Humanized Mice as an Effective Evaluation System for Peptide Vaccines and Immune Checkpoint Inhibitors
Abstract
1. Introduction
2. Difficulties in the Development of Peptide Vaccines
2.1. Selection of the Adequate Peptide for Vaccination
2.2. Antigens which Enable Activation of the Patient Immune System
2.3. Immune Suppression in Patients Prevents the Effectiveness of Vaccines
3. Immune Checkpoint Inhibitors and Reagents for Side-Effect Regulation
3.1. Patients with Cancer
3.2. Patients with Infectious Diseases
3.3. Steroid Hormones and ICI Side Effects
4. Humanized Mouse Models for the Evaluation of the Human Immune Environment
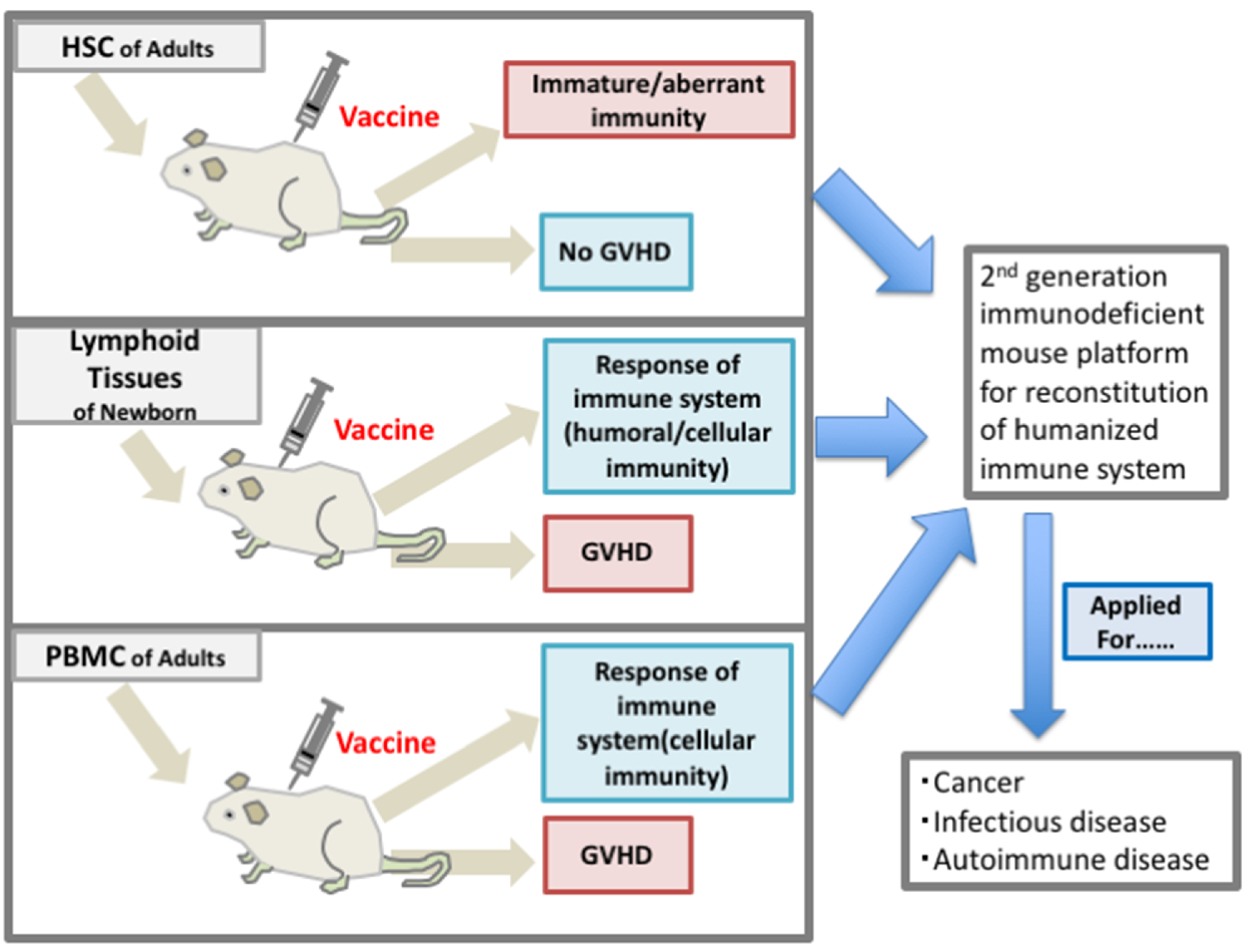
4.1. Humanized Mice for Reconstitution of the Human Immune System with Hematopoietic Cells
4.2. Humanized Mouse System to Evaluate Antigen-Specific Antibody Production
5. Future Perspectives
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
| PBMC | peripheral blood mononuclear cell |
| MHC | major histocompatibility complex |
| DC | dendritic cell |
| irAE | immune-related adverse events |
| ICI | immune checkpoint inhibitors |
| HER2 | Human epidermal growth factor receptor 2 |
| IHC | immunohistochemistry |
| PD-L1 | programmed-death-L1 |
| NOD scid | nonobese diabetic severe combined immunodeficient |
| HSC | hematopoietic stem cells |
| NOG | NOD/Shi-scid-IL2Rγnull |
| NSG | NOD scid gamma |
| GVHD | graft-versus-host disease |
References
- Marshall, H.; Djamgoz, M. Immuno-Oncology: Emerging Targets and Combination Therapies. Front. Oncol. 2018, 8, 315. [Google Scholar] [CrossRef] [PubMed]
- Wilkinson, K.; Wei, Y.; Szwajcer, A.; Rabbani, R.; Zarychanski, R.; Abou-Setta, A.; Mahmud, S. Efficacy and safety of high-dose influenza vaccine in elderly adults: A systematic review and meta-analysis. Vaccine 2017, 35, 2775–2780. [Google Scholar] [CrossRef] [PubMed]
- Nakashima, K.; Aoshima, M.; Ohfuji, S.; Suzuki, K.; Katsurada, M.; Katsurada, N.; Misawa, M.; Otsuka, Y.; Kondo, K.; Hirota, Y. Immunogenicity of trivalent influenza vaccine in patients with lung cancer undergoing anticancer chemotherapy. Hum. Vaccin Immunother. 2017, 13, 543–550. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Waqar, S.; Boehmer, L.; Morgensztern, D.; Wang-Gillam, A.; Sorscher, S.; Lawrence, S.; Gao, F.; Guebert, K.; Williams, K.; Govindan, R. Immunogenicity of Influenza Vaccination in Patients With Cancer. Am. J. Clin. Oncol. 2018, 41, 248–253. [Google Scholar] [CrossRef]
- Andreatta, M.; Karosiene, E.; Rasmussen, M.; Stryhn, A.; Buus, S.; Nielsen, M. Accurate pan-specific prediction of peptide-MHC class II binding affinity with improved binding core identification. Immunogenetics 2015, 67, 641–650. [Google Scholar] [CrossRef]
- Andreatta, M.; Nielsen, M. Gapped sequence alignment using artificial neural networks: Application to the MHC class I system. Bioinformatics 2016, 32, 511–517. [Google Scholar] [CrossRef]
- Rasmussen, M.; Fenoy, E.; Harndahl, M.; Kristensen, A.; Nielsen, I.; Nielsen, M.; Buus, S. Pan-Specific Prediction of Peptide-MHC Class I Complex Stability, a Correlate of T Cell Immunogenicity. J. Immunol. 2016, 197, 1517–1524. [Google Scholar] [CrossRef]
- Wang, J.; Ji, X.; Ou, G.; Su, P.; Liu, Z. LA-B*46:40:02, a novel HLA-B*46 allele identified in a Chinese individual by sequence-based typing. Hla 2016, 87, 462–464. [Google Scholar] [CrossRef]
- Li, J.; Zhang, X.; Lin, F.; Zhang, K.; Li, X.F. Identification of the novel HLA allele, HLA-B*40:06:07, by sequence-based typing. Hla 2018, 92, 326–327. [Google Scholar] [CrossRef]
- Proust, B.; Masson, D.; Proust, B.; Baudron, M.; Dehaut, F. Identification of a novel HLA allele, HLA-B*08:163, in a platelet donor. Hla 2016, 88, 263–264. [Google Scholar] [CrossRef]
- Moyle, P.; Toth, I. Self-adjuvanting lipopeptide vaccines. Curr. Med. Chem. 2008, 15, 506–516. [Google Scholar] [CrossRef] [PubMed]
- Pasquevich, K.; García Samartino, C.; Coria, L.; Estein, S.; Zwerdling, A.; Ibañez, A.; Barrionuevo, P.; Oliveira, F.; Carvalho, N.; Borkowski, J.; et al. The protein moiety of Brucella abortus outer membrane protein 16 is a new bacterial pathogen-associated molecular pattern that activates dendritic cells in vivo, induces a Th1 immune response, and is a promising self-adjuvanting vaccine against systemic and oral acquired brucellosis. J. Immunol. 2010, 184, 5200–5212. [Google Scholar]
- Shen, K.; Chang, L.; Leng, C.; Liu, S. Self-adjuvanting lipoimmunogens for therapeutic HPV vaccine development: Potential clinical impact. Expert Rev. Vaccines 2015, 14, 383–394. [Google Scholar] [CrossRef] [PubMed]
- Zeng, B.; Middelberg, A.; Gemiarto, A.; MacDonald, K.; Baxter, A.; Talekar, M.; Moi, D.; Tullett, K.; Caminschi, I.; Lahoud, M.; et al. Self-adjuvanting nanoemulsion targeting dendritic cell receptor Clec9A enables antigen-specific immunotherapy. J. Clin. Investig. 2018, 128, 1971–1984. [Google Scholar] [CrossRef] [PubMed]
- Wang, R. Human tumor antigens: Implications for cancer vaccine development. J. Mol. Med. 1999, 77, 640–655. [Google Scholar] [CrossRef]
