Sponges of Carboxymethyl Chitosan Grafted with Collagen Peptides for Wound Healing
Abstract
1. Introduction
2. Results and Discussion
2.1. Amino Acid Composition of COP
2.2. Preparation of CMC–COP Sponges
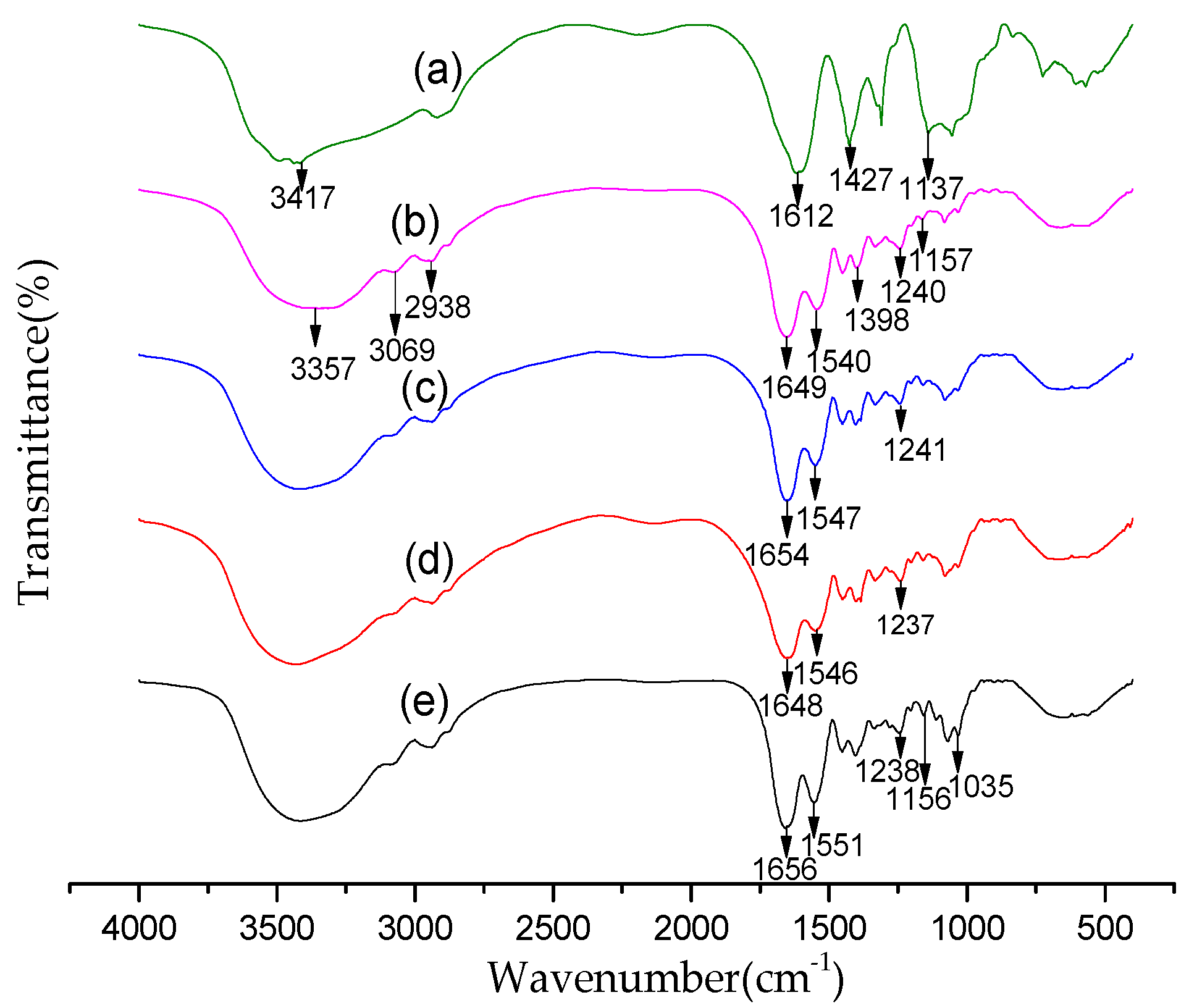
2.3. FT-IR Analysis
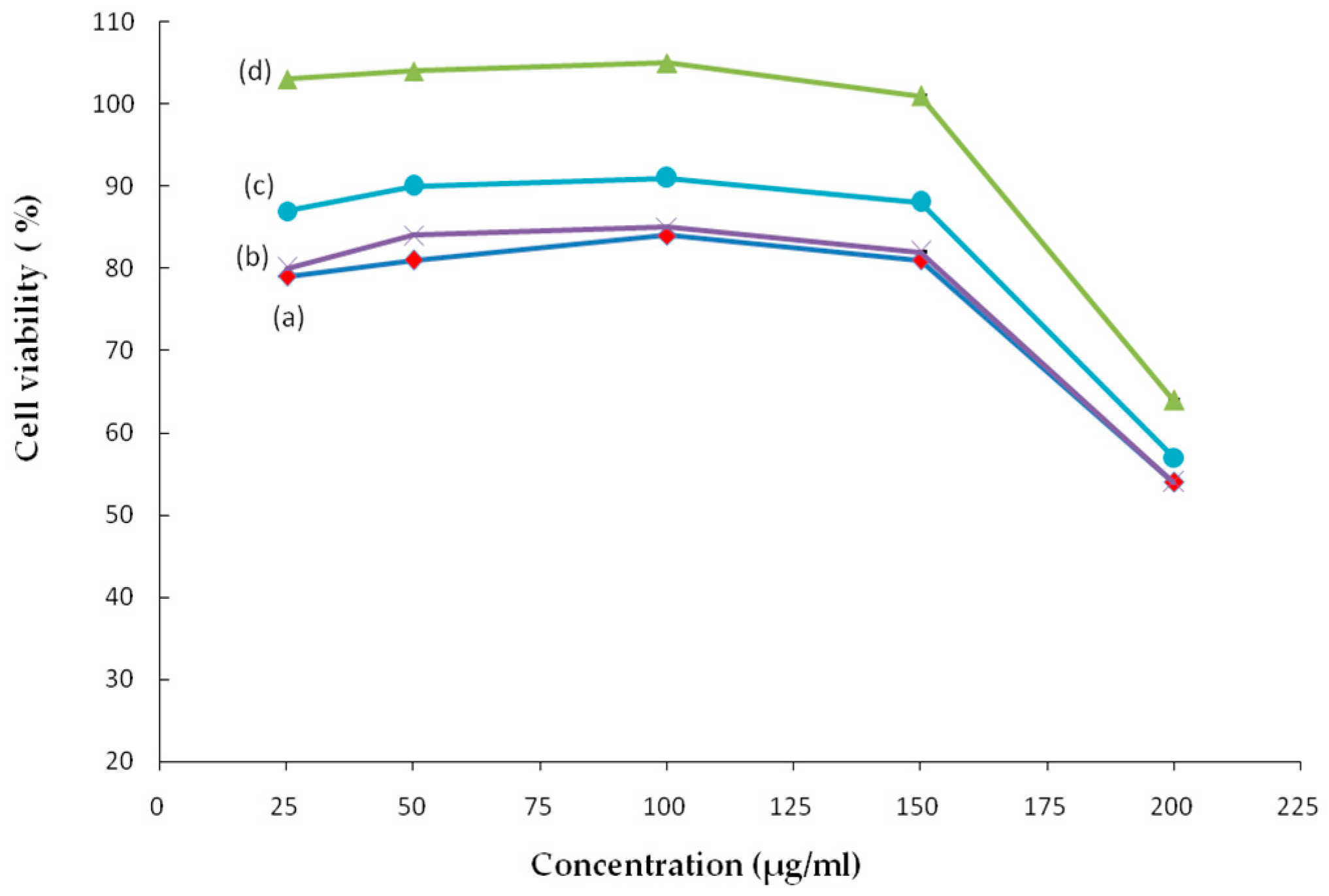
2.4. Evaluation of Cell Viability
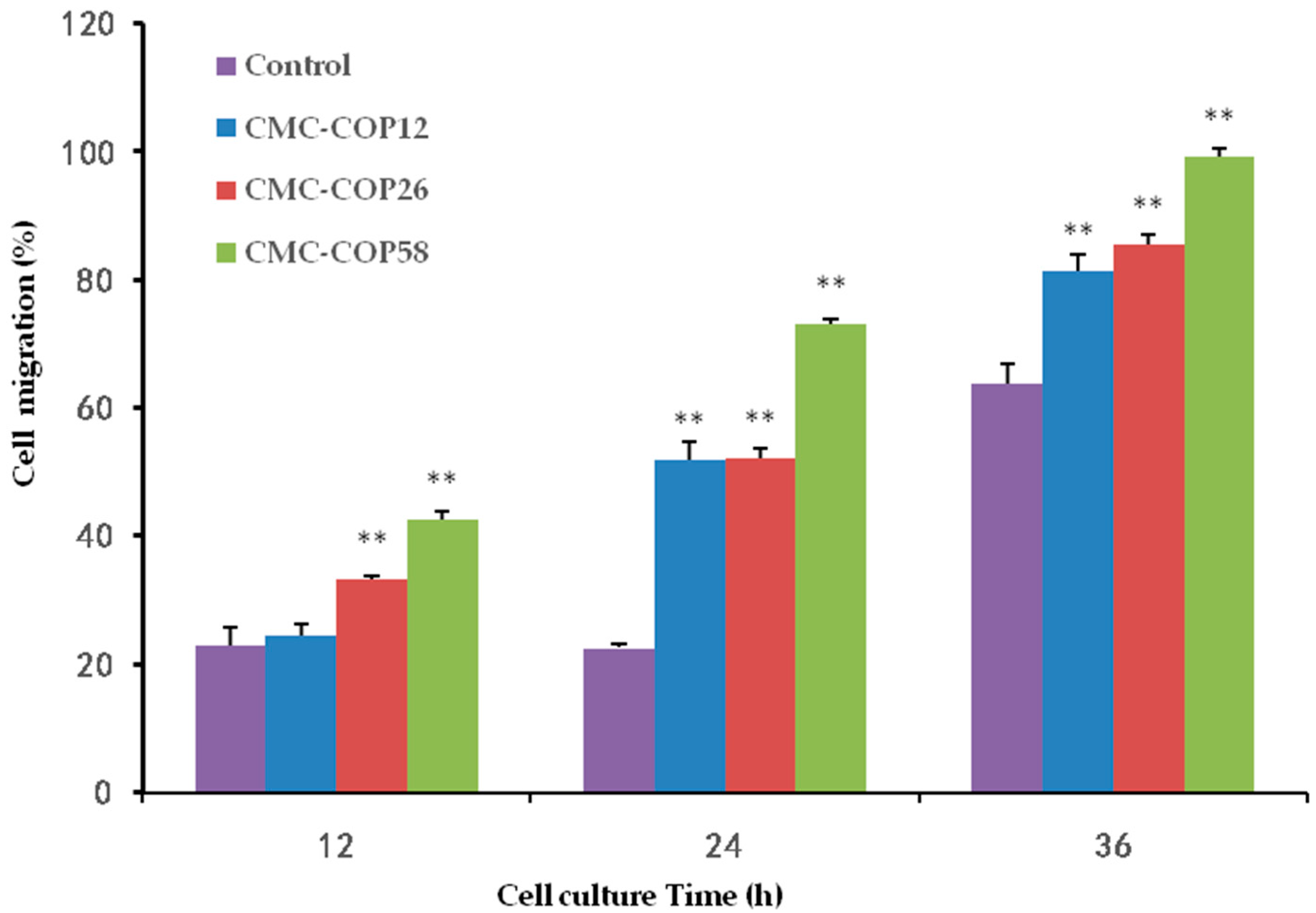
2.5. CMC–COP Synergizes the Migration of L929 Cells
2.6. Animal Scald Experiment
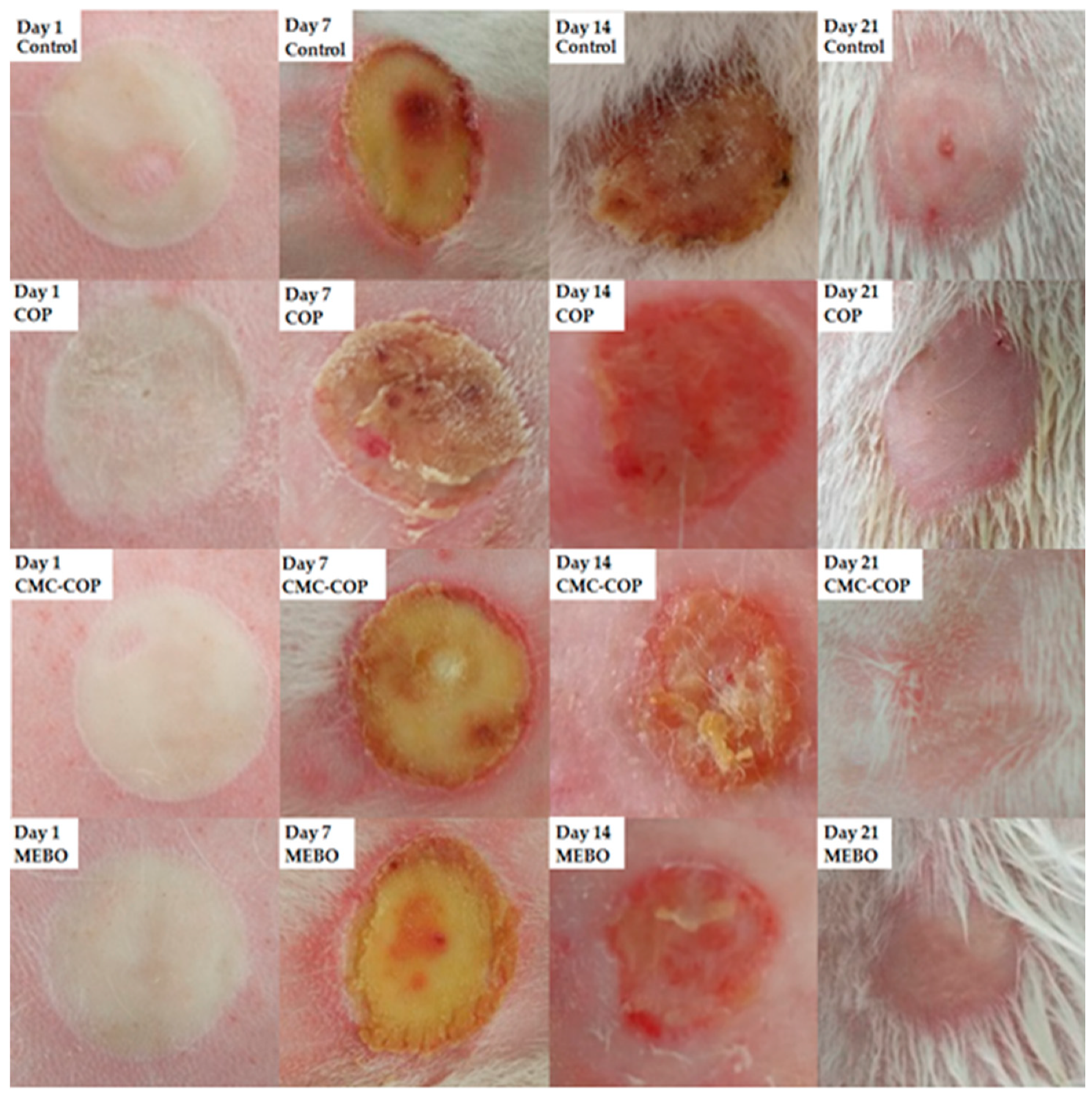
2.6.1. Macroscopic Analysis of Wounds
2.6.2. Wound Healing Rate
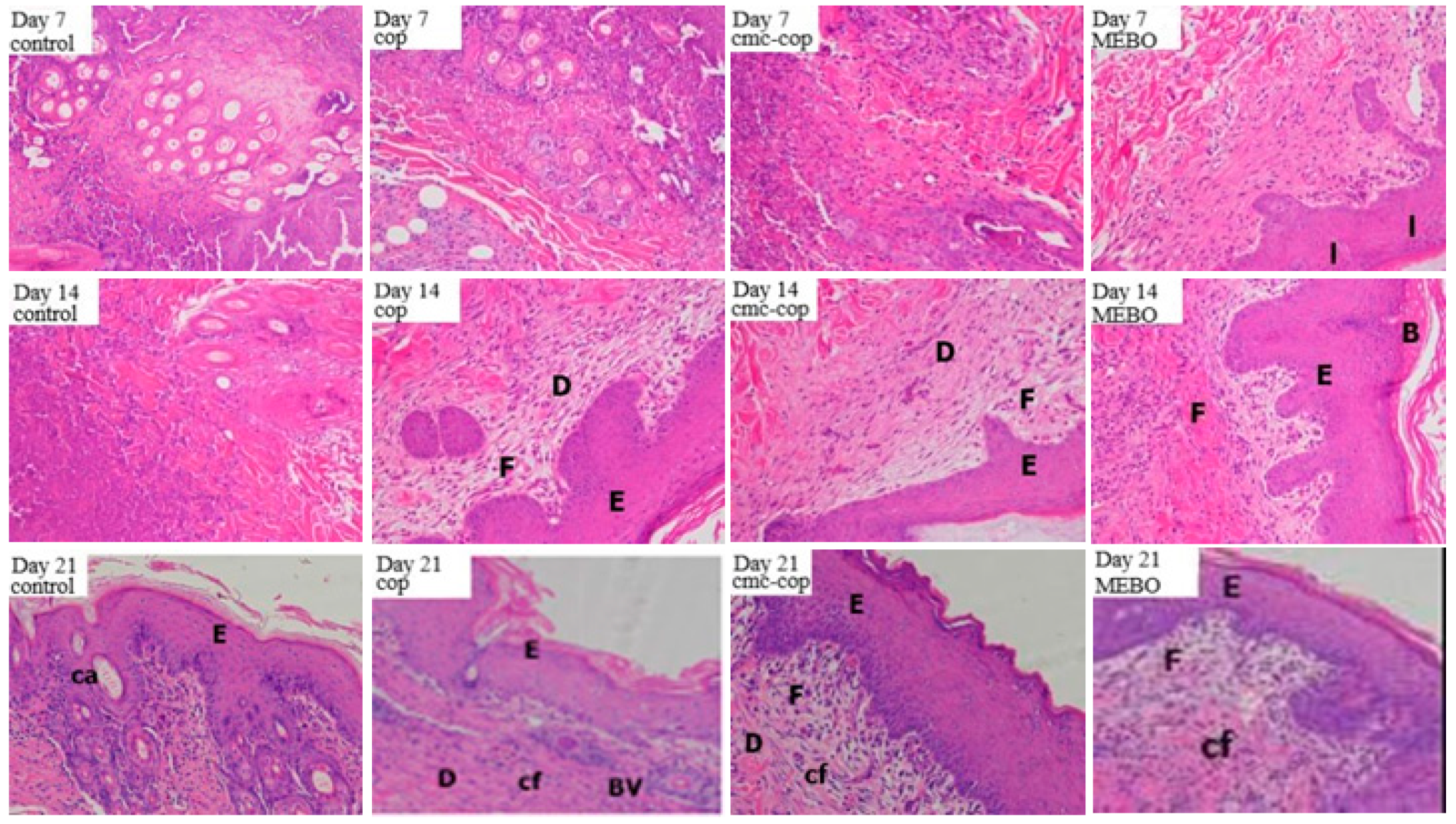
2.6.3. Histological Evaluation
3. Materials and Methods
3.1. Materials
3.2. Preparation of the CMC–COP
3.3. Determination of the Degree of Substitution (DS) of the CMC–COP
3.4. Appearance of CMC–COP
3.5. FTIR Analysis
3.6. Cell Viability Assay
3.7. In Vitro Scratch Wound Healing Assay
3.8. Wound Healing Assay
3.8.1. Animals
3.8.2. Burn Model
3.8.3. Macroscopic Evaluation of Burn Wounds in Rabbits
3.8.4. Histological Evaluation of Burn Wounds in Rabbits
3.9. Statistical Analysis
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Khor, E.; Lim, L.Y. Implantable applications of chitin and chitosan. Biomaterials 2003, 24, 2339–2349. [Google Scholar] [CrossRef]
