110, 6021–6026. [Google Scholar] [CrossRef]
- Liu, X.; Bishop, J.; Shan, Y.; Pai, S.; Liu, D.; Murugan, A.K.; Sun, H.; El-Naggar, A.K.; Xing, M. Highly prevalent TERT promoter mutations in aggressive thyroid cancers. Endocr. Relat. Cancer 2013, 20, 603–610. [Google Scholar] [CrossRef]
- Vinagre, J.; Almeida, A.; Populo, H.; Batista, R.; Lyra, J.; Pinto, V.; Coelho, R.; Celestino, R.; Prazeres, H.; Lima, L.; et al. Frequency of TERT promoter mutations in human cancers. Nat. Commun. 2013, 4, 2185. [Google Scholar] [CrossRef]
- Nault, J.C.; Mallet, M.; Pilati, C.; Calderaro, J.; Bioulac-Sage, P.; Laurent, C.; Laurent, A.; Cherqui, D.; Balabaud, C.; Zucman-Rossi, J. High frequency of telomerase reverse-transcriptase promoter somatic mutations in hepatocellular carcinoma and preneoplastic lesions. Nat. Commun. 2013, 4, 2218. [Google Scholar] [CrossRef] [PubMed]
- Griewank, K.G.; Schilling, B.; Murali, R.; Bielefeld, N.; Schwamborn, M.; Sucker, A.; Zimmer, L.; Hillen, U.; Schaller, J.; Brenn, T.; et al. TERT promoter mutations are frequent in atypical fibroxanthomas and pleomorphic dermal sarcomas. Mod. Pathol.: Off. J. US Can. Acad. Pathol. Inc. 2014, 27, 502–508. [Google Scholar] [CrossRef] [PubMed]
- Allory, Y.; Beukers, W.; Sagrera, A.; Flandez, M.; Marques, M.; Marquez, M.; van der Keur, K.A.; Dyrskjot, L.; Lurkin, I.; Vermeij, M.; et al. Telomerase reverse transcriptase promoter mutations in bladder cancer: high frequency across stages, detection in urine, and lack of association with outcome. Eur. Urol. 2014, 65, 360–366. [Google Scholar] [CrossRef] [PubMed]
- Hurst, C.D.; Platt, F.M.; Knowles, M.A. Comprehensive mutation analysis of the TERT promoter in bladder cancer and detection of mutations in voided urine. Eur. Urol. 2014, 65, 367–369. [Google Scholar] [CrossRef]
- Scott, G.A.; Laughlin, T.S.; Rothberg, P.G. Mutations of the TERT promoter are common in basal cell carcinoma and squamous cell carcinoma. Mod. Pathol.: Off. J. US Can. Acad. Pathol. Inc. 2014, 27, 516–523. [Google Scholar] [CrossRef]
- Liu, X.; Wu, G.; Shan, Y.; Hartmann, C.; von Deimling, A.; Xing, M. Highly prevalent TERT promoter mutations in bladder cancer and glioblastoma. Cell Cycle 2013, 12, 1637–1638. [Google Scholar] [CrossRef]
- Kinde, I.; Munari, E.; Faraj, S.F.; Hruban, R.H.; Schoenberg, M.; Bivalacqua, T.; Allaf, M.; Springer, S.; Wang, Y.; Diaz, L.A., Jr.; et al. TERT promoter mutations occur early in urothelial neoplasia and are biomarkers of early disease and disease recurrence in urine. Cancer Res. 2013, 73, 7162–7167. [Google Scholar] [CrossRef]
- Rachakonda, P.S.; Hosen, I.; de Verdier, P.J.; Fallah, M.; Heidenreich, B.; Ryk, C.; Wiklund, N.P.; Steineck, G.; Schadendorf, D.; Hemminki, K.; et al. TERT promoter mutations in bladder cancer affect patient survival and disease recurrence through modification by a common polymorphism. Proc. Natl. Acad. Sci. USA 2013, 110, 17426–17431. [Google Scholar] [CrossRef]