- Bezu, L.; Kepp, O.; Cerrato, G.; Pol, J.; Fucikova, J.; Spisek, R.; Zitvogel, L.; Kroemer, G.; Galluzzi, L. Trial watch: Peptide-based vaccines in anticancer therapy. Oncoimmunology 2018, 7, e1511506. [Google Scholar] [CrossRef]
- Wang, Y.; Yang, L.; Zuo, J. Recent developments in antivirals against hepatitis B virus. Virus Res. 2016, 213, 205–213. [Google Scholar] [CrossRef]
- Kanduc, D.; Shoenfeld, Y. From HBV to HPV: Designing vaccines for extensive and intensive vaccination campaigns worldwide. Autoimmun. Rev. 2016, 15, 1054–1061. [Google Scholar] [CrossRef]
- Cheever, M.; Higano, C. PROVENGE (Sipuleucel-T) in prostate cancer: The first FDA-approved therapeutic cancer vaccine. Clin. Cancer Res. 2011, 17, 3520–3526. [Google Scholar] [CrossRef]
- Guevara, M.; Persano, S.; Persano, F. Lipid-Based Vectors for Therapeutic mRNA-Based Anti-Cancer Vaccines. Curr. Pharm. Des. 2019, 25, 1443–1454. [Google Scholar] [CrossRef]
- Park, S.; Kim, D.; Wu, G.; Jung, H.; Park, J.; Kwon, H.; Lee, Y. A peptide-CpG-DNA-liposome complex vaccine targeting TM4SF5 suppresses growth of pancreatic cancer in a mouse allograft model. Onco Targets Ther. 2018, 11, 8655–8672. [Google Scholar] [CrossRef] [PubMed]
- Schwartzentruber, D.; Lawson, D.; Richards, J.; Conry, R.; Miller, D.; Treisman, J.; Gailani, F.; Riley, L.; Conlon, K.; Pockaj, B.; et al. gp100 peptide vaccine and interleukin-2 in patients with advanced melanoma. N. Engl. J. Med. 2011, 364, 2119–2127. [Google Scholar] [CrossRef] [PubMed]
- Wargo, J.; Reddy, S.; Reuben, A.; Sharma, P. Monitoring immune responses in the tumor microenvironment. Curr. Opin. Immunol. 2016, 41, 23–31. [Google Scholar] [CrossRef] [PubMed]
- Desjarlais, J.; Lazar, G.; Zhukovsky, E.; Chu, S. Optimizing engagement of the immune system by anti-tumor antibodies: An engineer’s perspective. Drug Discov. Today 2007, 12, 898–910. [Google Scholar] [CrossRef] [PubMed]
- Wong, K.; Li, W.; Mooney, D.; Dranoff, G. Advances in Therapeutic Cancer Vaccines. Adv. Immunol. 2016, 130, 191–249. [Google Scholar]
- Papayannopoulos, V. Neutrophil extracellular traps in immunity and disease. Nat. Rev. Immunol. 2018, 18, 134–147. [Google Scholar] [CrossRef]
- Skopelja-Gardner, S.; Jones, J.; Rigby, W. “NETtling” the host: Breaking of tolerance in chronic inflammation and chronic infection. J. Autoimmun. 2018, 88, 1–10. [Google Scholar] [CrossRef]
- Steinman, R.; Nussenzweig, M. Avoiding horror autotoxicus: The importance of dendritic cells in peripheral T cell tolerance. Proc. Natl. Acad. Sci. USA 2002, 99, 351–358. [Google Scholar] [CrossRef]
- Abiko, K.; Matsumura, N.; Hamanishi, J.; Horikawa, N.; Murakami, R.; Yamaguchi, K.; Yoshioka, Y.; Baba, T.; Konishi, I.; Mandai, M. IFN-γ from lymphocytes induces PD-L1 expression and promotes progression of ovarian cancer. Br. J. Cancer 2015, 112, 150–159. [Google Scholar] [CrossRef]
- Taube, J.; Anders, R.; Young, G.; Xu, H.; Sharma, R.; McMiller, T.; Chen, S.; Klein, A.; Pardoll, D.; Topalian, S.; et al. Colocalization of inflammatory response with B7-h1 expression in human melanocytic lesions supports an adaptive resistance mechanism of immune escape. Sci. Transl. Med. 2012, 4, 127ra37. [Google Scholar] [CrossRef]
- Mazanet, M.; Hughes, C. B7-H1 is expressed by human endothelial cells and suppresses T cell cytokine synthesis. J. Immunol. 2002, 169, 3581–3588. [Google Scholar] [CrossRef] [PubMed]
- Brown, J.; Dorfman, D.; Ma, F.; Sullivan, E.; Munoz, O.; Wood, C.; Greenfield, E.; Freeman, G. Blockade of programmed death-1 ligands on dendritic cells enhances T cell activation and cytokine production. J. Immunol. 2003, 170, 1257–1266. [Google Scholar] [CrossRef] [PubMed]
- Wintterle, S.; Schreiner, B.; Mitsdoerffer, M.; Schneider, D.; Chen, L.; Meyermann, R.; Weller, M.; Wiendl, H. Expression of the B7-related molecule B7-H1 by glioma cells: A potential mechanism of immune paralysis. Cancer Res. 2003, 63, 7462–7467. [Google Scholar] [PubMed]
- Schoop, R.; Wahl, P.; Le Hir, M.; Heemann, U.; Wang, M.; Wüthrich, R. Suppressed T-cell activation by IFN-gamma-induced expression of PD-L1 on renal tubular epithelial cells. Nephrol. Dial. Transplant. 2004, 19, 2713–2720. [Google Scholar] [CrossRef] [PubMed]
- de Kleijn, S.; Langereis, J.; Leentjens, J.; Kox, M.; Netea, M.; Koenderman, L.; Ferwerda, G.; Pickkers, P.; Hermans, P. IFN-γ-stimulated neutrophils suppress lymphocyte proliferation through expression of PD-L1. PLoS ONE 2013, 8, e72249. [Google Scholar] [CrossRef]
- Garcia-Diaz, A.; Shin, D.; Moreno, B.; Saco, J.; Escuin-Ordinas, H.; Rodriguez, G.; Zaretsky, J.; Sun, L.; Hugo, W.; Wang, X.; et al. Interferon Receptor Signaling Pathways Regulating PD-L1 and PD-L2 Expression. Cell Rep. 2017, 19, 1189–1201. [Google Scholar] [CrossRef]
- Lim, S.; Li, C.; Xia, W.; Cha, J.; Chan, L.; Wu, Y.; Chang, S.; Lin, W.; Hsu, J.; Hsu, Y.; et al. Deubiquitination and Stabilization of PD-L1 by CSN5. Cancer Cell 2016, 30, 925–939. [Google Scholar] [CrossRef]
- Grinberg-Bleyer, Y.; Ghosh, S. A Novel Link between Inflammation and Cancer. Cancer Cell 2016, 30, 829–830. [Google Scholar] [CrossRef]