- Upadhyaya, L.; Singh, J.; Agarwal, V.; Tewari, R.P. Biomedical applications of carboxymethyl chitosans. Carbohyd. Polym. 2013, 91, 452–466. [Google Scholar] [CrossRef] [PubMed]
- Chen, X.G.; Park, H.J. Chemical characteristics of o-carboxymethyl chitosans related to the preparation conditions. Carbohyd. Polym. 2003, 53, 355–359. [Google Scholar] [CrossRef]
- Chen, L.Y.; Tian, Z.G.; Du, Y.M. Synthesis and pH sensitivity of carboxymethyl chitosan-based polyam- pholyte hydrogels for protein carrier matrices. Biomaterials 2003, 25, 3725–3732. [Google Scholar] [CrossRef] [PubMed]
- Zhu, X.; Chian, K.S.; Chanpark, M.B.; Lee, S.T. Effect of argon-plasma treatment on proliferation of human-skin-derived fibroblast on chitosan membrane in vitro. J. Biomed. Mater. Res. A 2005, 73, 264. [Google Scholar] [CrossRef] [PubMed]
- Chen, X.G.; Wang, Z.; Liu, W.S.; Park, H.J. The effect of carboxymethyl-chitosan on proliferation and collagen secretion of normal and keloid skin fibroblasts. Biomaterials 2002, 23, 4609–4614. [Google Scholar] [CrossRef]
- Lu, G.; Kong, L.; Sheng, B.; Wang, G.; Gong, Y.; Zhang, X. Degradation of covalently cross-linked carboxymethyl chitosan and its potential application for peripheral nerve regeneration. Eur. Polym. J. 2007, 43, 3807–3818. [Google Scholar] [CrossRef]