- Wu, S.; Huang, P.; Li, C.; Huang, Y.; Li, X.; Wang, Y.; Chen, C.; Lv, Z.; Tang, A.; Sun, X.; et al. Telomerase reverse transcriptase gene promoter mutations help discern the origin of urogenital tumors: a genomic and molecular study. Eur. Urol. 2014, 65, 274–277. [Google Scholar] [CrossRef]
- Ko, E.; Seo, H.W.; Jung, E.S.; Kim, B.H.; Jung, G. The TERT promoter SNP rs2853669 decreases E2F1 transcription factor binding and increases mortality and recurrence risks in liver cancer. Oncotarget 2016, 7, 684–699. [Google Scholar] [CrossRef]
- Batista, R.; Cruvinel-Carloni, A.; Vinagre, J.; Peixoto, J.; Catarino, T.A.; Campanella, N.C.; Menezes, W.; Becker, A.P.; de Almeida, G.C.; Matsushita, M.M.; et al. The prognostic impact of TERT promoter mutations in glioblastomas is modified by the rs2853669 single nucleotide polymorphism. Int. J. Cancer 2016, 139, 414–423. [Google Scholar] [CrossRef] [PubMed]
- Babjuk, M.; Oosterlinck, W.; Sylvester, R.; Kaasinen, E.; Bohle, A.; Palou-Redorta, J.; Roupret, M.; European Association of U. EAU guidelines on non-muscle-invasive urothelial carcinoma of the bladder, the 2011 update. Eur. Urol. 2011, 59, 997–1008. [Google Scholar] [CrossRef] [PubMed]
- Askeland, E.J.; Newton, M.R.; O’Donnell, M.A.; Luo, Y. Bladder Cancer Immunotherapy: BCG and Beyond. Adv. Urol. 2012, 2012, 181987. [Google Scholar] [CrossRef] [PubMed]
- Yates, D.R.; Roupret, M. Contemporary management of patients with high-risk non-muscle-invasive bladder cancer who fail intravesical BCG therapy. World J. Urol. 2011, 29, 415–422. [Google Scholar] [CrossRef] [PubMed]
- Billerey, C.; Chopin, D.; Aubriot-Lorton, M.H.; Ricol, D.; Gil Diez de Medina, S.; Van Rhijn, B.; Bralet, M.P.; Lefrere-Belda, M.A.; Lahaye, J.B.; Abbou, C.C.; et al. Frequent FGFR3 mutations in papillary non-invasive bladder (pTa) tumors. Am. J. Pathol. 2001, 158, 1955–1959. [Google Scholar] [CrossRef]
- Roe, J.S.; Kim, H.; Lee, S.M.; Kim, S.T.; Cho, E.J.; Youn, H.D. p53 Stabilization and Transactivation by a von Hippel-Lindau Protein. Mol. Cell 2006, 22, 395–405. [Google Scholar] [CrossRef]
- Kawai, K.; Miyazaki, J.; Joraku, A.; Nishiyama, H.; Akaza, H. Bacillus Calmette-Guerin (BCG) immunotherapy for bladder cancer: current understanding and perspectives on engineered BCG vaccine. Cancer Sci. 2013, 104, 22–27. [Google Scholar] [CrossRef]
- Herr, H.W.; Morales, A. History of bacillus Calmette-Guerin and bladder cancer: an immunotherapy success story. J. Urol. 2008, 179, 53–56. [Google Scholar] [CrossRef]
- Dabora, S.L.; Jozwiak, S.; Franz, D.N.; Roberts, P.S.; Nieto, A.; Chung, J.; Choy, Y.-S.; Reeve, M.P.; Thiele, E.; Egelhoff, J.C.; et al. Mutational Analysis in a Cohort of 224 Tuberous Sclerosis Patients Indicates Increased Severity of TSC2, Compared with TSC1, Disease in Multiple Organs. Am. J. Hum. Genet. 2001, 68, 64–80. [Google Scholar] [CrossRef]