- Kondo, A.; Yamashita, T.; Tamura, H.; Zhao, W.; Tsuji, T.; Shimizu, M.; Shinya, E.; Takahashi, H.; Tamada, K.; Chen, L.; et al. Interferon-gamma and tumor necrosis factor-alpha induce an immunoinhibitory molecule, B7-H1, via nuclear factor-kappaB activation in blasts in myelodysplastic syndromes. Blood 2010, 116, 1124–1131. [Google Scholar] [CrossRef]
- Quandt, D.; Jasinski-Bergner, S.; Müller, U.; Schulze, B.; Seliger, B. Synergistic effects of IL-4 and TNFα on the induction of B7-H1 in renal cell carcinoma cells inhibiting allogeneic T cell proliferation. J. Transl. Med. 2014, 12, 151. [Google Scholar] [CrossRef]
- Li, N.; Wang, J.; Zhang, N.; Zhuang, M.; Zong, Z.; Zou, J.; Li, G.; Wang, X.; Zhou, H.; Zhang, L.; et al. Cross-talk between TNF-α and IFN-γ signaling in induction of B7-H1 expression in hepatocellular carcinoma cells. Cancer Immunol. Immunother. 2018, 67, 271–283. [Google Scholar] [CrossRef] [PubMed]
- Weyand, C.; Berry, G.; Goronzy, J. The immunoinhibitory PD-1/PD-L1 pathway in inflammatory blood vessel disease. J. Leukoc. Biol. 2018, 103, 565–575. [Google Scholar] [CrossRef] [PubMed]
- Kythreotou, A.; Siddique, A.; Mauri, F.; Bower, M.; Pinato, D. PD-L1. J. Clin. Pathol. 2018, 71, 189–194. [Google Scholar] [CrossRef]
- Butte, M.; Peña-Cruz, V.; Kim, M.; Freeman, G.; Sharpe, A. Interaction of human PD-L1 and B7-1. Mol. Immunol. 2008, 45, 3567–3572. [Google Scholar] [CrossRef] [PubMed]
- Xiao, Y.; Yu, S.; Zhu, B.; Bedoret, D.; Bu, X.; Francisco, L.; Hua, P.; Duke-Cohan, J.; Umetsu, D.; Sharpe, A.; et al. RGMb is a novel binding partner for PD-L2 and its engagement with PD-L2 promotes respiratory tolerance. J. Exp. Med. 2014, 211, 943–959. [Google Scholar] [CrossRef]
- Balar, A.; Weber, J. PD-1 and PD-L1 antibodies in cancer: Current status and future directions. Cancer Immunol. Immunother. 2017, 66, 551–564. [Google Scholar] [CrossRef]
- Agata, Y.; Kawasaki, A.; Nishimura, H.; Ishida, Y.; Tsubata, T.; Yagita, H.; Honjo, T. Expression of the PD-1 antigen on the surface of stimulated mouse T and B lymphocytes. Int. Immunol. 1996, 8, 765–772. [Google Scholar] [CrossRef]
- Haynes, N.; Allen, C.; Lesley, R.; Ansel, K.; Killeen, N.; Cyster, J. Role of CXCR5 and CCR7 in follicular Th cell positioning and appearance of a programmed cell death gene-1high germinal center-associated subpopulation. J. Immunol. 2007, 179, 5099–5108. [Google Scholar] [CrossRef]
- Freeman, G.; Long, A.; Iwai, Y.; Bourque, K.; Chernova, T.; Nishimura, H.; Fitz, L.; Malenkovich, N.; Okazaki, T.; Byrne, M.; et al. Engagement of the PD-1 immunoinhibitory receptor by a novel B7 family member leads to negative regulation of lymphocyte activation. J. Exp. Med. 2000, 192, 1027–1034. [Google Scholar] [CrossRef]
- Yamazaki, T.; Akiba, H.; Iwai, H.; Matsuda, H.; Aoki, M.; Tanno, Y.; Shin, T.; Tsuchiya, H.; Pardoll, D.; Okumura, K.; et al. Expression of programmed death 1 ligands by murine T cells and APC. J. Immunol. 2002, 169, 5538–5545. [Google Scholar] [CrossRef]
- D’Arrigo, P.; Tufano, M.; Rea, A.; Vigorito, V.; Novizio, N.; Russo, S.; Romano, M.; Romano, S. Manipulation of the immune system for cancer defeat: A focus on the T cell inhibitory checkpoint molecules. Curr. Med. Chem. 2018. [Google Scholar] [CrossRef] [PubMed]
- De Sousa Linhares, A.; Leitner, J.; Grabmeier-Pfistershammer, K.; Steinberger, P. Not All Immune Checkpoints Are Created Equal. Front. Immunol. 2018, 9, 1909. [Google Scholar] [CrossRef] [PubMed]
- Wolchok, J.; Kluger, H.; Callahan, M.; Postow, M.; Rizvi, N.; Lesokhin, A.; Segal, N.; Ariyan, C.; Gordon, R.; Reed, K.; et al. Nivolumab plus ipilimumab in advanced melanoma. N. Engl. J. Med. 2013, 369, 122–133. [Google Scholar] [CrossRef] [PubMed]
- Carlino, M.; Long, G.; Schadendorf, D.; Robert, C.; Ribas, A.; Richtig, E.; Nyakas, M.; Caglevic, C.; Tarhini, A.; Blank, C.; et al. Outcomes by line of therapy and programmed death ligand 1 expression in patients with advanced melanoma treated with pembrolizumab or ipilimumab in KEYNOTE-006: A randomised clinical trial. Eur. J. Cancer 2018, 101, 236–243. [Google Scholar] [CrossRef]
- Daud, A.; Wolchok, J.; Robert, C.; Hwu, W.; Weber, J.; Ribas, A.; Hodi, F.; Joshua, A.; Kefford, R.; Hersey, P.; et al. Programmed Death-Ligand 1 Expression and Response to the Anti-Programmed Death 1 Antibody Pembrolizumab in Melanoma. J. Clin. Oncol. 2016, 34, 4012–4109. [Google Scholar] [CrossRef]
- Festino, L.; Botti, G.; Lorigan, P.; Masucci, G.; Hipp, J.; Horak, C.; Melero, I.; Ascierto, P. Cancer Treatment with Anti-PD-1/PD-L1 Agents: Is PD-L1 Expression a Biomarker for Patient Selection? Drugs 2016, 76, 925–945. [Google Scholar] [CrossRef]
- Hodi, F.; Chiarion-Sileni, V.; Gonzalez, R.; Grob, J.; Rutkowski, P.; Cowey, C.; Lao, C.; Schadendorf, D.; Wagstaff, J.; Dummer, R.; et al. Nivolumab plus ipilimumab or nivolumab alone versus ipilimumab alone in advanced melanoma (CheckMate 067): 4-year outcomes of a multicentre, randomised, phase 3 trial. Lancet Oncol. 2018, 19, 1480–1492. [Google Scholar] [CrossRef]
- Conroy, J.; Pabla, S.; Nesline, M.; Glenn, S.; Papanicolau-Sengos, A.; Burgher, B.; Andreas, J.; Giamo, V.; Wang, Y.; Lenzo, F.; et al. Next generation sequencing of PD-L1 for predicting response to immune checkpoint inhibitors. J. Immunother. Cancer 2019, 7, 18. [Google Scholar] [CrossRef]