- Min, S.K.; Lee, S.C.; Hong, S.D.; Chung, C.P.; Park, W.H.; Min, B.M. The effect of a laminin-5-derived peptide coated onto chitin microfibers on re-epithelialization in early-stage wound healing. Biomaterials 2010, 31, 4725–4730. [Google Scholar] [CrossRef]
- Liu, X.Y.; Gohi, B.F.; Zeng, H.Y.; Liao, M.C.; Sun, J.W. Effect of collagen peptides-carboxymethyl chitosan microspheres on ultraviolet-induced damages. Mater. Express 2015, 5, 497–504. [Google Scholar] [CrossRef]
- Ruszczak, Z. Effect of collagen matrices on dermal wound healing. Adv. Drug Deliv. Rev. 2003, 55, 1595–1611. [Google Scholar] [CrossRef]
- Ramshaw, J.A.M.; Peng, Y.Y.; Glattauer, V.; Werkmeister, J.A. Collagens as biomaterials. J. Mater. Sci.-Mater. Med. 2009, 20, 3–8. [Google Scholar] [CrossRef] [PubMed]
- Liu, C.; Liu, X.; Xue, Y. Hydrolyzed tilapia fish collagenmodulates the biological behavior of macrophages under inflammatory conditions. RSC Adv. 2015, 5, 30727–30736. [Google Scholar] [CrossRef]
- Mahboob, S. Isolation and characterization of collagen from fish waste material skin, scales and fins of Catla catla and cirrhinus mrigala. J. Food Sci. Technol. 2015, 52, 4296–4305. [Google Scholar] [CrossRef] [PubMed]