- Saitoh, H.; Mori, K.; Kudoh, S.; Itoh, H.; Takahashi, N.; Suzuki, T. BCG effects on telomerase activity in bladder cancer cell lines. Int. J. Clin. Oncol. 2002, 7, 165–170. [Google Scholar] [CrossRef]
- Edge, S.B.; Compton, C.C. The American Joint Committee on Cancer: the 7th edition of the AJCC cancer staging manual and the future of TNM. Ann. Surg. Oncol. 2010, 17, 1471–1474. [Google Scholar] [CrossRef] [PubMed]
- Davis, C.J.; Woodward, P.J.; Dehner, L.P.; Eble, J.N.; Sauter, G.; Epstein, J.I. WHO Classification of Tumors. Pathology and Genetics of Tumors of the Urinary System and Male Genital Organs. IARC Press 2004, 267–276. [Google Scholar]
- Lima, L.; Oliveira, D.; Tavares, A.; Amaro, T.; Cruz, R.; Oliveira, M.J.; Ferreira, J.A.; Santos, L. The predominance of M2-polarized macrophages in the stroma of low-hypoxic bladder tumors is associated with BCG immunotherapy failure. Urol. Oncol. 2014, 32, 449–457. [Google Scholar] [CrossRef] [PubMed]
| BCG-NMIBC, n (%) | |
|---|---|
| TERTp | |
| Wild type | 55 (44.0) |
| Mutated | 70 (56.0) |
| Specific mutations | |
| c.1-124G>A | 46 (36.8) |
| c.1-146G>A | 22 (17.6) |
| c.1-124G>A/c.1-146G>A | 2 (1.6) |
| FGFR3 | |
| Wild type | 59 (55.1) |
| Mutated | 48 (44.9) |
| Specific mutations | |
| Exon 7 p.R248C | 19 (39.6) |
| Exon 7 p.S249C | 25 (52.0) |
| Exon 10 p.Y375C | 1 (2.1) |
| Exon 7 p.R248C + p.S249C | 1(2.1) |
| Exon 7 p.R248C + Exon 10 p.Y375C | 1(2.1) |
| Exon 7 p.R248C + Exon 15 p.K652E | 1(2.1) |
| rs2853669 | |
| AA | 39 (39.8) |
| AG | 47 (48.0) |
| GG | 12 (12.2) |
| TERTp | |||
|---|---|---|---|
| Wild Type, n (%) | Mutated, n (%) | p-value | |
| Age group | |||
| <65 years | 21 (38.2) | 33 (47.1) | 0.315 |
| ≥65 years | 34 (61.8) | 37 (52.9) | |
| Gender | |||
| Female | 11 (20.0) | 8 (11.4) | 0.185 |
| Male | 44 (80.0) | 62 (88.6) | |
| Stage | |||
| Ta | 23 (41.8) | 28 (40.0) | 0.837 |
| T1 | 32 (58.2) | 42 (60.0) | |
| Grade | |||
| Low | 15 (27.3) | 25 (35.7) | 0.315 |
| High | 40 (72.7) | 45 (64.3) | |
| Tumour size | |||
| <3 cm | 34 (63.0) | 41 (58.6) | 0.620 |
| ≥3 cm | 20 (37.0) | 29 (41.4) | |
| Multifocality | |||
| No | 28 (50.9) | 32 (45.7) | 0.564 |
| Yes | 27 (49.1) | 38 (54.3) | |
| Recurrence status | |||
| Primary | 24 (43.6) | 43 (61.4) | 0.048 |
| Recurrent | 31 (56.4) | 27 (38.6) | |
| rs2853669 | |||
|---|---|---|---|
| AA, n (%) | G Carrier, n (%) | p-value | |
| Age group | |||
| <65 years | 17 (41.5) | 22 (38.6) | 0.775 |
| ≥65 years | 24 (58.5) | 35 (61.4) | |
| Gender | |||
| Female | 5 (37.5) | 34 (40.5) | 0.736 |
| Male | 9 (64.3) | 50 (59.5) | |
| Stage | |||
| Ta | 15 (39.5) | 24 (40.0) | 0.959 |
| T1 | 23 (60.5) | 36 (60.0) | |
| Grade | |||
| Low | 7 (22.6) | 32 (47.8) | 0.018 |
| High | 24 (77.4) | 35 (52.2) | |
| Tumour size | |||
| <3 cm | 22 (34.9) | 17 (50.0) | 0.148 |
| ≥3 cm | 41 (65.1) | 17 (50.0) | |