- Robert, C.; Long, G.; Brady, B.; Dutriaux, C.; Maio, M.; Mortier, L.; Hassel, J.; Rutkowski, P.; McNeil, C.; Kalinka-Warzocha, E.; et al. Nivolumab in previously untreated melanoma without BRAF mutation. N. Engl. J. Med. 2015, 372, 320–330. [Google Scholar] [CrossRef]
- Kambayashi, Y.; Fujimura, T.; Hidaka, T.; Aiba, S. Biomarkers for Predicting Efficacies of Anti-PD1 Antibodies. Front. Med. 2019, 6, 174. [Google Scholar] [CrossRef]
- Franzen, A.; Vogt, T.; Müller, T.; Dietrich, J.; Schröck, A.; Golletz, C.; Brossart, P.; Bootz, F.; Landsberg, J.; Kristiansen, G.; et al. PD-L1 (CD274) and PD-L2 (PDCD1LG2) promoter methylation is associated with HPV infection and transcriptional repression in head and neck squamous cell carcinomas. Oncotarget 2017, 9, 641–650. [Google Scholar] [CrossRef] [PubMed]
- Said, E.; Al-Reesi, I.; Al-Riyami, M.; Al-Naamani, K.; Al-Sinawi, S.; Al-Balushi, M.; Koh, C.; Al-Busaidi, J.; Idris, M.; Al-Jabri, A. A Potential Inhibitory Profile of Liver CD68+ Cells during HCV Infection as Observed by an Increased CD80 and PD-L1 but Not CD86 Expression. PLoS ONE 2016, 11, e0153191. [Google Scholar] [CrossRef] [PubMed]
- Okuma, Y.; Hishima, T.; Kashima, J.; Homma, S. High PD-L1 expression indicates poor prognosis of HIV-infected patients with non-small cell lung cancer. Cancer Immunol. Immunother. 2018, 67, 495–505. [Google Scholar] [CrossRef] [PubMed]
- Choschzick, M.; Gut, A.; Fink, D. PD-L1 receptor expression in vulvar carcinomas is HPV-independent. Virchows Arch. 2018, 473, 513–516. [Google Scholar] [CrossRef] [PubMed]
- Green, M.; Rodig, S.; Juszczynski, P.; Ouyang, J.; Sinha, P.; O’Donnell, E.; Neuberg, D.; Shipp, M. Constitutive AP-1 activity and EBV infection induce PD-L1 in Hodgkin lymphomas and posttransplant lymphoproliferative disorders: Implications for targeted therapy. Clin. Cancer Res. 2012, 18, 1611–1618. [Google Scholar] [CrossRef] [PubMed]
- Severa, M.; Giacomini, E.; Gafa, V.; Anastasiadou, E.; Rizzo, F.; Corazzari, M.; Romagnoli, A.; Trivedi, P.; Fimia, G.; Coccia, E. EBV stimulates TLR- and autophagy-dependent pathways and impairs maturation in plasmacytoid dendritic cells: Implications for viral immune escape. Eur. J. Immunol. 2013, 43, 147–158. [Google Scholar] [CrossRef] [PubMed]
- Fang, W.; Zhang, J.; Hong, S.; Zhan, J.; Chen, N.; Qin, T.; Tang, Y.; Zhang, Y.; Kang, S.; Zhou, T.; et al. EBV-driven LMP1 and IFN-γ up-regulate PD-L1 in nasopharyngeal carcinoma: Implications for oncotargeted therapy. Oncotarget 2014, 5, 12189–12202. [Google Scholar] [CrossRef]
- Outh-Gauer, S.; Alt, M.; Le Tourneau, C.; Augustin, J.; Broudin, C.; Gasne, C.; Denize, T.; Mirghani, H.; Fabre, E.; Scotte, F.; et al. Immunotherapy in head and neck cancers: A new challenge for immunologists, pathologists and clinicians. Cancer Treat. Rev. 2018, 665, 54–64. [Google Scholar] [CrossRef]
- Sun, C.; Lan, P.; Han, Q.; Huang, M.; Zhang, Z.; Xu, G.; Song, J.; Wang, J.; Wei, H.; Zhang, J.; et al. Oncofetal gene SALL4 reactivation by hepatitis B virus counteracts miR-200c in PD-L1-induced T cell exhaustion. Nat. Commun. 2018, 9, 1241. [Google Scholar] [CrossRef]
- Balsitis, S.; Gali, V.; Mason, P.; Chaniewski, S.; Levine, S.; Wichroski, M.; Feulner, M.; Song, Y.; Granaldi, K.; Loy, J.; et al. Safety and efficacy of anti-PD-L1 therapy in the woodchuck model of HBV infection. PLoS ONE 2018, 13, e0190058. [Google Scholar] [CrossRef]
- Park, C.; Cho, J.; Lee, J.; Kang, S.; An, J.; Choi, M.; Lee, J.; Sohn, T.; Bae, J.; Kim, S.; et al. Host immune response index in gastric cancer identified by comprehensive analyses of tumor immunity. Oncoimmunology 2017, 6, e1356150. [Google Scholar] [CrossRef] [PubMed]
- Fouad, H.; Raziky, M.; Aziz, R.; Sabry, D.; Aziz, G.; Ewais, M.; Sayed, A. Dendritic cell co-stimulatory and co-inhibitory markers in chronic HCV: An Egyptian study. World J. Gastroenterol. 2013, 19, 7711–7718. [Google Scholar] [CrossRef] [PubMed]
- Choi, Y.; Jin, N.; Kelly, F.; Sakthivel, S.; Yu, T. Elevation of Alanine Aminotransferase Activity Occurs after Activation of the Cell-Death Signaling Initiated by Pattern-Recognition Receptors but before Activation of Cytolytic Effectors in NK or CD8+ T Cells in the Liver During Acute HCV Infection. PLoS ONE 2016, 11, e0165533. [Google Scholar] [CrossRef] [PubMed]
- Ojiro, K.; Qu, X.; Cho, H.; Park, J.; Vuidepot, A.; Lissin, N.; Molloy, P.; Bennett, A.; Jakobsen, B.; Kaplan, D.; et al. Modulation of Hepatitis C Virus-Specific CD8 Effector T-Cell Function with Antiviral Effect in Infectious Hepatitis C Virus Coculture Model. J. Virol. 2017, 91, e02129-16. [Google Scholar] [CrossRef]
- Abdellatif, H.; Shiha, G. PD-L1 Expression on Circulating CD34 + Hematopoietic Stem Cells Closely Correlated with T-cell Apoptosis in Chronic Hepatitis C Infected Patients. Int. J. Stem. Cells 2018, 11, 78–86. [Google Scholar] [CrossRef]
- Domblides, C.; Antoine, M.; Hamard, C.; Rabbe, N.; Rodenas, A.; Vieira, T.; Crequit, P.; Cadranel, J.; Lavolé, A.; Wislez, M. Nonsmall cell lung cancer from HIV-infected patients expressed programmed cell death-ligand 1 with marked inflammatory infiltrates. AIDS 2018, 32, 461–468. [Google Scholar]