- Anitha, A.; Sowmya, S.; Kumar, P.T.S.; Deepthi, S.; Chennazhi, K.P.; Ehrlich, H. Chitin and chitosan in selected biomedical applications. Prog. Polym. Sci. 2014, 39, 1644–1667. [Google Scholar] [CrossRef]
- Salsas, E.R.; Stultz, C.M. The molecular mechanics of collagen degradation: Implications for human disease. Exp. Mech. 2009, 49, 65–77. [Google Scholar] [CrossRef]
- Harnedy, P.A.; Fitzgerald, R.J. Bioactive peptides from marine processing waste and shellfish: A review. J. Funct. Foods 2012, 4, 6–24. [Google Scholar]
- Sun, X.; Chai, Y.; Wang, Q.; Liu, H.; Wang, S.; Xiao, J. A natural interruption displays higher global stability and local conformational flexibility than a similar Gly mutation sequence in collagen mimic peptides. Biochemistry 2015, 54, 6106–6113. [Google Scholar] [CrossRef] [PubMed]
- Bin, W.; Yu, M.W.; Chang, F.C.; Hong, Y.L.; Shang, G.D.; Jian, Y.M. Isolation and characterization of collagen and antioxidant collagen peptides from scales of croceine croaker (pseudosciaena crocea). Mar. Drugs 2013, 11, 4641–4661. [Google Scholar]
- Kim, S.K.; Kim, Y.T.; Byun, H.G.; Nam, K.S.; Joo, D.S.; Shahidi, F. Isolation and characterization of antioxidative peptides from gelatin hydrolysate of alaska Pollack skin. J. Agric. Food Chem. 2001, 49, 1984–1989. [Google Scholar] [CrossRef] [PubMed]