| Multifocality | |||
| No | 19 (43.2) | 20 (37.0) | 0.536 |
| Yes | 25 (56.8) | 34 (63.0) | |
| Recurrence status | |||
| Primary | 22 (43.1) | 17 (36.2) | 0.481 |
| Recurrent | 29 (56.9) | 30 (63.8) | |
| BCG Therapy | ||||
|---|---|---|---|---|
| Success, n (%) | Failure, n (%) | HR (95% CI) | p-value | |
| TERTp | ||||
| Wild type | 34 (43.0) | 21 (45.7) | 1.0 | 0.580 |
| Mutated | 45 (57.0) | 25 (54.3) | 0.848 (0.473–1.520) | |
| TERTp genotype | ||||
| Wild type | 34 (43.0) | 21 (45.6) | 1.0 | |
| c.1-124G > A | 26 (32.9) | 20 (43.5) | 1.158 (0.626–2.143) | 0.639 |
| c.1-146G > A | 17 (21.5) | 5 (10.9) | 0.410 (0.152–1.108) | 0.079 |
| c.1-124G>A/c.1-146G>A | 2 (2.5) | 0 (0.0) | 0.464 (0.040–5.327) | 0.464 |
| TERTp c.1-146G>A status | ||||
| c.1-146G>A carriers | 60 (75.9) | 41 (89.1) | 1.0 | 0.043 |
| non c.1-146G>A carriers | 19 (24.1) | 5 (10.9) | 0.382 (0.150–0.971) | |
| FGFR3 | ||||
| Wild type Mutated | 39 (60.0) 26 (40.0) | 20 (51.3) 19 (48.7) | 1.0 1.336 (0.712–2.507) | 0.367 |
| FGFR3 status | ||||
| Wild type | 39 (60.0) | 20 (51.3) | 1.0 | |
| p.R248C | 12 (18.5) | 7 (17.9) | 1.158 (0.524–3.015) | 0.608 |
| p.S249C | 14 (21.5) | 11 (28.2) | 0.410 (0.650–2.842) | 0.415 |
| p.R248C/p.S249C | 0 (0.0) | 1 (2.6) | 1.584 (0.804–3.120) | 0.184 |
| TERTp c.1-146G>A Status | HR a | 95% CI | p-value |
|---|---|---|---|
| c.1-146G>A carriers | 1.0 | Referent | |
| non c.1-146G>A carriers | 0.256 | 0.098-0.667 | 0.005 |
| Age ≥ 65 years | 2.370 | 1.206-4.661 | 0.012 |
| Multifocality | 1.883 | 0.964-3.677 | 0.064 |
| Recurrent tumor | 1.352 | 0.703-2.600 | 0.367 |
| iBCG schedule | 2.225 | 1.211-4.088 | 0.010 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Batista, R.; Lima, L.; Vinagre, J.; Pinto, V.; Lyra, J.; Máximo, V.; Santos, L.; Soares, P. TERT Promoter Mutation as a Potential Predictive Biomarker in BCG-Treated Bladder Cancer Patients. Int. J. Mol. Sci. 2020, 21, 947. https://doi.org/10.3390/ijms21030947
Batista R, Lima L, Vinagre J, Pinto V, Lyra J, Máximo V, Santos L, Soares P. TERT Promoter Mutation as a Potential Predictive Biomarker in BCG-Treated Bladder Cancer Patients. International Journal of Molecular Sciences. 2020; 21(3):947. https://doi.org/10.3390/ijms21030947
Chicago/Turabian StyleBatista, Rui, Luís Lima, João Vinagre, Vasco Pinto, Joana Lyra, Valdemar Máximo, Lúcio Santos, and Paula Soares. 2020. "TERT Promoter Mutation as a Potential Predictive Biomarker in BCG-Treated Bladder Cancer Patients" International Journal of Molecular Sciences 21, no. 3: 947. https://doi.org/10.3390/ijms21030947
APA StyleBatista, R., Lima, L., Vinagre, J., Pinto, V., Lyra, J., Máximo, V., Santos, L., & Soares, P. (2020). TERT Promoter Mutation as a Potential Predictive Biomarker in BCG-Treated Bladder Cancer Patients. International Journal of Molecular Sciences, 21(3), 947. https://doi.org/10.3390/ijms21030947