- Muthumani, K.; Shedlock, D.; Choo, D.; Fagone, P.; Kawalekar, O.; Goodman, J.; Bian, C.; Ramanathan, A.; Atman, P.; Tebas, P.; et al. HIV-mediated phosphatidylinositol 3-kinase/serine-threonine kinase activation in APCs leads to programmed death-1 ligand upregulation and suppression of HIV-specific CD8 T cells. J. Immunol. 2011, 187, 29322–29343. [Google Scholar] [CrossRef]
- Meier, A.; Bagchi, A.; Sidhu, H.; Alter, G.; Suscovich, T.; Kavanagh, D.; Streeck, H.; Brockman, M.; LeGall, S.; Hellman, J.; et al. Upregulation of PD-L1 on monocytes and dendritic cells by HIV-1 derived TLR ligands. AIDS 2008, 22, 655–658. [Google Scholar] [CrossRef]
- Planès, R.; BenMohamed, L.; Leghmari, K.; Delobel, P.; Izopet, J.; Bahraoui, E. HIV-1 Tat protein induces PD-L1 (B7-H1) expression on dendritic cells through tumor necrosis factor alpha- and toll-like receptor 4-mediated mechanisms. J. Virol. 2014, 88, 6672–6689. [Google Scholar] [CrossRef]
- Hong, A.; Vilain, R.; Romanes, S.; Yang, J.; Smith, E.; Jones, D.; Scolyer, R.; Lee, C.; Zhang, M.; Rose, B. PD-L1 expression in tonsillar cancer is associated with human papillomavirus positivity and improved survival: Implications for anti-PD1 clinical trials. Oncotarget 2016, 7, 77010–77020. [Google Scholar] [CrossRef]
- Lyford-Pike, S.; Peng, S.; Young, G.; Taube, J.; Westra, W.; Akpeng, B.; Bruno, T.; Richmon, J.; Wang, H.; Bishop, J.; et al. Evidence for a role of the PD-1:PD-L1 pathway in immune resistance of HPV-associated head and neck squamous cell carcinoma. Cancer Res. 2013, 73, 1733–1741. [Google Scholar] [CrossRef] [PubMed]
- Yang, W.; Song, Y.; Lu, Y.; Sun, J.; Wang, H. Increased expression of programmed death (PD)-1 and its ligand PD-L1 correlates with impaired cell-mediated immunity in high-risk human papillomavirus-related cervical intraepithelial neoplasia. Immunology 2013, 139, 513–522. [Google Scholar] [CrossRef] [PubMed]
- Lin, P.; Cheng, Y.; Wu, D.; Huang, Y.; Lin, H.; Chen, C.; Lee, H. A combination of anti-PD-L1 mAb plus Lm-LLO-E6 vaccine efficiently suppresses tumor growth and metastasis in HPV-infected cancers. Cancer Med. 2017, 6, 2052–2062. [Google Scholar] [CrossRef] [PubMed]
- Lipson, E.; Vincent, J.; Loyo, M.; Kagohara, L.; Luber, B.; Wang, H.; Xu, H.; Nayar, S.; Wang, T.; Sidransky, D.; et al. PD-L1 expression in the Merkel cell carcinoma microenvironment: Association with inflammation, Merkel cell polyomavirus and overall survival. Cancer Immunol. Res. 2013, 1, 54–63. [Google Scholar] [CrossRef] [PubMed]
- Ikebuchi, R.; Konnai, S.; Shirai, T.; Sunden, Y.; Murata, S.; Onuma, M.; Ohashi, K. Increase of cells expressing PD-L1 in bovine leukemia virus infection and enhancement of anti-viral immune responses in vitro via PD-L1 blockade. Vet. Res. 2011, 42, 103. [Google Scholar] [CrossRef]
- Host, K.; Jacobs, S.; West, J.; Zhang, Z.; Costantini, L.; Stopford, C.; Dittmer, D.; Damania, B. Kaposi’s Sarcoma-Associated Herpesvirus Increases PD-L1 and Proinflammatory Cytokine Expression in Human Monocytes. MBio 2017, 8, e00917-17. [Google Scholar] [CrossRef]
- Good-Jacobson, K.; Szumilas, C.; Chen, L.; Sharpe, A.; Tomayko, M.; Shlomchik, M. PD-1 regulates germinal center B cell survival and the formation and affinity of long-lived plasma cells. Nat. Immunol. 2010, 11, 535–542. [Google Scholar] [CrossRef]
- Lino, A.; Dang, V.; Lampropoulou, V.; Welle, A.; Joedicke, J.; Pohar, J.; Simon, Q.; Thalmensi, J.; Baures, A.; Flühler, V.; et al. LAG-3 Inhibitory Receptor Expression Identifies Immunosuppressive Natural Regulatory Plasma Cells. Immunity 2018, 49, 1. [Google Scholar] [CrossRef]
- Cain, D.; Cidlowski, J. Immune regulation by glucocorticoids. Nat. Rev. Immunol. 2017, 17, 233–247. [Google Scholar] [CrossRef]
- Franco, L.; Gadkari, M.; Howe, K.; Sun, J.; Kardava, L.; Kumar, P.; Kumari, S.; Hu, Z.; Fraser, I.; Moir, S.; et al. Immune regulation by glucocorticoids can be linked to cell type-dependent transcriptional responses. J. Exp. Med. 2019, 216, 384–406. [Google Scholar] [CrossRef]
- Obradović, M.; Hamelin, B.; Manevski, N.; Couto, J.; Sethi, A.; Coissieux, M.; Münst, S.; Okamoto, R.; Kohler, H.; Schmidt, A.; et al. Glucocorticoids promote breast cancer metastasis. Nature 2019, 567, 540–544. [Google Scholar] [CrossRef] [PubMed]
- Torino, F.; Barnabei, A.; Paragliola, R.; Marchetti, P.; Salvatori, R.; Corsello, S. Endocrine side-effects of anti-cancer drugs: mAbs and pituitary dysfunction: Clinical evidence and pathogenic hypotheses. Eur. J. Endocrinol. 2013, 169, R153–R164. [Google Scholar] [CrossRef] [PubMed]
- Sznol, M.; Postow, M.; Davies, M.; Pavlick, A.; Plimack, E.; Shaheen, M.; Veloski, C.; Robert, C. Endocrine-related adverse events associated with immune checkpoint blockade and expert insights on their management. Cancer Treat. Rev. 2017, 58, 70–76. [Google Scholar] [CrossRef] [PubMed]
- Kametani, Y.; Miyamoto, A.; Seki, T.; Ito, R.; Habu, S.; Tokuda, Y. The significance of humanized mouse models for the evaluation of the humoral immune response against cancer vaccines. Pers. Med. Univ. 2018, 7, 13–18. [Google Scholar] [CrossRef]
- Chen, Q.; Wang, J.; Liu, W.; Zhao, Y. Cancer Immunotherapies and Humanized Mouse Drug Testing Platforms. Transl. Oncol. 2019, 12, 987–995. [Google Scholar] [CrossRef]