- Wissink, M.J.; Beernink, R.; Pieper, J.S. Immobilization of Heparin to EDC/NHS-crosslinked Collagen. Characterization and in vitro Evaluation. Biomaterials 2001, 22, 151–163. [Google Scholar] [CrossRef]
- Tsai, S.P.; Hsieh, C.Y.; Hsieh, C.Y.; Wang, D.M.; Huang, L.L.H.; Hsieh, H.J. Preparation and Cell Compatibility Evaluation of Chitosan/Collagen Composite Scaffolds Using Amino Acids as Crosslinking Bridges. J. Appl. Polym. Sci. 2007, 105, 1774–1785. [Google Scholar] [CrossRef]
- Ikeda, T.; Ikeda, K.; Yamamoto, K.; Ishizaki, H.; Yoshizawa, Y.; Yanagiguchi, K. Fabrication and characteristics of chitosan sponge as a tissue engineering scaffold. BioMed. Res. Int. 2014. [Google Scholar] [CrossRef] [PubMed]
- Fan, L.; Wu, H.; Cao, M.; Zhou, X.; Peng, M.; Xie, W. Enzymatic synthesis of collagen peptide– carboxymethylated chitosan copolymer and its characterization. React. Funct. Polym. 2014, 76, 26–31. [Google Scholar] [CrossRef]
- Yang, H.; Yang, S.; Kong, J.; Dong, A.; Yu, S. Obtaining information about protein secondary structures in aqueous solution using fourier transform ir spectroscopy. Nat. Protoc. 2015, 10, 382–396. [Google Scholar] [CrossRef] [PubMed]
- Mohajer, S.; Rezaei, M.; Hosseini, S.F. Physico-chemical and microstructural properties of fish gelatin/agar bio-based blend films. Carbohyd. Polym. 2017, 157, 784–793. [Google Scholar] [CrossRef] [PubMed]
- Li, Q.; Tan, W.; Zhang, C.; Gu, G.; Guo, Z. Synthesis of water soluble chitosan derivatives with halogeno-1,2,3-triazole and their antifungal activity. Int. J. Biol. Macromol. 2016, 91, 623–629. [Google Scholar] [CrossRef] [PubMed]
- Saito, M.; Kiyose, C.; Higuchi, T. Effect of collagen hydrolysatesfrom salmon and trout skins on the lipid profile in rats. J. Agric. Food Chem. 2009, 57, 10477–10482. [Google Scholar] [CrossRef] [PubMed]
- Lloyd, L.L.; Kennedy, J.F.; Methacanon, P.; Paterson, M.; Knill, C.J. Carbohydrate polymers as wound management aids. Carbohyd. Polym. 1998, 37, 315–322. [Google Scholar] [CrossRef]
- Sun, L.P.; Du, Y.M.; Shi, X.W.; Chen, X.; Yang, J.H.; Xu, Y.M. A new approach to chemically modified carboxymethyl chitosan and study of its moisture-absorption and moisture-retention abilities. J. Appl. Polym. Sci. 2006, 102, 1303–1309. [Google Scholar] [CrossRef]
- Chen, R.; Wang, G.; Chen, C. Development of N,O (carboxymethyl) chitosan/collagen matrixes as a wound dressing. Biomacromolecules 2006, 7, 1058–1064. [Google Scholar] [CrossRef] [PubMed]
- Jayakumar, R.; Prabaharan, M.; Nair, S.V.; Tamura, H. Novel chitin and chitosan nanofibers in biomedical applications. Biotechnol. Adv. 2010, 28, 142–150. [Google Scholar] [CrossRef] [PubMed]