- Ukai, H.; Sumiyama, K.; Ueda, H. Next-generation human genetics for organism-level systems biology. Curr. Opin. Biotechnol. 2019, 58, 137–145. [Google Scholar] [CrossRef]
- Ito, M.; Kobayashi, K.; Nakahata, T. NOD/Shi-scid IL2rgamma(null) (NOG) mice more appropriate for humanized mouse models. Curr. Top. Microbiol. Immunol. 2008, 324, 53–76. [Google Scholar]
- Yajima, M.I.K. Nakagawa A, Watanabe S, Terashima K, Nakamura H, Ito M, Shimizu N, Honda M, Yamamoto N, Fujiwara S, A new humanized mouse model of Epstein-Barr virus infection that reproduces persistent infection, lymphoproliferative disorder, and cell-mediated and humoral immune responses. J. Infect. Dis. 2008, 198, 673–682. [Google Scholar]
- Brehm, M.; Wiles, M.; Greiner, D.; Shultz, L. Generation of improved humanized mouse models for human infectious diseases. J. Immunol. Methods 2014, 410, 3–17. [Google Scholar] [CrossRef]
- Hasgur, S.; Aryee, K.; Shultz, L.; Greiner, D.; Brehm, M. Generation of Immunodeficient Mice Bearing Human Immune Systems by the Engraftment of Hematopoietic Stem Cells. Methods Mol. Biol. 2016, 1438, 67–78. [Google Scholar]
- Willinger, T.; Rongvaux, A.; Takizawa, H.; Yancopoulos, G.; Valenzuela, D.; Murphy, A.; Auerbach, W.; Eynon, E.; Stevens, S.; Manz, M.; et al. Human IL-3/GM-CSF knock-in mice support human alveolar macrophage development and human immune responses in the lung. Proc. Natl. Acad. Sci. USA 2011, 108, 2390–2395. [Google Scholar] [CrossRef] [PubMed]
- Singh, M.; Singh, P.; Gaudray, G.; Musumeci, L.; Thielen, C.; Vaira, D.; Vandergeeten, C.; Delacroix, L.; Van Gulck, E.; Vanham, G.; et al. An improved protocol for efficient engraftment in NOD/LTSZ-SCIDIL-2Rγnull mice allows HIV replication and development of anti-HIV immune responses. PLoS ONE 2012, 7, e38491. [Google Scholar] [CrossRef] [PubMed]
- Ito, R.; Takahashi, T.; Katano, I.; Kawai, K.; Kamisako, T.; Ogura, T.; Ida-Tanaka, M.; Suemizu, H.; Nunomura, S.; Ra, C.; et al. Establishment of a human allergy model using human IL-3/GM-CSF-transgenic NOG mice. J. Immunol. 2013, 191, 2890–2899. [Google Scholar] [CrossRef] [PubMed]
- Goyama, S.; Wunderlich, M.; Mulloy, J. Xenograft models for normal and malignant stem cells. Blood 2015, 125, 2630–2640. [Google Scholar] [CrossRef]
- Villaudy, J.; Schotte, R.; Legrand, N.; Spits, H. Critical assessment of human antibody generation in humanized mouse models. J. Immunol. Methods 2014, 410, 18–27. [Google Scholar] [CrossRef]
- Ito, M.; Hiramatsu, H.; Kobayashi, K.; Suzue, K.; Kawahata, M.; Hioki, K.; Ueyama, Y.; Koyanagi, Y.; Sugamura, K.; Tsuji, K.; et al. NOD/SCID/gamma(c)(null) mouse: An excellent recipient mouse model for engagement of human cells. Blood 2002, 100, 3175–3182. [Google Scholar] [CrossRef]
- Shultz, L.; Ishikawa, F.; Greiner, D. Humanized mice in translational biomedical research. Nat. Rev. Immunol. 2007, 7, 118–130. [Google Scholar] [CrossRef]
- Shultz, L.D.; Lang, P.A.; Christianson, S.W.; Gott, B.; Lyons, B.; Umeda, S.; Leiter, E.; Hesselton, R.; Wagar, E.J.; Leif, J.H.; et al. NOD/LtSz-Rag1null mice: An immunodeficient and radioresistant model for engraftment of human hematolymphoid cells, HIV infection, and adoptive transfer of NOD mouse diabetogenic T cells. J. Immunol. 2000, 164, 2496–2507. [Google Scholar] [CrossRef]
- Matumura, T.; Kametani, Y.; Ando, K.; Hirano, Y.; Katano, I.; Ito, R.; Shiina, M.; Tsukmoto, H.; Saito, Y.; Tokuda, Y.; et al. Functional CD5+ B cells develop predominantly in the spleen of NOD/SCID/gcnull (NOG) mice transplanted either with human umbilical cord blood, bone marrow, or mobilized peripheral blood CD34+ cells. Exp. Hematol. 2003, 31, 789–797. [Google Scholar] [CrossRef]
- Watanabe, S.; Terashima, K.; Ohta, S.; Horibata, S.; Yajima, M.; Shiozawa, Y.; Dewan, M.; Yu, Z.; Ito, M.; Morio, T.; et al. Hematopoietic stem cell-engrafted NOD/SCID/IL2Rgamma null mice develop human lymphoid systems and induce long-lasting HIV-1 infection with specific humoral immune responses. Blood 2007, 109, 212–218. [Google Scholar] [CrossRef]
- Lepus, C.; Gibson, T.; Gerber, S.; Kawikova, I.; Szczepanik, M.; Hossain, J.; Ablamunits, V.; Kirkiles-Smith, N.; Herold, K.; Donis, R.; et al. Comparison of human fetal liver, umbilical cord blood, and adult blood hematopoietic stem cell engraftment in NOD-scid/gammac-/-, Balb/c-Rag1-/-gammac-/-, and C.B-17-scid/bg immunodeficient mice. Hum. Immunol. 2009, 70, 790–802. [Google Scholar] [CrossRef] [PubMed]
- Watanabe, Y.; Takahashi, T.; Okajima, A.; Shiokawa, M.; Ishii, N.; Katano, I.; Ito, R.; Ito, M.; Minegishi, M.; Minegishi, N.; et al. The analysis of the functions of human B and T cells in humanized NOD/shi-scid/gammac(null) (NOG) mice (hu-HSC NOG mice). Int Immunol. 2009, 21, 843–858. [Google Scholar] [CrossRef] [PubMed]
- Biswas, S.; Chan, G.H.; Sarkis, P.; Fikrig, E.; Zhu, Q.; Marasco, W. Humoral immune responses in humanized BLT mice immunized with West Nile virus and HIV-1 envelope proteins are largely mediated via human CD5+ B cells. Immunology 2011, 134, 419–433. [Google Scholar] [CrossRef] [PubMed]