- Hu, Z.; Yang, P.; Zhou, C.X.; Li, S.D.; Hong, P.Z. Marine Collagen Peptides from the Skin of NileTilapia (Oreochromisniloticus): Characterization and Wound Healing Evaluation. Mar. Drugs 2017, 15, 102. [Google Scholar] [CrossRef] [PubMed]
- Yamada, S.; Yamamoto, K.; Ikeda, T.; Yanagiguchi, K.; Hayashi, Y. Potency of fish collagen as a scaffold for regenerative medicine. Biomed. Res. Int. 2014. [Google Scholar] [CrossRef] [PubMed]
- Mosmann, T. Rapid colorimetric assay for cellular growth and Survival:application to proliferation and cytoxicityassays. J. Immunol. Methods 1983, 65, 55–63. [Google Scholar] [CrossRef]



| NO. | Amino Acid | Content (g/100 g) |
|---|---|---|
| 1 | ASP | 5.46 |
| 2 | THR | 2.84 |
| 3 | SER | 3.61 |
| 4 | GLU | 10.7 |
| 5 | GLY | 22.1 |
| 6 | ALA | 9.77 |
| 7 | VAL | 2.47 |
| 8 | MET | 1.75 |
| 9 | ILEl | 1.35 |
| 10 | LEU | 2.68 |
| 11 | TYR | 0.71 |
| 12 | PHE | 1.68 |
| 13 | HIS | 0.94 |
| 14 | LYS | 3.31 |
| 15 | ARG | 6.94 |
| 16 | PRO | 11.3 |
| 17 | Hyp | 11.85 |
| Free amino acid | 0.54 | |
| Total | 100 |
| Group | Day 3 | Day 5 | Day 7 | Day 14 | Day 21 |
|---|---|---|---|---|---|
| Control | −1.53 ± 0.55 | 3.56 ± 1.80 | 8.90 ± 1.03 | 35.47 ± 1.77 | 89.42 ± 1.96 |
| COP | −0.73 ± 0.61 | 7.86 ± 1.88 | 13.17 ± 0.92 ** | 46.29 ± 0.84 ** | 90.88 ± 0.22 |