- Kametani, Y.; Shiina, M.; Katano, I.; Ito, R.; Ando, K.; Toyama, K.; Tsukamoto, H.; Matsumura, T.; Saito, Y.; Ishikawa, D.; et al. Development of human-human hybridoma from anti-Her-2 peptide-producing B cells in immunized NOG mouse. Exp. Hematol. 2006, 34, 1240–1248. [Google Scholar] [CrossRef]
- Kametani, Y.; Shimada, S.; Mori, S.; Kojima, M.; Ohshima, S.; Kitaura, K.; Matsutani, T.; Okada, Y.; Yahata, T.; Ito, R.; et al. Antibody-secreting plasma cells with unique CD5+IgG+CD21lo phenotype developed in humanized NOG mice. Clin. Res. Trials 2016, 2, 164–173. [Google Scholar] [CrossRef]
- Kametani, Y.; Katano, I.; Miyamoto, A.; Kikuchi, Y.; Ito, R.; Muguruma, Y.; Tsuda, B.; Habu, S.; Tokuda, Y.; Ando, K.; et al. NOG-hIL-4-Tg, a new humanized mouse model for producing tumor antigen-specific IgG antibody by peptide vaccination. PLoS ONE 2017, 12, e0179239. [Google Scholar] [CrossRef]
- McCune, J. Development and applications of the SCID-hu mouse model. Semin. Immunol. 1996, 8, 187–196. [Google Scholar] [CrossRef]
- Aaberge, I.; Michaelsen, T.; Rolstad, A.; Groeng, E.; Solberg, P.; Løvik, M. SCID-Hu mice immunized with a pneumococcal vaccine produce specific human antibodies and show increased resistance to infection. Infect. Immunol. 1992, 60, 4146–4153. [Google Scholar]
- Suzuki, M.; Takahashi, T.; Katano, I.; Ito, R.; Ito, M.; Harigae, H.; Ishii, N.; Sugamura, K. Induction of human humoral immune responses in a novel HLA-DR-expressing transgenic NOD/Shi-scid/γcnull mouse. Int. Immunol. 2012, 24, 243–252. [Google Scholar] [CrossRef]
- Huang, J.; Li, X.; Coelho-dos-Reis, J.; Zhang, M.; Mitchell, R.; Nogueira, R.; Tsao, T.; Noe, A.; Ayala, R.; Sahi, V.; et al. Human immune system mice immunized with Plasmodium falciparum circumsporozoite protein induce protective human humoral immunity against malaria. J. Immunol. Methods 2015, 427, 42–50. [Google Scholar] [CrossRef]
- Williams, S.; Umemoto, T.; Kida, H.; Repasky, E.; Bankert, R. Engraftment of human peripheral blood leukocytes into severe combined immunodeficient mice results in the long term and dynamic production of human xenoreactive antibodies. J. Immunol. 1992, 149, 2830–2836. [Google Scholar] [PubMed]
- Aono, S.; Tatsumi, T.; Yoshioka, T.; Tawara, S.; Nishio, A.; Onishi, Y.; Fukutomi, K.; Nakabori, T.; Kodama, T.; Shigekawa, M.; et al. Immunological responses against hepatitis B virus in human peripheral blood mononuclear cell-engrafted mice. Biochem. Biophys Res. Commun. 2018, 503, 1457–1464. [Google Scholar] [CrossRef] [PubMed]
- McCune, J.; Namikawa, R.; Kaneshima, H.; Shultz, L.; Lieberman, M.; Weissman, I. The SCID-hu mouse: Murine model for the analysis of human hematolymphoid differentiaiton and function. Schience 1988, 241, 1632–1639. [Google Scholar] [CrossRef] [PubMed]
- Jaiswal, S.; Smith, K.; Ramirez, A.; Woda, M.; Pazoles, P.; Shultz, L.; Greiner, D.; Brehm, M.; Mathew, A. Dengue virus infection induces broadly cross-reactive human IgM antibodies that recognize intact virions in humanized BLT-NSG mice. Exp. Biol. Med. 2015, 240, 67–78. [Google Scholar] [CrossRef] [PubMed]
- Jangalwe, S.; Shultz, L.; Mathew, A.; MA, B. Improved B cell development in humanized NOD-scid IL2Rγnull mice transgenically expressing human stem cell factor, granulocyte-macrophage colony-stimulating factor and interleukin-3. Immunol. Inflamm. Dis. 2016, 4, 427–440. [Google Scholar] [CrossRef]
- Schmitt, K.; Charlins, P.; Veselinovic, M.; Kinner-Bibeau, L.; Hu, S.; Curlin, J.; Remling-Mulder, L.; Olson, K.; Aboellail, T.; Akkina, R. Zika viral infection and neutralizing human antibody response in a BLT humanized mouse model. Virology 2018, 515, 235–242. [Google Scholar] [CrossRef]
- Gawron, M.; Duval, M.; Carbone, C.; Jaiswal, S.; Wallace, A.; Martin, J.C.; Dauphin, A.; Brehm, M.; Greiner, D.; Shultz, L.; et al. Human Anti-HIV-1 gp120 Monoclonal Antibodies with Neutralizing Activity Cloned from Humanized Mice Infected with HIV-1. J. Immunol. 2019, 202, 799–804. [Google Scholar] [CrossRef]
- Srivastava, R.; Khan, A.; Spencer, D.; Vahed, H.; Lopes, P.; Thai, N.; Wang, C.; Pham, T.; Huang, J.; Scarfone, V.; et al. HLA-A02:01-restricted epitopes identified from the herpes simplex virus tegument protein VP11/12 preferentially recall polyfunctional effector memory CD8+ T cells from seropositive asymptomatic individuals and protect humanized HLA-A*02:01 transgenic mice against ocular herpes. J. Immunol. 2015, 194, 2232–2248. [Google Scholar]
- Najima, Y.; Tomizawa-Murasawa, M.; Saito, Y.; Watanabe, T.; Ono, R.; Ochi, T.; Suzuki, N.; Fujiwara, H.; Ohara, O.; Shultz, L.; et al. Induction of WT1-specific human CD8+ T cells from human HSCs in HLA class I Tg NOD/SCID/IL2rgKO mice. Blood 2016, 127, 722–734. [Google Scholar] [CrossRef]
- Jespersen, H.; Lindberg, M.; Donia, M.; Söderberg, E.; Andersen, R.; Keller, U.; Ny, L.; Svane, I.; Nilsson, L.; Nilsson, J. Clinical responses to adoptive T-cell transfer can be modeled in an autologous immune-humanized mouse model. Nat. Commun. 2017, 8, 707. [Google Scholar] [CrossRef]
- Meehan, T.; Conte, N.; Goldstein, T.; Inghirami, G.; Murakami, M.; Brabetz, S.; Gu, Z.; Wiser, J.; Dunn, P.; Begley, D.; et al. PDX-MI: Minimal Information for Patient-Derived Tumor Xenograft Models. Cancer Res. 2017, 77, e62–e66. [Google Scholar] [CrossRef] [PubMed]
- Okada, S.; Vaeteewoottacharn, K.; Kariya, R. Application of Highly Immunocompromised Mice for the Establishment of Patient-Derived Xenograft (PDX) Models. Cells 2019, 8, 889. [Google Scholar] [CrossRef] [PubMed]
- Shi, J.; Li, Y.; Jia, R.; Fan, X. The fidelity of cancer cells in PDX models: Characteristics, mechanism and clinical significance. Int. J. Cancer 2019. [Google Scholar] [CrossRef] [PubMed]
- Marangoni, E.; Poupon, M. Patient-derived tumour xenografts as models for breast cancer drug development. Curr. Opin. Oncol. 2014, 26, 556–561. [Google Scholar] [CrossRef]
- Ashizawa, T.; Iizuka, A.; Nonomura, C.; Kondou, R.; Maeda, C.; Miyata, H.; Sugino, T.; Mitsuya, K.; Hayashi, N.; Nakasu, Y.; et al. Antitumor Effect of Programmed Death-1 (PD-1) Blockade in Humanized the NOG-MHC Double Knockout Mouse. Clin. Cancer Res. 2017, 23, 149–158. [Google Scholar] [CrossRef]
- Joo, S.Y.; Chung, Y.S.; Choi, B.; Kim, M.; Kim, J.H.; Jun, T.G.; Chang, J.; Sprent, J.; Surh, C.D.; Joh, J.W.; et al. Systemic human T cell developmental processes in humanized mice cotransplanted with human fetal thymus/liver tissue and hematopoietic stem cells. Transplantation 2012, 94, 1095–1102. [Google Scholar] [CrossRef]
- Ito, R.; Katano, I.; Kawai, K.; Yagoto, M.; Takahashi, T.; Ka, Y.; Ogura, T.; Takahashi, R.; Ito, M. A Novel Xenogeneic Graft-Versus-Host Disease Model for Investigating the Pathological Role of Human CD4+ or CD8+ T Cells Using Immunodeficient NOG Mice. Am. J. Transplant. 2017, 17, 1216–1228. [Google Scholar] [CrossRef]
- Seki, T.; Miyamoto, A.; Ohshima, S.; Ohno, Y.; Yasuda, A.; Tokuda, Y.; Ando, K.; Kametani, Y. Expression of glucocorticoid receptor shows negative correlation with human B-cell engraftment in PBMC-transplanted NOGhIL-4-Tg mice. Biosci. Trends 2018, 12, 247–256. [Google Scholar] [CrossRef]
| Mouse Strain. | Transplanted Tissues | Antigen | Isotype | Reference | |
|---|---|---|---|---|---|
| SCID-Hu | SCID | human fetal liver and thymic fragments under kidney capsule | pneumococcal vaccine | IgG | McCune JM 1988 [117], Aaberge IS et al., 1992 [118] |
| Hu-HSC | NOG | HSC(CB/MPB/BM) i.v. | DNP-KLH/CH401MAP/TSST-1 | IgM | Matsumura T et al., 2003 [109], Kametani Y et al., 2006 [114] |
| NSG; Balb/c-Rag1(-/-) gammac(-/-); C.B-17-scid/bg | HSC(CB/MPB/HFL) i.v. | KLH/inactivated H5N1 influenza virus | IgM, IgG | Lepus CM et al., 2009 [111] | |
| NOG | CD34 + HSC i.v. | OVA | Igs | Yajima M et al., 2008 [98], Watanabe Y et al., 2009 [112] | |
| NSG | human CD34 + HSC i.v. | OVA, HIV | IgM, IgG | Wtanabe S et al., 2007 [110], Singh M et al., 2012 [102] | |
| NOG-HLA-DR4/Ab KO | human CD34 + HSC i.v. | OVA | IgM, IgG | Suzuki M et al., 2012 [119] | |
| NSG-HIS-CD4/B | human CD34 + HSC i.v. | Plasmodium falciparum, circumsporo-zoite (PFCS) protein | IgG | Huang J et al., 2015 [120] | |
| Hu-PBL | SCID | human PBMC i.v. | xenograft | IgM, IgG | Williams S et al., 1992 [121] |
| NOG-IL-4-Tg | human PBMC i.v. | KLH/CH401MAP | IgG | Kametani Y et al., 2017 [116] | |
| DKO-NOG | human PBMC i.v. | human Liver xenograft, | Igs | Aono S et al. 2018 [122] | |
| BLT | SCID | human fetal liver and thymic fragments under kidney capsule with autologous CD34 + HSC | IgG | McCune JM et al., 1988 [123], Aaberge IS et al., 1992 [118] | |
| NOD-SCID | human fetal liver and thymic fragments under kidney capsule with autologous CD34 + HSC | HIV-1, WNV envelope protein | IgM, IgG | Biswas et al., 2011 [113] | |
| NSG | human fetal liver and thymic fragments under kidney capsule with autologous CD34 + HSC | pneumococcal vaccine, Dengue virus infection, Zika virus, HIV -1 gp120 | IgM, IgG, IgA | Jaiswal S et al., 2015 [124], Jangalwe S et al., 2016 [125], Schmitt K et al., 2018 [126], Gawron MA et al., 2019 [127] | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kametani, Y.; Ohno, Y.; Ohshima, S.; Tsuda, B.; Yasuda, A.; Seki, T.; Ito, R.; Tokuda, Y. Humanized Mice as an Effective Evaluation System for Peptide Vaccines and Immune Checkpoint Inhibitors. Int. J. Mol. Sci. 2019, 20, 6337. https://doi.org/10.3390/ijms20246337
Kametani Y, Ohno Y, Ohshima S, Tsuda B, Yasuda A, Seki T, Ito R, Tokuda Y. Humanized Mice as an Effective Evaluation System for Peptide Vaccines and Immune Checkpoint Inhibitors. International Journal of Molecular Sciences. 2019; 20(24):6337. https://doi.org/10.3390/ijms20246337
Chicago/Turabian StyleKametani, Yoshie, Yusuke Ohno, Shino Ohshima, Banri Tsuda, Atsushi Yasuda, Toshiro Seki, Ryoji Ito, and Yutaka Tokuda. 2019. "Humanized Mice as an Effective Evaluation System for Peptide Vaccines and Immune Checkpoint Inhibitors" International Journal of Molecular Sciences 20, no. 24: 6337. https://doi.org/10.3390/ijms20246337
APA StyleKametani, Y., Ohno, Y., Ohshima, S., Tsuda, B., Yasuda, A., Seki, T., Ito, R., & Tokuda, Y. (2019). Humanized Mice as an Effective Evaluation System for Peptide Vaccines and Immune Checkpoint Inhibitors. International Journal of Molecular Sciences, 20(24), 6337. https://doi.org/10.3390/ijms20246337