| CMC–COP | 1.71 ± 0.53 | 9.82 ± 1.72 | 19.59 ± 0.78 ** | 66.97 ± 1.31 ** | 99.93 ± 0.15 |
| MEBO | 1.76 ± 0.42 | 9.10 ± 1.18 | 24.16 ± 1.18 ** | 72.65 ± 0.57 ** | 99.97 ± 0.07 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cheng, Y.; Hu, Z.; Zhao, Y.; Zou, Z.; Lu, S.; Zhang, B.; Li, S. Sponges of Carboxymethyl Chitosan Grafted with Collagen Peptides for Wound Healing. Int. J. Mol. Sci. 2019, 20, 3890. https://doi.org/10.3390/ijms20163890
Cheng Y, Hu Z, Zhao Y, Zou Z, Lu S, Zhang B, Li S. Sponges of Carboxymethyl Chitosan Grafted with Collagen Peptides for Wound Healing. International Journal of Molecular Sciences. 2019; 20(16):3890. https://doi.org/10.3390/ijms20163890
Chicago/Turabian StyleCheng, Yu, Zhang Hu, Yuntao Zhao, Zuhao Zou, Sitong Lu, Bijun Zhang, and Sidong Li. 2019. "Sponges of Carboxymethyl Chitosan Grafted with Collagen Peptides for Wound Healing" International Journal of Molecular Sciences 20, no. 16: 3890. https://doi.org/10.3390/ijms20163890
APA StyleCheng, Y., Hu, Z., Zhao, Y., Zou, Z., Lu, S., Zhang, B., & Li, S. (2019). Sponges of Carboxymethyl Chitosan Grafted with Collagen Peptides for Wound Healing. International Journal of Molecular Sciences, 20(16), 3890. https://doi.org/10.3390/ijms20163890





